Parents’ Perception of Food Insecurity and of Its Effects on Their Children in Italy Six Months after the COVID-19 Pandemic Outbreak
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Survey Development
2.2. Survey Conduction and Distribution
2.3. Ethics
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A. Questionnaire Composition and Key Definitions
Key Definitions
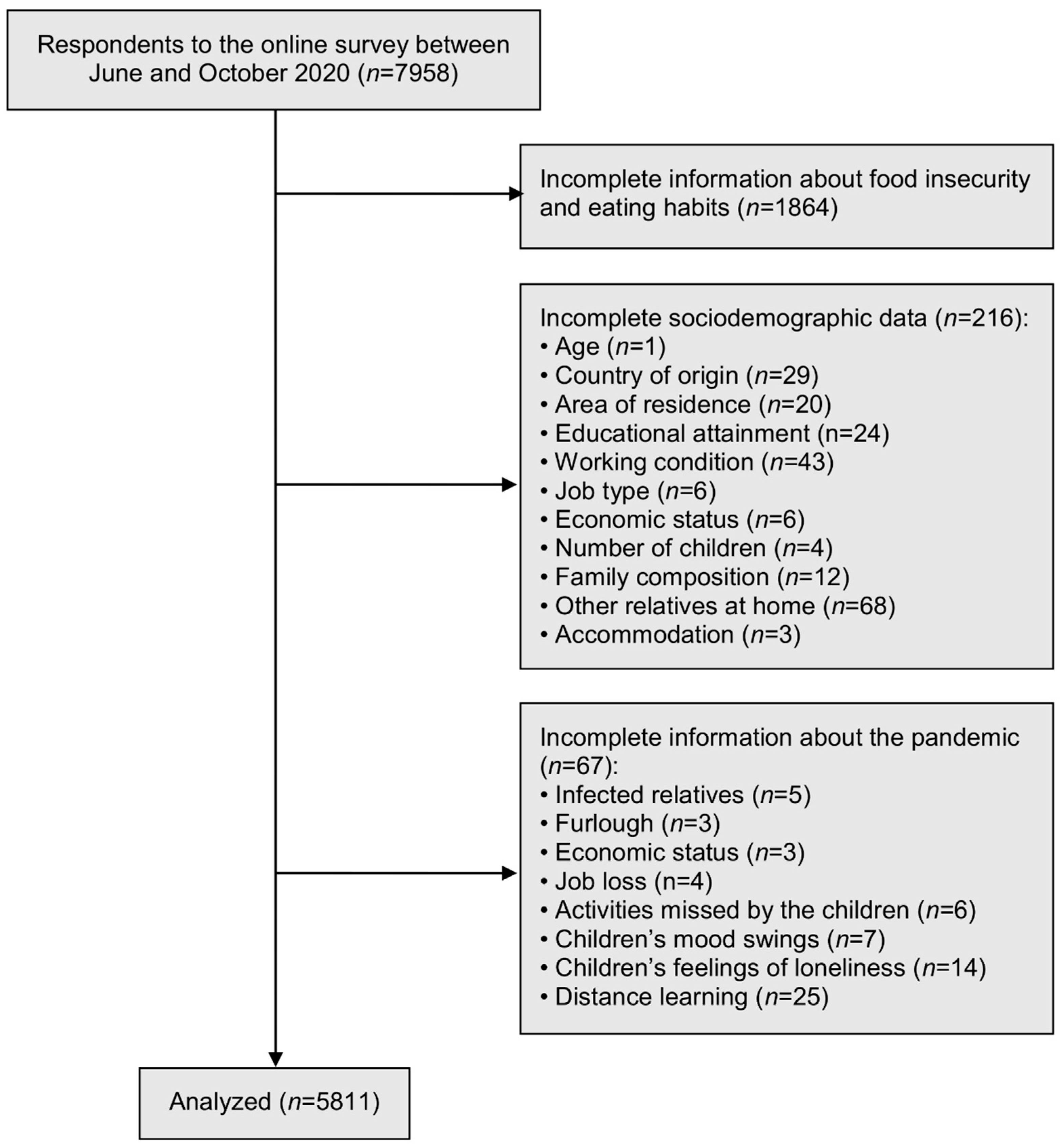
Appendix B. Exclusion of Participants with Missing Data
References
- Nord, M.; Andrews, M.S.; Carlson, S. Household Food Security in the United States, 2008; Department of Agriculture, Economic Research Service: Washington, DC, USA, 2008. [Google Scholar]
- Cook, J.T.; Frank, D.A.; Levenson, S.M.; Neault, N.B.; Heeren, T.C.; Black, M.M.; Berkowitz, C.; Casey, P.H.; Meyers, A.F.; Cutts, D.B.; et al. Child food insecurity increases risks posed by household food insecurity to young children’s health. J. Nutr. 2006, 136, 1073–1076. [Google Scholar] [CrossRef] [PubMed]
- Cook, J.T.; Frank, D.A.; Berkowitz, C.; Black, M.M.; Casey, P.H.; Cutts, D.B.; Meyers, A.F.; Zaldivar, N.; Skalicky, A.; Levenson, S.M.; et al. Food insecurity is associated with adverse health outcomes among human infants and toddlers. J. Nutr. 2004, 134, 1432–1438. [Google Scholar] [CrossRef] [PubMed]
- Ruel-Bergeron, J.C.; Stevens, G.A.; Sugimoto, J.D.; Roos, F.F.; Ezzati, M.; Black, R.E.; Kraemer, K. Global Update and Trends of Hidden Hunger, 1995–2011: The Hidden Hunger Index. PLoS ONE 2015, 10, e0143497. [Google Scholar] [CrossRef] [PubMed]
- Loopstra, R.; Reeves, A.; Stuckler, D. Rising food insecurity in Europe. Lancet 2015, 385, 2041. [Google Scholar] [CrossRef]
- Loopstra, R.; Reeves, A.; McKee, M.; Stuckler, D. Food insecurity and social protection in Europe: Quasi-natural experiment of Europe’s great recessions 2004–2012. Prev. Med. 2016, 89, 44–50. [Google Scholar] [CrossRef]
- Zaçe, D.; Di Pietro, M.L.; Caprini, F.; de Waure, C.; Ricciardi, W. Prevalence and correlates of food insecurity among children in high-income European countries. A systematic review. Ann. Ist Super Sanita 2020, 56, 90–98. [Google Scholar]
- European Union. European Commission Database. EUROSTAT. Available online: http://ec.europa.eu/eurostat/data/database (accessed on 18 March 2018).
- Koo, J.R.; Cook, A.R.; Park, M.; Sun, Y.; Sun, H.; Lim, J.T.; Tam, C.; Dickens, B.L. Interventions to mitigate early spread of SARS-CoV-2 in Singapore: A modelling study. Lancet Infect. Dis. 2020, 20, 678–688. [Google Scholar] [CrossRef]
- Smith, M.D.; Wesselbaum, D. COVID-19, food insecurity and migration. J. Nutr. 2020, 270, 2855–2858. [Google Scholar] [CrossRef]
- Committee on World Food Security 2020. High-Level Panel of Experts on Food Security and Nutrition (HLPE). Impact of COVID-19 on Food Security and Nutrition (FSN). Available online: http://www.fao.org/fileadmin/templates/cfs/Docs1920/Chair/HLPE_English.pdf (accessed on 16 November 2020).
- Niles, M.T.; Bertmann, F.; Belarmino, E.H.; Wentworth, T.; Biehl, E.; Neff, R. The early food insecurity impact of COVID19. Nutrients 2020, 12, 2096. [Google Scholar] [CrossRef]
- World Food Programme. Global Monitoring of School Meals During COVID-19 School Closures. 2020. Available online: https://cdn.wfp.org/2020/school-feeding-map/_ga=2.193001774.201527761.15888481561274318049.1588848156 (accessed on 16 November 2020).
- Martini, M.; Gazzaniga, V.; Bragazzi, N.L.; Barberis, I. The Spanish influenza pandemic: A lesson from history 100 years after 1918. J. Prev. Med. Hyg. 2019, 60, E64–E67. [Google Scholar]
- Althoff, R.R.; Ametti, M.; Bertmann, F. The role of food insecurity in developmental psychopathology. Prev. Med. 2016, 92, 106–109. [Google Scholar] [CrossRef] [PubMed]
- Post, J.D. Famine, mortality, and epidemic disease in the process of modernization. Econ. Hist. Rev. 1976, 29, 14–37. [Google Scholar] [CrossRef] [PubMed]
- Belanger, M.J.; Hill, M.A.; Angelidi, A.M.; Dalamaga, M.; Sowers, J.R.; Mantzoros, C.S. Covid-19 and disparities in nutrition and obesity. N. Engl. J. Med. 2020, 383, e69. [Google Scholar] [CrossRef] [PubMed]
- Razzoli, M.; Pearson, C.; Crow, S.; Bartolomucci, A. Stress, overeating, and obesity: Insights from human studies and preclinical models. Neurosci. Biobehav. Rev. 2017, 76, 154–162. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Maunder, R.; Hunter, J.; Vincent, L.; Bennett, J.; Peladeau, N.; Leszcz, M.; Sadavoy, J.; Verhaeghe, L.M.; Steinberg, R.; Mazzulli, T. The immediate psychological and occupational impact of the 2003 SARS outbreak in a teaching hospital. CMAJ 2003, 168, 1245–1251. [Google Scholar]
- Hawryluck, L.; Gold, W.L.; Robinson, S.; Pogorski, S.; Galea, S.; Styra, R. SARS control and psychological effects of quarantine, Toronto, Canada. Emerg. Infect. Dis. 2004, 10, 1206–1212. [Google Scholar] [CrossRef]
- DiGiovanni, C.; Conley, J.; Chiu, D.; Zaborski, J. Factors influencing compliance with quarantine in Toronto during the 2003 SARS outbreak. Biosecur. Bioterror. 2004, 2, 265–272. [Google Scholar] [CrossRef]
- Lee, S.; Chan, L.Y.; Chau, A.M.; Kwok, K.P.; Kleinman, A. The experience of SARS-related stigma at Amoy Gardens. Soc. Sci Med. 2005, 61, 2038–2046. [Google Scholar] [CrossRef]
- Reynolds, D.L.; Garay, J.R.; Deamond, S.L.; Moran, M.K.; Gold, W.; Styra, R. Understanding, compliance and psychological impact of the SARS quarantine experience. Epidemiol. Infect. 2008, 136, 997–1007. [Google Scholar] [CrossRef]
- Sprang, G.; Silman, M. Posttraumatic stress disorder in parents and youth after health-related disasters. Disaster Med. Public Health Prep. 2013, 7, 105–110. [Google Scholar] [CrossRef] [PubMed]
- WHO Regional Office for Europe. The Social Determinants of Health: The Solid Facts, 2nd ed.; Wilkinson, R., Marmot, M., Eds.; World Health Organization: Copenhagen, Denmark, 2003; ISBN 978-92-8901-287-4. [Google Scholar]
- Hager, E.R.; Quigg, A.M.; Black, M.M.; Coleman, S.M.; Heeren, T.; Rose-Jacobs, R.; Cook, J.T.; Ettinger de Cuba, S.A.; Casey, P.H.; Chilton, M.; et al. Development and validity of a 2-item screen to identify families at risk for food insecurity. Pediatrics 2010, 126, e26–e32. [Google Scholar] [CrossRef] [PubMed]
- Beymer, M.R.; Holloway, I.W.; Grov, C. Comparing Self-Reported Demographic and Sexual Behavioral Factors Among Men Who Have Sex with Men Recruited Through Mechanical Turk, Qualtrics, and a HIV/STI Clinic-Based Sample: Implications for Researchers and Providers. Arch. Sex. Behav. 2018, 47, 133–142. [Google Scholar] [CrossRef] [PubMed]
- White, I.R.; Royston, P.; Wood, A.M. Multiple imputation using chained equations: Issues and guidance for practice. Stat. Med. 2011, 30, 377–399. [Google Scholar] [CrossRef] [PubMed]
- The Lancet Global Health. Food insecurity will be the sting in the tail of COVID-19. Lancet Glob. Health 2020, 8, e737. [Google Scholar] [CrossRef]
- Pérez-Escamilla, R.; Cunningham, K.; Moran, V.H. COVID-19 and maternal and child food and nutrition insecurity: A complex syndemic. Matern. Child. Nutr. 2020, 16, e13036. [Google Scholar] [CrossRef] [PubMed]
- Wolfson, J.A.; Leung, C.W. Food Insecurity and COVID-19: Disparities in Early Effects for US Adults. Nutrients 2020, 12, 1648. [Google Scholar] [CrossRef]
- Owens, M.R.; Brito-Silva, F.; Kirkland, T.; Moore, C.E.; Davis, K.E.; Patterson, M.A.; Miketinas, D.C.; Tucker, W.J. Prevalence and Social Determinants of Food Insecurity among College Students during the COVID-19 Pandemic. Nutrients 2020, 12, 2515. [Google Scholar] [CrossRef]
- World Food Program. Covid-19 Will Double Number of People Facing Food Crisis Unless Swift Action is Taken. 2020. Available online: https://www.wfp.org/news/covid-19-will-double-number-people-facing-food-crises-unless-swift-action-taken (accessed on 15 November 2020).
- Eurostat. GDP per Capita in EU Regions. Regional GDP per Capita Ranged from 30% to 263% of the EU Average in 2018. Available online: https://ec.europa.eu/eurostat/documents/2995521/10474907/1-05032020-AP-EN.pdf/81807e19-e4c8-2e53-c98a-933f5bf30f58#:~:text=The%20leading%20regions%20in%20the,Prague%20in%20Czechia%20(192%25) (accessed on 16 November 2020).
- GBD 2017 Italy Collaborators. Italy’s health performance, 1990–2017: Findings from the Global Burden of Disease Study 2017. Lancet Public Health 2019, 4, e645–e657. [Google Scholar] [CrossRef]
- Tarasuk, V.; Fafard St-Germain, A.A.; Mitchell, A. Geographic and socio-demographic predictors of household food insecurity in Canada, 2011–2012. BMC Public Health 2019, 19, 12. [Google Scholar] [CrossRef]
- Dudek, H.; Myszkowska-Ryciak, J. The Prevalence and Socio-Demographic Correlates of Food Insecurity in Poland. Int. J. Environ. Res. Public Health 2020, 17, 6221. [Google Scholar] [CrossRef] [PubMed]
- Kent, K.; Murray, S.; Penrose, B.; Auckland, S.; Visentin, D.; Godrich, S.; Lester, E. Prevalence and Socio-Demographic Predictors of Food Insecurity in Australia during the COVID-19 Pandemic. Nutrients 2020, 12, 2682. [Google Scholar] [CrossRef] [PubMed]
- La performance sanitaria. Indice di Misurazione e Valutazione dei Sistemi Regionali Italiani. 2019. Available online: https://www.quotidianosanita.it/allegati/allegato8783063.pdf (accessed on 15 November 2020).
- Gundersen, C.; Ziliak, J.P. Childhood Food Insecurity in the U.S.: Trends, Causes, and Policy Options. Available online: http://www.princeton.edu/futureofchildren/publications/docs/ResearchReport-Fall2014.pdf (accessed on 19 December 2020).
- Ziliak, J.P.; Gundersen, C.; Haist, M. The Causes, Consequences, and Future of Senior Hunger in America. Available online: http://www.mowaa.org/document.doc?id=13 (accessed on 18 December 2020).
- Omidvar, N.; Ghazi-Tabatabie, M.; Sadeghi, R.; Mohammadi, F.; Abbasi-Shavazi, M.J. Food insecurity and its sociodemographic correlates among Afghan immigrants in Iran. J. Health Popul. Nutr. 2013, 31, 356–366. [Google Scholar] [CrossRef] [PubMed]
- Gundersen, C.; Kreider, B.; Pepper, J. The economics of food insecurity in the United States. Appl. Econ. Perspect. Policy 2011, 33, 281–303. [Google Scholar] [CrossRef]
- Ekhlaspour, P.; Foroumandi, E.; Ebrahimi-Mameghani, M.; Jafari-Koshki, T.; Arefhosseini, S.R. Household food security status and its associated factors in Baft-Kerman, IRAN: A cross-sectional study. Ecol. Food Nutr. 2019, 58, 608–619. [Google Scholar] [CrossRef] [PubMed]
- Gundersen, C.; Ziliak, J.P. Food Insecurity and Health Outcomes. Health Aff. 2015, 34, 1830–1839. [Google Scholar] [CrossRef] [PubMed]
- Dondi, A.; Piccinno, V.; Morigi, F.; Sureshkumar, S.; Gori, D.; Lanari, M. Food Insecurity and Major Diet-Related Morbidities in Migrating Children: A Systematic Review. Nutrients 2020, 12, 379. [Google Scholar] [CrossRef]
- Morales, D.X.; Morales, S.A.; Beltran, T.F. Racial/Ethnic Disparities in Household Food Insecurity During the COVID-19 Pandemic: A Nationally Representative Study. J. Racial Ethn. Health Disparities 2020, 14, 1–15. [Google Scholar] [CrossRef]
- Oliveira, T.C.; Abranches, M.V.; Lana, R.M. Food (in)security in Brazil in the context of the SARS-CoV-2 pandemic. Cad. Saude Publica 2020, 36, e00055220. [Google Scholar] [CrossRef]
- Torero, M. Without food, there can be no exit from the pandemic. Nature 2020, 580, 588–589. [Google Scholar] [CrossRef]
- Paslakis, G.; Dimitropoulos, G.; Katzman, D.K. A call to action to address COVID-19-induced global food insecurity to prevent hunger, malnutrition, and eating pathology. Nutr. Rev. 2021, 79, 114–116. [Google Scholar] [CrossRef] [PubMed]
- Gao, F.; Zheng, K.I.; Wang, X.-B.; Sun, Q.-F.; Pan, K.-H.; Wang, T.-Y.; Chen, Y.P.; Targher, G.; Byrne, C.D.; George, J.; et al. Obesity Is a Risk Factor for Greater COVID-19 Severity. Diabetes Care 2020, 43, e72–e74. [Google Scholar] [CrossRef] [PubMed]
- Food and Agriculture Organization of the United Nations (FAO). Addressing the Impacts of COVID-19 in Food Crises. Available online: http://www.fao.org/emergencies/appeals/detail/en/c/1276086/ (accessed on 19 December 2020).
- Adams, E.L.; Caccavale, L.J.; Smith, D.; Bean, M.K. Food Insecurity, the Home Food Environment, and Parent Feeding Practices in the Era of COVID-19. Obesity 2020, 28, 2056–2063. [Google Scholar] [CrossRef] [PubMed]
- Pietrobelli, A.; Pecoraro, L.; Ferruzzi, A.; Heo, M.; Faith, M.; Zoller, T.; Antoniazzi, F.; Piacentini, G.; Fearnbach, S.N.; Heymsfield, S.B. Effects of COVID-19 Lockdown on Lifestyle Behaviors in Children with Obesity Living in Verona, Italy: A Longitudinal Study. Obesity 2020, 28, 1382–1385. [Google Scholar] [CrossRef] [PubMed]
- Thivel, D.; Tremblay, M.S.; Katzmarzyk, P.T.; Fogelholm, M.; Hu, G.; Maher, C.; Maia, J.; Olds, T.; Sarmiento, O.L.; Standage, M.; et al. Associations between meeting combinations of 24-h movement recommendations and dietary patterns of children: A 12-country study. Prev. Med. 2019, 118, 159–165. [Google Scholar] [CrossRef] [PubMed]
- Baysun, Ş.; Akar, M.N. Weight gain in children during the COVID-19 quarantine period. J. Paediatr. Child. Health 2020, 56, 1487–1488. [Google Scholar] [CrossRef] [PubMed]
- He, M.; Xian, Y.; Lv, X.; He, J.; Ren, Y. Changes in Body Weight, Physical Activity, and Lifestyle During the Semi-lockdown Period After the Outbreak of COVID-19 in China: An Online Survey. Disaster Med. Public Health Prep. 2020, 1–6. [Google Scholar] [CrossRef]
- Sidor, A.; Rzymski, P. Dietary Choices and Habits during COVID-19 Lockdown: Experience from Poland. Nutrients 2020, 12, 1657. [Google Scholar] [CrossRef]
- Barrea, L.; Pugliese, G.; Framondi, L.; Di Matteo, R.; Laudisio, D.; Savastano, S.; Colao, A.; Muscogiuri, G. Does Sars-Cov-2 threaten our dreams? Effect of quarantine on sleep quality and body mass index. J. Transl. Med. 2020, 18, 318. [Google Scholar] [CrossRef]
- Zachary, Z.; Brianna, F.; Brianna, L.; Garrett, P.; Jade, W.; Alyssa, D.; Mikayla, K. Self-quarantine and weight gain related risk factors during the COVID-19 pandemic. Obes. Res. Clin. Pract. 2020, 14, 210–216. [Google Scholar] [CrossRef]
- Mayasari, N.R.; Ho, D.K.N.; Lundy, D.J.; Skalny, A.V.; Tinkov, A.A.; Teng, I.C.; Wu, M.C.; Faradina, A.; Mohammed, A.Z.M.; Park, J.M.; et al. Impacts of the COVID-19 Pandemic on Food Security and Diet-Related Lifestyle Behaviors: An Analytical Study of Google Trends-Based Query Volumes. Nutrients 2020, 2, 3103. [Google Scholar] [CrossRef] [PubMed]
- Tester, J.M.; Rosas, L.G.; Leung, C.W. Food Insecurity and Pediatric Obesity: A Double Whammy in the Era of COVID-19. Curr. Obes. Rep. 2020, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Delgado Floody, P.A.; Caamaño Navarrete, F.; Guzmán-Guzmán, I.P.; Jerez Mayorga, D.; Cofré, A.; Alvarez Lepin, C.G. Negative feelings and behaviour are associated with low nutritional level, unhealthy lifestyle, and cardiometabolic risk factors in Chilean schoolchildren. Nutr. Hosp. 2020, 37, 707–714. [Google Scholar] [CrossRef] [PubMed]
- Michels, N.; Sioen, I.; Boone, L.; Braet, C.; Vanaelst, B.; Huybrechts, I.; De Henauw, S. Longitudinal association between child stress and lifestyle. Health Psychol. 2015, 34, 40. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Rio, J.; Cecchini, J.A.; Mendez-Gimenez, A.; Carriedo, A. Weight changes during the COVID-19 home confinement. Effects on psychosocial variables. Obes. Res. Clin. Pract. 2020, 14, 383–385. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, S.; Cortés-García, L.; Warschburger, P. Weight/shape and muscularity concerns and emotional problems in adolescent boys and girls: A cross-lagged panel analysis. J. Adolesc. 2018, 68, 70–77. [Google Scholar] [CrossRef] [PubMed]
- Gallè, F.; Sabella, E.A.; Da Molin, G.; De Giglio, O.; Caggiano, G.; Di Onofrio, V.; Ferracuti, S.; Montagna, M.T.; Liguori, G.; Orsi, G.B.; et al. Understanding Knowledge and Behaviors Related to CoViD-19 Epidemic in Italian Undergraduate Students: The EPICO Study. Int. J. Environ. Res. Public Health 2020, 17, 3481. [Google Scholar] [CrossRef]
- Van den Berg, P.A.; Mond, J.; Eisenberg, M.; Ackard, D.; Neumark-Sztainer, D. The link between body dissatisfaction and self-esteem in adolescents: Similarities across gender, age, weight status, race/ethnicity, and socioeconomic status. J. Adolesc. Health 2010, 47, 290–296. [Google Scholar] [CrossRef]
- Paxton, S.J.; Neumark-Sztainer, D.; Hannan, P.J.; Eisenberg, M.E. Body dissatisfaction prospectively predicts depressive mood and low self-esteem in adolescent girls and boys. J. Clin. Child. Adolesc. Psychol. 2006, 35, 539–549. [Google Scholar] [CrossRef]
- Kim, D.S.; Kim, H.S. Body-image dissatisfaction as a predictor of suicidal ideation among Korean boys and girls in different stages of adolescence: A two-year longitudinal study. J. Adolesc. Health 2009, 45, 47–54. [Google Scholar] [CrossRef]
- Johnson, F.; Wardle, J. Dietary restraint, body dissatisfaction, and psychological distress: A prospective analysis. J. Abnorm Psychol. 2005, 114, 119–125. [Google Scholar] [CrossRef] [PubMed]
- Razzoli, M.; Bartolomucci, A. The Dichotomous Effect of Chronic Stress on Obesity. Trends Endocrinol. Metab. 2016, 27, 504–515. [Google Scholar] [CrossRef] [PubMed]
- Polivy, J.; Herman, C.P. Mental health and eating behaviours: A bi-directional relation. Can. J. Public Health 2005, 96, S43–S46. [Google Scholar] [PubMed]
- Marty, L.; de Lauzon-Guillain, B.; Labesse, M.; Nicklaus, S. Food choice motives and the nutritional quality of diet during the COVID-19 lockdown in France. Appetite 2020, 157, 105005. [Google Scholar] [CrossRef]
- Leddy, A.M.; Weiser, S.D.; Palar, K.; Seligman, H. A conceptual model for understanding the rapid COVID-19–related increase in food insecurity and its impact on health and healthcare. Am. J. Clin. Nutr. 2020, 112, 1162–1169. [Google Scholar] [CrossRef]
- Baer, T.E.; Scherer, E.A.; Fleegler, E.W.; Hassan, A. Food Insecurity and the Burden of Health-Related Social Problems in an Urban Youth Population. J. Adolesc Health 2015, 57, 601–607. [Google Scholar] [CrossRef]
- Gundersen, C.; Engelhard, E.E.; Crumbaugh, A.S.; Seligman, H.K. Brief assessment of food insecurity accurately identifies high-risk US adults. Public Health Nutr. 2017, 20, 1367–1371. [Google Scholar] [CrossRef]
- Bruni, O.; Ottaviano, S.; Guidetti, V.; Romoli, M.; Innocenzi, M.; Cortesi, F.; Giannotti, F. The Sleep Disturbance Scale for Children (SDSC). Construction and validation of an instrument to evaluate sleep disturbances in childhood and adolescence. J. Sleep Res. 1996, 5, 251–261. [Google Scholar] [CrossRef]
- World Health Organization. Commission on the Social Determinants of Health. Closing the Gap in a Generation. Final Report of the Commission on Social Determinants of Health. Available online: www.who.int›final_report›csdh_finalreport_2008 (accessed on 16 November 2020).
| Characteristic | n | % |
|---|---|---|
| Age, y | ||
| ≤30 | 246 | 4.2 |
| 31–35 | 910 | 15.7 |
| 36–40 | 1696 | 29.2 |
| 41–45 | 1587 | 27.3 |
| 46–50 | 943 | 16.2 |
| >50 | 429 | 7.4 |
| Sex | ||
| Female | 5327 | 91.7 |
| Male | 484 | 8.3 |
| Country of origin | ||
| Italy | 5645 | 97.1 |
| Outside Italy * | 166 | 2.9 |
| Area of residence † | ||
| Northern Italy | 5171 | 89.0 |
| Central Italy | 348 | 6.0 |
| Southern Italy | 292 | 5.0 |
| Educational attainment | ||
| Middle school (8th grade) or less | 230 | 4.0 |
| High school (12/13th grade) | 2100 | 36.1 |
| University degree or more | 3481 | 59.9 |
| Educational attainment of the other parent | ||
| Middle school (8th grade) or less | 889 | 15.3 |
| High school (12/13th grade) | 2588 | 44.5 |
| University degree or more | 2334 | 41.2 |
| Working condition of the parents | ||
| Both employed | 4983 | 85.8 |
| One unemployed | 794 | 13.7 |
| Both unemployed | 34 | 0.6 |
| Job type | ||
| Clerk | 2913 | 50.1 |
| Retired | 781 | 13.4 |
| Homemaker | 648 | 11.2 |
| Freelancer | 276 | 4.7 |
| Laborer | 263 | 4.5 |
| Health-care worker | 132 | 2.3 |
| Dealer | 118 | 2.0 |
| Other ‡ | 680 | 11.7 |
| Economic status | ||
| Well-off | 2307 | 39.7 |
| Somewhat difficult but overall satisfactory | 3123 | 53.7 |
| Quite difficult | 356 | 6.1 |
| Often unsustainable | 25 | 0.4 |
| Number of children in the family | ||
| 1 | 2405 | 41.4 |
| 2 | 2827 | 48.6 |
| 3 | 446 | 7.7 |
| >3 | 133 | 2.3 |
| Age of the youngest or only child, y | ||
| ≤2 | 1759 | 30.3 |
| 3–5 | 1419 | 24.4 |
| 6–10 | 1523 | 26.2 |
| 11–14 | 685 | 11.8 |
| >14 | 425 | 7.3 |
| Children with disorders or disabilities | ||
| No | 5147 | 88.6 |
| Learning disabilities | 252 | 4.3 |
| Other disabilities | 85 | 1.5 |
| Chronic conditions | 67 | 1.2 |
| Autism spectrum disorders | 48 | 0.8 |
| Multiple conditions | 47 | 0.8 |
| Unspecified | 165 | 2.8 |
| The parents live together | ||
| Yes | 5329 | 91.7 |
| No | 431 | 7.4 |
| Single parenthood | 51 | 0.9 |
| Other relatives at home | ||
| No | 5397 | 92.9 |
| Grandparents | 329 | 5.7 |
| Other relatives | 85 | 1.5 |
| Type of accommodation | ||
| Own property | 5083 | 87.5 |
| Renting | 720 | 12.4 |
| Hotel/pension, reception center or with others | 8 | 0.1 |
| Characteristic | n | % |
|---|---|---|
| A member of the family got COVID-19 | ||
| No | 5031 | 86.6 |
| Yes | 420 | 7.2 |
| Yes, hospitalized | 192 | 3.3 |
| Yes, passed away | 168 | 2.9 |
| Smart working for either parent | ||
| Yes | 2925 | 50.3 |
| No | 1464 | 25.2 |
| Unspecified | 1422 | 24.5 |
| Furlough for either parent | ||
| No | 3587 | 61.7 |
| Yes | 2224 | 38.3 |
| Economic status after the outbreak | ||
| Improved | 159 | 2.7 |
| Unchanged | 3203 | 55.1 |
| Slightly worsened | 2161 | 37.2 |
| Worsened | 246 | 4.2 |
| Become critical | 42 | 0.7 |
| Either parent has lost their job | ||
| No | 5558 | 95.6 |
| Yes | 253 | 4.4 |
| How the parent sees her/his means after the pandemic | ||
| Better | 126 | 2.2 |
| Unchanged | 2349 | 40.4 |
| More difficult | 2938 | 50.6 |
| Much more difficult | 332 | 5.7 |
| Seriously at risk | 66 | 1.1 |
| What have your children missed more? * | ||
| Going to school | 1770 | 30.5 |
| Outdoor activities | 2723 | 46.9 |
| Meeting friends | 4676 | 80.5 |
| Meeting relatives | 2411 | 41.5 |
| Playing sports | 2462 | 42.4 |
| Any mood swing in your children? | ||
| Yes, more nervous, troubled or sad | 4269 | 73.5 |
| No | 1389 | 23.9 |
| Yes, their mood has improved | 153 | 2.6 |
| Did your children have feelings of loneliness? | ||
| Yes, putting it into words | 2151 | 37.0 |
| Yes, not putting it into words | 1852 | 31.9 |
| No | 1808 | 31.1 |
| Any child attending distance-learning classes? | ||
| Yes | 3737 | 64.3 |
| No | 2074 | 35.7 |
| Characteristic | Worrying About Food Supplies | Running Out of Food |
|---|---|---|
| OR (99% CI) | OR (99% CI) | |
| Age, y (ref: ≤30) | ||
| 31–35 | 1.16 (0.66–2.04) | 0.66 (0.26–1.71) |
| 36–40 | 1.03 (0.59–1.78) | 1.08 (0.45–2.62) |
| 41–45 | 0.77 (0.44–1.35) | 0.61 (0.24–1.56) |
| 46-50 | 0.68 (0.37–1.25) | 0.54 (0.19–1.53) |
| >50 | 0.37 (0.17–0.81) * | 0.56 (0.16–2.00) |
| Sex (ref: male) | ||
| Female | 1.38 (0.81–2.35) | 1.38 (0.46–4.16) |
| Country of origin (ref: Italy) | ||
| Outside Italy | 1.28 (0.70–2.32) | 1.34 (0.51–3.50) |
| Area of residence (ref: Northern Italy) | ||
| Central Italy | 0.89 (0.54–1.48) | 0.88 (0.34–2.23) |
| Southern Italy | 1.66 (1.01–2.72) * | 1.56 (0.59–4.11) |
| Educational attainment of the parents (ref: both secondary school) | ||
| Secondary school & graduate school | 0.68 (0.50–0.92) * | 0.68 (0.38–1.20) |
| Both graduate school | 0.69 (0.48–0.98) * | 0.43 (0.18–1.02) |
| Working condition of the parents (ref: either unemployed) | ||
| Both employed | 0.63 (0.42–0.94) * | 1.00 (0.48–2.10) |
| Job type (ref: health-care worker) | ||
| Clerk | 1.40 (0.56–3.54) | 0.97 (0.16–5.82) |
| Retired | 1.62 (0.60–4.38) | 0.73 (0.10–5.34) |
| Homemaker | 1.75 (0.66–4.64) | 0.63 (0.09–4.32) |
| Freelancer | 0.87 (0.34–2.25) | 0.67 (0.11–4.08) |
| Laborer | 1.52 (0.56–4.11) | 1.50 (0.24–9.46) |
| Dealer | 2.19 (0.71–6.77) | 1.06 (0.13–8.91) |
| Other | 1.40 (0.54–3.64) | 1.03 (0.16–6.56) |
| Economic status (ref: well-off) | ||
| Somewhat difficult but overall satisfactory | 2.11 (1.48–3.01) * | 5.18 (1.34–20.06) * |
| Difficult/unsustainable | 3.90 (2.39–6.38) * | 10.72 (2.53–45.33) * |
| Number of children (ref: 1) | ||
| 2 | 1.37 (1.05–1.79) * | 0.81 (0.48–1.37) |
| 3 | 1.43 (0.91–2.26) | 1.15 (0.50–2.63) |
| >3 | 1.74 (0.83–3.67) | 1.63 (0.42–6.37) |
| Type of accommodation (ref: own property) | ||
| Renting/other | 1.19 (0.86–1.63) | 1.68 (0.99–2.86) |
| Smart working for either parent (ref: no) | ||
| Yes | 0.95 (0.69–1.32) | 0.90 (0.47–1.70) |
| Furlough for either parent (ref: no) | ||
| Yes | 1.43 (1.10–1.87) * | 1.21 (0.72–2.02) |
| Economic status after the outbreak (ref: improved/unchanged) | ||
| Slightly worsened | 2.14 (1.57–2.92) * | 7.96 (2.85–22.21) * |
| Worsened | 5.77 (3.63–9.16) * | 22.70 (7.23–71.23) * |
| How the parent sees her/his means after the pandemic (ref: better/unchanged) | ||
| More difficult | 2.17 (1.52–3.09) * | 1.05 (0.47–2.35) |
| Much more difficult/seriously at risk | 3.74 (2.32–6.01) * | 2.08 (0.82–5.24) |
| Any mood swing in your children? (ref: no) | ||
| Yes, more nervous, troubled or sad | 1.23 (0.89–1.70) | 2.43 (1.07–5.53) * |
| Yes, their mood has improved | 0.87 (0.33–2.30) | 1.36 (0.17–11.03) |
| Characteristic | Increased Food Intake | Decreased Food Intake |
|---|---|---|
| OR (99% CI) | OR (99% CI) | |
| Age, y (ref: ≤30) | ||
| 31–35 | 0.80 (0.50–1.28) | 0.95 (0.54–1.64) |
| 36–40 | 0.86 (0.55–1.35) | 1.03 (0.60–1.75) |
| 41–45 | 0.79 (0.50–1.26) | 0.91 (0.52–1.59) |
| 46–50 | 0.67 (0.41–1.10) | 0.95 (0.51–1.79) |
| >50 | 0.60 (0.34–1.07) | 0.97 (0.47–2.04) |
| Sex (ref: male) | ||
| Female | 1.84 (1.29–2.63) * | 1.36 (0.90–2.07) |
| Educational attainment of the parents (ref: both secondary school) | ||
| Secondary school & graduate school | 0.95 (0.77–1.17) | 0.99 (0.75–1.30) |
| Both graduate school | 0.71 (0.57–0.89) * | 0.95 (0.71–1.27) |
| Economic status (ref: well-off) | ||
| Somewhat difficult but overall satisfactory | 1.12 (0.92–1.36) | 1.25 (0.97–1.61) |
| Difficult/unsustainable | 1.53 (1.03–2.26) * | 1.39 (0.82–2.34) |
| Number of children (ref: 1) | ||
| 2 | 1.33 (1.09–1.62) * | 1.28 (1.00–1.65) |
| 3 | 1.79 (1.28–2.51) * | 1.34 (0.84–2.15) |
| >3 | 1.47 (0.82–2.63) | 1.07 (0.48–2.37) |
| Age of the youngest or only child, y (ref: ≤2) | ||
| 3–5 | 1.54 (1.20–1.98) * | 0.82 (0.61–1.10) |
| 6–10 | 1.51 (1.12–2.04) * | 0.58 (0.38–0.86) * |
| 11–14 | 1.91 (1.30–2.80) * | 0.87 (0.52–1.48) |
| >14 | 1.47 (0.92–2.35) | 1.22 (0.67–2.23) |
| Economic status after the outbreak (ref: improved/unchanged) | ||
| Slightly worsened | 1.20 (0.98–1.46) | 0.96 (0.74–1.24) |
| Worsened | 1.09 (0.70–1.70) | 1.02 (0.58–1.79) |
| How the parent sees her/his means after the pandemic (ref: better/unchanged) | ||
| More difficult | 1.21 (0.99–1.47) | 1.27 (0.98–1.63) |
| Much more difficult/seriously at risk | 1.38 (0.94–2.04) | 1.99 (1.24–3.18) * |
| Increased worry about running out of food (ref: no) | ||
| Yes | 1.27 (0.95–1.70) | 1.15 (0.78–1.69) |
| Children have missed outdoor activities (ref: no) | ||
| Yes | 1.23 (1.03–1.46) * | 1.07 (0.86–1.35) |
| Children have missed playing sports (ref: no) | ||
| Yes | 1.15 (0.97–1.37) | 1.03 (0.82–1.29) |
| Any mood swing in your children? (ref: no) | ||
| Yes, more nervous, troubled or sad | 2.57 (2.02–3.27) * | 2.51 (1.82–3.47) * |
| Yes, their mood has improved | 3.28 (1.93–5.55) * | 2.13 (0.96–4.69) |
| Did your children have feelings of loneliness? (ref: no) | ||
| Yes, not putting it into words | 1.39 (1.11–1.76) * | 1.77 (1.31–2.39) * |
| Yes, putting it into words | 1.68 (1.34–2.10) * | 1.97 (1.46–2.66) * |
| Characteristic | Weight Gain | Weight Loss |
|---|---|---|
| OR (99% CI) | OR (99% CI) | |
| Age, y (ref: ≤30) | ||
| 31–35 | 0.66 (0.40–1.09) | 0.98 (0.38–2.55) |
| 36–40 | 0.86 (0.54–1.38) | 1.29 (0.52–3.18) |
| 41–45 | 0.95 (0.59–1.53) | 1.35 (0.53–3.45) |
| 46–50 | 0.97 (0.58–1.63) | 1.88 (0.70–5.04) |
| >50 | 1.19 (0.66–2.16) | 1.48 (0.49–4.42) |
| Sex (ref: male) | ||
| Female | 1.35 (0.97–1.87) | 1.34 (0.71–2.55) |
| Economic status (ref: well-off) | ||
| Somewhat difficult but overall satisfactory | 1.09 (0.91–1.31) | 1.51 (1.05–2.16) * |
| Difficult/unsustainable | 1.24 (0.85–1.81) | 1.98 (1.01–3.86) * |
| Number of children (ref: 1) | ||
| 2 | 1.45 (1.18–1.77) * | 0.98 (0.68–1.41) |
| 3 | 1.86 (1.31–2.64) * | 1.67 (0.88–3.19) |
| >3 | 1.79 (0.99–3.21) | 1.49 (0.49–4.49) |
| Age of the youngest or only child, y (ref: ≤2) | ||
| 3–5 | 1.15 (0.89–1.48) | 0.75 (0.45–1.26) |
| 6–10 | 1.41 (1.04–1.91) * | 1.28 (0.70–2.33) |
| 11–14 | 1.25 (0.84–1.85) | 1.55 (0.74–3.26) |
| >14 | 0.86 (0.53–1.38) | 3.19 (1.44–7.09) * |
| Children with disorders or disabilities (ref: no) | ||
| Learning disabilities | 1.39 (0.92–2.10) | 2.21 (1.09–4.46) * |
| Other conditions | 1.11 (0.73–1.68) | 1.54 (0.75–3.18) |
| Unspecified | 1.02 (0.62–1.69) | 1.46 (0.61–3.51) |
| Increased worry about running out of food (ref: no) | ||
| Yes | 0.84 (0.62–1.14) | 0.78 (0.44–1.38) |
| Changes in children’s food intake (ref: no) | ||
| More food | 7.25 (6.02–8.74) * | 0.72 (0.36–1.44) |
| Less food | 0.60 (0.42–0.87) * | 14.43 (10.10–20.6) * |
| Children have missed going to school (ref: no) | ||
| Yes | 1.19 (0.99–1.44) | 0.82 (0.57–1.18) |
| Did your children have feelings of loneliness? (ref: no) | ||
| Yes, not putting it into words | 1.24 (0.99–1.55) | 1.20 (0.77–1.87) |
| Yes, putting it into words | 1.43 (1.15–1.77) * | 1.70 (1.11–2.61) * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dondi, A.; Candela, E.; Morigi, F.; Lenzi, J.; Pierantoni, L.; Lanari, M. Parents’ Perception of Food Insecurity and of Its Effects on Their Children in Italy Six Months after the COVID-19 Pandemic Outbreak. Nutrients 2021, 13, 121. https://doi.org/10.3390/nu13010121
Dondi A, Candela E, Morigi F, Lenzi J, Pierantoni L, Lanari M. Parents’ Perception of Food Insecurity and of Its Effects on Their Children in Italy Six Months after the COVID-19 Pandemic Outbreak. Nutrients. 2021; 13(1):121. https://doi.org/10.3390/nu13010121
Chicago/Turabian StyleDondi, Arianna, Egidio Candela, Francesca Morigi, Jacopo Lenzi, Luca Pierantoni, and Marcello Lanari. 2021. "Parents’ Perception of Food Insecurity and of Its Effects on Their Children in Italy Six Months after the COVID-19 Pandemic Outbreak" Nutrients 13, no. 1: 121. https://doi.org/10.3390/nu13010121
APA StyleDondi, A., Candela, E., Morigi, F., Lenzi, J., Pierantoni, L., & Lanari, M. (2021). Parents’ Perception of Food Insecurity and of Its Effects on Their Children in Italy Six Months after the COVID-19 Pandemic Outbreak. Nutrients, 13(1), 121. https://doi.org/10.3390/nu13010121









