-
 Artificial Intelligence in Burn Assessment: A Scoping Review with an LLM-Generated Decision Tree
Artificial Intelligence in Burn Assessment: A Scoping Review with an LLM-Generated Decision Tree -
 Clinical Parameters for Inhalation Injury Prognosi
Clinical Parameters for Inhalation Injury Prognosi -
 A Precursor to Pulmonary Dysfunction Post-Burn
A Precursor to Pulmonary Dysfunction Post-Burn -
 Attenuation Coefficient and Blood Flow at Depth in Pediatric Thermal Hand Injuries Using Optical Coherence Tomography
Attenuation Coefficient and Blood Flow at Depth in Pediatric Thermal Hand Injuries Using Optical Coherence Tomography -
 Topical TXA with Epinephrine for Perioperative Bleeding
Topical TXA with Epinephrine for Perioperative Bleeding
Journal Description
European Burn Journal
European Burn Journal
(formerly European Journal of Burn Care) is an international, peer-reviewed, open access journal on burn care and burn prevention, published quarterly online. It is the official journal of the European Burns Association (EBA).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), PMC, PubMed, Scopus and other databases.
- Journal Rank: CiteScore - Q2 (Health Professions (miscellaneous))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 20.7 days after submission; acceptance to publication is undertaken in 4.6 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Companion journal: Healthcare.
Impact Factor:
1.2 (2024);
5-Year Impact Factor:
1.3 (2024)
Latest Articles
Japanese Consensus Document on NexoBrid®, a Burn Eschar Removal Agent
Eur. Burn J. 2026, 7(2), 29; https://doi.org/10.3390/ebj7020029 - 13 May 2026
Abstract
Background: NexoBrid® (NXB), an enzymatic debridement agent approved in Japan in 2022, provides a less invasive alternative to surgical excision for burn treatment. However, its optimal therapeutic benefit depends on appropriate patient selection and proper application technique. Existing international consensus documents are
[...] Read more.
Background: NexoBrid® (NXB), an enzymatic debridement agent approved in Japan in 2022, provides a less invasive alternative to surgical excision for burn treatment. However, its optimal therapeutic benefit depends on appropriate patient selection and proper application technique. Existing international consensus documents are not fully applicable to clinical practice in Japan because of differences in available devices and drugs. Therefore, a Japan-specific consensus document was developed by a panel of seven Japanese burn experts, including four plastic surgeons and three emergency physicians. Methods: A questionnaire-based survey was conducted using the Delphi method to achieve expert consensus. Consensus was defined as agreement by at least 80% of committee members for each statement. A total of 27 statements were evaluated over two rounds. Results: Consensus was achieved for 20 of 27 statements (74.1%) in the first round and for 21 of 27 statements (77.8%) in the second round. The finalised statements were organised into seven categories according to their attributes: indications, pain management, application timing, application technique, post-application wound care, skin grafting, and scarring/aesthetic outcomes. Conclusions: This consensus document integrates the opinions of plastic surgeons and emergency physicians in Japan, while also incorporating relevant international perspectives, to provide practical guidance on the use of NXB for burn treatment. It is intended to improve the quality of burn care by clarifying efficacy, safety, and precautions associated with NXB use. These recommendations should be updated as further clinical experience accumulates.
Full article
Open AccessArticle
Predictors of Mortality in Burn Patients at Selected Tertiary Public Hospitals in Addis Ababa, Ethiopia: A Two-Year Retrospective Study
by
Rahel Kassa Bayou, Meheret Befekadu Demmissie, Bethelhem Kassa Bayou, Laura Pompermaier, Hanna Yemane Berhane and Bacha Mirkena Dhabi
Eur. Burn J. 2026, 7(2), 28; https://doi.org/10.3390/ebj7020028 - 12 May 2026
Abstract
Background: Burn injuries are a major cause of morbidity and mortality in low- and middle-income countries, yet remain underreported due to limited data systems. This study describes the epidemiology of burn patients admitted to two major burn centers in Addis Ababa, Ethiopia, and
[...] Read more.
Background: Burn injuries are a major cause of morbidity and mortality in low- and middle-income countries, yet remain underreported due to limited data systems. This study describes the epidemiology of burn patients admitted to two major burn centers in Addis Ababa, Ethiopia, and identifies predictors of in-hospital mortality. Methods: A cross-sectional study was conducted among patients with new burn injuries admitted between 1 September 2021, and 1 November 2023, at the Addis Ababa Burn, Emergency, and Trauma Center (AaBET) and Yekatit 12 Medical College (Y12MC) hospitals. Data were extracted from medical records. Descriptive statistics summarized patient characteristics, and binary logistic regression with multivariable analysis identified factors associated with in-hospital mortality using adjusted odds ratios (AORs) and 95% confidence intervals (CIs). Results: Chart completeness was 96.2%. Among 800 patients, 57% were female, with a median age of 18 years (range: 0–89); approximately 80% were under 30 years. Scalds were the leading cause (49.1%). In-hospital mortality was 8.5% (95% CI: 6.5–10.4). Significant predictors included inhalation injury (AOR 6.53), TBSA ≥ 15% (AOR 3.33), deep burns (AOR 1.96), and ICU admission (AOR 14.42). Conclusions: In-hospital mortality was moderate, disproportionately affecting children and young adults, underscoring the need to strengthen critical care and management of severe burns.
Full article
(This article belongs to the Special Issue Global Perspectives on Burn Prevention, Management, Collaboration, and Disparities)
Open AccessArticle
The UK Consensus Statement for the Use of Enzymatic Debridement in Burn Care
by
Nicole Lee, Ascanio Tridente, Niall Martin, Odhran Shelley and on behalf of the UK Working Group for Enzymatic Debridement
Eur. Burn J. 2026, 7(2), 27; https://doi.org/10.3390/ebj7020027 (registering DOI) - 12 May 2026
Abstract
Background: Over the past ten years, enzymatic debridement has been used more often to treat burn injuries in the UK and Europe. Even though it is increasingly adopted, there are still major differences in how it is practiced. These differences are mainly
[...] Read more.
Background: Over the past ten years, enzymatic debridement has been used more often to treat burn injuries in the UK and Europe. Even though it is increasingly adopted, there are still major differences in how it is practiced. These differences are mainly due to varying levels of professional experience, differences in the interpretation of available evidence, and concerns about safety and effectiveness. Methods: To help resolve these issues and create more consistent care, the UK National Consensus Working Group was formed. This group brought together burn care experts from different backgrounds to review current methods, published research, and consensus guidelines. They used a structured approach that included educational webinars, a thorough review of the literature, and a national survey using the Delphi method to gather expert opinions and real-world experiences. Results: As a result of this process, the UK Consensus Statement for the Use of Enzymatic Debridement in Burn Care was created and officially approved after extensive consultation at national meetings. The main recommendations focus on safely and effectively including enzymatic debridement in burn care, the need for clear procedures, and identifying areas where further research is needed, such as patient outcomes and dressing methods. Conclusions: The goal of this consensus statement is to unify practices, guide future research, and support ongoing improvements in burn care throughout the UK.
Full article
(This article belongs to the Special Issue Global Perspectives on Burn Prevention, Management, Collaboration, and Disparities)
Open AccessFeature PaperArticle
Recommendations on Sexuality and Intimacy After Burn Injuries
by
Jill Meirte, Stefania Anna Simone, Sabrina Belemkasser and Jonathan Bayuo
Eur. Burn J. 2026, 7(2), 26; https://doi.org/10.3390/ebj7020026 - 12 May 2026
Abstract
Background: Burn injuries profoundly impact the survivors’ physical, psychological and social well-being, with sexuality, intimacy and body image remaining among the most disrupted yet least addressed areas of rehabilitation. Limited professional training, social discomfort, and a lack of clinical guidance contribute to these
[...] Read more.
Background: Burn injuries profoundly impact the survivors’ physical, psychological and social well-being, with sexuality, intimacy and body image remaining among the most disrupted yet least addressed areas of rehabilitation. Limited professional training, social discomfort, and a lack of clinical guidance contribute to these unmet needs. Recognizing sexuality as an essential part of health, this interdisciplinary project developed evidence-informed recommendations and communication tools to support both burn survivors and healthcare professionals in discussing intimacy, sexuality, and body image after burn injury. Methods: An interdisciplinary expert group conducted a narrative literature review, supplemented with grey literature and lived experience resources. These insights informed two practical tools: a poster for healthcare professionals and burn centers, and a patient-focused brochure. Both underwent iterative refinement through multicultural feedback from patients and professionals across Europe, Asia and Africa, followed by final validation during an interdisciplinary workshop at the 2025 European Burns Association (EBA) Conference. Results: The literature indicated that burn injuries affect sexuality and body image through interacting physiological, psychological, sensory, relational, and sociocultural factors. Common challenges included reduced desire, anxiety, fear of rejection, altered self-perception, and discomfort initiating conversations about intimacy. Professionals reported limited training, insufficient privacy and cultural barriers. Conclusions: The developed tools and these recommendations aim to normalize dialog, support proactive screening, and promote culturally sensitive patient-centered burn rehabilitation. Embedding sexuality and intimacy within burn care requires ongoing professional training and the identification of dedicated resource persons within each team.
Full article
(This article belongs to the Special Issue 2nd Edition of Enhancing Psychosocial Burn Care)
►▼
Show Figures
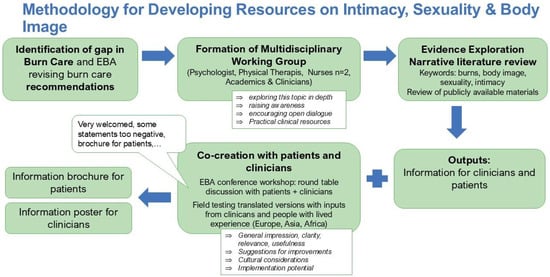
Figure 1
Open AccessArticle
The Efficacy of UV-C Disinfection in Decreasing Hospital-Acquired Infections and Bioburden in an Adult Burns Service
by
Elad Zvi, Melissa Neely, Louise Higgins, Maja Garcia, Melinda Pacquola, Eldho Paul, Alex Padiglione, Heather Cleland and Cheng Hean Lo
Eur. Burn J. 2026, 7(2), 25; https://doi.org/10.3390/ebj7020025 - 11 May 2026
Abstract
Background: Burn patients are highly susceptible to hospital-acquired infections (HAIs), and contaminated near-patient surfaces can act as reservoirs for multidrug-resistant organisms (MROs). Ultraviolet-C (UV-C) room disinfection is increasingly used as an adjunct to manual cleaning, but real-world data in adult burns settings remain
[...] Read more.
Background: Burn patients are highly susceptible to hospital-acquired infections (HAIs), and contaminated near-patient surfaces can act as reservoirs for multidrug-resistant organisms (MROs). Ultraviolet-C (UV-C) room disinfection is increasingly used as an adjunct to manual cleaning, but real-world data in adult burns settings remain limited. Methods: We evaluated adjunctive UV-C disinfection in a tertiary adult trauma and burns surgical ward using a two-part observational design. Part A compares MRO-related HAI incidence before UV-C implementation (12 May 2015–11 May 2020; retrospective) with its incidence after implementation (14 July 2020–13 July 2021; prospective). Part B is a matched pre/post environmental sampling study (December 2022–December 2024) of 44 vacant rooms. Paired swabs from a single randomised high-touch surface per room were collected immediately before and after UV-C disinfection and processed by an independent laboratory. Results: Part A included 7589 admissions (6415 before-UV-C; 1174 after-UV-C) with 2728 UV-C cycles delivered after implementation. MRO-related HAI incidence decreased from 18.3 to 10.2 per 1000 bed-days (p < 0.01). In Part B, the proportion of swabs with <10 CFU increased after UV-C disinfection (66% vs. 50%, p = 0.02). Among swabs with non-negligible baseline contamination and excluding increases, the median CFU reduction was 97% (SD 12%; p < 0.001), with no significant differences in reduction across sampled surface types. Conclusion: In an adult burns surgical ward, adjunctive UV-C disinfection was associated with reduced MRO-related HAI incidence and a substantial reduction in environmental bioburden on high-touch surfaces. These real-world findings support UV-C as a feasible adjunct to standard cleaning in high-risk burn services and inform future controlled evaluations.
Full article
Open AccessSystematic Review
The Scalp as a Donor Site in Pediatric Burns: Systematic Review of the Literature and Proposal of a Management Algorithm
by
Carlotta Paola Maria Canonica, Irene Paraboschi, Eleonora Durante, Francesca Izzo, Anna Mandelli, Sara Costanzo, Elvira Conti, Gloria Pelizzo and Anne Le Touze
Eur. Burn J. 2026, 7(2), 24; https://doi.org/10.3390/ebj7020024 - 8 May 2026
Abstract
►▼
Show Figures
Background: Deep burns in pediatric population often require split-thickness skin grafts (STSGs) and the identification of an optimal donor site is crucial to minimize morbidity, accelerate healing and reduce short- and long-term complications. The scalp appears to be increasingly used in clinical practice,
[...] Read more.
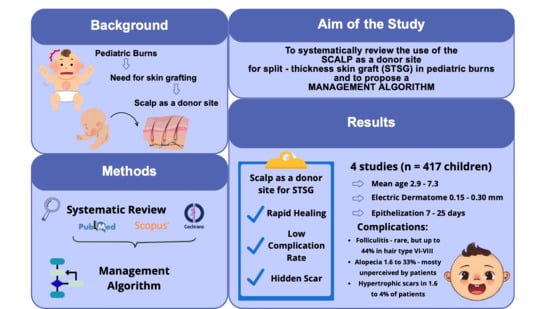
Background: Deep burns in pediatric population often require split-thickness skin grafts (STSGs) and the identification of an optimal donor site is crucial to minimize morbidity, accelerate healing and reduce short- and long-term complications. The scalp appears to be increasingly used in clinical practice, but evidence remains limited, despite the promise of novel bioengineering and regenerative approaches. Methods: A systematic review about the use of scalp for STSG in pediatrics was conducted across PubMed, Scopus, and Cochrane (2005–2025). Clinical outcomes considered were donor-site healing time, early and late complications, perioperative practices, and quality of scars. Results: Four studies met the inclusion criteria (n = 417, mean age 2.9–7.3 years) with follow-up periods up to 27 years. Epithelialization occurred between 7 and 25 days. Early complications included folliculitis (up to 44% in certain hair types) and delayed healing (n = 13; 52%). A rigorous harvesting technique is needed to avoid preventable complications. Late sequelae included alopecia (1.6% to 33%—the latter largely unperceived by patients) and hypertrophic scarring (1.6–4%). Scar quality was rated good in >80% of cases. Conclusions: Evidence supports the scalp as a safe, efficient, and cosmetically favorable donor site for pediatric STSG. Based on evidence and clinical experience, we propose the first structured scalp-donor management algorithm to optimize safety, reduce complications, and standardize perioperative care in the management of pediatric burns.
Full article
Graphical abstract
Open AccessArticle
Hand Involvement and Its Association with Burn Characteristics, Surgical Management, and Length of Stay in Paediatric Inpatients: A 10-Year Cross-Sectional Study from Western Australia
by
Lachlan James Madge, Lisa J. Martin, Emma Catherine Mill, Fiona M. Wood and Tiffany L. Grisbrook
Eur. Burn J. 2026, 7(2), 23; https://doi.org/10.3390/ebj7020023 - 30 Apr 2026
Abstract
►▼
Show Figures
Background: Hand burns are a key criterion for immediate referral to tertiary burn centres in Australia, New Zealand, and internationally, yet few studies have examined how paediatric burn epidemiology, surgical management, and length of stay (LOS) differ according to the extent of hand
[...] Read more.
Background: Hand burns are a key criterion for immediate referral to tertiary burn centres in Australia, New Zealand, and internationally, yet few studies have examined how paediatric burn epidemiology, surgical management, and length of stay (LOS) differ according to the extent of hand involvement. The objective of this study was to describe and compare the demographic profiles, burn injury characteristics, and clinical management between three groups: children with (1) burns involving only the hands, (2) burns involving the hands and other sites, and (3) burns not involving the hands who were admitted to the paediatric Burns Service of Western Australia (BSWA) over a 10-year period. Methods: This cross-sectional study included all burn admissions to the state paediatric burn unit between July 2012 and June 2022. Descriptive statistics and univariate regression used to compare groups. A multivariate log-linear regression model was used to assess the independent association between hand involvement and length of hospital stay, adjusting for identified confounders. T Results: Children with burns isolated to the hands were younger, had a smaller percentage of total body surface area (%TBSA), were more likely to have sustained contact or friction burns, and were more likely to undergo skin grafting procedures compared to those with burns involving the hands and other sites, and those with burns not involving the hands. Despite these differences, hand involvement was not identified as an independent predictor of initial LOS. Conclusion: Paediatric patients with hand burns did not have longer initial hospital admissions than those without hand involvement. Future research needs to assess longer term impacts of hand burns.
Full article

Figure 1
Open AccessArticle
Scheduled Bronchoscopy with Nebulized Heparin and N-Acetylcysteine in Burn Patients with Inhalation Injury: A Randomized Trial
by
Thai Ngoc Minh Nguyen, Nhu Lam Nguyen and Dinh Hung Tran
Eur. Burn J. 2026, 7(2), 22; https://doi.org/10.3390/ebj7020022 - 29 Apr 2026
Abstract
►▼
Show Figures
Inhalation injury (II) exacerbates burn mortality via obstructive fibrin casts. We evaluated a protocol combining scheduled flexible bronchoscopy (FOB) with nebulized heparin and N-acetylcysteine (NAC). This single-center, randomized controlled trial enrolled 76 mechanically ventilated adult burn patients with bronchoscopically confirmed II. The intervention
[...] Read more.
Inhalation injury (II) exacerbates burn mortality via obstructive fibrin casts. We evaluated a protocol combining scheduled flexible bronchoscopy (FOB) with nebulized heparin and N-acetylcysteine (NAC). This single-center, randomized controlled trial enrolled 76 mechanically ventilated adult burn patients with bronchoscopically confirmed II. The intervention (n = 38) comprised a 7-day protocol of scheduled FOB with alternating nebulized heparin (5000 IU) and 20% NAC every 4 h. Controls (n = 38) received standard care with on-demand FOB. Primary outcomes were 28-day mortality and day-7 Lung Injury Score (LIS). Unadjusted 28-day mortality was lower in the intervention group (57.9% vs. 81.6%; p = 0.025), alongside a decreased median day-7 LIS (1.0 vs. 1.38; p = 0.021). Respiratory mechanics improved significantly, demonstrating reduced driving pressure and increased static compliance (p < 0.001). However, in multivariable Cox regression, baseline injury severity independently predicted mortality, while the intervention indicated a non-significant hazard reduction trend (aHR = 0.66, 95% CI: 0.36–1.23). No systemic anticoagulation occurred. In conclusion, scheduled FOB with nebulized heparin and NAC improves respiratory mechanics and attenuates lung injury in II. Although unadjusted mortality decreased, baseline severity remains the primary mortality driver, suggesting this protocol is a physiologically beneficial adjunct requiring further multicenter validation. Trial registration: Thai Clinical Trials Registry, TCTR20260408001 (retrospectively registered).
Full article

Figure 1
Open AccessReview
From Evaporation to Edema: A Scoping Review of Physical and Biological Determinants of Early Fluid Distribution in Burn Patients
by
Sergio Arlati and Paolo Aseni
Eur. Burn J. 2026, 7(2), 21; https://doi.org/10.3390/ebj7020021 - 16 Apr 2026
Abstract
►▼
Show Figures
Background: Evaporative water loss from burn wounds is a major but often neglected component of early fluid requirements. Despite its physiological importance, no dedicated review has quantified acute post-burn evaporative water loss (TEWL) and its interaction with modern resuscitation strategies in over
[...] Read more.
Background: Evaporative water loss from burn wounds is a major but often neglected component of early fluid requirements. Despite its physiological importance, no dedicated review has quantified acute post-burn evaporative water loss (TEWL) and its interaction with modern resuscitation strategies in over 40 years. Recent mass-casualty burn events in specialized centers have re-emphasized the clinical importance of accurate early fluid balance, which is particularly challenging. Methods: A scoping review (PRISMA-ScR) of historical quantitative studies and 23 contemporary (2015–2025) adult major-burn resuscitation cohorts was conducted. Expected TEWL was derived from Lamke benchmarks; interstitial edema was estimated from the only available regression of simultaneous fluid input and 24 h weight change. A novel TEWL/edema ratio was tested against resuscitation volume (mL/kg/%TBSA) and the established input/output (I/O) ratio. Results: In the acute phase, the median TEWL normalized to total body surface area was 71 mL/m2/h [52–79 mL/m2/h], allowing for calculation of the TEWL/edema ratio. The TEWL/edema ratio was inversely correlated with the resuscitation fluid dose (R2 = 0.811) and the I/O ratio as well (R2 = 0.86), crossing unity at 2.85 mL/kg/%TBSA. A ratio > 1 signals high evaporative drive and/or possible under-resuscitation; a ratio < 1 alerts to fluid creep before significant weight gain. Conclusions: The TEWL/edema ratio is the first physiology-grounded, easily calculable resuscitation endpoint that complements urine output by providing insight into whether administered fluid is lost as obligatory evaporation or sequestered as edema. Routine estimation of expected TEWL and early monitoring of the TEWL/edema ratio may help guide goal-directed burn resuscitation, especially when early excision is delayed or impossible. Given the substantial inter-individual variability, the ratio derived from aggregate data should not be interpreted as a patient-specific predictor.
Full article

Figure 1
Open AccessPerspective
From Low-Resource Innovation to High-Resource Learning: Head-Mounted Cameras as a Tool to Strengthen Surgical and Burn Care Training
by
Einar Logi Snorrason, Fredrik Huss, Ali Modarressi and Morten Kildal
Eur. Burn J. 2026, 7(2), 20; https://doi.org/10.3390/ebj7020020 - 1 Apr 2026
Abstract
While the global surgeon deficit continues to demand urgent action, traditional “over-the-shoulder” teaching is increasingly constrained by infection-control demands and crowded operating rooms. Over the past four years, we integrated head-mounted smart cameras into reconstructive-surgery workshops across East Africa. Utilizing voice-controlled, stabilized video
[...] Read more.
While the global surgeon deficit continues to demand urgent action, traditional “over-the-shoulder” teaching is increasingly constrained by infection-control demands and crowded operating rooms. Over the past four years, we integrated head-mounted smart cameras into reconstructive-surgery workshops across East Africa. Utilizing voice-controlled, stabilized video technology, we provided trainees with a high-definition, wearer’s-perspective view that enhanced visualization without compromising the sterile field. Following remarkably high acceptance in Africa, we have initiated a pilot study at the National Burn Centre in Sweden to apply these lessons to a high-income setting. Our findings suggest that this technology improves surgical education while supporting infection-control stewardship through reduced overcrowding. This experience illustrates a reverse innovation, where tools refined under the logistical constraints of African operating theatres offer scalable solutions for universal challenges in surgical training and patient safety.
Full article
(This article belongs to the Special Issue Innovative Applications and Challenges of Emerging Materials and Technologies in Burn Treatment)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
The Diagnostic Value of Indocyanine Green in the Assessment of Depth of Burn Injuries: A Systematic Review
by
Marie K. Hilgarth, Samuel Knoedler, Gabriel Hundeshagen, Adriana C. Panayi, Bong-Sung Kim, Jochen-Frederick Hernekamp and Valentin F. M. Haug
Eur. Burn J. 2026, 7(1), 19; https://doi.org/10.3390/ebj7010019 - 19 Mar 2026
Abstract
Background: Accurate assessment of burn depth remains a clinical challenge and requires specific training. To improve diagnostic accuracy, various technical methods have been developed. This review summarizes current evidence on indocyanine green (ICG) fluorescence imaging for burn depth assessment and compares its performance
[...] Read more.
Background: Accurate assessment of burn depth remains a clinical challenge and requires specific training. To improve diagnostic accuracy, various technical methods have been developed. This review summarizes current evidence on indocyanine green (ICG) fluorescence imaging for burn depth assessment and compares its performance with clinical, histological, and alternative modalities such as Laser Doppler imaging (LDI). Methods: A systematic literature search was conducted in PubMed/MEDLINE, Cochrane and Google Scholar to identify studies evaluating burn depth using ICG fluorescence imaging. Studies from 1995 to 2024 were included if they compared ICG to at least one reference method (clinical assessment, biopsy, or other technical modalities). Data extraction was performed independently by two reviewers. Risk of bias was assessed using the Newcastle–Ottawa Scale. The study selection workflow is shown in the PRISMA 2020 flow diagram for systematic reviews. Results: Nine studies with a total of 151 patients, published between 1995 and 2024, met the inclusion criteria. Results were synthesized descriptively due to substantial methodological heterogeneity. Two studies reported high accuracy of ICG fluorescence imaging for identifying nonviable tissue and supporting surgical planning, although differentiation between superficial and deep partial-thickness burns (SPTBs/DPTBs) was inconsistent. In one study, ICGA-guided assessment reduced or avoided excision in 10 of 20 burn sites (50%). Yet heterogeneity in measurement protocols, cut-off values, and reference standards limited comparability across studies. Conclusions: Due to its limited accuracy in differentiating SPTBs and DPTBs, ICG imaging has restricted utility for burn depth assessment, though it may still offer intraoperative benefit during necrosectomy. Registration: PROSPERO International prospective register of SRs by the National Institute of Health Research (CRD420251161190).
Full article
(This article belongs to the Special Issue Innovative Applications and Challenges of Emerging Materials and Technologies in Burn Treatment)
►▼
Show Figures

Figure 1
Open AccessArticle
Prognostic Scoring Systems for Burns: A Comparative Analysis of Their Predictive Accuracies for Mortality in Burn Patients
by
Susanne Rein, Jule Schmiechen, Jochen Gille and Thomas Kremer
Eur. Burn J. 2026, 7(1), 18; https://doi.org/10.3390/ebj7010018 - 19 Mar 2026
Abstract
►▼
Show Figures
Introduction: Various scoring systems are applied to burn patients to assess the perioperative and mortality risks as well as comorbidities. Objective: The purpose of this study was to compare the predictive accuracies for mortality of different scoring systems: the Abbreviated Burn Severity Index
[...] Read more.
Introduction: Various scoring systems are applied to burn patients to assess the perioperative and mortality risks as well as comorbidities. Objective: The purpose of this study was to compare the predictive accuracies for mortality of different scoring systems: the Abbreviated Burn Severity Index (ABSI), Bogenhausen ABSI (BABSI), American Society of Anesthesiologists (ASA) classification, Charlson Comorbidity Index (CCI) and modified Frailty Index-5 (mFI-5). Materials and Methods: We retrospectively analyzed 644 burn patients treated at one burn center between September 2018 and May 2022. Results: Median scores were 5 (range: 1–16), 5 (range: 2–17.5), 2 (range: 1–5), 0 (range: 0–14) and 0 (range: 0–5) for the ABSI, BABSI, ASA, CCI and mFI-5, respectively. Significantly different median score results were observed between survivors and non-survivors: ABSI: 5 vs. 10; BABSI: 5 vs. 10.5; ASA: 2 vs. 4; CCI: 0 vs. 5; and mFI-5: 0 vs. 2 (p < 0.001 for all scores). Predictive accuracies were excellent for the BABSI (AUC = 0.963), ABSI (AUC = 0.952), and ASA (AUC = 0.916), whereas fair predictive accuracies were found for the CCI (AUC = 0.851) and mFI-5 (AUC = 0.760). Good calibration was observed for the BABSI, ABSI, CCI, and mFI-5, whereas calibration was poor for the ASA. Conclusion: All five scores significantly differentiate between survivors and non-survivors. However, the strongest discriminatory power and best calibration for mortality prediction were observed for the BABSI and ABSI scores. Therefore, the application of both scores is recommended in daily routine.
Full article

Figure 1
Open AccessArticle
From Injury to Independence: Investigating the Impact of Hand Burn Severity on Functional Outcomes in Children and Adolescents Followed for 24 Months After Injury—A Prospective Cohort Study
by
Ingrid Parry, Cameron Ward, Jeffrey Fine, David G. Greenhalgh, Michelle A. James and Katharine M. Hinchcliff
Eur. Burn J. 2026, 7(1), 17; https://doi.org/10.3390/ebj7010017 - 18 Mar 2026
Abstract
►▼
Show Figures
Background: Hand burns are common in children and can result in long-term functional impairment. The Hand Burn Severity (HABS) score is an anatomy-specific measure of hand burn severity, but its relationship to functional outcomes in pediatric patients has not been well defined. The
[...] Read more.
Background: Hand burns are common in children and can result in long-term functional impairment. The Hand Burn Severity (HABS) score is an anatomy-specific measure of hand burn severity, but its relationship to functional outcomes in pediatric patients has not been well defined. The purpose of this study was to determine whether HABS, measured at the time of injury, is associated with longitudinal upper extremity functional outcomes in children. Methods: We conducted a 24-month prospective longitudinal study of children aged 2–18 years with hand burns. Burn severity was determined using HABS at enrollment, and outcomes were measured using the Burn Outcomes Questionnaire (BOQ) and the eight-item Patient-Reported Outcomes Measurement Information System-Upper Extremity (PROMIS-UE8). Repeated-measures linear regression models evaluated associations between HABS and outcomes over time, adjusting for age, dominant- and bilateral-hand involvement, and surgery. Results: A total of 119 children with 165 hand burns were enrolled. Higher HABS scores, indicating more severe injury, were significantly associated with lower BOQ upper extremity function domain scores, indicating poorer health, at 2- and 6-months post burn, but not at later time points. Higher HABS scores were independently associated with lower patient-reported PROMIS-UE8 scores, indicating poorer health, across the 2-year follow-up period. Conclusions: These findings indicate that higher HABS scores at the time of injury are associated with poorer upper extremity outcomes, particularly in the early post-burn period, suggesting that HABS may help identify children who could benefit from closer monitoring or early rehabilitation planning.
Full article

Figure 1
Open AccessFeature PaperArticle
Surgical Management of Tracheostomy in Patients with Severe Burns and Cervical Involvement: Impact on Cervical Wound-Healing Disturbance
by
Julien-Moritz Thielmann, Wolfram Heitzmann, Michael Ried, Jan-Philipp Stromps, Maria von Kohout, Paul Christian Fuchs and Till Markowiak
Eur. Burn J. 2026, 7(1), 16; https://doi.org/10.3390/ebj7010016 - 10 Mar 2026
Abstract
►▼
Show Figures
Background: Major cervical burns often require tracheostomy (TT); however, it remains unclear whether TT timing relative to cervical wound coverage (WC) and the choice of coverage modality affect peristomal wound healing. Methods: In this retrospective single-center cohort study, we included 48 adults with
[...] Read more.
Background: Major cervical burns often require tracheostomy (TT); however, it remains unclear whether TT timing relative to cervical wound coverage (WC) and the choice of coverage modality affect peristomal wound healing. Methods: In this retrospective single-center cohort study, we included 48 adults with thermally induced cervical burns who underwent TT between 2015 and 2024 in a specialized burn ICU. Eleven patients died before decannulation and were excluded from the primary endpoint analysis. Cervical wound-healing disturbance (CWHD) as a primary endpoint was assessed in the remaining 37 patients, including 13 treated with advanced cervical dressings and 24 treated with split-thickness skin grafts (STSG). Results: CWHD occurred in 2/13 (15.4%) with advanced dressings and 11/24 (45.8%) after STSG. Within the grafted subgroup, complication rates did not differ significantly according to TT sequencing relative to WC, TT–WC interval, grafting technique (mesh vs. Meek), or tracheostoma closure method (all p > 0.05). In multivariable logistic regression, only cervical burn depth independently predicted CWHD. Conclusion: In patients with cervical burns requiring TT, burn depth/severity, rather than TT timing, grafting strategy, or closure technique, appears to drive peristomal wound complications, supporting individualized planning instead of rigid algorithms.
Full article

Figure 1
Open AccessArticle
Objective Longitudinal Monitoring of Burn Wound Area Using 3D Surface Scanning: A Pilot Study
by
Bibiána Ondrejová, Katarína Dudová, Monika Michalíková, Lucia Bednarčíková, Jozef Živčák, Tomáš Demčák and Peter Lengyel
Eur. Burn J. 2026, 7(1), 15; https://doi.org/10.3390/ebj7010015 - 6 Mar 2026
Abstract
Background: Burn assessment traditionally relies on visual inspection and 2D estimation, which introduces substantial variability in determining wound size and healing progression. Three-dimensional (3D) surface scanning offers a more objective alternative, yet the clinical utility of area-based metrics obtained from 3D surface data
[...] Read more.
Background: Burn assessment traditionally relies on visual inspection and 2D estimation, which introduces substantial variability in determining wound size and healing progression. Three-dimensional (3D) surface scanning offers a more objective alternative, yet the clinical utility of area-based metrics obtained from 3D surface data remains insufficiently defined. This pilot study aimed to evaluate structured-light 3D scanning for objective longitudinal quantification of the burn wound surface area and a description of area-based healing dynamics derived from repeated measurements. Methods: Eighteen patients with 43 acute thermal burns underwent serial structured-light scanning, followed by manual segmentation of wound regions and the calculation of absolute and percentage area reduction as well as TBSA-normalized metrics. Longitudinal monitoring was performed by comparing sequential 3D surface models acquired at defined clinical follow-ups, enabling the calculation of absolute area change (ΔA), percentage reduction, daily healing rate, and ΔTBSA%. Results: Baseline wound areas ranged from 7.27 to 2137.98 cm2. Percentage area reduction ranged from 5.25% to 92.30%. The overall reduction in burn burden (ΔTBSA) ranged from 0.07% to 12.94%. Large wounds tended to show rapid absolute area reduction (>100–300 cm2/day) during early follow-up, while small superficial burns frequently achieved >80% reduction within 10–15 days. Conclusions: These findings suggest that 3D surface scanning may support the objective longitudinal assessment of burn wound healing. This pilot provides a basis for future studies evaluating additional topographic parameters and broader clinical applications.
Full article
(This article belongs to the Special Issue Innovative Applications and Challenges of Emerging Materials and Technologies in Burn Treatment)
►▼
Show Figures

Figure 1
Open AccessArticle
Validity and Reliability of the Fatigue Severity Scale in an Adult Swedish Burn Population
by
Sara Enblom and Fredrik Huss
Eur. Burn J. 2026, 7(1), 14; https://doi.org/10.3390/ebj7010014 - 2 Mar 2026
Abstract
Background: A burn injury is a complex trauma often followed by complications, one of which is fatigue. The objective of this study was to validate the Fatigue Severity Scale (FSS) in an adult Swedish burn cohort. Methods: A prospective cohort study
[...] Read more.
Background: A burn injury is a complex trauma often followed by complications, one of which is fatigue. The objective of this study was to validate the Fatigue Severity Scale (FSS) in an adult Swedish burn cohort. Methods: A prospective cohort study was performed at the Burn Center at Uppsala University Hospital in Uppsala, Sweden. All patients who were registered for follow-up 6 months after their burn injury were asked to participate. Included patients completed questionnaires at 6 and 12 months postburn. Psychometric properties were investigated, including internal consistency (Cronbach’s alpha) and concurrent validity, comparing FSS with the Brief Fatigue Inventory (BFI), which was considered to be the “gold standard.” Convergent validity was investigated among the fatigue assessments and quality of life, depression/anxiety, and daily activities. Results: In total, 70 included patients attended both visits. FSS demonstrated high internal consistency (Cronbach’s alpha: 0.96 at both timepoints). There was high concurrent validity between FSS and BFI on both occasions (Spearman’s rho: 0.816 and 0.863, respectively), and the convergent validity was strong. Conclusions: The result indicates that the two fatigue scales correspond well to each other and that the FSS, therefore, is a valid and reliable assessment of fatigue in adult Swedish burn patients.
Full article
(This article belongs to the Special Issue 2nd Edition of Enhancing Psychosocial Burn Care)
►▼
Show Figures

Figure 1
Open AccessCase Report
Lessons Learned from Surgical Management of the Largest Burned Patient Covered with Skin Isograft from His Monozygotic Twin Brother
by
Maurice Mimoun, Marc Chaouat, Nathaniel Malca, Oren Marco, David Boccara and Kevin Serror
Eur. Burn J. 2026, 7(1), 13; https://doi.org/10.3390/ebj7010013 - 21 Feb 2026
Abstract
►▼
Show Figures
Background: Early excision and autologous split-thickness skin grafting are the cornerstone of surgical management in severe burn injuries. In patients with extremely extensive deep burns, the lack of available donor sites represents a major life-threatening limitation. In the exceptional situation of monozygotic twins,
[...] Read more.
Background: Early excision and autologous split-thickness skin grafting are the cornerstone of surgical management in severe burn injuries. In patients with extremely extensive deep burns, the lack of available donor sites represents a major life-threatening limitation. In the exceptional situation of monozygotic twins, skin isografting offers a unique solution by providing immunologically compatible skin without the risk of rejection. Case report: We report the case of a 33-year-old man who sustained flame burns involving 95% of his total body surface area, resulting in an extremely poor initial prognosis (ABSI 14, UBS 245). After early resuscitation and staged surgical excisions, the absence of sufficient autologous donor sites precluded definitive coverage using conventional techniques. On day 3, the existence of a monozygotic twin brother was identified. HLA genotyping confirmed complete identity, and skin donation was authorized by an independent ethics committee. Methods: Definitive wound coverage was achieved using staged split-thickness skin isografts harvested from the donor twin. Ultra-thin grafts (<0.2 mm) were obtained in three procedures (days 7, 11, and 45), primarily from the scalp, thighs, and back, and applied following sequential excisions. Results: All grafts survived without immunological rejection. Donor-site morbidity was minimal, with rapid healing and only mild residual hypopigmentation. The patient was discharged to rehabilitation on day 145. At 5-year follow-up, wounds were fully healed, functional outcome was satisfactory, and quality of life was good, with return to work and full independence. Conclusions: Skin isografting from a monozygotic twin is a rare but effective salvage strategy for patients with massive deep burns when autologous donor sites are insufficient, provided that ethical, legal, and donor safety considerations are rigorously addressed.
Full article

Figure 1
Open AccessArticle
The Influence of BMI on Mortality and Clinical Outcomes After Burns
by
Julia Kleinhapl, Rudy Ji, Lucineia Gainski Danielski, George Golovko, Alen Palackic, Philong Nguyen, Ludwik K. Branski, Steven E. Wolf, Celeste C. Finnerty and Oscar E. Suman
Eur. Burn J. 2026, 7(1), 12; https://doi.org/10.3390/ebj7010012 - 12 Feb 2026
Abstract
►▼
Show Figures
Background: Weight extremes are linked to morbidity, yet their impact on burn outcomes remains underinvestigated. Prior studies suggest an ‘obesity paradox’, showing survival benefits and better functional outcomes in obese patients. Methods: This study used the global real-world database TriNetX to assess the
[...] Read more.
Background: Weight extremes are linked to morbidity, yet their impact on burn outcomes remains underinvestigated. Prior studies suggest an ‘obesity paradox’, showing survival benefits and better functional outcomes in obese patients. Methods: This study used the global real-world database TriNetX to assess the association between body mass index (BMI) and clinical outcomes in adult burn patients, categorized using WHO definitions. After 1:1 propensity score matching for demographics, burn severity, and smoke inhalation injury, clinical outcomes were analyzed over a six-month period following burn injury. Outcomes included mortality, sepsis, pneumonia, acute kidney injury (AKI), cardiovascular events, graft complications, skin infections, and psychological impairment. Results: After matching, 9736 patients were included in the underweight versus normal weight comparison, 72,274 in overweight versus normal weight, 71,195 in obesity versus normal weight, and 9732 in underweight versus obesity. Underweight patients were associated with higher mortality and increased risks of sepsis, pneumonia, cardiovascular events, and psychological impairment. Overweight and obese patients showed higher survival rates and overall better clinical outcome associations. Conclusions: These findings are consistent with the previously described ‘obesity paradox’ in burn care and identify underweight burn patients as a distinct high-risk subgroup.
Full article

Figure 1
Open AccessArticle
Effect of a 6-Week Structured Exercise Intervention on TNF-α During the Chronic Recovery Phase of a Burn Injury Compared to Regular Daily Activities: A Pilot Randomised Cross-Over Trial
by
Tyler Jerome Osborne, Grant Rowe, Dale W. Edgar, Mark Fear, Fiona M. Wood, Timothy Fairchild, Brook Galna, Pippa Kenworthy and Brad Wall
Eur. Burn J. 2026, 7(1), 11; https://doi.org/10.3390/ebj7010011 - 12 Feb 2026
Abstract
►▼
Show Figures
Background: Burn injury induces a prolonged inflammatory response that may contribute to long-term metabolic dysfunction. Exercise is known to reduce inflammation in various clinical populations; however, its effect on chronic post-burn inflammation remains unclear. This crossover trial investigated the impact of a 6-week
[...] Read more.
Background: Burn injury induces a prolonged inflammatory response that may contribute to long-term metabolic dysfunction. Exercise is known to reduce inflammation in various clinical populations; however, its effect on chronic post-burn inflammation remains unclear. This crossover trial investigated the impact of a 6-week exercise intervention on tumour necrosis factor-alpha (TNF-α) in adults with non-severe burns sustained more than one year prior. Methods: Twenty-one participants were randomised to complete either a 6-week exercise program or a control period first, separated by a 4-week washout. The exercise program comprised three supervised sessions per week of combined resistance and cardiovascular training. Primary (TNF-α) and secondary (muscle strength, cardiovascular fitness) outcomes were assessed pre- and post-intervention. Results: Fifteen participants completed the protocol with high adherence (90.4%). Exercise significantly improved quadriceps strength and cardiovascular fitness, confirming the intervention’s safety and efficacy in this cohort. However, TNF-α concentrations were not elevated at baseline and did not significantly change following exercise compared with control (mean difference: +0.5 pg·mL−1, p = 0.249). Exercise is safe and beneficial for non-severely burned patients who sustained their injury > 1 year ago. However, inflammation was not elevated in this cohort, precluding our ability to test the effects of exercise on chronic inflammation.
Full article

Figure 1
Open AccessCase Report
Intravascular Rewarming in Major Burns: A Rare but Serious Catheter-Related Complication
by
Theodora Ligomenou, Eirini Nikolaidou, Argiro Pipinia, Georgios Trellopoulos, Stavros Galanis, Myrto Tzimou, Georgia Vasileiadou and Sophia Papadopoulou
Eur. Burn J. 2026, 7(1), 10; https://doi.org/10.3390/ebj7010010 - 9 Feb 2026
Abstract
Introduction: Patients with major burn injuries are highly susceptible to hypothermia due to extensive skin loss, aggressive fluid resuscitation, repeated surgical procedures, and exposure during wound care. Hypothermia is associated with coagulation disorders, increased blood loss, impaired immune response, prolonged hospitalization, and
[...] Read more.
Introduction: Patients with major burn injuries are highly susceptible to hypothermia due to extensive skin loss, aggressive fluid resuscitation, repeated surgical procedures, and exposure during wound care. Hypothermia is associated with coagulation disorders, increased blood loss, impaired immune response, prolonged hospitalization, and increased mortality. When conventional warming strategies fail, intravascular temperature management systems may be employed, although they carry risks inherent to central venous catheters. Case Report: We report the case of a 26-year-old male with 66% total body surface area flame burns and inhalational injury, admitted to the Burns Intensive Care Unit with persistent hypothermia despite standard warming measures. An intravascular temperature management catheter was inserted via the femoral vein and successfully restored normothermia. Due to clinical instability, the catheter remained in situ beyond the recommended duration. During attempted catheter removal, significant resistance was encountered, raising concern for mechanical malfunction. Imaging confirmed catheter entrapment without fracture. Multidisciplinary management involving vascular surgery and interventional radiology enabled successful removal using endovascular snare techniques. A detached balloon fragment was identified and secured with venous stenting. Conclusions: This report describes the first documented case of complicated removal of an intravascular warming catheter due to balloon detachment in burn patients. Physicians using these devices should be aware of this possible complication and be prepared for its management.
Full article
(This article belongs to the Special Issue Innovative Applications and Challenges of Emerging Materials and Technologies in Burn Treatment)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Special Issues
Special Issue in
EBJ
2nd Edition of Enhancing Psychosocial Burn Care
Guest Editors: Anna Pittermann, Koen MaertensDeadline: 31 October 2026






