-
 The Impact of Intraoperative Traffic and Door Openings on Surgical Site Infections: An Umbrella Review
The Impact of Intraoperative Traffic and Door Openings on Surgical Site Infections: An Umbrella Review -
 Examining the Most Influential Publications Regarding Tracheal Reconstruction: A Bibliometric Review
Examining the Most Influential Publications Regarding Tracheal Reconstruction: A Bibliometric Review -
 Clinical and Demographics Aspects of Foot Angioleiomyomas: Case Reports and Systematic Review
Clinical and Demographics Aspects of Foot Angioleiomyomas: Case Reports and Systematic Review -
 Venous Malformation of the Maxilla: A Systematic Review and a Report of an Unusual Case
Venous Malformation of the Maxilla: A Systematic Review and a Report of an Unusual Case
Journal Description
Surgeries
Surgeries
is an international, peer-reviewed, open access journal on findings and developments in surgery published quarterly online by MDPI. The Academy of Surgical Research (ASR) and the Italian Society of Hand Surgery (SICM) are affiliated with Surgeries and their members receive discounts on the article processing charges.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), Scopus, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 24.4 days after submission; acceptance to publication is undertaken in 3.7 days (median values for papers published in this journal in the second half of 2025).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.1 (2024);
5-Year Impact Factor:
1.0 (2024)
Latest Articles
From Imaging to Implementation: Computed-Tomography-Based Surgical Artificial Intelligence Using DIEP Flap Reconstruction as a Model System
Surgeries 2026, 7(2), 61; https://doi.org/10.3390/surgeries7020061 - 20 May 2026
Abstract
Background/Objectives: Artificial intelligence (AI) is increasingly proposed to improve surgical planning, guidance, and postoperative surveillance. Yet many promising applications remain disconnected from the full surgical pathway and the feasible limitations of clinical deployment. In contrast to prior reviews that primarily catalog AI use
[...] Read more.
Background/Objectives: Artificial intelligence (AI) is increasingly proposed to improve surgical planning, guidance, and postoperative surveillance. Yet many promising applications remain disconnected from the full surgical pathway and the feasible limitations of clinical deployment. In contrast to prior reviews that primarily catalog AI use cases, this review combines the literature to define the translational pathway—from label design through staged validation to workflow integration—required for clinically deployable computed tomography (CT)-based surgical AI. CT and particularly computed tomography angiography (CTA) are especially usable sources for surgical AI because they provide a standardized three-dimensional anatomic model that is already embedded in many clinical workflows. In autologous breast reconstruction, deep inferior epigastric perforator (DIEP) flap CTA offers an unusually strong model system: the anatomy is discrete, surgeon decisions are actionable, and downstream operative and postoperative outcomes are measurable. These characteristics make DIEP reconstruction suitable not only for technical model development, but also for exacting testing of how CT-based AI should be annotated, validated, displayed, and governed. Methods: This focused narrative review combines evidence across the surgical workflow, spanning preoperative planning and risk stratification, intraoperative support, and postoperative monitoring. Reporting standards, implementation frameworks, governance, and regulatory sources were also considered when directly relevant to clinical deployment. Results: Across the available literature on breast reconstruction with the DIEP flap, preoperative CTA has been associated with reductions in operative time of approximately 54–76 min in individual studies. Semi-automated perforator mapping can reduce review time from 2 to 3 h to approximately 30 min. Intraoperative extended-reality tools and surgeon-facing navigation systems illustrate the importance of the ‘last mile’ of translation, while postoperative monitoring models show how imaging-linked data can support a closed-loop learning system. Across these stages, recurring limits include target mismatch, weak external validation, protocol variability, inconsistent reporting, limited subgroup analysis, and inadequate integration of economic and governance considerations. Conclusions: We argue that the next important step is not a generic autonomous model, but a clinically deployable DIEP-CTA-AI program. The practical blueprint proposed here is staged: structured anatomical labels, separate imaging, surgeons’ decisions, and outcome reference standards, dense intermediate endpoints, retrospective and external validation, reader studies, prospective silent deployment, and workflow-impact assessment. If implemented in this way, DIEP flap CTA can serve as a practical blueprint for CT-based AI translation in surgery more broadly.
Full article
(This article belongs to the Special Issue The Application of Artificial Intelligence in Surgical Procedures)
Open AccessArticle
Reconstruction of Elbow Soft-Tissue Defects Using the Reverse Lateral Arm Flap: A Case Series
by
Pasquale Zona, Luca Folini, Alfio Luca Costa, Daniele Brunelli, Francesca Mazzarella, Franco Bassetto and Cesare Tiengo
Surgeries 2026, 7(2), 60; https://doi.org/10.3390/surgeries7020060 - 11 May 2026
Abstract
Background: Complex elbow soft-tissue defects often combine exposed critical structures, unstable scars, and high mechanical stress, making durable coverage and early mobilization challenging. Among regional options, the reverse lateral arm flap provides thin fasciocutaneous tissue based on a reliable collateral circulation and preserves
[...] Read more.
Background: Complex elbow soft-tissue defects often combine exposed critical structures, unstable scars, and high mechanical stress, making durable coverage and early mobilization challenging. Among regional options, the reverse lateral arm flap provides thin fasciocutaneous tissue based on a reliable collateral circulation and preserves major forearm vessels. The aim of this study was to report our single-center experience with the pedicled reverse lateral arm flap for elbow soft-tissue reconstruction, focusing on stable coverage, donor-site morbidity, and functional recovery. Methods: A retrospective single-center case series was conducted at the Division of Plastic Surgery, University Hospital of Padua, Italy. All consecutive patients treated between 2013 and 2023 with a pedicled reverse lateral arm flap for elbow soft-tissue defects were included. Recorded variables included defect etiology, donor-site management, complications, range of motion, and follow-up. Elbow flexion–extension was recorded clinically preoperatively and at last follow-up. Minimum follow-up was 12 months in all patients. Results: Seven patients underwent reconstruction. Defect etiology was burn-related in four cases, shotgun trauma in one, crush injury in one, and melanoma resection in one. All defects were covered with a pedicled reverse lateral arm flap. All flaps survived completely without partial necrosis or flap-related reoperation. Donor-site closure was primary in four patients and required split-thickness skin grafting in three. One patient developed donor-site keloid, and one had donor-site skin-graft partial loss with delayed healing. Elbow flexion–extension improved in all seven cases, with a median gain in arc of motion of 25° (range 15–41°). Conclusions: In this series, the reverse lateral arm flap provided complete coverage of selected elbow defects with preserved motion and limited donor-site morbidity at a minimum follow-up of 12 months. Our findings suggest that it may represent a useful regional option in selected posterior and lateral elbow defects, particularly in post-burn and traumatic settings where thin vascularized tissue is needed, and free-flap reconstruction may be avoidable.
Full article
(This article belongs to the Special Issue Feature Papers in Hand Surgery and Research)
►▼
Show Figures

Figure 1
Open AccessCase Report
Total Reconstruction of the Donor Site After Toe-to-Thumb Transfer: Introducing a Novel Technique
by
Pierfrancesco Pugliese, Serafina Pepe, Mara Franza and Adriana Cordova
Surgeries 2026, 7(2), 59; https://doi.org/10.3390/surgeries7020059 - 8 May 2026
Abstract
Traumatic thumb loss causes severe functional impairment, as the thumb provides approximately 40% of total hand function. Toe-to-thumb transfer remains the gold standard for thumb reconstruction, yet donor site morbidity represents a significant functional and aesthetic limitation. A total thumb reconstruction using a
[...] Read more.
Traumatic thumb loss causes severe functional impairment, as the thumb provides approximately 40% of total hand function. Toe-to-thumb transfer remains the gold standard for thumb reconstruction, yet donor site morbidity represents a significant functional and aesthetic limitation. A total thumb reconstruction using a “trimmed” right great toe transfer, combined with immediate donor site reconstruction using a free SCIP (superficial circumflex iliac perforator) flap and iliac crest bone graft. The flap was designed as a tubular skin island to create a neo-hallux with optimal contour and volume, minimizing visible scarring and avoiding microcirculatory compression. The patient, a 33-year-old man with post-traumatic thumb avulsion, underwent delayed reconstruction three months after injury. The postoperative course was uneventful, with no vascular or wound complications. At 12 months, he resumed full ambulation and manual activities, including motorcycle driving and work tasks. Baropodometric analysis demonstrated symmetric load distribution and gait dynamics. Thumb opposition was satisfactory (Kapandji score: seven); the patient rated the aesthetic results as excellent. This case demonstrates that SCIP flap reconstruction with iliac crest bone graft enables complete functional and aesthetic restoration of the great toe donor site after total toe transfer. Compared to previous techniques using cross-flaps, skin grafts, or peroneal flaps, this approach minimizes morbidity, optimizes cosmetic outcomes, and preserves gait. Although representing a single case, this constitutes the first documented instance of total hallux reconstruction following toe-to-thumb transfer, emphasizing the importance of the foot as a functional and aesthetic unit and the need for donor-site preservation in microsurgical reconstructive planning.
Full article
(This article belongs to the Section Hand Surgery and Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Trapeziectomy with Ligament Reconstruction and Tendon Interposition Versus Transosseous Suture Suspensionplasty for Thumb Trapeziometacarpal Osteoarthritis: A Retrospective Comparative Study
by
Morena Anna Basso, Simona Scarpa, Alessio Bernasconi, Andrea Poggetti, Lucian Lior Marcovici and Francesco Smeraglia
Surgeries 2026, 7(2), 58; https://doi.org/10.3390/surgeries7020058 - 7 May 2026
Abstract
Background: Several surgical techniques are available for the treatment of thumb trapeziometacarpal (TMC) osteoarthritis. Trapeziectomy with ligament reconstruction and tendon interposition (LRTI) is a widely accepted procedure, while suspensionplasty techniques have been introduced to improve first metacarpal stability after trapeziectomy. A simplified transosseous
[...] Read more.
Background: Several surgical techniques are available for the treatment of thumb trapeziometacarpal (TMC) osteoarthritis. Trapeziectomy with ligament reconstruction and tendon interposition (LRTI) is a widely accepted procedure, while suspensionplasty techniques have been introduced to improve first metacarpal stability after trapeziectomy. A simplified transosseous suture suspensionplasty (SUSP) has recently been introduced as an alternative to implant-based constructs, but comparative clinical data remain limited. This study aimed to compare the clinical and functional outcomes between LRTI and SUSP techniques in patients with TMC osteoarthritis. Methods: A retrospective comparative study was conducted on 54 consecutive patients treated surgically for TMC osteoarthritis between 2018 and 2022. Thirty-three patients underwent trapeziectomy with ligament reconstruction and tendon interposition (LRTI group), and 21 underwent trapeziectomy with transosseous suture suspensionplasty (SUSP group). At a minimum follow-up of 2 years, 44 patients were available for evaluation. Assessments were performed using DASH, 10 cm VAS, key pinch strength, Kapandji score, and radial/palmar abduction. Results: At 2 years, there were no significant between-group differences in DASH (median 4 vs. 16.5; p = 0.190), VAS (2.0 ± 2.1 vs. 2.9 ± 2.3; p = 0.235), key pinch (median 4 vs. 3 kg; p = 0.136), Kapandji score, or abduction. Both groups improved significantly over time in DASH and VAS (p < 0.001). Key pinch increased progressively in LRTI group (p < 0.001) but showed less consistent change in SUSP group. Conclusions: Both techniques provided comparable mid-term clinical and functional outcomes in patients with TMC osteoarthritis. No clear clinical advantage of suspensionplasty over tendon interposition was demonstrated. Transosseous suture suspensionplasty represents a valid alternative, while tendon interposition arthroplasty remains a reliable reference technique.
Full article
(This article belongs to the Section Hand Surgery and Research)
►▼
Show Figures
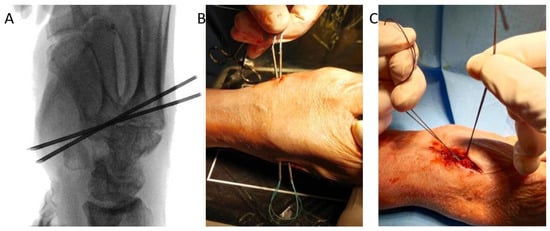
Figure 1
Open AccessArticle
Examining the Relationships and Differences of Satisfaction, Kinesiophobia, and Pain Between Rehabilitation Phases in Patients After Total Knee Replacement
by
Anna Christakou, Danai Georgitsi, Manolis Papadopoulos, Nikolaos Zacharakis and Panayiotis Papagelopoulos
Surgeries 2026, 7(2), 57; https://doi.org/10.3390/surgeries7020057 - 5 May 2026
Abstract
Background/objectives: Total knee arthroplasty is one of the most commonly performed orthopedic procedures of the lower extremities, primarily for patients with osteoarthritis or rheumatoid arthritis. Despite its widespread use, evidence remains limited regarding the association between patient satisfaction, kinesiophobia, and pain during the
[...] Read more.
Background/objectives: Total knee arthroplasty is one of the most commonly performed orthopedic procedures of the lower extremities, primarily for patients with osteoarthritis or rheumatoid arthritis. Despite its widespread use, evidence remains limited regarding the association between patient satisfaction, kinesiophobia, and pain during the early postoperative period. The purpose of the present study was to examine the relationships and differences among satisfaction, kinesiophobia, and pain in hospitalized patients following total knee arthroplasty, as well as to compare these variables across four postoperative time points. Methods: A total of 41 patients, aged 65–85 years, participated in this study. Patient satisfaction was assessed using a structured satisfaction questionnaire, kinesiophobia was assessed using the Greek version of Tampa Scale of Kinesiophobia, and pain was assessed using the Visual Analogue Scale. Measurements were obtained on the first postoperative day, on the day of hospital discharge, fifteen days after discharge, and four weeks after discharge. Normality was assessed using the Shapiro–Wilk test, indicating non-normally distributed data. The relationship between the variables were examined using Spearman’s correlation coefficient. Comparisons between the four postoperative time points were conducted using the Friedman test with Kendall’s W for effect size estimation, followed by Wilcoxon post hoc analyses with Bonferroni corrections. Results: The results showed that a significant negative correlation between satisfaction and kinesiophobia was observed at the fourth phase (r = −0.41, p = 0.04). Satisfaction was also negatively correlated with pain from the third to the fourth phase (r = −0.41, p = 0.008), whereas kinesiophobia demonstrated a significant positive correlation with pain from the second to the fourth phase (r = 0.47–0.56, p = 0.002). Friedman test comparisons revealed a significant increase in satisfaction over time (χ2 (3) = 13.88, p = 0.003), a significant progressive decrease in kinesiophobia with a moderate effect size (χ2 (3) = 76.40, p < 0.001; Kendall’s W = 0.62), and a significant progressive reduction in pain with a large effect size (χ2 (3) = 89.60, p < 0.001; Kendall’s W = 0.73). Conclusions: These findings indicate that satisfaction, kinesiophobia, and pain are significantly interrelated during the early postoperative period following total knee arthroplasty. Further studies with larger samples and longer follow-up periods are required to confirm these associations and support the development of targeted rehabilitation strategies.
Full article
(This article belongs to the Special Issue Advances in Total Hip and Knee Arthroplasty)
Open AccessCase Report
Delayed Presentation of Nasal Glioma—Case Report and Literature Review
by
Prabhpreet Kaur, Yilong Wu, Henry K. K. Tan, Sze Jet Aw, Wan Tew Seow and Sharon Y. Y. Low
Surgeries 2026, 7(2), 56; https://doi.org/10.3390/surgeries7020056 - 4 May 2026
Abstract
►▼
Show Figures
Background: Nasal glioma (NG), also known as nasal glial heterotopia, is an extremely rare congenital anomaly characterized by the presence of mature glial tissue outside the cranial cavity. Most patients present with midline craniofacial malformations at birth. However, a small subset of them
[...] Read more.
Background: Nasal glioma (NG), also known as nasal glial heterotopia, is an extremely rare congenital anomaly characterized by the presence of mature glial tissue outside the cranial cavity. Most patients present with midline craniofacial malformations at birth. However, a small subset of them is entirely intranasal and have no accompanying visible features. We present an unusual case of delayed diagnosis of NG, in tandem with a systematic literature review. Methods: A previously well 2-year-old male presented with obstructive apnea secondary to an intranasal mass. Neuroimaging of his paranasal sinuses demonstrated a bony defect in the anterior cribriform plate with herniation of a soft tissue structure into the right nasal cavity. He underwent craniotomy, total excision of the lesion and repair of skull base defect. His postoperative period was uneventful with resolution of his symptoms. Histology reported infiltrates of mature glial tissue with rare neurons forming the excised nasal mass. We conducted a structured literature review using PRISMA guidelines to evaluate clinical features of NG. Results: A comprehensive search of PubMed and Scopus databases featured 133 published cases of NG relevant to our case. Overall, NG is more common in males, with most cases diagnosed within the first year of life. Clinical presentation usually involved an external nasal mass (82.8%) and/or respiratory symptoms (28.7%), with prenatal detection reported in a subset of cases. Magnetic resonance imaging was the preferred imaging modality. Surgical excision was the mainstay of treatment. Postoperative outcomes were favorable in most patients, with 84.7% showing no complications or recurrence. Incomplete excision was associated with recurrence (10%). Conclusions: We present an intranasal case of NG with late diagnosis that was successfully managed with surgery. Our review underscores the importance of early imaging, accurate diagnosis, and complete surgical resection for best outcomes in affected children.
Full article

Figure 1
Open AccessCase Report
Extracorporeal Membrane Oxygenation in Pregnancy and the Postpartum Period: Two Case Reports and Narrative Review
by
Mitch Daniel, Alex Cao, Suvikram Puri, Joby Chandy, Maksim Federau, Carlos Miranda, Christopher Ketchey, David Koontz, Cameron Dang, Nicholas Martini, John Hodgson, Jeffrey Weiss, Tanjina Jalil and Enrico Camporesi
Surgeries 2026, 7(2), 55; https://doi.org/10.3390/surgeries7020055 - 30 Apr 2026
Abstract
In recent times, extracorporeal membrane oxygenation is increasingly employed in pregnant and postpartum patients with severe cardiopulmonary failure. This article presents two illustrative cases from our tertiary care center, highlighting the complexities of obstetric extracorporeal membrane oxygenation management. These cases are described within
[...] Read more.
In recent times, extracorporeal membrane oxygenation is increasingly employed in pregnant and postpartum patients with severe cardiopulmonary failure. This article presents two illustrative cases from our tertiary care center, highlighting the complexities of obstetric extracorporeal membrane oxygenation management. These cases are described within a synthesis of recent systematic reviews, registry data, and large case series focusing on maternal and fetal outcomes, extracorporeal membrane oxygenation modality impacts, timing of intervention, complication profiles, and anesthetic considerations. The concordance and contrasts between these cases and the existing literature underscore the evolving indications, improving survival rates, and critical perioperative management issues. Emphasis on multidisciplinary care and planning remains essential to optimize outcomes in this unique patient population.
Full article
(This article belongs to the Special Issue Postoperative Support of CPAP for Respiratory Depression)
Open AccessCase Report
Laparoscopic Resection of Oesophagal Bronchogenic Cyst During Nissen Fundoplication Procedure
by
Jarosław Lichota, Piotr Rękawek, Jan Pawlus, Piotr Janik and Tadeusz Sulikowski
Surgeries 2026, 7(2), 54; https://doi.org/10.3390/surgeries7020054 - 29 Apr 2026
Abstract
Background/Objectives: Bronchogenic cysts are rare congenital cystic lesions caused by congenital bronchopulmonary dysplasia; incidental discovery during preoperative investigations or unrelated procedures raises operative management questions. We report successful concurrent resection during laparoscopic Nissen fundoplication. Methods/Case presentation: During elective laparoscopic Nissen fundoplication, a cystic
[...] Read more.
Background/Objectives: Bronchogenic cysts are rare congenital cystic lesions caused by congenital bronchopulmonary dysplasia; incidental discovery during preoperative investigations or unrelated procedures raises operative management questions. We report successful concurrent resection during laparoscopic Nissen fundoplication. Methods/Case presentation: During elective laparoscopic Nissen fundoplication, a cystic lesion adjacent to the distal oesophagus, previously identified on preoperative imaging, was encountered. Laparoscopic enucleation was performed without compromising the integrity of the gastrointestinal tract or the cyst wall, and the 360° fundoplication was then completed. The specimen was sent for histopathology. Results: Resection was completed without conversion. Histology showed a glandular epithelial lining without features of malignancy, consistent with a bronchogenic cyst. The patient recovered uneventfully with resolution of reflux symptoms. Conclusions: Distal oesophageal bronchogenic cysts accessible via the hiatus can be safely enucleated during laparoscopic Nissen fundoplication in experienced hands, allowing definitive treatment in a single operation. Careful dissection, assessment of gastrointestinal patency and integrity, and histopathological confirmation are essential.
Full article
(This article belongs to the Section Minimally Invasive and Robotic Surgery Group)
►▼
Show Figures
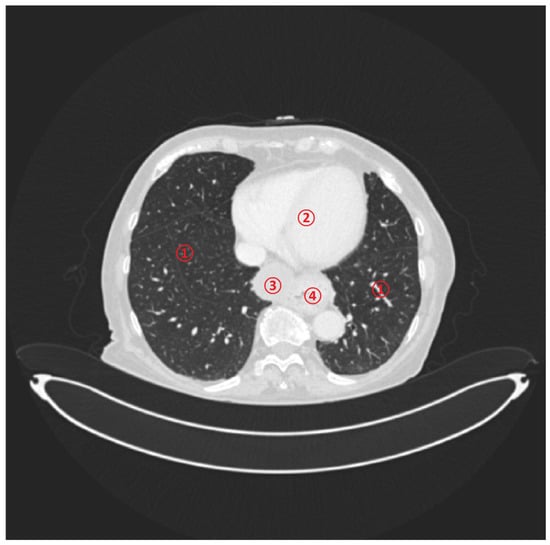
Figure 1
Open AccessArticle
Dual Mobility Prostheses Versus Suspension Arthroplasty for the Treatment of the First Carpometacarpal Joint Osteoarthritis: A 2-Year Follow-Up Prospective Study
by
Matteo Guzzini, Giulia Frittella, Giorgio Carrozzi, Rocco De Vitis and Leopoldo Arioli
Surgeries 2026, 7(2), 53; https://doi.org/10.3390/surgeries7020053 - 25 Apr 2026
Abstract
Background/Objectives: Trapeziometacarpal osteoarthritis (TMC OA) is a common disabling condition. This study compared clinical and radiographic outcomes of trapeziectomy with suspension arthroplasty and dual mobility TMC joint replacement in a prospective comparative cohort study design. Methods: A prospective comparative study was
[...] Read more.
Background/Objectives: Trapeziometacarpal osteoarthritis (TMC OA) is a common disabling condition. This study compared clinical and radiographic outcomes of trapeziectomy with suspension arthroplasty and dual mobility TMC joint replacement in a prospective comparative cohort study design. Methods: A prospective comparative study was conducted on 122 patients contributing 129 hands with Eaton–Littler stage II–III TMC osteoarthritis. Patients were treated with trapeziectomy with suspension arthroplasty (58 patients, 60 hands) or TMC joint replacement with a dual mobility prosthesis (64 patients, 69 hands), based on surgical indication and shared decision-making. Clinical and radiographic evaluations were performed up to 24 months postoperatively. Results: Both techniques significantly improved pain, function, range of motion, and strength (p < 0.05). Joint replacement provided faster pain relief and functional recovery, with superior strength at all follow-up points. At 12 months, pain and functional outcomes were comparable between groups. No implant loosening or failures were observed. Conclusions: Both surgical techniques are effective for TMC osteoarthritis. Dual mobility TMC joint replacement allows faster recovery and greater strength, while achieving comparable mid-term clinical outcomes to suspension arthroplasty.
Full article
(This article belongs to the Section Hand Surgery and Research)
Open AccessSystematic Review
Robotic Surgery Conservative Approaches for Uterine Adenomyosis: A Systematic Review
by
Mario Ardovino, Davide Pisani, Pasquale De Franciscis, Ester Picone, Antonio Conte, Fatima Cherifi, Maria Izzo, Emanuele Amabile and Marco La Verde
Surgeries 2026, 7(2), 52; https://doi.org/10.3390/surgeries7020052 - 23 Apr 2026
Abstract
Background/Objectives: Adenomyosis is a common disorder of the uterus in those of reproductive age. Robotic-assisted surgery has been adopted to address the technical challenges of adenomyomectomy. This systematic review evaluated the current evidence regarding the feasibility, safety, and clinical outcomes of robotic-assisted
[...] Read more.
Background/Objectives: Adenomyosis is a common disorder of the uterus in those of reproductive age. Robotic-assisted surgery has been adopted to address the technical challenges of adenomyomectomy. This systematic review evaluated the current evidence regarding the feasibility, safety, and clinical outcomes of robotic-assisted conservative surgery for uterine adenomyosis. Methods: A systematic review of literature was performed on five databases, from the beginning to 21 December 2025, to identify studies reporting robotic-assisted uterus-sparing surgical approaches to adenomyosis. Data were collected on patient characteristics, surgical techniques used, pre- and post-operative pain, fertility outcomes, and complications. Risk of bias was evaluated using the ROBINS-I framework. Results: A total of 514 articles were found; six studies met the inclusion criteria. Most included studies were small and retrospective. The operative time ranged from 279 to 147 min. Mean blood loss ranged between 25 and 296 mL with a low rate of conversion and perioperative complications. Dysmenorrhea improved after surgery as reflected by the post operative visual analog scale pain score and serum CA-125 level. Few reproductive data were collected about successive spontaneous pregnancies. Risk of bias was serious or moderate in all studies included. Conclusions: Robotic-assisted conservative surgery for adenomyosis may represent a feasible and safe option for women with symptomatic adenomyosis who wish preserve the uterus, with a positive impact on patients’ symptoms. Large prospective, multicenter studies with standardized protocols and long-term follow-up are needed to clarify the real impact of robotic surgery in adenomyosis management.
Full article
(This article belongs to the Section Minimally Invasive and Robotic Surgery Group)
►▼
Show Figures
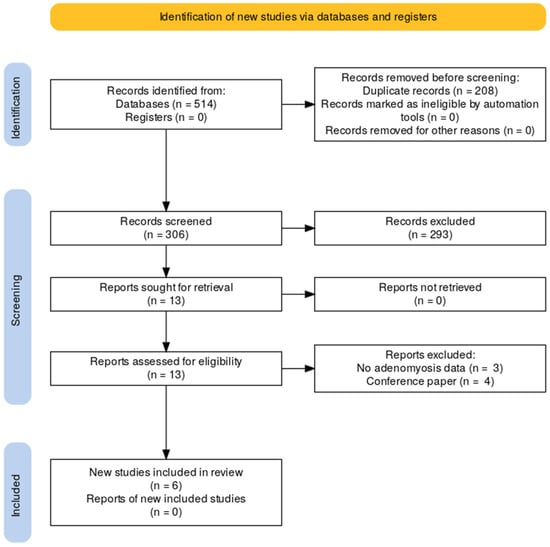
Figure 1
Open AccessArticle
Direct Antiviral Agents May Obviate the Need for Liver Transplantation for HCV Cirrhosis by the End of the Decade
by
Nathanael Haynes, Allyson Cochran, Maria Baimas-George, William Archie, Namratha Mylarapu, Vincent Casingal, Jose Soto, Philippe Zamor, Andrew DeLemos, Paul Schmeltzer, Steven Zacks, Natasha Adlakha, Roger Denny, Mark Russo, Lon Eskind and Dionisios Vrochides
Surgeries 2026, 7(2), 51; https://doi.org/10.3390/surgeries7020051 - 23 Apr 2026
Abstract
Background: Hepatitis C viral infection (HCV) has historically been a leading indication for liver transplantation (LTx), primarily due to its progression to cirrhosis and hepatocellular carcinoma (HCC). However, the advent of direct-acting antiviral agents (DAAs) over a decade ago has revolutionized HCV treatment,
[...] Read more.
Background: Hepatitis C viral infection (HCV) has historically been a leading indication for liver transplantation (LTx), primarily due to its progression to cirrhosis and hepatocellular carcinoma (HCC). However, the advent of direct-acting antiviral agents (DAAs) over a decade ago has revolutionized HCV treatment, achieving sustained virologic response (SVR) in over 90% of patients and potentially altering LTx indications. Aim: To investigate the impact of DAAs on HCV-related indications, with or without HCC, and model future trends in LTx indications. Methods: We retrospectively reviewed 1504 liver transplants performed between 2000 and 2024 at a single center. Patients were categorized into three cohorts: HCV-only, HCC-only, and HCC with HCV co-infection (HCC/HCV). Relative transplant volumes by-year, post-operative outcomes, and HCC recurrence rates were analyzed across pre- and post-DAA eras. ARIMA modeling was employed to project trends in transplant indications through the year 2030. Results: The proportion of transplants for HCV alone declined by 82.3% from 2015 to 2020, while HCC/HCV transplants decreased by 68.8%. Conversely, the total number of transplants for HCC alone increased during this period, with a modest proportional decrease of 8.3% from 2015 to 2020. ARIMA modeling suggests that by 2030, LTxs for HCV alone may be nearly eliminated. The projected proportion of transplants conducted for HCC alone remains the highest of all three study indications at 4.3%. Conclusions: DAAs have reduced LTx due to HCV. By 2030, LTx for HCV-related cirrhosis, particularly without HCC, may be obviated. This underscores the need to reevaluate allocation for emerging oncologic indications.
Full article
(This article belongs to the Special Issue Novel Insights into Liver Transplantation Surgery)
►▼
Show Figures

Figure 1
Open AccessArticle
Pediatric and Adolescent Pancreatic Tumors: Population-Based Outcomes and Machine Learning Analysis
by
Dimitrios Moris, Pejman Radkani and Piyush Gupta
Surgeries 2026, 7(2), 50; https://doi.org/10.3390/surgeries7020050 - 23 Apr 2026
Abstract
►▼
Show Figures
Background: Pancreatic tumors in pediatric and adolescent patients are rare, and guidance on prognostication and management is limited. Methods: Using the Surveillance, Epidemiology, and End Results (SEER) database (2004–2021), we analyzed clinicopathological characteristics, treatment patterns, and survival outcomes in patients younger than 20
[...] Read more.
Background: Pancreatic tumors in pediatric and adolescent patients are rare, and guidance on prognostication and management is limited. Methods: Using the Surveillance, Epidemiology, and End Results (SEER) database (2004–2021), we analyzed clinicopathological characteristics, treatment patterns, and survival outcomes in patients younger than 20 years with pancreatic tumors. Analyses integrated conventional survival models with machine learning approaches to identify key predictors. Results: The cohort included 203 patients, of whom 108 (53.2%) had solid pseudopapillary neoplasms (SPNs), 59 (29.1%) neuroendocrine neoplasms, 16 (7.9%) pancreatoblastomas, 5 (2.5%) adenocarcinoma variants, 4 (2.0%) acinar cell carcinomas, and 11 (5.4%) other rare histologies. Most patients had localized disease (61.1%) and underwent surgical resection (85.2%). Estimated 5-year and 10-year overall survival rates were 87.8% and 84.0%, respectively. Survival differed significantly by histology, stage, and surgery status (all log-rank p < 0.001). In multivariable analysis, SPN histology was associated with lower mortality (hazard ratio (HR) 0.03, 95% confidence interval (CI) 0.01–0.13; p < 0.001), whereas distant disease was associated with markedly higher mortality (HR 21.49, 95% CI 7.52–133.41; p < 0.001). Surgical resection was independently associated with lower mortality (HR 0.13, 95% CI 0.02–0.29; p = 0.003). Among patients with known 5-year status, the Random Forest and Gradient Boosting models achieved cross-validated area under the curve values of 0.935 ± 0.060 and 0.886 ± 0.093, respectively; stage and surgery were the dominant predictors in both models. Conclusions: Surgery remains the cornerstone of management for pediatric pancreatic tumors, and advanced analytic approaches may enhance risk stratification in this rare population.
Full article

Figure 1
Open AccessSystematic Review
Prehabilitation in Patients Undergoing Cardiac Surgery: An Umbrella Review of Systematic Reviews and Meta-Analysis
by
Abubakar I. Sidik, Maxim L. Khavandeev, Malik K. Al-Ariki, Vladislav V. Dontsov, Ivan G. Karpenko, Anvar K. Djumanov, Alina V. Ogurchikova, Sergey A. Kurnosov and Dadaev Shirin
Surgeries 2026, 7(2), 49; https://doi.org/10.3390/surgeries7020049 - 23 Apr 2026
Abstract
Background/Objective: Prehabilitation aims to improve physiological reserve before surgery to enhance postoperative outcomes. Multiple systematic reviews have evaluated preoperative interventions in adult cardiac surgery; however, variability in scope, methodological quality, and overlap of primary trials complicates interpretation. The aim of this study
[...] Read more.
Background/Objective: Prehabilitation aims to improve physiological reserve before surgery to enhance postoperative outcomes. Multiple systematic reviews have evaluated preoperative interventions in adult cardiac surgery; however, variability in scope, methodological quality, and overlap of primary trials complicates interpretation. The aim of this study is to synthesise and critically appraise evidence from systematic reviews and meta-analyses evaluating prehabilitation interventions in adults undergoing cardiac surgery. No funding was received for this study. Methods: We conducted an umbrella systematic review following a prospectively registered protocol (PROSPERO: CRD420261292354) and PRISMA 2020 guidance. PubMed, Web of Science, and Scopus were searched from inception to 31 December 2025. Eligible reviews included adults (≥18 years) undergoing cardiac surgery, evaluated and compared preoperative inspiratory muscle training (IMT), respiratory muscle training, and exercise-based, educational, or multimodal prehabilitation with usual care or sham intervention. Reviews focused solely on postoperative interventions or non-cardiac surgery were excluded. Methodological quality was assessed using AMSTAR-2. Certainty of evidence was evaluated using GRADE. Overlap of primary studies was quantified using the Corrected Covered Area (CCA). A structured narrative synthesis with a direction-of-effect framework was applied. Results: Eighteen systematic reviews (published 2012–2025) were included, comprising 46 unique primary studies and more than 6674 participants (exact totals unavailable due to incomplete reporting in at least one review). Overall overlap was high (CCA 12.5%). Respiratory-focused prehabilitation, particularly IMT, demonstrated consistent reductions in postoperative pulmonary complications (PPCs) (risk ratios approximately 0.42–0.53), pneumonia (RR ~0.44–0.45), and atelectasis (RR ~0.49–0.59), favouring prehabilitation over usual care. Hospital length of stay was reduced by approximately 1.5–3 days across multiple reviews. Inspiratory muscle strength improved consistently (mean difference ~+12 to +17 cmH2O). Effects on ICU length of stay and mechanical ventilation duration were inconsistent or non-significant. Exercise-based programmes improved functional capacity (6 min walk distance increase ~50–75 m) and showed modest reductions in hospital stay, but heterogeneity was substantial. No intervention demonstrated a consistent reduction in postoperative mortality. Evidence was limited by clinical heterogeneity, performance bias in primary trials, inconsistent outcome definitions, and high overlap of key IMT trials across reviews. Mortality outcomes were underpowered. Conclusions: Preoperative IMT provides evidence for reducing pulmonary complications and shortening hospital stays in adult cardiac surgery. Exercise-based prehabilitation improves functional capacity but requires further high-quality, standardised trials. Integration of respiratory prehabilitation into cardiac surgical pathways appears supported by the current evidence.
Full article
(This article belongs to the Section Cardiothoracic and Vascular Surgery)
►▼
Show Figures

Figure 1
Open AccessTechnical Note
A Mini-Invasive Dorsal Capsulodesis for the Treatment of Chronic Scapholunate Instability: Surgical Technique and Preliminary Outcomes in a Retrospective Case Series
by
Matteo Guzzini, Federica Presutti, Rosa Ballis and Alice Patrignani
Surgeries 2026, 7(2), 48; https://doi.org/10.3390/surgeries7020048 - 23 Apr 2026
Abstract
Background: Chronic reducible scapholunate instability (SLI) remains a challenging condition, with multiple surgical options described, often associated with soft tissue disruption and postoperative stiffness. We describe a mini-invasive dorsal capsulodesis technique aimed at restoring carpal alignment while minimizing surgical morbidity, and we report
[...] Read more.
Background: Chronic reducible scapholunate instability (SLI) remains a challenging condition, with multiple surgical options described, often associated with soft tissue disruption and postoperative stiffness. We describe a mini-invasive dorsal capsulodesis technique aimed at restoring carpal alignment while minimizing surgical morbidity, and we report preliminary clinical and radiographic outcomes. Methods: This study includes a retrospective analysis of the first 10 consecutive patients treated with this technique who had a minimum follow-up of 3 years. All patients presented with chronic, reducible scapholunate instability. Clinical outcomes were assessed using the Visual Analog Scale (VAS) for pain and the Quick Disabilities of the Arm, Shoulder and Hand (QuickDASH) score. Radiographic evaluation was performed to assess maintenance of scapholunate alignment and progression to degenerative changes. Results: At a mean follow-up of approximately 4 years, patients showed a substantial reduction in pain (mean VAS from 8 preoperatively to 2 postoperatively) and improvement in function (mean QuickDASH from 74.6 to 16.5). Radiographic evaluation demonstrated maintenance of carpal alignment in all cases, with no progression to scapholunate advanced collapse (SLAC) observed. Wrist range of motion improved postoperatively, with extension reaching approximately 80° and flexion 70°, without significant functional limitations. No major complications or reoperations were recorded. Patient satisfaction was high, with 9 patients reporting being extremely satisfied and 1 satisfied. Conclusions: This mini-invasive dorsal capsulodesis appears to be a feasible and tissue-sparing option for selected cases of chronic reducible scapholunate instability. In this preliminary series, the technique was associated with favorable clinical and radiographic outcomes at mid-term follow-up. Further studies with larger cohorts and comparative designs are needed to confirm these findings.
Full article
(This article belongs to the Section Hand Surgery and Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Transcutaneous Fibrosis Perforation (Needle Fasciotomy) in Dupuytren’s Disease—A Retrospective Analysis of 1803 Cases
by
Philipp Groeben and Ole Ackermann
Surgeries 2026, 7(2), 47; https://doi.org/10.3390/surgeries7020047 - 16 Apr 2026
Abstract
Background: Percutaneous needle fasciotomy has been practiced for many years as a therapeutic alternative to open fasciectomy in Dupuytren’s disease. In addition to collagenase injection, it has established itself as a minimally invasive procedure in everyday clinical practice. This study analyzes the treatment
[...] Read more.
Background: Percutaneous needle fasciotomy has been practiced for many years as a therapeutic alternative to open fasciectomy in Dupuytren’s disease. In addition to collagenase injection, it has established itself as a minimally invasive procedure in everyday clinical practice. This study analyzes the treatment results of 1146 patients. Methods: Patients at a center for needle fasciotomy were surveyed retrospectively by means of a questionnaire. In addition to previous illnesses and the localization and number of affected fingers, the frequency of recurrences, the need for renewed treatment, and satisfaction with the surgical result were also surveyed. Results: Between 1994 and 2012, 1146 patients with 1803 finger rays were treated and their data analyzed on the basis of records. In addition, a questionnaire survey on patient satisfaction was conducted and 174 questionnaires were analyzed. Overall, 83% of the patients were male and 16% female. In 50% of cases the right side was treated, in 45% of cases the left side (5% unknown), while 46% of the finger rays treated were on the little finger and ring finger. In all but one case, an improvement in the contracture was achieved. Complications included skin tears (264 cases), increased swelling (five cases), hypesthesia (one case), flexor tendon rupture (four cases) and a mid-limb base fracture (one case). The mean operation time was 26.9 min, the duration of pain was 2.7 days, and patient satisfaction on a scale of 1–10 was 7.2. Overall, 77% of patients stated that there had been a further deterioration or recurrence within one year of treatment, and 35% of these patients stated that further treatment was necessary. Conclusions: Needle fasciotomy is a safe and effective method with a low complication rate, but targeted and stringent follow-up treatment is necessary, as is information about possible recurrences or further deterioration of the result.
Full article
(This article belongs to the Section Hand Surgery and Research)
►▼
Show Figures

Figure 1
Open AccessArticle
The Effect of Marginal Ischemia on Colonic Anastomotic Leakage: A Rat Model
by
Guy Barsky, Grace Haj, Anton Osyntsov, Ivan Kukeev, Yulia Vaynshtein, Elchanan Quint, Ilia Vasiliev, Nur Alkrinawi, Sergey Yerep, Dmitry Likalter, Sofyan Abu Freih, Nir Nessim Cohen and David Czeiger
Surgeries 2026, 7(2), 46; https://doi.org/10.3390/surgeries7020046 - 10 Apr 2026
Abstract
Background: Anastomotic leakage remains a serious complication of colorectal surgery, often linked to impaired blood supply at the incision site. Objective: To develop and validate a reproducible rat model of colonic anastomotic leakage induced by graded mesocolon ischemia. Methods: Of 144 operated rats,
[...] Read more.
Background: Anastomotic leakage remains a serious complication of colorectal surgery, often linked to impaired blood supply at the incision site. Objective: To develop and validate a reproducible rat model of colonic anastomotic leakage induced by graded mesocolon ischemia. Methods: Of 144 operated rats, 138 survived surgery and underwent end-to-end colonic anastomosis with five levels of mesocolon ligation (0–2 cm of unilateral mesocolic ischemia). Postoperative outcomes, including anastomotic integrity, abscess formation, and mortality, were assessed on postoperative day 10. Anastomotic bursting pressures were also measured in a subset of animals. Results: Leak rates increased with ischemia severity: 0% in controls, 16.7% at 0.2 cm, 42.6% at 0.4 cm, 95.8% at 1 cm, and 100% at 2 cm (p < 0.0001, trend test). Bursting pressures decreased progressively with increasing anastomotic severity. The 0.4 cm ischemia condition produced a reproducible intermediate leak rate suitable for experimental interventions. Conclusions: This rat model reliably induces graded anastomotic leaks and can serve as a platform for testing strategies to prevent leakage in high-risk colorectal surgery.
Full article
(This article belongs to the Special Issue Interdisciplinary Experimental Surgical Research and Technologies, Featured by the Academy of Surgical Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Cost–Benefit Analysis in the Surgical Management of Thumb Carpometacarpal Osteoarthritis: Dual-Mobility Total Joint Replacement Versus Trapeziectomy with Ligament Reconstruction and Suspension Arthroplasty
by
Leopoldo Arioli, Giulia Frittella, Fatma Abidi, Edoardo Venturini and Matteo Guzzini
Surgeries 2026, 7(2), 45; https://doi.org/10.3390/surgeries7020045 - 1 Apr 2026
Abstract
Background: Trapeziometacarpal (TM) osteoarthritis (OA) is a common condition, especially among postmenopausal women, often requiring surgical intervention when conservative treatment fails. In recent years, dual-mobility prostheses have been increasingly used as an alternative to traditional trapeziectomy with suspension arthroplasty. However, limited data exist
[...] Read more.
Background: Trapeziometacarpal (TM) osteoarthritis (OA) is a common condition, especially among postmenopausal women, often requiring surgical intervention when conservative treatment fails. In recent years, dual-mobility prostheses have been increasingly used as an alternative to traditional trapeziectomy with suspension arthroplasty. However, limited data exist regarding their comparative cost-effectiveness in public healthcare systems. Purpose: The aim of this study was to compare the cost–benefit ratio and clinical outcomes of two surgical techniques for TM OA: trapeziectomy with suspension arthroplasty and total joint arthroplasty with a dual-mobility prosthesis. Methods: We conducted a retrospective cohort study of 116 hands treated between 2020 and 2024. Patients were divided into two groups based on the surgery they received: trapeziectomy with suspension arthroplasty or implantation of a dual-mobility TM prosthesis. Clinical outcomes were assessed using VAS, DASH, Kapandji score, grip strength, and pinch strength at 12, 36, and 48 months postoperatively. A cost analysis was performed based on hospital reimbursement (Diagnosis-Related Group) and estimated productivity loss. Results: Both techniques yielded significant improvements in pain and function. Patients who were operated on with a prosthesis showed faster recovery and better early outcomes, while the trapeziectomy group had lower direct surgical costs and fewer complications. At 48 months, clinical scores were comparable. The overall cost–benefit ratio favoured trapeziectomy with suspension arthroplasty, while TM prosthesis’s higher costs were justified due to improved short-term functional recovery. Conclusions: Both surgical techniques achieved satisfactory long-term clinical outcomes. The prosthetic option allows for quicker recovery and reduces indirect social costs, while suspension arthroplasty remains more cost-effective for direct costs. These findings highlight the importance of balancing clinical benefit and economic sustainability in surgical decision-making for TM osteoarthritis. Level of Evidence: Level III, retrospective comparative study.
Full article
(This article belongs to the Section Hand Surgery and Research)
Open AccessArticle
Massive Pulmonary Hemorrhage After Pulmonary Endarterectomy: Updated Outcomes of a Standardized Management Protocol over 14 Years
by
Cagatay Cetinkaya, Sehnaz Olgun Yildizeli, Altug Sagir, Mustafa Emre Kavlak and Bedrettin Yildizeli
Surgeries 2026, 7(2), 44; https://doi.org/10.3390/surgeries7020044 - 30 Mar 2026
Abstract
Background: Massive pulmonary hemorrhage is a life-threatening complication of pulmonary endarterectomy (PEA) with limited evidence to guide standardized management. Methods: We retrospectively evaluated consecutive PEA procedures performed at a high-volume center and analyzed the incidence, perioperative characteristics, management strategies, and early outcomes of
[...] Read more.
Background: Massive pulmonary hemorrhage is a life-threatening complication of pulmonary endarterectomy (PEA) with limited evidence to guide standardized management. Methods: We retrospectively evaluated consecutive PEA procedures performed at a high-volume center and analyzed the incidence, perioperative characteristics, management strategies, and early outcomes of patients who developed massive pulmonary hemorrhage. Results: Among 1123 patients who underwent PEA, massive pulmonary hemorrhage occurred in 51 (4.54%) and developed intraoperatively after completion of PEA and separation from total circulatory arrest. Primary suturing achieved hemostasis in 12 patients (23.5%), and bronchial isolation was applied in 18 (35.3%). Local adjuncts included intraoperative bronchial clamping in 1 patient (2.0%) and biological glue occlusion in 2 (3.9%). Extracorporeal membrane oxygenation (ECMO) was required in 25 patients (49.0%), initiated intraoperatively in 22 and postoperatively in 3. Overall in-hospital mortality was 41.2%, while 30 patients (58.8%) survived to hospital discharge; among survivors, mean hospital length of stay was 16.1 ± 6.8 days. Conclusions: Massive pulmonary hemorrhage after PEA remains associated with substantial early mortality and resource utilization; a stepwise institutional algorithm combining bronchoscopy-guided localization, targeted airway/surgical control, and timely ECMO support may help standardize management in this critical setting.
Full article
(This article belongs to the Section Cardiothoracic and Vascular Surgery)
►▼
Show Figures

Figure 1
Open AccessFeature PaperArticle
Reassessing Routine Postoperative Imaging in Acromegaly: Insights from a Cohort with Biochemical Remission
by
Jelena Maletkovic, Marvin Bergsneider, Won Kim, Marilene B. Wang, Jeffrey D. Suh, Michael Linetsky, Noriko Salamon, Sandra Pekic Djurdjevic and Anthony P. Heaney
Surgeries 2026, 7(2), 43; https://doi.org/10.3390/surgeries7020043 - 26 Mar 2026
Abstract
Background: Postoperative evaluation for growth hormone-producing pituitary tumors entails assessing remission via biochemical markers alongside MRI to detect residual tumors. While postoperative imaging provides important anatomical information regarding potential residual tumor, it is reasonable to ask if imaging offers largely redundant data
[...] Read more.
Background: Postoperative evaluation for growth hormone-producing pituitary tumors entails assessing remission via biochemical markers alongside MRI to detect residual tumors. While postoperative imaging provides important anatomical information regarding potential residual tumor, it is reasonable to ask if imaging offers largely redundant data when biochemical remission is already established. This study aimed to determine the clinical utility of post-surgical surveillance imaging in patients who achieved biochemical remission with normal age- and sex-matched IGF-1 at ~3 months postoperatively. Furthermore, we sought to evaluate the long-term durability of biochemical control in this patient subset. Methods: We conducted a retrospective analysis on patients who underwent endoscopic endonasal approach surgery for acromegaly and had a minimum of 3 years of follow-up clinical, biochemical and imaging data. Results: In total, 15 of 28 patients (54%) achieved initial biochemical remission and had a 100% sustained remission rate during the follow-up period of 3–14 years, underscoring the importance of surgical radicality for achieving durable remission. Conclusions: Our findings suggest that for patients who achieved biochemical remission following transsphenoidal surgery for acromegaly, routine postoperative imaging provides negligible additional diagnostic information from an endocrinological perspective. As such, we propose that no further postoperative imaging is needed for patients in clinical and biochemical remission. This approach offers a significant reduction in the clinical burden and healthcare costs for patients associated with long-term management of their disease.
Full article
(This article belongs to the Special Issue Surgery in Head and Neck Cancer)
►▼
Show Figures

Figure 1
Open AccessArticle
Stratified Procedural Risk Assessment in Colorectal Surgery: A Comparative Analysis of Statistical and Machine Learning Approaches Using Combined Surgical Approach and Operative Duration Categories
by
Dennis Elengickal, Michael Nizich and Milan Toma
Surgeries 2026, 7(2), 42; https://doi.org/10.3390/surgeries7020042 - 25 Mar 2026
Cited by 1
Abstract
Background: Postoperative complications following colorectal surgery remain a persistent clinical challenge. Traditional risk stratification has focused on patient characteristics, while conventional modeling approaches treat procedural factors such as operative duration and surgical approach as independent predictors, potentially obscuring interaction effects. Methods: This study
[...] Read more.
Background: Postoperative complications following colorectal surgery remain a persistent clinical challenge. Traditional risk stratification has focused on patient characteristics, while conventional modeling approaches treat procedural factors such as operative duration and surgical approach as independent predictors, potentially obscuring interaction effects. Methods: This study developed a machine learning model stratifying 7908 colorectal surgery patients into four distinct procedural risk categories based on combined surgical approach and operative duration (laparoscopic-short, laparoscopic-long, open-short, open-long), rather than treating these factors as separate variables. A gradient boosting ensemble classifier with RUSBoost resampling was trained on predictor variables including patient demographics, comorbidities, and intraoperative factors. Results: Feature importance analysis revealed that the open-long category emerged as the single most important predictor, substantially exceeding all other variables. Weight loss, body mass index, patient age, and electrolyte abnormalities ranked as the next most important predictors. Stratified complication rates demonstrated a critical interaction: prolonged duration more than doubled complication risk in open procedures (short-duration: 9.99%, long-duration: 20.46%), whereas laparoscopic procedures showed only a modest increase from short-duration (10.45%) to long-duration (14.08%) cases. Logistic regression benchmark analysis confirmed the duration-approach interaction (OR = 1.53, 95% CI: 0.97–2.39), achieving comparable discrimination (c-statistic 0.678 vs. 0.665 for the ensemble model). Decision curve analysis demonstrated logistic regression provided superior clinical utility across most threshold probabilities. Conclusions: The dual analytical framework (i.e., statistical inference for quantifying associations and machine learning for predictive feature ranking) offers complementary insights for clinical application. These findings demonstrate that stratified feature engineering can elucidate complex risk phenotypes that may be obscured when procedural factors are analyzed independently.
Full article
(This article belongs to the Special Issue The Application of Artificial Intelligence in Surgical Procedures)
►▼
Show Figures

Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
CIMB, Gastrointestinal Disorders, IJMS, Surgeries
Gastrointestinal and Metabolic Diseases: From Mechanisms to Surgery
Topic Editors: Alin Constantin Pînzariu, Ionela Lacramioara Serban, Daniel TimofteDeadline: 20 June 2027

Special Issues
Special Issue in
Surgeries
Feature Papers in Hand Surgery and Research
Guest Editor: Francesco De FrancescoDeadline: 15 July 2026
Special Issue in
Surgeries
Advances in Wrist Arthroscopy: From Diagnosis to Reconstruction
Guest Editor: Francesco SmeragliaDeadline: 31 July 2026
Special Issue in
Surgeries
Novel Insights into Liver Transplantation Surgery
Guest Editors: Maheswaran Pitchaimuthu, Amit NairDeadline: 31 July 2026
Special Issue in
Surgeries
Interdisciplinary Experimental Surgical Research and Technologies, Featured by the Academy of Surgical Research
Guest Editor: Melanie GrahamDeadline: 31 August 2026






