Abstract
(1) Background: Final-year medical students often feel under prepared for their transition into clinical practice. Clinical ward rounds and shadowing approach this issue by building transferable skills; however, they are highly variable, with teaching clinicians experiencing a large number of work-related interruptions. Simulated ward rounds have garnered significant interest by translating clinical encounters into standardised educational opportunities for students. This review evaluates the impact of simulated ward rounds in promoting the clinical competencies required for work in final-year medical students and assesses the impact of simulated ward rounds on the experience of clinical learning for medical students. (2) Methods: A computer-assisted search was performed in the Medline, Embase, and CINAHL databases. Studies that evaluated simulated ward rounds in final-year medical student cohorts were included. (3) Results: In total, 107 articles were identified by the search and 26 articles were eligible for full-text analysis. The analysis of these studies showed that simulated ward rounds were effective in improving confidence, as well as the technical and non-technical skills of final-year medical students; however this is on the basis of highly heterogeneous and lower-quality evidence. (4) Conclusion: Our systematic review highlights that simulated ward rounds provide final-year medical students with increased confidence and preparedness for clinical work and identifies the need to pursue more methodologically rigorous research to inform the best practice delivery of simulated ward rounds.
1. Introduction
One of the greatest demands facing medical schools is the development of future doctors that are well-prepared, competent, and safe by the time they graduate and begin their clinical careers. This requires the culmination of multiple important competencies such as medical expertise, as well as non-technical skills including interprofessional communication and ethical and patient-centred practice. Given the enormity of this task, it is understandable that final-year medical students often feel unprepared for this transition [1,2].
Clinical ward rounds are performed daily as the standard for patient care in hospital settings and demand the expertise of a well-rounded doctor. However, there is clear evidence that final-year medical students often feel underprepared for ward rounds [3]. The impact of this is well-documented, with poor-quality ward rounds leading to delays in diagnoses and increased morbidity attributed to preventable complications [4]. Traditionally, medical educators approach this challenge through ward-based teaching and shadowing, allowing medical students to practice and build confidence in their bedside clinical skills, diagnostic reasoning, and administrative duties under the safe supervision of trained and qualified clinicians [5]. Despite this, the quality of this education is often disputed. Doctors are reported to spend 16–24% of their work engaged in multiple simultaneous activities, experiencing an estimated 5.3 interruptions per hour [6,7,8,9]. These variations and interruptions can ultimately impact the quality of ward-based education for medical students.
Simulation as a modality of training health professionals has increasingly garnered interest for this purpose. Simulation has been shown to be highly effective in refining the necessary technical and non-technical skills for clinical practice [10]. For final-year medical students, recent studies have shown that ward round simulations are an effective modality for bypassing the variability and interruptions of clinical practice and providing opportunities to practice the skills required of junior doctors. These simulations involve the development of clinical patient scenarios in line with the medical curriculum, implemented with the assistance of actors and adjunct materials, including simulated laboratory tests and imaging reports. Ward round simulations, therefore, offer the potential for final-year students to develop their diagnostic and management skills, interprofessional teamwork and communication skills, and administrative skills in a realistic, safe, and standardised environment [10]. Despite this, simulations are also limited by the variable transferability of skills into the clinical setting and lack of ability of simulations themselves to represent real-world environments. Overall, given the paucity of high-quality evidence in the literature, the key impacts of simulated ward rounds, particularly on the final-year medical student population, is poorly characterised. This review herein aims to explore the main research questions. Firstly, this review seeks to evaluate the key clinical competencies that are built and honed with simulated ward rounds, and secondly, this review evaluates the perceived impact on these competencies of final-year medical students.
2. Materials and Methods
2.1. Search Strategy
This review was performed in adherence to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. The review protocol was prospectively registered in the PROSPERO database (PROSPERO ID: CRD42023440670). A literature search of the Medline, Embase, and CINAHL databases was conducted on 22 June 2023. The reference lists of relevant articles were further used to identify additional papers by hand searching. The search strategy combined keywords and medical subject headings (MeSH) terms related to ward round simulation and final-year medical students. Subject terms and truncation symbols were used to find all relevant studies.
2.2. Inclusion and Exclusion Criteria
Full-text peer-reviewed publications available in the English language, which explored outcomes including improvement in technical skills (clinical history, examination, and management planning) and non-technical skills (confidence, empathy, patient advocacy, professionalism, and ethical practice) and perceived insights into simulation ward rounds from final-year medical students, were included in this review. The criteria used to select these articles included: 1. original randomised controlled trials and prospective or retrospective observational studies, 2. final-year medical students as the population of interest, and 3. use of any style of ward round simulation. Studies were excluded if they were: 1. of the following study types: reviews, meta-analyses, non-human studies, conference paper, letters, abstract only, commentaries, case reports or case series, opinion pieces, and editorials, 2. had incomplete data, 3. evaluated cohorts that were not final-year medical students, and 4. implemented interventions that did not have an in-person simulated ward round such as simulation games online and simulated pages without ward rounds.
2.3. Literature Screening
Screening by the title and abstract of the papers identified by the search strategy was performed by two independent investigators (KL, ED). Abstracts that did not provide sufficient information regarding the inclusion and exclusion criteria were selected for full-text analysis. The same two investigators subsequently performed a full-text analysis of the studies for eligibility. Disagreement during this process was resolved by consensus.
2.4. Outcomes
The outcomes of interest included quantitative and qualitative data that reported on improvements in key junior doctor clinical competencies as a result of simulated ward rounds to ensure that final-year medical students are work ready. The clinical competency outcomes of interest included technical skills such as the evaluation and management of patients, prescribing, and clinical decision making, and non-technical skills including communication skills and teamwork. The outcomes of interest when considering the perceived experience of simulated ward rounds of final-year medical students included evaluating and improving the understanding of key themes that may be considered with the delivery of this modality of teaching, such as the realistic nature of simulated ward rounds, relevance to the competencies expected of junior doctors, and qualitative experiences of medical students, including building the confidence and emotions experienced during the implementation of simulated ward rounds.
2.5. Data Extraction
Data were systematically extracted from the included articles based on the parameters outlined by our outcomes of interest. The findings of all the included studies were analysed thematically using metasynthesis to integrate and interpret the results to achieve a novel finding from variable source data, including quantitative and qualitative studies [11]. The data analysis was performed independently by two investigators (KL, ED) and included an iterative comparison of the included studies to identify and cluster recurrent themes. The findings were organised into categories and compared across the studies to identify common themes and relationships within the data.
2.6. Quality and Risk of Bias Assessment
The quality of evidence of the included studies was assessed using the Quality Assessment Tool (QATSDD) developed by the University of Leeds, United Kingdom [12,13]. Risk of bias was subsequently assessed using the Mixed Methods Appraisal Tool (MMAT) [14,15]. Both of these tools allow for the simultaneous evaluation of all the empirical literature, including qualitative only, quantitative only, and mixed-methods studies, therefore appropriate for this systematic review. Quality and risk of bias assessments were performed independently by two investigators (KL, ED). Disagreements during this process were resolved by consensus.
3. Results
3.1. Literature Search Results
A total of 107 publications were retrieved following a computer-assisted search (Figure 1). Following the removal of duplicates, 62 articles were screened by title and abstract to assess their eligibility, resulting in the exclusion of 36 articles. The remaining 26 articles progressed to full-text analysis in accordance with our eligibility criteria. A total of 6 articles were excluded during this process, with 3 studies including the wrong intervention, 1 study identifying outcomes not of interest, and 2 studies with study populations that were not of interest.
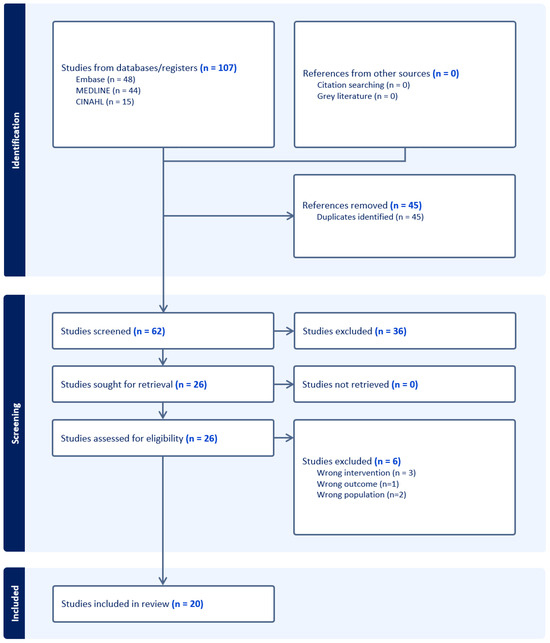
Figure 1.
Search strategy and workflow in accordance with PRISMA guidelines.
3.2. Overview of Included Studies
A total of 20 articles were included in this review (Table 1). All 20 studies assessed the impact of a simulated ward round intervention on final-year medical students. Interventions were variable across the studies. Cohort sizes ranged from small cohorts (n = 8) to larger cohorts (n = 217). All 20 studies were prospective single-arm trials of a simulation ward round intervention. Recruitment, in all cases, was by invitation or as part of the training curriculum of relevant final-year medical student cohorts from associated institutions in these studies. Overall, the studies were of lower-level evidence according to the Oxford Centre for Evidence-Based Medicine; 12 studies were categorised as level 2C and 8 studies were categorised as level 3 based on the study type and category of outcome data [16].

Table 1.
Overview of included studies by year of publication.
The 20 papers encompassed quantitative prospective studies (n = 5), qualitative prospective studies (n = 8), and mixed-methods studies (n = 7) (Figure 2). The studies were predominantly published within Europe, with 16 studies performed in the United Kingdom and 2 studies performed in Germany (Figure 3). An additional two studies were performed in Chile, South America. All studies were single-institution studies within those relevant locations. The earliest study identified was published in 2006 (Figure 4).
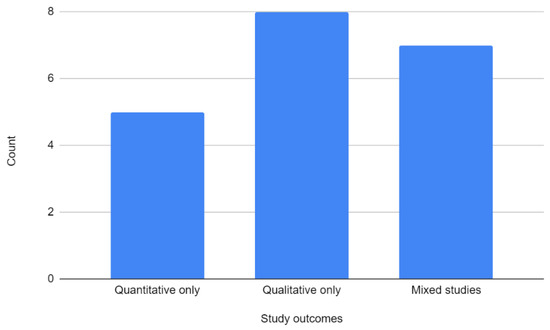
Figure 2.
Data outcomes of included studies.
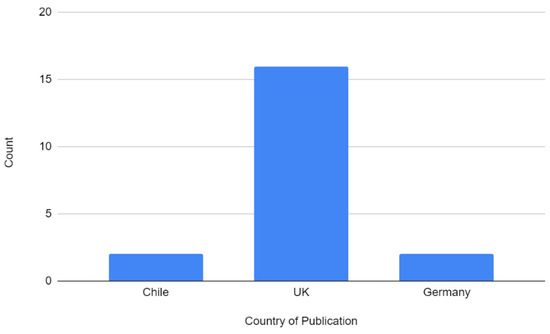
Figure 3.
Location of publication of included studies.
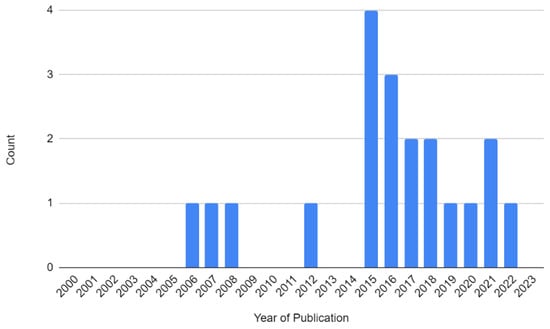
Figure 4.
Year of publication of included studies.
3.3. Key Themes from Quantitative and Qualitative Meta-Synthesis
The key outcomes qualitatively evaluated by the papers are highlighted in Table 2, and where possible, were synthesised alongside quantitative data to provide a deeper understanding of the impact of simulated ward rounds on final-year medical students.

Table 2.
Key themes identified from eligible studies following thematic analysis.
3.3.1. Negative Emotions
In total, 10 studies reported on the negative emotions perceived by final-year medical students when performing simulated ward rounds [17,18,19,20,21,22,23,24,25,26]. Of these studies, eight provided qualitative data and two provided quantitative data, indicating that the students developed an array of negative emotions, with a temporal relationship to the act of performing simulated ward rounds. The emotions experienced and reported included anxiety, nervousness and nervous anticipation, shock, stress, frustration, fear, and awkwardness. These emotions mainly centred around situations in which multiple stimuli were experienced or multiple tasks were required, including unwell patient situations and when multiple distractions or interruptions occurred. The students also found that simulated ward rounds, in general, brought upon these emotions, as well as genuine concern that they were doing the wrong thing. This appeared to be felt to a high degree. MacDowall et al. reported that, in their cohort, an average Likert score of 4.22 out of 5 (where 5 is strongly agree) applied to students being concerned regarding doing the right thing, and Manalayil et al. similarly found Likert scores ranging from 4.0 to 4.4 out of 5 over 3 separate years when the students were asked if they were nervous prior to performing the simulation [25,26]. Negative emotions were found to be highly dependent on the simulated ward round scenario, as they were quick to dissipate following the completion of the simulated rounds.
3.3.2. Information Overload
Six studies overall reported on the information overload experienced throughout simulated ward rounds [10,17,18,20,22,24]. Of these, three studies provided qualitative data, one study provided quantitative data, and two studies provided mixed data. The predominant reason perceived by the students to account for feelings of being overwhelmed with information was the multiple and variable cues and stimuli received. These ranged from equipment alarms or distractions to the increasing number of tasks requiring frequent re-prioritisation and the need to manage multiple patients simultaneously. This is supported by quantitative scores. Behrens et al. reported that, on a scale from 1 to 5 (very poor to outstanding), students, on average, self-scored their ability to respond to interruptions as 3.7 out of 5 and ability to manage tasks as 3.43 out of 5, indicating moderate performance [10]. Similarly, Morgan et al. scored students based on their ability to prioritise clinical workload on a Likert scale out of 10 [22]. In this case, the students, on average, achieved a score of 5.65 out of 10 prior to the simulated ward round and 7.16 out of 10 following the simulation [22]. Similar findings were also noted in other studies, including that by Harvey et al., who noted that task management was rated 2.91 pre-simulation (where 2 is marginal and 3 is acceptable) and improved to 2.97 post-intervention [27]. Therefore, despite feelings of information overload arising from the various stimuli received, it is clear that addressing issues such as improving task prioritisation can be achieved through simulated ward rounds as an educational tool to refine these skills.
3.3.3. Improving Relevant and Transferrable Skills
In total, 16 studies reported on simulated ward rounds as a useful educational tool to promote the learning of relevant and transferrable technical and non-technical skills for final-year medical students as they transition to clinical practice [3,10,17,18,20,22,23,24,26,27,28,29,30,31,32,33]. Of these, nine studies provided qualitative data, four studies provided quantitative data, and three studies provided mixed data. Students, in general, found simulated ward rounds to be highly useful for developing relevant skills in the lead up to clinical practice. In particular, through qualitative analysis, the common themes amongst the students were that these sessions assisted with key technical skills, including prescribing, diagnostic reasoning, and clinical assessment, as well as non-technical skills including task prioritisation, empathy, leadership, communication, and coping with fatigue and stress. Scoring tools in quantitative studies supported these findings. Harvey et al. assessed the mean scores in various domains, including communication, decision making, situational awareness, teamwork, and task management and found improvement in each of these domains following the implementation of a simulated ward round program [27]. Nikendei et al. also found that a sound proportion of students reached the appropriate learning outcomes in the domains of communication, physical examination, and team communication, however, there was room for improvement in information gathering, chart review, prescription, and documentation skills [3]. With respect to quality and safety, Parker et al. demonstrated that students had moderate to high mean scores in domains such as the understanding of management plans, communication and interprofessional discussion, and actively seeking and clarifying information [32]. Furthermore, Thomas et al. demonstrated that the overall number of errors was reduced following simulated ward rounds with feedback (n = 72) compared to no feedback (n = 76) [33]. Overall, both students and educators recognise that simulated ward rounds have potential when it comes to promoting the development of key technical and non-technical skills for future doctors.
3.3.4. Realism
A total of 11 studies reported on the realistic nature of simulated ward rounds [19,20,21,22,23,24,25,29,30,31]. Of these, 10 studies provided qualitative data and 1 provided quantitative data. The general consensus from final-year medical students was that the simulations were authentic and realistic representations of the work expected from a junior doctor. On a Likert scale out of 5 (1 = strongly disagree, 5 = strongly agree), Manalayil et al. reported that all students within their cohort rated the quality of these simulations as 5 across 3 different years [25]. These sessions were reported by students to have multiple benefits, including allowing an appreciation of the complexities and nuances of junior doctor life and the opportunity to practice and hone technical and non-technical skills. The students understood, in all cases, that the simulated sessions were artificial, but this provided an element of safety to their engagement. Overall, there was a strong opinion that the realistic nature of the simulated sessions made them very useful, with a high proportion of students indicating they would repeat these simulations again to enhance their learning.
3.3.5. Feelings of Unpreparedness
Two studies reported on final-year medical students’ perceptions of unpreparedness prior to simulated ward rounds [10,19]. Of these, all studies provided qualitative data. These sentiments were mainly attributed to students feeling they lacked clinical practice, resulting in variable and underprepared performances.
3.3.6. Feedback
Six studies reported on the usefulness of feedback obtained from simulated ward rounds [10,24,25,26,28,29]. Of these, five studies provided qualitative data and one study provided mixed data. In general, students valued the opportunity to be provided with feedback after simulated ward round sessions, as they viewed the feedback as highly useful and relevant for their progression towards working as a junior doctor. This is supported by Manalayil et al., who, using a 5-point Likert scale (1 = strongly disagree, 5= strongly agree), reported a score for feedback ranging between 4.6 and 5.0 across 3 different years [25]. The key aspects of feedback that the students appreciated included the individuality of the feedback, coverage of technical and non-technical skills, and opportunity for future developmental goals to be identified. Poorer-quality feedback was identified as being rushed when provided.
3.3.7. Application of Knowledge
One qualitative study reported on the difficulty of applying knowledge learnt from medical school in the simulated ward round [20]. This study found that the main factors that contributed to this were the high-pressure environment and the requirement of the simulation to manage diverse caseloads of patients (including both medical and surgical conditions), which impaired timely recall. Students also noted that prior learning with respect to such patients were performed in silos, such as solely learning about surgical issues and solely learning about medical issues, which meant accessing such information in a timely manner was not efficient and intuitive in the simulated scenarios.
3.3.8. Improving Confidence
Five studies reported on the role of simulated ward rounds in increasing the confidence of final-year medical students [19,24,25,26,34]. Of these studies, three provided qualitative data and two provided quantitative data. The general trend noted was that final-year medical students predominantly felt underprepared for simulated ward rounds, however, with increasing opportunity to practice in the simulated environment, the students began to develop more confidence [24]. In particular, improved confidence was highlighted in the context of communication with patients and managing deteriorating patient scenarios [19,26]. This is further supported by Powell et al., who demonstrated via a 5 point Likert scale (1 = poor, 5 = outstanding) that students improved their confidence in other domains, including leadership (2.08 to 3.33) and documentation (3.30 to 3.73), following simulated ward rounds [34]. Similarly, Manalayil et al. supports this finding in reporting that final-year medical students found that simulated ward rounds boosted their confidence on a 5-point Likert scale (1 = strongly disagree, 5 = strongly agree), with a mean score of 4.6 to 5.0 across 3 years of implementation [25].
3.3.9. Quality and Risk of Bias Assessment
The methodological quality of the papers was assessed utilising the QATDD tool and ranged from very low (37.5%) to high (97.6%) (Table 3). The median score out of 100 for quality in these studies was 73.1 (IQR: 21.5) and the mean with standard error was 71.52 +/− 7.183 (95% confidence interval), indicating moderate quality. The most frequent limitations were in the studies’ ability to consider sample size within the methods for data analysis and an appropriate and well-informed justification of the methodology used for analysis.

Table 3.
Methodological quality assessment through the use of the Quality Assessment Tool (QATDD).
Risk of bias was further assessed utilising the MMAT tool and was variable in its result, ranging from very low (2/7) to high (7/7) (Table 4). The overall median score out of 7 was 6.5 (IQR: 3) and the overall mean with standard error was 5.45 +/− 0.785 (95% confidence interval), indicating a moderate to low risk of bias. With respect to the quantitative studies, the median score was 6 (IQR: 2.5) and mean with standard error was 5.8 +/− 1.143 (95% confidence interval), indicating a moderate risk of bias. For the qualitative studies, the median score was 7 (IQR:0) and mean with standard error was 6.75 +/− 0.49 (95% confidence interval), indicating a low risk of bias. For the mixed-method studies, the median score was 3 (IQR: 1) and mean with standard error was 3.7143 +/− 1.188 (95% confidence interval), indicating a high risk of bias. The greater risk of bias in the mixed-method studies and, to an extent, the quantitative studies was attributable to their small sample sizes, lack of methodological rigour in measuring outcomes of interest, high attrition, and potential for more appropriate statistical analyses of the acquired data. The qualitative studies had lower potential for bias. Publication bias could not be assessed with a funnel plot given the paucity of homogeneous quantitative data allowing for an appropriate assessment.

Table 4.
Risk of bias assessment through the use of the mixed methods appraisal tool (MMAT).
4. Discussion
Our review demonstrates the preliminary benefit of simulated ward rounds, including the ability to focus on specific skills, acquire real-time feedback, understand hospital-based administrative and clinical processes, and practice clinical assessment and decision making without the variability, responsibility, time pressure, and bureaucracy that junior doctors experience in their day-to-day work. Additionally, students were able to work through the challenges of clinical practice in scenarios, allowing them to manage difficult emotions, information overload, and feelings of unpreparedness. Overall, these findings were consistent across various institutions and jurisdictions worldwide, supported by both qualitative and quantitative evidence from students in terms of improved clinical competencies including communication, decision making, task management, and situational awareness, in conjunction with an appreciation for the simulated ward round process. In order to obtain a better understanding of the effect of simulated ward rounds on final-year medical students’ competencies and whether a demonstrable improvement could be observed following the implementation of a simulation-based program, we considered meta-analysing the quantitative outcome data between studies. Due to substantial heterogeneity between the studies related to the approach, delivery, and evaluation of simulated ward rounds, the quantitative data collected were non-homogenous, making meta-analysis unfeasible. Therefore, a meta-synthesis of the available qualitative and quantitative data was chosen to best gain insight into the efficacy, key insights, considerations, and future avenues to explore with respect to research regarding simulated ward rounds. Despite the positive results demonstrated in this review, the value of simulated ward rounds remains relatively unexplored.
Notably, it is important to recognise that, although these benefits are highly appealing, students, at times, found participating in simulated ward rounds to be confronting, with many studies highlighting negative emotions that emerged during the simulated sessions. Furthermore, these negative experiences were exacerbated by situations in which information overload and low confidence were experienced. It can be argued that a benefit of simulated ward rounds is that it allows students to experience, troubleshoot, and improve their approach to such situations in a safe manner. Importantly, it is clear that, for effective and more supportive simulation practices, it is important for educators to consider judicious briefing and debriefing, the opportunity for repeated sessions for practice and reinforcement, and adopting a high standard of feedback provided to students to enhance the value of difficult simulation settings. The latter was further emphasised in the student surveys, whereby it was clear that the students appreciated real-time, individualised feedback to support their learning and development following simulated ward rounds.
Our review also demonstrated that students felt less confident in areas involving end-of-life care discussions, high task loads with the need for frequent task reprioritisation, and managing unwell patients. In the clinical setting, it is unlikely a final-year medical student cohort may have the same opportunities to refine their skills consistently in these domains. Our review suggests that these opportunities are possible with the incorporation of targeted simulation ward rounds into the medical program and, therefore, may assist with deficiencies in current clinical rotations. However, educators must consider that the implementation of these programs is highly complex. Better-informed practices of implementing simulated ward rounds, ideally, should consider a systematic approach to program development that is unique to the challenges of the individual medical school and the limitations of its curriculum. Such practices should consider consultation with key faculty educators and support staff, clinicians involved with hospital-based teaching and supervision, and final-year medical students themselves. Overall, the included articles reported the delivery of highly variable simulated ward rounds. For educators, the interpretation of how simulated ward rounds can be implemented is important, as it is clear that more immersive and elaborate sessions can quickly become resource-intensive and, therefore, costly. It is important to recognise that a well-funded simulated program does not necessarily correlate with a higher quality of educational standard. In particular, Ford et al. highlighted that a cost reduction approach did not impact the quality of the educational goals provided through their iteration of a simulated ward round [28]. Our review demonstrates that rather than cost, effective simulated ward round programs should aim to deliver an experience that addresses the gaps of current ward-based teaching, offers personalised and real-time feedback, and is repeated to allow for progression and improvement in technical and non-technical outcomes in a way that is feasible within the resources of the respective institutions. With these considerations, it is expected that simulated ward rounds may offer a valuable opportunity as an additional tool to improve technical and non-technical skills and, therefore, produce work-ready junior doctors who are then capable of contributing to improving patient outcomes through improved medical expertise, improved patient-centred practice, and better interdisciplinary teamwork.
A strength of this systematic review is the diverse variety of studies, utilising a range of methods (both quantitative and qualitative), objectives, and outcomes to broadly evaluate the impact that simulated ward rounds can have on the training and development of final-year medical students. In fact, this review, to our knowledge, is the first to explore outcomes of this intervention in this space. Given that the majority of studies implementing simulated ward rounds are small-sample single-arm trials within single institutions, this review provides an insightful overview of the current quantitative and qualitative positives and negatives of simulated ward rounds across multiple institutions, various countries, and two continents, with rigorous methodology in accordance with the PRISMA guidelines. Another key strength of this review is in the metasynthesis of qualitative, quantitative, and mixed-methods data. Simulated ward rounds and their impact of clinical skills can be evaluated in both methods. Quantitative methods provide tangible ways to assess improvement on strict or standardised scales, whilst qualitative studies allow for the investigation and understanding of the key themes and experiences of simulated ward rounds. In metasynthesising these outcomes, this review is able to provide a deeper understanding of the impacts of this pedagogical approach to education with respect to clinical competencies, as well as the medical student experience of simulated ward rounds. The limitations of this review include those due to the complexities of integrating and assessing qualitative and quantitative findings. As discussed earlier, due to the paucity of homogeneous quantitative data, as well as the fact that all studies were single-arm, we were unable to perform a meta-analysis to gain a true understanding of the effect size of the quantitative outcomes. With respect to the qualitative outcomes, given the breadth of evaluation by the individual studies, we captured additional qualitative themes within our outcomes beyond those originally identified within our research protocol, thus representing a deviation from our a priori design. Additionally, due to the small sample sizes of the included studies and the predominant method of invitation-only recruitment, there was a high risk of selection bias within some studies, and therefore, the validity, generalisability, and reliability of the outcomes should be considered with caution. For example, the predominance of studies published within the United Kingdom limits the generalisability and relevance of the study findings toward culturally diverse medical education institutions, whereby the approach to simulation may differ. The small study populations are also highly relevant for qualitative studies, where there is a risk that those providing feedback on the simulated ward round sessions are students that are more enthusiastic and engaged in their education and development. Furthermore, within our quality and risk of bias assessment, it was clear that many of the included studies were of a low to moderate quality with a moderate to high risk of bias. Therefore, the results of this systematic review should also be considered with caution, and more rigorous trials of simulated ward rounds need to occur for medical educators to critically examine the true qualitative and quantitative benefits of this educational intervention to support their more widespread application in the global medical curriculum. Lastly, an overarching and highly relevant limitation that must be considered in simulated ward rounds, as highlighted by the included studies, is the interpretation of the transferability of skills. At this point in time, it is important to note that the transferability of the positive outcomes, with respect to clinical competencies towards real-life work and practice, is yet to be evaluated in the literature. A key reason for this is these studies which evaluate simulated programs lack in their design follow-up of such students in their working careers to assess the efficacy and effectiveness of the original simulated training. In theory, it would be expected that improvements in task prioritisation, situational awareness, empathy, communication, and other technical and non-technical competencies would translate into clinical work following practice in standardised settings, as seen with trauma training scenarios and approaches to basic and advanced life support. However, given the variability of hospital settings, the diversity of patient interactions, and the demands of busy hospital units, the real impact on clinical outcomes is not as clear, particularly with the highly heterogeneous methods of interpreting, designing, and implementing simulated ward rounds. Nonetheless, it is clear that simulated ward rounds offer students the ability to hone their technical and non-technical competencies that otherwise are not possible with the heterogeneity and variability of current hospital placements. Therefore, as an educational adjunct, simulated ward rounds can be useful to fill in gaps and provide ability for repeated practice, provided that the limitations are recognised and supplemented with clinical learning opportunities, lectures, and other pedagogical approaches to medical education.
With regard to future directions, our review found that many students find it particularly challenging to navigate clinical situations involving palliative care, end-of-life care discussions, ethical dilemmas, and conflict with interprofessional colleagues. Therefore, as part of developing more highly relevant simulated ward rounds to best allow final-year medical students to acquire transferable skills for clinical work, future simulations should include a contemporary curriculum with scenarios exploring these situations, as well as other potentially important psychosocial circumstances such as in working with patients with specific cultural, indigenous, or LBGTQI+ considerations. Lastly, the implementation of simulated ward rounds must also consider appropriate resource allocation and costs. Notwithstanding the need for multiple staff for implementation, simulated ward round development is also labour-intensive, requiring significant time and resources to develop appropriate scenarios and supporting materials, including consumables, mock radiology images and reports, and mock laboratory results. In some cases, the use of a high-fidelity simulation mannequin (such as SimMan) is also used and would incur significant costs to purchase as well as to maintain. It is likely the true cost of implementation will be highly variable, and further research, such as cost-effectiveness analyses and auditing, is required to best identify the most appropriate balance of resource allocation in developing these educational experiences. With the current landscape of generative artificial intelligence and the evolving multi-sectoral adoption of this technology, the potential for popular open-access forms of these tools (e.g., ChatGPT [OpenAI, San Francisco, CA, USA]) is exciting. Educators may be able to save the time and costs required to develop appropriate and curriculum-relevant simulated ward rounds that capture all pre-identified learning outcomes through the use of these tools. Certainly, this is an exciting possibility in the broader field of education, however, it also highlights the necessary role of educators to audit and verify the outputs of these tools to ensure they remain evidence-based, appropriate, and relevant with respect to the curriculum. Further, the implementation of generative artificial intelligence for this purpose must also be considered in the realms of ethical practice, particularly when it comes to ownership of the materials generated, confidentiality and privacy.
5. Conclusions
Simulated ward rounds offer a highly valuable and exciting method for medical educators to address the current challenges of delivering quality, standardised, and highly relevant clinical teaching to final-year medical students to ensure they are competent and work=ready. Despite this potential, current studies exploring their implementation are limited and of low to moderate scientific rigour. Due to this, it is difficult at this time to understand the true educational value of implementing simulated ward rounds in the current medical curriculum. The findings of this review are promising, suggesting simulated ward rounds have the potential for technical skill building and improving the confidence and preparedness of final-year medical students for clinical practice. Further research is required to better support best-practice development and delivery of simulated ward rounds.
Author Contributions
Conceptualization, K.D.R.L. and E.D.; methodology, K.D.R.L., E.D. and C.S.; software, K.D.R.L.; validation, K.D.R.L., E.D., E.A.-Y. and C.S.; formal analysis, K.D.R.L., E.D., E.A.-Y. and C.S.; investigation, K.D.R.L., E.D., E.A.-Y. and C.S.; resources, K.D.R.L., E.D., E.A.-Y. and C.S.; data curation, K.D.R.L., E.D., E.A.-Y. and C.S.; writing—original draft preparation, K.D.R.L., E.D. and C.S.; writing—review and editing, K.D.R.L., E.D., E.A.-Y. and C.S.; visualization, K.D.R.L., E.D. and C.S.; supervision, C.S.; project administration, K.D.R.L.; funding acquisition, N/A. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The data used to create this manuscript were obtained from publicly available, open-access peer reviewed literature.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Goldacre, M.J.; Lambert, T.W.; Svirko, E. Foundation doctors’ views on whether their medical school prepared them well for work: UK graduates of 2008 and 2009. Postgrad. Med. J. 2014, 90, 63–68. [Google Scholar] [CrossRef]
- Monrouxe, L.V.; Grundy, L.; Mann, M.; John, Z.; Panagoulas, E.; Bullock, A.; Mattick, K. How prepared are UK medical graduates for practice? A rapid review of the literature 2009–2014. BMJ Open 2017, 7, e013656. [Google Scholar] [CrossRef]
- Nikendei, C.; Kraus, B.; Schrauth, M.; Briem, S.; Jünger, J. Ward rounds: How prepared are future doctors? Med. Teach. 2008, 30, 88–91. [Google Scholar] [CrossRef]
- Pucher, P.H.; Aggarwal, R.; Darzi, A. Surgical ward round quality and impact on variable patient outcomes. Ann. Surg. 2014, 259, 222–226. [Google Scholar] [CrossRef]
- Brennan, N.; Corrigan, O.; Allard, J.; Archer, J.; Barnes, R.; Bleakley, A.; Collett, T.; de Bere, S.R. The transition from medical student to junior doctor: Today’s experiences of Tomorrow’s Doctors. Med. Educ. 2010, 44, 449–458. [Google Scholar] [CrossRef]
- Spencer, R.; Coiera, E.; Logan, P. Variation in communication loads on clinical staff in the emergency department. Ann. Emerg. Med. 2004, 44, 268–273. [Google Scholar] [CrossRef]
- Tipping, M.D.; Forth, V.E.; O’Leary, K.J.; Malkenson, D.M.; Magill, D.B.; Englert, K.; Williams, M.V. Where did the day go?—A time-motion study of hospitalists. J. Hosp. Med. 2010, 5, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Weigl, M.; Müller, A.; Sevdalis, N.; Angerer, P. Relationships of multitasking, physicians’ strain, and performance: An observational study in ward physicians. J. Patient Saf. 2013, 9, 18–23. [Google Scholar] [CrossRef] [PubMed]
- Weigl, M.; Müller, A.; Zupanc, A.; Glaser, J.; Angerer, P. Hospital doctors’ workflow interruptions and activities: An observation study. BMJ Qual. Saf. 2011, 20, 491–497. [Google Scholar] [CrossRef] [PubMed]
- Behrens, C.; Dolmans, D.H.J.M.; Leppink, J.; Gormley, G.J.; Driessen, E.W. Ward round simulation in final year medical students: Does it promote students learning? Med. Teach. 2018, 40, 199–204. [Google Scholar] [CrossRef] [PubMed]
- Whittemore, R.; Knafl, K. The integrative review: Updated methodology. J. Adv. Nurs. 2005, 52, 546–553. [Google Scholar] [CrossRef]
- Sirriyeh, R.; Lawton, R.; Gardner, P.; Armitage, G. Reviewing studies with diverse designs: The development and evaluation of a new tool. J. Eval. Clin. Pract. 2012, 18, 746–752. [Google Scholar] [CrossRef] [PubMed]
- Harrison, R.; Jones, B.; Gardner, P.; Lawton, R. Quality assessment with diverse studies (QuADS): An appraisal tool for methodological and reporting quality in systematic reviews of mixed- or multi-method studies. BMC Health Serv. Res. 2021, 21, 144. [Google Scholar]
- Pluye, P.; Gagnon, M.P.; Griffiths, F.; Johnson-Lafleur, J. A scoring system for appraising mixed methods research, and concomitantly appraising qualitative, quantitative and mixed methods primary studies in Mixed Studies Reviews. Int. J. Nurs. Stud. 2009, 46, 529–546. [Google Scholar] [CrossRef] [PubMed]
- Pace, R.; Pluye, P.; Bartlett, G.; Macaulay, A.C.; Salsberg, J.; Jagosh, J.; Seller, R. Testing the reliability and efficiency of the pilot Mixed Methods Appraisal Tool (MMAT) for systematic mixed studies review. Int. J. Nurs. Stud. 2012, 49, 47–53. [Google Scholar] [CrossRef] [PubMed]
- OCEBM Levels of Evidence Working Group. “The Oxford 2011 Levels of Evidence”. Oxford Centre for Evidence-Based Medicine. 2011. Available online: http://wwwcebmnet/indexaspx?o=5653 (accessed on 22 June 2023).
- Behrens, C.C.; Driessen, E.W.; Dolmans, D.H.; Gormley, G.J. ‘A roller coaster of emotions’: A phenomenological study on medical students lived experiences of emotions in complex simulation. Adv. Simul. 2021, 6, 24. [Google Scholar] [CrossRef]
- Harvey, R.; Mellanby, E.; Dearden, E.; Medjoub, K.; Edgar, S. Developing non-technical ward-round skills. Clin. Teach. 2015, 12, 336–340. [Google Scholar] [CrossRef]
- Hawkins, A.; Tredgett, K. Use of high-fidelity simulation to improve communication skills regarding death and dying: A qualitative study. BMJ Support. Palliat. Care 2016, 6, 474–478. [Google Scholar] [CrossRef]
- Hawkins, N.; Younan, H.-C.; Fyfe, M.; Parekh, R.; McKeown, A. Exploring why medical students still feel underprepared for clinical practice: A qualitative analysis of an authentic on-call simulation. BMC Med. Educ. 2021, 21, 165. [Google Scholar] [CrossRef]
- Lewis, G.; McCullough, M.; Maxwell, A.P.; Gormley, G.J. Ethical reasoning through simulation: A phenomenological analysis of student experience. Adv. Simul. 2016, 1, 26. [Google Scholar] [CrossRef]
- Morgan, J.; Green, V.; Blair, J. Using simulation to prepare for clinical practice. Clin. Teach. 2018, 15, 57–61. [Google Scholar] [CrossRef]
- Smith, S.D.; Henn, P.; Gaffney, R.; Hynes, H.; McAdoo, J.; Bradley, C. A study of innovative patient safety education. Clin. Teach. 2012, 9, 37–40. [Google Scholar] [CrossRef]
- Thomas, I. Student views of stressful simulated ward rounds. Clin. Teach. 2015, 12, 346–352. [Google Scholar] [CrossRef]
- Manalayil, J.; Muston, A.; Ball, A.; Chevalier, D. 1HR ON-CALL—Using Simulated ON-CALL to Underpin Experiential Learning in Final Year Medical Students. J. Eur. CME. 2020, 9, 1832749. [Google Scholar] [CrossRef] [PubMed]
- MacDowall, J. The assessment and treatment of the acutely ill patient--the role of the patient simulator as a teaching tool in the undergraduate programme. Med. Teach. 2006, 28, 326–329. [Google Scholar] [CrossRef] [PubMed]
- Harvey, R.; Murray, K.; McKenzie, K.; Mellanby, E.; Crichton, F.; Henderson, D. Improving the non-technical ward round skills of medical students. Br. J. Hosp. Med. 2016, 77, 481–484. [Google Scholar] [CrossRef] [PubMed]
- Ford, H.; Cleland, J.; Thomas, I. Simulated ward round: Reducing costs, not outcomes. Clin. Teach. 2017, 14, 49–54. [Google Scholar] [CrossRef]
- Nikendei, C.; Kraus, B.; Lauber, H.; Schrauth, M.; Weyrich, P.; Zipfel, S.; Jünger, J.; Briem, S. An innovative model for teaching complex clinical procedures: Integration of standardised patients into ward round training for final year students. Med. Teach. 2007, 29, 246–252. [Google Scholar] [CrossRef] [PubMed]
- Pollard, J.; Tombs, M. Teaching Undergraduate Medical Students Non-Technical Skills: An Evaluation Study of a Simulated Ward Experience. Adv. Med. Educ. Pract. 2022, 13, 485–494. [Google Scholar] [CrossRef] [PubMed]
- Teagle, A.R.; George, M.; Gainsborough, N.; Haq, I.; Okorie, M. Preparing medical students for clinical practice: Easing the transition. Perspect. Med. Educ. 2017, 6, 277–280. [Google Scholar] [CrossRef]
- Parker, R.; Hodierne, L.; Anderson, E.S.; Davies, R.S.; Elloy, M. Academic ability and teamworking in medical students. Clin. Teach. 2019, 16, 209–213. [Google Scholar] [CrossRef] [PubMed]
- Thomas, I.; Nicol, L.; Regan, L.; Cleland, J.; Maliepaard, D.; Clark, L.; Walker, K.; Duncan, J. Driven to distraction: A prospective controlled study of a simulated ward round experience to improve patient safety teaching for medical students. BMJ Qual. Saf. 2015, 24, 154–161. [Google Scholar] [CrossRef] [PubMed]
- Powell, N.; Bruce, C.G.; Redfern, O. Teaching a ‘good’ ward round. Clin. Med. 2015, 15, 135–138. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).