Wedge Osteotomy of the Maxilla for the Treatment of Obstructive Sleep Apnea (OSA) Through Virtual Surgical Planning, CAD/CAM Technology: Consecutive Case Series
Abstract
1. Introduction
1.1. Clinical Signs
1.2. Therapeutic Approach
2. Materials and Methods
- Diagnosis of moderate to severe obstructive sleep apnea (OSA), confirmed by polysomnography with an apnea-hypopnea index (AHI) > 15.
- Multidisciplinary evaluation by the institutional OSA team, including a maxillofacial surgeon, dentist, pulmonologist, ENT specialist, and bariatric surgeon, with a consensus recommendation for mandibular advancement (MA).
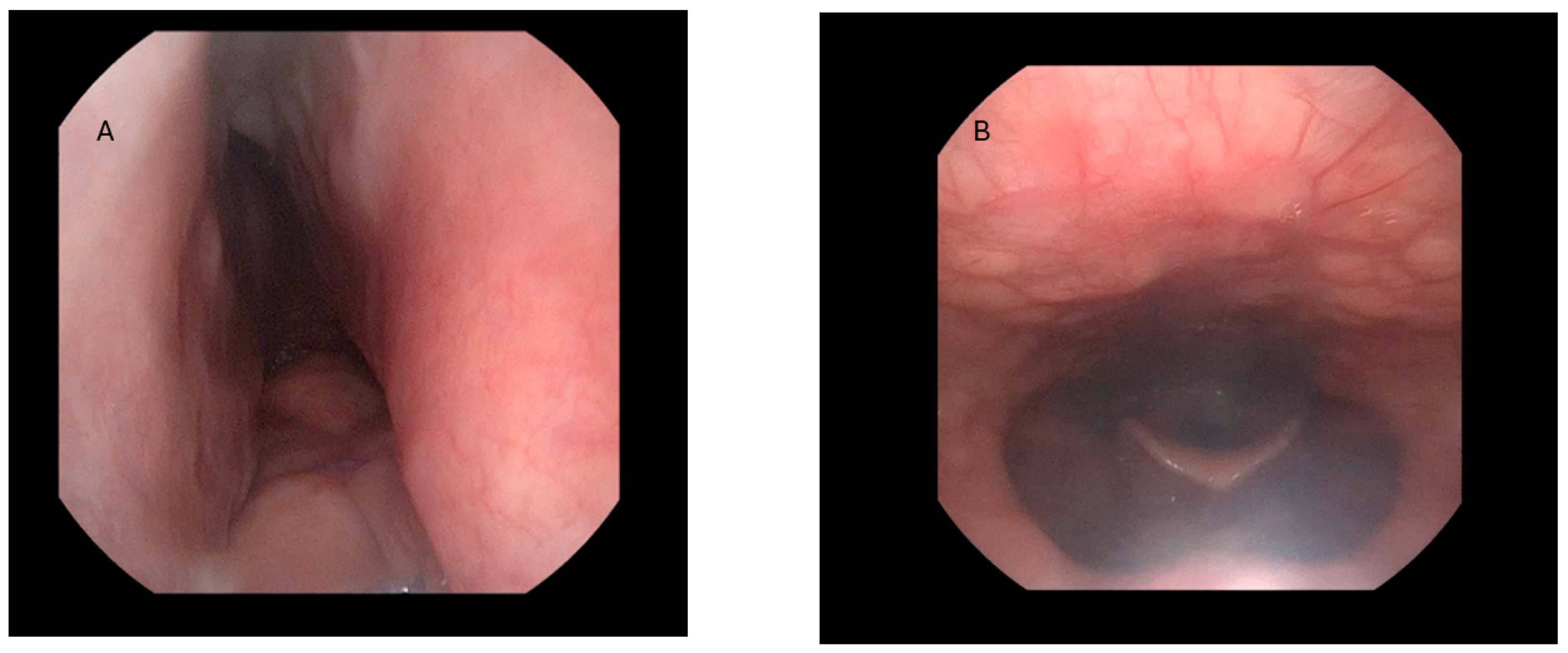
- Preoperative drug-induced sleep endoscopy (DISE) demonstrating potential benefit from MA, confirmed through mandibular advancement maneuvers.
- Good general health status with no contraindications to general anesthesia (ASA physical status classification ≤ 3).
- Patients not requiring maxillary advancement.
- Pediatric age group (<18 years).
- Presence of respiratory diseases or specific craniofacial malformations.
- Severe systemic conditions contraindicating general anesthesia (ASA ≥ 4).
- History of severe cardiovascular disease.
- Presence of psychiatric disorders.
- Syndromic conditions.
- Previous orthognathic surgery.
- Requirement for maxillary advancement.
- Refusal to provide informed consent.
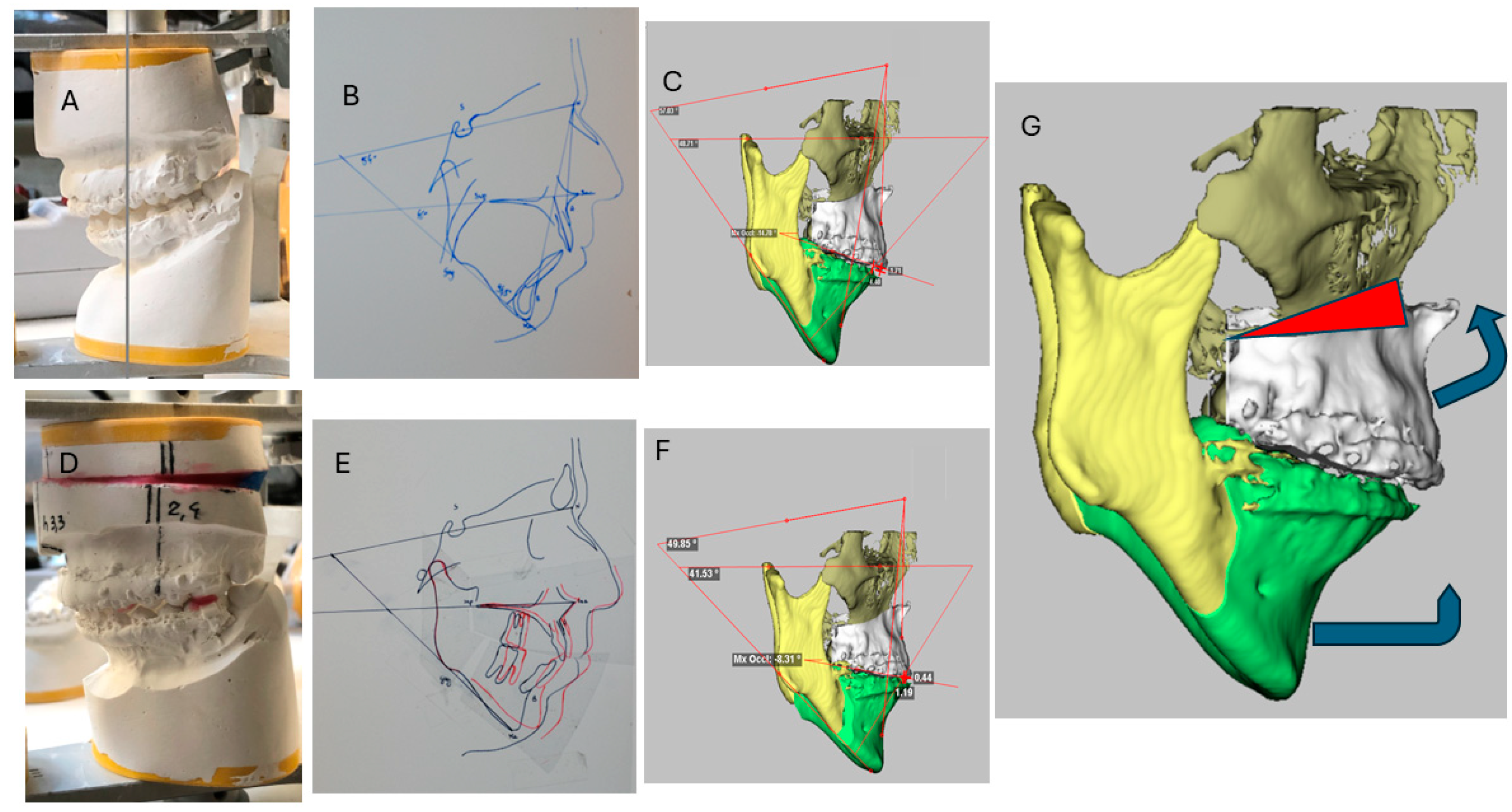
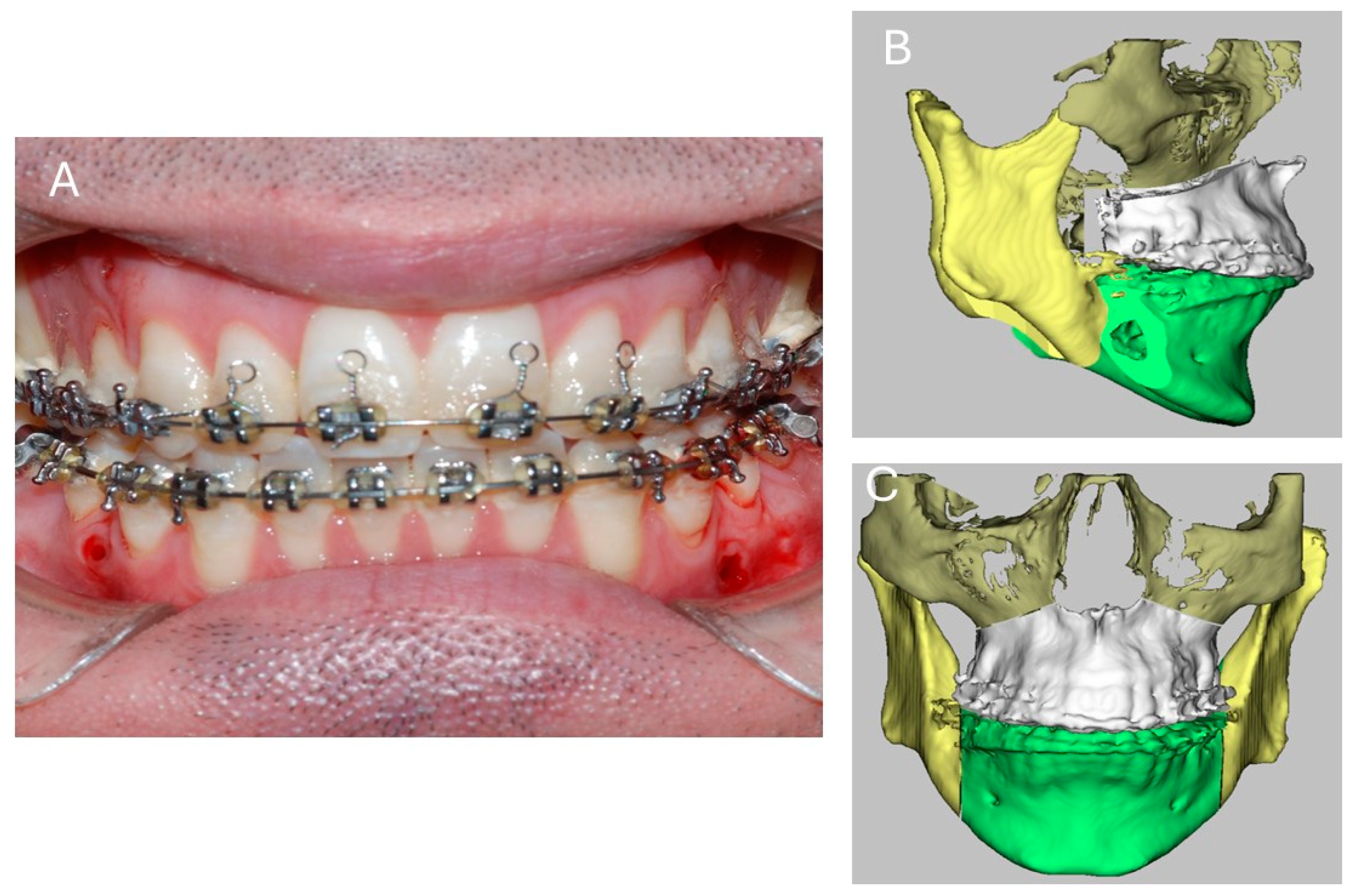
2.1. Surgical Procedures
2.2. Bilateral Sagittal Split Osteotomy (BSSO)
2.3. Statistical Analysis
3. Results
4. Discussion
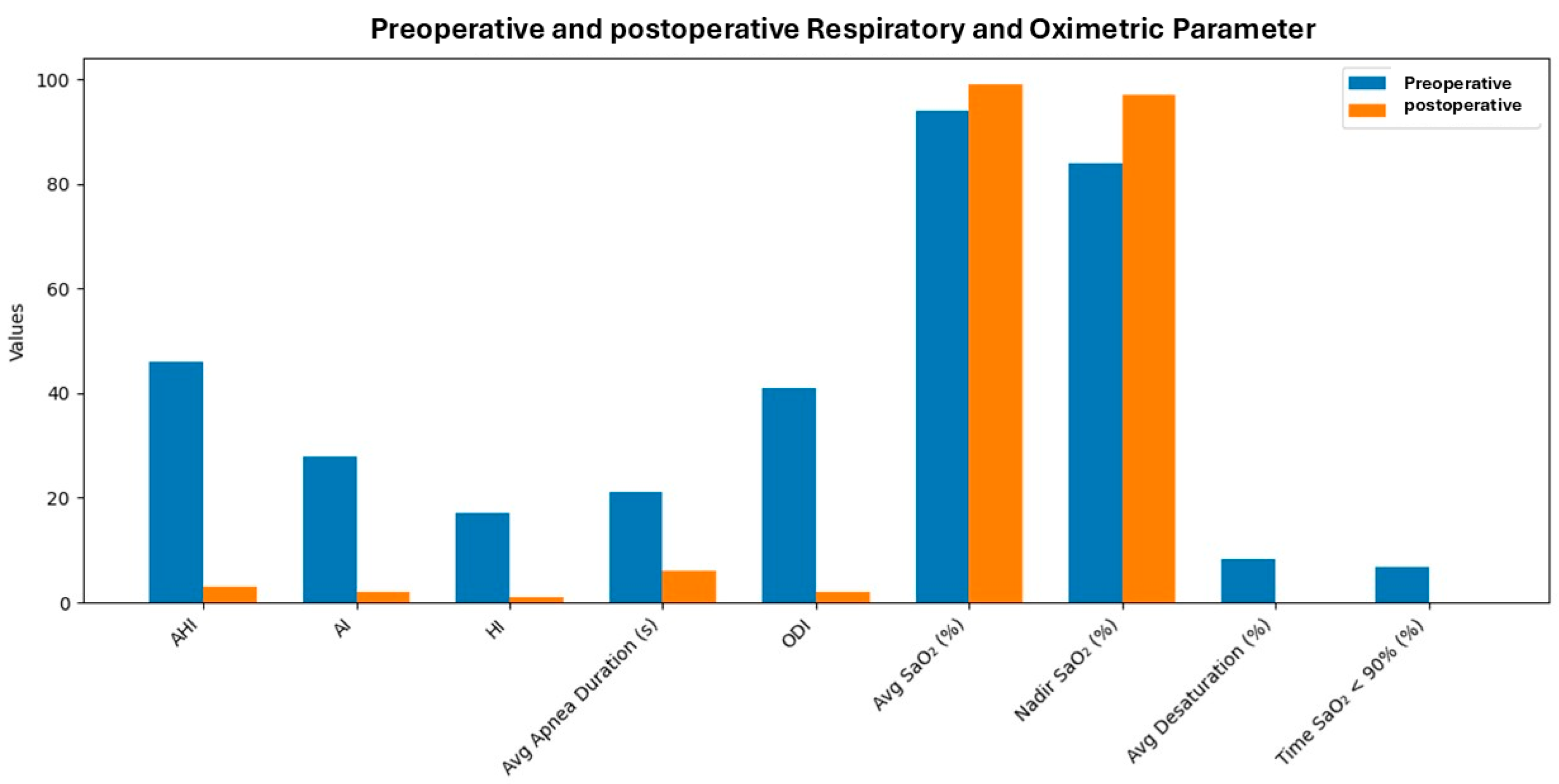
4.1. Impact on Respiratory and Oximetric Parameters
4.2. Advantages of Wedge Osteotomy
4.3. Comparisons with Other Studies
4.4. Impact on Airspace
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Locke, B.W.; Lee, J.J.; Sundar, K.M. OSA and Chronic Respiratory Disease: Mechanisms and Epidemiology. Int. J. Environ. Res. Public Health 2022, 19, 5473. [Google Scholar] [CrossRef] [PubMed]
- Gaffey, A.E.; Burg, M.M.; Yaggi, H.K.; Wang, K.; Brandt, C.A.; Haskell, S.G.; Bastian, L.A.; Chang, T.E.; Levine, A.; Skanderson, M.; et al. Insomnia, Sleep Apnea, and Incidence of Hypertension and Cardiovascular Disease. medRxiv 2025. [Google Scholar] [CrossRef] [PubMed]
- Seet, E.; Chung, F.; Wang, C.Y.; Tam, S.; Kumar, C.M.; Ubeynarayana, C.U.; Yim, C.C.; Chew, E.F.F.; Lam, C.K.M.; Cheng, B.C.P.; et al. Association of Obstructive Sleep Apnea With Difficult Intubation: Prospective Multicenter Observational Cohort Study. Anesth. Analg. 2021, 133, 196–204. [Google Scholar] [CrossRef] [PubMed]
- He, J.-M.; Yang, Y. Association between Neutrophil-Lymphocyte Ratio and All-Cause and Cardiovascular Mortality in Patients with Diabetes or Prediabetes with Comorbid Obstructive Sleep Apnea Symptoms: Evidence from NHANES 2005–2008 and 2015–2018. Front. Endocrinol. 2025, 16, 1512621. [Google Scholar] [CrossRef] [PubMed]
- Weaver, T.E.; Maislin, G.; Dinges, D.F.; Bloxham, T.; George, C.F.P.; Greenberg, H.; Kader, G.; Mahowald, M.; Younger, J.; Pack, A.I. Relationship between Hours of CPAP Use and Achieving Normal Levels of Sleepiness and Daily Functioning. Sleep 2007, 30, 711–719. [Google Scholar] [CrossRef] [PubMed]
- Knauert, M.P.; Adekolu, O.; Xu, Z.; Deng, A.; Chu, J.-H.; Baldassarri, S.R.; Kushida, C.; Yaggi, H.K.; Zinchuk, A. Morning Chronotype Is Associated with Improved Adherence to Continuous Positive Airway Pressure among Individuals with Obstructive Sleep Apnea. Ann. Am. Thorac. Soc. 2023, 20, 1182–1191. [Google Scholar] [CrossRef] [PubMed]
- Riley, R.W.; Powell, N.B.; Guilleminault, C.; Nino-Murcia, G. Maxillary, Mandibular, and Hyoid Advancement: An Alternative to Tracheostomy in Obstructive Sleep Apnea Syndrome. Otolaryngol. Head. Neck Surg. 1986, 94, 584–588. [Google Scholar] [CrossRef] [PubMed]
- Varghese, R.; Adams, N.G.; Slocumb, N.L.; Viozzi, C.F.; Ramar, K.; Olson, E.J. Maxillomandibular Advancement in the Management of Obstructive Sleep Apnea. Int. J. Otolaryngol. 2012, 2012, 373025. [Google Scholar] [CrossRef] [PubMed]
- Yu, M.S.; Ibrahim, B.; Riley, R.W.; Liu, S.Y.-C. Maxillomandibular Advancement and Upper Airway Stimulation: Extrapharyngeal Surgery for Obstructive Sleep Apnea. Clin. Exp. Otorhinolaryngol. 2020, 13, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Christino, M.; Vinha, P.P.; Faria, A.C.; Garcia, D.M.; de Mello-Filho, F.V. Impact of Counterclockwise Rotation of the Occlusal Plane on the Mandibular Advancement, Pharynx Morphology, and Polysomnography Results in Maxillomandibular Advancement Surgery for the Treatment of Obstructive Sleep Apnea Patients. Sleep. Breath. 2021, 25, 2307–2313. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.W.; Jeong, W.S.; Kang, M.K.; Lee, J.Y.; Chung, Y.S. Counterclockwise Rotational Orthognathic Surgery for the Obstructive Sleep Apnea in Class II Dentofacial Deformity: Polysomnography and 3D Computed Tomographic Analysis. Ann. Plast. Surg. 2021, 86, 640–646. [Google Scholar] [CrossRef] [PubMed]
- Shah, N.; Waite, P.D.; Kau, C.H. A Combined Orthodontic / Orthognathic Approach in the Management of Obstructive Sleep Apnoea: Balancing Treatment Efficacy and Facial Aesthetics. J. Orthod. 2020, 47, 354–362. [Google Scholar] [CrossRef] [PubMed]
- Jeong, W.S.; Kim, Y.C.; Chung, Y.S.; Lee, C.Y.; Choi, J.W. Change in Posterior Pharyngeal Space After Counterclockwise Rotational Orthognathic Surgery for Class II Dentofacial Deformity Diagnosed With Obstructive Sleep Apnea Based on Cephalometric Analysis. J. Craniofac Surg. 2017, 28, e488–e491. [Google Scholar] [CrossRef] [PubMed]
- Louro, R.S.; Calasans-Maia, J.A.; Mattos, C.T.; Masterson, D.; Calasans-Maia, M.D.; Maia, L.C. Three-Dimensional Changes to the Upper Airway after Maxillomandibular Advancement with Counterclockwise Rotation: A Systematic Review and Meta-Analysis. Int. J. Oral. Maxillofac. Surg. 2018, 47, 622–629. [Google Scholar] [CrossRef] [PubMed]
- Zinser, M.J.; Zachow, S.; Sailer, H.F. Bimaxillary “rotation Advancement” Procedures in Patients with Obstructive Sleep Apnea: A 3-Dimensional Airway Analysis of Morphological Changes. Int. J. Oral. Maxillofac. Surg. 2013, 42, 569–578. [Google Scholar] [CrossRef] [PubMed]
- Knudsen, T.B.; Laulund, A.S.; Ingerslev, J.; Homøe, P.; Pinholt, E.M. Improved Apnea-Hypopnea Index and Lowest Oxygen Saturation after Maxillomandibular Advancement with or without Counterclockwise Rotation in Patients with Obstructive Sleep Apnea: A Meta-Analysis. J. Oral. Maxillofac. Surg. 2015, 73, 719–726. [Google Scholar] [CrossRef] [PubMed]
- Trevisiol, L.; Bersani, M.; Lobbia, G.; Scirpo, R.; D’Agostino, A. Sequencing in Orthognathic Bimaxillary Surgery: Which Jaw Should Be Operated First? A Scoping Review. J. Clin. Med. 2023, 12, 6826. [Google Scholar] [CrossRef] [PubMed]

| Parameter | Preoperative | Postoperative | Clinical Interpretation |
|---|---|---|---|
| Snoring | 68% | 0% | Complete resolution of snoring, indicating reduced obstruction. |
| Apnea-Hypopnea Index (AHI) | 46 events/hour | 3 events/hour | >90% reduction; normalization of respiratory pattern. |
| Apnea Index (AI) | 28 events/hour | 2 events/hour | Significant reduction in complete apneas. |
| Hypopnea Index (HI) | 17 events/hour | 1 event/hour | Near-complete resolution of hypopneas. |
| Average Apnea Duration | 21 ± 6 s | 6 s | Shorter events, reduced hemodynamic impact. |
| Parameter | Preoperative | Postoperative | Clinical Interpretation |
|---|---|---|---|
| Oxygen Desaturation Index (ODI) | 41 events/hour | 2 events/hour | Marked reduction in desaturation episodes. |
| Average Oxygen Saturation (SaO2) | 94 ± 2% | 99% | Improved systemic oxygenation. |
| Nadir Oxygen Saturation (SaO2) | 84% | 97% | Higher minimum saturation; reduced hypoxic burden. |
| Average Desaturation | 8.4% | 0% | Elimination of oxygen desaturation events. |
| Time with SaO2 < 90% | 6.9% | 0% | No time spent in clinically significant hypoxemia. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Scarano, A.; Pistilli, R.; Govoni, F.A.; Di Nezza, S.; Tarascio, L.; Pica, F.; De Paolis, L.; Celebrini, A.; Magliacani, V.; Bellocchi, G.; et al. Wedge Osteotomy of the Maxilla for the Treatment of Obstructive Sleep Apnea (OSA) Through Virtual Surgical Planning, CAD/CAM Technology: Consecutive Case Series. Surgeries 2025, 6, 74. https://doi.org/10.3390/surgeries6030074
Scarano A, Pistilli R, Govoni FA, Di Nezza S, Tarascio L, Pica F, De Paolis L, Celebrini A, Magliacani V, Bellocchi G, et al. Wedge Osteotomy of the Maxilla for the Treatment of Obstructive Sleep Apnea (OSA) Through Virtual Surgical Planning, CAD/CAM Technology: Consecutive Case Series. Surgeries. 2025; 6(3):74. https://doi.org/10.3390/surgeries6030074
Chicago/Turabian StyleScarano, Antonio, Roberto Pistilli, Flavio Andrea Govoni, Silvio Di Nezza, Luca Tarascio, Filippo Pica, Luca De Paolis, Alessandra Celebrini, Vinicio Magliacani, Gianluca Bellocchi, and et al. 2025. "Wedge Osteotomy of the Maxilla for the Treatment of Obstructive Sleep Apnea (OSA) Through Virtual Surgical Planning, CAD/CAM Technology: Consecutive Case Series" Surgeries 6, no. 3: 74. https://doi.org/10.3390/surgeries6030074
APA StyleScarano, A., Pistilli, R., Govoni, F. A., Di Nezza, S., Tarascio, L., Pica, F., De Paolis, L., Celebrini, A., Magliacani, V., Bellocchi, G., & Marcelli, V. A. (2025). Wedge Osteotomy of the Maxilla for the Treatment of Obstructive Sleep Apnea (OSA) Through Virtual Surgical Planning, CAD/CAM Technology: Consecutive Case Series. Surgeries, 6(3), 74. https://doi.org/10.3390/surgeries6030074








