Protocol for the Development and Initial Validation of the COG-IMPACT Tool: A Purpose-Built Unmet Needs Assessment for Cancer-Related Cognitive Impairment
Abstract
1. Introduction
2. Design
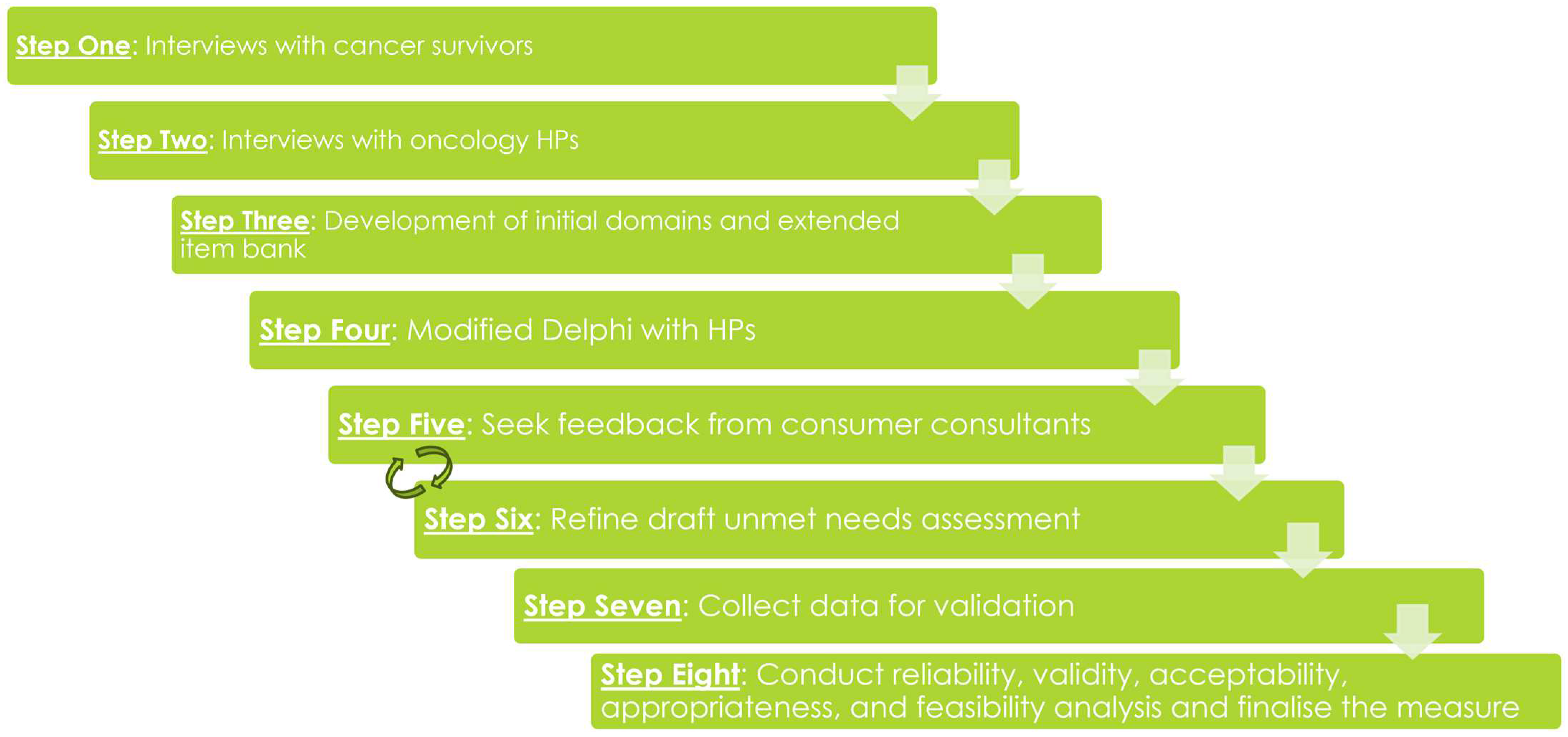
3. Procedure
3.1. Step #1
3.2. Step #2
3.3. Step #3
3.4. Step #4
3.5. Step #5
3.6. Step #6
3.7. Step #7
3.8. Step #8
4. Participants
4.1. Participant Descriptions
4.2. Recruitment
4.3. Sample Sizes
4.4. Data Collection Methods and Measures
4.5. Analyses
5. Expected Results
6. Future Research
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lange, M.; Licaj, I.; Clarisse, B.; Humbert, X.; Grellard, J.M.; Tron, L.; Joly, F. Cognitive complaints in cancer survivors and expectations for support: Results from a web–based survey. Cancer Med. 2019, 8, 2654–2663. [Google Scholar] [CrossRef] [PubMed]
- Lange, M.; Joly, F.; Vardy, J.; Ahles, T.; Dubois, M.; Tron, L.; Winocur, G.; De Ruiter, M.B.; Castel, H. Cancer-related cognitive impairment: An update on state of the art, detection, and management strategies in cancer survivors. Ann. Oncol. 2019, 30, 1925–1940. [Google Scholar] [CrossRef] [PubMed]
- Binarelli, G.; Duivon, M.; Joly, F.; Ahmed-Lecheheb, D.; Lange, M. Cancer-related cognitive impairment: Current perspectives on the management of cognitive changes following cancer treatment. Expert Rev. Neurother. 2023, 23, 249–268. [Google Scholar] [CrossRef] [PubMed]
- Mayo, S.J.; Lustberg, M.; M Dhillon, H.; Nakamura, Z.M.; Allen, D.H.; Von Ah, D.; C Janelsins, M.; Chan, A.; Olson, K.; Tan, C.J. Cancer-related cognitive impairment in patients with non-central nervous system malignancies: An overview for oncology providers from the MASCC Neurological Complications Study Group. Support. Care Cancer 2021, 29, 2821–2840. [Google Scholar] [CrossRef]
- Janelsins, M.C.; Kesler, S.R.; Ahles, T.A.; Morrow, G.R. Prevalence, mechanisms, and management of cancer-related cognitive impairment. Int. Rev. Psychiatry 2014, 26, 102–113. [Google Scholar] [CrossRef] [PubMed]
- Yap, N.Y.; Toh, Y.L.; Tan, C.J.; Acharya, M.M.; Chan, A. Relationship between cytokines and brain-derived neurotrophic factor (BDNF) in trajectories of cancer-related cognitive impairment. Cytokine 2021, 144, 155556. [Google Scholar] [CrossRef]
- Bray, V.J.; Dhillon, H.M.; Vardy, J.L. Cancer-related cognitive impairment in adult cancer survivors: A review of the literature. Cancer Forum 2017, 41, 46–54. [Google Scholar]
- Wei, Y.; Womer, F.Y.; Sun, K.; Zhu, Y.; Sun, D.; Duan, J.; Zhang, R.; Wei, S.; Jiang, X.; Zhang, Y. Applying dimensional psychopathology: Transdiagnostic prediction of executive cognition using brain connectivity and inflammatory biomarkers. Psychol. Med. 2022, 53, 3557–3567. [Google Scholar] [CrossRef] [PubMed]
- Joormann, J.; Yoon, K.L.; Zetsche, U. Cognitive inhibition in depression. Appl. Prev. Psychol. 2007, 12, 128–139. [Google Scholar] [CrossRef]
- Daban, C.; Mathieu, F.; Raust, A.; Cochet, B.; Scott, J.; Etain, B.; Leboyer, M.; Bellivier, F. Is processing speed a valid cognitive endophenotype for bipolar disorder? J. Affect. Disord. 2012, 139, 98–101. [Google Scholar] [CrossRef]
- Malekizadeh, H.; Saed, O.; Rashtbari, A.; Sajjadi, M.; Ahmadi, D.; Ronold, E.H. Deficits in specific executive functions manifest by severity in major depressive disorder: A comparison of antidepressant naïve inpatient, outpatient, subclinical, and healthy control groups. Front. Psychiatry 2023, 14, 1225062. [Google Scholar] [CrossRef] [PubMed]
- Romer, A.L.; Pizzagalli, D.A. Is executive dysfunction a risk marker or consequence of psychopathology? A test of executive function as a prospective predictor and outcome of general psychopathology in the adolescent brain cognitive development study®. Dev. Cogn. Neurosci. 2021, 51, 100994. [Google Scholar] [CrossRef] [PubMed]
- Hu, S.; Baraghoshi, D.; Chang, C.P.; Rowe, K.; Snyder, J.; Deshmukh, V.; Newman, M.; Fraser, A.; Smith, K.; Peoples, A.R. Mental health disorders among ovarian cancer survivors in a population-based cohort. Cancer Med. 2023, 12, 1801–1812. [Google Scholar] [CrossRef] [PubMed]
- Haywood, D.; Kotov, R.; Krueger, R.F.; Wright, A.G.C.; Forbes, M.K.; Dauer, E.; Baughman, F.D.; Rossell, S.L.; Hart, N.H. Is it time to discard the diagnostic and Statistical Manual of mental disorders (DSM) in psycho-oncology? Cancer Lett. 2024, 589, 216818. [Google Scholar] [CrossRef] [PubMed]
- Ji, X.; Cummings, J.R.; Gilleland Marchak, J.; Han, X.; Mertens, A.C. Mental health among nonelderly adult cancer survivors: A national estimate. Cancer 2020, 126, 3768–3776. [Google Scholar] [CrossRef] [PubMed]
- Lloyd, S.; Baraghoshi, D.; Tao, R.; Garrido-Laguna, I.; Gilcrease Iii, G.W.; Whisenant, J.; Weis, J.R.; Scaife, C.; Pickron, T.B.; Huang, L.C. Mental health disorders are more common in colorectal cancer survivors and associated with decreased overall survival. Am. J. Clin. Oncol. 2019, 42, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Haywood, D.; Kotov, R.; Krueger, R.F.; Wright, A.G.C.; Forbes, M.K.; Dauer, E.; Baughman, F.D.; Rossell, S.L.; Hart, N.H. Reconceptualizing mental health in cancer survivorship. Trends Cancer 2024. [Google Scholar] [CrossRef] [PubMed]
- Haywood, D.; Baughman, F.D.; Dauer, E.; Haywood, J.; Rossell, S.; Hart, N.H. It’s About Time: Mitigating Cancer-Related Cognitive Impairments Through Findings from Computational Models of the Wisconsin Card Sorting Task. BMC Cancer 2024, 24, 798. [Google Scholar] [CrossRef] [PubMed]
- Henderson, F.M.E.; Cross, A.J.; Baraniak, A.R. ‘A new normal with chemobrain’: Experiences of the impact of chemotherapy-related cognitive deficits in long-term breast cancer survivors. Health Psychol. Open 2019, 6, 2055102919832234. [Google Scholar] [CrossRef]
- Haywood, D.; Dauer, E.; Baughman, F.D.; Lawrence, B.J.; Rossell, S.L.; Hart, N.H.; O’Connor, M. “Is My Brain Ever Going to Work Fully Again?”: Challenges and Needs of Cancer Survivors with Persistent Cancer-Related Cognitive Impairment. Cancers 2023, 15, 5331. [Google Scholar] [CrossRef]
- He, S.; Lim, C.Y.S.; Dhillon, H.M.; Shaw, J. Australian oncology health professionals’ knowledge, perceptions, and clinical practice related to cancer-related cognitive impairment and utility of a factsheet. Support. Care Cancer 2022, 30, 4729–4738. [Google Scholar] [CrossRef]
- Duijts, S.F.A.; Van Der Beek, A.J.; Boelhouwer, I.G.; Schagen, S.B. Cancer-related cognitive impairment and patients’ ability to work: A current perspective. Curr. Opin. Support. Palliat. Care 2017, 11, 19–23. [Google Scholar] [CrossRef]
- Hart, N.H.; Stout, N.L.; Haywood, D.; Ashbury, F.D.; Chan, R.J.; Fitch, M.I.; Jefford, M.; Lustberg, M.B.; Etemadi, Y.; Rauch, A.; et al. World Health Organization package of interventions for rehabilitation for cancer: A MASCC-endorsed resource for global action to address unmet rehabilitation needs of people affected by cancer. Support. Care Cancer 2024, 32, 417. [Google Scholar] [CrossRef] [PubMed]
- Moreno, A.M.; Hamilton, R.A.; Currier, M.B. Cancer-Related Cognitive Impairment: Diagnosis, Pathogenesis, and Management. In Breast Cancer and Gynecologic Cancer Rehabilitation; Elsevier: Amsterdam, The Netherlands, 2021; pp. 211–223. [Google Scholar]
- Campbell, K.L.; Zadravec, K.; Bland, K.A.; Chesley, E.; Wolf, F.; Janelsins, M.C. The effect of exercise on cancer-related cognitive impairment and applications for physical therapy: Systematic review of randomized controlled trials. Phys. Ther. 2020, 100, 523–542. [Google Scholar] [CrossRef]
- Ehlers, D.K.; Fanning, J.; Salerno, E.A.; Aguiñaga, S.; Cosman, J.; Severson, J.; Kramer, A.F.; McAuley, E. Replacing sedentary time with physical activity or sleep: Effects on cancer-related cognitive impairment in breast cancer survivors. BMC Cancer 2018, 18, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Zimmer, P.; Baumann, F.T.; Oberste, M.; Wright, P.; Garthe, A.; Schenk, A.; Elter, T.; Galvao, D.A.; Bloch, W.; Hübner, S.T. Effects of exercise interventions and physical activity behavior on cancer related cognitive impairments: A systematic review. BioMed Res. Int. 2016, 2016, 1820954. [Google Scholar] [CrossRef]
- Henneghan, A.M.; Van Dyk, K.; Kaufmann, T.; Harrison, R.; Gibbons, C.; Heijnen, C.; Kesler, S.R. Measuring self-reported cancer-related cognitive impairment: Recommendations from the cancer neuroscience initiative working group. JNCI J. Natl. Cancer Inst. 2021, 113, 1625–1633. [Google Scholar] [CrossRef] [PubMed]
- Haywood, D.; Wallace, I.N.; Lawrence, B.; Baughman, F.D.; Dauer, E.; O’Connor, M. Oncology healthcare professionals’ perceptions and experiences of’chemobrain’in cancer survivors and persons undergoing cancer treatment. Gen. Hosp. Psychiatry 2023, 84, 271–272. [Google Scholar] [CrossRef]
- Shim, E.-J.; Lee, K.-S.; Park, J.-H.; Park, J.-H. Comprehensive needs assessment tool in cancer (CNAT): The development and validation. Support. Care Cancer 2011, 19, 1957–1968. [Google Scholar] [CrossRef]
- Campbell, H.S.; Sanson-Fisher, R.; Turner, D.; Hayward, L.; Wang, X.S.; Taylor-Brown, J. Psychometric properties of cancer survivors’ unmet needs survey. Support. Care Cancer 2011, 19, 221–230. [Google Scholar] [CrossRef]
- Ottati, A.; Feuerstein, M. Brief self-report measure of work-related cognitive limitations in breast cancer survivors. J. Cancer Surviv. 2013, 7, 262–273. [Google Scholar] [CrossRef]
- Linstone, H.A.; Turoff, M. The Delphi Method; Addison-Wesley: Reading, MA, USA, 1975. [Google Scholar]
- Meadows, K. Cognitive Interviewing Methodologies; SAGE Publications Sage CA: Los Angeles, CA, USA, 2021; Volume 30, pp. 375–379. [Google Scholar]
- Palan, S.; Schitter, C. Prolific. ac—A subject pool for online experiments. J. Behav. Exp. Financ. 2018, 17, 22–27. [Google Scholar] [CrossRef]
- Uittenhove, K.; Jeanneret, S.; Vergauwe, E. From lab-based to web-based behavioural research: Who you test is more important than how you test. PsyArXiv 2022, preprint. [Google Scholar]
- Moadel, A.B.; Morgan, C.; Dutcher, J. Psychosocial needs assessment among an underserved, ethnically diverse cancer patient population. Cancer Interdiscip. Int. J. Am. Cancer Soc. 2007, 109, 446–454. [Google Scholar] [CrossRef] [PubMed]
- Braun, V.; Clarke, V. One size fits all? What counts as quality practice in (reflexive) thematic analysis? Qual. Res. Psychol. 2021, 18, 328–352. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Chapman, B.; Derakshan, N.; Grunfeld, E.A. Experiences of cognitive training on primary breast cancer survivor’s cognitive impairments at work: A longitudinal qualitative study. Br. J. Health Psychol. 2023, 28, 252–270. [Google Scholar] [CrossRef] [PubMed]
- Henry, J.D.; Crawford, J.R. The short-form version of the Depression Anxiety Stress Scales (DASS-21): Construct validity and normative data in a large non-clinical sample. Br. J. Clin. Psychol. 2005, 44, 227–239. [Google Scholar] [CrossRef]
- Hodgkinson, K.; Butow, P.; Hunt, G.E.; Pendlebury, S.; Hobbs, K.M.; Lo, S.K.; Wain, G. The development and evaluation of a measure to assess cancer survivors’ unmet supportive care needs: The CaSUN (Cancer Survivors’ Unmet Needs measure). Psycho-Oncol. J. Psychol. Soc. Behav. Dimens. Cancer 2007, 16, 796–804. [Google Scholar] [CrossRef]
- Hawthorne, G.; Richardson, J.; Osborne, R. The Assessment of Quality of Life (AQoL) instrument: A psychometric measure of health-related quality of life. Qual. Life Res. 1999, 8, 209–224. [Google Scholar] [CrossRef]
- Riley, W.T.; Pilkonis, P.; Cella, D. Application of the National Institutes of Health patient-reported outcomes measurement information system (PROMIS®) to mental health research. J. Ment. Health Policy Econ. 2011, 14, 201. [Google Scholar] [PubMed]
- Creswell, J.W.; Hanson, W.E.; Clark Plano, V.L.; Morales, A. Qualitative research designs: Selection and implementation. Couns. Psychol. 2007, 35, 236–264. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Is thematic analysis used well in health psychology? A critical review of published research, with recommendations for quality practice and reporting. Health Psychol. Rev. 2023, 17, 695–718. [Google Scholar] [CrossRef] [PubMed]
- Braun, V.; Clarke, V. Reflecting on reflexive thematic analysis. Qual. Res. Sport Exerc. Health 2019, 11, 589–597. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Haywood, D.; O’Connor, M.; Baughman, F.D.; Chan, A.; Chan, R.J.; Dauer, E.; Dhillon, H.M.; Henneghan, A.M.; Lawrence, B.J.; Lustberg, M.; et al. Protocol for the Development and Initial Validation of the COG-IMPACT Tool: A Purpose-Built Unmet Needs Assessment for Cancer-Related Cognitive Impairment. Methods Protoc. 2024, 7, 54. https://doi.org/10.3390/mps7040054
Haywood D, O’Connor M, Baughman FD, Chan A, Chan RJ, Dauer E, Dhillon HM, Henneghan AM, Lawrence BJ, Lustberg M, et al. Protocol for the Development and Initial Validation of the COG-IMPACT Tool: A Purpose-Built Unmet Needs Assessment for Cancer-Related Cognitive Impairment. Methods and Protocols. 2024; 7(4):54. https://doi.org/10.3390/mps7040054
Chicago/Turabian StyleHaywood, Darren, Moira O’Connor, Frank D. Baughman, Alexandre Chan, Raymond J. Chan, Evan Dauer, Haryana M. Dhillon, Ashley M. Henneghan, Blake J. Lawrence, Maryam Lustberg, and et al. 2024. "Protocol for the Development and Initial Validation of the COG-IMPACT Tool: A Purpose-Built Unmet Needs Assessment for Cancer-Related Cognitive Impairment" Methods and Protocols 7, no. 4: 54. https://doi.org/10.3390/mps7040054
APA StyleHaywood, D., O’Connor, M., Baughman, F. D., Chan, A., Chan, R. J., Dauer, E., Dhillon, H. M., Henneghan, A. M., Lawrence, B. J., Lustberg, M., Vardy, J. L., Rossell, S. L., & Hart, N. H. (2024). Protocol for the Development and Initial Validation of the COG-IMPACT Tool: A Purpose-Built Unmet Needs Assessment for Cancer-Related Cognitive Impairment. Methods and Protocols, 7(4), 54. https://doi.org/10.3390/mps7040054







