Worsening Renal Function and Adverse Outcomes in Patients with HFpEF with or without Atrial Fibrillation
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Definition of WRF
2.3. Study Outcomes
2.4. Follow-Up Method
2.5. Statistical Analysis
3. Results
3.1. Baseline Patient Characteristics
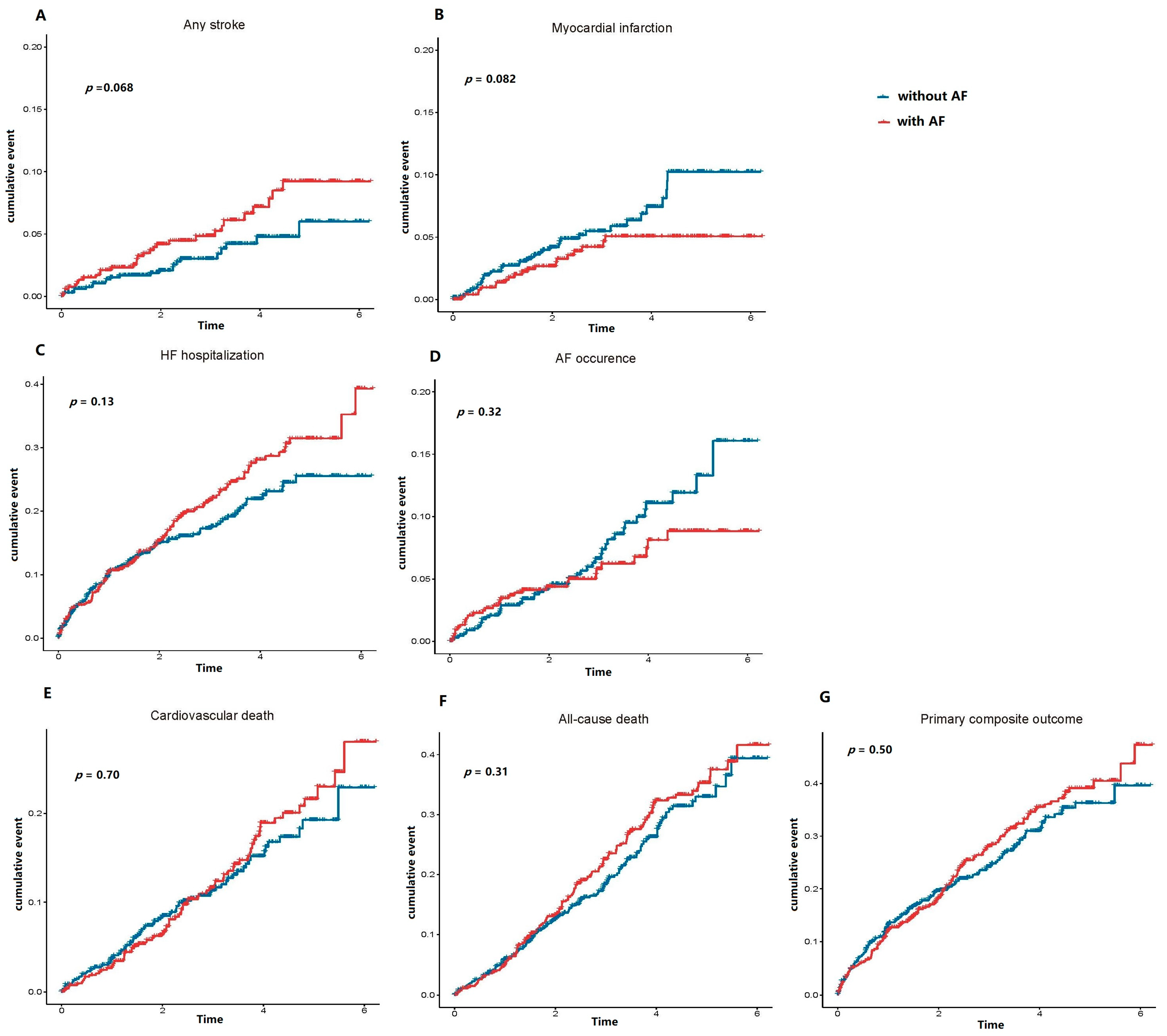
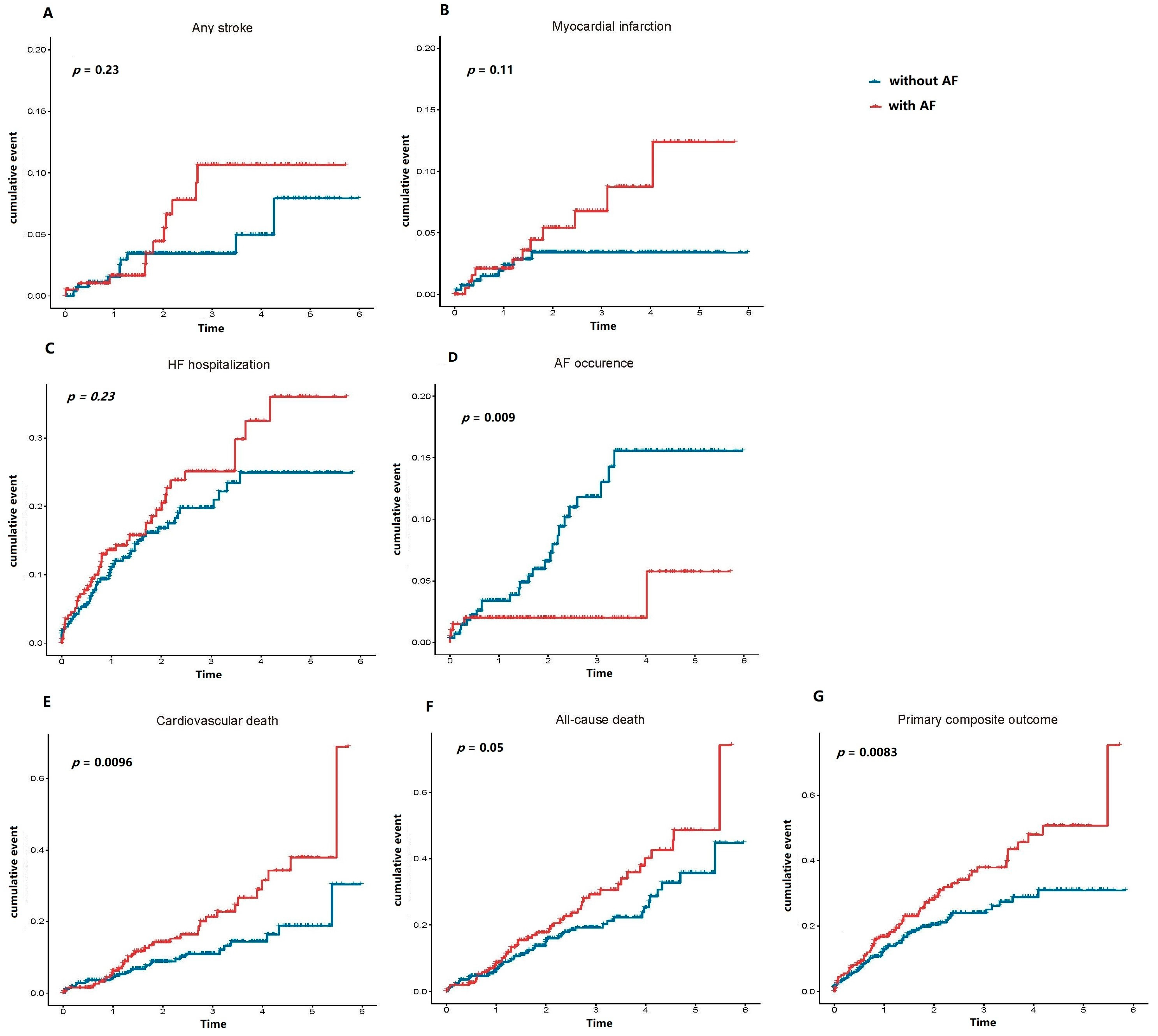
3.2. Cumulative Probability of Adverse Outcomes
3.3. Incidence Rates of Adverse Outcomes
3.4. Associations of WRF with Adverse Outcomes
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Snipelisky, D.; Chaudhry, S.P.; Stewart, G.C. The many faces of heart failure. Card. Electrophysiol. Clin. 2019, 11, 11–20. [Google Scholar] [CrossRef] [PubMed]
- Bock, J.S.; Gottlieb, S.S. Cardiorenal syndrome: New perspectives. Circulation 2010, 121, 2592–2600. [Google Scholar] [CrossRef] [PubMed]
- Damman, K.; Valente, M.A.; Voors, A.A.; O’Connor, C.M.; van Veldhuisen, D.J.; Hillege, H.L. Renal impairment, worsening renal function, and outcome in patients with heart failure: An updated meta-analysis. Eur. Heart J. 2014, 35, 455–469. [Google Scholar] [CrossRef] [PubMed]
- Dries, D.L.; Exner, D.V.; Domanski, M.J.; Greenberg, B.; Stevenson, L.W. The prognostic implications of renal insufficiency in asymptomatic and symptomatic patients with left ventricular systolic dysfunction. J. Am. Coll. Cardiol. 2000, 35, 681–689. [Google Scholar] [CrossRef]
- Hillege, H.L.; Girbes, A.R.; de Kam, P.J.; Boomsma, F.; de Zeeuw, D.; Charlesworth, A.; Hampton, J.R.; van Veldhuisen, D.J. Renal function, neurohormonal activation, and survival in patients with chronic heart failure. Circulation 2000, 102, 203–210. [Google Scholar] [CrossRef]
- Damman, K.; Solomon, S.D.; Pfeffer, M.A.; Swedberg, K.; Yusuf, S.; Young, J.B.; Rouleau, J.L.; Granger, C.B.; Mcmurray, J.J. Worsening renal function and outcome in heart failure patients with reduced and preserved ejection fraction and the impact of angiotensin receptor blocker treatment: Data from the CHARM-study programme. Eur. J. Heart Fail. 2016, 18, 1508–1517. [Google Scholar] [CrossRef]
- Tam, M.C.; Lee, R.; Cascino, T.M.; Konerman, M.C.; Hummel, S.L. Current perspectives on systemic hypertension in heart failure with preserved ejection fraction. Curr. Hypertens. Rep. 2017, 19, 12. [Google Scholar] [CrossRef]
- Lyle, M.A.; Brozovich, F.V. HFpEF, a disease of the vasculature: A closer look at the other half. Mayo Clin. Proc. 2018, 93, 1305–1314. [Google Scholar] [CrossRef]
- Kallistratos, M.S.; Poulimenos, L.E.; Manolis, A.J. Atrial fibrillation and arterial hypertension. Pharmacol. Res. 2018, 128, 322–326. [Google Scholar] [CrossRef]
- Rivero-Ayerza, M.; Scholte, O.R.W.; Lenzen, M.; Theuns, D.A.; Jordaens, L.; Komajda, M.; Follath, F.; Swedberg, K.; Cleland, J.G. New-onset atrial fibrillation is an independent predictor of in-hospital mortality in hospitalized heart failure patients: Results of the EuroHeart Failure Survey. Eur. Heart J. 2008, 29, 1618–1624. [Google Scholar] [CrossRef]
- Kotecha, D.; Lam, C.S.; Van Veldhuisen, D.J.; Van Gelder, I.C.; Voors, A.A.; Rienstra, M. Heart failure with preserved ejection fraction and atrial fibrillation: Vicious twins. J. Am. Coll. Cardiol. 2016, 68, 2217–2228. [Google Scholar] [CrossRef] [PubMed]
- Mamas, M.A.; Caldwell, J.C.; Chacko, S.; Garratt, C.J.; Fath-Ordoubadi, F.; Neyses, L. A meta-analysis of the prognostic significance of atrial fibrillation in chronic heart failure. Eur. J. Heart Fail. 2009, 11, 676–683. [Google Scholar] [CrossRef] [PubMed]
- Pitt, B.; Pfeffer, M.A.; Assmann, S.F.; Boineau, R.; Anand, I.S.; Claggett, B.; Clausell, N.; Desai, A.S.; Diaz, R.; Fleg, J.L.; et al. Spironolactone for heart failure with preserved ejection fraction. N. Engl. J. Med. 2014, 370, 1383–1392. [Google Scholar] [CrossRef] [PubMed]
- Bristow, M.R.; Enciso, J.S.; Gersh, B.J.; Grady, C.; Rice, M.M.; Singh, S.; Sopko, G.; Boineau, R.; Rosenberg, Y.; Greenberg, B.H. Detection and management of geographic disparities in the TOPCAT trial: Lessons learned and derivative recommendations. JACC Basic. Transl. Sci. 2016, 1, 180–189. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Pfeffer, M.A.; Claggett, B.; Assmann, S.F.; Boineau, R.; Anand, I.S.; Clausell, N.; Desai, A.S.; Diaz, R.; Fleg, J.L.; Gordeev, I.; et al. Regional variation in patients and outcomes in the Treatment of Preserved Cardiac Function Heart Failure with an Aldosterone Antagonist (TOPCAT) trial. Circulation 2015, 131, 34–42. [Google Scholar] [CrossRef]
- Beldhuis, I.E.; Myhre, P.L.; Bristow, M.; Claggett, B.; Damman, K.; Fang, J.C.; Fleg, J.L.; Mckinlay, S.; Lewis, E.F.; O’Meara, E.; et al. Spironolactone in patients with heart failure, preserved ejection fraction, and worsening renal function. J. Am. Coll. Cardiol. 2021, 77, 1211–1221. [Google Scholar] [CrossRef]
- Levey, A.S.; Inker, L.A.; Matsushita, K.; Greene, T.; Willis, K.; Lewis, E.; de Zeeuw, D.; Cheung, A.K.; Coresh, J. GFR decline as an end point for clinical trials in CKD: A scientific workshop sponsored by the National Kidney Foundation and the US Food and Drug Administration. Am. J. Kidney Dis. 2014, 64, 821–835. [Google Scholar] [CrossRef]
- Costanzo, M.R. The cardiorenal syndrome in heart failure. Heart Fail. Clin. 2020, 16, 81–97. [Google Scholar] [CrossRef]
- Rosner, M.H.; Ronco, C.; Okusa, M.D. The role of inflammation in the cardio-renal syndrome: A focus on cytokines and inflammatory mediators. Semin. Nephrol. 2012, 32, 70–78. [Google Scholar] [CrossRef]
- Testani, J.M.; Brisco-Bacik, M.A. Worsening renal function and mortality in heart failure: Causality or confounding? Circ. Heart Fail. 2017, 10, e003835. [Google Scholar] [CrossRef]
- Yancy, C.W.; Jessup, M.; Bozkurt, B.; Butler, J.; Casey, D.J.; Colvin, M.M.; Drazner, M.H.; Filippatos, G.S.; Fonarow, G.C.; Givertz, M.M.; et al. 2017 ACC/AHA/HFSA focused update of the 2013 ACCF/AHA guideline for the management of heart failure: A report of the american college of Cardiology/American heart association task force on clinical practice guidelines and the heart failure society of america. J. Card. Fail. 2017, 23, 628–651. [Google Scholar]
- Kang, J.; Park, J.J.; Cho, Y.J.; Oh, I.Y.; Park, H.A.; Lee, S.E.; Kim, M.S.; Cho, H.J.; Lee, H.Y.; Choi, J.O.; et al. Predictors and prognostic value of worsening renal function during admission in HFpEF versus HFrEF: Data from the KorAHF (Korean acute heart failure) registry. J. Am. Heart Assoc. 2018, 7, e007910. [Google Scholar] [CrossRef] [PubMed]
- Kotecha, D.; Holmes, J.; Krum, H.; Altman, D.G.; Manzano, L.; Cleland, J.G.; Lip, G.Y.; Coats, A.J.; Andersson, B.; Kirchhof, P.; et al. Efficacy of beta blockers in patients with heart failure plus atrial fibrillation: An individual-patient data meta-analysis. Lancet 2014, 384, 2235–2243. [Google Scholar] [CrossRef] [PubMed]
- Guo, Y.; Gao, J.; Ye, P.; Xing, A.; Wu, Y.; Wu, S.; Luo, Y. Comparison of atrial fibrillation in CKD and non-CKD populations: A cross-sectional analysis from the Kailuan study. Int. J. Cardiol. 2019, 277, 125–129. [Google Scholar] [CrossRef] [PubMed]
- Carrero, J.J.; Trevisan, M.; Sood, M.M.; Barany, P.; Xu, H.; Evans, M.; Friberg, L.; Szummer, K. Incident atrial fibrillation and the risk of stroke in adults with chronic kidney disease: The stockholm CREAtinine measurements (SCREAM) project. Clin. J. Am. Soc. Nephrol. 2018, 13, 1314–1320. [Google Scholar] [CrossRef] [PubMed]
- Ding, W.Y.; Gupta, D.; Wong, C.F.; Lip, G. Pathophysiology of atrial fibrillation and chronic kidney disease. Cardiovasc. Res. 2021, 117, 1046–1059. [Google Scholar] [CrossRef]
- Ellis, E.R.; Josephson, M.E. Heart failure and tachycardia-induced cardiomyopathy. Curr. Heart Fail. Rep. 2013, 10, 296–306. [Google Scholar] [CrossRef]
- Uzieblo-Zyczkowska, B.; Krzesinski, P.; Maciorowska, M.; Gorczyca, I.; Jelonek, O.; Wojcik, M.; Blaszczyk, R.; Kaplon-Cieslicka, A.; Gawalko, M.; Tokarek, T.; et al. Antithrombotic therapy in patients with atrial fibrillation undergoing percutaneous coronary intervention, including compliance with current guidelines-data from the POLish Atrial Fibrillation (POL-AF) Registry. Cardiovasc. Diagn. Ther. 2021, 11, 14–27. [Google Scholar] [CrossRef]
- Welnicki, M.; Gorczyca-Glowacka, I.; Lubas, A.; Wojcik, W.; Jelonek, O.; Maciorowska, M.; Uzieblo-Zyczkowska, B.; Wojcik, M.; Blaszczyk, R.; Rajtar-Salwa, R.; et al. Association of hyperuricemia with impaired left ventricular systolic function in patients with atrial fibrillation and preserved kidney function: Analysis of the POL-AF registry cohort. Int. J. Environ. Res. Public. Health 2022, 19, 7288. [Google Scholar] [CrossRef]
| Overall (n = 1763) | HFpEF without AF (n = 1004) | HFpEF with AF (n = 759) | p-Value | |
|---|---|---|---|---|
| Demographics | ||||
| Age, yrs | 71.5 ± 9.7 | 69.6 ± 10.0 | 74.0 ± 8.6 | <0.001 |
| Male, n (%) | 884 (50.1%) | 476 (47.3%) | 408 (53.8%) | 0.028 |
| Race (white), n (%) | 1382 (78.3%) | 727 (72.3%) | 655 (86.3%) | <0.001 |
| Current smoker, n (%) | 117 (6.6%) | 86 (8.6%) | 31 (4.1%) | <0.001 |
| BMI, kg/m2 | 33.83 ± 8.2 | 34.4 ± 8.5 | 33.0 ± 7.6 | <0.001 |
| Physical examinations | ||||
| HR, bpm | 69.1 ± 11.2 | 69.2 ± 11.6 | 68.9 ± 10.8 | 0.772 |
| SBP, mmHg | 127.5 ± 15.7 | 129.5 ± 16.1 | 124.8 ± 14.7 | <0.001 |
| DBP, mmHg | 71.3 ± 11.5 | 71.7 ± 11.8 | 70.9 ± 11.0 | 0.095 |
| EF, % | 58.2 ± 7.8 | 58.6 ± 8.0 | 57.5 ± 7.4 | 0.002 |
| eGFR, mL/min × 1.73 m2 | 60.7 ± 19.4 | 62.4 ± 20.5 | 58.6 ± 17.6 | <0.001 |
| Morbidities, n (%) | ||||
| WRF | 756 (42.9%) | 440 (43.8%) | 316 (41.6%) | 0.357 |
| DM | 788 (44.7%) | 516 (50.8%) | 278 (36.6%) | <0.001 |
| Asthma | 194 (11.0%) | 122 (12.2%) | 72 (9.5%) | 0.158 |
| HTN | 1586 (90.0%) | 913 (90.9%) | 673 (88.7%) | 0.149 |
| Angina pectoris | 485 (27.5%) | 291 (29.0%) | 194 (25.6%) | 0.158 |
| Previous MI | 359 (20.4%) | 221 (22.0%) | 138 (18.2%) | 0.08 |
| Previous stroke | 158 (9.0%) | 84 (8.4%) | 74 (9.7%) | 0.312 |
| NYHA functional class, n (%) | 0.899 | |||
| I–II | 1141 (64.8%) | 662 (65.0) | 479 (64.6) | |
| III–IV | 620 (35.2%) | 354 (35.3) | 266 (35.0) | |
| COPD | 291 (16.5%) | 163 (16.2) | 128 (16.9) | 0.697 |
| ICD | 42 (2.4%) | 20 (2.0%) | 22 (2.9%) | 0.372 |
| CABG | 336 (19.1%) | 200 (19.9%) | 136 (17.9%) | 0.222 |
| PCI | 344 (19.5%) | 221 (22.0%) | 123 (16.2%) | 0.009 |
| Pacemaker | 242 (13.7%) | 81 (8.1%) | 161 (21.2%) | <0.001 |
| Medications, n (%) | ||||
| Beta blocker | 1386 (78.6%) | 784 (78.1%) | 602 (79.3%) | 0.502 |
| CCB | 681 (38.6%) | 390 (38.8%) | 291 (38.3%) | 0.94 |
| Diuretics | 1571 (89.1%) | 874 (87.1%) | 697 (91.8%) | 0.002 |
| ACEI/ARB | 1393 (79.0%) | 797 (79.4%) | 596 (78.5%) | 0.503 |
| Aspirin | 1026 (58.2%) | 681 (67.8%) | 345 (45.5%) | <0.001 |
| Long-acting nitrate | 305 (17.3%) | 191 (19.0%) | 114 (15.0%) | 0.042 |
| Statins | 1148 (65.1%) | 664 (66.1%) | 484 (63.8%) | 0.441 |
| Warfarin | 592 (33.6%) | 59 (5.9%) | 533 (70.2%) | <0.001 |
| Outcomes | Overall | HFpEF with AF | HFpEF without AF |
|---|---|---|---|
| Primary endpoint | |||
| Prior to WRF | 10.3 (8.6–20.0) | 10.6 (8.0–13.2) | 10.0 (7.8–12.2) |
| Post-WRF | 12.1 (9.3–14.9) | 16.5 (11.6–21.5) | 9.3 (6.0–12.6) |
| All-cause death | |||
| Prior to WRF | 7.9 (6.4–9.4) | 8.5 (6.1–10.8) | 7.4 (5.5–9.4) |
| Post-WRF | 9.4 (6.9–11.9) | 11.5 (7.3–15.8) | 8.0 (4.9–11.0) |
| Cardiovascular death | |||
| Prior to WRF | 4.4 (3.2–5.5) | 4.6 (2.8–6.3) | 4.2 (2.7–5.7) |
| Post-WRF | 6.0 (4.0–8.0) | 8.3 (4.6–12.0) | 4.5 (2.2–6.9) |
| HF hospitalization | |||
| Prior to WRF | 7.4 (6.0–8.9) | 8.2 (5.9–10.5) | 6.8 (5.0–8.7) |
| Post-WRF | 8.8 (6.3–11.2) | 10.9 (6.7–15.0) | 7.4 (4.5–10.4) |
| Stroke | |||
| Prior to WRF | 1.5 (0.8–2.1) | 1.9 (0.7–3.0) | 1.1 (0.4–1.9) |
| Post-WRF | 2.0 (0.8–3.2) | 2.6 (0.5–4.7) | 1.5 (0.1–2.9) |
| MI | |||
| Prior to WRF | 1.7 (1.0–2.4) | 1.3 (0.3–2.2) | 2.1 (1.0–3.1) |
| Post-WRF | 1.7 (0.6–2.9) | 2.6 (0.4–4.7) | 1.2 (0–3.1) |
| * AF occurrence | |||
| Prior to WRF | 2.3 (1.5–3.1) | 2.0 (0.8–3.2) | 2.5 (1.4–3.7) |
| Post-WRF | 2.6 (1.2–4.0) | 0.9 (0.3–2.2) | 3.7 (1.6–5.9) |
| Outcomes | Overall | HFpEF with AF | HFpEF without AF | p for Interaction | |||
|---|---|---|---|---|---|---|---|
| Unadjusted | Adjusted | Unadjusted | Adjusted | Unadjusted | Adjusted | ||
| Primary composite outcome | 1.30 (1.07–1.57) | 1.29 (1.05–1.57) | 1.64 (1.24–2.16) | 1.58 (1.19–2.11) | 1.08 (0.82–1.41) | 1.10 (0.83–1.46) | 0.008 |
| All–cause death | 1.28 (1.04–1.57) | 1.36 (1.09–1.70) | 1.36 (1.01–1.84) | 1.50 (1.10–2.06) | 1.22 (0.91–1.64) | 1.24 (0.91–1.70) | 0.450 |
| Cardiovascular death | 1.33 (1.01–1.76) | 1.41 (1.06–1.88) | 1.84 (1.26–2.71) | 2.00 (1.34–3.00) | 0.99 (0.66–1.48) | 1.00 (0.65–1.53) | 0.005 |
| HF hospitalization | 1.31 (1.05–1.64) | 1.27 (1.00–1.60) | 1.44 (1.04–1.98) | 1.32 (0.94–1.85) | 1.28 (0.94–1.73) | 1.28 (0.93–1.76) | 0.319 |
| Stroke | 1.05 (0.64–1.73) | 1.05 (0.63–1.77) | 0.82 (0.40–1.68) | 0.82 (0.39–1.72) | 1.45 (0.71–2.98) | 1.49 (0.70–3.16) | 0.361 |
| MI | 1.23 (0.79–1.90) | 1.17 (0.75–1.85) | 1.33 (0.66–2.66) | 1.15 (0.55–2.41) | 1.14 (0.65–1.99) | 1.15 (0.64–2.06) | 0.651 |
| AF * | 1.01 (0.68–1.50) | 1.00 (0.66–1.50) | 0.46 (0.17–1.21) | 0.43 (0.16–1.16) | 1.17 (0.74–1.83) | 1.21 (0.76–1.94) | 0.015 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Guo, L.; Wu, X. Worsening Renal Function and Adverse Outcomes in Patients with HFpEF with or without Atrial Fibrillation. Biomedicines 2023, 11, 2484. https://doi.org/10.3390/biomedicines11092484
Guo L, Wu X. Worsening Renal Function and Adverse Outcomes in Patients with HFpEF with or without Atrial Fibrillation. Biomedicines. 2023; 11(9):2484. https://doi.org/10.3390/biomedicines11092484
Chicago/Turabian StyleGuo, Linjuan, and Xiaojuan Wu. 2023. "Worsening Renal Function and Adverse Outcomes in Patients with HFpEF with or without Atrial Fibrillation" Biomedicines 11, no. 9: 2484. https://doi.org/10.3390/biomedicines11092484
APA StyleGuo, L., & Wu, X. (2023). Worsening Renal Function and Adverse Outcomes in Patients with HFpEF with or without Atrial Fibrillation. Biomedicines, 11(9), 2484. https://doi.org/10.3390/biomedicines11092484






