Abstract
The present study emphasizes the importance of documenting ethnomedicinal plants and herbal practices of the local rural communities of Tehsil Hajira (Pakistan). The aim was to document, explore and quantify the traditional ethnomedicinal knowledge. Ethnobotanical data were collected using semi-structured questionnaires and analyzed using various quantitative indices. The results showed that 144 medicinal plant species from 70 families and 128 genera play an important role in herbal preparations. The most common type of preparation was powder (19.0%), followed by paste (16.7%), aqueous extract (15.7%), decoction (14.7%) and juice (11.0%). Fragaria nubicola (0.94) and Viola canescens (0.93) had the highest relative frequency of mention (RFC), while Berberis lycium (1.22) and Fragaria nubicola (1.18) had the highest use value (UV). Geranium wallichianum (85.5), Ligustrum lucidum (83) and Indigofera heterantha (71.5) were the most important species in the study area with the highest relative importance (RI) value. The diseases treated were categorized into 17 classes, with diseases of the digestive system and liver having the highest Informant Consensus Factor (ICF) value, followed by diseases of the oropharynx and musculoskeletal system. Important plants mentioned for the treatment of various diseases of the gastrointestinal tract are Zanthoxylum alatum, Berberis lycium, Mentha longifolia, Punica granatum, Rubus ellipticus and Viola canescens. New applications of rarely documented plants from this area are: Oxalis corniculata paste of the whole plant to treat vitiligo, Carthamus tinctorius flowers to treat chicken pox, Dioscorea deltoidea tuber powder to treat productive cough, Inula cappa root decoction to treat miscarriage, Habenaria digitata tuber juice for the treatment of fever, Viola canescens leaves and flowers for the treatment of sore throat and Achillea millefolium root and leaf juice for the treatment of pneumonia. These plants may contain interesting biochemical compounds and should be subjected to further pharmacological studies to develop new drugs. Traditional medicinal knowledge in the area under study is mainly limited to the elderly, traditional healers and midwives. Therefore, resource conservation strategies and future pharmacological studies are strongly recommended.
1. Introduction
Traditional medicine (TM) is based on the knowledge and beliefs of local communities and is considered the oldest form of medical practice [1,2]. The ingredients used in TM are usually naturally occurring plants, animals and minerals [3]. About 60% of the world’s population and 80% of the population in developing countries rely on traditional medicine [4], mainly because of its ease of access [5,6], its belief and trust [7,8], its perceived safety and efficacy [9] and its inaccessibility to modern medicine. One-third of the world’s population has no regular access to modern primary health care [10], while half of the population in Africa, Asia and Latin America faces a lack of minimal medical care [11], although in many areas a coexistence of conventional and traditional medicine has been observed [12].
Of the approximately 295,000 flowering plants in the world, less than 10% have been studied for their medicinal properties [13]. There is indeed a growing interest in researching medicinal plants for the development of allopathic medicines, and this trend is driven by various factors such as the search for new sources of medicines, the need for more sustainable and natural alternatives and the recognition of traditional systems of medicine [14,15,16]. Herbal products and their derivatives still account for about 25–50% of pharmaceuticals worldwide [17,18,19]. A variety of chemical constituents are extracted from plants, which are valuable resources for the pharmaceutical, cosmetics and food industries. Alkaloids such as morphine, quinine and nicotine, terpenes found in essential oils of plants such as lavender, citrus and cannabis, and flavonoids abundant in fruits such as berries (anthocyanins), citrus fruits and vegetables such as onions (quercetin) serve a variety of purposes [20]. The ethnomedicinal use of plants should be documented in a standardized format [21,22,23,24]. Standardized documentation ensures consistency and facilitates the comparison and analysis of traditional knowledge in different cultures and regions. This approach records detailed information about the plant species, parts used, preparation methods, dosage, therapeutic use and associated cultural practices or beliefs. Such standardized documentation not only preserves valuable traditional knowledge but also makes it more accessible for scientific research, nature conservation and the sustainable use of plant resources. Understanding the properties of raw materials is important to preserve a national heritage [25,26], but the understanding of traditional medicine is still limited, even in Asian countries [27,28].
Since the Alma Ata Declaration (late 1970s), the WHO has reaffirmed its commitment to promote the development of public policies to incorporate traditional practices into the health systems of all Member States [29]. The inhabitants of developing countries are the most frequent users of these practices, and 67% of the world’s plant species are found in these countries [30]. Herbal medicines are a cost-effective source of primary health care, especially where modern health facilities are lacking [31,32]. Efforts have been made to integrate herbal preparations into modern medical systems to improve access to health care [33,34,35,36], and patients often take traditional and allopathic medicines simultaneously [12]. Unfortunately, plant resources are often under significant anthropogenic stress, leading to an alarming decline in plant diversity and associated traditional knowledge. Other factors contributing to the loss of traditional knowledge are modern schooling, land use changes, the market economy, and the process of industrialization and globalization [37].
In the mountainous regions of Azad Kashmir in northern Pakistan, there is a great diversity of plant habitats, soil types and climatic conditions. Many endemic plants of Pakistan are restricted to this region. There are increasing reports of local societies in Azad Jammu and Kashmir (AJK) using traditional medicinal plants [38,39,40], but comprehensive documentation of local useful flora and associated traditional knowledge is still lacking. Local traditional healers and herbalists play an important role as they provide health services to about 75% of the rural population [41,42]. The Poonch Valley, an administrative division of Azad Jammu and Kashmir, is particularly rich in biodiversity but hardly explored for ethnobotanical knowledge [43,44]. Many remote areas like Tehsil Hajira are still unexplored. We hypothesized that ethnomedicinal knowledge varies widely across different regions of Pakistan and that there are some novel uses of plants, especially in remote areas like Tehsil Hajira. This hypothesis is based on the assumption that geographical isolation and different cultural practices may lead to unique ethnomedicinal traditions within specific communities. Therefore, we hypothesize that the ethnomedicinal knowledge documented in the Tehsil Hajira area would show remarkable differences compared to other regions of Pakistan. The aim of the current study was to (a) document the traditional knowledge of medicinal plants used to cure various diseases, (b) compare the documented ethnomedicinal knowledge using quantitative indices, specifically use value, relative frequency of mention, degree of fidelity, and informant approval factor, and (c) identify new medicinal plants and novel uses by comparing the present findings with previously reported uses from neighboring areas.
2. Results and Discussion
2.1. Demographic Data of the Informants
A total of 70 informants (40 men and 30 women) were interviewed as part of the present study (Table 1). Mainly due to the traditional concept of gender segregation, honor and covering (parda) in the study area, the proportion of female respondents was 25% less than that of males. Furthermore, women are not allowed to communicate with strangers. Nevertheless, female respondents in the study area had more knowledge (they named an average of 6.22 species) than male respondents (who named an average of 5.56 species). This reflects their important contribution to household management and maintaining the health of the family. Similar trends have been observed in other parts of the country such as the Chail Valley [45], Balochistan [46] and Toli Peer [47] as well as globally, e.g., in Brazil [48].

Table 1.
Demographic data of the informants.
The informants were categorized into three age groups, namely 20–40 years, 41–60 years and 61–80 years old. The older informants were more knowledgeable (they named an average of 12.10 species with 10.90 uses), followed by the middle-aged participants (8.96 species with 5.40 uses) and the younger ones (4.22 species with 3.56 uses; Table 1), suggesting that the older ones had more knowledge that they had acquired during their lifetime. Nowadays, the social fabric is changing due to socioeconomic changes and advances in science and technology, even though the study area is remote and close to the Line of Control between India and Pakistan, where mobility is restricted due to the tense security situation. Nevertheless, the young generation is no longer very interested in learning about this traditional wealth. This phenomenon was frequently observed, both on the Asian continent and in various cultural contexts worldwide [45,46,49,50].
Most of the informants had a very low level of education, and only seven informants had a higher education. The level of education was inversely related to traditional knowledge, as uneducated natives were generally more familiar with the use of ethnomedicinal plants than educated individuals (Table 1). The reason for this appears to be a lack of preference for learning and applying ethnobotanical knowledge as part of “modern education”. The same findings have been documented by other researchers in other areas of Pakistan [49,50,51] and abroad [52,53].
2.2. Traditional Health Systems
Local health systems make an important contribution to primary health care worldwide, especially in Asian and African countries. Many people in Pakistan and Azad Kashmir rely on traditional remedies to cure various diseases, especially in marginalized communities [54]. The present data (Table 1) show that among different occupational groups, ethnomedicinal knowledge was highest among traditional health practitioners (mean 23.55 species; 12.4 uses) and midwives (14.2 species; 9.83 uses). In the region, traditional health practitioners (THPs) were often old men and had the most information on the medicinal use of plants, minerals and animals to cure chronic diseases, while midwives were experienced older women who were familiar with pregnancy problems and treated them with herbal medicines. These details have also been described elsewhere in the literature [55,56,57,58]. Pastoralists also had significant ethnomedicinal information (9.18 species; 8.62 uses), as nomadic pastoralist communities not only have direct experience with the use of plants but are also important collectors of medicinal plants, especially at higher altitudes, as also reported from Mustang, Nepal [59]. However, as reported earlier, traditional knowledge of herbal medicine is steadily declining due to better availability of modern health facilities and changing lifestyles [54,60,61], a trend also observed in the study area.
2.3. The Diversity of Ethnoflora
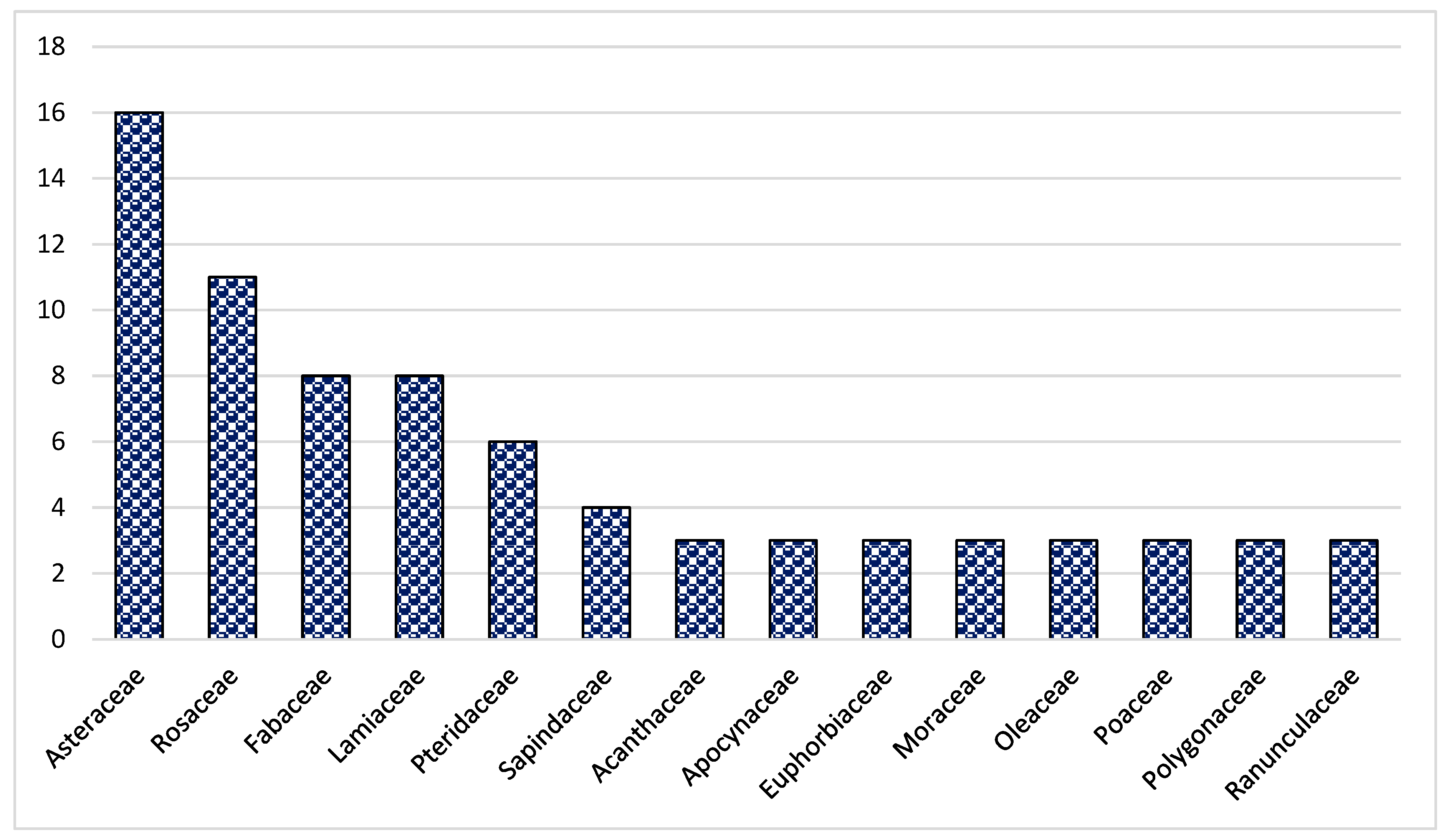
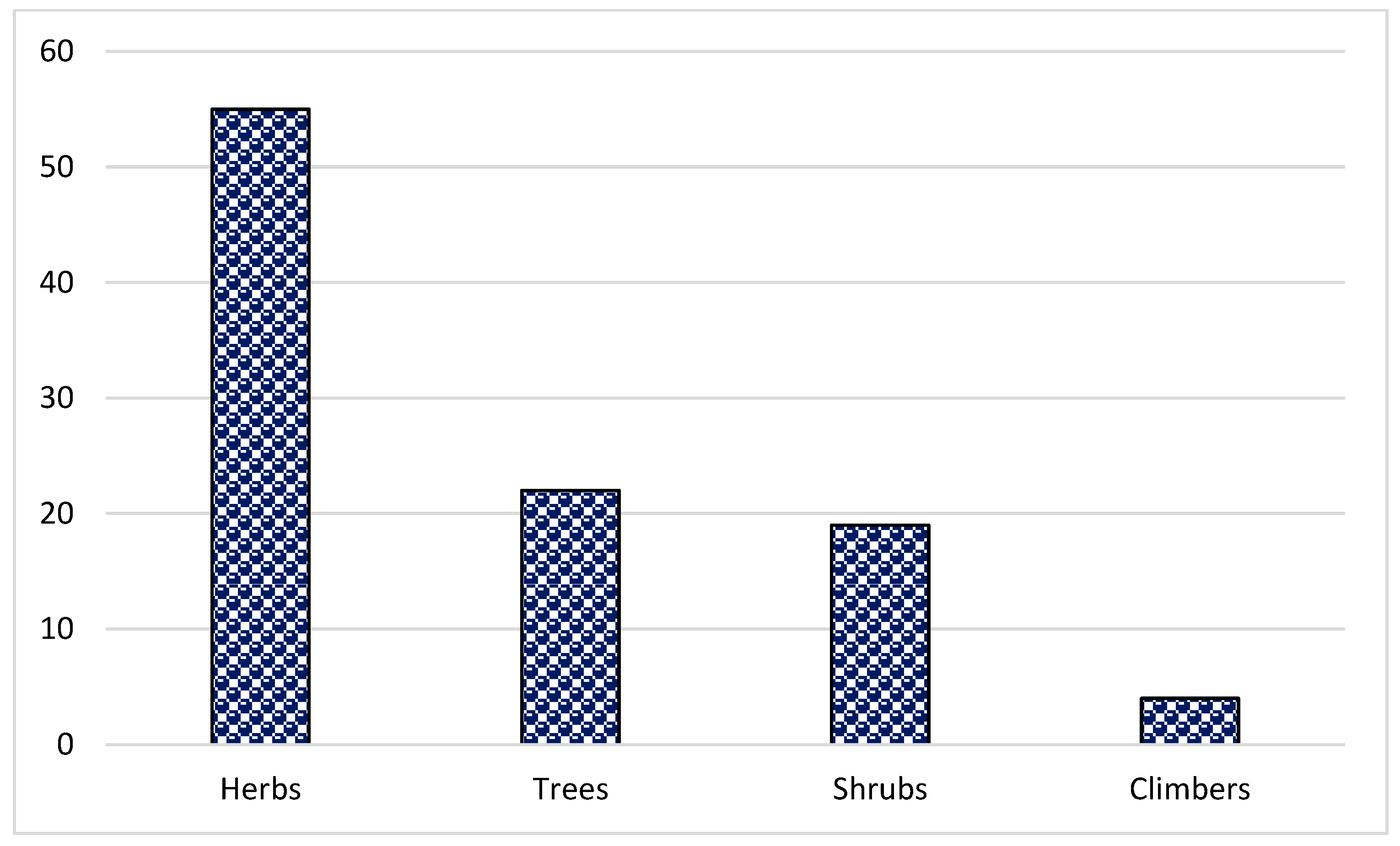
In the present study, 144 species from 70 families and 128 genera were found (Table 2). Asteraceae was the dominant family (16 species), followed by Rosaceae (11 species), Lamiaceae (8 species) and Fabaceae (8 species) (Figure 1). The dominance of these families in the study area could be due to the suitability of the habitat and environment for the members of these families. Similar results were reported in Brazil, Ethiopia and India [47,51,62,63,64]. The frequent use of these families could also be due to easy access, knowledge of long-term use and high content of bioactive constituents. Most of the herbal preparations in the study area were based on herbaceous species followed by shrubs and trees (Figure 2). The probable reason for this is the abundant growth and easy availability of herbaceous species, while the lesser number of trees could be due to climatic and environmental factors such as altitude, etc. These findings are in line with other studies from Pakistan [65,66,67,68,69,70,71]. Indeed, land use practices such as deforestation and the conversion of natural habitats to intensive agriculture can contribute significantly to genetic erosion, especially in regions such as Pakistan. These factors can lead to a loss of biodiversity, both in herbaceous and tree species, affecting the availability and abundance of medicinal plants. In addition, changing land use patterns can disrupt ecosystems and affect the distribution and survival of plant species. Therefore, although altitude and other environmental factors play a role, it is important to consider the broader effects of land use change on genetic erosion and the diversity of medicinal plants in the region.

Table 2.
Medicinal uses of the reported taxa in Tehsil Hajira (Pakistan) and their comparison with previous reports.
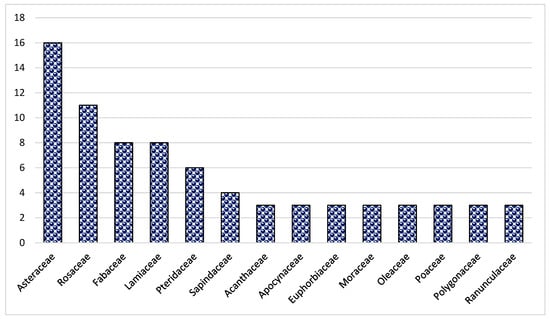
Figure 1.
The most abundant medicinal plant families in Tehsil Hajira.
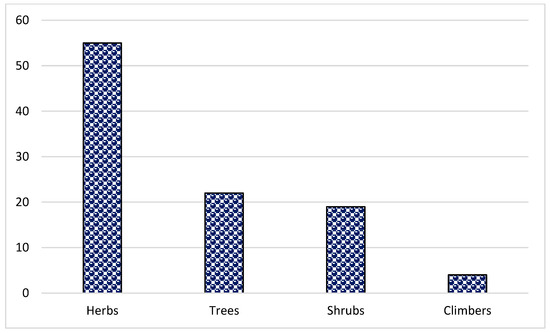
Figure 2.
Distribution pattern of life forms of the reported plant species in the study area of Tehsil Hajira (Pakistan).
2.4. Mode of Administration and Plant Part(s) Used in Herbal Preparations
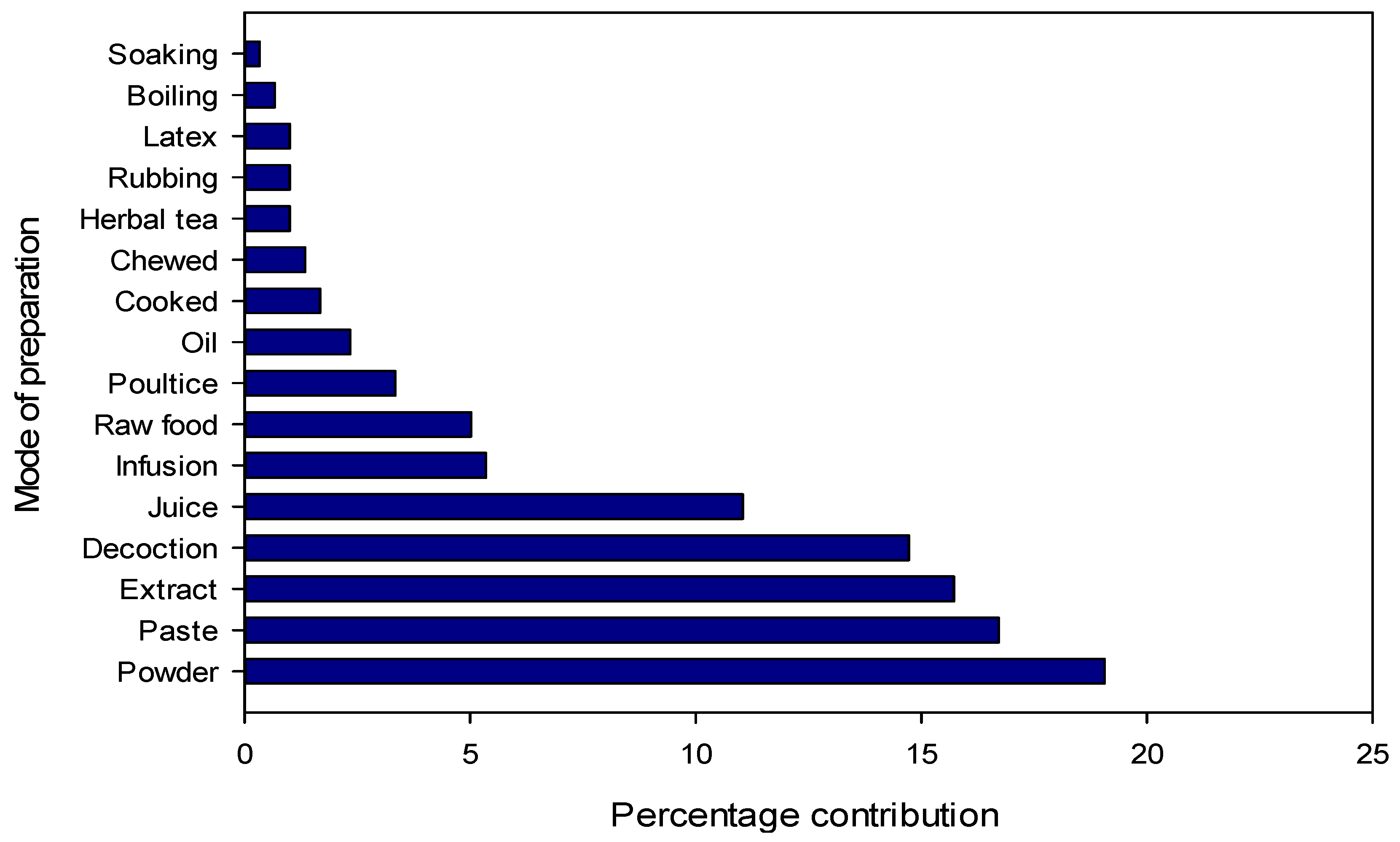
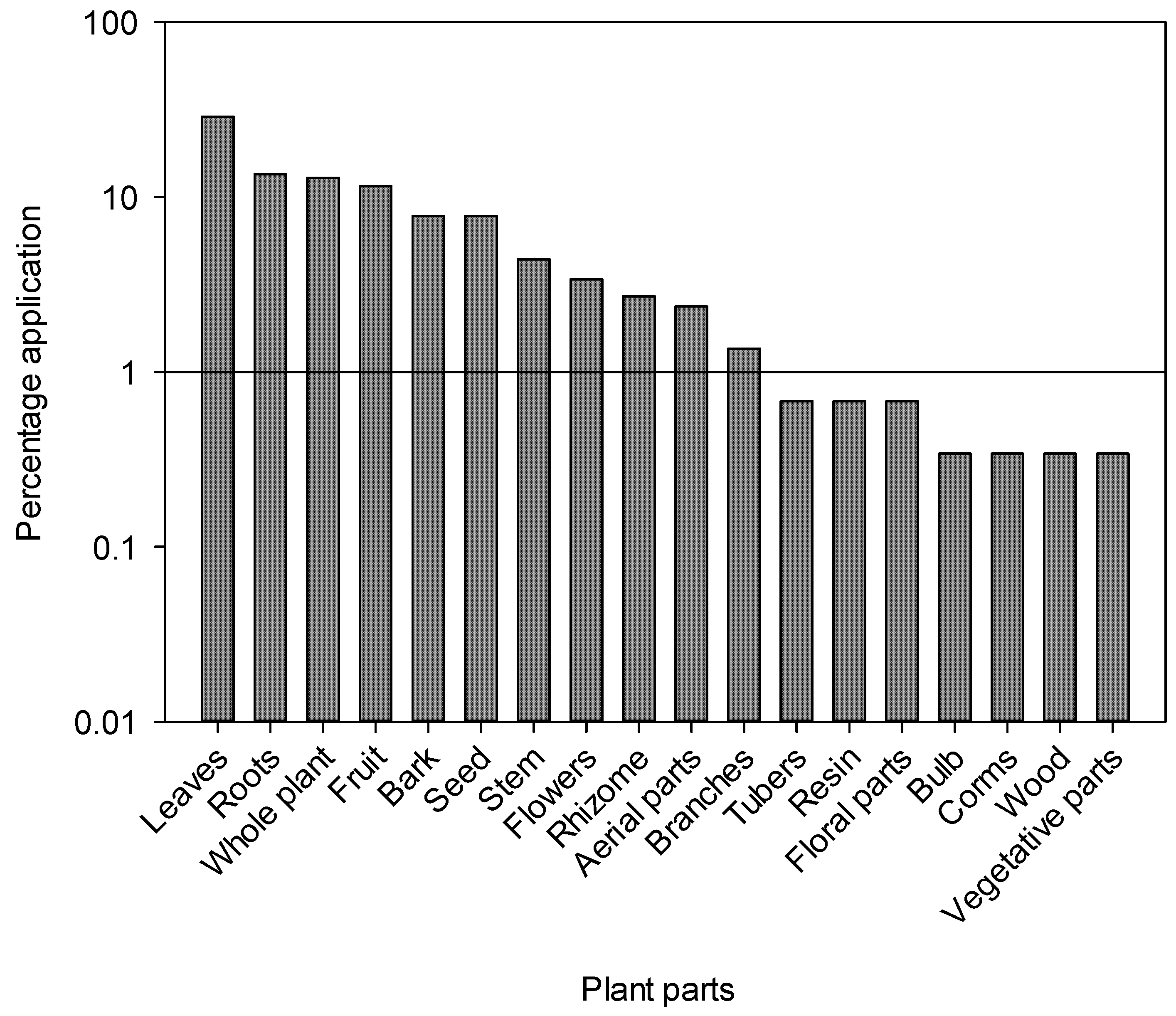
The most common type of preparation was powder (19.0%), followed by paste (16.7%) in which the plant material is usually mixed with water, aqueous extract (15.7%), decoction (14.7%) and juice (11.0%) (Figure 3). The frequent use of powder could be due to its ease of preparation and efficacy in herbal medicines as reported from Pakistan and other countries [46,49,79,86,87]. However, it should be noted that powder is not always the easiest method of using herbal remedies. In the area of internal use, for example, infusions can offer a simpler approach. Other well-known preparation methods include decoctions, infusions, herbal teas and decoctions. “Herbal tea” refers to a beverage made by briefly steeping dried herbs, flowers, fruits or other botanicals in hot water, extracting flavors and some medicinal compounds, while “infusion” encompasses a broader range of beverages made by steeping botanicals in hot water, including herbal teas as well as leaves, fruits or spices. Decoction, on the other hand, “involves the boiling of harder plant parts such as roots or seeds in water for a prolonged period of time, often at low heat, to release medicinal compounds,” while “cooking” is a general cooking technique in which water is heated to boiling point for various culinary purposes, including the preparation of infusions or herbal teas, but without the particular emphasis on prolonged boiling required for decoctions. The most commonly used plant parts were leaves (28.8%), followed by roots (13.5%), whole plants (12.8%) and fruits (11.5%) (Figure 4). A large number of bioactive constituents stored in the various parts of the plant could be beneficial for local residents in the treatment of various ailments [82,88,89]. Certain classes of bioactive compounds such as alkaloids, flavonoids and terpenes are often favored in traditional medicine for their therapeutic properties. However, further analysis would be required to identify specific trends in the use of these ingredients. The leaves are particularly abundant and more easily accessible than other parts of the plant such as seeds and roots. Another reason for collecting leaves is their higher sustainability compared to other parts [47]. Leaves have been reported to be used by many different communities worldwide for the preparation of various herbal products [47,49,90,91,92,93,94]. For example, crushed or ground leaves of plants such as Aloe vera, eucalyptus and neem are used to make poultices to treat skin diseases, wounds and insect bites. In addition, the leaves of culinary herbs such as basil, coriander, parsley and bay leaf are often used as flavorings in the kitchen to enhance the taste and aroma of food. The fact that roots are the second most used plant part in herbal medicine after leaves can be attributed to their rich concentration of bioactive compounds. Roots serve as a reservoir for various phytochemicals, including alkaloids, flavonoids, terpenoids and phenolic compounds, which exhibit various pharmacological activities such as anti-inflammatory, antioxidant, antimicrobial and anticancer properties. In addition, specialized structures within the roots, such as rhizomes or tubers, store energy reserves and protective substances, which further increases their medicinal potential. The physiological functions of roots, including water and nutrient uptake, can also influence their biochemical composition, making them valuable resources for traditional healers and herbalists seeking effective herbal remedies.
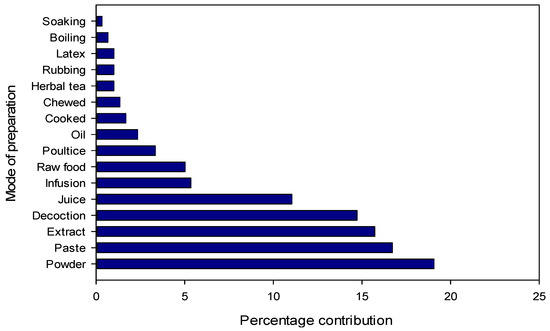
Figure 3.
Method of preparation of medicinal plants in Tehsil Hajira (Pakistan).
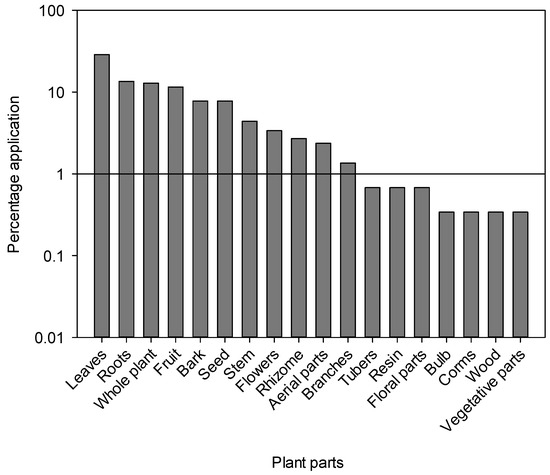
Figure 4.
Percentage of use of various plant parts of medicinal plants from the Tehsil Hajira area (Pakistan).
2.5. Relative Frequency of Citation (RFC)
The RFC defines the most frequently occurring plant species in various diseases used by the locals. In our study, the RFC ranged from 0.02 to 0.94. Fragaria nubicola (0.94), Viola canescens (0.92) and Mentha longifolia (0.87) had the highest RFC values, while Cyperus rotundus and Bidens bipinnata (0.02) had the lowest values (Appendix A Table A1). A high RFC value indicates that the availability and knowledge of a particular plant species is very high. Such species may be of interest for marketing, pharmacological and phytochemical studies to assess and prove their validity [60,95]. These species should be protected as a priority, as their overexploitation can endanger the local populations. Many species with maximum RFC are collected by healers and cultivated in gardens not only for ethnomedicinal purposes but also for ornamental and conservation purposes. The present results are consistent with other studies [47,50].
2.6. Utilization Value (UV)
The use value is the quantity of uses recognized for a particular plant species. It indicates the extent to which a species is used in a particular area. Species with a high UV are well known to informants and are extensively used in ethnomedicinal preparations [49,89], probably because they contain more biologically active compounds [96]. Indeed, certain classes of compounds are often associated with high UV, such as alkaloids, flavonoids and phenolic compounds. These bioactive compounds are known for their medicinal properties and are often used in ethnomedicinal practice for their potential therapeutic effects. In the current study, Berberis lycium (1.22), Fragaria nubicola (1.18) and Viola canescens (1.07) had the highest use values (Appendix A Table A1). However, plants with low RFC and UV values are not insignificant, but young people are less aware of their use, and knowledge may eventually disappear, as in other areas [97]. We compared the documented plant uses with previously published studies from other areas (Appendix A Table A1) [42,60,84,98]. Similar to Bano et al. [60], Hippophae rhamnoides and Rosa brunonii had the highest values, ranging from 1.64 to 1.47. The correlation analysis showed a strong positive correlation between UV and RFC at a significant level of 0.01 (Figure 5). This can be attributed to the fact that the plants that are well known in the local communities are extensively used in herbal preparations. Thus, if a plant is well known in the communities, it has a higher use value and is important for pharmacological evaluation.
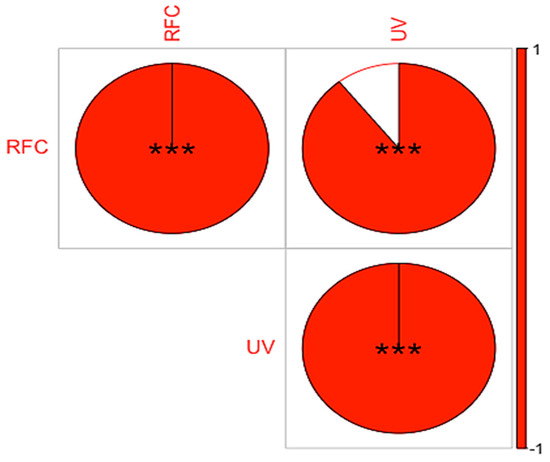
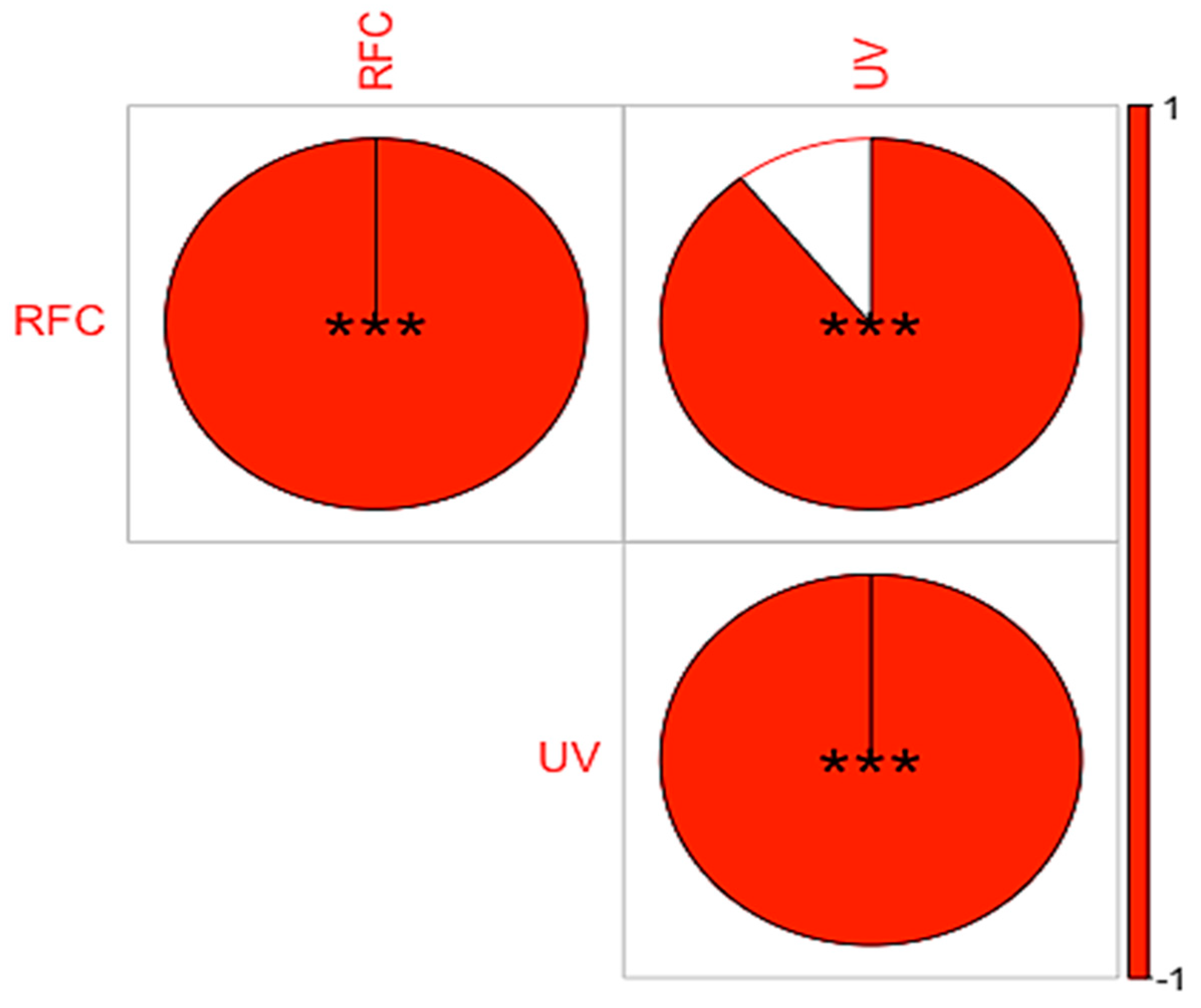
Figure 5.
Correlation between RFC and UV of ethnomedicinal plant use in Tehsil Hajira (UV = Use value; RFC = Relative frequency of citation).*** indicate strong positive correlation between UV and RFC at a significant level of 0.01.
2.7. Relative Importance (RI)
The species with high values for relative importance are often versatile. The highest RI values were found for Geranium wallichianum (85.5), Ligustrum lucidum (83) and Indigofera heterantha (71.5) (Table 3). Plants with a high RI showed a higher number of uses in the treatment of various body systems, and local people passed on a wealth of information about these plant species. The importance of plant species is increasing due to their ability to cure diseases [99]. This suggests that these plants are highly valued in traditional medicine, possibly due to their purported efficacy in treating ailments in various body systems. As a result, the importance of these plant species is increasing, especially among the general population, where their potential to cure diseases is increasingly recognized.
2.8. Informant Consensus Factor (ICF)
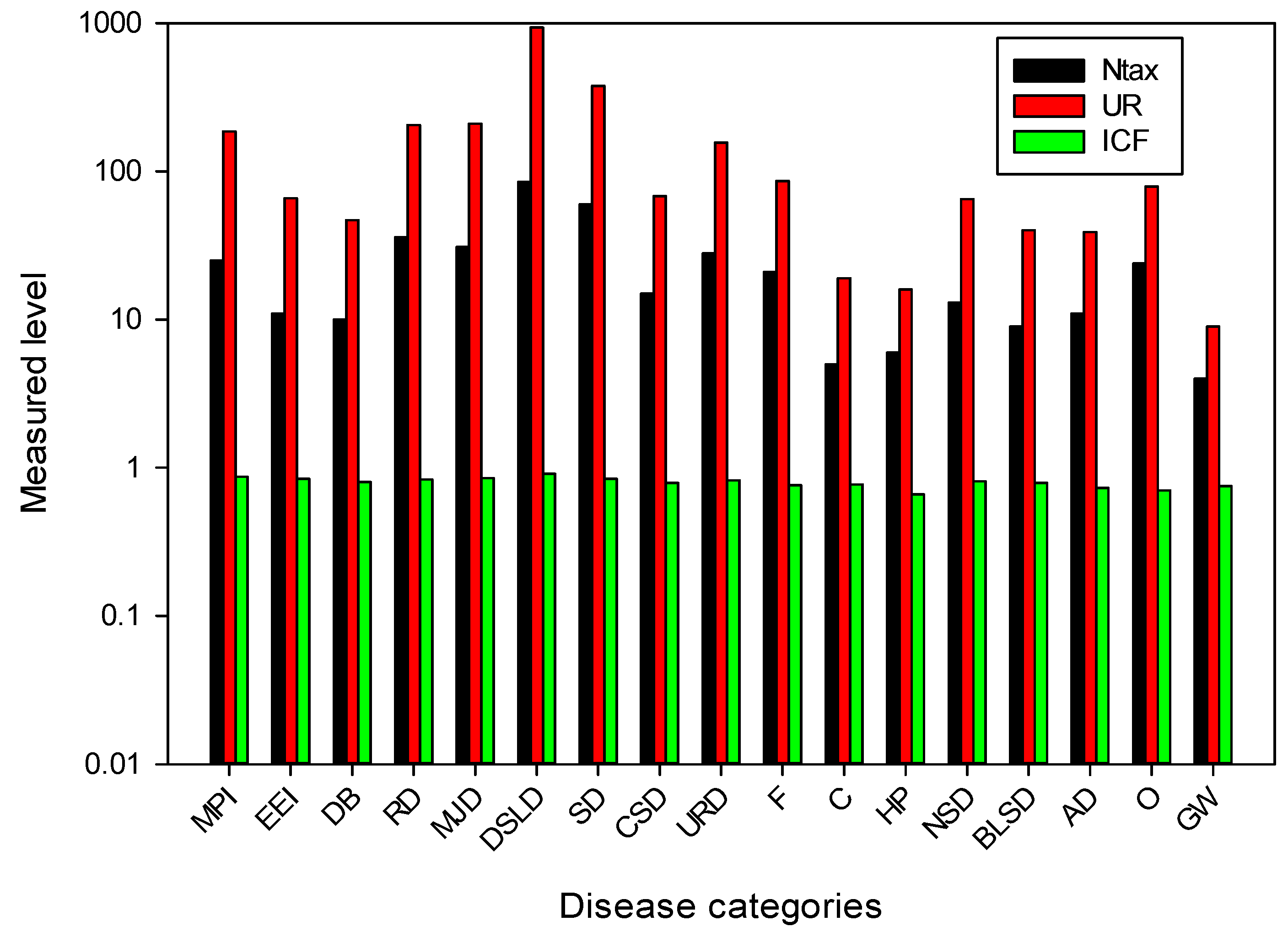
The ICF values ranged from 0.66 to 0.91 (Figure 6). All diseases were categorized into 17 different types. The highest ICF score was found for digestive disorders (0.91). Due to the insufficient availability of clean drinking water and hygienic food, digestive disorders are widespread in this area [100,101]. Important plants in this category were Zanthoxylum alatum, Berberis lycium, Mentha longifolia, Punica granatum, Rubus ellipticus and Viola canescens (Figure 6). Important plants for curing various gastrointestinal ailments have been documented for different ethnic communities around the world [102,103]. These plants contain active ingredients that are recognized by the local population and are used to treat various gastrointestinal disorders. Other studies have also found a high consensus factor value for gastrointestinal complaints [46,104,105,106,107,108]. The local population was very familiar with these species, which were used to treat a variety of ailments. The lowest ICF value (0.66) was found for hair care.
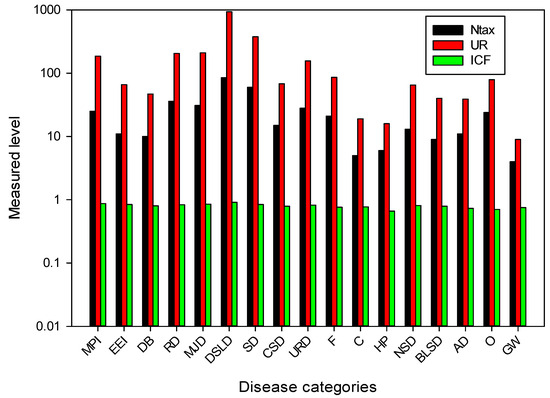
Figure 6.
Number of taxa and usage reports of plant species used in the treatment of various diseases in Tehsil Hajira (Pakistan). (Ntax, total number of species used by all informants for a disease group; UR, total number of utilization reports in each disease group; ICF, consensus factor of informants; MPI, mouth and throat infection; EEI, eye and ear infection; DB, diabetes; RD, respiratory diseases; MJD, muscle and joint diseases; DSLD, diseases of the digestive system and liver; SD, skin diseases; CSD, diseases of the circulatory system; URD, diseases of the urinary tract and reproductive organs; F, fever; C, cancer; HP, hair problems; NSD, diseases of the nervous system; BLSD, diseases of the blood and lymphatic system; AD, antidote; O, other; GW, general weakness).
2.9. Fidelity Level (FL)
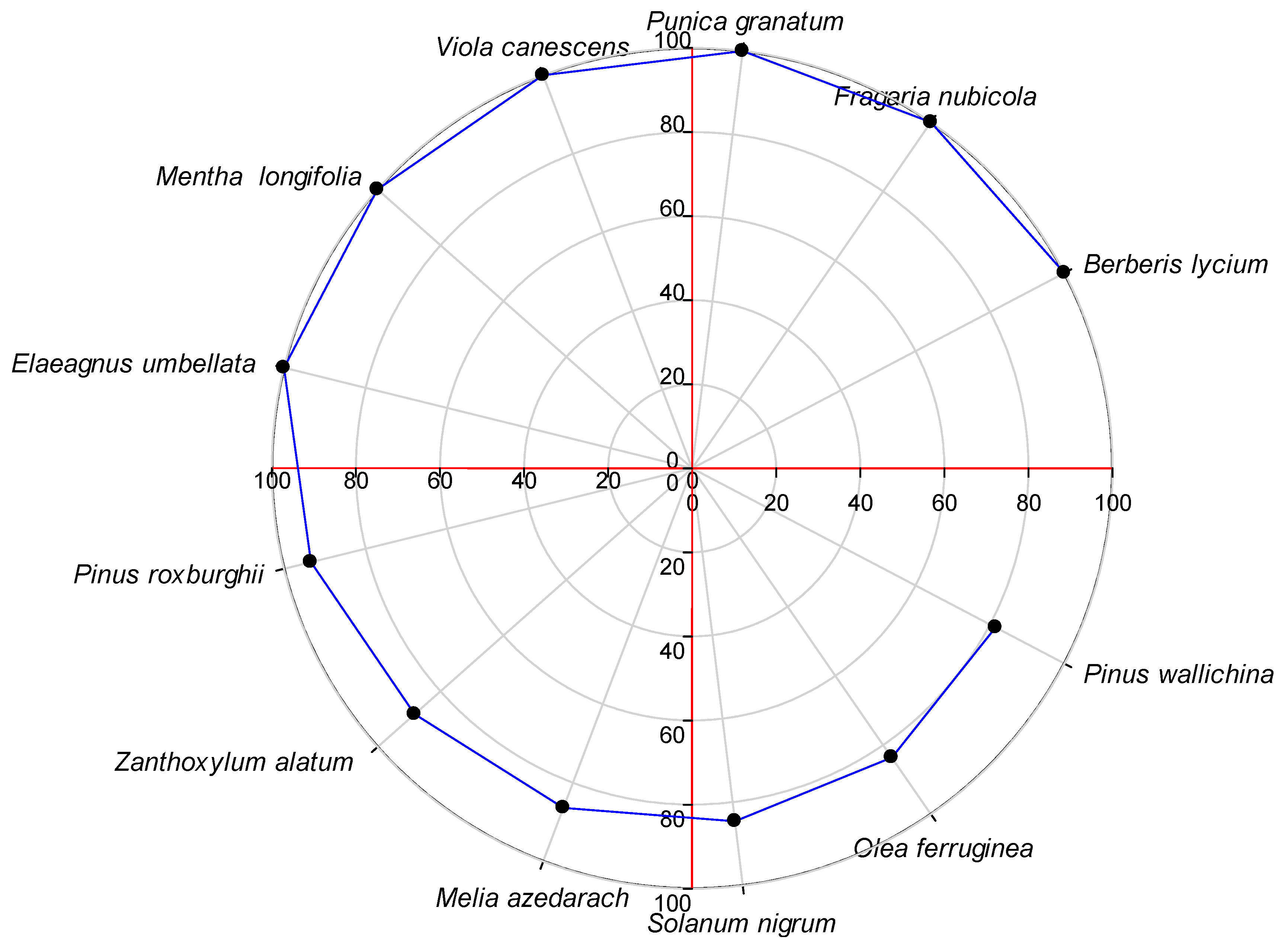
The Fidelity Level (FL) of the 69 most important plant species ranged from 12.5% to 100%. A high FL value generally indicates the dominance of a particular ailment in a region and the use of the same species to treat it [46,109]. The species with an FL value of 100 were Berberis lycium, Fragaria nubicola, Punica granatum, Viola canescens, Mentha longifolia and Elaeagnus umbellata, which were used for wound healing, mouth infections, jaundice, fever, stomach ailments and toothache (Figure 7). Plant species with a high FL are considered ideal for ethnopharmacological studies [110]. However, plants with a low FL should not be underestimated [111].
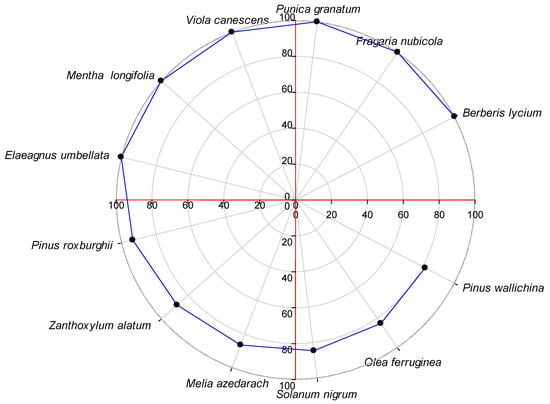
Figure 7.
Top ethnomedicinal plant species with a fidelity level of over 80 in Tehsil Hajira.
2.10. Novelty and Future Implications
The present study was compared with 22 different ethnobotanical studies from other parts of Azad Kashmir and the rest of Pakistan using the Jaccard index. The value of the Jaccard index ranged from 1.02 to 22.27. The highest degree of similarity was found for nearby areas like Pearl Valley [44] and Toli Peer [47] (Table 3).
This higher degree of similarity could be due to similar climatic conditions, vegetation types and frequent intercultural exchanges between these ethnic communities. The lowest similarity with other studies could be the result of extensive changes in population and habitat structure, showing a high degree of cultural adaptation [112]. Any change in these parameters would lead to a change in the similarity index values, as these indices are very sensitive to changes in population size [72].


Table 3.
Jaccard index comparing the present study in Tehsil Hajira with previous published studies.
Table 3.
Jaccard index comparing the present study in Tehsil Hajira with previous published studies.
| Study Area | SY | NRPs | NPSU | NPDU | TSCBA | SEAA | SESA | PPSU | PPDU | JI | C |
|---|---|---|---|---|---|---|---|---|---|---|---|
| From Azad Jammu and Kashmir (AJK), Pakistan | |||||||||||
| Poonch Valley | 2012 | 68 | 4 | 23 | 27 | 41 | 117 | 5.88 | 33.8 | 14.59 | [72] |
| Leepa Valley | 2012 | 36 | 2 | 11 | 13 | 23 | 131 | 5.55 | 30.55 | 7.78 | [74] |
| Pearl Valley | 2017 | 136 | 37 | 14 | 51 | 85 | 93 | 27.2 | 10.29 | 22.27 | [44] |
| Toli Peer | 2017 | 121 | 30 | 15 | 45 | 76 | 99 | 24.7 | 12.3 | 20.45 | [47] |
| Kotli | 2017 | 128 | 20 | 25 | 45 | 83 | 99 | 15.6 | 19.5 | 19.82 | [23] |
| Neelum Valley | 2017 | 50 | 2 | 18 | 20 | 30 | 124 | 4.00 | 36.00 | 11.49 | [21] |
| Kotli | 2019 | 80 | 12 | 28 | 40 | 40 | 104 | 15 | 35 | 21.74 | [82] |
| From Khyber Pakhtunkhwa (KPK), Pakistan | |||||||||||
| Dir Valley, KPK, | 2011 | 65 | 3 | 23 | 26 | 39 | 118 | 4.61 | 35.3 | 14.21 | [113] |
| Chail Valley, Swat | 2014 | 50 | 15 | 8 | 23 | 27 | 121 | 30 | 16 | 13.47 | [45] |
| Kabal, Swat | 2015 | 45 | 2 | 17 | 19 | 26 | 125 | 4.44 | 37.7 | 11.17 | [114] |
| Alpine and Sub-alpine regions of Pakistan | 2015 | 125 | 7 | 7 | 14 | 111 | 130 | 5.6 | 5.6 | 5.49 | [49] |
| Manoor Valley, KPK | 2016 | 44 | 1 | 13 | 14 | 30 | 130 | 2.27 | 29.54 | 8.05 | [80] |
| Northern Pakistani Afghan borders | 2018 | 92 | 1 | 26 | 27 | 65 | 117 | 1.09 | 18.06 | 12.91 | [85] |
| Mohmand Agency, FATA | 2018 | 64 | 1 | 12 | 13 | 51 | 131 | 1.56 | 8.33 | 6.67 | [31] |
| From other areas of Pakistan | |||||||||||
| Mastung District, Baluchistan | 2014 | 102 | 1 | 11 | 12 | 90 | 132 | 0.98 | 10.7 | 5.13 | [46] |
| Turmic Valley, Gilgit-Baltistan | 2015 | 42 | 1 | 2 | 3 | 39 | 141 | 2.38 | 4.76 | 1.63 | [115] |
| Hafizabad, Punjab, | 2017 | 85 | 6 | 10 | 16 | 69 | 128 | 7.05 | 11.7 | 7.51 | [79] |
| Wazirabad, Punjab, | 2018 | 31 | 1 | 7 | 8 | 23 | 136 | 3.22 | 22.5 | 4.79 | [81] |
| Chenab riverine area, Punjab Pakistan | 2019 | 129 | 9 | 11 | 20 | 109 | 124 | 6.97 | 8.52 | 7.91 | [83] |
| From other parts of the world | |||||||||||
| Blue Nile State, Sudan | 2011 | 53 | 0 | 2 | 2 | 51 | 142 | 0 | 3.77 | 1.02 | [77] |
| Alasehir (Manisa), Turkey | 2013 | 137 | 0 | 9 | 9 | 128 | 135 | 0 | 6.56 | 3.30 | [76] |
| Jhalawar, Rajasthan, India | 2015 | 19 | 0 | 2 | 2 | 17 | 42 | 0 | 10.5 | 1.24 | [78] |
Legend: SY: Study year, NRPs: Number of reported plant species, NPSU: Number of plants with similar uses, NPDU: Number of plants with different uses, TSCBA: Total species common in both areas, SEAA: Species found in aligned areas, SESA: Species found only in study area, PPSU: Percentage of plant with similar uses, PPDU: Percentage of plant with different uses, JI: Jaccard index, C: citation.
The comparative analysis has brought to light some new uses of plant species rarely documented in this region, such as the use of a paste made from the whole plant of Oxalis corniculata to treat vitiligo, the flowers of Carthamus tinctorius to treat chicken pox, the tuber powder of Dioscorea deltoidea to treat productive cough, the root decoction of Inula cappa for the treatment of miscarriages, the tuber juice of Habenaria digitata for the treatment of fever, the leaves and flowers of Viola canescens for the treatment of sore throat and the root and leaf juice of Achillea millefolium for the treatment of pneumonia. These plants may contain interesting bio-chemical compounds and should be subjected to further pharmacological studies to develop new drugs. However, it is important not to forget efficacy and toxicity studies, among others, to ensure the safety and effectiveness of potential pharmaceuticals derived from these plants.
3. Materials and Methods
3.1. Study Area
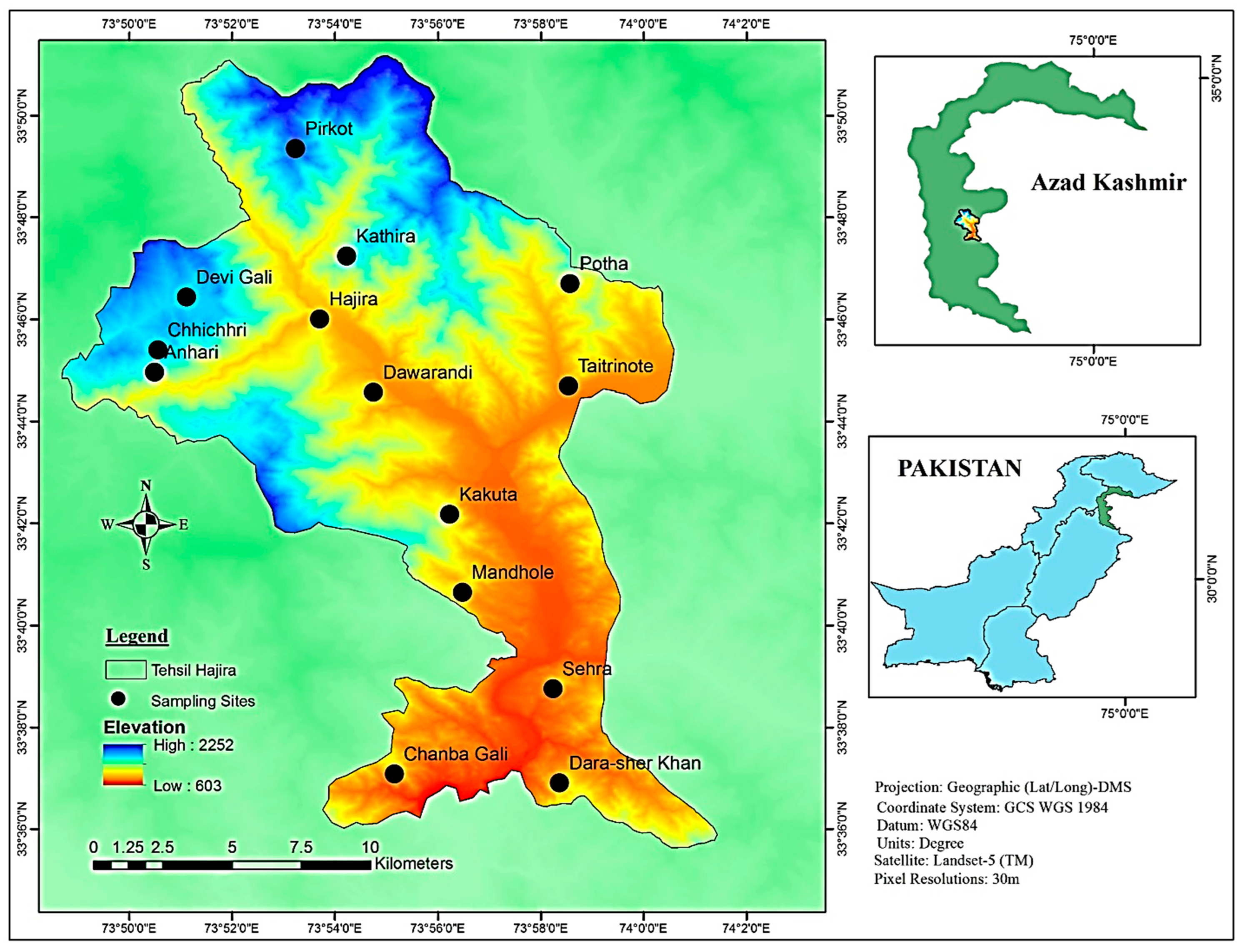
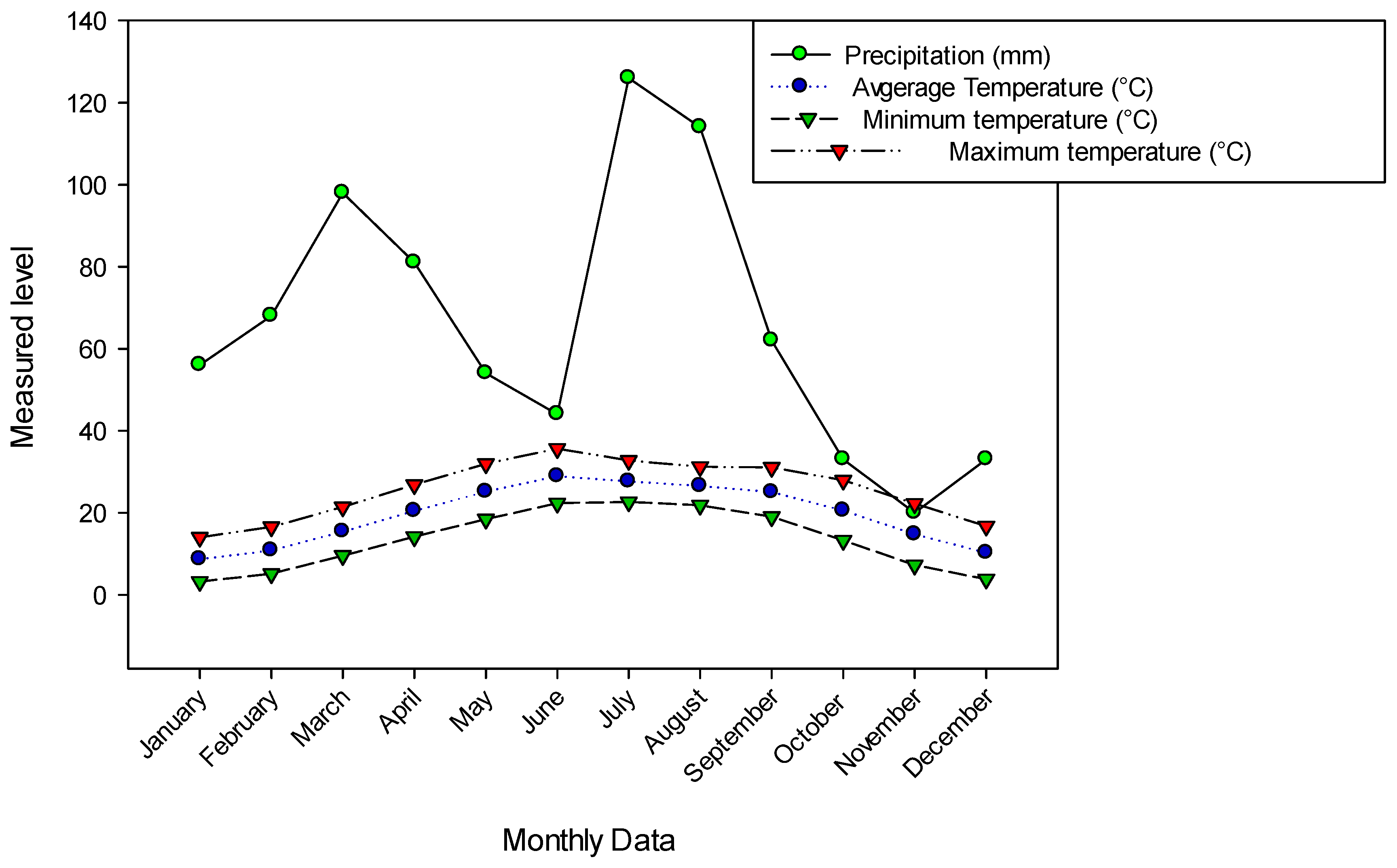
Tehsil Hajira is a sub-district of Poonch District in Azad Kashmir in Pakistan and lies at an altitude between 650 and 1950 meters. It is located between longitude 73°53′45.96″ E and latitude 33°37′18.12″ N (Figure 8). The study area includes steep slopes, high mountains and dissected small terraces. The region is located 130 km from Muzaffarabad (the capital of Azad Kashmir) and 160 km from Islamabad (the capital of Pakistan). The total area of Hajira, Azad Jammu and Kashmir is 970 km2, and the population is 140,000 according to the 2017 census. The sampling sites were selected based on altitude, vegetation heterogeneity and physiognomy. The climate in the region varies from subtropical to temperate, with an average monthly rainfall of 66 mm. The highest amount of precipitation falls in August (114 mm). Temperatures vary between 3.2 °C and 35.6 °C, with June and July being the warmest months with average temperatures of 28.9 °C and 27.6 °C, respectively, while the coldest months are January and December with average temperatures of 8.6 °C and 10.2 °C, respectively (Figure 9). The vegetation is mainly dominated by Pinus roxburghaii (Chir), Pinus wallichiana (Biar) and Quercus incana (Iriana). The ground flora is dominated by various angiosperms as well as mosses and ferns.
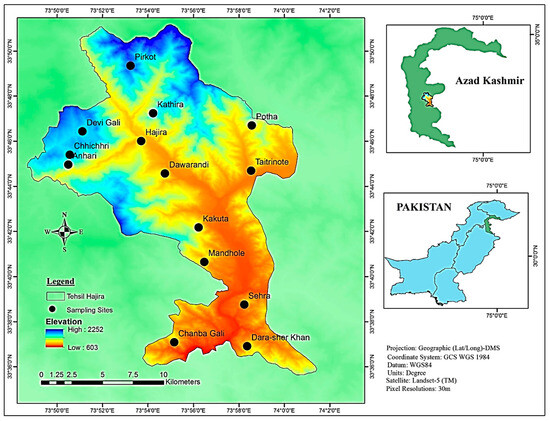
Figure 8.
Map of the study area of Tehsil Hajira (Poonch District of Azad Kashmir, Pakistan).
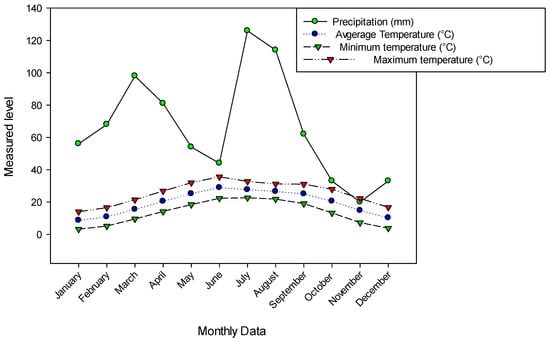
Figure 9.
Precipitation and temperature of the study area of Tehsil Hajira.
Tehsil Hajira has a diverse and complex ethnic composition, including Suddhans, Pathans, Awans, Malik Khwajas, Janjua Rajputs, Dullies, Jaats, Gujars, Ghakhars, Mughals and Qureshis. Most of the people have migrated from Jammu and Kashmir. Among them, the Suddhans and Rajputs are the most influential tribes. The entire population is Muslim. The majority of the people speak Pahari, Hindko and Gujari, and many are also familiar with Urdu. The area has a rural culture with old traditions and its own principles of village life, home, family, festivals and ceremonies. Most of the inhabitants live in poor socio-economic conditions with limited sources of income. Most are farmers, some are employees and laborers, and only a few have their own small businesses. Few public dispensaries and only one small tehsil main hospital (Khai Gata-Hajira Rd., Hajira) provide primary health care, but people living in higher altitudes and remote places have very limited access to these facilities and therefore mainly use herbal remedies for primary health care.
3.2. Ethnobotanical Data Collection
The field studies were conducted from March 2017 to September 2017. Data collection involved several visits to each site to ensure a comprehensive understanding and clarification of the information gathered. The ethnobotanical information on the use of plants was collected from a total of 70 informants (40 men and 30 women) through semi-structured interviews and focus group discussions (Table 1). Participants were selected randomly [35] or, in some cases, by snowballing [32]. First, key people with knowledge of the community were identified, and then, as part of a snowballing process, further informants were recommended by these people, thereby expanding the network. Ethical clearance to conduct the study was obtained from the ethics committee of Azad Jammu & Kashmir Women’s College, Bagh, prior to the commencement of the surveys. In addition, legal approval was obtained from the members of the local union council. The code of ethics of the International Society of Ethnobiology (http://www.ethnobiology.net/) was followed. Informed consent was obtained verbally from the informants before the interview commenced. Detailed information about the medicinal use of the plant, the method of preparation and the parts used were recorded.
3.3. Floristic Inventory and Botanical Identification
During the field survey, the specimens of each plant species were collected, dried, preserved and mounted on standard-sized herbarium sheets. Identification of the plant specimens was conducted with the help of a taxonomist using the Flora of Pakistan (https://www.eflora.com) [116,117]. The correct family name was determined using APG-IV (2016) [118]. The correct and legitimate names were determined using the Plant List 2013 [119]. Further verification of the identified species was carried out in the Herbarium of Medicinal and Aromatic Plants of Pakistan Agriculture Research Council (PARC). The fully identified voucher specimens were submitted to the herbarium of the Botany Department of AJK Women’s University, Bagh, for further utilization.
3.4. Data Analysis
The collected primary ethnobotanical data were converted into quantitative data using the following quantitative indices:
3.4.1. Relative Frequency of Citation (RFC)
The relative frequency of citation of the reported species was calculated according to Vijayakumar et al. [120]:
- FC = number of respondents who reported the use of a particular species;
- N = total number of respondents.
3.4.2. Use Value (UV)
The use value was determined according to Vijayakumar et al. [120] by applying the following formula:
where Ui is the number of uses mentioned by each informant for a particular species, and N is the total number of informants.
3.4.3. Informant Consensus Factor (ICF)
The informant consensus factor was derived to determine the consensus among informants on the reported remedies for each disease category. It was calculated based on Heinrich et al. [121]:
where Nur is the use reports for each disease group and Nt is the number of species cited by all respondents.
3.4.4. Relative Importance (RI)
The relative importance was determined according to Khan [43] with the following formula:
- PH = pharmacological property of the selected plant;
Rel PH = the relative number of pharmacological properties reported for a selected plant.
- BS = total body systems cured by a given plant species;
Rel BS = relative number of body systems cured by a particular plant species.
3.4.5. Jaccard Index (JI)
This index was used here to identify novel uses by comparing the medicinal uses reported in the current study with previously published work from neighboring regions. It was calculated following Gonza et al. [122] as follows:
- a = species of our study area;
- b = species of the neighboring area;
- c = species occurring in both areas.
3.4.6. Fidelity Level (FL)
Fidelity level reflects the preference of certain species by the local population for the treatment of a certain disease in the studied region. The valuesfor FL were calculated according to Alexiades and Sheldon [123]:
- Np = informants who requested the use of a specific plant species for a specific condition;
- N = respondents who named the plant species for any ailment.
The maximum FL of reported plant species shows high preference of plant species for curing a specific disease by the local inhabitants in the investigated region.
3.4.7. Pearson Correlation Analysis
Correlation analysis between Relative Frequency of Citation and use value was made using the Cor function in R v. 4.3.1 Software.
4. Conclusions
Medicinal plants are the basis of traditional health practices in Tehsil Hajira in Poonch District, where, despite the availability of modern health facilities, reliance on herbal remedies remains high, especially among the elderly and alternative practitioners. However, this knowledge is in danger of dwindling due to the dwindling interest of the younger generation. The selection of plant species is of immense importance, not only for local communities but also for research and the pharmaceutical and food industries, as it offers the potential for new therapeutic discoveries. However, this biodiversity is threatened by overexploitation, grazing and deforestation, so urgent conservation measures are needed. Concerted efforts are therefore needed to preserve ethnomedicinal knowledge, sustainably manage medicinal plant resources and unlock their full therapeutic potential through future pharmacological studies.
Author Contributions
Conceptualization, M.S.A. and T.J.; methodology, M.S.A. and T.J.; software, M.S.A., R.W.B. and T.J.; validation, M.S.A. and R.W.B.; formal analysis, K.A.; investigation, T.J.; resources, M.S.A., T.J. and I.V.-K.; data curation, T.J.; writing—original draft preparation, T.J.; writing—review and editing, I.V.-K., H.Q. and R.W.B.; visualization, M.S.A. and I.V.-K.; supervision, M.S.A. and I.V.-K. All authors have read and agreed to the published version of the manuscript.
Funding
The authors are grateful to the University of Zagreb Faculty of Agriculture for financial support for the publication of this manuscript through the Open Access Publication Fund of the University of Zagreb Faculty of Agriculture. The current research is purely conducted on a self-finance basis.
Institutional Review Board Statement
The present research is purely based on field surveys. Ethical approval to conduct the study was given by the Ethics Committee of the Women University of Azad Jammu & Kashmir, Bagh, before initiating the surveys. In addition to this, legal permission was obtained from members of the local union council. Ethical guideline of the International Society of Ethnobiology (http://www.ethnobiology.net/, accessed on 19 February 2017). The prior informed consent from participants was obtained verbally before starting any interview.
Data Availability Statement
The original contributions presented in the study are included in the article; further inquiries can be directed to the corresponding authors.
Acknowledgments
The authors are thankful to the local inhabitants of the area for sharing their knowledge.
Conflicts of Interest
The authors declare no conflicts of interest.
Appendix A

Table A1.
Quantitative analysis of ethnobotanical data.
Table A1.
Quantitative analysis of ethnobotanical data.
| Plant Species | FC | RFC | UI | UV | Rel PH | Rel BS | RI |
|---|---|---|---|---|---|---|---|
| Vachellia nilotica | 52 | 0.74 | 62 | 0.88 | 0.18 | 0.28 | 23 |
| Acer platanoides | 22 | 0.31 | 32 | 0.45 | 0.54 | 0.57 | 55.5 |
| Achillea millefolium | 41 | 0.59 | 61 | 0.87 | 0.18 | 0.28 | 23 |
| Achyranthes aspera | 23 | 0.33 | 31 | 0.44 | 0.27 | 0.42 | 34.5 |
| Acorus calamus | 10 | 0.14 | 17 | 0.24 | 0.27 | 0.28 | 27.5 |
| Adhatoda zeylanica | 23 | 0.33 | 36 | 0.51 | 0.36 | 0.28 | 32 |
| Adiantum capillus-veneris | 32 | 0.46 | 41 | 0.58 | 0.45 | 0.42 | 43.5 |
| Adiantum incisum | 34 | 0.49 | 40 | 0.57 | 0.45 | 0.57 | 51 |
| Aesculus indica | 28 | 0.40 | 56 | 0.8 | 0.27 | 0.42 | 34.5 |
| Ailanthus altissima | 35 | 0.50 | 45 | 0.64 | 0.18 | 0.14 | 16 |
| Ajuga bracteosa | 43 | 0.61 | 58 | 0.82 | 0.36 | 0.57 | 46.5 |
| Allium sativum | 59 | 0.84 | 64 | 0.91 | 0.27 | 0.28 | 27.5 |
| Amaranthus viridis | 46 | 0.66 | 51 | 0.72 | 0.27 | 0.42 | 34.5 |
| Anaphalis margaritacea | 13 | 0.19 | 23 | 0.32 | 0.54 | 0.57 | 55.5 |
| Arisaema utile | 34 | 0.49 | 44 | 0.62 | 0.27 | 0.42 | 34.5 |
| Artemisia dubia | 41 | 0.59 | 48 | 0.68 | 0.27 | 0.28 | 27.5 |
| Artemisia tridentata | 14 | 0.20 | 29 | 0.41 | 0.36 | 0.57 | 46.5 |
| Artemisia vulgaris | 6 | 0.09 | 12 | 0.17 | 0.18 | 0.28 | 23 |
| Asparagus racemosus | 31 | 0.44 | 41 | 0.58 | 0.36 | 0.42 | 39 |
| Asparagus gracilis | 26 | 0.37 | 36 | 0.51 | 0.27 | 0.28 | 27.5 |
| Asplenium dalhousiae | 16 | 0.23 | 27 | 0.38 | 0.36 | 0.42 | 39 |
| Astragalus psilocentros | 19 | 0.27 | 38 | 0.54 | 0.09 | 0.85 | 47 |
| Bauhinia variegata | 13 | 0.19 | 17 | 0.24 | 0.18 | 0.28 | 23 |
| Berberis lycium | 59 | 0.84 | 86 | 1.22 | 45 | 0.42 | 43.5 |
| Bidens bipinnata | 2 | 0.03 | 6 | 0.08 | 0.18 | 0.14 | 16 |
| Bidens biternata | 29 | 0.41 | 31 | 0.44 | 0.18 | 0.14 | 16 |
| Brassica compestris | 55 | 0.79 | 62 | 0.88 | 0.45 | 0.42 | 43.5 |
| Buddleja asiatica | 27 | 0.39 | 38 | 0.54 | 0.45 | 0.71 | 58 |
| Calendula officinalis | 24 | 0.34 | 39 | 0.55 | 0.18 | 0.28 | 23 |
| Cannabis sativa | 41 | 0.59 | 52 | 0.74 | 0.27 | 0.28 | 27.5 |
| Capsella bursa-pastoris | 21 | 0.30 | 37 | 0.52 | 0.45 | 0.57 | 51 |
| Carissa spinarum | 32 | 0.46 | 45 | 0.64 | 0.27 | 0.42 | 34.5 |
| Carthamus tinctorius | 41 | 0.59 | 56 | 0.8 | 0.27 | 0.28 | 27.5 |
| Caryopteris odorata | 11 | 0.16 | 22 | 0.31 | 0.81 | 0.57 | 69 |
| Cedrela toona | 36 | 0.51 | 42 | 0.6 | 0.54 | 0.71 | 62.5 |
| Chenopodium album | 26 | 0.37 | 33 | 0.47 | 0.45 | 0.42 | 43.5 |
| Dysphania ambrosioides | 4 | 0.06 | 16 | 0.22 | 0.36 | 0.14 | 25 |
| Cirsium vulgare | 11 | 0.16 | 26 | 0.41 | 0.36 | 0.42 | 39 |
| Cissampelos pareira | 21 | 0.30 | 34 | 0.45 | 0.36 | 0.42 | 39 |
| Clematis grata | 9 | 0.13 | 18 | 0.25 | 0.18 | 0.14 | 16 |
| Clematis orientalis | 7 | 0.10 | 10 | 0.14 | 0.36 | 0.57 | 46.5 |
| Colchicum luteum | 24 | 0.34 | 30 | 0.42 | 0.63 | 0.57 | 60 |
| Convolvulus arvensis | 15 | 0.21 | 19 | 0.27 | 0.27 | 0.28 | 27.5 |
| Erigeron canadensis | 14 | 0.20 | 26 | 0.37 | 0.36 | 0.28 | 32 |
| Cotinus coggygria | 6 | 0.09 | 10 | 0.14 | 0.36 | 0.57 | 46.5 |
| Cuscuta reflexia | 47 | 0.67 | 57 | 0.81 | 0.18 | 0.28 | 23 |
| Cynodon dactylon | 42 | 0.60 | 51 | 0.72 | 0.27 | 0.42 | 34.5 |
| Cyperus rotundus | 2 | 0.03 | 13 | 0.18 | 0.36 | 0.57 | 46.5 |
| Desmodium elegans | 20 | 0.29 | 48 | 0.68 | 0.45 | 0.42 | 43.5 |
| Dicliptera bupleuroides | 29 | 0.41 | 36 | 0.51 | 0.45 | 0.42 | 43.5 |
| Dioscorea deltoidea | 27 | 0.39 | 33 | 0.47 | 0.45 | 0.42 | 43.5 |
| Diospyros lotus | 25 | 0.36 | 36 | 0.51 | 0.27 | 0.14 | 20.5 |
| Dodonaea viscosa | 28 | 0.40 | 41 | 0.58 | 0.18 | 0.28 | 23 |
| Dryopteris filix-mas | 18 | 0.26 | 21 | 0.3 | 0.81 | 0.14 | 16 |
| Duchesnea indica | 43 | 0.61 | 54 | 0.77 | 0.36 | 0.42 | 39 |
| Elaeagnus umbellata | 52 | 0.74 | 71 | 1.01 | 0.36 | 0.57 | 46.5 |
| Eleusine indica | 13 | 0.19 | 28 | 0.4 | 0.63 | 0.71 | 67 |
| Eriobotrya japonica | 29 | 0.41 | 60 | 0.85 | 0.27 | 0.42 | 34.5 |
| Euphorbia helioscopia | 36 | 0.51 | 47 | 0.67 | 0.36 | 0.28 | 32 |
| Ficus carica | 53 | 0.76 | 64 | 0.91 | 0.54 | 0.57 | 55.5 |
| Ficus palmata | 33 | 0.47 | 62 | 0.88 | 0.27 | 0.28 | 27.5 |
| Fragaria nubicola | 66 | 0.94 | 83 | 1.18 | 0.45 | 0.57 | 51 |
| Galium aparine | 27 | 0.39 | 35 | 0.5 | 0.45 | 0.71 | 58 |
| Geranium wallichianum | 27 | 0.39 | 40 | 0.57 | 1 | 0.71 | 85.5 |
| Gerbera gossypina | 10 | 0.14 | 24 | 0.34 | 0.36 | 0.28 | 32 |
| Grewia asiatica | 22 | 0.31 | 34 | 0.48 | 0.09 | 1 | 54.5 |
| Habenaria digitata | 20 | 0.29 | 36 | 0.51 | 0.45 | 0.57 | 51 |
| Hedera nepalensis | 14 | 0.20 | 23 | 0.32 | 0.18 | 0.28 | 23 |
| Hypericum perforatum | 38 | 0.54 | 44 | 0.62 | 0.45 | 0.42 | 43.5 |
| Impatiens bicolor | 13 | 0.19 | 25 | 0.35 | 0.27 | 0.42 | 34.5 |
| Indigofera heterantha | 42 | 0.60 | 54 | 0.77 | 0.72 | 0.71 | 71.5 |
| Inula cappa | 28 | 0.40 | 38 | 0.54 | 0.45 | 0.42 | 43.5 |
| Ipomoea purpurea | 22 | 0.31 | 33 | 0.47 | 0.27 | 0.42 | 34.5 |
| Jasminum officinale | 25 | 0.36 | 50 | 0.71 | 0.18 | 0.28 | 23 |
| Juglans regia | 41 | 0.59 | 58 | 0.82 | 0.45 | 0.57 | 51 |
| Lespedeza juncea | 11 | 0.16 | 22 | 0.31 | 0.27 | 0.42 | 34.5 |
| Ligustrum lucidum | 22 | 0.31 | 37 | 0.52 | 0.81 | 0.85 | 83 |
| Lycopodium japonicum | 22 | 0.31 | 34 | 0.4 | 0.27 | 0.28 | 27.5 |
| Mallotus philippensis | 39 | 0.56 | 48 | 0.68 | 0.45 | 0.28 | 36.5 |
| Malvastrum Coromandelianum | 26 | 0.37 | 34 | 0.48 | 0.36 | 0.42 | 39 |
| Momordica charanta | 38 | 0.54 | 49 | 0.7 | 0.36 | 0.42 | 39 |
| Martynia annua | 23 | 0.33 | 30 | 0.42 | 0.63 | 0.57 | 60 |
| Melia azedarach | 41 | 0.59 | 69 | 0.98 | 0.36 | 0.57 | 46.5 |
| Mentha longifolia | 61 | 0.87 | 69 | 0.98 | 0.18 | 0.28 | 23 |
| Micromeria biflora | 22 | 0.31 | 44 | 0.62 | 0.54 | 3 | 48 |
| Mirabilis jalapa | 27 | 0.39 | 35 | 0.5 | 0.36 | 0.42 | 39 |
| Morus alba | 32 | 0.46 | 64 | 0.91 | 0.36 | 0.28 | 32 |
| Mucuna pruriens | 19 | 0.27 | 33 | 0.47 | 0.36 | 0.28 | 32 |
| Myrsine africana | 17 | 0.24 | 34 | 0.48 | 0.27 | 0.28 | 27.5 |
| Nepta lavigata | 6 | 0.09 | 18 | 0.25 | 0.09 | 0.14 | 11.5 |
| Olea ferruginea | 52 | 0.74 | 61 | 0.87 | 0.54 | 0.57 | 55.5 |
| Onychium japonicum | 11 | 0.16 | 27 | 0.38 | 0.18 | 0.14 | 16 |
| Oplismenus ndulatifolius | 12 | 0.17 | 27 | 0.38 | 0.45 | 0.57 | 51 |
| Origanum vulgare | 5 | 0.07 | 9 | 0.12 | 0.36 | 0.42 | 39 |
| Otostegia limbata | 10 | 0.14 | 16 | 0.22 | 0.45 | 0.42 | 43.5 |
| Oxalis corniculata | 39 | 0.56 | 51 | 0.72 | 0.63 | 0.71 | 67 |
| Parthenium hysterophorus | 31 | 0.44 | 40 | 0.57 | 0.18 | 0.28 | 23 |
| Physalis divaricata | 14 | 0.20 | 24 | 0.34 | 0.36 | 0.42 | 39 |
| Pinus roxburghii | 56 | 0.80 | 69 | 0.98 | 0.18 | 0.28 | 23 |
| Pinus wallichiana | 48 | 0.69 | 59 | 0.84 | 0.36 | 0.42 | 39 |
| Piper nigrum | 36 | 0.51 | 42 | 0.6 | 0.36 | 0.42 | 39 |
| Plantago lanceolata | 48 | 0.69 | 55 | 0.78 | 0.27 | 0.42 | 34.5 |
| Plantago major | 22 | 0.31 | 36 | 0.51 | 0.45 | 0.57 | 51 |
| Plumbago zeylanica | 8 | 0.11 | 16 | 0.22 | 0.36 | 0.42 | 39 |
| Polygonum aviculare | 25 | 0.36 | 44 | 0.42 | 0.72 | 0.42 | 57 |
| Populus alba | 42 | 0.60 | 53 | 0.75 | 0.72 | 0.71 | 71.5 |
| Prinsepia utilis | 12 | 0.17 | 22 | 0.31 | 0.36 | 0.28 | 32 |
| Prunus domestica | 33 | 0.47 | 41 | 0.58 | 0.18 | 0.28 | 23 |
| Prunus persica | 40 | 0.57 | 54 | 0.77 | 0.63 | 0.85 | 74 |
| Pteracanthus urticifolius | 5 | 0.07 | 15 | 0.21 | 0.36 | 0.42 | 39 |
| Pteris cretica | 8 | 0.11 | 8 | 0.11 | 0.09 | 0.14 | 11.5 |
| Pteris vittata | 5 | 0.07 | 11 | 0.15 | 0.27 | 0.28 | 27.5 |
| Punica granatum | 51 | 0.73 | 72 | 1.02 | 0.63 | 0.71 | 67 |
| Pyrus pashia | 41 | 0.59 | 52 | 0.74 | 0.45 | 0.42 | 43.5 |
| Quercus incana | 45 | 0.64 | 56 | 0.8 | 0.45 | 0.42 | 43.5 |
| Ricinus communis | 38 | 0.54 | 52 | 0.74 | 0.27 | 0.28 | 27.5 |
| Robinia pseudoacacia | 28 | 0.40 | 28 | 0.4 | 0.09 | 0.14 | 11.5 |
| Rosa brunonii | 41 | 0.59 | 56 | 0.8 | 0.63 | 0.57 | 60 |
| Rubia cordifolia | 21 | 0.30 | 34 | 0.48 | 0.45 | 0.42 | 43.5 |
| Rubus ellipticus | 34 | 0.49 | 49 | 0.7 | 0.18 | 0.28 | 23 |
| Rubus fruticosus | 53 | 0.76 | 62 | 0.88 | 0.36 | 0.57 | 46.5 |
| Rubus niveus | 38 | 0.54 | 61 | 0.87 | 0.45 | 0.42 | 43.5 |
| Rumex dentatus | 29 | 0.41 | 39 | 0.55 | 0.18 | 0.14 | 16 |
| Rumex hastatus | 33 | 0.47 | 42 | 0.6 | 0.27 | 0.28 | 27.5 |
| Salix nigra | 33 | 0.47 | 44 | 0.62 | 0.45 | 0.42 | 43.5 |
| Sapindus mukorossi | 46 | 0.66 | 57 | 0.81 | 0.18 | 0.28 | 23 |
| Sarcococca saligna | 32 | 0.46 | 46 | 0.65 | 0.36 | 0.57 | 46.5 |
| Smilax aspera | 8 | 0.11 | 13 | 0.18 | 0.36 | 0.57 | 46.5 |
| Solanum nigrum | 42 | 0.60 | 58 | 0.82 | 0.45 | 0.71 | 58 |
| Solena heterophylla | 17 | 0.24 | 27 | 0.38 | 0.63 | 0.71 | 67 |
| Swertia angustifolia | 5 | 0.07 | 15 | 0.21 | 0.36 | 0.57 | 46.5 |
| Swertia cordata | 4 | 0.06 | 10 | 0.14 | 0.54 | 0.42 | 48 |
| Tagetes minuta | 14 | 0.20 | 25 | 0.35 | 0.09 | 0.14 | 11.5 |
| Taraxacum officinale | 38 | 0.54 | 41 | 0.58 | 0.45 | 0.57 | 51 |
| Taxus wallichiana | 39 | 0.56 | 48 | 0.68 | 0.36 | 0.14 | 25 |
| Thalictrum foliolosum | 7 | 0.10 | 18 | 0.25 | 0.18 | 0.14 | 16 |
| Tylophora hirsuta | 11 | 0.16 | 24 | 0.34 | 0.45 | 0.57 | 51 |
| Verbascum thapsus | 12 | 0.17 | 23 | 0.32 | 0.27 | 0.28 | 27.5 |
| Vinca major | 12 | 0.17 | 25 | 0.35 | 0.54 | 0.42 | 52.5 |
| Viola canescens | 65 | 0.93 | 75 | 1.07 | 0.36 | 0.57 | 46.5 |
| Vitex negundo | 13 | 0.19 | 23 | 0.32 | 0.36 | 0.42 | 39 |
| Zanthoxylum alatum | 49 | 0.70 | 66 | 0.94 | 0.45 | 0.14 | 29.5 |
| Ziziphus jujuba | 19 | 0.27 | 30 | 0.42 | 0.27 | 0.42 | 34.5 |
| Ziziphus oxyphylla | 20 | 0.29 | 32 | 0.45 | 0.36 | 0.42 | 39 |
FC: Frequency of Citation; RFC: Relative frequency of citation; Ui: number of uses mentioned by each informant for a given species; UV: Use value; Rel. PH: Relative number of pharmacological properties attributed to a single plant; Rel. BS: Relative number of body systems treated by a single species; RI: Relative Importance.
References
- Domfeh, K.A. Indigenous knowledge systems and the need for policy and institutional reforms. Tribes Tribals 2007, 1, 41–52. [Google Scholar]
- World Health Organization. Traditional Medicine: Report by the Secretariat; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Tilburt, J.C.; Kaptchuk, T.J. Herbal medicine research and global health: An ethical analysis. Bull. World Health Organ. 2008, 86, 594–599. [Google Scholar] [CrossRef]
- Farnsworth, N.R. Ethnopharmacology and drug development. Ciba Found. Symp. Ethnobot. Search New Drugs 1994, 185, 42–51. [Google Scholar]
- Stickley, A.; Koyanagi, A.; Richardson, E.; Roberts, B.; Balabanova, D.; McKee, M. Prevalence and factors associated with the use of alternative (folk) medicine practitioners in 8 countries of the former Soviet Union. BMC Complement. Altern. Med. 2013, 13, 83. [Google Scholar] [CrossRef] [PubMed]
- El Nimr, N.; Wahdan, I.; Wahdan, A.; Kotb, R. Self-medication with drugs and complementary and alternative medicines in Alexandria, Egypt: Prevalence, patterns and determinants. EMHJ East. Mediterr. Health J. 2015, 21, 256–265. [Google Scholar] [CrossRef] [PubMed]
- Karou, S.D.; Tchacondo, T.; Djikpo Tchibozo, M.A.; Abdoul-Rahaman, S.; Anani, K.; Koudouvo, K.; Batawila, K.; Agbonon, A.; Simpore, J.; de Souza, C. Ethnobotanical study of medicinal plants used in the management of diabetes mellitus and hypertension in the Central Region of Togo. Pharm. Biol. 2011, 49, 1286–1297. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHO Traditional Medicine Strategy 2002–2005; World Health Organization: Geneva, Switzerland, 2002. [Google Scholar]
- James, P.B.; Wardle, J.; Steel, A.; Adams, J. Traditional, complementary and alternative medicine use in Sub-Saharan Africa: A systematic review. BMJ Glob. Health 2018, 3, e000895. [Google Scholar] [CrossRef]
- World Health Organization. The World Medicines Situation Report 2004; No. WHO/EDM/PAR/2004.5; World Health Organization: Geneva, Switzerland, 2004. [Google Scholar]
- Payyappallimana, U. Role of traditional medicine in primary health care: An overview of perspectives and challenging. Yokohama Int. Soc. Sci. Res. 2010, 14, e77. [Google Scholar]
- Langlois-Klassen, D.; Kipp, W.; Jhangri, G.S.; Rubaale, T. Use of traditional herbal medicine by AIDS patients in Kabarole District, western Uganda. Am. J. Trop. Med. Hyg. 2007, 77, 757–763. [Google Scholar] [CrossRef] [PubMed]
- Christenhusz, M.J.M.; Byng, J.W. The number of known plants species in the world and its annual increase. Phytotaxa 2000, 261, 201–217. [Google Scholar] [CrossRef]
- Gazzaneo, L.R.S.; De Lucena, R.F.P.; de Albuquerque, U.P. Knowledge and use of medicinal plants by local specialists in an region of Atlantic Forest in the state of Pernambuco (Northeastern Brazil). J. Ethnobiol. Ethnomed. 2005, 1, 9. [Google Scholar] [CrossRef] [PubMed]
- Hanazaki, N.; Tamashiro, J.Y.; Leitão-Filho, H.F.; Begossi, A. Diversity of plant uses in two Caiçara communities from the Atlantic Forest coast, Brazil. Biodivers. Conserv. 2000, 9, 597–615. [Google Scholar] [CrossRef]
- Verpoorte, R. Pharmacognosy in the new millennium: Lead finding and biotechnology. J. Pharm. Andppharmacol. 2000, 52, 253–262. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.-Y.; Wang, J.-D.; Lo, T.-C.; Chen, P.-C. Increased mortality risk for cancers of the kidney and other urinary organs among Chinese herbalists. J. Epidemiol. 2009, 19, 17–23. [Google Scholar] [CrossRef]
- Van Wyk, B.-E.; Wink, M. Medicinal Plants of the World; CABI: Houston, TX, USA, 2018. [Google Scholar]
- Ishtiaq, M.; Qing, H.; Wang, Y.; Cheng, Y. A comparative study using chemometric and numerical taxonomic approaches in the identification and classification of traditional Chinese medicines of the genus Clematis. Plant Biosyst. 2010, 144, 288–297. [Google Scholar] [CrossRef]
- Verpoorte, R.; Choi, Y.H.; Kim, H.K. Ethnopharmacology and systems biology: A perfect holistic match. J. Ethnopharmacol. 2005, 100, 53–56. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, K.S.; Qureshi, R.; Hameed, M.; Ahmad, F.; Nawaz, T. Conservation assessment and medicinal importance of someplants resources from Sharda, Neelum Valley, Azad Jammu and Kashmir, Pakistan. Int. J. Agric. Biol. 2012, 14, 997–1000. [Google Scholar]
- Jamila, F.; Mostafa, E. Ethnobotanical survey of medicinal plants used by people in Oriental Morocco to manage various ailments. J. Ethnopharmacol. 2014, 154, 76–87. [Google Scholar] [CrossRef]
- Amjad, M.S.; Arshad, M.; Saboor, A.; Page, S.; Chaudhari, S.K. Ethnobotanical profiling of the medicinal flora of Kotli, Azad Jammu and Kashmir, Pakistan: Empirical reflections on multinomial logit specifications. Asian Pac. J. Trop. Med. 2017, 10, 503–514. [Google Scholar] [CrossRef] [PubMed]
- Salhi, S.; Fadli, M.; Zidane, L.; Douira, A. Floristic and ethnobotanical study of medicinal plants of Kénitra (Maroc). Lazaroa 2010, 31, 133–146. [Google Scholar] [CrossRef]
- Salhi, N.; Bouyahya, A.; Fettach, S.; Zellou, A.; Cherrah, Y. Ethnopharmacological study of medicinal plants used in the treatment of skin burns in occidental Morocco (area of Rabat). South Afr. J. Bot. 2019, 121, 128–142. [Google Scholar] [CrossRef]
- Liu, Z.-H.; Niu, F.-J.; Xie, Y.-X.; Xie, S.-M.; Liu, Y.-N.; Yang, Y.-Y.; Zhou, C.-Z.; Wan, X.-H. A review: Natural polysaccharides from medicinal plants and microorganisms and their anti-herpetic mechanism. Biomed. Pharmacother. 2020, 129, 110469. [Google Scholar] [CrossRef] [PubMed]
- Fitzgerald, M.; Heinrich, M.; Booker, A. Medicinal Plant Analysis: A Historical and Regional Discussion of Emergent Complex Techniques. Front. Pharmacol. 2019, 10, 1480. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. The Promotion and Development of Traditional Medicine. In Proceedings of the Report of a WHO Meeting, Geneva, Switzerland, 28 November–2 December 1977; World Health Organization: Geneva, Switzerland, 1978. [Google Scholar]
- Boccolini, P.d.M.M.; Boccolini, C.S. Prevalence of complementary and alternative medicine (CAM) use in Brazil. BMC Complement. Med. Ther. 2020, 20, 1–10. [Google Scholar]
- Bannerman, R.H.; Burton, J.; Wen-Chieh, C. Traditional Medicine and Health Care Coverage: A Reader for Health Administrators and Practitioners; World Health Organization: Geneva, Switzerland, 1983; p. 342. [Google Scholar]
- Aziz, M.A.; Adnan, M.; Khan, A.H.; Shahat, A.A.; Al-Said, M.S.; Ullah, R. Traditional uses of medicinal plants practiced by the indigenous communities at Mohmand Agency, FATA, Pakistan. J. Ethnobiol. Ethnomed. 2018, 14, 2. [Google Scholar] [CrossRef] [PubMed]
- Mallick, S. Challenges of mainstreaming: Ayurvedic practice in Delhi Government health institutions. J. Ayurveda Integr. Med. 2016, 7, 57–61. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Li, X.; Lu, J.; Hu, S.; Cheng, K.; De Maeseneer, J.; Meng, Q.; Mossialos, E.; Xu, D.R.; Yip, W.; Zhang, H. The primary health-care system in China. Lancet 2017, 390, 2584–2594. [Google Scholar] [CrossRef] [PubMed]
- Sen, S.; Chakraborty, R. Revival, modernization and integration of Indian traditional herbal medicine in clinical practice: Importance, challenges and future. J. Tradit. Complement. Med. 2017, 7, 234–244. [Google Scholar] [CrossRef] [PubMed]
- Redvers, N.; Marianayagam, J.; Blondin, B. Improving access to Indigenous medicine for patients in hospital-based settings: A challenge for health systems in northern Canada. Int. J. Circumpolar Health 2019, 78, 1589208. [Google Scholar] [CrossRef] [PubMed]
- Reyes-García, V. The values of traditional ecological knowledge. In Handbook of Ecological Economics; Edward Elgar Publishing: Northampton, MA, USA, 2015. [Google Scholar]
- Dar, E.M. Ethnobotanical uses of plants of Lawat district Muzaffarabad, Azad Jammu & Kashmir. Asian J. Plant Sci. 2014, 2, 3. [Google Scholar]
- Amjad, M.S.; Arshad, M. Ethnobotanical inventory and medicinal uses of some important woody plant species of Kotli, Azad Kashmir, Pakistan. Asian Pac. J. Trop. Biomed. 2014, 4, 952–958. [Google Scholar] [CrossRef]
- Rashid, S.; Ahmad, M.; Zafar, M.; Sultana, S.; Ayub, M.; Khan, M.A.; Yaseen, G. Ethnobotanical survey of medicinally important shrubs and trees of Himalayan region of Azad Jammu and Kashmir, Pakistan. J. Ethnopharmacol. 2015, 166, 340–351. [Google Scholar] [CrossRef] [PubMed]
- Shaukat, S.A.; Shah, S.Z.A.; Ahmad, M.J.; Shaukat, S.K.; Shoukat, S.W. Ethnobotanical study of some medicinal plants of union council Bangoin, Tehsil Rawalakot, AJ&K. Agric. Adv. 2012, 1, 105–109. [Google Scholar]
- Ikram, A.U.; Nadia, B.Z.; Zabta, K.S.; Mohammad, Q. Ethnomedicinal review resources and their utilization practices in village populations of Kashmir himalayas. Pak. J. Bot. 2012, 44, 739–745. [Google Scholar]
- Hamayun, M. Ethnobotanical profile of Utror and Gabral valleys, district Swat, Pakistan. Ethnobot. Leafl. 2005, 2005, 9. [Google Scholar]
- Khan, M.A.; Khan, M.A.; Hussain, M.; Ghulam, G.M. An ethnobotanical inventory of Himalayan region Poonch valley Azad Kashmir (Pakistan). Ethnobot. Res. Appl. 2010, 8, 107–123. [Google Scholar] [CrossRef]
- Shaheen, H.; Qaseem, M.F.; Amjad, M.S.; Bruschi, P. Exploration of ethno-medicinal knowledge among rural communities of Pearl Valley, Rawalakot, District Poonch Azad Jammu and Kashmir. PLoS ONE 2017, 12, e0183956. [Google Scholar] [CrossRef]
- Ahmad, M.; Sultana, S.; Fazl-i-Hadi, S.; Ben Hadda, T.; Rashid, S.; Zafar, M.; Khan, M.A.; Khan, M.P.Z.; Yaseen, G. An Ethnobotanical study of Medicinal Plants in high mountainous region of Chail valley (District Swat-Pakistan). J. Ethnobiol. Ethnomed. 2014, 10, 36. [Google Scholar] [CrossRef] [PubMed]
- Bibi, T.; Ahmad, M.; Tareen, R.B.; Tareen, N.M.; Jabeen, R.; Rehman, S.U.; Zafar, M. Ethnobotany medicinal Plants in district Mastung of Balochistan province-Pakistan. J. Ethnopharmacol. 2014, 157, 79–89. [Google Scholar] [PubMed]
- Amjad, M.S.; faisal Qaeem, M.; Ahmad, I.; Khan, S.U.; Chaudhari, S.K.; Malik, N.Z.; Shaheen, H.; Khan, A.M. Descriptive study of plant resources in the context of the ethnomedicinal relevance of indigenous flora: A case study from Toli Peer National Park, Azad Jammu and Kashmir, Pakistan. PLoS ONE 2017, 12, e0171896. [Google Scholar]
- Albuquerque, U.P.D.; Soldati, G.T.; Sieber, S.S.; Ramos, M.A.; Sa, J.C.D.; Souza, L.C.D. The use of plants in the medical system of the Fulni-o-people (NE Brazil): A perspective on age and gender. J. Ethnopharmacol. 2011, 133, 866–873. [Google Scholar] [CrossRef] [PubMed]
- Kayani, S.; Ahmad, M.; Sultana, S.; Shinwari, Z.K.; Zafar, M.; Yaseen, G.; Hussain, M.; Bibi, T. Ethnobotany of medicinal plants among the communities of Alpine and Sub-alpine regions of Pakistan. J. Ethnopharmacol. 2015, 164, 186–202. [Google Scholar] [CrossRef] [PubMed]
- Abbasi, A.M.; Khan, M.A.; Zafar, M. Ethnomedicinal assessment of some selected wild edible fruits and vegetables of lesser Himalayas, Pakistan. J. Ethnopharmacol. 2013, 45, 215–222. [Google Scholar]
- Giday, M.; Asfaw, Z.; Woldu, Z. Medicinal plants of the Meinit ethnic group of Ethiopia: An ethnobotanical study. J. Ethnopharmacol. 2009, 124, 513–521. [Google Scholar] [CrossRef] [PubMed]
- Tugume, P.; Esezah, K.K.; Buyinza, M.; Namaalwa, J.; Kamatenesi, M.; Mucunguzi, P.; Kalema, J. Ethnobotanical survey of medicinal plant species used by communities around Mabira Central Forest Reserve, Uganda. J. Ethnobiol. Ethnomed. 2010, 12, 5. [Google Scholar] [CrossRef] [PubMed]
- Farooq, A.; Amjad, M.S.; Ahmad, K.; Altaf, M.; Umair, M.; Abbasi, A.M. Ethnomedicinal knowledge of the rural communities of Dhirkot, Azad Jammu and Kashmir, Pakistan. J. Ethnobiol. Ethnomed. 2019, 15, 45. [Google Scholar] [CrossRef] [PubMed]
- Zuma, T.; Wight, D.; Rochat, T.; Moshabela, M. The role of traditional health practitioners in Rural KwaZulu-Natal, South Africa: Generic or mode specific? BMC Complement. Altern. Med. 2016, 16, 304. [Google Scholar] [CrossRef]
- Aletor, G. Domiciliary midwifery care, including traditional birth attendants. In Maternal and Child Health around the World; Springer: Berlin/Heidelberg, Germany, 1981; pp. 89–98. [Google Scholar]
- Campero, L.; García, C.; Díaz, C.; Ortiz, O.; Reynoso Sa Langer, A. “Alone, I wouldn’t have known what to do”: A qualitative study on social supportduring labor and delivery in Mexico. Soc. Sci. Med. 1998, 47, 395–403. [Google Scholar] [CrossRef] [PubMed]
- Napagoda, M.T.; Sundarapperuma, T.; Fonseka, D.; Amarasiri, S.; Gunaratna, P. An Ethnobotanical Study of the Medicinal Plants Used as Anti-Inflammatory Remedies in Gampaha District, Western Province, Sri Lanka. Scientifica 2018, 2018, 9395052. [Google Scholar] [CrossRef]
- Acharya, K.P.; Kaphle, K. Ethnomedicinal plants used by yak herders for management of health disorders. J. Intercult. Ethnopharmacol. 2015, 4, 270. [Google Scholar] [CrossRef]
- Yaseen, G.; Ahmad, M.; Shinwari, S.; Potter, D.; Zafar, M.; Zhang, G.; Shinwari, Z.K.; Sultana, S. Medicinal plants diversity used for livelihood of public health in desert and arid regions of Sindh, Pakistan. Pak. J. Bot. 2019, 2, 2409–2419. [Google Scholar] [CrossRef]
- Bano, A.; Ahmad, M.; Hadda, B.T.; Saboor, A.; Zafar, M.; Khan, M.P.Z.; Arshad, M.; Ashra, M.A. Quantitative ethnomedicinal study of plants used in the Skardu valley at high altitude of Karakoram-Himalayan range, Pakistan. J. Ethnobiol. Ethnomed. 2014, 10, 43–71. [Google Scholar] [CrossRef] [PubMed]
- Gebeyehu, G.; Asfaw, Z.; Enyew, A.; Raja, N. Ethnobotanical study of traditional medicinal plants and their conservation status in Mecha Wereda West Gojjam Zone of Ethiopia. Int. J. Pharm. Health Care Res. 2014, 2, 137–154. [Google Scholar]
- Merétika, A.H.C.; Peroni, N.; Hanazaki, N. Local knowledge of medicinal plants in three artisanal fishing communities (Itapoá, Southern Brazil), according to gender, age, and urbanization. Acta Bot. Bras. 2010, 24, 386–394. [Google Scholar] [CrossRef]
- Agarwal, K.; Varma, R. Some ethnomedicinal plants of Bhopal district used for treating stone diseases. Int. J. Pharm. Life Sci. 2012, 3, 1356. [Google Scholar]
- Khattak, N.S.; Nouroz, F.; Rahman, I.U.; Noreen, S. Ethno veterinary uses of medicinal plants of district Karak, Pakistan. J. Ethnopharmacol. 2015, 171, 273–279. [Google Scholar] [CrossRef] [PubMed]
- Giday, M.; Asfaw, Z.; Elmqvist, T.; Woldu, Z. An ethnobotanical study of medicinal plants used by the Zay people in Ethiopia. J. Ethnopharmacol. 2003, 85, 43–52. [Google Scholar] [CrossRef]
- Giday, M.; Teklehaymanot, T.; Animut, A.; Mekonnen, Y. Medicinal plants of the Shinasha, Agew-awi and Amhara peoples in northwest Ethiopia. J. Ethnopharmacol. 2007, 110, 516–525. [Google Scholar] [CrossRef] [PubMed]
- Uprety, Y.; Asselin, H.; Boon, E.K.; Yadav, S.; Shrestha, K.K. Indigenous use and bio-efficacy of medicinal plants in the Rasuwa District, Central Nepal. J. Ethnobiol. Ethnomed. 2010, 6, 3. [Google Scholar] [CrossRef]
- Megersa, M.; Asfaw, Z.; Kelbessa, E.; Beyene, A.; Woldeab, B. An ethnobotanical study of medicinal plants in Wayu Tuka district, east Welega zone of oromia regional state, West Ethiopia. J. Ethnobiol. Ethnomed. 2013, 9, 68. [Google Scholar] [CrossRef] [PubMed]
- Uniyal, S.K.; Singh, K.; Jamwal, P.; Lal, B. Traditional use of medicinal plants among the tribal communities of Chhota Bhangal, Western Himalaya. J. Ethnobiol. Ethnomed. 2006, 2, 14. [Google Scholar] [CrossRef] [PubMed]
- Mesfin, F.; Demissew, S.; Teklehaymanot, T. An ethnobotanical study of medicinal plants in Wonago Woreda, SNNPR, Ethiopia. J. Ethnobiol. Ethnomed. 2009, 5, 28. [Google Scholar] [CrossRef] [PubMed]
- Rashid, S.; Ahmad, M.; Zafar, M.; Anwar, A.; Sultana, S.; Tabassum, S.; Ahmed, S.N. Ethnopharmacological evaluation and antioxidant activity of some important herbs used in traditional medicines. J. Tradit. Chin. Med. 2016, 36, 689–694. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.A.; Khan, M.A.; Hussain, M.; Mujtaba, G. Medicinal plants used in folk recipes by the inhabitants of Himalayan region Poonch Valley Azad Kashmir (Pakistan). J. Basic Appl. Sci. 2012, 8, 35–45. [Google Scholar] [CrossRef]
- Jan, G.; Khan, M.A.; Farhatullah, J.F.; Ahmad, M.; Jan, M.; Zafar, M. Ethnobotanical studies on some useful plants of Dir Kohistan valleys, KPK, Pakistan. Pak. J. Bot. 2011, 43, 1849–1852. [Google Scholar]
- Ishtiaq, M.; Mumtaz, A.S.; Hussain, T.; Ghani, A. Medicinal plant diversity in the flora of Leepa Valley, Muzaffarabad (AJK), Pakistan. Afr. J. Biotechnol. 2012, 11, 3087–3098. [Google Scholar]
- Ahmad, K.S.; Hamid, A.F.; Nawaz, F.; Hameed, M.; Ahmad, F.; Deng, J.; Mahroof, S. Ethnopharmacological studies of indigenous plants in Kel village, Neelum Valley, Azad Kashmir, Pakistan. J. Ethnobiol. Ethnomed. 2017, 13, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Sargın, S.A.; Akçicek, E.; Selvi, S. An ethnobotanical study of medicinal plants used by the local people of Alaşehir (Manisa) in Turkey. J. Ethnopharmacol. 2013, 150, 860–874. [Google Scholar] [CrossRef] [PubMed]
- Musa, M.S.; Abdelrasool, F.E.; Elsheikh, E.A.; Ahmed, L.A.; Mahmoud, A.L.E.; Yagi, S.M. Ethnobotanical study of medicinal plants in the Blue Nile State, South-eastern Sudan. J. Med. Plants Res. 2011, 5, 4287–4297. [Google Scholar]
- Hada, B.S.; Katewa, S. Ethnomedicinal plants used against various diseases in Jhalawar district, Rajasthan, India. J. Glob. Biosci. 2015, 4, 2077–2086. [Google Scholar]
- Umair, M.; Altaf, M.; Abbasi, A.M. An ethnobotanical survey of indigenous medicinal plants in Hafizabad district, Punjab—Pakistan. PLoS ONE 2017, 12, e0177912. [Google Scholar] [CrossRef] [PubMed]
- Rahman, I.U.; Ijaz, F.; Afzal, A.; Iqbal, Z.; Ali, N.; Khan, S.M. Contributions to the phytotherapies of digestive disorders: Traditional knowledge and cultural drivers of Manoor Valley, Northern Pakistan. J. Ethnopharmacol. 2016, 192, 30–52. [Google Scholar] [CrossRef]
- Noreen, F.; Tamoor, M.; Adil, M.; Mushtaq, U.; Nisa, Q. Data of Ethnomedicinal Plants in Wazirabad, District Gujranwala, Punjab. Pak. J. Pharmacol. Care Health Syst. 2018, 5, 2376-0419. [Google Scholar]
- Qaseem, M.F.; Qureshi, R.; Amjad, M.S.; Waseem, M.; Sajid, A. Ethnobotanical evaluation of traditional medicinal plants among three rural communities of Goi and Dhanwa union council, District Kotli, Azad Jammu & Kashmir. Appl. Ecol. Environ. Res. 2019, 6, 340–349. [Google Scholar]
- Umair, M.; Altaf, M.; Bussmann, R.W.; Abbasi, A.M. Ethnomedicinal uses of the local flora in Chenab riverine area, Punjab province Pakistan. J. Ethnobiol. Ethnomed. 2019, 15, 7. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.P.Z.; Ahmad, M.; Zafar, M.; Sultana, S.; Ali, M.I.; Sun, H. Ethnomedicinal uses of edible wild fruits (EWFs) in Swat Valley, Northern Pakistan. J. Ethnopharmacol. 2015, 173, 191–203. [Google Scholar] [CrossRef] [PubMed]
- Hussain, W.; Badshah, L.; Ullah, M.; Ali, M.; Ali, A.; Hussain, F. Quantitative study of medicinal plants used by the communities residing in Koh-e-Safaid Range, northern Pakistani-Afghan borders. J. Ethnobiol. Ethnomed. 2018, 14, 30. [Google Scholar] [CrossRef] [PubMed]
- Khan, S.M.; Page, S.; Ahmad, H.; Shaheen, H.; Ullah, Z.; Ahmad, M.; Harper, D.M. Medicinal flora and ethnoecological knowledge in the Naran Valley, Western Himalaya, Pakistan. J. Ethnobiol. Ethnomed. 2013, 9, 4. [Google Scholar] [CrossRef] [PubMed]
- Ngarivhume, T.; van’t Klooster, C.I.; de Jong, J.T.; Van der Westhuizen, J.H. Medicinal plants used by traditional healers for the treatment of malaria in the Chipinge district in Zimbabwe. J. Ethnopharmacol. 2015, 159, 224–237. [Google Scholar] [CrossRef] [PubMed]
- Shah, N.A.; Khan, M.R.; Adhmans, A.N. Antileishmanial, toxicity, and phytochemical evaluation of medicinal plants collected from Pakistan. Bio. Med. Res. Int. 2014, 2014, 384204. [Google Scholar] [CrossRef] [PubMed]
- Datta, T.; Patra, A.K.; Dastidar, S.G. Medicinal plants used by the tribal population of Coochbehar district, West Bengal, India-an ethnobotanical survey. Asian Pac. J. Trop. Biomed. 2014, 4, 478–482. [Google Scholar] [CrossRef] [PubMed]
- Belayneh, A.; Asfaw, Z.; Demissew, S.; Bussa, N.F. Medicinal plants potential and use by pastoral and agro-pastoral communities in Erer Valley of Babile Wereda, Eastern Ethiopia. J. Ethnobiol. Ethnomed. 2012, 8, 42. [Google Scholar] [CrossRef] [PubMed]
- Balde, A.M.; Traore, M.S.; Diallo, M.S.T.; Balde, E.S.; Huang, Y.; Liu, Z.; Pieters, L. Ethnobotanical survey, antimicrobial and anticomplementary activities of Guinean medicinal plants traditionally used in the treatment of inflammatory diseases in Conakry and Dubreka. J. Plant Sci. 2015, 3, 11–19. [Google Scholar]
- Cornara, L.; Rocca, A.L.; Marsili, S.; Mariotti, M.G. Raditional uses of plants in the Eastern Riviera (Liguria, Italy). J. Ethnopharmacol. 2009, 125, 16–30. [Google Scholar] [CrossRef]
- Neves, J.M.; Matos, C.; Moutinho, C.; Queiroz, G.; Gomes, L.R. Ethnopharmacological notes about ancient uses of medicinal plants inTras-os-Montes (northern of Portugal). J. Ethnopharmacol. 2009, 124, 270–283. [Google Scholar] [CrossRef] [PubMed]
- Mukherjee, P.K.; Nema, N.K.; Venkatesh, P.; Debnath, P.K. Changing scenario for promotion and development of Ayurveda±way forward. J. Ethnopharmacol. 2012, 43, 424–434. [Google Scholar] [CrossRef] [PubMed]
- Trotter, I.I.R.T.; Logan, M.H. Informant consensus: A new approach for identifying potentially effective medicinal plants. In Plants in Indigenous Medicine and Diet: Biobehavioral Approaches; Redgrave Publishing Company: Bedford Hills, NY, USA, 1986. [Google Scholar]
- Camou-Guerrero, A.; GarcõÂa, V.R.; Ramos, M.M.; Casas, A. Knowledge and use value of plant species in a RaraÂmuri community: A gender perspective for conservation. Hum. Ecol. 2008, 36, 259–272. [Google Scholar] [CrossRef]
- Bano, A.; Ahmad, M.; Zafar, M.; Sultana, S.; Rashid, S.; Khan, M.A. Ethnomedicinal knowledge of the most commonly used plants from Deosai Plateau, Western Himalayas, Gilgit Baltistan, Pakistan. J. Ethnopharmacol. 2014, 155, 1046–1052. [Google Scholar] [CrossRef] [PubMed]
- Albuquerque, U.P.; Lucena, R.F.; Monteiro, J.M.; Florentino, A.T.; Cecília de Fátima, C. Evaluating two quantitative ethnobotanical techniques. Ethnobot. Res. Appl. 2006, 4, 051–060. [Google Scholar] [CrossRef]
- Adzu, B.; Amos, S.; Amizan, M.; Gamaniel, K. Evaluation of the antidiarrheal effects of Zizyphus spina-christi stem bark in rats. Acta Trop. 2003, 87, 245–250. [Google Scholar] [CrossRef] [PubMed]
- Schlage, C.; Mabula, C.; Heinrich, R.M. Medicinal plants of the Washambaa (Tanzania): Documentation and ethnopharmacological evaluation. Plant Biol. 2000, 2, 83–92. [Google Scholar] [CrossRef]
- Ankli, A.; Sticher, O.; Heinrich, M. Medical ethnobotany of the Yucatec Maya: Healers’ consensus as a quantitative criterion. Econ. Bot. 1999, 53, 144–160. [Google Scholar] [CrossRef]
- Bennett, B.C.; Prance, G.T. Introduced plants in the indigenous pharmacopoeia of Northern South America. Econ. Bot. 2000, 54, 90–102. [Google Scholar] [CrossRef]
- Tangjitman, K.; Wongsawad, C.; Kamwong, K.; Sukkho, T.; Trisonthi, C. Ethnomedicinal plants used for digestive system disorders by the Karen of northern Thailand. J. Ethnobiol. Ethnomed. 2015, 11, 27. [Google Scholar] [CrossRef]
- Malla, B.; Gauchan, D.P.; Chhetri, R.B. An ethnobotanical study of medicinal plants used by ethnic people in Parbat district of western Nepal. J. Ethnopharmacol. 2015, 165, 103–117. [Google Scholar] [CrossRef] [PubMed]
- Murad, W.; Azizullah, A.; Adnan, M.; Tariq, A.; Khan, K.U.; Waheed, S. Ethnobotanical assessment of plant resources of Banda Daud Shah, District Karak, Pakistan. J. Ethnobiol. Ethnomed. 2013, 9, 77. [Google Scholar] [CrossRef] [PubMed]
- Rokaya, M.B.; Uprety, Y.; Poudel, R.C.; Timsina, B.; Münzbergová, Z.; Asselin, H.; Tiwari, A.; Shrestha, S.S.; Sigdel, S.R. Traditional uses of medicinal plants in gastrointestinal disorders in Nepal. J. Eethnopharmacol. 2014, 158, 221–229. [Google Scholar] [CrossRef]
- Ridvan, P.; Ugur, C.; Kaan, K.; Denizhan, U.M.; Zafer, T. An ethnobotanical study on medicinal plants in Espiye and its surrounding (Giresun-Turkey). J. Ethnopharmacol. 2015, 163, 1–11. [Google Scholar]
- Srithi, K.; Balslev, H.; Wangpakapattanawong, P.; Srisanga, P.; Trisonthi, C. Medicinal plant knowledge and its erosion among the Mien (Yao) in northern Thailand. J. Ethnopharmacol. 2009, 123, 335–342. [Google Scholar] [CrossRef]
- Hassan-Abdallah, A.; Merit, A.; Hassan, S.; DAboubaker Djama, M.; Asfaw, Z.; Kelbessa, E. Medicinal plants and their uses by the people in the region of Randa, Djibouti. J. Ethnopharmacol. 2013, 148, 8701–8713. [Google Scholar] [CrossRef] [PubMed]
- Chaudhary, N.I.; Schnapp, A.; Park, J.E. Pharmacologic differentiation of inflammation and fibrosis in the rat bleomycin model. Am. J. Respir. Crit. Care Med. 2006, 173, 769–776. [Google Scholar] [CrossRef] [PubMed]
- Leonti, M.; Casu, L.; Sanna, F.; Bonsignore, L. A comparison of medicinal plant use in Sardinia and Sicily—Ve material medicare visited. J. Ethnopharmacol. 2009, 121, 255–267. [Google Scholar] [CrossRef]
- Wolda, H. Similarity indices, sample size and diversity. Oecologia 1981, 50, 296–302. [Google Scholar] [CrossRef] [PubMed]
- Hazrat, A.; Nisar, M.; Sher, K.; Zaman, S. Role of economic plants in the community development of Dir valley Khyber Pakhtunkhwa, Pakistan. FUUAST J. Biol. 2015, 5, 137–143. [Google Scholar]
- Khan, S.; Din, N.U.; Sohail, I.; Rahman, F.I.; Iqbal, Z.; Ali, Z. Ethnobotanical study of some medicinal plants of tehsil Kabal, District Swat, KP, Pakistan. Med. Aromat. Plants 2015, 4, 2167-0412. [Google Scholar]
- Khan, S.W.; Abbas, Q.; Hassan, S.N.; Khan, H.; Hussain, A. Medicinal Plants of Turmic Valley (Central Karakoram National Park), Gilgit-Baltistan, Pakistan. J. Bioresour. Manag. 2015, 2, 11. [Google Scholar]
- Nasir, E.; Ali, S.; Stewart, R.R. Flora of West Pakistan: An annotated catalogue of the vascular plants of West Pakistan and Kashmir; Fakhri: Karachi, Pakistan, 1972. [Google Scholar]
- Nasir, Y.J.; Ali, S. Flora of Pakistan: Department of Botany, University of Karachi; National Herbarium 1994–2010.
- Chase, M.W.; Christenhusz, M.; Fay, M.; Byng, J.; Judd, W.S.; Soltis, D.; Mabberley, D.; Sennikov, A.; Soltis, P.S.; Stevens, P.F. An update of the Angiosperm Phylogeny Group classification for the orders and families of flowering plants: APG IV. Bot. J. Linn. Soc. 2016, 181, 1–20. [Google Scholar]
- Gardens, R.B. Kew MBG: The Plant List, Version 1.1.
- Vijayakumar, J.; Yabesh, M.; Prabhu, S.; Manikandanz, R.; Muralidharan, B. Quantitative ethnomedicinal study of plants used in the Nelliyampathy hills of Kerala, India. J. Ethnopharmacol. 2015, 161, 238–254. [Google Scholar] [CrossRef] [PubMed]
- Heinrich, M.; Ankli, A.; Frei, B.; Weimann, C.; Sticher, O. Medicinal plants in Mexico: Healers’ consensus and cultural importance. Soc. Sci. Med. 1998, 4, 1859–1871. [Google Scholar] [CrossRef] [PubMed]
- Gonza, T.M.; Casares, R.P.M.; Sanchez, R.C.P.; Ramiro, G.J.M.; Molero, M.J.; Pieroni, A. Medicinal plants in the Mediterranean area: Synthesis of the results of the project RUBIA. J. Ethnopharmacol. 2008, 116, 341–357. [Google Scholar]
- Alexiades, M.N.; Sheldon, J.W. Selected Guidelines for Ethnobotanical Research: A Field Manual; The New York Botanical Garden: Bronx, NY, USA, 1996. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).