Pancreatic Cancer Surgery: What Matters to Patients?
Abstract
1. Introduction
2. Patient-Reported Outcome Measures (PROMs) in Pancreatic Cancer Surgery
3. Patient-Reported Experience Measures (PREMs) in Pancreatic Cancer Surgery
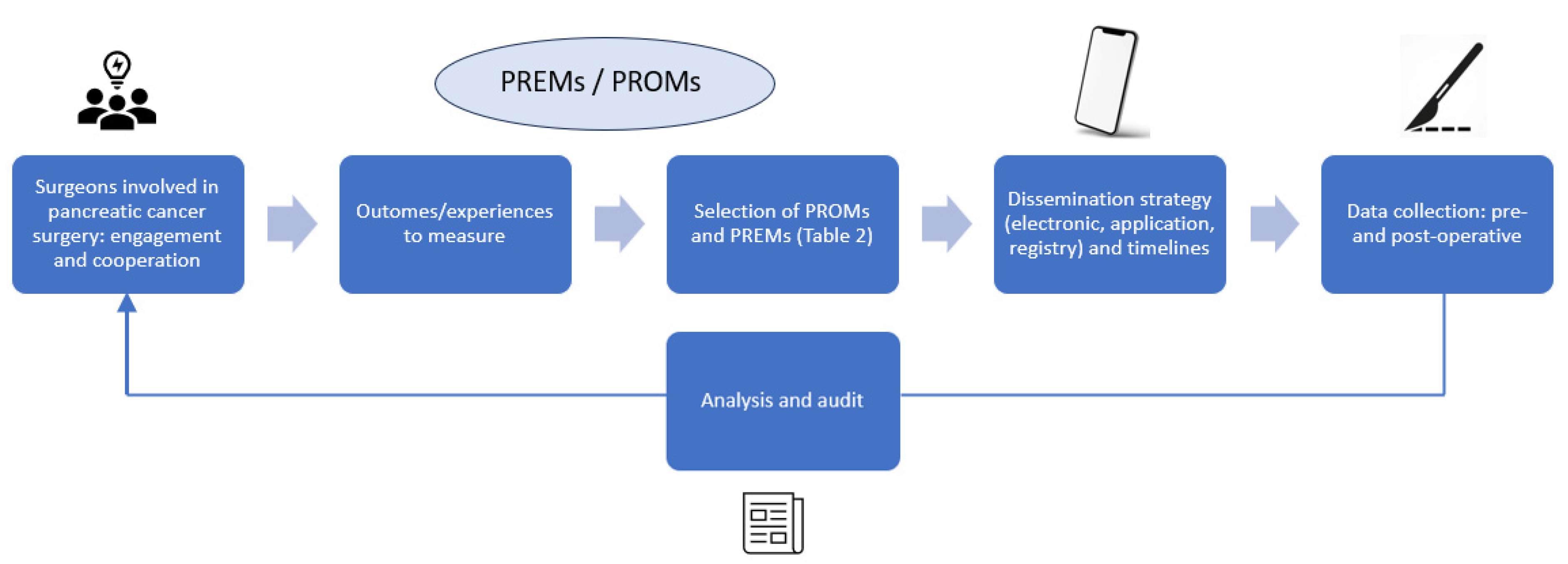
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Martin-Perez, E.; Domínguez-Muñoz, J.E.; Botella-Romero, F.; Cerezo, L.; Matute Teresa, F.; Serrano, T.; Vera, R. Multidisciplinary consensus statement on the clinical management of patients with pancreatic cancer. Clin. Transl. Oncol. 2020, 22, 1963–1975. [Google Scholar] [CrossRef] [PubMed]
- Rahib, L.; Smith, B.D.; Aizenberg, R.; Rosenzweig, A.B.; Fleshman, J.M.; Matrisian, L.M. Projecting cancer incidence and deaths to 2030: The unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 2014, 74, 2913–2921. [Google Scholar] [CrossRef] [PubMed]
- Strobel, O.; Lorenz, P.; Hinz, U.; Gaida, M.; König, A.K.; Hank, T.; Niesen, W.; Kaiser JÖ, R.; Al-Saeedi, M.; Bergmann, F.; et al. Actual Five-year Survival After Upfront Resection for Pancreatic Ductal Adenocarcinoma: Who Beats the Odds? Ann. Surg. 2022, 275, 962–971. [Google Scholar] [CrossRef] [PubMed]
- Ilic, M.; Ilic, I. Epidemiology of pancreatic cancer. World J. Gastroenterol. 2016, 22, 9694–9705. [Google Scholar] [CrossRef]
- Garces-Descovich, A.; Beker, K.; Jaramillo-Cardoso, A.; James Moser, A.; Mortele, K.J. Applicability of current NCCN Guidelines for pancreatic adenocarcinoma resectability: Analysis and pitfalls. Abdom. Radiol. 2018, 43, 314–322. [Google Scholar] [CrossRef]
- Tempero, M.A.; Malafa, M.P.; Al-Hawary, M.; Behrman, S.W.; Benson, A.B.; Cardin, D.B.; Chiorean, E.G.; Chung, V.; Czito, B.; Del Chiaro, M.; et al. Pancreatic Adenocarcinoma, Version 2.2021, NCCN Clinical Practice Guidelines in Oncology. J. Natl. Compr. Cancer Netw. 2021, 19, 439–457. [Google Scholar] [CrossRef]
- Yamamoto, T.; Uchida, Y.; Terajima, H. Clinical impact of margin status on survival and recurrence pattern after curative-intent surgery for pancreatic cancer. Asian J. Surg. 2019, 42, 93–99. [Google Scholar] [CrossRef]
- Molinari, M.; El-Tawil, K.; Swaid, F.; Fiorentini, G.; Bou-Samra, P.; Sharma, C.; Liu, H.; Rahman, S.H.; Hurton, S.; Tsung, A. Patients’ treatment preferences for potentially resectable tumors of the head of the pancreas. HPB 2020, 22, 265–274. [Google Scholar] [CrossRef]
- Gupta, R.; Amanam, I.; Chung, V. Current and future therapies for advanced pancreatic cancer. J. Surg. Oncol. 2017, 116, 25–34. [Google Scholar] [CrossRef]
- Carrato, A.; Falcone, A.; Ducreux, M.; Valle, J.W.; Parnaby, A.; Djazouli, K.; Alnwick-Allu, K.; Hutchings, A.; Palaska, C.; Parthenaki, I. A Systematic Review of the Burden of Pancreatic Cancer in Europe: Real-World Impact on Survival, Quality of Life and Costs. J. Gastrointest. Cancer 2015, 46, 201–211. [Google Scholar] [CrossRef]
- Rajabiyazdi, F.; Alam, R.; Pal, A.; Montanez, J.; Law, S.; Pecorelli, N.; Watanabe, Y.; Chiavegato, L.D.; Falconi, M.; Hirano, S.; et al. Understanding the Meaning of Recovery to Patients Undergoing Abdominal Surgery. JAMA Surg. 2021, 156, 758–765. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine Committee on Quality of Health Care in America. Crossing the Quality Chasm: A New Health System for the 21st Century; National Academies Press (US): Washington, DC, USA, 2001. [Google Scholar]
- van Rijssen, L.B.; Gerritsen, A.; Henselmans, I.; Sprangers, M.A.; Jacobs, M.; Bassi, C.; Busch, O.R.; Fernández-Del Castillo, C.; Fong, Z.V.; He, J.; et al. Core Set of Patient-reported Outcomes in Pancreatic Cancer (COPRAC): An International Delphi Study Among Patients and Health Care Providers. Ann. Surg. 2019, 270, 158–164. [Google Scholar] [CrossRef] [PubMed]
- Basch, E.; Deal, A.M.; Kris, M.G.; Scher, H.I.; Hudis, C.A.; Sabbatini, P.; Rogak, L.; Bennett, A.V.; Dueck, A.C.; Atkinson, T.M.; et al. Symptom Monitoring With Patient-Reported Outcomes During Routine Cancer Treatment: A Randomized Controlled Trial. J. Clin. Oncol. 2016, 34, 557–565. [Google Scholar] [CrossRef]
- Martin, D.; Demartines, N.; Hübner, M. Patient Perspectives in Cancer Surgery. J. Clin. Med. 2022, 11, 789. [Google Scholar] [CrossRef] [PubMed]
- Di Maio, M.; Basch, E.; Denis, F.; Fallowfield, L.J.; Ganz, P.A.; Howell, D.; Kowalski, C.; Perrone, F.; Stover, A.M.; Sundaresan, P.; et al. The role of patient-reported outcome measures in the continuum of cancer clinical care: ESMO Clinical Practice Guideline. Ann. Oncol. 2022, 33, 878–892. [Google Scholar] [CrossRef]
- U.S. Department of Health and Human Services FDA Center for Drug Evaluation and Research; U.S. Department of Health and Human Services FDA Center for Biologics Evaluation and Research; U.S. Department of Health and Human Services FDA Center for Devices and Radiological Health. Guidance for industry: Patient-reported outcome measures: Use in medical product development to support labeling claims: Draft guidance. Health Qual. Life Outcomes 2006, 4, 79. [Google Scholar] [CrossRef]
- Maharaj, A.D.; Samoborec, S.; Evans, S.M.; Zalcberg, J.; Neale, R.E.; Goldstein, D.; Merrett, N.; White, K.; Croagh, D.; Pilgrim, C.H.C.; et al. Patient-reported outcome measures (PROMs) in pancreatic cancer: A systematic review. HPB 2020, 22, 187–203. [Google Scholar] [CrossRef]
- Gerritsen, A.; Jacobs, M.; Henselmans, I.; van Hattum, J.; Efficace, F.; Creemers, G.J.; de Hingh, I.H.; Koopman, M.; Molenaar, I.Q.; Wilmink, H.W.; et al. Developing a core set of patient-reported outcomes in pancreatic cancer: A Delphi survey. Eur. J. Cancer 2016, 57, 68–77. [Google Scholar] [CrossRef]
- Petzel, M.Q.; Parker, N.H.; Valentine, A.D.; Simard, S.; Nogueras-Gonzalez, G.M.; Lee, J.E.; Pisters, P.W.; Vauthey, J.N.; Fleming, J.B.; Katz, M.H. Fear of cancer recurrence after curative pancreatectomy: A cross-sectional study in survivors of pancreatic and periampullary tumors. Ann. Surg. Oncol. 2012, 19, 4078–4084. [Google Scholar] [CrossRef]
- Alam, R.; Montanez, J.; Law, S.; Lee, L.; Pecorelli, N.; Watanabe, Y.; Chiavegato, L.D.; Falconi, M.; Hirano, S.; Mayo, N.E.; et al. Development of a conceptual framework of recovery after abdominal surgery. Surg. Endosc. 2020, 34, 2665–2674. [Google Scholar] [CrossRef]
- Heiberg, T.; Baekelandt, B.; Kvien, T.K.; Buanes, T. Psychometric performance of the Pancreatic Cancer disease impact (PACADI) score. Pancreatology 2019, 19, 971–978. [Google Scholar] [CrossRef]
- Fitzsimmons, D.; Johnson, C.D.; George, S.; Payne, S.; Sandberg, A.A.; Bassi, C.; Beger, H.G.; Birk, D.; Büchler, M.W.; Dervenis, C.; et al. Development of a disease specific quality of life (QoL) questionnaire module to supplement the EORTC core cancer QoL questionnaire, the QLQ-C30 in patients with pancreatic cancer. EORTC Study Group on Quality of Life. Eur. J. Cancer 1999, 35, 939–941. [Google Scholar] [CrossRef] [PubMed]
- Eaton, A.A.; Karanicolas, P.; McHir, J.; Bottomley, A.; Allen, P.J.; Gonen, M. Psychometric validation of the EORTC QLQ-PAN26 pancreatic cancer module for assessing health related quality of life after pancreatic resection. JOP J. Pancreas 2017, 18, 19–25. [Google Scholar]
- Heiberg, T.; Nordby, T.; Kvien, T.K.; Buanes, T. Development and preliminary validation of the pancreatic cancer disease impact score. Support. Care Cancer 2013, 21, 1677–1684. [Google Scholar] [CrossRef] [PubMed]
- Yount, S.; Cella, D.; Webster, K.; Heffernan, N.; Chang, C.; Odom, L.; van Gool, R. Assessment of patient-reported clinical outcome in pancreatic and other hepatobiliary cancers: The FACT Hepatobiliary Symptom Index. J. Pain. Symptom Manag. 2002, 24, 32–44. [Google Scholar] [CrossRef] [PubMed]
- Heffernan, N.; Cella, D.; Webster, K.; Odom, L.; Martone, M.; Passik, S.; Bookbinder, M.; Fong, Y.; Jarnagin, W.; Blumgart, L. Measuring health-related quality of life in patients with hepatobiliary cancers: The functional assessment of cancer therapy-hepatobiliary questionnaire. J. Clin. Oncol. 2002, 20, 2229–2239. [Google Scholar] [CrossRef]
- Cella, D.; Butt, Z.; Kindler, H.L.; Fuchs, C.S.; Bray, S.; Barlev, A.; Oglesby, A. Validity of the FACT Hepatobiliary (FACT-Hep) questionnaire for assessing disease-related symptoms and health-related quality of life in patients with metastatic pancreatic cancer. Qual. Life Res. 2013, 22, 1105–1112. [Google Scholar] [CrossRef]
- Wang, X.S.; Williams, L.A.; Eng, C.; Mendoza, T.R.; Shah, N.A.; Kirkendoll, K.J.; Shah, P.K.; Trask, P.C.; Palos, G.R.; Cleeland, C.S. Validation and application of a module of the M. D. Anderson Symptom Inventory for measuring multiple symptoms in patients with gastrointestinal cancer (the MDASI-GI). Cancer 2010, 116, 2053–2063. [Google Scholar] [CrossRef]
- McLeod, R.S.; Taylor, B.R.; O’Connor, B.I.; Greenberg, G.R.; Jeejeebhoy, K.N.; Royall, D.; Langer, B. Quality of life, nutritional status, and gastrointestinal hormone profile following the Whipple procedure. Am. J. Surg. 1995, 169, 179–185. [Google Scholar] [CrossRef]
- Ong, H.S.; Ng, E.H.; Heng, G.; Soo, K.C. Pancreaticoduodenectomy with pancreaticogastrostomy: Assessment of patients’ nutritional status, quality of life and pancreatic exocrine function. Aust. N. Z. J. Surg. 2000, 70, 199–203. [Google Scholar] [CrossRef]
- Lelond, S.; Ward, J.; Lambert, P.J.; Kim, C.A. Symptom Burden of Patients with Advanced Pancreas Cancer (APC): A Provincial Cancer Institute Observational Study. Curr. Oncol. 2021, 28, 2789–2800. [Google Scholar] [CrossRef] [PubMed]
- Tung, S.; Davis, L.E.; Hallet, J.; Mavros, M.N.; Mahar, A.L.; Bubis, L.D.; Hammad, A.; Zhao, H.; Earle, C.C.; Barbera, L.; et al. Population-Level Symptom Assessment Following Pancreaticoduodenectomy for Adenocarcinoma. JAMA Surg. 2019, 154, e193348. [Google Scholar] [CrossRef] [PubMed]
- Johnston, M.; Pollard, B.; Hennessey, P. Construct validation of the hospital anxiety and depression scale with clinical populations. J. Psychosom. Res. 2000, 48, 579–584. [Google Scholar] [CrossRef] [PubMed]
- Angelino, A.F.; Treisman, G.J. Major depression and demoralization in cancer patients: Diagnostic and treatment considerations. Support. Care Cancer 2001, 9, 344–349. [Google Scholar] [CrossRef] [PubMed]
- Zigmond, A.S.; Snaith, R.P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 1983, 67, 361–370. [Google Scholar] [CrossRef]
- Mayr, M.; Schmid, R.M. Pancreatic cancer and depression: Myth and truth. BMC Cancer 2010, 10, 569. [Google Scholar] [CrossRef]
- Osborne, R.H.; Elsworth, G.R.; Sprangers, M.A.; Oort, F.J.; Hopper, J.L. The value of the Hospital Anxiety and Depression Scale (HADS) for comparing women with early onset breast cancer with population-based reference women. Qual. Life Res. 2004, 13, 191–206. [Google Scholar] [CrossRef]
- Liu, P.; Wang, Z. Postoperative anxiety and depression in surgical gastric cancer patients: Their longitudinal change, risk factors, and correlation with survival. Medicine 2022, 101, e28765. [Google Scholar] [CrossRef]
- Janda, M.; Neale, R.E.; Klein, K.; O’Connell, D.L.; Gooden, H.; Goldstein, D.; Merrett, N.D.; Wyld, D.K.; Rowlands, I.J.; Beesley, V.L. Anxiety, depression and quality of life in people with pancreatic cancer and their carers. Pancreatology 2017, 17, 321–327. [Google Scholar] [CrossRef]
- Krajewski, W.; Mazur, M.; Poterek, A.; Pastuszak, A.; Halska, U.; Tukiendorf, A.; Rymaszewska, J.; Zdrojowy, R. Assessment of Pain Management, Acceptance of Illness, and Adjustment to Life with Cancer in Patients with Nonmuscle Invasive Bladder Cancer. Biomed. Res. Int. 2018, 2018, 7598632. [Google Scholar] [CrossRef]
- Czerw, A.; Religioni, U.; Banaś, T. Perception of cancer in patients diagnosed with the most common gastrointestinal cancers. BMC Palliat. Care 2020, 19, 144. [Google Scholar] [CrossRef]
- Katz, S.; Downs, T.D.; Cash, H.R.; Grotz, R.C. Progress in development of the index of ADL. Gerontologist 1970, 10, 20–30. [Google Scholar] [CrossRef] [PubMed]
- Ivanova, J.I.; Mytelka, D.S.; Duh, M.S.; Birnbaum, H.G.; Cummings, A.K.; San Roman, A.M.; Price, G.L.; Swindle, R.W. Evaluating the utility of existing patient-reported outcome scales in novel patient populations with pancreatic cancer, lung cancer, and myeloproliferative neoplasms using medicare current beneficiary survey data. Patient 2013, 6, 189–200. [Google Scholar] [CrossRef] [PubMed]
- Fiore, J.F., Jr.; Figueiredo, S.; Balvardi, S.; Lee, L.; Nauche, B.; Landry, T.; Mayo, N.E.; Feldman, L.S. How Do We Value Postoperative Recovery?: A Systematic Review of the Measurement Properties of Patient-reported Outcomes After Abdominal Surgery. Ann. Surg. 2018, 267, 656–669. [Google Scholar] [CrossRef] [PubMed]
- Miller, A.M.; Ashing, K.T.; Modeste, N.N.; Herring, R.P.; Sealy, D.A. Contextual factors influencing health-related quality of life in African American and Latina breast cancer survivors. J. Cancer Surviv. 2015, 9, 441–449. [Google Scholar] [CrossRef]
- Gupta, A.; Khalid, O.; Moravek, C.; Lamkin, A.; Matrisian, L.M.; Doss, S.; Denlinger, C.S.; Coveler, A.L.; Weekes, C.D.; Roeland, E.J.; et al. Leveraging patient-reported outcomes (PROs) in patients with pancreatic cancer: The Pancreatic Cancer Action Network (PanCAN) online patient registry experience. Cancer Med. 2021, 10, 7152–7161. [Google Scholar] [CrossRef]
- Rudolph, C.; Petersen, G.S.; Pritzkuleit, R.; Storm, H.; Katalinic, A. The acceptance and applicability of a patient-reported experience measurement tool in oncological care: A descriptive feasibility study in northern Germany. BMC Health Serv. Res. 2019, 19, 786. [Google Scholar] [CrossRef]
- Moens, K.; Peeters, M.; Van den Bulcke, M.; Leys, M.; Horlait, M. Development, Testing, and Implementation of the Belgian Patient Reported Experience Measure for Pancreatic Cancer Care (PREPARE) Project: Protocol for a Multi-Method Research Project. JMIR Res. Protoc. 2022, 11, e29004. [Google Scholar] [CrossRef]
- Anhang Price, R.; Elliott, M.N.; Zaslavsky, A.M.; Hays, R.D.; Lehrman, W.G.; Rybowski, L.; Edgman-Levitan, S.; Cleary, P.D. Examining the role of patient experience surveys in measuring health care quality. Med. Care Res. Rev. 2014, 71, 522–554. [Google Scholar] [CrossRef]
- Manary, M.P.; Boulding, W.; Staelin, R.; Glickman, S.W. The patient experience and health outcomes. N. Engl. J. Med. 2013, 368, 201–203. [Google Scholar] [CrossRef]
- Bull, C.; Byrnes, J.; Hettiarachchi, R.; Downes, M. A systematic review of the validity and reliability of patient-reported experience measures. Health Serv. Res. 2019, 54, 1023–1035. [Google Scholar] [CrossRef] [PubMed]
- Saunders, C.; Carter, D.J.; Jordan, A.; Duffield, C.; Bichel-Findlay, J. Cancer patient experience measures: An evidence review. J. Psychosoc. Oncol. 2016, 34, 200–222. [Google Scholar] [CrossRef] [PubMed]
- Petersen, G.S.; Knudsen, J.L.; Vinter, M.M. Cancer patients’ preferences of care within hospitals: A systematic literature review. Int. J. Qual. Health Care 2015, 27, 384–395. [Google Scholar] [CrossRef]
- Watson, E.K.; Brett, J.; Hay, H.; Witwicki, C.; Perris, A.; Poots, A.J.; Sizmur, S.; Soonawalla, Z.; Tallett, A. Experiences and supportive care needs of UK patients with pancreatic cancer: A cross-sectional questionnaire survey. BMJ Open 2019, 9, e032681. [Google Scholar] [CrossRef] [PubMed]
- Jenkinson, C.; Coulter, A.; Bruster, S. The Picker Patient Experience Questionnaire: Development and validation using data from in-patient surveys in five countries. Int. J. Qual. Health Care 2002, 14, 353–358. [Google Scholar] [CrossRef]
- Brédart, A.; Bottomley, A.; Blazeby, J.M.; Conroy, T.; Coens, C.; D’Haese, S.; Chie, W.C.; Hammerlid, E.; Arraras, J.I.; Efficace, F.; et al. An international prospective study of the EORTC cancer in-patient satisfaction with care measure (EORTC IN-PATSAT32). Eur. J. Cancer 2005, 41, 2120–2131. [Google Scholar] [CrossRef]
- Mackay, T.M.; van Rijssen, L.B.; Andriessen, J.O.; Suker, M.; Creemers, G.J.; Eskens, F.A.; de Hingh, I.H.; van de Poll-Franse, L.V.; Sprangers, M.A.G.; Busch, O.R.; et al. Patient Satisfaction and Quality of Life Before and After Treatment of Pancreatic and Periampullary Cancer: A Prospective Multicenter Study. J. Natl. Compr. Cancer Netw. 2020, 18, 704–711. [Google Scholar] [CrossRef]
- Skudal, K.E.; Garratt, A.M.; Eriksson, B.; Leinonen, T.; Simonsen, J.; Bjertnaes, O.A. The Nordic Patient Experiences Questionnaire (NORPEQ): Cross-national comparison of data quality, internal consistency and validity in four Nordic countries. BMJ Open 2012, 2, e000864. [Google Scholar] [CrossRef]
- Oltedal, S.; Garratt, A.; Bjertnaes, Ø.; Bjørnsdottìr, M.; Freil, M.; Sachs, M. The NORPEQ patient experiences questionnaire: Data quality, internal consistency and validity following a Norwegian inpatient survey. Scand. J. Public. Health 2007, 35, 540–547. [Google Scholar] [CrossRef]
- Steine, S.; Finset, A.; Laerum, E. A new, brief questionnaire (PEQ) developed in primary health care for measuring patients’ experience of interaction, emotion and consultation outcome. Fam. Pract. 2001, 18, 410–418. [Google Scholar] [CrossRef]
- Felton, B.J.; Revenson, T.A.; Hinrichsen, G.A. Stress and coping in the explanation of psychological adjustment among chronically ill adults. Soc. Sci. Med. 1984, 18, 889–898. [Google Scholar] [CrossRef] [PubMed]
- Bruera, E.; Kuehn, N.; Miller, M.J.; Selmser, P.; Macmillan, K. The Edmonton Symptom Assessment System (ESAS): A simple method for the assessment of palliative care patients. J. Palliat. Care 1991, 7, 6–9. [Google Scholar] [CrossRef] [PubMed]
- Eypasch, E.; Williams, J.I.; Wood-Dauphinee, S.; Ure, B.M.; Schmülling, C.; Neugebauer, E.; Troidl, H. Gastrointestinal Quality of Life Index: Development, validation and application of a new instrument. Br. J. Surg. 1995, 82, 216–222. [Google Scholar] [CrossRef]
- Cleeland, C.S.; Mendoza, T.R.; Wang, X.S.; Chou, C.; Harle, M.T.; Morrissey, M.; Engstrom, M.C. Assessing symptom distress in cancer patients: The M.D. Anderson Symptom Inventory. Cancer 2000, 89, 1634–1646. [Google Scholar] [CrossRef]
- Warrington, L.; Absolom, K.; Conner, M.; Kellar, I.; Clayton, B.; Ayres, M.; Velikova, G. Electronic Systems for Patients to Report and Manage Side Effects of Cancer Treatment: Systematic Review. J. Med. Internet Res. 2019, 21, e10875. [Google Scholar] [CrossRef] [PubMed]
- Basch, E.; Deal, A.M.; Dueck, A.C.; Scher, H.I.; Kris, M.G.; Hudis, C.; Schrag, D. Overall Survival Results of a Trial Assessing Patient-Reported Outcomes for Symptom Monitoring During Routine Cancer Treatment. JAMA 2017, 318, 197–198. [Google Scholar] [CrossRef]
- Patel, C.K.S. Patient-reported outcome measures and patient-reported experience measures. BJA Educ. 2017, 17, 137–144. [Google Scholar] [CrossRef]
| PROMs | |||||
| Work/Routines | Health/Symptoms | Mental Issues | Independence | Quality of Life | |
|
|
|
|
| |
| Tools | QLQ-PAN26, FACT-HEP | PAN26, PACADI FACT-HEP, ESAS, MDASI-GI | PAN26, PACADI, FACT-HEP, AIS, MDASI-GI, HADS | Katz index | QLQ-PAN26 |
| PREMs | |||||
| Professional Standards | Diagnosis/Information | Organization | Decisions | Support | |
|
|
|
|
| |
| Tools | PPE, IN-PATSAT32, interviews | PPE, IN-PATSAT32, patient portals, social media | PPE, IN-PATSAT32, mobile applications | Interviews | PPE, mobile applications, patient portals |
| Study/Year | Year | Instrument | Items | Scope | Validation Cohort | |
|---|---|---|---|---|---|---|
| PROMs | Katz et al. [43] | 1970 | Katz index | 8 | Daily activities: bathing, dressing, toileting, transferring, continence, feeding | All stages of PC [44] |
| Zigmond et al. [36] | 1983 | HADS | 14 | Anxiety and depression | All stages of PC [40] | |
| Felton et al. [62] | 1984 | AIS | 8 | Disease acceptance | All stages of PC [42] | |
| Bruera et al. [63] | 1991 | ESAS | 10 | Pain, tiredness, nausea, depression, anxiety, drowsiness, appetite, well-being, shortness of breath | Resectable PC [33] | |
| Fitzsimmons et al. [23] | 1997 | QLQ-PAN26 | 26 | Functional, physical, emotional, social, cognitive | Resectable PC [24] | |
| Eypasch et al. [64] | 1995 | GIQLI | 36 | Physical, emotional, social, symptoms | Resectable PC [30,31] | |
| Cleeland et al. [65] | 2000 | MDASI-GI | 24 | Physical/psychological symptoms | All stages of PC [29] | |
| Yount et al. [26] | 2002 | FACT-HEP | 45 | Quality of life, symptoms and function | Unresectable PC [28] | |
| Heiberg et al. [25] | 2013 | PACADI | 8 | Pain/discomfort, fatigue, anxiety, digestive problems, loss of appetite, dry mouth, itchiness, nausea | All stages of PC [22] | |
| PREMS | Steine et al. [61] | 2001 | PEQ | 18 | Communication, emotions, outcome, barriers, relations with staff | Not specifically for PC [61] |
| Jenkinson et al. [56] | 2002 | PPE | 15 | Information/education, coordination of care, physical comfort, emotional support, respect for patient preferences, involvement of family/friends, continuity and transition, overall impression | Not specifically for PC [56] | |
| Brédart et al. [57] | 2005 | IN-PATSAT32 | 32 | Satisfaction with doctors, nurses, services, care organization. Covers various aspects: communication, coordination of care, quality of medical treatment, physical comfort | All stages of PC [58] | |
| Oltedal et al. [60] | 2007 | NORPEQ | 8 | Doctors/nursing staff understanding, competence, interest, information delivered on tests/examinations, care satisfaction, relevance of treatment | Not specifically for PC [59] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martin, D.; Alberti, P.; Wigmore, S.J.; Demartines, N.; Joliat, G.-R. Pancreatic Cancer Surgery: What Matters to Patients? J. Clin. Med. 2023, 12, 4611. https://doi.org/10.3390/jcm12144611
Martin D, Alberti P, Wigmore SJ, Demartines N, Joliat G-R. Pancreatic Cancer Surgery: What Matters to Patients? Journal of Clinical Medicine. 2023; 12(14):4611. https://doi.org/10.3390/jcm12144611
Chicago/Turabian StyleMartin, David, Piero Alberti, Stephen J. Wigmore, Nicolas Demartines, and Gaëtan-Romain Joliat. 2023. "Pancreatic Cancer Surgery: What Matters to Patients?" Journal of Clinical Medicine 12, no. 14: 4611. https://doi.org/10.3390/jcm12144611
APA StyleMartin, D., Alberti, P., Wigmore, S. J., Demartines, N., & Joliat, G.-R. (2023). Pancreatic Cancer Surgery: What Matters to Patients? Journal of Clinical Medicine, 12(14), 4611. https://doi.org/10.3390/jcm12144611








