Evaluation of Noise Level in Intensive Care Units of Hospitals and Noise Mitigation Strategies, Case Study: Democratic Republic of Congo
Abstract
1. Introduction
- This study assesses noise in ICUs of hospitals in the DRC, a typical developing tropical country.
- Mixed methods were used to assess the exposure to noise levels and noise equivalent levels, correlating the findings while considering the potential influences of outdoor noise sources for two ICUs in residential and industrial zones in DRC.
- The study offers findings that may improve stakeholder knowledge in hospital building design and siting.
- Noise mitigation measures and recommendations for the abatement of noise are proposed.
- Furthermore, the study contributes to scientific data on noise assessment for DTC, which can be helpful for IEQ regulations in the covered geographical region.
2. Materials and Methods
Location Description
3. Methods
3.1. Perceptive Data on the Indoor Acoustic Environment
Survey Questionnaires
- Do you have any problems with the noise created inside the ICU?
- What proportion of noise generated inside the ward is staff-generated?
- Which is the most intrusive noise inside the ICU from the list below?
- Do you have any problems with outside noise entering the ICU room (this includes noise from adjacent rooms)?
- Which is the most intrusive noise from outside?
3.2. Physical Noise Measurements
- p(t) as the instantaneous value of the sound pressure
- P0 as the reference pressure equal to the audibility threshold (2 × 10−5 Pa)
- t as the integration time
3.3. Statistical Methods
4. Results
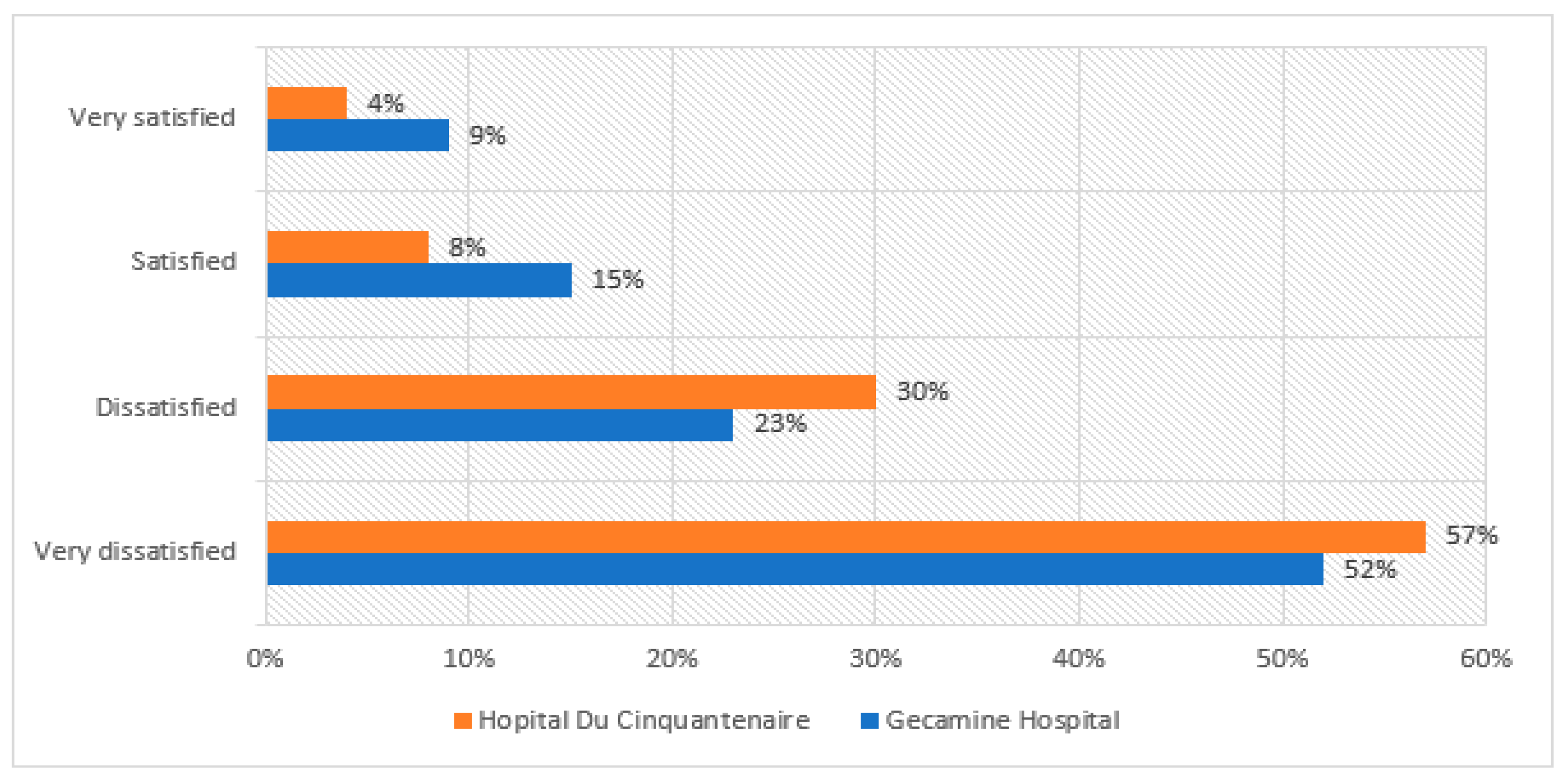
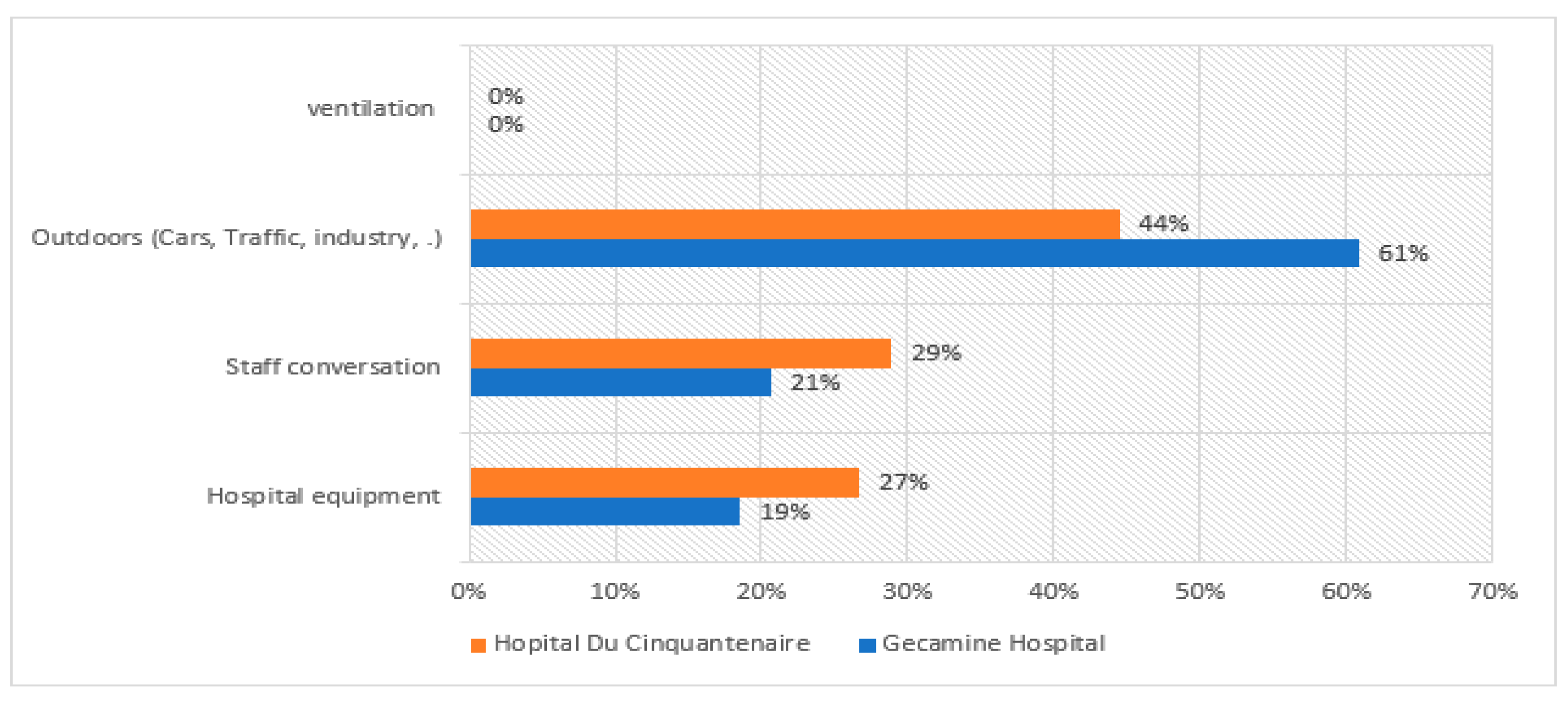
4.1. Perceptive Data Results
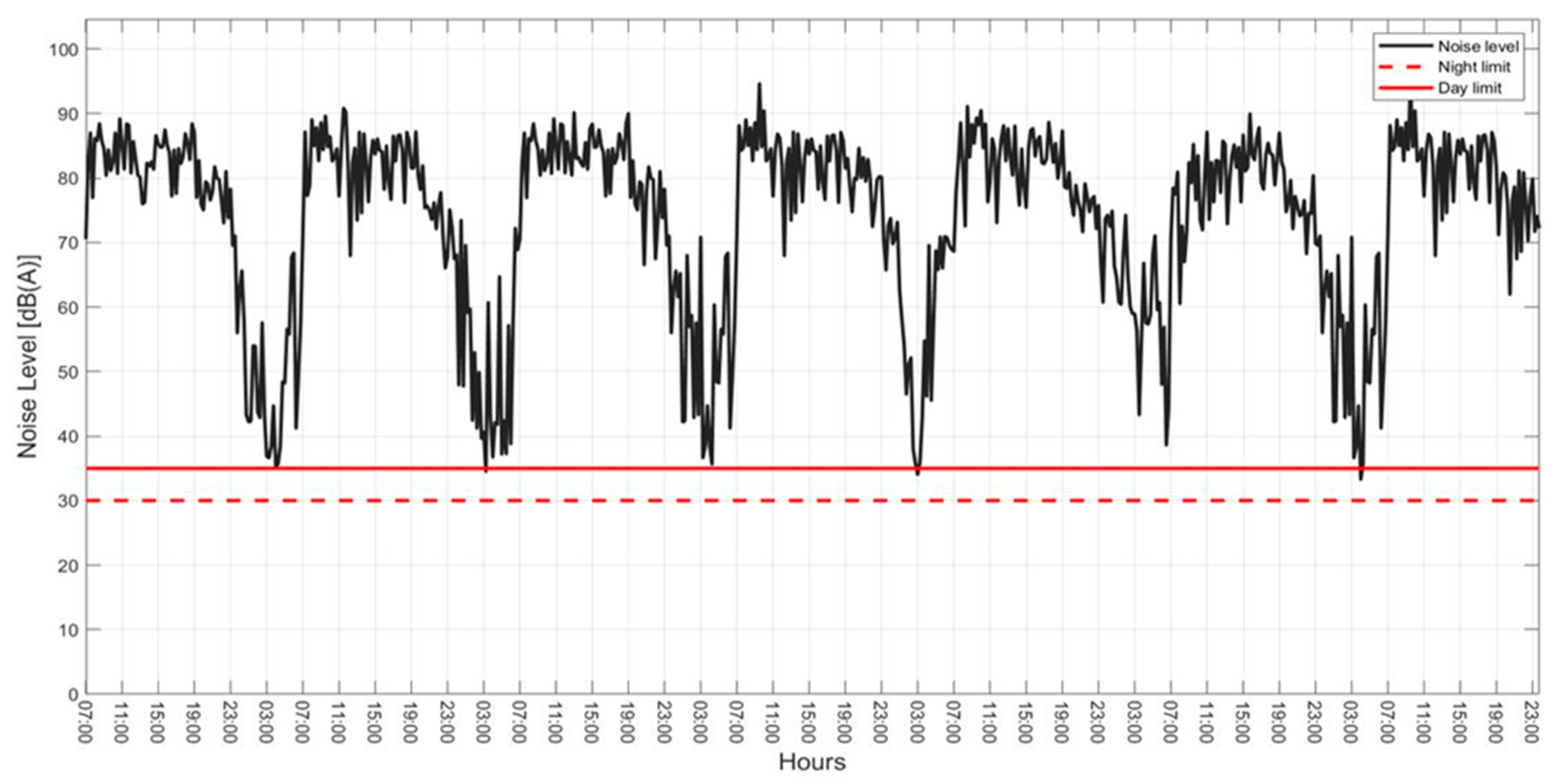
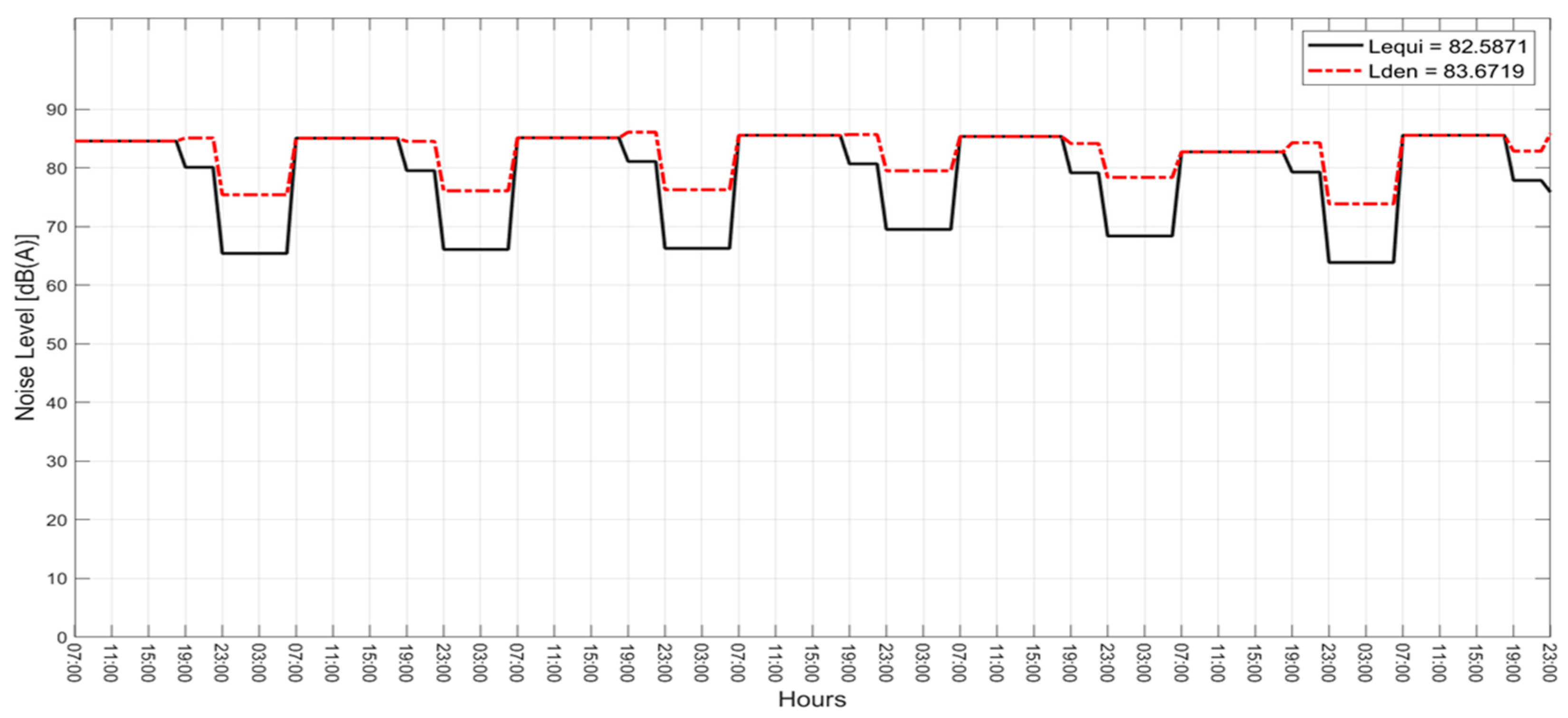
4.2. Results of Physical Measurements
5. Discussion
5.1. Proposed Noise Mitigation Strategies for the Studied Hospitals
- Noise abatement and control measures at the noise sources
- The immediate outdoor and building facade measures
- The indoor or internal mitigation measures
5.2. Noise Abatement and Control Measures at the Noise Sources
- Installing primary barriers beside the road with a possibility of reducing up to 5 to 15 dBA [47] of generated noise from road traffic and the industries flanking the dividing road between hospitals and industry. Planting trees and other plants to ensure an absorptive vegetable cover near these roads can also help in noise mitigation.
- There is a need to manage the ambient traffic by regulating the vehicle speeds on the nearby roads, since an increase in vehicle speed (higher levels of engine noise and noise from tires) can increase the vehicle noise. A speed limit not exceeding 30–40 km/h is recommended. Given that there are industries in proximity to these ICUs, it is understandable to consider the tendency of traffic from a significant number of heavy trucks and vehicle traffic, hence a good to introduce speed limits and changes to road design, like an acoustic improvement to the road surfaces that are near the ICUs and industry.
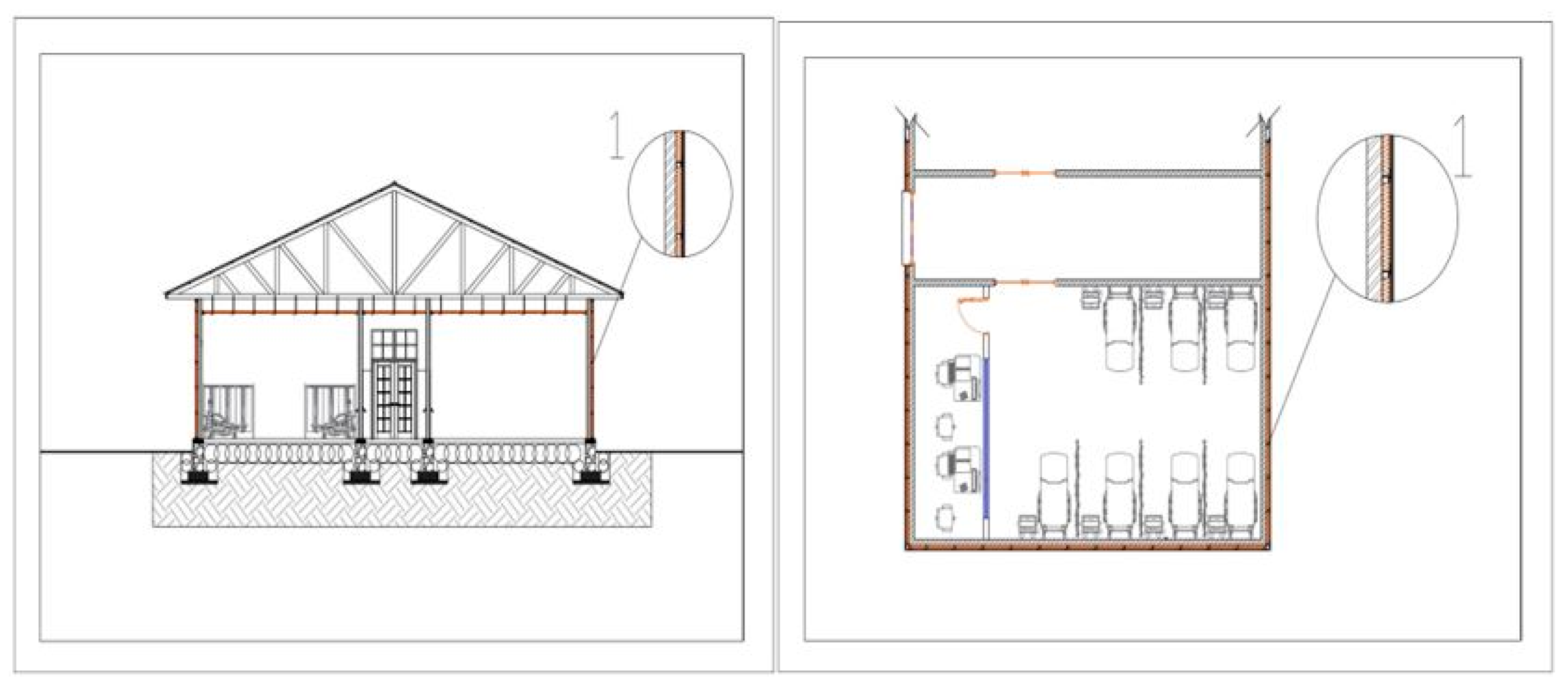
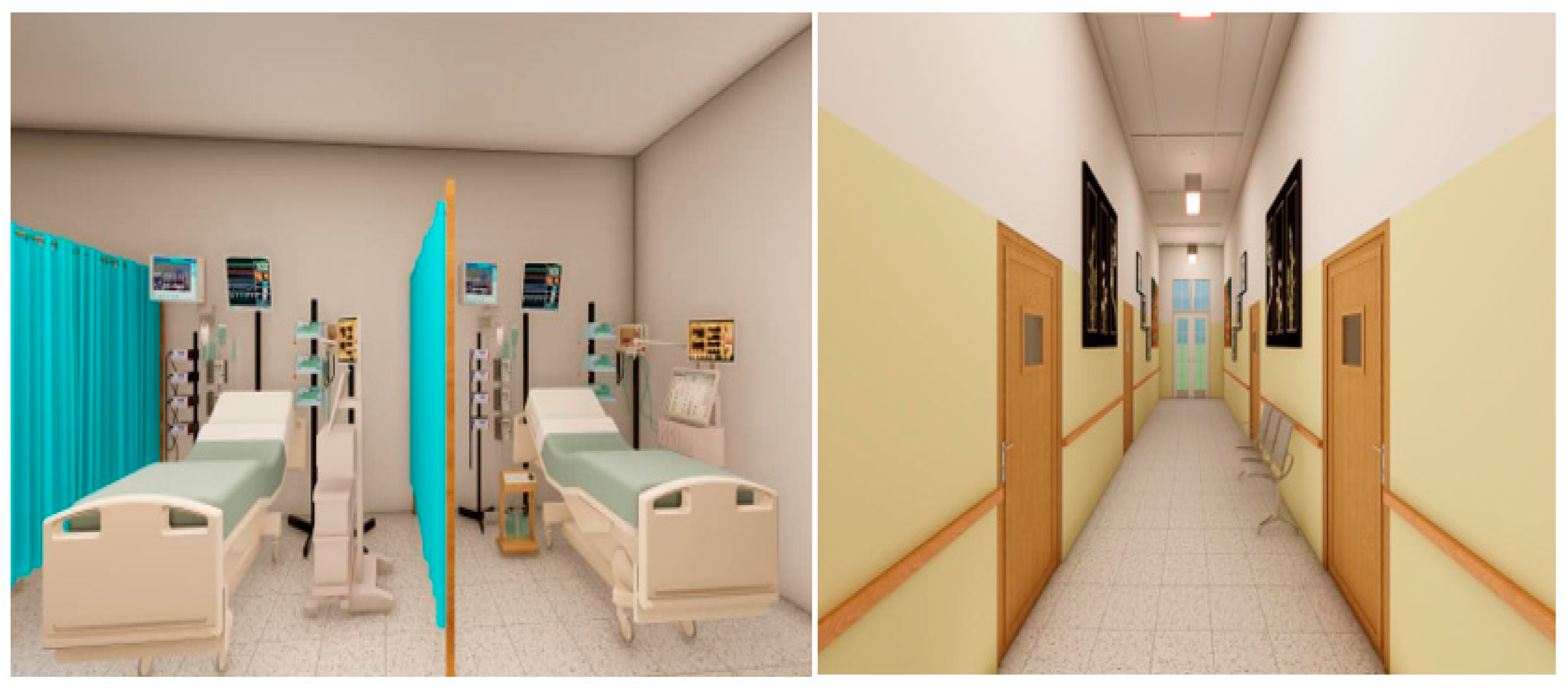
5.3. Immediate Outdoor and Building Facade Measures
5.4. The Indoor or Internal Mitigation Measures
5.5. Limitations of the Study
- This study has not distinguished the specific impact of each identifiable contributing noise source.
- A more robust evaluation of noise parameters and impact may be done in future works, as during this survey, the IEQ questionnaire was used to evaluate other IEQ parameters, and noise data were extracted from a wider group.
- A future study for this region would pay attention to the categorized impact of noise on the healthcare workers and hospital occupants concerning annoyance/irritations, short- and long-term health effects vis-à-vis the challenges associated with occupational exposure hours, stress, and performance variables.
- A control experiment to evaluate the effects of ambient noise between two groups of healthcare workers may be more revealing of the impact, although the current study has confirmed the presence of high noise levels beyond the WHO limits (35 dBA).
- In order to adequately evaluate the difference in the acoustic porosity of these ICUs for more adapted mitigation measures, it is recommended that a pre-study noise audit of the hospital buildings and equipment be performed, given that many hospitals in developing tropical countries are somewhat in deficit regarding compliance with global standards, separate from the peculiarities of the tropical climate, environmental, and socio-cultural factors.
6. Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Morrison, W.E.; Haas, E.C.; Shaffner, D.H.; Garrett, E.S.; Fackler, J.C. Noise, stress, and annoyance in a pediatric intensive care unit. Crit. Care Med. 2003, 31, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Bliefnick, J.M.; Ryherd, E.E.; Jackson, R. Evaluating hospital soundscapes to improve patient experience. J. Acoust. Soc. Am. 2019, 145, 1117–1128. [Google Scholar] [CrossRef] [PubMed]
- Delaney, L.J.; Currie, M.J.; Huang, H.-C.C.; Lopez, V.; Litton, E.; Van Haren, F. The nocturnal acoustical intensity of the intensive care environment: An observational study. J. Intensiv. Care 2017, 5, 41. [Google Scholar] [CrossRef]
- Berg, A.L. Monitoring Noise Levels in a Tertiary Neonatal Intensive Care Unit. Contemp. Issues Commun. Sci. Disord. 2010, 37, 69–72. [Google Scholar] [CrossRef]
- Environmental Protection Agency. Information on Levels of Environmental Noise Requisite to Protect; NPC Online Library: Montpelier, VT, USA, 1974; pp. 1–76. [Google Scholar]
- Schwela, D.H. The new World Health Organization guidelines for community noise. Noise Control Eng. J. 2001, 49, 193. [Google Scholar] [CrossRef]
- WHO. On Hand Hygiene in Health Care First Global Patient Safety Challenge Clean Care Is Safer Care. 2009. Available online: https://www.who.int/publications/i/item/9789241597906. (accessed on 1 December 2022).
- Van Reenen, C.A. A case study investigation of the indoor environmental noise in four urban South African hospitals. Proc. Mtgs. Acoust. 2015, 25, 015002. [Google Scholar] [CrossRef]
- Khademi, G.; Imani, B. Noise pollution in intensive care units: A systematic review article. Rev. Clin. Med. 2015, 2, 58–64. [Google Scholar] [CrossRef]
- Bhave, P.; Sayed, K. Noise pollution in sensitive zone and its effects: A review. Int. Adv. Res. J. Sci. Eng. Technol. 2015, 2, 78–83. [Google Scholar] [CrossRef]
- Bayo, M.V.; García, A.M.; Garcia, A. Noise Levels in an Urban Hospital and Workers’ Subjective Responses. Arch. Environ. Health Int. J. 1995, 50, 247–251. [Google Scholar] [CrossRef]
- Cmiel, C.A.; Karr, D.; Gasser, D.; Oliphant, L.; Neveau, A.J. Noise Control: A Nursing Team’s Approach to Sleep Promotion: Respecting the silence creates a healthier environment for your patients. AJN Am. J. Nurs. 2004, 104, 40–48. [Google Scholar] [CrossRef]
- Basner, M.; Babisch, W.; Davis, A.; Brink, M.; Clark, C.; Janssen, S.; Stansfeld, S. Auditory and non-auditory effects of noise on health. Lancet 2013, 383, 1325–1332. [Google Scholar] [CrossRef] [PubMed]
- Hunashal, R.B.; Patil, Y.B. Assessment of Noise Pollution Indices in the City of Kolhapur, India. Procedia-Soc. Behav. Sci. 2012, 37, 448–457. [Google Scholar] [CrossRef]
- Xie, H.; Kang, J.; Mills, G.H. Clinical review: The impact of noise on patients’ sleep and the effectiveness of noise reduction strategies in intensive care units. Crit. Care 2009, 13, 208. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Burden of Disease from Environmental Noise Quantification of Healthy Life Years Lost in Europe. WHO Regional Office for Europe: Copenhagen, Denmark, 2011. [Google Scholar]
- Flynn, E.A.; Barker, K.N.; Gibson, J.T.; Pearson, R.E.; Berger, B.A.; Smith, L.A. Impact of interruptions and distractions on dispensing errors in an ambulatory care pharmacy. Am. J. Health Pharm. 1999, 56, 1319–1325. [Google Scholar] [CrossRef]
- Lawson, S.M.; Masterson, E.A. Hearing Loss Among Health Care and Social Assistance Workers: A NIOSH Study. Hear. J. 2019, 72, 12–13. [Google Scholar] [CrossRef]
- Themann, C.L.; Masterson, E.A. Occupational noise exposure: A review of its effects, epidemiology, and impact with recommendations for reducing its burden. J. Acoust. Soc. Am. 2019, 146, 3879–3905. [Google Scholar] [CrossRef]
- Plack, C.J.; Barker, D.J.P.; Prendergast, G. Perceptual Consequences of “Hidden” Hearing Loss. Trends Hear. 2014, 18, 2331216514550621. [Google Scholar] [CrossRef]
- Ding, M.T.; Yan, A. What is noise-induced hearing loss? Br. J. Hosp. Med. 2019, 80, 525–529. [Google Scholar] [CrossRef]
- Blomkvist, V.; A Eriksen, C.; Theorell, T.; Ulrich, R.; Rasmanis, G. Acoustics and psychosocial environment in intensive coronary care. Occup. Environ. Med. 2005, 62, e1. [Google Scholar] [CrossRef]
- van Hoof, J.; Kort, H.; Duijnstee, M.; Rutten, P.; Hensen, J. The indoor environment and the integrated design of homes for older people with dementia. Build. Environ. 2010, 45, 1244–1261. [Google Scholar] [CrossRef]
- Schmidt, N.; Gerber, S.M.; Zante, B.; Gawliczek, T.; Chesham, A.; Gutbrod, K.; Müri, R.M.; Nef, T.; Schefold, J.C.; Jeitziner, M.-M. Effects of intensive care unit ambient sounds on healthcare professionals: Results of an online survey and noise exposure in an experimental setting. Intensiv. Care Med. Exp. 2020, 8, 34. [Google Scholar] [CrossRef] [PubMed]
- Andrade, E.D.L.; Silva, D.C.D.C.E.; de Lima, E.A.; de Oliveira, R.A.; Zannin, P.H.T.; Martins, A.C.G. Environmental noise in hospitals: A systematic review. Environ. Sci. Pollut. Res. 2021, 28, 19629–19642. [Google Scholar] [CrossRef] [PubMed]
- Khan, J.; Ketzel, M.; Kakosimos, K.; Sørensen, M.; Jensen, S.S. Road traffic air and noise pollution exposure assessment—A review of tools and techniques. Sci. Total. Environ. 2018, 634, 661–676. [Google Scholar] [CrossRef]
- Wallis, R.; Harris, E.; Lee, H.; Davies, W.; Astin, F. Environmental Noise Levels in Hospital Settings: A Rapid Review of Measurement Techniques and Implementation in Hospital Settings. Noise Health 2020, 21, 200–216. [Google Scholar]
- Okokon, E.O.; Taimisto, P.; Turunen, A.W.; Amoda, O.A.; Fasasi, A.E.; Adeyemi, L.G.; Juutilainen, J.; Lanki, T. Particulate air pollution and noise: Assessing commuter exposure in Africa’s most populous city. J. Transp. Health 2018, 9, 150–160. [Google Scholar] [CrossRef]
- Sieber, C.; Ragettli, M.S.; Brink, M.; Olaniyan, T.; Baatjies, R.; Saucy, A.; Vienneau, D.; Probst-Hensch, N.; Dalvie, M.A.; Röösli, M. Comparison of sensitivity and annoyance to road traffic and community noise between a South African and a Swiss population sample. Environ. Pollut. 2018, 241, 1056–1062. [Google Scholar] [CrossRef]
- Banerjee, D.; Chakraborty, S.; Bhattacharyya, S.; Gangopadhyay, A. Evaluation and analysis of road traffic noise in asansol, West Bengal. J. Inst. Eng. Environ. Eng. Div. 2008, 89, 9–16. [Google Scholar]
- Hsu, T.; Ryherd, E.; Waye, K.P.; Ackerman, J. Noise Pollution in Hospitals: Impact on Patients. JCOM 2012, 19, 301–309. [Google Scholar]
- A Alduais, S.; Salama, K.F. Assessment Of Ambient-Noise Exposure Among Female Nurses In Surgical Cardiac Intensive Care Unit. J. Multidiscip. Health 2019, 12, 1007–1011. [Google Scholar] [CrossRef]
- Vanwelde, B.; Calcut, T.; Young, H. Environmental and Social Impact Assessment in Countries with Limited Regulatory Frameworks: Lessons from the Democratic Republic of the Congo. 2013. Available online: www.iaia.org (accessed on 1 December 2022).
- Andreucci, M.B.; Marvuglia, A.; Baltov, M.; Hansen, P. Future City 15 Rethinking Sustainability Towards a Regenerative Economy. Available online: http://www.springer.com/series/8178 (accessed on 1 December 2022).
- Castro, F.L.; Iarossi, S.; Brambilla, G.; Mariconte, R.; Diano, M.; Bruzzaniti, V.; Strigari, L.; Raffaele, G.; Giliberti, C. Surveys on Noise in Some Hospital Wards and Self-Reported Reactions from Staff: A Case Study. Buildings 2022, 12, 2077. [Google Scholar] [CrossRef]
- Juang, D.F.; Lee, C.; Yang, T.; Chang, M.C. A BS T RA C T: Noise pollution and its effects on medical care workers and patients in hospitals. Int. J. Environ. Sci. Technol. 2010, 7, 705–716. [Google Scholar] [CrossRef]
- Wiese, C.H.; Wang, L.M. LV-11-C031: Measured Levels of Hospital Noise before, during, and after Renovation of a Hospital Wing, and a Survey of Resulting Patient Perception. 2011. Available online: https://digitalcommons.unl.edu/archengfacpub/44 (accessed on 1 December 2022).
- Montes-González, D.; Barrigón-Morillas, J.M.; Escobar, V.G.; Vílchez-Gómez, R.; Rey-Gozalo, G.; Atanasio-Moraga, P.; Méndez-Sierra, J.A. Environmental Noise around Hospital Areas: A Case Study. Environments 2019, 6, 41. [Google Scholar] [CrossRef]
- Khaiwal, R.; Singh, T.; Tripathy, J.P.; Mor, S.; Munjal, S.; Patro, B.; Panda, N. Assessment of noise pollution in and around a sensitive zone in North India and its non-auditory impacts. Sci. Total. Environ. 2016, 566–567, 981–987. [Google Scholar] [CrossRef]
- Hsu, S.; Ko, W.; Liao, W.; Huang, S.; Chen, R.J.; Li, C.; Hwang, S. Associations of exposure to noise with physiological and psychological outcomes among post-cardiac surgery patients in ICUs. Clinics 2010, 65, 985–989. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, W.B.; Pedreira, M.L.; Aguiar, M.A. Noise level in a pediatric intensive care unit. J. Pediatr. 2005, 81, 495–498. [Google Scholar] [CrossRef]
- Busch-Vishniac, I.J.; West, J.E.; Barnhill, C.; Hunter, T.; Orellana, D.; Chivukula, R. Noise levels in Johns Hopkins Hospital. J. Acoust. Soc. Am. 2005, 118, 3629–3645. [Google Scholar] [CrossRef]
- Padmakumar, A.D.; Bhasin, V.; Wenham, T.N.; Bodenham, A.R. Evaluation of Noise Levels in Intensive Care Units in Two Large Teaching Hospitals—A Prospective Observational Study. J. Intensiv. Care Soc. 2013, 14, 205–210. [Google Scholar] [CrossRef]
- MacKenzie, D.; Galbrun, L. Noise levels and noise sources in acute care hospital wards. Build. Serv. Eng. Res. Technol. 2007, 28, 117–131. [Google Scholar] [CrossRef]
- Konkani, A.; Oakley, B. Noise in hospital intensive care units—A critical review of a critical topic. J. Crit. Care 2012, 27, 522.e1–522.e9. [Google Scholar] [CrossRef]
- Bolaji, B.O.; Olanipekun, M.U.; Adekunle, A.A.; Adeleke, A.E. An analysis of noise and its environmental burden on the example of Nigerian manufacturing companies. J. Clean. Prod. 2018, 172, 1800–1806. [Google Scholar] [CrossRef]
- Glasson, J.; Therivel, R.; Chadwick, A. Methods of Environmental Impact Assessment, 2nd ed.; The Natural and Built Environment Series; Taylor and Francis: London, UK, 2000. [Google Scholar]
- MacLeod, M.; Dunn, J.; Busch-Vishniac, I.J.; West, J.E.; Reedy, A. Quieting Weinberg 5C: A case study in hospital noise control. J. Acoust. Soc. Am. 2007, 121, 3501–3508. [Google Scholar] [CrossRef] [PubMed]
- Smirnova, O.M.; de Navascués, I.M.P.; Mikhailevskii, V.R.; Kolosov, O.I.; Skolota, N.S. Sound-Absorbing Composites with Rubber Crumb from Used Tires. Appl. Sci. 2021, 11, 7347. [Google Scholar] [CrossRef]
- Peng, L.; Zhao, P.; Cheng, H.; He, Q.; Du, L. Improved low-frequency sound absorption of porous silicone rubber resonance sheet with periodic cavities. J. Low Freq. Noise Vib. Act. Control 2022, 41, 1151–1159. [Google Scholar] [CrossRef]



| GH, Kipushi | CH, Kinshasa | ||||
|---|---|---|---|---|---|
| Division | Category | Counts Ration (%) | Counts Ration (%) | ||
| Gender | Male | 50 | 46 | 43 | 36 |
| Female | 66 | 54 | 78 | 64 | |
| Total | 116 | 100 | 121 | 100 | |
| Age | Less than 30 | 18 | 14 | 15 | 12 |
| 31~40 | 25 | 22 | 39 | 32 | |
| 41~50 | 37 | 33 | 35 | 30 | |
| 51~60 | 29 | 25 | 29 | 24 | |
| Over 60 | 7 | 6 | 3 | 2 | |
| Total | 116 | 100 | 121 | 100 | |
| Occupation | Nurses | 75 | 65 | 83 | 68 |
| Physicians | 27 | 23 | 25 | 21 | |
| Allied health professionals | 14 | 12 | 13 | 11 | |
| Total | 116 | 100 | 121 | 100 | |
| Work experience | <5 years | 17 | 15 | 26 | 22 |
| 6–10 years | 43 | 37 | 42 | 34 | |
| >16 years | 56 | 48 | 53 | 44 | |
| Total | 116 | 100 | 121 | 100 | |
| Source of Variation | SS | df | MS | F | p-Value | F crit |
|---|---|---|---|---|---|---|
| Between Groups | 2.5 | 1 | 2.5 | 0.05 | 0.84 | 5.32 |
| Within Groups | 441.6 | 8 | 55.2 |
| Noise Comfort Parameters | GH | CH | Source of Variation | Ss | Df | Ms | F | p-Value | F Crit |
|---|---|---|---|---|---|---|---|---|---|
| Noise sources | 23 | 31 | Between Groups | 3.132 | 1 | 3.13 | 0.01 | 0.95 | 5.99 |
| 25 | 34 | Within Groups | 4176.75 | 6 | 696.13 | ||||
| 73 | 51 | ||||||||
| 0 | 0 | Total | 4179.86 | 7 | |||||
| Satisfaction | 62 | 66 | Between Groups | 3.13 | 1 | 3.13 | 0.01 | 0.95 | 5.99 |
| 28 | 35 | Within Groups | 3814.75 | 6 | 635.79 | ||||
| 19 | 10 | ||||||||
| 12 | 5 | Total | 3817.88 | 7 |
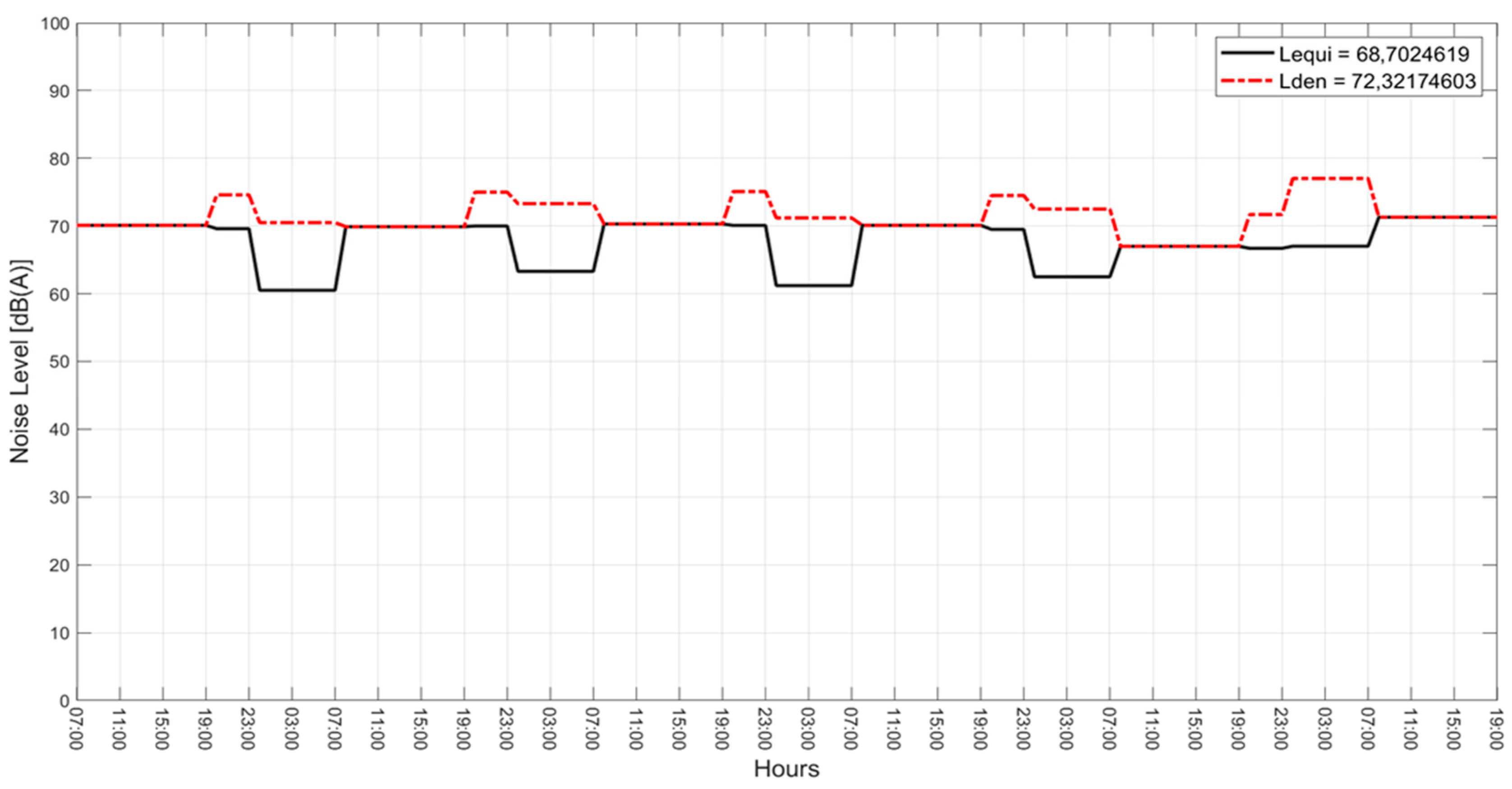
| Statistical Parameters | Lday1 | Levening1 | Lnight1 | Lday2 | Levening2 | Lnight2 | Lday3 | Levening3 | Lnight3 |
|---|---|---|---|---|---|---|---|---|---|
| Mean | 67.7 | 68 | 48.4 | 68.2 | 67 | 49.7 | 69.2 | 68.2 | 51.1 |
| Standard Error | 0.79 | 1.2 | 2.16 | 0.7 | 1.27 | 2.47 | 0.45 | 1.18 | 2.1 |
| Median | 68.6 | 69.4 | 45.9 | 69.4 | 66.7 | 46.9 | 69.45 | 69.3 | 53.6 |
| Mode | 70.4 | 72 | 69.3 | 72.1 | 78.2 | 39.4 | 73.4 | 75 | 68 |
| Standard Deviation | 3.88 | 4.79 | 12.42 | 4.8 | 5.2 | 13.73 | 3.15 | 4.86 | 11.67 |
| Sample Variance | 15.05 | 22.97 | 154.12 | 23.02 | 27 | 188.44 | 9.9 | 23.66 | 136.15 |
| Range | 13.7 | 16.1 | 39 | 22.9 | 21.2 | 42.4 | 13.3 | 17.4 | 37.7 |
| Minimum | 59.7 | 57.6 | 30.3 | 52.9 | 57 | 29.7 | 61.9 | 57.6 | 30.3 |
| Maximum | 73.4 | 73.7 | 69.3 | 75.8 | 78.2 | 72.1 | 75.2 | 75 | 68 |
| Sum | 1624.1 | 1087.3 | 1595.9 | 3209.6 | 1138.2 | 1539 | 3319.7 | 1159.6 | 1583.4 |
| Count | 24 | 16 | 33 | 47 | 17 | 31 | 48 | 17 | 31 |
| Confidence Level (95%) | 1.64 | 2.56 | 4.4 | 1.41 | 2.67 | 5.04 | 0.91 | 2.5 | 4.28 |
| Day | Source of Variation | SS | df | MS | F | p-Value | F Crit |
|---|---|---|---|---|---|---|---|
| Lden1 | Between Groups | 6823.32 | 2 | 3411.6 | 42.47 | 8.35 × 10−13 | 3.13 |
| Within Groups | 5622.65 | 70 | 80.33 | ||||
| Total | 12,445.97 | 72 | |||||
| Lden2 | Between Groups | 7007.97 | 2 | 3503.98 | 45.12 | 2.21 × 10−14 | 3.10 |
| Within Groups | 7144.30 | 92 | 77.66 | ||||
| Total | 14,152.7 | 94 | |||||
| Lden3 | Between Groups | 6687.73 | 2 | 3343.87 | 63.10 | 1.00 × 10−16 | 3.10 |
| Within Groups | 4928.05 | 93 | 52.99 | ||||
| Total | 11,615.78 | 95 |
| ICUs | Days | Leq Day dBA | Leq Evening dBA | Leq Night dBA |
|---|---|---|---|---|
| CH | 1 | 69.1 | 69.6 | 60.5 |
| 2 | 70.1 | 69.9 | 63.2 | |
| 3 | 70.3 | 70.1 | 61.8 | |
| GH | 1 | 72.4 | 71.6 | 64.3 |
| 2 | 70.4 | 68.5 | 65 | |
| 3 | 68 | 68.7 | 62.1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nyembwe, J.-P.K.B.; Ogundiran, J.O.; Gameiro da Silva, M.; Albino Vieira Simões, N. Evaluation of Noise Level in Intensive Care Units of Hospitals and Noise Mitigation Strategies, Case Study: Democratic Republic of Congo. Buildings 2023, 13, 278. https://doi.org/10.3390/buildings13020278
Nyembwe J-PKB, Ogundiran JO, Gameiro da Silva M, Albino Vieira Simões N. Evaluation of Noise Level in Intensive Care Units of Hospitals and Noise Mitigation Strategies, Case Study: Democratic Republic of Congo. Buildings. 2023; 13(2):278. https://doi.org/10.3390/buildings13020278
Chicago/Turabian StyleNyembwe, Jean-Paul Kapuya Bulaba, John Omomoluwa Ogundiran, Manuel Gameiro da Silva, and Nuno Albino Vieira Simões. 2023. "Evaluation of Noise Level in Intensive Care Units of Hospitals and Noise Mitigation Strategies, Case Study: Democratic Republic of Congo" Buildings 13, no. 2: 278. https://doi.org/10.3390/buildings13020278
APA StyleNyembwe, J.-P. K. B., Ogundiran, J. O., Gameiro da Silva, M., & Albino Vieira Simões, N. (2023). Evaluation of Noise Level in Intensive Care Units of Hospitals and Noise Mitigation Strategies, Case Study: Democratic Republic of Congo. Buildings, 13(2), 278. https://doi.org/10.3390/buildings13020278











