The Complexity of the Arterial Blood Pressure Regulation during the Stress Test
Abstract
1. Introduction
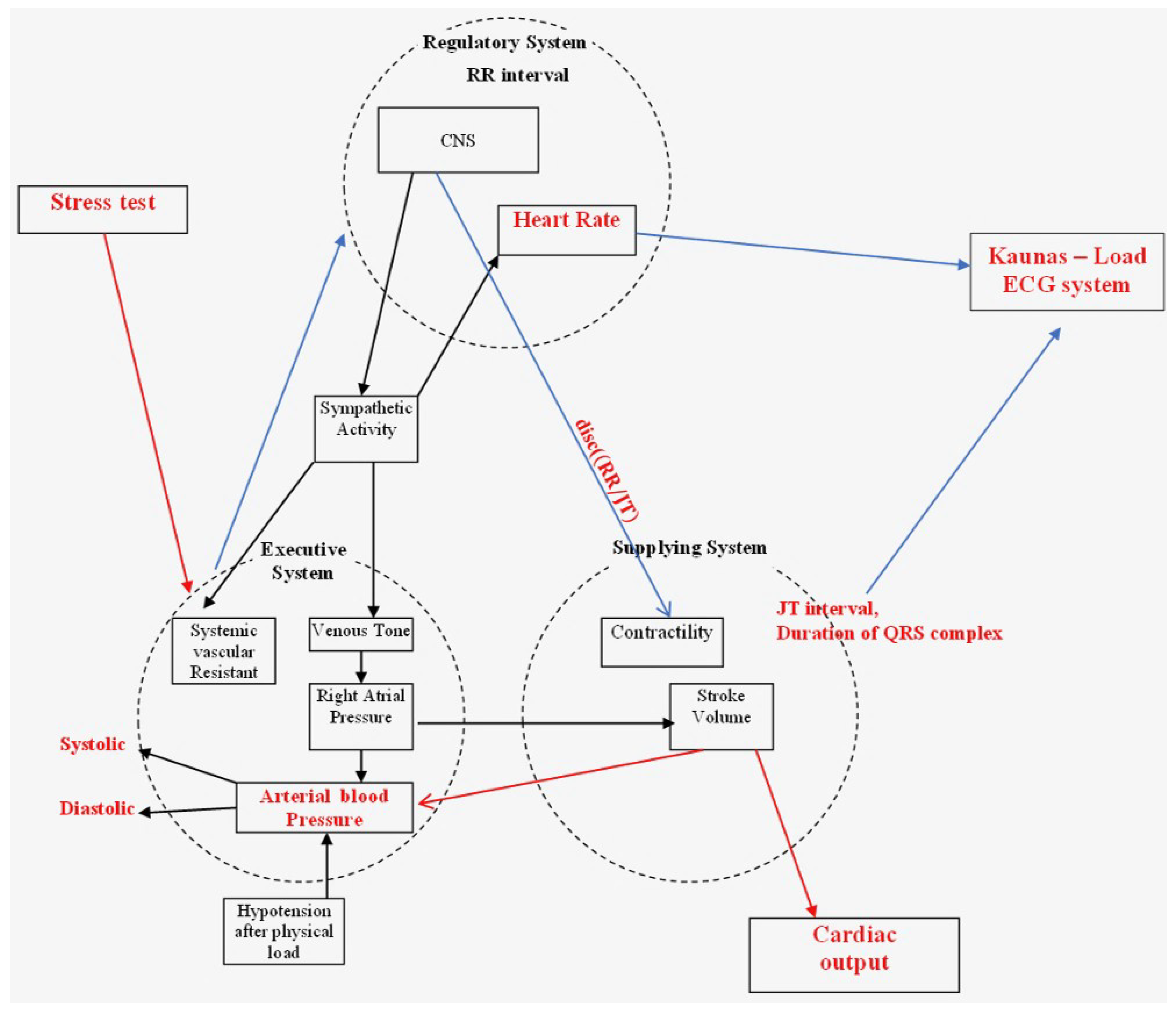
The Model of Integral Evaluation of the Human Cardiovascular System
2. Methods
2.1. The Description of the Experimental Setup
2.2. The Algorithm for the Identification of the RR/JT Algebraic Relationship
2.3. The Structure of Machine Learning Algorithms for the Classification
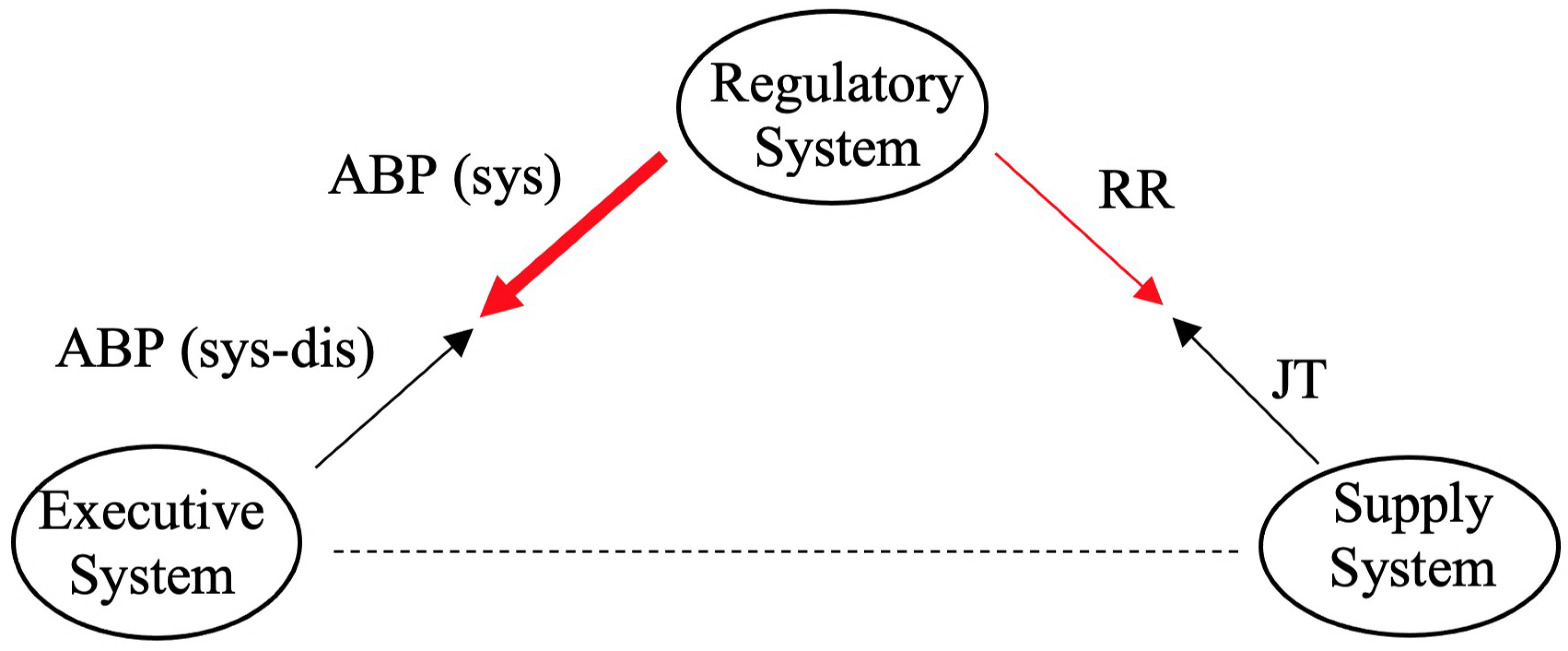
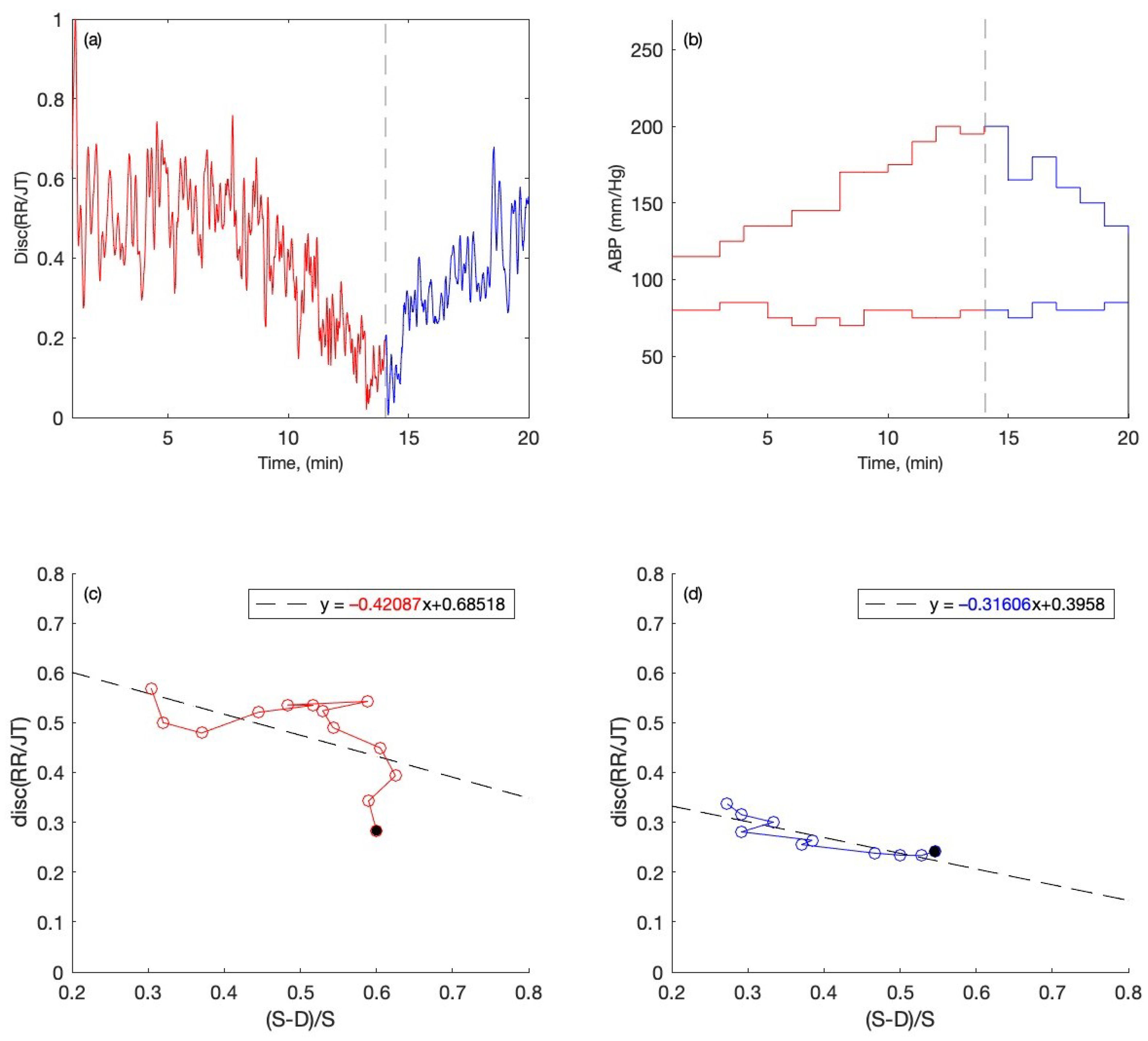
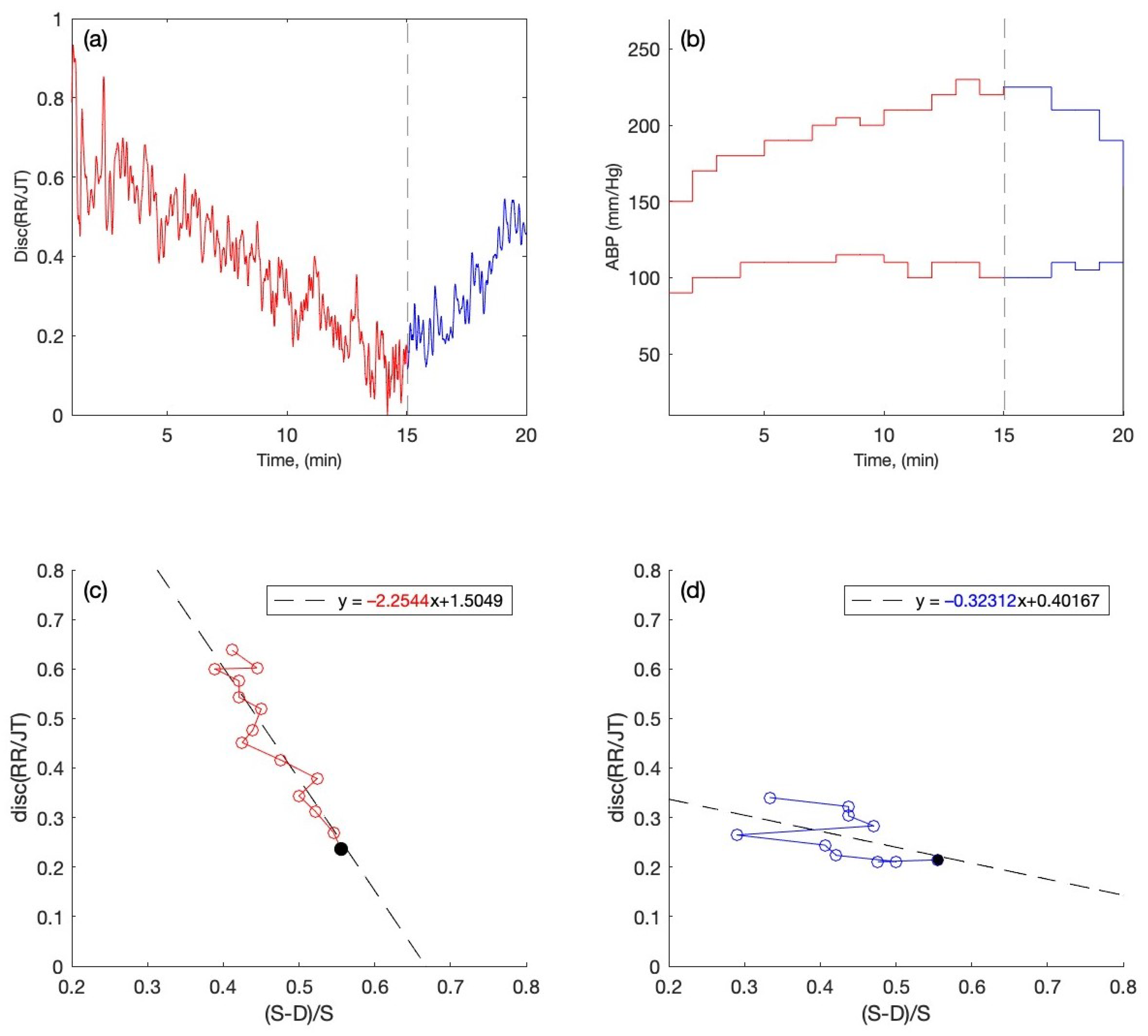
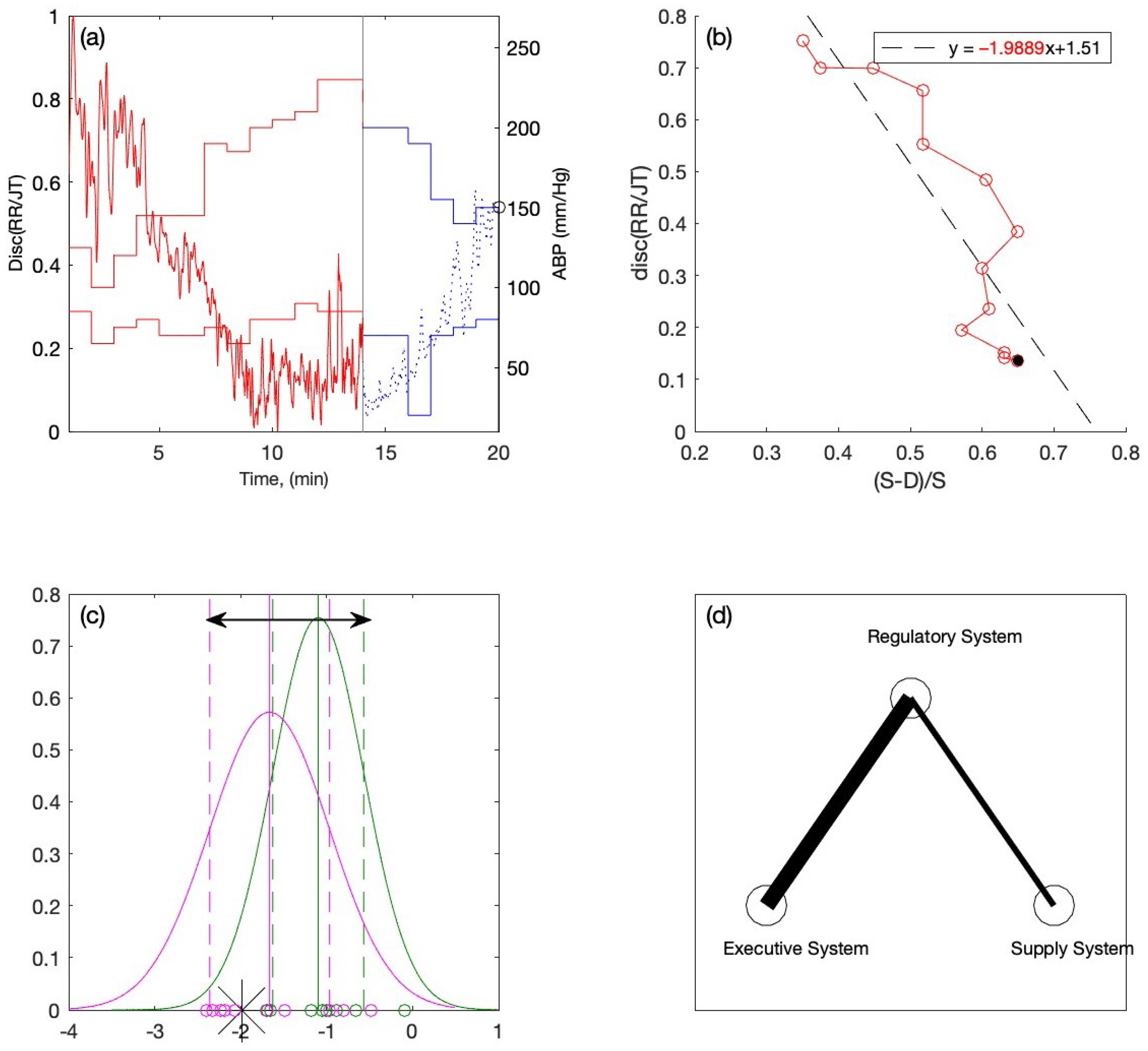
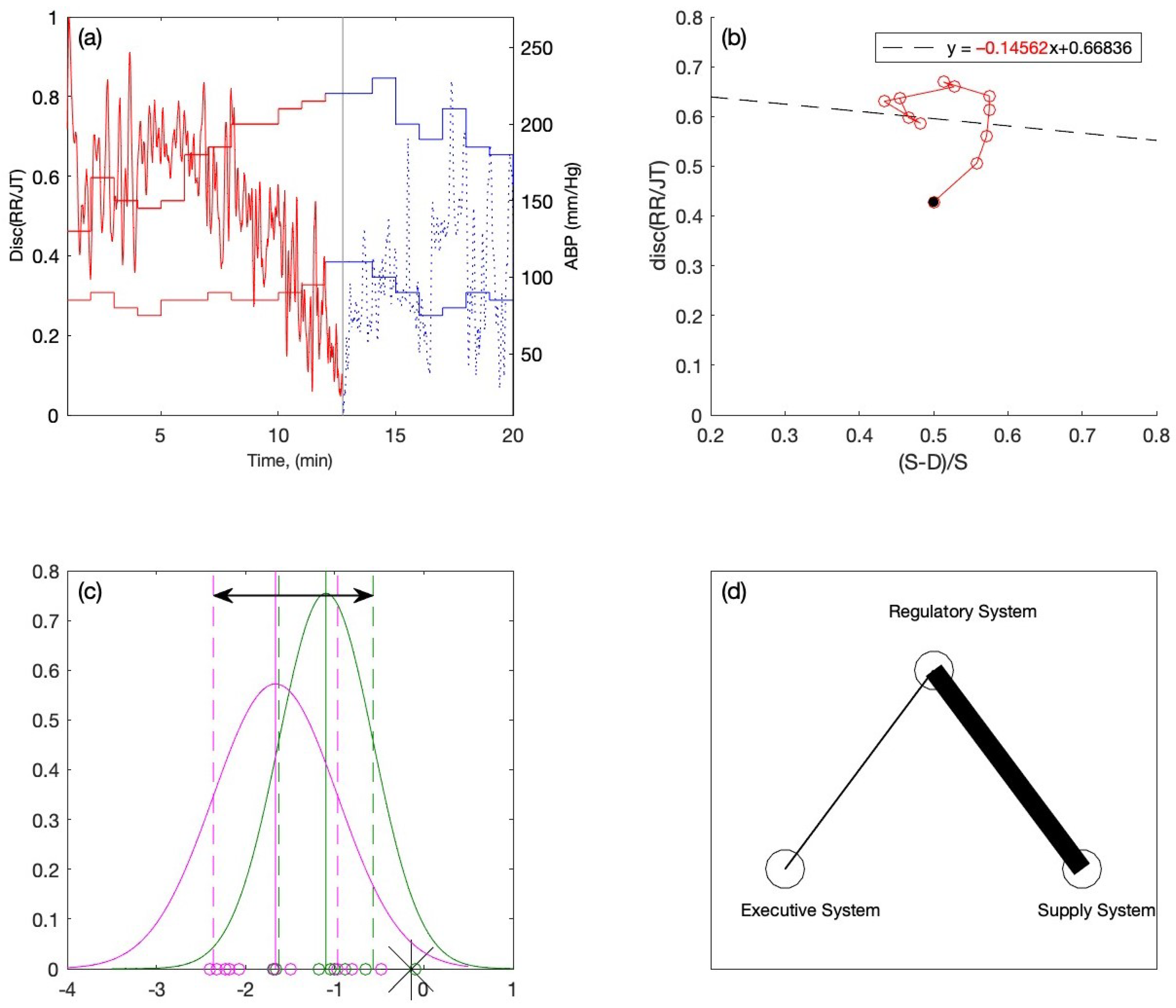
2.3.1. The Averaged RR/JT Algebraic Relationship and ABP Data in a Phase Plane
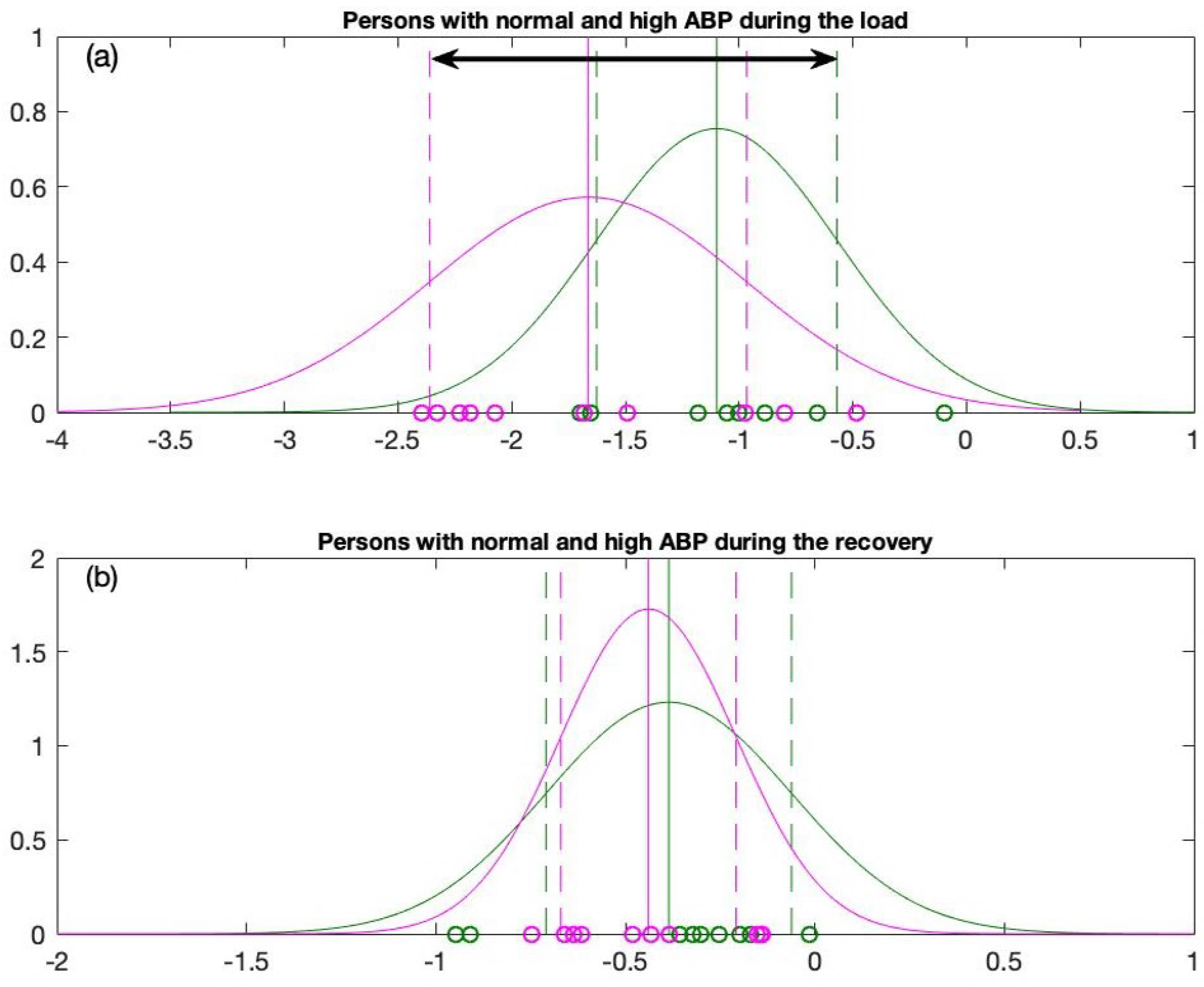
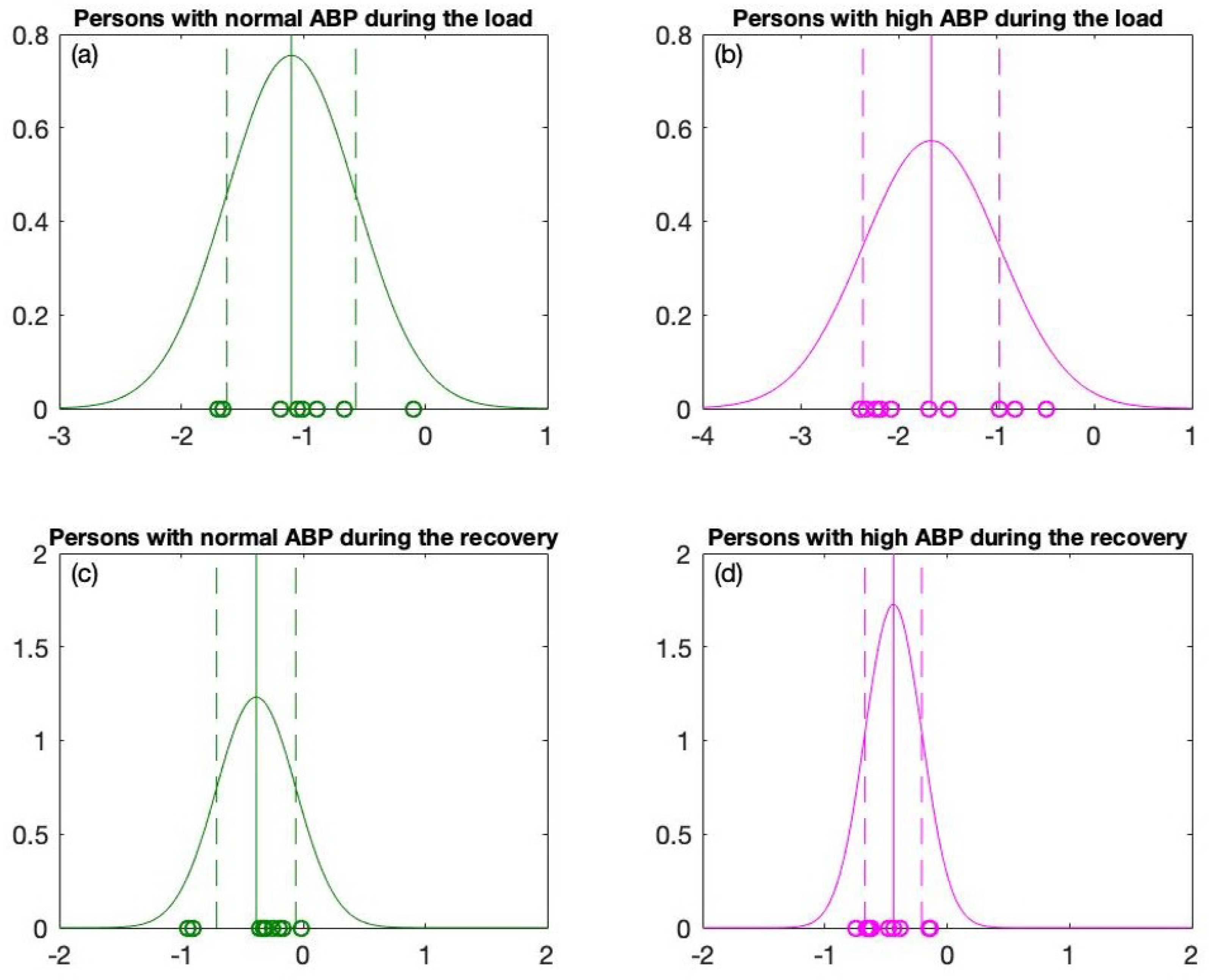
2.3.2. Data Fitting into the Gaussian Distribution
2.3.3. Classification Using the One Sigma Rule
3. Results and Discussions
3.1. The Implementation of the Classification Model
3.2. Classification of New Candidates
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CNS | central nervous system |
| ABP | arterial blood pressure |
| HR | heart rate |
| MET | metabolic equivalent |
| SV | stroke volume |
| ABP (sys) | systolic arterial blood pressure |
| ABP (dis) | diastolic arterial blood pressure |
| JTa | amplitude of the JT interval |
| JTd | the duration of the JT interval |
| ECG | electrocardiogram |
| AHA | American Heart Association |
References
- Clermont, G.; Angus, D. Towards understanding pathophysiology in critical care: The human body as a complex system. In Yearbook of Intensive Care and Emergency Medicine 2001; Springer: Berlin/Heidelberg, Germany, 2001; pp. 13–22. [Google Scholar]
- Pocock, G.; Richards, C.D.; Richards, D.A. Human Physiology; Springer Science & Business Media: Berlin/Heidelberg, Germany, 2013. [Google Scholar]
- Žemaitytė, M. Širdies Ritmo Autonominis Reguliavimas: Mechanizmai, Vertinimas, Klinikinė Reikšmė; KMA Leidykla: Kaunas, Lithuania, 1997. [Google Scholar]
- Kevelaitis, E.N.N.; Menasché, P. Coronary endothelial dysfunction of isolated hearts subjected to prolonged cold storage: Patterns and contributing factors. J. Heart Lung Transplant. 1999, 18, 239–247. [Google Scholar] [CrossRef]
- Rowell, L. Neural control of muscle blood flow: Importance during dynamic exercise. Clin. Exp. Pharmacol. Physiol. 1997, 24, 117–125. [Google Scholar] [CrossRef]
- Hollander, A.; Bouman, L. Cardiac acceleration in man elicited by a muscle-heart reflex. J. Appl. Physiol. 1975, 38, 272–278. [Google Scholar] [CrossRef]
- Faria, E.; Faria, I. Cardiorespiratory responses to exercises of equal relative intensity distributed between the upper and lower body. J. Sport. Sci. 1998, 16, 309–315. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, S.; Bell, C. The effects of exercise and training on human cardiovascular reflex control. J. Auton. Nerv. Syst. 2000, 81, 16–24. [Google Scholar] [CrossRef]
- Savin, W.M.; Davidson, D.M.; Haskell, W.L. Autonomic contribution to heart rate recovery from exercise in humans. J. Appl. Physiol. 1982, 53, 1572–1575. [Google Scholar] [CrossRef] [PubMed]
- Chapman, J.; Elliott, P. Cardiovascular effects of static and dynamic exercise. Eur. J. Appl. Physiol. Occup. Physiol. 1988, 58, 152–157. [Google Scholar] [CrossRef] [PubMed]
- Eriksen, M.O.; Waaler, B.A.; Walløe, L.; Wesche, J. Dynamics and dimensions of cardiac output changes in humans at the onset and at the end of moderate rhythmic exercise. J. Physiol. 1990, 426, 423–437. [Google Scholar] [CrossRef]
- Secher, N.H.; Clausen, J.P.; Klausen, K.; Noer, I.; Trap-Jensen, J. Central and regional circulatory effects of adding arm exercise to leg exercise. Acta Physiol. Scand. 1977, 100, 288–297. [Google Scholar] [CrossRef]
- Takahara, K.; Miura, Y.; Kouzuma, R.; Yasumasu, T.; Nakamura, T.; Nakashima, Y. Physical training augments plasma catecholamines and natural killer cell activity. J. UOEH 1999, 21, 277–287. [Google Scholar] [CrossRef]
- O’Brien, E.; Pickering, T.; Asmar, R.; Myers, M.; Parati, G.; Staessen, J.; Mengden, T.; Imai, Y.; Waeber, B.; Palatini, P.; et al. Working Group on Blood Pressure Monitoring of the European Society of Hypertension International Protocol for validation of blood pressure measuring devices in adults. Blood Press. Monit. 2002, 7, 3–17. [Google Scholar] [CrossRef]
- Yamaguchi, M.; Shimizu, M.; Ino, H.; Okeie, K.; Yasuda, T.; Fujino, N.; Fujii, H.; Mabuchi, T.; Mabuchi, H. Diagnostic usefulness of the post-exercise systolic blood pressure response for the detection of coronary artery disease in patients with diabetes mellitus. Jpn. Circ. J. 2000, 64, 949–952. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mansia, G.; De Backer, G.; Dominiczak, A.; Cifkova, R.; Fagard, R.; Germano, G.; Grassi, G.; Heagerty, A.M.; Kjeldsen, S.E.; Laurent, S.; et al. 2007 Guidelines for the management of arterial hypertension: The Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur. Heart J. 2007, 28, 1462–1536. [Google Scholar] [CrossRef]
- Mancia, G.; Laurent, S.; Agabiti-Rosei, E.; Ambrosioni, E.; Burnier, M.; Caulfield, M.J.; Cifkova, R.; Clément, D.; Coca, A.; Dominiczak, A.; et al. Reappraisal of European guidelines on hypertension management: A European Society of Hypertension Task Force document. Blood Press. 2009, 18, 308–347. [Google Scholar] [CrossRef]
- McHam, S.A.; Marwick, T.H.; Pashkow, F.J.; Lauer, M.S. Delayed systolic blood pressure recovery after graded exercise: An independent correlate of angiographic coronary disease. J. Am. Coll. Cardiol. 1999, 34, 754–759. [Google Scholar] [CrossRef]
- Skirius, J. Sportininkų širdies ir kraujagyslių sistemos funkcinės būklės tyrimas ir vertinimas. In Proceedings of the Sporto Mokslo Dabartis ir Naujosios Idejos, Kaunas, Lithuania, 10–12 September 2002; pp. 46–48. [Google Scholar]
- Fletcher, G.F.; Balady, G.J.; Amsterdam, E.A.; Chaitman, B.; Eckel, R.; Fleg, J.; Froelicher, V.F.; Leon, A.S.; Piña, I.L.; Rodney, R.; et al. Exercise standards for testing and training: A statement for healthcare professionals from the American Heart Association. Circulation 2001, 104, 1694–1740. [Google Scholar] [CrossRef]
- Bar-Yam, Y. About Complex Systems. In Reading; Addison-Wesley: Boston, MA, USA, 1997. [Google Scholar]
- Fonseca, C.G.; Backhaus, M.; Bluemke, D.A.; Britten, R.D.; Chung, J.D.; Cowan, B.R.; Dinov, I.D.; Finn, J.P.; Hunter, P.J.; Kadish, A.H.; et al. The Cardiac Atlas Project—An imaging database for computational modeling and statistical atlases of the heart. Bioinformatics 2011, 27, 2288–2295. [Google Scholar] [CrossRef] [PubMed]
- Bharti, R.; Khamparia, A.; Shabaz, M.; Dhiman, G.; Pande, S.; Singh, P. Prediction of heart disease using a combination of machine learning and deep learning. In Computational Intelligence and Neuroscience; Hindawi: London, UK, 2021. [Google Scholar]
- Maurer, M.S.; Burkhoff, D.; Fried, L.P.; Gottdiener, J.; King, D.L.; Kitzman, D.W. Ventricular structure and function in hypertensive participants with heart failure and a normal ejection fraction: The Cardiovascular Health Study. J. Am. Coll. Cardiol. 2007, 49, 972–981. [Google Scholar] [CrossRef] [PubMed]
- Spyropoulos, F.; Vitali, S.H.; Touma, M.; Rose, C.D.; Petty, C.R.; Levy, P.; Kourembanas, S.; Christou, H. Echocardiographic markers of pulmonary hemodynamics and right ventricular hypertrophy in rat models of pulmonary hypertension. Pulm. Circ. 2020, 10, 2045894020910976. [Google Scholar] [CrossRef]
- Rajput, J.S.; Sharma, M.; Tan, R.S.; Acharya, U.R. Automated detection of severity of hypertension ECG signals using an optimal bi-orthogonal wavelet filter bank. Comput. Biol. Med. 2020, 123, 103924. [Google Scholar] [CrossRef]
- Soh, D.C.K.; Ng, E.; Jahmunah, V.; Oh, S.L.; Tan, R.S.; Acharya, U. Automated diagnostic tool for hypertension using convolutional neural network. Comput. Biol. Med. 2020, 126, 103999. [Google Scholar] [CrossRef] [PubMed]
- Jain, P.; Gajbhiye, P.; Tripathy, R.; Acharya, U.R. A two-stage deep CNN architecture for the classification of low-risk and high-risk hypertension classes using multi-lead ECG signals. Inform. Med. Unlocked 2020, 21, 100479. [Google Scholar] [CrossRef]
- Parmar, K.S.; Kumar, A.; Kalita, U. ECG signal based automated hypertension detection using fourier decomposition method and cosine modulated filter banks. Biomed. Signal Process. Control 2022, 76, 103629. [Google Scholar] [CrossRef]
- Li, H.; Deng, J.; Feng, P.; Pu, C.; Arachchige, D.D.; Cheng, Q. Short-Ter, Nacelle Orientation Forecasting Using Bilinear Transformation and ICEEMDAN Framework. Front. Energy Res 2021, 9, 780928. [Google Scholar] [CrossRef]
- Li, H.; Deng, J.; Yuan, S.; Feng, P.; Arachchige, D.D. Monitoring and Identifying Wind Turbine Generation Bearing Faults Using Deep Belief Network and EWMA Control Charts. Front. Energy Res. 2021, 770, 3–17. [Google Scholar] [CrossRef]
- Batzel, J.J.; Kappel, F.; Schneditz, D.; Tran, H.T. Cardiovascular and Respiratory Systems: Modeling, Analysis, and Control; Society for Industrial and Applied Mathematics: Philadelphia, PA, USA, 2007; Volume 29, pp. 129–131. [Google Scholar]
- Šiaučiūnaitė, V.; Ragulskis, M.; Vainoras, A.; Dabiri, B.; Kaniusas, E. Visualization of complex processes in cardiovascular system during electrical auricular vagus nerve stimulation. Diagnostics 2021, 11, 2190. [Google Scholar] [CrossRef]
- Stock, M.; Ryan, M. Oxygen consumption calculated from the Fick equation has limited utility. Crit. Care Med. 1996, 24, 86–90. [Google Scholar] [CrossRef]
- Delong, C.; Sharma, S. Physiology, Peripheral Vascular Resistance; StatPearls Publishing: Treasure Island, FL, USA, 2019. [Google Scholar]
- Armstrong, R.B.; Warren, G.L.; Warren, J.A. Mechanisms of exercise-induced muscle fibre injury. Sport. Med. 1991, 12, 184–207. [Google Scholar] [CrossRef] [PubMed]
- Rowel, L. Circulatory responses to upright posture. In Human Cardiovascular Control: Reflex Control During Orthostasis; CRC Press: Boca Raton, FL, USA, 1993; pp. 39–74. [Google Scholar]
- Gargasas, L.; Vainoras, A.; Schwela, H.; Jaruševičius, G.; Ruseckas, R.; Miškinis, V. JT interval changes during bicycle ergometry. In Proceedings of the Kardiologia Polska II Miedzynarodowy Kongres Polskiego Towarzystwa Kardiologieznego, Katowice, Poland, 4–6 September 1998; Volume 49, p. 153. [Google Scholar]
- Shaffer, F.; McCraty, R.; Zerr, C.L. A healthy heart is not a metronome: An integrative review of the heart’s anatomy and heart rate variability. Front. Psychol. 2014, 5, 1040. [Google Scholar] [CrossRef]
- McCraty, R.; Atkinson, M.; Tomasino, D.; Bradley, R.T. The coherent heart heart-brain interactions, psychophysiological coherence, and the emergence of system-wide order. Integral Rev. Transdiscipl. Transcult. J. New Thought Res. Prax. 2009, 5, 10–115. [Google Scholar]
- Segerstrom, S.; Nes, L. Heart rate variability reflects self-regulatory strength, effort, and fatigue. Psychol. Sci. 2007, 18, 275–281. [Google Scholar] [CrossRef]
- Woods, K. QT Dispersion in Ischaemic Heart Disease; Oxford University Press: Oxford, UK, 2000; pp. 432–433. [Google Scholar]
- Roukema, G.; Singh, J.P.; Meijs, M.; Carvalho, C.; Hart, G. Effect of exercise-induced ischemia on QT interval dispersion. Am. Heart J. 1998, 135, 88–92. [Google Scholar] [CrossRef]
- Yoshimura, M.; Yasue, H.; Ogawa, H. Pathophysiological significance and clinical application of ANP and BNP in patients with heart failure. Can. J. Physiol. Pharmacol. 2001, 79, 730–735. [Google Scholar] [CrossRef]
- Vainoras, A.; Gargasas, L.; Ruseckas, R.; Miškinis, V.; Jurkonienė, R. Computerised exercise electrocardiogram analysis system “Kaunas-Load”. In Proceedings of the 24th International Congress on Electrocardiology and 38th International Symposium on Vectorcardiography: Abstracts Book, Bratislava, Slovak Republic, 24–28 June 1997. [Google Scholar]
- Gargasas, L.; Vainoras, A.; Ruseckas, R.; Jurkoniene, R.; Jurkonis, V.; Miskinis, V. A new software for ECG monitoring system. In Proceedings of the 6th Nordic Conference on eHealth and Telemedicine, Helsinki, Finland, 31 August–1 September 2006. [Google Scholar]
- Ziaukas, P.; Alabdulgader, A.; Vainoras, A.; Navickas, Z.; Ragulskis, M. New approach for visualization of relationships between RR and JT intervals. PLoS ONE 2017, 12, e0174279. [Google Scholar] [CrossRef] [PubMed]
- Saunoriene, L.; Siauciunaite, V.; Vainoras, A.; Bertasiute, V.; Navickas, Z.; Ragulskis, M. The characterization of the transit through the anaerobic threshold based on relationships between RR and QRS cardiac intervals. PLoS ONE 2019, 14, e0216938. [Google Scholar] [CrossRef] [PubMed]
- Laio, F. Cramer–von Mises and Anderson-Darling goodness of fit tests for extreme value distributions with unknown parameters. Water Resour. Res. 2004, 40. [Google Scholar] [CrossRef]
| Persons with Normal ABP | |||||
|---|---|---|---|---|---|
| No. | Names | Slope Coefficients during Load (W·ms),M1 | Spearman’s Rank Correlation Coefficient during Load | Slope Coefficients during Recovery (W·ms),M2 | Spearman’s Rank Correlation Coefficient during Recovery |
| 1 | BACCHR | −1.6963 | −0.8035 | −0.32249 | −0.8024 |
| 2 | BARHEL | −0.65793 | −0.9058 | −0.012758 | −0.0486 |
| 3 | BROSOR | −1.6554 | −0.9333 | −0.30205 | −0.4667 |
| 4 | ENGBER | −1.0524 | −0.8161 | −0.19906 | −0.8389 |
| 5 | PETTHO | −1.0029 | −0.8903 | −0.90867 | −0.9244 |
| 6 | STEMAR | −0.097479 | −0.2168 | −0.25354 | −0.8146 |
| 7 | HEIRAL | −1.6539 | −0.8908 | −0.94723 | −0.7538 |
| 8 | FLOPET | −1.1824 | −0.8389 | −0.35497 | −0.8024 |
| 9 | SCHMAR | −0.88493 | −0.9515 | −0.16869 | −0.8066 |
| Persons with Normal ABP | |||||
|---|---|---|---|---|---|
| No. | Names | Slope Coefficients during Load (W·ms),M3 | Spearman’s Rank Correlation Coefficient during Load | Slope Coefficients during Recovery (W·ms),M4 | Spearman’s Rank Correlation Coefficient during Recovery |
| 1 | ADAWOL | −2.3278 | −0.6960 | −0.61569 | −0.9119 |
| 2 | BRODOR | −2.229 | −0.7972 | −0.66062 | −0.9624 |
| 3 | ILLBJO | −2.1799 | −0.4745 | −0.43314 | −0.6869 |
| 4 | NAUTHO | −1.4895 | −0.9701 | −0.48034 | −0.9157 |
| 5 | STETHO | −1.6843 | −0.9066 | −0.748 | −0.9758 |
| 6 | PFEAND | −2.3957 | −0.8654 | −0.152 | −0.7833 |
| 7 | NEUCHR | −0.48277 | −0.6097 | −0.13909 | −0.8257 |
| 8 | LINUWE | −0.97304 | −0.4954 | −0.14123 | −0.7500 |
| 9 | KRAHAR | −0.80256 | −0.8742 | −0.38448 | −0.8074 |
| 10 | KLITOR | −2.071 | −0.9449 | −0.63648 | −0.9222 |
| Mean | Std. Deviation | Confidence Interval | Sig. Level | Difference in Means | The Statistical Condition | |
|---|---|---|---|---|---|---|
| Persons with normal ABP during the load | 0.4636 | Condition is satisfied | ||||
| Persons with high ABP during the load | 0.1789 | |||||
| Persons with normal ABP during the recovery | 0.0190 | Condition is not satisfied | ||||
| Persons with high ABP during the recovery | 0.2339 |
| Coordinate | Corresponds to |
|---|---|
| −1, 0 | E (the Executive System) |
| 0, 1 | R (the Regulatory System) |
| 1, 0 | S (the Supply System) |
| Condition 1 | Condition 2 | Condition 3 | |
|---|---|---|---|
| If | |||
| The interpolation coefficient | in between the variation interval | ||
| The thickness of the left branch in pixels | 1 | ||
| The thickness of the right branch in pixels | 1 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Qammar, N.W.; Orinaitė, U.; Šiaučiūnaitė, V.; Vainoras, A.; Šakalytė, G.; Ragulskis, M. The Complexity of the Arterial Blood Pressure Regulation during the Stress Test. Diagnostics 2022, 12, 1256. https://doi.org/10.3390/diagnostics12051256
Qammar NW, Orinaitė U, Šiaučiūnaitė V, Vainoras A, Šakalytė G, Ragulskis M. The Complexity of the Arterial Blood Pressure Regulation during the Stress Test. Diagnostics. 2022; 12(5):1256. https://doi.org/10.3390/diagnostics12051256
Chicago/Turabian StyleQammar, Naseha Wafa, Ugnė Orinaitė, Vaiva Šiaučiūnaitė, Alfonsas Vainoras, Gintarė Šakalytė, and Minvydas Ragulskis. 2022. "The Complexity of the Arterial Blood Pressure Regulation during the Stress Test" Diagnostics 12, no. 5: 1256. https://doi.org/10.3390/diagnostics12051256
APA StyleQammar, N. W., Orinaitė, U., Šiaučiūnaitė, V., Vainoras, A., Šakalytė, G., & Ragulskis, M. (2022). The Complexity of the Arterial Blood Pressure Regulation during the Stress Test. Diagnostics, 12(5), 1256. https://doi.org/10.3390/diagnostics12051256








