Abstract
Benefits of photobiomodulation (PBM) have been known for several decades. More recently, PBM applied in sports offers a special chance to support the modeling of the performance and recovery. Increasingly complex physical activities and fierce competition in the world of sports generate a state of psycho-emotional and physical stress that can induce chronic fatigue syndrome, failure in physical training, predisposition to muscle damage, physical and emotional exhaustion etc., for which PBM could be an excellent solution. To evaluate and identify all risk factors and the influence of PBM on health and performance in sport and for a better understanding of its effects, we did a search for “Photobiomodulation and Sports” on PubMed, to update the PBM science applied in sports, and we retained for analysis the articles published from 2014 to date. The term “PBM” is recent, and we did not include previous studies with “low level laser therapy” or “LLLT” before 2014. In the present research, PBM has been shown to have valuable protective and ergogenic effects in 25 human studies, being the key to success for high performance and recovery, facts supported also by 22 animal studies. PBM applied creatively and targeted depending on sport and size of the level of physical effort could perfectly modulate the mitochondrial activity and thus lead to remarkable improvements in performance. PBM with no conclusive results or without effects from this review (14 studies from a total of 39 on humans) was analyzed and we found the motivations of the authors from the perspective of multiple causes related to technological limitations, participants, the protocols for physical activity, the devices, techniques and PBM parameters. In the near future, dose–response experiments on physical activity should be designed and correlated with PBM dose–response studies, so that quantification of PBM parameters to allow the energy, metabolic, immune, and neuro-endocrine modulation, perfectly coupled with the level of training. There is an urgent need to continuously improve PBM devices, delivery methods, and protocols in new ingenious future sports trials. Latest innovations and nanotechnologies applied to perform intracellular signaling analysis, while examining extracellular targets, coupled with 3D and 4D sports motion analysis and other high-tech devices, can be a challenge to learn how to maximize PBM efficiency while achieving unprecedented sports performance and thus fulfilling the dream of millions of elite athletes.
1. Introduction
It is in the competitive human spirit to look for the best performance in both amateurs and sports professionals. In this search for incredible results and the implementation of new exercises and innovative training, a major role is played by the selection of the latest appropriate ergogenic means designed to improve physical and mental performance, endurance, but also recovery after intense muscle training.
Due to high competition, always staying on the top for professionals has become increasingly difficult due to permanent facing with the readjustments of the human body to high stress and intense training dictate by the huge tasks of physical activities. To increase muscle strength and endurance in athletes, new means of stimulating and regulating skeletal muscles are needed, in addition to improving hypertrophic and neuromuscular fitness.
An essential property of skeletal muscle is contraction, which needs energy and is achieved by sliding actin molecules (thin) on the myosin (thick) filaments, together forming the sarcomere. Myosin head also binds to adenosine triphosphate (ATP), which is the basis of the energy supply for muscle contraction. Myosin can bind to actin only when actin coupling sites are exposed to calcium ions. Tropomyosin covers the myosin-binding sites of the actin molecules, so it must be removed to uncover the binding sites on the actin, a process that also requires energy. Calcium ions will connect to troponin C molecules, modifying the pattern of the tropomyosin and obliging it to disclose the cross-bridge coupling sites on the actin. Transferring the sodium and potassium ions through the muscle membrane to keep the vital ionic gradients also needs energy, for which the ATP is the main muscle fuel.
ATP is the basic energy unit in the physiological enzymatic processes of (Na+/K + ATPase), (Ca2 + ATPase), and the myofilament cross-bridge cycling (myosin ATPase) in the excitable muscle cell membrane. However, the intake of ATP for muscles can last only 1–2 s. Intramuscular deposits of ATP are reduced (~5 mmol per kg wet muscle), and at a score of ATP utilization of 3.7 mmol ATP kg−1 s−1, the muscular activity could last less than 2 s if stocked ATP was the only energy source [1].
Creatine phosphate (CK), which, like ATP contains, a high-energy phosphate bond, is a rapid source of energy for ATP regeneration. CK deposits are also limited and could supply energy for muscle contractions for only 5 to 8 s. The main sources of energy for muscles remain glucose and fatty acids, whose consumption depends on the load and fitness of the subject, as well as the availability of oxygen. ATP production from cytosolic glycolysis, mitochondrial oxidation of beta fatty acids, and the citric acid cycle are tightly regulated and respond quickly to muscle demands for more ATP [2].
The amount of ATP and its supply at the right time during skeletal muscle contraction is essential both in explosive sportive events for noticeably short periods of time (seconds or minutes), for example in sprints and jumps, but also in case of long resistance efforts in which the athlete must prove endurance for hours [1,3].
Photobiomodulation (PBM), formerly known as low-power laser therapy or low-level laser therapy (LLLT), has its new terminology adopted at the joint conference of the North American Association for Light Therapy and the World Association for Laser Therapy in September 2014, with a consensus on nomenclature for photobiomodulation as an ideal term [4].
PBM involves the use of visible and/or infrared laser/light to biologically modulate cellular activity, to improve tissue and cell functions through the activation of cellular enzymes, so that the flux of photons is inducing several physiological changes such as: increasing ATP production, reduction in inflammation and pain, stimulation of the formation of new muscle fibers, acceleration of angiogenesis, repair, and regeneration of tissues [5,6].
PBM has been shown in several studies to be effective in cell proliferation, stimulating metabolism, reducing inflammation, and promoting tissue healing. Amidst the parameters used, the dose delivered to a certain type of tissue is crucial, because the effects will depend on it: the application of a small dose could lead to an important cellular response, but high doses can inhibit cell proliferation or even induce apoptosis. Among the most replicable consequences of PBM is the systemic decrease in inflammation, very significant for traumatic injuries or joint diseases, lung, and brain conditions [7].
Current studies on the effects of anti-inflammatory PBM at the cellular level are focused mainly on the expression of pro-inflammatory cytokines and on the migration and concentration of macrophages at the site of impact. It is known that the macrophage plays a crucial role during the inflammatory phase; the M1 phenotype has a physiological proinflammatory activity for the defense of the host in the invasion with pathogens, and the M2 phenotype participates in the remedy of injuries in the phase of extinguishing the inflammation [8].
PBM regulates through complex mechanisms a wide range of pro-inflammatory/anti-inflammatory cytokines and the level of polarization of macrophages responsible for an excessive inflammatory response or accelerated tissue healing.
Wavelength influences the propagation, flux, and rate of distribution of photons in irradiated tissues, as well as the effectiveness of non-invasive application of the laser. The wavelength used by PBM is a valuable parameter in the response to cell proliferation because the wavelength between 600–1070 nm (red/near-infrared (IR)) has the best non-invasive effects. It has been observed that the shorter wavelengths are absorbed by hemoglobin or melanin, producing cellular effects, while the longer wavelengths are absorbed by water, and give the sensation of warmth and induce pain relief [9].
From the first applications, PBM has been used for the treatment of many inflammatory diseases, musculoskeletal disorders, and especially for tissue regeneration and recovery. Intensive development of advanced laser systems—as well as other medical treatment devices—has led to the unprecedented expansion of the multitude of therapy options including stimulating and healing of muscles, tendons, ligaments, joints, etc. but also immunological conditions, the nervous system, as well as targeting the axis of the immune system—muscular system—brain, etc., and all in connection with training and physical exercises. The value of these therapies is the lack of side effects, of addiction, considered as energy methods that precisely address the energy processes inside the cells and what is most valuable, without drugs or toxic consequences.
2. Methodology
From previous randomized and placebo-controlled scientific LLLT studies, it is known that the wavelengths red to near-IR delivered from single laser diodes or clusters, LEDs, or arrangements of both in different impressively adaptable devices can supply energy to the cellular power plants to repair and regenerate muscles, painful joints due to intense physical activity, and restore the physiological balance. Specific muscle characteristics studied previously included parameters such as exhaustion, muscle fatigue, set of repetitions, twisting force impulse, muscle fiber hypertrophy, the degree of muscle damage, such as CK, lactate dehydrogenase (LDH), etc. and remaining muscle pain or delayed onset muscle soreness, as well as the recovery time [10].
To evaluate and identify all risk factors and the influence of PBM on health and performance in sport and for a better understanding of its effects in high elite athletes, we conducted a search for “Photobiomodulation and Sports” on PubMed, to update the PBM science applied in sports, and we retained for analysis all the articles published from 2014 to date.
The term “PBM” is recent, and we did not include previous studies with “low level laser therapy” or “LLLT” before 2014 [4].
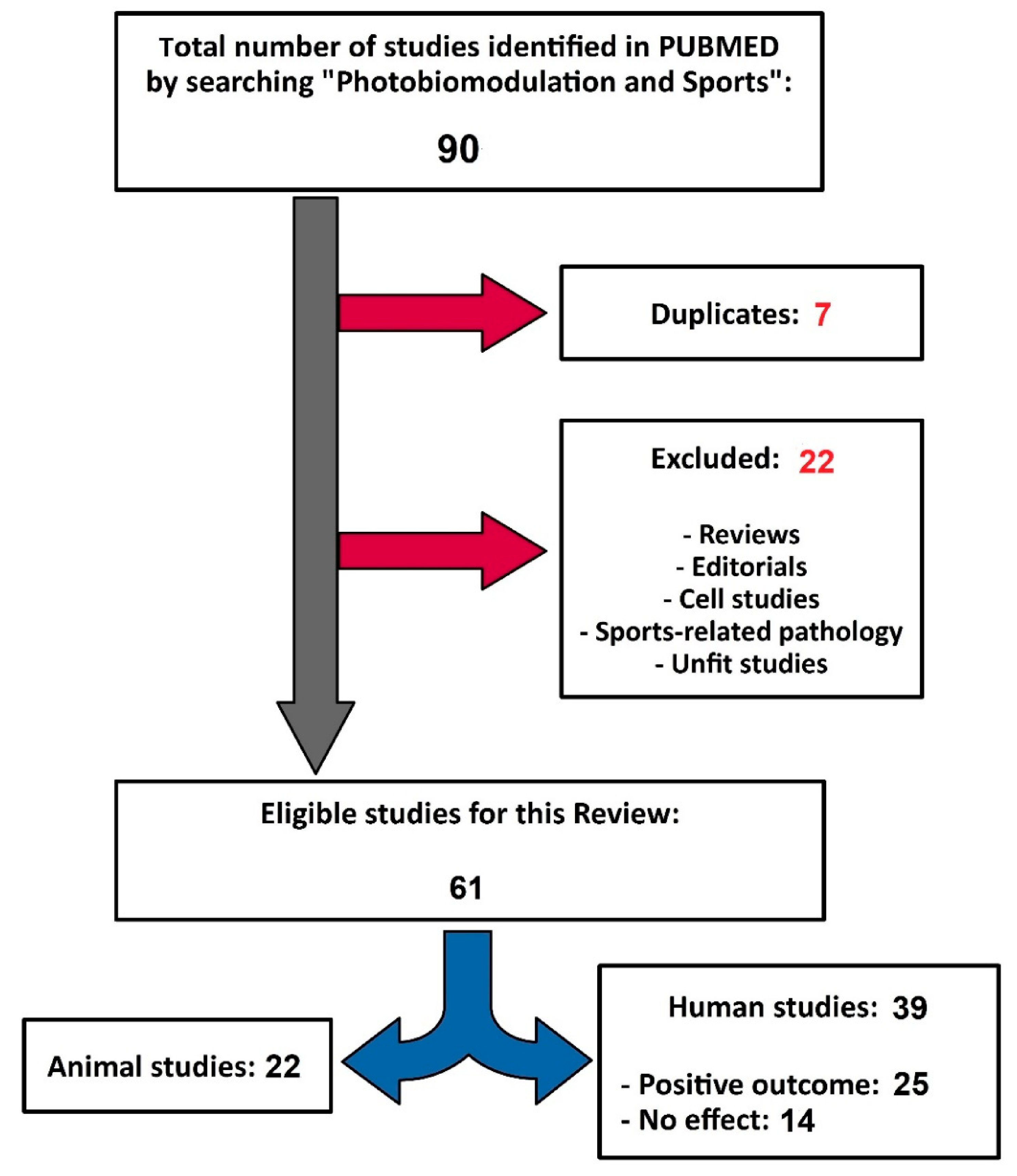
The search retrieved 90 studies, of which 29 studies were excluded (reviews, editorials, cellular studies, sports-related pathologies, inadequate studies due to lack of randomization or control group, duplicates, etc.), and the difference (61 studies) was included in the analysis (Figure 1).
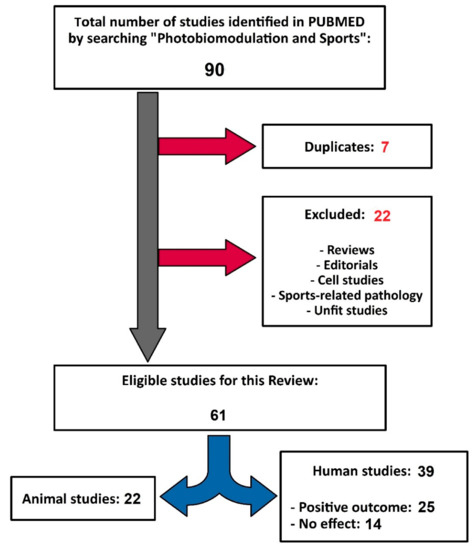
Figure 1.
Organization chart of the studies selection.
Of the last 61 studies considered in this review, 39 were in human subjects, and 22 were experimental animal studies. Analysis of research in human subjects revealed positive effects of PBM in 25 studies, which included 797 participants, and 14 studies did not indicate any relevant effect of PBM compared to control groups.
3. PBM Applied in Sports in Different Settings and Conditions
3.1. Positive Effects of PBM
Applying PBM both before and after training can have positive effects, so we classified the studies into applications of PBM before, after, before and after, and in experimental laboratory conditions when participants were running on the treadmill.
There were 39 randomized, placebo-controlled studies on humans, of which only 25 (with 797 subjects) had positive results due to PBM applied to various light physical activities or intensive training, before, after, both before and after, or under experimental laboratory conditions, of which 21 are summarized in Table 1, and four other studies with PBM and simultaneously applied static magnetic field are mentioned in the final discussions.

Table 1.
Positive effects of PBM in physical activities.
In order to set out the most favorable dose of PBM, Antonialli et al. [11] evaluated skeletal muscle efficiency and the recuperation after exercise including 40 vigorous male volunteers, but physically unprepared, into a randomized, double-blind, placebo-controlled study using 12 cluster diodes (4 IR laser diodes of 905 nm, 4 IR LEDs of 875 nm and, 4 red LEDs of 670 nm). They administered 10, 30, and 50 J, or placebo, in six points on the front of the thighs, using only one PBM treatment immediately after pre-exercise maximal voluntary contraction (MVC), and finally analyzing MVC, delayed-onset muscle soreness (DOMS), and the creatinine kinase (CK). Ratings were effectuated before, 1 min, 1 h, 24 h, 48 h, 72 h, and 96 h after the procedures to provoke muscular tiredness. PBM enhanced MVC from immediately after to 96 h after exercise with 10 or 30 J doses, remarkably diminished DOMS with 30 J dose from 24 h to 96 h after exercise, and with 50 J dose from immediately after to 96 h after exercise; and significantly decreased CK activity with all PBM doses, in comparison to the placebo group, concluding that the 30 J dose was the best.
In another study, Vanin et al. [12] evaluated the effects of 810 nm/200 mW PBM applied also in six sites on quadriceps with a cluster with only 5 diodes, applying 10, 30, or 50 J in a randomized, double-blind, placebo-controlled study in 28 high-level soccer athletes, also to identify the optimal dose for best recovery and performance. Researchers assessed MVC, DOMS, CK activity, IL-6 expression, before and after 1 min, 1 h, 1 day to 4 days, after the protocol to trigger the muscular exhaustion. PBM increased MVC from immediately after exercise to 24 h with 50 J dose, and from 1 day to 4 days with 10 J dose; it decreased CK and IL-6 with better results in favor of 50 J dose and had no effect on DOMS. Authors concluded that pre-exercise PBM with 50 J energy dose remarkably rose the performance and reduced the biochemical markers linked to damage and inflammation in the skeletal muscle system.
Also in athletes, but in an anaerobic field test using a randomized, crossover, double-blind, placebo-controlled clinical trial in twelve male high-level rugby players, Pinto et al. [13] demonstrated the effects of PBMT in improving performance and speeding up the rehabilitation time during the Bangsbo sprint test (BST). There were no interventions before BST in the familiarization phase (week 1) but in weeks 2 and 3, pre-exercise PBMT (at 17 points of each leg, employing a cluster with 12 diodes (4 super-pulsed IR laser diodes of 905 nm, 4 IR LEDs of 875 nm, and 4 red LEDs of 640 nm, 30 J per site) or placebo, was randomly delivered to every athlete. As a result, PBMT improved the average sprint time and fatigue index in BST and outstandingly fall down the percentage of blood lactate levels to 3, 10, 30, and 60 min after BST, initiating a novel pathway for large-scale applications of PBMT in real sports conditions.
The best PBMT output power for skeletal muscle recovery was identified by AR de Oliveira et al. [14] in a randomized, double-blind, placebo-controlled study involving 28 high-level football players. PBMT was applied before the eccentric contraction protocol with a cluster also with five diodes (810 nm, 10 J dose), but three different output powers (100, 200, 400 mW per diode) or placebo, at six sites of the knee extensors. Voluntary maximal isometric contraction (MIVC), DOMS, CK and lactate dehydrogenase, inflammation (IL-1β, IL-6, and TNF-α), and oxidative stress (catalase, superoxide dismutase, carbonylated proteins, and thiobarbituric acid) were evaluated before isokinetic exercise, as well as after 1 min and 1 h to 96 h. PBMT increased MIVC and decreased DOMS and the biochemical marker levels with the best results for 100 mW output power per diode (500 mW in total) in improving performance and post-exercise restauration.
Rossato et al. [15] aimed to identify the effects of two different time responses on knee extensor fatigue in sixteen male volunteers, distributed to perform the same protocol in 5 sessions. PBMT was applied to the knee extensor (9 sites, 30 J per site). MIVC was evaluated before and after isokinetic fatigue associated with electromyography (root mean square [RMS] and median frequency [MF]). Time effect was observed for peak torque (PT), RMS, and MF. The effect of treatment was checked for PT, and 6 h before + immediately before the condition showed higher PT during MIVC (pre to post) than control or placebo. Applying PBMT with 6 h + directly before exercises is capable to diminish tiredness.
To test PBMT effects on futsal players’ performance and recovery, De Marchi et al. [16] included six professional athletes in a randomized, triple-blinded, placebo-controlled, crossover clinical trial. PBMT was performed 40 min before matches at 17 points of every leg, also employing a cluster with 12 diodes (4 IR laser diodes of 905 nm, 4 IR LEDs of 875 nm, and 4 red LEDs of 640 nm, 30 J per site). Blood samples were collected before treatments, immediately after the matches, and 48 h after (evaluated for CK, LDH, blood lactate, and oxidative damage of lipids and proteins). Time spent by athletes on the pitch and the distance covered were video quantified. PBMT significantly increased the time of staying in the pitch and determined a meaningful improvement in all the evaluated biochemical markers, but without any statistically significant difference in the mileage. Concluding, pre-exercise PBMT can successfully increase the workout and speed up the rehabilitation process of high-level futsal players.
Because muscle tiredness is an inherent hazard for hamstring stretch lesions in soccer players, Dornelles et al. [17] investigated the effects of PBMT (300 J per thigh or placebo on the hamstrings, before the match) on twelve young male amateur soccer players in a randomized, crossover, double-blinded, placebo-controlled trial, assessed in two sessions at least at 7-day apart. Muscle endurance and useful workout were evaluated through isokinetic dynamometry and countermovement jump (CMJ) tests, respectively, before and immediately after the match. PBMT had beneficial effects on hamstring eccentric peak torque, hamstring-to-quadriceps torque ratio, and the CMJ height, respectively, compared to placebo, attenuating hamstring muscle tiredness, and thus hindering hamstring stretch injuries, which usually occur in football players.
PBM before neuromuscular electrical stimulation (NMES) is a remarkably interesting topic, investigated in a randomized, double-blind crossover trial by Jówko et al. [18] on twenty-four moderately active, healthy young men, who received 45 electrically evoked tetanic, isometric contractions of the quadriceps, preceded by PBM or placebo-PBM. The impact of PBM on muscle impairs and causes oxidative stress, as well as the return to a normal state of the muscular function after a single session of NMES, quantified by the maximal isometric voluntary muscle torques, pain, and blood samples analyzed for the muscle impairment (CK), and inflammation (C-reactive protein), were assessed from baseline to 96 h post intervention. PBM had a shielding effect on NMES-induced fall in enzymatic antioxidant protection and cut the duration of inflammation, but did not affect lipid peroxidation, muscle impairment, or restauration after NMES.
The action of pre-exercise PBMT to increase workout, speed up recuperation and attenuate the oxidative stress were examined in twenty-two male high-level soccer players treated with IR PBMT or placebo prior to a progressive running test (ergo-spirometry) until exhaustion, by Tomazoni et al. [19] in a randomized, triple-blind, placebo-controlled crossover trial (identical group). PBMT enhanced the VO2max, fatigue time, volume and time for both anaerobic and aerobic threshold appearance, and diminished CK and LDH activities, as well as TBARS, IL-6, and carbonylated protein levels; it increases SOD and CAT activities so that PBMT before exercise plays an important antioxidant effect and therefore improves athletic presentation and the post-exercise regeneration.
Da Cunha et al. [20] investigated the effects of PBM and NMES on muscle endurance, jumps’ frequency and abilities, general reactions, assessed at baseline and during follow-up at 6 and 8 weeks in a study including thirty-six volleyball athletes, randomized into three groups: control, pre-exercise PBM (IR, 850 nm, CW, 0.8 J/cm2, 6 J/point, total energy equal 36 J) and operational NMES on quadriceps femoris as a muscular workout (1 kHz base, 70 Hz modulation, highest intensity supportable). The greatest increase in dominant lower limb endurance was in the NMES group, as opposed to control, but for non-dominant lower limbs, the increase was present in both PBM and NMES groups (highest effect), as well as better skills to jump in the last two groups, for which muscle-stamina growth kept on for two weeks after the end of the workout, in comparison to the control.
In another study, Rossato et al. investigated the effects of PBMT applied 6 h before and immediately before exercise with a cluster of 5 IR lasers (850 nm) and 28 LEDs, as follows: 12 red LEDs (670 nm), 8 IR LEDs (880 nm) and 8 IR LEDs (950 nm) on quadricep, in a randomized, crossover, double-blind placebo-controlled study on eighteen physically active men during a complex isokinetic exercise protocol of knee extensions. It was found that exercise performance was not affected by PBMT (135 J, 270 J, or 540 J) compared with placebo, but all doses of applied PBMT led to presumptive positive effects on isometric peak torque, concentric peak torque, and concentric work compared to placebo, facilitating the same total work with less fatigue, i.e., additional sets would be possible for a higher training volume [21].
Zagatto et al. [22] have evaluated in a randomized, double-blind, placebo-controlled research, the influence of 810 nm PBM applied on the adductors directly after each physical daily workout, on inflammation, muscle impairment, and operation capacity in twenty young water polo players. Daily, before training, the physical performance was evaluated by P200 (intense swimming of 200 m) and a 30 CJ (30 s cross-jump test). Blood tests were performed for interleukins (IL) and muscle damage both before and after the physical protocol. There was no important shift in P200 in the PBMT group compared to placebo, but there was a moderate improvement in 30 CJ. IL-1β and TNF-alpha had elevated values in the PBM group at 48 h after the last treatment, compared to pre, 0 and 24 h, but did not differentiate in the two groups. IL-10 slightly increased over time in the placebo group compared to the PBM group, where creatinine kinase decreased significantly, but no important variation in lactate dehydrogenase was observed. PBM had no important effect on inflammation and muscle damage, with only a medium impact on performance. Failure of reliable results could be caused by the undersized photobiostimulation area.
PBMT and cryotherapy alone or combined for skeletal muscle rehabilitation after eccentric contractions of knee extensors were applied by de Paiva et al. [23] in 50 healthy male volunteers, randomly distributed into five groups (PBMT, cryotherapy, cryotherapy + PBMT, PMBT + cryotherapy, or placebo) for a double-blinded, placebo-controlled trial to study MVC, DOMS and the muscle damage (CK). Estimations were conducted at the starting point, immediately after, and from 1 h to 96 h, at each 24 h interval. Comparative therapies were applied 3 min after exercise and repeated every 24 h until 72 h. PBMT (905 nm super-pulsed laser and 875 and 640 nm LEDs) and cryotherapy by ice packs on pliable caoutchouc were utilized. The best for post-exercise recovery with better MVC, diminished DOMS, and CK activity from 24–96 h was singular PBMT, compared to placebo, cryotherapy, and cryotherapy + PBMT. In the PBMT + cryotherapy lot, the influence of photobiomodulation was reduced but proved important betterment in MVC, diminished DOMS and CK activity. Singular cryotherapy and cryotherapy + PBMT were comparable to placebo. Therefore, only PBMT alone could best enhance the post-physical recovery to original physiological degrees, one day after high-intensity eccentric exercises.
The efficacy of PBMT and cryotherapy, single or mixed, for muscle rehabilitation after the administration of muscular soreness exercises was one year later investigated by De Marchi et al. [24] who randomly divided forty volunteers into five groups: placebo (PG); PBMT (PBMT), cryotherapy (CG), cryotherapy-PBMT (CPG), and PBMT-cryotherapy (PCG), which underwent a protocol of four physical sessions every 24 h, measuring their MVC and testing the blood in the pre-exercise period and at 5 and 60 min post-exercise, as well as 24, 48, and 72 h later. In the first session, with a 5 min delay, it was applied 2 min PBMT and/or cryotherapy, after the MVC test. Significant increases in MVC capacity in PBMT, CPG, and PCG, compared with PG and CG, as well as a dramatic reduction in concentrations of oxidative damage biochemical markers in all muscle groups and muscular lesions (CK) in PBMT, PCG, and CPG, were registered compared with PG. PBMT really has a higher output in muscle rehabilitation than cryotherapy, which, when simultaneously applied, reduces the effectiveness of PBMT.
Recently, Vassão et al. [25] applied PBMT with a cluster consisting of 14 LEDs, as follows: 7 red diodes (630 nm) and 7 IR diodes (850 nm) on biceps brachii muscles in 32 healthy male participants randomly distributed into 3 groups: red PBM group (RPG), infrared PBM group (IPG) and control group (CG). There were analyzed the muscle fatigue using surface electromyography (EMG), blood lactate concentration, and the rate of perceived exertion (RPE) using the Borg Scale. Comparisons between groups pointed out that electromyography fatigue index decreased in the control group, but RPE and lactate concentrations increased significantly in all groups. There was no significant difference between red and infrared PBM in the reduction in muscle fatigue, but the electromyography fatigue index delta value was greater in the IPG compared with the CG, suggesting that infrared could be more effective than red in decreasing muscle fatigue.
Consecutive stimulation with PBMT (180 J) for three successive days on the bilateral femoral quadriceps with different wavelengths: infrared (IR 940 ± 10 nm), red (RED 620 ± 10 nm), mixed red and IR (RED/IR 620 + 940 nm) or placebo, on 48 male cyclists with a mean age of 33.77 years, subjected to an assessment by an incremental test, VO2max, blood lactates, exercise perception, IR detection to study heat distribution in muscles and isokinetic summing up, was performed by Carvalho et al. [26]. For 7 days long, there were accomplished reassessments 24 h from the moment of last praxis. There were no important disparities in the examined parameters under the exploratory setup. PBMT with no connection to workout was unsuccessful in improving the cyclists’ goal. Still, applying two wavelengths reveals higher success.
Although PBM with lasers and/or LEDs on sports perfecting has been extensively investigated, not many experiments have explored the impact on strength muscular workout regarding the most favorable time for stimulation. Vanin et al. [27] randomly divided forty-eight male volunteers (18–35 years old) into four groups, who executed a robust workout, and were stimulated with PBM and/or placebo in advance, and/or after each session, using a band of probes (4 laser diodes of 905 nm, 4 IR LEDs of 875 nm, and 4 red LEDs of 640 nm). Time was 12 weeks with measurements of peak torque touched in MVC, the load in 1-RM test, and the circumference of the thigh at baseline, 4 weeks, 8 weeks, and 12 weeks. Volunteers treated with PBM before, and placebo after workout, manifested important shifts in MVC and 1-RM tests for legs, compared to other groups. Safe and without adverse effects, PBM has the capacity to rise endurance, when used before physical activities, with extra benefits in post-lesions recovery.
Felismino et al. evaluated the effects of laser irradiation on muscle injury markers after resistance exercise in a double-blind, placebo-controlled study on 22 physically active men who were randomized into two groups: laser (n = 11) and placebo (n = 11). Laser irradiation (808 nm; 100 mW; 35.7 W/cm2, 357.14 J/cm2 per point) was applied to the arms, 1 J per point for 10 s at four points of the brachial biceps of each arm, or placebo, between each set of biceps curl exercise. The following parameters were investigated: creatine kinase (CK) activity and maximal strength performance (1 RM) before, immediately after, 24 h, 48 h, and 72 h after the exercise-induced muscle damage protocol. Results suggested a partial attenuation of muscle injury when laser irradiation was used during exercise intervals. Maximum CK activity was attenuated after 72 h in the laser group compared to placebo, but there was no obvious positive effect on strength performance recovery [28].
De Brito Vieira et al. investigated the effects of LLLT (808 nm, 100 mW, 4 J/point), or placebo, applied to quadriceps femoris muscles between sets, and after the last series of intense exercises on fatigue resistance via the number of maximum repetitions (RM) and the electromyography fatigue index (EFI), in a randomized, double-blind, crossover trial with placebo. The participants, seven young men, clinically healthy, were allocated into two groups: active laser and placebo laser. Both groups were assessed at baseline and until the end of the study, registering the number of maximum repetitions (RM) of knee flexion-extensions in conjunction with EFI recorded by median frequency (MF). After 1 week (washout period), all volunteers were exchanged among groups, and then all assessments were repeated. LLLT increased the maximum number of RM, comparatively with the control group. For both groups, MF significantly decreased for all muscles, comparing pre- and post- evaluations at baseline and end-point. Heart rate between groups had no statistical significance. LLLT increased RM and reduced EFI, compared with the placebo group, which is helpful for high performance that demands a fast return to a normal state and less tiredness [29].
Recently, Florianovicz et al.—in a randomized controlled trial—studied the effects of two distinct PBMT protocols (red 660 nm vs. infrared 830 nm) combined with a blood flow restriction (BFR) training arrangement in wrist extensor muscles on handgrip, wrist extension force, and electromyographic comportment. Fifty-eight volunteers (clinically healthy women, aged 18–25 years old) were randomly divided into 4 groups: (1) control; (2) BFR (strengthening with blood flow restriction); (3) 660 nm + BFR; and (4) 830 nm + BFR. The hypothesis was that PBMT + BFR would increase muscle strength gain. Handgrip strength, wrist extensor muscle strength, and electromyography (EMG) of the radial carpal extensor muscle were recorded. A statistically significant increase was obtained for handgrip strength in the 660 nm group compared with the 830 nm group, and for wrist extensor strength in the 660 nm and BFR groups compared with the control group. The best increase was found for the 660 nm (red) group comparatively with the control, BFR, and the 830 nm (IR) group. Joining PBMT (660 nm) and BFR was effective for growing the handgrip strength of the wrist extensors, related to an enhancement of the electromyographic behavior [30].
Miranda et al. [31] projected in a laboratory setting, a cross-sectional study that included 20 unprepared and unexperienced male participants to receive PBMT with super-pulsed lasers combined with LEDs and to evaluate the muscle efficiency resulting from the gradual cardiopulmonary attempt on the treadmill. Subjects were administered PBMT with a 12-diode cluster in 17 points (30 J/site) on each lower limb, either with combined superpulsed lasers and LEDs, or with placebo at one session, and vice versa at the next session, and completed a cardiopulmonary test on a treadmill each time. They were evaluated for: distance traveled, time to exhaustion, and pulmonary ventilation, all three parameters that increased after effective PBMT, as well as for the dyspnea score, which decreased for real PBMT, compared to placebo.
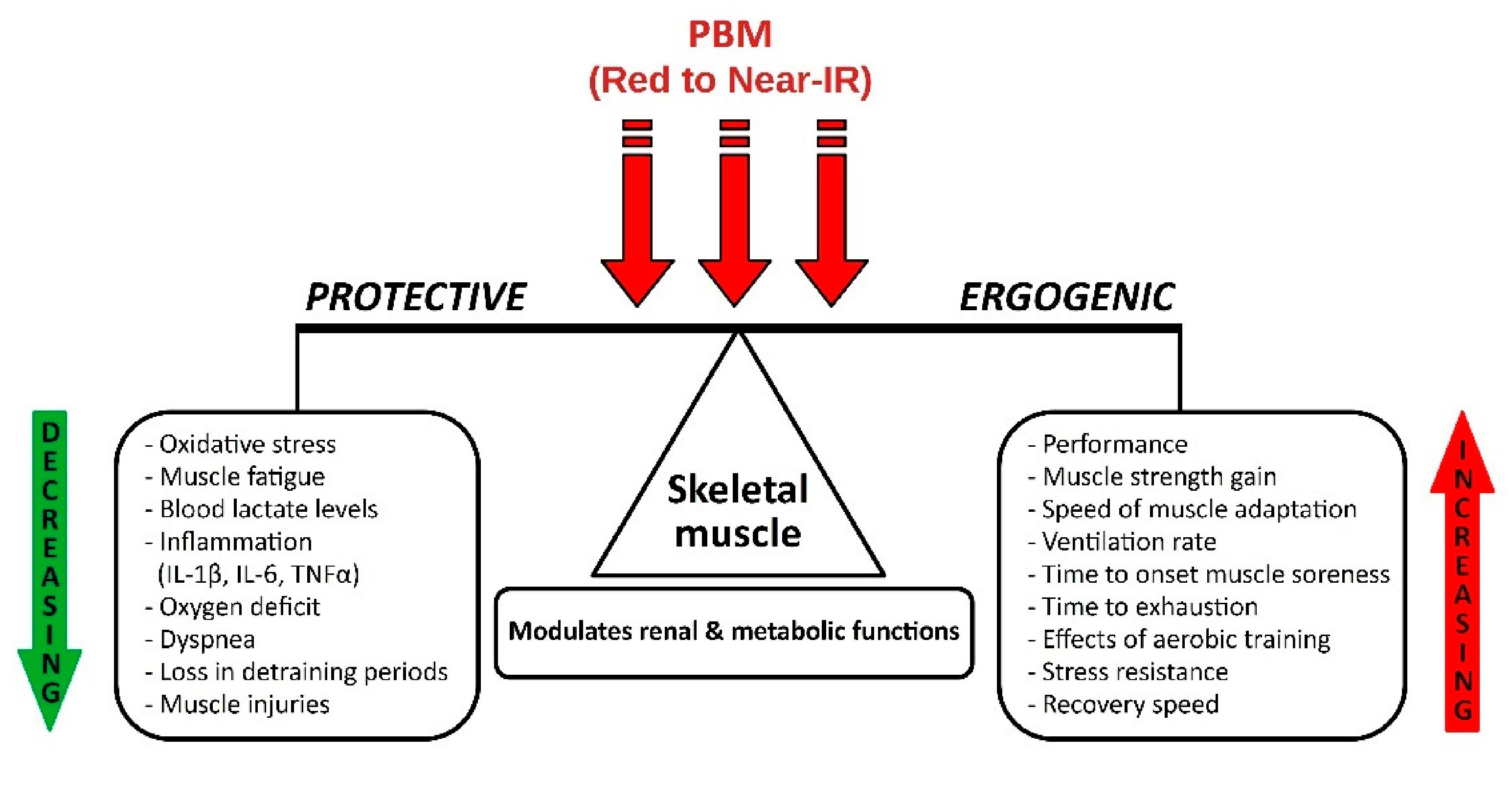
A synthesis of the multitude of interdependent positive effects of PBM action in physical activities and sports, especially the plethora of ergogenic and protective properties, scientifically demonstrated by the positive studies analyzed, is illustrated in the original diagram designed and presented in Figure 2.
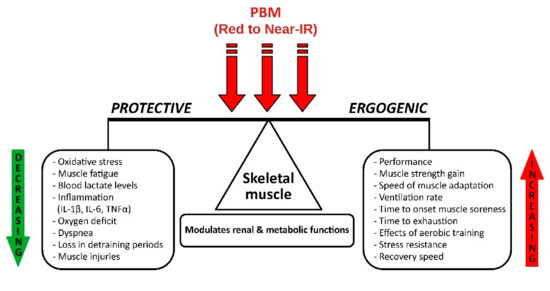
Figure 2.
Effects of PBM on skeletal muscle in physical activity and sports.
Photobiomodulation from red to near infrared had ergogenic effects by increasing performance, muscle strength, speed of muscle adaptation, ventilation rate, time to onset muscle soreness, time to exhaustion, effects of aerobic training, stress resistance, and speed of recovery.
As protective effects, PBM decreased oxidative stress, muscle fatigue, blood lactate levels, inflammation (IL-1, IL-6, TNFα), oxygen deficit, dyspnea, losses during periods without training, and muscle injuries. PBM modulates renal and metabolic functions.
3.2. Studies with No Effects of PBM
Fourteen studies were included in this analysis (see Figure 1).
PBMT is used today as a possible ergogenic aid for exercise performance [32] because it is believed that PBMT could have positive effects on mitochondrial enzymatic activities for ATP release [33], with beneficial effects in potential increased phosphocreatine resynthesis [34].
An increasing number of recently published studies have demonstrated the positive results of the acute application of PBMT on performance endurance exercises [31,35]. Although the way in which it acts and the exact mechanisms by which PBMT works successfully in increasing endurance performance in athletes are not completely elucidated, it is still considered that mitochondrial metabolism plays an essential role in this process [34,36].
PBMT through the released energy could activate the mitochondrial complex IV, increase the flow of electrons in the respiratory chain and the concentration of H+, with beneficial consequences in the high synthesis of ATP that more vigorously supports cellular activities [36] and better exercise results [37].
On the contrary, many other studies are published, some even recent, but without effects, as will be discussed below.
Dutra et al. [38] in a randomized, crossover design on 13 untrained healthy men, investigated the effects of PBMT administered 30 min or 6 h before cycling, analyzing plasma nitrogen concentrations, blood acid-base equilibrium, K+, and lactate concentrations, as well as cardiorespiratory responses were monitored during exercise. PBMT was applied to the quadriceps, hamstrings, and gastrocnemius muscles of both limbs using a multi-diode array (11 cm × 30 cm with 264 diodes) at doses of 152 J or false irradiation (with the device off, placebo). The authors demonstrated that PBMT did not improve exercise-induced changes in cardiorespiratory responses or metabolic blood markers, nor time to exhaustion during the severe intensity cycling performed by untrained men.
Malta et al. [39] investigated the effects of PBMT on muscle recovery based on inflammation (IL-10, TNFα), markers of muscle damage (CK), LDH, DOMS, and counter-current jumping (CMJ) after two sprint interval training (SIT) sessions compared to placebo (part I) and PBMT efficacy with active recovery (AR) and cold-water immersion (CWI) [part II]. PBMT with 56 diodes 660 nm and 48 diodes 850 nm was applied at a total energy of 600 J (300 J per foot in 5 spots). In Part I, a time effect was found with increases in LDH, CK, and IL-10, as well as a decrease in DOMS to 72 h compared to 24 h. In Part II, an increase in CK and IL-10, while DOMS decreased to 48 and 72 h compared to 24 h. In summary, PBMT had no effect on inflammation, muscle injury, CMJ, or DOMS performance after two consecutive sprint interval training sessions compared to placebo, CWI, and AR strategies.
The stretching-shortening performance of the lower limb muscles during training or competition in athletes is influenced by fatigue and muscle damage. PBMT is used as a strategy to alleviate fatigue and muscle damage when applied before different types of exercises. In a placebo-controlled study, Orssatto et al. [40] investigated the effects of PBM (LASERs 850 nm, LEDs 670 nm, LEDs 880 nm, LEDs 950 nm; number of diodes = 33) applied to 15 lower limb sites with a dose per site of 30 J and a total dose of 450 J (Quadriceps = 240 J, Hamstrings = 120 J, and Gastrocnemius = 60 J). There was no effect of PBMT before exercise to reduce lower limb muscle fatigue and damage during and following a stretch-shortening cycle protocol in judo athletes. In another randomized cross-over, placebo-controlled, and double-blind design study on fourteen well-trained adults, Orssatto et al. [41] investigated the effects of PBMT on endurance training and the generated pain. PBMT (60 J per site, 6 sites per member, total dose = 360 J) was used to reduce tiredness. PBMT has not been helpful in increasing volume or reducing discomfort during resistance training and conducted to concentric failure to well-trained participants.
In another two studies (study 1 with 14 male cyclists and study 2 with 13 cyclists), pseudorandomized and balanced crossover performed by Dutra et al. [42] analyzed the ergogenic effects of two doses of PBMT (18 × 38 cm matrix with 200 diodes, at doses 260 J and 130 J or 0 J for placebo) applied before exertion, on markers of respiratory and muscular activity, blood-base acid, ion and lactate concentrations, indicators of muscle fatigue (global, central and peripheral) and time to exhaustion in the severe cycle. In conclusion, it is shown that PBMT at doses of 260 J and 130 J had no beneficial effects on muscle fatigue, cyclic performance, metabolic parameters, and muscle activity in men with recreational cycling.
Santos et al. [43] in a counterbalanced randomized crossover design (one week between PBMT/placebo (SHAM) at thirteen amateur futsal players, evaluated the effect of previous acute application of PBMT (diodes: 69; wavelength: mixed, 34 diodes 660 nm and 35 diodes 850 nm; CW, cluster area: 44.2 cm2; optical output: 53 mW/cm2; spot site area: 0.234 cm2; dose: 200 J; energy density: 4.5 J/cm2) on the performance of high and intermittent intensity exercises, muscle oxygenation, and physiological/perceptual indicators. Overall, PBMT before a battery of physical tests did not alter the performance of high and intermittent exercise, nor the physiological and perceptual responses in amateur futsal players.
As the authors claim, this research used CMJ as an essential parameter in the assessment of neuromuscular fatigue and at the same time is the first study to test the influence of PBMT in physical recovery after intense exercise performed on an ergometric cycle. Results of this research are similar to those published by Malta et al. [39] in the sense that no improvement in CMJ performance was observed after PBMT at doses of 200 and 300 J, i.e., at 4–5 J/cm2. Although the site chosen for local application of PBM was most appropriate in stimulating the muscle group participating in physical activity, the “ideal dose” remains the most important issue because it is not known exactly which would be most appropriate.
In many sports activities, hamstring strain injury (HSI) is the most common non-contact injury [44] and through classic rehabilitation programs [45] many athletes return to sports with a low level of performance and high risk of recurrence [46] of the disease.
Muscle injuries caused by physical activity are repaired both structurally and functionally slowly. Experimental animal studies have tested the positive biochemical and histological effects of PBM [47,48]. The use of PBM in experimental models began immediately, i.e., in the first 24 h after muscle injury, the time essential for intervention on the inflammatory process [49]. This hypothesis could explain the inefficiency of PBMT reported by Medeiros et al. [50] following a randomized controlled study with 24 amateur athletes who received adjunct therapy PMB (859 nm, 100 mW, CW, 5 diodes, 30 J site for 3 sites) for functional rehabilitation of the HSI produced through an intense program of physical exercises, 48 to 96 h ago. As the authors point out, the published study has limitations: first, the two-arm design prevented them from identifying whether other doses of PBM would have had different effects on the results; second, no patient-reported outcome measures were used, and ultimately, the number of participants did not constitute a large-scale study.
Mechanisms by which PBM regulates ergogenic activity are supported by the fact that radiation emitted in the red and near-infrared is absorbed into the cell by subcellular chromophores in the mitochondria [51]. Then, the enzyme cytochrome C oxidase is activated, which stimulates the production of ATP in the mitochondrial respiratory chain and thus will stimulate fiber maturation and muscle repair through increased synthesis of myoregulatory factors such as myogenin and MRF4 [52,53]. As already shown in the study published by de Oliveira et al. [14], PBM can induce muscle protection in athletes through the action of reducing inflammation and CK levels [54] produced during physical activity.
Results of the PBMT depend on many factors, among which we mention the parameters of the devices to work with: wavelength, fluency, illumination time, spot size, and the method of delivery (e.g., contact, punctual, wide beam). Among the mentioned PBM parameters, the ones that matter the most are the estimated power density in mW/cm2, and the fluence expressed in J/cm2 [55].
Ghigiarelli et al. [56] included twelve men in a randomized counterbalanced crossover project, and examined the effects of PBMT (mixed, 660 nm and 850 nm, with 2800 diodes, total energy emitted in 15 min 473 J, respectively 400 J) administered for 15 min immediately before and after high-intensity resistance training. They measured CK and IL-6 levels. Finally, PBMT did not significantly reduce the activity of salivary IL-6 or CK concentration during post-intensity recovery endurance training for 24 to 72 h. These negative results could be explained, according to the authors, by not using the recommended doses of 60–300 J for large muscle groups and 20–60 J for small muscles suggested by Leal-Junior et al. [57].
PBM has begun to be used in athletes as a recent way to prevent muscle injury and pain after strenuous physical activity [58,59]. As already mentioned, this treatment is scientifically based on the assumption that PBM stimulates mitochondrial chains and the cytochrome C oxidase enzyme, which increases ATP production and thus delays muscle fatigue and protects muscle from injury [60,61]. PBM stops the release of muscle damage markers (LDH and CK), proinflammatory protein production (CRP), improves the oxidative system, and increases muscle plugging power [62,63]. Studies on the effects of PBM on muscle performance and fatigue, with various protocols related to wavelength, power density, irradiation time, and laser light sources still reported discordant results [64,65].
In a double-blind, placebo-controlled randomized clinical trial, Yekta et al. [65] investigated the effect of PBM on muscle strength and endurance and post-exercise recovery of 50 young adults aged 20 to 35 years. The first group received pre-exercise laser at 810 nm, 60 mW, and 60 Hz frequency for 30 s on the three-point rectus femoris muscle. The influence of PBM on lactate level, weight repetition, fatigue, and muscle pain in both the treatment group and the placebo group was studied. The authors conclude that taking PBM before exercise can improve muscle performance and reduce muscle pain and fatigue.
In a double-blind crossover design study, placebo-controlled with 15 moderately active and healthy males, Malta et al. [66] investigated the acute effects of PBMN using cluster light-emitting diodes (LEDT; 104 diodes) (wavelength 660 and 850 nm; energy density 1.5 and 4.5 J/cm2; energy 60 J at each point; total energy delivered 600 J) on the maximal deficit of oxygen (MAODALT) and time to exhaustion, during a high-intensity running effort. No significant differences were found for the values of oxygen equivalents from each energetic metabolism between PBMT subjects and placebo, or for the time to exhaustion, except for the respiratory exchange ratio. PBMT after a high-intensity running effort did not alter the MAODALT, metabolic energy pathways, or high-intensity running performance.
Peserico et al. [67] investigated the effects of PBM on endurance training in thirty untrained individuals in a randomized, placebo-controlled study. PBMT was administered in 5-foot locations, with a dose of 60 J at each point and a total energy delivered per foot of 300 J, using LED equipment with 56 red light (660 nm) and 48 infrared (850 nm). The authors claim that the results of the research parameters in the two groups did not vary significantly, but in sports, a small boost can separate the winner from the loser. The inferential analysis did not show clear significant differences in Vpeak and t5-km for the PBM group compared with placebo, and only a moderate effect in relieving muscle pain in the third week of training.
In another randomized, parallel, and double-blind study in 13 young male athletes, Zagatto et al. applied whole-body photobiomodulation therapy or placebo after official water polo matches and investigated the markers of inflammation, hormonal responses (testosterone and cortisol), heart rate variability, maximal voluntary contraction, squat jump, and the muscular damage. Whole-body PBMT had no effect in improving hormonal and cardiac responses or recovery from the inflammatory muscle damage, except a decrease in LDH, but only after one match [68].
Segabinazi Peserico et al. investigated in 15 physically active males in a randomized, crossover, double-blind, and placebo-controlled study, the acute effects of PBM [56 diodes of red light (660 nm; 50 mW/cm2 and 1.5 J/cm2 each diode) and 48 diodes of infrared light (850 nm; 150 mW/cm2 and 4.5 J/cm2 each diode)] using different doses, as follows: 30 J per area (PBM1), 120 J per area (PBM2), and 180 J per area (PBM3) applied in two regions of the quadriceps muscle, two regions of the femoral biceps muscle, and one region of the gastrocnemius muscle in both legs, performed 5 min before the maximal incremental treadmill tests for the determination of peak running velocity (Vpeak) and other physiological parameters. Various doses of PBMT did not alter Vpeak and other physiological and perceptual parameters in any of the four groups [69].
Dellagrana et al. studied the running performance at 1500 m and the individual response capabilities of nineteen recreationally trained runners in a randomized, crossover, double-blind, placebo-controlled trial, applying PBMT (or placebo) 30 J per site, with a total energy dose of 840 J, in 14 sites per lower limb immediately before the stopwatch test, using a mixed-wavelength device [33 diodes: 5 LASERs (850 nm), 12 LEDs (670 nm), 8 LEDs (880 nm), and 8 LEDs (950 nm)]. In this experiment, PBMT applied immediately before running did not improve the performance of runners at 1500 m, however, 10 participants had only a higher aerobic capacity than those who did not respond at all [70].
Moreover, Abreu et al. included 30 healthy, physically active young men in a randomized, double-blind, placebo-controlled, crossover study with two equal arms: PBMT (60 J; 1152 mW; 52 s; and 166.75 cm2) applied to brachial biceps through a flexible series of LEDs and placebo, investigating the time response (5 min, 1 h, 3 h, and 6 h) of PBMT on maximum torque (PT), torque development rate (RTD), fatigue strength and subjective perception of effort in maximal voluntary isometric contractions (MVIC) of elbow flexion. PBMT by LEDs was performed using a flexible array of 132 LEDs, as follows: 60 red LEDs (635 ± 10 nm; 1.2 mW), 72 IR LEDs (880 ± 20 nm; 15 mW), with 4.7 kHz emission frequency and an effective irradiation surface of 166.75 cm2. PBMT failed to increase muscle performance, nor did it reduce fatigue [71].
Regarding the influence of PBM on the chronic effects of endurance running training, research is needed to analyze the result on biomarkers related to muscle pain, inflammation, and oxidative metabolism, depending on the doses administered.
A summary of the no-effects studies included in this review, discussed above, is presented in Table 2.

Table 2.
PBM in human studies without effects.
4. Discussions
PBM applied in sports offers a special chance to support the modeling of the performance both of amateurs and athletes for better training and, also, for excellent results in high elite competitions.
Increasingly complex physical activities and fierce competition in the world of sports generate a state of psycho-emotional and physical stress that can induce chronic fatigue syndrome, failure in physical training, predisposition to muscle and other tissue damage, low capacity, physical and emotional exhaustion, and the setup of different other diseases.
The biggest questions about PBM applied in sports are still open, as follows [10]:
- -
- Optimal wavelengths, optimal time, before or after, or both, and at what interval of physical activity?
- -
- Optimal PBM parameters (power density, fluency, modulation frequency)?
- -
- The number of points for each muscle?
- -
- The interaction of PBM with muscles and the chain of biochemical reactions triggered inside cells and ultimately reflected in increased performance in sports?
- -
- Considering the notorious biphasic dose response, typical of PBM and its interaction with muscles, i.e., could it be managed, controlled or achieved without great difficulty to apply exactly as much energy as we need and not too much irradiation?
- -
- Is it right to combine different light sources, i.e., both lasers and LEDs?
Optical profile (or focus on different deep tissues) affects the power density in tissue and should be addressed in clinical trials, as it may influence the effects of PBM.
PBM in sports, even it is a controversial subject, has real effects as a non-invasive therapy that works at different levels in the human body, causing chemical reactions of light in cells, tissues, treated organs, and even throughout the body, via the immune system, nervous system, etc.
However, so far, the use of PBM in increasing performance and athletic recovery is mainly affected by inconsistency in research, lack of standardized protocols, comparing the results of studies conducted on amateurs, with others on elite athletes, but also on different sports, etc., as we found in this review.
For recovery and for achieving high levels of performance, specific metabolic needs of the athlete must be met, dictated by the nature of the practiced sport.
During sports, intense muscle mobilization causes the release of chemical mediators with pro-inflammatory activity, by increasing the level of lactate and creatine kinase in the blood, which will cause pain, muscle fatigue, local hypoxia, change in electrolytes and membrane potentials, with consequences in the muscular recovery and the subsequent performance of the athlete [72]. With respect to the decrease in the chemical mediators in the blood (lactate and CK), PBM is effective when applied pre-exercise or post-exercise, but the lowest level of these blood parameters was found in some studies when is applied post-exercise [12,73,74].
Of all the means, as we found in the studies analyzed in this review, the best protective and ergogenic effects were obtained by using high-performance PBM applied with doses between 10–60 J, especially before exercising.
Very recent research has studied the immediate effects of exercise on antioxidant proteins, such as Nrf2 (nuclear factor erythroid 2-related factor 2), naturally present in living organisms, with a safeguarding function against oxidative stress, whose number grew very quickly after several tens of seconds of physical activity [75], and future research is also aimed at long-term reactions, i.e., such chronic reactions to training.
Nrf2 activity multiplicates with physical activity and is necessary for the basic activity of mitochondria and for the synthesis of specific mitochondrial proteins after training, providing cellular defense by upregulation of enzymes that inhibit the production and accumulation of ROS in striated muscles [76].
Nrf2 is a key regulator of the endogenous defense system in cells, ruling the expression of hundreds of cytoprotective proteins, in addition to many antioxidant enzymes [77].
Experimental animal research (Table 3) supports the beneficial effects of PBM applied before and after exercise in physical activity, through improved performance in endurance training [78,79], decreased level of proinflammatory cytokines [80,81,82,83,84], positive effects on aerobic metabolism [85,86], oxidative stress [86,87,88] and increased ATP [89,90]. Histopathological examination performed after PBM showed that it can protect myonecrosis, reduce pro-inflammatory cell infiltration, muscle destruction, inflammation and can help accelerate tissue repair [91,92,93].

Table 3.
Effects of experimental PBM on animals.
Six other animal studies with positive effects of PBM and improved muscular function in a dose- and wavelength-dependent manner, the last of which with a simultaneously applied static magnetic field, are presented below [94,95,96,97,98,99].
In an experiment conducted by Leal-Junior et al. to evaluate the effects of preventive treatment with superpulsed LLLT (904 nm, 15 mW, 700 Hz, 1 J) or placebo-LLLT at one point overlying the tibialis anterior muscle (bilaterally), 5 times per week for 14 weeks on the progression of dystrophy in ten mdx (with a point mutation within the dystrophin gene) mice, randomly divided into two experimental groups, studying the morphological changes, creatine kinase (CK) activity, and mRNA gene expression, proved to decrease morphological changes, skeletal muscle damage, and inflammation, therefore, LLLT has potential to decrease the progression of Duchenne muscular dystrophy [94].
A subsequent study by Silva et al. showed that mdx mice treated with LLLT (808 nm, 30 mW output power, 1071 W/cm2 power density, 3 J/point, 100 s) at a single point of gastrocnemius muscle of the hind paw showed significantly lower levels of creatine kinase and oxidative stress than controls, when subjected to high-intensity forced exercise on an electric treadmill, had a beneficial role on the performance of skeletal muscle, but LLLT could not change the morphology of dystrophic muscles [95].
In a very recent study, Tomazoni et al. investigated comparatively the influence of PBMT and anti-inflammatory drugs following a diversified protocol in mdx mice. Finally, the researchers concluded that only PBMT treatments in combination with corticosteroids or nonsteroidal anti-inflammatory drugs gave promising and optimistic results in the skeletal muscle of mdx mice. Therefore, it opens up a possible future alternative in the treatment of Duchenne muscular dystrophy [96].
In an investigation conducted by Santos et al. which aimed to evaluate the effects of PBM immediately before tetanic contractions in the development of skeletal muscle fatigue and possible tissue damage in rats, which received 1, 3, or 10 J with three lengths of different wavelengths (660, 830 and 905 nm) before six tetanus contractions induced by electrical stimulation, it was shown that the doses of 1–3 J/660 nm and 1, 3 and 10 J/905 nm provided the best results, protecting skeletal muscle tissue against damage, i.e., the combined use of wavelengths can have therapeutic advantages [97].
A study by Albuquerque-Pontes et al. by applying LLLT before exercise with different doses (1, 3, and 10 J) and distinct wavelengths (660, 830, and 905 nm) with a power of 50 mW on healthy intact muscles in rats, showed an increase in cytochrome c oxidase expression and the delayed onset of fatigue, in a dose- and wavelength-dependent manner. The authors believe that the simultaneous combined use of different wavelengths can increase the performance of skeletal muscle in different conditions [98].
In another study, Albuquerque-Pontes et al. demonstrated that PBMT and a simultaneously applied 35 mT static magnetic field had positive effects, stopping the degradation of skeletal muscles and delaying the progression of Duchenne muscular dystrophy and thus paving the way for new possibilities for the non-pharmacological treatment of this genetic disease by modulating dystrophin gene and protein expression [99].
Over the last decade, the ergogenic effects of PBMT performed with laser diodes or LEDs have been shown to increase athletic performance and speed up recovery after training. Yet, many of these repercussions, as well as the complex clinical applications are still incompletely known. Some positive effects were also obtained by simultaneously applying PBMT and static magnetic fields, which we considered in this review [100,101,102,103].
It is not well known how the magnetic field acts at the subcellular level simultaneously with PBM, which directly modulates mitochondrial activity. Indeed, mitochondria stimulated by PBM play an important role in muscle recovery but concerning simultaneously static magnetic field exposure we do not know to date the exact role it plays in living cells. Future and more standardized studies are required for a better understanding of the molecular mechanisms underlying PBM and magnetic field potential challenges in order to improve research strategies.
Some studies have tried to use devices with high-power laser/light and short irradiation time. To date, high-power laser/light research is rare, the effects are not yet fully understood, and it is possible that the high-power laser/light in a very short time will cause unforeseen muscle damage to elite sportsmen (estimated at USD millions), on long-term. In a study by De Marchi et al., the low-power pulsed laser/light showed better results than the low-power continuous laser/light or the high-power continuous laser/light on a group of forty untrained healthy male participants. It is possible that muscle cells and subcellular organelles need time to organize and use a large amount of received photoenergy and cannot receive as much energy in a very short time, but only quantified. This study clearly demonstrated that high-power continuous laser/light had no effect on improving performance or post-exercise recovery [104].
Application of PBM lacking conclusive positive results or without effects in the analyzed studies was discussed in each paper by the authors (the majority of these studies was published by the same research group) and the causes were multiple, among which we mention:
- -
- Most authors consider that the optimal parameters of PBMT (wavelength, output power, energy density, energy per stimulated point, total energy delivered, the optical profile or the shape of the beam emitted by the probe, etc.) are not strictly stipulated, but only in intervals of acceptance or recommendations.
- -
- Another important influencing factor was the multitude of devices for PBM applications in sports (cluster, single or multiple diodes, etc.), from which researchers could choose.
- -
- In some studies, researchers have failed to measure vessel diameter and local microcirculation in order to draw an objective conclusion on the impact of PBM.
- -
- The effectiveness of PBM in improving sports performance is supported by some studies, but not all findings are consistent, as the PBM doses used in simple joint tests may not be sufficient for other complex sports, for example, cycling. Doses of PBM and the exercises adopted in some studies did not correspond to the complexity of the sport investigated, in order to increase the performance.
- -
- The motivation for the lack of PBM effects in some studies was related to the choice of the study group as training level (amateur or elite), differences in adaptive muscle structure and cellular bioenergetics, age, sex, skin color, subcutaneous adipose tissue structure, etc.
- -
- Other factors involved in the results obtained were the time (before/after, or both) chosen for PBM stimulation in relation to the exercises protocol, the evaluation times of PBM effects but also of physiological parameters, well-controlled recovery methods between two successive tests (for example, the quantity and quality of sleep between two experimental sessions), accumulation of fatigue from one exercise test to the next, etc.
- -
- Some studies did not perform histopathological muscle examinations, and others did not perform all the blood collections necessary to draw relevant conclusions at the right time.
In terms of results carried out with whole-body PBM devices, these did not produce positive outcomes, as reported by Ghigiarelli et al. [56], or other researchers in a very recent study [68].
The underlying mechanisms of muscle injury are not universal due to inter-subject variability and training programs, and the previous muscle damage, the so-called “repeat bout effect” provides resistance to subsequent damage, therefore, in their experiment, Ghigiarelli et al. found the presence of the above-mentioned effect from week 1 to week 2, which may have attenuated the possible positive effects of PBMT. Meanwhile, the control treatment for different parts of the body was not possible because PBMT was performed with a bed, applied to the whole body and not to the limbs individually. In the future, the authors suggest the implementation of extended washing periods of at least 4 weeks or the use of parallel groups. Limitations to be considered in this study were a great between-subject variability post-exercise for salivary IL-6, lack of blinding of PBMT to the participants and primary investigator, absence of direct contact with the skin/target tissue of the PBM whole-body device, and the presence of the repeat bout effect [56].
Therefore, we consider that whole-body PBMT has as its main limitation the lack of contact with the target tissue, and the optical profile (or focus on different deep tissue) affects substantially the power density in the muscles and the modulation of the mitochondrial activity, and so the effects of the whole clinical trial are corrupted.
In addition, in a series of three studies recently published in 2020 in the same volume and issue of the journal Photobiomodul Photomed Laser Surg., the results of PBMT were negative [69,70,71], although a study with positive effects was published here, too [30].
There is an urgent need to improve PBM devices and delivery methods. Recently, Hanna et al. [105] demonstrated an improved cell growth and differentiation of the osteoblasts with treatments using a flat-tipped hand-piece profile in comparison with the standard Gaussian probes, and that the treatment power varied greatly by moving the standard gaussian probe from the position in contact, at several centimeters away. The huge therapeutic potential of PBM has been very recently reaffirmed in a new article published by Amaroli et al. The authors designed a novel hand-piece with a flat-top beam profile of irradiation and they compared it with other classical beam profiles, investigating the effects on mitochondrial activity (by assessing ATP synthesis) and the mitochondrial damage. The uniform distribution of the power density with this new flat-top prototype increased homogenously the production of ATP, both in the center and the edges of the beam, so using an optimum optical profile can improve the rigor and reproducibility of PBM clinical outcomes [106].
Recently, Leal-Junior et al. published some current clinical and scientific recommendations and future directions for the application of PBMT in sports. In this masterclass article, the authors, as pioneers in the field, analyzed the exponential progress made over a decade since the publication of the first randomized controlled trial on improving athletic performance and accelerating post-exercise recovery by applying PBMT to date, based on the most obvious scientific evidence with meta-analysis and randomized controlled trials. All the guidance and directions presented are only for youth/adult healthy participants, using lasers and/or LEDs. It is recommended that devices for the application of PBMT have wavelengths between 640 nm–950 nm, more recently combined simultaneously red and infrared, pulsed or continuous mode, with a power of 50–200 mW per diode (individual probes) and 10–35 mW per diode (for cluster probes), without caloric effects, in direct contact with the tegument with a slight pressure. The doses that should be applied are 20–60 J for small muscle groups and 60–300 J for large ones, at least 30 s per point, from 5 min to 6 h before physical exercises. The authors recommend that all future experiments comply with this guide [57].
In a Guest Editorial, Ferraresi C. made valuable comments on the action of PBMT with lasers and/or LEDs in sports, starting on the historical vein with the first concrete examples that had no obvious positive effects, followed a decade by two other representative studies on rats, which opened the premises of the two main modalities of applying photobiomodulation today on skeletal muscle, before and after physical exercise. The author mentions that the first two randomized clinical trials (RCTs) published simultaneously in 2008, were followed by numerous other randomized clinical trials or in vivo laboratory studies that have shown as following main effects of PBMT improved exhaustion resistance, higher peak torque, or maximum force, and prophylaxis of muscle injuries. In addition to the mechanisms of action of PBMT being highly introspected, two other essential aspects have been intensively researched: the beneficial therapeutic window, i.e., the dose–response, and the temporal physiological response in case of prior application of PBMT to physical exercises. Based on updated publications, the energy therapeutic windows for acute responses are 20–80 J (small muscle groups) or 56–315 J (large) and 18–240 J in chronic responses; and a time window of 3 to 6 h for preconditioning. Contradictory results of the published PBMT efficiency are based more only on the analysis of the applied energy (J), but not on the way of supplying this energy, i.e., high or low power (W) in a short or longer time (s), which depend on the characteristics of so many devices applied in sports (laser probes, LED probes, group of LEDs or plus laser diodes, matrices displayed in the form of blankets, LEDs plus laser diodes combined with magnetic field therapy and, more recently, light beds for full-body PBM), with different irradiation areas and especially, diverse energy densities [107].
Published papers analyzed in this review reveal the important link between the applied dose, but especially its deep penetration into the tissue (optical profile), which remains an open problem to be optimized and applied creatively in sports reality, which covers as an umbrella of different sports, the diverse exercise protocols, various subjects involved in the research (athletes or amateurs), trained or untrained, different in age, sex, healthy, or with various diseases.
A permanent supply of muscle cells with ATP during sports activities modulates sports performance from very short times (seconds) to several hours, so it is necessary to activate other metabolic pathways, “anaerobic” and “aerobic” to resynthesize ATP so necessary, adapted to the intensity and duration of exercise. PBM has been shown in some studies to interfere with muscle metabolism with ergogenic benefits in sports activities. However, scientific approaches to whole-body exercise metabolism are either physiological or, more recently, through intricate analysis of cell signaling and molecular changes, which use integrated elements of genomics, proteomics, metabolomics, and systems biology in complex statistical evaluations to reveal molecular aspects of the exercise metabolism. Many questions remain open about optimal training interventions and the potential for manipulating metabolic responses, for example, through PBM, for ergogenic benefits and athlete success [1,3].
The effectiveness of PBM is not always easy to demonstrate and comprehend because its effects are present but may occur later and are not always obviously expressed. Understanding the mechanisms of action of PBM at the molecular and cellular level will allow researchers to more accurately establish optimal parameters for benefits in sports [108]. These are based on the processes of mitochondrial fission and fusion that are permanently dynamic and make the mitochondria lastingly adapt their function to the cellular requirements [109].
The best athletes bring meaningful information about their own high health costs that they “pay” in competitions or intense physical training. Regular exercise is beneficial, but strenuous competition and extreme physical training sessions could lead to significant metabolic disorders. Extremely intense exercises affect mitochondria, the cellular bioenergetic powerhouses, and decrease the body’s ability to regulate various physiological parameters in the blood. Mitochondrial impairment is associated with other dysfunctionalities [110].
Flockhart et al. studied the link between the muscular effort during physical training and the body’s response in healthy subjects, which satisfies a dose–response connection. There is a metabolic disadvantage of excessive exercise because it affects the mitochondria and reduces the body’s ability to regulate carbohydrates in the blood. Sports performance improves as the intensity of training increases, and at the same time there is an acceleration of energy production by mitochondria; at a certain level of physical effort, there is stagnation and even a decrease in performance, simultaneously with the disruption of mitochondrial activity, which decreases drastically in strong workouts, aspects proven on muscle biopsies. The research was performed on both professional athletes during endurance training but also on amateur, non-athletes. This reduction in mitochondrial activity coincided with affecting the body’s ability to metabolize glucose in the blood. Professionals showed a higher level of carbohydrates in the blood over a longer period than amateurs did. In conclusion, extreme training results in decreased performance, it induces significant mitochondrial respiratory breakdown, which is well correlated with low glucose tolerance, but despite all this, the parameters of global oxidative stress remained unchanged [110].
Multiple differences between the devices with which PBMT can be applied, constantly growing through new inventions in laser/LEDs technology and the manufacturing industry, the total amount of laser/light energy that can be used in therapy, the energy density applied to muscles, and more recently the importance of the optimum optical profile (or focus on different deep tissues) that affects the power density in tissue, and especially the mitochondrial activity, the ATP synthesis, and the mitochondrial repair, should be addressed dedicated in the future clinical trials.
Uniform distribution of the power density with the newest flat-top probes could increase homogenously the production of ATP within each cell, so using an optimum optical profile for rigorous contact and quantum-controlled muscle photobiomodulation, could improve in the near future the rigor and the reproducibility of clinical outcomes.
Many other scientific studies are still needed to elucidate all the real effects of PBM in sports, which could benefit from the unprecedented technological evolution in recent years, and which would reveal new aspects of the influence of PBM from the molecular, to the whole-body level.
5. Conclusions
Of all physical factors applied for the modulation of sports activities and rehabilitation, PBM has the most valuable proven protective and ergogenic effects, being the key to success for high performance and recovery.
PBMT with no conclusive results or without effects from this review was analyzed and we found the motivations of the authors from the perspective of multiple causes related to technological limitations, participants, the protocols for physical activity, the devices, techniques, and PBM parameters.
It is possible in a short time that PBM applied creatively and targeted depending on the sport and the size of the level of physical effort to perfectly modulate the mitochondrial activity and thus lead to remarkable improvements in performance, coupled with the molecular energy processes in muscle cells and their energetic inner powerplants, the regenerative mitochondria.
In the near future, dose–response experiments on physical activity should be inspired and correlated with PBM dose-response studies, so that quantification of PBM parameters to allow the energy, metabolic, immune, and neuro-endocrine modulation, perfectly coupled with the level of training.
There is an urgent need to continuously improve PBM devices, delivery methods, and protocols in new ingenious future sports trials.
Uniform distribution of the power density with the newest flat-top probes could increase homogenously the production of ATP within each cell, so using an optimum optical profile for rigorous contact and quantum-controlled muscle photobiomodulation, could quickly improve the rigor and the reproducibility of clinical outcomes.
Latest innovations and nanotechnologies applied to perform intracellular signaling analysis, while examining extracellular targets, coupled with 3D and 4D sports motion analysis and other high-tech devices, can be a challenge to learn how to maximize PBM efficiency while achieving unprecedented sports performance and thus fulfilling the dream of millions of elite athletes.
Author Contributions
Conceptualization, L.M.A.; writing and original draft preparation, L.M.A.; review and editing, G.L. and L.M.A. All authors have read and agreed to the published version of the manuscript.
Funding
TCM Research Center Graz (the research did not receive specific funding but was performed as part of the employment of the corresponding author at Medical University of Graz, Austria).
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Data Availability Statement
The original data and references used to support the findings of this study are available from the first and corresponding author upon request.
Conflicts of Interest
The authors declare no conflict of interest regarding the publication of this work.
Abbreviations
| AP | Aerobic performance |
| AR | Active recovery |
| AR | Androgen receptor |
| AT | Anaerobic threshold |
| ATM | Ataxia telangiectasia mutated |
| ATP | Adenosine triphosphate |
| CAT | Catalase |
| CB1 and CB2 | Cannabinoid receptors 1 and 2 |
| CBF | Cerebral blood flow |
| CCO | Cytochrome c oxidase |
| cDNA | Complementary DNA |
| CINC-1 | Cytokine-induced neutrophil chemoattractant-1 |
| CK | Creatine kinase |
| CMJ | Counter movement jump |
| COD | Crossover design |
| CON | Concentric |
| COX-1/COX-2 | Cyclooxygenases- 1 and -2 |
| Cr | Creatine |
| CS | Citrate synthase |
| CSA | Larger cross-sectional area |
| CW | Continuous wave |
| CWI | Cold water immersion |
| DOMS | Delayed onset muscle soreness |
| ECC | Eccentric |
| GAPDH | Glyceraldehyde-3-phosphate dehydrogenase primers |
| GPCRs | G-protein-coupled receptors |
| GPx | Glutathione peroxidase |
| HFD | High-fat diet |
| HI | Neonatal hypoxia-ischemia |
| HPRT | Hypoxanthine-guanine phosphoribosyl transferase |
| HR | Heart rate |
| HRV | Heart rate variability |
| HSI | Hamstring strain injury |
| ICC | Intra-class correlation coefficient |
| IL-10 | Interleukin 10 |
| IL-1β | Interleukin-1β |
| IL-6 | Interleukin-6 |
| IMP | Impulse |
| IR | Infrared |
| iVO2MAX | Intensity at which VO2MAX was reached |
| KET test | Knee extension test |
| La−P | Peak lactate concentration after exercise |
| LDH | Lactate dehydrogenase |
| LEDs | Light-emitting diodes |
| LEDT | Light-emitting diode therapy |
| LFD | Low-fat diet |
| MAOD | Maximal accumulated oxygen deficit |
| MAODALT | Alternative maximal accumulated oxygen deficit |
| MAP-2 | Microtubule-associated protein-2 |
| MCP-1 | Monocyte chemoattractant protein-1 |
| MDA | Level of malondialdehyde |
| MHFAKE | Maximal hip flexion active knee extension |
| MMPs | Matrix metalloproteinases |
| MOP | Mean output power |
| MPO | Myeloperoxidase |
| MRF4 | Myogenic regulatory factor (herculin) |
| MRS | Maximum running speed |
| mT | mili Testa (magnetic field) |
| mTOR | Mammalian (or mechanistic) target of rapamycin |
| MVC | Maximum voluntary contraction |
| myHC | Myosin heavy chain |
| NMES | Neuromuscular electrical stimulation |
| Nrf2 | Nuclear factor erythroid 2-related factor 2 |
| NSAIDs | Non-steroidal anti-inflammatory drugs |
| OA | Osteoarthritis |
| P200 | Performance of 200 m |
| P53 | Tumor protein p53 |
| PBMT | Photobiomodulation therapy |
| PCR | Polymerase chain reaction |
| PF | Peak force |
| PGE2 | Prostaglandin E2 |
| PNS | Peripheral nerve stimulation |
| PPO | Peak power output |
| PSLR | Passive straight leg raise |
| PV | Peak velocity |
| R | Red |
| RCT | Double-blind randomized controlled trial |
| REREX | Exhaustion respiratory exchange ratio |
| RCTs | Placebo-controlled randomized trials |
| RPE | Rating of perceived exertion |
| RPEex | Exhaustion perceived exertion |
| SIT | Sprint interval training |
| SJ | Squat jump |
| SLR | Straight leg raise |
| sMF | Static magnetic field |
| SmO2 | Muscle oxygen saturation |
| SOD | Superoxide dismutase |
| SSC | Stretch-shortening cycle |
| TAC | Total antioxidant capacity |
| TBARS | 2-thiobarbituric acid |
| TNF-α | Tumor necrosis factor-alpha |
| TRF1/TRF2 | Telomeric repeat binding factors |
| VCO2 | Volume carbon dioxide |
| VO2 | O2 uptake |
| VO2EX | Exhaustion oxygen consumption |
| VO2MAX | Maximal oxygen uptake |
| YYIR1 | YoYo intermittent recovery level 1 |
| 1-RM | Load in 1-repetition maximum test |
| 30 CJ | 30-s crossbar jump test |
| ↑ | Increase |
| ↓ | Decrease |
References
- Hargreaves, M.; Spriet, L.L. Skeletal muscle energy metabolism during exercise. Nat. Metab. 2020, 2, 817–828. [Google Scholar] [CrossRef] [PubMed]
- Atalay, M.; Hänninen, O.O.P. Muscle energy metabolism. Encycl. Life Support Syst. Physiol. Maint. 2010, 4, 26–47. [Google Scholar]
- Hawley, J.A.; Hargreaves, M.; Joyner, M.J.; Zierath, J.R. Integrative biology of exercise. Cell 2014, 159, 738–749. [Google Scholar] [CrossRef] [PubMed]
- Anders, J.J.; Lanzafame, R.J.; Arany, P.R. Low-level light/laser therapy versus photobiomodulation therapy. Photomed. Laser Surg. 2015, 33, 183–184. [Google Scholar] [CrossRef]
- Tsuk, S.; Lev, Y.H.; Fox, O.; Carasso, R.; Dunsky, A. Does photobiomodulation therapy enhance maximal muscle strength and muscle recovery? J. Hum. Kinet. 2020, 73, 35–144. [Google Scholar] [CrossRef]
- De Jesus, J.F.; Spadacci-Morena, D.D.; dos Anjos Rabelo, N.D.; Pinfildi, C.E.; Fukuda, T.Y.; Plapler, H. Low-level laser therapy in IL-1β, COX-2, and PGE2 modulation in partially injured Achilles’ tendon. Lasers Med. Sci. 2015, 30, 153–158. [Google Scholar] [CrossRef]
- Hamblin, M.R. Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophys. 2017, 4, 337–361. [Google Scholar] [CrossRef]
- Atri, C.; Guerfali, F.Z.; Laouini, D. Role of human macrophage polarization in inflammation during infectious diseases. Int. J. Mol. Sci. 2018, 19, 1801. [Google Scholar] [CrossRef]
- Marshall, R.P.; Vlková, K. Spectral dependence of laser light on light-tissue interactions and its influence on laser therapy: An experimental study. Insights Biomed. 2020, 5, 1. [Google Scholar]
- Ferraresi, C.; Huang, Y.Y.; Hamblin, M.R. Photobiomodulation in human muscle tissue: An advantage in sports performance? J. Biophotonics 2016, 9, 1273–1299. [Google Scholar] [CrossRef]
- Antonialli, F.C.; De Marchi, T.; Tomazoni, S.S.; Vanin, A.A.; dos Santos Grandinetti, V.; de Paiva, P.R.; Pinto, H.D.; Miranda, E.F.; de Tarso Camillo de Carvalho, P.; Leal-Junior, E.C. Phototherapy in skeletal muscle performance and recovery after exercise: Effect of combination of super-pulsed laser and light-emitting diodes. Lasers Med. Sci. 2014, 29, 1967–1976. [Google Scholar] [CrossRef]
- Vanin, A.A.; De Marchi, T.; Tomazoni, S.S.; Tairova, O.; Leão Casalechi, H.; de Tarso Camillo de Carvalho, P.; Bjordal, J.M.; Leal-Junior, E.C. Pre-Exercise Infrared Low-Level Laser Therapy (810 nm) in Skeletal Muscle Performance and Postexercise Recovery in Humans, What Is the Optimal Dose? A Randomized, Double-Blind, Placebo-Controlled Clinical Trial. Photomed. Laser Surg. 2016, 34, 473–482. [Google Scholar] [CrossRef]
- Pinto, H.D.; Vanin, A.A.; Miranda, E.F.; Tomazoni, S.S.; Johnson, D.S.; Albuquerque-Pontes, G.M.; Aleixo, I.O., Jr.; Grandinetti, V.D.; Casalechi, H.L.; de Carvalho, P.T.; et al. Photobiomodulation Therapy Improves Performance and Accelerates Recovery of High-Level Rugby Players in Field Test: A Randomized, Crossover, Double-Blind, Placebo-Controlled Clinical Study. J. Strength Cond. Res. 2016, 30, 3329–3338. [Google Scholar] [CrossRef]
- De Oliveira, A.R.; Vanin, A.A.; Tomazoni, S.S.; Miranda, E.F.; Albuquerque-Pontes, G.M.; De Marchi, T.; Dos Santos Grandinetti, V.; de Paiva, P.; Imperatori, T.; de Carvalho, P.; et al. Pre-Exercise Infrared Photobiomodulation Therapy (810 nm) in Skeletal Muscle Performance and Postexercise Recovery in Humans: What Is the Optimal Power Output? Photomed. Laser Surg. 2017, 35, 595–603. [Google Scholar] [CrossRef]
- Rossato, M.; Dellagrana, R.A.; Sakugawa, R.L.; Lazzari, C.D.; Baroni, B.M.; Diefenthaeler, F. Time Response of Photobiomodulation Therapy on Muscular Fatigue in Humans. J. Strength Cond. Res. 2018, 32, 3285–3293. [Google Scholar] [CrossRef]
- De Marchi, T.; Leal-Junior, E.; Lando, K.C.; Cimadon, F.; Vanin, A.A.; da Rosa, D.P.; Salvador, M. Photobiomodulation therapy before futsal matches improves the staying time of athletes in the court and accelerates post-exercise recovery. Lasers Med. Sci. 2019, 34, 139–148. [Google Scholar] [CrossRef]
- Dornelles, M.P.; Fritsch, C.G.; Sonda, F.C.; Johnson, D.S.; Leal-Junior, E.; Vaz, M.A.; Baroni, B.M. Photobiomodulation therapy as a tool to prevent hamstring strain injuries by reducing soccer-induced fatigue on hamstring muscles. Lasers Med. Sci. 2019, 34, 1177–1184. [Google Scholar] [CrossRef]
- Jówko, E.; Płaszewski, M.; Cieśliński, M.; Sacewicz, T.; Cieśliński, I.; Jarocka, M. The effect of low-level laser irradiation on oxidative stress, muscle damage and function following neuromuscular electrical stimulation. A double blind, randomised, crossover trial. BMC Sports Sci. Med. Rehabil. 2019, 11, 38. [Google Scholar] [CrossRef]
- Tomazoni, S.S.; Machado, C.; De Marchi, T.; Casalechi, H.L.; Bjordal, J.M.; de Carvalho, P.; Leal-Junior, E. Infrared Low-Level Laser Therapy (Photobiomodulation Therapy) before Intense Progressive Running Test of High-Level Soccer Players: Effects on Functional, Muscle Damage, Inflammatory, and Oxidative Stress Markers-A Randomized Controlled Trial. Oxid Med. Cell Longev. 2019, 6239058. [Google Scholar] [CrossRef]
- da Cunha, R.A.; Pinfildi, C.E.; de Castro Pochini, A.; Cohen, M. Photobiomodulation therapy and NMES improve muscle strength and jumping performance in young volleyball athletes: A randomized controlled trial study in Brazil. Lasers Med. Sci. 2020, 35, 621–631. [Google Scholar] [CrossRef]
- Rossato, M.; Dellagrana, R.A.; Sakugawa, R.L.; Baroni, B.M.; Diefenthaeler, F. Dose-Response Effect of Photobiomodulation Therapy on Muscle Performance and Fatigue During a Multiple-Set Knee Extension Exercise: A Randomized, Crossover, Double-Blind Placebo-Controlled Trial. Photobiomodul. Photomed. Laser Surg. 2020, 38, 758–765. [Google Scholar] [CrossRef] [PubMed]
- Zagatto, A.M.; de Paula Ramos, S.; Nakamura, F.Y.; de Lira, F.S.; Lopes-Martins, R.Á.; de Paiva Carvalho, R.L. Effects of low-level laser therapy on performance, inflammatory markers, and muscle damage in young water polo athletes: A double-blind, randomized, placebo-controlled study. Lasers Med. Sci. 2016, 31, 511–521. [Google Scholar] [CrossRef] [PubMed]
- de Paiva, P.R.; Tomazoni, S.S.; Johnson, D.S.; Vanin, A.A.; Albuquerque-Pontes, G.M.; Machado, C.D.; Casalechi, H.L.; de Carvalho, P.T.; Leal-Junior, E.C. Photobiomodulation therapy (PBMT) and/or cryotherapy in skeletal muscle restitution, what is better? A randomized, double-blinded, placebo-controlled clinical trial. Lasers Med. Sci. 2016, 31, 1925–1933. [Google Scholar] [CrossRef] [PubMed]
- De Marchi, T.; Schmitt, V.M.; Machado, G.P.; de Sene, J.S.; de Col, C.D.; Tairova, O.; Salvador, M.; Leal-Junior, E.C. Does photobiomodulation therapy is better than cryotherapy in muscle recovery after a high-intensity exercise? A randomized, double-blind, placebo-controlled clinical trial. Lasers Med. Sci. 2017, 32, 429–437. [Google Scholar] [CrossRef]
- Vassão, P.G.; Baldini, G.S.; Vieira, K.; Balão, A.B.; Pinfildi, C.E.; Campos, R.; Tucci, H.T.; Renno, A. Acute Photobiomodulation Effects Through a Cluster Device on Skeletal Muscle Fatigue of Biceps Brachii in Young and Healthy Males: A Randomized Double-Blind Session. Photobiomodul. Photomed. Laser Surg. 2020, 38, 773–779. [Google Scholar] [CrossRef]
- de Carvalho, G.; Gobbi, A.; Gobbi, R.B.; Alfredo, D.; do Carmo Furquim, T.H.; Barbosa, R.I.; Papoti, M.; de Jesus Guirro, R.R. Photobiomodulation by light emitting diode applied sequentially does not alter performance in cycling athletes. Lasers Med. Sci. 2020, 35, 1769–1779. [Google Scholar] [CrossRef]
- Vanin, A.A.; Miranda, E.F.; Machado, C.S.; de Paiva, P.R.; Albuquerque-Pontes, G.M.; Casalechi, H.L.; de Tarso Camillo de Carvalho, P.; Leal-Junior, E.C. What is the best moment to apply phototherapy when associated to a strength training program? A randomized, double-blinded, placebo-controlled trial: Phototherapy in association to strength training. Lasers Med. Sci. 2016, 31, 1555–1564. [Google Scholar] [CrossRef]
- Felismino, A.S.; Costa, E.C.; Aoki, M.S.; Ferraresi, C.; de Araújo Moura Lemos, T.M.; de Brito Vieira, W.H. Effect of low-level laser therapy (808 nm) on markers of muscle damage: A randomized double-blind placebo-controlled trial. Lasers Med. Sci. 2014, 29, 933–938. [Google Scholar] [CrossRef]
- de Brito Vieira, W.H.; Bezerra, R.M.; Queiroz, R.A.; Maciel, N.F.; Parizotto, N.A.; Ferraresi, C. Use of low-level laser therapy (808 nm) to muscle fatigue resistance: A randomized double-blind crossover trial. Photomed. Laser Surg. 2014, 32, 678–685. [Google Scholar] [CrossRef]
- Florianovicz, V.C.; Ferraresi, C.; Kuriki, H.U.; Marcolino, A.M.; Barbosa, R.I. Effects of Photobiomodulation Therapy and Restriction of Wrist Extensor Blood Flow on Grip: Randomized Clinical Trial. Photobiomodul. Photomed. Laser Surg. 2020, 38, 743–749. [Google Scholar] [CrossRef]
- Miranda, E.F.; Vanin, A.A.; Tomazoni, S.S.; Grandinetti, V.; de Paiva, P.R.; Machado, C.; Monteiro, K.K.; Casalechi, H.L.; de Tarso, P.; de Carvalho, C.; et al. Using Pre-Exercise Photobiomodulation Therapy Combining Super-Pulsed Lasers and Light-Emitting Diodes to Improve Performance in Progressive Cardiopulmonary Exercise Tests. J. Athl. Train. 2016, 51, 129–135. [Google Scholar] [CrossRef]
- Dellagrana, R.A.; Rossato, M.; Sakugawa, R.L.; Baroni, B.M.; Diefenthaeler, F. Photobiomodulation therapy on physiological and performance parameters during running tests: Dose-response effects. J. Strength Cond. Res. 2018, 32, 2807–2815. [Google Scholar] [CrossRef]
- Manteifel, V.M.; Karu, T.I. Structure of mitochondria and activity of their respiratory chain in successive generations of yeast cells exposed to He-Ne laser light. Biol. Bull. 2005, 32, 556–566. [Google Scholar] [CrossRef]
- Ferraresi, C.; Hamblin, M.R.; Parizotto, N.A. Low-level laser (light) therapy (LLLT) on muscle tissue: Performance, fatigue and repair benefited by the power of light. Photonics Lasers Med. 2012, 1, 267–286. [Google Scholar] [CrossRef]
- De Marchi, T.; Leal Junior, E.C.; Bortoli, C.; Tomazoni, S.S.; Lopes-Martins, R.A.; Salvador, M. Low-level laser therapy (LLLT) in human progressive-intensity running: Effects on exercise performance, skeletal muscle status, and oxidative stress. Lasers Med. Sci. 2012, 27, 231–236. [Google Scholar] [CrossRef]
- Hamblin, M.R.; Liebert, A. Photobiomodulation Therapy Mechanisms Beyond Cytochrome c Oxidase. Photobiomodul. Photomed. Laser Surg. 2021, XX, 1–3. [Google Scholar] [CrossRef]
- Ferraresi, C.; Kaippert, B.; Avci, P.; Huang, Y.Y.; de Sousa, M.V.; Bagnato, V.S.; Parizotto, N.A.; Hamblin, M.R. Low-level laser (light) therapy increases mitochondrial membrane potential and ATP synthesis in C2C12 myotubes with a peak response at 3-6 h. Photochem. Photobiol. 2015, 91, 411–416. [Google Scholar] [CrossRef]
- Dutra, Y.M.; Claus, G.M.; Malta, E.S.; Seda, D.; Zago, A.S.; Campos, E.Z.; Ferraresi, C.; Zagatto, A.M. Photobiomodulation 30 min or 6 h Prior to Cycling Does Not Alter Resting Blood Flow Velocity, Exercise-Induced Physiological Responses or Time to Exhaustion in Healthy Men. Front. Physiol. 2021, 11, 607302. [Google Scholar] [CrossRef]
- Malta, E.S.; de Lira, F.S.; Machado, F.A.; Zago, A.S.; do Amaral, S.L.; Zagatto, A.M. Photobiomodulation by Led Does Not Alter Muscle Recovery Indicators and Presents Similar Outcomes to Cold-Water Immersion and Active Recovery. Front. Physiol. 2019, 9, 1948. [Google Scholar] [CrossRef]
- Orssatto, L.B.R.; Detanico, D.; Kons, R.L.; Sakugawa, R.L.; da Silva, J.N., Jr.; Diefenthaeler, F. Photobiomodulation Therapy Does Not Attenuate Fatigue and Muscle Damage in Judo Athletes: A Randomized, Triple-Blind, Placebo-Controlled Trial. Front. Physiol. 2019, 10, 811. [Google Scholar] [CrossRef]
- Orssatto, L.B.R.; Rossato, M.; Vargas, M.; Diefenthaeler, F.; de la Rocha Freitas, C. Photobiomodulation therapy effects on resistance training volume and discomfort in well-trained adults: A randomized, double-blind, placebo-controlled trial. Photobiomodul. Photomed. Laser Surg. 2020, 38, 720–726. [Google Scholar] [CrossRef] [PubMed]
- Dutra, Y.M.; Claus, G.M.; Malta, E.S.; Brisola, G.; Esco, M.R.; Ferraresi, C.; Zagatto, A.M. Acute photobiomodulation by LED does not alter muscle fatigue and cycling performance. Med. Sci. Sports Exerc. 2020, 52, 2448–2458, Erratum in 2021, 53, 1099. [Google Scholar] [CrossRef] [PubMed]
- Santos, I.A.d.; Lemos, M.d.P.; Coelho, V.H.M.; Zagatto, A.M.; Marocolo, M.; Soares, R.N.; Barbosa Neto, O.; Mota, G.R. Acute Photobiomodulation Does Not Influence Specific High-Intensity and Intermittent Performance in Female Futsal Players. Int. J. Environ. Res. Public Health 2020, 17, 7253. [Google Scholar] [CrossRef] [PubMed]
- Opar, D.A.; Williams, M.D.; Shield, A.J. Hamstring strain injuries. Sports Med. 2012, 42, 209–226. [Google Scholar] [CrossRef]
- Buckthorpe, M.; Wright, S.; Bruce-Low, S.; Nanni, G.; Sturdy, T.; Gross, A.S.; Bowen, L.; Styles, B.; Della Villa, S.; Davison, M.; et al. Recommendations for hamstring injury prevention in elite football: Translating research into practice. Br. J. Sports Med. 2019, 53, 449–456. [Google Scholar] [CrossRef]
- Van Dyk, N.; Behan, F.P.; Whiteley, R. Including the nordic hamstring exercise in injury prevention programmes halves the rate of hamstring injuries: A systematic review and meta-analysis of 8459 athletes. Br. J. Sports Med. 2019, 53, 1362–1370. [Google Scholar] [CrossRef]
- Alves, A.N.; Fernandes, K.P.S.; Melo, C.A.V.; Yamaguchi, R.Y.; França, C.M.; Teixeira, D.F.; Bussadori, S.K.; Nunes, F.D.; Mesquita-Ferrari, R.A. Modulating effect of low level-laser therapy on fibrosis in the repair process of the tibialis anterior muscle in rats. Lasers Med. Sci. 2014, 29, 813–821. [Google Scholar] [CrossRef]
- Ramos, L.; Marcos, R.L.; Torres-Silva, R.; Pallota, R.C.; Magacho, T.; Mafra, F.; Macedo, M.M.; Carvalho, R.; Bjordal, J.M.; Lopes-Martins, R. Characterization of Skeletal Muscle Strain Lesion Induced by Stretching in Rats: Effects of Laser Photobiomodulation. Photomed. Laser Surg. 2018, 36, 460–467. [Google Scholar] [CrossRef]
- Tidball, J.G. Inflammatory processes in muscle injury and repair. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2005, 288, R345–R353. [Google Scholar] [CrossRef]
- Medeiros, D.M.; Aimi, M.; Vaz, M.A.; Baroni, B.M. Effects of low-level laser therapy on hamstring strain injury rehabilitation: A randomized controlled trial. Phys. Ther. Sport 2020, 42, 124–130. [Google Scholar] [CrossRef]
- Huang, Y.Y.; Chen, A.C.; Carroll, J.D.; Hamblin, M.R. Biphasic dose response in low level light therapy. Dose Response 2009, 7, 358–383. [Google Scholar] [CrossRef]
- Alves, A.N.; Fernandes, K.P.; Deana, A.M.; Bussadori, S.K.; Mesquita-Ferrari, R.A. Effects of low-level laser therapy on skeletal muscle repair: A systematic review. Am. J. Phys. Med. Rehabil. 2014, 93, 1073–1085. [Google Scholar] [CrossRef]
- Hernández-Hernández, J.M.; García-González, E.G.; Brun, C.E.; Rudnicki, M.A. The myogenic regulatory factors, determinants of muscle development, cell identity and regeneration. Semin. Cell Dev. Biol. 2017, 72, 10–18. [Google Scholar] [CrossRef]
- Ferraresi, C.; dos Santos, R.V.; Marques, G.; Zangrande, M.; Leonaldo, R.; Hamblin, M.R.; Bagnato, V.S.; Parizotto, N.A. Light-emitting diode therapy (LEDT) before matches prevents increase in creatine kinase with a light dose response in volleyball players. Lasers Med. Sci. 2015, 30, 1281–1287. [Google Scholar] [CrossRef]
- Zein, R.; Selting, W.; Hamblin, M.R. Review of light parameters and photobiomodulation efficacy: Dive into complexity. J. Biomed. Optics 2018, 23, 1–17. [Google Scholar] [CrossRef]
- Ghigiarelli, J.J.; Fulop, A.M.; Burke, A.A.; Ferrara, A.J.; Sell, K.M.; Gonzalez, A.M.; Pelton, L.M.; Zimmerman, J.A.; Coke, S.G.; Marshall, D.G. Effects of whole-body photobiomodulation light-bed therapy on creatine kinase and salivary interleukin-6 in a sample of trained males: A randomized, crossover study. Front. Sports Act. Living 2020, 29, 48. [Google Scholar] [CrossRef]
- Leal-Junior, E.C.P.; Lopes-Martins, R.A.B.; Bjordal, J.M. Clinical and scientific recommendations for the use of photobiomodulation therapy in exercise performance enhancement and post-exercise recovery: Current evidence and future directions. Braz. J. Phys. Ther. 2019, 23, 71–75. [Google Scholar] [CrossRef]
- Baroni, B.M.; Rodrigues, R.; Freire, B.B.; Franke, R.; Geremia, J.M.; Vaz, M.A. Effect of low-level laser therapy on muscle adaptation to knee extensor eccentric training. Eur. J. Appl. Physiol. 2015, 115, 639–647. [Google Scholar] [CrossRef]
- Nampo, F.K.; Cavalheri, V.; Ramos, S.; Camargo, E.A. Effect of low-level phototherapy on delayed onset muscle soreness: A systematic review and meta-analysis. Lasers Med. Sci. 2016, 31, 165–177. [Google Scholar] [CrossRef]
- Leal-Junior, E.C.; Vanin, A.A.; Miranda, E.F.; de Carvalho, P.; Dal Corso, S.; Bjordal, J.M. Effect of phototherapy (low-level laser therapy and light-emitting diode therapy) on exercise performance and markers of exercise recovery: A systematic review with meta-analysis. Lasers Med. Sci. 2015, 30, 925–939. [Google Scholar] [CrossRef]
- Bublitz, C.; Renno, A.C.; Ramos, R.S.; Assis, L.; Sellera, C.A.; Trimer, R.; Borghi-Silva, A.; Arena, R.; Guizilini, S. Acute effects of low-level laser therapy irradiation on blood lactate and muscle fatigue perception in hospitalized patients with heart failure-a pilot study. Lasers Med. Sci. 2016, 31, 1203–1209. [Google Scholar] [CrossRef] [PubMed]
- Miranda, E.F.; Tomazoni, S.S.; de Paiva, P.; Pinto, H.D.; Smith, D.; Santos, L.A.; de Tarso Camillo de Carvalho, P.; Leal-Junior, E. When is the best moment to apply photobiomodulation therapy (PBMT) when associated to a treadmill endurance-training program? A randomized, triple-blinded, placebo-controlled clinical trial. Lasers Med. Sci. 2018, 33, 719–727. [Google Scholar] [CrossRef] [PubMed]
- Toma, R.L.; Oliveira, M.X.; Renno, A.; Laakso, E.L. Photobiomodulation (PBM) therapy at 904 nm mitigates effects of exercise-induced skeletal muscle fatigue in young women. Lasers Med. Sci. 2018, 33, 1197–1205. [Google Scholar] [CrossRef] [PubMed]
- Kakihata, C.M.; Malanotte, J.A.; Higa, J.Y.; Errero, T.K.; Balbo, S.L.; Bertolini, G.R. Influence of low-level laser therapy on vertical jump in sedentary individuals. Einstein 2015, 13, 41–46. [Google Scholar] [CrossRef]
- Abedi Yekta, A.; Tabeii, F.; Salehi, S.; Sohrabi, M.; Poursaeidesfahani, M.; Hassabi, M.; Hazegh, N.; Mahdaviani, B. Effect of low-level laser therapy on muscle strength and endurance and post-exercise recovery of young adult: A double-blind, placebo-controlled, randomized clinical trial. Ann. Appl. Sport Sci. 2021, 9, 2. [Google Scholar] [CrossRef]
- Malta, E.; De Poli, R.A.; Brisola, G.M.; Milioni, F.; Miyagi, W.E.; Machado, F.A.; Zagatto, A.M. Acute LED irradiation does not change the anaerobic capacity and time to exhaustion during a high-intensity running effort: A double-blind, crossover, and placebo-controlled study: Effects of LED irradiation on anaerobic capacity and performance in running. Lasers Med. Sci. 2016, 31, 1473–1480. [Google Scholar] [CrossRef]
- Peserico, C.S.; Zagatto, A.M.; Machado, F.A. Effects of endurance running training associated with photobiomodulation on 5-km performance and muscle soreness: A randomized placebo-controlled trial. Front. Physiol. 2019, 10, 211. [Google Scholar] [CrossRef]
- Zagatto, A.M.; Dutra, Y.M.; Lira, F.S.; Antunes, B.M.; Faustini, J.B.; Malta, E.S.; Lopes, V.; de Poli, R.; Brisola, G.; Dos Santos, G.V.; et al. Full Body Photobiomodulation Therapy to Induce Faster Muscle Recovery in Water Polo Athletes: Preliminary Results. Photobiomodul. Photomed. Laser Surg. 2020, 38, 766–772. [Google Scholar] [CrossRef]
- Segabinazi Peserico, C.; Garozi, L.; Zagatto, A.M.; Machado, F.A. Does Previous Application of Photobiomodulation Using Light-Emitting Diodes at Different Energy Doses Modify the Peak Running Velocity and Physiological Parameters? A Randomized, Crossover, Double-Blind, and Placebo-Controlled Study. Photobiomodul. Photomed. Laser Surg. 2020, 38, 727–733. [Google Scholar] [CrossRef]
- Dellagrana, R.A.; Rossato, M.; Orssatto, L.; Sakugawa, R.L.; Baroni, B.M.; Diefenthaeler, F. Effect of Photobiomodulation Therapy in the 1500 m Run: An Analysis of Performance and Individual Responsiveness. Photobiomodul. Photomed. Laser Surg. 2020, 38, 734–742. [Google Scholar] [CrossRef]
- Abreu, J.; Dos Santos, G.V.; Fonsati, L.; Marques, N.R.; Ferraresi, C. Time-Response of Photobiomodulation Therapy by Light-Emitting Diodes on Muscle Torque and Fatigue Resistance in Young Men: Randomized, Double-Blind, Crossover and Placebo-Controlled Study. Photobiomodul. Photomed. Laser Surg. 2020, 38, 750–757. [Google Scholar] [CrossRef]
- Bettleyon, J.; Kaminski, T.W. Does low-level laser therapy decrease muscle-damaging mediators after performance in soccer athletes versus sham laser treatment? A critically appraised topic. J. Sport Rehabil. 2020, 29, 1210–1213. [Google Scholar] [CrossRef]
- Dos Reis, F.A.; da Silva, B.A.; Laraia, E.M.; de Melo, R.M.; Silva, P.H.; Leal-Junior, E.C.; de Carvalho, P. Effects of pre- or post-exercise low-level laser therapy (830 nm) on skeletal muscle fatigue and biochemical markers of recovery in humans: Double-blind placebo-controlled trial. Photomed. Laser Surg. 2014, 32, 106–112. [Google Scholar] [CrossRef]
- Leal Junior, E.C.; Lopes-Martins, R.A.; Baroni, B.M.; De Marchi, T.; Taufer, D.; Manfro, D.S.; Rech, M.; Danna, V.; Grosselli, D.; Generosi, R.A.; et al. Effect of 830 nm low-level laser therapy applied before high-intensity exercises on skeletal muscle recovery in athletes. Lasers Med. Sci. 2009, 24, 857–863. [Google Scholar] [CrossRef]
- Gallego-Selles, A.; Martin-Rincon, M.; Martinez-Canton, M.; Perez-Valera, M.; Martín-Rodríguez, S.; Gelabert-Rebato, M.; Santana, A.; Morales-Alamo, D.; Dorado, C.; Calbet, J. Regulation of Nrf2/Keap1 signaling in human skeletal muscle during exercise to exhaustion in normoxia, severe acute hypoxia and post-exercise ischaemia: Influence of metabolite accumulation and oxygenation. Redox Biol. 2020, 36, 101627. [Google Scholar] [CrossRef]
- Crilly, M.J.; Tryon, L.D.; Erlich, A.T.; Hood, D.A. The role of Nrf2 in skeletal muscle contractile and mitochondrial function. J. Appl. Physiol. 2016, 121, 730–740. [Google Scholar] [CrossRef]
- Gao, L.; Wang, H.J.; Tian, C.; Zucker, I.H. Skeletal muscle Nrf2 contributes to exercise-evoked systemic antioxidant defense via extracellular vesicular communication. Exerc. Sport Sci. Rev. 2021, 49, 213–222. [Google Scholar] [CrossRef]
- Macedo, M.M.; Mafra, F.; Teixeira, C.B.; Torres-Silva, R.; Dos Santos Francisco, R.P.; Gattai, P.P.; Boim, M.A.; Bjordal, J.M.; Nascimento, F.D.; Leonardo, P.S.; et al. Photobiomodulation therapy modulates muscle gene expression and improves performance of rats subjected to a chronic resistance exercise protocol. Photobiomodul. Photomed. Laser Surg. 2020, 38, 713–719. [Google Scholar] [CrossRef]
- Malta, E.S.; Ferraresi, C.; Monte, M.G.; de Poli, R.; Bjordal, J.M.; Lopes-Martins, R.; Marcos, R.L.; Zagatto, A.M.; Carvalho, R. Effect of 12 weeks of endurance training combined with creatine supplement, photobiomodulation therapy, or both on performance and muscle damage in rats. Photobiomodul. Photomed. Laser Surg. 2020, 38, 708–712. [Google Scholar] [CrossRef]
- Yamada, E.F.; Bobinski, F.; Martins, D.F.; Palandi, J.; Folmer, V.; da Silva, M.D. Photobiomodulation therapy in knee osteoarthritis reduces oxidative stress and inflammatory cytokines in rats. J. Biophotonics 2020, 13, 201900204. [Google Scholar] [CrossRef]
- Neves, L.; Gonçalves, E.; Cavalli, J.; Vieira, G.; Laurindo, L.R.; Simões, R.R.; Coelho, I.S.; Santos, A.; Marcolino, A.M.; Cola, M.; et al. Photobiomodulation therapy improves acute inflammatory response in mice: The role of cannabinoid receptors/ATP-sensitive K+ channel/p38-MAPK signalling pathway. Mol. Neurobiol. 2018, 55, 5580–5593. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, L.S.; Saltorato, J.C.; Monte, M.G.; Marcos, R.L.; Lopes-Martins, R.; Tomazoni, S.S.; Leal-Junior, E.; de Paiva Carvalho, R.L. PBMT and topical diclofenac as single and combined treatment on skeletal muscle injury in diabetic rats: Effects on biochemical and functional aspects. Lasers Med. Sci. 2019, 34, 255–262. [Google Scholar] [CrossRef] [PubMed]
- Tomazoni, S.S.; Frigo, L.; Dos Reis Ferreira, T.C.; Casalechi, H.L.; Teixeira, S.; de Almeida, P.; Muscara, M.N.; Marcos, R.L.; Serra, A.J.; de Carvalho, P.; et al. Effects of photobiomodulation therapy and topical non-steroidal anti-inflammatory drug on skeletal muscle injury induced by contusion in rats—Part 1: Morphological and functional aspects. Lasers Med. Sci. 2017, 32, 2111–2120. [Google Scholar] [CrossRef] [PubMed]
- Tomazoni, S.S.; Frigo, L.; Dos Reis Ferreira, T.C.; Casalechi, H.L.; Teixeira, S.; de Almeida, P.; Muscara, M.N.; Marcos, R.L.; Serra, A.J.; de Carvalho, P.; et al. Effects of photobiomodulation therapy and topical non-steroidal anti-inflammatory drug on skeletal muscle injury induced by contusion in rats—Part 2: Biochemical aspects. Lasers Med. Sci. 2017, 32, 1879–1887. [Google Scholar] [CrossRef] [PubMed]
- Silva, G.; Ferraresi, C.; de Almeida, R.T.; Motta, M.L.; Paixão, T.; Ottone, V.O.; Fonseca, I.A.; Oliveira, M.X.; Rocha-Vieira, E.; Dias-Peixoto, M.F.; et al. Insulin resistance is improved in high-fat fed mice by photobiomodulation therapy at 630 nm. J. Biophotonics 2020, 13, e201960140. [Google Scholar] [CrossRef]
- de Brito Vieira, W.H.; Ferraresi, C.; Schwantes, M.; de Andrade Perez, S.E.; Baldissera, V.; Cerqueira, M.S.; Parizotto, N.A. Photobiomodulation increases mitochondrial citrate synthase activity in rats submitted to aerobic training. Lasers Med. Sci. 2018, 33, 803–810. [Google Scholar] [CrossRef]
- de Brito Vieira, W.H.; Ferraresi, C.; Schwantes, M.; de Andrade Perez, S.E.; Baldissera, V.; Cerqueira, M.S.; Parizotto, N.A. Effect of photobiomodulation therapy on oxidative stress markers of gastrocnemius muscle of diabetic rats subjected to high-intensity exercise. Lasers Med. Sci. 2018, 33, 1781–1790. [Google Scholar] [CrossRef]
- da Silva Neto Trajano, L.A.; Trajano, E.; da Silva Sergio, L.P.; Teixeira, A.F.; Mencalha, A.L.; Stumbo, A.C.; de Souza da Fonseca, A. Photobiomodulation effects on mRNA levels from genomic and chromosome stabilization genes in injured muscle. Lasers Med. Sci. 2018, 33, 1513–1519. [Google Scholar] [CrossRef]
- Ferraresi, C.; de Sousa, M.V.; Huang, Y.Y.; Bagnato, V.S.; Parizotto, N.A.; Hamblin, M.R. Time response of increases in ATP and muscle resistance to fatigue after low-level laser (light) therapy (LLLT) in mice. Lasers Med. Sci. 2015, 30, 1259–1267. [Google Scholar] [CrossRef]
- Ferraresi, C.; Parizotto, N.A.; Pires de Sousa, M.V.; Kaippert, B.; Huang, Y.Y.; Koiso, T.; Bagnato, V.S.; Hamblin, M.R. Light-emitting diode therapy in exercise-trained mice increases muscle performance, cytochrome c oxidase activity, ATP and cell proliferation [J. Biophotonics 8, No. 9, 740-754 (2015)]. J. Biophotonics 2016, 9, 976. [Google Scholar] [CrossRef]
- Tomazoni, S.S.; Leal-Junior, E.C.; Frigo, L.; Pallotta, R.C.; Teixeira, S.; de Almeida, P.; Bjordal, J.M.; Lopes-Martins, R.Á. Isolated and combined effects of photobiomodulation therapy, topical nonsteroidal anti-inflammatory drugs, and physical activity in the treatment of osteoarthritis induced by papain. J. Biomed. Opt. 2016, 21, 108001. [Google Scholar] [CrossRef]
- Yang, L.; Dong, Y.; Wu, C.; Li, Y.; Guo, Y.; Yang, B.; Zong, X.; Hamblin, M.R.; Liu, T.C.; Zhang, Q. Photobiomodulation preconditioning prevents cognitive impairment in a neonatal rat model of hypoxia-ischemia. J. Biophotonics 2019, 12, e201800359. [Google Scholar] [CrossRef]
- De Oliveira, H.A.; Antonio, E.L.; Silva, F.A.; de Carvalho, P.; Feliciano, R.; Yoshizaki, A.; Vieira, S.S.; de Melo, B.L.; Leal-Junior, E.; Labat, R.; et al. Protective effects of photobiomodulation against resistance exercise-induced muscle damage and inflammation in rats. J. Sports Sci. 2018, 36, 2349–2357. [Google Scholar] [CrossRef]
- Leal-Junior, E.C.; de Almeida, P.; Tomazoni, S.S.; de Carvalho, P.; Lopes-Martins, R.Á.; Frigo, L.; Joensen, J.; Johnson, M.I.; Bjordal, J.M. Superpulsed Low-Level Laser Therapy Protects Skeletal Muscle of mdx Mice against Damage, Inflammation and Morphological Changes Delaying Dystrophy Progression. PLoS ONE 2014, 9, e89453. [Google Scholar] [CrossRef]
- Silva, A.A.; Leal-Junior, E.C.; D’Avila, K.; Serra, A.J.; Albertini, R.; França, C.M.; Nishida, J.A.; de Carvalho, P. Pre-exercise low-level laser therapy improves performance and levels of oxidative stress markers in mdx mice subjected to muscle fatigue by high-intensity exercise. Lasers Med. Sci. 2015, 30, 1719–1727. [Google Scholar] [CrossRef]
- Tomazoni, S.S.; Casalechi, H.L.; Ferreira, C.; Serra, A.J.; Dellê, H.; Brito, R.; de Melo, B.L.; Vanin, A.A.; Ribeiro, N.F.; Pereira, A.L.; et al. Can photobiomodulation therapy be an alternative to pharmacological therapies in decreasing the progression of skeletal muscle impairments of mdx mice? PLoS ONE 2020, 15, e0236689. [Google Scholar] [CrossRef]
- Santos, L.A.; Marcos, R.L.; Tomazoni, S.S.; Vanin, A.A.; Antonialli, F.C.; Grandinetti, V.; Albuquerque-Pontes, G.M.; de Paiva, P.R.; Lopes-Martins, R.Á.; de Carvalho, P.; et al. Effects of pre-irradiation of low-level laser therapy with different doses and wavelengths in skeletal muscle performance, fatigue, and skeletal muscle damage induced by tetanic contractions in rats. Lasers Med. Sci. 2014, 29, 1617–1626. [Google Scholar] [CrossRef]
- Albuquerque-Pontes, G.M.; Vieira, R.P.; Tomazoni, S.S.; Caires, C.O.; Nemeth, V.; Vanin, A.A.; Santos, L.A.; Pinto, H.D.; Marcos, R.L.; Bjordal, J.M. Effect of pre-irradiation with different doses, wavelengths, and application intervals of low-level laser therapy on cytochrome c oxidase activity in intact skeletal muscle of rats. Lasers Med. Sci. 2015, 30, 59–66. [Google Scholar] [CrossRef]
- Albuquerque-Pontes, G.M.; Casalechi, H.L.; Tomazoni, S.S.; Serra, A.J.; Ferreira, C.; Brito, R.; de Melo, B.L.; Vanin, A.A.; Monteiro, K.; Dellê, H. Photobiomodulation therapy protects skeletal muscle and improves muscular function of mdx mice in a dose-dependent manner through modulation of dystrophin. Lasers Med. Sci. 2018, 33, 755–764. [Google Scholar] [CrossRef]
- De Paiva, P.; Casalechi, H.L.; Tomazoni, S.S.; Machado, C.; Miranda, E.F.; Ribeiro, N.F.; Pereira, A.L.; da Costa, A.S.; Dias, L.B.; Souza, B. Effects of photobiomodulation therapy in aerobic endurance training and detraining in humans: Protocol for a randomized placebo-controlled trial. Medicine 2019, 98, e15317. [Google Scholar] [CrossRef]
- De Paiva, P.; Casalechi, H.L.; Tomazoni, S.S.; Machado, C.; Ribeiro, N.F.; Pereira, A.L.; de Oliveira, M.; Alves, M.; Dos Santos, M.C.; Takara, I.; et al. Does the combination of photobiomodulation therapy (PBMT) and static magnetic fields (sMF) potentiate the effects of aerobic endurance training and decrease the loss of performance during detraining? A randomised, triple-blinded, placebo-controlled trial. BMC Sports Sci. Med. Rehabil. 2020, 12, 23. [Google Scholar] [CrossRef] [PubMed]
- Leal-Junior, E.; de Oliveira, M.; Joensen, J.; Stausholm, M.B.; Bjordal, J.M.; Tomazoni, S.S. What is the optimal time-response window for the use of photobiomodulation therapy combined with static magnetic field (PBMT-sMF) for the improvement of exercise performance and recovery, and for how long the effects last? A randomized, triple-blinded, placebo-controlled trial. BMC Sports Sci. Med. Rehabil. 2020, 12, 64. [Google Scholar] [CrossRef]
- Machado, C.; Casalechi, H.L.; Vanin, A.A.; de Azevedo, J.B.; de Carvalho, P.; Leal-Junior, E. Does photobiomodulation therapy combined to static magnetic field (PBMT-sMF) promote ergogenic effects even when the exercised muscle group is not irradiated? A randomized, triple-blind, placebo-controlled trial. BMC Sports Sci. Med. Rehabil. 2020, 12, 49. [Google Scholar] [CrossRef] [PubMed]
- De Marchi, T.; Schmitt, V.M.; Danúbia da Silva Fabro, C.; da Silva, L.L.; Sene, J.; Tairova, O.; Salvador, M. Phototherapy for Improvement of Performance and Exercise Recovery: Comparison of 3 Commercially Available Devices. J. Athl. Train. 2017, 52, 429–438. [Google Scholar] [CrossRef]
- Hanna, R.; Agas, D.; Benedicenti, S.; Ferrando, S.; Laus, F.; Cuteri, V.; Lacava, G.; Sabbieti, M.G.; Amaroli, A. A Comparative Study Between the Effectiveness of 980 nm Photobiomodulation Delivered by Hand-Piece with Gaussian vs. Flat-Top Profiles on Osteoblasts Maturation. Front. Endocrinol. 2019, 10, 92. [Google Scholar] [CrossRef]
- Amaroli, A.; Arany, P.; Pasquale, C.; Benedicenti, S.; Bosco, A.; Ravera, S. Improving Consistency of Photobiomodulation Therapy: A Novel Flat-Top Beam Hand-Piece versus Standard Gaussian Probes on Mitochondrial Activity. Int. J. Mol. Sci. 2021, 22, 7788. [Google Scholar] [CrossRef]
- Ferraresi, C. Use of Photobiomodulation Therapy in Exercise Performance Enhancement and Postexercise Recovery: True or Myth? Photobiomodul. Photomed. Laser Surg. 2020, 38, 705–707. [Google Scholar] [CrossRef]
- Zivic, Y. Photobiomodulation in cells’ repair. Dermatol. Open J. 2020, 5, 12–25. [Google Scholar] [CrossRef]
- Shutt, T. Mitochondrial Dynamics in Signaling and Disease. Mitochondrion 2019, 49, 233. [Google Scholar] [CrossRef]
- Flockhart, M.; Nilsson, L.C.; Tais, S.; Ekblom, B.; Apró, W.; Larsen, F.J. Excessive exercise training causes mitochondrial functional impairment and decreases glucose tolerance in healthy volunteers. Cell Metab. 2021, 33, 957–970. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).