Predictors of Anxiety in the COVID-19 Pandemic from a Global Perspective: Data from 23 Countries
Abstract
1. Introduction
2. Methodology of the Study
2.1. Ethics Statement
2.2. Participants
2.3. Procedure
2.4. Instruments
2.4.1. Measure of Anxiety
Generalized Anxiety Disorder Scale (GAD-7)
State Trait Anxiety Inventory (STAI)
2.5. Global Indices
2.6. Data Analysis
3. Results
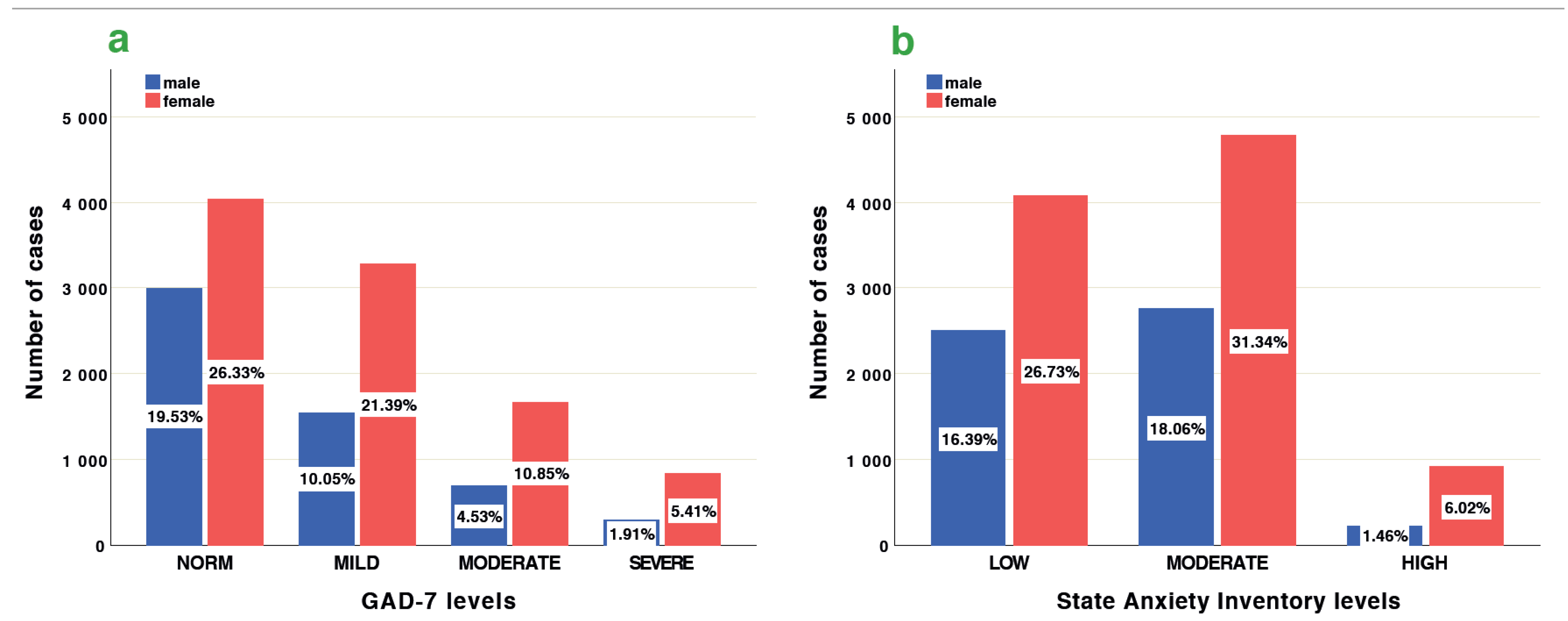
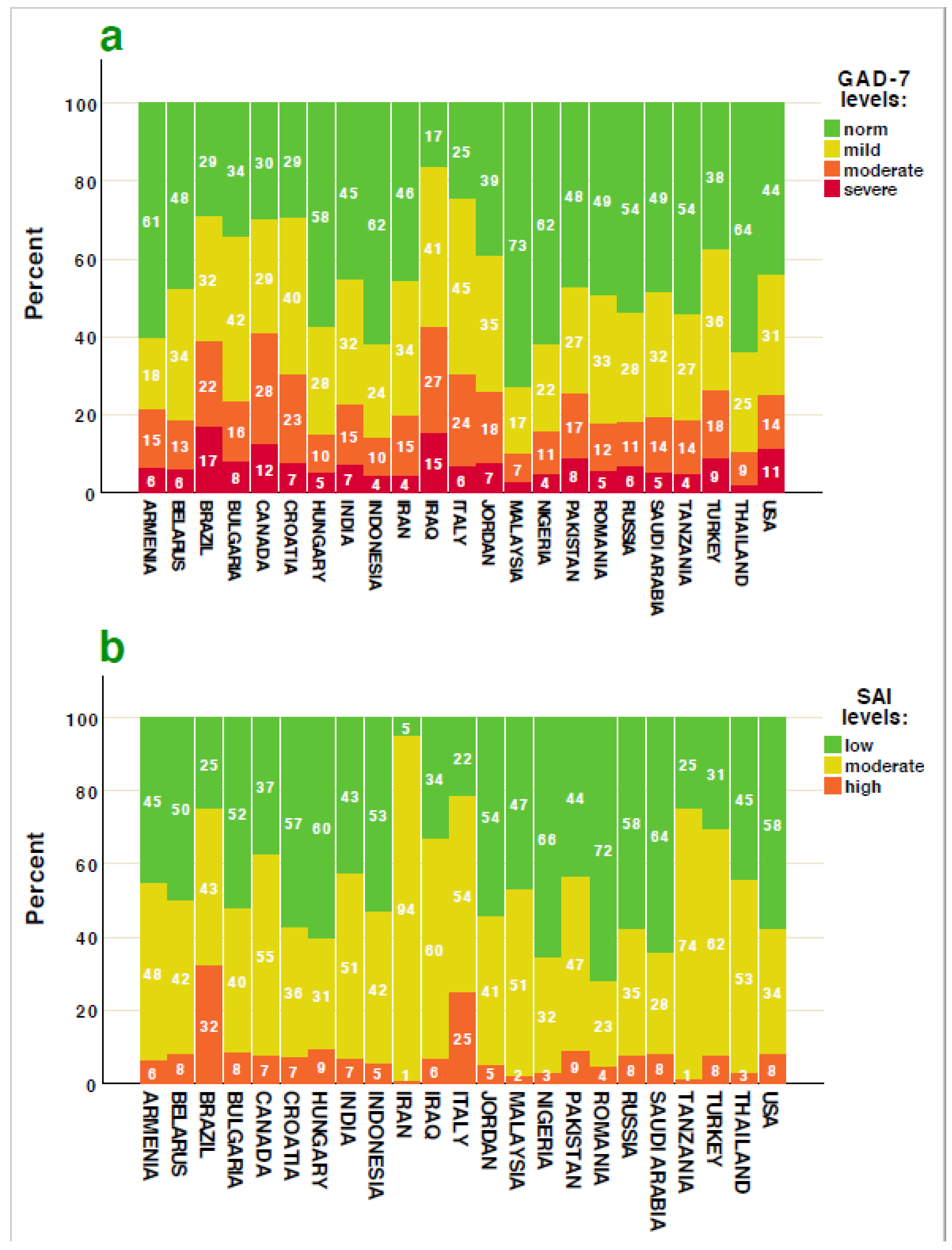
3.1. Sex and Country Differences of Anxiety Scales
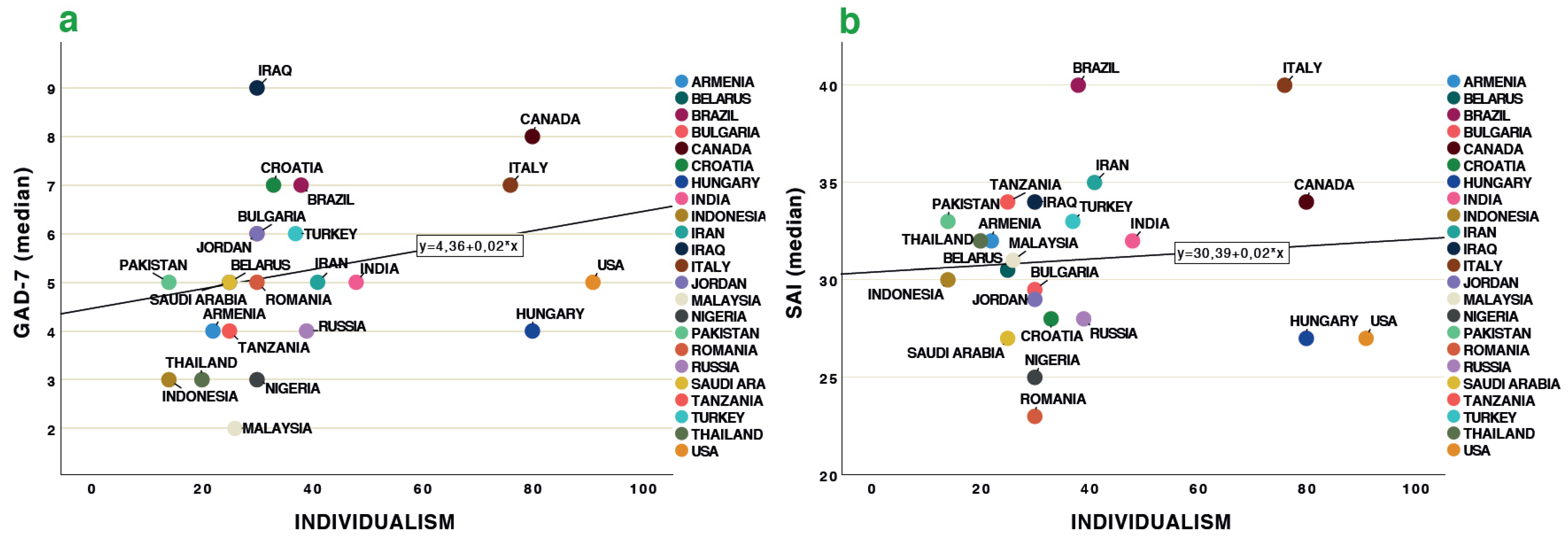
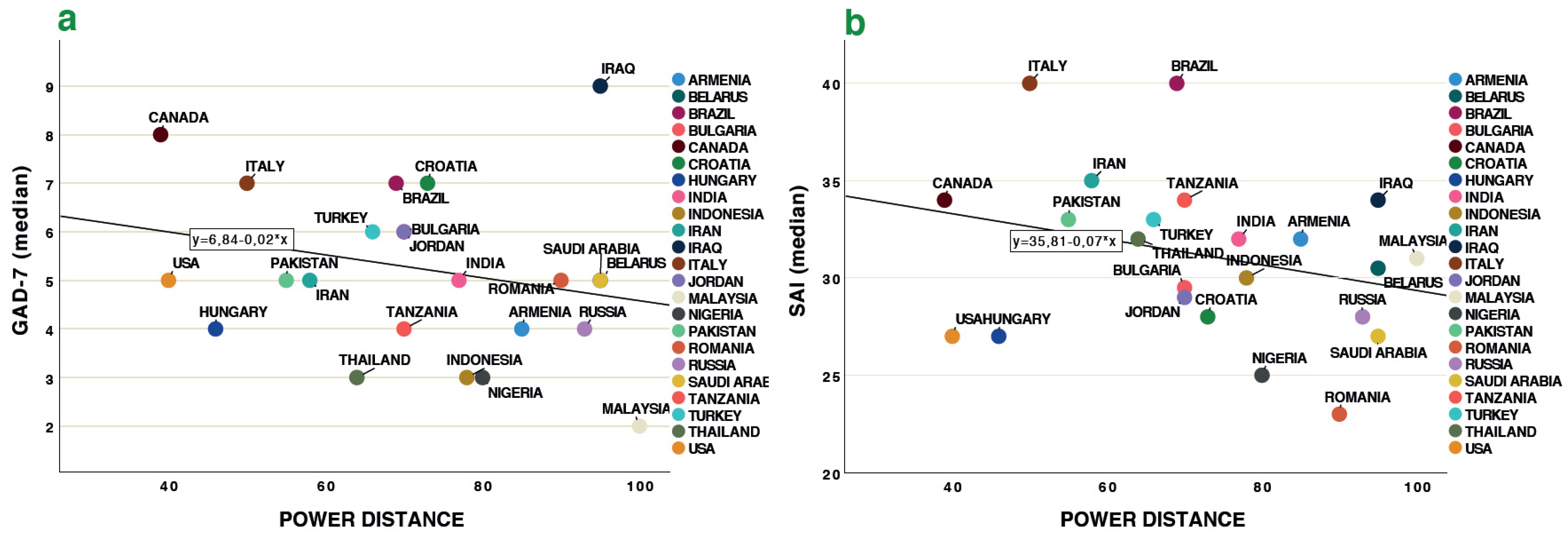
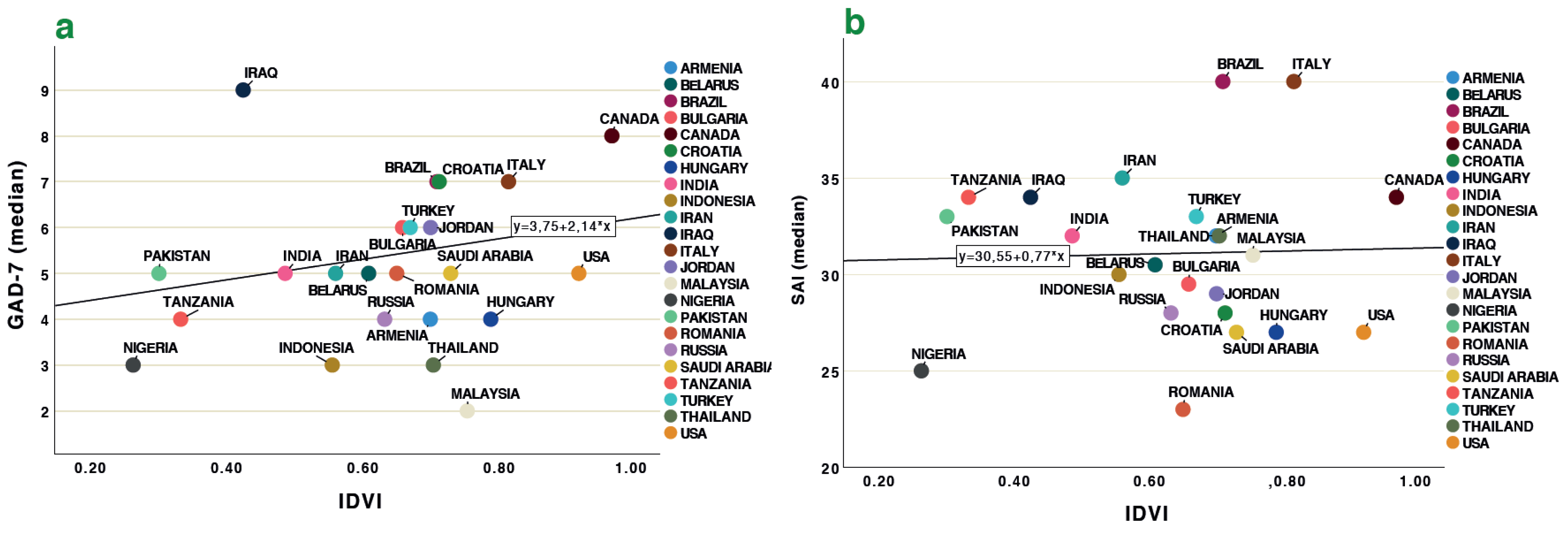
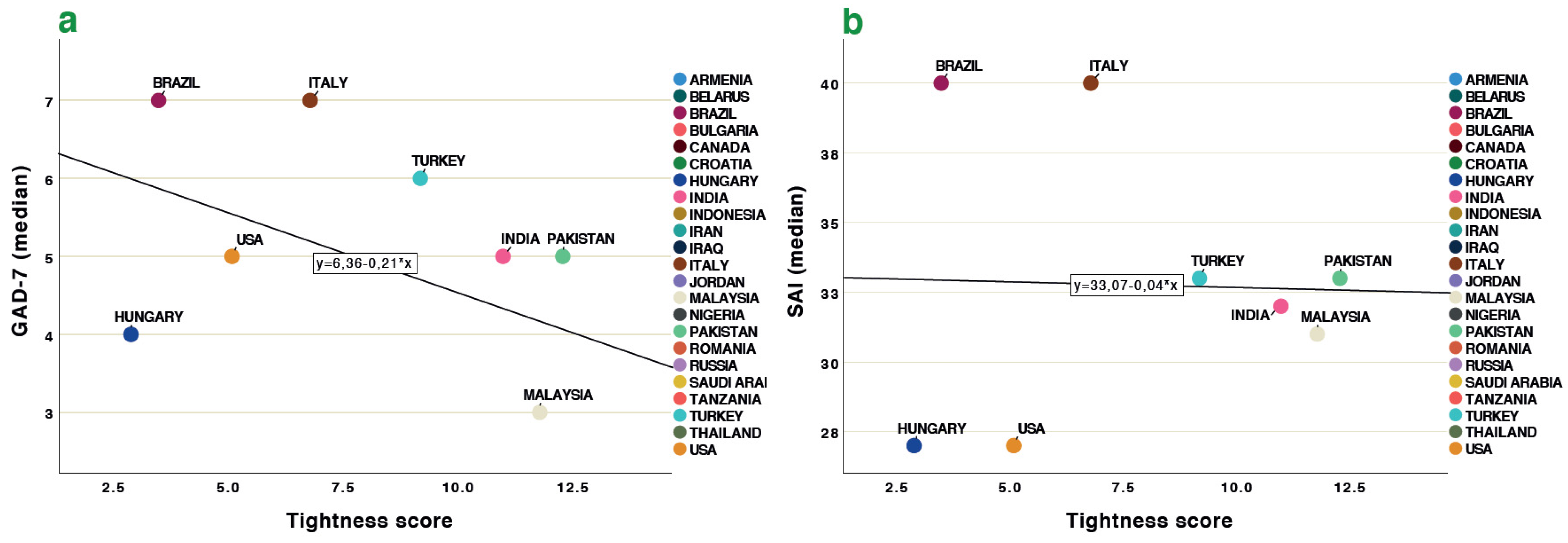
3.2. Global Indices
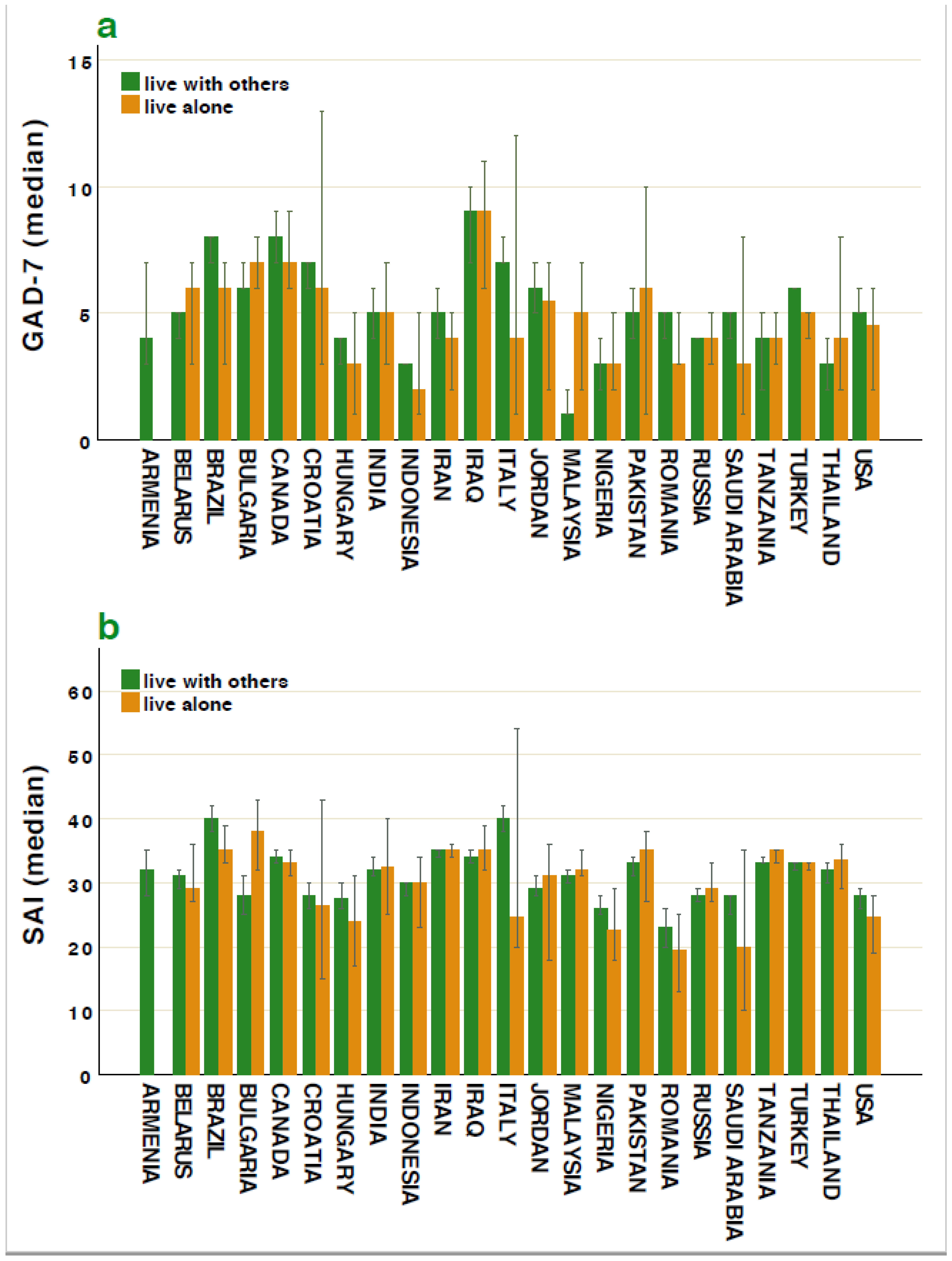
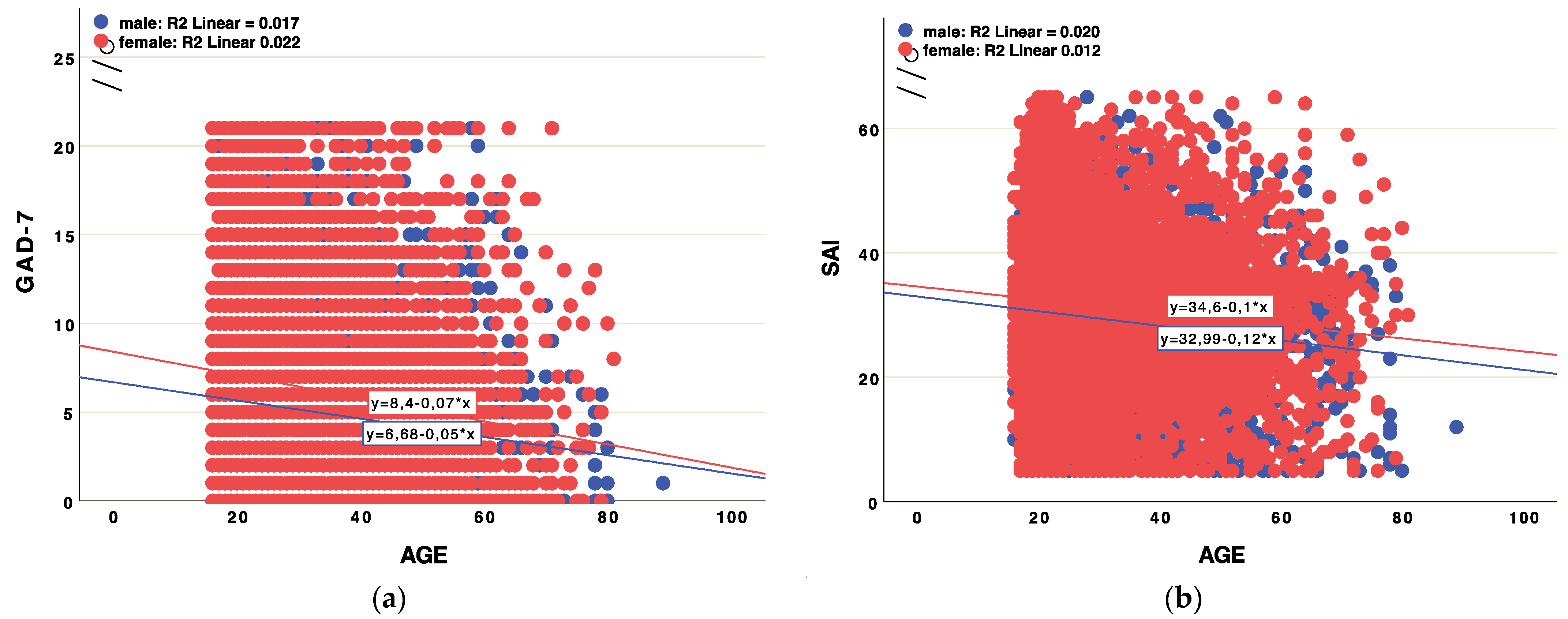
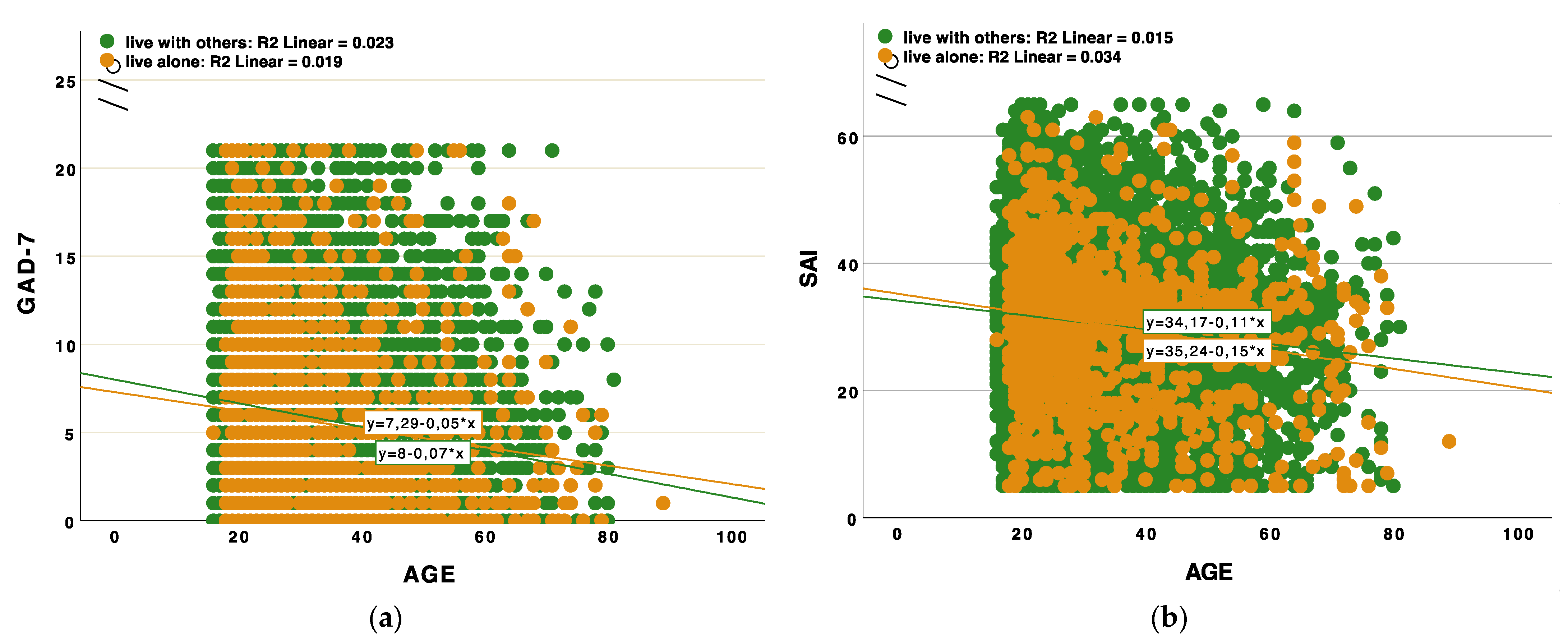
3.3. Anxiety Scales, Age and Cohabitation/Loneliness
4. Discussion
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- World Health Organization. WHO Director-General’s Opening Remarks at the Media Briefing on COVID-19—11 March 2020. Available online: https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19---11-march-2020 (accessed on 12 February 2021).
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef]
- Kowal, M.; Coll-Martín, T.; Ikizer, G.; Rasmussen, J.; Eichel, K.; Studzińska, A.; Ahmed, O. Who is the most stressed during the covid-19 pandemic? Data from 26 countries and areas. Appl. Psychol. Health Well-Being 2020, 12, 946–966. [Google Scholar] [CrossRef]
- Mækelæ, M.J.; Reggev, N.; Dutra, N.; Tamayo, R.M.; Silva-Sobrinho, R.A.; Klevjer, K.; Pfuhl, G. Perceived efficacy of COVID-19 restrictions, reactions and their impact on mental health during the early phase of the outbreak in six countries. R. Soc. Open Sci. 2020, 7200644. [Google Scholar] [CrossRef]
- Ornell, F.; Schuch, J.B.; Sordi, A.O.; Kessler, F.H.P. Pandemic fear and COVID-19: Mental health burden and strategies. Braz. J. Psychiatry 2020, 42, 232–235. [Google Scholar] [CrossRef]
- van Bavel, J.J.; Baicker, K.; Boggio, P.S.; Capraro, V.; Cichocka, A.; Cikara, M.; Ellemers, N. Using social and behavioural science to support COVID-19 pandemic response. Nat. Hum. Behav. 2020, 4, 460–471. [Google Scholar] [CrossRef]
- Fedenok, J.N.; Burkova, V.N. Social distancing as altruism in the context of the coronavirus pandemic: A cross-cultural study. Sib. Hist. Res. 2020, 2, 6–40. [Google Scholar] [CrossRef]
- Cao, W.; Fang, Z.; Hou, G.; Han, M.; Xu, X.; Dong, J.; Zheng, J. The psychological impact of the COVID-19 epidemic on college students in China. Psychiatry Res. 2020, 112934. [Google Scholar] [CrossRef] [PubMed]
- Chen, Q.; Liang, M.; Li, Y.; Guo, J.; Fei, D.; Wang, L.; He, L.; Sheng, C.; Cai, Y.; Li, X.; et al. Mental health care for medical staff in China during the COVID-19 outbreak. Lancet Psychiatry 2020, 7, e15–e16. [Google Scholar] [CrossRef]
- Li, S.W.; Wang, Y.; Yang, Y.Y.; Lei, X.M.; Yang, Y.F. Analysis of influencing factors of anxiety and emotional disorders in children and adolescents during home isolation during the epidemic of novel coronavirus pneumonia. Chin. J. Child Health 2020, 28, 1–9. [Google Scholar]
- Yang, Y.; Li, W.; Zhang, Q.; Zhang, L.; Cheung, T.; Xiang, Y.T. Mental health services for older adults in China during the COVID-19 outbreak. Lancet Psychiatry 2020, 7, e11. [Google Scholar] [CrossRef]
- Bults, M.; Beaujean, D.J.M.A.; de Zwart, O.; Kok, G.; van Empelen, P.; van Steenbergen, J.E.; Richardus, J.H.; Voeten, H.A.C.M. Perceived risk, anxiety, and behavioural responses of the general public during the early phase of the Influenza A (H1N1) pandemic in the Netherlands: Results of three consecutive online surveys. BMC Public Health 2020, 11, 2. [Google Scholar] [CrossRef] [PubMed]
- Jalloh, M.F.; Li, W.; Bunnell, R.E.; Ethier, K.A.; O’Leary, A.; Hageman, K.M.; Sengeh, P.; Jalloh, M.B.; Morgan, O.; Hersey, S.; et al. Impact of Ebola experiences and risk perceptions on mental health in Sierra Leone, July 2015. BMJ Glob. Health 2018, 3, e000471. [Google Scholar] [CrossRef] [PubMed]
- Jones, J.H.; Salathe, M. Early assessment of anxiety and behavioral response to novel swine-origin influenza A (H1N1). PLoS ONE 2009, 4, e8032. [Google Scholar] [CrossRef] [PubMed]
- Main, A.; Zhou, Q.; Ma, Y.; Luecken, L.J.; Liu, X. Relations of SARS-related stressors and coping to Chinese college students’ psychological adjustment during the 2003 Beijing SARS epidemic. J. Couns. Psychol. 2011, 58, 410–423. [Google Scholar] [CrossRef]
- Semenova, O.; Apalkova, J.; Butovskaya, M. Sex differences in spatial activity and anxiety levels in the COVID-19 pandemic from evolutionary perspective. Sustainability 2021, 13, 1110. [Google Scholar] [CrossRef]
- Uehara, M.; Fujii, M.; Kobayashi, K. A model of stress change under the first COVID-19 pandemic among the general public in Japanese major cities and rural areas. Sustainability 2021, 13, 1207. [Google Scholar] [CrossRef]
- Karwowski, M.; Kowal, M.; Groyecka, A.; Białek, M.; Lebuda, I.; Sorokowska, A.; Sorokowski, P. When in danger, turn right: Does Covid-19 threat promote social conservatism and right-wing presidential candidates? PsyArXiv 2020. Available online: https://psyarxiv.com/pjfhs/ (accessed on 8 February 2021). [CrossRef]
- Cohen, S.; Janicki-Deverts, D.; Doyle, W.J.; Miller, G.E.; Frank, E.; Rabin, B.S.; Turner, R.B. Chronic stress, glucocorticoid receptor resistance, inflammation, and disease risk. Proc. Natl. Acad. Sci. USA 2012, 109, 5995–5999. [Google Scholar] [CrossRef]
- Craske, M.; Rauch, S.; Ursano, R.; Prenoveau, J.; Pine, D.; Zinbarg, R. What is an anxiety disorder? Depress. Anxiety 2009, 26, 1066–1085. [Google Scholar] [CrossRef]
- Toussaint, A.; Hüsing, P.; Gumz, A.; Wingenfeld, K.; Härter, M.; Schramm, E.; Löwe, B. Sensitivity to change and minimal clinically important difference of the 7-item Generalized Anxiety Disorder Questionnaire (GAD-7). J. Affect. Disord. 2020, 265, 395–401. [Google Scholar] [CrossRef]
- Ahmed, M.A.-K.; Alansari, B.M. Gender differences in anxiety among undergraduates from ten Arab countries. Soc. Behav. Pers. 2004, 32, 649–655. [Google Scholar] [CrossRef]
- Bergdahl, J.; Bergdahl, M. Perceived stress in adults: Prevalence and association of depression, anxiety and medication in a Swedish population. Stress Health 2002, 18, 235–241. [Google Scholar] [CrossRef]
- Feingold, A. Gender differences in personality: A meta-analysis. Psychol. Bull. 1994, 116, 429–456. [Google Scholar] [CrossRef] [PubMed]
- Burkova, V.N.; Butovskaya, M.L.; Dronova, D.A.; Apalkova, Y.I. Empathy, Anxiety, and Aggression among Moscow Students. Etnograficheskoe Obozr. 2019, 5, 169–188. (In Russian) [Google Scholar] [CrossRef]
- Limcaoco, R.S.G.; Mateos, M.E.; Fernandez, M.J.; Roncero, C. Anxiety, worry and perceived stress in the world due to the COVID-19 pandemic. medRxiv 2020. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; Ho, C.S.; Ho, R.C. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int. J. Environ. Res. Public Health 2020, 17, 1729. [Google Scholar] [CrossRef] [PubMed]
- Jacob, L.; Haro, J.M.; Koyanagi, A. Relationship between living alone and common mental disorders in the 1993, 2000 and 2007 National Psychiatric Morbidity Surveys. PLoS ONE 2019, 14, e0215182. [Google Scholar] [CrossRef]
- Kyprianides, A.; Easterbrook, M.J. Social factors boost well-being behind bars: The importance of individual and group ties for prisoner well-being. Appl. Psychol. Health Well-Being 2020, 12, 7–29. [Google Scholar] [CrossRef]
- Vermeulen, L.P. Small-group behaviour in long-term isolation. S. Afr. J. Sociol. 1977, 15, 35–40. [Google Scholar] [CrossRef]
- Rico-Uribe, L.A.; Caballero, F.F.; Martín-María, N.; Cabello, M.; Ayuso-Mateos, J.L.; Miret, M. Association of loneliness with all-cause mortality: A meta-analysis. PLoS ONE 2018, 13, e0190033. [Google Scholar] [CrossRef]
- Epstein, Y.M. Crowding stress and human behavior. J. Soc. Issues 1981, 37, 126–144. [Google Scholar] [CrossRef]
- Fuller, T.D.; Edwards, J.N.; Vorakitphokatorn, S.; Sermsri, S. Chronic stress and psychological well-being: Evidence from Thailand on household crowding. Soc. Sci. Med. 1996, 42, 265–280. [Google Scholar] [CrossRef]
- Heppner, P.P. Expanding the conceptualization and measurement of applied problem solving and coping: From stages to dimensions to the almost forgotten cultural context. Am. Psychol. 2008, 63, 805–816. [Google Scholar] [CrossRef] [PubMed]
- Wong, P.T.P.; Wong, L.C.J. Handbook of Multicultural Perspectives on Stress and Coping; Springer: New York, NY, USA, 2006. [Google Scholar]
- Hofstede, G. Culture’s Consequences: Comparing Values, Behaviors, Institutions and Organizations across Nations; Sage: Thousand Oaks, CA, USA, 2001. [Google Scholar]
- Hofstede, G. Dimensionalizing cultures: The Hofstede model in context. Online Read. Psychol. Cult. (ORPC) 2011, 2, 3–26. [Google Scholar] [CrossRef]
- Triandis, H.C.; McCusker, C.; Hui, C.H. Multimethod probes of individualism and collectivism. J. Personal. Soc. Psychol. 1990, 59, 1006–1020. [Google Scholar] [CrossRef]
- Gelfand, M.J.; Raver, J.L.; Nishii, L.; Leslie, L.M.; Lun, J.; Lim, B.C.; Yamaguchi, S. Differences between tight and loose cultures: A 33-nation study. Science 2011, 332, 1100–1104. [Google Scholar] [CrossRef]
- Brueck, H.; Business Insider. Singapore is Working “Round the Clock” to Find Coronavirus Cases. Lying about Where You’ve Been can Result in 6 Months of Jail or a Fine of up to $10,000. Available online: https://www.businessinsider.com/singapore-coronavirus-quarantine-lying-to-investigators-jail-fine-2020-3?r=US&IR=T (accessed on 5 March 2020).
- Carpenter, S. Effects of cultural tightness and collectivism on self-concept and causal attributions. Cross-Cult. Res. 2000, 34, 38–56. [Google Scholar] [CrossRef]
- Cao, C.; Li, N.; Liu, L. Do national cultures matter in the containment of COVID-19? Int. J. Sociol. Soc. Policy 2020. [Google Scholar] [CrossRef]
- de Kloet, E.R.; Joels, M.; Holsboer, F. Stress and the brain: From adaptation to disease. Nat. Rev. Neurosci. 2005, 6, 463–475. [Google Scholar] [CrossRef]
- Siervo, M.; Wells, J.C.; Cizza, G. Contribution of psychosocial stress to the obesity epidemic: An evolutionary approach. Horm. Metab. Res. 2009, 41, 261. [Google Scholar] [CrossRef]
- Vinkers, C.H.; van Amelsvoort, T.; Bisson, J.I.; Branchi, I.; Cryan, J.F.; Domschke, K.; van der Wee, N.J. Stress resilience during the coronavirus pandemic. Eur. Neuropsychopharmacol. 2020, 35, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Reissman, D.B.; Watson, P.J.; Klomp, R.W.; Tanielian, T.L.; Prior, S.D. Pandemic influenza preparedness: Adaptive responses to an evolving challenge. J. Homel. Secur. Emerg. Manag. 2006, 3, 1–26. [Google Scholar] [CrossRef]
- O’Connor, R.; Wetherall, K.; Cleare, S.; McClelland, H.; Melson, A.; Niedzwiedz, C.; Robb, K. Mental health and well-being during the COVID-19 pandemic: Longitudinal analyses of adults in the UK COVID-19 Mental Health & Wellbeing study. Br. J. Psychiatry 2020, 1–8. [Google Scholar] [CrossRef]
- Brislin, R.W. Back-translation for cross-cultural research. J. Cross-Cult. Psychol. 1970, 1, 185–216. [Google Scholar] [CrossRef]
- Sousa, V.D.; Rojjanasrirat, W. Translation, adaptation and validation of instruments or scales for use in cross-cultural health care research: A clear and user-friendly guideline. J. Eval. Clin. Pract. 2011, 17, 268–274. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.W.; Lowe, B. A brief measure for assessing generalized anxiety disorder. Arch. Int. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef] [PubMed]
- Spielberger, C.D. Manual for the State-Trait Anxiety Inventory: STAI (Form Y); Consulting Psychologists Press: Palo Alto, CA, USA, 1983. [Google Scholar]
- Al-Rabiaah, A.; Temsah, M.H.; Al-Eyadhy, A.A.; Hasan, G.M.; Al-Zamil, F.; Al-Subaie, S.; Somily, A.M. Middle East Respiratory Syndrome-Corona Virus (MERS-CoV) associated stress among medical students at a university teaching hospital in Saudi Arabia. J. Infect. Public Health 2020, 13, 687–691. [Google Scholar] [CrossRef]
- Dzhambov, A.M.; Tilov, B.G.; Makakova, D.R.; Dimitrova, D.D. Psychometric properties and contribution to mental health of the Bulgarian version of the 4-factor Ruminative Thought Style Questionnaire. Folia Med. (Plovdiv) 2019, 61, 529–539. [Google Scholar] [CrossRef]
- Silva, M.T.; Roa, M.C.; Martins, S.S.; da Silva, A.T.C.; Galvao, T.F. Generalized anxiety disorder and associated factors in adults in the Amazon, Brazil: A population-based study. J. Affect. Disord. 2018, 236, 180–186. [Google Scholar] [CrossRef] [PubMed]
- Sidik, S.M.; Arroll, B.; Goodyear-Smith, F. Validation of the GAD-7 (Malay version) among women attending a primary care clinic in Malaysia. J. Prim. Health Care 2012, 4, 5–11. [Google Scholar] [CrossRef]
- Esipenko, E.A.; Beloplotova, K.E.; Sharafieva, K.R.; Ismatullina, V.I. Anxiety (personal and spatial among students of different sex as factor of success in decision of spatial dillems. Subj. Pers. Psychol. Self-Regul. 2018, 77–82. (In Russian) [Google Scholar] [CrossRef]
- Musumari, P.M.; Tangmunkongvorakul, A.; Srithanaviboonchai, K.; Techasrivichien, T.; Suguimoto, S.P.; Ono-Kihara, M.; Kihara, M. Grit is associated with lower level of depression and anxiety among university students in Chiang Mai, Thailand: A cross-sectional study. PLoS ONE 2018, 13, e0209121. [Google Scholar] [CrossRef]
- Bozukluğu, Y.A.; Uyarlaması, T.T.; ve Güvenirliği, G. Validity and reliability study for the Turkish adaptation of the Generalized Anxiety Disorder-7 (GAD-7) scale. Arch. Neuropsychiatry 2013, 50, 53–58. [Google Scholar] [CrossRef]
- Bahammam Maha, A. Validity and reliability of an Arabic version of the state-trait anxiety inventory in a Saudi dental setting. Saudi Med. J. 2016, 37, 668–674. [Google Scholar] [CrossRef]
- Hanin, Y.L.; Spielberger, C.D. The development and validation of the Russian form of the state-trait anxiety inventory. In Series in Clinical & Community Psychology: Stress & Anxiety; HarperCollins: New York, NY, USA, 1980; pp. 15–26. [Google Scholar]
- Sipos, K.; Sipos, M. The development and validation of the Hungarian form of the state-trait anxiety inventory. In Series in Clinical & Community Psychology: Stress & Anxiety; HarperCollins: New York, NY, USA, 1980; pp. 27–39. [Google Scholar]
- Moreno, E.; Muñoz-Navarro, R.; Medrano, L.A.; González-Blanch, C.; Ruiz-Rodríguez, P.; Limonero, J.T.; Moretti, L.S.; Cano-Vindel, A.; Moriana, J.A. Factorial invariance of a computerized version of the GAD-7 across various demographic groups and over time in primary care patients. J. Affect. Disord. 2019, 252, 114–121. [Google Scholar] [CrossRef]
- Uz, I. The index of cultural tightness and looseness among 68 countries. J. Cross-Cult. Psychol. 2015, 46, 319–335. [Google Scholar] [CrossRef]
- Moore, M.; Gelfeld, B.; Okunogbe, A.; Paul, C. Identifying Future Disease Hot Spots. Infectious Disease Vulnerability Index; RAND Corporation: Santa Monica, CA, USA, 2016; p. 81. [Google Scholar] [CrossRef]
- Ahmad, S.; Hussain, S.; Shah, F.S.; Akhtar, F. Urdu translation and validation of GAD-7: A screening and rating tool for anxiety symptoms in primary health care. J. Pak. Med. Assoc. 2017, 67, 1536–1540. [Google Scholar]
- Baxter, A.J.; Vos, T.; Scott, K.M.; Norman, R.E.; Flaxman, A.D.; Blore, J.; Whiteford, H.A. The regional distribution of anxiety disorders: Implications for the Global Burden of Disease Study, 2010. Int. J. Methods Psychiatr. Res. 2014, 23, 422–438. [Google Scholar] [CrossRef]
- Byrd-Bredbenner, C.; Eck, K.; Quick, V. Psychometric properties of the generalized anxiety disorder-7 and generalized anxiety disorder-mini in United States university students. Front. Psychol. 2020, 11, 2512. [Google Scholar] [CrossRef] [PubMed]
- Jaehn, P.; Bobrova, N.; Saburova, L.; Kudryavtsev, A.V.; Malyutina, S.; Cook, S. The relation of gender role attitudes with depression and generalised anxiety disorder in two Russian cities. J. Affect. Disord. 2020, 264, 348–357. [Google Scholar] [CrossRef] [PubMed]
- Stone, A.A.; Schwartz, J.E.; Broderick, J.E.; Deaton, A. A snapshot of the age distribution of psychological well-being in the United States. Proc. Natl. Acad. Sci. USA 2010, 107, 9985–9990. [Google Scholar] [CrossRef] [PubMed]
- Parkerson, H.A.; Thibodeau, M.A.; Brandt, C.P.; Zvolensky, M.J.; Asmundson, G.J. Cultural-based biases of the GAD-7. J. Anxiety Disord. 2015, 31, 38–42. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Ruscio, A.M.; Shear, K.; Wittchen, H.-U. Epidemiology of anxiety disorders. In Behavioral Neurobiology of Anxiety and its Treatment, Current Topics in Behavioral Neurosciences; Stein, M.B., Steckler, V.T., Eds.; Springer: Berlin/Heidelberg, Germany, 2010; pp. 21–35. [Google Scholar]
- Baxter, A.J.; Scott, K.M.; Vos, T.; Whiteford, H.A. Global prevalence of anxiety disorders: A systematic review and metaregression. Psychol. Med. 2013, 43, 897–910. [Google Scholar] [CrossRef] [PubMed]
- Archer, J.A.; Lim, Z.M.T.; Teh, H.C.; Chang, W.C.; Chen, S.H.A. The effect of age on the relationship between stress, well-being and health in a Singaporean sample. Ageing Int. 2015, 40, 413–425. [Google Scholar] [CrossRef]
- Feizi, A.; Aliyari, R.; Roohafza, H. Association of perceived stress with stressful life events, lifestyle and sociodemographic factors: A large-scale community-based study using logistic quantile regression. Comput. Math. Methods Med. 2012, 151865. [Google Scholar] [CrossRef]
- Cohen, S.; Wills, T.A. Stress, social support, and the buffering hypothesis. Psychol. Bull. 1985, 98, 310–357. [Google Scholar] [CrossRef]
- Odriozola-Gonzalez, P.; Planchuelo-Gomez, A.; Irurtia-Muniz, M.J.; de Luis-Garcıa, R. Psychological symptoms of the outbreak of the COVID-19 crisis and confinement in the population of Spain. PsyArXiv 2020. [Google Scholar] [CrossRef]
- Tian, F.; Li, H.; Tian, S.; Yang, J.; Shao, J.; Tian, C. Psychological symptoms of ordinary Chinese citizens based on SCL-90 during the level I emergency response to COVID-19. Psychiatry Res. 2020, 288, 112992. [Google Scholar] [CrossRef]
- Steptoe, A.; Wardle, J. Locus of control and health behaviour revisited: A multivariate analysis of young adults from 18 countries. Br. J. Psychol. 2001, 92, 659–672. [Google Scholar] [CrossRef]
- Cheng, C.; Cheung, S.F.; Chio, J.H.; Chan, M.P. Cultural meaning of perceived control: A meta-analysis of locus of control and psychological symptoms across 18 cultural regions. Psychol. Bull. 2013, 139, 152–188. [Google Scholar] [CrossRef]
- Chiao, J.Y.; Blizinsky, K.D. Culture–gene coevolution of individualism–collectivism and the serotonin transporter gene. Proc. R. Soc. B 2010, 277, 529–537. [Google Scholar] [CrossRef] [PubMed]

| COUNTRY | Survey Language | Total N | SEX | Mean Age | |
|---|---|---|---|---|---|
| Men | Women | (±SD) | |||
| ARMENIA | Armenian | 33 | 27 | 6 | 20.45 (±2.37) |
| BELARUS | Russian | 338 | 143 | 195 | 19.20 (±2.85) |
| BRAZIL | Portuguese | 515 | 82 | 430 | 38.80 (±13.78) |
| BULGARIA | Bulgarian | 322 | 129 | 193 | 28.34 (±8.75) |
| CANADA | English | 692 | 446 | 246 | 30.33 (±8.74) |
| CROATIA | English | 275 | 71 | 204 | 24.10 (±8.40) |
| HUNGARY | Hungarian | 235 | 35 | 198 | 31.95 (±11.84) |
| INDIA | English | 383 | 213 | 170 | 29.95 (±9.85) |
| INDONESIA | Indonesian | 930 | 504 | 424 | 32.05 (±12.09) |
| IRAN | Persian | 306 | 88 | 217 | 33.68 (±7.34) |
| IRAQ | Arabic | 173 | 88 | 85 | 35.03 (±10.63) |
| ITALY | Italian | 253 | 44 | 208 | 23.50 (±4.15) |
| JORDAN | Arabic | 449 | 121 | 328 | 33.68 (±10.52) |
| MALAYSIA | Malay | 1087 | 478 | 609 | 33.19 (±11.12) |
| NIGERIA | English | 316 | 214 | 102 | 34.09 (±11.24) |
| PAKISTAN | English | 484 | 212 | 272 | 27.06 (±11.11) |
| ROMANIA | Romanian | 269 | 42 | 226 | 36.22 (±10.94) |
| RUSSIA | Russian | 1903 | 486 | 1417 | 20.99 (±4.72) |
| SAUDI ARABIA | Arabic | 414 | 98 | 316 | 26.76 (±9.72) |
| TANZANIA | English | 341 | 185 | 156 | 23.95 (±4.25) |
| TURKEY | Turkish | 4717 | 1609 | 3093 | 27.57 (±10.84) |
| THAILAND | Thai | 300 | 49 | 250 | 32.82 (±13.00) |
| USA | English | 666 | 189 | 477 | 45.16 (±17.15) |
| TOTAL | 15,375 | 5553 | 9822 | 29.15 (±11.80) | |
| COUNTRY | Start Date | End Date | Median |
|---|---|---|---|
| ARMENIA | 8 June 2020 | 21 June 2020 | 11 June 2020 |
| BELARUS | 29 April 2020 | 21 June 2020 | 7 May 2020 |
| BRAZIL | 15 May 2020 | 27 July 2020 | 10 June 2020 |
| BULGARIA | 18 May 2020 | 30 June 2020 | 23 June 2020 |
| CANADA | 13 May 2020 | 24 May 2020 | 16 May 2020 |
| CROATIA | 18 May 2020 | 27 August 2020 | 17 July 2020 |
| HUNGARY | 30 June 2020 | 08 August 2020 | 22 May 2020 |
| INDIA | 16 May 2020 | 31 August 2020 | 16 May 2020 |
| INDONESIA | 3 June 2020 | 14 August 2020 | 23 June 2020 |
| IRAN | 21 May 2020 | 17 July 2020 | 28 May 2020 |
| IRAQ | 7 June 2020 | 14 July 2020 | 8 June 2020 |
| ITALY | 4 June 2020 | 29 November 2020 | 12 June 2020 |
| JORDAN | 1 June 2020 | 13 June 2020 | 1 June 2020 |
| MALAYSIA | 12 May 2020 | 22 July 2020 | 10 June 2020 |
| NIGERIA | 4 May 2020 | 9 August 2020 | 31 May 2020 |
| PAKISTAN | 13 May 2020 | 3 August 2020 | 21 May 2020 |
| ROMANIA | 18 May 2020 | 31 August 2020 | 5 June 2020 |
| RUSSIA | 2 May 2020 | 8 August 2020 | 5 May 2020 |
| SAUDI ARABIA | 22 May 2020 | 20 June 2020 | 30 May 2020 |
| TANZANIA | 1 May 2020 | 1 July 2020 | 26 June 2020 |
| TURKEY | 23 May 2020 | 16.07.2020 | 6 June 2020 |
| THAILAND | 12 May 2020 | 30 May 2020 | 14 May2020 |
| USA | 19 May 2020 | 30 August 2020 | 10 June 2020 |
| TOTAL | 5 June 2020 |
| COUNTRY | Scales | Sex | N | meanM | t | df | P | 95% CI | Effect Size (Hedges’ Correction) * | |
|---|---|---|---|---|---|---|---|---|---|---|
| Lower | Upper | |||||||||
| ARMENIA | GAD-7 | men women | 27 6 | 5.81 4.00 | 0.808 | 31 | 0.425 | −2.767 | 6.397 | 0.356 |
| SAI | men women | 27 6 | 30.93 26.17 | 0.847 | 31 | 0.403 | −6.701 | 16.219 | 0.373 | |
| BELARUS | GAD-7 | men women | 143 195 | 5.10 6.46 | −2.702 | 336 | 0.007 | −2.344 | −0.369 | −0.297 |
| SAI | men women | 143 195 | 29.01 32.43 | −3.055 | 336 | 0.002 | −5.617 | −1.217 | −0.336 | |
| BRAZIL | GAD-7 | men women | 82 430 | 7.99 8.49 | −0.800 | 126 | 0.425 | −1.738 | 0.737 | −0.087 |
| SAI | men women | 82 430 | 36.27 39.94 | −2.513 | 510 | 0.012 | −6.541 | −0.801 | −0.302 | |
| BULGARIA | GAD-7 | men women | 129 193 | 5.87 7.32 | −2.821 | 308 | 0.005 | −2.467 | −0.440 | −0.307 |
| SAI | men women | 129 193 | 26.18 30.48 | −3.325 | 314 | 0.001 | −6.842 | −1.755 | −0.358 | |
| CANADA | GAD-7 | men women | 420 239 | 7.75 8.71 | −2.209 | 657 | 0.028 | −1.812 | −0.107 | −0.179 |
| SAI | men women | 382 227 | 31.03 33.18 | −2.403 | 607 | 0.017 | −3.902 | −0.393 | −0.201 | |
| CROATIA | GAD-7 | men women | 71 204 | 6.44 7.77 | −2.056 | 273 | 0.041 | −2.610 | −0.056 | −0.282 |
| SAI | men women | 71 204 | 24.61 29.61 | −3.049 | 273 | 0.003 | −8.249 | −1.774 | −0.419 | |
| HUNGARY | GAD-7 | men women | 35 198 | 3.69 5.16 | −1.784 | 231 | 0.076 | −3.096 | 0.154 | −0.326 |
| SAI | men women | 35 198 | 24.83 28.73 | −1.750 | 231 | 0.081 | −8.299 | 0.491 | −0.320 | |
| INDIA | GAD-7 | men women | 213 170 | 5.37 6.79 | −2.822 | 381 | 0.005 | −2.413 | −0.431 | −0.290 |
| SAI | men women | 213 170 | 30.23 33.54 | −3.553 | 381 | 0.0004 | −5.151 | −1.481 | −0.365 | |
| INDONESIA | GAD-7 | men women | 504 424 | 3.27 5.59 | −7.797 | 828 | <0.001 | −2.912 | −1.741 | −0.521 |
| SAI | men women | 504 424 | 26.48 30.47 | −5.617 | 926 | <0.001 | −5.380 | −2.594 | −0.370 | |
| IRAN | GAD-7 | men women | 88 217 | 5.57 5.77 | −0.373 | 303 | 0.710 | −1.294 | 0.882 | −0.047 |
| SAI | men women | 88 217 | 34.75 35.00 | −0.656 | 303 | 0.513 | −1.019 | 0.510 | −0.083 | |
| IRAQ | GAD-7 | men women | 88 85 | 8.81 9.52 | −0.944 | 171 | 0.347 | −2.197 | 0.776 | −0.143 |
| SAI | men women | 88 85 | 31.16 33.74 | −1.726 | 171 | 0.086 | −5.535 | 0.371 | −0.261 | |
| ITALY | GAD-7 | men women | 44 208 | 6.09 7.96 | −2.712 | 250 | 0.007 | −3.229 | −0.512 | −0.449 |
| SAI | men women | 44 208 | 35.20 39.05 | −2.152 | 250 | 0.032 | −7.371 | −0.326 | −0.356 | |
| JORDAN | GAD-7 | men women | 121 328 | 4.94 7.13 | −4.326 | 447 | <0.001 | −3.174 | −1.191 | −0.459 |
| SAI | men women | 121 328 | 26.43 29.06 | −2.305 | 447 | 0.022 | −4.875 | −0.388 | −0.245 | |
| MALAYSIA | GAD-7 | men women | 478 609 | 2.68 3.54 | −3.484 | 1072 | 0.001 | −1.337 | −0.374 | −0.329 |
| SAI | men women | 477 609 | 28.98 27.57 | 2.267 | 1064 | 0.024 | 0.189 | 2.627 | 0.137 | |
| NIGERIA | GAD-7 | men women | 214 102 | 3.98 5.26 | −2.003 | 158 | 0.047 | −2.549 | −0.018 | −0.265 |
| SAI | men women | 214 102 | 24.77 25.51 | −0.572 | 314 | 0.567 | −3.278 | 1.801 | −0.069 | |
| PAKISTAN | GAD-7 | men women | 212 272 | 5.20 6.90 | −3.624 | 482 | <0.001 | −2.631 | −0.781 | −0.331 |
| SAI | men women | 212 272 | 28.20 32.72 | −4.282 | 482 | <0.001 | −6.592 | −2.445 | −0.392 | |
| ROMANIA | GAD-7 | men women | 42 226 | 4.12 5.79 | −2.138 | 266 | 0.033 | −3.205 | −0.132 | −0.358 |
| SAI | men women | 42 226 | 21.45 24.19 | −1.395 | 266 | 0.164 | −6.612 | 1.127 | −0.234 | |
| RUSSIA | GAD-7 | men women | 486 1417 | 3.80 5.71 | −7.951 | 938 | <0.001 | −2.381 | −1.438 | −0.394 |
| SAI | men women | 486 1417 | 25.34 29.47 | −6.761 | 1901 | <0.001 | −5.335 | −2.936 | −0.355 | |
| SAUDI ARABIA | GAD-7 | men women | 98 316 | 5.40 5.55 | −0.290 | 412 | 0.772 | −1.211 | 0.899 | −0.034 |
| SAI | men women | 98 316 | 26.15 27.34 | −0.843 | 412 | 0.400 | −3.949 | 1.578 | −0.097 | |
| TANZANIA | GAD-7 | men women | 185 156 | 4.39 5.65 | −2.304 | 339 | 0.022 | −2.332 | −0.184 | −0.250 |
| SAI | men women | 185 156 | 32.43 33.25 | −1.261 | 339 | 0.208 | −2.107 | 0.461 | −0.137 | |
| THAILAND | GAD-7 | men women | 49 250 | 3.33 4.20 | −1.679 | 88 | 0.097 | −1.898 | 0.159 | −0.212 |
| SAI | men women | 49 250 | 28.59 31.01 | −1.864 | 297 | 0.063 | −4.967 | 0.134 | −0.291 | |
| TURKEY | GAD-7 | men women | 1609 3093 | 5.76 7.42 | −11.412 | 3473 | <0.001 | −1.942 | −1.372 | −0.354 |
| SAI | men women | 1609 3093 | 32.14 33.74 | −6.836 | 3718 | <0.001 | −2.057 | −1.140 | −0.200 | |
| USA | GAD-7 | men women | 189 477 | 5.85 6.52 | −1.447 | 664 | 0.148 | −1.587 | 0.241 | −0.124 |
| SAI | men women | 184 461 | 25.80 27.72 | −1.620 | 643 | 0.106 | −4.248 | 0.407 | 0.141 | |
| TOTAL SAMPLE | GAD-7 | men women | 5527 9815 | 5.10 6.55 | −17.620 | 12,056 | <0.001 | −1.614 | −1.288 | −0.292 |
| SAI | men women | 5483 9787 | 29.34 31.65 | −13.133 | 11,997 | <0.001 | −2.655 | −1.965 | −0.216 | |
| Scales | Cohabitation/ Loneliness | N | Mean | t | df | P | 95% CI | Effect Size | |
|---|---|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||||
| GAD-7 | live with others live alone | 13,889 1408 | 6.08 5.61 | 3.328 | 15295 | <0.001 | 0.193 | 0.745 | 0.093 |
| SAI | live with others live alone | 13,830 1397 | 30.88 30.46 | 1.376 | 15,225 | NS | −0.175 | 1.001 | 0.039 |
| Predictors | Dependent Variable | df | F | p | η2 |
|---|---|---|---|---|---|
| Sex | GAD-7 | 1 | 34.961 | <0.001 | 0.002 |
| SAI | 1 | 14.199 | <0.001 | 0.001 | |
| cohabitation/loneliness | GAD-7 | 1 | 2.808 | 0.094 | 0.000 |
| SAI | 1 | 0.199 | 0.656 | 0.000 | |
| sex × cohabitation/loneliness | GAD-7 | 1 | 0.109 | 0.742 | 0.000 |
| SAI | 1 | 0.946 | 0.331 | 0.000 | |
| Country | GAD-7 | 22 | 7.770 | <0.001 | 0.011 |
| SAI | 22 | 9.566 | <0.001 | 0.014 | |
| Age | GAD-7 | 1 | 26.639 | <0.001 | 0.002 |
| SAI | 1 | 21.149 | <0.001 | 0.001 | |
| country × age | GAD-7 | 22 | 4.921 | <0.001 | 0.007 |
| SAI | 22 | 6.245 | <0.001 | 0.009 | |
| cohabitation/loneliness × country | GAD-7 | 21 | 1.192 | 0.246 | 0.002 |
| SAI | 21 | 1.835 | 0.011 | 0.003 | |
| sex × country | GAD-7 | 22 | 1.357 | 0.122 | 0.002 |
| SAI | 22 | 3.875 | <0.001 | 0.006 | |
| cohabitation/loneliness × age | GAD-7 | 1 | 3.562 | 0.059 | 0.000 |
| SAI | 1 | 0.022 | 0.883 | 0.000 | |
| sex × age | GAD-7 | 1 | 14.066 | <0.001 | 0.001 |
| SAI | 1 | 0.997 | 0.318 | 0.000 |
| Countries | Sample: N (age) | GAD-7 * | GAD-7 Men | GAD-7 Women | Present Study | Source |
|---|---|---|---|---|---|---|
| Bulgaria | 529 (21.00) | 3.0 (median) | 6.0 (median) | [53] | ||
| Brazil | 4001 (18–60) | 2.2% severe level | - | - | 17% severe level | [54] |
| Canada | 610 (21.35) | 5.82 (mean) | 8.23 | [70] | ||
| Malaysia | 895 (30.9 ± 10.4) | 7.8% moderate and severe levels | - | - | 10% moderate and severe levels | [55] |
| Pakistan | 285 (16–80) | 5.18 (mean) | - | - | 6.05 | [65] |
| Russia | 132 (18–46) | 3.35 (mean) | 3.51 | 3.19 | 4.76 (3.80; 5.71) | [56] |
| Thailand | 800 (18–24) | 3.78 (mean) 7.8% moderate and severe levels | 3.65 | 3.91 | 3.77 (3.33; 4:20) 11% moderate and severe levels | [57] |
| Turkey | 134 (34.67 ± 12.55) | 6.11 (mean) | - | - | 6.59 | [58] |
| Saudi Arabia | 200 (21.6) medical students during MERS-CoV 2014 192 (20.50 ± 1.96) | 5.09 (mean) 0% severe level - | 4.56 5.26 | 5.61 - | 5.48 (5.40;5.55) | [52] |
| USA 2009–2010 2015 2018–2019 | 2740 (47.4 ± 15.5) 447 (23.43) 1897 (19.60 ± 1.62) 426 (20.19 ± 1.82) 1805 (20.44 ± 1.47) | 4.68% severe level 5.06 (mean) 5.71 (mean) 6.28 (mean) 7.45 (mean) | - - 4.84 5.99 6.09 | - - 6.57 8.34 8.81 | 11% severe level 6.19 (mean) | [50] [70] [67] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Burkova, V.N.; Butovskaya, M.L.; Randall, A.K.; Fedenok, J.N.; Ahmadi, K.; Alghraibeh, A.M.; Allami, F.B.M.; Alpaslan, F.S.; Al-Zu’bi, M.A.A.; Biçer, D.F.; et al. Predictors of Anxiety in the COVID-19 Pandemic from a Global Perspective: Data from 23 Countries. Sustainability 2021, 13, 4017. https://doi.org/10.3390/su13074017
Burkova VN, Butovskaya ML, Randall AK, Fedenok JN, Ahmadi K, Alghraibeh AM, Allami FBM, Alpaslan FS, Al-Zu’bi MAA, Biçer DF, et al. Predictors of Anxiety in the COVID-19 Pandemic from a Global Perspective: Data from 23 Countries. Sustainability. 2021; 13(7):4017. https://doi.org/10.3390/su13074017
Chicago/Turabian StyleBurkova, Valentina N., Marina L. Butovskaya, Ashley K. Randall, Julija N. Fedenok, Khodabakhsh Ahmadi, Ahmad M. Alghraibeh, Fathil Bakir Mutsher Allami, Fadime Suata Alpaslan, Mohammad Ahmad Abdelaziz Al-Zu’bi, Derya Fatma Biçer, and et al. 2021. "Predictors of Anxiety in the COVID-19 Pandemic from a Global Perspective: Data from 23 Countries" Sustainability 13, no. 7: 4017. https://doi.org/10.3390/su13074017
APA StyleBurkova, V. N., Butovskaya, M. L., Randall, A. K., Fedenok, J. N., Ahmadi, K., Alghraibeh, A. M., Allami, F. B. M., Alpaslan, F. S., Al-Zu’bi, M. A. A., Biçer, D. F., Cetinkaya, H., David, O. A., Donato, S., Dural, S., Erickson, P., Ermakov, A. M., Ertuğrul, B., Fayankinnu, E. A., Fisher, M. L., ... Zinurova, R. I. (2021). Predictors of Anxiety in the COVID-19 Pandemic from a Global Perspective: Data from 23 Countries. Sustainability, 13(7), 4017. https://doi.org/10.3390/su13074017


















