Parametric Design of Porous Structure and Optimal Porosity Gradient Distribution Based on Root-Shaped Implants
Abstract
1. Introduction
2. Structural Design of Gyroid Porous Bone Scaffolds
3. Modelling and Finite Element Simulation
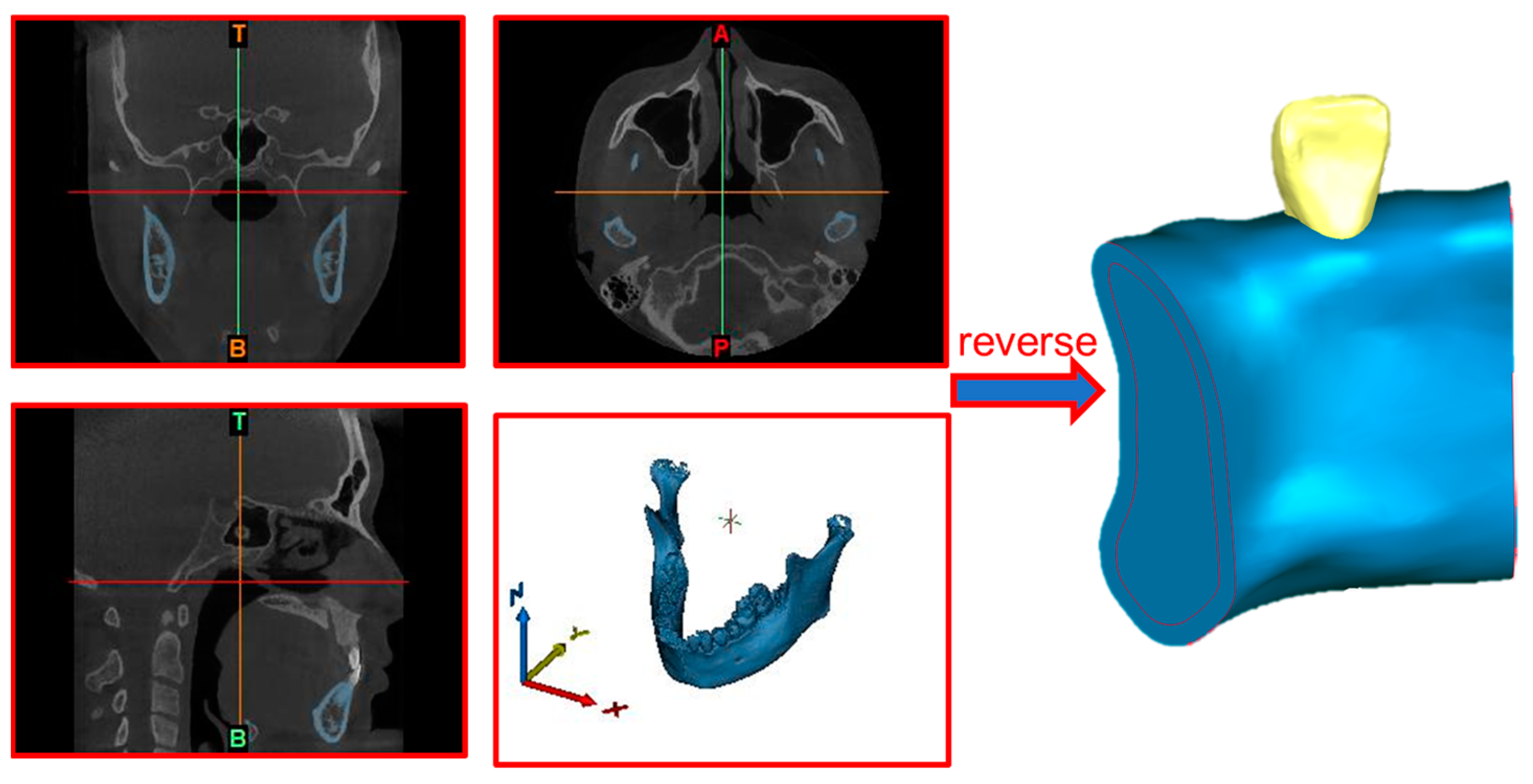
3.1. Modelling
3.2. Compression Simulation Settings
3.3. Fluid Simulation Settings
3.4. Biomechanical Properties Simulation Setup
4. Results and Discussion
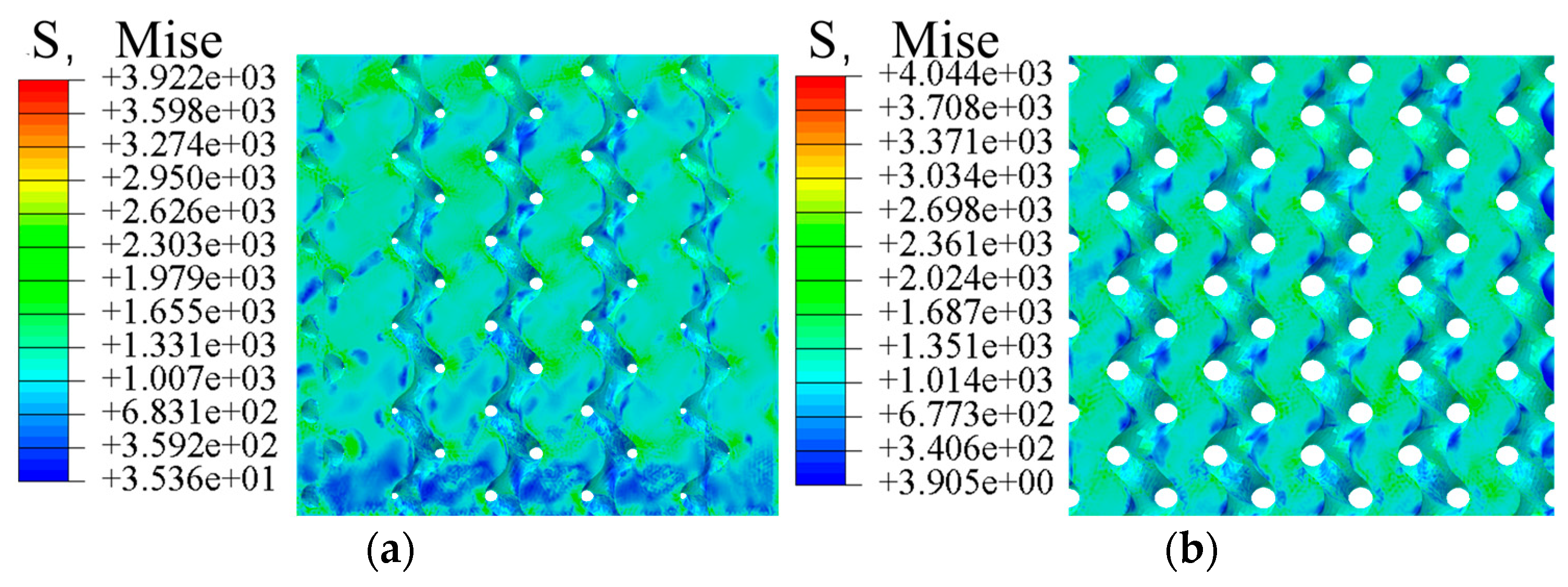
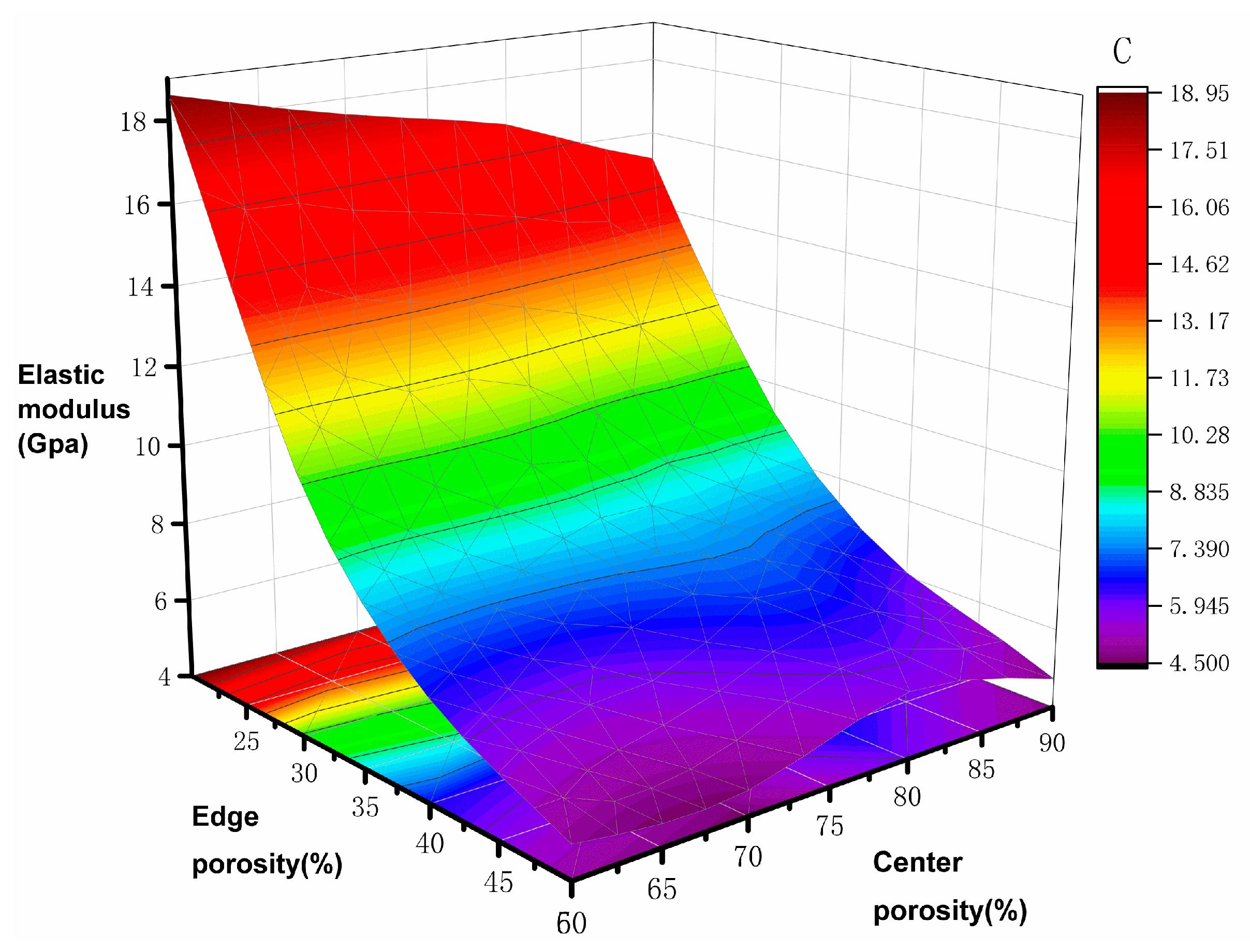
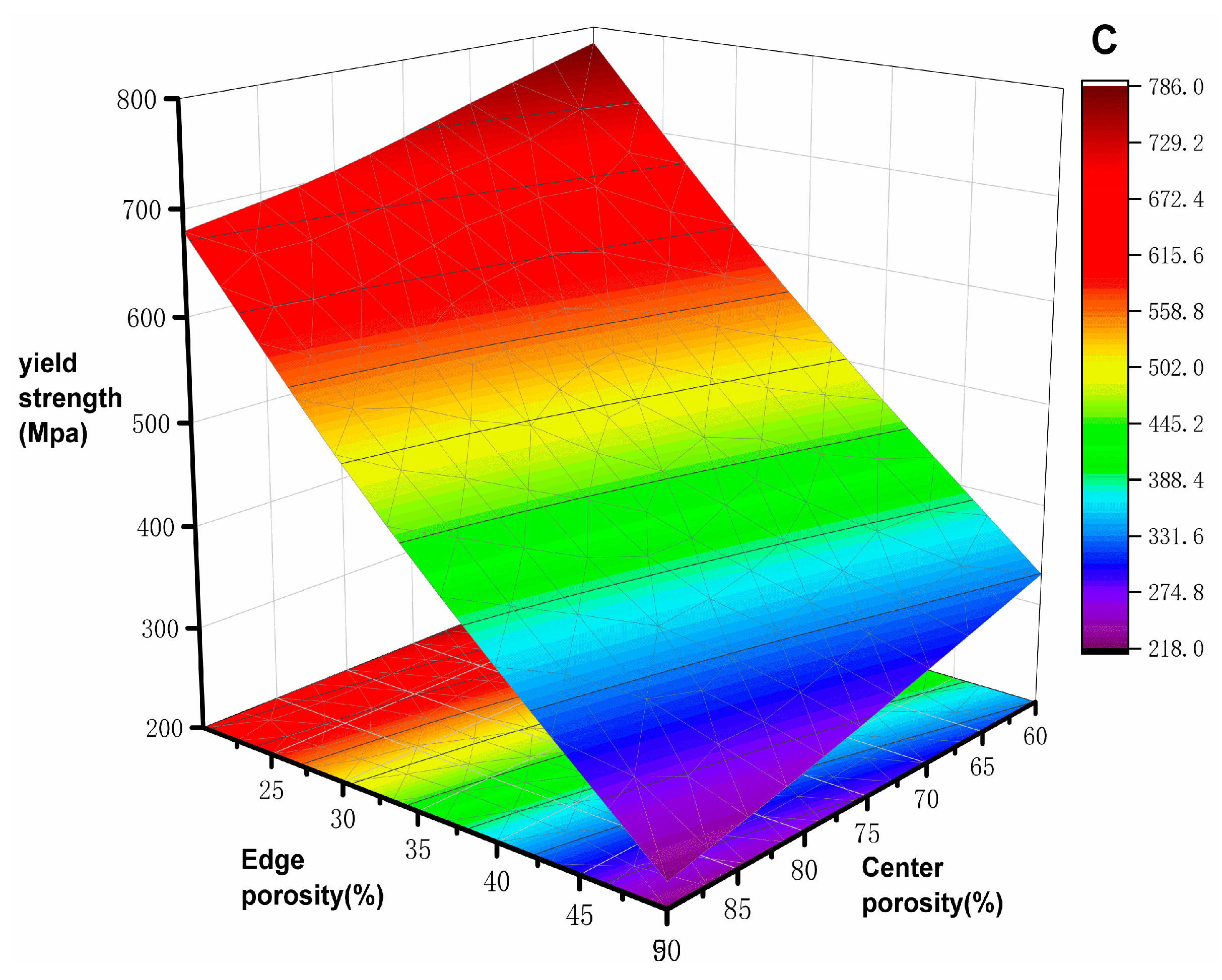
4.1. Mechanical Properties Analysis
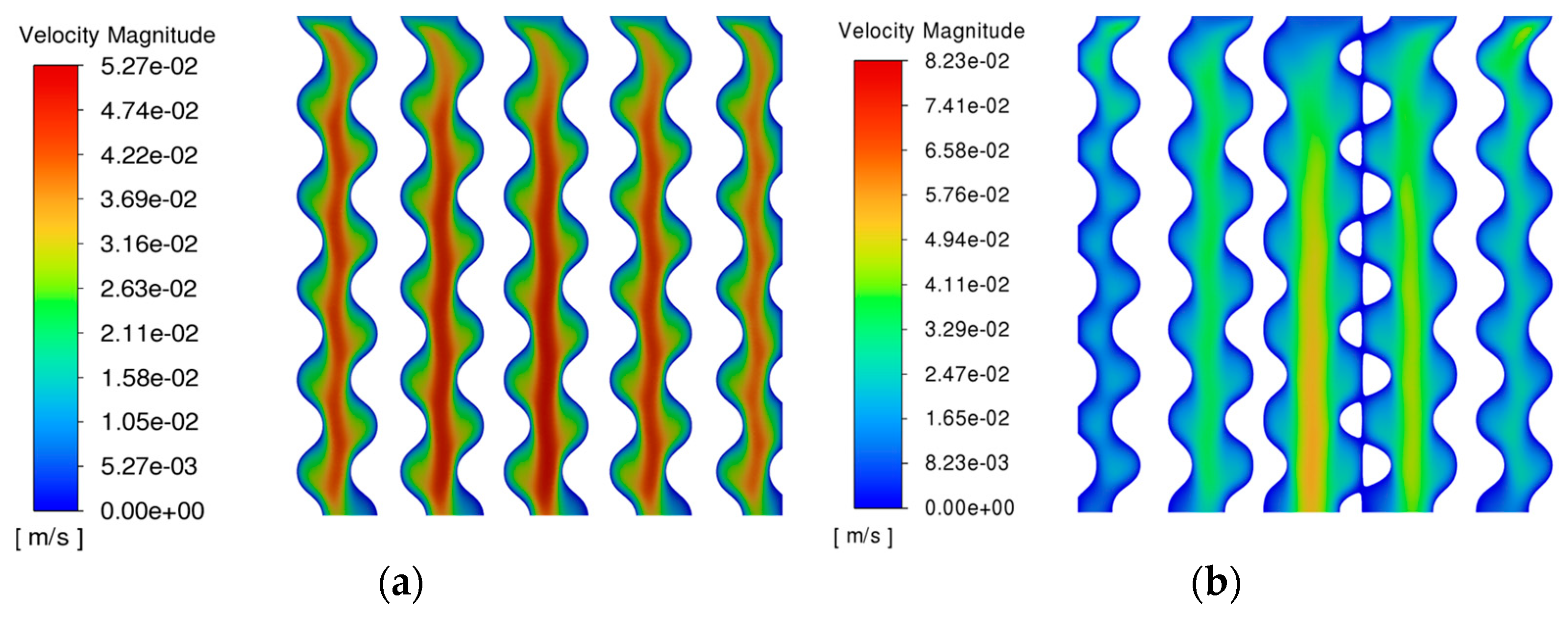
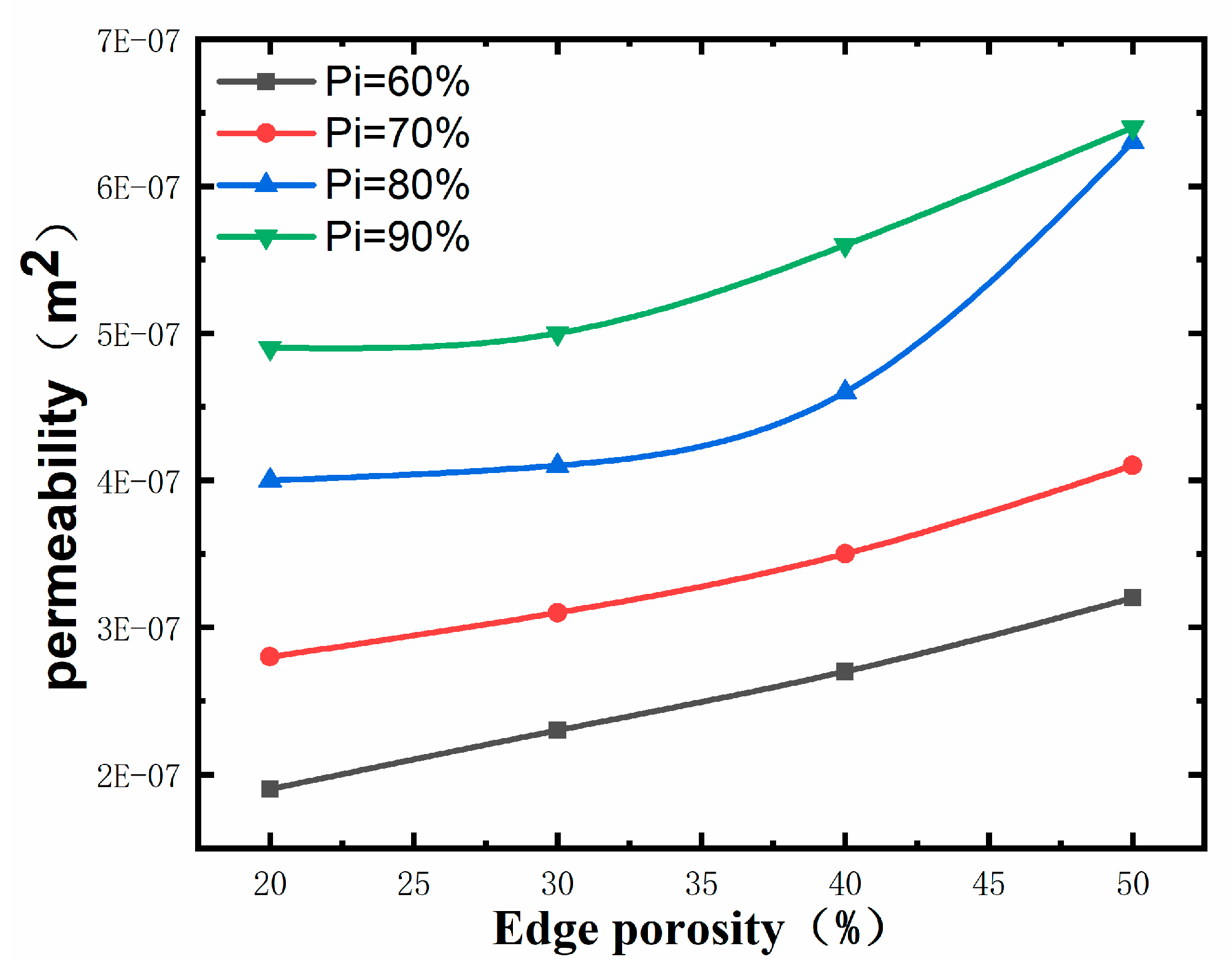
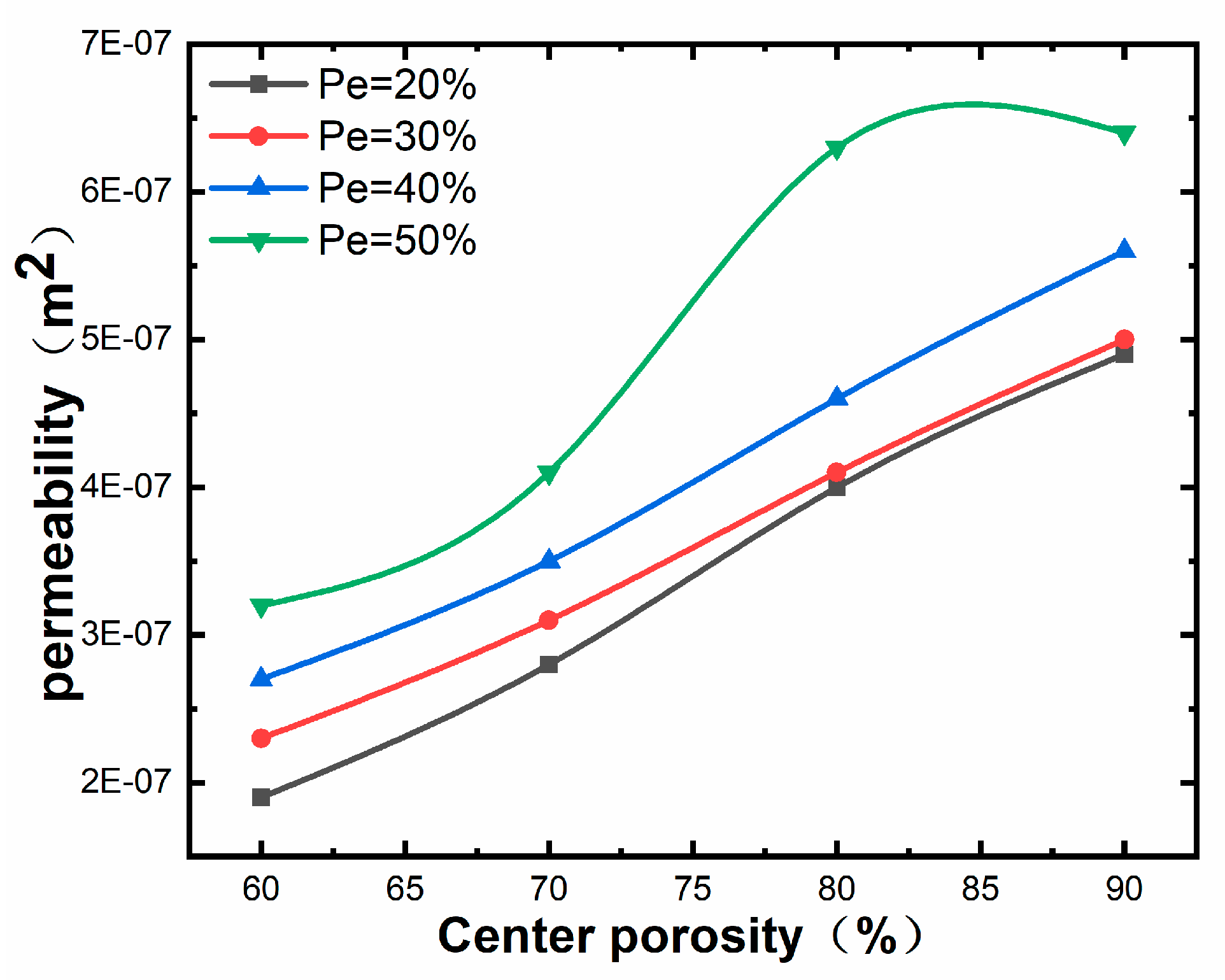
4.2. Fluid Dynamics Analysis
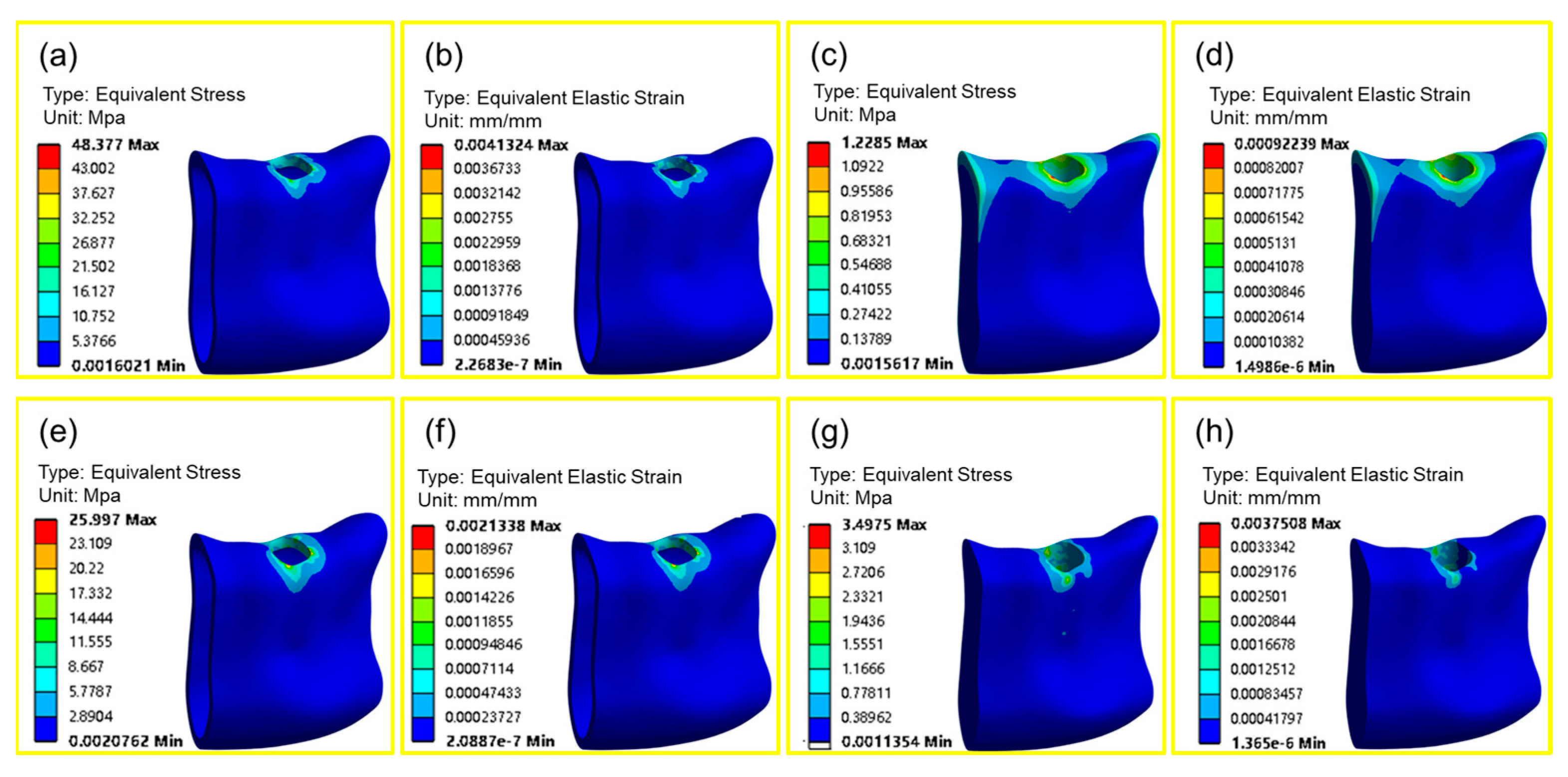
4.3. Biomechanical Analysis
5. Conclusions
- The mechanical properties of the gradient porous structure have a more significant effect on the elastic modulus than the edge porosity, and the effect is more meaningful when the edge porosity is in the range of 20–35%.
- The central porosity has a more significant effect on permeability reduction, but the change of central porosity has almost no impact on permeability when the marginal porosity is more important.
- The biomechanical properties of the gradient porous structure and the homogeneous porous structure can be analyzed to conclude that the stress-shielding effect of the gradient porous structure is more evident than that of the homogeneous porous structure, which can significantly reduce the stress concentration.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Santos, G.M. The impact of tooth loss and the role of implantology in the elderly population. MOJ Gerontol. Geriatr. 2023, 8, 79–81. [Google Scholar] [CrossRef]
- Wang, J.Q.; Zhang, Y.; Pang, M.; Wang, Y.Q.; Yuan, J.; Peng, H.; Li, H.W. Biomechanical Comparison of Six Different Root-Analog Implants and the Conventional Morse Taper Implant by Finite Element Analysis. Front. Genet. 2022, 13, 915679. [Google Scholar] [CrossRef]
- Baltazar, C.M.; Salinas, B.G.; Franco, N.R.; Sandoval, G.M.; González, G.M.; Whitney, A.B.; Baltazar-Ruiz, A. Root morphology and angulation analysis of mandibular first molar for the planning of immediate implants. A cross-sectional study using CBCT. J. Osseointegration 2023, 15, 233–237. [Google Scholar]
- Nimmawitt, P.; Aliyu, A.A.A.; Lohwongwatana, B.; Arunjaroensuk, S.; Puncreobutr, C.; Mattheos, N.; Pimkhaokham, A. Understanding the stress distribution on anatomic customized root-analog dental implant at bone-implant interface for different bone densities. Materials 2022, 15, 6379. [Google Scholar] [CrossRef]
- Dantas, T.; Madeira, S.; Gasik, M.; Vaz, P.; Silva, F. Customized root-analogue implants: A review on outcomes from clinical trials and case reports. Materials 2021, 14, 2296. [Google Scholar] [CrossRef]
- Naghavi, S.A.; Hua, J.; Moazen, M.; Taylor, S.; Liu, C. On the FE Modelling of Short Stem Porous Hip Implant Design for Preventing Stress Shielding & Promoting Osseointegration. In Proceedings of the 2nd International Conference on Biomaterials, BIO-DES MANUF 2019, Vienna, Austria, 20–21 May 2019. [Google Scholar]
- Zhang, W. Study on the Structure Design of Porous Dental Implants Based on SLM Technology. Master’s Thesis, Zhejiang University of Technology, Hangzhou, China, 2018; pp. 4–5. [Google Scholar]
- Wang, F.; Jiang, Z.; Si, P.; Lan, J. Biomechanical Analysis of Functionally Graded Root Analog Implants on Alveolar Bone: A 3D Finite Element Study. Int. J. Oral Maxillofac. Implant. 2021, 36, e63. [Google Scholar] [CrossRef]
- Kladovasilakis, N.; Tsongas, K.; Tzetzis, D. Finite element analysis of orthopedic hip implant with functionally graded bioinspired lattice structures. Biomimetics 2020, 5, 44. [Google Scholar] [CrossRef] [PubMed]
- Abate, K.M.; Nazir, A.; Jeng, J.Y. Design, optimization, and selective laser melting of vin tiles cellular structure-based hip implant. J. Adv. Manuf. Technol. 2021, 112, 2037–2050. [Google Scholar] [CrossRef]
- Tang, Z.; Zhou, Y.; Ma, L.; Li, J. Flow performance of porous implants with different geometry: Line, surface, and volume structures. Int. J. Bioprinting 2023, 9, 700. [Google Scholar] [CrossRef]
- Chen, Z.; Chen, Y.; Wang, Y.; Deng, J.; Wang, X.; Wang, Q.; Yu, L. Polyetheretherketone implants with hierarchical porous structure for boosted osseointegration. Biomater. Res. 2023, 27, 61. [Google Scholar] [CrossRef] [PubMed]
- Jetté, B.; Brailovski, V.; Dumas, M.; Simoneau, C.; Terriault, P. Femoral stem incorporating a diamond cubic lattice structure: Design, manufacture and testing. J. Mech. Behav. Biomed. Mater. 2018, 77, 58–72. [Google Scholar] [CrossRef]
- Xu, W.; Yu, A.; Lu, X.; Tamaddon, M.; Wang, M.; Zhang, J.; Su, B. Design and performance evaluation of additively manufactured composite lattice structures of commercially pure Ti (CP–Ti). Bioact. Mater. 2021, 6, 1215–1222. [Google Scholar] [CrossRef]
- Sarkari, M.; Rahmati, S.; Nikkhoo, M. Design and Analysis of Porous Structure Implant Based on Primitive Triply Periodic Minimal Surface. In Additive Manufacturing in Multidisciplinary Cooperation and Production; Springer International Publishing: Cham, Switzerland, 2023; pp. 219–233. [Google Scholar]
- Feng, J.; Fu, J.; Yao, X.; He, Y. Triply periodic minimal surface (TPMS) porous structures: From multi-scale design, precise additive manufacturing to multidisciplinary applications. Int. J. Extrem. Manuf. 2022, 4, 022001. [Google Scholar] [CrossRef]
- Shang, P.; Ma, B.; Hou, G.; Zhang, Y.; Cui, L.; Song, W.; Liu, Y. A novel artificial vertebral implant with Gyroid porous structures for reducing the subsidence and mechanical failure rate after vertebral body replacement. J. Orthop. Res. 2023, 18, 828. [Google Scholar] [CrossRef] [PubMed]
- Korshunova, N.; Alaimo, G.; Hosseini, S.B.; Carraturo, M.; Reali, A.; Niiranen, J.; Kollmannsberger, S. Image-based numerical characterization and experimental validation of tensile behavior of octet-truss lattice structures. Addit. Manuf. 2021, 41, 101949. [Google Scholar] [CrossRef]
- Ren, L.; Zhang, D. A Simple and Effective Modeling Method for 3D Porous Irregular Structures. Processes 2022, 10, 464. [Google Scholar] [CrossRef]
- Armendáriz-Mireles, E.N.; Raudi-Butrón, F.D.; Olvera-Carreño, M.A.; Rocha-Rangel, E. Design of bio-inspired irregular porous structure applied to intelligent mobility products. Nexo Rev. Científica 2023, 36, 110–121. [Google Scholar] [CrossRef]
- Wang, C. Research on the Design and Mechanical Properties of Controllable Porous Structure Based on Laser Selective Melting Technology. Master’s Thesis, Nanjing University of Aeronautics and Astronautics, Nanjing, China, 2018; pp. 3–6. [Google Scholar]
- Rajagopalan, S.; Robb, R.A. Schwarz meets Schwann: Design and fabrication of biomorphic and durataxic tissue engineering scaffolds. Med. Image Anal. 2006, 10, 693–712. [Google Scholar] [CrossRef]
- Sun, C.; Wang, L.; Kang, J.; Li, D.; Jin, Z. Biomechanical optimization of elastic modulus distribution in porous femoral stem for artificial hip joints. J. Bionic Eng. 2018, 15, 693–702. [Google Scholar] [CrossRef]
- Matena, J.; Petersen, S.; Gieseke, M.; Kampmann, A.; Teske, M.; Beyerbach, M.; Nolte, I. SLM produced porous titanium implant improvements for enhanced vascularization and osteoblast seeding. Int. J. Mol. Sci. 2015, 16, 7478–7492. [Google Scholar] [CrossRef] [PubMed]
- Chang, B.; Song, W.; Han, T.; Yan, J.; Li, F.; Zhao, L.; Zhang, Y. Influence of pore size of porous titanium fabricated by vacuum diffusion bonding of titanium meshes on cell penetration and bone ingrowth. Acta Biomater. 2016, 33, 311–321. [Google Scholar] [CrossRef]
- Shi, J.; Liang, H.; Jiang, J.; Tang, W.; Yang, J. Design and performance evaluation of porous titanium alloy structures for bone implantation. Math. Probl. Eng. 2019, 2019, 5268280. [Google Scholar] [CrossRef]
- Chen, Z.; Yan, X.; Yin, S.; Liu, L.; Liu, X.; Zhao, G.; Fang, H. Influence of the pore size and porosity of selective laser melted Ti6Al4V ELI porous scaffold on cell proliferation, osteogenesis and bone ingrowth. Mater. Sci. Eng. C 2020, 106, 110289. [Google Scholar] [CrossRef]
- Ataee, A.; Li, Y.; Fraser, D.; Song, G.; Wen, C. Anisotropic Ti-6Al-4V gyroid scaffolds manufactured by electron beam melting (EBM) for bone implant applications. Mater. Des. 2018, 137, 345–354. [Google Scholar] [CrossRef]
- Yánez, A.; Cuadrado, A.; Martel, O.; Afonso, H.; Monopoli, D. Gyroid porous titanium structures: A versatile solution to be used as scaffolds in bone defect reconstruction. Mater. Des. 2018, 140, 21–29. [Google Scholar] [CrossRef]
- Lu, X.; Zhang, D.; Xu, W.; Yu, A.; Zhang, J.; Tamaddon, M.; Su, B. The effect of Cu content on corrosion, wear and tribocorrosion resistance of Ti-Mo-Cu alloy for load-bearing bone implants. Corros. Sci. 2020, 177, 109007. [Google Scholar] [CrossRef]
- Zadpoor, A.A.; Hedayati, R. Analytical relationships for prediction of the mechanical properties of additively manufactured porous biomaterials. J. Biomed. Mater. Res. A 2016, 104, 3164–3174. [Google Scholar] [CrossRef] [PubMed]
- Esen, Z.; Bor, Ş. Processing of titanium foams using magnesium spacer particles. Scr. Mater. 2007, 56, 341–344. [Google Scholar] [CrossRef]
- Huang, C.C.; Li, M.J.; Tsai, P.I.; Kung, P.C.; Chen, S.Y.; Sun, J.S.; Tsou, N.T. Novel design of additive manufactured hollow porous implants. Dent. Mater. 2020, 36, 1437–1451. [Google Scholar] [CrossRef]
- Cheng, Z.; Xu, R.; Jiang, P.X. Morphology, flow and heat transfer in triply periodic minimal surface based porous structures. Int. J. Heat. Mass. Transf. 2021, 170, 120902. [Google Scholar] [CrossRef]
- Zhang, L.; Song, B.; Yang, L.; Shi, Y. Tailored mechanical response and mass transport characteristic of selective laser melted porous metallic biomaterials for bone scaffolds. Acta Biomater. 2020, 112, 298–315. [Google Scholar] [CrossRef]
- Syahrom, A.; Kadir, M.R.A.; Abdullah, J.; Öchsner, A. Permeability studies of artificial and natural cancellous bone structures. Med. Eng. Phys. 2013, 35, 792–799. [Google Scholar] [CrossRef]
- Kitagawa, T.; Tanimoto, Y.; Nemoto, K.; Aida, M. Influence of cortical bone quality on stress distribution in bone around dental implant. Dent. Mater. J. 2005, 24, 219–224. [Google Scholar] [CrossRef]
- Zhai, Y.; Zhang, H.; Liu, T.; Zou, C.; Zhou, C. Mechanical property of Ti6Al4V cylindrical porous structure for dental implants fabricated by selective laser melting. Comput. Methods Biomech. Biomed. Engin 2023, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Bora, R.; Shukla, M.; Kumar, A. Finite element analysis based design of biomimetic functionally graded Ti-6Al-4V alloy scaffolds for human cortical bone applications. Mater. Today Proc. 2023, 90, 81–85. [Google Scholar] [CrossRef]
- Zeng, S.; Liu, G.; He, W.; Wang, J.; Ye, J.; Sun, C. Design and performance prediction of selective laser melted porous structure for femoral stem. Mater. Today Commun. 2023, 34, 104987. [Google Scholar] [CrossRef]
- Rakesh, P.; Pal, B. Finite element analysis of Ti6Al4V porous structures for low-stiff hip implant application. Int. J. Simul. Multidiscip. Des. Optim. 2021, 12, 12. [Google Scholar] [CrossRef]
- Lebea, L.C.; Ngwangwa, H.; Desai, D.; Nemavhola, F. Life prediction and experimental validation of a 3D printed dental Titanium Ti64ELI implant. Preprints 2021, 2021080379. [Google Scholar] [CrossRef]
- Liu, F.; Cheng, W.M.; Shao, J.B. Structure optimization and finite element analysis of the human body exoskeletons lower limb power. In Proceedings of the Social Robotics: 4th International Conference 2012, ICSR 2012, Chengdu, China, 29–31 October 2012; Proceedings 4. Springer: Berlin/Heidelberg, Germany, 2012; pp. 631–640. [Google Scholar]
- Ma, Z.; Zhang, D.Z.; Liu, F.; Jiang, J.; Zhao, M.; Zhang, T. Lattice structures of Cu-Cr-Zr copper alloy by selective laser melting: Microstructures, mechanical properties and energy absorption. Mater. Des. 2020, 187, 108406. [Google Scholar] [CrossRef]



| Project | Parameter |
|---|---|
| Laser power | 200 W |
| Scanning speed | 1200 m/s |
| Scanning distance | 140 μm |
| Thickness of powder layer | 30 μm |
| Structure | Structure Modulus of Elasticity (Gpa) | Poisson’s Ratio |
|---|---|---|
| Porous implants | 110 | 0.35 |
| Cortical bone | 13.7 | 0.3 |
| Cancellous bone | 1.37 | 0.3 |
| Type of Structure | Modulus of Elasticity (Experimental) | Yield Strength (Experimental) | Modulus of Elasticity (Simulation) | Yield Strength (Simulation) |
|---|---|---|---|---|
| G60-20 | 13.9 GPa | 415.68 MPa | 18.9 GPa | 784.3 MPa |
| G60-30 | 6.6 GPa | 420.59 MPa | 10.1 GPa | 615.5 MPa |
| G60-40 | 4.1 GPa | 409.88 MPa | 6.6 GPa | 476.6 MPa |
| G60-50 | 3.9 GPa | 175.8 MPa | 5.0 GPa | 331.7 MPa |
| G70-20 | 13.5 GPa | 433.14 MPa | 17.6 GPa | 746.8 MPa |
| G70-30 | 6.3 GPa | 460.24 MPa | 10.6 GPa | 575.3 MPa |
| G70-40 | 4.3 GPa | 312.33 MPa | 5.9 GPa | 427.0 MPa |
| G70-50 | 3.8 GPa | 191.45 MPa | 4.5 GPa | 293.3 MPa |
| G80-20 | 13.4 GPa | 423.26 MPa | 17.1 GPa | 705.0 MPa |
| G80-30 | 4.4 GPa | 499.79 MPa | 9.0 GPa | 535.5 MPa |
| G80-40 | 4.2 GPa | 273.84 MPa | 7.5 GPa | 391.2 MPa |
| G80-50 | 3.8 GPa | 138.94 MPa | 5.9 GPa | 219.5 MPa |
| G90-20 | 11.6 GPa | 354.38 MPa | 15.3 GPa | 681.5 MPa |
| G90-30 | 4.8 GPa | 405.76 MPa | 9.1 GPa | 507.2 MPa |
| G90-40 | 3.9 GPa | 300.08 MPa | 5.9 GPa | 360.1 MPa |
| G90-50 | 3.8 GPa | 176.13 MPa | 4.8 GPa | 230.7 MPa |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, L.; Ma, S.; Zhang, Y.; Zhu, S.; Wu, S.; Liu, G.; Yang, G. Parametric Design of Porous Structure and Optimal Porosity Gradient Distribution Based on Root-Shaped Implants. Materials 2024, 17, 1137. https://doi.org/10.3390/ma17051137
Liu L, Ma S, Zhang Y, Zhu S, Wu S, Liu G, Yang G. Parametric Design of Porous Structure and Optimal Porosity Gradient Distribution Based on Root-Shaped Implants. Materials. 2024; 17(5):1137. https://doi.org/10.3390/ma17051137
Chicago/Turabian StyleLiu, Lijian, Shaobo Ma, Yongkang Zhang, Shouxiao Zhu, Shuxuan Wu, Guang Liu, and Guang Yang. 2024. "Parametric Design of Porous Structure and Optimal Porosity Gradient Distribution Based on Root-Shaped Implants" Materials 17, no. 5: 1137. https://doi.org/10.3390/ma17051137
APA StyleLiu, L., Ma, S., Zhang, Y., Zhu, S., Wu, S., Liu, G., & Yang, G. (2024). Parametric Design of Porous Structure and Optimal Porosity Gradient Distribution Based on Root-Shaped Implants. Materials, 17(5), 1137. https://doi.org/10.3390/ma17051137







