Community-Based Participatory Research: Partnering with College Students to Develop a Tailored, Wellness-Focused Intervention for University Campuses
Abstract
1. Introduction
2. Materials and Methods
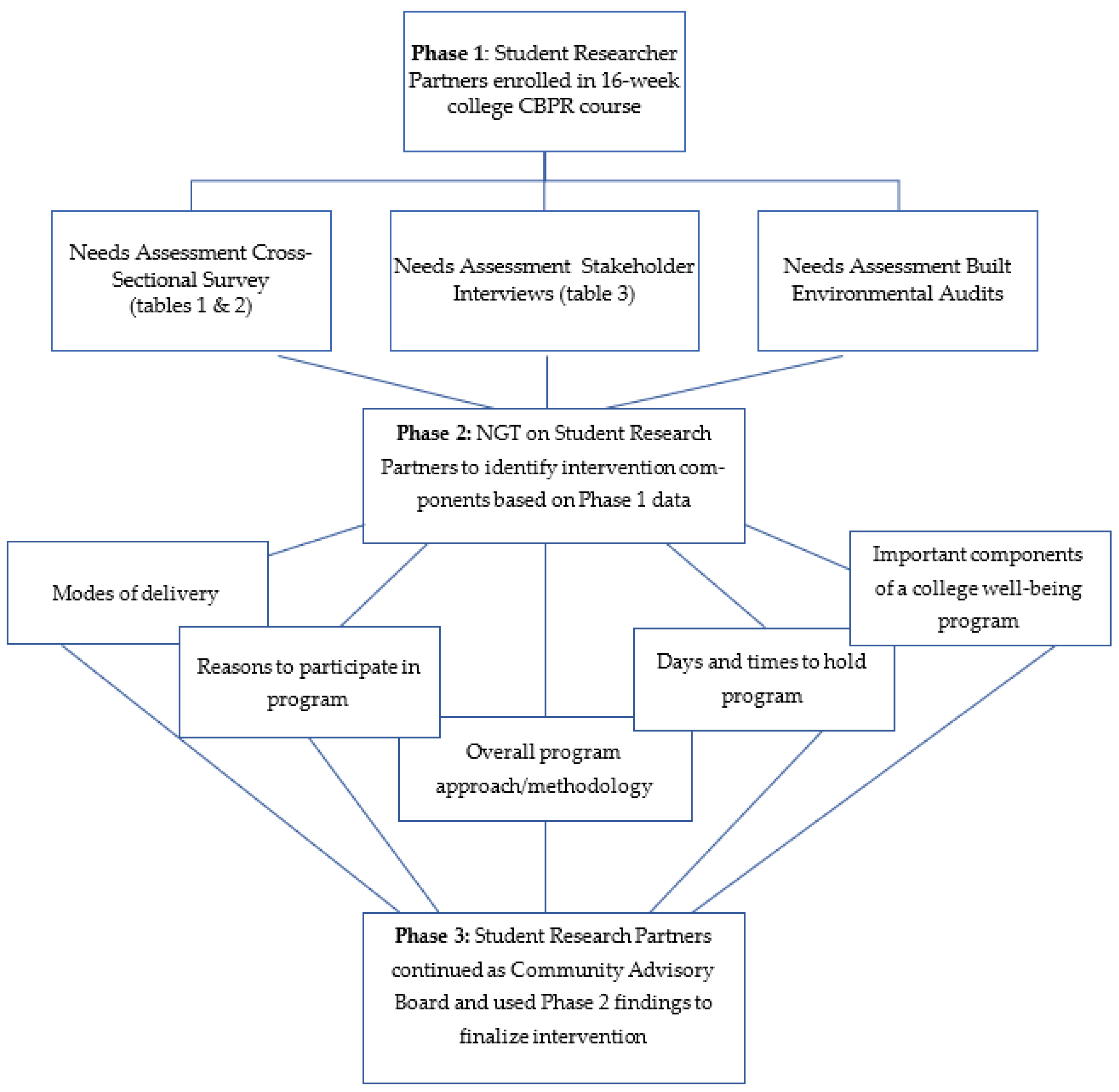
2.1. Phase 1: Community-Based Participatory Research Course for Undergraduate Student Research Partners
2.1.1. Student Led Campus Health Needs Assessment
2.1.2. Campus-Wide Cross-Sectional Needs Assessment Survey
2.1.3. Campus Health Stakeholder Interviews
2.1.4. Environment Assessment
2.2. Phase 2: Hybrid Program Planning Workshop
2.3. Community Advisory Board
2.4. Data Analysis
2.4.1. Phase 1: Needs Assessment Data
2.4.2. Phase 2: NGT Findings
2.4.3. Phase 3: Community Advisory Board
3. Results
3.1. Phase 1 Needs Assessment Data
3.2. Phase 2: NGT Outcomes
3.3. Phase 3: Community Advisory Board Outcomes and Program Plans
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Cunningham, S.A.; Hardy, S.T.; Jones, R.; Ng, C.; Kramer, M.R.; Narayan, K. Changes in the incidence of childhood obesity. Pediatrics 2022, 150, e2021053708. [Google Scholar] [CrossRef] [PubMed]
- Wilson, E. Where next for youth mental health? Reflections on current research and considerations for the future. J. Ment. Health 2020, 29, 371–375. [Google Scholar] [CrossRef] [PubMed]
- United States Department of Education. Fall Enrollment component (provisional data). Washington, D.C. Natl. Cent. Educ. Stat. IPEDS 2021. [Google Scholar]
- Terry, P.; Lagergren, J.; Hansen, H.; Wolk, A.; Nyren, O. Fruit and vegetable consumption in the prevention of oesophageal and cardia cancers. Eur. J. Cancer Prev. 2001, 10, 365–369. [Google Scholar] [CrossRef]
- Oyebode, O.; Gordon-Dseagu, V.; Walker, A.; Mindell, J.S. Fruit and vegetable consumption and all-cause, cancer and CVD mortality: Analysis of Health Survey for England data. J. Epidemiol. Community Health 2014, 68, 856–862. [Google Scholar] [CrossRef]
- Substance Abuse and Mental Health Services Administration, Key substance use and mental health indicators in the United States: Results from the 2018 National Survey on Drug Use and Health (HHS Publication No. PEP19-5068, NSDUH Series H-54). In Substance Abuse and Mental Health Services Administration; Center for Behavioral Health Statistics and Quality: Rockville, MD, USA, 2019.
- Hussain, R.; Guppy, M.; Robertson, S.; Temple, E. Physical and mental health perspectives of first year undergraduate rural university students. BMC Public Health 2013, 13, 848. [Google Scholar] [CrossRef]
- Wattick, R.A.; Hagedorn, R.L.; Olfert, M.D. Relationship between diet and mental health in a young adult Appalachian college population. Nutrients 2018, 10, 957. [Google Scholar] [CrossRef]
- Pryor, L.; Lioret, S.; Van Der Waerden, J.; Fombonne, É.; Falissard, B.; Melchior, M. Food insecurity and mental health problems among a community sample of young adults. Soc. Psychiatry Psychiatr. Epidemiol. 2016, 51, 1073–1081. [Google Scholar] [CrossRef]
- Oh, H.; Smith, L.; Jacob, L.; Du, J.; Shin, J.I.; Zhou, S.; Koyanagi, A. Food insecurity and mental health among young adult college students in the United States. J. Affect. Disord. 2022, 303, 359–363. [Google Scholar] [CrossRef]
- Pelletier, J.E.; Lytle, L.A.; Laska, M.N. Stress, health risk behaviors, and weight status among community college students. Health Educ. Behav. 2016, 43, 139–144. [Google Scholar] [CrossRef]
- Collins, S.; Dash, S.; Allender, S.; Jacka, F.; Hoare, E. Diet and mental health during emerging adulthood: A systematic review. Emerg. Adulthood 2022, 10, 645–659. [Google Scholar] [CrossRef]
- Kwon, S.C.; Tandon, S.D.; Islam, N.; Riley, L.; Trinh-Shevrin, C. Applying a community-based participatory research framework to patient and family engagement in the development of patient-centered outcomes research and practice. Transl. Behav. Med. 2018, 8, 683–691. [Google Scholar] [CrossRef]
- Wallerstein, N.; Duran, B. The theoretical, historical and practice roots of CBPR. Community-Based Particip. Res. Health Adv. Soc. Health Equity 2017, 17–29. [Google Scholar]
- Korn, A.R.; Hennessy, E.; Tovar, A.; Finn, C.; Hammond, R.A.; Economos, C.D. Engaging coalitions in community-based childhood obesity prevention interventions: A mixed methods assessment. Child. Obes. 2018, 14, 537–552. [Google Scholar] [CrossRef]
- Bulmer, S.M.; Barton, B.A.; Liefeld, J.; Montauti, S.; Santos, S.; Richard, M.; Hnath, L.; Pelletier, K.; Lalanne, J. Using CBPR methods in college health research: Exploring excessive alcohol consumption. J. Adolesc. Res. 2016, 31, 232–258. [Google Scholar] [CrossRef]
- Olfert, M.; Barr, M.; Riggsbee, K.; Kattelmann, K.; Leischner, K.; Mathews, A.; Vilaro, M.; Colby, S. A Community Based Participatory Approach to Training Young Adults to Design and Implement a Social Marketing Framed Lifestyle Intervention on Their College Campus. Educ. Sci. 2018, 8, 150. [Google Scholar] [CrossRef]
- Graham, L.F.; Aronson, R.E.; Pulliam, R.M.; Mann, L.; Rhodes, S.D. Preventing HIV among black men in college using a CBPR approach. In Innovations in HIV Prevention Research and Practice through Community Engagement; Springer: Berlin/Heidelberg, Germany, 2014; pp. 35–54. [Google Scholar]
- Coffield, E.; Nihiser, A.; Carlson, S.; Collins, J.; Cawley, J.; Lee, S.; Economos, C. Shape Up Somerville’s return on investment: Multi-group exposure generates net-benefits in a child obesity intervention. Prev. Med. Rep. 2019, 16, 100954. [Google Scholar] [CrossRef]
- Budgen, C.; Callaghan, D.; Gamble, D.; Wiebe, R.; Reimer, C.; Fedderson, M.; Dunn, S.; Johnson, R.; McHugh, N.; Morrison, H. Creating a Healthier Campus Community Using Action Research and Health Promotion Strategies: Students and Organizational Leaders as Partners; University of British Columbia: Vancouver, BC, USA, 2011. [Google Scholar]
- Chen, S.-P.; Horgan, S.; Jones, J.; Krauss, E.; Stuart, H. Involving student peer researchers for gender-informed health promotion: A community-based participatory action research. Educ. Action Res. 2021, 1–19. [Google Scholar] [CrossRef]
- Corwin, L.A.; Graham, M.J.; Dolan, E.L. Modeling course-based undergraduate research experiences: An agenda for future research and evaluation. CBE—Life Sci. Educ. 2015, 14, es1. [Google Scholar] [CrossRef]
- Turner, A.N.; Challa, A.K.; Cooper, K.M. Student perceptions of authoring a publication stemming from a course-based undergraduate research experience (CURE). CBE—Life Sci. Educ. 2021, 20, ar46. [Google Scholar] [CrossRef]
- Barr, M.L.; Colby, S.E.; Riggsbee, K.; Leischner, K.; Mathews, A.E.; Vilaro, M.J.; Kattelmann, K.K.; Olfert, M.D. Health behaviors of student community research partners when designing and implementing a healthy lifestyle intervention on college campuses. Behav. Sci. 2018, 8, 99. [Google Scholar] [CrossRef] [PubMed]
- Zhang, E.; Yigletu, S.; Lieberman, H.; Kosinski, K.; Mukthineni, R.; McLeod, D.; Rubel, B.; Tendulkar, S. Perspectives on initiating community-based participatory research partnerships. J. Community Engagem. Scholarsh. 2020, 12, 7. [Google Scholar] [CrossRef]
- Olfert, M.D.; Barr, M.L.; Charlier, C.M.; Famodu, O.A.; Zhou, W.; Mathews, A.E.; Byrd-Bredbenner, C.; Colby, S.E. Self-reported vs. measured height, weight, and BMI in young adults. Int. J. Environ. Res. Public Health 2018, 15, 2216. [Google Scholar] [CrossRef] [PubMed]
- Colby, S.; Zhou, W.; Allison, C.; Mathews, A.E.; Olfert, M.D.; Morrell, J.S.; Byrd-Bredbenner, C.; Greene, G.; Brown, O.; Kattelmann, K.; et al. Development and Validation of the Short Healthy Eating Index Survey with a College Population to Assess Dietary Quality and Intake. Nutrients 2020, 12, 2611. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. Perceived stress scale. Meas. Stress A Guide Health Soc. Sci. 1994, 10, 1–2. [Google Scholar]
- Moriarty, D.G.; Zack, M.M.; Kobau, R. The Centers for Disease Control and Prevention’s Healthy Days Measures–Population tracking of perceived physical and mental health over time. Health Qual. Life Outcomes 2003, 1, 37. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds III, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Coleman-Jensen, A.; Rabbitt, M.; Gregory, C.; Singh, A. Household Food Security in the United States in 2018; ERR-270; Economic Research Service: Washington, DC, USA, 2019. [Google Scholar]
- Byrd-Bredbenner, C. Food preparation knowledge and attitudes of young adults: Implications for nutrition practice. Top. Clin. Nutr. 2004, 19, 154–163. [Google Scholar] [CrossRef]
- Byrd-Bredbenner, C. Food preparation knowledge and confidence of young adults. J. Nutr. Recipe Menu Dev. 2005, 3, 37–50. [Google Scholar] [CrossRef]
- Horacek, T.M.; Simon, M.; Dede Yildirim, E.; White, A.A.; Shelnutt, K.P.; Riggsbee, K.; Olfert, M.D.; Morrell, J.S.; Mathews, A.E.; Zhou, W. Development and validation of the policies, opportunities, initiatives and notable topics (POINTS) audit for campuses and worksites. Int. J. Environ. Res. Public Health 2019, 16, 778. [Google Scholar] [CrossRef]
- Nikolaus, C.J.; Laurent, E.; Loehmer, E.; An, R.; Khan, N.; McCaffrey, J. Nutrition environment food pantry assessment tool (NEFPAT): Development and evaluation. J. Nutr. Educ. Behav. 2018, 50, 724–728.e721. [Google Scholar] [CrossRef]
- Lim, R.B.T.; Teng, C.W.C.; Azfar, J.; Bun, D.; Goh, G.J.; Lee, J.J.-M. An integrative approach to needs assessment and curriculum development of the first public health major in Singapore. Front. Public Health 2020, 8, 182. [Google Scholar] [CrossRef]
- Anstey, J.E.; Jensen, T.P.; Afshar, N. Point-of-Care Ultrasound Needs Assessment, Curriculum Design, and Curriculum Assessment in a Large Academic Internal Medicine Residency Program. South. Med. J. 2018, 111, 444–448. [Google Scholar] [CrossRef]
- Browning-Keen, V.; Camel, S.P. Use of Get FRUVED™ Healthy Campus Environmental Audits to Teach Community Nutrition Program Planning and Leadership. J. Nutr. Educ. Behav. 2018, 50, S198–S199. [Google Scholar] [CrossRef]
- Hamilton, K.C.; Howard-Baptiste, S.; Hahn, K.J.; Powell, M.C.; E’tienne, F.E.; Graham, M.J. Mixed Methods with Strategic Collaborations: Systematically Designing an After-School Physical Activity and Nutrition Program. Prog. Community Health Partnersh. Res. Educ. Action 2020, 14, 431–442. [Google Scholar] [CrossRef]
- Riggsbee, K.; Colby, S.; Kidd, T.; Brown, O.; White, A.; Horacek, T.; Olfert, M.D.; Mathews, A.; Kattelmann, K.; Shelnutt, K. Development and Pilot Testing of a Community Based Participatory Research Obesity Prevention Program on College Campuses. J. Nutr. Educ. Behav. 2018, 50, S55. [Google Scholar] [CrossRef]
- Kattelmann, K.K.; White, A.A.; Greene, G.W.; Byrd-Bredbenner, C.; Hoerr, S.L.; Horacek, T.M.; Kidd, T.; Colby, S.; Phillips, B.W.; Koenings, M.M. Development of Young Adults Eating and Active for Health (YEAH) internet-based intervention via a community-based participatory research model. J. Nutr. Educ. Behav. 2014, 46, S10–S25. [Google Scholar] [CrossRef]
- Merhout, F.; Doyle, J. Socioeconomic status and diet quality in college students. J. Nutr. Educ. Behav. 2019, 51, 1107–1112. [Google Scholar] [CrossRef]
- Whatnall, M.; Patterson, A.; Burrows, T.; Hutchesson, M. Higher diet quality in university students is associated with higher academic achievement: A cross-sectional study. J. Hum. Nutr. Diet. 2019, 32, 321–328. [Google Scholar] [CrossRef]
- Pelletier, J.E.; Laska, M.N. Campus food and beverage purchases are associated with indicators of diet quality in college students living off campus. Am. J. Health Promot. 2013, 28, 80–87. [Google Scholar] [CrossRef] [PubMed]
- Hurst, C.S.; Baranik, L.E.; Daniel, F. College student stressors: A review of the qualitative research. Stress Health 2013, 29, 275–285. [Google Scholar] [CrossRef]
- Nazmi, A.; Martinez, S.; Byrd, A.; Robinson, D.; Bianco, S.; Maguire, J.; Crutchfield, R.M.; Condron, K.; Ritchie, L. A systematic review of food insecurity among US students in higher education. J. Hunger. Environ. Nutr. 2019, 14, 725–740. [Google Scholar] [CrossRef]
- Hagedorn-Hatfield, R.L.; Hood, L.B.; Hege, A. A Decade of College Student Hunger: What We Know and Where We Need to Go. Front. Public Health 2022, 10, 269. [Google Scholar] [CrossRef]
- Olfert, M.D.; Barr, M.L.; Charlier, C.C.; Greene, G.W.; Zhou, W.; Colby, S.E. Sex differences in lifestyle behaviors among US college freshmen. Int. J. Environ. Res. Public Health 2019, 16, 482. [Google Scholar] [CrossRef] [PubMed]
- McNamara, J.; Olfert, M.D.; Sowers, M.; Colby, S.; White, A.; Byrd-Bredbenner, C.; Kattelmann, K.; Franzen-Castle, L.D.; Brown, O.; Kidd, T. Development of an instrument measuring perceived environmental healthfulness: Behavior environment perception survey (BEPS). J. Nutr. Educ. Behav. 2020, 52, 152–161. [Google Scholar] [CrossRef]
- Szczepanski, J.R.; Litchfield, R.E.; Beirman, E.A.; Nolting, L.M.; Genschel, U. Effects of a Culinary Boot Camp intervention on food/nutrition aptitudes and dietary intake of college students. J. Am. Coll. Health 2021, 1–10. [Google Scholar] [CrossRef]
- Gustafson, A.; Jilcott Pitts, S.B.; McQuerry, K.; Babtunde, O.; Mullins, J. A Mentor-Led Text-Messaging Intervention Increases Intake of Fruits and Vegetables and Goal Setting for Healthier Dietary Consumption among Rural Adolescents in Kentucky and North Carolina, 2017. Nutrients 2019, 11, 593. [Google Scholar] [CrossRef] [PubMed]
| Variable | n | Mean (SD), or % |
|---|---|---|
| Age, year | 896 | 19.7 (1.6) |
| Body mass index | 961 | 24.7 (5.1) |
| Gender | ||
| Female | 614 | 62.6 |
| Male | 316 | 32.3 |
| Other | 49 | 5.1 |
| Race/Ethnicity | ||
| White | 885 | 90.4 |
| Hispanic or Latino | 29 | 3.0 |
| Native American Black or African American | 26 | 2.7 |
| Other | 28 | 2.8 |
| Sexual Identity | ||
| Heterosexual | 692 | 70.8 |
| Homosexual | 43 | 4.4 |
| Bisexual | 143 | 14.6 |
| Queer | 37 | 3.8 |
| Questioning/Unsure | 35 | 3.6 |
| Something else | 28 | 2.9 |
| Year in college | ||
| Freshman | 346 | 35.4 |
| Sophomore | 234 | 23.9 |
| Junior | 191 | 19.5 |
| Senior | 207 | 21.1 |
| Dining plan | ||
| Yes | 507 | 51.8 |
| No | 471 | 48.2 |
| Living situation | ||
| On campus | 500 | 51.2 |
| Off campus | 471 | 48.8 |
| Variable | Mean (SD), or % (n) |
|---|---|
| Perceived general health status (n = 971) | |
| Excellent | 6.8 (66) |
| Very Good | 19.9 (193) |
| Good | 43.6 (423) |
| Fair | 23.3 (226) |
| Poor | 6.5 (63) |
| Perceived nutrition health status (n = 954) | |
| Excellent | 5.1 (49) |
| Very good | 15.2 (145) |
| Good | 37.9 (362) |
| Fair | 27.3 (260) |
| Poor | 14.5 (138) |
| Hours of Sleep per night (n = 899) | 6.9 (1.4) |
| Overall sleep quality (n = 976) | |
| Very good | 9.2 (90) |
| Fairly good | 62.4 (609) |
| Fairly bad | 25.6 (250) |
| Very bad | 2.8 (976) |
| Diet Quality (n = 983) | |
| Total Healthy Eating Index | 47.6 (10.1) |
| Servings of Fruit | 0.92 (0.35) |
| Servings of Vegetables | 2.4 (0.52) |
| Cooking Confidence (n = 970) | |
| Cooking methods | 3.8 (0.7) |
| Cooking with specific foods | 4.0 (0.8) |
| Preparing recipes | 4.0 (0.8) |
| Food Security (n = 981) | |
| High | 38.6 (377) |
| Marginal | 25.1 (245) |
| Low | 19.9 (194) |
| Very Low | 16.4 (160) |
| Perceived Stress (n = 970) | |
| Low | 2.8 (27) |
| Moderate | 54.9 (533) |
| High | 42.3 (410) |
| NGT Questions | Top 3 Choices in Ranking Order |
|---|---|
| If you were to participate in a health/well-being program on your campus, what would influence you to participate? | Incentives Convenience Personal Benefit |
| How often would you/others attend program events throughout a semester? Why? | 1–2 times per month Once per week Twice per month |
| Probe: What time of day & day of the week do you believe would work best for events throughout the semester? | Weekday afternoon Weekday 3–4 p.m. Weekday after 4 p.m. |
| In ranking order, what top 3 topic areas/ideas for the intervention do you feel are most important to design for students at your university? | Communication of campus resources Nutrition knowledge and skills Mental health support |
| What top 2 modes of delivery do you feel would work best for our program? (in-person, online, text, mixture, etc.) | A mix of in-person and text Online More in-person |
| Overall, which idea from you and your peers’ presentations do you feel would be best received (people would be most excited to participate in) on your campus? Why? | Education (nutrition, budget, cooking) Sharing campus resources via text Incentive-based punch card |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barr, M.L.; McNamara, J. Community-Based Participatory Research: Partnering with College Students to Develop a Tailored, Wellness-Focused Intervention for University Campuses. Int. J. Environ. Res. Public Health 2022, 19, 16331. https://doi.org/10.3390/ijerph192316331
Barr ML, McNamara J. Community-Based Participatory Research: Partnering with College Students to Develop a Tailored, Wellness-Focused Intervention for University Campuses. International Journal of Environmental Research and Public Health. 2022; 19(23):16331. https://doi.org/10.3390/ijerph192316331
Chicago/Turabian StyleBarr, Makenzie L., and Jade McNamara. 2022. "Community-Based Participatory Research: Partnering with College Students to Develop a Tailored, Wellness-Focused Intervention for University Campuses" International Journal of Environmental Research and Public Health 19, no. 23: 16331. https://doi.org/10.3390/ijerph192316331
APA StyleBarr, M. L., & McNamara, J. (2022). Community-Based Participatory Research: Partnering with College Students to Develop a Tailored, Wellness-Focused Intervention for University Campuses. International Journal of Environmental Research and Public Health, 19(23), 16331. https://doi.org/10.3390/ijerph192316331






