Inflammatory Markers in Dysmenorrhea and Therapeutic Options
Abstract
1. Introduction
The Course of the Menstrual Cycle
2. Pathogenesis of Dysmenorrhea
3. Uterus, Myometrium, Hormone Synthesis, and Inflammation
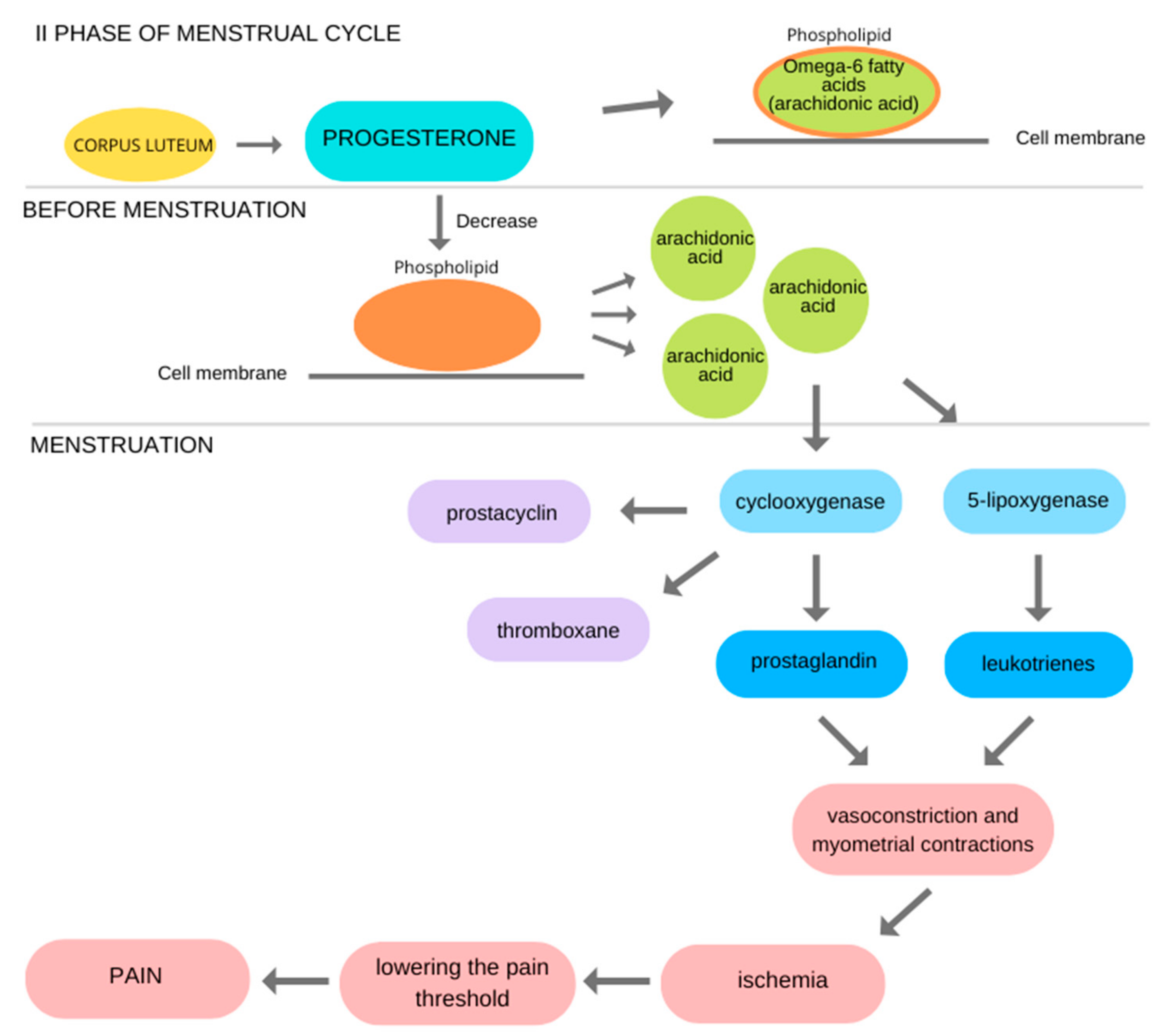
4. The Role of Progesterone in the Menstrual Cycle and the Development of Inflammation
5. The Role of Prostaglandins in Dysmenorrhea and the Development of Inflammation
6. Vasopressin
7. Cytokines and Other Proinflammatory Factors as Inflammatory Mediators in Primary Dysmenorrhea
7.1. Tumour Necrosis Factors Alpha (TNFα)
7.2. Interleukin 6 (IL6) in the Menstrual Cycle
7.3. Vascular Endothelial Growth Factor (VEGF)
7.4. C-Reactive Protein (CRP) in the Menstrual Cycle
8. Pharmacological Treatment Options for Menstrual Pain
9. Physiotherapy for Dysmenorrhea
10. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Dawood, M.Y. Primary Dysmenorrhea Advances in Pathogenesis and Management. Obstet. Gynecol. 2006, 108, 428–441. [Google Scholar] [CrossRef] [PubMed]
- Harel, Z. Dysmenorrhea in Adolescents and Young Adults: Etiology and Management. J. Pediatric Adolesc. Gynecol. 2006, 19, 363–371. [Google Scholar] [CrossRef] [PubMed]
- Coco, A.S. Primary dysmenorrhea. Am. Fam. Physician 1999, 60, 489–496. [Google Scholar] [CrossRef] [PubMed]
- Iacovides, S.; Avidon, I.; Baker, F.C. What we know about primary dysmenorrhea today: A critical review. Hum. Reprod. Update 2015, 21, 762–778. [Google Scholar] [CrossRef] [PubMed]
- Latthe, P.; Latthe, M.; Say, L.; Gülmezoglu, M.; Khan, K.S. WHO systematic review of prevalence of chronic pelvic pain: A neglected reproductive health morbidity. BMC Public Health 2006, 6, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Messinis, I.E.; Messini, C.I.; Dafopoulos, K. Novel aspects of the endocrinology of the menstrual cycle. Reprod. Biomed. Online 2014, 28, 714–722. [Google Scholar] [CrossRef] [PubMed]
- Ryan, S.A. The Treatment of Dysmenorrhea. Pediatric Clin. N. Am. 2017, 64, 331–342. [Google Scholar] [CrossRef]
- Draper, C.F.; Duisters, K.; Weger, B.; Chakrabarti, A.; Harms, A.C.; Brennan, L.; Hankemeier, T.; Goulet, L.; Konz, T.; Martin, F.P.; et al. Menstrual cycle rhythmicity: Metabolic patterns in healthy women. Sci. Rep. 2018, 8, 1–15. [Google Scholar] [CrossRef]
- Maybin, J.A.; Critchley, H.O.D. Progesterone: A pivotal hormone at menstruation. Ann. N. Y. Acad. Sci. 2011, 1221, 88–97. [Google Scholar] [CrossRef]
- Hailemeskel, S.; Demissie, A.; Assefa, N. Primary dysmenorrhea magnitude, associated risk factors, and its effect on academic performance: Evidence from female university students in Ethiopia. Int. J. Womens Health 2016, 8, 489–496. [Google Scholar] [CrossRef]
- Bulletti, C.; De Ziegler, D.; Polli, V.; Diotallevi, L.; Del Ferro, E.; Flamigni, C. Uterine contractility during the menstrual cycle. Hum. Reprod. 2000, 15, 81–89. [Google Scholar] [CrossRef] [PubMed]
- Dawood, M.Y. Dysmenorrhea and prostaglandins. In Gynecologic Endocrinology, 4th ed.; Gold, J.J., Josimovich, J.B., Eds.; Plenum Publishing Corporation: New York, NY, USA, 1987; pp. 405–421. ISBN 1461292727. [Google Scholar]
- Pickles, V.R.; Hall, W.J.; Best, F.A.; Smith, G.N. Prostaglandins in endometrium and menstrual fluid from normal and dysmenorrhoeic Subjects. BJOG 1965, 72, 185–192. [Google Scholar] [CrossRef] [PubMed]
- Lundström, V.; Green, K. Endogenous levels of prostaglandin F2α and its main metabolites in plasma and endometrium of normal and dysmenorrheic women. Am. J. Obstet. Gynecol. 1978, 130, 640–646. [Google Scholar] [CrossRef]
- Balbi, C.; Musone, R.; Menditto, A.; Di Prisco, L.; Cassese, E.; D’Ajello, M.; Ambrosio, D.; Cardone, A. Influence of menstrual factors and dietary habits on menstrual pain in adolescence age. Eur. J. Obstet. Gynecol. Reprod. Biol. 2000, 91, 143–148. [Google Scholar] [CrossRef]
- Kitamura, M.; Takeda, T.; Koga, S.; Nagase, S.; Yaegashi, N. Relationship between premenstrual symptoms and dysmenorrhea in Japanese high school students. Arch. Womens Ment. Health 2012, 15, 131–133. [Google Scholar] [CrossRef]
- Najafi, N.; Khalkhali, H.; Moghaddam Tabrizi, F.; Zarrin, R. Major dietary patterns in relation to menstrual pain: A nested case control study. BMC Womens Health 2018, 18, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Finn, C.A. Implantation, menstruation and inflammation. Biol. Rev. Camb. Philosphical Soc. 1986, 61, 313–328. [Google Scholar] [CrossRef]
- Salamonsen, L.A. Tissue injury and repair in the female human reproductive tract. Reproduction 2003, 125, 301–311. [Google Scholar] [CrossRef]
- Hawkins, S.M.; Matzuk, M.M. The menstrual cycle: Basic biology. Ann. N. Y. Acad. Sci. 2008, 1135, 10–18. [Google Scholar] [CrossRef]
- King, A.E.; Critchley, H.O.D. Oestrogen and progesterone regulation of inflammatory processes in the human endometrium. J. Steroid Biochem. Mol. Biol. 2010, 120, 116–126. [Google Scholar] [CrossRef]
- Xu, C.; Liu, W.; You, X.; Leimert, K.; Popowycz, K.; Fang, X.; Wood, S.L.; Slater, D.M.; Sun, Q.; Gu, H.; et al. PGF2α modulates the output of chemokines and pro-inflammatory cytokines in myometrial cells from term pregnant women through divergent signaling pathways. Mol. Hum. Reprod. 2015, 21, 603–614. [Google Scholar] [CrossRef]
- Leimert, K.B.; Verstraeten, B.S.; Messer, A.; Nemati, R.; Blackadar, K.; Fang, X.; Robertson, S.A.; Chemtob, S.; Olson, D.M. Cooperative effects of sequential PGF2α and IL-1β on IL-6 and COX-2 expression in human myometrial cells. Biol. Reprod. 2019, 100, 1370–1385. [Google Scholar] [CrossRef] [PubMed]
- Evans, J.; Salamonsen, L.A. Inflammation, leukocytes and menstruation. Rev. Endocr. Metab. Disord. 2012, 13, 277–288. [Google Scholar] [CrossRef] [PubMed]
- Harel, Z. Dysmenorrhea in adolescents and young adults: An update on pharmacological treatments and management strategies. Expert Opin. Pharmacother. 2012, 13, 2157–2170. [Google Scholar] [CrossRef]
- Strömberg, P.; Åkerlund, M.; Forsling, M.L.; Granström, E.; Kindahl, H. Vasopressin and Prostaglandins in Premenstrual Pain and Primary Dysmenorrhea. Acta Obstet. Gynecol. Scand. 1984, 63, 533–538. [Google Scholar] [CrossRef] [PubMed]
- Liedman, R.; Hansson, S.R.; Howe, D.; Igidbashian, S.; Mcleod, A.; Russell, R.J.; Åkerlund, M. Reproductive hormones in plasma over the menstrual cycle in primary dysmenorrhea compared with healthy subjects. Gynecol. Endocrinol. 2008, 24, 508–513. [Google Scholar] [CrossRef] [PubMed]
- Forsling, M.L.; Akerlund, M.; Stromberg, P. Variations in plasma concentrations of vasopressin during the menstrual cycle. J. Endocrinol. 1981, 89, 263–266. [Google Scholar] [CrossRef] [PubMed]
- Liedman, R.; Hansson, S.R.; Howe, D.; Igidbashian, S.; Russell, R.J.; Åkerlund, M. Endometrial expression of vasopressin, oxytocin and their receptors in patients with primary dysmenorrhoea and healthy volunteers at ovulation. Eur. J. Obstet. Gynecol. Reprod. Biol. 2008, 137, 189–192. [Google Scholar] [CrossRef]
- Valentin, L.; Sladkevicius, P.; Kindahl, H.; Broeders, A.; Marsal, K.; Melin, P. Effects of a vasopressin antagonist in women with dysmenorrhea. Gynecol. Obstet. Investig. 2000, 50, 170–177. [Google Scholar] [CrossRef]
- Grulović, B.; Pucelj, M.R.; Krnić, M.; Kokić, V. Impact of prostaglandin F2-alpha and tumor necrosis factor-alpha (TNF-α) on pain in patients undergoing thermal balloon endometrial ablation. Coll. Antropol. 2013, 37, 1185–1190. [Google Scholar]
- Critchley, H.O.D.; Jones, R.L.; Lea, R.G.; Drudy, T.A.; Kelly, R.W.; Williams, A.R.W.; Baird, D.T. Role of inflammatory mediators in human endometrium during progesterone withdrawal and early pregnancy. J. Clin. Endocrinol. Metab. 1999, 84, 240–248. [Google Scholar] [CrossRef]
- Ma, H.; Hong, M.; Duan, J.; Liu, P.; Fan, X.; Shang, E.; Su, S.; Guo, J.; Qian, D.; Tang, Y. Altered Cytokine Gene Expression in Peripheral Blood Monocytes across the Menstrual Cycle in Primary Dysmenorrhea: A Case-Control Study. PLoS ONE 2013, 8, e55200. [Google Scholar] [CrossRef]
- Kannan, P.; Cheung, K.K.; Lau, B.W.M. Does aerobic exercise induced-analgesia occur through hormone and inflammatory cytokine-mediated mechanisms in primary dysmenorrhea? Med. Hypotheses 2019, 123, 50–54. [Google Scholar] [CrossRef] [PubMed]
- Ciebiera, M.; Włodarczyk, M.; Zgliczyńska, M.; Łukaszuk, K.; Męczekalski, B.; Kobierzycki, C.; Łoziński, T.; Jakiel, G. The role of tumor necrosis factor α in the biology of uterine fibroids and the related symptoms. Int. J. Mol. Sci. 2018, 19, e3869. [Google Scholar] [CrossRef] [PubMed]
- Dogru, H.Y.; Ozsoy, A.Z.; Karakus, N.; Delibas, I.B.; Isguder, C.K.; Yigit, S. Association of Genetic Polymorphisms in TNF and MIF Gene with the Risk of Primary Dysmenorrhea. Biochem. Genet. 2016, 54, 457–466. [Google Scholar] [CrossRef] [PubMed]
- Hunter, C.A.; Jones, S.A. IL-6 as a keystone cytokine in health and disease. Nat. Immunol. 2015, 16, 448–457. [Google Scholar] [CrossRef]
- Whitcomb, B.W.; Mumford, S.L.; Perkins, N.J.; Wactawski, J.; Bertone-Johnson, E.R.; Lynch, K.E.; Schisterman, E.F. Urinary cytokine and chemokine profiles across the menstrual cycle in healthy reproductive-aged women. Fertil. Steril. 2014, 101, 1383–1391. [Google Scholar] [CrossRef]
- Bertone-Johnson, E.R.; Ronnenberg, A.G.; Houghton, S.C.; Nobles, C.; Zagarins, S.E.; Takashima-Uebelhoer, B.B.; Faraj, J.L.; Whitcomb, B.W. Association of inflammation markers with menstrual symptom severity and premenstrual syndrome in young women. Hum. Reprod. 2014, 29, 1987–1994. [Google Scholar] [CrossRef]
- Angstwurm, M.W.A.; Gärtner, R.; Ziegler-Heitbrock, H.W.L. Cyclic plasma IL-6 levels during normal menstrual cycle. Cytokine 1997, 9, 370–374. [Google Scholar] [CrossRef]
- Yeh, M.L.; Chen, H.H.; So, E.C.; Liu, C.F. A study of serum malondialdehyde and interleukin-6 levels in young women with dysmenorrhea in Taiwan. Life Sci. 2004, 75, 669–673. [Google Scholar] [CrossRef]
- Konecna, L.; Yan, M.S.; Miller, L.E.; Schölmerich, J.; Falk, W.; Straub, R.H. Modulation of IL-6 production during the menstrual cycle in vivo and in vitro. Brain Behav. Immun. 2000, 14, 49–61. [Google Scholar] [CrossRef] [PubMed]
- Zhang, F.; Liu, X.; Wang, W.; Dong, H.; Xia, Y.; Ruan, L.; Liu, L. Expression of MMIF, HIF-1 α and VEGF in Serum and Endometrial Tissues of Patients with Endometriosis. Curr. Med. Sci. 2018, 38, 499–504. [Google Scholar] [CrossRef] [PubMed]
- Xu, H.; Zhang, T.; Chi, G.; Man, W.; May, K.E.; Becker, C.M.; Davis, T.N.; Kung, A.L.; Birsner, A.E.; Amato, R.J.; et al. Vascular endothelial growth factor C is increased in endometrium and promotes endothelial functions, vascular permeability and angiogenesis and growth of endometriosis. Angiogenesis 2013, 16, 541–551. [Google Scholar] [CrossRef]
- Ferrara, N.; Gerber, H.; LeCouter, J. The biology of VEGF and its receptors. Nat. Med. 2003, 9, 669–676. [Google Scholar] [CrossRef]
- Reynolds, L.P.; Grazul-Bilska, A.T.; Redmer, D.A. Angiogenesis in the female reproductive system. Int. J. Exp. Pathol. 2002, 83, 151–163. [Google Scholar] [CrossRef]
- Volanakis, J.E. Human C-reactive protein: Expression, structure, and function. Mol. Immunol. 2001, 38, 189–197. [Google Scholar] [CrossRef]
- Rosalki, S. C-reactive protein. Int. J. Clin. Pract. 2001, 55, 269–270. [Google Scholar]
- Lorenz, T.K.; Worthman, C.M.; Vitzthum, V.J. Links among inflammation, sexual activity and ovulation: Evolutionary trade-offs and clinical implications. Evol. Med. Public Health 2015, 2015, 304–324. [Google Scholar] [CrossRef]
- Sproston, N.R.; Ashworth, J.J. Role of C-reactive protein at sites of inflammation and infection. Front. Immunol. 2018, 9, 1–11. [Google Scholar] [CrossRef]
- Gaskins, A.J.; Wilchesky, M.; Mumford, S.L.; Whitcomb, B.W.; Browne, R.W.; Wactawski-Wende, J.; Perkins, N.J.; Schisterman, E.F. Endogenous reproductive hormones and C-reactive protein across the menstrual cycle: The BioCycle Study. Am. J. Epidemiol. 2012, 175, 423–431. [Google Scholar] [CrossRef]
- Wander, K.; Brindle, E.; O’Connor, K.A. C-reactive protein across the menstrual cycle. Am. J. Phys. Anthropol. 2008, 136, 138–146. [Google Scholar] [CrossRef] [PubMed]
- Puder, J.J.; Blum, C.A.; Mueller, B.; De Geyter, C.; Dye, L.; Keller, U. Menstrual cycle symptoms are associated with changes in low-grade inflammation. Eur. J. Clin. Investig. 2006, 36, 58–64. [Google Scholar] [CrossRef] [PubMed]
- Oladosu, F.A.; Tu, F.F.; Hellman, K.M. Nonsteroidal antiinflammatory drug resistance in dysmenorrhea: Epidemiology, causes, and treatment. Am. J. Obstet. Gynecol. 2018, 218, 390–400. [Google Scholar] [CrossRef]
- Marjoribanks, J.; Ayeleke, R.; Farquhar, C.; Proctor, M. Nonsteroidal anti-inflammatory drugs for dysmenorrhoea. Cochrane Database Syst. Rev. 2015, 7, 1–188. [Google Scholar] [CrossRef] [PubMed]
- Zahradnik, H.P.; Hanjalic-Beck, A.; Groth, K. Nonsteroidal anti-inflammatory drugs and hormonal contraceptives for pain relief from dysmenorrhea: A Review. Contraception 2010, 81, 185–196. [Google Scholar] [CrossRef] [PubMed]
- Yu, A. Complementary and alternative treatments for primary dysmenorrhea in adolescents. Nurse Pract. 2014, 39, 1–12. [Google Scholar] [CrossRef]
- Kotsopoulos, J.; Lubinski, J.; Moller, P.; Lynch, H.T.; Singer, C.F.; Eng, C.; Neuhausen, S.L.; Karlan, B.; Kim-Sing, C.; Huzarski, T. Timing of oral contraceptive use and the risk of breast cancer in BRCA1 mutation carriers. Breast Cancer Res. Treat. 2014, 143, 579–586. [Google Scholar] [CrossRef]
- Dragoman, M.V. The combined oral contraceptive pill- recent developments, risks and benefits. Best Pract. Res. Clin. Obstet. Gynaecol. 2014, 28, 825–834. [Google Scholar] [CrossRef]
- Suhonen, S.; Haukkamaa, M.; Jakobsson, T.; Rauramo, I. Clinical performance of a levonorgestrel-releasing intrauterine system and oral contraceptives in young nulliparous women: A comparative study. Contraception 2004, 69, 407–412. [Google Scholar] [CrossRef]
- Funk, S.; Miller, M.M.; Mishell, D.R.; Archer, D.F.; Poindexter, A.; Schmidt, J.; Zampaglione, E. Safety and efficacy of ImplanonTM, a single-rod implantable contraceptive containing etonogestrel. Contraception 2005, 71, 319–326. [Google Scholar] [CrossRef]
- Turkel, A.N.; Ziylan, Y.Z. Protection of blood-brain barrier breakdown by nifedipine in adrenaline-induced acute hypertension. Int. J. Neurosci. 2004, 114, 517–528. [Google Scholar] [CrossRef] [PubMed]
- Leavitt, K.; Običan, S.; Yankowitz, J. Treatment and Prevention of Hypertensive Disorders During Pregnancy. Clin. Perinatol. 2019, 46, 173–185. [Google Scholar] [CrossRef]
- Ulmsten, U. Calcium blockade as a rapid pharmacological test to evaluate primary dysmenorrhea. Gynecol. Obstet. Investig. 1985, 20, 78–83. [Google Scholar] [CrossRef]
- Ra, E.; Rm, G. Nifedipine for primary dysmenorrhoea. Cochrane Database Syst. Rev. 2017, 12, 1–13. [Google Scholar] [CrossRef]
- Åkerlund, M. Involvement of oxytocin and vasopressin in the pathophysiology of preterm labor and primary dysmenorrhea. Prog. Brain Res. 2002, 139, 359–365. [Google Scholar] [CrossRef]
- Mrugacz, G.; Grygoruk, C.; Sieczynski, P.; Grusza, M.; Pietrewicz, P.; Pietrzycki, B. Influence of naloxone on uterine contractions in patients with primary dysmenorrhea. Pol. Merkur. Lek. 2013, 35, 151–153. [Google Scholar]
- Liedman, R.; Grant, L.E.E.; Igidbashian, S.; James, I.A.N.; Mcleod, A.; Skillern, L.; Mats, A. Intrauterine pressure, ischemia markers, and experienced pain during administration of a vasopressin V 1a receptor antagonist in spontaneous and vasopressin-induced dysmenorrhea. Acta Obstet. Gynecol. Scand. 2006, 85, 207–211. [Google Scholar] [CrossRef] [PubMed]
- Brouard, R.; Bossmar, T.; Fournié-Lloret, D.; Chassard, D.; Åkerlund, M. Effect of SR49059, an orally active VIavasopressin receptor antagonist, in the prevention of dysmenorrhoea. BJOG Int. J. Obstet. Gynaecol. 2000, 107, 614–619. [Google Scholar] [CrossRef]
- Smith, C.A.; Armour, M.; Zhu, X.; Li, X.; Lu, Z.Y.; Song, J. Acupuncture for dysmenorrhoea. Cochrane Database Syst. Rev. 2016, 4, CD007854. [Google Scholar] [CrossRef]
- Yang, N.Y.; Kim, S.D. Effects of a Yoga Program on Menstrual Cramps and Menstrual Distress in Undergraduate Students with Primary Dysmenorrhea: A Single-Blind, Randomized Controlled Trial. J. Altern. Complement. Med. 2016, 22, 732–738. [Google Scholar] [CrossRef]
- Azima, S.; Bakhshayesh, H.R.; Kaviani, M.; Abbasnia, K.; Sayadi, M. Comparison of the Effect of Massage Therapy and Isometric Exercises on Primary Dysmenorrhea: A Randomized Controlled Clinical Trial. J. Pediatric Adolesc. Gynecol. 2015, 28, 486–491. [Google Scholar] [CrossRef] [PubMed]
- Ortiz, M.I.; Cortés-Márquez, S.K.; Romero-Quezada, L.C.; Murguía-Cánovas, G.; Jaramillo-Díaz, A.P. Effect of a physiotherapy program in women with primary dysmenorrhea. Eur. J. Obstet. Gynecol. Reprod. Biol. 2015, 194, 24–29. [Google Scholar] [CrossRef]
- Lauretti, G.R.; Oliveira, R.; Parada, F.; Mattos, A.L. The New Portable Transcutaneous Electrical Nerve Stimulation Device Was Efficacious in the Control of Primary Dysmenorrhea Cramp Pain. Neuromodulation 2015, 18, 522–527. [Google Scholar] [CrossRef] [PubMed]
- Barcikowska, Z.; Rajkowska-Labon, E.; Grzybowska, M.E.; Dijakiewicz, G.; Hansdorfer-Korzon, R.; Zorena, K. The influence of manual therapy on the level of dysmenorrhea and concentration of sex hormones in young women—A pilot study. In Proceedings of the XVII Congress of Polish Society Physiotherapy, Pabianice, Poland, 6–7 December 2019; pp. 89–90. [Google Scholar]
- Özgül, S.; Üzelpasaci, E.; Orhan, C.; Baran, E.; Beksaç, M.S. Short-term effects of connective tissue manipulation in women with primary dysmenorrhea: A randomized controlled trial. Complement. Ther. Clin. Pract. 2018, 33, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Barassi, G.; Bellomo, R.G.; Porreca, A.; Di Felice, P.A.; Prosperi, L.; Saggini, R. Somato-Visceral Effects in the Treatment of Dysmenorrhea: Neuromuscular Manual Therapy and Standard Pharmacological Treatment. J. Altern. Complement. Med. 2017, 24, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Molins-Cubero, S.; Ricard, F. Changes in Pain Perception after Pelvis Manipulation in Women with Primary Dysmenorrhea: A Randomized Controlled Trial. Pain Med. 2014, 15, 1455–1463. [Google Scholar] [CrossRef] [PubMed]
- Kokjohn, K.; Schmid, D.M.; Triano, J.J.; Brennan, P. The effect of spinal manipulation on pain and prostaglandin levels in women with primary dysmenorrhea. J. Manip. Physiol. Ther. 1992, 15, 279–285. [Google Scholar]
- Wang, S.F.; Lee, J.P.; Hwa, H.L. Effect of transcutaneous electrical nerve stimulation on primary dysmenorrhea. Neuromodulation Technol. Neural Interface 2009, 12, 302–309. [Google Scholar] [CrossRef]
- Thabet, A.A.E.; Battecha, K.H.; Elsodany, A.M.; Alshehri, M.A.; Refaat, B. High-intensity laser therapy versus pulsed electromagnetic field in the treatment of primary dysmenorrhea. J. Phys. Ther. Sci. 2017, 29, 1742–1748. [Google Scholar] [CrossRef]
- Perez Machado, A.F.; Perracini, M.R.; Cruz Saraiva de Morais, A.; da Silva, B.O.; Driusso, P.; Liebano, R.E. Microwave diathermy and transcutaneous electrical nerve stimulation effects in primary dysmenorrhea: Clinical trial protocol. Pain Manag. 2017, 7, 359–366. [Google Scholar] [CrossRef]
- Schiøtz, H.A.; Jettestad, M.; Al-Heeti, D. Treatment of dysmenorrhoea with a new TENS device (OVA). J. Obstet. Gynaecol. 2007, 27, 726–728. [Google Scholar] [CrossRef] [PubMed]
- Motahari-Tabari, N.; Shirvani, M.A.; Alipour, A. Comparison of the effect of stretching exercises and mefenamic acid on the reduction of pain and menstruation characteristics in primary dysmenorrhea: A randomized clinical trial. Oman Med. J. 2017, 32, 47–53. [Google Scholar] [CrossRef] [PubMed]
- Rakhshaee, Z. Effect of Three Yoga Poses (Cobra, Cat and Fish Poses) in Women with Primary Dysmenorrhea: A Randomized Clinical Trial. J. Pediatric Adolesc. Gynecol. 2011, 24, 192–196. [Google Scholar] [CrossRef]
- Yonglitthipagon, P.; Muansiangsai, S.; Wongkhumnger, W.; Donpunha, W.; Chanavirut, R.; Siritaratiwat, W.; Mato, L.; Eungpinichpong, W.; Janyacharoen, T. Effect of yoga on the menstrual pain, physical fitness, and quality of life of young women with primary dysmenorrhea. J. Bodyw. Mov. Ther. 2017, 21, 840–846. [Google Scholar] [CrossRef] [PubMed]
- Chien, L.W.; Chang, H.C.; Liu, C.F. Effect of Yoga on Serum Homocysteine and Nitric Oxide Levels in Adolescent Women With and Without Dysmenorrhea. J. Altern. Complement. Med. 2013, 19, 20–23. [Google Scholar] [CrossRef]
- Sriprasert, I.; Suerungruang, S.; Athilarp, P.; Matanasarawoot, A.; Teekachunhatean, S. Efficacy of Acupuncture versus Combined Oral Contraceptive Pill in Treatment of Moderate-to-Severe Dysmenorrhea: A Randomized Controlled Trial. Evid. Based Complement. Altern. Med. 2015, 2015, 1–10. [Google Scholar] [CrossRef]
- Schwerla, F.; Wirthwein, P.; Rütz, M.; Resch, K.L. Osteopathic treatment in patients with primary dysmenorrhoea: A randomized controlled trial. Int. J. Osteopath. Med. 2014, 17, 222–231. [Google Scholar] [CrossRef]
- Uysal, M.; Doğru, H.Y.; Sapmaz, E.; Tas, U.; Çakmak, B.; Ozsoy, A.Z.; Sahin, F.; Ayan, S.; Esen, M. Investigating the effect of rose essential oil in patients with primary dysmenorrhea. Complement. Ther. Clin. Pract. 2016, 24, 45–49. [Google Scholar] [CrossRef]
- Lim, C.; Park, Y.; Bae, Y. The effect of the kinesio taping and spiral taping on menstrual pain and premenstrual syndrome. J. Phys. Ther. Sci. 2013, 25, 761–764. [Google Scholar] [CrossRef]
- Potur, D.C.; Kömürcü, N. The effects of local low-dose heat application on dysmenorrhea. J. Pediatric Adolesc. Gynecol. 2014, 27, 216–221. [Google Scholar] [CrossRef]
| Factors | Authors | Changes in the Concentration of Inflammatory Factors |
|---|---|---|
| PGF2α | Lundstrom and Green [14] | higher concentration during menstruation among women with dysmenorrhea |
| Stromberg et al. [26] | higher in women with dysmenorrhea than in women without pain during menstruation | |
| Liedman et al. [27] | no difference between dysmenorrheic women and women without pain | |
| Vasopressin | Stromberg et al. [26] | higher in women with dysmenorrhea than in women without pain during menstruation |
| Liedman et al. [29] | lower during ovulation in women with dysmenorrhea than in healthy women, during menstruation without changes | |
| Valentin et al. [30] | absence of difference in concentration between group with dysmenorrhea and healthy women | |
| TNFα | Ma et. al. [33] | increase in genes encoding pro-inflammatory cytokines TNFα |
| IL6 | Angstwurm et al. [40] | increase in the follicular phase, decrease in the luteal phase |
| Yeh et. al. [41] | higher in the dysmenorrhea women than in the healthy women | |
| VEGF | Zhang F et al. [43] | the expression of VEGF in the serum and endometrial tissues may be used to assess the stage of endometriosis and the severity of dysmenorrhea. |
| Xu H et al. [44] | supplementation and over-expression of VEGF-C significantly reversed the inhibitory effects on the endothelial functions, vascular permeability and endometriotic growth | |
| CRP | Gaskins et. al. [51] | highest during menses, decrease during the follicular phase, lowest on the expected day of ovulation, and increase in the luteal phase |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Barcikowska, Z.; Rajkowska-Labon, E.; Grzybowska, M.E.; Hansdorfer-Korzon, R.; Zorena, K. Inflammatory Markers in Dysmenorrhea and Therapeutic Options. Int. J. Environ. Res. Public Health 2020, 17, 1191. https://doi.org/10.3390/ijerph17041191
Barcikowska Z, Rajkowska-Labon E, Grzybowska ME, Hansdorfer-Korzon R, Zorena K. Inflammatory Markers in Dysmenorrhea and Therapeutic Options. International Journal of Environmental Research and Public Health. 2020; 17(4):1191. https://doi.org/10.3390/ijerph17041191
Chicago/Turabian StyleBarcikowska, Zofia, Elżbieta Rajkowska-Labon, Magdalena Emilia Grzybowska, Rita Hansdorfer-Korzon, and Katarzyna Zorena. 2020. "Inflammatory Markers in Dysmenorrhea and Therapeutic Options" International Journal of Environmental Research and Public Health 17, no. 4: 1191. https://doi.org/10.3390/ijerph17041191
APA StyleBarcikowska, Z., Rajkowska-Labon, E., Grzybowska, M. E., Hansdorfer-Korzon, R., & Zorena, K. (2020). Inflammatory Markers in Dysmenorrhea and Therapeutic Options. International Journal of Environmental Research and Public Health, 17(4), 1191. https://doi.org/10.3390/ijerph17041191






