Prediction Equations of the Multifrequency Standing and Supine Bioimpedance for Appendicular Skeletal Muscle Mass in Korean Older People
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
2.2. Appendicular Skeletal Muscle Mass from Dual-Energy X-Ray Absorptiometry
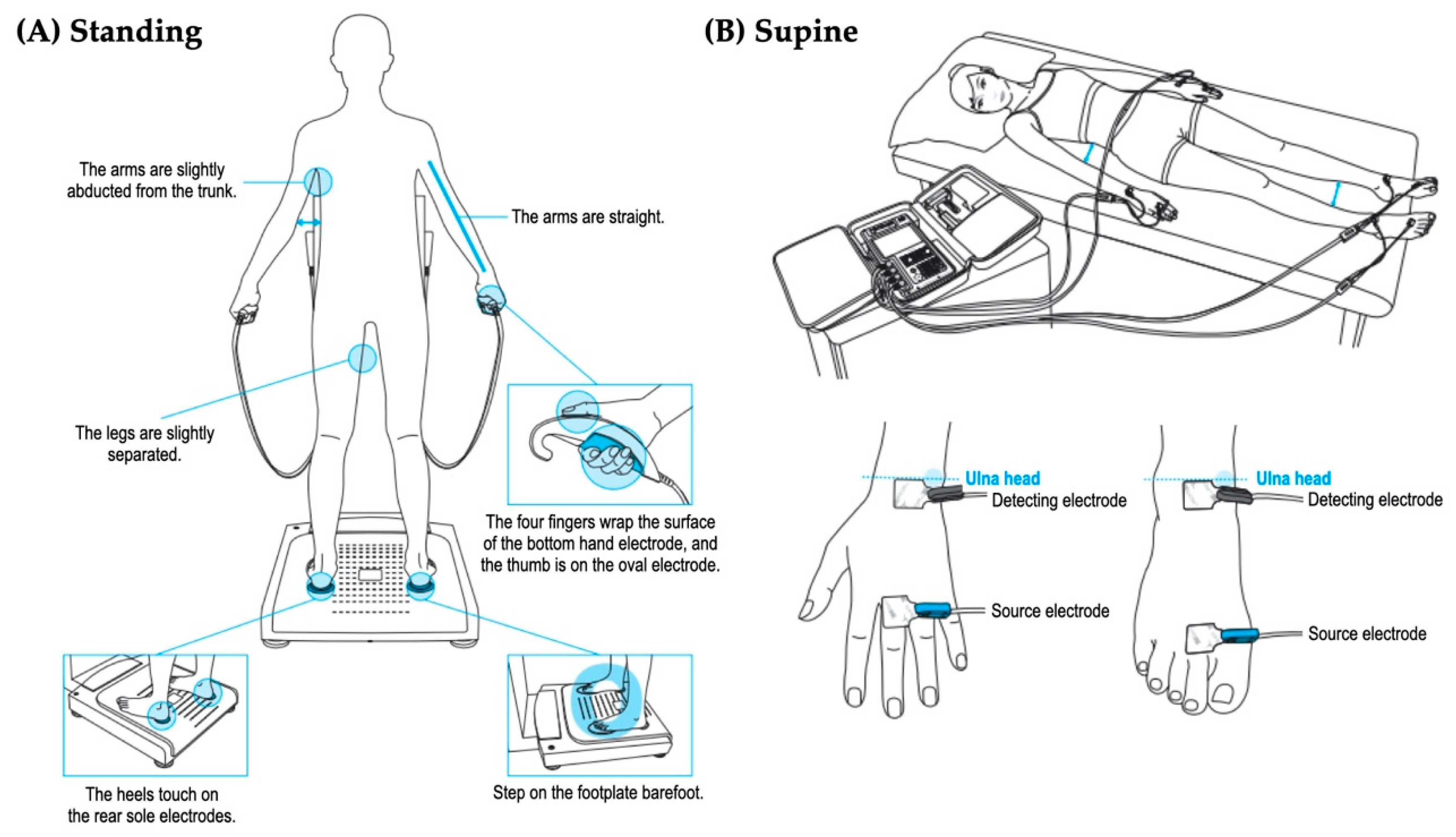
2.3. Multifrequency 8-Electrodes Bioimpedance Analysis
2.4. Published Prediction Equations
2.5. Statistical Analysis
3. Results
3.1. Characteristics of the Study Population
3.2. Development and Cross-Validation of BIA Prediction Equations for ASM
3.3. The Final Standing and Supine BIA Prediction Equations for ASM
3.4. External Cross-Validation of Published and Built-in Equations for ASM
3.5. The Agreement of Sarcopenia between DXA-Measured and BIA-Predicted ASMI
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Meynial-Denis, D. Sarcopenia: Molecular, Cellular, and Nutritional Aspects—Applications to Humans; CRC Press: Boca Raton, FL, USA, 2020. [Google Scholar]
- Anker, S.D.; Morley, J.E.; von Haehling, S. Welcome to the ICD-10 code for sarcopenia. J. Cachexia Sarcopenia Muscle 2016, 7, 512–514. [Google Scholar] [CrossRef] [PubMed]
- Rosenberg, I.H. Sarcopenia: Origins and clinical relevance. Clin. Geriatr. Med. 2011, 27, 337–339. [Google Scholar] [CrossRef] [PubMed]
- Baumgartner, R.N.; Koehler, K.M.; Gallagher, D.; Romero, L.; Heymsfield, S.B.; Ross, R.R.; Garry, P.J.; Lindeman, R.D. Epidemiology of sarcopenia among the elderly in New Mexico. Am. J. Epidemiol. 1998, 147, 755–763. [Google Scholar] [CrossRef] [PubMed]
- Cruz-Jentoft, A.J.; Bahat, G.; Bauer, J.; Boirie, Y.; Bruyere, O.; Cederholm, T.; Cooper, C.; Landi, F.; Rolland, Y.; Sayer, A.A.; et al. Sarcopenia: Revised European consensus on definition and diagnosis. Age Ageing 2019, 48, 601. [Google Scholar] [CrossRef] [PubMed]
- Cruz-Jentoft, A.J.; Baeyens, J.P.; Bauer, J.M.; Boirie, Y.; Cederholm, T.; Landi, F.; Martin, F.C.; Michel, J.P.; Rolland, Y.; Schneider, S.M.; et al. Sarcopenia: European consensus on definition and diagnosis: Report of the European working group on sarcopenia in older people. Age Ageing 2010, 39, 412–423. [Google Scholar] [CrossRef] [PubMed]
- Chen, L.K.; Woo, J.; Assantachai, P.; Auyeung, T.W.; Chou, M.Y.; Iijima, K.; Jang, H.C.; Kang, L.; Kim, M.; Kim, S.; et al. Asian working group for sarcopenia: 2019 consensus update on sarcopenia diagnosis and treatment. J. Am. Med. Dir. Assoc. 2020, 21, 300–307 e2. [Google Scholar] [CrossRef]
- Chen, L.K.; Liu, L.K.; Woo, J.; Assantachai, P.; Auyeung, T.W.; Bahyah, K.S.; Chou, M.Y.; Chen, L.Y.; Hsu, P.S.; Krairit, O.; et al. Sarcopenia in Asia: Consensus report of the Asian working group for sarcopenia. J. Am. Med. Dir. Assoc. 2014, 15, 95–101. [Google Scholar] [CrossRef]
- Chen, L.K.; Lee, W.J.; Peng, L.N.; Liu, L.K.; Arai, H.; Akishita, M.; Asian working group for sarcopenia. Recent advances in sarcopenia research in asia: 2016 update from the Asian working group for sarcopenia. J. Am. Med. Dir. Assoc. 2016, 17, 767.e1–767.e7. [Google Scholar] [CrossRef]
- Tosato, M.; Marzetti, E.; Cesari, M.; Savera, G.; Miller, R.R.; Bernabei, R.; Landi, F.; Calvani, R. Measurement of muscle mass in sarcopenia: From imaging to biochemical markers. Aging Clin. Exp. Res. 2017, 29, 19–27. [Google Scholar] [CrossRef]
- Buckinx, F.; Landi, F.; Cesari, M.; Fielding, R.A.; Visser, M.; Engelke, K.; Maggi, S.; Dennison, E.; Al-Daghri, N.M.; Allepaerts, S.; et al. Pitfalls in the measurement of muscle mass: A need for a reference standard. J. Cachexia Sarcopenia Muscle 2018, 9, 269–278. [Google Scholar] [CrossRef]
- Gonzalez, M.C.; Barbosa-Silva, T.G.; Heymsfield, S.B. Bioelectrical impedance analysis in the assessment of sarcopenia. Curr. Opin. Clin. Nutr. Metab. Care 2018, 21, 366–374. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez, M.C.; Heymsfield, S.B. Bioelectrical impedance analysis for diagnosing sarcopenia and cachexia: What are we really estimating? J. Cachexia Sarcopenia Muscle 2017, 8, 187–189. [Google Scholar] [CrossRef] [PubMed]
- Vermeiren, S.; Beckwee, D.; Vella-Azzopardi, R.; Beyer, I.; Knoop, V.; Jansen, B.; Delaere, A.; Antoine, A.; Bautmans, I.; Scafoglieri, A.; et al. Evaluation of appendicular lean mass using bio impedance in persons aged 80+: A new equation based on the BUTTERFLY-study. Clin. Nutr. 2019, 38, 1756–1764. [Google Scholar] [CrossRef]
- Scafoglieri, A.; Clarys, J.P.; Bauer, J.M.; Verlaan, S.; Van Malderen, L.; Vantieghem, S.; Cederholm, T.; Sieber, C.C.; Mets, T.; Bautmans, I.; et al. Predicting appendicular lean and fat mass with bioelectrical impedance analysis in older adults with physical function decline—The PROVIDE study. Clin. Nutr. 2017, 36, 869–875. [Google Scholar] [CrossRef]
- Sergi, G.; De Rui, M.; Veronese, N.; Bolzetta, F.; Berton, L.; Carraro, S.; Bano, G.; Coin, A.; Manzato, E.; Perissinotto, E. Assessing appendicular skeletal muscle mass with bioelectrical impedance analysis in free-living Caucasian older adults. Clin. Nutr. 2015, 34, 667–673. [Google Scholar] [CrossRef]
- Kyle, U.G.; Genton, L.; Hans, D.; Pichard, C. Validation of a bioelectrical impedance analysis equation to predict appendicular skeletal muscle mass (ASMM). Clin. Nutr. 2003, 22, 537–543. [Google Scholar] [CrossRef]
- Kim, J.H.; Choi, S.H.; Lim, S.; Kim, K.W.; Lim, J.Y.; Cho, N.H.; Park, K.S.; Jang, H.C. Assessment of appendicular skeletal muscle mass by bioimpedance in older community-dwelling Korean adults. Arch. Gerontol. Geriatr. 2014, 58, 303–307. [Google Scholar] [CrossRef]
- Rangel Peniche, D.B.; Raya Giorguli, G.; Alemán-Mateo, H. Accuracy of a predictive bioelectrical impedance analysis equation for estimating appendicular skeletal muscle mass in a non-Caucasian sample of older people. Arch. Gerontol. Geriatr. 2015, 61, 39–43. [Google Scholar] [CrossRef]
- Yamada, Y.; Nishizawa, M.; Uchiyama, T.; Kasahara, Y.; Shindo, M.; Miyachi, M.; Tanaka, S. Developing and validating an age-independent equation using multi-frequency bioelectrical impedance analysis for estimation of appendicular skeletal muscle mass and establishing a cutoff for sarcopenia. Int. J. Environ. Res. Public Health 2017, 14, 809. [Google Scholar] [CrossRef]
- Bosy-Westphal, A.; Jensen, B.; Braun, W.; Pourhassan, M.; Gallagher, D.; Müller, M.J. Quantification of whole-body and segmental skeletal muscle mass using phase-sensitive 8-electrode medical bioelectrical impedance devices. Eur. J. Clin. Nutr. 2017, 71, 1061–1067. [Google Scholar] [CrossRef]
- Heymsfield, S.B.; Smith, R.; Aulet, M.; Bensen, B.; Lichtman, S.; Wang, J.; Pierson, R.N., Jr. Appendicular skeletal muscle mass: Measurement by dual-photon absorptiometry. Am. J. Clin. Nutr. 1990, 52, 214–218. [Google Scholar] [CrossRef] [PubMed]
- Lohman, T.G. Advances in Body Composition Assessment; Human Kinetics: Champaign, IL, USA, 1992. [Google Scholar]
- Heyward, V.H.; Wagner, D.R. Applied Body Composition Assessment, 2nd ed.; Human Kinetics: Champaign, IL, USA, 2004. [Google Scholar]
- Watson, P.F.; Petrie, A. Method agreement analysis: A review of correct methodology. Theriogenology 2010, 73, 1167–1179. [Google Scholar] [CrossRef] [PubMed]
- Reiter, R.; Iglseder, B.; Treschnitzer, W.; Alzner, R.; Mayr-Pirker, B.; Kreutzer, M.; Pirich, C.; Kässmann, H.; Dovjak, P.; Reiss, J. Quantifying appendicular muscle mass in geriatric inpatients: Performance of different single frequency BIA equations in comparison to dual X-ray absorptiometry. Arch. Gerontol. Geriatr. 2019, 80, 98–103. [Google Scholar] [CrossRef]
- De Rui, M.; Veronese, N.; Bolzetta, F.; Berton, L.; Carraro, S.; Bano, G.; Trevisan, C.; Pizzato, S.; Coin, A.; Perissinotto, E.; et al. Validation of bioelectrical impedance analysis for estimating limb lean mass in free-living Caucasian elderly people. Clin. Nutr. 2017, 36, 577–584. [Google Scholar] [CrossRef] [PubMed]
- Segal, K.R.; Burastero, S.; Chun, A.; Coronel, P.; Pierson, R.N., Jr.; Wang, J. Estimation of extracellular and total body water by multiple-frequency bioelectrical-impedance measurement. Am. J. Clin. Nutr. 1991, 54, 26–29. [Google Scholar] [CrossRef]
- Lukaski, H.C. Biological indexes considered in the derivation of the bioelectrical impedance analysis. Am. J. Clin. Nutr. 1996, 64, 397S–404S. [Google Scholar] [CrossRef]
- Erlandson, M.C.; Lorbergs, A.L.; Mathur, S.; Cheung, A.M. Muscle analysis using pQCT, DXA and MRI. Eur. J. Radiol. 2016, 85, 1505–1511. [Google Scholar] [CrossRef]
- Clark, R.V.; Walker, A.C.; Miller, R.R.; O’Connor-Semmes, R.L.; Ravussin, E.; Cefalu, W.T. Creatine (methyl-d3) dilution in urine for estimation of total body skeletal muscle mass: Accuracy and variability vs. MRI and DXA. J. Appl. Physiol. 2018, 124, 1–9. [Google Scholar] [CrossRef]
- Freda, P.U.; Shen, W.; Reyes-Vidal, C.M.; Geer, E.B.; Arias-Mendoza, F.; Gallagher, D.; Heymsfield, S.B. Skeletal muscle mass in acromegaly assessed by magnetic resonance imaging and dual-photon x-ray absorptiometry. J. Clin. Endocrinol. Metab. 2009, 94, 2880–2886. [Google Scholar] [CrossRef]
- Fuller, N.J.; Hardingham, C.R.; Graves, M.; Screaton, N.; Dixon, A.K.; Ward, L.C.; Elia, M. Assessment of limb muscle and adipose tissue by dual-energy X-ray absorptiometry using magnetic resonance imaging for comparison. Int. J. Obesity 1999, 23, 1295–1302. [Google Scholar] [CrossRef][Green Version]
- Koster, A.; Ding, J.; Stenholm, S.; Caserotti, P.; Houston, D.K.; Nicklas, B.J.; You, T.; Lee, J.S.; Visser, M.; Newman, A.B.; et al. Does the amount of fat mass predict age-related loss of lean mass, muscle strength, and muscle quality in older adults? J. Gerontol. A Biol. Sci. Med. Sci. 2011, 66, 888–895. [Google Scholar] [CrossRef] [PubMed]
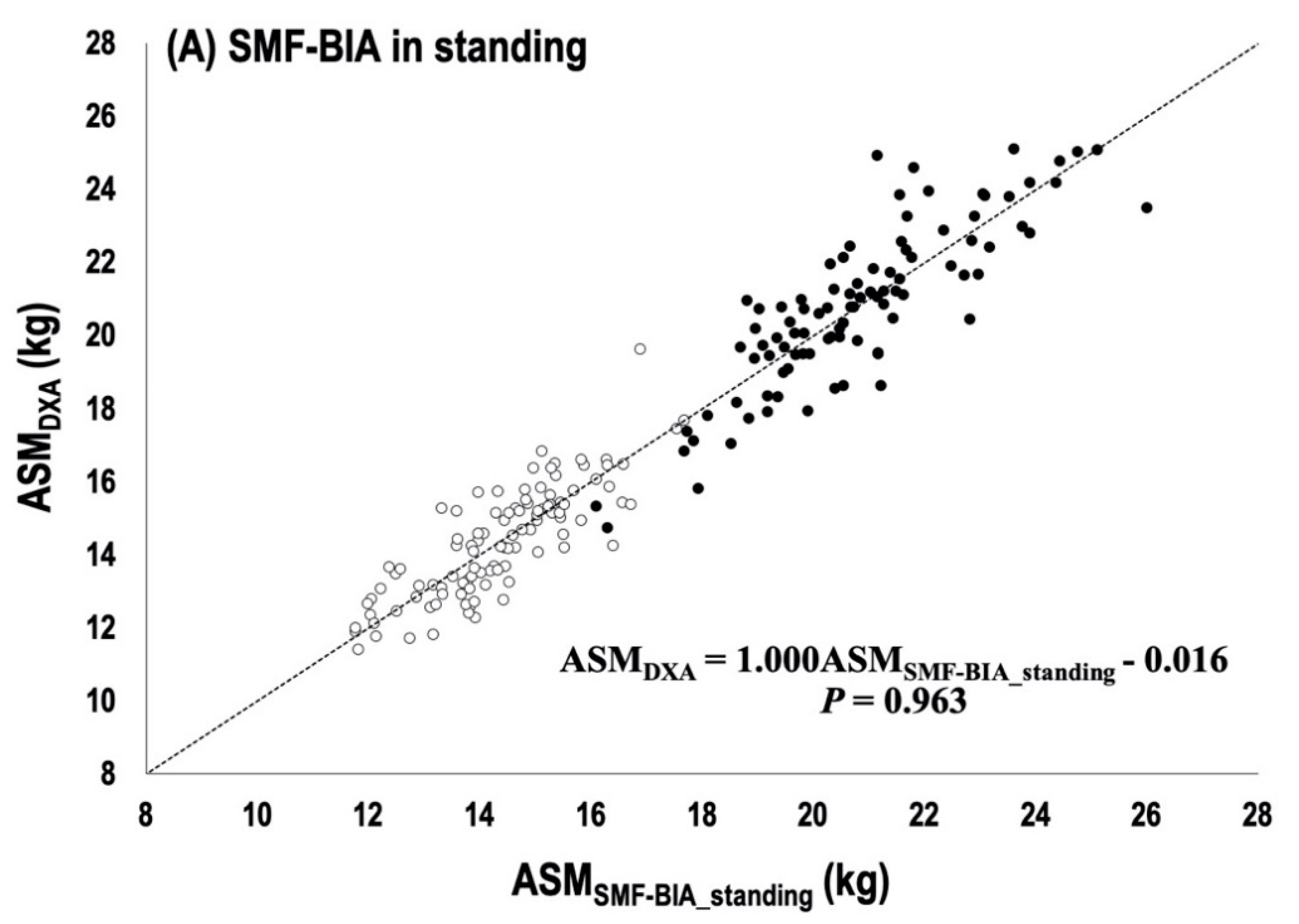
 = women within 1.16 kg ASM,
= women within 1.16 kg ASM,  = men within 1.45 kg ASM,
= men within 1.45 kg ASM,  = individuals who are out of the minimum acceptable standard for prediction errors (i.e., good rating) [11,24,25].
= individuals who are out of the minimum acceptable standard for prediction errors (i.e., good rating) [11,24,25].
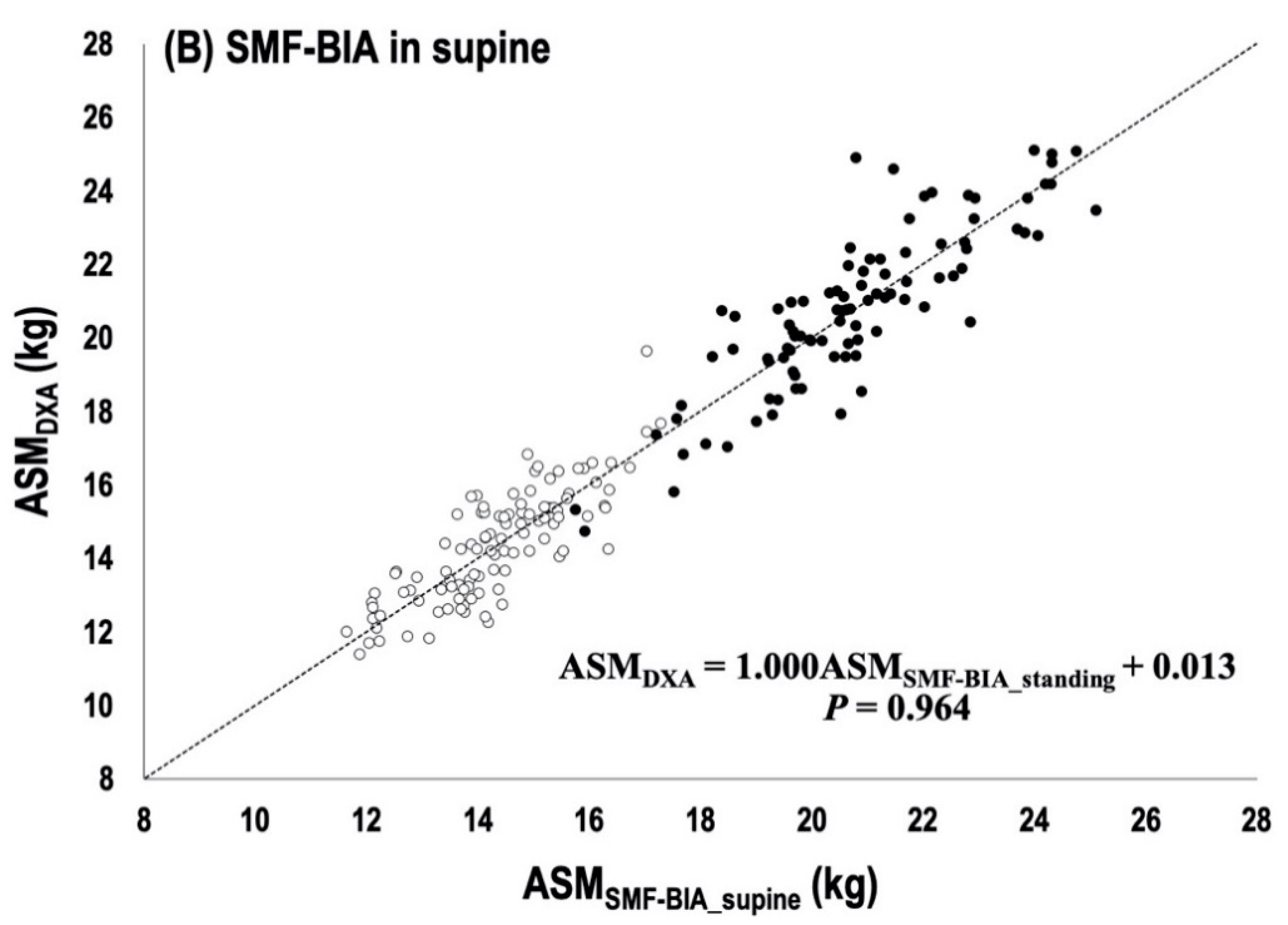
 = women within 1.16 kg ASM,
= women within 1.16 kg ASM, 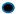 = men within 1.45 kg ASM,
= men within 1.45 kg ASM,  = individuals who are out of the minimum acceptable standard for prediction errors (i.e., good rating) [11,24,25].
= individuals who are out of the minimum acceptable standard for prediction errors (i.e., good rating) [11,24,25].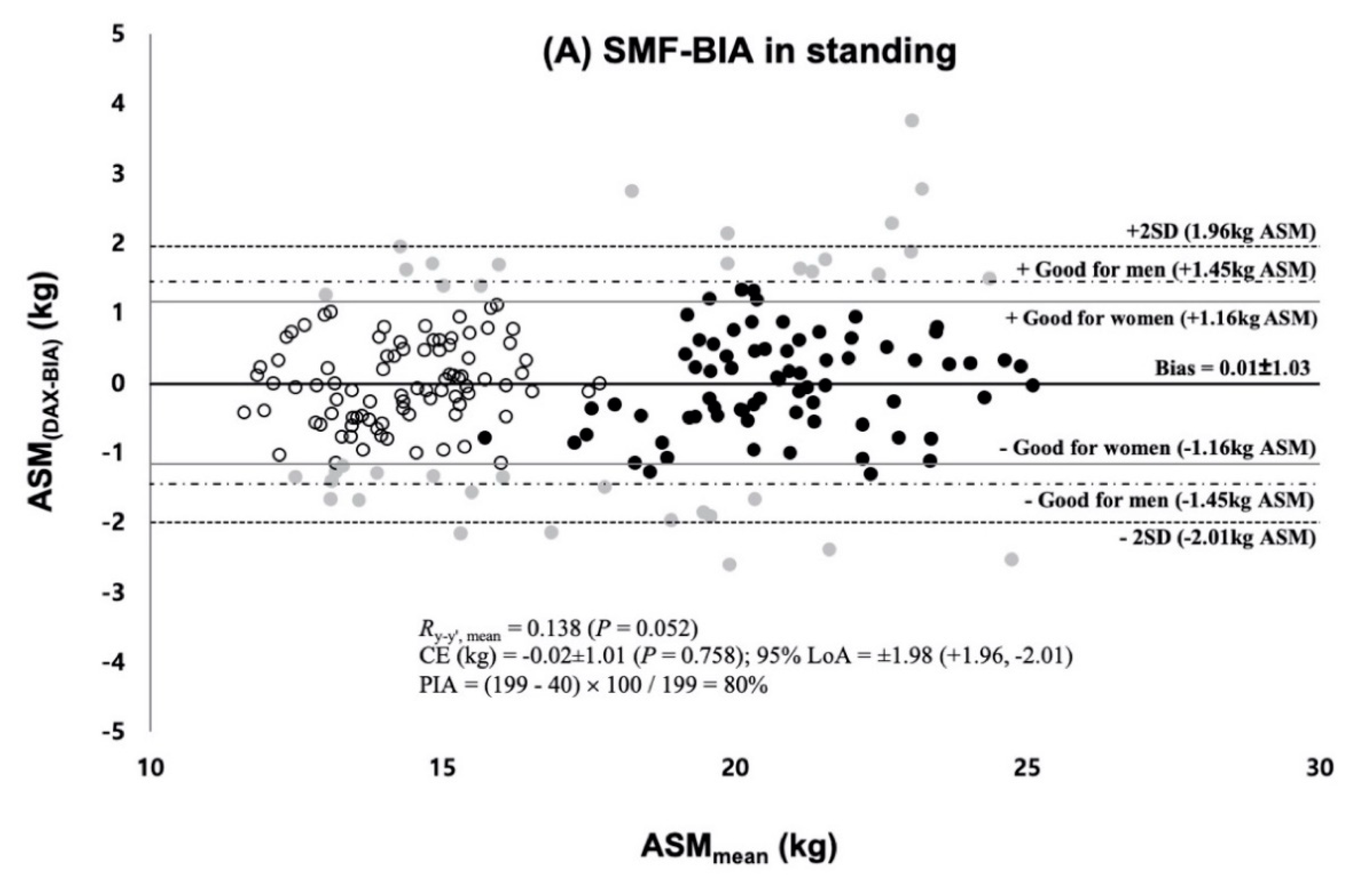
| Variables | Development Group | Cross-Validation Group | ||
|---|---|---|---|---|
| Men (n = 63) | Women (n = 70) | Men (n = 31) | Women (n = 35) | |
| Age (years) | 76.4 ± 4.2 | 76.1 ± 4.1 | 75.9 ± 4.1 | 75.6 ± 4.3 |
| Height (cm) | 166.5 ± 5.1 | 152.7 ± 5.0 * | 167.6 ± 4.3 | 153.3 ± 4.2 * |
| Weight (kg) | 65.6 ± 7.7 | 55.4 ± 5.8 * | 66.0 ± 6.8 | 54.8 ± 7.3 * |
| BMI (kg·m−2) | 23.7 ± 2.3 | 23.8 ± 2.2 | 23.5 ± 2.3 | 23.3 ± 2.7 |
| FFM (kg) | 50.2 ± 4.6 | 36.9 ± 3.1 * | 51.1 ± 4.0 | 37.0 ± 3.9 * |
| FM (kg) | 15.7 ± 5.3 | 17.3 ± 4.6 * | 15.1 ± 5.1 | 18.6 ± 4.1 * |
| PBF (%) | 23.2 ± 6.9 | 32.5 ± 4.9 * | 22.4 ± 5.0 | 31.5 ± 5.5 * |
| ASM (kg) | 20.6 ± 2.4 | 14.4 ± 1.4 * | 21.1 ± 2.0 | 14.3 ± 1.8 * |
| Standing mode of BIA | ||||
| R@50kHz | 528 ± 55 | 616 ± 50 * | 532 ± 42 | 663 ± 61 * |
| R@250kHz | 480 ± 50 | 564 ± 46 * | 484 ± 39 | 571 ± 57 * |
| Xc@5kHz | 24.5 ± 4.6 | 24.8 ± 4.0 | 24.7 ± 3.6 | 24.9 ± 4.1 |
| Xc@50kHz | 47.2 ± 7.4 | 48.1 ± 6.1 | 47.5 ± 4.7 | 49.2 ± 6.5 |
| RI@50kHz | 53.1 ± 6.7 | 38.1 ± 3.9 * | 53.1 ± 4.8 | 38.1 ± 4.5 * |
| RI@250tand | 58.4 ± 7.3 | 41.6 ± 4.3 * | 58.4 ± 5.3 | 41.6 ± 5.0 * |
| Supine mode of BIA | ||||
| R@50kHz | 488 ± 49 | 575 ± 46 * | 487 ± 41 | 582 ± 57 * |
| R@250kHz | 438 ± 44 | 521 ± 41 * | 437 ± 38 | 527 ± 54 * |
| Xc@5kHz | 24.3 ± 4.7 | 25.1 ± 4.3 | 25.0 ± 2.9 | 25.0 ± 3.6 |
| Xc@50kHz | 47.9 ± 7.2 | 49.3 ± 6.9 | 47.9 ± 4.5 | 50.0 ± 5.7 |
| RI@50kHz | 57.3 ± 40.8 | 40.8 ± 4.0 * | 58.1 ± 5.3 | 40.8 ± 4.8 * |
| RI@250tand | 64.0 ± 7.9 | 45.0 ± 4.4 * | 64.8 ± 6.0 | 45.1 ± 5.5 * |
| Standing Mode of SMF-BIA | ||
| Development group (n = 133) | Cross-validation group (n = 66) | |
| Measured ASM | 17.3 ± 3.66 kg | 17.5 ± 3.92 kg |
| ASM prediction equation | 0.273RI@250 kHz + 1.369sex + 0.049Xc@50 kHz + 0.032 BW − 1.118 | |
| ‡R2 = 0.923, SEE = 1.10 kg, CV = 6.4%, | ||
| SR(M) = Very good, SR(W) = Good | ||
| VIF: RI = 6.88, Xc = 1.45, BW = 2.74, | ||
| sex = 3.87 | ||
| Predicted ASM | 17.5 ± 3.73 kg | 17.6 ± 3.73 kg, * p = 0.693 |
| R2 = 0.934, TE = 1.00 kg, CV = 5.7% | ||
| SR = Excellent (M), SR = Very good (W) | ||
| Supine Mode of SMF-BIA | ||
| Development group (n = 133) | Validation group (n = 66) | |
| Measured ASM | 17.3 ± 3.66 kg | 17.5 ± 3.92 kg |
| ASM prediction equation | 0.266RI@250 kHz + 1.227sex + 0.057Xc@5kHz + 0.960 | |
| ‡R2 = 0.919, SEE = 1.06 kg, CV = 6.1%, | ||
| SR(M) = Very good, SR(W) = Good | ||
| VIF: RI = 4.34, Xc = 1.40, sex = 3.73 | ||
| Predicted ASM | 17.3 ± 3.51 kg | 17.4 ± 3.58 kg, * p = 0.291 R2 = 0.948, TE = 0.93 kg, CV = 5.3% |
| SR = Excellent (M), SR = Very good (W) | ||
| Final Prediction Equations | |
|---|---|
| Standing Mode of SMF-BIA (n = 199) | |
| Measured ASM | 17.4 ± 3.74 kg |
| ASM prediction equation | 0.286RI@250 kHz + 1.367sex + 0.054Xc@50 kHz + 0.031 BW − 1.864 |
| ‡R2 = 0.925, SEE = 1.02 kg, CV = 5.9%, SR = Excellent (M), SR = Good (W) | |
| VIF: RI@250kHz = 7.48, sex = 4.04, Xc@50kHz = 1.41, BW = 2.91 | |
| Predicted ASM | 17.4 ± 3.60 kg, * p = 0.758 |
| Supine Mode of SMF-BIA (n = 199) | |
| Measured ASM | 17.4 ± 3.74 kg |
| ASM prediction equation | 0.276RI@250kHz + 1.151sex + 0.059Xc@5 kHz + 0.429 |
| ‡R2 = 0.927, SEE = 1.01 kg, CV = 5.8%, SR = Excellent (M), SR = Very good (W) | |
| VIF: RI = 3.91, Xc= 1.11, sex = 3.73 | |
| Predicted ASM | 17.4 ± 3.60 kg, * p = 0.835 |
| Device | ASM (Mean ± SD) | R2 | TE (kg) | Subjective Rating | CE (Mean ± SD) | LoA (Kg) | ry-y’,mean | PIA | |
|---|---|---|---|---|---|---|---|---|---|
| Women | Man | ||||||||
| DXA | 17.38 ± 3.74 | ||||||||
| Standing Modes of BIA | |||||||||
| BIAstanding_New | 17.39 ± 3.59 | 0.924 | 1.04 | Good | Excellent | − 0.02 ± 1.03 | −2.04, 2.01 | −0.145 * | 81.4 |
| BIAInBody770 | 17.35 ± 4.00 | 0.917 | 1.15 | Good | Very good | 0.03 ± 1.15 | −2.22, 2.29 | −0.223 * | 77.9 |
| BIAYamada | 18.67 ± 4.07 | 0.891 | 1.86 | Poor | Poor | −1.29 ± 1.35 ** | −3.94, −1.35 | −0.252 ** | 48.7 |
| Supine Modes of BIA | |||||||||
| BIAsupine_New | 17.37 ± 3.60 | 0.928 | 1.00 | Very good | Excellent | 0.02 ± 1.10 | −1.95, 1.98 | 0.138 | 83.9 |
| BIAInBodyS10 | 19.08 ± 4.43 | 0.914 | 2.20 | Poor | Poor | −1.71 ± 1.38 ** | −4.42, 1.00 | −0.464 ** | 37.4 |
| BIAVermeiren | 15.80 ± 3.38 | 0.916 | 1.81 | Poor | Poor | 1.42 ± 1.13 ** | −0.80, 3.64 | −0.327 ** | 39.7 |
| BIAScaroflieri | 17.77 ± 3.46 | 0.906 | 1.21 | Fairly good | Very good | −0.39 ± 1.16 ** | −2.66, 1.89 | −0.243 ** | 74.9 |
| BIASergi | 16.60 ± 3.45 | 0.919 | 1.33 | Fair | Good | 0.78 ± 1.08 ** | −1.34, 2.90 | −0.275 ** | 67.3 |
| BIAKyle | 17.34 ± 4.09 | 0.923 | 1.15 | Good | Very good | 0.04 ± 1.16 | −2.23, 2.30 | −0.307 ** | 74.4 |
| BIAKim | 11.64 ± 2.79 | 0.899 | 5.91 | Poor | Poor | 5.75 ± 1.42 ** | 2.96, 8.53 | −0.098 | 0.0 |
| BIARangel | 16.81 ± 4.06 | 0.919 | 1.30 | Fairly good | Good | 0.57 ± 1.17 ** | −1.72, 2.87 | −0.276 ** | 64.3 |
| Equations/Device | Overall Agreement N (%) | Cohen’s Kappa | Sensitivity | Specificity | PPV | NPV |
|---|---|---|---|---|---|---|
| Standing Modes of BIA | ||||||
| BIAInBody770_NEW | 184 (92.5) | 0.664 * | 60.0 | 98.2 | 85.7 | 93.3 |
| BIAInBody770 | 165 (82.9) | 0.397 * | 51.5 | 89.2 | 48.6 | 90.2 |
| Supine Modes of BIA | ||||||
| BIAInBodyS10_NEW | 185 (93.0) | 0.691 * | 63.3 | 98.2 | 86.4 | 93.8 |
| BIAKyle | 168 (84.4) | 0.416 * | 48.5 | 91.6 | 53.3 | 89.9 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jeon, K.C.; Kim, S.-Y.; Jiang, F.L.; Chung, S.; Ambegaonkar, J.P.; Park, J.-H.; Kim, Y.-J.; Kim, C.-H. Prediction Equations of the Multifrequency Standing and Supine Bioimpedance for Appendicular Skeletal Muscle Mass in Korean Older People. Int. J. Environ. Res. Public Health 2020, 17, 5847. https://doi.org/10.3390/ijerph17165847
Jeon KC, Kim S-Y, Jiang FL, Chung S, Ambegaonkar JP, Park J-H, Kim Y-J, Kim C-H. Prediction Equations of the Multifrequency Standing and Supine Bioimpedance for Appendicular Skeletal Muscle Mass in Korean Older People. International Journal of Environmental Research and Public Health. 2020; 17(16):5847. https://doi.org/10.3390/ijerph17165847
Chicago/Turabian StyleJeon, Kwon Chan, So-Young Kim, Fang Lin Jiang, Sochung Chung, Jatin P. Ambegaonkar, Jae-Hyeon Park, Young-Joo Kim, and Chul-Hyun Kim. 2020. "Prediction Equations of the Multifrequency Standing and Supine Bioimpedance for Appendicular Skeletal Muscle Mass in Korean Older People" International Journal of Environmental Research and Public Health 17, no. 16: 5847. https://doi.org/10.3390/ijerph17165847
APA StyleJeon, K. C., Kim, S.-Y., Jiang, F. L., Chung, S., Ambegaonkar, J. P., Park, J.-H., Kim, Y.-J., & Kim, C.-H. (2020). Prediction Equations of the Multifrequency Standing and Supine Bioimpedance for Appendicular Skeletal Muscle Mass in Korean Older People. International Journal of Environmental Research and Public Health, 17(16), 5847. https://doi.org/10.3390/ijerph17165847





