Identification of a Dual Inhibitor of Secreted Phospholipase A2 (GIIA sPLA2) and SARS-CoV-2 Main Protease
Abstract
1. Introduction
2. Results
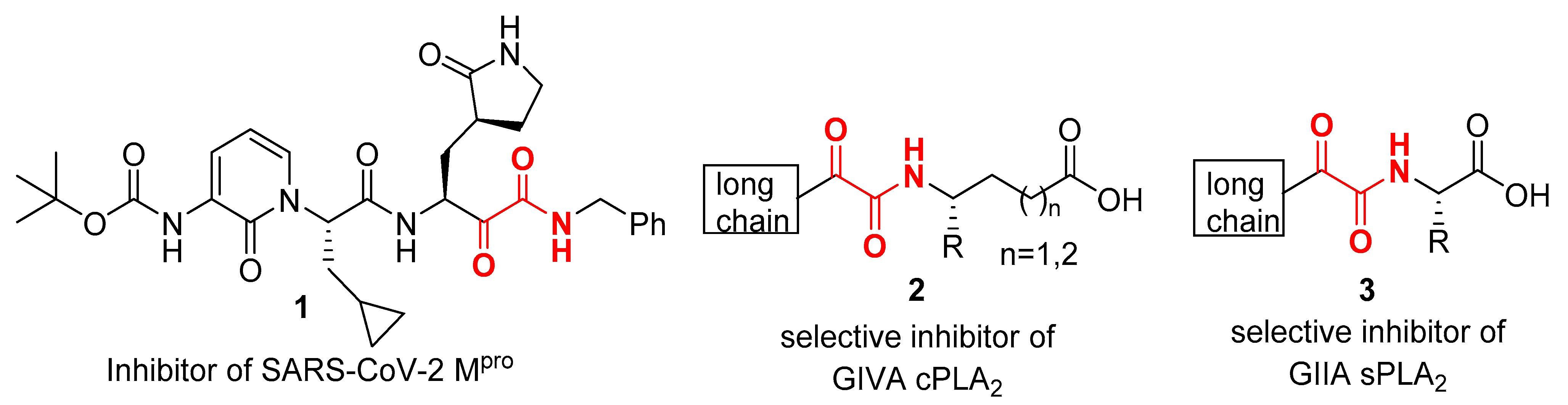
2.1. Design of Inhibitors
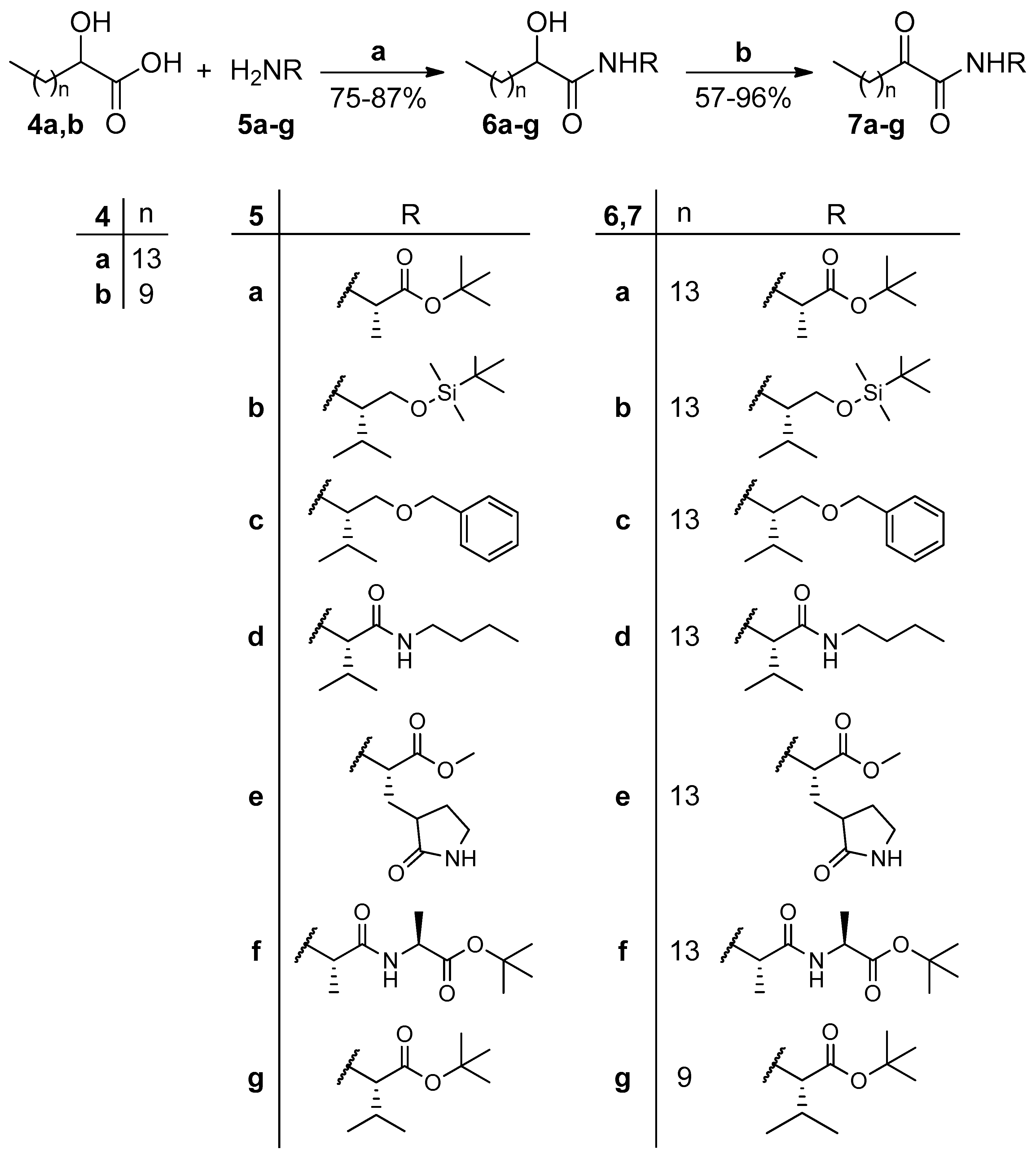
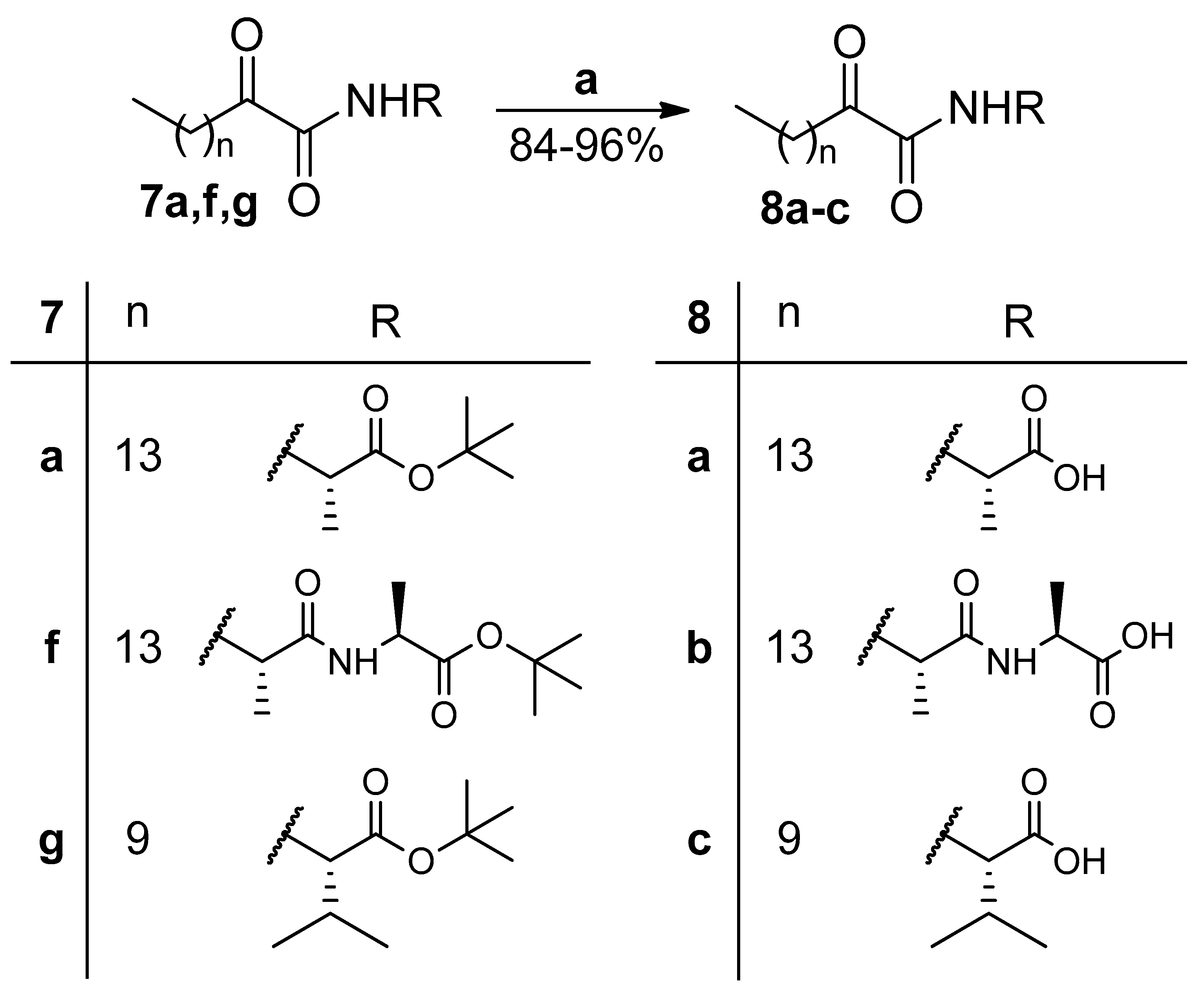
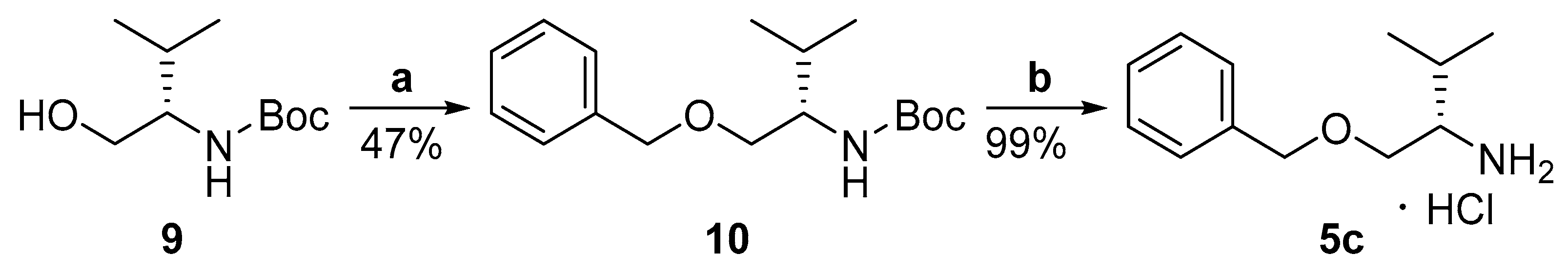
2.2. Synthesis
2.3. Inhibition of SARS-CoV-2 Mpro by 2-Oxoamide PLA2 Inhibitors and Analogs
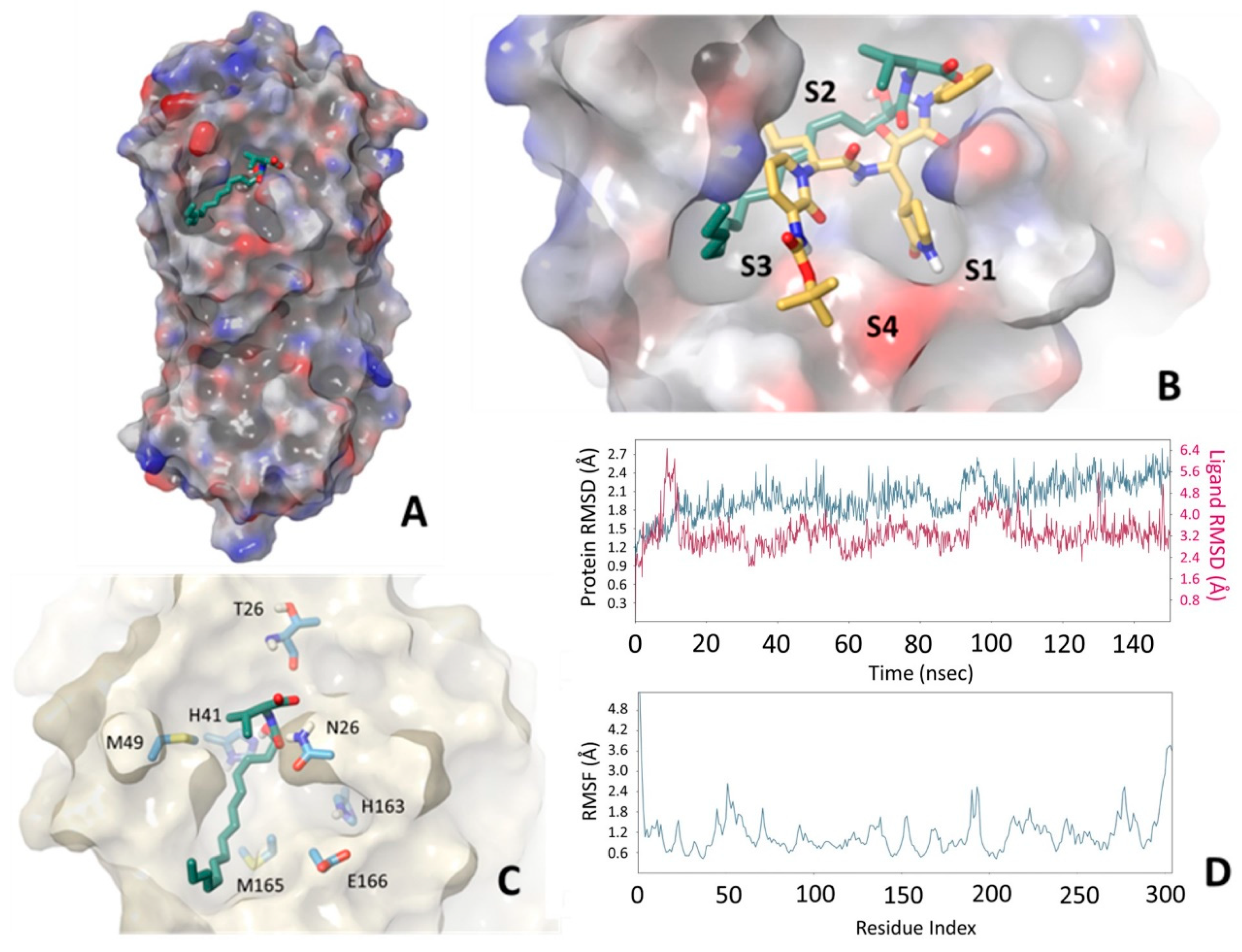
2.4. Molecular Mechanics Docking and Molecular Dynamics Calculations
3. Discussion
4. Materials and Methods
4.1. General Chemistry Methods
4.2. General Procedure for the Coupling of α-Hydroxycarboxylic Acids 4a,b with Amines 5a–g
4.2.1. (2S)-tert-Butyl 2-(2-hydroxyhexadecanamido)propanoate (6a)
4.2.2. N-((S)-1-((tert-Butyldimethylsilyl)oxy)-3-methylbutan-2-yl)-2-hydroxyhexadecanamide (6b)
4.2.3. N-((S)-1-(Benzyloxy)-3-methylbutan-2-yl)-2-hydroxyhexadecanamide (6c)
4.2.4. N-((S)-1-(Butylamino)-3-methyl-1-oxobutan-2-yl)-2-hydroxyhexadecanamide (6d)
4.2.5. (2S)-Methyl 2-(2-hydroxyhexadecanamido)-3-(2-oxopyrrolidin-3-yl)propanoate (6e)
4.2.6. (2S)-tert-Butyl 2-((2S)-2-(2-hydroxyhexadecanamido)propanamido)propanoate (6f)
4.2.7. (2S)-tert-Butyl 2-(2-hydroxydodecanamido)-3-methylbutanoate (6g)
4.3. General Procedure for the Oxidation of Hydroxyamides 6a–g to Oxoamides 7a–g
4.3.1. (S)-tert-Butyl 2-(2-oxohexadecanamido)propanoate (7a)
4.3.2. (S)-N-(1-((tert-Butyldimethylsilyl)oxy)-3-methylbutan-2-yl)-2-oxohexadecanamide (7b)
4.3.3. (S)-N-(1-(Benzyloxy)-3-methylbutan-2-yl)-2-oxohexadecanamide (7c)
4.3.4. (S)-N-(1-(Butylamino)-3-methyl-1-oxobutan-2-yl)-2-oxohexadecanamide (7d)
4.3.5. (2S)-Methyl 2-(2-oxohexadecanamido)-3-(2-oxopyrrolidin-3-yl)propanoate (7e)
4.3.6. (S)-tert-Butyl 2-((S)-2-(2-oxohexadecanamido)propanamido)propanoate (7f)
4.3.7. (S)-tert-Butyl 3-methyl-2-(2-oxododecanamido)butanoate (7g)
4.4. General Procedure of Deprotection of tert-Butyl Esters to Carboxylic Acids 8a–c
4.4.1. (S)-2-(2-Oxohexadecanamido)propanoic Acid (8a)
4.4.2. (S)-2-((S)-2-(2-Oxohexadecanamido)propanamido)propanoic Acid (8b)
4.4.3. (S)-3-Methyl-2-(2-oxododecanamido)butanoic Acid (8c)
4.5. (S)-1-((tert-Butyldimethylsilyl)oxy)-3-methylbutan-2-amine (5b)
4.6. (S)-tert-Butyl (1-(benzyloxy)-3-methylbutan-2-yl)carbamate (10)
4.7. (S)-1-(Benzyloxy)-3-methylbutan-2-aminium chloride (5c)
4.8. Enzyme Assay
4.9. Covalent Docking Calculations
4.9.1. Protein Preparation
4.9.2. Covalent Docking
4.10. Molecular Dynamics Simulations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AA | arachidonic acid |
| DMF | N,N-dimethylformamide |
| EDC∙HCl | 1-ethyl-3-(3-dimethylaminopropyl)carbodiimide hydrochloride |
| EDTA | ethylene diamine tetra-acetic acid |
| FDA | Food and Drug Administration |
| FFAs | free fatty acids |
| FRET | fluorescence resonance energy transfer |
| GIIA sPLA2 | secreted PLA2 |
| GIVA cPLA2 | cytosolic PLA2 |
| GVIA iPLA2 | calcium-independent PLA2 |
| HOBt | 1-hydroxybenzotriazole |
| HRMS | high-resolution mass spectrometry |
| Mpro | main protease |
| MD | molecular dynamics |
| OA | oleic acid |
| PCs | phosphatidylcholines |
| PLA2 | phospholipase A2 |
| RdRp | RNA-dependent RNA polymerase |
| r.t. | room temperature |
| SARS-CoV-2 | severe acute respiratory syndrome coronavirus-2 |
| TFA | trifluoroacetic acid |
| THF | tetrahydrofuran |
| TLC | thin-layer chromatography |
| Tris | tris(hydroxymethyl)aminomethane |
References
- Coronavirus Disease (COVID-19) Pandemic. Available online: https://www.who.int/emergencies/diseases/novel-coronavirus-2019 (accessed on 26 March 2022).
- Cannalire, R.; Cerchia, C.; Beccari, A.R.; Saverio Di Leva, F.; Summa, V. Targeting SARS-CoV-2 proteases and polymerase for COVID-19 treatment: State of the art and future opportunities. J. Med. Chem. 2022, 65, 2716–2746. [Google Scholar] [CrossRef] [PubMed]
- Citarella, A.; Scala, A.; Piperno, A.; Micale, N. SARS-CoV-2 Mpro: A potential target for peptidomimetics and small-molecule inhibitors. Biomolecules 2021, 11, 607. [Google Scholar] [CrossRef]
- Casari, I.; Manfredi, M.; Metharom, P.; Falasca, M. Dissecting lipid metabolism alterations in SARS-CoV-2. Prog. Lipid Res. 2021, 82, 101092. [Google Scholar] [CrossRef]
- Pimentel, L.L.; Rodríguez-Alcalá, L.M. Cholesterol, inflammation, and phospholipids: COVID-19 share traits with cardiovascular disease. BBA—Mol. Cell Biol. Lipids 2021, 1866, 158839. [Google Scholar] [CrossRef]
- Murakami, M.; Taketomi, Y.; Miki, Y.; Sato, H.; Yamamoto, K.; Lambeau, G. Emerging roles of secreted phospholipase A2 enzymes: The 3rd edition. Biochimie 2014, 107, 105–113. [Google Scholar] [CrossRef]
- Mouchlis, V.D.; Dennis, E.A. Phospholipase A2 catalysis and lipid mediator lipidomics. BBA—Mol. Cell Biol. Lipids 2019, 1864, 766–771. [Google Scholar] [CrossRef]
- Vasquez, A.M.; Mouchlis, V.D.; Dennis, E.A. Review of four major distinct types of human phospholipase A2. Adv. Biol. Regul. 2018, 67, 212–218. [Google Scholar] [CrossRef] [PubMed]
- Bock, J.-O.; Ortea, I. Re-analysis of SARS-CoV-2-infected host cell proteomics time-course data by impact pathway analysis and network analysis: A potential link with inflammatory response. Aging 2020, 12, 11277–11286. [Google Scholar] [CrossRef] [PubMed]
- Wu, D.; Shu, T.; Yang, X.; Song, J.-X.; Zhang, M.; Yao, C.; Liu, W.; Huang, M.; Yu, Y.; Yang, Q.; et al. Plasma metabolomic and lipidomic alterations associated with COVID-19. Natl. Sci. Rev. 2020, 7, 1157–1168. [Google Scholar] [CrossRef]
- Barberis, E.; Timo, S.; Amede, E.; Vanella, V.V.; Puricelli, C.; Cappellano, G.; Raineri, D.; Cittone, M.G.; Rizzi, E.; Pedrinelli, A.R.; et al. Large-scale plasma analysis revealed new mechanisms and molecules associated with the host response to SARS-CoV-2. Int. J. Mol. Sci. 2020, 21, 8623. [Google Scholar] [CrossRef]
- Snider, J.M.; You, J.K.; Wang, X.; Snider, A.J.; Hallmark, B.; Zec, M.M.; Seeds, M.C.; Sergeant, S.; Johnstone, L.; Wang, Q.; et al. Group IIA secreted phospholipase A2 is associated with the pathobiology leading to COVID-19 mortality. J. Clin. Investig. 2021, 131, 149236. [Google Scholar] [CrossRef] [PubMed]
- Nikolaou, A.; Kokotou, M.G.; Vasilakaki, S.; Kokotos, G. Small-molecule inhibitors as potential therapeutics and as tools to understand the role of phospholipases A2. BBA—Mol. Cell Biol. Lipids 2019, 1864, 941–956. [Google Scholar] [CrossRef]
- Scott, K.F.; Mann, T.J.; Fatima, S.; Sajinovic, M.; Razdan, A.; Kim, R.R.; Cooper, A.; Roohullah, A.; Bryant, K.J.; Gamage, K.K.; et al. Human group IIA phospholipase A2—Three decades on from its discovery. Molecules 2021, 26, 7267. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Lin, D.; Sun, X.; Curth, U.; Drosten, C.; Sauerhering, L.; Becker, S.; Rox, K.; Hilgenfeld, R. Crystal structure of SARS-CoV-2 main protease provides a basis for design of improved α-ketoamide inhibitors. Science 2020, 368, 409–412. [Google Scholar] [CrossRef]
- Ma, C.; Sacco, M.D.; Hurst, B.; Townsend, J.A.; Hu, Y.; Szeto, T.; Zhang, X.; Tarbet, B.; Marty, M.T.; Chen, Y.; et al. Boceprevir, GC-376, and calpain inhibitors II, XII inhibit SARS-CoV-2 viral replication by targeting the viral main protease. Cell Res. 2020, 30, 678–692. [Google Scholar] [CrossRef] [PubMed]
- Dai, W.; Zhang, B.; Jiang, X.-M.; Su, H.; Li, J.; Zhao, Y.; Xie, X.; Jin, Z.; Peng, J.; Liu, F.; et al. Structure-based design of antiviral drug candidates targeting the SARS-CoV-2 main protease. Science 2020, 368, 1331–1339. [Google Scholar] [CrossRef] [PubMed]
- Chan, H.T.H.; Moesser, M.A.; Walters, R.K.; Malla, T.R.; Twidale, R.M.; John, T.; Deeks, H.M.; Johnston-Wood, T.; Mikhailov, V.; Sessions, R.B.; et al. Discovery of SARS-CoV-2 Mpro peptide inhibitors from modelling substrate and ligand binding. Chem. Sci. 2021, 12, 13686–13703. [Google Scholar] [CrossRef]
- Breidenbach, J.; Lemke, C.; Pillaiyar, T.; Schäkel, L.; Al Hamwi, G.; Diett, M.; Gedschold, R.; Geiger, N.; Lopez, V.; Mirza, S.; et al. Targeting the main protease of SARS-CoV-2: From the establishment of high throughput screening to the design of tailored inhibitors. Angew. Chem. Int. Ed. 2021, 60, 10423–10429. [Google Scholar] [CrossRef]
- Dampalla, C.S.; Rathnayake, A.D.; Perera, K.D.; Jesri, A.-R.M.; Nguyen, H.N.; Miller, M.J.; Thurman, H.A.; Zheng, J.; Kashipathy, M.M.; Battaile, K.P.; et al. Structure-guided design of potent inhibitors of SARS-CoV-2 3CL protease: Structural, biochemical, and cell-based studies. J. Med. Chem. 2021, 64, 17846–17865. [Google Scholar] [CrossRef] [PubMed]
- Dampalla, C.S.; Kim, Y.; Bickmeier, N.; Rathnayake, A.D.; Nguyen, H.N.; Zheng, J.; Kashipathy, M.M.; Baird, M.A.; Battaile, K.P.; Lovell, S.; et al. Structure-guided design of conformationally constrained cyclohexane inhibitors of severe acute respiratory syndrome coronavirus-2 3CL protease. J. Med. Chem. 2021, 64, 10047–10058. [Google Scholar] [CrossRef]
- Stephens, D.; Barbayianni, E.; Constantinou-Kokotou, V.; Peristeraki, A.; Six, D.A.; Cooper, J.; Harkewicz, R.; Deems, R.A.; Dennis, E.A.; Kokotos, G. Differential inhibition of group IVA and group VIA phospholipases A2 by 2-oxoamides. J. Med. Chem. 2006, 49, 2821–2828. [Google Scholar] [CrossRef][Green Version]
- Six, D.A.; Barbayianni, E.; Loukas, V.; Constantinou-Kokotou, V.; Hadjipavlou-Litina, D.; Stephens, D.; Wong, A.C.; Magrioti, V.; Moutevelis-Minakakis, P.; Baker, S.F.; et al. Structure-activity relationship of 2-oxoamide inhibition of group IVA cytosolic phospholipase A2 and group V secreted phopholipase A2. J. Med. Chem. 2007, 50, 4222–4235. [Google Scholar] [CrossRef] [PubMed]
- Vasilakaki, S.; Barbayianni, E.; Leonis, G.; Papadopoulos, M.G.; Mavromoustakos, T.; Gelb, M.H.; Kokotos, G. Development of a potent 2-oxoamide inhibitor of secreted phospholipase A2 guided by molecular docking calculations and molecular dynamics simulations. Bioorg. Med. Chem. 2016, 24, 1683–1695. [Google Scholar] [CrossRef] [PubMed]
- Magrioti, V.; Nikolaou, A.; Smyrniotou, A.; Shah, I.; Constantinou-Kokotou, V.; Dennis, E.A.; Kokotos, G. New potent and selective polyfluoroalkyl ketone inhibitors of GVIA calcium-independent phospholipase A2. Bioorg. Med. Chem. 2013, 21, 5823–5829. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Burkhart, J.P.; Peet, N.P.; Bey, P. Oxidation of α-hydroxy esters to α-keto esters using the Dess-Martin periodinane reagent. Tetrahedron Lett. 1988, 29, 3433–3436. [Google Scholar] [CrossRef]
- So, R.C.; Ndonye, R.; Izmirian, D.P.; Richardson, S.K.; Guerrera, R.L.; Howell, A.R. Straightforward synthesis of sphinganines via a serine-derived Weinreb amide. J. Org. Chem. 2004, 69, 3233–3235. [Google Scholar] [CrossRef]
- Sacco, M.D.; Ma, C.; Lagarias, P.; Gao, A.; Townsend, J.A.; Meng, X.; Dube, P.; Zhang, X.; Hu, Y.; Kitamura, N.; et al. Structure and inhibition of the SARS-CoV-2 main protease reveal strategy for developing dual inhibitors against Mpro and cathepsin L. Sci. Adv. 2020, 6, eabe0751. [Google Scholar] [CrossRef]
- Dennis, E.A.; Norris, P.C. Eicosanoid storm in infection and inflammation. Nat. Rev. Immunol. 2015, 15, 511–523. [Google Scholar] [CrossRef]
- Pungerčar, J.; Bihl, F.; Lambeau, G.; Križaj, I. What do secreted phospholipases A2 have to offer in combat against different viruses up to SARS-CoV-2? Biochimie 2021, 189, 40–50. [Google Scholar] [CrossRef]
- Hoffman, R.; Kania, R.S.; Brothers, M.A.; Davies, J.F.; Ferre, R.A.; Gajiwala, K.S.; He, M.; Hogan, R.J.; Kozminski, K.; Li, L.Y.; et al. Discovery of ketone-based covalent inhibitors of coronavirus 3CL proteases for the potential therapeutic treatment of COVID-19. J. Med. Chem. 2020, 63, 12725–12747. [Google Scholar] [CrossRef]
- Owen, D.R.; Allerton, C.M.N.; Anderson, A.S.; Aschenbrenner, L.; Avery, M.; Berritt, S.; Boras, B.; Cardin, R.D.; Carlo, A.; Coffman, K.J.; et al. An oral SARS-CoV-2 Mpro inhibitor clinical candidate for the treatment of COVID-19. Science 2021, 374, 1586–1593. [Google Scholar] [CrossRef]
- Merad, M.; Martin, J.C. Pathological inflammation in patients with COVID-19: A key role for monocytes and macrophages. Nat. Rev. Immunol. 2020, 20, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Schwarz, B.; Sharma, L.; Roberts, L.; Peng, X.; Bermejo, S.; Leighton, I.; Casanovas-Massana, A.; Minasyan, M.; Farhadian, S.; Ko, A.I.; et al. Cutting edge: Severe SARS-CoV-2 infection in humans is defined by a shift in the serum lipidome, resulting in dysregulation of eicosanoid immune mediators. J. Immunol. 2021, 206, 329–334. [Google Scholar] [CrossRef] [PubMed]
- Sastry, G.M.; Adzhigirey, M.; Day, T.; Annabhimoju, R.; Sherman, W. Protein and ligand preparation: Parameters, protocols, and influence on virtual screening enrichments. J. Comput. Aided Mol. Des. 2013, 27, 221–234. [Google Scholar] [CrossRef]
- Schrödinger, LLC. Schrödinger Release 2021-4. LigPrep; Schrödinger, LLC: New York, NY, USA, 2021. [Google Scholar]
- Zhu, K.; Borrelli, K.W.; Greenwood, J.R.; Day, T.; Abel, R.; Farid, R.S.; Harder, E. Docking covalent inhibitors: A parameter free approach to pose prediction and scoring. J. Chem. Inf. Model. 2014, 54, 1932–1940. [Google Scholar] [CrossRef]
- D. E. Shaw Research. Schrödinger Release 2021-4. Desmond Molecular Dynamics System; Maestro-Desmond Interoperability, Tools; D. E. Shaw Research: New York, NY, USA; Schrödinger: New York, NY, USA, 2021. [Google Scholar]
| Entry | Code | Structure | Inhibition Rate (%) (40 μM) a | Inhibition Rate (%) (100 μM) a |
|---|---|---|---|---|
| 1 | AX109 | 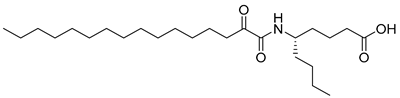 | 20.38 ± 2.75 | 32.11 ± 5.44 |
| 2 | AX074 |  | 47.83 ± 3.27 | 50.52 ± 2.63 |
| 3 | GK241 | 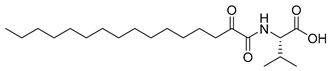 | 76.90 ± 0.41 | 97.33 ± 1.15 |
| 4 | GK187 | 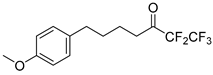 | 26.72 ± 3.50 | 32.62 ± 4.67 |
| Entry | Code | Structure | Inhibition Rate (%) a (40 μM) |
|---|---|---|---|
| 1 | 7a |  | - b |
| 2 | 7b |  | - b |
| 3 | 7c |  | - b |
| 4 | 7d | 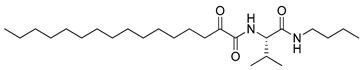 | - b |
| 5 | 7e | 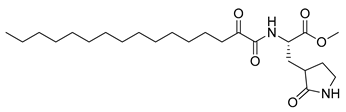 | - b |
| 6 | 7f | 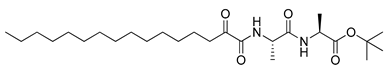 | 3.83 ± 1.34 |
| 7 | 8a | 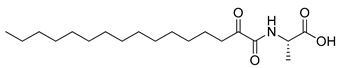 | 65.49 ± 2.79 |
| 8 | 8b | 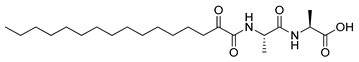 | 6.21 ± 5.24 |
| 9 | 8d | 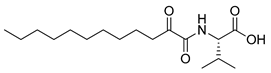 | - c |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Theodoropoulou, M.A.; Koutoulogenis, G.S.; Zhang, L.; Akrani, I.; Mikros, E.; Hilgenfeld, R.; Kokotos, G. Identification of a Dual Inhibitor of Secreted Phospholipase A2 (GIIA sPLA2) and SARS-CoV-2 Main Protease. Pharmaceuticals 2022, 15, 961. https://doi.org/10.3390/ph15080961
Theodoropoulou MA, Koutoulogenis GS, Zhang L, Akrani I, Mikros E, Hilgenfeld R, Kokotos G. Identification of a Dual Inhibitor of Secreted Phospholipase A2 (GIIA sPLA2) and SARS-CoV-2 Main Protease. Pharmaceuticals. 2022; 15(8):961. https://doi.org/10.3390/ph15080961
Chicago/Turabian StyleTheodoropoulou, Maria A., Giorgos S. Koutoulogenis, Linlin Zhang, Ifigeneia Akrani, Emmanuel Mikros, Rolf Hilgenfeld, and George Kokotos. 2022. "Identification of a Dual Inhibitor of Secreted Phospholipase A2 (GIIA sPLA2) and SARS-CoV-2 Main Protease" Pharmaceuticals 15, no. 8: 961. https://doi.org/10.3390/ph15080961
APA StyleTheodoropoulou, M. A., Koutoulogenis, G. S., Zhang, L., Akrani, I., Mikros, E., Hilgenfeld, R., & Kokotos, G. (2022). Identification of a Dual Inhibitor of Secreted Phospholipase A2 (GIIA sPLA2) and SARS-CoV-2 Main Protease. Pharmaceuticals, 15(8), 961. https://doi.org/10.3390/ph15080961








