Displacement Micropump with Check Valves for Diabetes Care—The Challenge of Pumping Insulin at Negative Pressure
Definition
1. Introduction
2. Description of a Displacement MEMS Micropump
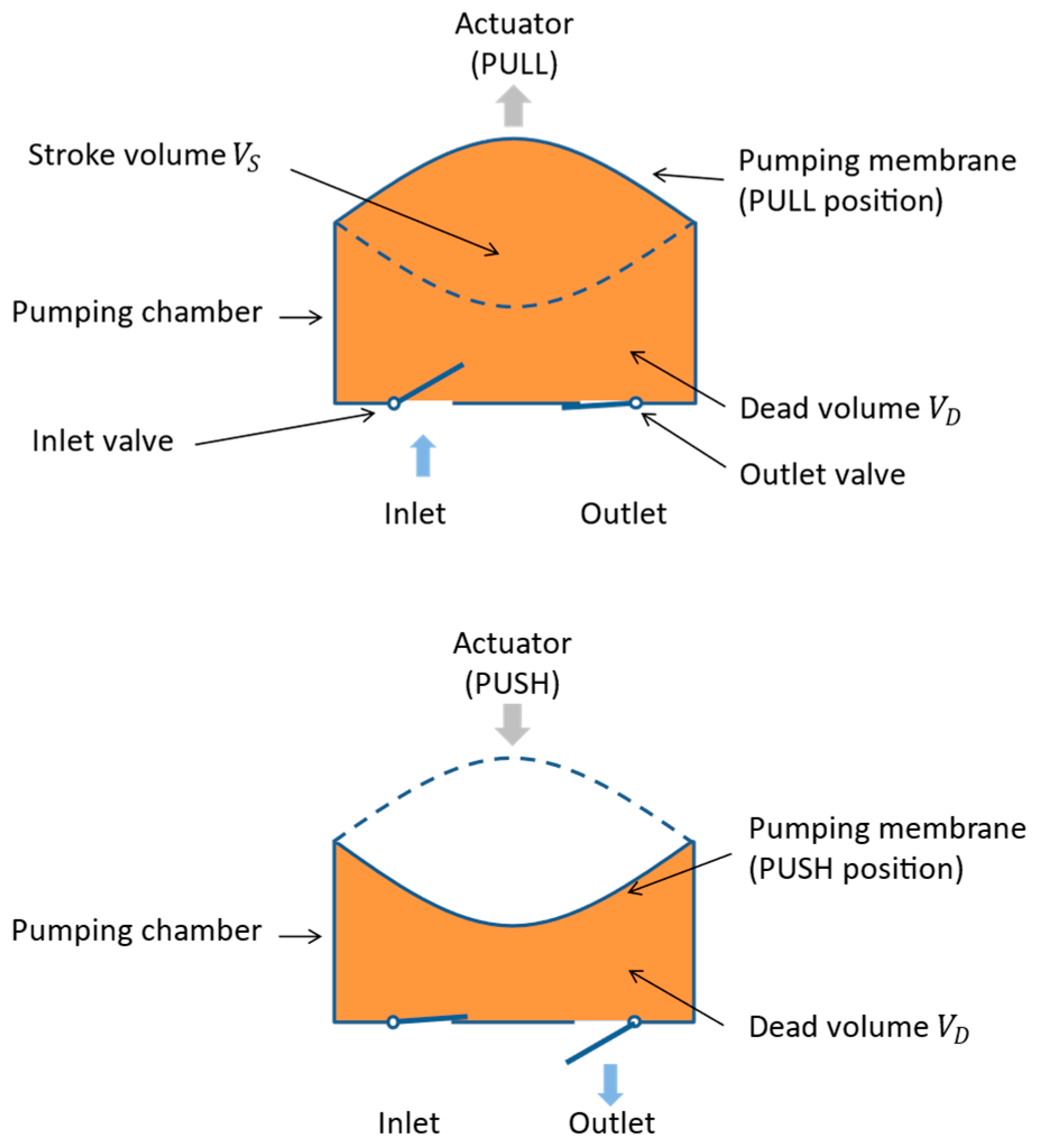
2.1. Basic Operation
- The supply phase, wherein the displacement of the membrane induces an increase of the pumping chamber volume; the generated underpressure leads to an opening of the inlet valve and the filling of the pumping chamber cavity with insulin that comes from the non-pressurized reservoir.
- The infusion phase, wherein the displacement of the membrane reduces the pumping chamber volume; the induced overpressure opens the outlet valve and generates a net flow from the pumping chamber toward the patient through the infusion set or the cannula.
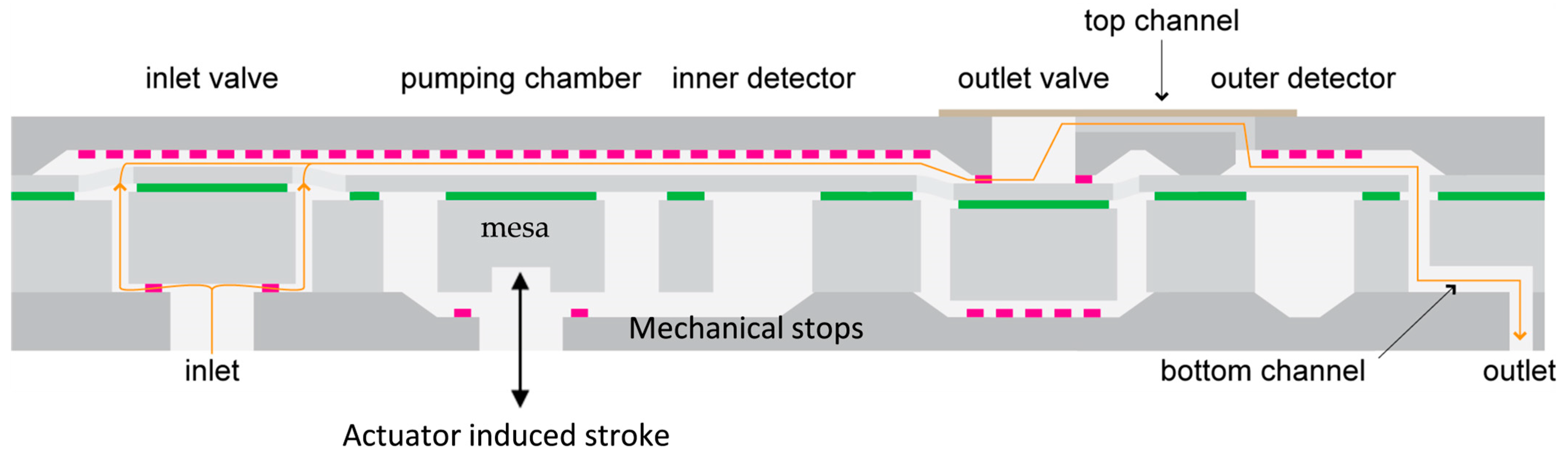
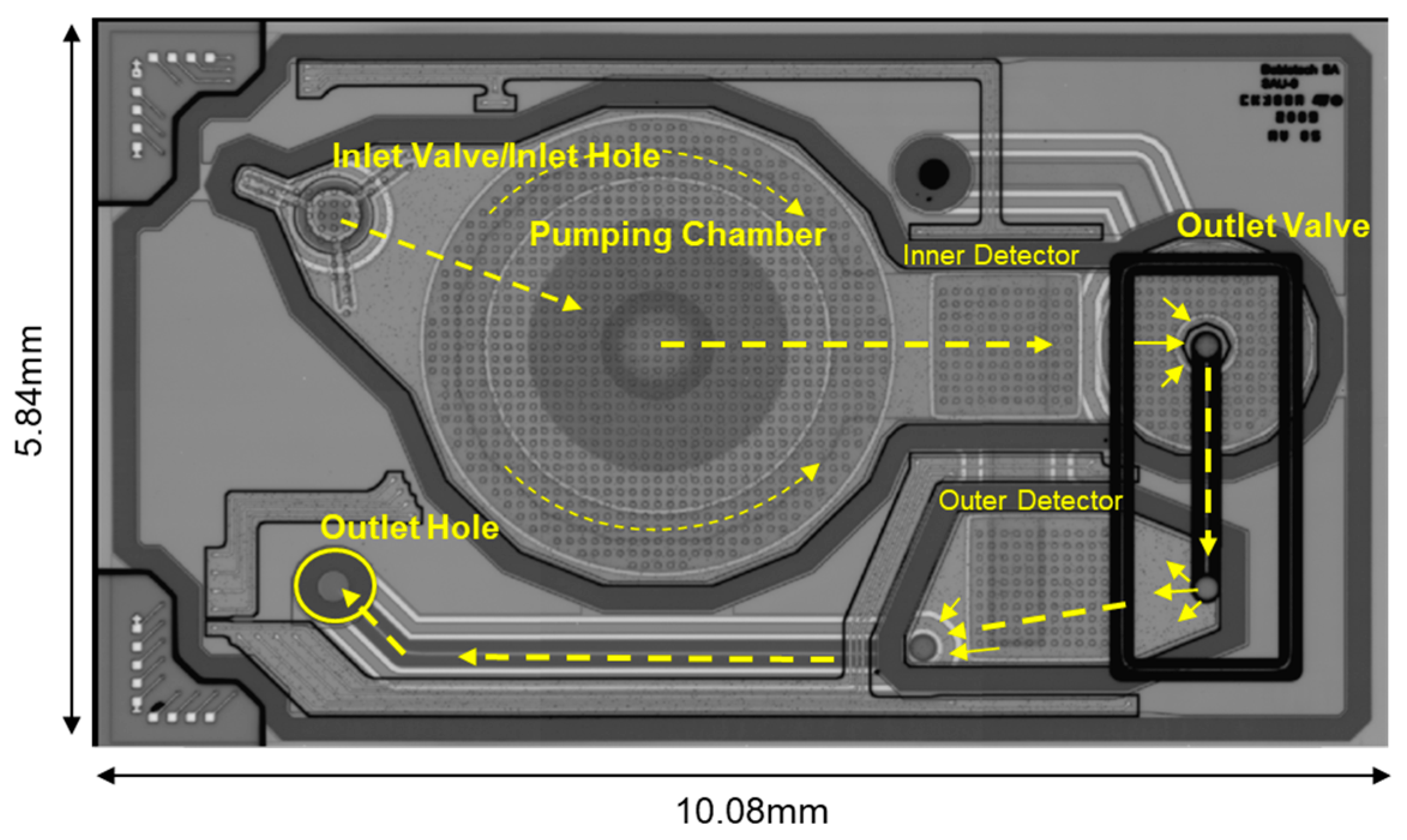
2.2. Detailed Structure of a MEMS Micropump
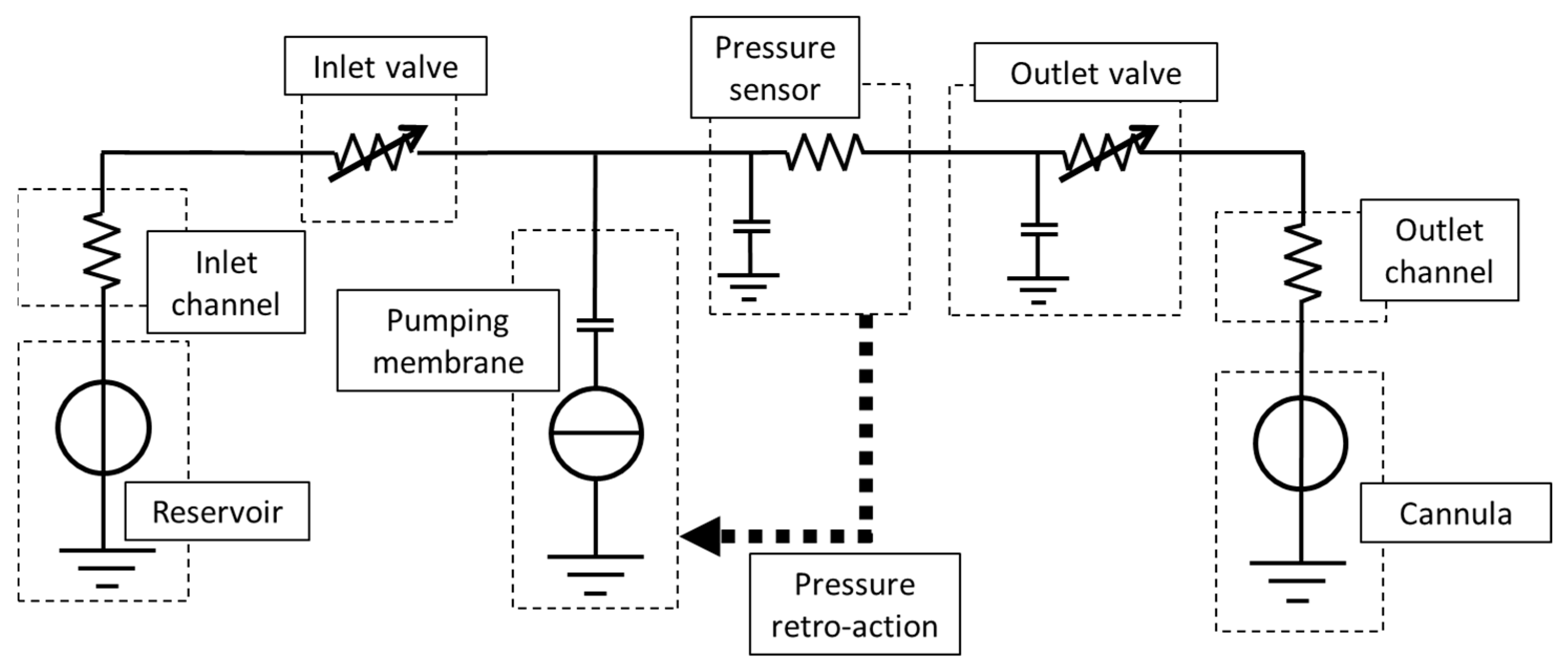
2.3. Micropump Modeling
3. Specific Factors Influencing the Design of such an Insulin Displacement Micropump
3.1. Insulin Aggregation
3.2. Shear Stress and Hydrophobic Surfaces
3.3. Air Management
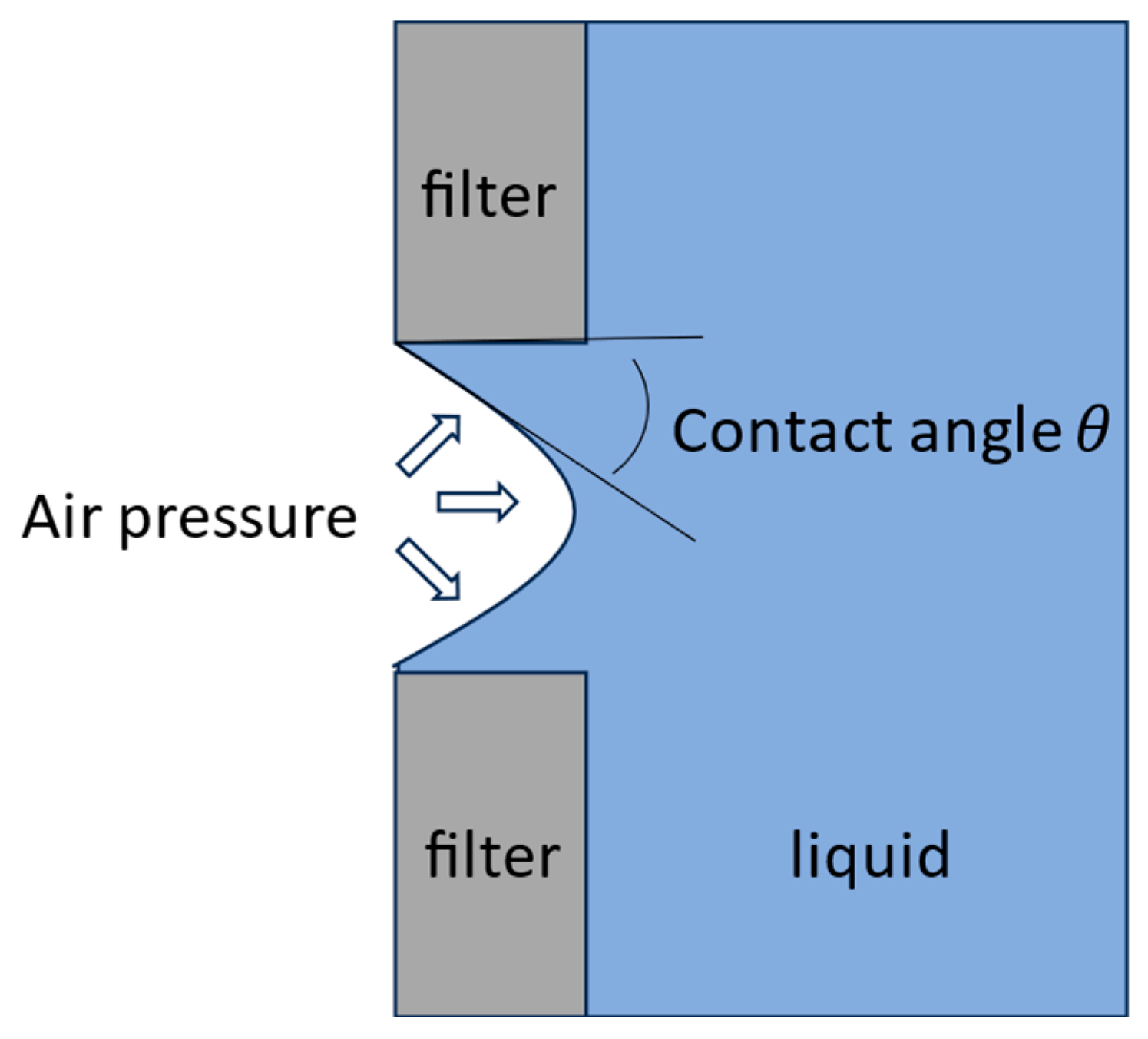
3.3.1. Air in the Insulin Reservoir and Air Filter
3.3.2. Self-Priming Capability
3.3.3. Capillary Adhesion
3.3.4. Valve Pretension
3.3.5. Air in the Pumping Chamber: Underdelivery, Foam, and Cavitation
4. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Pickup, J.C.; Keen, H.; Parsons, J.A.; Alberti, K.G. Continuous subcutaneous insulin infusion: An approach to achieving normoglycaemia. Br. Med. J. 1978, 1, 204–207. [Google Scholar] [CrossRef] [PubMed]
- Bode, B.W.; Steed, R.D.; Davidson, P.C. Reduction in severe hypoglycemia with long-term continuous subcutaneous insulin infusion in type I diabetes. Diabetes Care 1996, 19, 324–327. [Google Scholar] [CrossRef] [PubMed]
- Lenhard, M.J.; Reeves, G.D. Continuous subcutaneous insulin infusion: A comprehensive review of insulin pump therapy. Arch. Intern. Med. 2001, 161, 2293–2300. [Google Scholar] [CrossRef] [PubMed]
- Misso, M.L.; Egberts, K.J.; Page, M.; O’Connor, D.; Shaw, J. Cochrane review: Continuous subcutaneous insulin infusion (CSII) versus multiple insulin injections for type 1 diabetes mellitus. Evid.-Based Child Health A Cochrane Rev. J. 2010, 5, 1726–1867. [Google Scholar] [CrossRef]
- Bruttomesso, D.; Costa, S.; Baritussio, A. Continuous subcutaneous insulin infusion (CSII) 30 years later: Still the best option for insulin therapy. Diabetes/Metab. Res. Rev. 2009, 25, 99–111. [Google Scholar] [CrossRef] [PubMed]
- Priesterroth, L.; Grammes, J.; Clauter, M.; Kubiak, T. Diabetes technologies in people with type 1 diabetes mellitus and disordered eating: A systematic review on continuous subcutaneous insulin infusion, continuous glucose monitoring and automated insulin delivery. Diabet. Med. 2021, 38, e14581. [Google Scholar] [CrossRef] [PubMed]
- Dos Santos, T.J.; Campos JD, M.D.; Argente, J.; Rodríguez-Artalejo, F. Effectiveness and equity of continuous subcutaneous insulin infusions in pediatric type 1 diabetes: A systematic review and meta-analysis of the literature. Diabetes Res. Clin. Pract. 2021, 172, 108643. [Google Scholar] [CrossRef]
- Steil, G.M.; Panteleon, A.E.; Rebrin, K. Closed-loop insulin delivery—The path to physiological glucose control. Adv. Drug Deliv. Rev. 2004, 56, 125–144. [Google Scholar] [CrossRef]
- Hovorka, R. Closed-loop insulin delivery: From bench to clinical practice. Nat. Rev. Endocrinol. 2011, 7, 385–395. [Google Scholar] [CrossRef]
- Bally, L.; Thabit, H.; Hartnell, S.; Andereggen, E.; Ruan, Y.; Wilinska, M.E.; Evans, M.L.; Wertli, M.M.; Coll, A.P.; Stettler, C.; et al. Closed-loop insulin delivery for glycemic control in noncritical care. N. Engl. J. Med. 2018, 379, 547–556. [Google Scholar] [CrossRef]
- Bergenstal, R.M.; Garg, S.; Weinzimer, S.A.; Buckingham, B.A.; Bode, B.W.; Tamborlane, W.V.; Kaufman, F.R. Safety of a hybrid closed-loop insulin delivery system in patients with type 1 diabetes. JAMA 2016, 316, 1407–1408. [Google Scholar] [CrossRef] [PubMed]
- Tauschmann, M.; Thabit, H.; Bally, L.; Allen, J.M.; Hartnell, S.; Wilinska, M.E.; Ruan, Y.; Sibayan, J.; Kollman, C.; Cheng, P.; et al. Closed-loop insulin delivery in suboptimally controlled type 1 diabetes: A multicentre, 12-week randomised trial. Lancet 2018, 392, 1321–1329. [Google Scholar] [CrossRef] [PubMed]
- Bombaci, B.; Passanisi, S.; Alibrandi, A.; D’Arrigo, G.; Patroniti, S.; Averna, S.; Salzano, G.; Lombardo, F. One-year real-world study on comparison among different continuous subcutaneous insulin infusion devices for the management of pediatric patients with type 1 diabetes: The supremacy of hybrid closed-loop systems. Int. J. Environ. Res. Public Health 2022, 19, 10293. [Google Scholar] [CrossRef]
- Freckmann, G.; Buck, S.; Waldenmaier, D.; Kulzer, B.; Schnell, O.; Gelchsheimer, U.; Ziegler, R.; Heinemann, L. Insulin pump therapy for patients with type 2 diabetes mellitus: Evidence, current barriers, and new technologies. J. Diabetes Sci. Technol. 2021, 15, 901–915. [Google Scholar] [CrossRef] [PubMed]
- Wong, E.Y.; Vadlapatla, R.; Morello, C.M. Diabetes type 1 and type 2—Insulin delivery systems. In Drug Delivery Devices and Therapeutic Systems; Academic Press: New York, NY, USA, 2021; pp. 475–489. [Google Scholar]
- Leelarathna, L.; Roberts, S.A.; Hindle, A.; Markakis, K.; Alam, T.; Chapman, A.; Morris, J.; Urwin, A.; Jinadev, P.; Rutter, M.K. Comparison of different insulin pump makes under routine care conditions in adults with Type 1 diabetes. Diabet. Med. 2017, 34, 1372–1379. [Google Scholar] [CrossRef] [PubMed]
- Freckmann, G.; Kamecke, U.; Waldenmaier, D.; Haug, C.; Ziegler, R. Accuracy of bolus and basal rate delivery of different insulin pump systems. Diabetes Technol. Ther. 2019, 21, 201–208. [Google Scholar] [CrossRef] [PubMed]
- Borot, S.; Franc, S.; Cristante, J.; Penfornis, A.; Benhamou, P.Y.; Guerci, B.; Hanaire, H.; Renard, E.; Reznik, Y.; Simon, C.; et al. Accuracy of a new patch pump based on a microelectromechanical system (MEMS) compared to other commercially available insulin pumps: Results of the first in vitro and in vivo studies. J. Diabetes Sci. Technol. 2014, 8, 1133–1141. [Google Scholar] [CrossRef] [PubMed]
- Bissig, H.; Tschannen, M.; de Huu, M. Traceability of pulsed flow rates consisting of constant delivered volumes at given time interval. Flow Meas. Instrum. 2020, 73, 101729. [Google Scholar] [CrossRef]
- Thornton, J.; Sakhrani, V. How lubricant choice affects dose accuracy in insulin pumps. ONdrugDelivery Mag. 2017, 78, 32–36. [Google Scholar]
- Chappel, E.; Dumont-Fillon, D. Micropumps for drug delivery. In Drug Delivery Devices and Therapeutic Systems; Academic Press: New York, NY, USA, 2021; pp. 31–61. [Google Scholar]
- Chappel, E. Implantable drug delivery devices. In Drug Delivery Devices and Therapeutic Systems; Academic Press: New York, NY, USA, 2021; pp. 129–156. [Google Scholar]
- Fournier, S.; Chappel, E. Modeling of a Piezoelectric MEMS Micropump Dedicated to Insulin Delivery and Experimental Validation Using Integrated Pressure Sensors: Application to Partial Occlusion Management. J. Sens. 2017, 2017, 3719853. [Google Scholar] [CrossRef]
- Chappel, E. Robust alarm design strategy for medical devices: Application to air-in-line detection and occlusion management. Glob. J. Eng. Technol. Adv. 2023, 16, 030–040. [Google Scholar] [CrossRef]
- Cescon, M.; DeSalvo, D.J.; Ly, T.T.; Maahs, D.M.; Messer, L.H.; Buckingham, B.A.; Doyle, F.J., III; Dassau, E. Early detection of infusion set failure during insulin pump therapy in type 1 diabetes. J. Diabetes Sci. Technol. 2016, 10, 1268–1276. [Google Scholar] [CrossRef] [PubMed]
- Gibney, M.; Xue, Z.; Swinney, M.; Bialonczyk, D.; Hirsch, L. Reduced silent occlusions with a novel catheter infusion set (BD FlowSmart): Results from two open-label comparative studies. Diabetes Technol. Ther. 2016, 18, 136–143. [Google Scholar] [CrossRef] [PubMed]
- Freckmann, G.; Kamecke, U.; Waldenmaier, D.; Haug, C.; Ziegler, R. Occlusion detection time in insulin pumps at two different basal rates. J. Diabetes Sci. Technol. 2018, 12, 608–613. [Google Scholar] [CrossRef]
- Deiss, D.; Adolfsson, P.; Alkemade-van Zomeren, M.; Bolli, G.B.; Charpentier, G.; Cobelli, C.; Danne, T.; Girelli, A.; Mueller, H.; Verderese, C.A.; et al. Insulin infusion set use: European perspectives and recommendations. Diabetes Technol. Ther. 2016, 18, 517–524. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, N.T.; Huang, X.; Chuan, T.K. MEMS-micropumps: A review. J. Fluids Eng. 2002, 124, 384–392. [Google Scholar] [CrossRef]
- Laser, D.J.; Santiago, J.G. A review of micropumps. J. Micromech. Microeng. 2004, 14, R35. [Google Scholar] [CrossRef]
- Woias, P. Micropumps—Past, progress and future prospects. Sens. Actuators B Chem. 2005, 105, 28–38. [Google Scholar] [CrossRef]
- Amirouche, F.; Zhou, Y.; Johnson, T. Current micropump technologies and their biomedical applications. Microsyst. Technol. 2009, 15, 647–666. [Google Scholar] [CrossRef]
- Wang, Y.N.; Fu, L.M. Micropumps and biomedical applications–A review. Microelectron. Eng. 2018, 195, 121–138. [Google Scholar] [CrossRef]
- Bußmann, A.B.; Grünerbel, L.M.; Durasiewicz, C.P.; Thalhofer, T.A.; Wille, A.; Richter, M. Microdosing for drug delivery application—A review. Sens. Actuators A Phys. 2021, 330, 112820. [Google Scholar] [CrossRef]
- Van Lintel HT, G.; van De Pol FC, M.; Bouwstra, S. A piezoelectric micropump based on micromachining of silicon. Sens. Actuators 1988, 15, 153–167. [Google Scholar] [CrossRef]
- Maillefer, D.; Gamper, S.; Frehner, B.; Balmer, P.; Van Lintel, H.; Renaud, P. A high-performance silicon micropump for disposable drug delivery systems. In Proceedings of the Technical Digest. MEMS 2001. 14th IEEE International Conference on Micro Electro Mechanical Systems (Cat. No. 01CH37090), Interlaken, Switzerland, 25 January 2001; pp. 413–417. [Google Scholar]
- Schneeberger, N.; Blondel, A.; Boutaud, B.; Chappel, E.; Maillefer, D.; Schneider, V. Disposable insulin pump-a medical case study. In Proceedings of the DTIP of MEMS & MOEMS, Montreux, Switzerland, 12–14 May 2004; pp. 25–27. [Google Scholar]
- Schneeberger, N.; Allendes, R.; Bianchi, F.; Chappel, E.; Conan, C.; Gamper, S.; Schlund, M. Drug delivery micropump with built-in monitoring. Procedia Chem. 2009, 1, 1339–1342. [Google Scholar] [CrossRef][Green Version]
- Chappel, E.; Mefti, S.; Lettieri, G.L.; Proennecke, S.; Conan, C. High precision innovative micropump for artificial pancreas. In Microfluidics, BioMEMS, and Medical Microsystems XII; San Francisco, USA, 2–4 February 2014; SPIE: Bellingham, WA, USA, 2014; Volume 8976, pp. 279–290. [Google Scholar]
- Dumont-Fillon, D.; Tahriou, H.; Conan, C.; Chappel, E. Insulin micropump with embedded pressure sensors for failure detection and delivery of accurate monitoring. Micromachines 2014, 5, 1161–1172. [Google Scholar] [CrossRef]
- Bußmann, A.; Leistner, H.; Zhou, D.; Wackerle, M.; Congar, Y.; Richter, M.; Hubbuch, J. Piezoelectric silicon micropump for drug delivery applications. Appl. Sci. 2021, 11, 8008. [Google Scholar] [CrossRef]
- Junwu, K.; Zhigang, Y.; Taijiang, P.; Guangming, C.; Boda, W. Design and test of a high-performance piezoelectric micropump for drug delivery. Sens. Actuators A Phys. 2005, 121, 156–161. [Google Scholar] [CrossRef]
- Stehr, M.; Messner, S.; Sandmaier, H.; Zengerle, R. The VAMP—A new device for handling liquids or gases. Sens. Actuators A Phys. 1996, 57, 153–157. [Google Scholar] [CrossRef]
- Zengerle, R.; Ulrich, J.; Kluge, S.; Richter, M.; Richter, A. A bidirectional silicon micropump. Sens. Actuators A Phys. 1995, 50, 81–86. [Google Scholar] [CrossRef]
- Uhlig, S.; Gaudet, M.; Langa, S.; Schimmanz, K.; Conrad, H.; Kaiser, B.; Schenk, H. Electrostatically driven in-plane silicon micropump for modular configuration. Micromachines 2018, 9, 190. [Google Scholar] [CrossRef]
- Guo, S.; Nakamura, T.; Fukuda, T.; Oguro, K. Development of the micro pump using ICPF actuator. In Proceedings of the International Conference on Robotics and Automation, Albuquerque, NM, USA, 25 April 1997; Volume 1, pp. 266–271. [Google Scholar]
- Van de Pol FC, M.; Van Lintel HT, G.; Elwenspoek, M.; Fluitman JH, J. A thermopneumatic micropump based on micro-engineering techniques. Sens. Actuators A Phys. 1990, 21, 198–202. [Google Scholar] [CrossRef]
- Böhm, S.; Olthuis, W.; Bergveld, P. A plastic micropump constructed with conventional techniques and materials. Sens. Actuators A Phys. 1999, 77, 223–228. [Google Scholar] [CrossRef]
- Benard, W.L.; Kahn, H.; Heuer, A.H.; Huff, M.A. Thin-film shape-memory alloy actuated micropumps. J. Microelectromech. Syst. 1998, 7, 245–251. [Google Scholar] [CrossRef]
- Makino, E.; Mitsuya, T.; Shibata, T. Fabrication of TiNi shape memory micropump. Sens. Actuators A Phys. 2001, 88, 256–262. [Google Scholar] [CrossRef]
- Xu, D.; Wang, L.; Ding, G.; Zhou, Y.; Yu, A.; Cai, B. Characteristics and fabrication of NiTi/Si diaphragm micropump. Sens. Actuators A Phys. 2001, 93, 87–92. [Google Scholar] [CrossRef]
- Zhan, C.; Lo, T.; Liu, L.; Peihsin, T. A silicon membrane micropump with integrated bimetallic actuator. Chin. J. Electron. 1996, 5, 33. [Google Scholar]
- Renard, E. Continuous intraperitoneal insulin infusion from implantable pumps. In Technological Advances in the Treatment of Type 1 Diabetes; Karger Publishers: 2015; Volume 24, pp. 190–209.
- Renard, E. Implantable insulin delivery pumps. Minim. Invasive Ther. Allied Technol. 2004, 13, 328–335. [Google Scholar] [CrossRef] [PubMed]
- Bally, L.; Thabit, H.; Hovorka, R. Finding the right route for insulin delivery–an overview of implantable pump therapy. Expert Opin. Drug Deliv. 2017, 14, 1103–1111. [Google Scholar] [CrossRef] [PubMed]
- Sefton, M.V. Implantable pumps. Crit. Rev. Biomed. Eng. 1987, 14, 201–240. [Google Scholar]
- King, B.R.; Goss, P.W.; Paterson, M.A.; Crock, P.A.; Anderson, D.G. Changes in altitude cause unintended insulin delivery from insulin pumps: Mechanisms and implications. Diabetes Care 2011, 34, 1932–1933. [Google Scholar] [CrossRef]
- Richter, M.; Linnemann, R.; Woias, P. Robust design of gas and liquid micropumps. Sens. Actuators A Phys. 1998, 68, 480–486. [Google Scholar] [CrossRef]
- Chappel, E. Dry Test Methods for Micropumps. Appl. Sci. 2022, 12, 12258. [Google Scholar] [CrossRef]
- Chappel, E.; Allendes, R.; Bianchi, F.; Calcaterra, G.; Cannehan, F.; Conan, C.; Lefrique, J.; Lettieri, G.L.; Mefti, S.; Noth, A.; et al. Industrialized functional test for insulin micropumps. Procedia Eng. 2011, 25, 795–798. [Google Scholar] [CrossRef]
- Zengerle, R.; Richter, M. Simulation of microfluid systems. J. Micromech. Microeng. 1994, 4, 192. [Google Scholar] [CrossRef]
- Carmona, M.; Marco, S.; Samitier, J.; Morante, J.R. Dynamic simulations of micropumps. J. Micromech. Microeng. 1996, 6, 128. [Google Scholar] [CrossRef]
- Bourouina, T.; Grandchamp, J.P. Modeling micropumps with electrical equivalent networks. J. Micromech. Microeng. 1996, 6, 398. [Google Scholar] [CrossRef]
- Bourouina, T.; Bosseboeuf, A.; Grandchamp, J.P. Design and simulation of an electrostatic micropump for drug-delivery applications. J. Micromech. Microeng. 1997, 7, 186. [Google Scholar] [CrossRef]
- Morganti, E.; Fuduli, I.; Montefusco, A.; Petasecca, M.; U Pignatel, G. SPICE modelling and design optimization of micropumps. Int. J. Environ. Anal. Chem. 2005, 85, 687–698. [Google Scholar] [CrossRef]
- Hsu, Y.C.; Le, N.B. Equivalent electrical network for performance characterization of piezoelectric peristaltic micropump. Microfluid. Nanofluid. 2009, 7, 237–248. [Google Scholar] [CrossRef]
- Bardaweel, H.K. Understanding frequency response of thermal micropumps using electrical network analogy. Can. J. Phys. 2014, 92, 1178–1184. [Google Scholar] [CrossRef]
- Wang, X.Y.; Ma, Y.T.; Yan, G.Y.; Huang, D.; Feng, Z.H. High flow-rate piezoelectric micropump with two fixed ends polydimethylsiloxane valves and compressible spaces. Sens. Actuators A Phys. 2014, 218, 94–104. [Google Scholar] [CrossRef]
- Fournier, S.; Chappel, E. Dynamic simulations of a piezoelectric driven MEMS micropump. Procedia Eng. 2016, 168, 860–863. [Google Scholar] [CrossRef]
- Karmozdi, M.; Afshin, H.; Shafii, M.B. Electrical analogies applied on MMR micropump. Sens. Actuators A Phys. 2020, 301, 111675. [Google Scholar] [CrossRef]
- Cornaggia, L.; Conti, L.; Hannebelle, M.; Gamper, S.; Dumont-Fillon, D.; Van Lintel, H.; Renaud, P.; Chappel, E. Passive flow control valve for protein delivery. Cogent Eng. 2017, 4, 1413923. [Google Scholar] [CrossRef]
- Shah, R.K.; London, A.L. Laminar Flow Forced Convection in Ducts; Academic Press: New York, NY, USA, 1978. [Google Scholar]
- White, F.M. Viscous Fluid Flow, 2nd ed.; McGraw-Hill: New York, NY, USA, 1991. [Google Scholar]
- Bahrami, M.; Yovanovich, M.M.; Culham, J.R. Pressure drop of fully-developed, laminar flow in microchannels of arbitrary cross-section. In Proceedings of the International Conference on Nanochannels, Microchannels, and Minichannels, Toronto, ON, Canada, 13–15 June 2005; Volume 41855, pp. 269–280. [Google Scholar]
- Bruus, H. Theoretical Microfluidics; Oxford University Press: New York, NY, USA, 2007. [Google Scholar]
- Cottet, J.; Renaud, P. Introduction to microfluidics. In Drug Delivery Devices and Therapeutic Systems; Academic Press: New York, NY, USA, 2021; pp. 3–17. [Google Scholar]
- Young, W.C.; Budynas, R.G.; Sadegh, A.M. Roark’s Formulas for Stress and Strain; McGraw-Hill: New York, NY, USA, 2002; Volume 7, pp. 125–127. [Google Scholar]
- Resch, M.; Scheidl, R. A model for fluid stiction of quickly separating circular plates. Proc. Inst. Mech. Eng. Part C J. Mech. Eng. Sci. 2014, 228, 1540–1556. [Google Scholar] [CrossRef]
- Krogh, A.; Hemmingsen, A.M. The destructive action of heat on insulin solutions. Biochem. J. 1928, 22, 1231. [Google Scholar] [CrossRef] [PubMed]
- Brange, J.; Havelund, S. Insulin pumps and insulin quality—Requirements and problems. Acta Med. Scand. 1983, 213, 135–138. [Google Scholar] [CrossRef] [PubMed]
- Lougheed, W.D.; Woulfe-Flanagan, H.; Clement, J.R.; Albisser, A.M. Insulin aggregation in artificial delivery systems. Diabetologia 1980, 19, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Brange, J.; Andersen, L.; Laursen, E.D.; Meyn, G.; Rasmussen, E. Toward understanding insulin fibrillation. J. Pharm. Sci. 1997, 86, 517–525. [Google Scholar] [CrossRef] [PubMed]
- Das, A.; Shah, M.; Saraogi, I. Molecular aspects of insulin aggregation and various therapeutic interventions. ACS Bio Med Chem Au 2022, 2, 205–221. [Google Scholar] [CrossRef]
- Haas, J.; Vöhringer-Martinez, E.; Bögehold, A.; Matthes, D.; Hensen, U.; Pelah, A.; Abel, B.; Grubmüller, H. Primary steps of pH-dependent insulin aggregation kinetics are governed by conformational flexibility. ChemBioChem 2009, 10, 1816–1822. [Google Scholar] [CrossRef]
- Sluzky, V.; Tamada, J.A.; Klibanov, A.M.; Langer, R. Kinetics of insulin aggregation in aqueous solutions upon agitation in the presence of hydrophobic surfaces. Proc. Natl. Acad. Sci. USA 1991, 88, 9377–9381. [Google Scholar] [CrossRef]
- Sluzky, V.; Klibanov, A.M.; Langer, R. Mechanism of insulin aggregation and stabilization in agitated aqueous solutions. Biotechnol. Bioeng. 1992, 40, 895–903. [Google Scholar] [CrossRef]
- Vilasi, S.; Iannuzzi, C.; Portaccio, M.; Irace, G.; Sirangelo, I. Effect of trehalose on W7FW14F apomyoglobin and insulin fibrillization: New insight into inhibition activity. Biochemistry 2008, 47, 1789–1796. [Google Scholar] [CrossRef] [PubMed]
- Nault, L.; Guo, P.; Jain, B.; Bréchet, Y.; Bruckert, F.; Weidenhaupt, M. Human insulin adsorption kinetics, conformational changes and amyloidal aggregate formation on hydrophobic surfaces. Acta Biomater. 2013, 9, 5070–5079. [Google Scholar] [CrossRef]
- Buell, A.K.; Hung, P.; Salvatella, X.; Welland, M.E.; Dobson, C.M.; Knowles, T.P. Electrostatic effects in filamentous protein aggregation. Biophys. J. 2013, 104, 1116–1126. [Google Scholar] [CrossRef]
- Woods, R.J.; Alarcón, J.; McVey, E.; Pettis, R.J. Intrinsic fibrillation of fast-acting insulin analogs. J. Diabetes Sci. Technol. 2012, 6, 265–276. [Google Scholar] [CrossRef] [PubMed]
- Ryan, S.; Dudley, N.; Green, M.; Pruitt, C.; Jackman, G. Altered mental status at high altitude. Pediatrics 2018, 142, e20173973. [Google Scholar] [CrossRef]
- Dumont-Fillon, D.; Lamaison, D.; Chappel, E. Design and characterization of 3-stack MEMS-based passive flow regulators for implantable and ambulatory infusion pumps. J. Microelectromech. Syst. 2020, 29, 170–181. [Google Scholar] [CrossRef]
- Heinemann, L. Air Bubbles in Insulin Pumps: A Clinically Relevant Issue? J. Diabetes Sci. Technol. 2022, 16, 1351–1355. [Google Scholar] [CrossRef]
- Lindsley, W.G. Filter pore size and aerosol sample collection. In NIOSH Manual of Analytical Methods, 5th Edition. National Institute for Occupational Safety and Health (NIOSH): Atlanta, GA, USA, 2016.
- Maboudian, R.; Howe, R.T. Critical review: Adhesion in surface micromechanical structures. J. Vac. Sci. Technol. B Microelectron. Nanometer Struct. Process. Meas. Phenom. 1997, 15, 1–20. [Google Scholar] [CrossRef]
- Gennes, P.G.; Brochard-Wyart, F.; Quéré, D. Capillarity and Wetting Phenomena: Drops, Bubbles, Pearls, Waves; Springer: New York, NY, USA, 2004. [Google Scholar]
- Bhushan, B. Adhesion and stiction: Mechanisms, measurement techniques, and methods for reduction. J. Vac. Sci. Technol. B Microelectron. Nanometer Struct. Process. Meas. Phenom. 2003, 21, 2262–2296. [Google Scholar] [CrossRef]
- Wang, B.; Demuren, A.; Gyuricsko, E.; Hu, H. An experimental study of pulsed micro-flows pertinent to continuous subcutaneous insulin infusion therapy. Exp. Fluids 2011, 51, 65–74. [Google Scholar] [CrossRef]
- Leighton, T.G. The Rayleigh–Plesset equation in terms of volume with explicit shear losses. Ultrasonics 2008, 48, 85–90. [Google Scholar] [CrossRef]
- Fisher, J.C. The fracture of liquids. J. Appl. Phys. 1948, 19, 1062–1067. [Google Scholar] [CrossRef]
- Caupin, F.; Herbert, E. Cavitation in water: A review. C. R. Phys. 2006, 7, 1000–1017. [Google Scholar] [CrossRef]

| Mechanical and Fluidic Parameters | Electrical Equivalent Parameters | ||
|---|---|---|---|
| P | pressure | e | voltage |
| flow rate | i | current | |
| m is the mass | L | inductance | |
| is the friction coefficient | R | resistance | |
| k is the stiffness | C | capacitance | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chappel, E. Displacement Micropump with Check Valves for Diabetes Care—The Challenge of Pumping Insulin at Negative Pressure. Encyclopedia 2024, 4, 818-835. https://doi.org/10.3390/encyclopedia4020052
Chappel E. Displacement Micropump with Check Valves for Diabetes Care—The Challenge of Pumping Insulin at Negative Pressure. Encyclopedia. 2024; 4(2):818-835. https://doi.org/10.3390/encyclopedia4020052
Chicago/Turabian StyleChappel, Eric. 2024. "Displacement Micropump with Check Valves for Diabetes Care—The Challenge of Pumping Insulin at Negative Pressure" Encyclopedia 4, no. 2: 818-835. https://doi.org/10.3390/encyclopedia4020052
APA StyleChappel, E. (2024). Displacement Micropump with Check Valves for Diabetes Care—The Challenge of Pumping Insulin at Negative Pressure. Encyclopedia, 4(2), 818-835. https://doi.org/10.3390/encyclopedia4020052





