Pure yolk sac tumor (YST) is most commonly seen in infants and young children, accounting for 80% of all germ cell tumors in this age group [1]. Pure YST is rare in adults, constituting up to 2.4% of tumors, and is associated with a less favorable prognosis in adults than in children [2,3]. Here, we describe a rare case of pure YST of the testis in an adult with scrotal invasion.
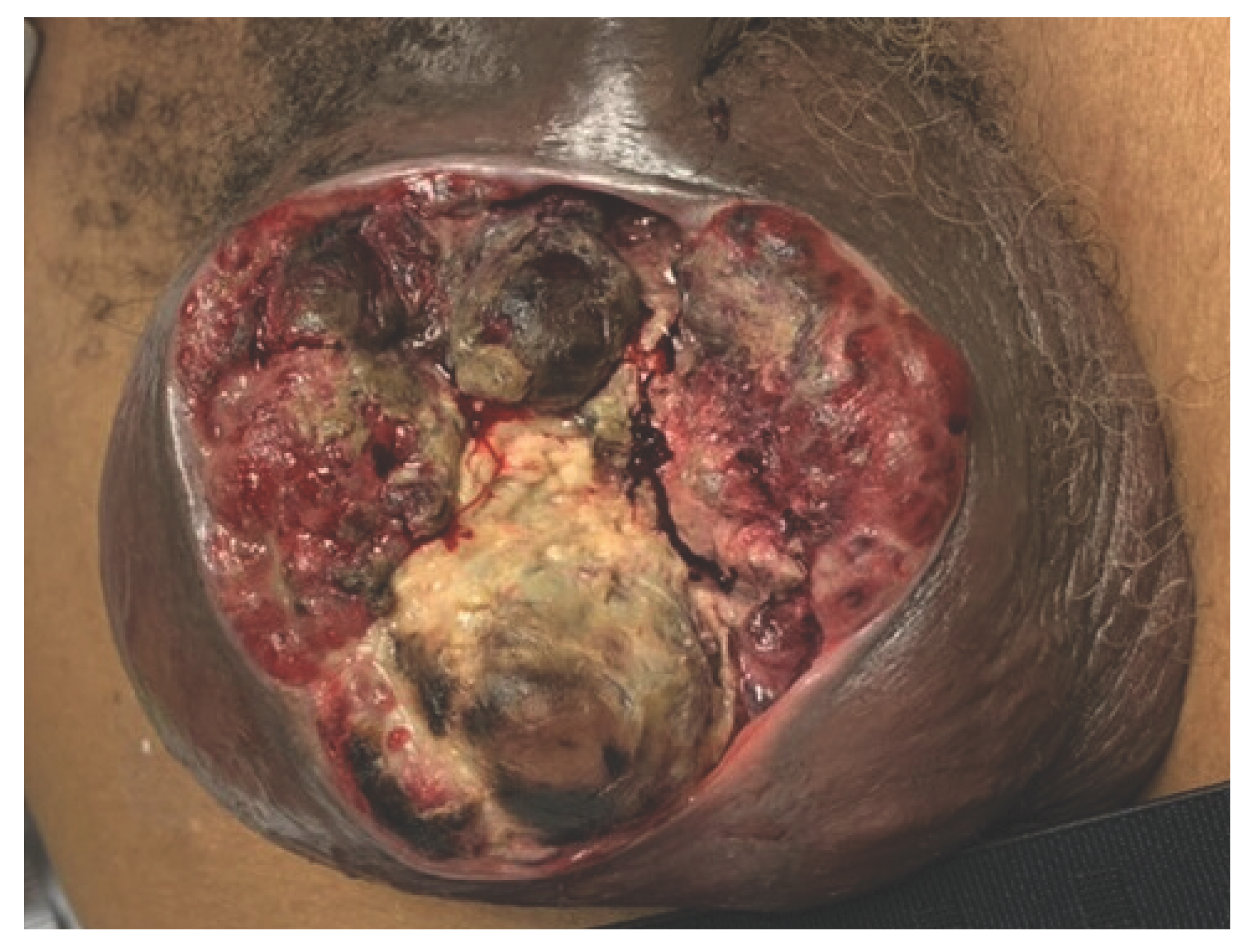
A 62-year-old male presented with a 3-month history of an enlarging scrotal mass. On examination, the patient was found to have a 10 cm to 12cm fungating and necrotic mass with superficial bleeding, ulceration, and breakdown of the overlying skin (Figure 1). Only the left testicle was palpable. Bilateral inguinal lymphadenopathy with mobile, firm, rubbery lymph nodes was noted. Given the lymphatic drainage networks of the scrotum, these may represent reactive adenopathy from infection or regional metastases [4].
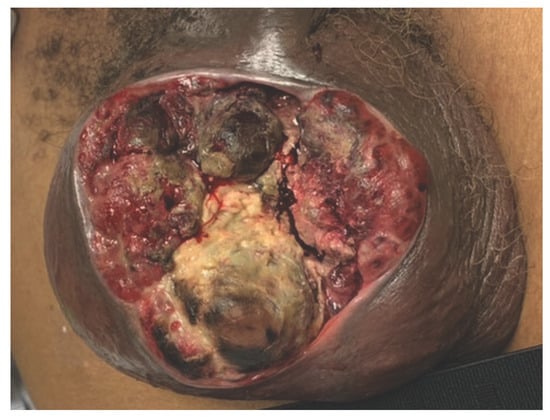
Figure 1.
Anterior view of the large fungating, ulcertative scrotal mass with breakdown of the overlying skin.
Serum tumor markers included AFP 17 418 ng/mL, β-hCG <0.06 IU/L, LDH 234 U/L. Contrast-CT was negative for lymphadenopathy of the chest, abdomen, and pelvis. No abdominal and pelvic visceral metastases were visualized. In the scrotum, there was a 10.9 cm heterogenous mass without demonstration of the right testicle. Radiologic lymphadenopathy of the bilateral inguinal regions was confirmed. The patient was taken to the operating room for biopsy, and surgical pathology demonstrated extensive necrosis and pure yolk sac pathology. Immunohistochemistry was positive for Sall4, Glypican-3, AFP, and CD117, and negative for OCT3/4 and CD30. Microscopic inspection revealed classic Schiller-Duval bodies.
The patient was initiated on neoadjuvant chemo- therapy with etoposide and cisplatin for 4 cycles. Bleomycin was withheld from the regimen because the patient had a long-standing smoking history. He tolerated the treatment protocol without significant adverse events.
On follow-up, the patient had experienced a reduction in the size of the scrotal mass and resolution of the inguinal lymphadenopathy, and he will be scheduled for surgical consolidation.
Conflicts of Interest
None declared.
References
- Leão, R.; Ahmad, A.E.; Hamilton, R.J. Testicular cancer biomarkers: A role for precision medicine in testicular cancer. Clin Genitourin Cancer. 2019, 17, e176–e183. [Google Scholar] [CrossRef] [PubMed]
- Khan, S.; Jetley, S.; Pujani, M.; Neogi, S. Pure yolk sac tumor of testis in an adult: A rare occurrence. J Postgrad Med. 2014, 60, 351–353. [Google Scholar] [PubMed]
- Pagaro, P.M.; Bedarshi, B. Pure yolk sac tumor of testis in a 50 years old: A rare case report. Med J DY Patil Univ. 2016, 9, 499–502. [Google Scholar] [CrossRef]
- O’Leary, C.G.; Allen, J.A.; O’Brien, F.; Tuthill, A.; Power, D.G. Scrotal involvement with testicular nonseminomatous germ cell tumour. Case Rep Oncol Med. 2016, 2016, 1–3. [Google Scholar] [CrossRef] [PubMed]
This is an open access article under the terms of a license that permits non-commercial use, provided the original work is properly cited. © 2021 The Authors. Société Internationale d'Urologie Journal, published by the Société Internationale d'Urologie, Canada.