Daytime Sleepiness and Quality of Life in Obstructive Sleep Apnoea Patients before and after Long-Term Mandibular Advancement Device Treatment
Abstract
1. Introduction
2. Materials and Methods
2.1. Subjects
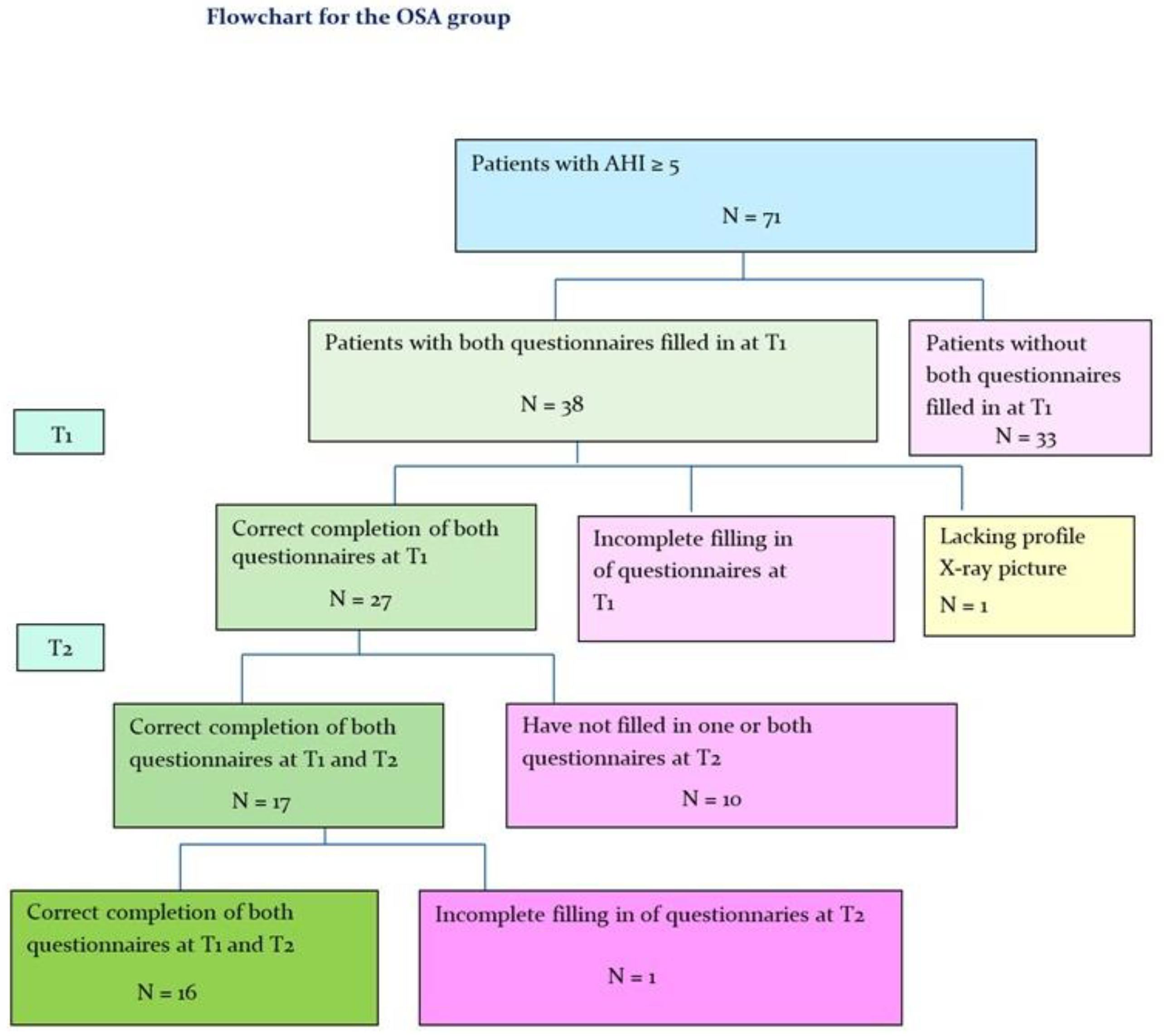
2.1.1. OSA Patients
- AHI > 5
- Minimum of 20 teeth, including the two first lower molars
- Bone loss <50%
- Evenly distributed teeth in occlusal contact
- Filled-in Epworth questionnaire on daytime sleepiness and SF-36 questionnaire on quality of life at treatment start
- Lateral cephalograms at treatment start
- AHI < 5
- Severe somatic and/or mental disease
- Severe cardiovascular disease
- Chronic pronounced nasal stenosis
- Hypertrophic tonsils
- Symptoms from TMJ and/or masticatory muscles that required treatment before MAD-treatment
- Open bite malocclusion
- Angle class 2 div.2
- Severe craniofacial deformities
- Facial wear of lower incisors
- Jaw protrusion <6 mm
- Insufficiently filled-in questionnaires
- Missing lateral cephalograms
2.1.2. Control Group
- Employed between June 2015 and April 2016
- No known OSA
- Neutral or minor malocclusion traits that did not require orthodontic treatment
- Known OSA
- Severe malocclusion traits or craniofacial anomalies
2.2. Methods
2.2.1. Daytime Sleepiness
2.2.2. Quality of Life
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Løvschall, C.; Søbjerg, L.M.; Nørregaard, O.; Prætorius, C.; Hilberg, O.; Jennum, P.; Tipsmark, L.S.; Pedersen, T.V.; Nielsen, C.P. Medicinsk Teknologi Vurdering af Obstruktiv Søvnapnø [Technological Medical Assessment of Obstructive Sleep Apnoea]; CFK-Folkesundhed og Kvalitetsudvikling, Region Midtjylland: Aarhus, Denmark, 2013. [Google Scholar]
- Guilleminault, C.; Tilkian, A.; Dement, W.C. The Sleep Apnea Syndromes. Annu. Rev. Med. 1976, 27, 465–484. [Google Scholar] [CrossRef] [PubMed]
- Balachandran, J.S.; Patel, S.R.; Cotton, D.; Rao, J.K.; Taichman, D.; Williams, S. In the Clinic: Obstructive Sleep Apnea. Ann. Intern. Med. 2014, 161, ITC5-1. [Google Scholar] [CrossRef] [PubMed]
- Jordan, A.S.; McSharry, D.G.; Malhotra, A. Adult obstructive sleep apnoea. Lancet 2014, 383, 736–747. [Google Scholar] [CrossRef]
- Johns, M.W. Daytime Sleepiness, Snoring, and Obstructive Sleep Apnea: The Epworth Sleepiness Scale. Chest 1993, 103, 30–36. [Google Scholar] [CrossRef]
- Gottlieb, D.J.; Whitney, C.W.; Bonekat, W.H.; Iber, C.; James, G.D.; Lebowitz, M.; Nieto, J.; Rosenberg, C.E. Relation of Sleepiness to Respiratory Disturbance Index: The Sleep Heart Health Study. Am. J. Respir. Crit. Care Med. 1999, 159, 502–507. [Google Scholar] [CrossRef] [PubMed]
- Ohayon, M.M. Determining the level of sleepiness in the American population and its correlates. J. Psychiatr. Res. 2012, 46, 422–427. [Google Scholar] [CrossRef] [PubMed]
- Sunitha, C.; Aravindkumar, S. Obstructive sleep apnea: Clinical and diagnostic features. Ind. J. Dent Res. 2009, 20, 487–491. [Google Scholar] [CrossRef]
- Gonzaga, C.; Bertolami, A.; Bertolami, M.; Amodeo, C.; Calhoun, D. Obstructive sleep apnea, hypertension and cardiovascular diseases. J. Hum. Hypertens. 2015, 29, 705–712. [Google Scholar] [CrossRef]
- Tahrani, A.A.; Ali, A.; Raymond, N.T.; Begum, S.; Dubb, K.; Altaf, Q.A.; Piya, M.K.; Barnett, A.H.; Stevens, M.J. Obstructive Sleep Apnea and Diabetic Nephropathy: A cohort study. Diabetes Care 2013, 36, 3718–3725. [Google Scholar] [CrossRef]
- Jennum, P.; Kjellberg, J. Health, social and economical consequences of sleep-disordered breathing: A controlled national study. Thorax 2011, 66, 560–566. [Google Scholar] [CrossRef]
- Ward, K.L.; Hillman, D.R.; James, A.; Bremner, A.P.; Simpson, L.; Cooper, M.N.; Palmer, L.J.; Fedson, A.C.; Mukherjee, S. Excessive Daytime Sleepiness Increases the Risk of Motor Vehicle Crash in Obstructive Sleep Apnea. J. Clin. Sleep Med. 2013, 9, 1013–1021. [Google Scholar] [CrossRef] [PubMed]
- Hirsch Allen, M.A.J.; Bansback, N.; Ayas, N.T. The Effect of OSA on Work Disability and Work-Related Injuries. Chest 2015, 147, 1422–1428. [Google Scholar] [CrossRef] [PubMed]
- Gall, R.; Isaac, L.; Kryger, M. Quality of Life in Mild Obstructive Sleep Apnea. Sleep 1993, 16, S59–S61. [Google Scholar] [CrossRef] [PubMed]
- Moyer, C.A.; Sonnad, S.S.; Garetz, S.L.; Helman, J.I.; Chervin, R.D. Quality of life in obstructive sleep apnea: A systematic review of the literature. Sleep Med. 2001, 2, 477–491. [Google Scholar] [CrossRef] [PubMed]
- Yang, E.H.; Hla, K.M.; McHorney, C.A.; Havighurst, T.; Badr, M.S.; Weber, S. Sleep apnea and quality of life. Sleep 2000, 23, 535–541. [Google Scholar] [CrossRef] [PubMed]
- Shapiro, G.K.; Shapiro, C.M. Factors that influence CPAP adherence: An overview. Sleep Breath 2010, 14, 323–335. [Google Scholar] [CrossRef] [PubMed]
- Hoffstein, V. Review of oral appliances for treatment of sleep-disordered breathing. Sleep Breath 2007, 11, 1–22. [Google Scholar] [CrossRef]
- Petri, N.; Svanholt, P.; Solow, B.; Wildschiødtz, G.; Winkel, P. Mandibular advancement appliance for obstructive sleep apnoea: Results of a randomised placebo controlled trial using parallel group design. J. Sleep Res. 2008, 17, 221–229. [Google Scholar] [CrossRef]
- Levrini, L.; Sacchi, F.; Milano, F.; Polimeni, A.; Cozza, P.; Bernkopf, E.; Segù, M.; Zucconi, M.; Vicini, C.; Brunello, E.; et al. Italian recommendations on dental support in the treatment of adult obstructive sleep apnea syndrome (OSAS). Ann. Stomatol. 2016, 6, 81–86. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Knappe, S.W.; Sonnesen, L. Mandibular positioning techniques to improve sleep quality in patients with obstructive sleep apnea: Current perspectives. Nat. Sci. Sleep 2018, 10, 65–72. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Petri, N.; Christensen, I.J.; Svanholt, P.; Sonnesen, L.; Wildschiødtz, G.; Berg, S. Mandibular advancement device therapy for obstructive sleep apnea: A prospective study on predictors of treatment success. Sleep Med. 2019, 12, 187–194. [Google Scholar] [CrossRef] [PubMed]
- Knappe, S.W.; Bakke, M.; Svanholt, P.; Petersson, A.; Sonnesen, L. Long-term side effects on the temporomandibular joints and oro-facial function in patients with obstructive sleep apnoea treated with a mandibular advancement device. J. Oral. Rehabil. 2017, 44, 354–362. [Google Scholar] [CrossRef] [PubMed]
- Svanholt, P.; Petri, N.; Wildschiødtz, G.; Sonnesen, L. Influence of craniofacial and upper spine morphology on mandibular advancement treatment in patients with sleep apnoea: A pilot study. Eur. J. Orthod. 2015, 37, 391–397. [Google Scholar] [CrossRef]
- Epstein, L.J.; Kristo, D.; Strollo, P.J., Jr.; Friedmann, N.; Malhotra, A.; Patil, S.P.; Ramar, K.; Rogers, R.; Schwab, R.J.; Weaver, E.M.; et al. Clinical guideline for the evaluation, management and long-term care of obstructive sleep apnea in adults. J. Clin. Sleep Med. 2009, 5, 263–276. [Google Scholar] [CrossRef] [PubMed]
- Sharples, L.D.; Clutterbuck-James, A.L.; Glover, M.J.; Bennett, M.S.; Chadwick, R.; Pittman, M.A.; Quinnell, T.G. Meta-analysis of andomized controlled trials of oral mandibular advancement devices and continuous positive airway pressure for obstructive sleep apnoea-hypopnoea. Sleep Med. Rev. 2016, 27, 108–124. [Google Scholar] [CrossRef]
- Sutherland, K.; Cistulli, P. Mandibular advancement splints for the treatment of sleep apnea syndrome. Swiss Med. Wkly 2011, 141, w13276. [Google Scholar] [CrossRef]
- Ramar, K.; Dort, L.C.; Katz, S.G.; Lettieri, C.J.; Harrod, C.G.; Thomas, S.M.; Chervin, R.D. Clinical Practice Guideline for the Treatment of Obstructive Sleep Apnea and Snoring with Oral Appliance Therapy: An Update for 2015. J. Clin. Sleep Med. 2015, 11, 773–827. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Fagundes, N.C.; Minervini, G.; Alonso, B.F.; Nucci, L.; Grassia, V.; d’Apuzzo, F.; Puigdollers, A.; Perillo, L.; Flores-Mir, C. Patient-reported outcomes while managing obstructive sleep apnea with oral appliances: A scoping review. J. Evid Base Dent Pract. 2022, 101786. [Google Scholar] [CrossRef]
- Gotsopoulos, H.; Chen, C.; Qian, J.; Cistulli, P.A. Oral appliance therapy improves symptoms in obstructive sleep apnea: A randomized, controlled trial. Am. J. Respir. Crit. Care Med. 2002, 166, 743–748. [Google Scholar] [CrossRef]
- Serra-Torres, S.; Bellot-Arcís, C.; Montiel-Company, J.M.; Marco-Algarra, J.; Almerich-Silla, J.M. Effectiveness of Mandibular Advancement Appliances in Treating Obstructive Sleep Apnea Syndrome: A Systematic Review. Laryngoscope 2016, 126, 507–514. [Google Scholar] [CrossRef]
- Ghazal, A.; Sorichter, S.; Jonas, I.; Rose, E.C. A randomized prospective long-term study of two oral appliances for sleep apnoea treatment. J. Sleep Res. 2009, 18, 321–328. [Google Scholar] [CrossRef] [PubMed]
- Johns, M.W. A New Method for Measuring Daytime Sleepiness: The Epworth Sleepiness Scale. Sleep 1991, 14, 540–545. [Google Scholar] [CrossRef] [PubMed]
- Jenkinson, C. The SF-36 physical and mental health summary measures: An example of how to interpret scores. J. Health Serv. Res. Policy 1998, 3, 92–96. [Google Scholar] [CrossRef]
- Bjorner, J.B.; Thunedborg, K.; Kristensen, T.S.; Modvig, J.; Bech, P. The Danish SF-36 Health Survey: Translation and preliminary validity studies. J. Clin. Epidemiol. 1998, 51, 991–999. [Google Scholar] [CrossRef] [PubMed]
- Sleep-Related Breathing Disorders in Adults: Recommendations for Syndrome Definition and Measurement Techniques in Clinical Research. The Report of an American Academy of Sleep Medicine Task Force. Sleep 1999, 22, 667–689. Available online: https://pubmed.ncbi.nlm.nih.gov/10450601/ (accessed on 14 October 2022).
- Fietze, I.; Laharnar, N.; Obst, A.; Ewert, R.; Felix, S.B.; Garcia, C.; Gläser, S.; Glos, M.; Schmidt, C.O.; Stubbe, B.; et al. Prevalence and association analysis of obstructive sleep apnea with gender and age differences—Results of SHIP-Trend. J. Sleep Res. 2019, 28, e12770. [Google Scholar] [CrossRef] [PubMed]
- Bjørner, J.B.; Damsgaard, M.T.; Watt, T.; Bech, P.; Rasmussen, N.K.; Kristensen, T.S.; Modvig, J.; Thunedborg, K. Dansk Manual til SF-36: Et Spørgeskema om Helbredsstatus [Danish Manual for SF-36: A Questionnaire about Health Status]; Lægemiddelindustriforeningen: Copenhagen, Denmark, 1997. [Google Scholar]
- Smith, I.E.; Shneerson, J.M. Is the SF 36 sensitive to sleep disruption? A study in subjects with sleep apnoea. J. Sleep Res. 1995, 4, 183–188. [Google Scholar] [CrossRef]
- Sil, A.; Barr, G. Assessment of predictive ability of Epworth scoring in screening of patients with sleep apnoea. J. Laryngol. Otol. 2012, 126, 372–379. [Google Scholar] [CrossRef]
- Colt, H.G.; Haas, H.; Rich, G.B. Hypoxemia vs sleep fragmentation as cause of excessive daytime sleepiness in obstructive sleep apnea. Chest 1991, 100, 1542–1548. [Google Scholar] [CrossRef]
- Punjabi, N.M.; Bandeen-Roche, K.; Marx, J.J.; Neubauer, D.N.; Smith, P.L.; Schwartz, A.R. The association between daytime sleepiness and sleep-disordered breathing in NREM and REM sleep. Sleep 2002, 25, 307–314. Available online: https://pubmed.ncbi.nlm.nih.gov/12003161/ (accessed on 14 October 2022).
- Baldwin, C.M.; Griffith, K.A.; Nieto, F.J.; O’Connor, G.T.; Walsleben, J.A.; Redline, S. The Association of Sleep-Disordered Breathing and Sleep Symptoms with Quality of Life in the Sleep Heart Health Study. Sleep 2001, 24, 96–105. [Google Scholar] [CrossRef]
- Bulcun, E.; Ekici, A.; Ekici, M. Quality of life and metabolic disorders in patients with obstructive sleep apnea. Clin. Investig. Med. 2012, 35, E105–E113. [Google Scholar] [CrossRef] [PubMed]
- Sampaio, R.; Pereira, M.G.; Winck, J.C. Psychological morbidity, illness representations, and quality of life in female and male patients with obstructive sleep apnea syndrome. Psychol. Health Med. 2012, 17, 136–149. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Blanco, J.; Zamarrón, C.; Abeleira Pazos, M.T.; Lamela, C.; Suarez Quintanilla, D. Prospective evaluation of an oral appliance in the treatment of obstructive sleep apnea syndrome. Sleep Breath 2005, 9, 20–25. [Google Scholar] [CrossRef]
- Marklund, M.; Carlberg, B.; Forsgren, L.; Olsson, T.; Stenlund, H.; Franklin, K.A. Oral Appliance Therapy in Patients With Daytime Sleepiness and Snoring or Mild to Moderate Sleep Apnea: A Randomized Clinical Trial. JAMA Intern. Med. 2015, 175, 1278–1285. [Google Scholar] [CrossRef] [PubMed]
- Barnes, M.; McEvoy, R.D.; Banks, S.; Tarquinio, N.; Murray, C.G.; Vowles, N.; Pierce, R.J. Efficacy of Positive Airway Pressure and Oral Appliance in Mild to Moderate Obstructive Sleep Apnea. Am. J. Respir. Crit. Care Med. 2004, 170, 656–664. [Google Scholar] [CrossRef] [PubMed]
- Engleman, H.M.; McDonald, J.P.; Graham, D.; Lello, G.E.; Kingshott, R.N.; Coleman, E.L.; Mackey, T.W.; Douglas, N.J. Randomized Crossover Trial of Two Treatments for Sleep Apnea/Hypopnea Syndrome: Continuous Positive Airway Pressure and Mandibular Repositioning Splint. Am. J. Respir. Crit. Care Med. 2002, 166, 855–859. [Google Scholar] [CrossRef] [PubMed]

| Variables | Difference OSA vs. Control (95% Confidence Interval) | r2 (Coefficient of Determination) | p-Value |
|---|---|---|---|
| Daytime sleepiness | |||
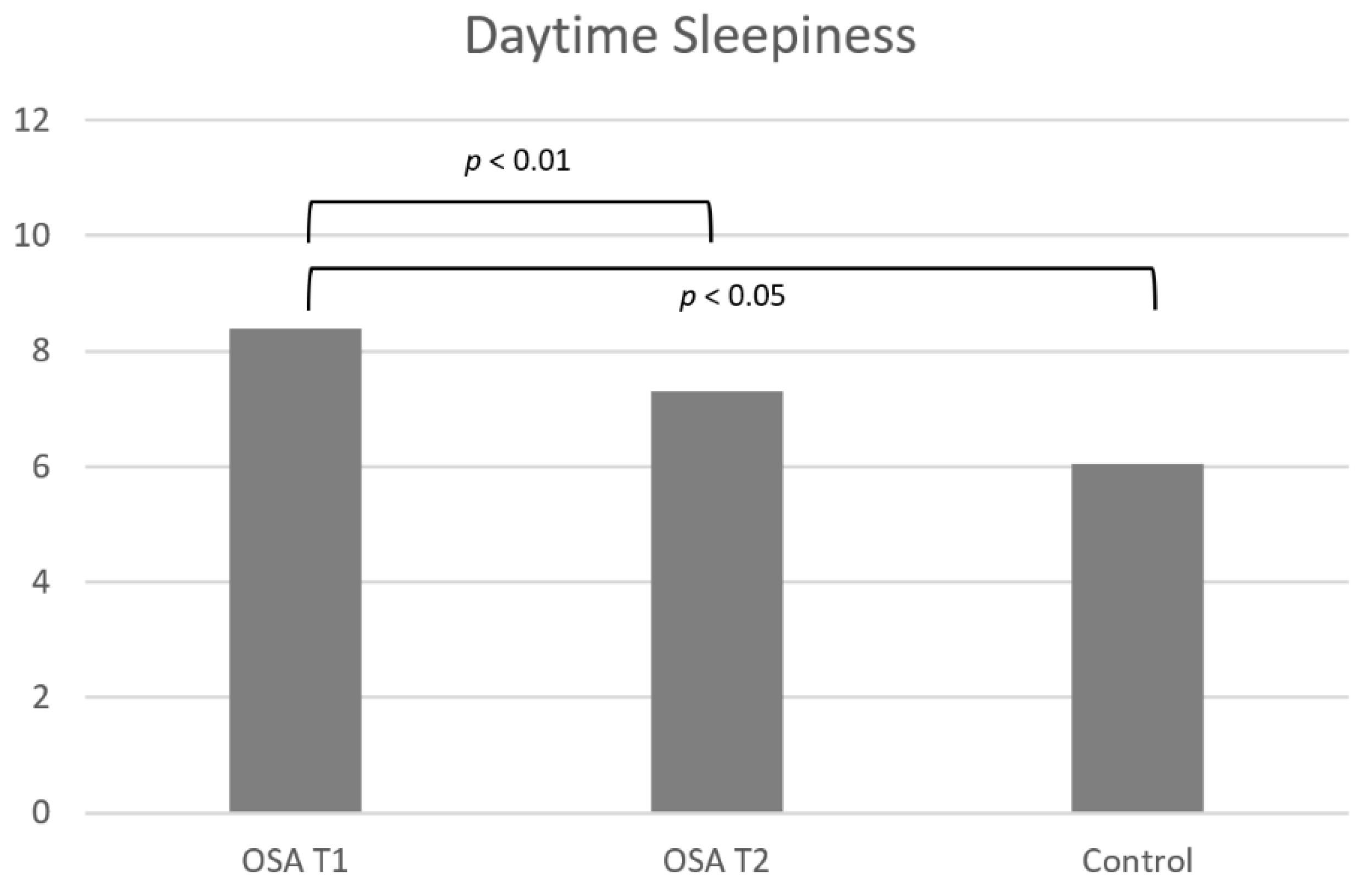
| ESS | 2.36 (0.56−4.15) | 0.16 | 0.0110 * |
| Quality of life | |||
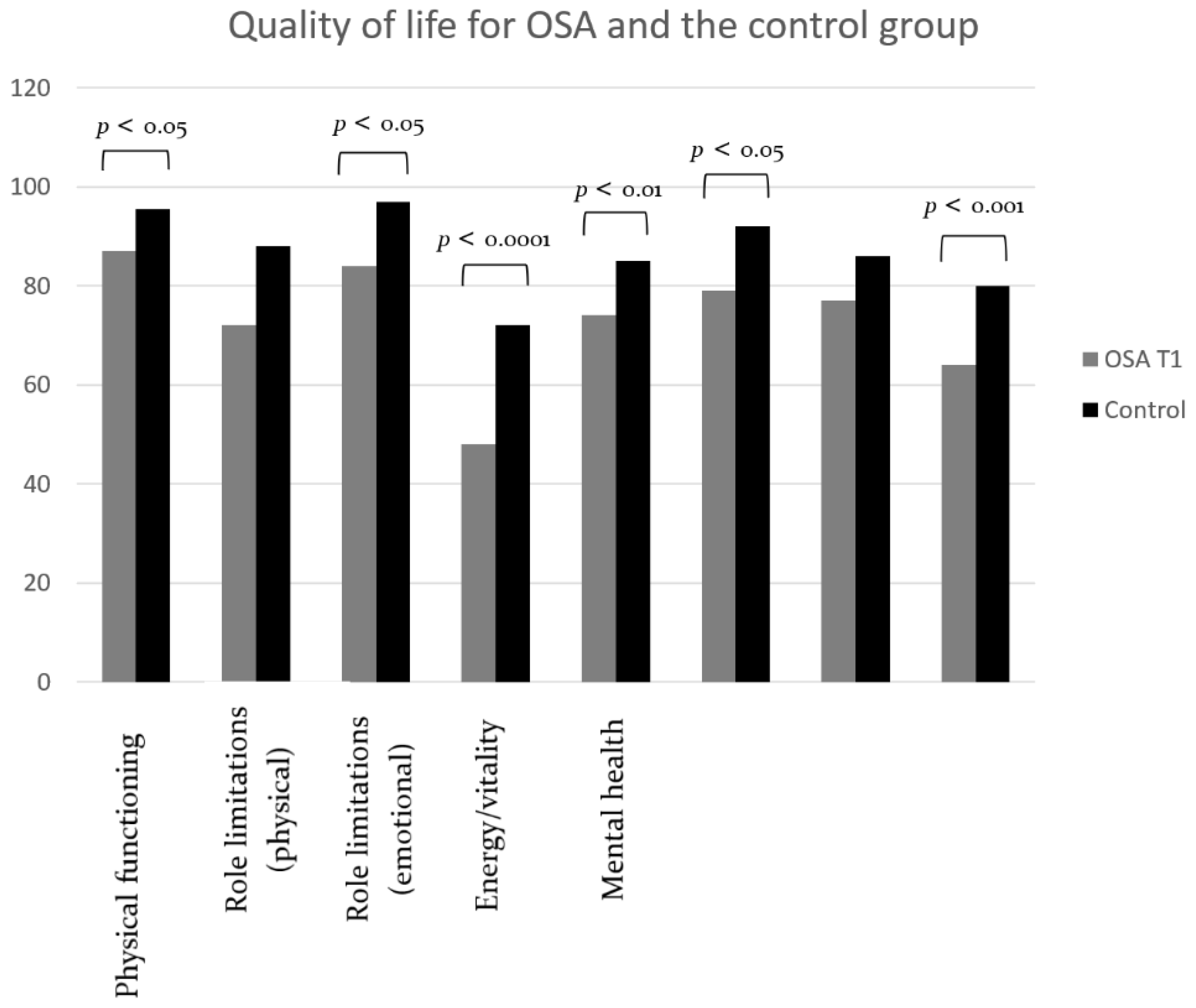
| Physical functioning | −7.67 (−14.23–(−1.12)) | 0.10 | 0.0226 * |
| Role limitations (physical) | −16.32 (33.58–0.94) | 0.06 | 0.06 |
| Role limitations (emotional) | −14.57 (−26.46–(−2.68)) | 0.13 | 0.0173 * |
| Energy/vitality | −24.51 (−34.44–(−14.58)) | 0.33 | <0.0001 **** |
| Mental health | −11.72 (−19.31–(−4.13)) | 0.22 | 0.0031 ** |
| Social functioning | −13.72 (−24.28–(−3.15)) | 0.19 | 0.0119 * |
| Pain | −8.08 (−20.12–3.96) | 0.04 | 0.18 |
| General health perceptions | −16.29 (−24.54–(−8.04)) | 0.25 | 0.0002 *** |
| Variables | Difference T2 vs. T1 (95% Confidence Interval) | r (Correlation Coefficient) | p-Value |
|---|---|---|---|
| Daytime sleepiness | |||
| ESS | −2.25 (−3.52−(−0.98)) | 0.85 | 0.0018 * |
| Quality of life | |||
| Physical functioning | −2.19 (−6.75–2.37) | 0.84 | 0.32 |
| Role limitations (physical) | 7.81 (−11.47–27.10) | 0.56 | 0.40 |
| Role limitations (emotional) | 6.26 (−11.17–23.69) | 0.56 | 0.46 |
| Energy/vitality | 18.13 (6.87–28.38) | 0.47 | 0.0037 * |
| Mental health | 4.75 (−7.97–17.47) | 0.04 | 0.44 |
| Social functioning | 10.84 (−0.17–22.05) | 0.54 | 0.05 |
| Pain | 7.50 (−7.27–22.27) | 0.30 | 0.30 |
| General health perceptions | 4.38 (−1.45–10.20) | 0.85 | 0.13 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Halfeld, S.; Sonnesen, L. Daytime Sleepiness and Quality of Life in Obstructive Sleep Apnoea Patients before and after Long-Term Mandibular Advancement Device Treatment. Dent. J. 2022, 10, 226. https://doi.org/10.3390/dj10120226
Halfeld S, Sonnesen L. Daytime Sleepiness and Quality of Life in Obstructive Sleep Apnoea Patients before and after Long-Term Mandibular Advancement Device Treatment. Dentistry Journal. 2022; 10(12):226. https://doi.org/10.3390/dj10120226
Chicago/Turabian StyleHalfeld, Signe, and Liselotte Sonnesen. 2022. "Daytime Sleepiness and Quality of Life in Obstructive Sleep Apnoea Patients before and after Long-Term Mandibular Advancement Device Treatment" Dentistry Journal 10, no. 12: 226. https://doi.org/10.3390/dj10120226
APA StyleHalfeld, S., & Sonnesen, L. (2022). Daytime Sleepiness and Quality of Life in Obstructive Sleep Apnoea Patients before and after Long-Term Mandibular Advancement Device Treatment. Dentistry Journal, 10(12), 226. https://doi.org/10.3390/dj10120226












