Association between Experiences in Life and Quality of Life among Lebanese University Students in a Collapsing Country: The Moderating Role of Religious Coping and Positivity
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Minimal Sample Size Calculation
2.3. Questionnaire
2.3.1. The 12-Item Short Form Health Survey (SF-12)
2.3.2. Positivity Scale
2.3.3. The Brief Religious Coping Methods Scale (Brief RCOPE Scale)
2.3.4. Scale of Positive and Negative Experience
2.4. Statistical Analysis
3. Results
3.1. Sociodemographic and Other Characteristics of the Participants
3.2. Bivariate Analysis
3.3. Multivariable Analysis
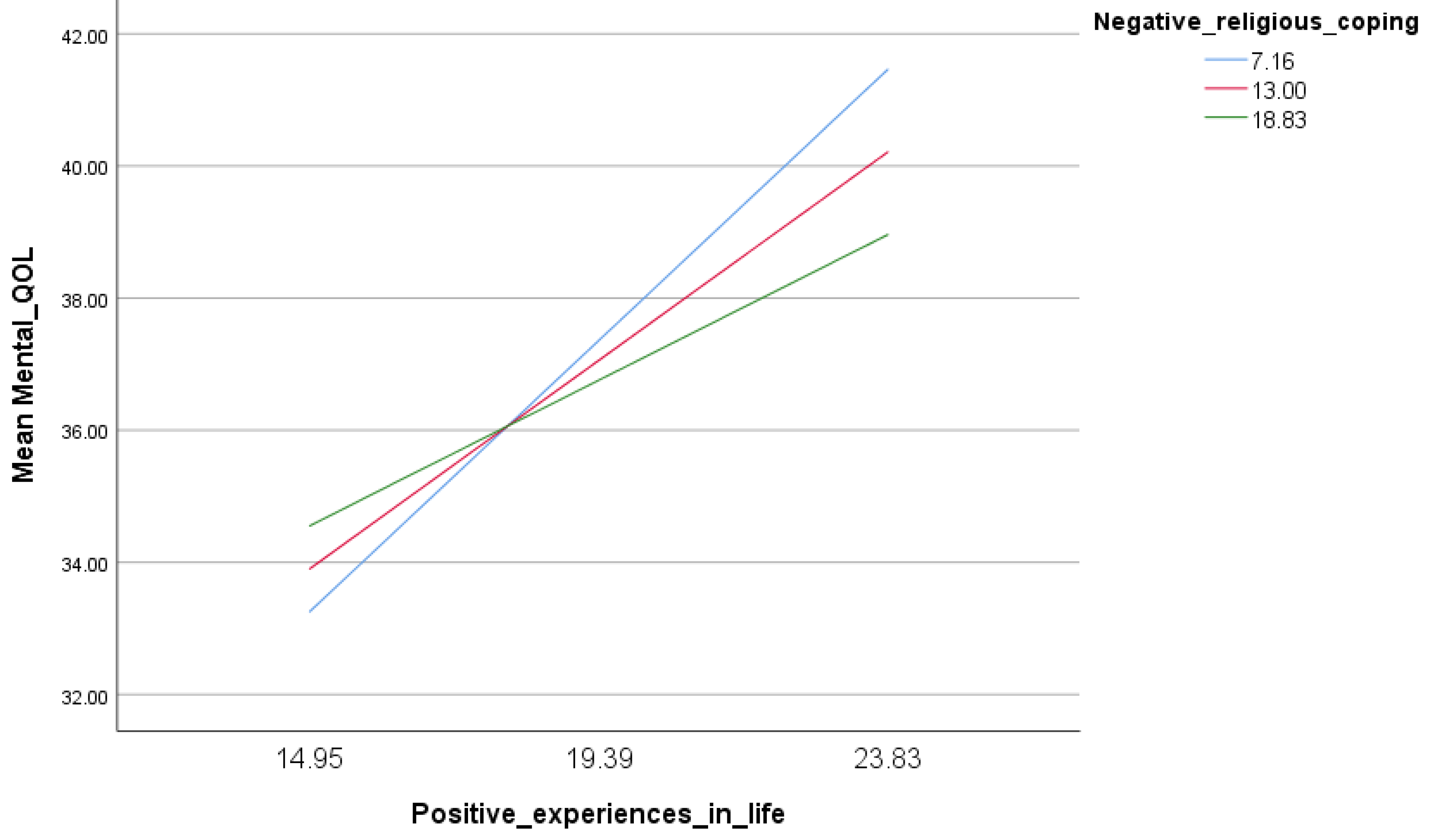
3.4. Moderation Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cella, D.F. Quality of life: Concepts and definition. J. Pain Symptom Manag. 1994, 9, 186–192. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. WHOQOL: Measuring Quality of Life. Available online: https://www.who.int/tools/whoqol#:~:text=WHO%20defines%20Quality%20of%20Life,%2C%20expectations%2C%20standards%20and%20concerns (accessed on 17 December 2021).
- Theofilou, P. Quality of life: Definition and measurement. Eur. J. Psychol. 2013, 9, 150–162. [Google Scholar] [CrossRef]
- Bossola, M.; Murri, R.; Onder, G.; Turriziani, A.; Fantoni, M.; Padua, L. Physicians’ knowledge of health-related quality of life and perception of its importance in daily clinical practice. Health Qual. Life Outcomes 2010, 8, 43. [Google Scholar] [CrossRef] [PubMed]
- Lange, S.; Zschocke, I.; Seidenglanz, K.; Schiffler, A.; Zöllinger, A.; Amon, U.; Augustin, M. Predictors of the quality of life in patients with atopic dermatitis. Dermatol. Psychosom. Dermatol. Psychosom. 2000, 1, 66–70. [Google Scholar] [CrossRef]
- Wanic, R.; Kulik, J. Toward an understanding of gender differences in the impact of marital conflict on health. Sex Roles 2011, 65, 297–312. [Google Scholar] [CrossRef]
- Song, Y.-S. Stressful life events and quality of life in nursing students. J. Korean Acad. Soc. Nurs. Educ. 2012, 18, 71–80. [Google Scholar] [CrossRef]
- Rubenstein, L.M.; Freed, R.D.; Shapero, B.G.; Fauber, R.L.; Alloy, L.B. Cognitive attributions in depression: Bridging the gap between research and clinical practice. J. Psychother. Integr. 2016, 26, 103–115. [Google Scholar] [CrossRef]
- Golden-Kreutz, D.M.; Thornton, L.M.; Wells-Di Gregorio, S.; Frierson, G.M.; Jim, H.S.; Carpenter, K.M.; Shelby, R.A.; Andersen, B.L. Traumatic stress, perceived global stress, and life events: Prospectively predicting quality of life in breast cancer patients. Health Psychol. 2005, 24, 288–296. [Google Scholar] [CrossRef]
- Cummings, J.P.; Pargament, K.I. Medicine for the spirit: Religious coping in individuals with medical conditions. Religions 2010, 1, 28–53. [Google Scholar] [CrossRef]
- Bjorck, J.P.; Thurman, J.W. Negative life events, patterns of positive and negative religious coping, and psychological functioning. J. Sci. Study Relig. 2007, 46, 159–167. [Google Scholar] [CrossRef]
- Pargament, K.I.; Smith, B.W.; Koenig, H.G.; Perez, L. Patterns of positive and negative religious coping with major life stressors. J. Sci. Study Relig. 1998, 37, 710–724. [Google Scholar] [CrossRef]
- Abu, H.O.; Ulbricht, C.; Ding, E.; Allison, J.J.; Salmoirago-Blotcher, E.; Goldberg, R.J.; Kiefe, C.I. Association of religiosity and spirituality with quality of life in patients with cardiovascular disease: A systematic review. Qual. Life Res. 2018, 27, 2777–2797. [Google Scholar] [CrossRef] [PubMed]
- Mosqueiro, B.P.; da Rocha, N.S.; Fleck, M.P. Intrinsic religiosity, resilience, quality of life, and suicide risk in depressed inpatients. J. Affect. Disord. 2015, 179, 128–133. [Google Scholar] [CrossRef] [PubMed]
- Saffari, M.; Pakpour, A.H.; Naderi, M.K.; Koenig, H.G.; Baldacchino, D.R.; Piper, C.N. Spiritual coping, religiosity and quality of life: A study on Muslim patients undergoing haemodialysis. Nephrology 2013, 18, 269–275. [Google Scholar] [CrossRef] [PubMed]
- Zargani, A.; Nasiri, M.; Hekmat, K.; Abbaspour, Z.; Vahabi, S. A Survey on the Relationship between Religiosity and Quality of Life in Patients with Breast Cancer: A Study in Iranian Muslims. Asia Pac. J. Oncol. Nurs. 2018, 5, 217–222. [Google Scholar] [CrossRef] [PubMed]
- Abdel-Khalek, A.M. Quality of life, subjective well-being, and religiosity in Muslim college students. Qual. Life Res. 2010, 19, 1133–1143. [Google Scholar] [CrossRef]
- Frisch, M.B. Evidence-based well-being/positive psychology assessment and intervention with quality of life therapy and coaching and the Quality of Life Inventory (QOLI). Soc. Indic. Res. 2013, 114, 193–227. [Google Scholar] [CrossRef]
- Fredrickson, B.L.; Tugade, M.M.; Waugh, C.E.; Larkin, G.R. What good are positive emotions in crisis? A prospective study of resilience and emotions following the terrorist attacks on the United States on September 11th, 2001. J. Personal. Soc. Psychol. 2003, 84, 365–376. [Google Scholar] [CrossRef]
- Diener, E.; Napa-Scollon, C.K.; Oishi, S.; Dzokoto, V.; Suh, E.M. Positivity and the construction of life satisfaction judgments: Global happiness is not the sum of its parts. J. Happiness Stud. 2000, 1, 159–176. [Google Scholar] [CrossRef]
- Datu JA, D.; King, R.B. Prioritizing positivity optimizes positive emotions and life satisfaction: A three-wave longitudinal study. Personal. Individ. Differ. 2016, 96, 111–114. [Google Scholar] [CrossRef]
- Hashim, H.T.; Uakkas, S.; Reda, A.; Ramadhan, M.A.; Al Mostafa, M.Y. Beirut Explosion Effects on COVID-19 Situation in Lebanon. Disaster Med. Public Health Prep. 2021, 16, 1703–1704. [Google Scholar] [CrossRef] [PubMed]
- Fares, K.; Haddad, C.; Malaeb, D.; Sacre, H.; Akel, M.; Salameh, P.; Obeid, S.; Hallit, S. Social Anxiety and Its Correlates Among Lebanese Adults: Role of Self-Esteem, Depression, Alcohol Use Disorder, Alexithymia, and Work Fatigue. Prim. Care Companion CNS Disord. 2022, 24, 39101. [Google Scholar] [CrossRef] [PubMed]
- Zakhour, M.; Haddad, C.; Sacre, H.; Fares, K.; Akel, M.; Obeid, S.; Salameh, P.; Hallit, S. Suicidal ideation among Lebanese adults: Scale validation and correlates. BMC Psychiatry 2021, 21, 100. [Google Scholar] [CrossRef] [PubMed]
- El Othman, R.; Touma, E.; El Othman, R.; Haddad, C.; Hallit, R.; Obeid, S.; Salameh, P.; Hallit, S. COVID-19 pandemic and mental health in Lebanon: A cross-sectional study. Int. J. Psychiatry Clin. Pract. 2021, 25, 152–163. [Google Scholar] [CrossRef]
- Rayan, A.; Fawaz, M. Cultural misconceptions and public stigma against mental illness among Lebanese university students. Perspect. Psychiatr. Care 2018, 54, 258–265. [Google Scholar] [CrossRef] [PubMed]
- Karam, E.G.; Mneimneh, Z.N.; Karam, A.N.; Fayyad, J.A.; Nasser, S.C.; Chatterji, S.; Kessler, R.C. Prevalence and treatment of mental disorders in Lebanon: A national epidemiological survey. Lancet 2006, 367, 1000–1006. [Google Scholar] [CrossRef]
- Cohen, M. Acute stress disorder in older, middle-aged and younger adults in reaction to the second Lebanon war. Int. J. Geriatr. Psychiatry 2008, 23, 34–40. [Google Scholar] [CrossRef]
- Moussa, S.; Malaeb, D.; Obeid, S.; Hallit, S. Correlates of Positivity Among a Sample of Lebanese University Students. Front. Psychol. 2022, 13, 880437. [Google Scholar] [CrossRef]
- Melki, I.S.; Beydoun, H.A.; Khogali, M.; Tamim, H.; Yunis, K.A.; National Collaborative Perinatal Neonatal, N. Household crowding index: A correlate of socioeconomic status and inter-pregnancy spacing in an urban setting. J. Epidemiol. Community Health 2004, 58, 476–480. [Google Scholar] [CrossRef]
- Ware, J.; Kosinski, M.; Keller, S. How to Score the SF-12 Physical and Mental Health Summary Scales; Quality Metric Inc.: Johnston, RI, USA, 1998. [Google Scholar]
- Haddad, C.; Sacre, H.; Obeid, S.; Salameh, P.; Hallit, S. Validation of the Arabic version of the “12-item short-form health survey” (SF-12) in a sample of Lebanese adults. Arch. Public Health 2021, 79, 56. [Google Scholar] [CrossRef]
- Caprara, G.V.; Alessandri, G.; Eisenberg, N.; Kupfer, A.; Steca, P.; Caprara, M.G.; Yamaguchi, S.; Fukuzawa, A.; Abela, J. The positivity scale. Psychol. Assess. 2012, 24, 701–712. [Google Scholar] [CrossRef] [PubMed]
- Pargament, K.; Feuille, M.; Burdzy, D. The Brief RCOPE: Current psychometric status of a short measure of religious coping. Religions 2011, 2, 51–76. [Google Scholar] [CrossRef]
- Diener, E.; Wirtz, D.; Tov, W.; Kim-Prieto, C.; Choi, D.W.; Oishi, S.; Biswas-Diener, R. New well-being measures: Short scales to assess flourishing and positive and negative feelings. Soc. Indic. Res. 2010, 97, 143–156. [Google Scholar] [CrossRef]
- George, D. SPSS for Windows Step by Step: A Simple Study Guide and Reference, 17.0 Update, 10/e; Pearson Education India: Noida, India, 2011. [Google Scholar]
- Vandekerckhove, J.; Matzke, D.; Wagenmakers, E.-J. Model Comparison and the Principle of Parsimony; Oxford University Press: Oxford, UK, 2015. [Google Scholar]
- Nolan, J.A.; McEvoy, J.P.; Koenig, H.G.; Hooten, E.G.; Whetten, K.; Pieper, C.F. Religious coping and quality of life among individuals living with schizophrenia. Psychiatr. Serv. 2012, 63, 1051–1054. [Google Scholar] [CrossRef] [PubMed]
- Zamanian, H.; Eftekhar-Ardebili, H.; Eftekhar-Ardebili, M.; Shojaeizadeh, D.; Nedjat, S.; Taheri-Kharameh, Z.; Daryaafzoon, M. Religious coping and quality of life in women with breast cancer. Asian Pac. J. Cancer Prev. 2015, 16, 7721–7725. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Taheri-Kharameh, Z.; Zamanian, H.; Montazeri, A.; Asgarian, A.; Esbiri, R. Negative religious coping, positive religious coping, and quality of life among hemodialysis patients. Nephro-Urol. Mon. 2016, 8, e38009. [Google Scholar] [CrossRef]
- Lee, M.; Nezu, A.M.; Nezu, C.M. Positive and negative religious coping, depressive symptoms, and quality of life in people with HIV. J. Behav. Med. 2014, 37, 921–930. [Google Scholar] [CrossRef]
- Pedersen, H.F.; Pargament, K.I.; Pedersen, C.G.; Zachariae, R. Religious coping and quality of life among severely ill lung patients in a secular society. Int. J. Psychol. Relig. 2013, 23, 188–203. [Google Scholar] [CrossRef]
- Bagheri-Nesami, M.; Kazemi, A.; Goudarzian, A.H.; Nasiri, F.; Davari, J. Association between religious coping and quality of working life in nurses. Iran. J. Psychiatry Behav. Sci. 2017, 11, e4946. [Google Scholar]
- Santos, P.R.; Júnior, J.R.F.G.C.; Cavalcante Filho, J.R.M.; Ferreira, T.P.; dos Santos Filho, J.N.G.; da Silva Oliveira, S. Religious coping methods predict depression and quality of life among end-stage renal disease patients undergoing hemodialysis: A cross-sectional study. BMC Nephrol. 2017, 18, 197. [Google Scholar] [CrossRef]
- Vitorino, L.M.; Soares, R.D.C.E.S.; Santos, A.E.O.; Lucchetti, A.L.G.; Cruz, J.P.; Cortez, P.J.O.; Lucchetti, G. Two sides of the same coin: The positive and negative impact of spiritual religious coping on quality of life and depression in dialysis patients. J. Holist. Nurs. 2018, 36, 332–340. [Google Scholar] [CrossRef] [PubMed]
- Caprara, G.V.; Castellani, V.; Alessandri, G.; Mazzuca, F.; La Torre, M.; Barbaranelli, C.; Colaiaco, F.; Gerbino, M.; Pasquali, V.; D’Amelio, R.; et al. Being positive despite illness: The contribution of positivity to the quality of life of cancer patients. Psychol. Health 2016, 31, 524–534. [Google Scholar] [CrossRef] [PubMed]
- Alessandri, G.; Caprara, G.V.; Tisak, J. The unique contribution of positive orientation to optimal functioning: Further explorations. Eur. Psychol. 2012, 17, 44–54. [Google Scholar] [CrossRef]
- Applebaum, A.J.; Stein, E.M.; Lord-Bessen, J.; Pessin, H.; Rosenfeld, B.; Breitbart, W. Optimism, social support, and mental health outcomes in patients with advanced cancer. Psycho-Oncology 2014, 23, 299–306. [Google Scholar] [CrossRef]
- Beshkar, M.; Nikmanesh, Z.; Kahrazei, F. The effectiveness of positivity education on the students’ perception of competence and quality of life. Pajouhan Sci. J. 2021, 19, 59–67. [Google Scholar]
- Dehroyeh, S.; Naderi, H. The Effectiveness of Positivity Training on Reducing Burnout and Improving the Quality of Life of Nurses. J. Saf. Promot. Inj. Prev. 2021, 9, 274–284. [Google Scholar]
- Ghasemi Hosseinabadi, M.; Zandipour, T.; Hosseinian, S. Effectiveness of positivity group training on quality of life and resilience of female teachers of exceptional students. Empower. Except. Child. 2022, 12, 1–13. [Google Scholar]
- Wissing, M.P.; Schutte, L.; Wilson Fadiji, A. Cultures of positivity: Interconnectedness as a way of being. In Handbook of Quality of Life in African Societies; Springer: Cham, Switzerland, 2019; pp. 3–22. [Google Scholar]
- Carta, M.G.; Aguglia, E.; Caraci, F.; Dell’Osso, L.; Di Sciascio, G.; Drago, F.; Del Giudice, E.; Faravelli, C.; Hardoy, M.C.; Lecca, M.E.; et al. Quality of life and urban/rural living: Preliminary results of a community survey in Italy. Clin. Pract. Epidemiol. Ment. Health CP EMH 2012, 8, 169–174. [Google Scholar] [CrossRef]
- Mudey, A.; Ambekar, S.; Goyal, R.C.; Agarekar, S.; Wagh, V.V. Assessment of quality of life among rural and urban elderly population of Wardha District, Maharashtra, India. Stud. Ethno-Med. 2011, 5, 89–93. [Google Scholar] [CrossRef]
- Soh, S.-E.; McGinley, J.L.; Watts, J.J.; Iansek, R.; Morris, M.E. Rural living and health-related quality of life in Australians with Parkinson’s disease. Rural Remote Health 2012, 12, 1–9. [Google Scholar] [CrossRef]
- Grgić, I.; Žimbrek, T.; Tratnik, M.; Markovina, J.; Juračak, J. Quality of life in rural areas of Croatia: To stay or to leave. Afr. J. Agric. Res. 2010, 5, 653–660. [Google Scholar]
- Farhadi, A.; Foroughan, M.; Mohammadi, F. The quality of life among rural elderlies a cross-sectional study. Iran. J. Ageing 2011, 6. Available online: http://salmandj.uswr.ac.ir/article-1-419-en.html (accessed on 4 December 2022).
- Shogren, K.A.; Wehmeyer, M.L.; Palmer, S.B.; Forber-Pratt, A.J.; Little, T.J.; Lopez, S. Causal agency theory: Reconceptualizing a functional model of self-determination. Educ. Train. Autism Dev. Disabil. 2015, 50, 251–263. [Google Scholar]
- Tedrus, G.M.; Fonseca, L.C.; De Pietro Magri, F.; Mendes, P.H. Spiritual/religious coping in patients with epilepsy: Relationship with sociodemographic and clinical aspects and quality of life. Epilepsy Behav. 2013, 28, 386–390. [Google Scholar] [CrossRef] [PubMed]
- Enjedany, E.; Daryaafzoun, M.; Zamanian, H.; Meybodi, F.A.; Babaei, B.; Kiaee, N.; Hamzelouiyan, M.; Beigi, F.F. Religious coping and quality of life in Iranian cancer patients: Do coping styles affect quality of life? In Psychol Health; Taylor and Francis Ltd.: Oxon, UK, 2010; Volume 25. [Google Scholar]
| Variable | n (%) |
|---|---|
| Sex | |
| Male | 114 (34.2%) |
| Female | 219 (65.8%) |
| Marital status | |
| Single | |
| Married | |
| Region of living | |
| Urban | 210 (63.1%) |
| Rural | 123 (36.9%) |
| Mean ± SD | |
| Age (in years) | 22.95 ± 4.79 |
| Household crowding index | 1.09 ± 0.55 |
| Financial burden | 5.68 ± 2.66 |
| Physical quality of life | 44.77 ± 7.98 |
| Mental quality of life | 40.34 ± 8.95 |
| Variable | Physical QOL | Mental QOL | ||||
|---|---|---|---|---|---|---|
| Mean ± SD | p | Effect Size | Mean ± SD | p | Effect Size | |
| Sex | 0.014 | 0.009 | 0.008 | 0.310 | ||
| Male | 46.13 ± 6.39 | 42.14 ± 8.66 | ||||
| Female | 44.06 ± 8.62 | 39.40 ± 8.98 | ||||
| Marital status | 0.223 | 0.166 | 0.359 | 0.102 | ||
| Single | 45.04 ± 7.91 | 40.18 ± 9.69 | ||||
| Married | 43.69 ± 8.26 | 40.97 ± 4.49 | ||||
| Region of living | <0.001 | 0.689 | 0.270 | 0.137 | ||
| Urban | 43.31 ± 8.52 | 40.72 ± 8.49 | ||||
| Rural | 48.17 ± 5.17 | 39.45 ± 9.94 | ||||
| Variable | Physical QOL | Mental QOL | ||
|---|---|---|---|---|
| r | p | r | p | |
| Age | −0.106 | 0.053 | −0.156 | 0.004 |
| Household crowding index | −0.213 | <0.001 | −0.179 | 0.001 |
| Financial burden | 0.235 | <0.001 | −0.044 | 0.429 |
| Positivity score | 0.270 | <0.001 | 0.296 | <0.001 |
| Positive religious coping | −0.170 | 0.002 | 0.415 | <0.001 |
| Negative religious coping | −0.305 | <0.001 | −0.175 | 0.001 |
| Positive experiences in life | 0.266 | <0.001 | 0.552 | <0.001 |
| Negative experiences in life | −0.182 | 0.001 | −0.139 | 0.011 |
| Beta | β | p | 95% CI | |
|---|---|---|---|---|
| Negative religious coping | −0.30 | −0.22 | <0.001 | −0.45; −0.16 |
| Region of living (rural vs. urban *) | 2.91 | 0.17 | 0.003 | 1.02; 4.79 |
| Positivity | 0.24 | 0.15 | 0.006 | 0.07; 0.41 |
| Nagelkerke R2 = 15.6%. | ||||
| Beta | β | p | 95% CI | |
|---|---|---|---|---|
| Sex (females vs. males *) | −1.49 | −0.08 | 0.113 | −3.34; 0.36 |
| Positivity | 0.30 | 0.17 | 0.001 | 0.12; 0.48 |
| Positive experiences in life | 0.08 | 0.06 | 0.373 | −0.10; 0.26 |
| Positive religious coping | 0.48 | 0.32 | <0.001 | 0.29; 0.67 |
| Nagelkerke R2 = 21.1%. | ||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moussa, S.; Malaeb, D.; Barakat, M.; Sawma, T.; Obeid, S.; Hallit, S. Association between Experiences in Life and Quality of Life among Lebanese University Students in a Collapsing Country: The Moderating Role of Religious Coping and Positivity. Healthcare 2023, 11, 149. https://doi.org/10.3390/healthcare11010149
Moussa S, Malaeb D, Barakat M, Sawma T, Obeid S, Hallit S. Association between Experiences in Life and Quality of Life among Lebanese University Students in a Collapsing Country: The Moderating Role of Religious Coping and Positivity. Healthcare. 2023; 11(1):149. https://doi.org/10.3390/healthcare11010149
Chicago/Turabian StyleMoussa, Sara, Diana Malaeb, Muna Barakat, Toni Sawma, Sahar Obeid, and Souheil Hallit. 2023. "Association between Experiences in Life and Quality of Life among Lebanese University Students in a Collapsing Country: The Moderating Role of Religious Coping and Positivity" Healthcare 11, no. 1: 149. https://doi.org/10.3390/healthcare11010149
APA StyleMoussa, S., Malaeb, D., Barakat, M., Sawma, T., Obeid, S., & Hallit, S. (2023). Association between Experiences in Life and Quality of Life among Lebanese University Students in a Collapsing Country: The Moderating Role of Religious Coping and Positivity. Healthcare, 11(1), 149. https://doi.org/10.3390/healthcare11010149







