Pediatric AML: From Biology to Clinical Management
Abstract
:1. Clinical Introduction
1.1. Epidemiology of AML
1.2. Diagnostic Approach and Classification
| WHO Classification of AML and Related Neoplasms | |
|---|---|
| Acute myeloid leukemia with recurrent genetic abnormalities | AML with t(8;21)(q22;q22); RUNX1-RUNX1T1 |
| AML with inv(16)(p13.1q22) or t(16;16)(p13.1;q22); CBFB-MYH11 | |
| Acute promyelocytic leukemia with t(15;17)(q22;q12); PML-RARA | |
| AML with 11q23 (MLL) abnormalities | |
| AML with t(6;9)(p23;q34); DEK-NUP214 | |
| AML with inv(3)(q21q26.2) or t(3;3)(q21;q26.2); RPN1-EVI1 | |
| t(1;22)(p13;q13); RBM15-MKL1 | |
| Provisional entity: AML with mutated NPM1 | |
| Provisional entity: AML with mutated CEBPA | |
| Acute myeloid leukemia with myelodysplasia-related changes | |
| Therapy-related myeloid neoplasms | |
| Acute myeloid leukemia, not otherwise specified | AML with minimal differentiation |
| AML without maturation | |
| AML with maturation | |
| Acute myelomonocytic leukemia | |
| Acute monoblastic/monocytic leukemia | |
| Acute erythroid leukemia | |
| Pure erythroid leukemia | |
| Erythroleukemia, erythroid/myeloid | |
| Acute megakaryoblastic leukemia | |
| Acute basophilic leukemia | |
| Acute panmyelosis with myelofibrosis | |
| Myeloid sarcoma | |
| Myeloid proliferations related to Down syndrome | Transient abnormal myelopoiesis |
| Myeloid leukemia associated with Down syndrome | |
| Blastic plasmacytoid dendritic cell neoplasm | |
1.3. Treatment and Outcome
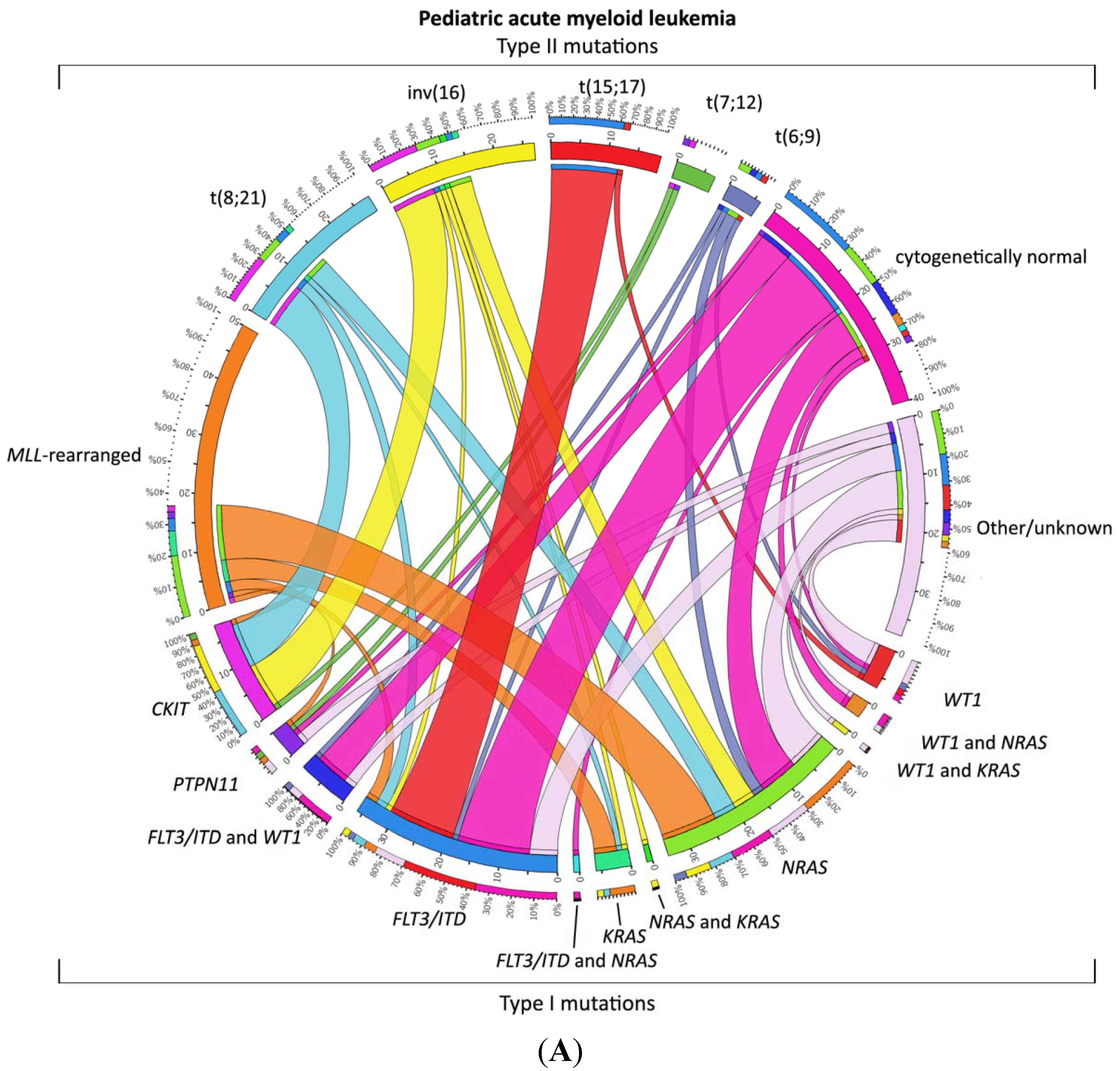
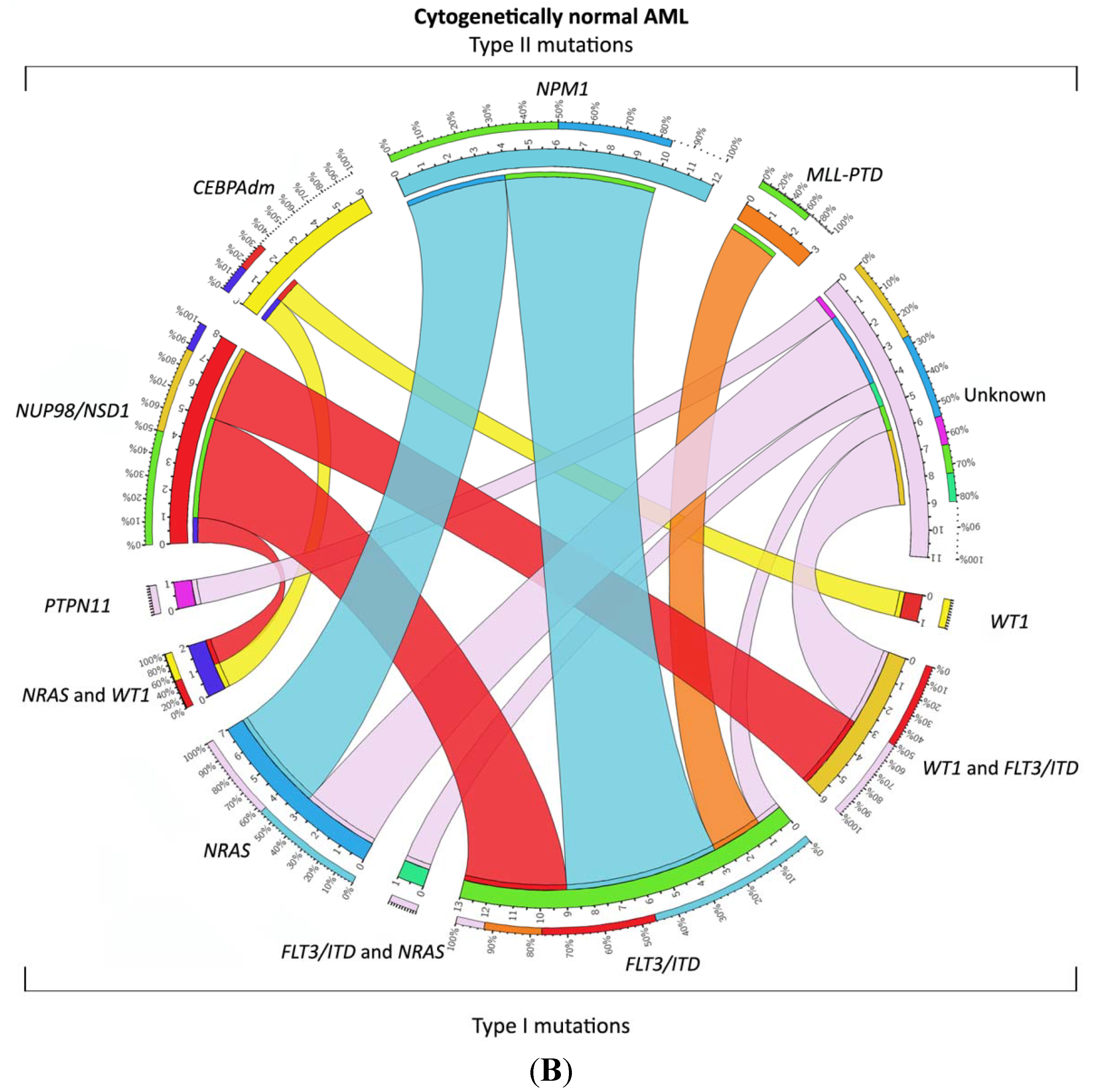
1.4. Relevant Molecular and Genetic Aberrations in Pediatric AML
| Study Group | Study and Inclusion Time (Calendar Years of Inclusion) | Patients (n) | Patients Treated with SCT (n) | EFS (%) | OS (%) | Relapse (%) | Source |
|---|---|---|---|---|---|---|---|
| BFM-SG | AML-BFM 2004 (2004–2010) | 521 | NA | 5 years 55 ± 2 | 5 years 74 ± 2 | 29 | Creutzig et al., 2013 [34] |
| JACLS | AML99 (2003–2006) | 146 | 22 (15%) | 5 years 66.7 ± 4.0 | 5 years 77.7 ± 8.0 | 30.2 | Imamura et al., 2012 [74] |
| AML99 (2000–2002) | 240 | Allo-SCT 41 (17%) Auto-SCT 5 (2%) | 5 years 61.6 ± 6.5 | 5 years 75.6 ± 5.3 | 32.2 | Tsukimoto et al., 2009 [27] | |
| AIEOP | AML2002/01 (2002–2011) | 482 | Allo-SCT 141 (29%) Auto-SCT 102 (21%) | 8 years 55.0 ± 2.6 | 8 years 67.7 ± 2.4 | 24 | Pession et al., 2013 [30] |
| COG | AAML03P1 (2003–2005) | 340 | 73 (21%) | 3 years 53 ± 6 | 3 years 66 ± 5 | 33 ± 6 | Cooper et al., 2012 [75] |
| NOPHO | NOPHO AML 2004 (2004–2009) | 151 | 22 (15%) | 3 years 57 ± 5 | 3 years 69 ± 5 | 30 | Abrahamsson et al., 2011 [20] |
| MRC | MRC AML12 (1995–2002) | 564 | 64 (11%) | 10 years 54 | 10 years 63 | 32 | Gibson et al., 2011 [33] |
| SJCRH | AML02 (2002–2008) | 216 | 59 (25%) | 3 years 63 | 3 years 71 | 21 | Rubnitz et al., 2010 [26] |
| PPLLSG | PPLLSG AML-98 (1998–2002) | 104 | Allo-SCT 14 (13%) Auto-SCT 8 (8%) | 5 years 47 ± 5 | 5 years 50 ± 5 | 24 | Dluzniewska et al., 2005 [76] |
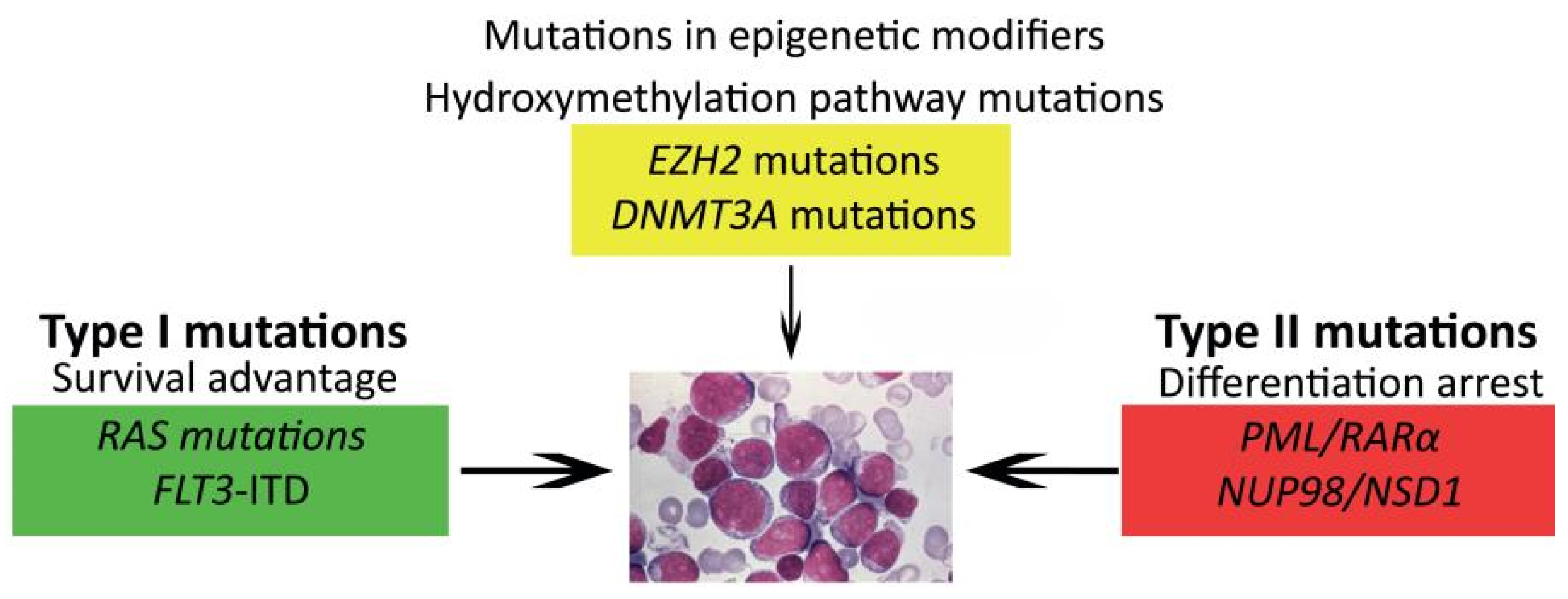
1.5. Prognostic Factors and Risk Group Stratification
2. Future Strategies
2.1. Genomic Approaches to Unravel the Biology of Pediatric AML
2.2. Towards Optimized Therapy
3. Conclusions
Acknowledgments
Author Contributions
Conflict of Interest
References
- Howlader, N.N.A.; Krapcho, M.; Garshell, J.; Miller, D.; Altekruse, S.F.; Kosary, C.L.; Yu, M.; Ruhl, J.; Tatalovich, Z.; Mariotto, A.; et al. SEER Cancer Statistics Review, 1975–2011; National Cancer Institute: Bethesda, MD, USA, 2012. [Google Scholar]
- Seif, A.E. Pediatric leukemia predisposition syndromes: Clues to understanding leukemogenesis. Cancer Genet. 2011, 204, 227–244. [Google Scholar] [CrossRef] [PubMed]
- Tonnies, H.; Huber, S.; Kuhl, J.S.; Gerlach, A.; Ebell, W.; Neitzel, H. Clonal chromosomal aberrations in bone marrow cells of Fanconi anemia patients: Gains of the chromosomal segment 3q26q29 as an adverse risk factor. Blood 2003, 101, 3872–3874. [Google Scholar] [CrossRef] [PubMed]
- Hahn, C.N.; Chong, C.E.; Carmichael, C.L.; Wilkins, E.J.; Brautigan, P.J.; Li, X.C.; Babic, M.; Lin, M.; Carmagnac, A.; Lee, Y.K.; et al. Heritable GATA2 mutations associated with familial myelodysplastic syndrome and acute myeloid leukemia. Nat. Genet. 2011, 43, 1012–1017. [Google Scholar] [CrossRef] [PubMed]
- Link, D.C.; Schuettpelz, L.G.; Shen, D.; Wang, J.; Walter, M.J.; Kulkarni, S.; Payton, J.E.; Ivanovich, J.; Goodfellow, P.J.; Le Beau, M.; et al. Identification of a novel TP53 cancer susceptibility mutation through whole-genome sequencing of a patient with therapy-related AML. JAMA 2011, 305, 1568–1576. [Google Scholar] [CrossRef] [PubMed]
- Owen, C.; Barnett, M.; Fitzgibbon, J. Familial myelodysplasia and acute myeloid leukaemia—A review. Br. J. Haematol. 2008, 140, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Smith, M.L.; Cavenagh, J.D.; Lister, T.A.; Fitzgibbon, J. Mutation of CEBPA in familial acute myeloid leukemia. N. Engl. J. Med. 2004, 351, 2403–2407. [Google Scholar] [CrossRef] [PubMed]
- Song, W.J.; Sullivan, M.G.; Legare, R.D.; Hutchings, S.; Tan, X.; Kufrin, D.; Ratajczak, J.; Resende, I.C.; Haworth, C.; Hock, R.; et al. Haploinsufficiency of CBFA2 causes familial thrombocytopenia with propensity to develop acute myelogenous leukaemia. Nat. Genet. 1999, 23, 166–175. [Google Scholar] [CrossRef] [PubMed]
- Zwaan, M.C.; Reinhardt, D.; Hitzler, J.; Vyas, P. Acute leukemias in children with Down syndrome. Pediatr. Clin. North Am. 2008, 55, 53–70. [Google Scholar] [CrossRef] [PubMed]
- Sandler, E.S.; Friedman, D.J.; Mustafa, M.M.; Winick, N.J.; Bowman, W.P.; Buchanan, G.R. Treatment of children with epipodophyllotoxin-induced secondary acute myeloid leukemia. Cancer 1997, 79, 1049–1054. [Google Scholar] [CrossRef] [PubMed]
- Weiss, B.; Vora, A.; Huberty, J.; Hawkins, R.A.; Matthay, K.K. Secondary myelodysplastic syndrome and leukemia following 131I-metaiodobenzylguanidine therapy for relapsed neuroblastoma. J. Pediatr. Hematol. Oncol. 2003, 25, 543–547. [Google Scholar] [CrossRef] [PubMed]
- Creutzig, U.; van den Heuvel-Eibrink, M.M.; Gibson, B.; Dworzak, M.N.; Adachi, S.; de Bont, E.; Harbott, J.; Hasle, H.; Johnston, D.; Kinoshita, A.; et al. Diagnosis and management of acute myeloid leukemia in children and adolescents: Recommendations from an international expert panel. Blood 2012, 120, 3187–3205. [Google Scholar] [CrossRef] [PubMed]
- Bennett, J.M.; Catovsky, D.; Daniel, M.T.; Flandrin, G.; Galton, D.A.; Gralnick, H.R.; Sultan, C. Proposals for the classification of the acute leukaemias. French-American-British (FAB) co-operative group. Br. J. Haematol. 1976, 33, 451–458. [Google Scholar] [CrossRef] [PubMed]
- Vardiman, J.W.; Thiele, J.; Arber, D.A.; Brunning, R.D.; Borowitz, M.J.; Porwit, A.; Harris, N.L.; Le Beau, M.M.; Hellstrom-Lindberg, E.; Tefferi, A.; et al. The 2008 revision of the World Health Organization (WHO) classification of myeloid neoplasms and acute leukemia: Rationale and important changes. Blood 2009, 114, 937–951. [Google Scholar] [CrossRef] [PubMed]
- Bennett, J.M.; Catovsky, D.; Daniel, M.T.; Flandrin, G.; Galton, D.A.; Gralnick, H.R.; Sultan, C. Criteria for the diagnosis of acute leukemia of megakaryocyte lineage (M7). A report of the French-American-British Cooperative Group. Ann. Intern. Med. 1985, 103, 460–462. [Google Scholar] [CrossRef] [PubMed]
- Mrozek, K.; Heinonen, K.; Bloomfield, C.D. Clinical importance of cytogenetics in acute myeloid leukaemia. Best Pract. Res. Clin. Haematol. 2001, 14, 19–47. [Google Scholar] [CrossRef] [PubMed]
- De Rooij, J.D.; Hollink, I.H.; Arentsen-Peters, S.T.; van Galen, J.F.; Berna Beverloo, H.; Baruchel, A.; Trka, J.; Reinhardt, D.; Sonneveld, E.; Zimmermann, M.; et al. NUP98/JARID1A is a novel recurrent abnormality in pediatric acute megakaryoblastic leukemia with a distinct HOX gene expression pattern. Leukemia 2013, 27, 2280–2288. [Google Scholar] [CrossRef] [PubMed]
- Mercher, T.; Busson-Le Coniat, M.; Nguyen Khac, F.; Ballerini, P.; Mauchauffe, M.; Bui, H.; Pellegrino, B.; Radford, I.; Valensi, F.; Mugneret, F.; et al. Recurrence of OTT-MAL fusion in t(1;22) of infant AML-M7. Genes Chromosomes Cancer 2002, 33, 22–28. [Google Scholar] [CrossRef] [PubMed]
- Von Bergh, A.R.; van Drunen, E.; van Wering, E.R.; van Zutven, L.J.; Hainmann, I.; Lonnerholm, G.; Meijerink, J.P.; Pieters, R.; Beverloo, H.B. High incidence of t(7;12)(q36;p13) in infant AML but not in infant ALL, with a dismal outcome and ectopic expression of HLXB9. Genes Chromosomes Cancer 2006, 45, 731–739. [Google Scholar] [CrossRef] [PubMed]
- Abrahamsson, J.; Forestier, E.; Heldrup, J.; Jahnukainen, K.; Jonsson, O.G.; Lausen, B.; Palle, J.; Zeller, B.; Hasle, H. Response-guided induction therapy in pediatric acute myeloid leukemia with excellent remission rate. J. Clin. Oncol. 2011, 29, 310–315. [Google Scholar] [CrossRef] [PubMed]
- Creutzig, U.Z.M.; Dworzak, M.; Bourquin, J.P.; Neuhoff, C.; Sander, A.; Stary, J.; Reinhardt, D. Study AML-BFM 2004: Improved Survival In Childhood Acute Myeloid Leukemia without Increased Toxicity. 2010. Available online: https://ash.confex.com/ash/2010/webprogram/Paper31036.html (accessed on 15 December 2014).
- Entz-Werle, N.; Suciu, S.; van der Werff ten Bosch, J.; Vilmer, E.; Bertrand, Y.; Benoit, Y.; Margueritte, G.; Plouvier, E.; Boutard, P.; Vandecruys, E.; et al. Results of 58,872 and 58,921 trials in acute myeloblastic leukemia and relative value of chemotherapy vs. allogeneic bone marrow transplantation in first complete remission: The EORTC Children Leukemia Group report. Leukemia 2005, 19, 2072–2081. [Google Scholar] [CrossRef] [PubMed]
- Gibson, B.E.; Wheatley, K.; Hann, I.M.; Stevens, R.F.; Webb, D.; Hills, R.K.; de Graaf, S.S.; Harrison, C.J. Treatment strategy and long-term results in paediatric patients treated in consecutive UK AML trials. Leukemia 2005, 19, 2130–2138. [Google Scholar] [CrossRef] [PubMed]
- Perel, Y.; Auvrignon, A.; Leblanc, T.; Michel, G.; Reguerre, Y.; Vannier, J.P.; Dalle, J.H.; Gandemer, V.; Schmitt, C.; Mechinaud, F.; et al. Treatment of childhood acute myeloblastic leukemia: Dose intensification improves outcome and maintenance therapy is of no benefit—Multicenter studies of the French LAME (Leucemie Aigue Myeloblastique Enfant) Cooperative Group. Leukemia 2005, 19, 2082–2089. [Google Scholar] [CrossRef] [PubMed]
- Pession, A.; Rondelli, R.; Basso, G.; Rizzari, C.; Testi, A.M.; Fagioli, F.; de Stefano, P.; Locatelli, F.; AML Strategy & Study Committee of the Associazione Italiana di Ematologia e Oncologia Pediatrica (AIEOP). Treatment and long-term results in children with acute myeloid leukaemia treated according to the AIEOP AML protocols. Leukemia 2005, 19, 2043–2053. [Google Scholar] [CrossRef] [PubMed]
- Rubnitz, J.E.; Inaba, H.; Dahl, G.; Ribeiro, R.C.; Bowman, W.P.; Taub, J.; Pounds, S.; Razzouk, B.I.; Lacayo, N.J.; Cao, X.; et al. Minimal residual disease-directed therapy for childhood acute myeloid leukaemia: Results of the AML02 multicentre trial. Lancet Oncol. 2010, 11, 543–552. [Google Scholar] [CrossRef] [PubMed]
- Tsukimoto, I.; Tawa, A.; Horibe, K.; Tabuchi, K.; Kigasawa, H.; Tsuchida, M.; Yabe, H.; Nakayama, H.; Kudo, K.; Kobayashi, R.; et al. Risk-stratified therapy and the intensive use of cytarabine improves the outcome in childhood acute myeloid leukemia: The AML99 trial from the Japanese Childhood AML Cooperative Study Group. J. Clin. Oncol. 2009, 27, 4007–4013. [Google Scholar] [CrossRef] [PubMed]
- Creutzig, U.; Zimmermann, M.; Dworzak, M.N.; Ritter, J.; Schellong, G.; Reinhardt, D. Development of a curative treatment within the AML-BFM studies. Klin. Padiatr. 2013, 225 (Suppl. S1), 79–86. [Google Scholar]
- Horibe, K.; Saito, A.M.; Takimoto, T.; Tsuchida, M.; Manabe, A.; Shima, M.; Ohara, A.; Mizutani, S. Incidence and survival rates of hematological malignancies in Japanese children and adolescents (2006–2010): Based on registry data from the Japanese Society of Pediatric Hematology. Int. J. Hematol. 2013, 98, 74–88. [Google Scholar] [CrossRef] [PubMed]
- Pession, A.; Masetti, R.; Rizzari, C.; Putti, M.C.; Casale, F.; Fagioli, F.; Luciani, M.; Lo Nigro, L.; Menna, G.; Micalizzi, C.; et al. Results of the AIEOP AML 2002/01 multicenter prospective trial for the treatment of children with acute myeloid leukemia. Blood 2013, 122, 170–178. [Google Scholar] [CrossRef] [PubMed]
- Van der Velden, V.H.; van der Sluijs-Geling, A.; Gibson, B.E.; te Marvelde, J.G.; Hoogeveen, P.G.; Hop, W.C.; Wheatley, K.; Bierings, M.B.; Schuurhuis, G.J.; de Graaf, S.S.; et al. Clinical significance of flowcytometric minimal residual disease detection in pediatric acute myeloid leukemia patients treated according to the DCOG ANLL97/MRC AML12 protocol. Leukemia 2010, 24, 1599–1606. [Google Scholar] [CrossRef] [PubMed]
- Becton, D.; Dahl, G.V.; Ravindranath, Y.; Chang, M.N.; Behm, F.G.; Raimondi, S.C.; Head, D.R.; Stine, K.C.; Lacayo, N.J.; Sikic, B.I.; et al. Randomized use of cyclosporin A (CsA) to modulate P-glycoprotein in children with AML in remission: Pediatric Oncology Group Study 9421. Blood 2006, 107, 1315–1324. [Google Scholar] [CrossRef] [PubMed]
- Gibson, B.E.; Webb, D.K.; Howman, A.J.; de Graaf, S.S.; Harrison, C.J.; Wheatley, K.; United Kingdom Childhood Leukaemia Working Group; the Dutch Childhood Oncology Group. Results of a randomized trial in children with Acute Myeloid Leukaemia: Medical research council AML12 trial. Br. J. Haematol. 2011, 155, 366–376. [Google Scholar] [CrossRef] [PubMed]
- Creutzig, U.; Zimmermann, M.; Bourquin, J.P.; Dworzak, M.N.; Fleischhack, G.; Graf, N.; Klingebiel, T.; Kremens, B.; Lehrnbecher, T.; von Neuhoff, C.; et al. Randomized trial comparing liposomal daunorubicin with idarubicin as induction for pediatric acute myeloid leukemia: Results from Study AML-BFM 2004. Blood 2013, 122, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Niewerth, D.; Creutzig, U.; Bierings, M.B.; Kaspers, G.J. A review on allogeneic stem cell transplantation for newly diagnosed pediatric acute myeloid leukemia. Blood 2010, 116, 2205–2214. [Google Scholar] [CrossRef] [PubMed]
- Reinhardt, D.K.B.; Zimmermann, M.; Vormoor, J.; Dworzak, M.; Peters, C.; Creutzig, U.; Klingebiel, T. No Improvement of Overall-Survival in Children with High-Risk Acute Myeloid Leukemia by Stem Cell Transplantation in 1st Complete Remission. 2006. Available online: http://abstractshematologylibraryorg/cgi/content/short/108/11/320 (accessed on 15 December 2014).
- Passweg, J.R.; Baldomero, H.; Peters, C.; Gaspar, H.B.; Cesaro, S.; Dreger, P.; Duarte, R.F.; Falkenburg, J.H.; Farge-Bancel, D.; Gennery, A.; et al. Hematopoietic SCT in Europe: Data and trends in 2012 with special consideration of pediatric transplantation. Bone Marrow Transpl. 2014, 49, 744–750. [Google Scholar] [CrossRef]
- Bastos-Oreiro, M.; Perez-Corral, A.; Martinez-Laperche, C.; Bento, L.; Pascual, C.; Kwon, M.; Balsalobre, P.; Munoz, C.; Buces, E.; Serrano, D.; et al. Prognostic impact of minimal residual disease analysis by flow cytometry in patients with acute myeloid leukemia before and after allogeneic hemopoietic stem cell transplantation. Eur. J. Haematol. 2014, 93, 239–246. [Google Scholar] [PubMed]
- Anthias, C.; Dignan, F.L.; Morilla, R.; Morilla, A.; Ethell, M.E.; Potter, M.N.; Shaw, B.E. Pre-transplant MRD predicts outcome following reduced-intensity and myeloablative allogeneic hemopoietic SCT in AML. Bone Marrow Transpl. 2014, 49, 679–683. [Google Scholar] [CrossRef]
- Hasle, H. A critical review of which children with acute myeloid leukaemia need stem cell procedures. Br. J. Haematol. 2014, 166, 23–33. [Google Scholar] [CrossRef] [PubMed]
- Sander, A.; Zimmermann, M.; Dworzak, M.; Fleischhack, G.; von Neuhoff, C.; Reinhardt, D.; Kaspers, G.J.; Creutzig, U. Consequent and intensified relapse therapy improved survival in pediatric AML: Results of relapse treatment in 379 patients of three consecutive AML-BFM trials. Leukemia 2010, 24, 1422–1428. [Google Scholar] [CrossRef] [PubMed]
- Kaspers, G.J.; Zimmermann, M.; Reinhardt, D.; Gibson, B.E.; Tamminga, R.Y.; Aleinikova, O.; Armendariz, H.; Dworzak, M.; Ha, S.Y.; Hasle, H.; et al. Improved outcome in pediatric relapsed acute myeloid leukemia: Results of a randomized trial on liposomal daunorubicin by the International BFM Study Group. J. Clin. Oncol. 2013, 31, 599–607. [Google Scholar] [CrossRef] [PubMed]
- Slats, A.M.; Egeler, R.M.; van der Does-van den Berg, A.; Korbijn, C.; Hahlen, K.; Kamps, W.A.; Veerman, A.J.; Zwaan, C.M. Causes of death—Other than progressive leukemia—In childhood acute lymphoblastic (ALL) and myeloid leukemia (AML): The Dutch Childhood Oncology Group experience. Leukemia 2005, 19, 537–544. [Google Scholar] [PubMed]
- Kelly, L.M.; Gilliland, D.G. Genetics of myeloid leukemias. Annu. Rev. Genomics Hum. Genet. 2002, 3, 179–198. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, M.; Sternberg, A.; Hall, G.; Thomas, A.; Smith, O.; O’Marcaigh, A.; Wynn, R.; Stevens, R.; Addison, M.; King, D.; et al. Natural history of GATA1 mutations in Down syndrome. Blood 2004, 103, 2480–2489. [Google Scholar] [CrossRef] [PubMed]
- Hollink, I.H.; van den Heuvel-Eibrink, M.M.; Arentsen-Peters, S.T.; Zimmermann, M.; Peeters, J.K.; Valk, P.J.; Balgobind, B.V.; Sonneveld, E.; Kaspers, G.J.; de Bont, E.S.; et al. Characterization of CEBPA mutations and promoter hypermethylation in pediatric acute myeloid leukemia. Haematologica 2011, 96, 384–392. [Google Scholar] [CrossRef] [PubMed]
- Hollink, I.H.; van den Heuvel-Eibrink, M.M.; Zimmermann, M.; Balgobind, B.V.; Arentsen-Peters, S.T.; Alders, M.; Willasch, A.; Kaspers, G.J.; Trka, J.; Baruchel, A.; et al. Clinical relevance of Wilms tumor 1 gene mutations in childhood acute myeloid leukemia. Blood 2009, 113, 5951–5960. [Google Scholar] [PubMed]
- Balgobind, B.V.; Hollink, I.H.; Arentsen-Peters, S.T.; Zimmermann, M.; Harbott, J.; Beverloo, H.B.; von Bergh, A.R.; Cloos, J.; Kaspers, G.J.; de Haas, V.; et al. Integrative analysis of type-I and type-II aberrations underscores the genetic heterogeneity of pediatric acute myeloid leukemia. Haematologica 2011, 96, 1478–1487. [Google Scholar] [CrossRef] [PubMed]
- Betts, D.R.; Ammann, R.A.; Hirt, A.; Hengartner, H.; Beck-Popovic, M.; Kuhne, T.; Nobile, L.; Caflisch, U.; Wacker, P.; Niggli, F.K. The prognostic significance of cytogenetic aberrations in childhood acute myeloid leukaemia. A study of the Swiss Paediatric Oncology Group (SPOG). Eur. J. Haematol. 2007, 78, 468–476. [Google Scholar] [CrossRef] [PubMed]
- Grimwade, D. The clinical significance of cytogenetic abnormalities in acute myeloid leukaemia. Best Pract. Res. Clin. Haematol. 2001, 14, 497–529. [Google Scholar] [CrossRef] [PubMed]
- Harrison, C.J.; Hills, R.K.; Moorman, A.V.; Grimwade, D.J.; Hann, I.; Webb, D.K.; Wheatley, K.; de Graaf, S.S.; van den Berg, E.; Burnett, A.K.; et al. Cytogenetics of childhood acute myeloid leukemia: United Kingdom Medical Research Council Treatment trials AML 10 and 12. J. Clin. Oncol. 2010, 28, 2674–2681. [Google Scholar] [CrossRef] [PubMed]
- Von Neuhoff, C.; Reinhardt, D.; Sander, A.; Zimmermann, M.; Bradtke, J.; Betts, D.R.; Zemanova, Z.; Stary, J.; Bourquin, J.P.; Haas, O.A.; et al. Prognostic impact of specific chromosomal aberrations in a large group of pediatric patients with acute myeloid leukemia treated uniformly according to trial AML-BFM 98. J. Clin. Oncol. 2010, 28, 2682–2689. [Google Scholar]
- Park, J.; Kim, M.; Lim, J.; Kim, Y.; Han, K.; Lee, J.; Chung, N.G.; Cho, B.; Kim, H.K. Three-way complex translocations in infant acute myeloid leukemia with t(7;12)(q36;p13): The incidence and correlation of a HLXB9 overexpression. Cancer Genet. Cytogenet. 2009, 191, 102–105. [Google Scholar] [CrossRef] [PubMed]
- Simmons, H.M.; Oseth, L.; Nguyen, P.; O’Leary, M.; Conklin, K.F.; Hirsch, B. Cytogenetic and molecular heterogeneity of 7q36/12p13 rearrangements in childhood AML. Leukemia 2002, 16, 2408–2416. [Google Scholar] [CrossRef] [PubMed]
- Slater, R.M.; von Drunen, E.; Kroes, W.G.; Weghuis, D.O.; van den Berg, E.; Smit, E.M.; van der Does-van den Berg, A.; van Wering, E.; Hahlen, K.; Carroll, A.J.; et al. t(7;12)(q36;p13) and t(7;12)(q32;p13)—Translocations involving ETV6 in children 18 months of age or younger with myeloid disorders. Leukemia 2001, 15, 915–920. [Google Scholar] [CrossRef] [PubMed]
- Torres, L.; Lisboa, S.; Vieira, J.; Cerveira, N.; Santos, J.; Pinheiro, M.; Correia, C.; Bizarro, S.; Almeida, M.; Teixeira, M.R. Acute megakaryoblastic leukemia with a four-way variant translocation originating the RBM15-MKL1 fusion gene. Blood Cancer 2011, 56, 846–849. [Google Scholar] [CrossRef]
- Hollink, I.H.; van den Heuvel-Eibrink, M.M.; Arentsen-Peters, S.T.; Pratcorona, M.; Abbas, S.; Kuipers, J.E.; van Galen, J.F.; Beverloo, H.B.; Sonneveld, E.; Kaspers, G.J.; et al. NUP98/NSD1 characterizes a novel poor prognostic group in acute myeloid leukemia with a distinct HOX gene expression pattern. Blood 2011, 118, 3645–3656. [Google Scholar] [CrossRef] [PubMed]
- Meyer, C.; Kowarz, E.; Hofmann, J.; Renneville, A.; Zuna, J.; Trka, J.; Ben Abdelali, R.; Macintyre, E.; De Braekeleer, E.; De Braekeleer, M.; et al. New insights to the MLL recombinome of acute leukemias. Leukemia 2009, 23, 1490–1499. [Google Scholar] [CrossRef] [PubMed]
- Meyer, C.; Hofmann, J.; Burmeister, T.; Groger, D.; Park, T.S.; Emerenciano, M.; Pombo de Oliveira, M.; Renneville, A.; Villarese, P.; Macintyre, E.; et al. The MLL recombinome of acute leukemias in 2013. Leukemia 2013, 27, 2165–2176. [Google Scholar] [CrossRef] [PubMed]
- Bernt, K.M.; Zhu, N.; Sinha, A.U.; Vempati, S.; Faber, J.; Krivtsov, A.V.; Feng, Z.; Punt, N.; Daigle, A.; Bullinger, L.; et al. MLL-rearranged leukemia is dependent on aberrant H3K79 methylation by DOT1L. Cancer Cell 2011, 20, 66–78. [Google Scholar] [CrossRef] [PubMed]
- Marschalek, R. Mechanisms of leukemogenesis by MLL fusion proteins. Br. J. Haematol. 2011, 152, 141–154. [Google Scholar] [CrossRef] [PubMed]
- Marcucci, G.; Haferlach, T.; Dohner, H. Molecular genetics of adult acute myeloid leukemia: Prognostic and therapeutic implications. J. Clin. Oncol. 2011, 29, 475–486. [Google Scholar] [CrossRef] [PubMed]
- Ley, T.J.; Ding, L.; Walter, M.J.; McLellan, M.D.; Lamprecht, T.; Larson, D.E.; Kandoth, C.; Payton, J.E.; Baty, J.; Welch, J.; et al. DNMT3A mutations in acute myeloid leukemia. N. Engl. J. Med. 2010, 363, 2424–2433. [Google Scholar] [CrossRef] [PubMed]
- Figueroa, M.E.; Abdel-Wahab, O.; Lu, C.; Ward, P.S.; Patel, J.; Shih, A.; Li, Y.; Bhagwat, N.; Vasanthakumar, A.; Fernandez, H.F.; et al. Leukemic IDH1 and IDH2 mutations result in a hypermethylation phenotype, disrupt TET2 function, and impair hematopoietic differentiation. Cancer Cell 2010, 18, 553–567. [Google Scholar] [CrossRef] [PubMed]
- Delhommeau, F.; Dupont, S.; Della Valle, V.; James, C.; Trannoy, S.; Masse, A.; Kosmider, O.; Le Couedic, J.P.; Robert, F.; Alberdi, A.; et al. Mutation in TET2 in myeloid cancers. N. Engl. J. Med. 2009, 360, 2289–2301. [Google Scholar] [CrossRef] [PubMed]
- Hollink, I.H.; Feng, Q.; Danen-van Oorschot, A.A.; Arentsen-Peters, S.T.; Verboon, L.J.; Zhang, P.; de Haas, V.; Reinhardt, D.; Creutzig, U.; Trka, J.; et al. Low frequency of DNMT3A mutations in pediatric AML, and the identification of the OCI-AML3 cell line as an in vitro model. Leukemia 2012, 26, 371–373. [Google Scholar] [CrossRef] [PubMed]
- Langemeijer, S.M.; Jansen, J.H.; Hooijer, J.; van Hoogen, P.; Stevens-Linders, E.; Massop, M.; Waanders, E.; van Reijmersdal, S.V.; Stevens-Kroef, M.J.; Zwaan, C.M.; et al. TET2 mutations in childhood leukemia. Leukemia 2011, 25, 189–192. [Google Scholar] [CrossRef] [PubMed]
- Ho, P.A.; Alonzo, T.A.; Kopecky, K.J.; Miller, K.L.; Kuhn, J.; Zeng, R.; Gerbing, R.B.; Raimondi, S.C.; Hirsch, B.A.; Oehler, V.; et al. Molecular alterations of the IDH1 gene in AML: A Children’s Oncology Group and Southwest Oncology Group study. Leukemia 2010, 24, 909–913. [Google Scholar] [CrossRef] [PubMed]
- Yan, X.J.; Xu, J.; Gu, Z.H.; Pan, C.M.; Lu, G.; Shen, Y.; Shi, J.Y.; Zhu, Y.M.; Tang, L.; Zhang, X.W.; et al. Exome sequencing identifies somatic mutations of DNA methyltransferase gene DNMT3A in acute monocytic leukemia. Nat. Genet. 2011, 43, 309–315. [Google Scholar] [CrossRef] [PubMed]
- Valerio, D.G.; Katsman-Kuipers, J.E.; Jansen, J.H.; Verboon, L.J.; de Haas, V.; Stary, J.; Baruchel, A.; Zimmermann, M.; Pieters, R.; Reinhardt, D.; et al. Mapping epigenetic regulator gene mutations in cytogenetically normal pediatric acute myeloid leukemia. Haematologica 2014, 99. [Google Scholar] [CrossRef]
- Mardis, E.R.; Ding, L.; Dooling, D.J.; Larson, D.E.; McLellan, M.D.; Chen, K.; Koboldt, D.C.; Fulton, R.S.; Delehaunty, K.D.; McGrath, S.D.; et al. Recurring mutations found by sequencing an acute myeloid leukemia genome. N. Engl. J. Med. 2009, 361, 1058–1066. [Google Scholar] [CrossRef] [PubMed]
- Stumpel, D.J.; Schneider, P.; van Roon, E.H.; Boer, J.M.; de Lorenzo, P.; Valsecchi, M.G.; de Menezes, R.X.; Pieters, R.; Stam, R.W. Specific promoter methylation identifies different subgroups of MLL-rearranged infant acute lymphoblastic leukemia, influences clinical outcome, and provides therapeutic options. Blood 2009, 114, 5490–5498. [Google Scholar] [CrossRef] [PubMed]
- Krzywinski, M.; Schein, J.; Birol, I.; Connors, J.; Gascoyne, R.; Horsman, D.; Jones, S.J.; Marra, M.A. Circos: An information aesthetic for comparative genomics. Genome Res. 2009, 19, 1639–1645. [Google Scholar] [CrossRef] [PubMed]
- Imamura, T.; Iwamoto, S.; Kanai, R.; Shimada, A.; Terui, K.; Osugi, Y.; Kobayashi, R.; Tawa, A.; Kosaka, Y.; Kato, K.; et al. Outcome in 146 patients with paediatric acute myeloid leukaemia treated according to the AML99 protocol in the period 2003–06 from the Japan Association of Childhood Leukaemia Study. Br. J. Haematol. 2012, 159, 204–210. [Google Scholar] [CrossRef] [PubMed]
- Cooper, T.M.; Franklin, J.; Gerbing, R.B.; Alonzo, T.A.; Hurwitz, C.; Raimondi, S.C.; Hirsch, B.; Smith, F.O.; Mathew, P.; Arceci, R.J.; et al. AAML03P1, a pilot study of the safety of gemtuzumab ozogamicin in combination with chemotherapy for newly diagnosed childhood acute myeloid leukemia: A report from the Children’s Oncology Group. Cancer 2012, 118, 761–769. [Google Scholar] [CrossRef] [PubMed]
- Dluzniewska, A.; Balwierz, W.; Armata, J.; Balcerska, A.; Chybicka, A.; Kowalczyk, J.; Matysiak, M.; Ochocka, M.; Radwanska, U.; Rokicka-Milewska, R.; et al. Twenty years of Polish experience with three consecutive protocols for treatment of childhood acute myelogenous leukemia. Leukemia 2005, 19, 2117–2124. [Google Scholar] [CrossRef] [PubMed]
- Bachas, C.; Schuurhuis, G.J.; Reinhardt, D.; Creutzig, U.; Kwidama, Z.J.; Zwaan, C.M.; van den Heuvel-Eibrink, M.M.; de Bont, E.S.; Elitzur, S.; Rizzari, C.; et al. Clinical relevance of molecular aberrations in paediatric acute myeloid leukaemia at first relapse. Br. J. Haematol. 2014, 166, 902–910. [Google Scholar] [CrossRef] [PubMed]
- Creutzig, U.; Zimmermann, M.; Dworzak, M.N.; Gibson, B.; Tamminga, R.; Abrahamsson, J.; Ha, S.Y.; Hasle, H.; Maschan, A.; Bertrand, Y.; et al. The prognostic significance of early treatment response in pediatric relapsed acute myeloid leukemia: Results of the international study Relapsed AML 2001/01. Haematologica 2014, 99, 1472–1478. [Google Scholar] [CrossRef] [PubMed]
- Rubnitz, J.E.; Raimondi, S.C.; Halbert, A.R.; Tong, X.; Srivastava, D.K.; Razzouk, B.I.; Pui, C.H.; Downing, J.R.; Ribeiro, R.C.; Behm, F.G. Characteristics and outcome of t(8;21)-positive childhood acute myeloid leukemia: A single institution’s experience. Leukemia 2002, 16, 2072–2077. [Google Scholar] [CrossRef] [PubMed]
- Balgobind, B.V.; Raimondi, S.C.; Harbott, J.; Zimmermann, M.; Alonzo, T.A.; Auvrignon, A.; Beverloo, H.B.; Chang, M.; Creutzig, U.; Dworzak, M.N.; et al. Novel prognostic subgroups in childhood 11q23/MLL-rearranged acute myeloid leukemia: Results of an international retrospective study. Blood 2009, 114, 2489–2496. [Google Scholar] [CrossRef] [PubMed]
- Coenen, E.A.; Raimondi, S.C.; Harbott, J.; Zimmermann, M.; Alonzo, T.A.; Auvrignon, A.; Beverloo, H.B.; Chang, M.; Creutzig, U.; Dworzak, M.N.; et al. Prognostic significance of additional cytogenetic aberrations in 733 de novo pediatric 11q23/MLL-rearranged AML patients: Results of an international study. Blood 2011, 117, 7102–7111. [Google Scholar] [CrossRef] [PubMed]
- Hasle, H.; Alonzo, T.A.; Auvrignon, A.; Behar, C.; Chang, M.; Creutzig, U.; Fischer, A.; Forestier, E.; Fynn, A.; Haas, O.A.; et al. Monosomy 7 and deletion 7q in children and adolescents with acute myeloid leukemia: An international retrospective study. Blood 2007, 109, 4641–4647. [Google Scholar] [CrossRef] [PubMed]
- Johnston, D.L.; Alonzo, T.A.; Gerbing, R.B.; Hirsch, B.; Heerema, N.A.; Ravindranath, Y.; Woods, W.G.; Lange, B.J.; Gamis, A.S.; Raimondi, S.C. Outcome of pediatric patients with acute myeloid leukemia (AML) and -5/5q- abnormalities from five pediatric AML treatment protocols: A report from the Children’s Oncology Group. Pediatr. Blood Cancer 2013, 60, 2073–2078. [Google Scholar] [PubMed]
- Kelly, M.J.; Horan, J.T.; Alonzo, T.A.; Eapen, M.; Gerbing, R.B.; He, W.; Lange, B.J.; Parsons, S.K.; Woods, W.G. Comparable survival for pediatric acute myeloid leukemia with poor-risk cytogenetics following chemotherapy, matched related donor, or unrelated donor transplantation. Pediatr. Blood Cancer 2014, 61, 269–275. [Google Scholar] [CrossRef] [PubMed]
- Manola, K.N.; Panitsas, F.; Polychronopoulou, S.; Daraki, A.; Karakosta, M.; Stavropoulou, C.; Avgerinou, G.; Hatzipantelis, E.; Pantelias, G.; Sambani, C.; et al. Cytogenetic abnormalities and monosomal karyotypes in children and adolescents with acute myeloid leukemia: Correlations with clinical characteristics and outcome. Cancer Genet. 2013, 206, 63–72. [Google Scholar] [CrossRef] [PubMed]
- Balgobind, B.V.; Lugthart, S.; Hollink, I.H.; Arentsen-Peters, S.T.; van Wering, E.R.; de Graaf, S.S.; Reinhardt, D.; Creutzig, U.; Kaspers, G.J.; de Bont, E.S.; et al. EVI1 overexpression in distinct subtypes of pediatric acute myeloid leukemia. Leukemia 2010, 24, 942–949. [Google Scholar] [CrossRef] [PubMed]
- Groschel, S.; Lugthart, S.; Schlenk, R.F.; Valk, P.J.; Eiwen, K.; Goudswaard, C.; van Putten, W.J.; Kayser, S.; Verdonck, L.F.; Lubbert, M.; et al. High EVI1 expression predicts outcome in younger adult patients with acute myeloid leukemia and is associated with distinct cytogenetic abnormalities. J. Clin. Oncol. 2010, 28, 2101–2107. [Google Scholar] [CrossRef] [PubMed]
- Bachas, C.; Schuurhuis, G.J.; Hollink, I.H.; Kwidama, Z.J.; Goemans, B.F.; Zwaan, C.M.; van den Heuvel-Eibrink, M.M.; de Bont, E.S.; Reinhardt, D.; Creutzig, U.; et al. High-frequency type I/II mutational shifts between diagnosis and relapse are associated with outcome in pediatric AML: Implications for personalized medicine. Blood 2010, 116, 2752–2758. [Google Scholar] [CrossRef] [PubMed]
- Hollink, I.H.; Zwaan, C.M.; Zimmermann, M.; Arentsen-Peters, T.C.; Pieters, R.; Cloos, J.; Kaspers, G.J.; de Graaf, S.S.; Harbott, J.; Creutzig, U.; et al. Favorable prognostic impact of NPM1 gene mutations in childhood acute myeloid leukemia, with emphasis on cytogenetically normal AML. Leukemia 2009, 23, 262–270. [Google Scholar] [CrossRef] [PubMed]
- Raghavan, M.; Lillington, D.M.; Skoulakis, S.; Debernardi, S.; Chaplin, T.; Foot, N.J.; Lister, T.A.; Young, B.D. Genome-wide single nucleotide polymorphism analysis reveals frequent partial uniparental disomy due to somatic recombination in acute myeloid leukemias. Cancer Res. 2005, 65, 375–378. [Google Scholar] [PubMed]
- Balgobind, B.V.; van Vlierberghe, P.; van den Ouweland, A.M.; Beverloo, H.B.; Terlouw-Kromosoeto, J.N.; van Wering, E.R.; Reinhardt, D.; Horstmann, M.; Kaspers, G.J.; Pieters, R.; et al. Leukemia-associated NF1 inactivation in patients with pediatric T-ALL and AML lacking evidence for neurofibromatosis. Blood 2008, 111, 4322–4328. [Google Scholar] [CrossRef] [PubMed]
- Balgobind, B.V.; Van den Heuvel-Eibrink, M.M.; De Menezes, R.X.; Reinhardt, D.; Hollink, I.H.; Arentsen-Peters, S.T.; van Wering, E.R.; Kaspers, G.J.; Cloos, J.; de Bont, E.S.; et al. Evaluation of gene expression signatures predictive of cytogenetic and molecular subtypes of pediatric acute myeloid leukemia. Haematologica 2011, 96, 221–230. [Google Scholar] [CrossRef] [PubMed]
- Ross, M.E.; Mahfouz, R.; Onciu, M.; Liu, H.C.; Zhou, X.; Song, G.; Shurtleff, S.A.; Pounds, S.; Cheng, C.; Ma, J.; et al. Gene expression profiling of pediatric acute myelogenous leukemia. Blood 2004, 104, 3679–3687. [Google Scholar] [CrossRef] [PubMed]
- Valk, P.J.; Verhaak, R.G.; Beijen, M.A.; Barjesteh van Waalwijk van Doorn-Khosrovani, S.; Erpelinck, C.A.; Boer, J.M.; Beverloo, H.B.; Moorhouse, M.J.; van der Spek, P.J.; Lowenberg, B.; et al. Prognostically useful gene-expression profiles in acute myeloid leukemia. N. Engl. J. Med. 2004, 350, 1617–1628. [Google Scholar] [CrossRef] [PubMed]
- Wouters, B.J.; Jorda, M.A.; Keeshan, K.; Louwers, I.; Erpelinck-Verschueren, C.A.; Tielemans, D.; Langerak, A.W.; He, Y.; Yashiro-Ohtani, Y.; Zhang, P.; et al. Distinct gene expression profiles of acute myeloid/T-lymphoid leukemia with silenced CEBPA and mutations in NOTCH1. Blood 2007, 110, 3706–3714. [Google Scholar] [CrossRef] [PubMed]
- Balgobind, B.V.; Zwaan, C.M.; Reinhardt, D.; Arentsen-Peters, T.J.; Hollink, I.H.; de Haas, V.; Kaspers, G.J.; de Bont, E.S.; Baruchel, A.; Stary, J.; et al. High BRE expression in pediatric MLL-rearranged AML is associated with favorable outcome. Leukemia 2010, 24, 2048–2055. [Google Scholar] [CrossRef] [PubMed]
- Kuipers, J.E.; Coenen, E.A.; Balgobind, B.V.; Stary, J.; Baruchel, A.; de Haas, V.; de Bont, E.S.; Reinhardt, D.; Kaspers, G.J.; Cloos, J.; et al. High IGSF4 expression in pediatric M5 acute myeloid leukemia with t(9;11)(p22;q23). Blood 2011, 117, 928–935. [Google Scholar] [CrossRef] [PubMed]
- Ding, L.; Ley, T.J.; Larson, D.E.; Miller, C.A.; Koboldt, D.C.; Welch, J.S.; Ritchey, J.K.; Young, M.A.; Lamprecht, T.; McLellan, M.D.; et al. Clonal evolution in relapsed acute myeloid leukaemia revealed by whole-genome sequencing. Nature 2012, 481, 506–510. [Google Scholar] [CrossRef] [PubMed]
- Meshinchi, S.R.R.; Trevino, L.R.; Hampton, O.A.; Alonzo, T.A.; Farrar, J.E.; Guidry Auvil, J.M.; Davidsen, T.M.; Gesuwan, P.; Muzny, D.M.; Gamis, A.S.; et al. Identification of Novel Somatic Mutations, Regions of Recurrent Loss of Heterozygosity (LOH) and Significant Clonal Evolution From Diagnosis to Relapse in Childhood AML Determined by Exome Capture Sequencing-an NCI/COG Target AML Study. 2012. Available online: https://ash.confex.com/ash/2012/webprogram/Paper51517.html (accessed on 15 December 2014).
- Kohlmann, A.M.G.; Hofmann, W.-K.; Kronnie, G.; Chiaretti, C.; Preudhomme, C.; Tagliafico, E.; Hernandez, J.; Gabriel, C.; Lion, T.; Vandenberghe, P.; et al. The Interlaboratory Robustness of Next-Generation Sequencing (IRON) Study Phase II: Deep-Sequencing Analyses of Hematological Malignancies Performed by an International Network Involving 26 Laboratories. 2012. Available online: https://ash.confex.com/ash/2012/webprogram/Paper49866.html (accessed on 15 December 2014).
- Kohlmann, A.W.S.; Schoeck, U.; Grossmann, V.; Kern, W.; Haferlach, C.; Schnittger, S.; Haferlach, T. First Results of a 31-Gene Panel Targeted to Investigate Myeloid Malignancies by Next-Generation Amplicon Deep-Sequencing. 2012. Available online: https://ash.confex.com/ash/2012/webprogram/Paper48970.html (accessed on 15 December 2014).
- Figueroa, M.E.; Lugthart, S.; Li, Y.; Erpelinck-Verschueren, C.; Deng, X.; Christos, P.J.; Schifano, E.; Booth, J.; van Putten, W.; Skrabanek, L.; et al. DNA methylation signatures identify biologically distinct subtypes in acute myeloid leukemia. Cancer Cell 2010, 17, 13–27. [Google Scholar] [CrossRef] [PubMed]
- Juhl-Christensen, C.; Ommen, H.B.; Aggerholm, A.; Lausen, B.; Kjeldsen, E.; Hasle, H.; Hokland, P. Genetic and epigenetic similarities and differences between childhood and adult AML. Pediatr Blood Cancer 2012, 58, 525–531. [Google Scholar] [CrossRef] [PubMed]
- Lu, J.; Getz, G.; Miska, E.A.; Alvarez-Saavedra, E.; Lamb, J.; Peck, D.; Sweet-Cordero, A.; Ebert, B.L.; Mak, R.H.; Ferrando, A.A.; et al. MicroRNA expression profiles classify human cancers. Nature 2005, 435, 834–838. [Google Scholar] [CrossRef] [PubMed]
- Jongen-Lavrencic, M.; Sun, S.M.; Dijkstra, M.K.; Valk, P.J.; Lowenberg, B. MicroRNA expression profiling in relation to the genetic heterogeneity of acute myeloid leukemia. Blood 2008, 111, 5078–5085. [Google Scholar] [CrossRef] [PubMed]
- Garzon, R.; Volinia, S.; Liu, C.G.; Fernandez-Cymering, C.; Palumbo, T.; Pichiorri, F.; Fabbri, M.; Coombes, K.; Alder, H.; Nakamura, T.; et al. MicroRNA signatures associated with cytogenetics and prognosis in acute myeloid leukemia. Blood 2008, 111, 3183–3189. [Google Scholar] [CrossRef] [PubMed]
- Debernardi, S.; Skoulakis, S.; Molloy, G.; Chaplin, T.; Dixon-McIver, A.; Young, B.D. MicroRNA miR-181a correlates with morphological sub-class of acute myeloid leukaemia and the expression of its target genes in global genome-wide analysis. Leukemia 2007, 21, 912–916. [Google Scholar] [PubMed]
- Danen-van Oorschot, A.A.; Kuipers, J.E.; Arentsen-Peters, S.; Schotte, D.; de Haas, V.; Trka, J.; Baruchel, A.; Reinhardt, D.; Pieters, R.; Zwaan, C.M.; et al. Differentially expressed miRNAs in cytogenetic and molecular subtypes of pediatric acute myeloid leukemia. Pediatr. Blood Cancer 2012, 58, 715–721. [Google Scholar] [CrossRef] [PubMed]
- Zarrinkar, P.P.; Gunawardane, R.N.; Cramer, M.D.; Gardner, M.F.; Brigham, D.; Belli, B.; Karaman, M.W.; Pratz, K.W.; Pallares, G.; Chao, Q.; et al. AC220 is a uniquely potent and selective inhibitor of FLT3 for the treatment of acute myeloid leukemia (AML). Blood 2009, 114, 2984–2992. [Google Scholar] [CrossRef] [PubMed]
- Inaba, H.; Rubnitz, J.E.; Coustan-Smith, E.; Li, L.; Furmanski, B.D.; Mascara, G.P.; Heym, K.M.; Christensen, R.; Onciu, M.; Shurtleff, S.A.; et al. Phase I pharmacokinetic and pharmacodynamic study of the multikinase inhibitor sorafenib in combination with clofarabine and cytarabine in pediatric relapsed/refractory leukemia. J. Clin. Oncol. 2011, 29, 3293–3300. [Google Scholar] [CrossRef] [PubMed]
- Watt, T.C.; Cooper, T. Sorafenib as treatment for relapsed or refractory pediatric acute myelogenous leukemia. Pediatr. Blood Cancer 2012, 59, 756–757. [Google Scholar] [CrossRef] [PubMed]
- Levis, M.; Ravandi, F.; Wang, E.S.; Baer, M.R.; Perl, A.; Coutre, S.; Erba, H.; Stuart, R.K.; Baccarani, M.; Cripe, L.D.; et al. Results from a randomized trial of salvage chemotherapy followed by lestaurtinib for patients with FLT3 mutant AML in first relapse. Blood 2011, 117, 3294–3301. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.C.; Wang, Q.; Chin, C.S.; Salerno, S.; Damon, L.E.; Levis, M.J.; Perl, A.E.; Travers, K.J.; Wang, S.; Hunt, J.P.; et al. Validation of ITD mutations in FLT3 as a therapeutic target in human acute myeloid leukaemia. Nature 2012, 485, 260–263. [Google Scholar] [CrossRef] [PubMed]
- The world’s chilhood cancer experts. Available online: http://www.childrensoncologygroup.org/index.php/aaml1031 (accessed on 15 December 2014).
- Goemans, B.F.; Zwaan, C.M.; Miller, M.; Zimmermann, M.; Harlow, A.; Meshinchi, S.; Loonen, A.H.; Hahlen, K.; Reinhardt, D.; Creutzig, U.; et al. Mutations in KIT and RAS are frequent events in pediatric core-binding factor acute myeloid leukemia. Leukemia 2005, 19, 1536–1542. [Google Scholar] [CrossRef] [PubMed]
- Zwaan, C.M.; Rizzari, C.; Mechinaud, F.; Lancaster, D.L.; Lehrnbecher, T.; van der Velden, V.H.; Beverloo, B.B.; den Boer, M.L.; Pieters, R.; Reinhardt, D.; et al. Dasatinib in children and adolescents with relapsed or refractory leukemia: Results of the CA180–018 phase I dose-escalation study of the Innovative Therapies for Children with Cancer Consortium. J. Clin. Oncol. 2013, 31, 2460–2468. [Google Scholar] [CrossRef] [PubMed]
- Marcucci, G.G.S.; Zhao, J.; Carrol, A.J.; Bucci, D.; Vij, R.; Blum, W.; Pardee, T.; Wetzler, M.; Stock, W.; Bloomfield, C.D.; et al. Adding The KIT Inhibitor Dasatinib (DAS) To Standard Induction and Consolidation Therapy For Newly Diagnosed Patients (pts) With Core Binding Factor (CBF) Acute Myeloid Leukemia (AML): Initial Results Of The CALGB 10801 (Alliance) Study. 2013. Available online: https://ash.confex.com/ash/2013/webprogram/Paper63516.html (accessed on 15 December 2014).
- Burnett, A.K.; Russell, N.H.; Culligan, D.; Cavanagh, J.; Kell, J.; Wheatley, K.; Virchis, A.; Hills, R.K.; Milligan, D.; Institute AMLWGotUNCR. The addition of the farnesyl transferase inhibitor, tipifarnib, to low dose cytarabine does not improve outcome for older patients with AML. Br. J. Haematol. 2012, 158, 519–522. [Google Scholar] [CrossRef] [PubMed]
- Lamba, S.; Russo, M.; Sun, C.; Lazzari, L.; Cancelliere, C.; Grernrum, W.; Lieftink, C.; Bernards, R.; di Nicolantonio, F.; Bardelli, A. RAF Suppression Synergizes with MEK Inhibition in KRAS Mutant Cancer Cells. Cell Rep. 2014, 8, 1475–1483. [Google Scholar] [CrossRef] [PubMed]
- Sun, C.; Hobor, S.; Bertotti, A.; Zecchin, D.; Huang, S.; Galimi, F.; Cottino, F.; Prahallad, A.; Grernrum, W.; Tzani, A.; et al. Intrinsic resistance to MEK inhibition in KRAS mutant lung and colon cancer through transcriptional induction of ERBB3. Cell Rep. 2014, 7, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Deshpande, A.J.; Chen, L.; Fazio, M.; Sinha, A.U.; Bernt, K.M.; Banka, D.; Dias, S.; Chang, J.; Olhava, E.J.; Daigle, S.R.; et al. Leukemic transformation by the MLL-AF6 fusion oncogene requires the H3K79 methyltransferase Dot1l. Blood 2013, 121, 2533–2541. [Google Scholar] [CrossRef] [PubMed]
- O’Hear, C.; Inaba, H.; Pounds, S.; Shi, L.; Dahl, G.; Bowman, W.P.; Taub, J.W.; Pui, C.H.; Ribeiro, R.C.; Coustan-Smith, E.; et al. Gemtuzumab ozogamicin can reduce minimal residual disease in patients with childhood acute myeloid leukemia. Cancer 2013, 119, 4036–4043. [Google Scholar] [CrossRef] [PubMed]
- Petersdorf, S.H.; Kopecky, K.J.; Slovak, M.; Willman, C.; Nevill, T.; Brandwein, J.; Larson, R.A.; Erba, H.P.; Stiff, P.J.; Stuart, R.K.; et al. A phase 3 study of gemtuzumab ozogamicin during induction and postconsolidation therapy in younger patients with acute myeloid leukemia. Blood 2013, 121, 4854–4860. [Google Scholar] [CrossRef] [PubMed]
- Zwaan, C.M.; Reinhardt, D.; Zimmerman, M.; Hasle, H.; Stary, J.; Stark, B.; Dworzak, M.; Creutzig, U.; Kaspers, G.J.; International BFMSGoPAML. Salvage treatment for children with refractory first or second relapse of acute myeloid leukaemia with gemtuzumab ozogamicin: Results of a phase II study. Br. J. Haematol. 2010, 148, 768–776. [Google Scholar] [CrossRef] [PubMed]
- Hasle, H.; Abrahamsson, J.; Forestier, E.; Ha, S.Y.; Heldrup, J.; Jahnukainen, K.; Jonsson, O.G.; Lausen, B.; Palle, J.; Zeller, B.; et al. Gemtuzumab ozogamicin as postconsolidation therapy does not prevent relapse in children with AML: Results from NOPHO-AML 2004. Blood 2012, 120, 978–984. [Google Scholar] [CrossRef] [PubMed]
- Jeha, S.; Razzouk, B.; Rytting, M.; Rheingold, S.; Albano, E.; Kadota, R.; Luchtman-Jones, L.; Bomgaars, L.; Gaynon, P.; Goldman, S.; et al. Phase II study of clofarabine in pediatric patients with refractory or relapsed acute myeloid leukemia. J. Clin. Oncol. 2009, 27, 4392–4397. [Google Scholar] [CrossRef] [PubMed]
- Cooper, T.M.; Alonzo, T.A.; Gerbing, R.B.; Perentesis, J.P.; Whitlock, J.A.; Taub, J.W.; Horton, T.M.; Gamis, A.S.; Meshinchi, S.; Loken, M.R.; et al. AAML0523: A report from the Children’s Oncology Group on the efficacy of clofarabine in combination with cytarabine in pediatric patients with recurrent acute myeloid leukemia. Cancer 2014, 120, 2482–2489. [Google Scholar] [CrossRef] [PubMed]
- Hijiya, N.; Thomson, B.; Isakoff, M.S.; Silverman, L.B.; Steinherz, P.G.; Borowitz, M.J.; Kadota, R.; Cooper, T.; Shen, V.; Dahl, G.; et al. Phase 2 trial of clofarabine in combination with etoposide and cyclophosphamide in pediatric patients with refractory or relapsed acute lymphoblastic leukemia. Blood 2011, 118, 6043–6049. [Google Scholar] [CrossRef] [PubMed]
- Shukla, N.; Kobos, R.; Renaud, T.; Steinherz, L.J.; Steinherz, P.G. Phase II trial of clofarabine with topotecan, vinorelbine, and thiotepa in pediatric patients with relapsed or refractory acute leukemia. Pediatr. Blood Cancer 2014, 61, 431–435. [Google Scholar] [CrossRef] [PubMed]
- Leonard, S.M.; Perry, T.; Woodman, C.B.; Kearns, P. Sequential treatment with cytarabine and decitabine has an increased anti-leukemia effect compared to cytarabine alone in xenograft models of childhood acute myeloid leukemia. PLoS One 2014, 9, e87475. [Google Scholar] [CrossRef] [PubMed]
- Phillips, C.L.; Davies, S.M.; McMasters, R.; Absalon, M.; O’Brien, M.; Mo, J.; Broun, R.; Moscow, J.A.; Smolarek, T.; Garzon, R.; et al. Low dose decitabine in very high risk relapsed or refractory acute myeloid leukaemia in children and young adults. Br. J. Haematol. 2013, 161, 406–410. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.G.; Kim, I.; Yoon, S.S.; Park, S.; Cheong, J.W.; Min, Y.H.; Lee, J.O.; Bang, S.M.; Yi, H.G.; Kim, C.S.; et al. Comparative analysis between azacitidine and decitabine for the treatment of myelodysplastic syndromes. Br. J. Haematol. 2013, 161, 339–347. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Rooij, J.D.E.; Zwaan, C.M.; Van den Heuvel-Eibrink, M. Pediatric AML: From Biology to Clinical Management. J. Clin. Med. 2015, 4, 127-149. https://doi.org/10.3390/jcm4010127
De Rooij JDE, Zwaan CM, Van den Heuvel-Eibrink M. Pediatric AML: From Biology to Clinical Management. Journal of Clinical Medicine. 2015; 4(1):127-149. https://doi.org/10.3390/jcm4010127
Chicago/Turabian StyleDe Rooij, Jasmijn D. E., C. Michel Zwaan, and Marry Van den Heuvel-Eibrink. 2015. "Pediatric AML: From Biology to Clinical Management" Journal of Clinical Medicine 4, no. 1: 127-149. https://doi.org/10.3390/jcm4010127
APA StyleDe Rooij, J. D. E., Zwaan, C. M., & Van den Heuvel-Eibrink, M. (2015). Pediatric AML: From Biology to Clinical Management. Journal of Clinical Medicine, 4(1), 127-149. https://doi.org/10.3390/jcm4010127





