Simple Summary
A retrospective multicentric study of 322 patients with head and neck cancers of unknown primary (HNCUP) was performed testing the impact of neck dissection (ND) extent on nodal relapse, progression-free survival and survival. After 5 years, the incidence of nodal relapse was 13.4%, and progression-free survival (PFS) was 59.1%. In multivariate analysis after adjusting for nodal stage, the risk of nodal relapse or progression was reduced with lymphadenectomy, selective ND or radical/modified ND but survival rates were similar. Patients undergoing lymphadenectomy or ND had significantly better PFS and a lower nodal relapse incidence in the N1 + N2a group, but the improvement was not significant for the N2b or N2 + N3c patients. Severe toxicity rates exceeded 40% with radical ND. In HNCUP, ND improves PFS regardless of nodal stage but fails to improve survival. The magnitude of the benefit of ND did not appear to depend on ND extent and decreased with a more advanced nodal stage.
Abstract
Purpose: Management of head and neck cancers of unknown primary (HNCUP) combines neck dissection (ND) and radiotherapy, with or without chemotherapy. The prognostic value of ND has hardly been studied in HNCUP. Methods: A retrospective multicentric study assessed the impact of ND extent (adenectomy, selective ND, radical/radical-modified ND) on nodal relapse, progression-free survival (PFS) or survival, taking into account nodal stage. Results: 53 patients (16.5%) had no ND, 33 (10.2%) had lymphadenectomy, 116 (36.0%) underwent selective ND and 120 underwent radical/radical-modified ND (37.3%), 15 of which received radical ND (4.7%). With a 34-month median follow-up, the 3-year incidence of nodal relapse was 12.5% and progression-free survival (PFS) 69.1%. In multivariate analysis after adjusting for nodal stage, the risk of nodal relapse or progression was reduced with lymphadenectomy, selective or radical/modified ND, but survival rates were similar. Patients undergoing lymphadenectomy or ND had a better PFS and lowered nodal relapse incidence in the N1 + N2a group, but the improvement was not significant for the N2b or N2 + N3c patients. Severe toxicity rates exceeded 40% with radical ND. Conclusion: In HNCUP, ND improves PFS, regardless of nodal stage. The magnitude of the benefit of ND does not appear to depend on ND extent and decreases with a more advanced nodal stage.
1. Introduction
Optimal neck management for patients with head and neck cancer of unknown primary (HNCUP) is still controversial [1]. The American Association of Clinical Oncology (ASCO) guidelines and the US National Comprehensive Cancer Network (NCCN) recommend performing, for small-volume nodal disease, either definitive surgery or radiotherapy (with or without chemotherapy). For higher nodal stages or unresectable lymphadenopathies, they recommend definitive chemoradiotherapy, given the increased morbidity of trimodality therapy, including extensive neck dissection (ND) in advanced nodal disease [2,3]. According to French and British guidelines, current practice is to perform ND as first-line therapy for removable neck lymph nodes followed by adjuvant (chemo) radiotherapy [4,5]. ASCO and NCCN guidelines recommend limiting the treatment of small nodes to a single modality (surgery or radiotherapy). In HNCUP [6,7,8], there is insufficient evidence to prove the effects of ND on nodal control. In the mother publication of the current study by Pflumio et al., of 350 patients, 74.5% had unilateral disease and more than two-thirds of them had bilateral irradiation. The main objective of the study was to address the role of nodal and mucosal irradiation with an original hypothesis that unilateral irradiation would be responsible for 15% more relapses than bilateral irradiation. We showed that the regional control rate and occurrence of mucosal primaries did not differ between patients who had unilateral irradiation and those who had bilateral irradiation, and that severe toxicities were more frequent after bilateral than unilateral irradiation. Moreover, we found that ND improved locoregional control but not survival without addressing the specific role of ND by nodal stage and extent of ND.
To date, ND in combination with adjuvant radiotherapy has not been shown to improve overall survival in HNCUP in comparison with definitive radiotherapy [9,10]. De-intensification at nodal recurrence has evolved toward selective ND and appears to be as effective as modified or radical ND [11]. Moreover, the treatment of HNCUP is evolving toward more selective ND and personalization of radiotherapy volumes [12,13]. For bulky nodes, none of the ASCO, NCCN and British guidelines specifically define nodal resectability criteria.
The aim of our study was to investigate whether ND improved progression-free survival and to what extent it correlated with the extent of ND (selective to radical) and nodal stage in HNCUP patients treated by radiotherapy/chemoradiotherapy.
2. Materials and Methods
This multicenter retrospective international study included patients with squamous cell HNCUP diagnosed by nodal fine-needle aspiration (FNA), biopsy, lymphadenectomy or dissection, treated between 2000 and 2015 in 20 health centers from France, Italy and the United States. Exclusion criteria were history of head and neck cancer, history of skin cancer and initial metastatic disease. All the patients underwent nodal and mucosal irradiation (adapted to the site of nodes and their lymphatic drainage from the nasopharynx, oropharynx, hypopharynx, larynx or oral cavity). Radiation therapy was by conformal (3D) or intensity-modulated radiotherapy (IMRT) and was performed with cisplatin when indicated. Patients underwent upfront ND or planned ND after radiotherapy [14]. ND was classified into four types: radical ND, in which spinal nerve (XI), sternocleidomastoid muscle and internal jugular vein were removed; radical-modified ND, in which one or two of these structures were preserved; selective ND, in which all three structures were preserved [14]; as well as lymphadenectomy, where the pathologic node was removed. Additional grouping of cases into N1 + N2a (early-stage and favorable prognosis), N2b (intermediate prognosis) and N2c + N3 (advanced stage and unfavorable prognosis) was performed based on pre-established prognostic groups as in the mother study [13]. It was also helpful, for statistical purposes, to allow sufficiently large groups and powerful estimates. Moreover, involvement of the internal jugular vein, the sternocleidomastoid muscle or cervical nerves could lead to relatively radical neck dissection independently of nodal size. Patients with no information on clinical nodal stage or ND extent were excluded.
Follow-up was performed in accordance with the recommendations of the French Society of Otorhinolaryngology (SFORL) [15] and international NCCN recommendations. Disease evaluations were performed using clinical examination. PET-CT was performed at 12 weeks in case of an equivocal response to radiotherapy, on a case-by-case scenario in the early years of the study and systematically after the publication of the PET-neck study [16]. Local relapses were defined as the emergence of primary mucosal carcinoma of the upper aerodigestive tract and regional relapse as nodal persistence or recurrence. Progression-free survival (PFS) was defined as the time between the date of diagnosis and the date of first recurrence or death, whatever the cause. HNCUP-specific survival was calculated using data from patients who died from HNCUP. For HNCUP-specific survival, we only considered death due to head and neck cancer, and death due to other causes was considered as a competing risk [17,18]. Overall survival (OS) was defined as the time between diagnosis and all-cause death. Severe acute and late toxicities were graded using the National Cancer Institute Common Terminology Criteria for Adverse Events, Version 3.0. Patient, tumor and treatment characteristics, as well as information regarding local, regional and metastatic relapses, were collected as electronic report forms (www.easy-crf.com, accessed on 25 January 2021) based on patient medical records. This study is an ancillary of AMBICUP [13] and was approved by comité de protection des personnes (no. 13/26), Commission nationale de l’informatique et des libertés (CNIL) (National Reference: MMS/SBA/AR148528) and Comité consultatif en matière de recherche dans le domaine de la santé (no. 13.753). In addition, ethical approval was obtained for patient accrual in each participating country according to their own rules.
Statistics: Qualitative variables were described as the frequency and percentage. Quantitative variables were described as their median and interquartile range (IQR), or their mean and their standard deviation. The normality of the distribution was assessed by the Shapiro–Wilk test. Chi-square tests or Fisher exact tests were performed for the comparison of qualitative parameters. ANOVA t-tests or Kruskal–Wallis tests were carried out for quantitative parameters according to the normality of the distribution. Local and regional relapses were described according to the Fine and Gray model (FGm), with other relapses and death as competing risks. Metastatic relapse was described with the FGm with death as a competing risk. The Kaplan–Meier method was used to describe PFS and overall survival.
Independent prognostic factors were first investigated by bivariate analysis based on FGm for relapses or HNCUP-specific death and on the Cox proportional hazard model for PFS. Nodal stage, whatever its level of significance, and all parameters with a p-value of less than 0.1 in the bivariate analysis were included in a full multivariate model. In order to avoid overfitting, this full model was simplified with backward selection. Nodal stage was included in each model during the model selection procedure to take into account potential selection biases (i.e., the choice of ND extent could be performed according to nodal stage). Only parameters with a p-value of less than 0.05 after adjustment for nodal stage were kept in the final reduced multivariate model. Results were expressed as adjusted hazard ratio and 95% confidence interval (95% CI). For each nodal stage separately, the incidence of nodal relapse and PFS were described according to ND extent and were compared using the Gray test and log-rank tests, respectively.
Toxicities were compared across the groups (by separating modified radical and radical ND) with Chi-squared test or Fisher exact test; a sensitivity analysis was performed in the subgroup of patients with bilateral nodal irradiation. All statistical analyses were performed using SAS software (SAS Institute Inc., Cary, NC, USA). p-values of less than 0.05 were considered statistically significant.
3. Results
Out of the 350 patients of the AMBICUP study who underwent radiotherapy for HNCUP [14], 322 patients with comprehensive information on both clinical nodal stage and ND extent were analyzed. There were 271 males (84.2%), and the mean age was 62.3 +/− 10.3 years. A total of 53 patients (16.5%) had no ND, 33 (10.2%) had lymphadenectomy, 116 (36.0%) underwent selective ND and 120 underwent modified or radical ND (37.3%), 15 of which received radical ND (4.7%). Patient and tumor characteristics are reported in Table 1. ND extent was associated with clinical nodal stage (Table 1, p < 0.001). Patients without ND had a higher clinical nodal stage (p = 0.003).

Table 1.
Patient and tumor characteristics.
A total of 33 patients out of 322 patients underwent neoadjuvant chemotherapy: 24/53 (45.3%) in the group with no ND versus 9 (<10%) in patients undergoing lymphadenectomy or ND (p < 0.001). A total of 42 patients (79.2%) not undergoing ND, 25 patients (76.8%) undergoing lymphadenectomy, 64 patients (55.2%) undergoing selective ND and 70 patients (58.8%) undergoing modified radical/ radical ND also had chemotherapy in association with RT (p = 0.007). Characteristics of antineoplastic treatments are reported in Table S1.
The median follow-up was 34 months, IQR (17–60). The 3-year overall survival was 78.8%, 95% CI (73.3–83.3).
The 3-year incidence of local (mucosal) relapse was 5.8%, 95% CI (3.5–8.9). ND had no significant impact on mucosal relapse (Table 2). In multivariate analysis, after adjustment on clinical nodal stage, mucosal RT was a protective factor against mucosal relapse (Table 2).

Table 2.
Prognostic factors of local (mucosal), nodal and metastatic relapse of HNCUP in bivariate and multivariate analysis, using the Fine and Gray model for competitive factors.
The 3-year incidence of nodal relapse was 12.5% (95% CI (9.0–16.6)). ND was a protective factor against nodal relapse whatever the extent of ND in bivariate analysis (Table 2). In multivariate analysis, the risk of nodal relapse was reduced with lymphadenectomy (HR = 0.20, 95% CI (0.05; 0.85)), selective ND (HR = 0.20, 95% CI (0.08; 0.51)) or modified/radical ND (HR = 0.40, 95% CI (0.19; 0.83)) whereas N2c-N3 nodes and ≥4-day interruptions of radiotherapy were risk factors for nodal relapse (HR = 2.62, 95% CI (1.06; 6.48) and HR = 3.84, 95% CI (1.71; 8.62), respectively). Impact of ND extent on each nodal stage is presented in Figure 1. Lymphadenectomy or ND significantly decreased the risk of nodal relapse for N1 + N2a patients (p = 0.001) but not significantly for N2b or N2 + N3c patients (p = 0.682 and p = 0.053, respectively).
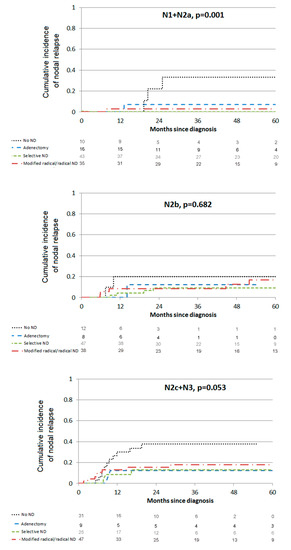
Figure 1.
Relapse node.
The 3-year incidence of metastatic relapse was 14.2%, 95% CI (10.5–18.5). ND had no impact on metastatic relapse (Table 2). In multivariate analysis, after adjustment on clinical nodal stage, the incidence of metastatic relapse increased with the largest node diameter (HR = 1.05, 95% CI (1.02–1.08)) whereas initial 18-FDG PET-CT was associated with a lower probability of metastases during follow-up (HR = 0.46, 95% CI (0.24; 0.89)) (Table 2).
The 3-year PFS was 69.1%, 95% CI (63.3–74.1). In multivariate analysis (Table 3), PFS was poorer in patients with N2b (HR = 1.99, 95% CI (1.18; 3.36)) and N2c-N3 nodes (HR = 3.00, 95% CI (1.83; 4.92)) whereas the PFS was improved with lymphadenectomy (HR=0.29, 95% CI (0.19; 0.67)), selective ND (HR = 0.35, 95% CI (0.21; 0.59)) or modified/radical ND (HR = 0.43, 95% CI (0.27; 0.69)). Prophylactic mucosal radiotherapy was a protective factor (HR = 0.41, 95% CI (0.25; 0.67)) as well as an initial 18-FDG PET-CT (HR = 0.56, 95% CI (0.36; 0.86)). Impact of ND extent for each nodal stage is presented in Figure 2. Patients undergoing lymphadenectomy or ND had significantly better PFS in the N1 + N2a group (p = 0.030) but PFS improvement was not significant for N2b or N2 + N3c patients (p = 0.206 and p = 0.062, respectively).

Table 3.
Prognostic factors of progression-free survival and HNCUP-specific death in bivariate and multivariate analysis, using the Fine and Gray model for competitive factors.
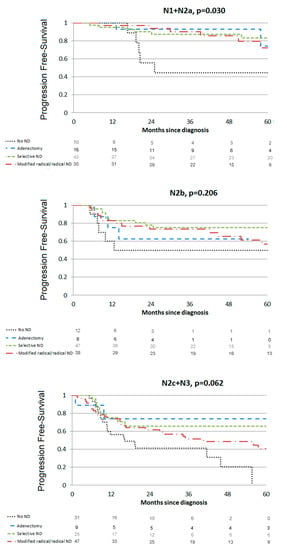
Figure 2.
Progression-free survival.
The 3-year HNCUP-specific death incidence was 16.8%, 95% CI (12.6–21.6). In bivariate analysis, ND, whatever the extent, was a protective factor on HNCUP-specific death (Figure S1), but it did not remain statistically significant in multivariate analysis after adjustment for nodal stage (Table 3). In multivariate analysis, the incidence of HNCUP-specific death was higher for patients with nodes ≥ N2c (HR = 2.55, 95% CI (1.26; 5.15)), with neoadjuvant chemotherapy (HR = 2.45, 95% CI (1.16; 5.18)) and with ≥4-day interruptions of radiotherapy (HR = 3.86, 95% CI (1.75; 8.53)). The incidence of HNCUP-specific death also increased with the largest node diameter (HR = 1.06, 95% CI (1.03; 1.09)) whereas an initial 18-FDG PET-CT was a protector (HR = 0.44, 95% CI (0.24; 0.83)).
Treatment-associated toxicities were more frequent after radical ND than after selective or modified radical ND (Table 4). Toxicity rates were similar between selective ND and no ND. In contrast, radical ND toxicity rates (≥40%) were at least two times higher than with radical-modified ND for late dysphagia and pain. Within the subgroup of the 232 patients with bilateral nodal irradiation, the results were similar (Table S2).

Table 4.
Impact of neck dissection on grade III-IV acute and late toxicities.
4. Discussion
This multicentric retrospective study included 322 patients of a relatively rare subgroup [13,19,20] of head and neck cancer patients with a median follow-up of at least 3 years. This population of patients is very rarely included in clinical trials.
Advanced stage and no neck dissection were associated with poorer regional control in the mother paper [13]. Better local control was reported with mucosal RT, and bilateral nodal irradiation yielded non-significant better nodal and mucosal control rates. The current study, therefore, focused on the impact of ND by nodal stages on oncologic outcomes. ND in combination with radiotherapy improved nodal control and PFS in HNCUP, and this was so for all nodal stages. Advanced nodal presentation was not compensated for by neoadjuvant chemotherapy. Adapted neck management from lymphadenectomy alone, which might be considered as hyper-selective ND, to radical ND, is based on clinical nodal stage and patient-related factors. Interestingly, a benefit of ND on nodal relapse and PFS was achieved with such a strategy. However, patients with advanced nodal stage, i.e., ≥ N2b nodes, did not benefit as much from ND as N1-N2a stages with respect to nodal relapse or PFS.
Lymphadenectomy is not recommended and is usually not considered as ND. However, this is a very intriguing observation of our study and this group (size sufficient for statistics) that we felt it was interesting to show as an exploratory finding that pushes the limits of ND toward even more than hyper-selective ND.
It should be noted that non-resectability and nodal kinetics are uneasily collected items. This is not only true in retrospective databases but also in clinical trials due to the lack of standardization of the definitions. This may reflect some heterogeneity in terms of resectability for the very advanced stages in our study. This might also explain some of the large differences observed between published studies. Demiroz et al. and Colletier et al. found no benefit from ND in locoregional control in comparison with chemoradiation alone, in their small retrospective studies [10,21]. In Colletier’s study, most patients had low nodal stages N1 and N2a (n = 80, 58%), and all nodal relapses occurred in patients who initially had extracapsular spread (n = 12). Other small to medium-size studies have reported better PFS but not better survival [22,23]. Further to our observation, French GETTEC guidelines for resectability criteria have been published to better assess the arguments for ND and the impact of strategies using ND [24].
Patients with N2b-to-N3 nodes had higher rates of HNCUP-specific death, and specific survival was similar in patients with or without ND in our study. In the meta-analysis of Balaker et al., patients undergoing radiotherapy/chemoradiotherapy with ND or without had a 5-year overall survival of 52.4%, compared to 46.6% [9], as in most studies [10,12,19,21,22,23,25,26]. An improvement of survival in patients with ND was shown in two studies only [27,28].
In the mother study [13], severe toxicities were more frequent after bilateral irradiation than unilateral irradiation. In the present study, treatment-related toxicities were more frequent after radical ND than modified radical ND or selective ND and lymphadenectomy. In a sensitivity analysis, we found that treatment-related toxicities were also more frequent for radical ND in the subgroup of patients with more toxicities, i.e., with bilateral radiotherapy. These results suggest that both radical ND and bilateral irradiation induce more toxicities. Altogether, and despite limitations of retrospective studies, our observations may also suggest that adapted ND was efficient across all nodal stages but was less efficient in controlling the nodal and metastatic disease. One intriguing new observation was that lymphadenectomy alone was also beneficial. Although lymphadenectomy is usually considered a diagnostic procedure, this observation suggests that it might be equivalent to hyper-selective ND. This should be investigated further before any therapeutic change is indicated.
Chemotherapy was associated with poor prognosis, suggesting that it did not compensate for advanced nodal stage and the associated risk of metastases. New systemic treatments and additional locoregional treatments, with new approaches such as nanoparticles in large nodes, might be worth being investigated.
In our study, prognostic factors for locoregional relapse, PFS and HNCUP-specific death included an interval of more than 10 weeks between diagnosis and radiotherapy. In head and neck cancers, the longer the delay between initial surgery and adjuvant radiotherapy, the shorter the survival [28,29,30]. The PET-CT prognostic value for HNCUP-specific in our study probably indicated better detection of synchronous metastatic lesions [11,19,29,31,32,33] (and further exclusion of these patients from our studies). It was performed on 20% of patients before 2005 only, 42% in 2005 and 95% after 2006 [13]. PET-CT has also become a standard of care for patients with residual nodes after chemoradiation. Mehanna et al. showed that survival was similar among N2-3 patients who underwent PET-CT-guided surveillance and those who underwent planned ND [33,34,35].
The main limitations of this retrospective study include inaccurate criteria for resectability and inaccurate assessment of the quality of ND (the number of resected nodes was not recorded) [27]. Differences in nodal stage and age were identified between operated and non-operated groups, suggesting unfair comparison. To address this bias, a propensity score analysis was performed (supplementary data). While tonsillectomy was the rule at the time of study, tongue-base biopsies and endoscopically-guided mucosectomies are increasingly used to maximize the chances of non-clinical primary diagnosis, suggesting that some HNCUP may indeed be small oropharyngeal primaries [36,37]. Similarly, HPV and Epstein–Barr virus (EBV) testing have been recommended as systematic in HNCUP only by the latest Union for International Cancer Control (UICC) TNM classification (8th TNM 2017) update. HPV and EBV testing were not feasible due to a lack of specific funding for translational analyses on >300 patients. Of note, p16 staining has only become broadly systematic in France since 2018 for oropharyngeal primaries. This may be different in the USA and in Northern countries [38] where the prevalence of HPV-positive oropharyngeal primaries is higher than in France and Italy. Motz et al. and Schroeder et al. reported that the frequency of HNCUP increased significantly in the past decade and was related to the incidence of HPV [39,40]. Therefore, updates from large HNCUP studies will be useful to compare outcomes with these new practices to those of the current study.
5. Conclusions
In patients with HNCUP, ND in combination with radiotherapy improves PFS, regardless of nodal stage but fails to improve specific survival. The magnitude of the benefit of ND did not appear to depend on ND extent and decreased with more advanced nodal stage while toxicity rates exceeded 40% with radical ND in our study. New approaches are warranted to improve nodal control and survival in advanced nodal stages of HNCUP.
Supplementary Materials
The following are available online at https://www.mdpi.com/article/10.3390/cancers13102416/s1, Table S1: Impact of neck dissection on grade III-IV acute and late toxicities in the subgroup of the 232 patients with bilateral nodal irradiation, Table S2: Impact of neck dissection on grade III-IV acute and late toxicities in the subgroup of the 232 patients with bilateral nodal irradiation. Figure S1: Incidence of HNCUP specific death according to the extent of ND.
Author Contributions
Y.A.-S., J.S., F.C., X.-S.S., C.P. (Carole Pflumio), I.T., C.P. (Claire Petit), M.C., A.B., V.C., S.S.-V., J.C., J.M., M.K., P.G., E.R., J.K., M.D., N.B., A.C., C.D., S.S., Y.T., V.R., L.G., B.T., D.T.N., J.-C.F. and J.T. contributed to the validation, writing, review, editing and visualization. J.S. and J.T. contributed to the statistics. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board (or Ethics Committee) of CHRU Besancon-Montbeliard (CNIL DR-2014-386, CPP 13/26 11252013, CTTIRS N13.753).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author.
Acknowledgments
Centre hospitalier universitaire de Besançon—Centre hospitalier de Belfort-Montbéliard for regulatory affairs and Institut de cancérologie de Lorraine for financial support. Camille Vidaud (French head and neck, InterGroup) for her help coordinating and editing the manuscript.
Conflicts of Interest
The authors declare no conflict of interest.
References
- Waltonen, J.D.; Ozer, E.; Hall, N.C.; Schuller, D.E.; Agrawal, A. Metastatic Carcinoma of the Neck of Unknown Primary Origin: Evolution and Efficacy of the Modern Workup. Arch. Otolaryngol. Head Neck Surg. 2009, 135, 1024–1029. [Google Scholar] [CrossRef]
- NCCN Clinical Pratice Guidelines in Oncology -Head and Neck Cancers 2018.
- Maghami, E.; Ismaila, N.; Alvarez, A.; Chernock, R.; Duvvuri, U.; Geiger, J.; Gross, N.; Haughey, B.; Paul, D.; Rodriguez, C.; et al. Diagnosis and Management of Squamous Cell Carcinoma of Unknown Primary in the Head and Neck: ASCO Guideline. J. Clin. Oncol. 2020, 38, 2570–2596. [Google Scholar] [CrossRef]
- Bugat, R.; Bataillard, A.; Lesimple, T.; Voigt, J.-J.; Culine, S.; Lortholary, A.; Merrouche, Y.; Ganem, G.; Kaminsky, M.C.; Negrier, S.; et al. Standards, Options and Recommendations for the management of patient with carcinoma of unknown primary site. Bull. Cancer 2002, 89, 869–875. [Google Scholar]
- Mackenzie, K.; Watson, M.; Jankowska, P.; Bhide, S.; Simo, R. Investigation and management of the unknown primary with metastatic neck disease: United Kingdom National Multidisciplinary Guidelines. J. Laryngol. Otol. 2016, 130, S170–S175. [Google Scholar] [CrossRef]
- Troussier, I.; Klausner, G.; Blais, E.; Giraud, P.; Lahmi, L.; Pflumio, C.; Faivre, J.C.; Geoffrois, L.; Babin, E.; Morinière, S.; et al. Évolutions dans la prise en charge des métastases ganglionnaires cervicales sans cancer primitif retrouvé: Doses et volumes cibles de la radiothérapie avec modulation d’intensité. Cancer/Radiothérapie 2018, 22, 438–446. [Google Scholar] [CrossRef] [PubMed]
- Arosio, A.D.; Pignataro, L.; Gaini, R.M.; Garavello, W. Neck lymph node metastases from unknown primary. Cancer Treat. Rev. 2017, 53, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Chen, A.M.; Li, B.-Q.; Farwell, D.G.; Marsano, J.; Vijayakumar, S.; Purdy, J.A. Improved Dosimetric and Clinical Outcomes with Intensity-Modulated Radiotherapy for Head-and-Neck Cancer of Unknown Primary Origin. Int. J. Radiat. Oncol. Biol. Phys. 2011, 79, 756–762. [Google Scholar] [CrossRef]
- Balaker, A.E.; Abemayor, E.; Elashoff, D.; St John, M.A. Cancer of unknown primary: Does treatment modality make a difference? Laryngoscope 2012, 122, 1279–1282. [Google Scholar] [CrossRef] [PubMed]
- Demiroz, C.; Vainshtein, J.M.; Koukourakis, G.V.; Gutfeld, O.; Prince, M.E.; Bradford, C.R.; Wolf, G.T.; McLean, S.; Worden, F.P.; Chepeha, D.B.; et al. Head and neck squamous cell carcinoma of unknown primary: Neck dissection and radiotherapy or definitive radiotherapy. Head Neck 2014, 36, 1589–1595. [Google Scholar] [CrossRef] [PubMed]
- Mehanna, H.; Kong, A.; Ahmed, S. Recurrent head and neck cancer: United Kingdom National Multidisciplinary Guidelines. J. Laryngol. Otol. 2016, 130, S181–S190. [Google Scholar] [CrossRef]
- Patel, R.S.; Clark, J.; Wyten, R.; Gao, K.; O’Brien, C.J. Squamous cell carcinoma from an unknown head and neck primary site: A “selective treatment” approach. Arch. Otolaryngol. Head Neck Surg. 2007, 133, 1282–1287. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Pflumio, C.; Troussier, I.; Sun, X.S.; Salleron, J.; Petit, C.; Caubet, M.; Beddok, A.; Calugaru, V.; Servagi-Vernat, S.; Castelli, J.; et al. Unilateral or bilateral irradiation in cervical lymph node metastases of unknown primary? A retrospective cohort study. Eur. J. Cancer 2019, 111, 69–81. [Google Scholar] [CrossRef] [PubMed]
- Robbins, K.T.; Shaha, A.R.; Medina, J.E.; Califano, J.A.; Wolf, G.T.; Ferlito, A.; Som, P.M.; Day, T.A.; Committee for Neck Dissection Classification, American Head and Neck Society. Consensus Statement on the Classification and Terminology of Neck Dissection. Arch. Otolaryngol. Head Neck Surg. 2008, 134, 536. [Google Scholar] [CrossRef]
- Blanchard, D.; Barry, B.; De Raucourt, D.; Choussy, O.; Dessard-Diana, B.; Hans, S.; Lafarge, D.; SFORL Work-Group. Guidelines update: Post-treatment follow-up of adult head and neck squamous cell carcinoma: Screening for metastasis and metachronous esophageal and bronchial locations. Eur. Ann. Otorhinolaryngol. Head Neck Dis. 2015, 132, 217–221. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Mehanna, H.; Wong, W.-L.; McConkey, C.C.; Rahman, J.K.; Robinson, M.; Hartley, A.G.J.; Nutting, C.; Powell, N.; Al-Booz, H.; Robinson, M.; et al. PET-CT Surveillance versus Neck Dissection in Advanced Head and Neck Cancer. N. Engl. J. Med. 2016, 374, 1444–1454. [Google Scholar] [CrossRef]
- Massa, S.T.; Osazuwa-Peters, N.; Christopher, K.M.; Arnold, L.D.; Schootman, M.; Varvares, R.J.W.M.A. Competing causes of death in the head and neck cancer population. Oral Oncol. 2017, 65, 8–15. [Google Scholar] [CrossRef] [PubMed]
- Rosenbaum, P.R. Optimal matching for observational studies. J. Am. Stat. Assoc. 1989, 84, 1024–1032. [Google Scholar] [CrossRef]
- Galloway, T.J.; Ridge, J.A. Management of squamous cancer metastatic to cervical nodes with an unknown primary site. J. Clin. Oncol. 2015, 33, 3328–3337. [Google Scholar] [CrossRef] [PubMed]
- Mani, N.; George, M.M.; Nash, L.; Anwar, B.; Homer, J.J. Role of 18-Fludeoxyglucose positron emission tomography-computed tomography and subsequent panendoscopy in head and neck squamous cell carcinoma of unknown primary. Laryngoscope 2016, 126, 1354–1358. [Google Scholar] [CrossRef]
- Colletier, P.J.; Garden, A.S.; Morrison, W.H.; Goepfert, H.; Geara, F.; Ang, K.K. Postoperative radiation for squamous cell carcinoma metastatic to cervical lymph nodes from an unknown primary site: Outcomes and patterns of failure. Head Neck 1998, 20, 674–681. [Google Scholar] [CrossRef]
- Lou, J.; Wang, S.; Wang, K.; Chen, C.; Zhao, J.; Guo, L. Squamous cell carcinoma of cervical lymph nodes from an unknown primary site: The impact of neck dissection. J. Cancer Res. Ther. 2015, 11 (Suppl. 2), C161–C167. [Google Scholar]
- Amsbaugh, M.J.; Yusuf, M.; Gaskins, J.; Silverman, C.; Potts, K.; Bumpous, J.; Redman, R.; Perez, C.; Dunlap, N. Neck dissection for unknown cancer of the head and neck in the era of chemoradiation. Am. J. Otolaryngol. 2017, 38, 588–592. [Google Scholar] [CrossRef] [PubMed]
- Carsuzaa, F.; Gorphe, P.; Vergez, S.; Malard, O.; Fakhry, N.; Righini, C.; Philouze, P.; Lasne-Cardon, A.; Gallet, P.; Tonnerre, D.; et al. Consensus on resectability in N3 head and neck squamous cell carcinomas: GETTEC recommendations. Oral Oncol. 2020, 106, 104733. [Google Scholar] [CrossRef] [PubMed]
- Aslani, M.; Sultanem, K.; Voung, T.; Hier, M.; Niazi, T.; Shenouda, G. Metastatic carcinoma to the cervical nodes from an unknown head and neck primary site: Is there a need for neck dissection? Head Neck 2007, 29, 585–590. [Google Scholar] [CrossRef]
- Beldì, D.; Jereczek-Fossa, B.A.; D’Onofrio, A.; Gambaro, G.; Fiore, M.R.; Pia, F.; Chiesa, F.; Orecchia, R.; Krengli, M. Role of radiotherapy in the treatment of cervical lymph node metastases from an unknown primary site: Retrospective analysis of 113 patients. Int. J. Radiat. Oncol. Biol. Phys. 2007, 69, 1051–1058. [Google Scholar] [CrossRef] [PubMed]
- Hauswald, H.; Lindel, K.; Rochet, N.; Debus, J.; Harms, W. Surgery with complete resection improves survival in radiooncologically treated patients with cervical lymph node metastases from cancer of unknown primary. Strahlenther. Onkol. Organ Dtsch. Röntgenges. 2008, 184, 150–156. [Google Scholar] [CrossRef]
- Zhou, M.J.; van Zante, A.; Lazar, A.A.; Groppo, E.R.; Garsa, A.A.; Ryan, W.R.; El-Sayed, I.H.; Eisele, D.W.; Yom, S.S. Squamous cell carcinoma of unknown primary of the head and neck: Favorable prognostic factors comparable to those in oropharyngeal cancer. Head Neck 2017, 40, 904–916. [Google Scholar] [CrossRef]
- Boros, A.; Blanchard, P.; Dade, A.; Gorphe, P.; Breuskin, I.; Even, C.; Nguyen, F.; Deutsch, E.; Bidault, F.; Janot, F.; et al. Outcomes in N3 Head and Neck Squamous Cell Carcinoma and Role of Upfront Neck Dissection. Laryngoscope 2020. [Google Scholar] [CrossRef]
- Thariat, J.; Ang, K.K.; Allen, P.K.; Ahamad, A.; Williams, M.D.; Myers, J.N.; El-Naggar, A.K.; Ginsberg, L.E.; Rosenthal, D.I.; Glisson, B.S.; et al. Prediction of neck dissection requirement after definitive radiotherapy for head-and-neck squamous cell carcinoma. Int. J. Radiat. Oncol. Biol. Phys. 2012, 82, e367–e374. [Google Scholar] [CrossRef]
- Huang, J.; Barbera, L.; Brouwers, M.; Browman, G.; Mackillop, W.J. Does delay in starting treatment affect the outcomes of radiotherapy? A systematic review. J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol. 2003, 21, 555–563. [Google Scholar] [CrossRef]
- Elicin, O.; Albrecht, T.; Haynes, A.G.; Bojaxhiu, B.; Nisa, L.; Caversaccio, M.; Dal Pra, A.; Schmücking, M.; Aebersold, D.M.; Giger, R.; et al. Outcomes in Advanced Head and Neck Cancer Treated with Up-front Neck Dissection prior to (Chemo)Radiotherapy. Otolaryngol. Head Neck Surg. 2016, 154, 300–308. [Google Scholar] [CrossRef] [PubMed]
- Mehanna, H.; McConkey, C.C.; Rahman, J.K.; Wong, W.L.; Smith, A.F.; Nutting, C.; Hartley, A.G.; Hall, P.; Hulme, C.; Patel, D.K.; et al. PET-NECK: A multicentre randomised Phase III non-inferiority trial comparing a positron emission tomography-computerised tomography-guided watch-and-wait policy with planned neck dissection in the management of locally advanced (N2/N3) nodal metastases in. Health Technol. Assess. 2017, 21, 1–122. [Google Scholar] [CrossRef] [PubMed]
- Sokoya, M.; Chowdhury, F.; Kadakia, S.; Ducic, Y. Combination of panendoscopy and positron emission tomography/computed tomography increases detection of unknown primary head and neck carcinoma. Laryngoscope 2018. [Google Scholar] [CrossRef]
- Noij, D.P.; Martens, R.M.; Zwezerijnen, B.; Koopman, T.; de Bree, R.; Hoekstra, O.S.; de Graaf, P.; Castelijns, J.A. Diagnostic value of diffusion-weighted imaging and 18F-FDG-PET/CT for the detection of unknown primary head and neck cancer in patients presenting with cervical metastasis. Eur. J. Radiol. 2018, 107, 20–25. [Google Scholar] [CrossRef] [PubMed]
- Wallis, S.; O’Toole, L.; Karsai, L.; Jose, J. Transoral endoscopic base of tongue mucosectomy for investigation of unknown primary cancers of head and neck. Clin. Otolaryngol. 2018, 43, 1139–1143. [Google Scholar] [CrossRef]
- Winter, S.C.; Ofo, E.; Meikle, D.; Silva, P.; Fraser, L.; O’Hara, J.; Kim, D.; Robinson, M.; Paleri, V. Trans-oral robotic assisted tongue base mucosectomy for investigation of cancer of unknown primary in the head and neck region. UK Exp. Clin. Otolaryngol. 2017, 42, 1247–1251. [Google Scholar] [CrossRef]
- Axelsson, L.; Nyman, J.; Haugen-Cange, H.; Bove, M.; Johansson, L.; de Lara, S.; Kovacs, A.; Hammerlid, E. Prognostic factors for head and neck cancer of unknown primary including the impact of human papilloma virus infection. J. Otolaryngol. Head Neck Surg. 2017, 46, 45. [Google Scholar] [CrossRef]
- Motz, K.; Qualliotine, J.R.; Rettig, E.; Richmon, J.D.; Eisele, D.W.; Fakhry, C. Changes in Unknown Primary Squamous Cell Carcinoma of the Head and Neck at Initial Presentation in the Era of Human Papillomavirus. JAMA Otolaryngol. Head Neck Surg. 2016, 142, 223. [Google Scholar] [CrossRef]
- Schroeder, L.; Boscolo-Rizzo, P.; Dal Cin, E.; Romeo, S.; Baboci, L.; Dyckhoff, G.; Hess, J.; Lucena-Porcel, C.; Byl, A.; Becker, N.; et al. Human papillomavirus as prognostic marker with rising prevalence in neck squamous cell carcinoma of unknown primary: A retrospective multicentre study. Eur. J. Cancer 2017, 74, 73–81. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).