Numerical Flow Simulation on the Virus Spread of SARS-CoV-2 Due to Airborne Transmission in a Classroom
Abstract
:1. Introduction
2. Model Approach
2.1. Modelling of the Viral Load
2.2. Assessment of Infection Risk
3. Application Model
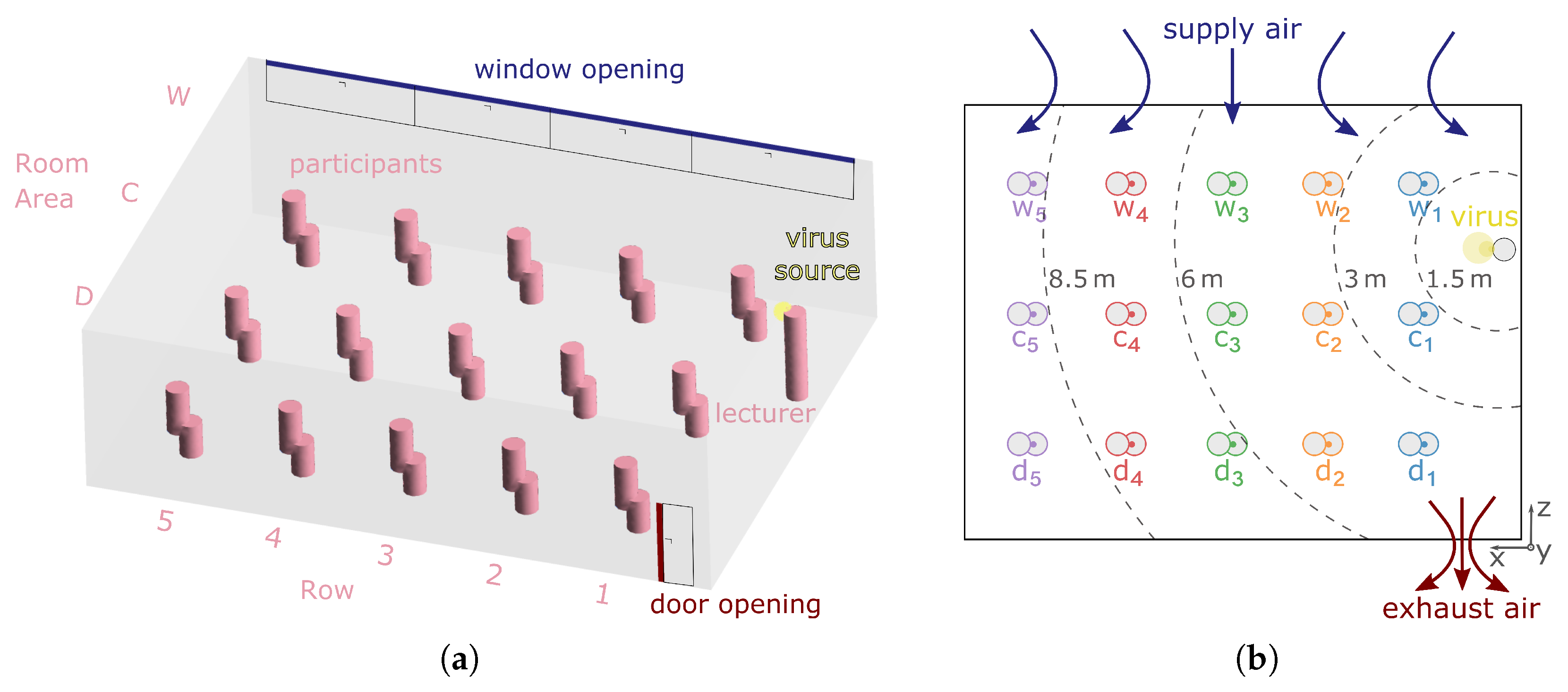
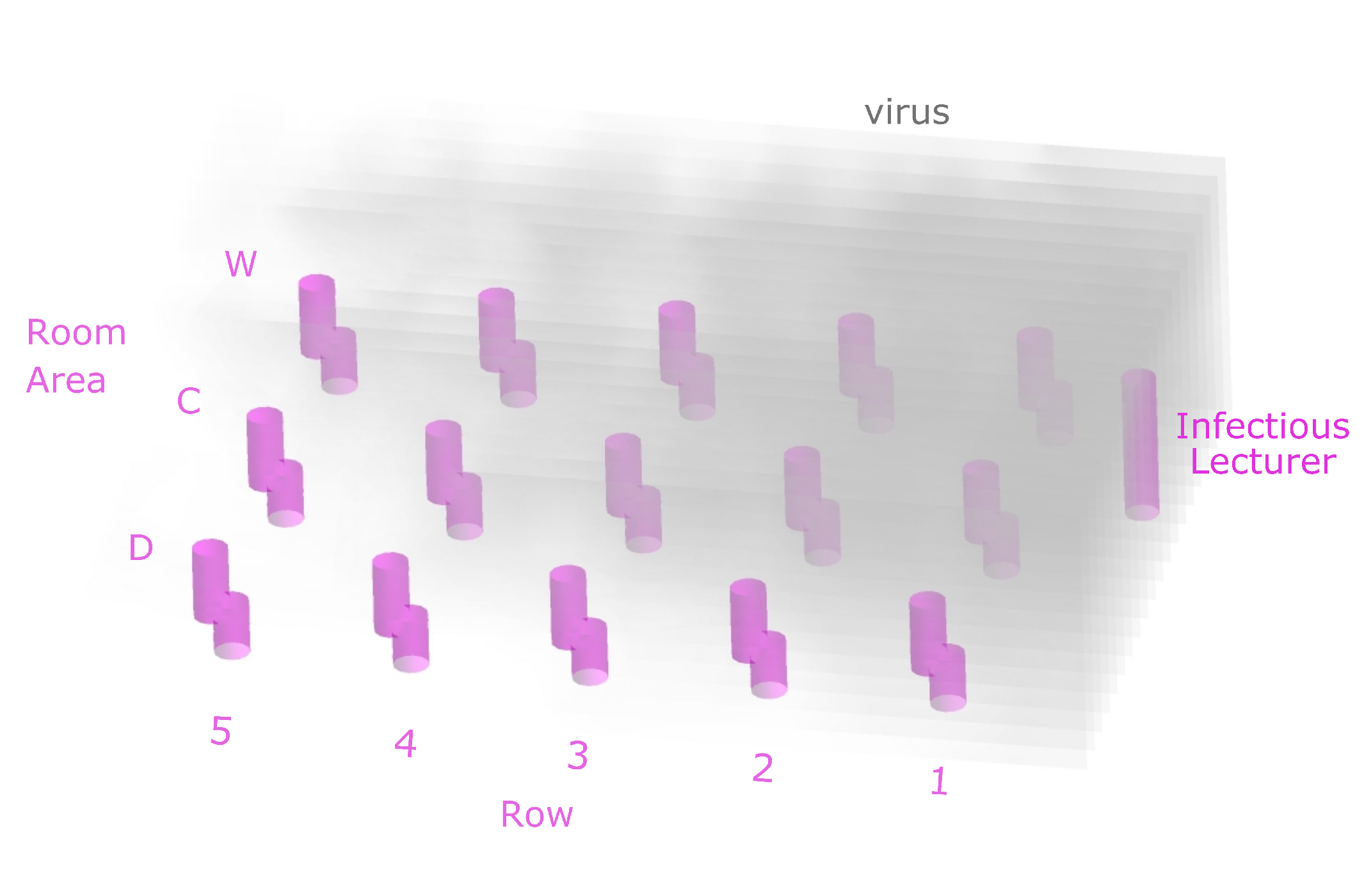
3.1. General Description
3.2. Numerical Treatment of Air Flow
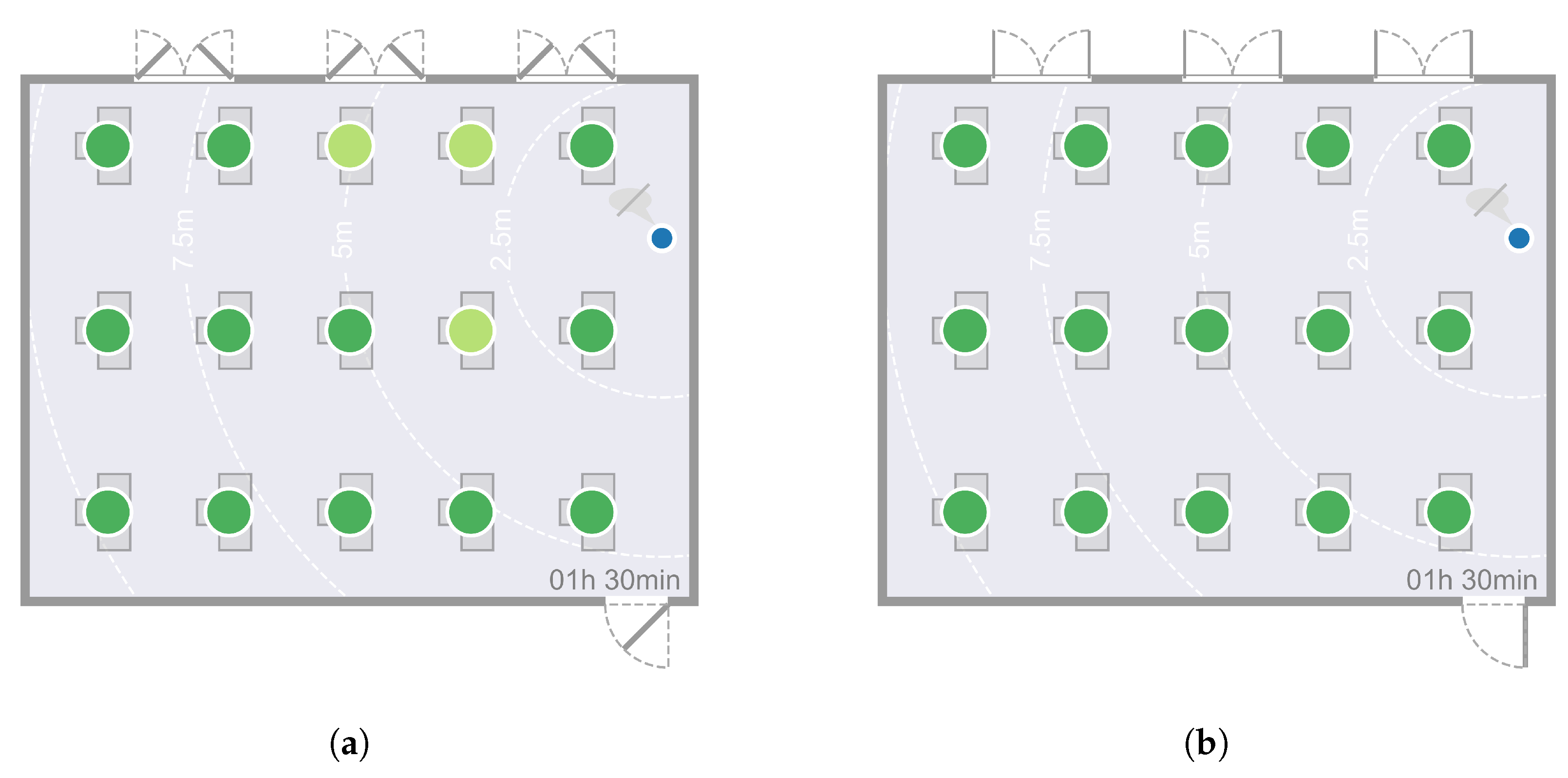
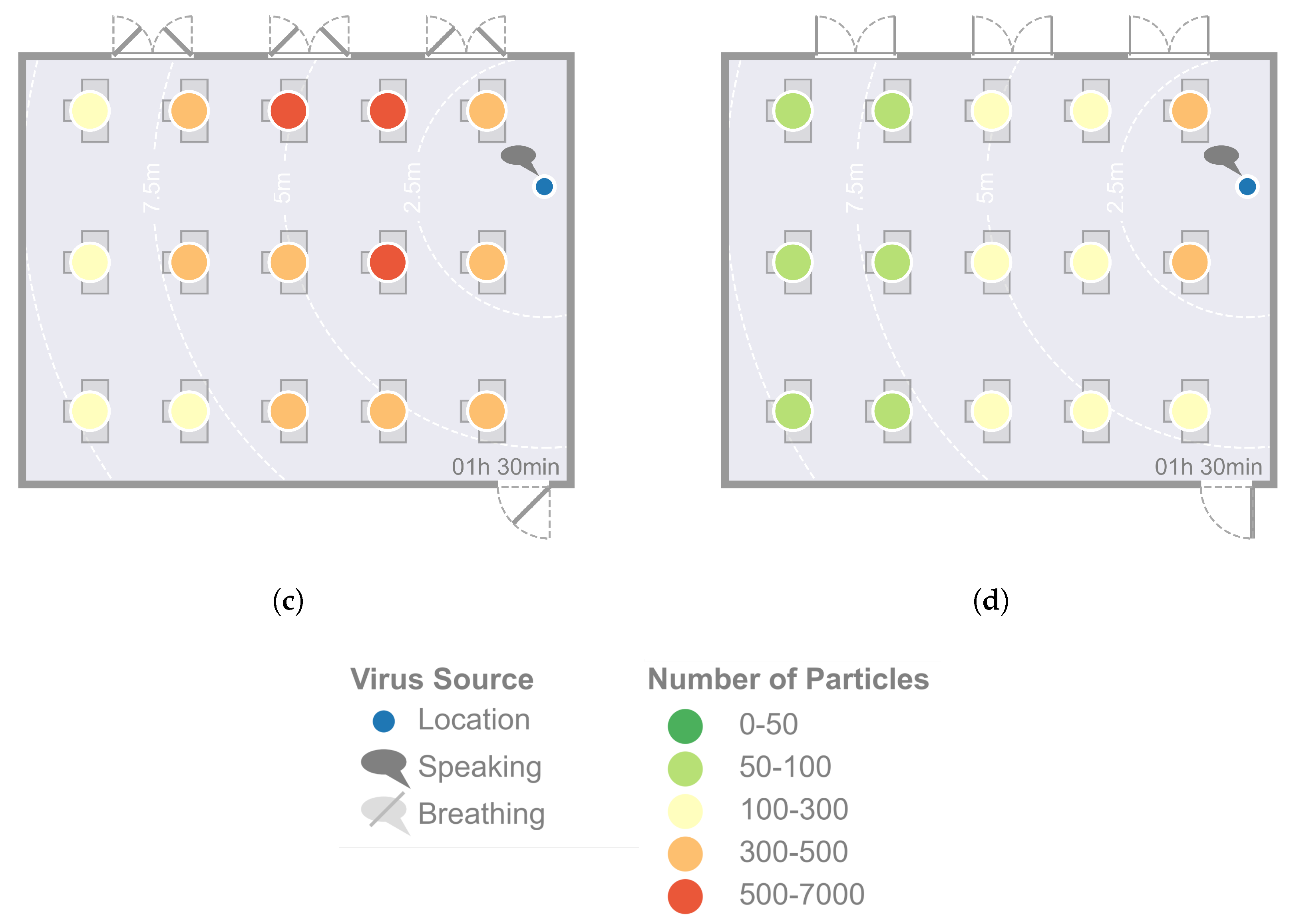
4. Results
5. Discussion
5.1. Effect of Supply Air Volume on the Risk of Infection
5.2. ‘Green Classroom’ Situation
5.3. Comparison with Available Models
6. Summary and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CFD | Computational Fluid Dynamics |
| RANS | Reynolds-Averaged Navier–Stokes |
| RNG | Renormalisation Group |
References
- World Health Organization. Press Briefing of the World Health Organization’s Health Emergencies Program. Available online: https://www.who.int/news/item/01-08-2020-covid-19-emergency-committee-highlights-need-for-response-efforts-over-long-term (accessed on 27 April 2022).
- Correia, G.; Rodrigues, L.; Gameiro da Silva, M.; Gonçalves, T. Airborne route and bad use of ventilation systems as non-negligible factors in SARS-CoV-2 transmission. Med. Hypotheses 2020, 141, 109781. [Google Scholar] [CrossRef] [PubMed]
- Seto, W. Airborne transmission and precautions: Facts and myths. J. Hosp. Infect. 2015, 89, 225–228. [Google Scholar] [CrossRef] [PubMed]
- Mohamadi, M.; Babington-Ashaye, A.; Lefort, A.; Flahault, A. Risks of Infection with SARS-CoV-2 Due to Contaminated Surfaces: A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 1019. [Google Scholar] [CrossRef] [PubMed]
- Delikhoon, M.; Guzman, M.I.; Nabizadeh, R.; Norouzian Baghani, A. Modes of Transmission of Severe Acute Respiratory Syndrome-Coronavirus-2 (SARS-CoV-2) and Factors Influencing on the Airborne Transmission: A Review. Int. J. Environ. Res. Public Health 2021, 18, 395. [Google Scholar] [CrossRef] [PubMed]
- Haslbeck, K.; Schwarz, K.; Hohlfeld, J.M.; Seume, J.R.; Koch, W. Submicron droplet formation in the human lung. J. Aerosol Sci. 2010, 41, 429–438. [Google Scholar] [CrossRef]
- Ji, Y.; Qian, H.; Ye, J.; Zheng, X. The impact of ambient humidity on the evaporation and dispersion of exhaled breathing droplets: A numerical investigation. J. Aerosol Sci. 2018, 115, 164–172. [Google Scholar] [CrossRef]
- Asadi, S.; Wexler, A.S.; Cappa, C.D.; Barreda, S.; Bouvier, N.M.; Ristenpart, W.D. Aerosol emission and superemission during human speech increase with voice loudness. Sci. Rep. 2019, 9, 2348. [Google Scholar] [CrossRef] [Green Version]
- Asadi, S.; Wexler, A.S.; Cappa, C.D.; Barreda, S.; Bouvier, N.M.; Ristenpart, W.D. Effect of voicing and articulation manner on aerosol particle emission during human speech. PLoS ONE 2020, 15, e0227699. [Google Scholar] [CrossRef] [Green Version]
- Li, Y.; Qian, H.; Hang, J.; Chen, X.; Hong, L.; Liang, P.; Li, J.; Xiao, S.; Wei, J.; Liu, L.; et al. Evidence for probable aerosol transmission of SARS-CoV-2 in a poorly ventilated restaurant. medRxiv 2020. [Google Scholar] [CrossRef] [Green Version]
- Tang, J.; Bahnfleth, W.; Bluyssen, P.; Buonanno, G.; Jimenez, J.; Kurnitski, J.; Li, Y.; Miller, S.; Sekhar, C.; Morawska, L.; et al. Dismantling myths on the airborne transmission of severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2). J. Hosp. Infect. 2021, 110, 89–96. [Google Scholar] [CrossRef]
- Birgand, G.; Peiffer-Smadja, N.; Fournier, S.; Kerneis, S.; Lescure, F.X.; Lucet, J.C. Assessment of Air Contamination by SARS-CoV-2 in Hospital Settings. JAMA Netw. Open 2020, 3, e2033232. [Google Scholar] [CrossRef] [PubMed]
- Peng, Z.; Rojas, A.P.; Kropff, E.; Bahnfleth, W.; Buonanno, G.; Dancer, S.; Kurnitski, J.; Li, Y.; Loomans, M.; Marr, L.; et al. Practical Indicators for Risk of Airborne Transmission in Shared Indoor Environments and Their Application to COVID-19 Outbreaks. Environ. Sci. Technol. 2022, 56, 1125–1137. [Google Scholar] [CrossRef] [PubMed]
- Morawska, L.; Milton, D.K. It Is Time to Address Airborne Transmission of Coronavirus Disease 2019 (COVID-19). Clin. Infect. Dis. 2020, 71, ciaa939. [Google Scholar] [CrossRef] [PubMed]
- van Doremalen, N.; Bushmaker, T.; Morris, D.H.; Holbrook, M.G.; Gamble, A.; Williamson, B.N.; Tamin, A.; Harcourt, J.L.; Thornburg, N.J.; Gerber, S.I.; et al. Aerosol and Surface Stability of SARS-CoV-2 as Compared with SARS-CoV-1. N. Engl. J. Med. 2020, 382, 1564–1567. [Google Scholar] [CrossRef] [PubMed]
- Sarti, D.; Campanelli, T.; Rondina, T.; Gasperini, B. COVID-19 in Workplaces: Secondary Transmission. Ann. Work Expo. Health 2021, 65, 1145–1151. [Google Scholar] [CrossRef]
- Morawska, L.; Tang, J.W.; Bahnfleth, W.; Bluyssen, P.M.; Boerstra, A.; Buonanno, G.; Cao, J.; Dancer, S.; Floto, A.; Franchimon, F.; et al. How can airborne transmission of COVID-19 indoors be minimised? Environ. Int. 2020, 142, 105832. [Google Scholar] [CrossRef]
- Liu, Y.; Ning, Z.; Chen, Y.; Guo, M.; Liu, Y.; Gali, N.K.; Sun, L.; Duan, Y.; Cai, J.; Westerdahl, D.; et al. Aerodynamic analysis of SARS-CoV-2 in two Wuhan hospitals. Nature 2020, 582, 557–560. [Google Scholar] [CrossRef]
- Stabile, L.; Pacitto, A.; Mikszewski, A.; Morawska, L.; Buonanno, G. Ventilation procedures to minimize the airborne transmission of viruses in classrooms. Build. Environ. 2021, 202, 108042. [Google Scholar] [CrossRef]
- Lelieveld, J.; Helleis, F.; Borrmann, S.; Cheng, Y.; Drewnick, F.; Haug, G.; Klimach, T.; Sciare, J.; Su, H.; Pöschl, U. Model Calculations of Aerosol Transmission and Infection Risk of COVID-19 in Indoor Environments. Int. J. Environ. Res. Public Health 2020, 17, 8114. [Google Scholar] [CrossRef]
- Hartmann, A.; Kriegel, M. Risk Assessment of Aerosols Loaded with Virus Based on CO2-Concentration; Technische Universität: Berlin, Germany, 2020. [Google Scholar] [CrossRef]
- Rudnick, S.N.; Milton, D.K. Risk of indoor airborne infection transmission estimated from carbon dioxide concentration: Indoor airborne transmission of infectious diseases. Indoor Air 2003, 13, 237–245. [Google Scholar] [CrossRef]
- Kriegel, M.; Hartmann, A. Covid-19 Contagion via Aerosol Particles—Comparative Evaluation of Indoor Environments with Respect to Situational R-Value; Technische Universität: Berlin, Germany, 2021. [Google Scholar] [CrossRef]
- Mirzaie, M.; Lakzian, E.; Khan, A.; Warkiani, M.E.; Mahian, O.; Ahmadi, G. COVID-19 spread in a classroom equipped with partition—A CFD approach. J. Hazard. Mater. 2021, 420, 126587. [Google Scholar] [CrossRef] [PubMed]
- Abuhegazy, M.; Talaat, K.; Anderoglu, O.; Poroseva, S.V. Numerical investigation of aerosol transport in a classroom with relevance to COVID-19. Phys. Fluids 2020, 32, 103311. [Google Scholar] [CrossRef] [PubMed]
- Löhner, R.; Antil, H.; Srinivasan, A.; Idelsohn, S.; Oñate, E. High-Fidelity Simulation of Pathogen Propagation, Transmission and Mitigation in the Built Environment. Arch. Comput. Methods Eng. 2021, 28, 4237–4262. [Google Scholar] [CrossRef] [PubMed]
- Ahmadzadeh, M.; Farokhi, E.; Shams, M. Investigating the effect of air conditioning on the distribution and transmission of COVID-19 virus particles. J. Clean. Prod. 2021, 316, 128147. [Google Scholar] [CrossRef] [PubMed]
- Duill, F.F.; Schulz, F.; Jain, A.; Krieger, L.; van Wachem, B.; Beyrau, F. The Impact of Large Mobile Air Purifiers on Aerosol Concentration in Classrooms and the Reduction of Airborne Transmission of SARS-CoV-2. Int. J. Environ. Res. Public Health 2021, 18, 1523. [Google Scholar] [CrossRef] [PubMed]
- Shao, S.; Zhou, D.; He, R.; Li, J.; Zou, S.; Mallery, K.; Kumar, S.; Yang, S.; Hong, J. Risk assessment of airborne transmission of COVID-19 by asymptomatic individuals under different practical settings. J. Aerosol Sci. 2021, 151, 105661. [Google Scholar] [CrossRef]
- Wan, M.P.; Sze To, G.N.; Chao, C.Y.H.; Fang, L.; Melikov, A. Modeling the Fate of Expiratory Aerosols and the Associated Infection Risk in an Aircraft Cabin Environment. Aerosol Sci. Technol. 2009, 43, 322–343. [Google Scholar] [CrossRef]
- Morawska, L.; Afshari, A.; Bae, G.N.; Buonanno, G.; Chao, C.Y.H.; Hänninen, O.; Hofmann, W.; Isaxon, C.; Jayaratne, E.R.; Pasanen, P.; et al. Indoor aerosols: From personal exposure to risk assessment. Indoor Air 2013, 23, 462–487. [Google Scholar] [CrossRef] [Green Version]
- Çengel, Y.A.; Cimbala, J.M. Fluid mechanics: Fundamentals and applications. McGraw-Hill Series in Mechanical Engineering; McGraw-HillHigher Education: Boston, MA, USA, 2006. [Google Scholar]
- Douglas, J.F. (Ed.) Fluid Mechanics, 5th ed.; Pearson/Prentice Hall: Harlow, UK; New York, NY, USA, 2005. [Google Scholar]
- Hartmann, A.; Lange, J.; Rotheudt, H.; Kriegel, M. Emission Rate and Particle Size of Bioaerosols during Breathing, Speaking and Coughing; Technische Universität: Berlin, Germany, 2020. [Google Scholar] [CrossRef]
- Pan, Y.; Zhang, D.; Yang, P.; Poon, L.L.M.; Wang, Q. Viral load of SARS-CoV-2 in clinical samples. Lancet Infect. Dis. 2020, 20, 411–412. [Google Scholar] [CrossRef]
- Pujadas, E.; Chaudhry, F.; McBride, R.; Richter, F.; Zhao, S.; Wajnberg, A.; Nadkarni, G.; Glicksberg, B.S.; Houldsworth, J.; Cordon-Cardo, C. SARS-CoV-2 viral load predicts COVID-19 mortality. Lancet Respir. Med. 2020, 8, e70. [Google Scholar] [CrossRef]
- To, K.K.W.; Tsang, O.T.Y.; Leung, W.S.; Tam, A.R.; Wu, T.C.; Lung, D.C.; Yip, C.C.Y.; Cai, J.P.; Chan, J.M.C.; Chik, T.S.H.; et al. Temporal profiles of viral load in posterior oropharyngeal saliva samples and serum antibody responses during infection by SARS-CoV-2: An observational cohort study. Lancet Infect. Dis. 2020, 20, 565–574. [Google Scholar] [CrossRef] [Green Version]
- He, X.; Lau, E.H.Y.; Wu, P.; Deng, X.; Wang, J.; Hao, X.; Lau, Y.C.; Wong, J.Y.; Guan, Y.; Tan, X.; et al. Temporal dynamics in viral shedding and transmissibility of COVID-19. Nat. Med. 2020, 26, 672–675. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Yu, X.; Sun, S.; Shi, Y.; Wang, H.; Zhao, R.; Sheng, J. SARS-CoV-2 viral load in sputum correlates with risk of COVID-19 progression. Crit. Care 2020, 24, 170. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kriegel, M.; Buchholz, U.; Gastmeier, P.; Bischoff, P.; Abdelgawad, I.; Hartmann, A. Predicted Infection Risk for Aerosol Transmission of SARS-CoV-2. medRxiv 2020. [Google Scholar] [CrossRef]
- Coleman, K.K.; Tay, D.J.W.; Tan, K.S.; Ong, S.W.X.; Than, T.S.; Koh, M.H.; Chin, Y.Q.; Nasir, H.; Mak, T.M.; Chu, J.J.H.; et al. Viral Load of Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2) in Respiratory Aerosols Emitted by Patients with Coronavirus Disease 2019 (COVID-19) While Breathing, Talking, and Singing. Clin. Infect. Dis. 2021, ciab691. [Google Scholar] [CrossRef] [PubMed]
- Hyldgaard, E. Humans as a Source of Heat and Air Pollution; Number 39 in Indoor Environmental Technology; Department of Building Technology and Structural Engineering: Tokyo, Japan, 1994. [Google Scholar]
- König, P.; Lipp, A. Lehrbuch für Forschungstaucher. Manuskript einer Vorlesung am Institut für Meereskunde der Universität Hamburg. 2007. Available online: https://flexikon.doccheck.com/de/atmung (accessed on 27 April 2022).
- Chourpiliadis, C.; Bhardwaj, A. Physiology, Respiratory Rate. In StatPearls; StatPearls Publishing: Treasure Island, FL, USA, 2022. [Google Scholar]
- Riediker, M.; Monn, C. Simulation of SARS-CoV-2 Aerosol Emissions in the Infected Population and Resulting Airborne Exposures in Different Indoor Scenarios. Aerosol Air Qual. Res. 2021, 21, 200531. [Google Scholar] [CrossRef]
- Garcia-Beltran, W.F.; St. Denis, K.J.; Hoelzemer, A.; Lam, E.C.; Nitido, A.D.; Sheehan, M.L.; Berrios, C.; Ofoman, O.; Chang, C.C.; Hauser, B.M.; et al. mRNA-based COVID-19 vaccine boosters induce neutralizing immunity against SARS-CoV-2 Omicron variant. Cell 2022, 185, 457–466.e4. [Google Scholar] [CrossRef]
- Mikszewski, A.; Stabile, L.; Buonanno, G.; Morawska, L. Increased close proximity airborne transmission of the SARS-CoV-2 Delta variant. Sci. Total Environ. 2022, 816, 151499. [Google Scholar] [CrossRef]
- Riediker, M.; Briceno-Ayala, L.; Ichihara, G.; Albani, D.; Poffet, D.; Tsa, D.H.; Monn, C.; Iff, S. Higher viral load and infectivity increase risk of aerosol transmission for Delta and Omicron variants of SARS-CoV-2. Swiss Med. Wkly. 2022, 152, w30133. [Google Scholar] [CrossRef]
- Moriske, H.J.; Szewzyk, R. Leitfaden für die Innenraumhygiene in Schulgebäuden; Technical Report; Umweltbundesamt Innenraumlufthygiene-Kommission des Umweltbundesamtes, KOMAG mbH: Berlin, Germany, 2008. [Google Scholar]
- ANSI/ASHRAE Standard 62.1-2019; Ventilation for Acceptable Indoor Air Quality. ANSI/ASHRAE: Atlantal, GA, USA, 2019.
- Clements-Croome, D.; Awbi, H.; Bakó-Biró, Z.; Kochhar, N.; Williams, M. Ventilation rates in schools. Build. Environ. 2008, 43, 362–367. [Google Scholar] [CrossRef] [Green Version]
- Haupt, W. Zur Simulation von auftriebsinduzierten Innenraumströmungen. Ph.D. Thesis, Universität Gesamthochschule Kassel, Kassel, Germany, 2001. [Google Scholar]
- Ansys Inc. Theory Reference Manual, Chapter 4: Turbulence|4.3. Standard, RNG and realizable k-e Models|Release R19; Ansys Inc.: Canonsburg, PA, USA, 2019. [Google Scholar]
- MPIC Max Planck Institute for Chemistry. Algorithm to Estimate COVID-19 Infection Risks by Aerosol Transmission in Indoor Environments. Available online: https://www.mpic.de/4747065/risk-calculation (accessed on 27 April 2022).
- Lam-Hine, T.; McCurdy, S.A.; Santora, L.; Duncan, L.; Corbett-Detig, R.; Kapusinszky, B.; Willis, M. Outbreak Associated with SARS-CoV-2 B.1.617.2 (Delta) Variant in an Elementary School— Marin County, California, May–June 2021. Morb. Mortal. Wkly. Rep. 2021, 70, 1214. [Google Scholar] [CrossRef] [PubMed]
- Allan, M.; Richardson, G.M. Probability Density Functions Describing 24-Hour Inhalation Rates For Use in Human Health Risk Assessments. Hum. Ecol. Risk Assess. Int. J. 1998, 4, 379–408. [Google Scholar] [CrossRef]
| Parameter | Low Vent./ Speaking | High Vent./ Speaking | Low Vent./ Breathing | High Vent./ Breathing |
|---|---|---|---|---|
| Supply air volume flow in | 35 | 432 | 35 | 432 |
| Air change rate in | 0.146 | 1.800 | 0.146 | 1.800 |
| Viral load of lecturer in virus particles/s | 100 | 100 | 10 | 10 |
| Parameter | Description | Value |
|---|---|---|
| Model approach | ||
| Virus variant | Virus variant considered in terms of spread and infection | Wildtype |
| Viral load | Viral emissions of an infectious person during breathing (a) and speaking (b) | (a) 10 SARS-CoV-2 virus particles/s and (b) 100 SARS-CoV-2 virus particles/s |
| Respiration rate | Respiration rate of all persons | |
| Calculation of viral distribution | Multispecies model approach for calculating the airborne viral load fraction | Species Transport model |
| Threshold for high risk | The risk of infection is assessed as high as soon as the cumulative number of virus particles in a person’s inhalation volume reaches the threshold value | 500 particles |
| Application model | ||
| Room size | Dimensions of the investigated room | () and high |
| Window area | Supply airflow into the room through the surface | |
| Supply air | Volume flow of supply air for (a) low ventilation and (b) high ventilation | (a) and (b) |
| Open door area | Indoor air escapes through the surface | |
| Susceptible persons | Number of uninfected persons in the room | 15 |
| Distance | Minimum distance between persons | |
| Infectious person | Number and location of the infectious persons | 1 lecturer, standing at the front of the room |
| Thermal boundary conditions | Thermal boundary conditions of persons (a), walls (b), fresh air (c), exhaled air (d) | (a) 37 °C, (b) adiabatic, (c) 25 °C, (d) 37 °C |
| Viscous model | Model for calculating the flow pattern | k- (RNG) model |
| Numerical mesh | Number of elements of the mesh | Approx. 2.6 million |
| Near-wall treatment | Near-wall treatment of the room walls that are parallel to the flow direction (from the window to the door) and for those of the bodies of people in the room | Enhanced Wall Treatment with the first near-wall node is set to |
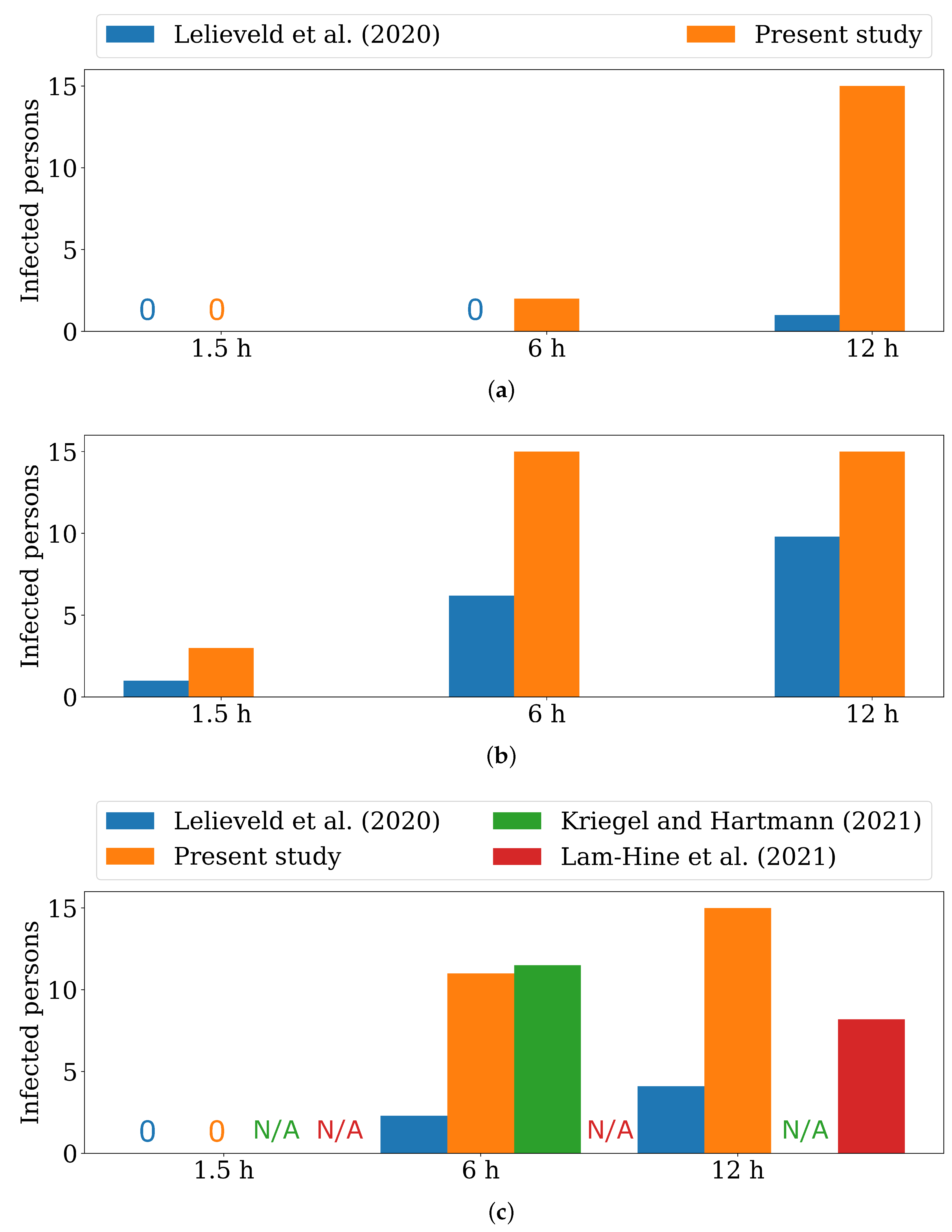
| Parameter | Lelieveld et al. (2020) [20]/MPIC | Kriegel and Hartmann (2021) [23] | Lam-Hine et al. (2021) [55] | Present Study | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Classroom size in | 80 | N/A | N/A | 80 | ||||||
| Infectious person | 1 ( before others in room) | 1 | 1 (lecturer) | 1 (lecturer) | ||||||
| Others | 15 unmasked | Normal occupancy, unmasked | 24 masked | 15 unmasked | ||||||
| Ventilation | Windows and door are open; air filter (no ventilation rate given) | |||||||||
| Virus variant | Wildtype | Wildtype | Delta | Wildtype | ||||||
| Viral load in parts/s | 10 | 100 | 10 | 100 | 100 | N/A | 10 | 100 | 10 | 100 |
| Result unit | Infected persons and probability that a least one susceptible person becoming infected | Number of susceptible persons becoming infected | Number of susceptible persons becoming infected | Number of susceptible persons with a high risk of infection | ||||||
| Result after 1.5 h | 1.0 () | 1.0 () | 1.0 () | 1.0 () | No result | No result | 0 | 3 | 0 | 0 |
| Result after 6 h | 1.0 () | 6.2 | 1.0 () | 2.2 | 11.5 | No result | 2 | All 15 | 0 | 11 |
| Result after 12 h | 1.0 () | 9.8 | 1.0 () | 4.2 | No result | 12 (out of 22 tested) | All 15 | All 15 | 0 | All 15 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moeller, L.; Wallburg, F.; Kaule, F.; Schoenfelder, S. Numerical Flow Simulation on the Virus Spread of SARS-CoV-2 Due to Airborne Transmission in a Classroom. Int. J. Environ. Res. Public Health 2022, 19, 6279. https://doi.org/10.3390/ijerph19106279
Moeller L, Wallburg F, Kaule F, Schoenfelder S. Numerical Flow Simulation on the Virus Spread of SARS-CoV-2 Due to Airborne Transmission in a Classroom. International Journal of Environmental Research and Public Health. 2022; 19(10):6279. https://doi.org/10.3390/ijerph19106279
Chicago/Turabian StyleMoeller, Lara, Florian Wallburg, Felix Kaule, and Stephan Schoenfelder. 2022. "Numerical Flow Simulation on the Virus Spread of SARS-CoV-2 Due to Airborne Transmission in a Classroom" International Journal of Environmental Research and Public Health 19, no. 10: 6279. https://doi.org/10.3390/ijerph19106279
APA StyleMoeller, L., Wallburg, F., Kaule, F., & Schoenfelder, S. (2022). Numerical Flow Simulation on the Virus Spread of SARS-CoV-2 Due to Airborne Transmission in a Classroom. International Journal of Environmental Research and Public Health, 19(10), 6279. https://doi.org/10.3390/ijerph19106279






