The Pathways to Participation (P2P) Program: A Pilot Outcomes Study
Abstract
1. Introduction
Interventions for Activity Participation in Recovery
2. Materials and Methods
2.1. Development of the P2P Program
2.2. Procedure
2.3. Data Collection
2.4. Sample
2.5. Data Analysis
3. Results
3.1. Sample Characteristics
3.2. Consumer Identified Needs
3.3. Time Use
3.4. Self Rated Recovery
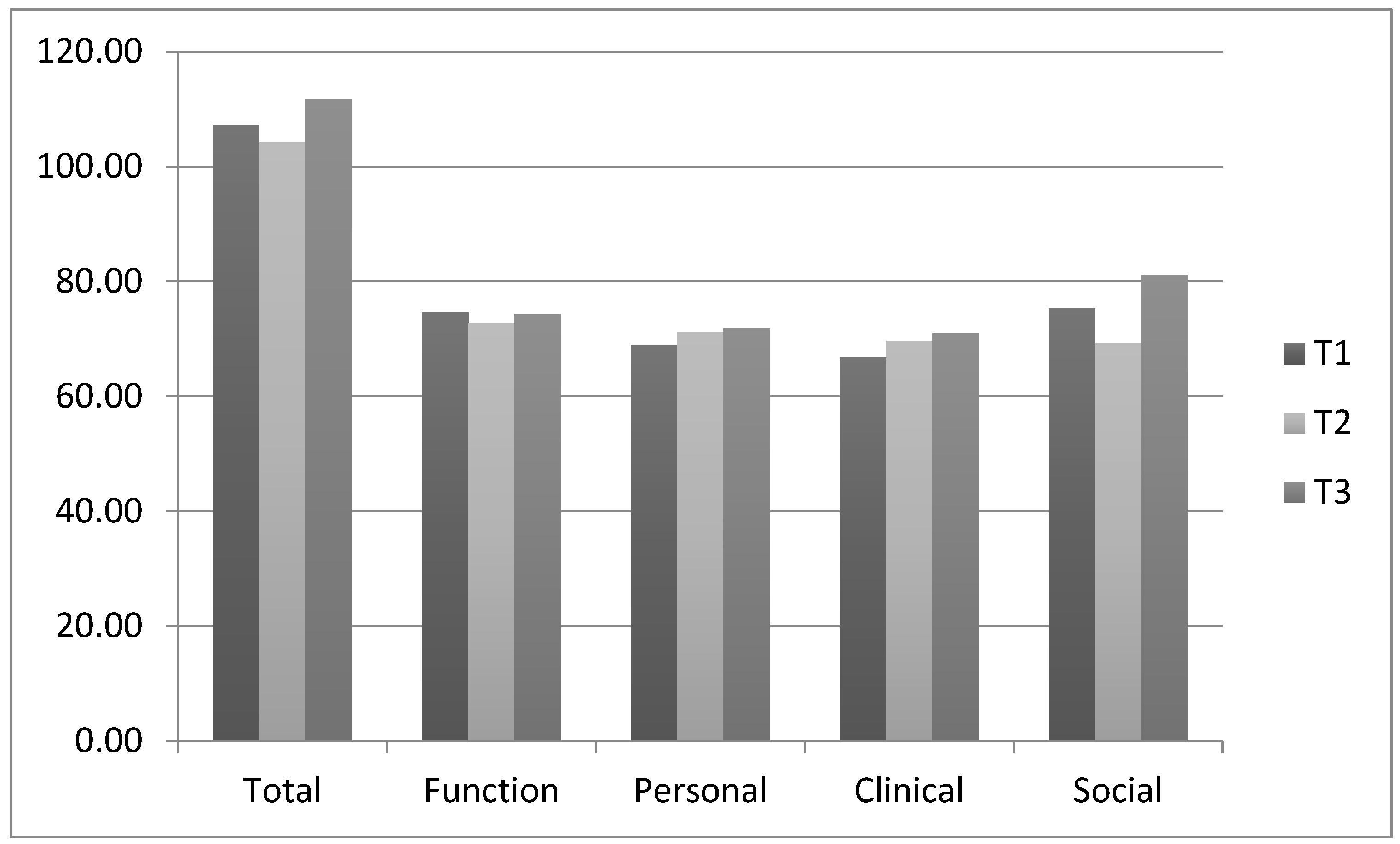
3.5. Psychosocial Health
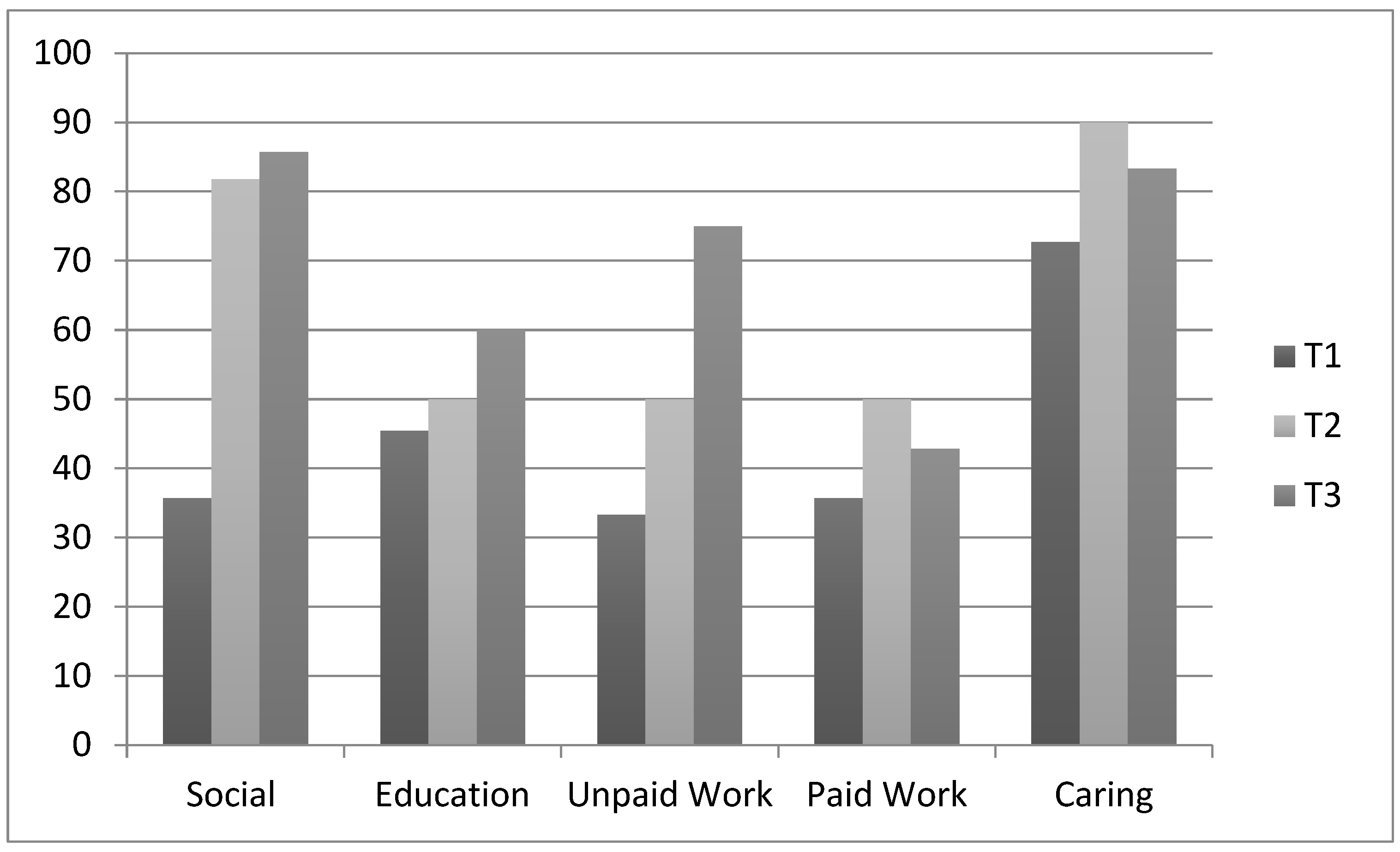
3.6. Community Participation and Well-Being
4. Discussion
Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Hunt, E.; McKay, E.A. A scoping review of time-use research in occupational therapy and occupational science. Scand. J. Occup. Ther. 2015, 22, 1–12. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Jacob, S.; Munro, I.; Taylor, B.; Griffiths, D. Mental health recovery: A review of the peer-reviewed published literature. Collegian 2017, 24, 53–61. [Google Scholar] [CrossRef] [PubMed]
- Thomas, N.; Farhall, J.; Foley, F.; Leitan, N.; Villagonzalo, K.; Ladd, E.; Nunan, C.; Farnan, S.; Frankish, R.; Smark, T.; et al. Promoting personal recovery in people with persisting psychotic disorders: Development and pilot study of a novel digital intervention. Front. Psychiatry 2016, 7, 196. [Google Scholar] [CrossRef] [PubMed]
- Jennings, C.; Lhuede, K.; Pepin, G.; Bradley, G.; Hitch, D. Activity participation patterns of community mental health consumers. Br. J. Occup. Ther. 2020, in press. [CrossRef]
- Waghorn, G.; Saha, S.; Harvey, C.; Morgan, V.A.; Waterreus, A.; Bush, R.; Castle, D.; Galletly, C.; Stain, H.J.; Neil, A.L.; et al. Earning and learning’ in those with psychotic disorders: The second Australian national survey of psychosis. Aust. N. Z. J. Psychiatry 2012, 46, 774–785. [Google Scholar] [CrossRef]
- Contreras, N.; Rossell, S.; Castle, D.; Fossey, E.; Morgan, D.; Crosse, C.; Harvey, C. Enhancing Work-Focused Supports for People with Severe Mental Illnesses in Australia. Rehabil. Res. Pract. 2012, 2012, 863203. [Google Scholar] [CrossRef]
- Eklund, M.; Leufstadius, C.; Bejerholm, U. Time use among people with psychiatric disabilities: Implications for practice. Psychiatr. Rehabil. J. 2009, 32, 177–191. [Google Scholar] [CrossRef]
- Shimitras, L.; Fossey, E.; Harvey, C. Time use of people living with schizophrenia in a North London catchment area. Br. J. Occup. Ther. 2003, 66, 46–54. [Google Scholar] [CrossRef]
- Morgan, V.; Waterreus, A.; Jablensky, A.; Mackinnon, A.; McGrath, J.; Carr, V.; Bush, R.; Castle, D.; Cohen, M.; Harvey, C.; et al. People Living with Psychotic Illness 2010: Report on the Second Australian National Survey; Australian Government: Canberra, Australia, 2011. [Google Scholar]
- Teychenne, M.; Ball, K.; Salmo, J. Sedentary Behavior and Depression Among Adults: A Review. Int. J. Behav. Med. 2010, 17, 246–254. [Google Scholar] [CrossRef]
- Galletly, C.; Foley, D.; Waterreus, A.; Watts, G.; Castle, D.; McGrath, J.; Mackinnon, A.; Morgan, V. Cardiometabolic risk factors in people with psychotic disorders: The second Australian national survey of psychosis. Aust. N. Z. J. Psychiatry 2012, 46, 753–761. [Google Scholar] [CrossRef]
- Cerimele, J.; Katon, W. Associations between health risk behaviors and symptoms of schizophrenia and bipolar disorder: A systematic review. Gen. Hosp. Psychiatry 2013, 35, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Dewa, C.S.; Trojanowski, L.; Cheng, C.; Loong, D. Examining the factors associated with paid employment of clients enrolled in first episode of psychosis programs. Schizophr. Res. Treat. 2012, 2012, 739616. [Google Scholar] [CrossRef] [PubMed]
- Cameron, J.; Sadlo, G.; Hart, A.; Walker, C. Return-to-work support for employees with mental health problems: Identifying and responding to key challenges of sick leave. Br. J. Occup. Ther. 2016, 79, 275–283. [Google Scholar] [CrossRef]
- Charzyńska, K.; Kucharska, K.; Mortimer, A. Does employment promote the process of recovery from schizophrenia? A review of the existing evidence. Int. J. Occup. Med. Environ. Health 2015, 28, 407–418. [Google Scholar] [CrossRef]
- Hitch, D.; Vernon, C.; Dun, L. Work and beyond: Vocational participation for mental health service users. Aust. N. Z. J. Psychiatry 2017, 51, 197. [Google Scholar] [CrossRef]
- Ramano, E.; Buys, T.; de Beer, M. Formulating a return-to-work decision for employees with major depressive disorders: Occupational therapists’ experiences. Afr. J. Prim. Health Care Fam. Med. 2016, 8, 1–5. [Google Scholar] [CrossRef]
- Ennals, P.; Fossey, E.; Howie, L. Postsecondary study and mental ill-health: A metasynthesis of qualitative research exploring students’ lived experiences. J. Ment. Health 2015, 24, 111–119. [Google Scholar] [CrossRef]
- Corbière, M.; Lecomte, T. Vocational services offered to people with severe mental illness. J. Ment. Health 2009, 18, 38–50. [Google Scholar] [CrossRef]
- Modini, M.; Tan, L.; Brinchmann, B.; Wang, M.J. Supported employment for people with severe mental illness: Systematic review and meta-analysis of the international evidence. Br. J. Psychiatry 2016, 209, 14–22. [Google Scholar] [CrossRef]
- Krupa, T.; Edgelow, M.; Chen, S.P.; Mieras, C.; Almas, A.; Perry, A.; Radloff-Gabriel, D.; Jackson, J.; Bransfield, M. Action over Inertia: Addressing the Activity-Health Needs of Individuals with Serious Mental Illness; Canadian Association of Occupational Therapists: Ottawa, ON, Canada, 2010. [Google Scholar]
- Edgelow, M.; Krupa, T. Randomized controlled pilot study of an occupational time-use intervention for people with serious mental illness. Am. J. Occup. Ther. 2011, 65, 267–276. [Google Scholar] [CrossRef]
- Rees, E. Implementing the Action over Inertia Program: Perspectives of Adults Experiencing Persistent Mental Illness and Occupational Therapists; LaTrobe University: Melbourne, Australia, 2017. [Google Scholar]
- Eklund, M.; Tjornstrand, C.; Sandlund, M.; Argentzell, E. Effectiveness of Balancing Everyday Life (BEL) versus standard occupational therapy for activity engagement and functioning among people with mental illness—A cluster RCT study. BMC Psychiatry 2017, 17, 363. [Google Scholar] [CrossRef] [PubMed]
- Bramley, S.; Mayne, N. The Works a Resource to Support You in Achieving Your Employment Ambitions; Sheffield Health and Social Care NHS Foundation Trust: Sheffield, UK, 2010. [Google Scholar]
- Fossey, E.; Bramley, S. Chapter 21: Work and vocational pursuits. In Creek’s Occupational Therapy in Mental Health, 5th ed.; Bannigan, K., Bryant, W., Fieldhouse, J., Eds.; Elsevier: London, UK, 2014. [Google Scholar]
- Robertson, J. Program Evaluation of Vocationally-Focused Workshops to Assist Consumers with Mental Illness in Their Journey to Employment. Master’s Thesis, LaTrobe University, Melbourne, VIC, Australia, 2015. [Google Scholar]
- Hitch, D.; Robertson, J.; Ochoteco, H.; McNeill, F.; Williams, A.; Lhuede, K.; Baini, A.; Hillman, A.; Fossey, E. An evaluation of a vocational group for people with mental health problems based on The WORKS framework. Br. J. Occup. Ther. 2017, 80, 717–725. [Google Scholar] [CrossRef]
- Curtin, J.; Hitch, D. Experiences and Perceptions of Facilitators of The WORKS. WORK J. Prev. Assess. Rehabil. 2017, 59, 607–616. [Google Scholar] [CrossRef]
- Curtin, J. Experiences and Perceptions of Facilitators of The WORKS Program; Deakin University: Geelong, Australia, 2015. [Google Scholar]
- Slade, M.; Phelan, M.; Thornicroft, G.; Parkman, S. The Camberwell Assessment of Need (CAN): Comparison of assessments by staff and patients of the needs of the severely mentally ill. Soc. Psychiatry Psychiatr. Epidemiol. 1996, 31, 109–113. [Google Scholar] [CrossRef] [PubMed]
- Trauer, T.; Tobias, G.; Slade, M. Development and evaluation of a patient-rated version of the Camberwell Assessment of Need Short Appraisal Schedule (CANSAS-P). Community Ment. Health J. 2008, 44, 113–124. [Google Scholar] [CrossRef]
- Ritsner, M.; Lisker, A.; Arbitman, M.; Grinshpoon, A. Factor structure in the Camberwell Assessment of Need-Patient Version: The correlations with dimensions of illness, personality and quality of life of schizophrenia patients. Psychiatry Clin. Neurosci. 2012, 66, 499–507. [Google Scholar] [CrossRef]
- Phipps, P.A.; Vernon, M.K. Twenty-Four Hours: An Overview of the Recall Diary Method and Data Quality in the American Time Use Survey. In Calendar and Time Diary: Methods in Life Course Research; Belli, R.F., Stafford, F.P., Alwin, D.F., Eds.; SAGE: Thousand Oaks, CA, USA, 2009. [Google Scholar]
- Hancock, N.; Scanlan, J.N.; Bundy, A.C.; Honey, A. Recovery Assessment Scale–Domain & Stages (RAS-DS) Manual; University of Sydney: Sydney, Australia, 2014. [Google Scholar]
- Scanlan, J.N.; Hancock, N.; Honey, A. The Recovery Assessment Scale-Domains and Stages (RAS-DS): Sensitivity to change over time and convergent validity with level of unmet need. Psychiatry Res. 2018, 216, 560–564. [Google Scholar] [CrossRef] [PubMed]
- Cameron, I.; Cunningham, L.; Crawford, J.; Eagles, J.; Eisen, S.; Lawton, K.; Naji, S.; Hamilton, R. Psychometric properties of the BASIS-24 (c) (Behaviour and Symptom Identification Scale-revised) Mental Health Outcome Measure. Int. J. Psychiatry Clin. Pract. 2007, 11, 36–43. [Google Scholar] [CrossRef]
- Pirkis, J.; Burgess, P.; Kirk, P.; Dodson, S.; Coombs, T. Review of Standardised Measures Used in the National Outcomes and Casemix Collection (NOCC); National Mental Health Strategy: Canberra, Australia, 2005. [Google Scholar]
- Australian Health Ministers Advisory Council Mental Health Information Strategy Standing Committee, Living in the Community Questionnaire (LCQ)—A Measure of Social Participaition: A Guide for the Use of the LCQ in Clinical Practice and for Service Development; National Mental Health Strategy: Canberra, Australia, 2016.
- Australian Health Ministers Advisory Council Mental Health Information Strategy Standing Committee, Living in the Community Questionnaire (LCQ)—A Measure of Social Participaition: Guide to the Technical Specifications of the LCQ for Organisations Seeking to Use the Instrument; National Mental Health Strategy: Canberra, Australia, 2016.
- Weber, N.S.; Cowan, D.N.; Millikan, A.M.; Niebuhr, D.W. Psychiatric and General Medical Conditions Comorbid With Schizophrenia in the National Hospital Discharge Survey. Psychiatr. Serv. 2009, 60, 1059–1067. [Google Scholar] [CrossRef]
- Werner, S. Needs assessment of individuals with serious mental illness: Can it help in promoting recovery? Community Ment. Health J. 2012, 48, 568–573. [Google Scholar] [CrossRef]
- Van Weeghel, J.; Boertien, D.; van Zelst, C.; Hasson-Ohayon, I. Conceptualisations, assessments, and implications of personal recovery in mental illness: A scoping review of systematic reviews and meta-analyses. Psychiatr. Rehabil. J. 2019, 42, 169–181. [Google Scholar] [CrossRef] [PubMed]
- Gehr, B.T.; Weiss, C.; Porzsolt, F. The fading of reported effectiveness. A meta-analysis of randomised controlled trials. BMC Med. Res. Methodol. 2006, 6, 25. [Google Scholar] [CrossRef] [PubMed]
- Allison, S.; Bastiampillai, T. Mental health services research the tipping point in Australian acute hospitals. Med. J. Aust. 2015, 203, 432–434. [Google Scholar] [CrossRef]
- Australian Institute of Health and Welfare (AIHW). Mental Health Services in Australia: Community Mental Health Care Services 2016–2017; AIHW: Canberra, Australia, 2018.
- Mental Health Council of Australia Submission to the Independent Review of the NDIS Act. Available online: https://mhaustralia.org/sites/default/files/docs/submission_to_the_independent_review_of_the_ndis_act.pdf (accessed on 7 May 2022).
- Turner-Crowson, J. The recovery vision for mental health services and research: A British perspective. Psychiatr. Rehabil. J. 2002, 25, 245–254. [Google Scholar] [CrossRef]
- Nagle, S.; Cook, J.V.; Polatajko, H.J. I’m doing as much as I can: Occupational choices of persons with a severe and persistent mental illness. J. Occup. Sci. 2011, 9, 72–81. [Google Scholar] [CrossRef]
- Hitch, D.; Pepin, G.; Richards, K. Facilitator and Consumer Experiences of Implementing the Pathways to Participation (P2P) Program; Deakin University: Geelong, Australia, 2020. [Google Scholar]
- Lamers, F.; Hoogendoorn, A.; Smit, J.; van Dyck, R.; Zitman, F.; Nolen, W.; Penninx, B. Sociodemographic and psychiatric determinants of attrition in the Netherlands Study of Depression and Anxiety (NESDA). Compr. Psychiatry 2012, 53, 63–70. [Google Scholar] [CrossRef]
| Week | Content |
|---|---|
| 1 |
|
| 2 |
|
| 3 |
|
| 4 |
|
| 5 |
|
| 6 |
|
| 7 |
|
| 8 |
|
| 9 |
|
| 10 |
|
| Activity Category | Time Use (Hours Per Day) Mean and Standard Deviation | ||
|---|---|---|---|
| T1 | T2 | T3 | |
| Sleep | 10.56 (±4.13) | 10.30 (±1.70) | 10.25 (±1.85) |
| Personal ADL | 2.72 (±1.56) | 2.40 (±0.97) | 2.89 (±0.91) |
| Instrumental ADL | 2.94 (±2.72) | 3.10 (±2.77) | 2.71 (±1.70) |
| Education/Work | 0.83 (±1.27) | 1.30 (±2.36) | 0.86 (±2.27) |
| Leisure | 6.56 (±2.89) | 6.80 (±3.33) | 6.14 (±3.13) |
| Social | 0.72 (±0.97) | 0.10 (±0.32) | 1.14 (±2.19) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hitch, D.; Vernon, L.; Collins, R.; Dun, C.; Palexas, S.; Lhuede, K. The Pathways to Participation (P2P) Program: A Pilot Outcomes Study. Int. J. Environ. Res. Public Health 2022, 19, 6088. https://doi.org/10.3390/ijerph19106088
Hitch D, Vernon L, Collins R, Dun C, Palexas S, Lhuede K. The Pathways to Participation (P2P) Program: A Pilot Outcomes Study. International Journal of Environmental Research and Public Health. 2022; 19(10):6088. https://doi.org/10.3390/ijerph19106088
Chicago/Turabian StyleHitch, Danielle, Lindsay Vernon, Rachel Collins, Carolyn Dun, Sarah Palexas, and Kate Lhuede. 2022. "The Pathways to Participation (P2P) Program: A Pilot Outcomes Study" International Journal of Environmental Research and Public Health 19, no. 10: 6088. https://doi.org/10.3390/ijerph19106088
APA StyleHitch, D., Vernon, L., Collins, R., Dun, C., Palexas, S., & Lhuede, K. (2022). The Pathways to Participation (P2P) Program: A Pilot Outcomes Study. International Journal of Environmental Research and Public Health, 19(10), 6088. https://doi.org/10.3390/ijerph19106088






