1. Introduction
Even if emphasis is placed on preserving limb length [
1], transfemoral amputations make up a substantial part of all amputations. Unfortunately, rehabilitation is especially difficult for transfemoral amputees, and research indicates that a high amputation level is associated with both prosthetic non-use and a decreased probability of remaining ambulatory [
2,
3]. Socket fit has been cited as one of the main factors affecting gait re-education, rehabilitation, and quality of life for amputees from the viewpoint of both amputees and clinicians [
4,
5,
6,
7,
8,
9]. Poor socket fit is the cause of at least one gait deviation, in people with lower limb amputation, which could be linked to premature long-term musculoskeletal degenerations [
6,
10,
11]. The importance of a well-fitting socket is highlighted by the fact that several patient evaluation questionnaires, which aim to measure the success of prosthetic devices, specifically refer to socket fit and comfort [
12,
13].
To solve this problem, sockets—which couple the residual limb and prosthesis—must provide sufficient support and stability during activities of daily living. This is complex as it largely depends on the inter-related performance of socket design, liner properties, suspension mechanisms, and prosthetic alignment [
14]. Large research efforts have thus been dedicated to prosthetic socket design [
15], and there are many different design philosophies for prosthetic sockets [
16]. There are two main socket types: total surface bearing (TSB), which aims to distribute the load evenly across the residual limb; and specific surface bearing (SSB) regions, which attempt to apply load through tolerant areas and hence off-load more sensitive regions [
16,
17,
18,
19]. For transfemoral amputees, these are most commonly ischial containment (IC) or sub-ischial–ramal containment sockets and quadrilateral (QUAD) sockets, respectively. IC sockets are considered to provide gait stability during single-limb support, which is partially achieved through TSB and by encasing the ischial tuberosity and ramus within the socket. In QUAD sockets, the ischium is outside of the socket, and weight is bored through the ischium on the socket brim, often resulting in gait instability [
15,
18]. Localized pressures from the socket are often causes of rejection by the patient; for example, on the medial ramus of IC sockets and on the perineum of QUAD sockets [
18]. For comparison, in transtibial amputees, the patellar-tendon bearing (PTB) is a commonly prescribed type of TSB socket. This relies on the localized loading of the patellar ligament to off-load more sensitive regions, such as the fibula head and tibial crest [
16,
17,
19,
20].
The inability of a socket to perform as expected can be highlighted through changes in pressure distributions at the interface between the residual limb and socket—caused by normal daily residual limb volume fluctuations, soft tissue adaptation during post-operative recovery, and edema, for example [
14,
21]. The effect of such residual limb volume changes on socket fit is known to result in pain, skin disease, and gait instability [
10,
11]. Whereby it has been reported that transfemoral residual limbs may exhibit larger volume fluctuations compared to transtibial residual limbs [
21]. Traditionally, and still predominantly, prosthetists utilize their experience and expertise to optimize socket design based on each individual patient’s characteristics, such as residual limb features and activity level [
15]. The current state-of-the-art employs the use of additional sock plies to accommodate for both daily volume changes and post-operative residual limb changes [
14]. Socks are worn over the residual limb when the socket is too loose or removed when the socket is too tight. However, this only uniformly alters the volume and is inconvenient and not always adhered to by prosthetics users [
11,
14,
22,
23,
24].
To address this issue, adjustable sockets have been developed in the field with both smart and manually controlled systems [
9,
14,
22,
25,
26,
27]. Pressure—whether qualitative or quantitative—is often the prescribed scale against which adjustable socket volumes are altered. For example, one of the aims of adjustable sockets is to reduce pressures and shear stresses at the stump–socket interface. In line with traditional socket design theory, the adjustable socket adapts to equally distribute pressure across the residual limb, or relieves pressure from sensitive regions by exerting more pressure through more tolerant regions [
14,
23,
27,
28,
29]. Furthermore, continuous socket volume adjustments have been shown to promote residual limb volume management [
9]. More generally, continuous monitoring, such as pressure and temperature at the stump–socket interface, can provide immediate feedback on socket fit [
4], which would enable more informed and timely intervention prescriptions by clinicians [
30,
31]. Thus, there has been growing interest in the development of such monitoring and sensing technologies to complement current clinical practice approaches to help overcome challenges in prosthetic use [
31,
32]. Indeed, pressure measurement and the mapping of lower-limb prosthetic sockets has already improved the understanding of prosthetic fit at a very fundamental level and has helped to facilitate objectively based socket designs [
15,
33]. During the last 50 years, a variety of measurement techniques have been employed in an effort to identify sites of excessive stresses [
32,
34,
35]. The objectives of this experimental research into the measurement of socket stresses were to improve the level of understanding of the stump–socket interface [
36], to evaluate the influence of prosthetic design parameters and alignment variations on the interface stress distribution, and to evaluate the quality of prosthetic fit [
37,
38]. Transfemoral amputees specifically, may thus benefit from the introduction of sensors to measure stress changes in both normal and tangential directions at the residuum–socket interface, both of which may be damaging to the soft tissues of the residuum [
39].
Arguably, the evolution of pressure sensor systems for this purpose has been limited by the technical difficulties in addressing the demanding requirements of the
day-to-day monitoring of the comfort and fit of prosthetic sockets. Walking in a laboratory and walking in “real life” is often not the same [
40], and clinical tools will always be a niche market in comparison to technology used in consumer goods. However, these technical challenges are being overcome due to the emergence of wearable, cheap, and technically sophisticated sensing technology for health monitoring [
41,
42,
43]. Breakthroughs, tested in the smart health domain, have occurred in wireless technology for data-intensive applications [
44], power harvesting [
45], security [
46], analytics [
47], rapid prototyping and manufacturing [
48], and materials [
49]. The likelihood that easily deployed, cheap, and reliable pressure sensors systems for clinical use will emerge has thus drastically increased during the last few years, even if several challenges remain.
One of the main challenges in the development of new and improved prosthetic technologies is the lack of practical inner socket sensors for monitoring the environment between the skin and the liner or socket [
37], or the region between the residual limb and the socket [
50]. Selecting suitable transducers is also challenging and relies on the specific experimental and clinical environment [
30,
37,
51]. In general, four main types of sensors are used for pressure measurements in the socket: strain gauges and piezoresistive, capacitive, and optical sensors [
32]. A review of research on interfacial stress measurements at the stump–socket interface of transtibial amputees found many merits in sensor development over the past 50 years; for instance, high sensitivity, reproducibility, higher spatial resolution, lightweight, ease of use, availability in various shapes and sizes, and the capability of conforming to irregular shapes. However, while some of these sensors provide valuable information, they are disadvantageous due to their bulkiness, weight, inflexibility, cost, and laborious integration methods with the socket [
38,
50]. In lower limb prostheses, measurements and mapping pressures to amputees’ anatomy are also commonly performed using commercially available, semi-flexible pressure monitoring systems such as the F-Socket (Tekscan, Inc., South Boston, MA, USA) [
34,
36,
52,
53,
54] or Pliance
® system (Novel
® GMBH, Munich, Germany) [
55,
56]. While these systems do not require socket modification, they are still spatially limited [
4], cannot be readily integrated into existing prosthetic components [
50], and are not sensitive to shear stresses [
39]. To be able to overcome some of the shortcomings associated with currently available pressure monitoring systems, textile-based sensors have also been studied due to their compliance and breathability, and relatively simple fabrication methods [
50]. Moreover, to be able to eliminate the dependency on bulky, rigid components inside the socket, and also to be able to support continuous, long-range wireless communication to standard consumer electronics, conformable sensors have also been investigated [
4].
Furthermore, this particular application of pressure sensors is a highly specialized endeavor, and transfemoral amputees are a specific cohort with many unique characteristics compared with those with other levels of amputation. Many of the previously mentioned research developments for lower limb prosthetics were solely tested with transtibial amputees [
4,
10,
11,
23,
50]. Several review articles on lower limb socket technology do not explicitly discriminate their findings against transfemoral or transtibial prostheses, but all instances cited more articles whose titles referred to the terms transtibial or below-knee compared with the terms transfemoral or above-knee, with a roughly 2.4 times higher prevalence on average [
9,
15,
32,
36,
57]. This is further emphasized by another review article that analyzed interface stress measurements in transtibial sockets only [
38], but similar analyses have not been published for transfemoral amputees; thus, the data for transfemoral amputees are very limited [
15]. It is thus unclear whether existing findings regarding the use of pressure sensors to improve comfort and fit are applicable, or whether associated studies are conducted in ways that are likely to lead to substantial breakthroughs. This is an especially pressing concern for studies with an experimental design, as these should reconcile multiple research and industry disciplines to arrive at valid results. This is further aggravated by the lack of research that is clinically powerful—for transfemoral prosthetic socket comfort and fitness—due to the low methodological quality of the study design in numerous biomechanical and patient-centric studies [
9].
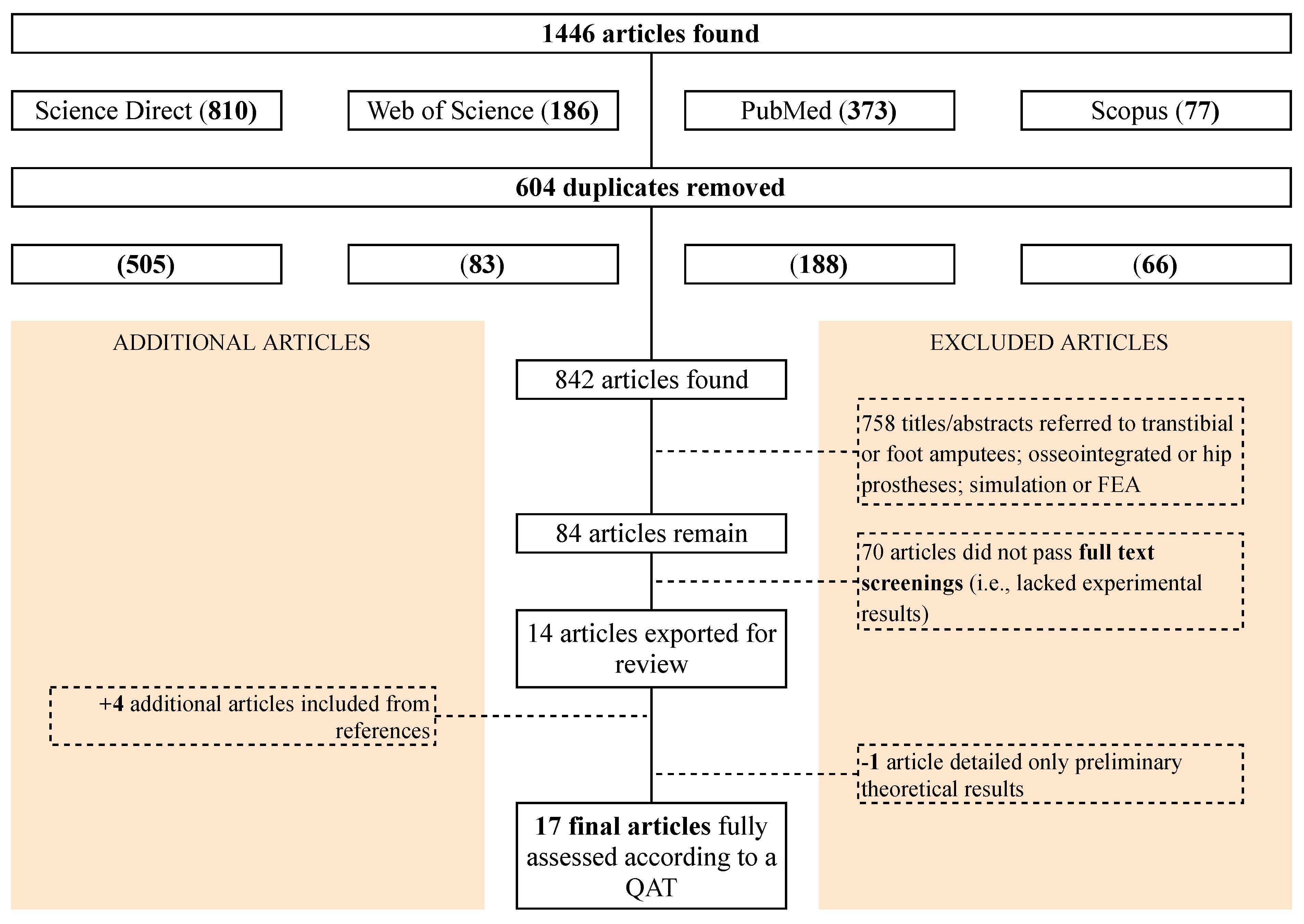
To investigate whether the use of pressure sensors in prostheses is relevant for transfemoral amputees and whether there is any possibility to help guide methodological choices in future studies, we surveyed the existing literature in a scoping review. The review was reported following the relevant extension to the PRISMA guidelines [
58,
59]. The focus was to map the existing research on the use of pressure sensors to support transfemoral amputees and identify knowledge gaps as well as the strengths and weaknesses in the associated study designs. In this study, we therefore aimed to address the following research questions:
- 1.
Is there a de facto methodology for experimental studies of the implications of intra-socket pressure sensors used by transfemoral amputees?
- 2.
How should sensors be designed for application in prosthetic sockets to monitor transfemoral amputees for evaluating comfort and fit?
Answering these questions should facilitate the emergence of sensing, monitoring, and actuator technologies, specifically for the application of lower limb prosthetics, with the potential to significantly improve socket design and provide effective residual limb health monitoring.
4. Synthesis and Discussion
The aim of this review was to identify the current practices of sensors in transfemoral sockets with the ultimate goal of advancing and improving prosthetic socket design, comfort, and fit for transfemoral amputees. To achieve this, two research questions came to light:
- 1.
Is there a de facto methodology for experimental studies of the implications of intra-socket pressure sensors used by transfemoral amputees?
- 2.
How should sensors be designed for application in prosthetic sockets to monitor transfemoral amputees towards evaluating comfort and fit?
In this section, the first question is addressed by discussing the descriptive codes in a more direct manner. Meanwhile, a holistic approach is taken with regards to the second question as it involves several different knowledge domains. Finally, the outcomes from these two research questions are concluded with considerations for future research.
4.1. De Facto Methodology
From the coding analysis of the literature, a few common methods were found that indicated a de facto methodology.
The importance of sensor selection was inferred by the numerous codes found relating to sensor characteristics for this application—lower-limb prosthetic sockets. A significantly large range of recorded maximum socket–residual limb interface pressures were cited across the literature. This indicates the importance of sensor calibration prior to experimental procedures, which is supported by the fact that seven of the reviewed papers reported on the calibration methods and measurable range of the sensors [
39,
64,
65,
66,
67,
68,
71]. Care should therefore be taken to select sensors with suitable capabilities and to appropriately calibrate the sensors to enable accurate recordings over the aforementioned large pressure ranges. For comparative pressure measurements, it may be necessary for the sensors to also be sensitive to low pressures. Sensor sensitivity and a suitable error measurement range should therefore also be considered. This is particularly important if the same sensors are used for different subjects and socket types. Individual patient characteristics can significantly influence the pressure readings. For example, patient weight in combination with the size of the sensing area are obvious factors that will influence the magnitude of pressure [
65]. It is therefore not only important to document the patient characteristics but also to consider their effect on the resulting intra-socket pressure distributions.
Current technological challenges and practical issues—such as sensor thickness, sensor accuracy for measurement in curved surfaces, and tethered measuring systems, as well as the highly personalized nature of prosthetic sockets—makes it unfeasible to measure dynamic pressures across the entire stump–socket interface simultaneously [
77]. Although it is possible to record section-wise pressure measurements until the whole residual limb has been mapped, it is time-consuming, impractical, and leads to other variabilities that could influence the pressure mapping results, and hence also socket comfort or fitting interpretations [
65]. The reviewed literature has presented various alternative solutions to address these limitations, such as methodically placing individual sensors at specified sites in the prosthetic socket. This systematic sensor placement must be based on each individual’s anatomy to ensure pressure comparisons are made in the same anatomical region for different patients. This is important as it is evident that the maximum recorded pressure values vary greatly depending on the anatomical region [
64]. This approach was proven beneficial for pressure distribution comparisons across different socket types and subjects in a number of studies [
64,
66,
67,
71]. There are strong implications from the synthesized evidence of our work that more valuable pressure information is obtained when sensors are positioned at specified known problematic regions; for example, the medial brim or the distal end [
64,
66,
67,
71].
To fulfill the need for repeatable sensor placement, a number of pre-defined sensor locations could be assigned. This assignment could be standardized based on anatomical segmentation; for example, by dividing the residuum into quadrants—anterior, posterior, medial, and lateral—and further discretizing them into proximal and distal regions. Additional sensors could then be given the flexibility of being positioned at subject-specific problematic sites, such as at the brim, or in sensitive areas prone to tissue breakdown. This standardized approach enables both intra-subject and inter-subject relative pressure comparisons, reducing the importance of absolute pressure values. To elaborate, measurements at low-pressure regions could provide insights regarding the implications of comparatively high-pressure regions for the individual patient—with regards to comfort or risk of tissue damage, for example. Meanwhile, the relative pressure difference in these separate regions can be compared between subjects to eliminate the need to account for subjects’ weights.
The method of sensor integration in the socket should also be considered to avoid co-intervention. It should be ensured that the subject feels the socket fits as it would without the sensing system in place. This highlights the importance of giving the subject time to adjust to the socket prior to tests, and noting if the socket fit is unusual. An unusual fit could cause the subject to walk with an atypical gait, which could result in abnormal pressure measurements and distributions.
One reason it is difficult to compare across different studies is the almost unlimited possibilities for presenting data. The time-dependent (i.e., days, weeks, months) variability of pressure in the socket strongly suggests average measurements to be an optimal method for presenting the data. As the pressure magnitudes vary greatly depending on the anatomical region, presenting the pressure information separately for each anatomical compartment is also recommended. Segmenting and averaging measurements with respect to the gait cycle to identify cyclic pressure patterns—and reporting the standard deviations—is at least arguably more informative than simply citing the maximum measured pressure values.
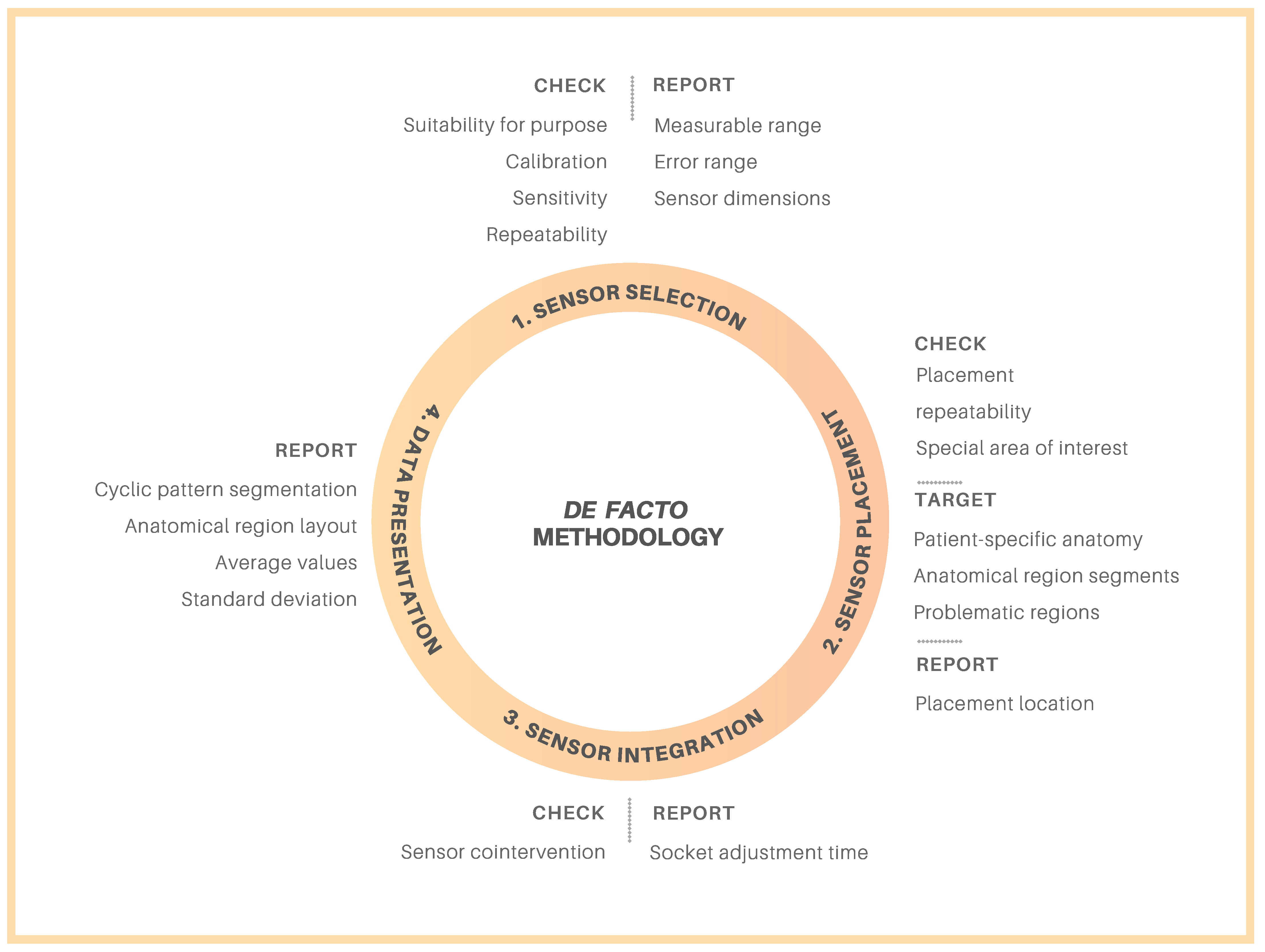
Overall, with regards to sensor implementation, a de facto methodology that was evaluated from the literature can be summarized into four major categories: (1) sensor selection, (2) sensor placement, (3) sensor integration, and (4) data presentation, as illustrated in
Figure 2. Although this methodology was primarily initiated considering transfemoral prosthetic socket users, and while these categories individually play a crucial role, many attributes from each category can be directly transferred for use by patients with transtibial amputations. However, some items must be specialized depending on whether the patient has a transtibial or transfemoral amputation. Firstly, the suitability of sensors is based on the ability to integrate the hardware into the socket. This includes the method of hardware integration with the socket as well as sensor dimensions to ensure the sensors neither interfere with the rest of the prosthetic system nor cause contraindications for the patient with regards to socket comfort and fit. Secondly, ensuring the technical suitability of the sensors is also recommended. For example, the measurable pressure range should cover the expected pressure ranges in the socket during activities of daily living. Furthermore, the establishment of a sensor calibration procedure for repeatable measurements should allow for comparable measurements between patients. It is likely that sensor calibration procedures and sensitivity and repeatability requirements will be the same for measurements in both transtibial and transfemoral sockets. Conversely, the sensor dimensions required may differ depending on amputation level as transtibial sockets tend to be much smaller with smaller radii of curvature, for instance.
A method for the repeatable placement of sensors is particularly advantageous for inter-subject comparisons, but is also helpful for testing different sockets for the same subject [
78]. This procedure is likely to be directly transferable between transtibial and transfemoral socket types. However, different socket types are designed to influence gait stability and interactive motions within the soft tissue, between the soft tissue and the socket [
15,
18,
20], and femoral movement within the residual limb [
79]. Furthermore, the specified anatomical locations of interest will differ between amputation levels. In transtibial sockets, for example, the tibial crest and tibial tubercle often require pressure relief [
20], and thus it would be meaningful to measure pressure at these locations. However, in transfemoral sockets, sensors located at the ischium would be valuable as this can be the most problematic region for transfemoral amputees [
18]. Individual patient residual limb characteristics, such as stump shape, tissue stiffness, the underlying muscle strength, and scar tissue, also significantly influence interfacial pressure patterns [
67,
69,
73]. This further highlights the need to target sensor placement not only based on the amputation level but ideally also customized for each patient to yield valuable results.
Strategic sensor selection (as previously described) should facilitate smooth hardware integration with the prosthetic socket. However, cointerventions can be minimized further by providing the patient with an adjustment period and by requesting feedback should their socket feel unusual.
Presenting relevant data in a coherent manner is essential in order to provide valuable information to the scientific community. The literature revealed the advantages of segmenting pressure into gait cycles and citing the average values. Given the contrasting pressure ranges and patterns depending on the anatomical location, the benefits of displaying the findings with respect to the patient’s anatomy was also highlighted from the reviewed literature. Furthermore, it is highly recommended that future studies record subjective feedback from the patients themselves.
The suggested de facto methodology is based on the studied literature, but as should be apparent, no single study makes use of all of its parts. This paper can thus highlight attributes that can be transferred from and for use by patients with transtibial amputations and others which require specialization for patients with transfemoral amputations. However, we must conclude that directly comparing pressure measurements between the included studies, or to measurements taken in studies including patients with transtibial amputations, cannot (yet) be justified. The characteristics of patients are seldom described well enough to ensure valid comparisons, and when these data are available, there is substantial variation in regard to important characteristics such as weight. In fact, none of the included studies broached the subject of known gait deviations due to the improper construction of transtibial and transfemoral prostheses. The impact of these on pressure readings can vary substantially, as they can lead to an exaggerated transfer of load to a patient’s healthy side and involve effects such as foot slaps [
80]. Sensor characteristics such as measurement and error range would most likely be most important when identifying such gait deviations with precision. However, the total error range of pressure sensors is, for example, seldom discussed, and when discussed, this is only in comparison to other sensor technologies. This does not help to define how large the total sensor error can be and remain acceptable, neither in the generic case nor for any specific patient type or gait deviation.
Hopefully, with more studies adhering to all parts of the suggested methodology, the acceptable and suitable ranges for measurements and errors can be identified.
4.2. Implications for the Design of Sensors
The implications of this survey for how sensors should be designed for application in prosthetic sockets of transfemoral amputees for monitoring to evaluate comfort and fit is strongly tied to what the discourse does not contain; almost all surveyed papers avoided defining hypotheses in lieu of large-scale data collection for inductive analysis.
Inductive analysis can be a powerful tool, and it would be speculative to attribute its widespread use among the papers to any particular motivation of the authors. Rowbottom and Alexander [
81] found that exploratory data gathering is actually more widespread in biomechanical research than a quick reading would imply. In other words, presentational hypotheses—i.e., hypotheses that do not influence the actual study—seem to be a frequent problem in the field. As this practice can be misleading regarding the significance of results, there is most likely a need for researchers within the field to start accepting such studies on their own merits (to avoid tempting researchers to present their studies as something they are not). However, exploratory data gathering seems to be especially difficult to use for designing sensors for monitoring to evaluate comfort and fit. Feelings of comfort or discomfort attributed to a well-fitting or ill-formed prosthesis can be influenced by many characteristics of the amputee, prosthesis, and surrounding environment. Generalizing across large amounts of data is easily confounded by such factors, as they for instance mean that comfort is not directly correlated to tightness or looseness [
73] and that discomfort can be “disguised” by an abnormal gait [
72]. Similarly, this means that the data are not necessarily suitable for analysis, as these characteristics can skew data sets. For example, both highly contoured sites on the residual limb [
34] and the way the environment in a prosthetic exposes sensors to wear [
34,
69] can confound measurements. To properly validate a sensor system, several different types of scenarios might have to be considered—a potentially costly requirement. As an example, a recently developed sensor system was validated in three scenarios: (1) a flat bench-top test, (2) in a prosthetic socket at a low curvature site, and (3) in a socket at a higher curvature site [
78]. In fact, the same sensors were also tested under dynamic cyclic loading to simulate realistic use conditions.
It is understandable if the sheer complexity provokes researchers working on sensor technology to focus more on technology and less on contextual factors (see e.g., [
69]). However, this limited perspective is likely an obstacle to innovation in sensor design in this context. Contemporary studies by researchers that actually use pressure sensors to investigate monitoring to evaluate comfort and fit have more specific needs. These include, for instance, attempts to identify whether amputees tense their muscles to avoid high pressure [
64]; the size of areas of local, high pressure [
65]; prosthetic migration and socket movement [
71]; and whether the prosthesis stabilizes the residual limb [
73]. Large-scale data measurements of pressure at several locations
could by pure chance help to solve these needs, but it is highly unlikely. To help address this issue, we propose guidance in three steps for researchers targeting this application domain.
- 1.
Define and operationalize hypothetical constructs: Fit and comfort are hypothetical constructs—i.e., qualitative variables—which are not directly observable. Unfortunately, with no agreed way of operationalizing these constructs for transfemoral amputees, the implications of any pressure measurements are unclear. Therefore, sensor designers should ensure that their pressure measurements can be related to a suitably limited part of fit and comfort—ideally, with the support of experts possessing relevant knowledge on the constructs.
- 2.
Ensure necessary coverage of the operationalized construct: This suggests that it would be fruitful to develop pressure sensors in close combination with other types of sensors. Otherwise, it might be difficult to ensure that the operationalization can be properly measured. As an example, several of the surveyed papers noted an interest in measuring shear [
39,
72,
74]. Presumably, a well-integrated combination of pressure and shear sensors is required to answer several of the aforementioned needs, such as identifying the existence, explanation, and effect of prosthetic migration on fit. The integration of other types of sensors with pressure sensors can provide a deeper understanding of the interaction between the residual limb and the prosthetic socket. For example, electromyography (EMG) [
82] and temperature sensors [
83] can provide insights to the relationship between muscle activities and intra-socket climate, respectively, with interface pressure. The integration of gait monitoring devices is undoubtedly useful to evaluate these sensor measurements as a function of the gait cycle, or with respect to level of activity [
4,
9,
32,
78,
82]. This might seem trivial to accomplish, but there are several reasons why researchers are currently avoiding this approach. To name a few, it requires knowledge of several types of sensor technology, it multiplies the difficulty of all problems related to handling large amounts of data, and it makes issues related to advanced prototyping even more likely to surface.
- 3.
Make use of relevant expertise when evaluating measurements: Finally, as achieving correct operationalization and measurement coverage are difficult, results must (also) be evaluated together with experts possessing relevant knowledge on the constructs. This is especially important as results might otherwise only be considered in relation to the most obvious use cases; i.e., level ground walking. As an example, not much effort has been devoted to studying the implications of sensor measurements for the wearing of prostheses, even though the pressures measured during this use case can be as high as during normal walking [
67]. Naturally, professionals working with prostheses can be uninterested in adopting pressure sensors, or risk misunderstanding their implications, if pressure readings are only fully understood for a small part of normal prosthesis usage.
If researchers who wish to have an impact on the medical application domain adopt these three steps during conceptual design and pressure sensor evaluation, the chance of breakthroughs in prosthetic design should increase substantially.
4.3. Implications for Research
It is clear that experts from several different domains need to cooperate in a consistent way to carry out the identified de facto methodology, especially when the aim is to achieve breakthroughs in sensor design. Two examples of when cooperation is required are as follows: (a) even if engineers are the foremost experts on identifying appropriate sensor capabilities and calibration, this activity will rely on prosthetists’ knowledge regarding prostheses and medical experts’ knowledge of patients; and (b) even if medical experts can identify problematic regions on stumps, recording pressure there requires engineers to develop portable, and yet powerful, data recording systems. As an example, Karamousadakis et al., [
84] developed a fuzzy logic-based decision support system for socket design modifications for improved fit. The fuzzy rules are based on the expert knowledge of prosthetist(s), and the patient-specific socket modification suggestions are governed by their own intra-socket pressure information. Furthermore, as noted, overcoming complexity and focusing on the most important questions will require all of these experts to share their domain knowledge with each other.
This study has two important implications in this regard. Firstly, the de facto methodology can form a base for comparing studies. However, it can also be help to make studies valuable to a wider group of experts. Dividing pressure data between anatomical regions might not be important for the purpose of an engineer designing a novel sensor, but it might be critical for a prosthetist to make further use of the study. Secondly, purely inductive, data-driven research might not be optimal for achieving breakthroughs in this area. Ideally, this should be solved by more hypothesis-driven research in each study through close cooperation between different domain experts. However, when this is not possible, researchers should consider creating fine-grained open research data to possibly support the hypotheses testing of other, future studies.