Novel Method for Sealing Tracheostomies Immediately after Decannulation—An Acute Clinical Feasibility Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design, Setting, and Study Population
2.2. Ethics
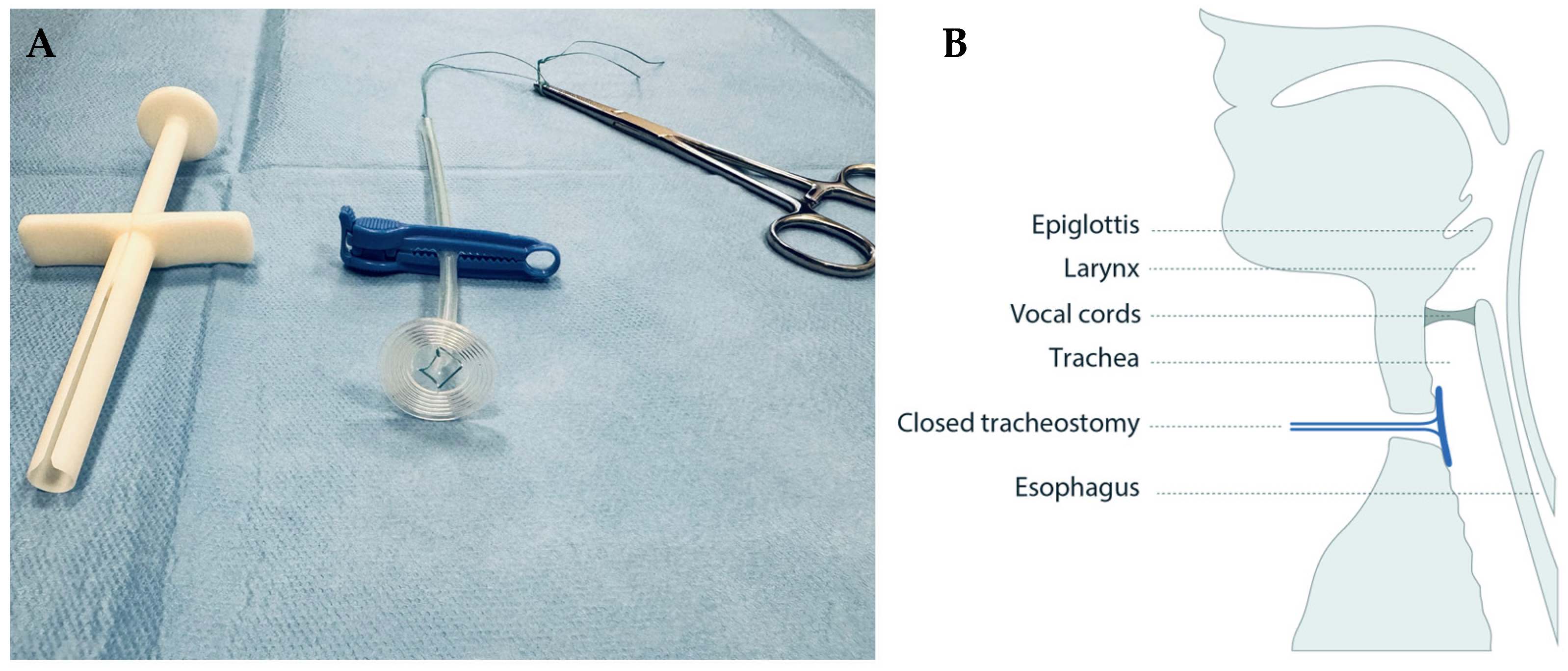
2.3. The Tracheostomy Sealing Disc
2.4. Procedure in Sub-Study One
2.5. Procedure in Sub-Study Two
2.6. Data Collection
2.7. Statistical Analysis
3. Results
3.1. Patient Characteristics
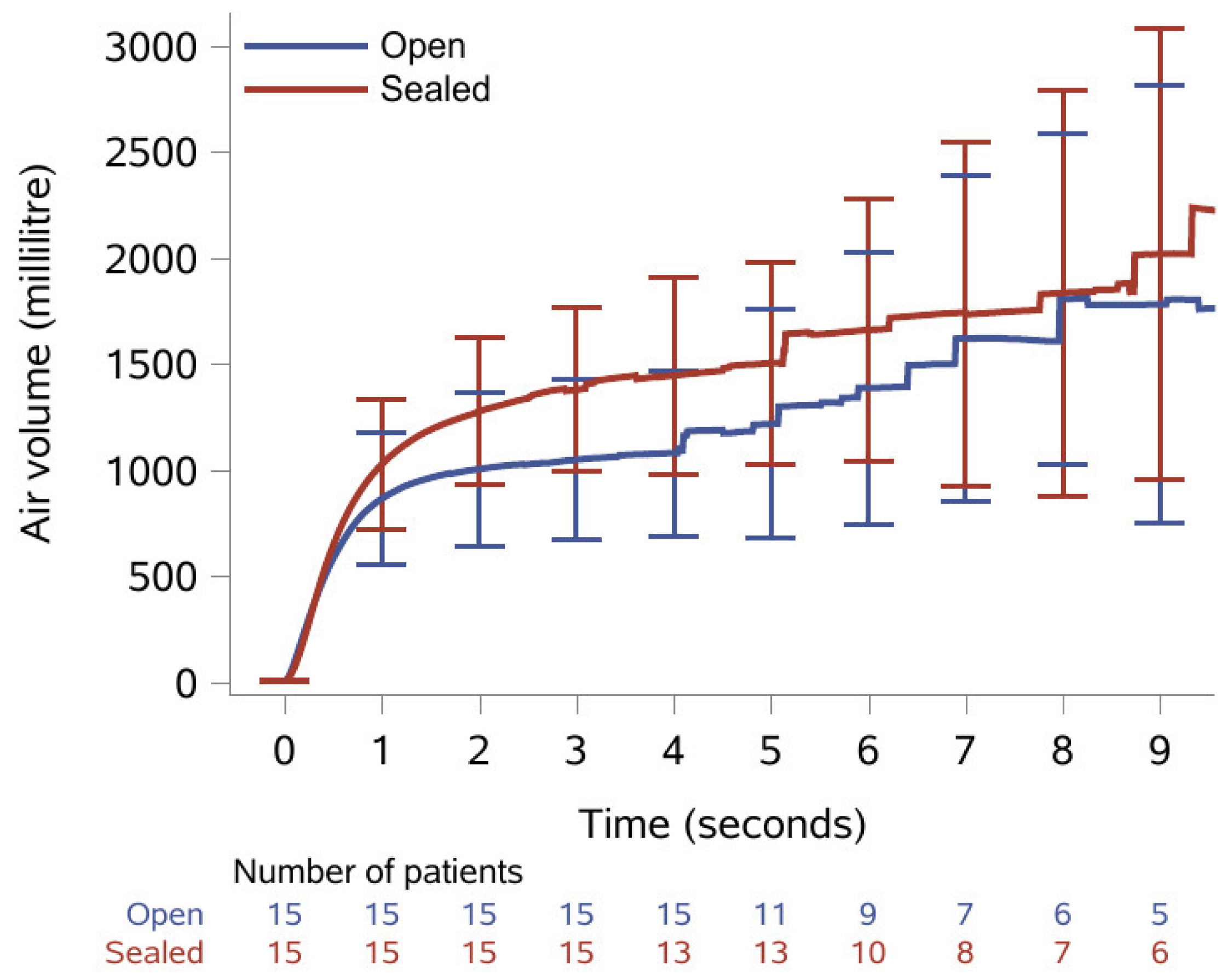
3.2. Spirometry
3.3. Voice Quality Assessment
4. Discussion
4.1. Limitations
4.2. Perspective
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Choby, G.; Goldenberg, D. The history of tracheotomy. Pharos Alpha Omega Alpha Honor Med. Soc. 2011, 74, 34–38. [Google Scholar]
- Durbin, C.G., Jr. Tracheostomy: Why, when, and how? Respir. Care 2010, 55, 1056–1068. [Google Scholar]
- Mussa, C.C.; Gomaa, D.; Rowley, D.D.; Schmidt, U.; Ginier, E.; Strickland, S.L. AARC Clinical Practice Guideline: Management of Adult Patients with Tracheostomy in the Acute Care Setting. Respir. Care 2021, 66, 156–169. [Google Scholar] [CrossRef] [PubMed]
- Bissett, B.; Gosselink, R.; van Haren, F.M.P. Respiratory Muscle Rehabilitation in Patients with Prolonged Mechanical Ventilation: A Targeted Approach. Crit. Care 2020, 24, 103. [Google Scholar] [CrossRef] [PubMed]
- Jang, M.H.; Shin, M.J.; Shin, Y.B. Pulmonary and Physical Rehabilitation in Critically Ill Patients. Acute Crit. Care 2019, 34, 1–13. [Google Scholar] [CrossRef]
- Choate, K.; Barbetti, J.; Currey, J. Tracheostomy decannulation failure rate following critical illness: A prospective descriptive study. Aust. Crit. Care 2009, 22, 8–15. [Google Scholar] [CrossRef]
- Stelfox, H.T.; Crimi, C.; Berra, L.; Noto, A.; Schmidt, U.; Bigatello, L.M.; Hess, D. Determinants of tracheostomy decannulation: An international survey. Crit. Care 2008, 12, R26. [Google Scholar] [CrossRef]
- Bishnoi, T.; Sahu, P.K.; Arjun, A.P. Evaluation of Factors Determining Tracheostomy Decannulation Failure Rate in Adults: An Indian Perspective Descriptive Study. Indian. J. Otolaryngol. Head Neck Surg. 2022, 74, 4849–4854. [Google Scholar] [CrossRef]
- Bach, J.R.; Saporito, L.R. Indications and criteria for decannulation and transition from invasive to noninvasive long-term ventilatory support. Respir. Care 1994, 39, 515–528; discussion 529–531. [Google Scholar] [PubMed]
- Cameron, J.L.; Reynolds, J.; Zuidema, G.D. Aspiration in patients with tracheostomies. Surg. Gynecol. Obstet. 1973, 136, 68–70. [Google Scholar] [CrossRef]
- Brenner, M.J.; Pandian, V.; Milliren, C.E.; Graham, D.A.; Zaga, C.; Morris, L.L.; Bedwell, J.R.; Das, P.; Zhu, H.; Lee, Y.A.J.; et al. Global Tracheostomy Collaborative: Data-driven improvements in patient safety through multidisciplinary teamwork, standardisation, education, and patient partnership. Br. J. Anaesth. 2020, 125, e104–e118. [Google Scholar] [CrossRef] [PubMed]
- Saliba, K.A.; Blackstock, F.; McCarren, B.; Tang, C.Y. Effect of Positive Expiratory Pressure Therapy on Lung Volumes and Health Outcomes in Adults with Chest Trauma: A Systematic Review and Meta-Analysis. Phys. Ther. 2022, 102, pzab254. [Google Scholar] [CrossRef] [PubMed]
- Guia, M.; Ciobanu, L.D.; Sreedharan, J.K.; Abdelrahim, M.E.; Gonçalves, G.; Cabrita, B.; Alqahtani, J.S.; Duan, J.; El-Khatib, M.; Diaz-Abad, M.; et al. The role of non-invasive ventilation in weaning and decannulating critically ill patients with tracheostomy: A narrative review of the literature. Pulmonology 2021, 27, 43–51. [Google Scholar] [CrossRef] [PubMed]
- Freeman-Sanderson, A.L.; Togher, L.; Elkins, M.; Kenny, B. Quality of life improves for tracheostomy patients with return of voice: A mixed methods evaluation of the patient experience across the care continuum. Intensive Crit. Care Nurs. 2018, 46, 10–16. [Google Scholar] [CrossRef] [PubMed]
- Newman, H.; Clunie, G.; Wallace, S.; Smith, C.; Martin, D.; Pattison, N. What matters most to adults with a tracheostomy in ICU and the implications for clinical practice: A qualitative systematic review and metasynthesis. J. Crit. Care 2022, 72, 154145. [Google Scholar] [CrossRef] [PubMed]
- Madsen, K.R.; Guldager, H.; Rewers, M.; Weber, S.O.; Købke-Jacobsen, K.; White, J. Danish Guidelines 2015 for percutaneous dilatational tracheostomy in the intensive care unit. Dan. Med. J. 2015, 62, C5042. [Google Scholar] [PubMed]
- Chadda, K.; Louis, B.; Benaïssa, L.; Annane, D.; Gajdos, P.; Raphaël, J.C.; Lofaso, F. Physiological effects of decannulation in tracheostomized patients. Intensive Care Med. 2002, 28, 1761–1767. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.K.; Saran, S.; Baronia, A.K. The practice of tracheostomy decannulation-a systematic review. J. Intensive Care 2017, 5, 38. [Google Scholar] [CrossRef] [PubMed]
- Kutsukutsa, J.; Mashamba-Thompson, T.P.; Saman, Y. Tracheostomy decannulation methods and procedures in adults: A systematic scoping review protocol. Syst. Rev. 2017, 6, 239. [Google Scholar] [CrossRef]
- Whitmore, K.A.; Townsend, S.C.; Laupland, K.B. Management of tracheostomies in the intensive care unit: A scoping review. BMJ Open Respir. Res. 2020, 7, e000651. [Google Scholar] [CrossRef]
- Andriolo, B.N.; Andriolo, R.B.; Saconato, H.; Atallah, Á.N.; Valente, O. Early versus late tracheostomy for critically ill patients. Cochrane Database Syst. Rev. 2015, 1, CD007271. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.L.; Burge, A.T.; Holland, A.E. Airway clearance techniques for bronchiectasis. Cochrane Database Syst. Rev. 2015, 2015, CD008351. [Google Scholar] [CrossRef] [PubMed]
- Wilson, L.M.; Morrison, L.; Robinson, K.A. Airway clearance techniques for cystic fibrosis: An overview of Cochrane systematic reviews. Cochrane Database Syst. Rev. 2019, 1, CD011231. [Google Scholar] [CrossRef] [PubMed]
- Lusquinhos, J.; Tavares, M.; Abelha, F. Postoperative Pulmonary Complications and Perioperative Strategies: A Systematic Review. Cureus 2023, 15, e38786. [Google Scholar] [CrossRef] [PubMed]
- Christiansen, K.J.; Kristensen, K.J.; Larsen, H.N. Device for Sealing a Tracheostoma in a Patient. European Patent 11,738,160 B2, 9 July 2020. [Google Scholar]
- Christiansen, K.J.; Moeslund, N.; Lauridsen, H.; Devantier, L.; Rohde, M.C.; Kjærgaard, B.; Pedersen, M. Intratracheal Seal Disc: A Novel Tracheostoma Closure Device. Respir. Care 2017, 62, 970–977. [Google Scholar] [CrossRef] [PubMed]
- Graham, B.L.; Steenbruggen, I.; Miller, M.R.; Barjaktarevic, I.Z.; Cooper, B.G.; Hall, G.L.; Hallstrand, T.S.; Kaminsky, D.A.; McCarthy, K.; McCormack, M.C.; et al. Standardization of Spirometry 2019 Update. An Official American Thoracic Society and European Respiratory Society Technical Statement. Am. J. Respir. Crit. Care Med. 2019, 200, e70–e88. [Google Scholar] [CrossRef]
- Yiu, E.M.; Ng, C.Y. Equal appearing interval and visual analogue scaling of perceptual roughness and breathiness. Clin. Linguist. Phon. 2004, 18, 211–229. [Google Scholar] [CrossRef]
- Brancamp, T.U.; Lewis, K.E.; Watterson, T. The relationship between nasalance scores and nasality ratings obtained with equal appearing interval and direct magnitude estimation scaling methods. Cleft Palate Craniofac. J. 2010, 47, 631–637. [Google Scholar] [CrossRef]
- Harris, P.A.; Taylor, R.; Minor, B.L.; Elliott, V.; Fernandez, M.; O’Neal, L.; McLeod, L.; Delacqua, G.; Delacqua, F.; Kirby, J.; et al. The REDCap consortium: Building an international community of software platform partners. J. Biomed. Inform. 2019, 95, 103208. [Google Scholar] [CrossRef] [PubMed]
- Harris, P.A.; Taylor, R.; Thielke, R.; Payne, J.; Gonzalez, N.; Conde, J.G. Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed. Inform. 2009, 42, 377–381. [Google Scholar] [CrossRef]
- Quanjer, P.H.; Stanojevic, S.; Cole, T.J.; Baur, X.; Hall, G.L.; Culver, B.H.; Enright, P.L.; Hankinson, J.L.; Ip, M.S.; Zheng, J.; et al. Multi-ethnic reference values for spirometry for the 3-95-yr age range: The global lung function 2012 equations. Eur. Respir. J. 2012, 40, 1324–1343. [Google Scholar] [CrossRef]
- Leivseth, L.; Nilsen, T.I.; Mai, X.M.; Johnsen, R.; Langhammer, A. Lung function and respiratory symptoms in association with mortality: The HUNT Study. COPD J. Chronic Obstr. Pulm. Dis. 2014, 11, 59–80. [Google Scholar] [CrossRef]
- Burney, P.G.; Hooper, R. Forced vital capacity, airway obstruction and survival in a general population sample from the USA. Thorax 2011, 66, 49–54. [Google Scholar] [CrossRef]

| Characteristic | Number (%) or Mean ± SD a n = 15 |
|---|---|
| Demographics | |
| Age (years) | 60 ± 12 |
| Sex (male) | 10 (66.7) |
| BMI (kg/m2) | 27.3 ± 5.1 |
| Smoking | |
| Never | 8 (53.3) |
| Previous | 3 (20.0) |
| Current | 4 (26.7) |
| Diabetes | 12 (80.0) |
| COPD | 13 (86.7) |
| Heart failure (EF < 45%) | 13 (86.7) |
| Previous stroke | 14 (93.3) |
| Cause of admission | |
| Respiratory failure | 6 (40.0) |
| Cardiovascular disease | 5 (33.3) |
| Sepsis | 3 (20.0) |
| Trauma | 1 (6.7) |
| Time | |
| LOS prior to ICU admission (days), median (IQR) | 0 (0–4) |
| ICU admission until tracheostomy (days) | 9.9 ± 4.0 |
| Duration of mechanical ventilation prior to tracheostomy (days), median (IQR) | 7 (6–11) |
| Duration of cannulation (days), median (IQR) | 15 (9–20) |
| Duration of mechanical ventilation until decannulation (days), median (IQR) | 22 (20–30) |
| Tracheostomy characteristics | |
| Type of tracheostomy | |
| PDT | 12 (80.0) |
| CST | 3 (20.0) |
| Cannula size (mm) | |
| 6.0 mm | 1 (6.7) |
| 7.0 mm | 2 (13.3) |
| 8.0 mm | 11 (73.3) |
| Missing | 1 (6.7) |
| Parameters | Open | Sealed | p-Value |
|---|---|---|---|
| FVC (mL) | 833 (510–1910) | 1260 (1005–1723) | <0.001 |
| FEV1 (mL) | 790 (465–1255) | 870 (617–1297) | <0.001 |
| PEF (L/min) | 103 (55–211) | 107 (62–173) | 0.720 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kraghede, R.E.; Christiansen, K.J.; Kaspersen, A.E.; Pedersen, M.; Petersen, J.J.; Hasenkam, J.M.; Devantier, L. Novel Method for Sealing Tracheostomies Immediately after Decannulation—An Acute Clinical Feasibility Study. Biomedicines 2024, 12, 852. https://doi.org/10.3390/biomedicines12040852
Kraghede RE, Christiansen KJ, Kaspersen AE, Pedersen M, Petersen JJ, Hasenkam JM, Devantier L. Novel Method for Sealing Tracheostomies Immediately after Decannulation—An Acute Clinical Feasibility Study. Biomedicines. 2024; 12(4):852. https://doi.org/10.3390/biomedicines12040852
Chicago/Turabian StyleKraghede, Rasmus Ellerup, Karen Juelsgaard Christiansen, Alexander Emil Kaspersen, Michael Pedersen, Johanne Juel Petersen, John Michael Hasenkam, and Louise Devantier. 2024. "Novel Method for Sealing Tracheostomies Immediately after Decannulation—An Acute Clinical Feasibility Study" Biomedicines 12, no. 4: 852. https://doi.org/10.3390/biomedicines12040852
APA StyleKraghede, R. E., Christiansen, K. J., Kaspersen, A. E., Pedersen, M., Petersen, J. J., Hasenkam, J. M., & Devantier, L. (2024). Novel Method for Sealing Tracheostomies Immediately after Decannulation—An Acute Clinical Feasibility Study. Biomedicines, 12(4), 852. https://doi.org/10.3390/biomedicines12040852







