1. Introduction
Hyaluronic acid (HA) has gained significant widespread usage by the cosmetic industry in limiting or reducing skin ageing [
1]. Low molecular weight HA has dramatically shaped an important role in products that promote skin hydration. Whereas high molecular weight HA is widely used as filler to shape lips, contour cheeks and correct facial lines [
2]. Thus, HA-based cosmetic formulations such as hydrogels, gels, dermal/intradermal filling injections, lotions, creams, and serums, have purported noticeable skin anti-wrinkle and anti-aging properties [
3]. HA has favourable properties due to its biocompatibility, non-immunogenicity, and biodegradability [
4]. It can also interact with receptors such as CD44, which is expressed in many types of tumour cells and accordingly, it is a candidate for delivery of imaging and anticancer agents [
5]. HA can embed fibroblast growth factor and is used to make scaffolds, which can be used to fasten wound healing [
6].
Hyaluronan is a non-sulphated glycosaminoglycan comprising repeating polymeric disaccharides of N-acetyl-D-glucosamine and D-glucuronic acid [
7]. These are linked together by alternative beta-1, 3 and beta-1,4 glycosidic bonds [
8]. It is a naturally occurring biodegradable polymer identical in molecular and chemical form in all tissues and has significant biological functions in all living cells [
9].
HA is in powder form in its natural state, but due to its multitude hydroxyl and carboxyl groups, it is an effective gelling agent that can form a hydrogel when added to a liquid solvent under mild conditions [
10]. The degree of crosslinking and modification determine its physical and chemical properties. Hydrogen atoms around the axis of the structure are non-polar and hydrophobic, while the side chains are more polar and hydrophilic [
8]. The H-bonds stabilize the conformation of HA in solution. However, the bonds are easily disrupted by temperature and pH. At intermediate pH levels, HA behaves like most other polymers with no strong intermolecular interactions, but as pH reduces towards 2.5, HA forms a gel due to decreasing carboxylate dissociation and increased intermolecular interaction [
11]. HA must be chemically modified to form a less degradable gel that is used in many biomedical applications [
11].
Type I hydrogels are crosslinked three-dimensional polymers holding hydrophilic groups in their structure able to retain water within their structure without dissolving [
12]. Hydrogels may be made up of one or more polymers. The spaces between the macromolecules fill with water, swelling the compound to form a hydrogel. The polymers have hydrophilic functional groups which hydrate in aqueous media and are responsible for the hydrogels’ ability to absorb water [
13]. The crosslinks in the polymer network chains prevent dissolution of the hydrogel in water [
14].
There are different types of hydrogels depending on their origin (natural versus synthetic hydrogels), polymer composition (copolymer, multipolymer and homopolymeric hydrogels), biodegradability (biodegradable hydrogels versus non-biodegradable hydrogels) and configuration (crystalline, non-crystalline, hydrocolloid aggregates, and semi-crystalline) [
15,
16]. Hydrogels can be categorized according to their type of crosslinking (chemical, biochemical and physically crosslinked hydrogels), physical appearance (matrix, microsphere, and matrix) as well as the network’s electrical charge (neutral, anionic, cationic) [
15,
16]. Hydrogels can also be classified according to their method of preparation (homopolymer, copolymer, interpenetrating network, self-assembly, and semi-interpenetrating network) [
15].
PT (Penta erythritol tetra acrylate) is a tetra-functional acrylate monomer widely used as crosslinker in polymerization. In previous studies, PT has been used as crosslinker for polyethylene oxide (PEO) via UV radiation [
17] and for HA via exposure to high temperature (80 °C) in the oven [
12]. Such crosslinked hydrogel films can be suitable for the delivery of drugs and cosmetic active ingredients by transdermal and topical (cosmetic) formulations, respectively, via application of the hydrogel film on the intact skin surface.
Vitamin B
3 is an important antioxidant in the body. It is vital in reducing the decline of NADH and NADPH, essential enzymes that play a significant function in the manufacture of cellular energy and lipids [
18]. The anti-ageing role of Vitamin B
3 is attributed to the fact that these two enzymes often decline in number with age; when these enzymes are sufficiently present in the skin, they can create an effective defense mechanism against ageing-induced external factors. Vitamin B
3 also assists the skin in remaining hydrated as it encourages the production of natural emollients [
19,
20,
21]. Niacinamide is an active amide form of vitamin B
3, and its chemical structure consists of 3-pyridine carboxamide. Due to vitamin B
3’s excretion from the body without in vivo storage, it should be taken from various food sources and supplements [
19]. Additionally, its small molecular size (122.1 Dalton) renders it a suitable active ingredient for transdermal delivery because it can diffuse systemically via the stratum corneum [
22].
Salicylic acid is a nonsteroidal anti-inflammatory (mono-hydroxy benzoic acid) which is the active form of aspirin. It is widely used in the cosmetic sector to enhance skin beauty [
23]. SA can exfoliate the dead skin cells (corneocytes) from the skin surface (stratum corneum) and it can also fade hyperpigmentations on the skin. Cosmetically, due to salicylic acid’s UV radiation-induced conversion reactions, it has been used in sunscreen formulations where it can convert the harmful radiation waves into safer warmer long radiation waves [
23]. Also, SA is keratolytic, which allows it to be utilized in wart healing [
24] and as anti-comedogenic in acne. The carboxylic group in the SA structure allows H-bonding interactions with other ingredients and with structural polymers in pharmaceutical and cosmetic formulations, therefore enabling a high loading capacity in the vehicle [
25]. The low molecular weight of SA (138 Dalton) enables its molecular diffusion via the stratum corneum for either a topical (cosmetic) or transdermal (pharmaceutical) effect.
The novelty of the HA hydrogel films was reported in our previous paper where we presented a new method of preparation of HA crosslinked hydrogel films, using PT (pentaerythritol tetra acrylate) as the crosslinking agent under high temperature conditions (oven-assisted thermal crosslinking) in high pH [
12]. The aim of this follow-up work was to investigate the efficiency of the crosslinked HA hydrogel film as a novel delivery system for pharmaceutical or cosmetic active ingredients; we achieved this aim via the following objectives: (i) feasibility of uploading basic and acidic active ingredients into the novel crosslinked HA hydrogel film via two different loading methods, (ii) characterisation of the properties of the loaded hydrogel films and, provided loading was successful, (iii) release behaviour of the active ingredient from the film.
2. Materials and Methods
2.1. Materials, Chemicals, and Reagents
Hyaluronic acid (HA) sodium salt with high molecular weight (1800–2200 KDa) was supplied by Infinity Ingredients (Binfield, UK), while PT (Pentaerythritol Tetracrylate) was purchased from Insight Biotechnology Limited (Middlesex, UK). Salicylic acid (SA) was purchased from BDH chemicals Ltd. Poole England and B3 Niacinamide from Western Drugs Limited, Madri, Udaipur, India.
These materials were used as received unless otherwise described. Other chemicals and reagents included NaOH (1.0 M) and HCl (1.0 M), which were used for pH adjustment. Deionized distilled water was available in the laboratory and was used as solvent for the HA polymer gelling and as a polar swelling agent for the HA hydrogel films.
2.2. Preparation of Hyaluronic Acid Hydrogels
The preparation of hydrogel was carried out according to [
12] with some changes to PT concentration. HA-based hydrogels were formulated with 5%
w/
w concentration of HA and 25% PT (to be noticed that the 25% PT was from the HA concentration. While in the whole film the PT concentration was 1.25%
w/
w). The hydrogels were prepared by dissolving HA in deionized distilled water; the mixtures were stirred with an IKA stirrer (IKA
® Werke GmbH. & Co. KG, Staufen, Germany) for 24 h to obtain homogeneously mixed HA hydrogels. This was followed by adjusting the pH to alkaline (11–12) using a pH meter from Hanna instruments (a wireless pH tester for cosmetic creams). Then, PT was added, and the mixture was subsequently stirred slowly for 24 h to obtain completely homogenized HA-PT hydrogels. The hydrogel was left to stand for 48 h to release air bubbles before casting in Petri dishes. The cast hydrogel samples were air-dried at room temperature for four to five days. The obtained xerogel films were cut in small pieces ready for crosslinking.
2.3. Crosslinking Reaction
The oven-assisted thermal crosslinking of the HA-PT xerogel films was done using an 80 °C oven (Binder GmbH Bergster, 14 D-78532 Tuttlingen). The hydrogel film samples were placed in the oven for 24 h.
2.4. Hydrogel Swelling Studies
Three samples (n = 3) of the loaded xerogel films from each loading batch were accurately weighed (Mo) and then were swollen in distilled water for 24 h at room temperature. During swelling, the films were periodically removed from water; excess surface water was drip-dried, and the films were reweighed (Ms).
The percentage swelling (%) was calculated using Equation (1) [
12]
where
Mo was the initial weight and
Ms was the weight of the swollen hydrogel film at equilibrium.
The maximum swelling equilibrium (EWC) was calculated using Equation (2) [
12].
After 1 h, they reached equilibrium.
The gel fraction for each film was calculated using Equation (3)
where
Mr is the weight of film after drip-drying excess water.
2.5. Comparisons of Average MW between Crosslinks, Crosslinking Density, and Mesh Size
The average MW between crosslinks (
), crosslinking density (
Ve), and mesh size (ξ) of the medicated and unmedicated hydrogel formulations were calculated according to the equilibrium swelling theory, which assumes Gaussian distribution of crosslinked polymer chains. The Flory Rehner Equation (4) was used to calculate
[
12].
where
is the volumetric swelling ratio,
is the specific volume of the dry polymer (
= 0.575 cm
3/g for HA),
v 1 is the molar volume of the solvent (18 cm
3 /mol for water), and
x is the Flory polymer solvent interaction parameter (for HA). The
x value was estimated to be 0.473 based on several assumptions [
13,
25].
Qv was determined as
Qm, which is the degree of mass swelling, according to Equation (5).
where,
Pp is the dry polymer density (1.229 g/cm
3) and
Ps is water density.
Qm is the swelling ratio using the weights of the films before (xerogel and loaded) and after swelling.
Qm was used to calculate
Qv. Equations (6) and (7) were used to calculate the effective crosslinking density (
Ve) and swollen hydrogel mesh size (ξ), respectively.
where
is the root-mean square (RMS) distance between crosslinks, which is dependent on the MW between crosslinks. For HA, an RMS distance value was used as previously calculated (Equation (8)) [
26].
where
n is the polymeric disaccharide units for HA with a given MW. For HA with an
n of 5305 and MW of 2 × 106 g/mol, RMS was estimated as follows (Equation (9)).
Then combining Equations (7) and (9) and substituting
for
Mn gives Equation (10).
2.6. Active Loading Studies
B
3 and SA were loaded into the HA hydrogel films as model active cosmetic ingredients via two different methods shown in
Table 1.
2.6.1. Post-Loading
Three replicates of unmedicated dry HA hydrogel films were immersed in saturated solutions at 32 °C for 24 h; solutions of B
3 and SA were prepared using distilled water as solvent. In order to obtain full saturated solutions, the amount of B
3 added was 37.5 gm and 0.19 gm for SA, respectively (
Table 1). Preliminary studies showed that 32 °C and 24 h were the optimum conditions to ensure maximum active load [
27].
After 24 h, the loaded hydrogel films were weighed and left for 24 h to dry. The dried loaded films were weighed, and the active load was determined by using Equation (1). This equation was adapted from Peppas et al., where the weight of active was considered [
27].
where
Mo is the initial weight of xerogel while
Md is the weight of active-loaded hydrogel films.
Regarding SA loading by osmosis method, preliminary studies showed the active did not load via this method. For this reason, the post-loading method for SA was not included in this paper.
2.6.2. In Situ Loading
HA/PT hydrogel films were loaded with either SA or vitamin B
3. The calculated amount of both actives (see
Table 1) was weighed and dissolved in distilled water. HA was then added to the solution under intensive stirring, as previously described in the hydrogel preparation section. To compare both loading methods (in situ and osmosis method), the exact amount of both actives was included in the mixture formulations, based on the corresponding active’s load obtained from immersions, as described in the post-loading method.
2.7. In Vitro Active Release Study
Active release studies were performed on selected active-containing hydrogel films from both loading methods in pH 7.4 PBS. The percentage of active release was evaluated by two methods at 32 °C [
13].
Firstly, each film was placed in 100 mL phosphate buffer under gentle stirring using a magnetic stirrer. Five mL PBS samples were collected at different times, followed by topping up the volume with fresh PBS. The concentration of active released into the buffer was evaluated using a UV spectrometer via a beer-Lambert plot linear regression equation, and the percentage of cumulative release was plotted as a function of time. The wavelengths used for the detection of actives were 262 nm for B
3 and 296 nm for SA [
28]. The measured absorbances were substituted in the calibration curve to obtain the amount of active released.
The percentage of cumulative active released was calculated using the Equation (12):
where
Mr is the amount of active released from the calibration curve and
Md is the amount of active loaded in the film.
After completion of the study, the hydrogels were removed from PBS and left to dry. The dried xerogels were then accurately weighed, and the obtained weights were used to check the total percentage active release using Equation (13), which was adapted from Equation (1).
where MD is the weight of xerogel before the release study, MR is the weight of xerogel after the release study.
To calculate the percentage of ionization of the actives, films from all medicated and unmedicated formulations were chosen and swollen in distilled water. The pH values were measured with Janaway 3010 pH meter (Cole-Palmer Ltd., Staffordshire, UK). The percentage of ionization of the SA was calculated using Equation (14) [
29].
And the percentage of ionization of the B
3 was calculated using the Equation (15)
Various release model kinetics equations were applied to all formulations:
Zero order Kinetics [
30].
where
is the ratio of active release, t is the time and Ko is the zero-order release constant.
First order Kinetics [
27].
where K1 is the first order release constant.
Higuchi model kinetics [
31].
where Kh is the Higuchi constant.
Korsmeyer-Peppas model [
32].
where Kp is kinetic constant,
n is the release exponent.
In Peppas model, the
n value characterizes the release mechanism. Depending on (
n) value, if (
n) value = 0.5 is Fickian diffusion, 0.43 <
n < 1 indicates non-Fickian diffusion, while
n > 1 refers to super case-II transport diffusion [
30].
2.8. Fourier Transform Infrared Spectroscopy (FT-IR)
FT-IR was done at room temperature using the Shimadzu IR Affinity-1S Fourier Transform Infrared Spectrometer (Shimadzu UK Ltd., Milton Keynes, UK) for all hydrogel film batches to evaluate the active loading and release in the HA-PT xerogel films. FT-IR analysis was also carried for blank films and pure actives. The spectral range was 4000–550 cm−1 with the resolution set at 2 cm−1.
2.9. Differential Scanning Calorimetry (DSC)
Differential scanning calorimetry experiments were performed using hermetic aluminium pans in DSC Q1000 thermal analyser (both TA Instruments, New Castle, DE, USA). The samples were analysed during three thermal cycles over 2.5 h. Pure actives and hydrogel film samples (xerogel and loaded) were weighed using a microbalance (Mettler-Toledo, Greifensee, Switzerland), placed in an aluminium hermetic sample pan, and closed with an aluminium lid: first cycle with a temperature range from 50 °C to 300 °C; second cycle with a temperature range from 300 °C to 50 °C; and third with a temperature range from 50 °C to 300 °C. All cycles were performed under liquid nitrogen (50 mL/min). Calibration was done using indium.
2.10. Scanning Electron Microscopy (SEM)
The morphology of hydrogel samples loaded with both loading methods, and films after the release study, were evaluated using a scanning electron microscope (Hitachi, Tokyo, Japan) operated in high-vacuum mode at an accelerating voltage of 5 kV. Prior to freeze drying, the swollen hydrogel samples were frozen in a −80 freezer and subsequently freeze-dried in an ALPHA 2-4/LSC device (Martin Christ Gefriertrocknungsanlagen GmbH, Osterode am Harz, Germany) under a vacuum of 0.1 Pa at −70 °C for 24 h to thoroughly remove the water. Due to HA’s hygroscopicity, the vials were filled with nitrogen gas to keep the films away from moisture. The freeze-dried hydrogel samples were put into liquid nitrogen for few minutes, fractured with a razor blade to expose the internal structures, and stuck onto the sample holder. All samples were sputter-coated with gold and palladium using Agar sputter coater (AGAR-Scientific, Ltd., Stansted, UK) for 60 s before observation.
2.11. Statistical Analysis
All obtained data were expressed as mean ± standard deviation. Also, one-way analysis of variance (ANOVA) was used to compare the release percentage, swelling percentage, mesh size, and degree of ionization between the formulations. Differences within and between treatments were significant at an acceptable p value of < 0.05 (p < 0.00001).
3. Results and Discussion
3.1. Active Loading in the Hydrogel Films
SA and B
3 were chosen as cosmetic active ingredients to load in the HA hydrogel. The post-loading method of B
3 was successfully achieved with a high percentage of loading (˃99%). The hydrophilic nature of B
3 is compatible with the HA polymer, while for SA there was no loading achieved by the osmosis method. Failure of loading was expected due to the negatively charged SA at high pH active repulsed by electrostatic interaction from the negatively charged HA [
28,
33].
The in situ loading method for B3 in concentration (45%) w/w and SA in concentration (3.55%, 45%) w/w has been achieved. These active concentrations were chosen to be close to the concentrations of the osmosis method and thus easier to compare between them. However, SA was loaded in two different concentrations instead to evaluate the effect of active concentration in the films with the same loading method.
B3 in higher concentration 37.5 gm was loaded in situ, but the film appeared low in mechanical strength. In contrast, the films which were loaded with 1 gm (45%) B3 exhibited better appearance. Therefore, the former has been omitted from the study.
3.2. Swelling Behaviour of the Hydrogel Films
The swelling and crosslinking properties of the HA hydrogel films are summarized in
Table 2. The blank unmedicated HA hydrogel films swelled rapidly and reached to equilibrium quickly. When the PT amount increased to 25%
w/
w (the ratio HA concentration), the swelling percentage was decreased. According to [
12], there was a correlation between increasing the crosslinker and lowest percentage of swelling,
Qv and ξ mesh size [
34].
From
Table 2, the swelling behaviour, EWC,
Qv of the loaded hydrogels showed differences in these parameters, especially the B
3 in situ loaded films showed significant difference from the unmedicated hydrogel films.
The lower percentage of swelling (405.55), ξ (38.77 nm),
(16929 gm/mol),
Qv (9.03 ± 1.00) for the in situ B
3-loaded films could be due to the active being embedded inside the polymer matrices [
17,
27]. While Ve appeared higher (7.36 × 10⁻
5) for the in situ B
3-loaded films, the lower swollen mesh size ξ of hydrogel, the higher the crosslink density [
12]. However, the percentage of swelling of both SA in situ loaded hydrogel films were close to the percentage of swelling of unmedicated hydrogel films. The percentage of gel fraction was decreased with increasing the actives’ concentration.
3.3. Actives Release Study
To investigate the active’s release from the HA films, quantitative drug detection was carried out via two methods: firstly, with UV absorbance measurements and secondly with hydrogel’s weight difference before and after release.
Figure 1 shows the release of B
3 from films prepared using both loading methods. It was found that B
3 was released immediately from the HA hydrogel films, irrespectively to the loading method. Similarly, the release from the films for both SA (3.55%) and SA (45%) was rapid and completed in 10 min; our results were in agreement with results of [
35].
The post-loading of B
3 showed over 99% release via both UV analysis and by weight difference. According to [
33], the HA’s high fluid uptake resulted in faster and complete release of the actives. This behaviour indicates that our crosslinked hydrogel is promising in the cosmetic sector and in wound dressing applications.
For the in situ loaded B
3 films (
Table 3), the % release was 90.1% according to UV analysis measurements, while the weight difference showed higher release at 95.47%. This could be because of the positively charged B
3 (
Table 4) retained in the negatively charged HA polymer, especially in the in situ loading method where the active was settled in the tortuous polymer structure, in contrast to the post-loaded B
3, where the morphologic study images with SEM revealed the active’s presence in the microporous linear structure. See below SEM section.
When looking at the percentage of ionization of B
3 (
Table 4), it is present in its non-ionized form, considering B
3 is a weak base, while SA being a weak acid had maximum ionization > 99% indicating that most of the active is solubilized in water.
Furthermore, the active release from the hydrogels could depend on different factors such as active’s molecular size, charge, chemical structure, the polymer matrix morphology, and the polymer-active interactions [
32]. This was indicated by the in situ loaded B
3 films’ lower mesh size and higher Ve resulting in a lower percentage release than the other formulations. The explanation for this could be that B
3 could be bound with the HA polymer via stronger bonds. Therefore, its full release from the hydrogel would require the hydrogel’s degradation [
32].
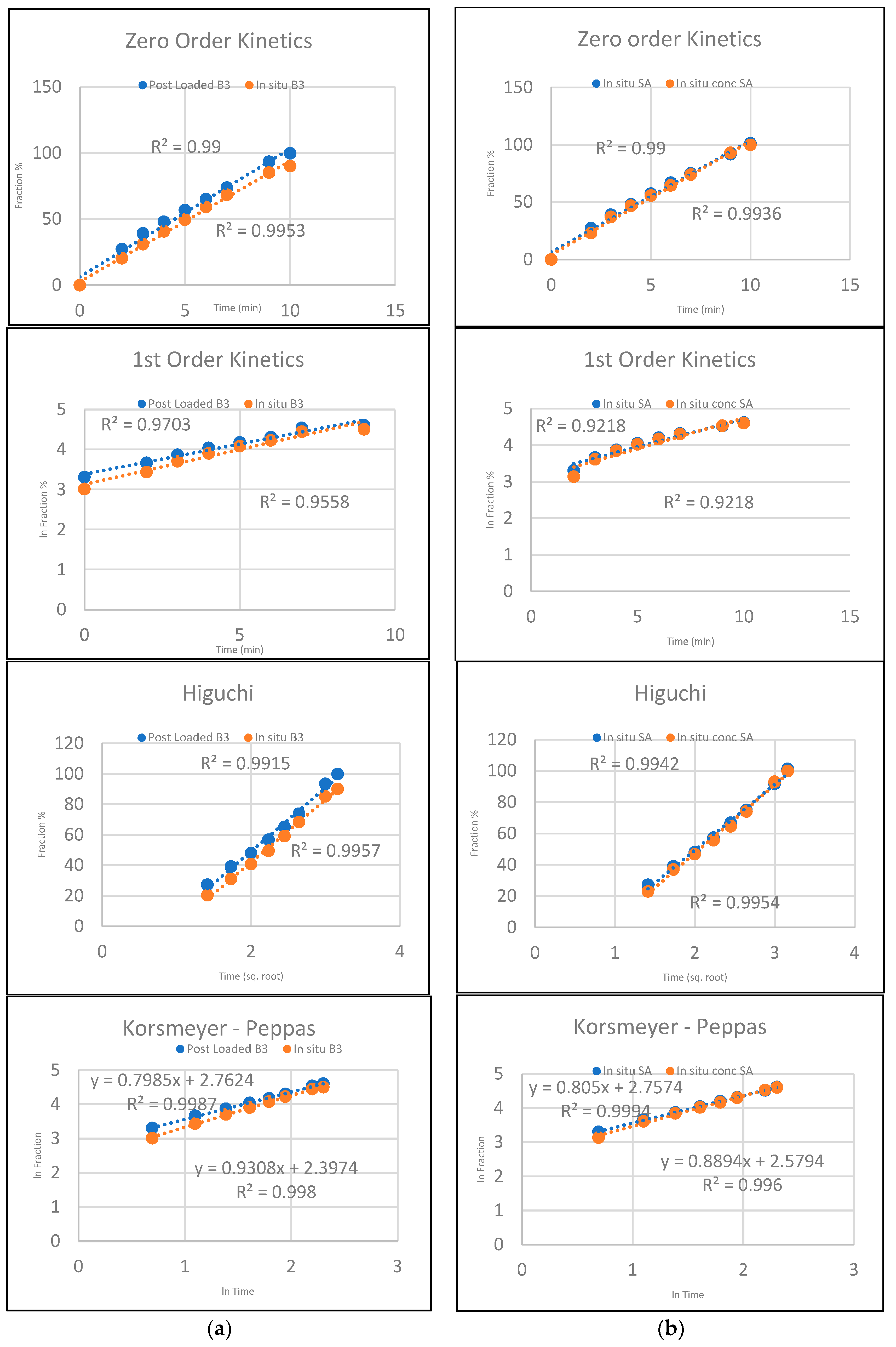
Release kinetic models were applied to the release data to illustrate the actives’ release kinetics from the hydrogel films (
Figure 2a,b and
Table 5). The R
2 values were employed for the determination of the best kinetic model for the release of each active from the films [
36]. On
Table 5, the highest R
2 is shown in bold for each film.
It was found that the highest R
2 was with the Korsmeyer–Peppas model regardless of the loading method for B
3 and the concentration difference for the SA (
Table 5). The
n value for all the formulations was within the range of 0.5 <
n < 1, which indicated that the diffusion mechanism followed non-Fickian diffusion, where the active’s release was via diffusion and hydrogel polymer chain relaxation [
27,
37,
38]; the high swelling capacity of the crosslinked HA hydrogel films allowed the quick penetration of water into the polymeric network, the subsequent polymer expansion, followed by the active’s quick dissolution, diffusion, and release from the hydrogel films. Our results agree with a recent study from Sang et.al [
36] who reported that the immediate release of 5-Fluorouracil from crosslinked aerogels was also best described by the Korsmeyer–Peppas model.
3.4. FTIR Analysis
The FTIR analysis was carried out to all loaded and released hydrogel films, as well as the unmedicated hydrogel films with pure (HA and PT), to explore the molecular interactions inside the polymer films [
39]. All FTIR spectra are presented in
Figure 3. Hyaluronic acid polymer was successfully crosslinked with PT via an ester bond (C-O-C) between the hydroxyl group of the HA and the carbonyl carbon of the crosslinker PT. Initially the free radicals of PT are activated under alkaline conditions to generate nucleophiles which activate radical polymerization. The generated PT radicals abstract hydrogen atoms from HA to generate HA radicals which then bind with PT radicals to form crosslinks [
12]. This reaction was illustrated in detail in our first paper [
12].
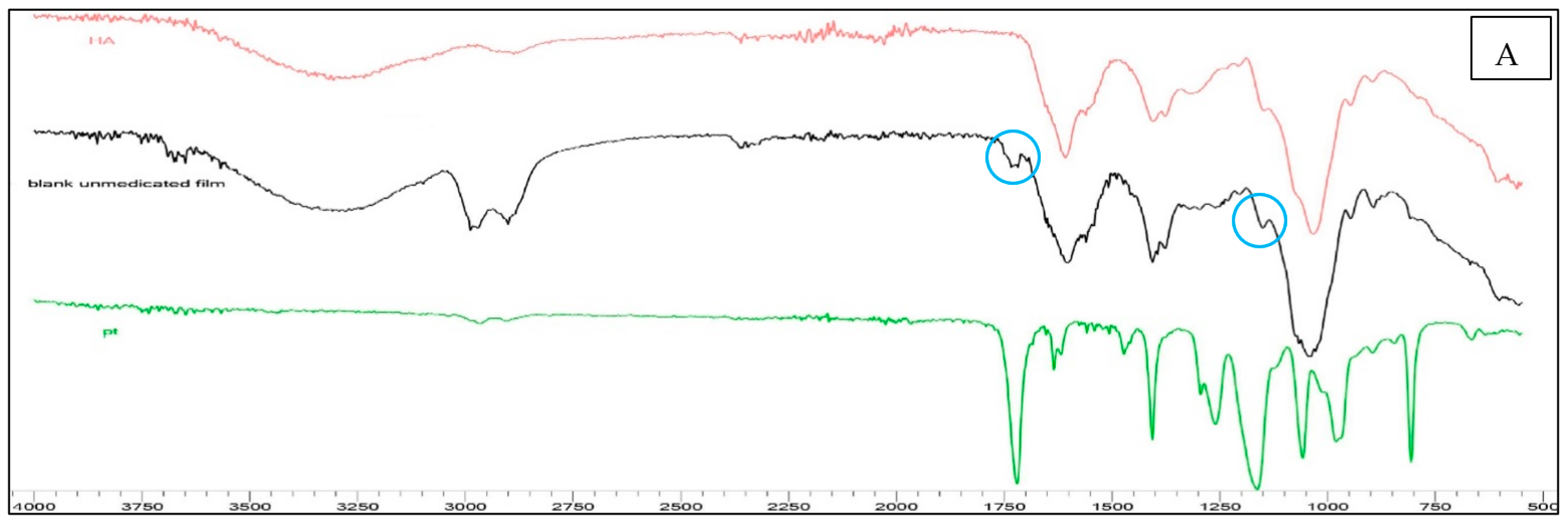
Figure 3A shows that the stretching peak at around 1738 cm
−1 in pure PT was reduced in intensity in the crosslinked blank hydrogel film, indicative of the reaction of the carbonyl group of PT with the hydroxyl group of HA, while the stretching peak around 1100–1300 cm
−1 corresponding to (C-O-C) is the new bond (crosslink) between HA and PT.
The peaks around 2900–3300 cm
−1 appearing in unmedicated film, stretched and disappeared in loaded B
3 films; this hydroxyl vibration region suggested the mixing of the active with the hydrogel polymer [
33].
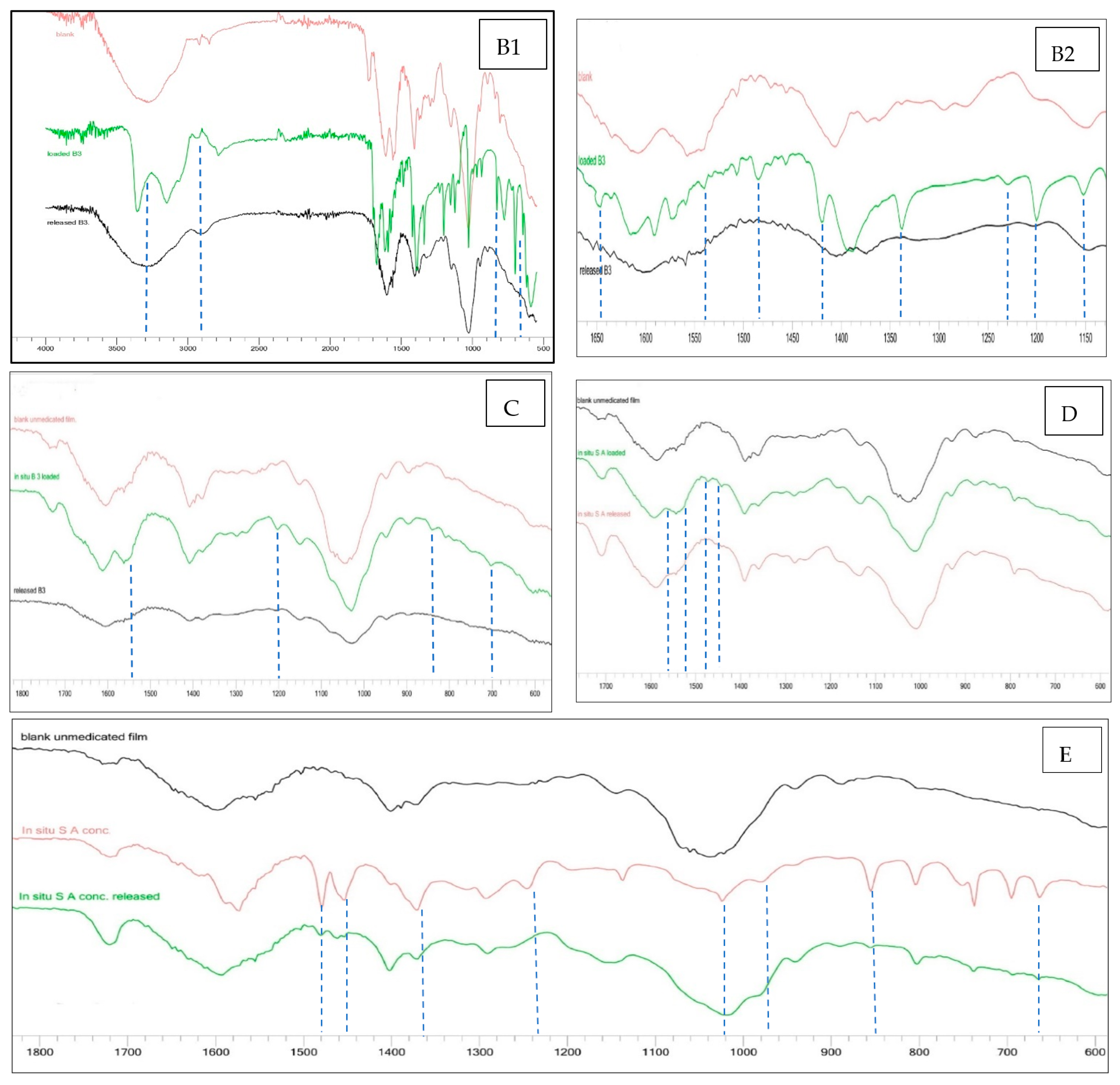
B
3-post-loaded spectra are shown in
Figure 3A. The FTIR spectra of B
3-post-loaded hydrogel films exhibited new peaks at 1649, 1540, 1484, 1420, 1340, 1229, 1200 and 1150 cm
−1 were (C=C, N˗H, O˗H, C˗O) stretching, respectively [
19,
40]. These peaks indicated the presence of B
3 active in the hydrogel films, confirming the loading of the active, while the peaks ranged from (840–680) cm
−1 were characteristic (C˗H) totally related to B
3 peaks. This also agreed with DSC and SEM, where the B
3 post-loading method showed less changes in the polymer structure.
Regarding the in situ loaded B
3 films (
Figure 3B), the peak around 1540 cm
−1 was C=C, while 1200 cm
−1 belongs to C˗O. Additionally, the 840, 700 cm
−1 peaks from B
3 were detected as described in post-loaded B
3 bands. However, the post-loaded B
3 peaks were sharper than the in situ loaded B
3 peaks, which could be due to the stronger embedding of the drug in the polymer matrix using the in situ method [
41].
SA 3.55%
w/
w in situ loaded hydrogel films exhibited strong N˗O amide stretch in area 1520–1560 cm
−1 [
28]. Both (3.55%, 45%)
w/
w in situ loaded SA were recorded the C˗H stretch in (1450–1480) cm
−1 presented in
Figure 3C,D. Notably, the peaks were sharper in 45%
w/
w SA in situ loaded films due to higher active concentration.
The FTIR spectra of 45% w/w in situ loaded SA evidenced bands at (96, 1018, 1240, 1460) cm−1 and symmetric C=C, strong C˗O, C˗N, C˗H stretching. Obviously, the sharper peaks ranging from 660 cm−1 to 850 cm−1 in the 45% w/w in situ SA loaded film, were C˗H band indicating the presence of SA in higher concentration.
Regarding the actives’ release from all the loaded hydrogel films, the spectra showed complete absence of the actives’ peaks after the release process, confirming that all active had been released.
3.5. DSC Analysis
DSC analysis was performed to investigate the thermal behaviour of the HA hydrogel films with and without actives. Firstly, the pure substances and the crosslinked xerogel films were analysed.
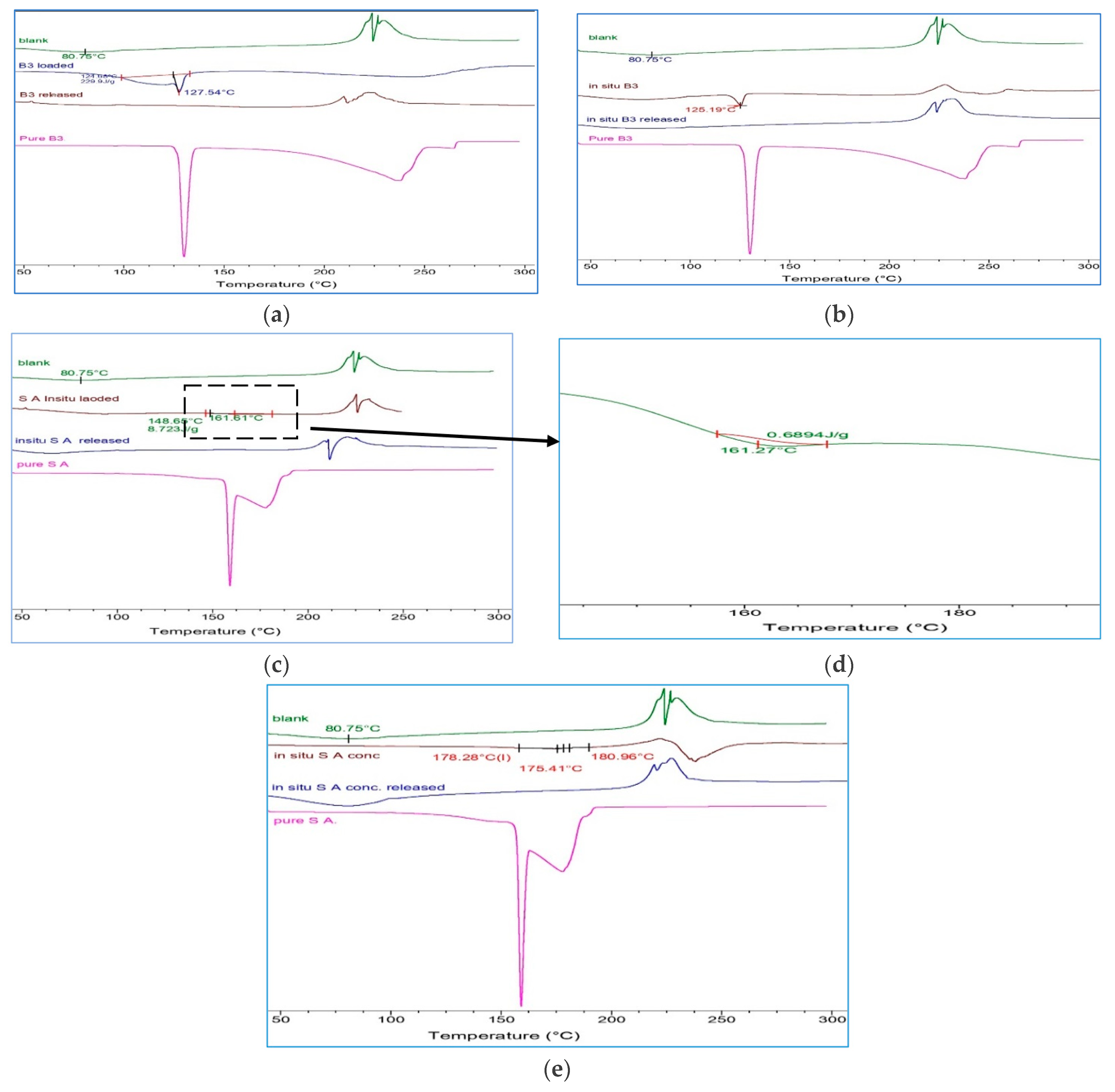
Figure 4a shows the thermal curves of medicated films (loaded, released) and pure B
3 and the unmedicated crosslinked hydrogel film. The exothermic peak of blank (unmedicated) films was obvious around 240 °C which indicated polysaccharide degradation [
33]. While the pure B
3 had an exothermic peak between 125–130 °C, this was suggested to Tm of the pure active in the first heating, which then disappeared on the second heating; presumably, it turned to an amorphous state [
19].
However, the thermal DSC curve of the unmedicated crosslinked film has presented two different melting points, presuming impurities in the polymer. The broad endothermic peak at 80.75 °C was shifted toward the pure actives melting points after loading the films with actives, indicating the interaction with the polymer.
The sharp endothermic peak at (125.19–127.54 °C) was obtained in loaded B
3 via both loading methods, proving the presence of B
3 in the HA hydrogel films (
Figure 4a,b). The main difference between in situ and osmosis loading was that the in situ B
3-loaded film kept the exothermic peak similarly to the unmedicated hydrogel; this could be attributed to the fact that the active was loaded inside the polymer matrices instead of settling in the porous structure; this was also confirmed by the SEM images, where the in situ B
3 loading caused marked changes in the HA hydrogel.
The analysis of DSC plots revealed that the thermal characteristics of the unmedicated film and the medicated film after B
3 release (
Figure 1c) were relatively similar. The identical melting temperatures in cycle 1 and 3 and the crystallisation temperatures in cycle 2 suggested that the active was fully released from the films.
The pure SA showed (
Figure 4c,e) a sharp melting endotherm peak in 158 °C, while in situ SA loaded (3.55%) presented Tm shifted to 161.61 °C and confirmed the SA presence altered the microstructure despite its low concentration. This was illustrated in the enlarged graph of loaded SA (
Figure 4d).
Moreover, the in situ SA loaded in concentration (45% w/w) showed melting endotherm in 175.41 °C.
Concentrated SA in situ loaded 45% w/w exhibited another Tm in 238 °C. This referred to the presence of high crystalline active amount loaded in situ. Due to SA’s lower solubility in water, the 45% w/w concentration was oversaturated in the solution used for producing the formulation. In addition, the presence of the various melting points can be explained by the presence of different polymorphic crystalline forms.
However, the graphs for SA (3.55% w/w) and (45% w/w) films after release appeared similar to the unmedicated films, indicating that complete release has been achieved, in agreement with the release study results.
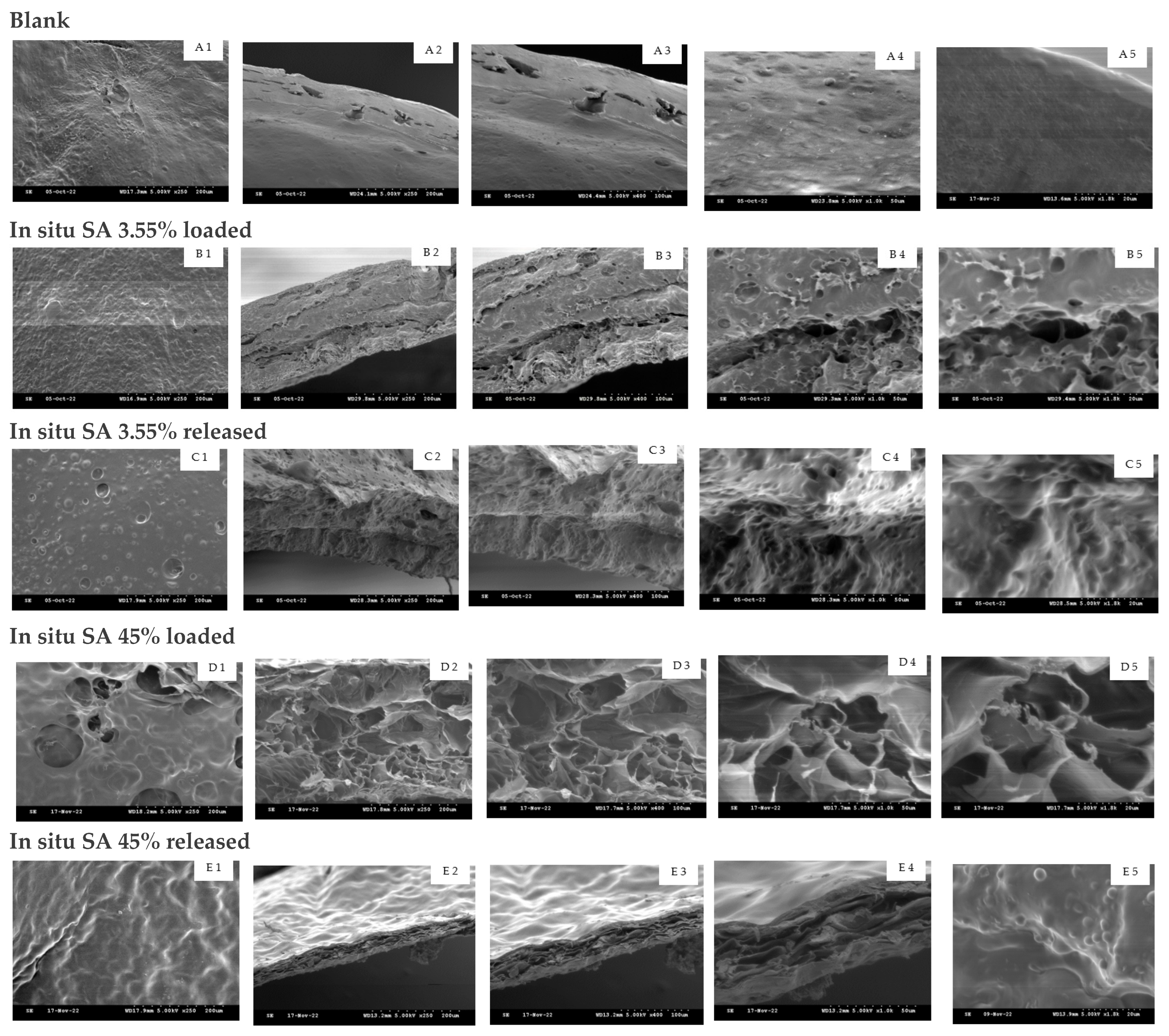
3.6. SEM
The morphological appearance of the unmedicated and medicated (loaded then released) hydrogel films has been studied with SEM.
Figure 5(A1–A5) show the freeze-dried blank hydrogel films. It was obvious that the post-loaded B
3 films developed more micropores, and the mesh size was clearly larger in contrast to the in situ loaded B
3 where the active was immersed inside the polymer structure with lower mesh size (ξ). The morphological appearance of the hydrogel films was particularly different when actives were loaded in situ [
27].
Regarding SA,
Figure 6(D1–D5) revealed the in situ loaded SA 45%
w/
w exhibited microporous structure with higher mesh size; moreover, these films were thinner. A possible explanation for this could be that more NaOH aqueous solution was added to the initial formulation to increase the pH to 11–12 for crosslinking; therefore, the polymer solution was diluted resulting in a thinner xerogel film upon drying [
41].
However, after release, all hydrogel films with both actives demonstrated the spongy structure of the films except the post-loaded B
3, where the hydrogel films looked similar to the blank unmedicated films after B
3 release. This was explained by the active in post- loading not being embedded inside the polymer. In addition, B
3 could be interacting via ionic bonding with the polymer which allowed the active to release without significant change in polymer structure [
27].
The results of this study confirmed that the crosslinked HA hydrogel films can be suitable carriers for either acidic or basic low molecular weight ingredients. The complete in vitro release of the actives within 10 min indicates that these hydrogel films could potentially be useful for various cosmetic applications such as anti-ageing facemasks for the immediate release of active ingredients onto the skin, body patches for the local treatment of cellulite, etc., or pharmaceutical applications such as transdermal drug delivery and wound healing.