In Vitro Microbiological and Drug Release of Silver/Ibuprofen Loaded Wound Dressing Designed for the Treatment of Chronically Infected Painful Wounds
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials and Reagents
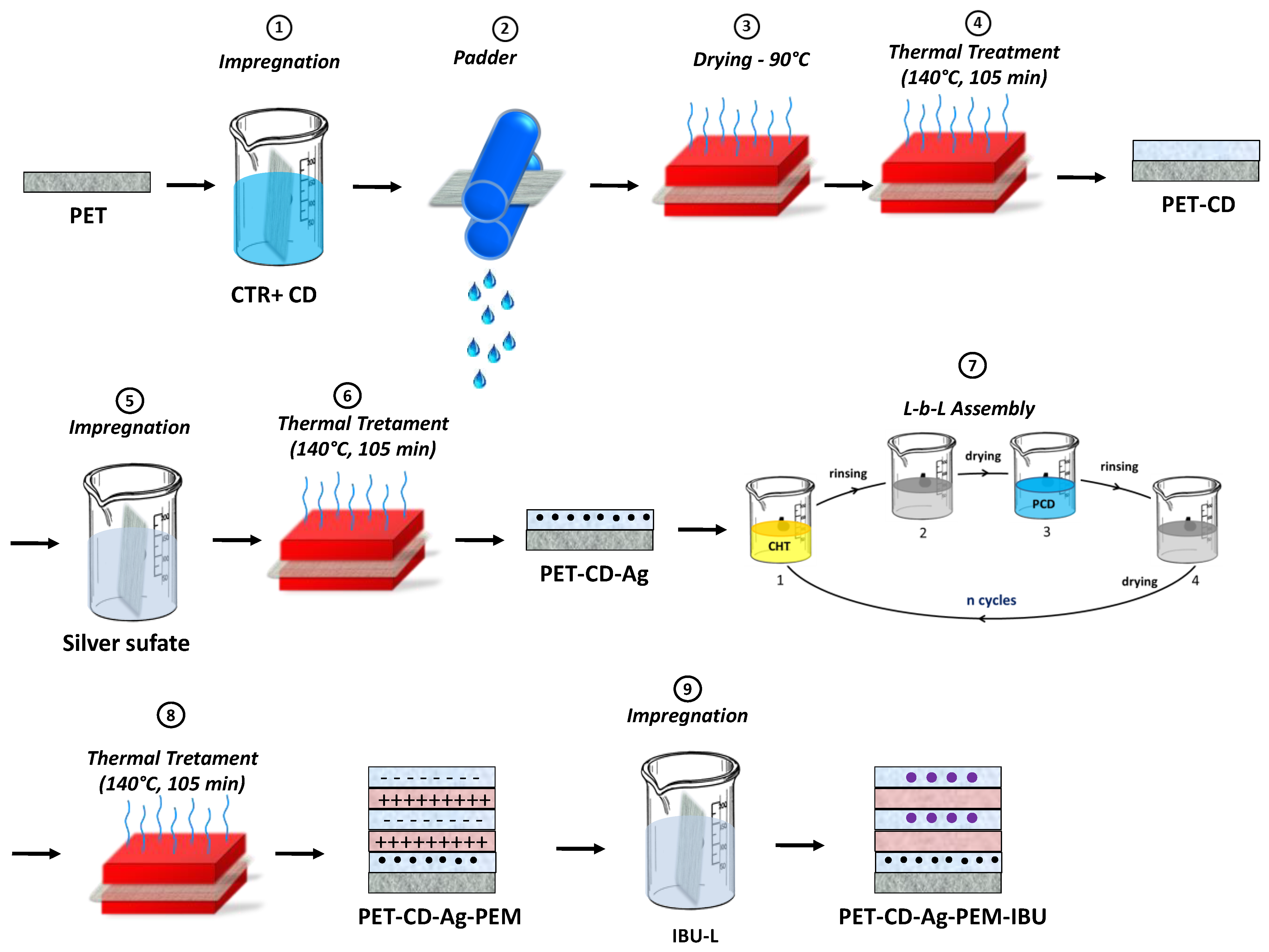
2.2. Development of Antibacterial Dressing
2.3. Ibuprofen-PCD Complexation Study
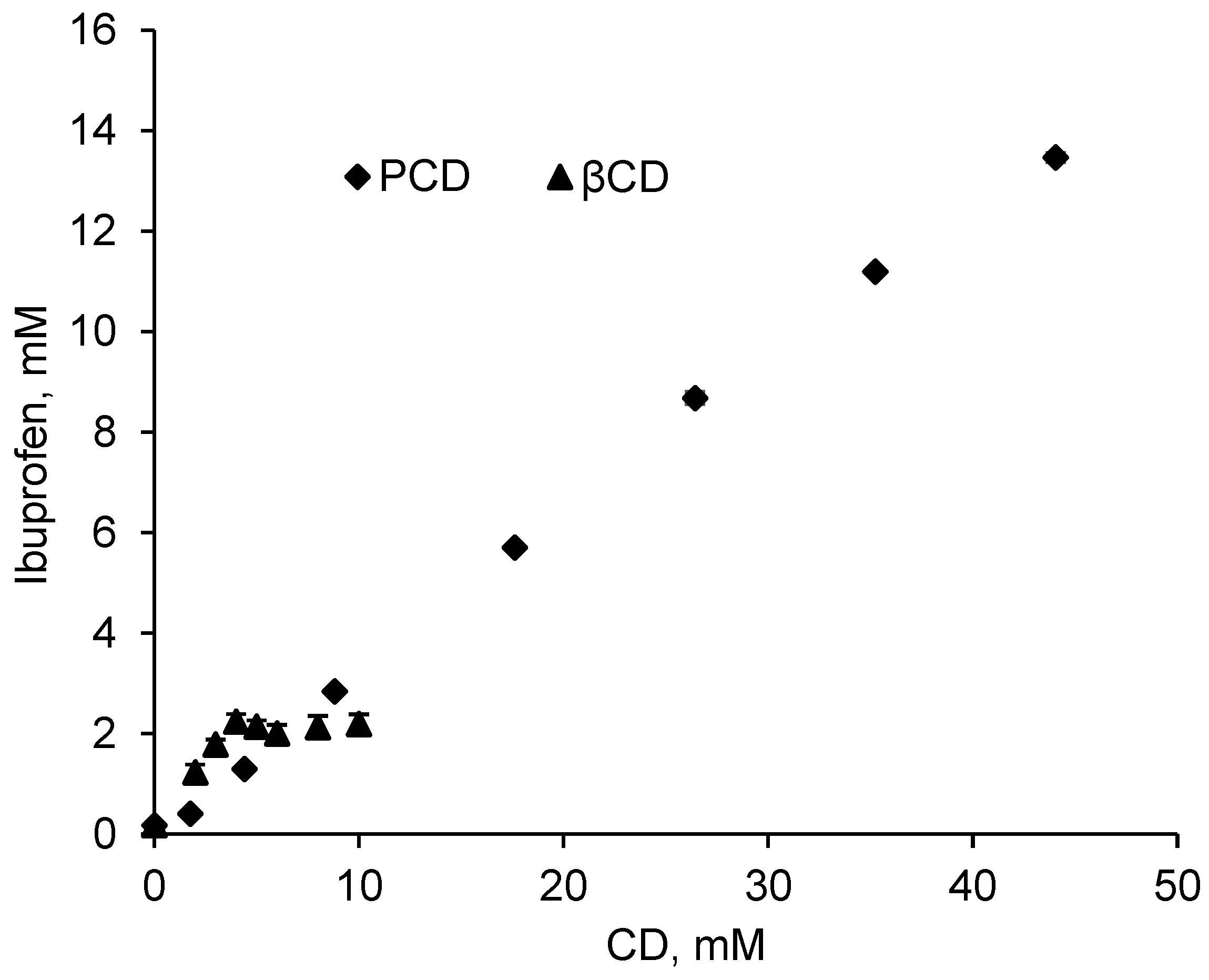
2.3.1. Phase Solubility Diagram of Ibuprofen
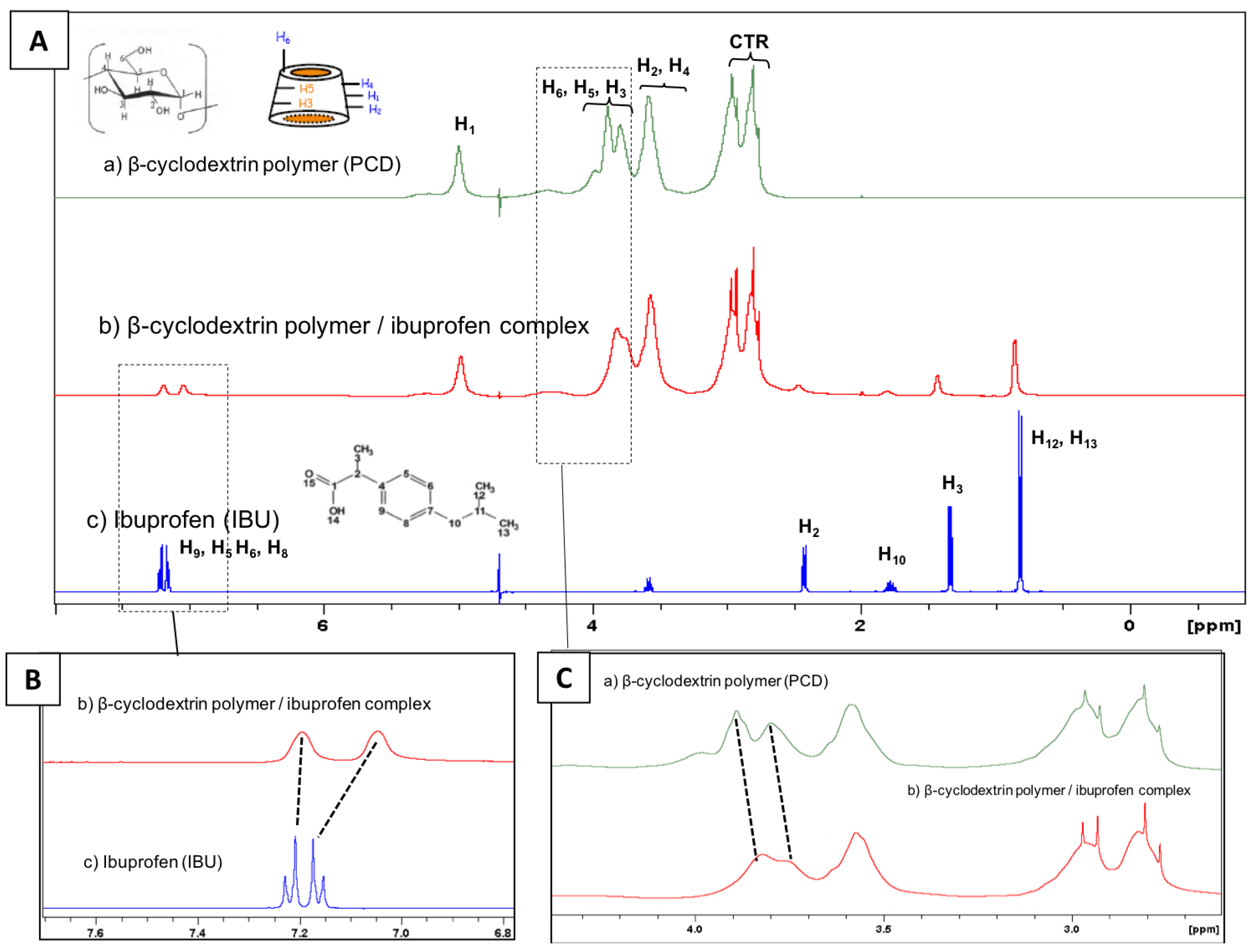
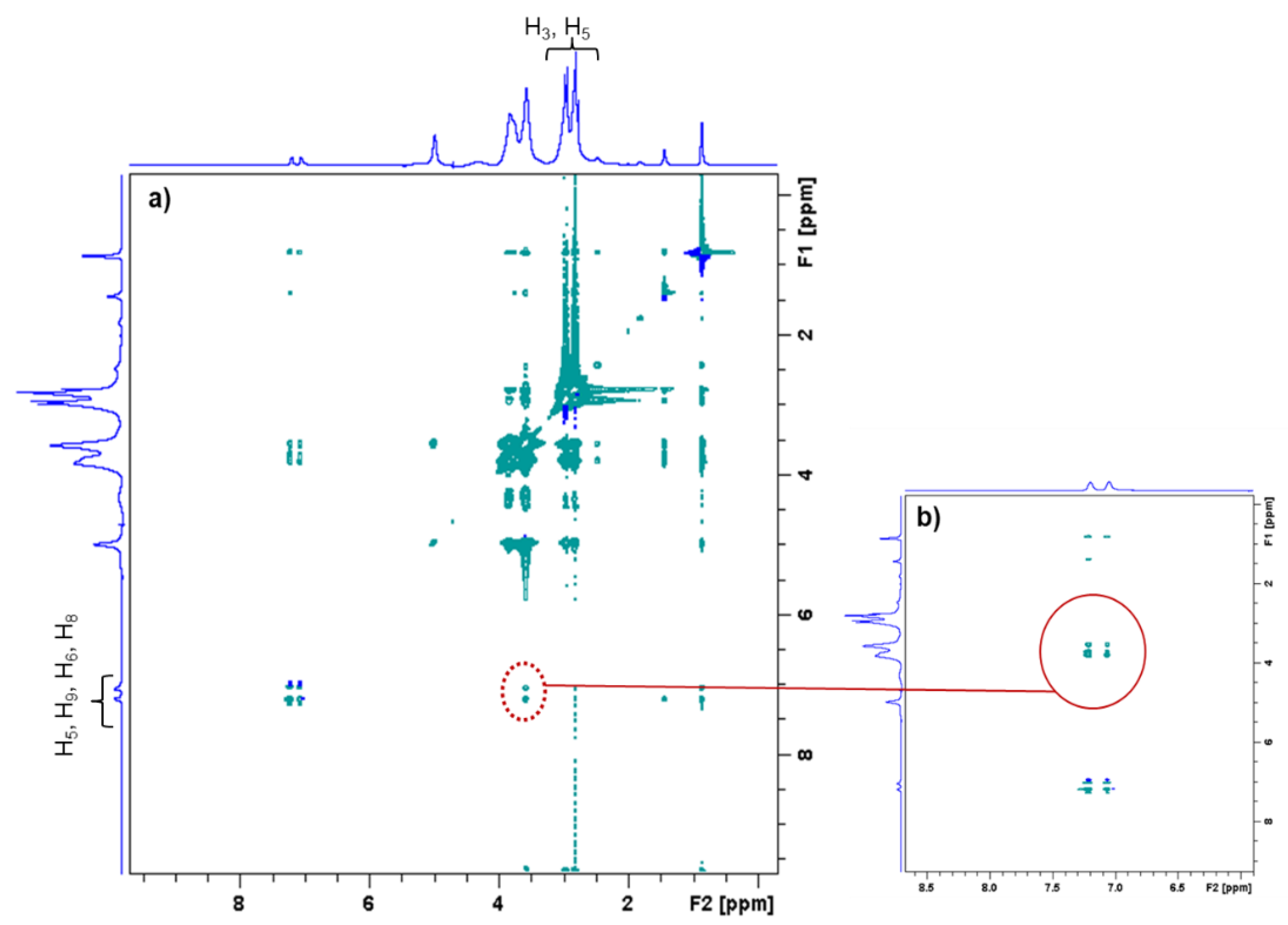
2.3.2. Proton NMR Spectroscopy
2.4. Drug Sorption and Drug Release
2.4.1. Ibuprofen Sorption and Isotherms Analyses
2.4.2. Ibuprofen Kinetic of Release
2.5. Biological Evaluation
2.6. Microbiological Evaluation
2.6.1. Kirby-Bauer Test
2.6.2. Kill-Time Test
3. Results
3.1. Study of the Interactions between IBU and PCD in Solution
3.2. NMR study of the PCD/IBU complex
3.3. Ibuprofen Lysinate Adsorption and Kinetic of Release
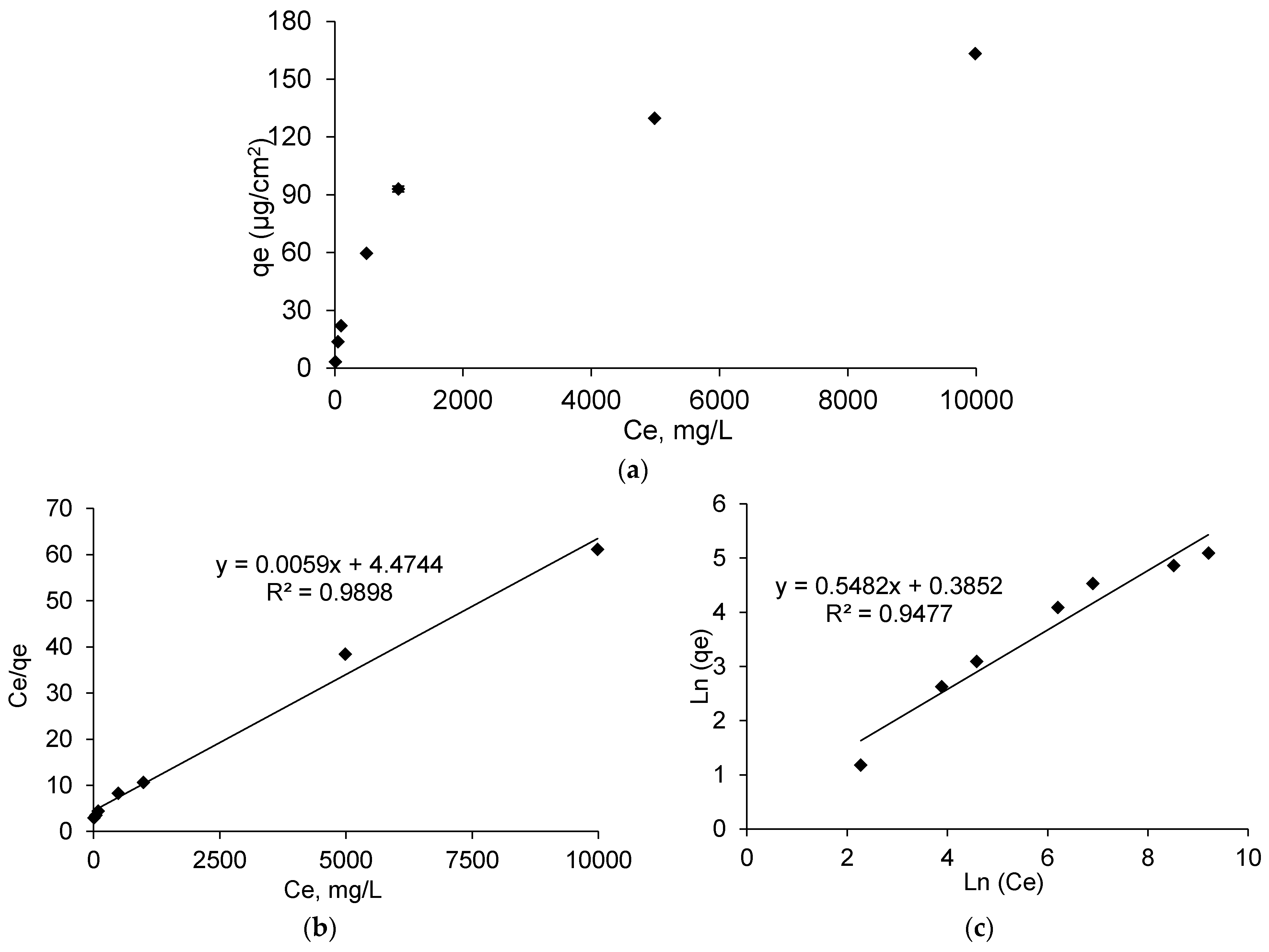
3.3.1. Adsorption Isotherms
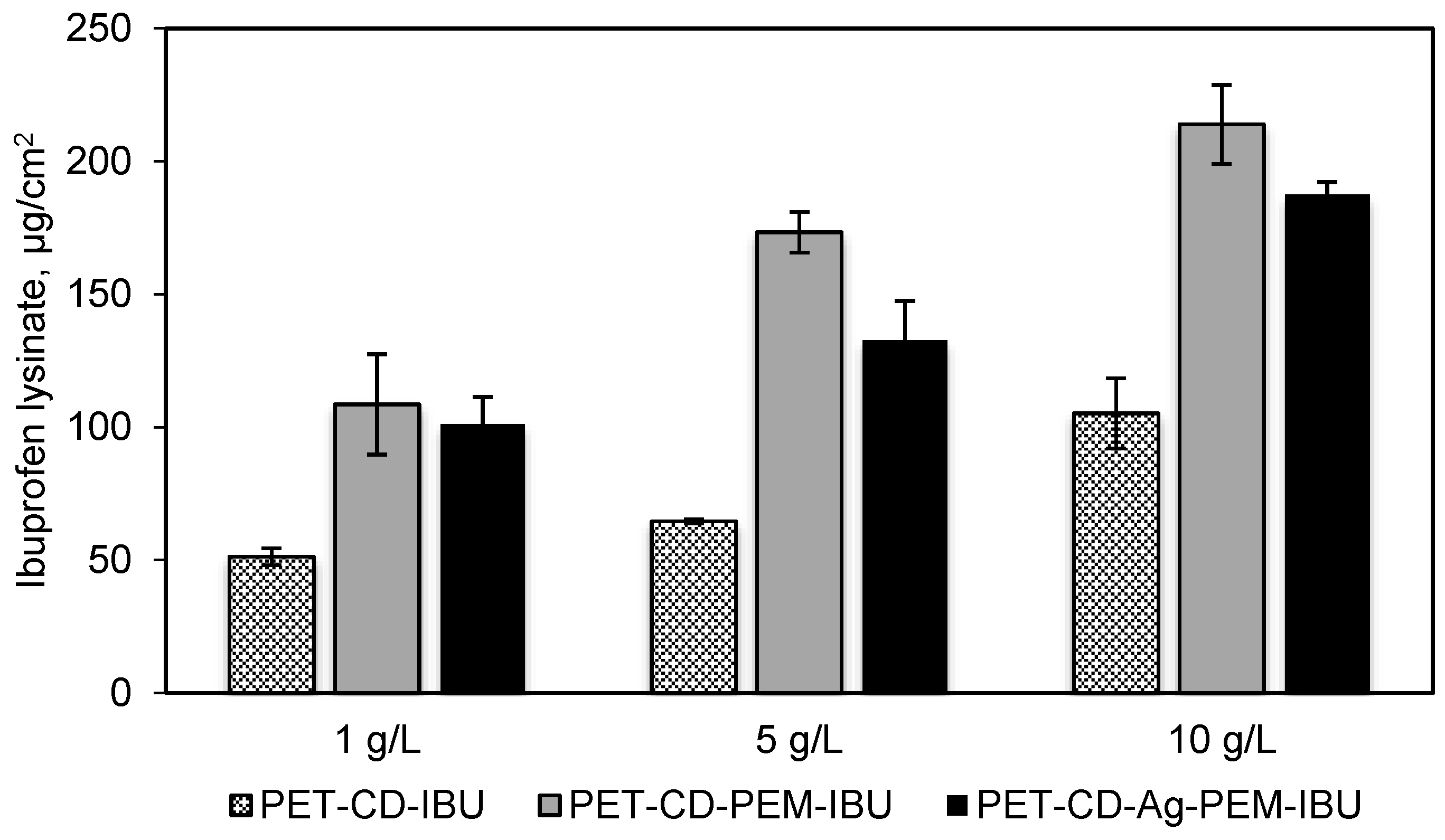
3.3.2. Ibuprofen Loading on Dressing Samples
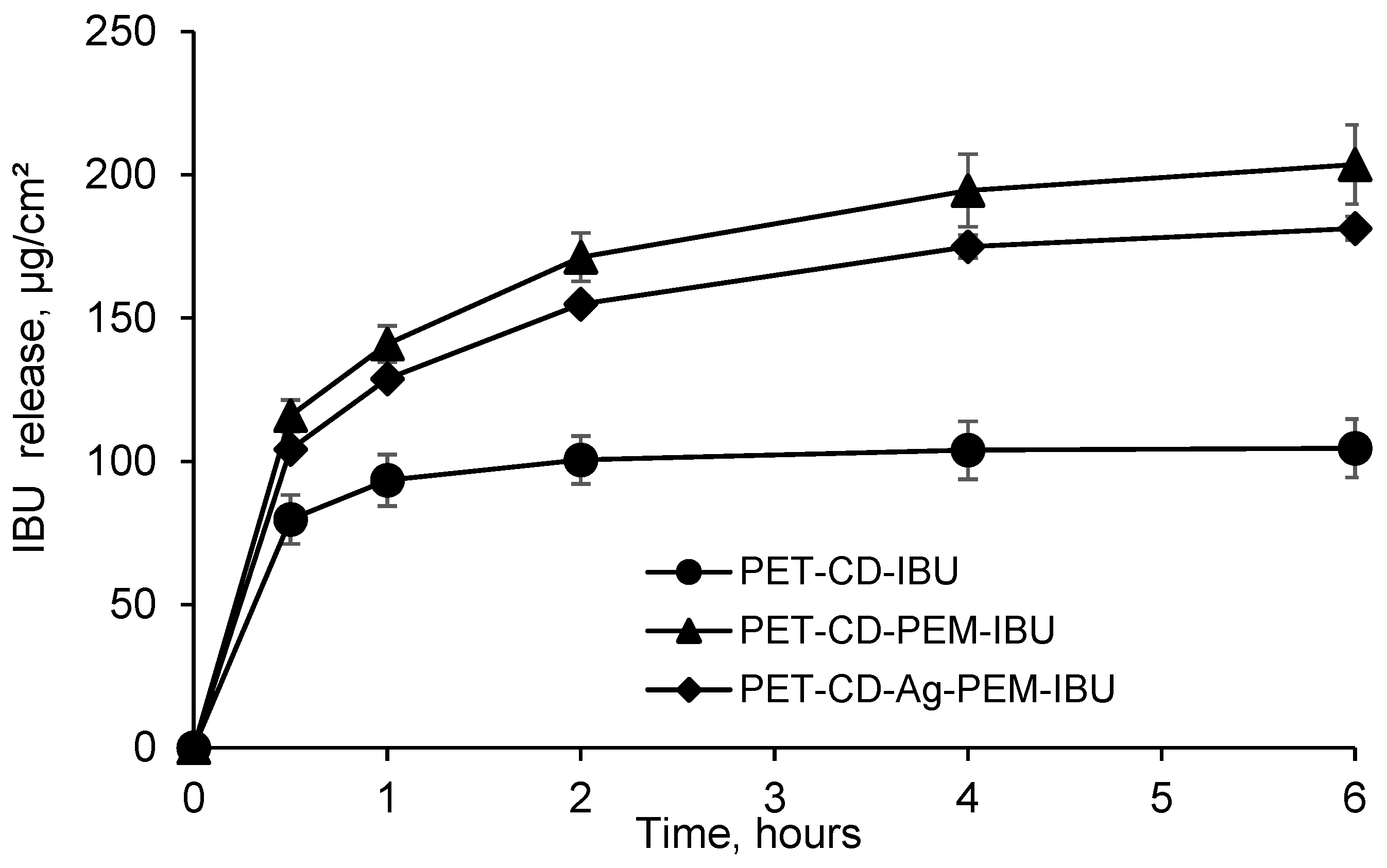
3.3.3. Ibuprofen Kinetics Release
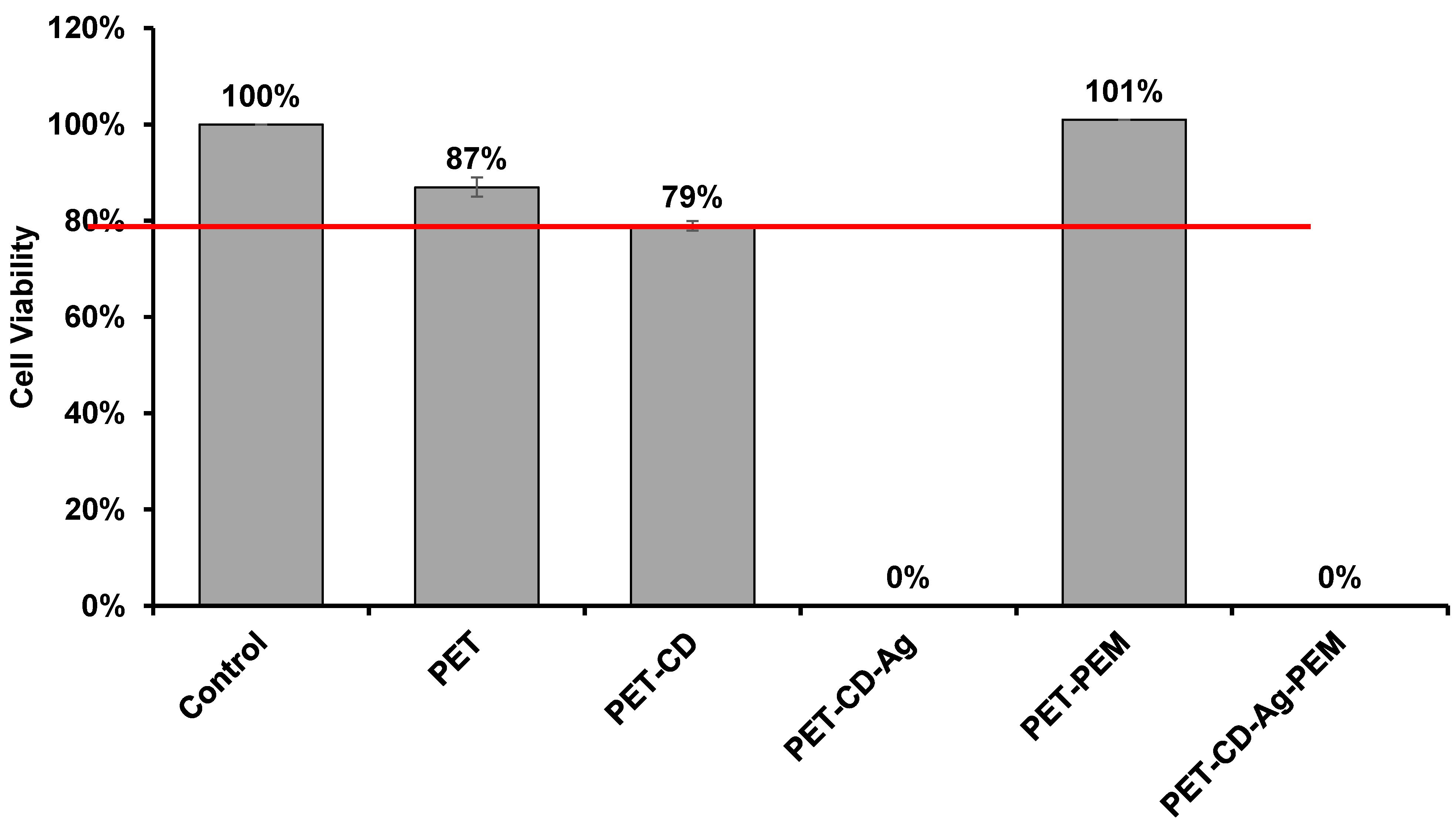
3.4. Biological Evaluation
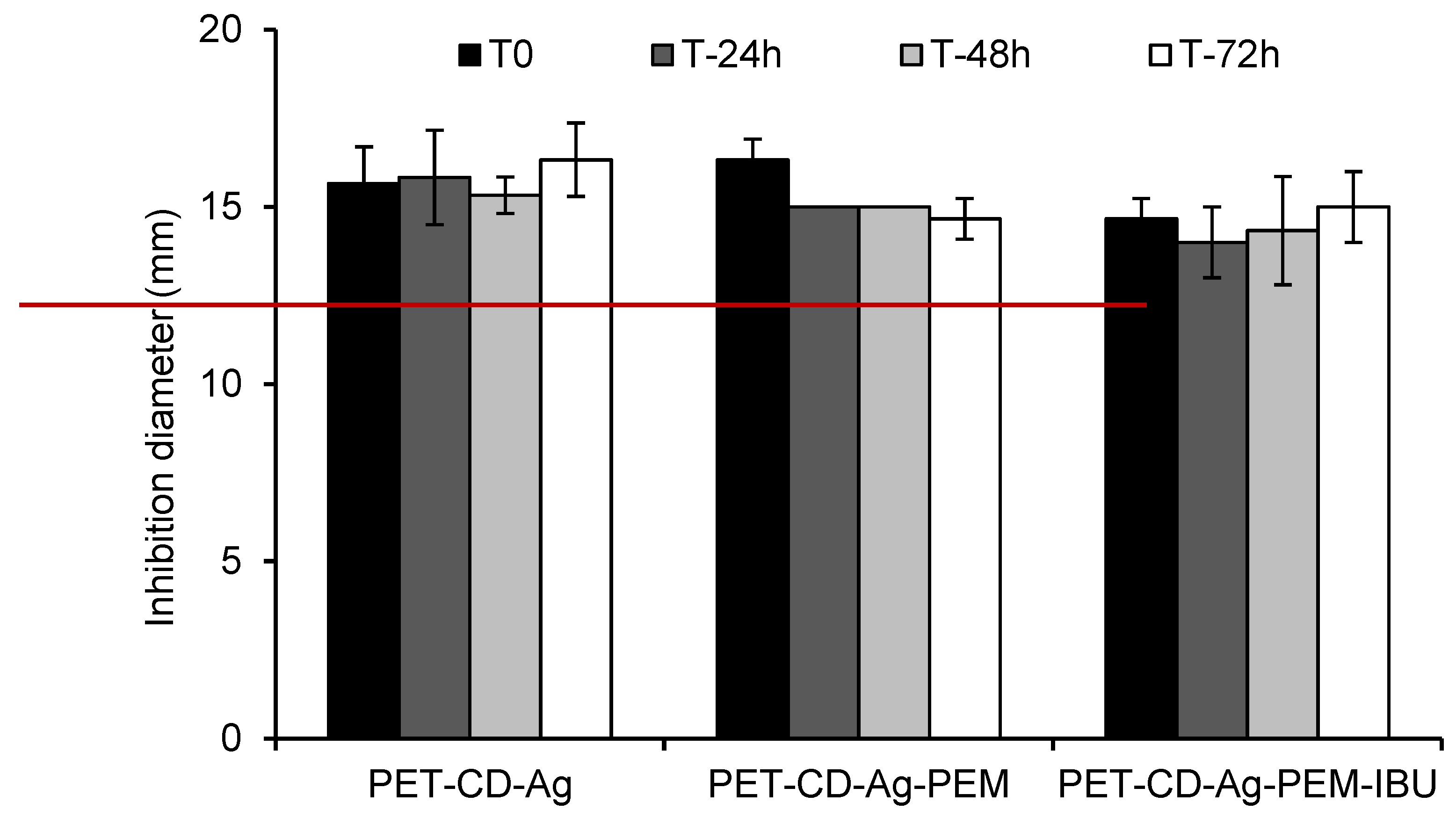
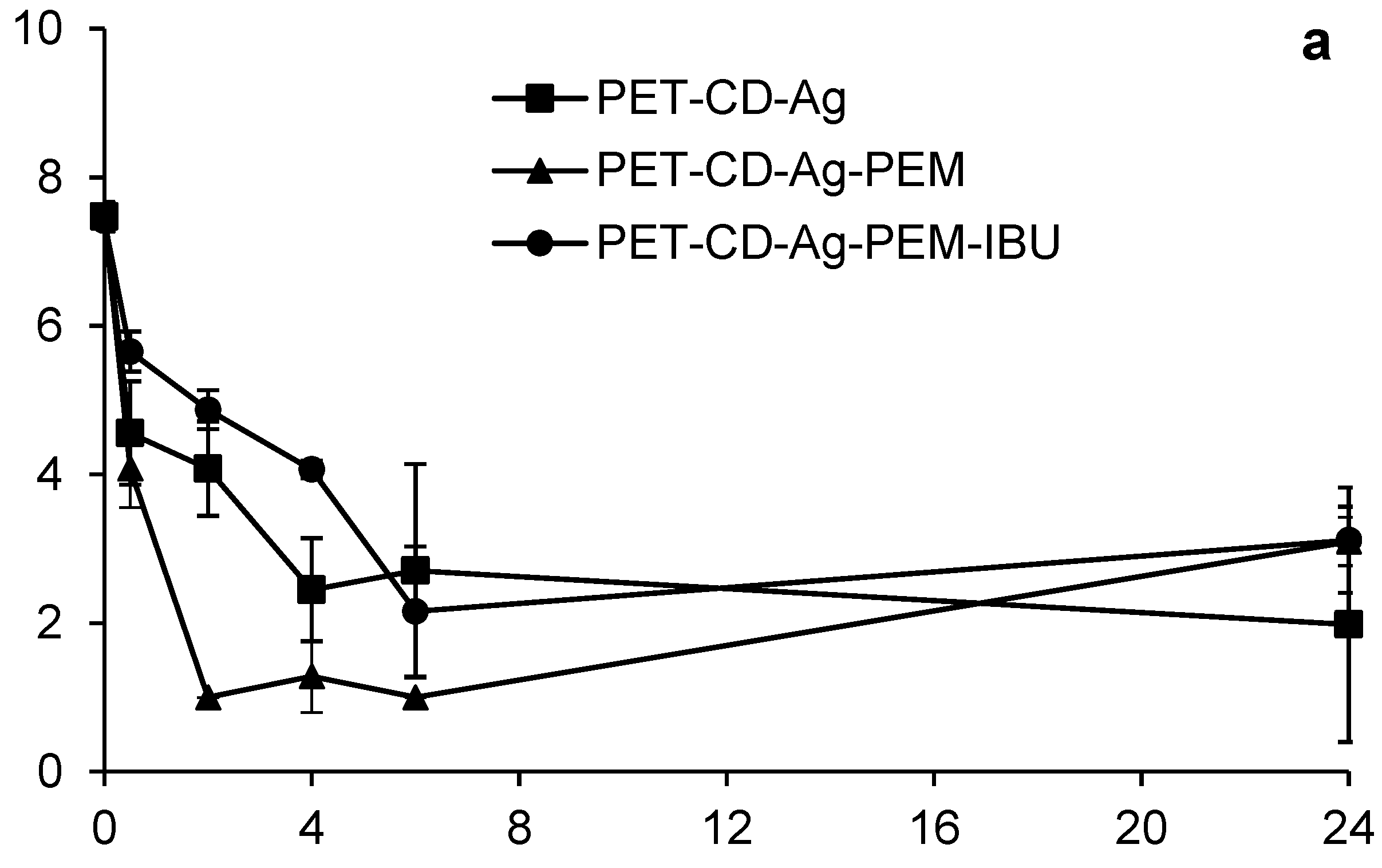
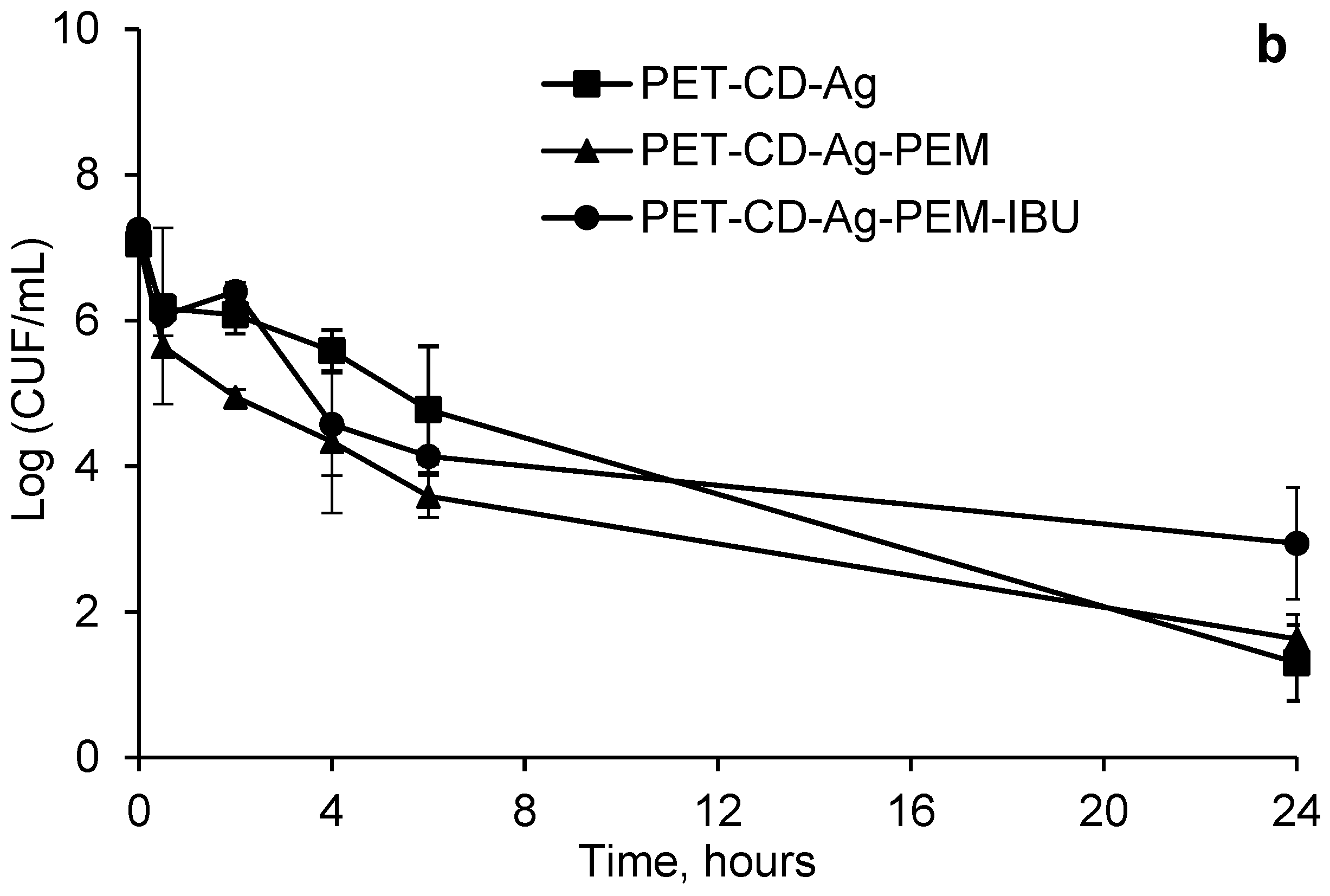
3.5. Microbiological Evaluation
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Järbrink, K.; Ni, G.; Sönnergren, H.; Schmidtchen, A.; Pang, C.; Bajpai, R.; Car, J. Prevalence and Incidence of Chronic Wounds and Related Complications: A Protocol for a Systematic Review. Syst. Rev. 2016, 5, 152. [Google Scholar] [CrossRef] [Green Version]
- Gottrup, F.; Jørgensen, B.; Karlsmark, T.; Sibbald, R.G.; Rimdeika, R.; Harding, K.; Price, P.; Venning, V.; Vowden, P.; Jünger, M.; et al. Reducing Wound Pain in Venous Leg Ulcers with Biatain Ibu: A Randomized, Controlled Double-Blind Clinical Investigation on the Performance and Safety. Wound Repair Regen. 2008, 16, 615–625. [Google Scholar] [CrossRef] [PubMed]
- Price, P.; Fogh, K.; Glynn, C.; Krasner, D.L.; Osterbrink, J.; Sibbald, R.G. Why Combine a Foam Dressing with Ibuprofen for Wound Pain and Moist Wound Healing? Int. Wound J. 2007, 4 (Suppl. 1), 1–3. [Google Scholar] [CrossRef]
- Swanson, T.; Angel, D.; Sussman, G.; Cooper, R. Wound Infection in Clinical Practice Update 2016; Wound Infection Institute (WII): 2016. Available online: https://www.woundinfection-institute.com/wp-content/uploads/2017/03/IWII-Wound-infection-in-clinical-practice.pdf (accessed on 3 June 2021).
- Atiyeh, B.S.; Costagliola, M.; Hayek, S.N.; Dibo, S.A. Effect of Silver on Burn Wound Infection Control and Healing: Review of the Literature. Burns 2007, 33, 139–148. [Google Scholar] [CrossRef]
- Jung, W.K.; Koo, H.C.; Kim, K.W.; Shin, S.; Kim, S.H.; Park, Y.H. Antibacterial Activity and Mechanism of Action of the Silver Ion in Staphylococcus Aureus and Escherichia Coli. Appl. Environ. Microbiol. 2008, 74, 2171–2178. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sripriya, J.; Anandhakumar, S.; Achiraman, S.; Antony, J.J.; Siva, D.; Raichur, A.M. Laser Receptive Polyelectrolyte Thin Films Doped with Biosynthesized Silver Nanoparticles for Antibacterial Coatings and Drug Delivery Applications. Int. J. Pharm. 2013, 457, 206–213. [Google Scholar] [CrossRef] [PubMed]
- Anandhakumar, S.; Raichur, A.M. Polyelectrolyte/Silver Nanocomposite Multilayer Films as Multifunctional Thin Film Platforms for Remote Activated Protein and Drug Delivery. Acta Biomater. 2013, 9, 8864–8874. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Cao, W.; Xiang, Q.; Jin, F.; Peng, X.; Li, Q.; Jiang, M.; Hu, B.; Xing, X. Silver Nanoparticle and Lysozyme/Tannic Acid Layer-by-Layer Assembly Antimicrobial Multilayer on Magnetic Nanoparticle by an Eco-Friendly Route. Mater. Sci. Eng. C 2017, 76, 886–896. [Google Scholar] [CrossRef] [PubMed]
- Mogrovejo-Valdivia, A.; Rahmouni, O.; Tabary, N.; Maton, M.; Neut, C.; Martel, B.; Blanchemain, N. In Vitro Evaluation of Drug Release and Antibacterial Activity of a Silver-Loaded Wound Dressing Coated with a Multilayer System. Int. J. Pharm. 2019, 556, 301–310. [Google Scholar] [CrossRef]
- Aubert-Viard, F.; Martin, A.; Chai, F.; Neut, C.; Tabary, N.; Martel, B. Nicolas Blanchemain Chitosan Finishing Nonwoven Textiles Loaded with Silver and Iodide for Antibacterial Wound Dressing Applications. Biomed. Mater. 2015, 10, 015023. [Google Scholar] [CrossRef] [PubMed]
- Burd, A.; Kwok, C.H.; Hung, S.C.; Chan, H.S.; Gu, H.; Lam, W.K.; Huang, L. A Comparative Study of the Cytotoxicity of Silver-Based Dressings in Monolayer Cell, Tissue Explant, and Animal Models. Wound Repair Regen. 2007, 15, 94–104. [Google Scholar] [CrossRef]
- Poon, V.K.M.; Burd, A. In Vitro Cytotoxity of Silver: Implication for Clinical Wound Care. Burns 2004, 30, 140–147. [Google Scholar] [CrossRef] [PubMed]
- Abboud, E.C.; Settle, J.C.; Legare, T.B.; Marcet, J.E.; Barillo, D.J.; Sanchez, J.E. Silver-Based Dressings for the Reduction of Surgical Site Infection: Review of Current Experience and Recommendation for Future Studies. Burns 2014, 40, S30–S39. [Google Scholar] [CrossRef] [PubMed]
- Jørgensen, B.; Gottrup, F.; Karlsmark, T.; Bech-Thomsen, N.; Sibbald, R.G. Combined Use of an Ibuprofen-Releasing Foam Dressing and Silver Dressing on Infected Leg Ulcers. J. Wound Care 2008, 17, 210–214. [Google Scholar] [CrossRef] [PubMed]
- Münter, K.C.; Beele, H.; Russell, L.; Crespi, A.; Gröchenig, E.; Basse, P.; Alikadic, N.; Fraulin, F.; Dahl, C.; Jemma, A.P. Effect of a Sustained Silver-Releasing Dressing on Ulcers with Delayed Healing: The CONTOP Study. J. Wound Care 2006, 15, 199–206. [Google Scholar] [CrossRef] [PubMed]
- Morgado, P.I.; Miguel, S.P.; Correia, I.J.; Aguiar-Ricardo, A. Ibuprofen Loaded PVA/Chitosan Membranes: A Highly Efficient Strategy towards an Improved Skin Wound Healing. Carbohydr. Polym. 2017, 159, 136–145. [Google Scholar] [CrossRef]
- Jørgensen, B.; Friis, G.J.; Gottrup, F. Pain and Quality of Life for Patients with Venous Leg Ulcers: Proof of Concept of the Efficacy of Biatain-Ibu, a New Pain Reducing Wound Dressing. Wound Repair Regen. 2006, 14, 233–239. [Google Scholar] [CrossRef]
- Sibbald, R.G.; Coutts, P.; Fierheller, M.; Woo, K. A Pilot (Real-Life) Randomised Clinical Evaluation of a Pain-Relieving Foam Dressing: (Ibuprofen-Foam versus Local Best Practice). Int. Wound J. 2007, 4 (Suppl. 1), 16–23. [Google Scholar] [CrossRef]
- Agarwal, A.; Nelson, T.B.; Kierski, P.R.; Schurr, M.J.; Murphy, C.J.; Czuprynski, C.J.; McAnulty, J.F.; Abbott, N.L. Polymeric Multilayers That Localize the Release of Chlorhexidine from Biologic Wound Dressings. Biomaterials 2012, 33, 6783–6792. [Google Scholar] [CrossRef] [Green Version]
- Maver, T.; Gradišnik, L.; Kurečič, M.; Hribernik, S.; Smrke, D.M.; Maver, U.; Kleinschek, K.S. Layering of Different Materials to Achieve Optimal Conditions for Treatment of Painful Wounds. Int. J. Pharm. 2017, 529, 576–588. [Google Scholar] [CrossRef]
- Shukla, A.; Fuller, R.C.; Hammond, P.T. Design of Multi-Drug Release Coatings Targeting Infection and Inflammation. J. Control. Release 2011, 155, 159–166. [Google Scholar] [CrossRef] [PubMed]
- Aubert-Viard, F.; Mogrovejo-Valdivia, A.; Tabary, N.; Maton, M.; Chai, F.; Neut, C.; Martel, B.; Blanchemain, N. Evaluation of Antibacterial Textile Covered by Layer-by-Layer Coating and Loaded with Chlorhexidine for Wound Dressing Application. Mater. Sci. Eng. C 2019, 100, 554–563. [Google Scholar] [CrossRef]
- Shukla, A.; Fang, J.C.; Puranam, S.; Hammond, P.T. Release of Vancomycin from Multilayer Coated Absorbent Gelatin Sponges. J. Control. Release 2012, 157, 64–71. [Google Scholar] [CrossRef] [PubMed]
- Decher, G. Fuzzy Nanoassemblies: Toward Layered Polymeric Multicomposites. Science 1997, 277, 1232–1237. [Google Scholar] [CrossRef]
- Zhou, B.; Hu, Y.; Li, J.; Li, B. Chitosan/Phosvitin Antibacterial Films Fabricated via Layer-by-Layer Deposition. Int. J. Biol. Macromol. 2014, 64, 402–408. [Google Scholar] [CrossRef] [PubMed]
- Zhou, B.; Li, Y.; Deng, H.; Hu, Y.; Li, B. Antibacterial Multilayer Films Fabricated by Layer-by-Layer Immobilizing Lysozyme and Gold Nanoparticles on Nanofibers. Colloids Surf. B Biointerfaces 2014, 116, 432–438. [Google Scholar] [CrossRef] [PubMed]
- Gomes, A.P.; Mano, J.F.; Queiroz, J.A.; Gouveia, I.C. Incorporation of Antimicrobial Peptides on Functionalized Cotton Gauzes for Medical Applications. Carbohydr. Polym. 2015, 127, 451–461. [Google Scholar] [CrossRef] [Green Version]
- Croisier, F.; Jérôme, C. Chitosan-Based Biomaterials for Tissue Engineering. Eur. Polym. J. 2013, 49, 780–792. [Google Scholar] [CrossRef] [Green Version]
- Jayakumar, R.; Prabaharan, M.; Sudheesh Kumar, P.T.; Nair, S.V.; Tamura, H. Biomaterials Based on Chitin and Chitosan in Wound Dressing Applications. Biotechnol. Adv. 2011, 29, 322–337. [Google Scholar] [CrossRef]
- Bano, I.; Arshad, M.; Yasin, T.; Ghauri, M.A.; Younus, M. Chitosan: A Potential Biopolymer for Wound Management. Int. J. Biol. Macromol. 2017, 102, 380–383. [Google Scholar] [CrossRef]
- Balan, V.; Verestiuc, L. Strategies to Improve Chitosan Hemocompatibility: A Review. Eur. Polym. J. 2014, 53, 171–188. [Google Scholar] [CrossRef]
- Patrulea, V.; Ostafe, V.; Borchard, G.; Jordan, O. Chitosan as a Starting Material for Wound Healing Applications. Eur. J. Pharm. Biopharm. 2015, 97, 417–426. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lee, Y.-H.; Chang, J.-J.; Yang, M.-C.; Chien, C.-T.; Lai, W.-F. Acceleration of Wound Healing in Diabetic Rats by Layered Hydrogel Dressing. Carbohydr. Polym. 2012, 88, 809–819. [Google Scholar] [CrossRef]
- Han, F.; Dong, Y.; Song, A.; Yin, R.; Li, S. Alginate/Chitosan Based Bi-Layer Composite Membrane as Potential Sustained-Release Wound Dressing Containing Ciprofloxacin Hydrochloride. Appl. Surf. Sci. 2014, 311, 626–634. [Google Scholar] [CrossRef]
- Brewster, M.E.; Loftsson, T. Cyclodextrins as Pharmaceutical Solubilizers. Adv. Drug Deliv. Rev. 2007, 59, 645–666. [Google Scholar] [CrossRef] [PubMed]
- Blanchemain, N.; Karrout, Y.; Tabary, N.; Bria, M.; Neut, C.; Hildebrand, H.F.; Siepmann, J.; Martel, B. Comparative Study of Vascular Prostheses Coated with Polycyclodextrins for Controlled Ciprofloxacin Release. Carbohydr. Polym. 2012, 90, 1695–1703. [Google Scholar] [CrossRef]
- Flores, C.; Lopez, M.; Tabary, N.; Neut, C.; Chai, F.; Betbeder, D.; Herkt, C.; Cazaux, F.; Gaucher, V.; Martel, B.; et al. Preparation and Characterization of Novel Chitosan and β-Cyclodextrin Polymer Sponges for Wound Dressing Applications. Carbohydr. Polym. 2017, 173, 535–546. [Google Scholar] [CrossRef]
- Ouerghemmi, S.; Degoutin, S.; Tabary, N.; Cazaux, F.; Maton, M.; Gaucher, V.; Janus, L.; Neut, C.; Chai, F.; Blanchemain, N.; et al. Triclosan Loaded Electrospun Nanofibers Based on a Cyclodextrin Polymer and Chitosan Polyelectrolyte Complex. Int. J. Pharm. 2016, 513, 483–495. [Google Scholar] [CrossRef]
- Garcia-Fernandez, M.J.; Maton, M.; Benzine, Y.; Tabary, N.; Baptiste, E.J.; Gargouri, M.; Bria, M.; Blanchemain, N.; Karrout, Y. Ciprofloxacin Loaded Vascular Prostheses Functionalized with Poly-Methylbeta-Cyclodextrin: The Importance of in Vitro Release Conditions. J. Drug Deliv. Sci. Technol. 2019, 53, 101166. [Google Scholar] [CrossRef]
- Vermet, G.; Degoutin, S.; Chai, F.; Maton, M.; Flores, C.; Neut, C.; Danjou, P.E.; Martel, B.; Blanchemain, N. Cyclodextrin Modified PLLA Parietal Reinforcement Implant with Prolonged Antibacterial Activity. Acta Biomater. 2017, 53, 222–232. [Google Scholar] [CrossRef]
- Vermet, G.; Degoutin, S.; Chai, F.; Maton, M.; Bria, M.; Danel, C.; Hildebrand, H.F.; Blanchemain, N.; Martel, B. Visceral Mesh Modified with Cyclodextrin for the Local Sustained Delivery of Ropivacaine. Int. J. Pharm. 2014, 476, 149–159. [Google Scholar] [CrossRef]
- Jansook, P.; Ogawa, N.; Loftsson, T. Cyclodextrins: Structure, Physicochemical Properties and Pharmaceutical Applications. Int. J. Pharm. 2018, 535, 272–284. [Google Scholar] [CrossRef] [PubMed]
- Tabary, N.; Garcia-Fernandez, M.J.; Danède, F.; Descamps, M.; Martel, B.; Willart, J.-F. Determination of the Glass Transition Temperature of Cyclodextrin Polymers. Carbohydr. Polym. 2016, 148, 172–180. [Google Scholar] [CrossRef]
- Palomino-Durand, C.; Lopez, M.; Cazaux, F.; Martel, B.; Blanchemain, N.; Chai, F. Influence of the SolubleInsoluble Ratios of Cyclodextrins Polymers on the Viscoelastic Properties of Injectable ChitosanBased Hydrogels for Biomedical Application. Polymers 2019, 11, 214. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Kersani, D.; Mougin, J.; Lopez, M.; Degoutin, S.; Tabary, N.; Cazaux, F.; Janus, L.; Maton, M.; Chai, F.; Sobocinski, J.; et al. Stent Coating by Electrospinning with Chitosan/Poly-Cyclodextrin Based Nanofibers Loaded with Simvastatin for Restenosis Prevention. Eur. J. Pharm. Biopharm. 2020, 150, 156–167. [Google Scholar] [CrossRef]
- Pérez-Anes, A.; Gargouri, M.; Laure, W.; Van Den Berghe, H.; Courcot, E.; Sobocinski, J.; Tabary, N.; Chai, F.; Blach, J.-F.; Addad, A.; et al. Bioinspired Titanium Drug Eluting Platforms Based on a Poly-β-Cyclodextrin—Chitosan Layer-by-Layer Self-Assembly Targeting Infections. ACS Appl. Mater. Interfaces 2015, 7, 12882–12893. [Google Scholar] [CrossRef] [PubMed]
- Weltrowski, M.; Morcellet, M.; Martel, B. Cyclodextrin Polymers and/or Cyclodextrin Derivatives with Complexing Properties and Ion-Exchange Properties and Method for the Production Thereof. U.S. Patent 6,660,804, 9 December 2003. [Google Scholar]
- Martin, A.; Tabary, N.; Chai, F.; Leclercq, L.; Junthip, J.; Aubert-Viard, F.; Neut, C.; Weltrowski, M.; Blanchemain, N.; Martel, B. Build-up of an Antimicrobial Multilayer Coating on a Textile Support Based on a Methylene Blue-Poly(Cyclodextrin) Complex. Biomed. Mater. 2013, 8, 065006. [Google Scholar] [CrossRef] [PubMed]
- Martin, A.; Tabary, N.; Leclercq, L.; Junthip, J.; Degoutin, S.; Aubert-Viard, F.; Cazaux, F.; Lyskawa, J.; Janus, L.; Bria, M.; et al. Multilayered Textile Coating Based on a β-Cyclodextrin Polyelectrolyte for the Controlled Release of Drugs. Carbohydr. Polym. 2013, 93, 718–730. [Google Scholar] [CrossRef]
- Jean-Baptiste, E.; Blanchemain, N.; Neut, C.; Chai, F.; Maton, M.; Martel, B.; Hildebrand, H.; Haulon, S. Evaluation of the Anti-Infectious Properties of Polyester Vascular Prostheses Functionalised with Cyclodextrin. J. Infect. 2014, 68, 116–124. [Google Scholar] [CrossRef]
- Blanchemain, N.; Karrout, Y.; Tabary, N.; Neut, C.; Bria, M.; Siepmann, J.; Hildebrand, H.F.; Martel, B. Methyl-β-Cyclodextrin Modified Vascular Prosthesis: Influence of the Modification Level on the Drug Delivery Properties in Different Media. Acta Biomater. 2011, 7, 304–314. [Google Scholar] [CrossRef]
- Decher, G.; Eckle, M.; Schmitt, J.; Struth, B. Layer-by-Layer Assembled Multicomposite Films. Curr. Opin. Colloid Interface Sci. 1998, 3, 32–39. [Google Scholar] [CrossRef]
- Higuchi, T.; Connors, K. Advances in Analytical Chemistry and Instrumentation. Adv. Anal. Chem. Instrum. 1965, 4, 117–212. [Google Scholar]
- Saokham, P.; Muankaew, C.; Jansook, P.; Loftsson, T. Solubility of Cyclodextrins and Drug/Cyclodextrin Complexes. Molecules 2018, 23, 1161. [Google Scholar] [CrossRef] [Green Version]
- Trotta, F.; Zanetti, M.; Cavalli, R. Cyclodextrin-Based Nanosponges as Drug Carriers. Beilstein J. Org. Chem. 2012, 8, 2091–2099. [Google Scholar] [CrossRef]
- García-Fernández, M.J.; Tabary, N.; Martel, B.; Cazaux, F.; Oliva, A.; Taboada, P.; Concheiro, A.; Alvarez-Lorenzo, C. Poly-(Cyclo)Dextrins as Ethoxzolamide Carriers in Ophthalmic Solutions and in Contact Lenses. Carbohydr. Polym. 2013, 98, 1343–1352. [Google Scholar] [CrossRef]
- Pereva, S.; Sarafska, T.; Bogdanova, S.; Spassov, T. Efficiency of “Cyclodextrin-Ibuprofen” Inclusion Complex Formation. J. Drug Deliv. Sci. Technol. 2016, 35, 34–39. [Google Scholar] [CrossRef] [Green Version]
- Di Cagno, M.; Stein, P.C.; Skalko-Basnet, N.; Brandl, M.; Bauer-Brandl, A. Solubilization of Ibuprofen with β-Cyclodextrin Derivatives: Energetic and Structural Studies. J. Pharm. Biomed. Anal. 2011, 55, 446–451. [Google Scholar] [CrossRef] [PubMed]
- Herbois, R.; Noël, S.; Léger, B.; Tilloy, S.; Menuel, S.; Addad, A.; Martel, B.; Ponchel, A.; Monflier, E. Ruthenium-Containing β-Cyclodextrin Polymer Globules for the Catalytic Hydrogenation of Biomass-Derived Furanic Compounds. Green Chem. 2015, 17, 2444–2454. [Google Scholar] [CrossRef]
- Kfoury, M.; Landy, D.; Auezova, L.; Greige-Gerges, H.; Fourmentin, S. Effect of Cyclodextrin Complexation on Phenylpropanoids’ Solubility and Antioxidant Activity. Beilstein J. Org. Chem. 2014, 10, 2322–2331. [Google Scholar] [CrossRef] [Green Version]
- Steffansen, B.; Herping, S.P.K. Novel Wound Models for Characterizing Ibuprofen Release from Foam Dressings. Int. J. Pharm. 2008, 364, 150–155. [Google Scholar] [CrossRef]
- Blanchemain, N.; Haulon, S.; Boschin, F.; Traisnel, M.; Morcellet, M.; Martel, B.; Hildebrand, H.F. Vascular Prostheses with Controlled Release of Antibiotics Part 2. In Vitro Biological Evaluation of Vascular Prostheses Treated by Cyclodextrins. Biomol. Eng. 2007, 24, 143–148. [Google Scholar] [CrossRef] [PubMed]
| Kf (mM−1) | CE | Slope | Solubilization Factor | |
|---|---|---|---|---|
| βCD | 6200 | 1.08 | 0.52062 | 12 b |
| PCD | 2600 | 0.45 | 0.31308 | 77 a |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mogrovejo-Valdivia, A.; Maton, M.; Garcia-Fernandez, M.J.; Tabary, N.; Chai, F.; Neut, C.; Martel, B.; Blanchemain, N. In Vitro Microbiological and Drug Release of Silver/Ibuprofen Loaded Wound Dressing Designed for the Treatment of Chronically Infected Painful Wounds. Antibiotics 2021, 10, 805. https://doi.org/10.3390/antibiotics10070805
Mogrovejo-Valdivia A, Maton M, Garcia-Fernandez MJ, Tabary N, Chai F, Neut C, Martel B, Blanchemain N. In Vitro Microbiological and Drug Release of Silver/Ibuprofen Loaded Wound Dressing Designed for the Treatment of Chronically Infected Painful Wounds. Antibiotics. 2021; 10(7):805. https://doi.org/10.3390/antibiotics10070805
Chicago/Turabian StyleMogrovejo-Valdivia, Alejandra, Mickael Maton, Maria Jose Garcia-Fernandez, Nicolas Tabary, Feng Chai, Christel Neut, Bernard Martel, and Nicolas Blanchemain. 2021. "In Vitro Microbiological and Drug Release of Silver/Ibuprofen Loaded Wound Dressing Designed for the Treatment of Chronically Infected Painful Wounds" Antibiotics 10, no. 7: 805. https://doi.org/10.3390/antibiotics10070805
APA StyleMogrovejo-Valdivia, A., Maton, M., Garcia-Fernandez, M. J., Tabary, N., Chai, F., Neut, C., Martel, B., & Blanchemain, N. (2021). In Vitro Microbiological and Drug Release of Silver/Ibuprofen Loaded Wound Dressing Designed for the Treatment of Chronically Infected Painful Wounds. Antibiotics, 10(7), 805. https://doi.org/10.3390/antibiotics10070805






