New Formulation of Platelet-Rich Plasma Enriched in Platelet and Extraplatelet Biomolecules Using Hydrogels
Abstract
1. Introduction
2. Results
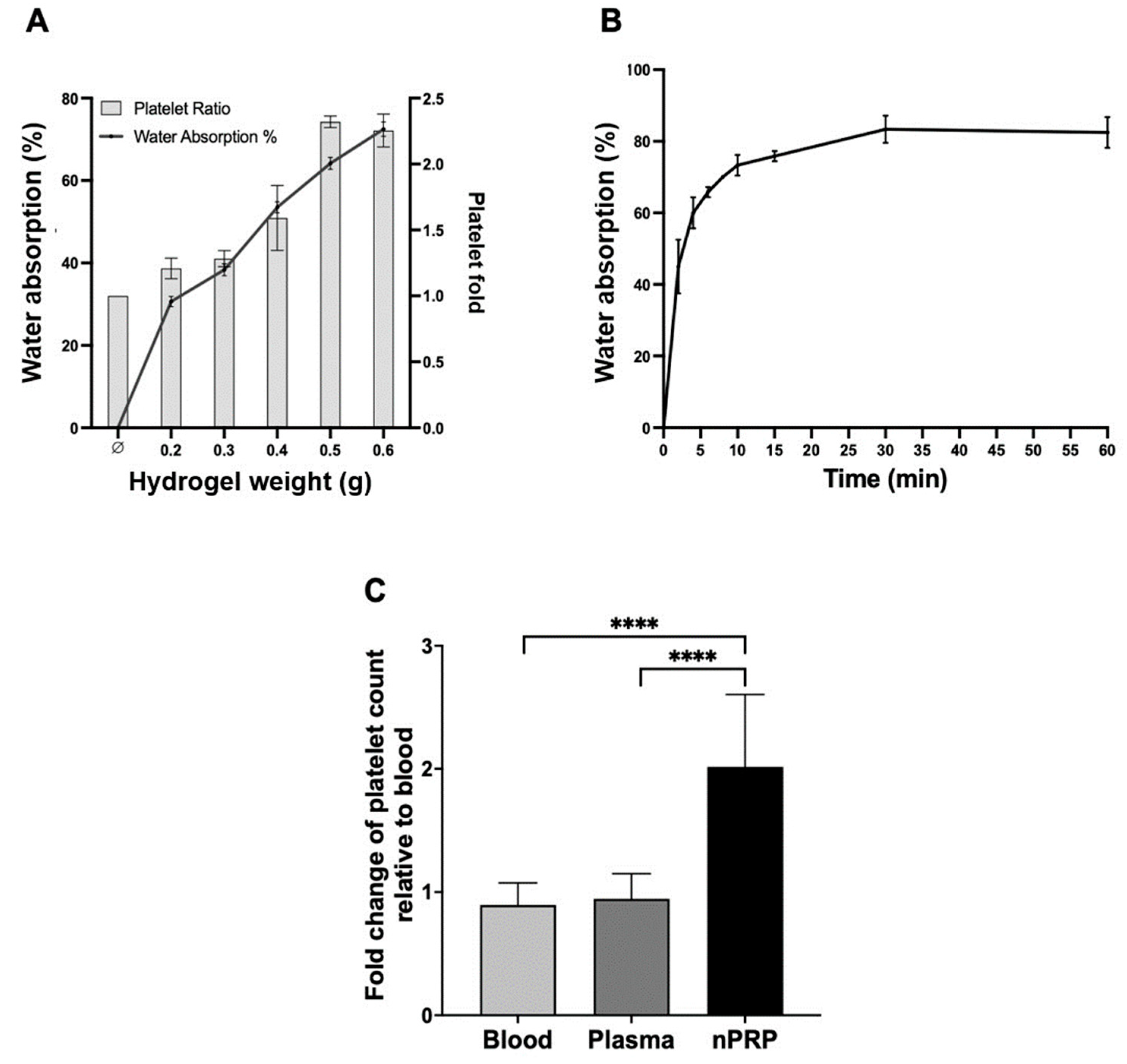
2.1. Water Absorption Parameters Optimization for nPRP Obtention
2.2. Comparison of Platelets and Total Proteins Concentration Capacity between a Standard (sPRP) and a Novel (nPRP) PRP
2.3. Concentration of Growth Factors in sPRP and nPRP
2.4. Ion Concentration Capacity of sPRP and nPRP
2.5. sPRP and nPRP Processing Impact on Platelet Activation
2.6. Fibrinogen Levels and Biomechanical Properties of the Clot Resulting from sPRP and nPRP
2.7. Viability of Fibroblasts Culture upon Exposure to nPRP
3. Discussion
4. Materials and Methods
4.1. Donors
4.2. Fabrication of the Hydroxyethyl Acrylamide (HEAA)-Based Hydrogel Powder
4.3. Standard Platelet-Rich Plasma (sPRP) Preparation
4.4. Novel Platelet-Rich Plasma (nPRP) Preparation
4.5. Platelet and Protein Fold Measurement
4.6. Platelet and Plasmatic Growth Factor Concentration Measurement
4.7. Ion Levels Measurement
4.8. Platelet Activation Test
4.9. Fibrinogen Levels Measurements and Biomechanical Tests on Fibrin Clots
4.10. Normal Human Dermal Fibroblast (NHDF) Cell Cultures
4.11. Isolation and Culture of Human Primary Chondrocytes
4.12. Cell Viability Assay
4.13. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ackerman, I.N.; Bohensky, M.A.; Zomer, E.; Tacey, M.; Gorelik, A.; Brand, C.A.; de Steiger, R. The Projected Burden of Primary Total Knee and Hip Replacement for Osteoarthritis in Australia to the Year 2030. BMC Musculoskelet. Disord. 2019, 20, 90. [Google Scholar] [CrossRef] [PubMed]
- Losina, E.; Paltiel, A.D.; Weinstein, A.M.; Yelin, E.; Hunter, D.J.; Chen, S.P.; Klara, K.; Suter, L.G.; Solomon, D.H.; Burbine, S.A.; et al. Lifetime Medical Costs of Knee Osteoarthritis Management in the United States: Impact of Extending Indications for Total Knee Arthroplasty. Arthritis Care Res. 2015, 67, 203–215. [Google Scholar] [CrossRef] [PubMed]
- Andia, I.; Atilano, L.; Maffulli, N. Moving toward Targeting the Right Phenotype with the Right Platelet-Rich Plasma (PRP) Formulation for Knee Osteoarthritis. Ther. Adv. Musculoskelet. Dis. 2021, 13, 1759720X211004336. [Google Scholar] [CrossRef] [PubMed]
- Sánchez, M.; Delgado, D.; Garate, A.; Sánchez, P.; Oraa, J.; Bilbao, A.M.; Guadilla, J.; Aizpurua, B.; Fiz, N.; Azofra, J.; et al. PRP Injections in Orthopaedic Surgery: Why, When and How to Use PRP Dynamic Liquid Scaffold Injections in Orthopaedic Surgery; IntechOpen: London, UK, 2018; ISBN 978-1-78923-113-7. [Google Scholar]
- Alsousou, J.; Thompson, M.; Hulley, P.; Noble, A.; Willett, K. The Biology of Platelet-Rich Plasma and Its Application in Trauma and Orthopaedic Surgery: A review of the literature. J. Bone Jt. 2009, 91, 987–996. [Google Scholar] [CrossRef]
- Zhang, M.; Park, G.; Zhou, B.; Luo, D. Applications and Efficacy of Platelet-Rich Plasma in Dermatology: A Clinical Review. J. Cosmet. Dermatol. 2018, 17, 660–665. [Google Scholar] [CrossRef]
- Emer, J. Platelet-Rich Plasma (PRP): Current Applications in Dermatology. Ski. Ther. Lett. 2019, 24, 1–6. [Google Scholar]
- Merchán, W.H.; Gómez, L.A.; Chasoy, M.E.; Alfonso-Rodríguez, C.A.; Muñoz, A.L. Platelet-Rich Plasma, a Powerful Tool in Dermatology. J. Tissue Eng. Regen. Med. 2019, 13, 892–901. [Google Scholar] [CrossRef]
- Nikolidakis, D.; Jansen, J.A. The Biology of Platelet-Rich Plasma and Its Application in Oral Surgery: Literature Review. Tissue Eng. Part B Rev. 2008, 14, 249–258. [Google Scholar] [CrossRef]
- Sánchez, M.; Beitia, M.; Pompei, O.; Jorquera, C.; Sánchez, P.; Knörr, J.; Soldado, F.; López, L.; Oraa, J.; Miren Bilbao, A.; et al. Isolation, Activation, and Mechanism of Action of Platelet-Rich Plasma and Its Applications for Joint Repair. In Regenerative Medicine; Choudhery, M.S., Ed.; IntechOpen: London, UK, 2020; ISBN 978-1-83881-927-9. [Google Scholar]
- Boilard, E.; Nigrovic, P.A. Platelets. In Kelley and Firestein’s Textbook of Rheumatology; Elsevier: Amsterdam, The Netherlands, 2017; pp. 264–273.e3. ISBN 978-0-323-31696-5. [Google Scholar]
- Rumbaut, R.E.; Thiagarajan, P. General Characteristics of Platelets; Morgan & Claypool Life Sciences: San Rafael, CA, USA, 2010. [Google Scholar]
- Ferrara, N. Role of Vascular Endothelial Growth Factor in the Regulation of Angiogenesis. Kidney Int. 1999, 56, 794–814. [Google Scholar] [CrossRef]
- Anitua, E.; Prado, R.; Sánchez, M.; Orive, G. Platelet-Rich Plasma: Preparation and Formulation. Oper. Tech. Orthop. 2012, 22, 25–32. [Google Scholar] [CrossRef]
- Carpenter, G.; Stoscheck, C.M.; Soderquist, A.M. Epidermal Growth Factor. Ann. N. Y. Acad. Sci. 1982, 397, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Foster, T.E.; Puskas, B.L.; Mandelbaum, B.R.; Gerhardt, M.B.; Rodeo, S.A. Platelet-Rich Plasma: From Basic Science to Clinical Applications. Am. J. Sports Med. 2009, 37, 2259–2272. [Google Scholar] [CrossRef] [PubMed]
- Kurten, R.C.; Chowdhury, P.; Sanders, R.C.; Pittman, L.M.; Sessions, L.W.; Chambers, T.C.; Lyle, C.S.; Schnackenberg, B.J.; Jones, S.M. Coordinating Epidermal Growth Factor-Induced Motility Promotes Efficient Wound Closure. Am. J. Physiol.-Cell Physiol. 2005, 288, C109–C121. [Google Scholar] [CrossRef]
- Yang, E.Y.; Moses, H.L. Transforming Growth Factor beta 1--Induced Changes in Cell Migration, Proliferation, and Angiogenesis in the Chicken Chorioallantoic Membrane. J. Cell Biol. 1990, 111, 731–741. [Google Scholar] [CrossRef] [PubMed]
- Ahmad, Z.; Howard, D.; Brooks, R.A.; Wardale, J.; Henson, F.M.; Getgood, A.; Rushton, N. The Role of Platelet Rich Plasma in Musculoskeletal Science. JRSM Short. Rep. 2012, 3, 40. [Google Scholar] [CrossRef]
- Laron, Z. Insulin-like Growth Factor 1 (IGF-1): A Growth Hormone. Mol. Pathol. 2001, 54, 311–316. [Google Scholar] [CrossRef] [PubMed]
- Oliveira, A.G.; Araújo, T.G.; Carvalho, B.d.M.; Rocha, G.Z.; Santos, A.; Saad, M.J.A. The Role of Hepatocyte Growth Factor (HGF) in Insulin Resistance and Diabetes. Front. Endocrinol. 2018, 9, 503. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, T. Structure and Function of Hepatocyte Growth Factor. Prog. Growth Factor. Res. 1991, 3, 67–85. [Google Scholar] [CrossRef]
- Zhang, J.; Middleton, K.K.; Fu, F.H.; Im, H.-J.; Wang, J.H.-C. HGF Mediates the Anti-Inflammatory Effects of PRP on Injured Tendons. PLoS ONE 2013, 8, e67303. [Google Scholar] [CrossRef]
- Garg, A.K. The Use of Platelet-Rich Plasma to Enhance the Success of Bone Grafts around Dental Implants. Dent. Implant. Update 2000, 11, 17–21. [Google Scholar]
- Lyras, D.N.; Kazakos, K.; Agrogiannis, G.; Verettas, D.; Kokka, A.; Kiziridis, G.; Chronopoulos, E.; Tryfonidis, M. Experimental Study of Tendon Healing Early Phase: Is IGF-1 Expression Influenced by Platelet Rich Plasma Gel? Orthop. Traumatol. Surg. Res. 2010, 96, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Ortolani, E.; Guerriero, M.; Coli, A.; Giannuario, A.D.; Minniti, G.; Polimeni, A. Effect of PDGF, IGF-1 and PRP on the Implant Osseointegration. An Histological and Immunohistochemical Study in Rabbits. Ann. Stomatol. 2014, 5, 66. [Google Scholar] [CrossRef]
- Bendinelli, P.; Matteucci, E.; Dogliotti, G.; Corsi, M.M.; Banfi, G.; Maroni, P.; Desiderio, M.A. Molecular Basis of Anti-Inflammatory Action of Platelet-Rich Plasma on Human Chondrocytes: Mechanisms of NF-ΚB Inhibition via HGF. J. Cell. Physiol. 2010, 225, 757–766. [Google Scholar] [CrossRef] [PubMed]
- Beitia, M.; Delgado, D.; Mercader, J.; Sánchez, P.; López de Dicastillo, L.; Sánchez, M. Action of Platelet-Rich Plasma on In Vitro Cellular Bioactivity: More than Platelets. Int. J. Mol. Sci. 2023, 24, 5367. [Google Scholar] [CrossRef] [PubMed]
- Lansdown, D.; Fortier, L. Platelet Rich Plasma: Formulations, Preparations, Constituents, and Their Effects. Oper. Tech. Sports Med. 2016, 25, 7–12. [Google Scholar] [CrossRef]
- Caló, E.; Khutoryanskiy, V.V. Biomedical Applications of Hydrogels: A Review of Patents and Commercial Products. Eur. Polym. J. 2015, 65, 252–267. [Google Scholar] [CrossRef]
- Ho, T.-C.; Chang, C.-C.; Chan, H.-P.; Chung, T.-W.; Shu, C.-W.; Chuang, K.-P.; Duh, T.-H.; Yang, M.-H.; Tyan, Y.-C. Hydrogels: Properties and Applications in Biomedicine. Molecules 2022, 27, 2902. [Google Scholar] [CrossRef]
- Wang, R.L.C.; Kreuzer, H.J.; Grunze, M. Molecular Conformation and Solvation of Oligo(Ethylene Glycol)-Terminated Self-Assembled Monolayers and Their Resistance to Protein Adsorption. J. Phys. Chem. B 1997, 101, 9767–9773. [Google Scholar] [CrossRef]
- Chen, S.; Li, L.; Zhao, C.; Zheng, J. Surface Hydration: Principles and Applications toward Low-Fouling/Nonfouling Biomaterials. Polymer 2010, 51, 5283–5293. [Google Scholar] [CrossRef]
- Utrata-Wesołek, A. Antifouling Surfaces in Medical Application. Polimery 2013, 58, 685–695. [Google Scholar] [CrossRef]
- Zhao, C.; Li, X.; Li, L.; Cheng, G.; Gong, X.; Zheng, J. Dual Functionality of Antimicrobial and Antifouling of Poly(N-Hydroxyethylacrylamide)/Salicylate Hydrogels. Langmuir 2013, 29, 1517–1524. [Google Scholar] [CrossRef] [PubMed]
- Zhao, C.; Chen, Q.; Patel, K.; Li, L.; Li, X.; Wang, Q.; Zhang, G.; Zheng, J. Synthesis and Characterization of PH-Sensitive Poly(N-2-Hydroxyethyl Acrylamide)–Acrylic Acid (Poly(HEAA/AA)) Nanogels with Antifouling Protection for Controlled Release. Soft Matter 2012, 8, 7848–7857. [Google Scholar] [CrossRef]
- Synthesis and Characterization of Poly(N-Hydroxyethylacrylamide) for Long-Term Antifouling Ability|Biomacromolecules. Available online: https://pubs.acs.org/doi/abs/10.1021/bm2011455 (accessed on 1 September 2023).
- Gertsiuk, M.; Samchenko, Y. Separation of Nonreacted Acrylamide from Polyacrylamide Gel for Endoprothesing. Ars. Separatoria Acta 2007, 5, 98–101. [Google Scholar]
- Peng, Z.; Xue, H.; Liu, X.; Wang, S.; Liu, G.; Jia, X.; Zhu, Z.; Orvy, M.J.; Yang, Y.; Wang, Y.; et al. Tough, Adhesive Biomimetic Hyaluronic Acid Methacryloyl Hydrogels for Effective Wound Healing. Front. Bioeng. Biotechnol. 2023, 11, 1222088. [Google Scholar] [CrossRef]
- Oudelaar, B.W.; Peerbooms, J.C.; Huis In ’t Veld, R.; Vochteloo, A.J.H. Concentrations of Blood Components in Commercial Platelet-Rich Plasma Separation Systems: A Review of the Literature. Am. J. Sports Med. 2019, 47, 479–487. [Google Scholar] [CrossRef]
- Olesen, J.L.; Heinemeier, K.M.; Haddad, F.; Langberg, H.; Flyvbjerg, A.; Kjaer, M.; Baldwin, K.M. Expression of Insulin-like Growth Factor I, Insulin-like Growth Factor Binding Proteins, and Collagen MRNA in Mechanically Loaded Plantaris Tendon. J. Appl. Physiol. 2006, 101, 183–188. [Google Scholar] [CrossRef]
- Taniguchi, Y.; Yoshioka, T.; Sugaya, H.; Gosho, M.; Aoto, K.; Kanamori, A.; Yamazaki, M. Growth Factor Levels in Leukocyte-Poor Platelet-Rich Plasma and Correlations with Donor Age, Gender, and Platelets in the Japanese Population. J. Exp. Orthop. 2019, 6, 4. [Google Scholar] [CrossRef]
- Henschen, A. On the Structure of Functional Sites in Fibrinogen. Thromb. Res. 1983, 29, 27–39. [Google Scholar] [CrossRef]
- Mihalyi, E. Clotting of Bovine Fibrinogen. Calcium Binding to Fibrin during Clotting and Its Dependence on Release of Fibrinopeptide B. Biochemistry 1988, 27, 967–976. [Google Scholar] [CrossRef]
- Weisel, J.W. Fibrinogen and Fibrin. In Advances in Protein Chemistry; Elsevier: Amsterdam, The Netherlands, 2005; Volume 70, pp. 247–299. ISBN 978-0-12-034270-9. [Google Scholar]
- Sánchez, M.; Delgado, D.; Sánchez, P.; Fiz, N.; Azofra, J.; Orive, G.; Anitua, E.; Padilla, S. Platelet Rich Plasma and Knee Surgery. Biomed. Res. Int. 2014, 2014, 890630. [Google Scholar] [CrossRef]
- Ghouri, A.; Conaghan, P.G. Update on Novel Pharmacological Therapies for Osteoarthritis. Ther. Adv. Musculoskelet. Dis. 2019, 11, 1759720X19864492. [Google Scholar] [CrossRef]
- Flow-Cytometric Analysis of Platelet-Membrane Glycoprotein Expression and Platelet Activation—PubMed. Available online: https://pubmed.ncbi.nlm.nih.gov/15226548/ (accessed on 29 November 2022).
- Naranda, J.; Gradišnik, L.; Gorenjak, M.; Vogrin, M.; Maver, U. Isolation and Characterization of Human Articular Chondrocytes from Surgical Waste after Total Knee Arthroplasty (TKA). PeerJ 2017, 5, e3079. [Google Scholar] [CrossRef]
- Riss, T.L.; Moravec, R.A.; Niles, A.L.; Duellman, S.; Benink, H.A.; Worzella, T.J.; Minor, L. Cell Viability Assays. In Assay Guidance Manual; Markossian, S., Grossman, A., Brimacombe, K., Arkin, M., Auld, D., Austin, C., Baell, J., Chung, T.D.Y., Coussens, N.P., Dahlin, J.L., et al., Eds.; Eli Lilly & Company and the National Center for Advancing Translational Sciences: Bethesda, MD, USA, 2004. [Google Scholar]







Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mercader Ruiz, J.; Beitia, M.; Delgado, D.; Sánchez, P.; Arnaiz, M.J.; López de Dicastillo, L.; Benito-Lopez, F.; Basabe-Desmonts, L.; Sánchez, M. New Formulation of Platelet-Rich Plasma Enriched in Platelet and Extraplatelet Biomolecules Using Hydrogels. Int. J. Mol. Sci. 2023, 24, 13811. https://doi.org/10.3390/ijms241813811
Mercader Ruiz J, Beitia M, Delgado D, Sánchez P, Arnaiz MJ, López de Dicastillo L, Benito-Lopez F, Basabe-Desmonts L, Sánchez M. New Formulation of Platelet-Rich Plasma Enriched in Platelet and Extraplatelet Biomolecules Using Hydrogels. International Journal of Molecular Sciences. 2023; 24(18):13811. https://doi.org/10.3390/ijms241813811
Chicago/Turabian StyleMercader Ruiz, Jon, Maider Beitia, Diego Delgado, Pello Sánchez, María Jesús Arnaiz, Leonor López de Dicastillo, Fernando Benito-Lopez, Lourdes Basabe-Desmonts, and Mikel Sánchez. 2023. "New Formulation of Platelet-Rich Plasma Enriched in Platelet and Extraplatelet Biomolecules Using Hydrogels" International Journal of Molecular Sciences 24, no. 18: 13811. https://doi.org/10.3390/ijms241813811
APA StyleMercader Ruiz, J., Beitia, M., Delgado, D., Sánchez, P., Arnaiz, M. J., López de Dicastillo, L., Benito-Lopez, F., Basabe-Desmonts, L., & Sánchez, M. (2023). New Formulation of Platelet-Rich Plasma Enriched in Platelet and Extraplatelet Biomolecules Using Hydrogels. International Journal of Molecular Sciences, 24(18), 13811. https://doi.org/10.3390/ijms241813811








