Pulse Pressure Variation Can Predict the Hemodynamic Response to Pneumoperitoneum in Dogs: A Retrospective Study
Abstract
:1. Introduction
2. Materials and Methods
2.1. Anesthetic Protocol
2.2. Study Protocol
2.3. Statistical Analysis
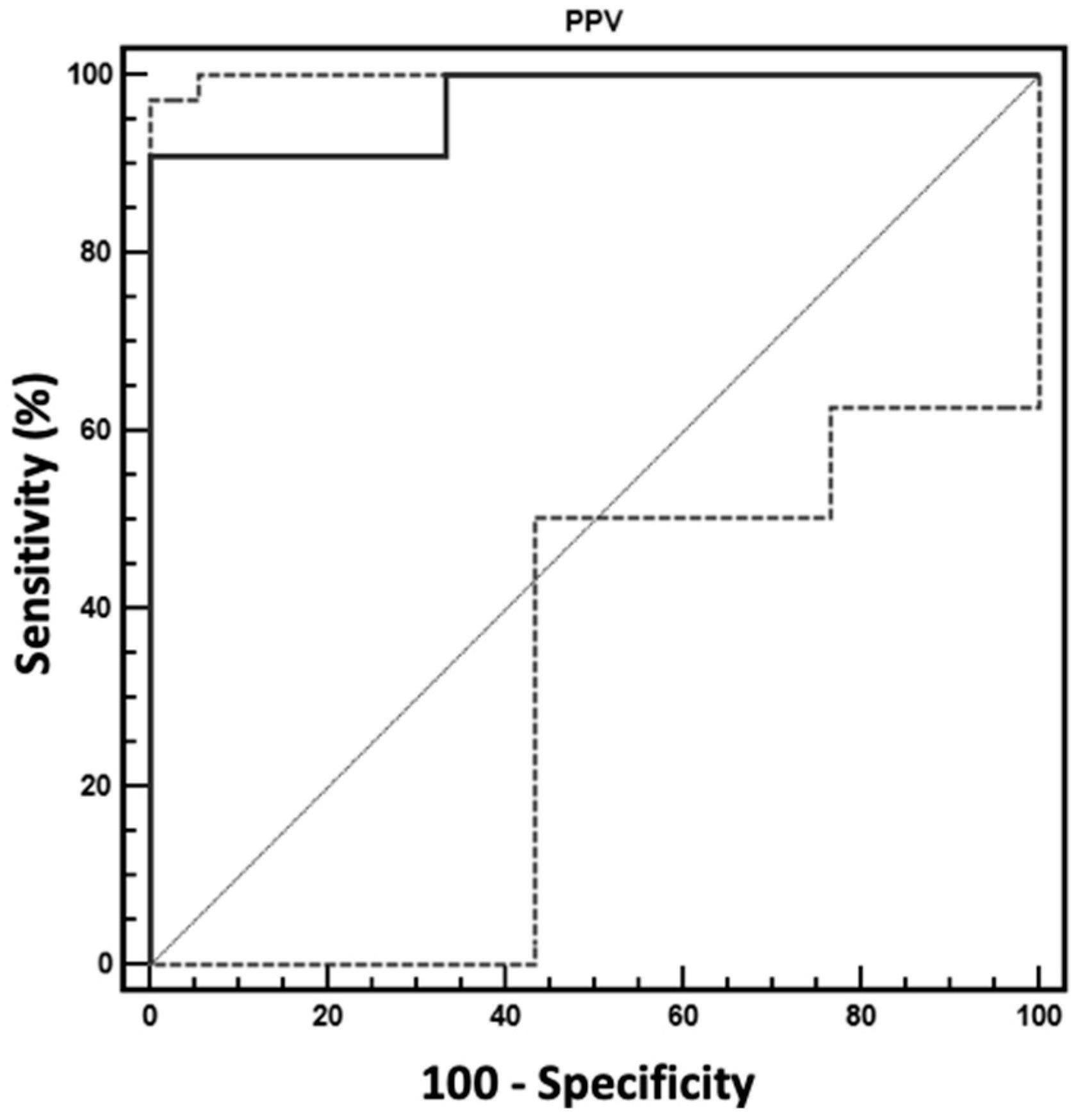
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Cheifetz, I.M. Cardiorespiratory interactions: The relationship between mechanical ventilation and hemodynamics. Respir. Care 2014, 59, 1937–1945. [Google Scholar] [CrossRef]
- Michard, F. Changes in arterial pressure during mechanical ventilation. Anesthesiology 2005, 103, 419–428. [Google Scholar] [CrossRef] [PubMed]
- Cannesson, M. Arterial pressure variation and goal-directed fluid therapy. J. Cardiothorac. Vasc. Anesth. 2010, 24, 487–497. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Du, B. Does pulse pressure variation predict fluid responsiveness in critically ill patients? A systematic review and meta-analysis. Crit. Care 2014, 18, 650. [Google Scholar] [CrossRef] [PubMed]
- Perel, A.; Pizov, R.; Cotev, S. Respiratory variations in the arterial pressure during mechanical ventilation reflect volume status and fluid responsiveness. Intensive Care Med. 2014, 40, 798–807. [Google Scholar] [CrossRef]
- Marik, P.E.; Cavallazzi, R.; Vasu, T.; Hirani, A. Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: A systematic review of the literature. Crit. Care Med. 2009, 37, 2642–2647. [Google Scholar] [CrossRef]
- Drozdzynska, M.J.; Chang, Y.M.; Stanzani, G.; Pelligand, L. Evaluation of the dynamic predictors of fluid responsiveness in dogs receiving goal-directed fluid therapy. Vet. Anaesth. Analg. 2018, 45, 22–30. [Google Scholar] [CrossRef] [PubMed]
- Berkenstadt, H.; Friedman, Z.; Preisman, S.; Keidan, I.; Livingstone, D.; Perel, A. Pulse pressure and stroke volume variations during severe haemorrhage in ventilated dogs. Br. J. Anaesth. 2005, 94, 721–726. [Google Scholar] [CrossRef] [Green Version]
- Sano, H.; Seo, J.; Wightman, P.; Cave, N.J.; Gieseg, M.A.; Johnson, C.B.; Chambers, P. Evaluation of pulse pressure variation and pleth variability index to predict fluid responsiveness in mechanically ventilated isoflurane-anesthetized dogs. J. Vet. Emerg. Crit. Care 2018, 28, 301–309. [Google Scholar] [CrossRef]
- Fantoni, D.T.; Ida, K.K.; Gimenes, A.M.; Mantovani, M.M.; Castro, J.R.; Patricio, G.C.F.; Ambrosio, A.M.; Otsuki, D.A. Pulse pressure variation as a guide for volume expansion in dogs undergoing orthopedic surgery. Vet. Anaesth. Analg. 2017, 44, 710–718. [Google Scholar] [CrossRef]
- Kashtan, J.; Green, J.F.; Parsons, E.Q.; Holcroft, J.W. Hemodynamic effect of increased abdominal pressure. J. Surg. Res. 1981, 30, 249–255. [Google Scholar] [CrossRef]
- Zuckerman, R.S.; Heneghan, S. The duration of hemodynamic depression during laparoscopic cholecystectomy. Surg. Endosc. 2002, 16, 1233–1236. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.; Zhu, S.; Ji, Q.; Li, W.; Liu, J. The impact of intra-abdominal pressure on the stroke volume variation and plethysmographic variability index in patients undergoing laparoscopic cholecystectomy. Biosci. Trends 2015, 9, 129–133. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Branche, P.E.; Duperret, S.L.; Sagnard, P.E.; Boulez, J.L.; Petit, P.L.; Viale, J.P. Left ventricular loading modifications induced by pneumoperitoneum: A time course echocardiographic study. Anesth. Analg. 1998, 86, 482–487. [Google Scholar] [CrossRef] [PubMed]
- Takata, M.; Wise, R.A.; Robotham, J.L. Effects of abdominal pressure on venous return: Abdominal vascular zone conditions. J. Appl. Physiol. 1990, 69, 1961–1972. [Google Scholar] [CrossRef] [PubMed]
- Briganti, A.; Evangelista, F.; Centonze, P.; Rizzo, A.; Bentivegna, F.; Crovace, A.; Staffieri, F. A preliminary study evaluating cardiac output measurement using Pressure Recording Analytical Method (PRAM) in anaesthetized dogs. BMC Vet. Res. 2018, 14, 72. [Google Scholar] [CrossRef]
- Struthers, A.D.; Cuschieri, A. Cardiovascular consequences of laparoscopic surgery. Lancet 1998, 352, 568–570. [Google Scholar] [CrossRef]
- Koivusalo, A.M.; Lindgren, L. Effects of carbon dioxide pneumoperitoneum for laparoscopic cholecystectomy. Acta Anaesthesiol. Scand. 2000, 44, 834–841. [Google Scholar] [CrossRef]
- Atkinson, T.M.; Giraud, G.D.; Togioka, B.M.; Jones, D.B.; Cigarroa, J.E. Cardiovascular and Ventilatory Consequences of Laparoscopic Surgery. Circulation 2017, 135, 700–710. [Google Scholar] [CrossRef]
- Ivankovich, A.D.; Miletich, D.J.; Albrecht, R.F.; Heyman, H.J.; Bonnet, R.F. Cardiovascular effects of intraperitoneal insufflation with carbon dioxide and nitrous oxide in the dog. Anesthesiology 1975, 42, 281–287. [Google Scholar] [CrossRef]
- Duke, T.; Steinacher, S.L.; Remedios, A.M. Cardiopulmonary effects of using carbon dioxide for laparoscopic surgery in dogs. Vet. Surg. 1996, 25, 77–82. [Google Scholar] [CrossRef] [PubMed]
- Dexter, S.P.; Vucevic, M.; Gibson, J.; McMahon, M.J. Hemodynamic consequences of high- and low-pressure capnoperitoneum during laparoscopic cholecystectomy. Surg. Endosc. 1999, 13, 376–381. [Google Scholar] [CrossRef] [PubMed]
- Safran, D.; Sgambati, S.; Orlando, R., 3rd. Laparoscopy in high-risk cardiac patients. Surg. Gynecol. Obstet. 1993, 176, 548–554. [Google Scholar] [CrossRef] [PubMed]
- Ho, H.S.; Saunders, C.J.; Corso, F.A.; Wolfe, B.M. The effects of CO2 pneumoperitoneum on hemodynamics in hemorrhaged animals. Surgery 1993, 114, 381–387, discussion 387–388. [Google Scholar] [PubMed]
| Dog | Phase | Breed | Age (Years) | HR (beats/min) | MAP (mmHg) | CI (L/min/m2) | PPV (%) | Crs (mL/cmH2O/kg) | Group |
|---|---|---|---|---|---|---|---|---|---|
| 1 | BASE | cocker spaniel | 2 | 87 | 98 | 2.9 | 21 | 0.9 | S |
| P10 | 86 | 117 | 1.1 | 11 | 0.8 | ||||
| 2 | BASE | mixed breed | 3 | 72 | 79 | 5.9 | 32 | 1.0 | S |
| P10 | 96 | 76 | 2.6 | 12 | 0.8 | ||||
| 3 | BASE | mixed breed | 3 | 75 | 79 | 2.2 | 18 | 1.6 | S |
| P10 | 84 | 128 | 1.4 | 7 | 0.9 | ||||
| 4 | BASE | bull terrier | 4 | 41 | 76 | 6.3 | 22 | 1.6 | S |
| P10 | 85 | 121 | 4.7 | 21 | 0.9 | ||||
| 5 | BASE | beagle | 4 | 108 | 64 | 6.5 | 13.6 | 2.1 | S |
| P10 | 109 | 89 | 4.5 | 18 | 0.6 | ||||
| 6 | BASE | beagle | 2 | 88 | 86 | 5.6 | 19 | 1 | S |
| P10 | 102 | 54 | 4.7 | 13 | 0.9 | ||||
| 7 | BASE | mixed breed | 4 | 116 | 76 | 2.7 | 20 | 1.1 | S |
| P10 | 131 | 59 | 1.6 | 7 | 1.1 | ||||
| 8 | BASE | boxer | 5 | 128 | 88 | 3.4 | 26 | 1.1 | S |
| P10 | 120 | 100 | 2.6 | 16 | 0.6 | ||||
| 9 | BASE | cocker spaniel | 2 | 72 | 75 | 3.6 | 33 | 1.8 | S |
| P10 | 83 | 82 | 2.3 | 12 | 0.9 | ||||
| 10 | BASE | mixed breed | 1 | 99 | 54 | 2.7 | 24 | 1.4 | S |
| P10 | 78 | 95 | 2.1 | 7.8 | 0.8 | ||||
| 11 | BASE | beagle | 4 | 71 | 81 | 5.3 | 18 | 1.9 | S |
| P10 | 71 | 91 | 4.6 | 12 | 0.7 | ||||
| 12 | BASE | mixed breed | 3 | 107 | 81 | 4.6 | 6.3 | 3.1 | NS |
| P10 | 101 | 87 | 4.4 | 5 | 1.1 | ||||
| 13 | BASE | cocker spaniel | 5 | 56 | 70 | 7.5 | 11 | 2.3 | NS |
| P10 | 80 | 99 | 7.6 | 10 | 1.3 | ||||
| 14 | BASE | mixed breed | 2 | 102 | 83 | 3.7 | 7.3 | 0.9 | NS |
| P10 | 73 | 74 | 4.1 | 10 | 0.5 | ||||
| 15 | BASE | mixed breed | 2 | 60 | 76 | 3.5 | 8.8 | 1.4 | NS |
| P10 | 91 | 96 | 4.6 | 7 | 1.2 | ||||
| 16 | BASE | beagle | 5 | 84 | 80 | 3.2 | 14 | 1.9 | NS |
| P10 | 90 | 101 | 3.7 | 9 | 1.2 | ||||
| 17 | BASE | bull terrier | 4 | 67 | 68 | 4.7 | 14 | 1.3 | NS |
| P10 | 89 | 100 | 5.7 | 9 | 1 | ||||
| 18 | BASE | boxer | 6 | 97 | 70 | 3.6 | 9 | 1.4 | NS |
| P10 | 89 | 95 | 3.3 | 14 | 1.4 | ||||
| 19 | BASE | mixed breed | 3 | 76 | 70 | 4.2 | 11 | 1.6 | NS |
| P10 | 102 | 76 | 4.4 | 9 | 1.3 | ||||
| 20 | BASE | mixed breed | 2 | 91 | 83 | 2.8 | 16 | 1.7 | NS |
| P10 | 76 | 96 | 2.6 | 7 | 1.1 |
| Parameter | BASE | P10 | p Value |
|---|---|---|---|
| HR (beats/min) | 84.8 ± 21.6 | 91.8 ± 15.4 | 0.111 |
| MV (L/min/kg) | 0.17 ± 0.03 | 0.19 ± 0.04 | 0.127 |
| MAP (mmHg) | 76.8 ± 9.4 | 91.8 ± 18.5 | 0.003 * |
| CI (L/min/m2) | 4.28 ± 1.4 | 3.67 ± 1.6 | 0.019 * |
| SVR (dyn*sec/cm5) | 3117 ± 1485 | 3003 ± 1341 | 0.775 |
| PPV (%) | 17.2 ± 7.6 | 11.1 ± 4.0 | 0.001* |
| EtCO2 (mmHg) | 45.9 ± 4.9 | 52.6 ± 7.4 | 0.067 |
| SpO2 (%) | 98.2 ± 1.1 | 97.6 ± 1.4 | 0.765 |
| Crs (mL/cmH2O/kg) | 1.6 ± 0.6 | 0.9 ± 0.2 | 0.001 * |
| Ppeak (cmH2O) | 8.9 ± 1.8 | 12.3 ± 2.9 | 0.001 * |
| Pplat (cmH2O) | 8.7 ± 1.8 | 11.6 ± 2.3 | 0.001 * |
| Parameter | Phase | S Group | NO-S Group | p Value |
|---|---|---|---|---|
| HR (beats/min) | BASE | 86.4 ± 25.1 | 81.1 ± 20.1 | 0.601 |
| P10 | 96.1 ± 26.8 | 94.1 ± 12.5 | 0.822 | |
| MAP (mmHg) | BASE | 77.9 ± 11.6 | 74.6 ± 6.8 | 0.471 |
| P10 | 89.1 ± 27.1 | 92.1 ± 7.4 | 0.742 | |
| CI (L/m2) | BASE | 4.32 ± 1.62 | 4.22 ± 1.38 | 0.88 |
| P10 | 2.97 ± 1.4 # | 4.51 ± 1.41 | 0.02 * | |
| SVR (dyn*sec/cm5) | BASE | 3081 ± 1007 | 3160 ± 1991 | 0.902 |
| P10 | 3573 ± 1245 | 2305 ±1138 | 0.032 * | |
| EtCO2 | BASE | 46.2 ± 5.24 | 43.2 ± 7.2 | 0.602 |
| P10 | 50.1 ± 7.32 | 48.2 ±5.6 | 0.732 | |
| PPV (%) | BASE | 22.4 ± 6.1 | 10.9 ± 3.3 | 0.000 * |
| P10 | 12.6 ± 4.3 # | 9.1 ± 2.5 | 0.05 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Bella, C.; Lacitignola, L.; Fracassi, L.; Skouropoulou, D.; Crovace, A.; Staffieri, F. Pulse Pressure Variation Can Predict the Hemodynamic Response to Pneumoperitoneum in Dogs: A Retrospective Study. Vet. Sci. 2019, 6, 17. https://doi.org/10.3390/vetsci6010017
Di Bella C, Lacitignola L, Fracassi L, Skouropoulou D, Crovace A, Staffieri F. Pulse Pressure Variation Can Predict the Hemodynamic Response to Pneumoperitoneum in Dogs: A Retrospective Study. Veterinary Sciences. 2019; 6(1):17. https://doi.org/10.3390/vetsci6010017
Chicago/Turabian StyleDi Bella, Caterina, Luca Lacitignola, Laura Fracassi, Despoina Skouropoulou, Antonio Crovace, and Francesco Staffieri. 2019. "Pulse Pressure Variation Can Predict the Hemodynamic Response to Pneumoperitoneum in Dogs: A Retrospective Study" Veterinary Sciences 6, no. 1: 17. https://doi.org/10.3390/vetsci6010017
APA StyleDi Bella, C., Lacitignola, L., Fracassi, L., Skouropoulou, D., Crovace, A., & Staffieri, F. (2019). Pulse Pressure Variation Can Predict the Hemodynamic Response to Pneumoperitoneum in Dogs: A Retrospective Study. Veterinary Sciences, 6(1), 17. https://doi.org/10.3390/vetsci6010017







