Diagnosis and Management of UTI in Primary Care Settings—A Qualitative Study to Inform a Diagnostic Quick Reference Tool for Women Under 65 Years
Abstract
Strengths and limitations of this study:
|
1. Introduction
- Determine the practices of primary health care staff when diagnosing and treating UTIs in patients under 65 years in the primary health care setting,
- identify where there are current barriers and facilitators to appropriate diagnosis and treatment, and
- identify how these gaps may be addressed through resource development or other measures.
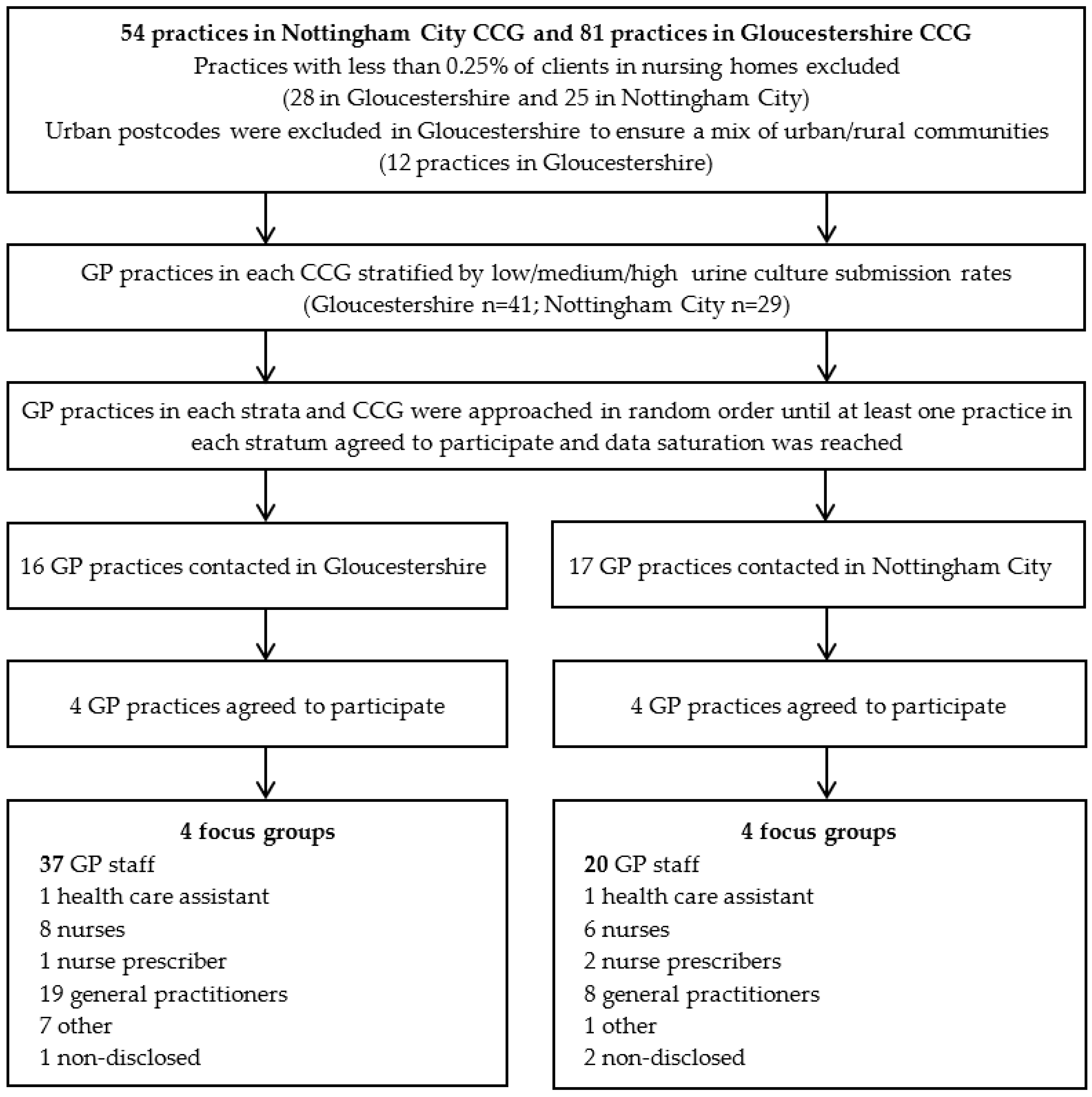
2. Methods
3. Consultations
3.1. Role and Professional Identity
3.2. Role and Professional Identity/Environmental Context and Resources
3.3. Diagnosis
3.3.1. Skills
3.3.2. Role and Professional Identity/Social Influence
3.3.3. Environment Context and Resources
3.3.4. Beliefs about Consequences/Environmental Context and Resources
3.4. Medical Management
3.4.1. Environmental Context and Resources
3.4.2. Reinforcement
3.4.3. Memory, Attention, and Decision Making/Social Influence/Optimism
3.4.4. Beliefs about Consequences/Memory, Attention and Decision Making/Knowledge
3.4.5. Social Influence/Memory, Attention and Decision Making
3.4.6. Knowledge
3.4.7. Behavioural Regulation
3.5. Self-Care and Prevention
3.5.1. Skills/Knowledge
3.5.2. Social Influence/Environmental Context and Resources
4. Discussion
4.1. Other Studies
4.2. Limitations and Strengths
5. Conclusions
6. Ethical Approval
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Laboratory Surveillance of Polymicrobial Bacteraemia and Fungaemia in England, Wales and Northern Ireland: 2017; Public Health England: London, UK, 2018.
- Abernethy, J.; Guy, R.; Sheridan, E.A.; Hopkins, S.; Kiernan, M.; Wilcox, M.H.; Johnson, A.P.; Hope, R.; the E. coli bacteraemia sentinel surveillance group. Epidemiology of Escherichia coli bacteraemia in England: Results of an enhanced sentinel surveillance programme. J. Hosp. Infect. 2017, 95, 365–375. [Google Scholar] [CrossRef]
- English Surveillance Programme for Antimicrobial Utilisation and Resistance (ESPAUR) 2018–2019; Public Health England: London, UK, 2019.
- Bhattacharya, A.; Nsonwu, O.; Johnson, A.P.; Hope, R. Estimating the incidence and 30-day all-cause mortality rate of Escherichia coli bacteraemia in England by 2020/21. J. Hosp. Infect. 2018, 98, 228–231. [Google Scholar] [CrossRef]
- Abernethy, J.K.; Johnson, A.P.; Guy, R.; Hinton, N.; Sheridan, E.A.; Hope, R.J. Thirty day all-cause mortality in patients with Escherichia coli bacteraemia in England. Clin. Microbiol. Infect. 2015, 21, 251.e1–251.e8. [Google Scholar] [CrossRef]
- Gray, J. Epidemiology of Escherichia coli bloodstream infections in children. J. Hosp. Infect. 2017, 95, 383–384. [Google Scholar] [CrossRef] [PubMed]
- Oppenheim, B. Escherichia coli bacteraemia papers. J. Hosp. Infect. 2017, 95, 363–364. [Google Scholar] [CrossRef]
- Laupland, K.B.; Gregson, D.B.; Church, D.L.; Ross, T.; Pitout, J.D. Incidence, risk factors and outcomes of Escherichia coli bloodstream infections in a large Canadian region. Clin. Microbiol. Infect. 2008, 14, 1041–1047. [Google Scholar] [CrossRef] [PubMed]
- Lishman, H.; Costelloe, C.; Hopkins, S.; Johnson, A.P.; Hope, R.; Guy, R.; Muller-Pebody, B.; Holmes, A.; Aylin, P. Exploring the relationship between primary care antibiotic prescribing for urinary tract infections, Escherichia coli bacteraemia incidence and antimicrobial resistance: An ecological study. Int. J. Antimicrob. Agents 2018, 52, 790–798. [Google Scholar] [CrossRef] [PubMed]
- McNulty, C.A. European Antibiotic Awareness Day 2012: General practitioners encouraged to TARGET antibiotics through guidance, education and tools. J. Antimicrob. Chemother. 2012, 67, 2543–2546. [Google Scholar] [CrossRef]
- Balinskaite, V.; Johnson, A.P.; Holmes, A.; Aylin, P. The Impact of a National Antimicrobial Stewardship Program on Antibiotic Prescribing in Primary Care: An Interrupted Time Series Analysis. Clin. Infect. Dis. 2019, 69, 227–232. [Google Scholar] [CrossRef]
- Dolk, F.C.K.; Pouwels, K.B.; Smith, D.R.M.; Robotham, J.V.; Smieszek, T. Antibiotics in primary care in England: Which antibiotics are prescribed and for which conditions? J. Antimicrob. Chemother. 2018, 73, ii2–ii10. [Google Scholar] [CrossRef]
- English Surveillance Programme for Antimicrobial Utilisation and Resistance (ESPAUR) 2010 to 2014; Public Health England: London, UK, 2015.
- Croker, R.; Walker, A.J.; Goldacre, B. Why did some practices not implement new antibiotic prescribing guidelines on urinary tract infection? A cohort study and survey in NHS England primary care. J. Antimicrob. Chemother. 2019, 74, 1125–1132. [Google Scholar] [CrossRef] [PubMed]
- Public Health England. Diagnosis of Urinary Tract Infections: Quick Reference Tool for Primary Care. 2018. Available online: https://www.gov.uk/government/publications/urinary-tract-infection-diagnosis. (accessed on 6 June 2020).
- 2011 Census Aggregate Data. Available online: https://www.ons.gov.uk/ (accessed on 6 June 2020).
- Clinical Commissioning Group Population Estimates (National Statistics). Available online: https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/datasets/clinicalcommissioninggroupmidyearpopulationestimates (accessed on 7 July 2020).
- District Profile-Nottingham City. Available online: https://www.nottinghaminsight.org.uk/document-library/district-profile-nottingham-city/ (accessed on 7 July 2020).
- Population Profile: Gloucestershire County Council. 2019. Available online: https://www.gloucestershire.gov.uk/media/12777/equality-profile-2019-final.pdf (accessed on 7 July 2020).
- Public Health England. Gloucestershire County Health Profile. 2017. Available online: https://www.gloucestershireccg.nhs.uk/wp-content/uploads/2018/03/Health-Profile-2017.pdf (accessed on 7 July 2020).
- Cane, J.; O’Connor, D.; Michie, S. Validation of the theoretical domains framework for use in behaviour change and implementation research. Implement. Sci. 2012, 7, 37. [Google Scholar] [CrossRef] [PubMed]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- NVivo Qualitative Data Analysis Software; QSR International Pty Ltd.: Doncaster, Australia, 2012.
- Jones, L.F.; Cooper, E.; Joseph, A.; Allison, R.; Gold, N.; Donald, I.; McNulty, C. Development of an information leaflet and diagnostic flow chart to improve the management of urinary tract infections in older adults: A qualitative study using the Theoretical Domains Framework. BJGP Open 2020. [Google Scholar] [CrossRef] [PubMed]
- Barry, H.C.; Hickner, J.; Ebell, M.H.; Ettenhofer, T. A Randomized Controlled Trial of Telephone Management of Suspected Urinary Tract Infections in Women. J. Fam. Pract. 2001, 50, 589–594. [Google Scholar]
- Schauberger, C.; Merkitch, K.; Prell, A. Acute cystitis in women: Experience with a telephone-based algorithm. Wis. Med. J. 2007, 106, 326–329. [Google Scholar]
- Rastogi, R.; Martinez, K.A.; Gupta, N.; Rood, M.; Rothberg, M.B. Management of Urinary Tract Infections in Direct to Consumer Telemedicine. J. Gen. Intern. Med. 2020, 35, 643–648. [Google Scholar] [CrossRef]
- Millions of Patients Benefiting from Remote Consultations as Family Doctors Respond to COVID-19. Available online: https://www.england.nhs.uk/2020/05/millions-of-patients-benefiting-from-remote-consultations-as-family-doctors-respond-to-covid-19/ (accessed on 27 June 2020).
- NHS. The NHS Long Term Plan; NHS: Leeds, UK, January 2019. Available online: https://www.longtermplan.nhs.uk/wp-content/uploads/2019/08/nhs-long-term-plan-version-1.2.pdf (accessed on 9 June 2020).
- Little, P.; Turner, S.; Rumsby, K.; Warner, G.; Moore, M.; Lowes, J.A.; Smith, H.; Hawke, C.; Turner, D.; Leydon, G.M.; et al. Dipsticks and diagnostic algorithms in urinary tract infection: Development and validation, randomised trial, economic analysis, observational cohort and qualitative study. Health Technol. Assess. 2009, 13, 1–73. [Google Scholar] [CrossRef]
- Giesen, L.G.; Cousins, G.; Dimitrov, B.D.; van de Laar, F.A.; Fahey, T. Predicting acute uncomplicated urinary tract infection in women: A systematic review of the diagnostic accuracy of symptoms and signs. BMC Fam. Pract. 2010, 11, 78. [Google Scholar] [CrossRef]
- Fenwick, E.A.; Briggs, A.H.; Hawke, C.I. Management of urinary tract infection in general practice: A cost-effectiveness analysis. Br. J. Gen. Pract. 2000, 50, 635–639. [Google Scholar]
- McIsaac, W.J.; Moineddin, R.; Ross, S. Validation of a Decision Aid to Assist Physicians in Reducing Unnecessary Antibiotic Drug Use for Acute Cystitis. Arch. Intern. Med. 2007, 167, 2201–2206. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Little, P.; Turner, S.; Rumsby, K.; Jones, R.; Warner, G.; Moore, M.; Lowes, J.A.; Smith, H.; Hawke, C.; Leydon, G.; et al. Validating the prediction of lower urinary tract infection in primary care: Sensitivity and specificity of urinary dipsticks and clinical scores in women. Br. J. Gen. Pract. 2010, 60, 495–500. [Google Scholar] [CrossRef]
- Royal College of General Practitioners. TARGET UTI Resource Suite: Uncomplicated UTI Audit for Women Under 65. Available online: https://www.rcgp.org.uk/clinical-and-research/resources/toolkits/amr/target-antibiotics-toolkit/uti-resource-suite.aspx (accessed on 9 July 2020).
- Ivers, N.; Jamtvedt, G.; Flottorp, S.; Young, J.M.; Odgaard-Jensen, J.; French, S.D.; O’Brien, M.A.; Johansen, M.; Grimshaw, J.; Oxman, A.D. Audit and feedback: Effects on professional practice and healthcare outcomes. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef] [PubMed]
- Kronenberg, A.; Butikofer, L.; Odutayo, A.; Muhlemann, K.; da Costa, B.R.; Battaglia, M.; Meli, D.N.; Frey, P.; Limacher, A.; Reichenbach, S.; et al. Symptomatic treatment of uncomplicated lower urinary tract infections in the ambulatory setting: Randomised, double blind trial. BMJ 2017, 359, j4784. [Google Scholar] [CrossRef]
- Lecky, D.M.; Howdle, J.; Butler, C.C.; McNulty, C.A. Optimising management of UTIs in primary care: A qualitative study of patient and GP perspectives to inform the development of an evidence-based, shared decision-making resource. Br. J. Gen. Pract. 2020, 70, e330–e338. [Google Scholar] [CrossRef]
- Little, P.; Moore, M.V.; Turner, S.; Rumsby, K.; Warner, G.; Lowes, J.A.; Smith, H.; Hawke, C.; Leydon, G.; Arscott, A.; et al. Effectiveness of five different approaches in management of urinary tract infection: Randomised controlled trial. BMJ 2010, 340, c199. [Google Scholar] [CrossRef] [PubMed]
- Urinary Tract Infection (Lower): Antimicrobial Prescribing; National Institute for Health and Care Excellence: London, UK, 2018.
- Larcombe, J.H. Urinary Tract Infection in Women Aged 18–64: Doctors’, Patients’, and Lay Perceptions and Understandings. Ph.D. Thesis, Durham University, Durham, UK, 2012. [Google Scholar]
- Butler, C.C.; Francis, N.A.; Thomas-Jones, E.; Longo, M.; Wootton, M.; Llor, C.; Little, P.; Moore, M.; Bates, J.; Pickles, T.; et al. Point-of-care urine culture for managing urinary tract infection in primary care: A randomised controlled trial of clinical and cost-effectiveness. Br. J. Gen. Pract. 2018, 68, e268–e278. [Google Scholar] [CrossRef]
- Urinary Tract Infection (Recurrent): Antimicrobial Prescribing; National Institute for Health and Care Excellence: London, UK, 2018.
- Hooton, T.M.; Vecchio, M.; Iroz, A.; Tack, I.; Dornic, Q.; Seksek, I.; Lotan, Y. Effect of Increased Daily Water Intake in Premenopausal Women with Recurrent Urinary Tract Infections: A Randomized Clinical Trial. JAMA Intern. Med. 2018, 178, 1509–1515. [Google Scholar] [CrossRef]
- Duane, S.; Domegan, C.; Callan, A.; Galvin, S.; Cormican, M.; Bennett, K.; Murphy, A.W.; Vellinga, A. Using qualitative insights to change practice: Exploring the culture of antibiotic prescribing and consumption for urinary tract infections. BMJ Open 2016, 6, e008894. [Google Scholar] [CrossRef]
- Bjorkman, I.; Berg, J.; Viberg, N.; Stalsby Lundborg, C. Awareness of antibiotic resistance and antibiotic prescribing in UTI treatment: A qualitative study among primary care physicians in Sweden. Scand. J. Prim. Health Care 2013, 31, 50–55. [Google Scholar] [CrossRef]
- NHS Digital. Patients Registered at a GP Practice—December 2018. Available online: https://digital.nhs.uk/data-and-information/publications/statistical/patients-registered-at-a-gp-practice/december-2018 (accessed on 3 September 2020).
| Indicators (2017/18) | Nottingham City CCG | Gloucestershire CCG | English Level Statistic |
|---|---|---|---|
| Total Population Estimates—mid 2018 [17] | 331,069 | 633,558 | 55,977,178 |
| Healthy life expectancy at birth for women in years | 53.5 [18] | 65.7 [19] | 63.8 [18] |
| Life expectancy gap for women in years | 8.6 [18] | 5.4 [20] | 7.5 [18] |
| % of all people with a limiting long-term illness | 18.1 [18] | 16.7 [19] | 17.6 [18] |
| % of all people who are black and ethnic minority (2011 census) [16] | 34.7 | 4.6 | 14.6 |
| Deprivation score | 36.9 [18] | 15.0 [19] | 21.8 [19] |
| Sections within the Interview Schedule | Main Domains Explored in the TDF |
|---|---|
| Section One: Current UTI Management | |
| Knowledge/skills/social professional role and identity |
| Environmental context and resources/beliefs about capabilities |
| Knowledge/skills/beliefs about consequences |
| Memory, attention and decision making/beliefs about consequences/social influence/beliefs about capabilities |
| Memory, attention and decision making/social influence |
| Behavioural regulation/social professional role and identity |
| Environmental context and resources/reinforcement |
| Environmental context and resources/social influences/emotions |
| Skill/intentions/goals |
| Memory, attention and decision making/beliefs about consequences/behavioural regulation |
| Knowledge/skills/beliefs about consequences/intentions |
| Optimism/social professional role and identity/motivation/goals |
| Section Two: Ways we could reduce UTIs or improve UTI management | |
| Environmental context and resources/behavioural regulation/reinforcement |
| Skills/environmental context and resources |
| Section Three: How a UTI resource might be used to improve diagnosis and treatment (corresponds with a step by step review of the previous or updated UTI diagnostic resources) | |
| Knowledge/memory, attention and decision making/skills |
| Environmental context and resources/memory, attention and decision making/beliefs about capabilities |
| Knowledge/memory, attention and decision making/skills |
| Environmental context and resources |
| Beliefs about capabilities/reinforcement |
| Domain and Findings * | Quote(F Stands for Female, M for Male, Int Stands for Interviewer and GP Stands for General Practice) | How the Findings Influenced the UTI Diagnostic Tool |
| Knowledge | ||
| Some general practice staff reported that they did not know about pivmecillinam or fosfomycin as second-line treatment for acute uncomplicated UTI. | “F1: I’ve never even heard of it before (pivmecillinam). What’s it called…? F3: Not seen it at all. M1: I’ve not seen that at all.” (GP 8) |
The updated diagnostic tool:
|
| GP practices discussed frequent/recent use of antibiotics, long duration/high doses of antibiotics, recurrent UTI, and positive lab results as risk factors for antibiotic resistance. | “Certainly, the people coming back, recurrent UTIs… you sometimes think are we actually missing something here are they having proper UTI, the dipstick might show it but actually having an MSU with a proven UTI can help in the long term, so that’s one group.” (GP 5) | |
| Practice suggestions for prevention of UTI focused on hydration, sachets/cranberry products, lemon barley water, and wiping front to back. | “M1: Occasionally Cystopurin. F1: …the sachets. Especially if the dipstick’s negative. M1: I’d even recommended sodium bicarbonate… F2: It used to be barley water in my day…. F3: Basically just get as much fluid down you as you can and flush it out.” (GP 6) | |
| Some GP staff discussed conflicting information regarding the use of cystitis sachets and cranberry products for prevention or treatment of UTIs. | “Cranberry juice seems to have fallen out of fashion. The wording… in the guidance now… is that cranberry juice is effective for some women, but there is very limited research to back it up. the impression that we get is that the reason why cranberry juice is working is because they’re drinking a lot of fluid.” (GP 1) | |
| Environmental context and resources | ||
| Some GP staff reported that phone consultations (sometimes with dipstick results) are being used to assess and treat patients at risk for a UTI. | “…we ask them relevant questions, how long they’ve had the symptoms for, have they tried any over the counter, what are their symptoms, whether it’s dysuria, frequency, back pain, temperature, nausea, vomiting, that sort of thing, and it depends on the answers… particularly at our surgery, if they’re under 65, we just, they give them a prescription over the phone.” (GP 1) |
The updated diagnostic tool:
|
| Some groups reported that they would prescribe antibiotics over the phone for a patient under the age of 65 with 2–3 urinary symptoms. | ||
| At the telephone consultation, some practice staff asked for a urine sample to be brought in but others considered this as unnecessary. | “Int: how would you diagnose a suspected UTI over the phone versus in face to face consultation? F1: Well just do the same but not examine them or dip it… we tend to not ask for a sample unless there was something complicated about them.” (GP 3) | |
| Some practice staff reported that patients ‘drop and run’, leaving urine samples at reception, often because they think they might have a UTI. Clinicians then ring the patient for a clinical history. | “M1: …we do end up with patients just turning up and leaving urine samples at the desk. Int: So what determines whether they get sent for culture? M1: Well, well they get dipped but then we want to know a bit more of the clinical information so… the nurses comes and says, I’ve checked this urine. We need a bit more than that… I think commonly we’d just end up phoning the patient and saying look… why have you dropped it off?” (GP 2) | |
| Some GP staff feel that easy availability of urine samples influences their decision to use urine dipsticks as part of the diagnostic process. | “…think for the vast majority we would test… even in females under 65 who… you certainly don’t need to send a culture for but if a urine is easily obtainable we’d normally get one.” (GP 2) | |
| Most GP staff followed 2017 PHE guidance for UTI diagnosis and which focused on the key symptoms of dysuria, urgency and frequency as symptoms and would not include findings from the most recent literature. | “…and I use the current guidance to decide whether to treat without dipping the urine or to just go ahead and treat. And I think it’s if they have three symptoms, that you don’t have to dip the urine and you just treat. If they’re under 65 and they’re a woman then I would tend to use that….” (GP 2) | |
| Most GP staff agreed that the exclusion of pyelonephritis and sepsis needed to be included in tools that are developed to diagnose UTI. | “I think sepsis has to be first, doesn’t it? It’s the trump card, is it?” (GP 4)“…and obviously, you’ve got to think about sepsis now.” (GP 6) | |
| Some GP staff expressed the need for more national guidance specific to the management of UTIs. | “…something on recurrent UTI would be really helpful because… some guidance… just sort of says consider this, consider that… there’s a lot more interpretation with recurrent UTI.” (GP 2) | |
| Some GP staff reported that lab specimen service pickups were not frequent enough to allow culture results to inform treatment, which leads to overcautious prescribing. | “…I’m going to treat because I won’t get the result of this MSU, this is a Thursday I’m not going to get it till Tuesday so we tend to treat.” (GP 7) | |
| Some GP staff reported that they did not have the option of using fosfomycin or pivmecillinam as second-line treatment. | “F1: But they didn’t actually have fosfomycin or pivmecillinam on the (sensitivity reporting) list. M1: No they don’t have fosfomycin….” (GP 2) | |
| Most GP staff indicated that more information or education for patients on UTI was needed, including a UTI leaflet and public health information/campaign that covers the prevention and treatment of UTI in line with national guidance. | “…like with coughs and colds everyone knows now that they’re not going to get an antibiotic necessarily, they’ve braced themselves for the bad news, haven’t they? But with UTI they wee once and it stings and… they separate it and somehow it doesn’t go under that hurt. It’s literally they’re right in, aren’t they, really quickly.” (GP 8) | |
| Role and professional identity | ||
| Some GP staff reported that receptionists in some surgeries ask patients who ring up to bring urine samples into the surgery and provide guidance on sample collection. | “The receptionists actually, if anybody rings up and says, I think I’ve got a UTI they, they say can you, next time you go can you make sure you keep a clean catch? So that we’ve already started a process of looking at having a… dip if needs be.” (GP 2) |
The updated diagnostic tool:
|
| Some GP staff reported that nurses may be responsible for testing urine samples left at reception and referring to clinicians if they are concerned the patient has a UTI. | “…often, they’ve already had a urine dipped by our nurses by the time that they get to us…. If the other nurses see someone and they’re suspecting a UTI they’ll… ask us to prescribe, but they’ll tell us what they’ve found, examination wise and history. So run it by us.” (GP 2) | |
| Some GP staff reported that nurse prescribers frequently see uncomplicated cases of UTI independently. | “…I (nurse prescriber) deal predominantly in the triage and assessment of acute illnesses and UTIs being probably quite an awful lot of it and it’s part of a team where we prescribe quite regularly for it following national guidelines.” (GP 8) | |
| Some GP staff reported that general practitioners will deal with UTIs but often focus on complicated cases or treatment failures. | “I tend to be seeing people who either they’ve got complicated features or they’ve had treatment already, or there’s something else…. I do quite a bit of telephone work, advice work.” (GP 1) | |
| Skills | ||
| Some GP staff asked about vaginal discharge during a consultation, and one group reported this was done after using a urine dipstick to rule out a UTI. | “…you ask for certain symptoms… if it sounds like a UTI and it seems like a UTI on a dipstick you treat as such. It would only be if you weren’t sure, if you needed to think about other symptoms then you would say have you got a vaginal discharge.” (GP 7) | The updated diagnostic tool:
|
| Most groups said they would send a culture following treatment failure or for a recurrent UTI but only some groups reported sending a urine for culture if the dipstick was negative but the patient symptomatic, if the patient was quite unwell, for male patients, pregnant women and for children. | “…I don’t use an age cut off. It’s more around their past history, for instance if they’re pregnant or something. Or if their symptoms aren’t very clear cut, or if they’re unwell or they’ve had recurrent then I will send off…. If it’s a treatment failure or they come back and their symptoms aren’t fully cleared up, second time round, then certainly we’d send it off at, on the second appointment if, if needed, if they come back...” (GP 3) | |
| Some groups indicated that they would not send a urine culture if the dipstick was negative or if the symptoms clearly indicated an uncomplicated UTI. | “With different things depending on the patient. So a pregnant or recurrent or, we’re more likely to send a urine off. We don’t send them off if it’s an uncomplicated UTI with typical symptoms.” (GP 3) | |
| Most GP staff reported discussing non-medical advice with their patients. This was in the context of self-care for mild symptoms (especially with a negative dipstick), or preventing UTI recurrence. | “Yeah, but if they’ve got relatively mild symptoms or few symptoms you can let them carry on flushing it out…” (GP 2) | |
| Some GP staff reported differences of opinion on interpretation/use of urine dipstick; especially when symptoms do not match urine dipstick results which challenge UTI diagnosis. | “…people with recurrent symptoms… doesn’t always match up the symptoms that they have with the findings in their urine and possibly their expectation for treatment.” (GP 2) | |
| Social Influence | ||
| Some GP staff feel that patient expectation influences their decision to use urine dipsticks as part of the diagnostic process. | “…if they’re young, fit, well, uncomplicated and got typical symptoms, technically you don’t need to do a dipstick. But you often still do it because the patients have that expectation because they want to be told this is definitely a urine infection. If you just say, you’ve got typical symptoms here are antibiotics, they still feel as though they want to be told this is an infection, so they will ask for it to be dipped or expect it to be dipped.” (GP 3) |
The updated diagnostic tool:
|
| Some practices generally felt that patients did not understand that a UTI can clear on its own safely and expected treatment and believe that patients react differently to a no antibiotic decision with respiratory infections due to more consistent messaging/campaigns in this area. | “Almost never, usually, if it’s for something like a sore throat or what have you, then… they’re getting more receptive, because it’s been a consistent message that they’re not going to get antibiotics unless X, Y, Z, but in urinary tract infections almost never, they just want them.” (GP 4) | |
| Some practices talked about how patients might obtain cystitis sachets from the community pharmacy and will only come for a consultation if symptoms don’t improve. | “…because we do get patients who have been to the pharmacist and I don’t see the ones who don’t come back, but I do see the ones who do, and… after week later they’re now going their urine is painful and they need antibiotics….” (GP 5) | |
| Beliefs about consequences | ||
| Some GP practices indicated that concern about issues like sepsis causes them to be overly cautious when diagnosing and treating UTIs. | “…it’s confidence around knowing… what happens if we don’t treat it, there is that risk or pyelonephritis and becoming septic… because of this lack of confidence we’ve always treated UTIs so I think it’s a number of different factors that apply.” (GP 7) |
The updated diagnostic tool:
|
| Most GP staff would not usually use a delayed/back-up prescription for UTIs. | “Usually not so much UTIs because by then they’ve already had the symptoms they’re coming in and they’re symptomatic, whereas a lot of people with sore throats come in and say it started yesterday. So, you can give them delayed, but I’m sure the percentage that cash in a delayed prescription is a lot higher” (GP 7) | |
| Most groups reported that they would discuss antibiotic resistance with some patients with an expected UTI, especially if there were additional risk factors. | “Occasionally, gradually, particularly if they’ve got a recurrent UTI or if they’ve had, say, side effects following antibiotics previously, like thrush. Then you might have a conversation about the pros and cons.” (GP 3) | |
| Hydration was discussed by most groups as a way to “flush out” the bladder/infection and was seen by some as the reason that cranberry juice is effective. | “Basically, just get as much fluid down you as you can and flush it out. Because if the urine analysis is negative each time, …that’s all you can advise them.” (GP 6) | |
| Beliefs about Capabilities | ||
| Though most practice staff used national guidance to manage UTIs, some would not refer to it every time. | “I intermittently look at the guideline and make sure what I think and I’m doing is correct, and then invariably I look and realise what I think I’m supposed to be doing is slightly changed over the couple of months since I last read it.” (GP 2) |
The updated diagnostic tool:
|
| Memory, Attention, and Decision Making | ||
| Some GP staff believe that 3 day courses of antibiotics were not sufficient. This was driven by patient expectations and perceived efficacy of the dose and pressured them to lengthen the dose or use a different antibiotic. | “M1: …I still find it quite hard to prescribe in three days, (some agreement) because patients don’t like three days. M2: They don’t do they, they don’t think it’s worth it… M3: They do not think that you’re giving them enough and that’s quite tricky I think, I still find that, trying to convince them that three days will be enough.” (GP 7) “I never find that three days of antibiotic works. I get so many people coming back (with UTI symptoms) that I don’t prescribe three days any more actually.” (GP 3) | The updated diagnostic tool:
|
| Some GP staff would delay antibiotics when waiting for results from urine culture if symptoms were mild. | “It depends on the day of the week, so if it’s a Thursday and the results aren’t going to come back, I might give them a prescription and say let me send it, if you get worse whilst you’re waiting for the results, that’s the context that I would do that.” (GP 3) | |
| Some GP staff would discuss completing the antibiotic course but were less inclined to discuss antibiotic resistance in relationship to UTIs than other infections, especially if they were confident in their diagnosis. | “I think it also depends on how convinced I am they’ve got a wee infection. So, if I’m convinced they’ve got a wee infection, and they’re quite systemically unwell with it, then I may not fight trying to give them the antibiotics as much as I might do if they’re going: I’ve had a bit of dysuria and I don’t know quite what’s going on.” (GP 4) | |
| Various factors that would influence the clinician’s decision to provide an immediate antibiotic include renal function; co-morbidity; diabetes; immunosuppression; cost of treatment; pregnancy; severity of symptoms; age of patient; and time before the weekend. | “EGFR, their diabetes status, the recurrence of the symptoms, whether they’re pregnant or not, that sort of thing, so there’s quite a few other issues that I need to then take on board despite the guidance that’s being given out.” (GP 8) | |
| Optimism | ||
| One GP group was optimistic that the message about not receiving an antibiotic immediately was becoming widely more accepted. | “People are starting to get that message now, with what’s been in the press, …it’s refreshing that you now come across more patients who will say… I don’t want one if I don’t have to have one. And if you say, let’s give this a few days or let’s wait for the culture to come back or whatever and see, they’re OK with that.” (GP 2) | The updated diagnostic tool:
|
| Behavioural Regulation | ||
| The usefulness of a having an accurate point-of-care test was mentioned by some groups, but the perceived benefit was often to provide reassurance to the patient. | “…oximetry, one thing I do with these people the ones who come with cold and cough, I put them on the machine, I say look, oxygen, pulse is level, temperature normal, you haven’t got an infection and they love it, so that reassures them. If there was a something which we got, where we put the urine and say look, it says there’s no infection. They will be happy.” (GP 6) | The updated diagnostic tool:
|
| Some groups had audited their antibiotic prescribing recently and none had audited antibiotic prescribing for UTIs specifically. | “Different members of staff have audited different topics, haven’t you? We’re doing one at the moment… on COPD antibiotics. We have our own internal audits and most of you do an audit for your appraisals and things as well don’t you?” (GP 7) | |
| Reinforcement | ||
| Most GP staff believed that patients expect to be prescribed an antibiotic if they have urinary symptoms | “M1: I think, as *** has said, it’s patient expectations. F1: So they have these symptoms and they’ve always had antibiotics. M1: They’ve had the symptoms. F1: So they need antibiotics again, or they’ve got the same, the same symptoms and don’t often consider that there might be another, another cause.” (GP 4) | The updated diagnostic tool:
|
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cooper, E.; Jones, L.; Joseph, A.; Allison, R.; Gold, N.; Larcombe, J.; Moore, P.; McNulty, C.A.M. Diagnosis and Management of UTI in Primary Care Settings—A Qualitative Study to Inform a Diagnostic Quick Reference Tool for Women Under 65 Years. Antibiotics 2020, 9, 581. https://doi.org/10.3390/antibiotics9090581
Cooper E, Jones L, Joseph A, Allison R, Gold N, Larcombe J, Moore P, McNulty CAM. Diagnosis and Management of UTI in Primary Care Settings—A Qualitative Study to Inform a Diagnostic Quick Reference Tool for Women Under 65 Years. Antibiotics. 2020; 9(9):581. https://doi.org/10.3390/antibiotics9090581
Chicago/Turabian StyleCooper, Emily, Leah Jones, Annie Joseph, Rosie Allison, Natalie Gold, James Larcombe, Philippa Moore, and Cliodna A. M. McNulty. 2020. "Diagnosis and Management of UTI in Primary Care Settings—A Qualitative Study to Inform a Diagnostic Quick Reference Tool for Women Under 65 Years" Antibiotics 9, no. 9: 581. https://doi.org/10.3390/antibiotics9090581
APA StyleCooper, E., Jones, L., Joseph, A., Allison, R., Gold, N., Larcombe, J., Moore, P., & McNulty, C. A. M. (2020). Diagnosis and Management of UTI in Primary Care Settings—A Qualitative Study to Inform a Diagnostic Quick Reference Tool for Women Under 65 Years. Antibiotics, 9(9), 581. https://doi.org/10.3390/antibiotics9090581






