Preventing and Managing Urinary Tract Infections: Enhancing the Role of Community Pharmacists—A Mixed Methods Study
Abstract
:1. Introduction
2. Methods
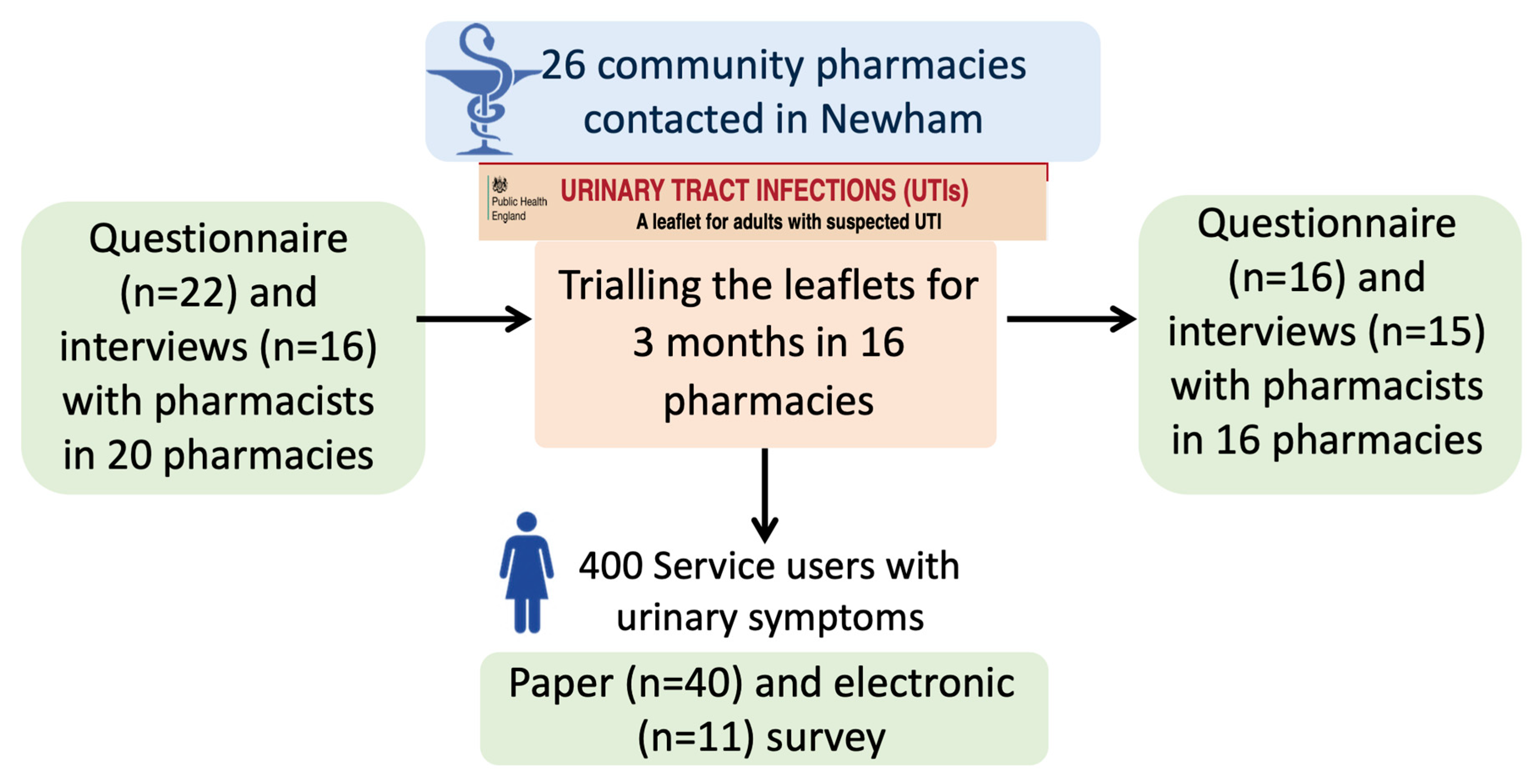
2.1. Study Design
2.2. Questionnaires and Interviews Schedules
2.3. Study Setting: Community Pharmacies in Newham
2.4. Participant Enrolment
2.5. Data Analysis
2.6. Ethics
3. Results
3.1. Participants: Pharmacists and Service Users
3.2. Survey Results: The Patient UTI Journey in the Community
3.3. Advice in the Pharmacy
3.4. Communication with the GP
“So, there’s not much, much of a connection between the two settings. For example, if there was a patient that we were particularly concerned about, we can’t call up the GP practice and say, oh, could you give them early appointment because I’ve seen them and I’ve noticed X, Y, Z. There’s not that rapport yet or there’s not that importance [placed in] a pharmacist’s view, I feel, in community.” P4.
3.5. The Role of Pharmacists
“Well, I think they [the patients] should come first to the pharmacy (…) and then you could screen them and see whether they need to be actually seen by the GP.” P13.
“Yeah, but you see having a role to play is one thing but you need to be remunerated for that role. You can’t expect pharmacists to do everything for nothing” P13.
“[Having a UTI PGD] …could be something which might take a bit of work off the GPs. And in that service, we do get a consultation fee as well and we do that service for Pharmacy First or the Minor Ailment. So, I think that’s some revenue, it works for the GP and it works for the patient” P3.
“That is where it should all start. We [pharmacy staff] should be highly focused on prevention, and providing advice for people to self-care and self-manage, and improve their health. And that will stop, forget the resistance [AMR], you will not even need to prescribe antibiotics if people are living a healthy lifestyle. (…) So, the biggest impact the pharmacist can make is in the prevention agenda” P10.
4. Discussion
4.1. Summary
4.2. Comparison with Existing Literature
4.3. Strengths and Limitations
4.4. Implications for Practice
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Foxman, B. Epidemiology of urinary tract infections: Incidence, morbidity, and economic costs. Am. J. Med. 2002, 113 (Suppl. 1A), 5S–13S. [Google Scholar] [CrossRef]
- Scholes, D.; Hooton, T.M.; Roberts, P.L.; Stapleton, A.E.; Gupta, K.; Stamm, W.E. Risk Factors for Recurrent Urinary Tract Infection in Young Women. J. Infect. Dis. 2000, 182, 1177–1182. [Google Scholar] [CrossRef] [Green Version]
- McNulty, C.A.M.; Richards, J.; Livermore, D.M.; Little, P.; Charlett, A.; Freeman, E.; Harvey, I.; Thomas, M. Clinical relevance of laboratory-reported antibiotic resistance in acute uncomplicated urinary tract infection in primary care. J. Antimicrob. Chemother. 2006, 58, 1000–1008. [Google Scholar] [CrossRef] [PubMed]
- Ong, D.S.Y.; Kuyvenhoven, M.M.; van Dijk, L.; Verheij, T.J.M. Antibiotics for respiratory, ear and urinary tract disorders and consistency among GPs. J. Antimicrob. Chemother. 2008, 62, 587–592. [Google Scholar] [CrossRef] [PubMed]
- Butler, C.C.; Francis, N.; Thomas-Jones, E.; Llor, C.; Bongard, E.; Moore, M.V.; Little, P.; Bates, J.; Lau, M.; Pickles, T.; et al. Variations in presentation, management, and patient outcomes of urinary tract infection: A prospective four-country primary care observational cohort study. Br. J. Gen. Pract. 2017, 67, e830–e841. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Shively, N.R.; Buehrle, D.J.; Clancy, C.J.; Decker, B.K. Prevalence of Inappropriate Antibiotic Prescribing in Primary Care Clinics within a Veterans Affairs Health Care System. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Abernethy, J.; Guy, R.; Sheridan, E.; Wilcox, M.; Johnson, A.P.; Hope, R.; Sen, R.; Mifsud, A.; O’Driscoll, J.; Brown, N.; et al. Epidemiology of Escherichia coli bacteraemia in England: Results of an enhanced sentinel surveillance programme. J. Hosp. Infect. 2017, 95, 365–375. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vihta, K.-D.; Stoesser, N.; Llewelyn, M.; Quan, T.P.; Davies, T.; Fawcett, N.J.; Dunn, L.; Jeffery, K.; Butler, C.C.; Hayward, G.; et al. Trends over time in Escherichia coli bloodstream infections, urinary tract infections, and antibiotic susceptibilities in Oxfordshire, UK, 1998–2016: A study of electronic health records. Lancet Infect. Dis. 2018, 18, 1138–1149. [Google Scholar] [CrossRef] [Green Version]
- Butler, C.C.; Hawking, M.K.D.; Quigley, A.; McNulty, C.A.M. Incidence, severity, help seeking, and management of uncomplicated urinary tract infection: A population-based survey. Br. J. Gen. Pract. 2015, 65, e702–e707. [Google Scholar] [CrossRef] [Green Version]
- UK Department of Health and Social Carer. UK 5-year Action Plan for Antimicrobial Resistance 2019 to 2024; Department of Health and Social Care: London, UK, 2019. [Google Scholar]
- Overview|Patient group directions|Guidance|N.I.C.E. Available online: https://www.nice.org.uk/guidance/mpg2 (accessed on 16 May 2020).
- Booth, J.L.; Mullen, A.B.; Thomson, D.A.; Johnstone, C.; Galbraith, S.J.; Bryson, S.M.; McGovern, E.M. Antibiotic treatment of urinary tract infection by community pharmacists: A cross-sectional study. Br. J. Gen. Pract. 2013, 63, e244–e249. [Google Scholar] [CrossRef]
- International Pharmaceutical Federation. Fighting Antimicrobial Resistance. The Contribution of Pharmacists. Published Online 2015. Available online: https://www.fip.org/www/streamfile.php?filename=fip/publications/2015-11-Fighting-antimicrobial-resistance.pdf (accessed on 25 August 2019).
- Canadian Pharmacists Association. Pharmacists’ Expanded Scope of Practice in Canada. Available online: https://www.pharmacists.ca/cpha-ca/assets/File/news-events/ExpandedScopeChart_June2015_EN.pdf (accessed on 17 August 2020).
- New Zealand Ministry of Health. Medicines Amendment Regulations (No. 2) 2015 (LI 2015/180)—New Zealand Legislation. Available online: http://www.legislation.govt.nz/regulation/public/2015/0180/12.0/whole.html (accessed on 17 August 2020).
- Public Health England. Leaflets to Share with Patients: The TARGET Antibiotics Toolkit. Available online: https://www.rcgp.org.uk/clinical-and-research/resources/toolkits/amr/target-antibiotics-toolkit/leaflets-to-share-with-patients.aspx (accessed on 28 January 2020).
- Lecky, D.M.; Howdle, J.; Butler, C.C.; McNulty, C.A. Optimising management of UTIs in primary care: A qualitative study of patient and GP perspectives to inform the development of an evidence-based, shared decision-making resource. Br. J. Gen. Pract. 2020, 70, e330–e338. [Google Scholar] [CrossRef] [PubMed]
- Damschroder, L.J.; Aron, D.C.; Keith, R.E.; Kirsh, S.R.; Alexander, J.A.; Lowery, J.C. Fostering implementation of health services research findings into practice: A consolidated framework for advancing implementation science. Implement. Sci. 2009, 4, 50. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Bradley, E.H.; Curry, L.A.; Devers, K.J. Qualitative data analysis for health services research: Developing taxonomy, themes, and theory. Health Serv. Res. 2007, 42, 1758–1772. [Google Scholar] [CrossRef] [Green Version]
- Thornley, T.; Kirkdale, C.L.; Beech, E.; Howard, P.; Wilson, P. Evaluation of a community pharmacy-led test-and-treat service for women with uncomplicated lower urinary tract infection in England. JAC-Antimicrob. Resist 2020, 2. [Google Scholar] [CrossRef] [Green Version]
- Du, H.C.T.; John, D.N.; Walker, R. An investigation of prescription and over-the-counter supply of ophthalmic chloramphenicol in Wales in the 5 years following reclassification. Int. J. Pharm. Pract. 2014, 22, 20–27. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jones, L.; Owens, R.; Sallis, A.; Ashiru-Oredope, D.; Thornley, T.; Francis, N.; Butler, C.; McNulty, C. Qualitative study using interviews and focus groups to explore the current and potential for antimicrobial stewardship in community pharmacy informed by the Theoretical Domains Framework. BMJ Open 2018, 8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Jones, L.F.; Meyrick, J.; Bath, J.; Dunham, O.; McNulty, C.A.M. Effectiveness of behavioural interventions to reduce urinary tract infections and Escherichia coli bacteraemia for older adults across all care settings: A systematic review. J. Hosp. Infect. 2019, 102, 200–218. [Google Scholar] [CrossRef] [Green Version]
- Platt, C.; Larcombe, J.; Dudley, J.; McNulty, C.; Banerjee, J.; Gyoffry, G.; Pike, K.; Jadresic, L.; Gyorffy, G. Implementation of NICE guidance on urinary tract infections in children in primary and secondary care. Acta Paediatr. 2015, 104, 630–637. [Google Scholar] [CrossRef]
- Royal College of General Practitioners (RCGP), Royal Pharmaceutical Society (RPS). Breaking Down the Barriers—How Community Pharmacists and GPs Can. Work Together to Improve Patient Care. 2012. Available online: http://www.rpharms.com/public-affairs-pdfs/RPSRCGPjointstatement.pdf (accessed on 25 August 2019).
- Department of Health and Social Care. Community Pharmacy Contractual Framework: 2019 to 2024. Published 22 July 2019. Available online: https://www.gov.uk/government/publications/community-pharmacy-contractual-framework-2019-to-2024 (accessed on 16 May 2020).
- Redwood, S.; Gill, P.S. Under-representation of minority ethnic groups in research—Call for action. Br. J. Gen. Pract. 2013, 63, 342–343. [Google Scholar] [CrossRef] [Green Version]
- Jones, L.; Hawking, M.K.D.; Owens, R.; Lecky, D.M.; Francis, N.; Butler, C.C.; Gal, M.; McNulty, C. An evaluation of the TARGET (Treat Antibiotics Responsibly; Guidance, Education, Tools) Antibiotics Toolkit to improve antimicrobial stewardship in primary care—Is it fit for purpose? Fam. Pract. 2017, 35, 461–467. [Google Scholar] [CrossRef] [Green Version]
- NHS. The NHS Long Term Plan. Published Online 2019. Available online: https://www.longtermplan.nhs.uk/wp-content/uploads/2019/08/nhs-long-term-plan-version-1.2.pdf (accessed on 25 August 2019).
- National Health Service. Primary Care Networks. NHS. 2019. Available online: https://www.england.nhs.uk/primary-care/primary-care-networks/ (accessed on 28 January 2020).
- Auta, A.; Hadi, M.A.; Oga, E.; Adewuyi, E.O.; Abdu-Aguye, S.; Adeloye, D.; Strickland-Hodge, B.; Morgan, D.J. Global access to antibiotics without prescription in community pharmacies: A systematic review and meta-analysis. J. Infect. 2019, 78, 8–18. [Google Scholar] [CrossRef] [PubMed]

| Pharmacists | n (%) or Median (IQR) (n = 22) |
|---|---|
| Women | 8 (36) |
| Job description | |
| Non-prescribing pharmacists | 18 (82) |
| Prescribing pharmacists | 3 (14) |
| Pharmacy technician* | 1 (4) |
| Years since qualification | 15 (5–30) |
| Years in the pharmacy | 9.5 (5–17) |
| Pharmacy staff (full time equivalent) in the pharmacy | 4 (3–5) |
| Service users per day | 55 (40–100) |
| Estimated percentage of male service users seen in the pharmacy | 61 (52–62) |
| Service users seen in the consultation room per day | 8 (5–12) |
| Estimated number of service users given healthcare advice | 20 (16–37) |
| Service Users | n (%) (n = 51) |
| Women | 43 (84) |
| Age | |
| Children | 1 (2) (completed by the mother) |
| 18–24 | 8 (16) |
| 25–34 | 10 (20) |
| 35–44 | 4 (8) |
| 45–54 | 11 (22) |
| 55–64 | 7 (14) |
| 65–74 | 4 (8) |
| >75 | 4 (8) |
| Ethnicity | |
| White | 27 (53) |
| Asian | 14 (27) |
| Black | 4 (8) |
| Mixed | 4 (8) |
| UTI history | |
| Recurrent UTIs | 21 (41) |
| One or two prior episodes | 23 (45) |
| No prior episode | 6 (12) |
| Pharmacists n = 22 (%) | |
|---|---|
| Barriers | |
| Lack of time or staff | 17 (77) |
| Language barrier | 13 (59) |
| No access to the medical record | 9 (41) |
| Not recognised or funded by health authorities | 5 (23) |
| No possibilities to prescribe medication | 5 (23) |
| Outside the scope of expertise of pharmacists | 3 (14) |
| Waiting time is unpredictable for service users | 2 (9) |
| Some service users prefer information from doctors | 2 (9) |
| Facilitators | |
| Pharmacists are confident and trained in giving advice | 22 (100) |
| No appointment needed | 17 (77) |
| Long opening hours | 14 (64) |
| Ease of access | 13 (59) |
| Multiple languages spoken by the staff | 12 (55) |
| Financial incentive to give additional advice | 10 (45) |
| Availability and use of a consultation room | 9 (41) |
| Close contact with the service users | 8 (36) |
| Flexible time for consultation (no time limit) | 6 (27) |
| Counter assistants and sufficient staff | 5 (23) |
| Local presence/community-based | 2 (9) |
| Possibility to give advice on the phone | 2 (9) |
| Management of Service Users with Suspected or Confirmed Urinary Tract Infection | n (%) (n = 16) |
|---|---|
| Pharmacists can act as a first-line triage | 11 (69) |
| They need funding or additional staff to do so | 10 (62) |
| They should have more possibilities to prescribe first line treatments (e.g., PGDs) | 5 (31) |
| They can give dipstick tests and check the results | 1 (6) |
| Strengthening the link between pharmacists and GPs | |
| Development of a special referral pathway between pharmacies and GPs | 16 (100) |
| Self-care advice relieves pressure on the NHS and the GPs | 6 (37) |
| Reducing the spread of AMR | |
| Education of service users about infections for which antibiotics are not always needed | 16 (100) |
| Screening patients who need to go to the GP | 10 (62) |
| Self-care advice for viral infections and benign bacterial infections | 12 (75) |
| Promotion of a healthy lifestyle | 5 (31) |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Peiffer-Smadja, N.; Allison, R.; Jones, L.F.; Holmes, A.; Patel, P.; Lecky, D.M.; Ahmad, R.; McNulty, C.A.M. Preventing and Managing Urinary Tract Infections: Enhancing the Role of Community Pharmacists—A Mixed Methods Study. Antibiotics 2020, 9, 583. https://doi.org/10.3390/antibiotics9090583
Peiffer-Smadja N, Allison R, Jones LF, Holmes A, Patel P, Lecky DM, Ahmad R, McNulty CAM. Preventing and Managing Urinary Tract Infections: Enhancing the Role of Community Pharmacists—A Mixed Methods Study. Antibiotics. 2020; 9(9):583. https://doi.org/10.3390/antibiotics9090583
Chicago/Turabian StylePeiffer-Smadja, Nathan, Rosalie Allison, Leah F. Jones, Alison Holmes, Parvesh Patel, Donna M. Lecky, Raheelah Ahmad, and Cliodna A. M. McNulty. 2020. "Preventing and Managing Urinary Tract Infections: Enhancing the Role of Community Pharmacists—A Mixed Methods Study" Antibiotics 9, no. 9: 583. https://doi.org/10.3390/antibiotics9090583
APA StylePeiffer-Smadja, N., Allison, R., Jones, L. F., Holmes, A., Patel, P., Lecky, D. M., Ahmad, R., & McNulty, C. A. M. (2020). Preventing and Managing Urinary Tract Infections: Enhancing the Role of Community Pharmacists—A Mixed Methods Study. Antibiotics, 9(9), 583. https://doi.org/10.3390/antibiotics9090583







