Clinician and Patient Factors Influencing Treatment Decisions: Ethnographic Study of Antibiotic Prescribing and Operative Procedures in Out-of-Hours and General Dental Practices
Abstract
:1. Introduction
2. Results
2.1. Description of Participants and Appointments
2.1.1. Demographics of Participants
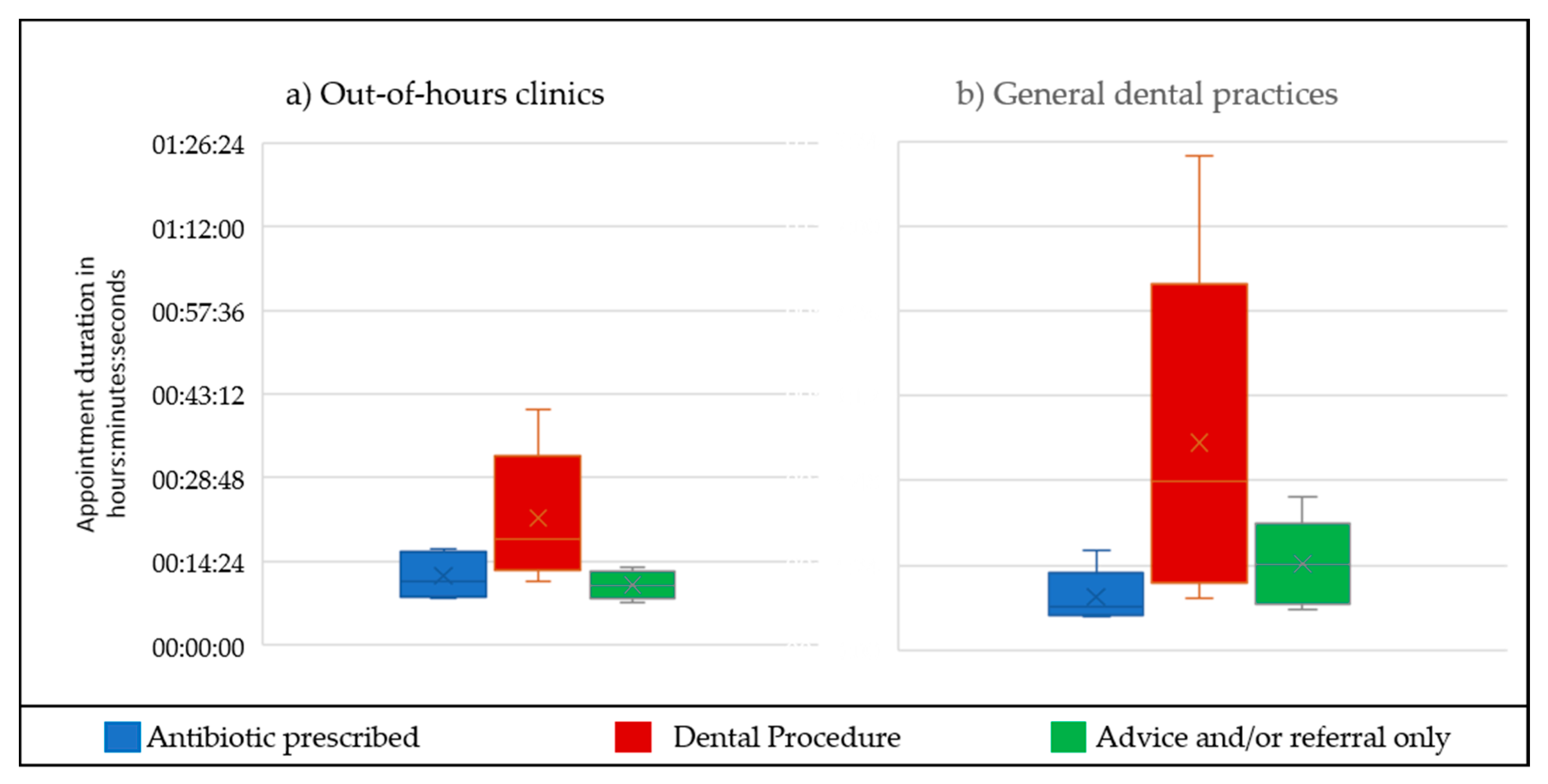
2.1.2. Treatment Provided and Duration of Appointments
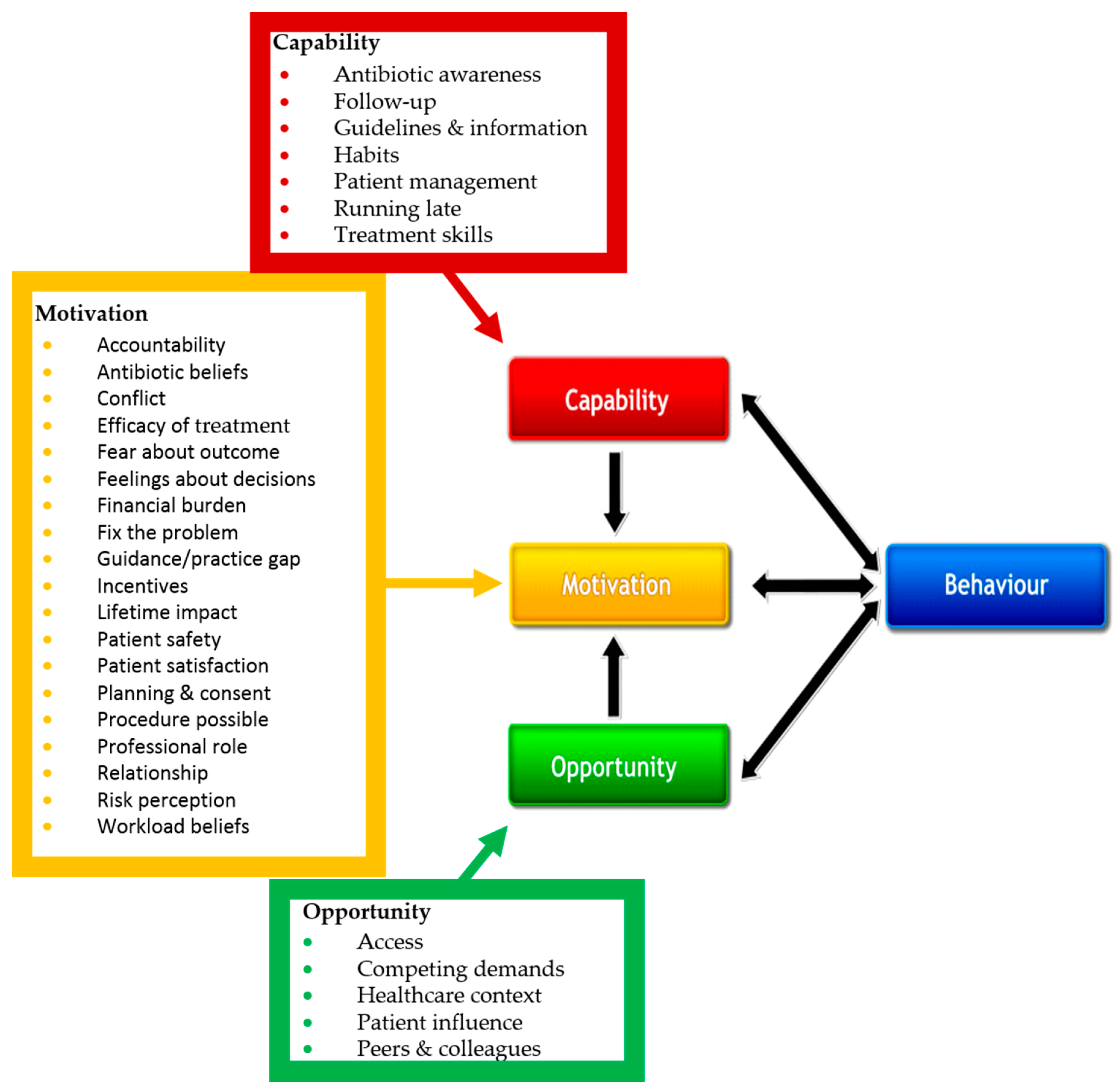
2.2. Dentist Factors Influencing Treatment Decisions
“The key factor behind today’s decision to prescribe antibiotics seemed to be the need to reduce swelling …this patient was anxious and didn’t have a regular GDP and was facing a denture. After the appointment, the dentist explained his frustration at the lack of options for patients like this one—not able to access NHS dental care—no one ‘taking on’ patients in [name of city]—possibly a 6 month waiting list leaving this patient with few options.”(Ethnographic observation—OOH)
‘the dentist seemed angry about [the cost of dental treatment not covered by the NHS] on behalf of the patient’(Ethnographic observation—OOH)
‘…he’s that scared that the fear of dentists overrides his pain … he’s in pain he’s got abscesses and there’s been an error or a mix up with his referral. Something like, he had been referred and they’d called him on the incorrect number, so he had failed to attend, so he had been taken off the referral list …. Oh, what do I do? I can’t refuse to give antibiotics if he’s in pain! But then how many antibiotics can we even prescribe?’(Interview—GDP Dentist)
“When you are in a lot of pain, you want the pain to go and don’t think about future consequences. So I think I sometimes worry that patients when they are out of pain and once they have calmed down will then worry about this gap that possibly will not be able to be replaced because they don’t have a dentist.”(Interview—GDP Dentist)
“…because of the way the patients are usually squeezed in it’s a time management thing…I mean I get stressed when I’m running late generally anyway but you accommodate.”(Interview—GDP Dentist)
“…sometimes [giving patients 5 to 10 minutes back in the waiting room] is needed … because you do have to think about the people that are waiting cos they do have appointments and they are often distressed too.”(Interview—OOH Dental Nurse)
“If someone’s been booked in literally for a five-minute appointment… [it] isn’t long enough [so the dentist] will give antibiotics instead.”(Interview—GDP Dental Nurse)
“To get the patient out of pain. But actually, that’s a secondary goal of mine. My first goal is to make sure they’re not in danger…”(Interview—GDP Dentist)
“You’re providing a service which, you know, is effectively saving lives…. Patients come in with a massive facial swelling, it could become quite severe and quite serious.’(Interview—OOH Dentist)
“It’s very rare that I don’t manage to convince the patients to have it out …. [but if a patient declines care] just give them antibiotics just to keep them happy: (1) to prevent a complaint and (2) to prevent any sort of subsequent swelling or infection that may take them to A&E.”(Interview—OOH Dentist)
“I gave her the option to book in herself rather than book [a review] in proactively and since then I’ve not seen her, so I’m assuming it must’ve been fine.”(Interview—GDP Dentist)
“…managing the patient and managing the patient’s expectations as well as managing the tooth…”(Interview—GDP Dentist)
“My first and second year, I would try everything on the first appointment. But … after a few times I was still disappointed and making the patient unhappy. So, I decided to change the way I do it [using antibiotics] and it’s a lot better.”(Interview—GDP Dentist)
2.3. Patient Factors Influencing Treatment Decisions
“Is there no way I can just have antibiotics and come back after Christmas and have this done and have it removed? And can I be knocked out? Because honestly I’m terrified.”(Appointment transcript—OOH)
“I wasn’t going to leave without any [antibiotics].”(Interview—OOH Patient)
Patient: “… [I’ve] been given amoxicillin before and that’s been twice now…”
Dentist: “…there’s absolutely no indication to give you that.”
Patient: “I was actually given it last time I was here…”
Dentist: “…Antibiotics will make no difference in this case… So I can [list of all options]”
Patient: “Erm, I don’t really want that tooth out to be honest….”(Appointment transcript—GDP)
“I tried to push it. So I did say it quite a few times… giving the same reason that it did help me before… [When the dentist declined to prescribe antibiotics] I sort of knew at that point. I sort of felt disappointed because of the fact that them saying no it means that [the tooth] was in a bad state and [antibiotics] wouldn’t help at all. So, I did feel disappointed … It was all leaning towards the tooth being taken out.”(Interview—GDP Patient)
2.4. Contextual Elements Affecting Treatment Decisions—Comparing OOH vs. GDP Settings
“My worst nightmare is that the anesthetic is not working and anything you touch, or try to go in the pulp, that the patient feels it.”(Interview—GDP Dentist)
“Sometimes when patients can’t decide, they’re sat there thinking ‘Oh I don’t know what to do. I might ring this person. I might ring that person…’ It does become quite frustrating …in the back of your mind, ‘Oh g*d, we’ve not got much time left.’”(Interview—OOH Dentist)
“I need [a dentist…the OOH dentist] put clean inside—after 10 days everything is out and painful… I am waiting [to find a dentist to finish the treatment].”(Interview—OOH patient)
“He just needs an extraction and, bless him, he’s that scared that the fear of dentists overrides his pain. [Now its infected again I had to] prescribe a further course of antibiotics [and called about] the referral to explain the situation to try and get him up the list faster.”(Interview—GDP Dentist)
3. Discussion
4. Materials and Methods
4.1. Sampling and Data Collection
4.1.1. Ethnographic Observation Sample
4.1.2. Interview Sample
4.2. Data Collection Methods
4.2.1. Ethnographic Observations
4.2.2. Interviews
4.2.3. Data Synthesis and Interpretation
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO. Antibiotic Resistance. Available online: https://www.who.int/news-room/fact-sheets/detail/antibiotic-resistance (accessed on 20 August 2020).
- Gajdács, M.; Albericio, F. Antibiotic Resistance: From the Bench to Patients. Antibiotics 2019, 8, 129. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- FDI. Meet Dr Wendy Thompson, Lead Author of FDI White Paper on Tackling Antibiotic Resistance. Available online: https://www.fdiworlddental.org/news/20191122/meet-dr-wendy-thompson (accessed on 30 August 2020).
- FDI. Antibiotic Stewardship in Dentistry-FDI Policy Statement; FDI World Dental Federation: Geneva, Switzerland, 2019. [Google Scholar]
- Sarmiento, M.A.; Maglutac, M.T., Jr.; Yanga-Mabunga, M.S. Antibiotic Prescribing Practices of Filipino Dentists. Int. J. Public Health Sci. 2019, 8, 332–340. [Google Scholar] [CrossRef] [Green Version]
- Lockhart, P.B.; Tampi, M.P.; Abt, E.; Aminoshariae, A.; Durkin, M.J.; Fouad, A.F.; Gopal, P.; Hatten, B.W.; Kennedy, E.; Lang, M.S. Evidence-based clinical practice guideline on antibiotic use for the urgent management of pulpal-and periapical-related dental pain and intraoral swelling: A report from the American Dental Association. J. Am. Dent. Assoc. 2019, 150, 906–921.e12. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Group OaDE. Therapeutic Guidelines: Oral and Dental Version 3; Therapeutic Guidelines Ltd.: Melbourne, Australia, 2019. [Google Scholar]
- Antimicrobial Prescribing for General Dental Practitioners. Available online: https://www.fgdp.org.uk/guidance-standards/antimicrobial-prescribing-gdps (accessed on 20 August 2020).
- Emergency Dental Care: Dental Clinical Guidance. Available online: http://www.sdcep.org.uk/published-guidance/emergency-dental-care/ (accessed on 20 August 2020).
- Nishimura, R.A.; Otto, C.M.; Bonow, R.O.; Carabello, B.A.; Erwin, J.P.; Fleisher, L.A.; Jneid, H.; Mack, M.J.; McLeod, C.J.; O’Gara, P.T. 2017 AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2017, 70, 252–289. [Google Scholar] [CrossRef] [PubMed]
- NICE. Antimicrobial Prophylaxis Against Infective Endocarditis in Adults and Children Undergoing Interventional Procedures. Available online: https://www.nice.org.uk/guidance/cg64 (accessed on 30 August 2020).
- Adler, Y.; Charron, P.; Imazio, M.; Badano, L.; Barón-Esquivias, G.; Bogaert, J.; Brucato, A.; Gueret, P.; Klingel, K.; Lionis, C. 2015 ESC Guidelines for the diagnosis and management of pericardial diseases: The Task Force for the Diagnosis and Management of Pericardial Diseases of the European Society of Cardiology (ESC) Endorsed by: The European Association for Cardio-Thoracic Surgery (EACTS). Eur. Heart J. 2015, 36, 2921–2964. [Google Scholar]
- Hicks, L.A.; Bartoces, M.G.; Roberts, R.M.; Suda, K.J.; Hunkler, R.J.; Taylor, T.H., Jr.; Schrag, S.J. US outpatient antibiotic prescribing variation according to geography, patient population, and provider specialty in 2011. Clin. Infect. Dis. 2015, 60, 1308–1316. [Google Scholar] [CrossRef] [Green Version]
- Suda, K.; Calip, G.; Zhou, J.; Rowan, S.; Gross, A.; Hershow, R.; Perez, R.; McGregor, J.; Evans, C. Assessment of the appropriateness of antibiotic prescriptions for infection prophylaxis before dental procedures, 2011 to 2015. JAMA Netw. Open 2019, 2, e193909. [Google Scholar] [CrossRef] [Green Version]
- Cope, A.L.; Francis, N.A.; Wood, F.; Chestnutt, I.G. Antibiotic prescribing in UK general dental practice: A cross-sectional study. Community Dent. Oral Epidemiol. 2016, 44, 145–153. [Google Scholar] [CrossRef]
- NHSDigital. NHS Dental Statistics for England-2015-16. Available online: https://digital.nhs.uk/data-and-information/publications/statistical/nhs-dental-statistics/nhs-dental-statistics-for-england-2015-16 (accessed on 20 August 2020).
- Charani, E.; Edwards, R.; Sevdalis, N.; Alexandrou, B.; Sibley, E.; Mullett, D.; Franklin, B.D.; Holmes, A. Behavior change strategies to influence antimicrobial prescribing in acute care: A systematic review. Clin. Infect. Dis. 2011, 53, 651–662. [Google Scholar] [CrossRef] [Green Version]
- Löffler, C.; Böhmer, F. The effect of interventions aiming to optimise the prescription of antibiotics in dental care—A systematic review. PLoS ONE 2017, 12, e0188061. [Google Scholar] [CrossRef] [Green Version]
- Atkins, L.; Francis, J.; Islam, R.; O’Connor, D.; Patey, A.; Ivers, N.; Foy, R.; Duncan, E.M.; Colquhoun, H.; Grimshaw, J.M. A guide to using the Theoretical Domains Framework of behaviour change to investigate implementation problems. Implement. Sci. 2017, 12, 77. [Google Scholar] [CrossRef] [PubMed]
- Thompson, W.; Douglas, G.; Pavitt, S.; Sandoe, J.; McEachan, R.; Tonkin-Crine, S. Factors associated with prescribing of systemic antibacterial drugs to adult patients in urgent primary health care, especially dentistry. J. Antimicrob. Chemother. 2019, 74, 2139–2152. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Reeves, S.; Kuper, A.; Hodges, B.D. Qualitative research methodologies: Ethnography. BMJ 2008, 337, a1020. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Szymczak, J.E. Are Surgeons Different? The Case for Bespoke Antimicrobial Stewardship. Clin. Infect. Dis. 2019, 69, 21–23. [Google Scholar] [CrossRef] [PubMed]
- Charani, E.; Ahmad, R.; Rawson, T.; Castro-Sanchez, E.; Tarrant, C.; Holmes, A.J.C.I.D. The Differences in Antibiotic Decision-making Between Acute Surgical and Acute Medical Teams: An Ethnographic Study of Culture and Team Dynamics. Clin. Infect. Dis. 2018, 69, 12–20. [Google Scholar] [CrossRef] [PubMed]
- Fetterman, D.M. Ethnography: Step-by-Step; SAGE Publications, Incorporated: Southend Oaks, CA, USA, 2019; Volume 17. [Google Scholar]
- McCambridge, J.; Witton, J.; Elbourne, D.R. Systematic review of the Hawthorne effect: New concepts are needed to study research participation effects. J. Clin. Epidemiol. 2014, 67, 267–277. [Google Scholar] [CrossRef] [Green Version]
- Dailey, Y.M. Are antibiotics being used appropriately for emergency dental treatment? Br. Dent. J. 2001, 191, 391–393. [Google Scholar] [CrossRef] [Green Version]
- Newlands, R.; Duncan, E.M.; Prior, M.; Elouafkaoui, P.; Elders, A.; Young, L.; Clarkson, J.E.; Ramsay, C.R. Barriers and facilitators of evidence-based management of patients with bacterial infections among general dental practitioners: A theory-informed interview study. Implement Sci. IS 2016, 11, 11. [Google Scholar] [CrossRef] [Green Version]
- Centre for Disease Control and Prevention. US National Action Plan for Combating Antibiotic-Resistant Bacteria (National Action Plan); The White House: Washington, DC, USA, 2015.
- Jamshed, S.; Padzil, F.; Shamsudin, S.H.; Bux, S.H.; Jamaluddin, A.A.; Bhagavathula, A.S.; Azhar, S.; Hassali, M.A. Antibiotic stewardship in community pharmacies: A scoping review. Pharmacy 2018, 6, 92. [Google Scholar] [CrossRef] [Green Version]
- Mortazhejri, S.; Patey, A.M.; Stacey, D.; Bhatia, R.S.; Abdulla, A.; Grimshaw, J.M. Understanding determinants of patients’ decisions to attend their family physician and to take antibiotics for upper respiratory tract infections: A qualitative descriptive study. BMC Fam. Pract. 2020, 21, 1–11. [Google Scholar] [CrossRef]
- Wellcome Trust. Reframing Resistance-How to Communicate about Antimicrobial Resistance Effectively; Wellcome Trust: London, UK, 2019. [Google Scholar]
- Roope, L.S.; Tonkin-Crine, S.; Herd, N.; Michie, S.; Pouwels, K.B.; Castro-Sanchez, E.; Sallis, A.; Hopkins, S.; Robotham, J.V.; Crook, D.W. Reducing expectations for antibiotics in primary care: A randomised experiment to test the response to fear-based messages about antimicrobial resistance. BMC Med. 2020, 18, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Glover, R.E.; Dangoor, M.; Mays, N. Antibiotic resistance: Don’t blame patients. Br. Med. J. 2019, 364, l1218. [Google Scholar] [CrossRef] [PubMed]
- Coles, E.; Anderson, J.; Maxwell, M.; Harris, F.M.; Gray, N.M.; Milner, G.; MacGillivray, S. The influence of contextual factors on healthcare quality improvement initiatives: A realist review. Syst. Rev. 2020, 9, 1–22. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- NHSE. GP Patient Survey Dental Statistics. Available online: https://www.england.nhs.uk/statistics/category/statistics/gp-dental-statistics/ (accessed on 20 August 2020).
- American Dental Association. Survey: More Americans Want to Visit the Dentist; ADA: Chicago, IL, USA, 2018.
- Goodwin, T.L.; Brocklehurst, P.; Hall, B.; McDonald, R.; Tickle, M.; Williams, L. How, and why, does capitation affect general dental practitioners’ behaviour? A rapid realist review. Br. J. Healthc. Manag. 2018, 24, 505–513. [Google Scholar]
- Giddon, D.B.; Swann, B.; Donoff, R.B.; Hertzman-Miller, R. Dentists as oral physicians: The overlooked primary health care resource. J. Prim. Prev. 2013, 34, 279–291. [Google Scholar] [CrossRef] [PubMed]
- Laverty, L.; Harris, R. Risk work in dental practices: An ethnographic study of how risk is managed in NHS dental appointments. Sociol. Health Illn. 2020. [Google Scholar] [CrossRef]
- GDC. Standards for the Dental Team. Available online: https://www.gdc-uk.org/professionals/standards (accessed on 20 August 2020).
- Williams, S.; Halls, A.; Tonkin-Crine, S.; Moore, M.; Latter, S.; Little, P.; Eyles, C.; Postle, K.; Leydon, G. General practitioner and nurse prescriber experiences of prescribing antibiotics for respiratory tract infections in UK primary care out-of-hours services (the UNITE study). J. Antimicrob. Chemother. 2017, 73, 795–803. [Google Scholar] [CrossRef] [Green Version]
- Salako, N.O.; Rotimi, V.O.; Adib, S.M.; Al-Mutawa, S. Pattern of antibiotic prescription in the management of oral diseases among dentists in Kuwait. J. Dent. 2004, 32, 503–509. [Google Scholar] [CrossRef]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef] [Green Version]
- Michie, S.; Atkins, L.; West, R. The Behaviour Change Wheel: A Guide to Designing Interventions; Silverback Publishing: Great Britain, UK, 2014. [Google Scholar]
| Patient Factor | Description |
|---|---|
| Access | Ease of access to routine or specialist dental care, such as referral for sedation. |
| Antibiotic beliefs | Patient expectation or beliefs about the need for, or ability of, antibiotics to treat acute dental conditions. Some saw antibiotics as a quick fix whilst others expressed concern about the risks of antibiotics. |
| Antibiotic goal | Goal of appointment was to obtain antibiotics. Some patients stated that they had a plan as to how they would obtain them. |
| Beliefs about procedures | Patient expectation or beliefs about dental procedures, such as extraction or endodontic (root canal) treatment. |
| Communication/negotiation | Patient communication/negotiation skills in relation to dental appointments, including patient recognition of constraints within which the dentist was working. |
| Costs | Views about cost effectiveness and affordability of dental care (including for private care such as implants to fill spaces left by urgent procedures). |
| Delaying tactic | Aim to delay losing a tooth or extensive dental work until no other options were possible. |
| Emotional attachment | Degree of emotional attachment a patient has to their teeth impacted on their willingness to agree to extraction. |
| Engagement in consent | Willingness or ability of the patient to engage in the process of consent and sharing decisions, including capacity to take in, weigh up and use information. |
| Family, friends and colleagues | Influence from family, friends and colleagues about appropriate treatment or legitimacy of time off work for dental problems. |
| Fear about outcome | Fear that the condition might become worse or cause a more severe problem. |
| Feelings about dentistry | Feelings such as anxiety, phobia, or desire with respect to urgent dental care. Some wished to avoid procedures/aesthetic injections, while others desired antibiotics. |
| Information and advice | Sources of information and advice about dental conditions and treatment options used by patients, including the internet. |
| Medicines knowledge | Knowledge about antibiotics and analgesics for dental conditions, including the risks and benefits of antibiotics for individuals and society. |
| Minimize disruption | Goal of appointment was to minimize disruption to their routine, such as reducing time off work by fixing the problem quickly. |
| Previous experience | Previous experience of treatment for a similar condition, such as antibiotics for pain. |
| Pain relief goal | Goal of appointment was to stop pain. |
| Trust | Degree of trust in the dental team. |
| Understanding the condition | Patient’s understanding of the causes of acute condition/symptoms |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Thompson, W.; McEachan, R.; Pavitt, S.; Douglas, G.; Bowman, M.; Boards, J.; Sandoe, J. Clinician and Patient Factors Influencing Treatment Decisions: Ethnographic Study of Antibiotic Prescribing and Operative Procedures in Out-of-Hours and General Dental Practices. Antibiotics 2020, 9, 575. https://doi.org/10.3390/antibiotics9090575
Thompson W, McEachan R, Pavitt S, Douglas G, Bowman M, Boards J, Sandoe J. Clinician and Patient Factors Influencing Treatment Decisions: Ethnographic Study of Antibiotic Prescribing and Operative Procedures in Out-of-Hours and General Dental Practices. Antibiotics. 2020; 9(9):575. https://doi.org/10.3390/antibiotics9090575
Chicago/Turabian StyleThompson, Wendy, Rosemary McEachan, Susan Pavitt, Gail Douglas, Marion Bowman, Jenny Boards, and Jonathan Sandoe. 2020. "Clinician and Patient Factors Influencing Treatment Decisions: Ethnographic Study of Antibiotic Prescribing and Operative Procedures in Out-of-Hours and General Dental Practices" Antibiotics 9, no. 9: 575. https://doi.org/10.3390/antibiotics9090575
APA StyleThompson, W., McEachan, R., Pavitt, S., Douglas, G., Bowman, M., Boards, J., & Sandoe, J. (2020). Clinician and Patient Factors Influencing Treatment Decisions: Ethnographic Study of Antibiotic Prescribing and Operative Procedures in Out-of-Hours and General Dental Practices. Antibiotics, 9(9), 575. https://doi.org/10.3390/antibiotics9090575






