Scoring System for Identification of “Survival Advantage” after Successful Percutaneous Coronary Intervention in Patients with Chronic Total Occlusion
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Definitions
2.3. Outcomes
2.4. Statistical Analysis
3. Results
3.1. Patient Characteristics
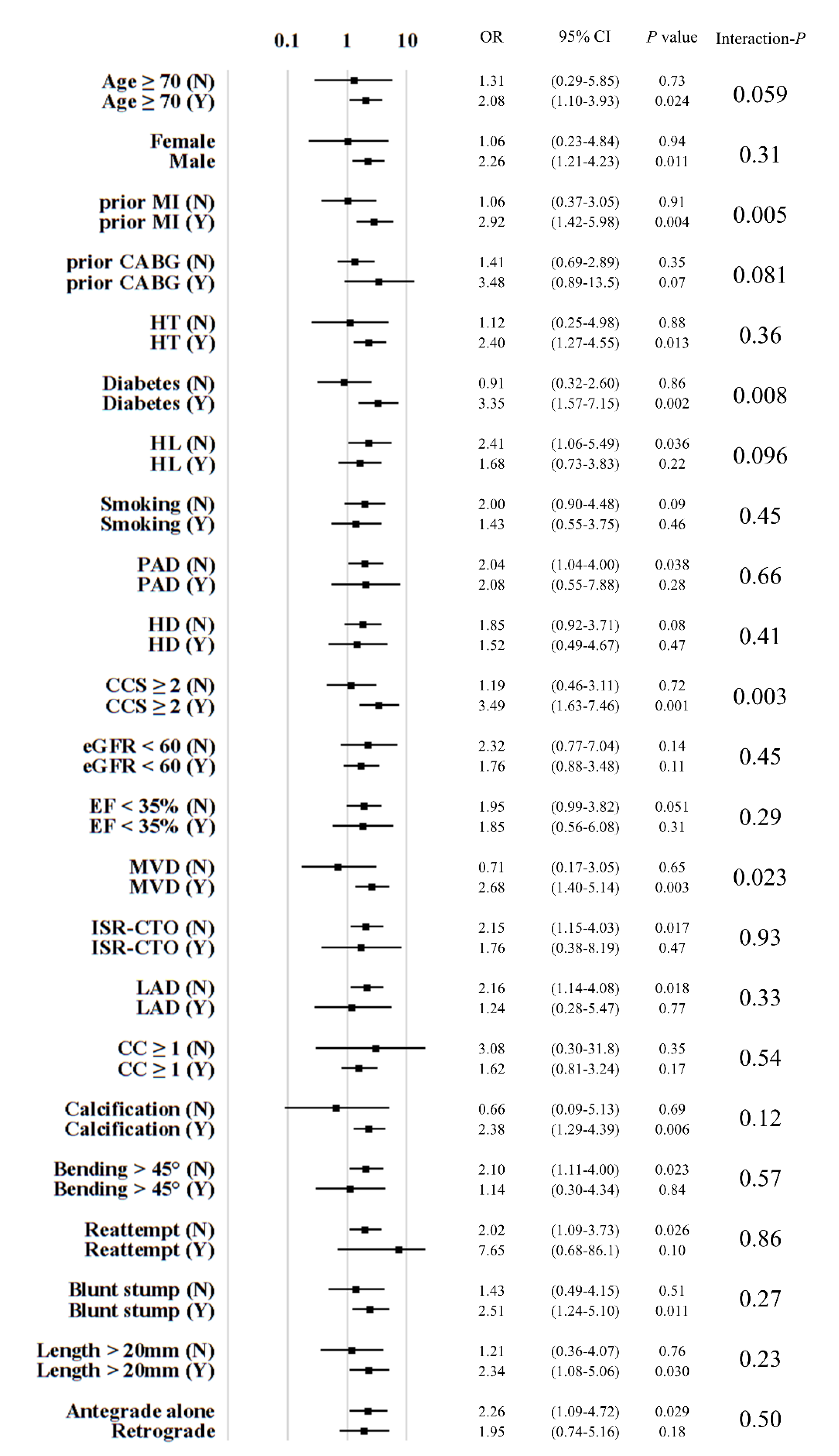
3.2. Development of a Scoring System
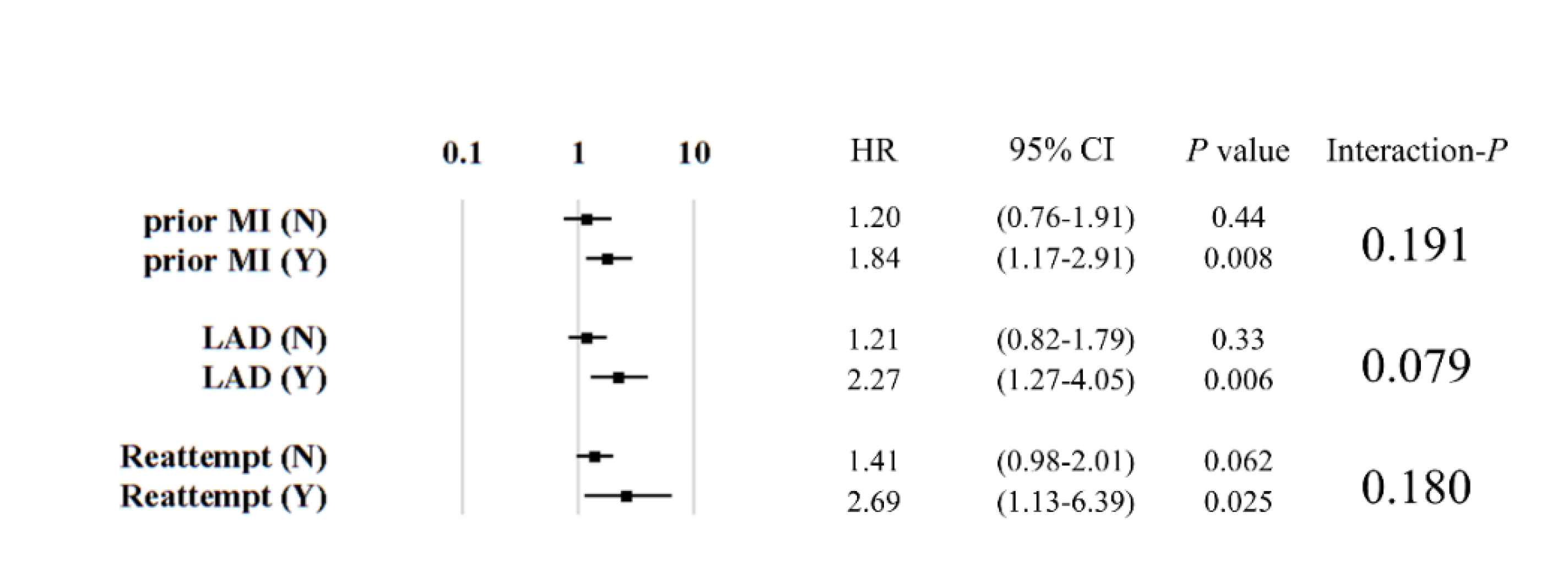
3.3. Depressed Left Ventricular (LV) Function and Involvement of the LAD
3.4. Performance of HABARA Score and J-CTO Score to be Used in Place of Each Other
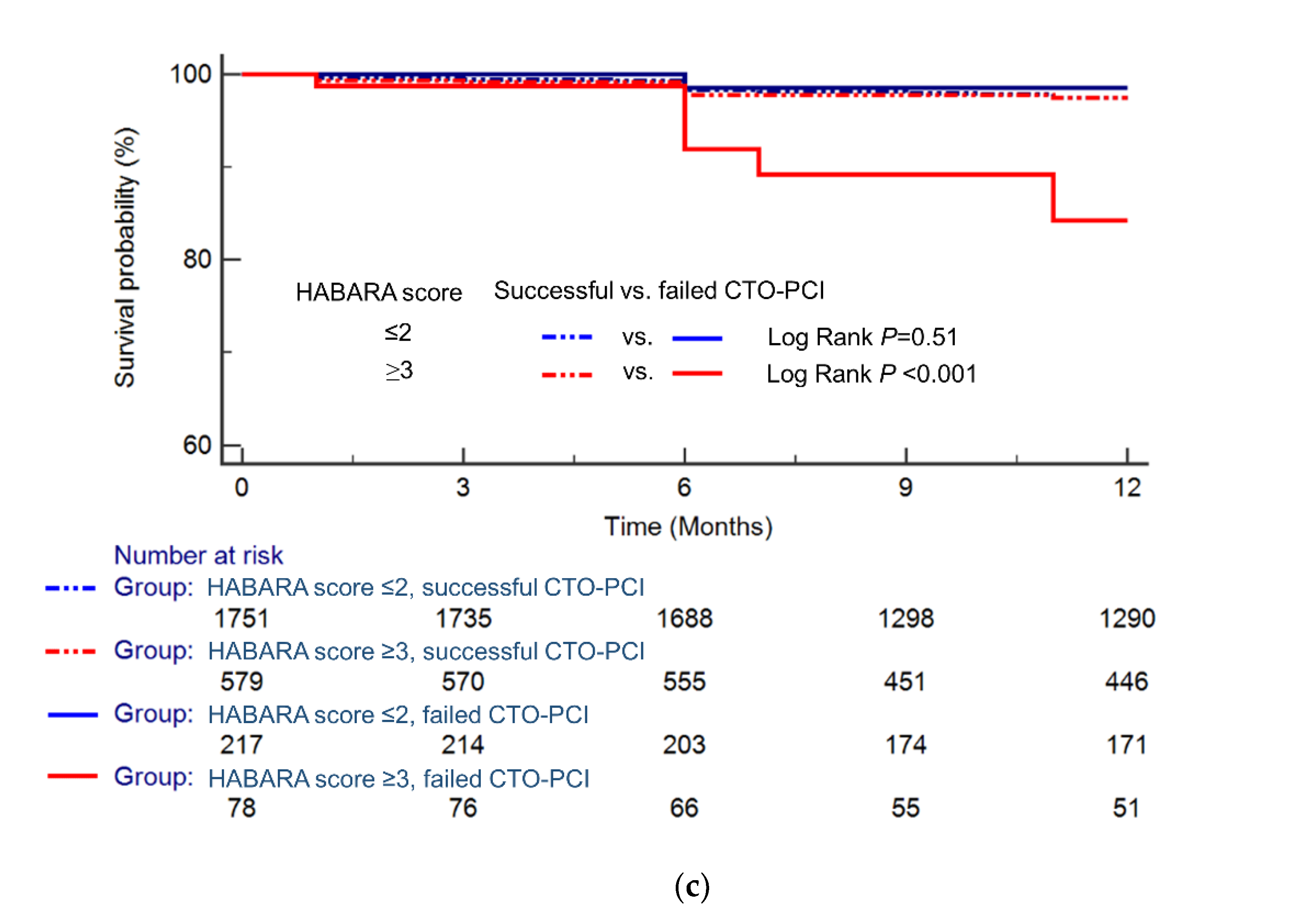
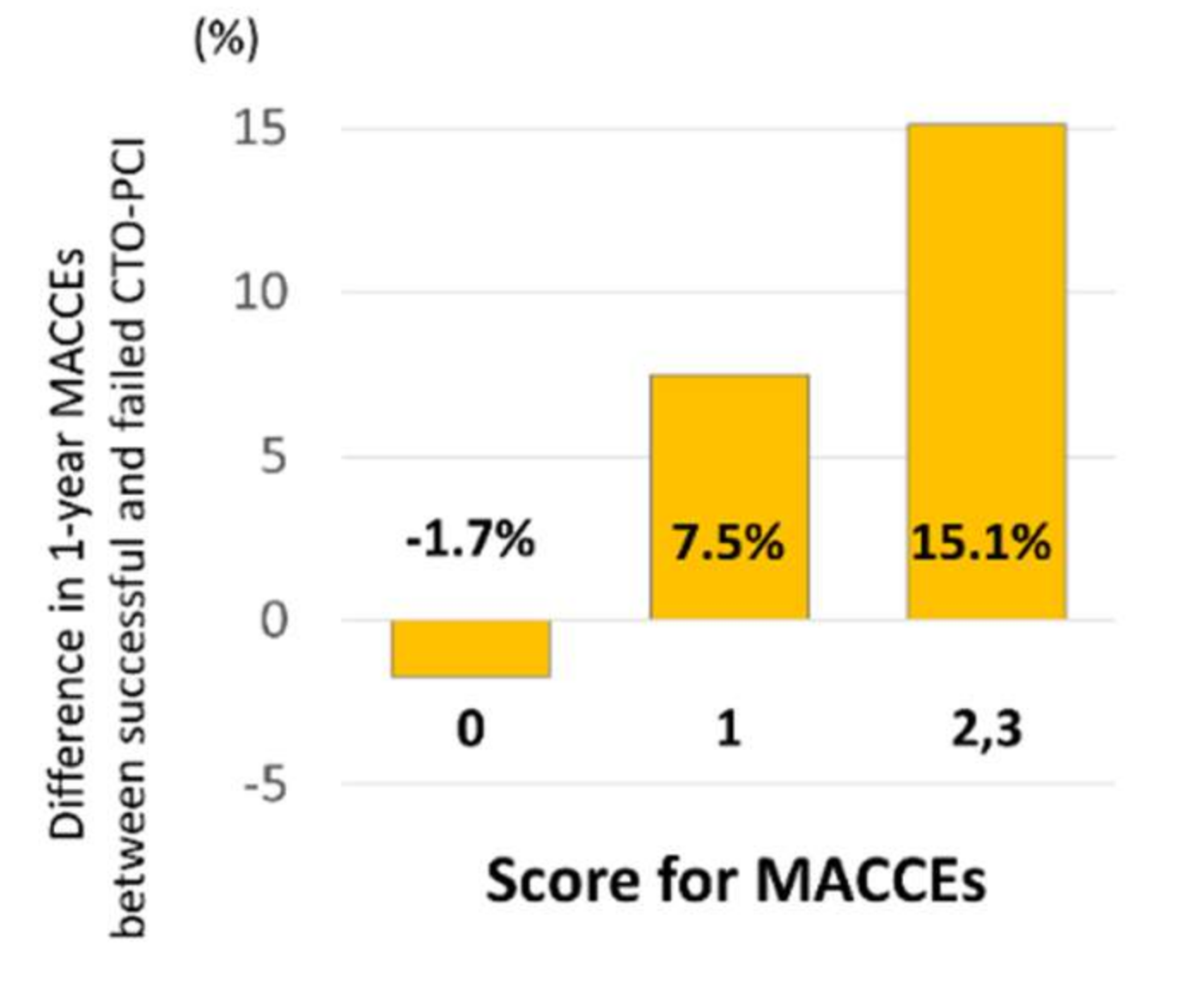
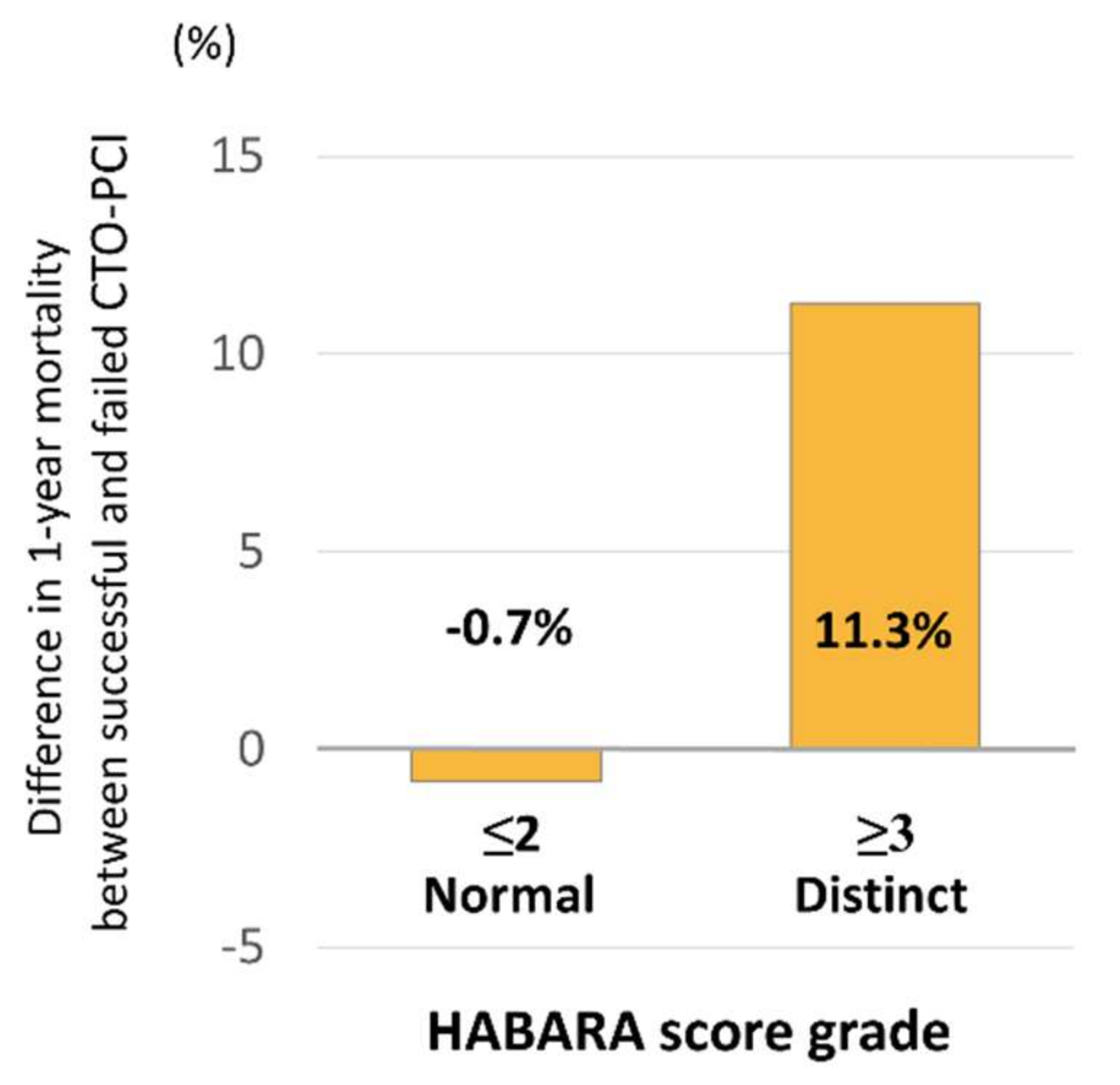
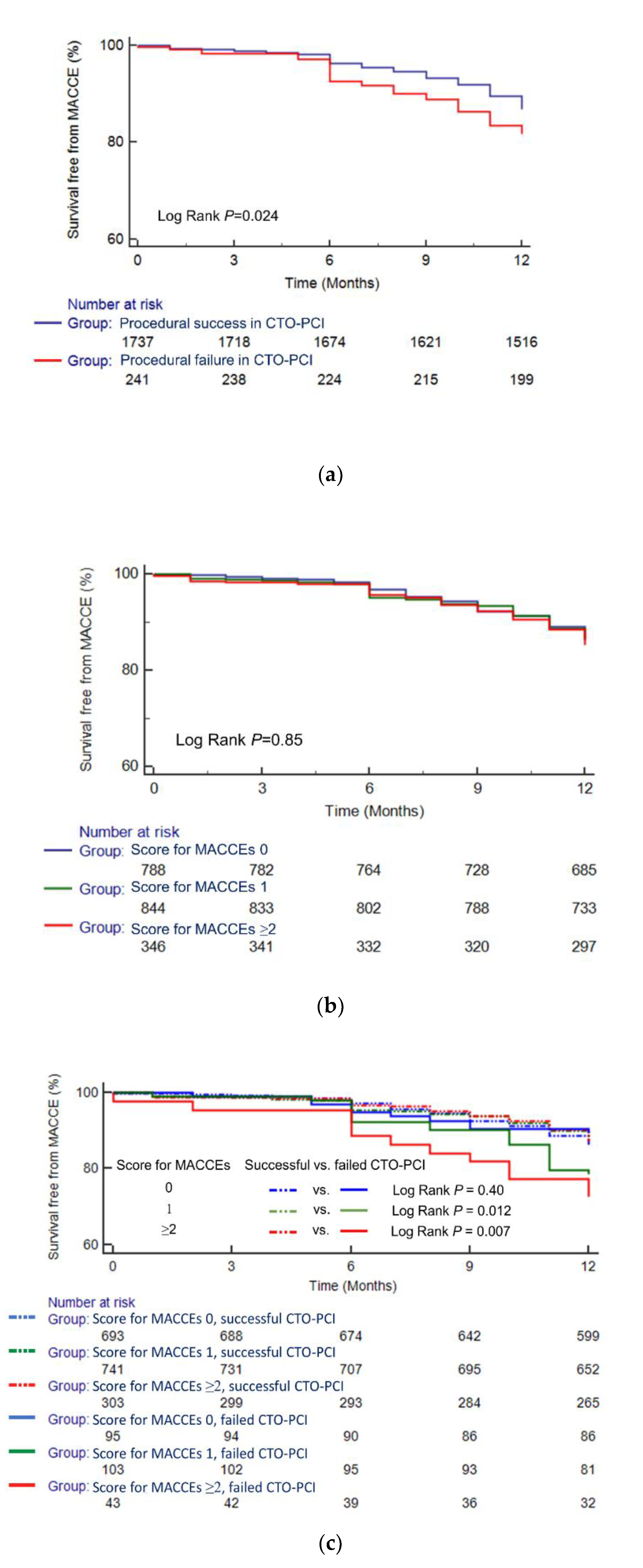
3.5. Prediction of the Influence of the Results of CTO-PCI on the MACCE Rate
4. Discussion
4.1. Utility of the HABARA Score
4.2. Score Components
4.3. Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Tsuchikane, E.; Yamane, M.; Mutoh, M.; Matsubara, T.; Fujita, T.; Nakamura, S.; Muramatsu, T.; Okamura, A.; Igarashi, Y.; Oida, A.; et al. Japanese multicenter registry evaluating the retrograde approach for chronic coronary total occlusion. Catheter. Cardiovasc. Interv. 2013, 82, E654–E661. [Google Scholar] [CrossRef] [PubMed]
- Sumitsuji, S.; Inoue, K.; Ochiai, M.; Tsuchikane, E.; Ikeno, F. Fundamental wire technique and current standard strategy of percutaneous intervention for chronic total occlusion with histopathological insights. JACC Cardiovasc. Interv. 2011, 4, 941–951. [Google Scholar] [CrossRef]
- Christopoulos, G.; Karmpaliotis, D.; Alaswad, K.; Lombardi, W.L.; Grantham, J.A.; Rangan, B.V.; Kotsia, A.P.; Lembo, N.; Kandzari, D.E.; Lee, J.; et al. The efficacy of “hybrid” percutaneous coronary intervention in chronic total occlusions caused by in-stent restenosis: Insights from a US multicenter registry. Catheter. Cardiovasc. Interv. 2014, 84, 646–651. [Google Scholar] [CrossRef] [PubMed]
- Harding, S.A.; Wu, E.B.; Lo, S.; Lim, S.T.; Ge, L.; Chen, J.Y.; Quan, J.; Lee, S.W.; Kao, H.L.; Tsuchikane, E. A new algorithm for crossing chronic total occlusions from the Asia Pacific Chronic Total Occlusion Club. JACC Cardiovasc. Interv. 2017, 10, 2135–2143. [Google Scholar] [CrossRef] [PubMed]
- Morino, Y.; Abe, M.; Morimoto, T.; Kimura, T.; Hayashi, Y.; Muramatsu, T.; Ochiai, M.; Noguchi, Y.; Kato, K.; Shibata, Y.; et al. Predicting successful guidewire crossing through chronic total occlusion of native coronary lesions within 30 minutes: The J-CTO (Multicenter CTO Registry in Japan) score as a difficulty grading and time assessment tool. JACC Cardiovasc. Interv. 2011, 4, 213–221. [Google Scholar] [CrossRef] [PubMed]
- Christopoulos, G.; Kandzari, D.E.; Yeh, R.W.; Jaffer, F.A.; Karmpaliotis, D.; Wyman, M.R.; Alaswad, K.; Lombardi, W.; Grantham, J.A.; Moses, J.; et al. Development and validation of a novel scoring system for predicting technical success of chronic total occlusion percutaneous coronary interventions: The PROGRESS CTO (Prospective Global Registry for the Study of Chronic Total Occlusion Intervention) Score. JACC Cardiovasc. Interv. 2016, 9, 1–9. [Google Scholar] [CrossRef]
- Alessandrino, G.; Chevalier, B.; Lefèvre, T.; Sanguineti, F.; Garot, P.; Unterseeh, T.; Hovasse, T.; Morice, M.C.; Louvard, Y. A clinical and angiographic scoring system to predict the probability of successful first-attempt percutaneous coronary intervention in patients with total chronic coronary occlusion. JACC Cardiovasc. Interv. 2015, 8, 1540–1548. [Google Scholar] [CrossRef]
- Szijgyarto, Z.; Rampat, R.; Werner, G.S.; Ho, C.; Reifart, N.; Lefevre, T.; Louvard, Y.; Avran, A.; Kambis, M.; Buettner, H.J.; et al. Derivation and Validation of a Chronic Total Coronary Occlusion Intervention Procedural Success Score From the 20,000-Patient EuroCTO Registry: The EuroCTO (CASTLE) Score. JACC Cardiovasc. Interv. 2019, 12, 335–342. [Google Scholar] [CrossRef]
- Karatasakis, A.; Danek, B.A.; Karmpaliotis, D.; Alaswad, K.; Jaffer, F.A.; Yeh, R.W.; Patel, M.; Bahadorani, J.N.; Lombardi, W.L.; Wyman, R.M.; et al. Comparison of various scores for predicting success of chronic total occlusion percutaneous coronary intervention. Int. J. Cardiol. 2016, 224, 50–56. [Google Scholar] [CrossRef]
- Lee, P.H.; Lee, S.W.; Park, H.S.; Kang, S.H.; Bae, B.J.; Chang, M.; Roh, J.H.; Yoon, S.H.; Ahn, J.M.; Park, D.W.; et al. Successful recanalization of native coronary chronic total occlusion is not associated with improved long-term survival. JACC Cardiovasc. Interv. 2016, 9, 530–538. [Google Scholar] [CrossRef]
- Toma, A.; Stähli, B.E.; Gick, M.; Gebhard, C.; Kaufmann, B.A.; Mashayekhi, K.; Ferenc, M.; Buettner, H.J.; Neumann, F.J. Comparison of benefit of successful percutaneous coronary intervention for chronic total occlusion in patients with versus without reduced (≤40%) left ventricular ejection fraction. Am. J. Cardiol. 2017, 120, 1780–1786. [Google Scholar] [CrossRef] [PubMed]
- Stähli, B.E.; Gebhard, C.; Gick, M.; Ferenc, M.; Mashayekhi, K.; Buettner, H.J.; Neumann, F.J.; Toma, A. Impact of anemia on long-term outcomes after percutaneous coronary intervention for chronic total occlusion. Catheter. Cardiovasc. Interv. 2018, 91, 226–233. [Google Scholar] [CrossRef]
- Nakachi, T.; Kohsaka, S.; Yamane, M.; Muramatsu, T.; Okamura, A.; Kashima, Y.; Matsuno, S.; Sakurada, M.; Kijima, M.; Tanabe, M.; et al. Impact of hemodialysis on procedural outcomes of percutaneous coronary intervention for chronic total occlusion: Insights from the Japanese Multicenter Registry. J. Am. Heart Assoc. 2017, 6, e006431. [Google Scholar] [CrossRef] [PubMed]
- Seino, Y.; Nanjo, K.; Tajima, N.; Kadowaki, T.; Kashiwagi, A.; Araki, E.; Ito, C.; Inagaki, N.; Iwamoto, Y.; Kasuga, M.; et al. Report of the committee on the classification and diagnostic criteria of diabetes mellitus. J. Diabetes. Investig. 2010, 1, 212–228. [Google Scholar] [CrossRef] [PubMed]
- Barrett, B.J.; Parfrey, P.S. Clinical practice. Preventing nephropathy induced by contrast medium. N. Engl. J. Med. 2006, 354, 379–386. [Google Scholar] [CrossRef]
- Werner, G.S.; Ferrari, M.; Heinke, S.; Kuethe, F.; Surber, R.; Richartz, B.M.; Figulla, H.R. Angiographic assessment of collateral connections in comparison with invasively determined collateral function in chronic coronary occlusions. Circulation 2003, 107, 1972–1977. [Google Scholar] [CrossRef]
- Serruys, P.W.; Morice, M.C.; Kappetein, A.P.; Colombo, A.; Holmes, D.R.; Mack, M.J.; Ståhle, E.; Feldman, T.E.; van den Brand, M.; Bass, E.J.; et al. Percutaneous coronary intervention versus coronary-artery bypass grafting for severe coronary artery disease. New Engl. J. Med. 2009, 360, 961–972. [Google Scholar] [CrossRef]
- Safley, D.M.; House, J.A.; Marso, S.P.; Grantham, J.A.; Rutherford, B.D. Improvement in survival following successful percutaneous coronary intervention of coronary chronic total occlusions: Variability by target vessel. JACC Cardiovasc. Interv. 2008, 1, 295–302. [Google Scholar] [CrossRef]
- Claessen, B.E.; Dangas, G.D.; Godino, C.; Henriques, J.P.; Leon, M.B.; Park, S.J.; Stone, G.W.; Moses, J.W.; Colombo, A.; Mehran, R.; et al. Impact of target vessel on long-term survival after percutaneous coronary intervention for chronic total occlusions. Catheter. Cardiovasc. Interv. 2013, 82, 76–82. [Google Scholar] [CrossRef]
- Mitomo, S.; Naganuma, T.; Jabbour, R.J.; Sato, K.; Takebayashi, H.; Kobayashi, T.; Obata, J.E.; Sakamoto, K.; Tsujita, K.; Kugiyama, K.; et al. Impact of target vessel on long-term cardiac mortality after successful chronic total occlusion percutaneous coronary intervention: Insights from a Japanese multicenter registry. Int. J. Cardiol. 2017, 245, 77–82. [Google Scholar] [CrossRef]
- Emond, M.; Mock, M.B.; Davis, K.B.; Fisher, L.D.; Holmes, D.R., Jr.; Chaitman, B.R.; Kaiser, G.C.; Alderman, E.; Killip, T., III. Long-term survival of medically treated patients in the Coronary Artery Surgery Study (CASS) Registry. Circulation 1994, 90, 2645–2657. [Google Scholar] [CrossRef] [PubMed]
- Olivari, Z.; Rubartelli, P.; Piscione, F.; Ettori, F.; Fontanelli, A.; Salemme, L.; Giachero, C.; Di Mario, C.; Gabrielli, G.; Spedicato, L.; et al. Immediate results and one-year clinical outcome after percutaneous coronary interventions in chronic total occlusions: Data from a multicenter, prospective, observational study (TOAST-GISE). J. Am. Coll. Cardiol. 2003, 41, 1672–1678. [Google Scholar] [CrossRef]
- Kirtane, A.J.; Doshi, D.; Leon, M.B.; Lasala, J.M.; Ohman, E.M.; O’Neill, W.W.; Shroff, A.; Cohen, M.G.; Palacios, I.F.; Beohar, N.; et al. Treatment of higher-risk patients with an indication for revascularization: Evolution within the field of contemporary percutaneous coronary intervention. Circulation 2016, 134, 422–431. [Google Scholar] [CrossRef] [PubMed]
- Kohsaka, S.; Kimura, T.; Goto, M.; Lee, V.V.; Elayda, M.; Furukawa, Y.; Fukushima, M.; Komeda, M.; Sakata, R.; Willerson, J.T.; et al. Difference in patient profiles and outcomes in Japanese versus American patients undergoing coronary revascularization (collaborative study by CREDO-Kyoto and the Texas Heart Institute Research Database). Am. J. Cardiol. 2010, 105, 1698–1704. [Google Scholar] [CrossRef] [PubMed]
- Kohsaka, S.; Miyata, H.; Ueda, I.; Masoudi, F.A.; Peterson, E.D.; Maekawa, Y.; Kawamura, A.; Fukuda, K.; Roe, M.T.; Rumsfeld, J.S.; et al. An international comparison of patients undergoing percutaneous coronary intervention: A collaborative study of the National Cardiovascular Data Registry (NCDR) and Japan Cardiovascular Database-Keio interhospital Cardiovascular Studies (JCD-KiCS). Am. Heart J. 2015, 170, 1077–1085. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Bryson, C.L.; Spertus, J.A.; McDonell, M.B.; Fihn, S.D. Anginal symptoms consistently predict total mortality among outpatients with coronary artery disease. Am. Heart J. 2003, 146, 1015–1022. [Google Scholar] [CrossRef]
- Steg, P.G.; Greenlaw, N.; Tendera, M.; Tardif, J.C.; Ferrari, R.; Al-Zaibag, M.; Dorian, P.; Hu, D.; Shalnova, S.; Sokn, F.J.; et al. Prevalence of anginal symptoms and myocardial ischemia and their effect on clinical outcomes in outpatients with stable coronary artery disease: Data from the International Observational CLARIFY Registry. JAMA Intern. Med. 2014, 174, 1651–1659. [Google Scholar] [CrossRef]
- Ermis, C.; Boz, A.; Tholakanahalli, V.; Yalcinkaya, S.; Semiz, E.; Sancaktar, O.; Benditt, D.G.; Deger, N. Assessment of percutaneous coronary intervention on regional and global left ventricular function in patients with chronic total occlusions. Can. J. Cardiol. 2005, 21, 275–280. [Google Scholar]
- Werner, G.S.; Martin-Yuste, V.; Hildick-Smith, D.; Boudou, N.; Sianos, G.; Gelev, V.; Rumoroso, J.R.; Erglis, A.; Christiansen, E.H.; Escaned, J.; et al. A randomized multicentre trial to compare revascularization with optimal medical therapy for the treatment of chronic total coronary occlusions. Eur. Heart J. 2018, 39, 2484–2493. [Google Scholar] [CrossRef]
- Sanguineti, F.; Garot, P.; O’Connor, S.; Watanabe, Y.; Spaziano, M.; Lefèvre, T.; Hovasse, T.; Benamer, H.; Unterseeh, T.; Chevalier, B.; et al. Chronic total coronary occlusion treated by percutaneous coronary intervention: Long-term outcome in patients with and without diabetes. EuroIntervention 2017, 12, e1889–e1897. [Google Scholar] [CrossRef]
- Lee, S.W.; Lee, P.H.; Ahn, J.M.; Park, D.W.; Yun, S.C.; Han, S.; Kang, H.; Kang, S.J.; Kim, Y.H.; Lee, C.W.; et al. Randomized trial evaluating percutaneous coronary intervention for the treatment of chronic total occlusion. Circulation 2019, 139, 1674–1683. [Google Scholar] [CrossRef] [PubMed]
- King, S.B., III; Gogas, B.D. Opening chronic coronary total occlusions: Light in the tunnel or sleeping in Seattle? Eur Heart J. 2018, 39, 2494–2496. [Google Scholar] [CrossRef] [PubMed]
- Nakachi, T.; Kato, S.; Kirigaya, H.; Iinuma, N.; Fukui, K.; Saito, N.; Iwasawa, T.; Kosuge, M.; Kimura, K.; Tamura, K. Prediction of functional recovery after percutaneous coronary revascularization for chronic total occlusion using late gadolinium enhanced magnetic resonance imaging. J. Cardiol. 2017, 69, 836–842. [Google Scholar] [CrossRef] [PubMed]



| Successful CTO-PCI | Failed CTO-PCI | P Value | |
|---|---|---|---|
| (n = 2330) | (n = 295) | ||
| Clinical characteristics | |||
| Age, years | 68 ± 10 | 69 ± 10 | 0.22 |
| Male | 1950 (84%) | 241 (82%) | 0.32 |
| Prior MI | 861 (38%) | 112 (39%) | 0.79 |
| Prior CABG | 179 (8%) | 44 (15%) | <0.001 |
| Hypertension | 1806 (78%) | 246 (84%) | 0.026 |
| Diabetes mellitus | 1014 (44%) | 128 (44%) | 0.93 |
| Hyperlipidemia | 1639 (71%) | 204 (70%) | 0.76 |
| Smoker | 1177 (54%) | 134 (48%) | 0.09 |
| Peripheral vascular disease | 273 (13%) | 41 (15%) | 0.27 |
| Hemodialysis | 114 (5%) | 33 (12%) | <0.001 |
| CCS 0 | 755 (34%) | 96 (33%) | 0.61 |
| CCS I | 630 (28%) | 92 (32%) | |
| CCS II | 656 (29%) | 82 (28%) | |
| CCS III | 144 (6%) | 14 (5%) | |
| CCS IV | 51 (2%) | 5 (2%) | |
| Cr, mg/dL | 1.4 ± 2.2 | 1.8 ± 2.6 | 0.001 |
| eGFR, mL/min/1.73 m2 | 61.9 ± 22.7 | 59.5 ± 49.3 | 0.153 |
| LVEF | |||
| <35% | 176 (8%) | 29 (10%) | 0.32 |
| 35%–50% | 513 (23%) | 70 (25%) | |
| >50% | 1523 (69%) | 185 (65%) | |
| Cerebrovascular disease | 92 (4%) | 17 (6%) | 0.14 |
| Angiographic characteristics | |||
| Multivessel disease | 1376 (60%) | 192 (66%) | 0.07 |
| CTO vessel | |||
| Right | 1073 (46%) | 159 (54%) | 0.012 |
| Left anterior descending | 745 (32%) | 67 (23%) | |
| Left circumferential | 497 (21%) | 68 (23%) | |
| Left main trunk | 8 (0.3%) | 1 (0.3%) | |
| In-stent occlusion | 360 (16%) | 35 (12%) | 0.102 |
| Blunt stump | 1222 (53%) | 185 (64%) | 0.001 |
| Lesion calcification | 1843 (80%) | 239 (83%) | 0.242 |
| Lesion bending | 174 (8%) | 46 (10%) | <0.001 |
| Occlusion length ≥20 mm | 988 (51%) | 136 (62%) | 0.003 |
| Reattempted lesion | 200 (9%) | 54 (19%) | <0.001 |
| Collateral channel classification | |||
| CC0 | 123 (6%) | 14 (6%) | 0.54 |
| CC1 | 1243 (64%) | 161 (68%) | |
| CC2 | 575 (30%) | 63 (27%) | |
| J-CTO score | 1.90±0.99 | 2.24±1.06 | <0.001 |
| Procedural characteristics | |||
| Air kerma, mGy | 4534 ± 4408 | 6175 ± 4661 | <0.001 |
| Procedural time, min | 149 ± 86 | 196 ± 94 | <0.001 |
| Fluoroscopy time, min | 66 ± 45 | 96 ± 52 | <0.001 |
| Contrast dose, mL | 214 ± 99 | 237 ± 119 | <0.001 |
| Retrograde procedure | 664 (29%) | 149 (51%) | <0.001 |
| Periprocedural complications | |||
| Periprocedural MI | 0 (0%) | 10 (3%) | <0.001 |
| Symptomatic cerebrovascular disease | 0 (0%) | 4 (1.4%) | <0.001 |
| Coronary perforation | 51 (2.2%) | 23 (7.9%) | <0.001 |
| Access site bleeding | 8 (0.3%) | 5 (1.7%) | 0.002 |
| Heart failure | 0 (0%) | 0 (0%) | - |
| Emergency CABG | 0 (0%) | 0 (0%) | - |
| Emergency TVR | 0 (0%) | 0 (0%) | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nakachi, T.; Kohsaka, S.; Yamane, M.; Muramatsu, T.; Okamura, A.; Kashima, Y.; Matsuno, S.; Sakurada, M.; Seino, Y.; Habara, M. Scoring System for Identification of “Survival Advantage” after Successful Percutaneous Coronary Intervention in Patients with Chronic Total Occlusion. J. Clin. Med. 2020, 9, 1319. https://doi.org/10.3390/jcm9051319
Nakachi T, Kohsaka S, Yamane M, Muramatsu T, Okamura A, Kashima Y, Matsuno S, Sakurada M, Seino Y, Habara M. Scoring System for Identification of “Survival Advantage” after Successful Percutaneous Coronary Intervention in Patients with Chronic Total Occlusion. Journal of Clinical Medicine. 2020; 9(5):1319. https://doi.org/10.3390/jcm9051319
Chicago/Turabian StyleNakachi, Tatsuya, Shun Kohsaka, Masahisa Yamane, Toshiya Muramatsu, Atsunori Okamura, Yoshifumi Kashima, Shunsuke Matsuno, Masami Sakurada, Yoshitane Seino, and Maoto Habara. 2020. "Scoring System for Identification of “Survival Advantage” after Successful Percutaneous Coronary Intervention in Patients with Chronic Total Occlusion" Journal of Clinical Medicine 9, no. 5: 1319. https://doi.org/10.3390/jcm9051319
APA StyleNakachi, T., Kohsaka, S., Yamane, M., Muramatsu, T., Okamura, A., Kashima, Y., Matsuno, S., Sakurada, M., Seino, Y., & Habara, M. (2020). Scoring System for Identification of “Survival Advantage” after Successful Percutaneous Coronary Intervention in Patients with Chronic Total Occlusion. Journal of Clinical Medicine, 9(5), 1319. https://doi.org/10.3390/jcm9051319





