Comparison of the Use of Arterial Doppler Waveform Classifications in Clinical Routine to Describe Lower Limb Flow
Abstract
1. Introduction
2. Experimental Section
2.1. Study Design and Population
2.2. Classifications
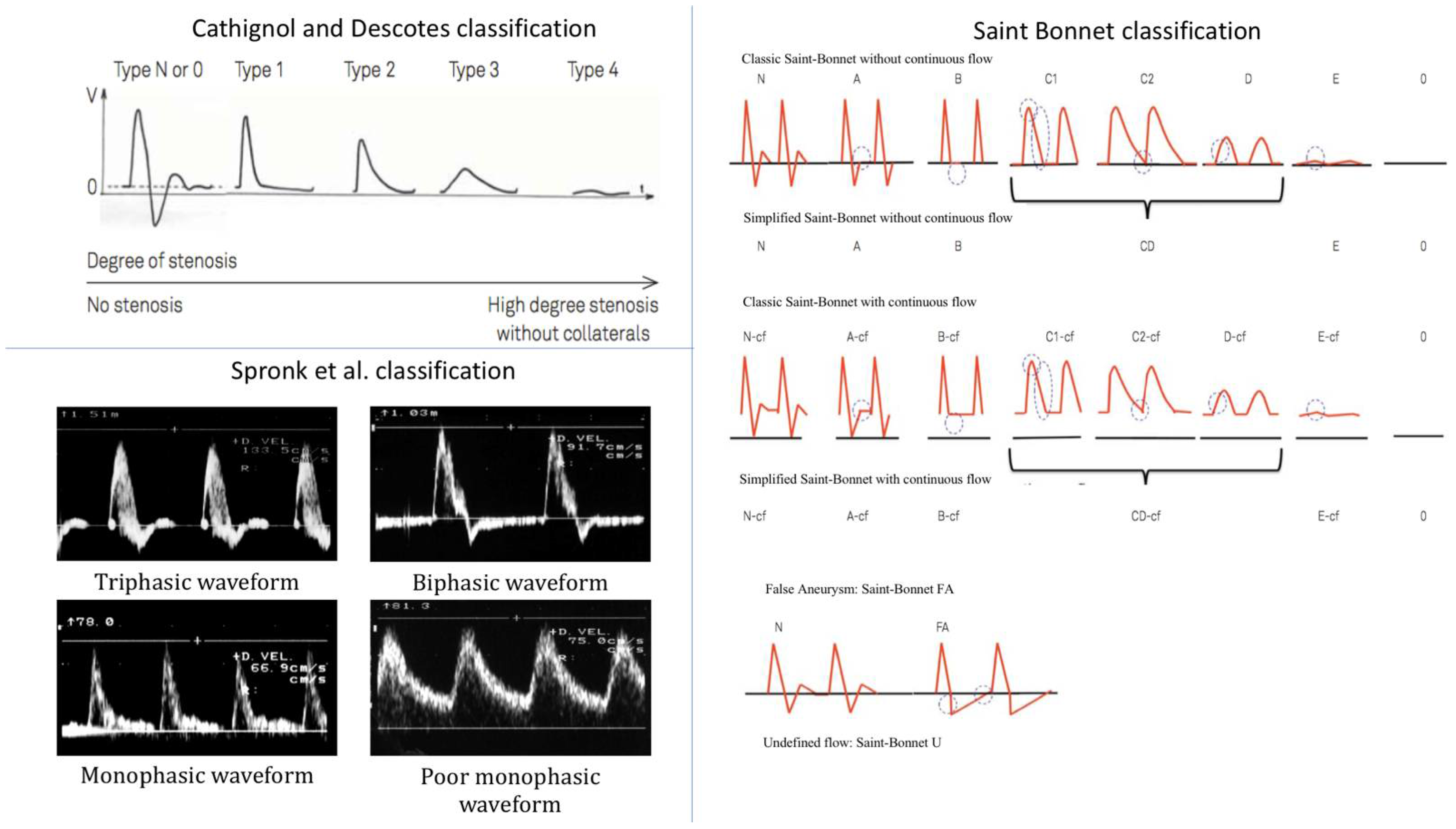
2.2.1. Descotes and Cathignol Classification
2.2.2. Spronk et al. Classification
2.2.3. The Simplified Saint-Bonnet Classification
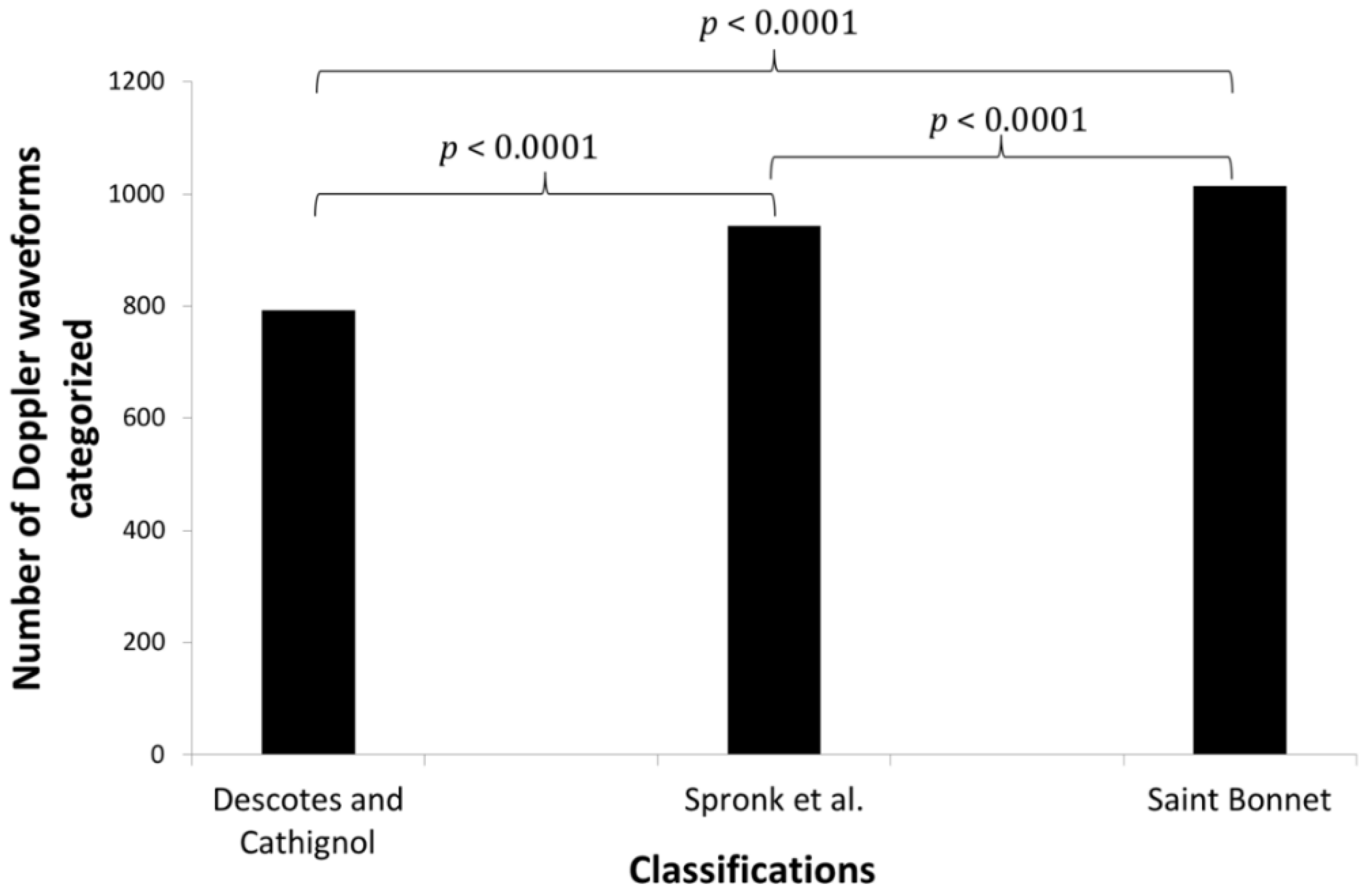
2.3. Statistics
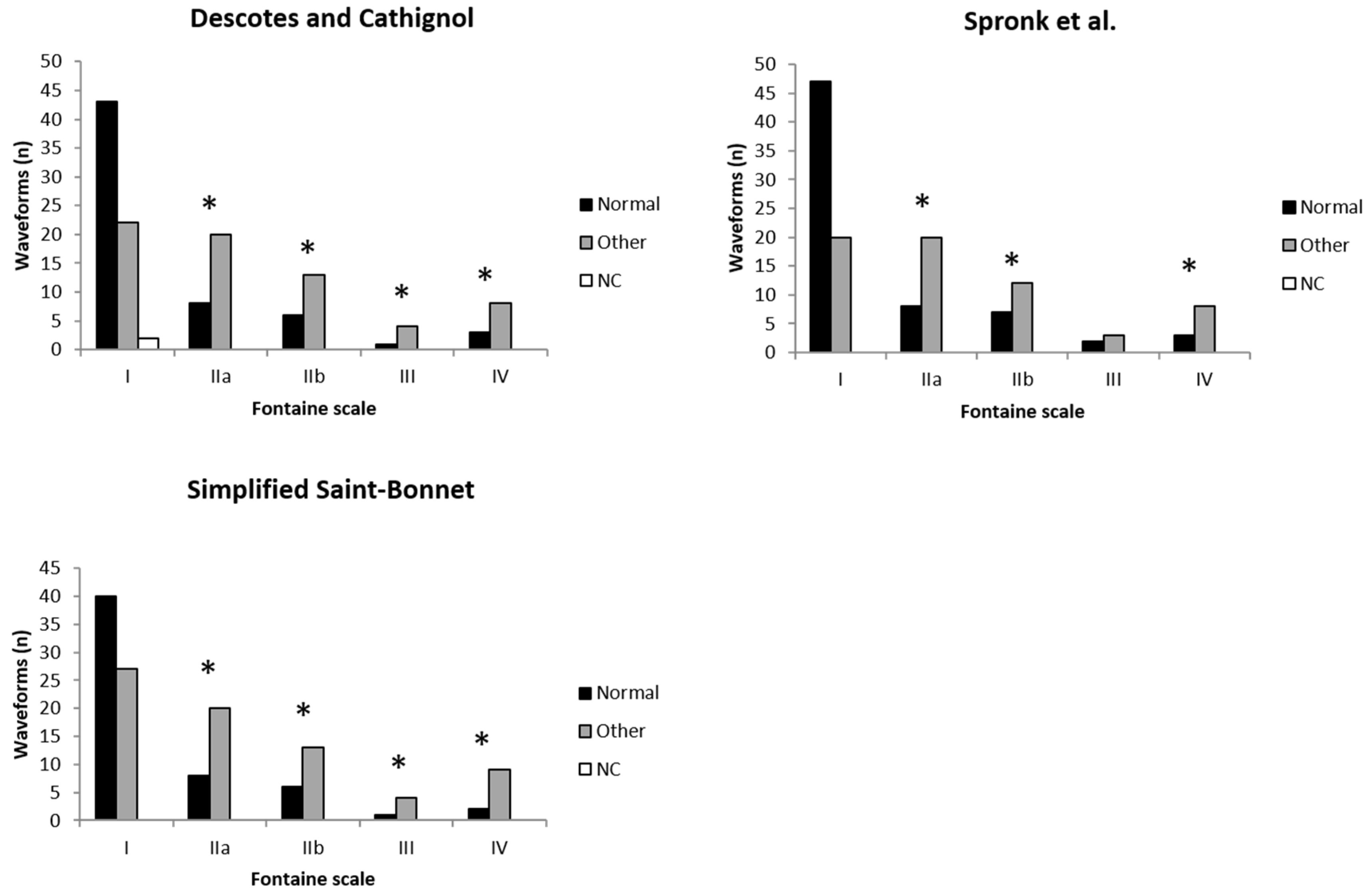
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Fowkes, F.G.R.; Rudan, D.; Rudan, I.; Aboyans, V.; Denenberg, J.O.; McDermott, M.M.; Norman, P.E.; Sampson, U.K.; Williams, L.J.; Mensah, G.A.; et al. Comparison of global estimates of prevalence and risk factors for peripheral artery disease in 2000 and 2010: A systematic review and analysis. Lancet 2013, 382, 1329–1340. [Google Scholar] [CrossRef]
- Criqui, M.H. Peripheral arterial disease—Epidemiological aspects. Vasc. Med. 2001, 6, 3–7. [Google Scholar] [CrossRef] [PubMed]
- Fowkes, F.G.; Housley, E.; Cawood, E.H.; Macintyre, C.C.; Ruckley, C.V.; Prescott, R.J. Edinburgh Artery Study: Prevalence of asymptomatic and symptomatic peripheral arterial disease in the general population. Int. J. Epidemiol. 1991, 20, 384–392. [Google Scholar] [CrossRef] [PubMed]
- Hirsch, A.T.; Criqui, M.H.; Treat-Jacobson, D.; Regensteiner, J.G.; Creager, M.A.; Olin, J.W.; Krook, S.H.; Hunninghake, D.B.; Comerota, A.J.; Walsh, M.E.; et al. Peripheral arterial disease detection, awareness, and treatment in primary care. JAMA 2001, 286, 1317–1324. [Google Scholar] [CrossRef] [PubMed]
- Hirsch, A.T.; Hartman, L.; Town, R.J.; Virnig, B.A. National health care costs of peripheral arterial disease in the Medicare population. Vasc. Med. 2008, 13, 209–215. [Google Scholar] [CrossRef]
- Bura Riviere, A.; Bouée, S.; Laurendeau, C.; Torreton, E.; Gourmelen, J.; Thomas-Delecourt, F. Outcomes and management costs of peripheral arterial disease in France. J. Vasc. Surg. 2018, 67, 1834–1843. [Google Scholar] [CrossRef]
- Mahoney, E.M.; Wang, K.; Keo, H.H.; Duval, S.; Smolderen, K.G.; Cohen, D.J.; Steg, G.; Bhatt, D.L.; Hirsch, A.T. Vascular Hospitalization Rates and Costs in Patients with Peripheral Artery Disease in the United States. Circ. Cardiovasc. Qual. Outcomes 2010, 3, 642–651. [Google Scholar] [CrossRef]
- Scully, R.E.; Smith, A.D.; Arnaoutakis, D.J.; Semel, M.; Nguyen, L.L. Annual Health Care Expenditures in Individuals with Peripheral Arterial Disease. J. Vasc. Surg. 2016, 64, 1180–1181. [Google Scholar] [CrossRef][Green Version]
- Aboyans, V.; Ricco, J.-B.; Bartelink, M.-L.E.L.; Björck, M.; Brodmann, M.; Cohnert, T.; Collet, J.-P.; Czerny, M.; De Carlo, M.; Debus, S.; et al. 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS) Document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteries Endorsed by: The European Stroke Organization (ESO) The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). Eur. Heart J. 2018, 39, 763–816. [Google Scholar] [CrossRef]
- Gerhard-Herman, M.D.; Gornik, H.L.; Barrett, C.; Barshes, N.R.; Corriere, M.A.; Drachman, D.E.; Fleisher, L.A.; Fowkes, F.G.R.; Hamburg, N.M.; Kinlay, S.; et al. AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J. Am. Coll. Cardiol. 2017, 69, 1465–1508. [Google Scholar] [CrossRef]
- Hyun, S.; Forbang, N.I.; Allison, M.A.; Denenberg, J.O.; Criqui, M.H.; Ix, J.H. Ankle-brachial index, toe-brachial index, and cardiovascular mortality in persons with and without diabetes mellitus. J. Vasc. Surg. 2014, 60, 390–395. [Google Scholar] [CrossRef] [PubMed]
- Xu, D.; Li, J.; Zou, L.; Xu, Y.; Hu, D.; Pagoto, S.L.; Ma, Y. Sensitivity and specificity of the ankle—Brachial index to diagnose peripheral artery disease: A structured review. Vasc. Med. 2010, 15, 361–369. [Google Scholar] [CrossRef]
- Høyer, C.; Sandermann, J.; Petersen, L.J. The toe-brachial index in the diagnosis of peripheral arterial disease. J. Vasc. Surg. 2013, 58, 231–238. [Google Scholar] [CrossRef] [PubMed]
- Stoekenbroek, R.M.; Ubbink, D.T.; Reekers, J.A.; Koelemay, M.J.W. Hide and Seek: Does the Toe-brachial Index Allow for Earlier Recognition of Peripheral Arterial Disease in Diabetic Patients? Eur. J. Vasc. Endovasc. Surg. 2015, 49, 192–198. [Google Scholar] [CrossRef] [PubMed]
- Gerhard-Herman, M.D.; Gornik, H.L.; Barrett, C.; Barshes, N.R.; Corriere, M.A.; Drachman, D.E.; Fleisher, L.A.; Fowkes, F.G.R.; Hamburg, N.M.; Kinlay, S.; et al. AHA/ACC Guideline on the Management of Patients With Lower Extremity Peripheral Artery Disease: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 2017, 135, e726–e779. [Google Scholar] [CrossRef]
- Campbell, W.B. Doppler waveform analysis in the management of lower limb arterial disease. Ann. R. Coll. Surg. Engl. 1986, 68, 103–106. [Google Scholar]
- Poe, P. Lower-Extremity Arterial Continuous-Wave Doppler Evaluation. J. Vasc. Ultrasound 2012, 36, 123–134. [Google Scholar] [CrossRef]
- Strandness, D.E.; Schultz, R.D.; Sumner, D.S.; Rushmer, R.F. Ultrasonic Flow Detection A Useful Technic in the Evaluation of Peripheral Vascular Disease. Am. J. Surg. 1967, 113, 311–320. [Google Scholar] [CrossRef]
- Dean, R.H.; Yao, J.S.T. Hemodynamic measurements in peripheral vascular disease. Curr. Probl. Surg. 1976, 13, 1–76. [Google Scholar] [CrossRef]
- Scissons, R.; Comerota, A. Confusion of Peripheral Arterial Doppler Waveform Terminology. J. Diagn. Med. Sonogr. 2009, 25, 185–194. [Google Scholar] [CrossRef]
- Scissons, R. Characterizing Triphasic, Biphasic, and Monophasic Doppler Waveforms: Should a Simple Task Be So Difficult? J. Diagn. Med. Sonogr. 2008, 24, 269–276. [Google Scholar] [CrossRef]
- Omarjee, L.; Stivalet, O.; Hoffmann, C.; Scissons, R.; Bressollette, L.; Mahé, G.; Jaquinandi, V. Heterogeneity of Doppler waveform description is decreased with the use of a dedicated classification. Vasa 2018, 47, 471–474. [Google Scholar] [CrossRef] [PubMed]
- Descotes, J.; Cathignol, D. Classifi cation of changes in circulatory rate in the arteries of the lower limbs. Transcutaneous measurement by Doppler effect. Nouv Presse Med. 1975, 4, 2091–2093. [Google Scholar] [PubMed]
- Spronk, S.; den Hoed, P.T.; de Jonge, L.C.W.; van Dijk, L.C.; Pattynama, P.M.T. Value of the duplex waveform at the common femoral artery for diagnosing obstructive aortoiliac disease. J. Vasc. Surg. 2005, 42, 236–242. [Google Scholar] [CrossRef]
- Mahé, G.; Boulon, C.; Desormais, I.; Lacroix, P.; Bressollette, L.; Guilmot, J.-L.; Le Hello, C.; Sevestre, M.-A.; Pernod, G.; Constans, J.; et al. Statement for Doppler waveforms analysis. Vasa 2017, 46, 337–345. [Google Scholar] [CrossRef]
- Fontaine, R.; Kim, M.; Kieny, R. Surgical treatment of peripheral circulation disorders. Helv. Chir. Acta 1954, 21, 499–533. [Google Scholar]
- Aboyans, V.; Criqui, M.H.; Abraham, P.; Allison, M.A.; Creager, M.A.; Diehm, C.; Fowkes, F.G.R.; Hiatt, W.R.; Jönsson, B.; Lacroix, P.; et al. Measurement and Interpretation of the Ankle-Brachial Index: A Scientific Statement from the American Heart Association. Circulation 2012, 126, 2890–2909. [Google Scholar] [CrossRef]
- Nicolaïdes, A.; Yao, S. Investigation of Vascular Disorders; Churchill Livingston: New York, NY, USA, 1981. [Google Scholar]
| Characteristics | Patients (n = 130) |
|---|---|
| Male (%) | 81 (62.3) |
| Female (%) | 49 (37.7) |
| Age (years) | 68 ± 11 |
| BMI (kg/m2) | 26.97 ± 6.2 |
| ABPI | Right: 1.01 ± 0.4 Left: 0.98 ± 0.39 |
| BP (mmHg) | 137± 25/75 ± 12 |
| CAD (%) | 33 (25.4) |
| Angioplasty (%) | 38 (29.2) |
| Stroke (%) | 17 (13.1) |
| AHT (%) | 94 (72.3) |
| Dyslipidaemia (%) | 82 (63.1) |
| Diabetes (%) | 44 (33.8) |
| Smokers (%) | 43 (33.1) |
| Fontaine scale | |
| Grade I (%) | 67 (51.5) |
| Grade IIa (%) | 28 (21.5) |
| Grade IIb (%) | 19 (14.6) |
| Grade III (%) | 5 (3.8) |
| Grade IV (%) | 11 (8.5) |
| Simplified Saint-Bonnet | Spronk et al. | Descotes and Cathignol | |||
|---|---|---|---|---|---|
| N = 1033 | N = 1033 | N = 1033 | |||
| N | 389 | Triphasic | 407 | Type N | 508 |
| A | 283 | Biphasic | 277 | Type 1 | 85 |
| B | 24 | Sharp monophasic | 124 | Type 2 | 98 |
| CD | 64 | Poor monophasic | 86 | Type 3 | 49 |
| E | 0 | No flow | 49 | Type 4 | 3 |
| N-CF | 52 | NC | 90 | No flow | 50 |
| A-CF | 10 | NC | 240 | ||
| B-CF | 27 | ||||
| CD-CF | 115 | ||||
| E-CF | 1 | ||||
| No flow | 49 | ||||
| NC | 19 | ||||
| Saint-Bonnet | Spronk et al. | Descotes and Cathignol | |||||
|---|---|---|---|---|---|---|---|
| NC | C | NC | C | NC | C | ||
| Saint-Bonnet | |||||||
| NC | 19 | 11 (58%) | 8 (42%) | 16 (84%) | 3 (16%) | ||
| Spronk et al. | |||||||
| NC | 90 | 11 (12%) | 79 (88%) | 64 (71%) | 26 (29%) | ||
| Descotes and Cathignol | |||||||
| NC | 240 | 16 (7%) | 234 (93) | 64 (27%) | 176 (73) | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Guilcher, A.; Lanéelle, D.; Hoffmann, C.; Guillaumat, J.; Constans, J.; Bressollette, L.; Le Hello, C.; Boissier, C.; Bura-Rivière, A.; Jaquinandi, V.; et al. Comparison of the Use of Arterial Doppler Waveform Classifications in Clinical Routine to Describe Lower Limb Flow. J. Clin. Med. 2021, 10, 464. https://doi.org/10.3390/jcm10030464
Guilcher A, Lanéelle D, Hoffmann C, Guillaumat J, Constans J, Bressollette L, Le Hello C, Boissier C, Bura-Rivière A, Jaquinandi V, et al. Comparison of the Use of Arterial Doppler Waveform Classifications in Clinical Routine to Describe Lower Limb Flow. Journal of Clinical Medicine. 2021; 10(3):464. https://doi.org/10.3390/jcm10030464
Chicago/Turabian StyleGuilcher, Antoine, Damien Lanéelle, Clément Hoffmann, Jérôme Guillaumat, Joel Constans, Luc Bressollette, Claire Le Hello, Christian Boissier, Alessandra Bura-Rivière, Vincent Jaquinandi, and et al. 2021. "Comparison of the Use of Arterial Doppler Waveform Classifications in Clinical Routine to Describe Lower Limb Flow" Journal of Clinical Medicine 10, no. 3: 464. https://doi.org/10.3390/jcm10030464
APA StyleGuilcher, A., Lanéelle, D., Hoffmann, C., Guillaumat, J., Constans, J., Bressollette, L., Le Hello, C., Boissier, C., Bura-Rivière, A., Jaquinandi, V., Omarjee, L., Lacroix, P., Pernod, G., Abbadie, F., Sevestre, M. A., Boulon, C., & Mahé, G. (2021). Comparison of the Use of Arterial Doppler Waveform Classifications in Clinical Routine to Describe Lower Limb Flow. Journal of Clinical Medicine, 10(3), 464. https://doi.org/10.3390/jcm10030464





