Overview on the Evolution of Laser Welding of Vascular and Nervous Tissues
Abstract
1. Introduction
2. Laser Welding of Vascular and Nervous Tissues
2.1. Contextualization
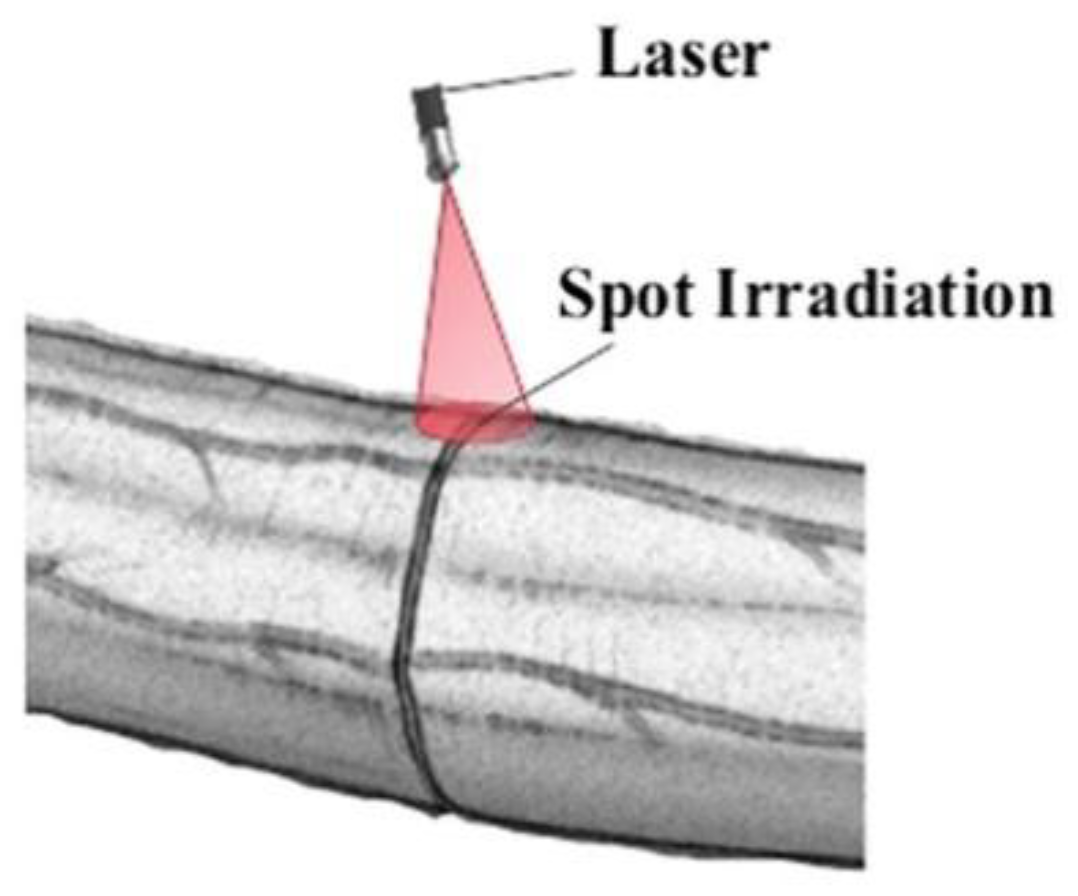
2.2. Welding Procedure
2.3. Laser Technology
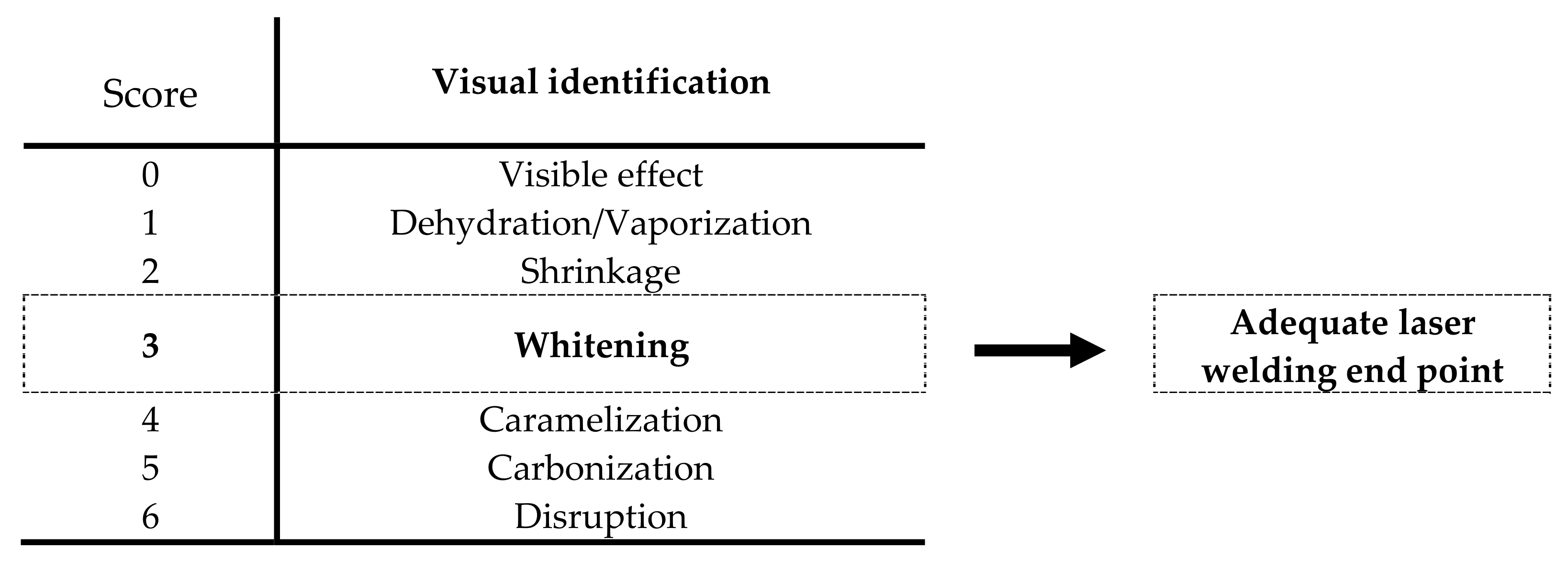
2.4. Welding Parameters and Bonding Conditions
3. Conclusions
- Although laser welding presents many advantages, such as increased accuracy, decreased operative time, reduction of foreign-body reactions, and reduction of aneurysms formation, an accurate control of several process variables is required. The laser type and parameters, the exposure time, the tissue apposition, the temperature, and the absorptive conditions present high relevance.
- Thermal damage may occur in vascular and nervous laser welding. Different strategies have been tested to overcome this concern. Temperature-controlled feedback systems present the advantage of reducing the thermal damage with a very precise control of the laser parameters.
- The bonding strength of vascular and nerve welds can be enhanced with the application of solder solutions, bonding materials, and laser-activated dyes. The use of dyes with albumin-based solution solders has presented an especially beneficial effect on the welding conditions.
- Alternative techniques to thermal laser welding, such as photochemical tissue bonding and electrosurgical high-frequency technologies, have been tested for vascular and nervous repairs.
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Costa, A.M.S.; Oliveira, J.P.; Pereira, V.F.; Nunes, C.A.; Ramirez, A.J.; Tschiptschin, A.P. Ni-Based Mar-M247 Superalloy as a Friction Stir Processing Tool. J. Mater. Process. Technol. 2018, 262, 605–614. [Google Scholar] [CrossRef]
- Liu, F.C.; Hovanski, Y.; Miles, M.P.; Sorensen, C.D.; Nelson, T.W. A Review of Friction Stir Welding of Steels: Tool, Material Flow, Microstructure, and Properties. J. Mater. Sci. Technol. 2018, 34, 39–57. [Google Scholar] [CrossRef]
- Jedrasiak, P.; Shercliff, H.R. Finite Element Analysis of Heat Generation in Dissimilar Alloy Ultrasonic Welding. Mater. Des. 2018, 158, 184–197. [Google Scholar] [CrossRef]
- Goto, K.; Imai, K.; Arai, M.; Ishikawa, T. Shear and Tensile Joint Strengths of Carbon Fiber-Reinforced Thermoplastics Using Ultrasonic Welding. Compos. Part A Appl. Sci. Manuf. 2019, 116, 126–137. [Google Scholar] [CrossRef]
- Assari, A.H.; Eghbali, B. Solid State Diffusion Bonding Characteristics at the Interfaces of Ti and Al Layers. J. Alloys Compd. 2019, 773, 50–58. [Google Scholar] [CrossRef]
- Varmazyar, J.; Khodaei, M. Diffusion Bonding of Aluminum-Magnesium Using Cold Rolled Copper Interlayer. J. Alloys Compd. 2019, 773, 838–843. [Google Scholar] [CrossRef]
- Lueg-Althoff, J.; Bellmann, J.; Gies, S.; Schulze, S.; Tekkaya, A.E.; Beyer, E. Influence of the Flyer Kinetics on Magnetic Pulse Welding of Tubes. J. Mater. Process. Technol. 2018, 262, 189–203. [Google Scholar] [CrossRef]
- Cui, J.; Li, Y.; Liu, Q.; Zhang, X.; Xu, Z.; Li, G. Joining of Tubular Carbon Fiber-Reinforced Plastic/Aluminum by Magnetic Pulse Welding. J. Mater. Process. Technol. 2019, 264, 273–282. [Google Scholar] [CrossRef]
- Mehrpouya, M.; Gisario, A.; Brotzu, A.; Natali, S. Laser Welding of NiTi Shape Memory Sheets Using a Diode Laser. Opt. Laser Technol. 2018, 108, 142–149. [Google Scholar] [CrossRef]
- Yao, R.; Dong, P.; Liaw, P.K.; Zhou, J.; Wang, W. Microstructure and Shape Memory Effect of Laser Welded Nitinol Wires. Mater. Lett. 2019, 238, 1–5. [Google Scholar] [CrossRef]
- Rezaei, M.-A.; Naffakh-Moosavy, H. The Effect of Pre-Cold Treatment on Microstructure, Weldability and Mechanical Properties in Laser Welding of Superalloys. J. Manuf. Process. 2018, 34, 339–348. [Google Scholar] [CrossRef]
- Hu, X.; Xue, Z.; Zhao, G.; Yun, J.; Shi, D.; Yang, X. Laser Welding of a Selective Laser Melted Ni-Base Superalloy: Microstructure and High Temperature Mechanical Property. Mater. Sci. Eng. A 2019, 745, 335–345. [Google Scholar] [CrossRef]
- Yu, H.; Li, F.; Yang, J.; Shao, J.; Wang, Z.; Zeng, X. Investigation on Laser Welding of Selective Laser Melted Ti-6Al-4V Parts: Weldability, Microstructure and Mechanical Properties. Mater. Sci. Eng. A 2018, 712, 20–27. [Google Scholar] [CrossRef]
- Sun, Y.Y.; Wang, P.; Lu, S.L.; Li, L.Q.; Nai, M.L.S.; Wei, J. Laser Welding of Electron Beam Melted Ti-6Al-4V to Wrought Ti-6Al-4V: Effect of Welding Angle on Microstructure and Mechanical Properties. J. Alloys Compd. 2018, 782, 967–972. [Google Scholar] [CrossRef]
- Zhou, X.; Huang, Y.; Hao, K.; Chen, Y. Cracking in Dissimilar Laser Welding of Tantalum to Molybdenum. Opt. Laser Technol. 2018, 102, 54–59. [Google Scholar] [CrossRef]
- Zhou, X.; Huang, Y.; Chen, Y.; Peng, P. Laser Joining of Mo and Ta Sheets with Ti6Al4V or Ni Filler. Opt. Laser Technol. 2018, 106, 487–494. [Google Scholar] [CrossRef]
- Oliveira, J.P.; Zeng, Z.; Andrei, C.; Braz Fernandes, F.M.; Miranda, R.M.; Ramirez, A.J.; Omori, T.; Zhou, N. Dissimilar Laser Welding of Superelastic NiTi and CuAlMn Shape Memory Alloys. Mater. Des. 2017, 128, 166–175. [Google Scholar] [CrossRef]
- Shojaei Zoeram, A.; Akbari Mousavi, S.A.A. Laser Welding of Ti–6Al–4V to Nitinol. Mater. Des. 2014, 61, 185–190. [Google Scholar] [CrossRef]
- Zhao, Y.; Wang, W.; Yan, K.; Liu, C.; Zou, J. Microstructure and Properties of Cu/Ti Laser Welded Joints. J. Mater. Process. Technol. 2018, 257, 244–249. [Google Scholar] [CrossRef]
- Bass, L.S.; Treat, M.R. Laser Tissue Welding: A Comprehensive Review of Current and Future. Lasers Surg. Med. 1995, 17, 315–349. [Google Scholar] [CrossRef]
- Pini, R.; Menabuoni, L.; Starnotti, L. First Application of Laser Welding in Clinical Transplantation of the Cornea. In Lasers in Surgery: Advanced Characterization, Therapeutics and Systems XI; Anderson, R.R., Bartels, K.E., Bass, L.S., Garrett, C.G., Gregory, K.W., Katzir, A., Kollias, N., Lucroy, M.D., Malek, R.S., Nelson, J.S., et al., Eds.; International Society for Optics and Photonics: Bellingham, WA, USA, 2001; Volume 4244, pp. 266–272. [Google Scholar] [CrossRef]
- Rossi, F.; Matteini, P.; Ratto, F.; Menabuoni, L.; Lenzetti, I.; Pini, R. Laser Tissue Welding in Ophthalmic Surgery. J. Biophotonics 2008, 1, 331–342. [Google Scholar] [CrossRef]
- Yilmaz, M.; Duzlu, M.; Catli, T.; Ustun, S.; Ceylan, A. Thermal Welding versus Cold Knife Tonsillectomy: A Prospective Randomized Study. Kaohsiung J. Med. Sci. 2012, 28, 270–272. [Google Scholar] [CrossRef] [PubMed]
- Bouzari, N.; Elsaie, M.L.; Nouri, K. Laser and Light for Wound Healing Stimulation. In Lasers in Dermatology and Medicine; Springer: London, UK, 2011; pp. 267–275. [Google Scholar] [CrossRef]
- Fida, A.R.; Sendi, K.S. Assessment of Postoperative Pain Scores in Thermal Welding and Conventional Tonsillectomy Techniques: A Randomized Control Study. Egypt. J. Ear Nose Throat Allied Sci. 2013, 14, 107–111. [Google Scholar] [CrossRef][Green Version]
- Canovetti, A.; Malandrini, A.; Lenzetti, I.; Rossi, F.; Pini, R.; Menabuoni, L. Laser-Assisted Penetrating Keratoplasty: 1-Year Results in Patients Using a Laser-Welded Anvil-Profiled Graft. Am. J. Ophthalmol. 2014, 158, 664–670.e2. [Google Scholar] [CrossRef] [PubMed]
- Matteini, P.; Rossi, F.; Ratto, F.; Pini, R. Laser Welding of Biological Tissue: Mechanisms, Applications and Perspectives. In Laser Imaging and Manipulation in Cell Biology; Pavone, F.S., Ed.; WILEY-VCH Verlag GmbH & Co. KGaA: Weinheim, Germany, 2010; pp. 203–231. [Google Scholar]
- Gerasimenko, A.Y.; Ichkitidze, L.P.; Pavlov, A.A.; Piyankov, E.S.; Ryabkin, D.I.; Savelyev, M.S.; Selishchev, S.V.; Rimshan, I.B.; Zhurbina, N.N.; Podgaetskii, V.M. Laser System with Adaptive Thermal Stabilization for Welding of Biological Tissues. Biomed. Eng. 2016, 49, 344–348. [Google Scholar] [CrossRef]
- Tal, K.; Strassmann, E.; Loya, N.; Ravid, A.; Kariv, N.; Weinberger, D.; Katzir, A.; Gaton, D.D. Corneal Cut Closure Using Temperature-Controlled CO2 Laser Soldering System. Lasers Med. Sci. 2015, 30, 1367–1371. [Google Scholar] [CrossRef]
- Menabuoni, L.; Malandrini, A.; Canovetti, A.; Lenzetti, I.; Pini, R.; Rossi, F. The Use of Femtosecond Laser and Corneal Welding in the Surgery of Keratoconus. In Icarus; Springer International Publishing: Cham, Switzerland, 2017; Volume 216, pp. 289–295. [Google Scholar] [CrossRef]
- Heriot, W.J. Thermofusion of the Retina with the RPE to Seal Tears during Retinal Detachment Repair. Graefe’s Arch. Clin. Exp. Ophthalmol. 2016, 254, 691–696. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.; Song, C.; Wang, Z. Novel Concave–Convex Electrode for Colonic Anastomoses by Radiofrequency Thermo-Fusion. Surg. Endosc. 2015, 1809–1816. [Google Scholar] [CrossRef] [PubMed]
- Papaspyrou, G.; Linxweiler, M.; Knöbber, D.; Schick, B.; Al Kadah, B. Laser CO2 Tonsillotomy versus Argon Plasma Coagulation (APC) Tonsillotomy: A Retrospective Study with 10-Year Follow-Up. Int. J. Pediatr. Otorhinolaryngol. 2017, 92, 56–60. [Google Scholar] [CrossRef]
- Lee, C.A.; Kessler, C.M.; Varon, D.; Martinowitz, U.; Heim, M.; POPPAS, D.P.; SCHERR, D.S. Laser Tissue Welding: A Urological Surgeon’s Perspective. Haemophilia 1998, 4, 456–462. [Google Scholar] [CrossRef]
- Ninan, N.; Thomas, S.; Grohens, Y. Wound Healing in Urology. Adv. Drug Deliv. Rev. 2015, 82–83, 93–105. [Google Scholar] [CrossRef]
- Amiel, G.; Shu, T.; Wadia, Y. MP23-19 Sutureless partial nephrectomy using laser tissue welding. J. Urol. 2016, 195, e269. [Google Scholar] [CrossRef][Green Version]
- Bertrand, C.; Poulon-Quintin, A. Proposals for Optimization of Laser Welding in Prosthetic Dentistry. J. Prosthodont. 2010, 19, 69–76. [Google Scholar] [CrossRef]
- Yamashita, Y.; Yamaguchi, Y.; Noguchi, N.; Goto, M. Mandibular Reconstruction Using a Titanium Mesh Sheet Processed by Laser Welding after Segmental Mandibulectomy for Implant Placement. J. Oral Maxillofac. Surg. Med. Pathol. 2014, 26, 511–514. [Google Scholar] [CrossRef]
- Paek, J.; Ahn, H.; Jeong, D.; Shim, J.; Kim, S.; Chung, K. Application of the 2-Piece Orthodontic C-Implant for Provisional Restoration with Laser Welded Customized Coping: A Case Report. Head Face Med. 2015, 11, 7. [Google Scholar] [CrossRef] [PubMed]
- Barton, M.J.; Morley, J.W.; Stoodley, M.A.; Lauto, A.; Mahns, D.A. Nerve Repair: Toward a Sutureless Approach. Neurosurg. Rev. 2014, 37, 585–595. [Google Scholar] [CrossRef]
- Lawrence, P.F.; Li, K.; Merrell, S.W.; Goodman, G.R. A Comparison of Absorbable Suture and Argon Laser Welding for Lateral Repair of Arteries. J. Vasc. Surg. 1991, 14, 183–189. [Google Scholar] [CrossRef]
- Hasegawa, M.; Sakurai, T.; Matsushita, M.; Nishikimi, N.; Nimura, Y.; Kobayashi, M. Comparison of Argon-Laser Welded and Sutured Repair of Inferior Vena Cava in a Canine Model. Lasers Surg. Med. 2001, 29, 62–69. [Google Scholar] [CrossRef]
- Curtis, N.J.; Lauto, A.; Trickett, R.; Owen, E.; Walker, D.M. Preliminary Study of Microsurgical Repairs of the Inferior Alveolar Nerve in Rats Using Primary Suturing and Laser Weld Techniques. Int. J. Oral Maxillofac. Surg. 1998, 27, 476–481. [Google Scholar] [CrossRef]
- White, R.A.; Patrick Abergel, R.; Lyons, R.; Klein, S.R.; Kopchok, G.; Dwyer, R.M.; Uitto, J. Biological Effects of Laser Welding on Vascular Healing. Lasers Surg. Med. 1986, 6, 137–141. [Google Scholar] [CrossRef]
- Menovsky, T.; Beek, J.F.; van Gemert, M.J.C. CO2 Laser Nerve Welding: Optimal Laser Parameters and the Use of Solders in Vitro. Microsurgery 1994, 15, 44–51. [Google Scholar] [CrossRef]
- Happak, W.; Neumayer, C.; Holak, G.; Kuzbari, R.; Burggasser, G.; Gruber, H. Morphometric and Functional Results after CO2 Laser Welding of Nerve Coaptations. Lasers Surg. Med. 2000, 27, 66–72. [Google Scholar] [CrossRef]
- Wolf-de Jonge, I.C.D.Y.M.; Heger, M.; van Marle, J.; Balm, R.; Beek, J.F. Suture-Free Laser-Assisted Vessel Repair Using CO2 Laser and Liquid Albumin Solder. J. Biomed. Opt. 2008, 13, 1–9. [Google Scholar] [CrossRef]
- Nakadate, R.; Omori, S.; Ikeda, T.; Akahoshi, T.; Oguri, S.; Arata, J.; Onogi, S.; Hashizume, M. Improving the Strength of Sutureless Laser-Assisted Vessel Repair Using Preloaded Longitudinal Compression on Tissue Edge. Lasers Surg. Med. 2017, 49, 533–538. [Google Scholar] [CrossRef]
- Pabittei, D.R.; Heger, M.; Van Tuijl, S.; Simonet, M. Ex Vivo Proof-of-Concept of End-to-End Scaffold-Enhanced Laser-Assisted Vascular Anastomosis of Porcine Arteries. J. Vasc. Surg. 2015, 62, 200–209. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Bhatt, N.K.; Mejias, C.; Kallogjeri, D.; Gale, D.C.; Park, A.M.; Paniello, R.C. Potassium Titanyl Phosphate Laser Welding Following Complete Nerve Transection. Laryngoscope 2017, 127, 1525–1530. [Google Scholar] [CrossRef]
- Ott, B.; Constantinescu, M.A.; Erni, D.; Banic, A.; Schaffner, T.; Frenz, M. Intraluminal Laser Light Source and External Solder: In Vivo Evaluation of a New Technique for Microvascular Anastomosis. Lasers Surg. Med. 2004, 35, 312–316. [Google Scholar] [CrossRef] [PubMed]
- O’Neill, A.C.; Winograd, J.M.; Zeballos, J.L.; Johnson, T.S.; Randolph, M.A.; Bujold, K.E.; Kochevar, I.E.; Redmond, R.W. Microvascular Anastomosis Using a Photochemical Tissue Bonding Technique. Lasers Surg. Med. 2007, 39, 716–722. [Google Scholar] [CrossRef]
- Barton, M.; Piller, S.C.; Mahns, D.A.; Morley, J.W.; Mawad, D.; Longo, L.; Lauto, A. In Vitro Cell Compatibility Study of Rose Bengal-Chitosan Adhesives. Lasers Surg. Med. 2012, 44, 762–768. [Google Scholar] [CrossRef]
- Ark, M.; Cosman, P.H.; Boughton, P.; Dunstan, C.R. Review: Photochemical Tissue Bonding (PTB) Methods for Sutureless Tissue Adhesion. Int. J. Adhes. Adhes. 2016, 71, 87–98. [Google Scholar] [CrossRef]
- Korsak, A.V.; Chaikovskii, Y.B. Immunohistochemical Analysis of the Structure of Injured Peripheral Nerve Neuroma after Electrosurgical Welding Intervention. Bull. Exp. Biol. Med. 2015, 159, 789–791. [Google Scholar] [CrossRef] [PubMed]
- Chuck, R.S.; Oz, M.C.; Delohery, T.M.; Johnson, J.P.; Bass, L.S.; Nowygrod, R.; Treat, M.R. Dye-Enhanced Laser Tissue Welding. Lasers Surg. Med. 1989, 9, 471–477. [Google Scholar] [CrossRef] [PubMed]
- White, R.A.; Kopchok, G.; Donayre, C.; Lyons, R.; White, G.; Klein, S.R.; Pizzurro, D.; Abergel, R.P.; Dwyer, R.M.; Uitto, J. Large Vessel Sealing with the Argon Laser. Lasers Surg. Med. 1987, 7, 229–235. [Google Scholar] [CrossRef]
- Kramer, E.A.; Rentschler, M.E. Energy-Based Tissue Fusion for Sutureless Closure: Applications, Mechanisms, and Potential for Functional Recovery. Annu. Rev. Biomed. Eng. 2018, 20, 1–20. [Google Scholar] [CrossRef]
- Alam, M.; Hsu, T.-S.; Dover, J.S.; Wrone, D.A.; Arndt, K.A. Nonablative Laser and Light Treatments: Histology and Tissue Effects? A Review. Lasers Surg. Med. 2003, 33, 30–39. [Google Scholar] [CrossRef]
- Liu, H.; Dang, Y.; Wang, Z.; Chai, X.; Ren, Q. Laser Induced Collagen Remodeling: A Comparative Study in Vivo on Mouse Model. Lasers Surg. Med. 2008, 40, 13–19. [Google Scholar] [CrossRef]
- Bodendorf, M.O.; Willenberg, A.; Anderegg, U.; Grunewald, S.; Simon, J.C.; Paasch, U. Connective Tissue Response to Fractionated Thermo-Ablative Erbium: YAG Skin Laser Treatment. Int. J. Cosmet. Sci. 2010, 32, 435–445. [Google Scholar] [CrossRef]
- Wang, X.; Khalil, R.A. Matrix Metalloproteinases, Vascular Remodeling, and Vascular Disease. In Advances in Pharmacology; Elsevier Inc.: Amsterdam, The Netherlands, 2018; Volume 81, pp. 241–330. [Google Scholar] [CrossRef]
- Kono, A.; Oguri, A.; Yokoo, K.; Watanabe, H. YAG Laser Treatment Causes Rapid Degeneration and Regeneration of Collagen Fibres in Pig Skin and Facilitates Fibroblast Growth. J. Plast. Surg. Hand Surg. 2012, 46, 308–312. [Google Scholar] [CrossRef] [PubMed]
- Lucke, L.D.; Bortolazzo, F.O.; Theodoro, V.; Fujii, L.; Bombeiro, A.L.; Felonato, M.; Dalia, R.A.; Carneiro, G.D.; Cartarozzi, L.P.; Vicente, C.P.; et al. Low-Level Laser and Adipose-Derived Stem Cells Altered Remodelling Genes Expression and Improved Collagen Reorganization during Tendon Repair. Cell Prolif. 2019, e12580. [Google Scholar] [CrossRef]
- Mordon, S.; Capon, A.; Fournier, N.; Iarmarcovai, G. Lasers Thermiques et Cicatrisation Cutanée. Médecine/Sciences 2010, 26, 89–94. [Google Scholar] [CrossRef] [PubMed]
- Vitenberga, Z.; Pilmane, M. Age-Related Lung Tissue Remodeling Due to the Local Distribution of MMP-2, TIMP-2, TGF-β and Hsp70. Biotech. Histochem. 2018, 93, 239–248. [Google Scholar] [CrossRef] [PubMed]
- Nagata, K. HSP47 as a Collagen-Specific Molecular Chaperone: Function and Expression in Normal Mouse Development. Semin. Cell Dev. Biol. 2003, 14, 275–282. [Google Scholar] [CrossRef] [PubMed]
- DeBruler, D.M.; Blackstone, B.N.; Baumann, M.E.; McFarland, K.L.; Wulff, B.C.; Wilgus, T.A.; Bailey, J.K.; Supp, D.M.; Powell, H.M. Inflammatory Responses, Matrix Remodeling, and Re-Epithelialization after Fractional CO 2 Laser Treatment of Scars. Lasers Surg. Med. 2017, 49, 675–685. [Google Scholar] [CrossRef] [PubMed]
- Nesi-Reis, V.; Lera-Nonose, D.S.S.L.; Oyama, J.; Silva-Lalucci, M.P.P.; Demarchi, I.G.; Aristides, S.M.A.; Teixeira, J.J.V.; Silveira, T.G.V.; Lonardoni, M.V.C. Contribution of Photodynamic Therapy in Wound Healing: A Systematic Review. Photodiagnosis Photodyn. Ther. 2018, 21, 294–305. [Google Scholar] [CrossRef]
- Fortuna, T.; Gonzalez, A.C.; Sá, M.F.; Andrade, Z.; de A Andrade, Z.; Reis, S.R.A.; Medrado, A.R.A.P. Effect of 670 Nm Laser Photobiomodulation on Vascular Density and Fibroplasia in Late Stages of Tissue Repair. Int. Wound J. 2018, 15, 274–282. [Google Scholar] [CrossRef]
- White, R.A.; Kopchok, G.E.; Donayre, C.E.; Peng, S.-K.; Fujitani, R.M.; White, G.H.; Uitto, J. Mechanism of Tissue Fusion in Argon Laser-Welded Vein-Artery Anastomoses. Lasers Surg. Med. 1988, 8, 83–89. [Google Scholar] [CrossRef] [PubMed]
- Pabittei, D.R.; Heger, M.; Simonet, M.; van Tuijl, S.; van der Wal, A.C.; Beek, J.F.; Balm, R.; de Mol, B.A. Biodegradable Polymer Scaffold, Semi-Solid Solder, and Single-Spot Lasing for Increasing Solder-Tissue Bonding in Suture-Free Laser-Assisted Vascular Repair. J. Tissue Eng. Regen. Med. 2012, 6, 803–812. [Google Scholar] [CrossRef]
- Menovsky, T.; Beek, J.F.; Thomsen, S.L. Laser(-Assisted) Nerve Repair. A Review. Neurosurg. Rev. 1995, 18, 225–235. [Google Scholar] [CrossRef]
- Fankell, D.P.; Kramer, E.; Cezo, J.; Taylor, K.D.; Ferguson, V.L.; Rentschler, M.E. A Novel Parameter for Predicting Arterial Fusion and Cutting in Finite Element Models. Ann. Biomed. Eng. 2016, 44, 3295–3306. [Google Scholar] [CrossRef]
- Leclère, F.M.; Vogt, P.; Schoofs, M.; Delattre, M.; Mordon, S. Current Laser Applications in Reconstructive Microsurgery: A Review of the Literature. J. Cosmet. Laser Ther. 2016, 18, 130–133. [Google Scholar] [CrossRef]
- Stewart, R.B.; Bass, L.S.; Thompson, J.K.; Nikoi, N.D.; Becker, G.; Kung, R.T.V. Improved Microvessel Repair: Laser Welding with an Anti-Thrombotic Solder. Lasers Surg. Med. 2002, 31, 36–40. [Google Scholar] [CrossRef]
- Bogni, S.; Stumpp, O.; Reinert, M.; Frenz, M. Thermal Model for Optimization of Vascular Laser Tissue Soldering. J. Biophotonics 2010, 3, 284–295. [Google Scholar] [CrossRef]
- Hiebl, B.; Ascher, L.; Luetzow, K.; Kratz, K.; Gruber, C.; Mrowietz, C.; Nehring, M.E.; Lendlein, A.; Franke, R.P.; Jung, F. Albumin Solder Covalently Bound to a Polymer Membrane: New Approach to Improve Binding Strength in Laser Tissue Soldering in-Vitro. Clin. Hemorheol. Microcirc. 2018, 69, 317–326. [Google Scholar] [CrossRef] [PubMed]
- Tünnermann, A. High-Power Cw Fiber Lasers–Present and Future. Laser Tech. J. 2005, 2, 54–56. [Google Scholar] [CrossRef]
- Zervas, M.N.; Codemard, C.A. High Power Fiber Lasers: A Review. IEEE J. Sel. Top. Quantum Electron. 2014, 20, 219–241. [Google Scholar] [CrossRef]
- Gursel, A.T. Fiber Lasers and Their Medical Applications. In Optical Amplifiers—A Few Different Dimensions; IntechOpen: London, UK, 2018; Volume I, p. 13. [Google Scholar] [CrossRef]
- Pierce, M.C.; Jackson, S.D.; Golding, P.S.; Dickinson, B.; Dickinson, M.R.; King, T.A.; Sloan, P. Development and Application of Fiber Lasers for Medical Applications. Proc. SPIE 2001, 4253, 144–154. [Google Scholar] [CrossRef]
- Ganguly, M.; Miller, S.; Mitra, K. Model Development and Experimental Validation for Analyzing Initial Transients of Irradiation of Tissues during Thermal Therapy Using Short Pulse Lasers. Lasers Surg. Med. 2015, 47, 711–722. [Google Scholar] [CrossRef] [PubMed]
- Fornaini, C.; Merigo, E.; Poli, F.; Cavatorta, C.; Rocca, J.-P.; Selleri, S.; Cucinotta, A. Use of 1070 Nm Fiber Lasers in Oral Surgery: Preliminary Ex Vivo Study with FBG Temperature Monitoring. Laser Ther. 2017, 26, 311–318. [Google Scholar] [CrossRef]
- Aaltonen, I.E.; Wahlström, M. Envisioning Robotic Surgery: Surgeons’ Needs and Views on Interacting with Future Technologies and Interfaces. Int. J. Med. Robot. Comput. Assist. Surg. 2018, 14, e1941. [Google Scholar] [CrossRef] [PubMed]
- Balkhy, H.H.; Lewis, C.T.P.; Kitahara, H. Robot-Assisted Aortic Valve Surgery: State of the Art and Challenges for the Future. Int. J. Med. Robot. Comput. Assist. Surg. 2018, 14, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Namdarian, B.; Dasgupta, P. What Robot for Tomorrow and What Improvement Can We Expect? Curr. Opin. Urol. 2018, 28, 1. [Google Scholar] [CrossRef] [PubMed]
- He, W.; Frueh, J.; Hu, N.; Liu, L.; Gai, M.; He, Q. Guidable Thermophoretic Janus Micromotors Containing Gold Nanocolorifiers for Infrared Laser Assisted Tissue Welding. Adv. Sci. 2016, 3, 1600206. [Google Scholar] [CrossRef] [PubMed]
- Urie, R.; Guo, C.; Ghosh, D.; Thelakkaden, M.; Wong, V.; Lee, J.K.; Kilbourne, J.; Yarger, J.; Rege, K. Rapid Soft Tissue Approximation and Repair Using Laser-Activated Silk Nanosealants. Adv. Funct. Mater. 2018, 28, 1802874. [Google Scholar] [CrossRef]




| Techniques for Nerve, Arteries, and Veins Repairs | ||
|---|---|---|
| Conventional techniques | Suture | Nonabsorbable suture [41,42,43] |
| Absorbable suture [41] | ||
| Nonconventional techniques | Laser welding | Argon laser welding [41,44] |
| CO2 laser welding [44,45,46,47] | ||
| Nd:YAG laser welding [44] | ||
| Infrared diode laser welding [48,49] | ||
| Potassium titanyl phosphate laser welding [50] | ||
| Laser welding with intraluminal light source [51] | ||
| Photochemical tissue bonding [40,52,53,54] | ||
| Electrosurgical high-frequency welding [55] | ||
| Study | Total No. of Welds | No. of Welds with Complementary Sutures | No. of Additional Sutures Per Weld |
|---|---|---|---|
| White et al. [44] | 5 a | 1 | 1 |
| White et al. [57] | 12 | 12 | 1 |
| White et al. [71] | 24 | 12 | 1 to 2 |
| Lawrence et al. [41] | 61 | 55 | 1 |
| Hasegawa et al. [42] | 12 | 8 | 1 to 3 |
| Laser | Suitable Surgeries | Advantages | Drawbacks |
|---|---|---|---|
| Argon | Vascular repairs | Deep vessel wall penetration with lower energy output [41] | Nerve absorption of laser light is minimum due to the lack of presence of significant chromophores [73] |
| CO2 | Nerve repairs | High energy output [41] | Used primarily to cut and vaporize tissue [44] |
| Low penetration depth [45] | Low strength in arterial repairs, cannot sustain systemic pressures [57] | ||
| Nd:YAG | Vascular repairs | Easy penetration of the tissue [44] | Limited to microvascular anastomoses surgeries [41] |
| Produces deep uncontrolled thermal injury due to excessive energy density [44] | |||
| Low strength in arterial repairs, cannot sustain systemic pressures [57] |
| Study | Laser Welding | Histologic Examination | |
|---|---|---|---|
| CO2 | Argon | ||
| White et al. [44] | - | x | Minimal inflammatory response, near normal collagen content, absent of aneurysm formation |
| White et al. [57] | - | x | Absent of hematomas, false aneurysms or luminal dilatation, and minimal inflammatory response |
| White et al. [71] | - | x | Minimal inflammatory response and near-normal collagen content |
| Lawrence et al. [41] | - | x | Absent aneurysm formation |
| Menosky et al. [45] | x | - | Absent foreign body reaction, minimized scar tissue formation |
| Happak et al. [46] | x | - | Minimized tissue thermal damage and no foreign body reactions |
| Hasegawa et al. [42] | - | x | Absent aneurysm formation although with no complete regeneration of the elastic lamina |
| Jonge et al. [47] | x | - | Minimal thermal necrosis and welding strength increase |
| Bhatt et al. [50] | x | - | Good functional recovery with no nerve dehiscence |
| Study | Surgery | Laser Type | Laser Mode | Welding Parameters | Time | |||
|---|---|---|---|---|---|---|---|---|
| Wavelength (nm) | Power (W) | Weld Time (s) | Pulse Time (s) | Pulse Interval (s) | ||||
| White et al. [44] | Vascular | Argon | CW | 458–515 | 1.5 | 300–400 | NR | NR |
| CO2 | CW | 10,600 | 1–2 | 20–40 | NR | NR | ||
| Nd:YAG | CW | 1060 | 7 | 20–25 | NR | NR | ||
| White et al. [57] | Vascular | Argon | CW | NR | 0.5 | 240 | 5 | 0.2 |
| White et al. [71] | Vascular | Argon | CW | NR | 0.5 | 125–150 | 5 | 0.2 |
| Chuck et al. [56] | Vascular | Argon | CW | 488 | 0.01–0.05 | 15–120 | NR | NR |
| Lawrence et al. [41] | Vascular | Argon | CW | NR | 0.75 | 100 | 5 | 0.2 |
| Menosky et al. [45] | Nerve | CO2 | CW | NR | 0.05–0.15 | NR | 0.1–3 | NR |
| Curtis et al. [43] | Nerve | IR diode | CW | 810 | 0.08 | NR | NR | NR |
| Happak et al. [46] | Nerve | CO2 with power reduction unit | CW | NR | 0.06 | NR | NR | NR |
| Hasegawa et al. [42] | Vascular | Argon | CW | NR | 0.17 | NR | 5 | NR |
| Stewart et al. [76] | Vascular | IR diode | CW | 808 | 0.08 | 4 × 0.5 | NR | NR |
| Ott et al. [51] | Vascular | IR diode | CW | 808 | 0.41 | 30 | NR | NR |
| 0.55 | 45 | |||||||
| O’Neill et al. [52] | Vascular | PTB with Nd:YAG | CW | 532 | 0.35 | 2 × 30 | NR | NR |
| Jonge et al. [47] | Vascular | CO2 | CW | 10,600 | 0.17 | 261 ± 40 | NR | NR |
| Bogni et al. [77] | Vascular | IR diode | CW | 808 | 0.4–3 | 2.5–30 | NR | NR |
| Pabittei et al. [72] | Vascular | IR diode single-spot | CW | 670 | 1.6 | 50 | NR | NR |
| IR diode scanning | 82 | NR | NR | |||||
| Pabittei et al. [49] | Vascular | IR diode | CW | 670 | 0.096 | NR | 25 | NR |
| Nakadate et al. [48] | Vascular | IR diode | CW | 970 | 2.4 | 30 | NR | NR |
| Bhatt et al. [50] | Vascular | CO2 | CW | 10,600 | 0.1 | NR | 1 | NR |
| KTP | CW | 532 | 3–4 | NR | 1 | NR | ||
| Hiebl et al. [78] | Vascular | IR diode | CW | 808 | 0.25–1.5 | 30 | NR | NR |
| Bonding Materials and Solders | Advantages | Drawbacks |
|---|---|---|
| Fibrin glue [40] | Reduces inflammatory tissues and easy application | Low tensile strength, infection risk |
| Cyanoacrylate glue [40,58] | High tensile strength and easy application | Requires support stay sutures, causes fibrosis, foreign-body toxicity |
| Polyethylene glycol (PEG) [40] | Nontoxic, biocompatible and reduces scar tissue | Slow degradation process (over 20 months) |
| Albumin-based solution [40,47,78] | In nerve repairs, protects the epineurium, increases bonding strength, reduces thermal damage | Leakage of fluid solder, thermal damage still present, viral infection risk, becomes brittle |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gomes, D.F.; Galvão, I.; Loja, M.A.R. Overview on the Evolution of Laser Welding of Vascular and Nervous Tissues. Appl. Sci. 2019, 9, 2157. https://doi.org/10.3390/app9102157
Gomes DF, Galvão I, Loja MAR. Overview on the Evolution of Laser Welding of Vascular and Nervous Tissues. Applied Sciences. 2019; 9(10):2157. https://doi.org/10.3390/app9102157
Chicago/Turabian StyleGomes, Diogo Francisco, Ivan Galvão, and Maria Amélia Ramos Loja. 2019. "Overview on the Evolution of Laser Welding of Vascular and Nervous Tissues" Applied Sciences 9, no. 10: 2157. https://doi.org/10.3390/app9102157
APA StyleGomes, D. F., Galvão, I., & Loja, M. A. R. (2019). Overview on the Evolution of Laser Welding of Vascular and Nervous Tissues. Applied Sciences, 9(10), 2157. https://doi.org/10.3390/app9102157