Comparative In Vitro Evaluation of the Primary Stability in D3 Synthetic Bone of Two Different Shapes and Pitches of the Implant Threads
Abstract
1. Introduction
2. Materials and Methods
- Group A: cylindrical one-stage wide thread pitch implant, 3.8 mm diameter × 12 mm length (Crystal, F.M.D., Rome Italy);
- Group B: cylindrical one-stage wide thread pitch implant, 4.8 mm diameter × 12 mm length (Crystal, F.M.D., Roma Italy);
- Group C: cylindrical two-stage narrow thread pitch, 3.8 mm diameter × 12 mm length (Elisir, FMD, Rome Italy);
- Group D: cylindrical two-stage narrow thread pitch, 4.8 mm diameter × 12 mm length (Elisir, FMD, Rome Italy).
2.1. Periotest Measurement
- From −8 to 0: good bone integration; the implant is well integrated and can be loaded.
- From +1 to +9: clinical control is required; the implant load is mostly not possible yet.
- From +10 to +50: bone integration is not enough; the system cannot be loaded.
2.2. Insertion Torque and Removal Measurements
2.3. Statistical Analysis
3. Results
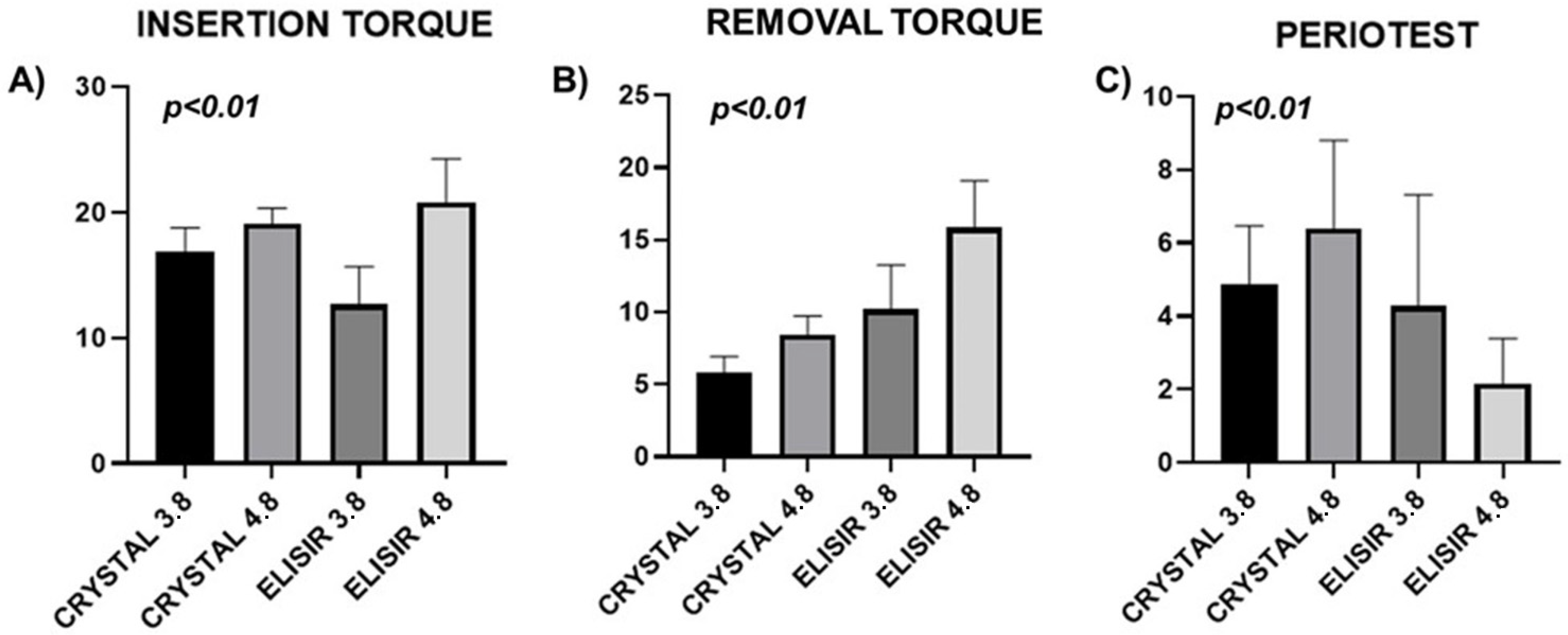
3.1. Insertion and Removal Torque
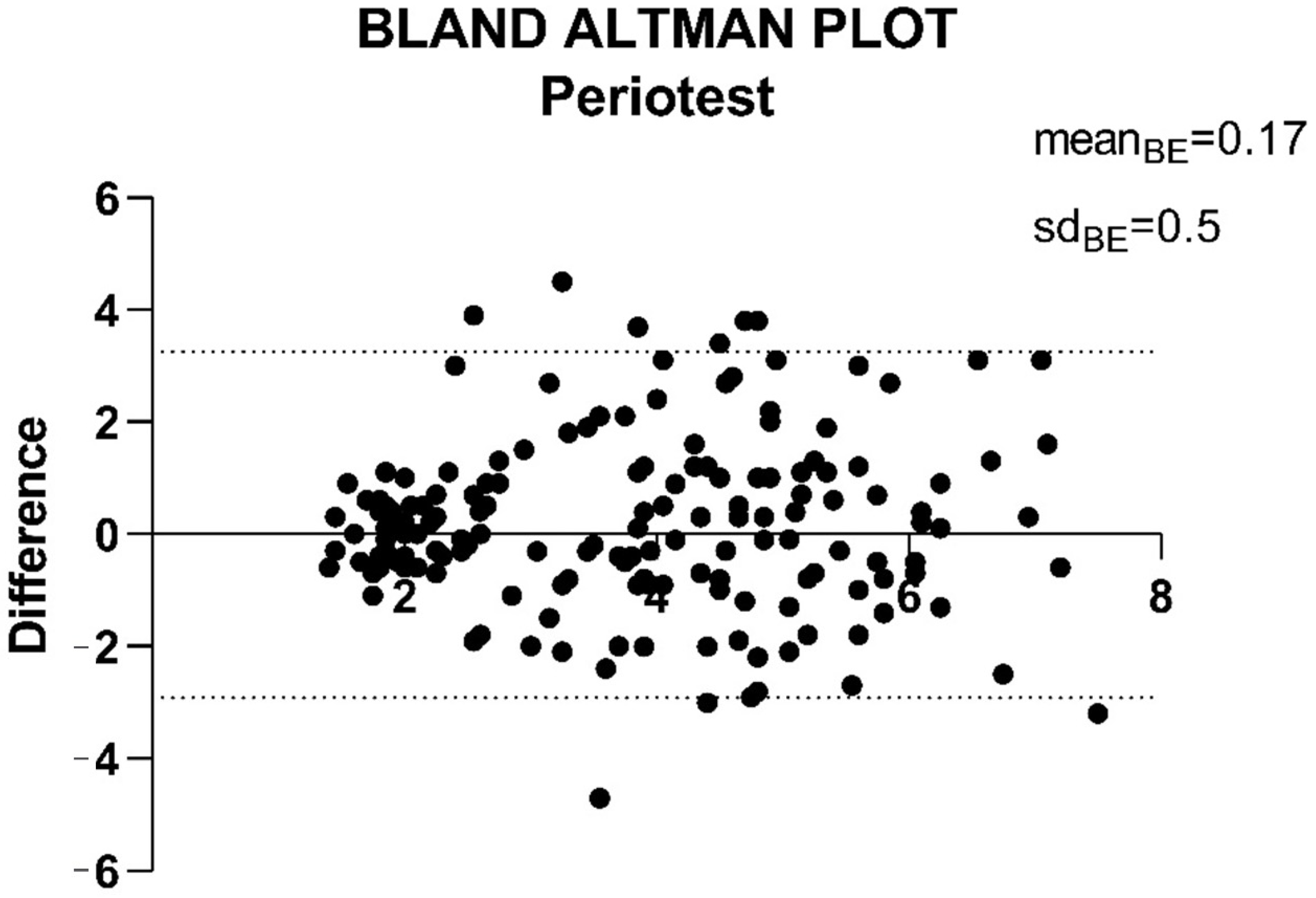
3.2. Periotest Stability Measurement
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Albrektsson, T.; Sennerby, L. State of the Art in Oral Implants. J. Clin. Periodontol. 1991, 18, 474–481. [Google Scholar] [CrossRef]
- Iezzi, G.; Degidi, M.; Scarano, A.; Perrotti, V.; Piattelli, A. Bone Response to Submerged, Unloaded Implants Inserted in Poor Bone Sites: A Histological and Histomorphometrical Study of 8 Titanium Implants Retrieved from Man. J. Oral Implantol. 2005, 31, 225–233. [Google Scholar] [CrossRef]
- Falco, A.; Berardini, M.; Trisi, P. Correlation between Implant Geometry, Implant Surface, Insertion Torque, and Primary Stability: In Vitro Biomechanical Analysis. Int. J. Oral Maxillofac. Implants 2018, 33, 824–830. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Lorusso, F.; Arcangelo, M.; D’Arcangelo, C.; Celletti, R.; de Oliveira, P.S. Lateral Sinus Floor Elevation Performed with Trapezoidal and Modified Triangular Flap Designs: A Randomized Pilot Study of Post-Operative Pain Using Thermal Infrared Imaging. Int. J. Environ. Res. Public Health 2018, 15, 1277. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Lorusso, F.; Staiti, G.; Sinjari, B.; Tampieri, A.; Mortellaro, C. Sinus Augmentation with Biomimetic Nanostructured Matrix: Tomographic, Radiological, Histological and Histomorphometrical Results after 6 Months in Humans. Front. Physiol. 2017, 8, 565. [Google Scholar] [CrossRef]
- Scarano, A.; Murmura, G.; Vantaggiato, G.; Lauritano, D.; Silvestre-Rangil, J.; DI Cerbo, A.; Lorusso, F. Delayed Expansion of Atrophic Mandible (Deam): A Case Report. ORAL Implantol. 2017, 10, 190–196. [Google Scholar] [CrossRef]
- Scarano, A.; Valbonetti, L.; Marchetti, M.; Lorusso, F.; Ceccarelli, M. Soft Tissue Augmentation of the Face with Autologous Platelet-Derived Growth Factors and Tricalcium Phosphate. Microtomography Evaluation of Mice. J. Craniofacial Surg. 2016, 27, 1212–1214. [Google Scholar] [CrossRef]
- Scarano, A.; Crincoli, V.; Di Benedetto, A.; Cozzolino, V.; Lorusso, F.; Podaliri Vulpiani, M.; Grano, M.; Kalemaj, Z.; Mori, G.; Grassi, F.R. Bone Regeneration Induced by Bone Porcine Block with Bone Marrow Stromal Stem Cells in a Minipig Model of Mandibular “Critical Size” Defect. Stem Cells Int. 2017, 2017, 9082869. [Google Scholar] [CrossRef]
- Degidi, M.; Daprile, G.; Piattelli, A. Influence of Underpreparation on Primary Stability of Implants Inserted in Poor Quality Bone Sites: An in Vitro Study. J. Oral Maxillofac. Surg. 2015, 73, 1084–1088. [Google Scholar] [CrossRef]
- Al-Sabbagh, M.; Eldomiaty, W.; Khabbaz, Y. Can Osseointegration Be Achieved without Primary Stability? Dent. Clin. N. Am. 2019, 63, 461–473. [Google Scholar] [CrossRef]
- Ahmad, O.K.; Kelly, J.R. Assessment of the Primary Stability of Dental Implants in Artificial Bone Using Resonance Frequency and Percussion Analyses. Int. J. Oral Maxillofac. Implants 2013, 28, 89–95. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Steigenga, J.; Al-Shammari, K.; Misch, C.; Nociti, F.H.; Wang, H.-L. Effects of Implant Thread Geometry on Percentage of Osseointegration and Resistance to Reverse Torque in the Tibia of Rabbits. J. Periodontol. 2004, 75, 1233–1241. [Google Scholar] [CrossRef] [PubMed]
- Scarano, A.; Piattelli, A.; Quaranta, A.; Lorusso, F. Bone Response to Two Dental Implants with Different Sandblasted/Acid-Etched Implant Surfaces: A Histological and Histomorphometrical Study in Rabbits. BioMed Res. Int. 2017, 2017, 8724951. [Google Scholar] [CrossRef] [PubMed]
- Degidi, M.; Perrotti, V.; Piattelli, A.; Iezzi, G. Mineralized Bone-Implant Contact and Implant Stability Quotient in 16 Human Implants Retrieved after Early Healing Periods: A Histologic and Histomorphometric Evaluation. Int. J. Oral Maxillofac. Implants 2010, 25, 45–48. [Google Scholar] [PubMed]
- Tumedei, M.; Savadori, P.; Del Fabbro, M. Synthetic Blocks for Bone Regeneration: A Systematic Review and Meta-Analysis. Int. J. Mol. Sci. 2019, 20, 4221. [Google Scholar] [CrossRef] [PubMed]
- Zizzari, V.L.; Berardi, D.; Congedi, F.; Tumedei, M.; Cataldi, A.; Perfetti, G. Morphological Aspect and INOS and Bax Expression Modification in Bone Tissue around Dental Implants Positioned Using Piezoelectric Bone Surgery Versus Conventional Drill Technique. J. Craniofacial Surg. 2015, 26, 741–744. [Google Scholar] [CrossRef]
- Coelho, P.G.; Granato, R.; Marin, C.; Bonfante, E.A.; Janal, M.N.; Suzuki, M. Biomechanical and Bone Histomorphologic Evaluation of Four Surfaces on Plateau Root Form Implants: An Experimental Study in Dogs. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2010, 109, e39–e45. [Google Scholar] [CrossRef]
- Al-Jetaily, S.; Al-Dosari, A.A. Assessment of OsstellTM and Periotest® Systems in Measuring Dental Implant Stability (In Vitro Study). Saudi Dent. J. 2011, 23, 17–21. [Google Scholar] [CrossRef]
- Gehrke, S.A.; Guirado, J.L.C.; Bettach, R.; Fabbro, M.D.; Martínez, C.P.-A.; Shibli, J.A. Evaluation of the Insertion Torque, Implant Stability Quotient and Drilled Hole Quality for Different Drill Design: An In Vitro Investigation. Clin. Oral Implants Res. 2018, 29, 656–662. [Google Scholar] [CrossRef]
- Comuzzi, L.; Iezzi, G.; Piattelli, A.; Tumedei, M. An In Vitro Evaluation, on Polyurethane Foam Sheets, of the Insertion Torque (IT) Values, Pull-Out Torque Values, and Resonance Frequency Analysis (RFA) of NanoShort Dental Implants. Polymers 2019, 11, 1020. [Google Scholar] [CrossRef]
- Comuzzi, L.; Tumedei, M.; De Angelis, F.; Lorusso, F.; Piattelli, A.; Iezzi, G. Influence of the dental implant macrogeometry and threads design on primary stability: An in vitro simulation on artificial bone blocks. Comput. Methods Biomech. Biomed. Eng. 2021, 25, 1–9. [Google Scholar] [CrossRef]
- Comuzzi, L.; Tumedei, M.; Pontes, A.E.; Piattelli, A.; Iezzi, G. Primary Stability of Dental Implants in Low-Density (10 and 20 Pcf) Polyurethane Foam Blocks: Conical vs. Cylindrical Implants. Int. J. Environ. Res. Public Health 2020, 17, 2617. [Google Scholar] [CrossRef]
- Comuzzi, L.; Tumedei, M.; Piattelli, A.; Iezzi, G. Short vs. Standard Length Cone Morse Connection Implants: An In Vitro Pilot Study in Low Density Polyurethane Foam. Symmetry 2019, 11, 1349. [Google Scholar] [CrossRef]
- Tumedei, M.; Piattelli, A.; Degidi, M.; Mangano, C.; Iezzi, G. A Narrative Review of the Histological and Histomorphometrical Evaluation of the Peri-Implant Bone in Loaded and Unloaded Dental Implants. A 30-Year Experience (1988–2018). Int. J. Environ. Res. Public Health 2020, 17, 2088. [Google Scholar] [CrossRef]
- Tumedei, M.; Piattelli, A.; Degidi, M.; Mangano, C.; Iezzi, G. A 30-Year (1988–2018) Retrospective Microscopical Evaluation of Dental Implants Retrieved for Different Causes: A Narrative Review. Int. J. Periodontics Restor. Dent. 2020, 40, e211–e227. [Google Scholar] [CrossRef]
- Fanali, S.; Tumedei, M.; Pignatelli, P.; Inchingolo, F.; Pennacchietti, P.; Pace, G.; Piattelli, A. Implant Primary Stability with an Osteocondensation Drilling Protocol in Different Density Polyurethane Blocks. Comput. Methods Biomech. Biomed. Eng. 2020, 24, 14–20. [Google Scholar] [CrossRef]
- Gehrke, S.A.; Tumedei, M.; Aramburú Júnior, J.; Treichel, T.L.E.; Kolerman, R.; Lepore, S.; Piattelli, A.; Iezzi, G. Histological and Histomorphometrical Evaluation of a New Implant Macrogeometry. A Sheep Study. Int. J. Environ. Res. Public Health 2020, 17, 3477. [Google Scholar] [CrossRef]
- Comuzzi, L.; Tumedei, M.; Piattelli, A.; Iezzi, G. Osseodensification Drilling vs. Standard Protocol of Implant Site Preparation: An In Vitro Study on Polyurethane Foam Sheets. Prosthesis 2020, 2, 76–86. [Google Scholar] [CrossRef]
- Van der Weijden, F.; Dell’Acqua, F.; Slot, D.E. Alveolar Bone Dimensional Changes of Post-Extraction Sockets in Humans: A Systematic Review. J. Clin. Periodontol. 2009, 36, 1048–1058. [Google Scholar] [CrossRef]
- Scarano, A.; Lorusso, F.; Ravera, L.; Mortellaro, C.; Piattelli, A. Bone Regeneration in Iliac Crestal Defects: An Experimental Study on Sheep. BioMed Res. Int. 2016, 2016, 4086870. [Google Scholar] [CrossRef]
- Scarano, A.; de Oliveira, P.S.; Traini, T.; Lorusso, F. Sinus Membrane Elevation with Heterologous Cortical Lamina: A Randomized Study of a New Surgical Technique for Maxillary Sinus Floor Augmentation without Bone Graft. Materials 2018, 11, 1457. [Google Scholar] [CrossRef]
- Scarano, A.; Inchingolo, F.; Murmura, G.; Traini, T.; Piattelli, A.; Lorusso, F. Three-Dimensional Architecture and Mechanical Properties of Bovine Bone Mixed with Autologous Platelet Liquid, Blood, or Physiological Water: An In Vitro Study. Int. J. Mol. Sci. 2018, 19, 1230. [Google Scholar] [CrossRef]
- Piattelli, A.; Artese, L.; Penitente, E.; Iaculli, F.; Degidi, M.; Mangano, C.; Shibli, J.A.; Coelho, P.G.; Perrotti, V.; Iezzi, G. Osteocyte Density in the Peri-Implant Bone of Implants Retrieved after Different Time Periods (4 Weeks to 27 Years). J. Biomed. Mater. Res. Part. B 2014, 102, 239–243. [Google Scholar] [CrossRef]
- Gehrke, A.; Mazon, P.; Del Fabbro, M.; Tumedei, M.; Aramburù, J.; Perez-Diaz, L.; De Aza, P. Histological and Histomorphometric Analyses of Two Bovine Bone Blocks Implanted in Rabbit Calvaria. Symmetry 2019, 11, 641. [Google Scholar] [CrossRef]
- Kotsu, M.; Urbizo Velez, J.; Bengazi, F.; Tumedei, M.; Fujiwara, S.; Kato, S.; Botticelli, D. Healing at Implants Installed from ~ 70- to <10-Ncm Insertion Torques: An Experimental Study in Dogs. Oral Maxillofac. Surg. 2020. [Google Scholar] [CrossRef]
- Fujiwara, S.; Kato, S.; Bengazi, F.; Urbizo Velez, J.; Tumedei, M.; Kotsu, M.; Botticelli, D. Healing at Implants Installed in Osteotomies Prepared Either with a Piezoelectric Device or Drills: An Experimental Study in Dogs. Oral Maxillofac. Surg. 2020. [Google Scholar] [CrossRef]
- Degidi, M.; Daprile, G.; Piattelli, A. Influence of Stepped Osteotomy on Primary Stability of Implants Inserted in Low-Density Bone Sites: An In Vitro Study. Int. J. Oral Maxillofac. Implants 2017, 32, 37–41. [Google Scholar] [CrossRef]
- Pereira, J.; Morsch, C.S.; Henriques, B.; Nascimento, R.M.; Benfatti, C.A.; Silva, F.S.; López-López, J.; Souza, J.C. Removal Torque and Biofilm Accumulation at Two Dental Implant-Abutment Joints after Fatigue. Int. J. Oral Maxillofac. Implants 2016, 31, 813–819. [Google Scholar] [CrossRef]
- Huang, Y.-F.; Liu, S.-P.; Muo, C.-H.; Chang, C.-T. Prosthetic Design Related to Peri-Implant Bone Resorption in Microvascular Free Fibular Flap among Patients with Oral Cancer: A Retrospective Clinical Study. J. Prosthet. Dent. 2020, 124, 395–399. [Google Scholar] [CrossRef]
- Madi, M.; Htet, M.; Zakaria, O.; Alagl, A.; Kasugai, S. Re-Osseointegration of Dental Implants after Periimplantitis Treatments: A Systematic Review. Implant Dent. 2018, 27, 101–110. [Google Scholar] [CrossRef]
- Dreyer, H.; Grischke, J.; Tiede, C.; Eberhard, J.; Schweitzer, A.; Toikkanen, S.E.; Glöckner, S.; Krause, G.; Stiesch, M. Epidemiology and Risk Factors of Peri-Implantitis: A Systematic Review. J. Periodontal Res. 2018, 53, 657–681. [Google Scholar] [CrossRef]
- Albrektsson, T.; Chrcanovic, B.; Östman, P.-O.; Sennerby, L. Initial and Long-Term Crestal Bone Responses to Modern Dental Implants. Periodontol. 2000 2017, 73, 41–50. [Google Scholar] [CrossRef] [PubMed]
- Akagawa, Y.; Ichikawa, Y.; Nikai, H.; Tsuru, H. Interface Histology of Unloaded and Early Loaded Partially Stabilized Zirconia Endosseous Implant in Initial Bone Healing. J. Prosthet. Dent. 1993, 69, 599–604. [Google Scholar] [CrossRef]
- Araujo, M.G.; Lindhe, J. Peri-Implant Health. J. Periodontol. 2018, 89 (Suppl. 1), S249–S256. [Google Scholar] [CrossRef] [PubMed]
- Shibli, J.A.; Melo, L.; Ferrari, D.S.; Figueiredo, L.C.; Faveri, M.; Feres, M. Composition of Supra- and Subgingival Biofilm of Subjects with Healthy and Diseased Implants. Clin. Oral Implants Res. 2008, 19, 975–982. [Google Scholar] [CrossRef] [PubMed]
- Misch, C.E. Bone Density: A Key Determinant for Treatment Planning. In Contemporary Implant Dentistry, 3rd ed.; Elsevier: Amsterdam, The Netherlands, 2007; pp. 130–146. [Google Scholar]
- Tyrovola, J.B.; Odont, X.X. The “Mechanostat Theory” of Frost and the OPG/RANKL/RANK System. J. Cell. Biochem. 2015, 116, 2724–2729. [Google Scholar] [CrossRef] [PubMed]
- Frost, H.M. Bone’s Mechanostat: A 2003 Update. Anat. Rec. A 2003, 275, 1081–1101. [Google Scholar] [CrossRef]
- Scarano, A.; Noumbissi, S.; Gupta, S.; Inchingolo, F.; Stilla, P.; Lorusso, F. Scanning Electron Microscopy Analysis and Energy Dispersion X-ray Microanalysis to Evaluate the Effects of Decontamination Chemicals and Heat Sterilization on Implant Surgical Drills: Zirconia vs. Steel. Appl. Sci. 2019, 9, 2837. [Google Scholar] [CrossRef]
- Maglione, M.; Bevilacqua, L.; Dotto, F.; Costantinides, F.; Lorusso, F.; Scarano, A. Observational Study on the Preparation of the Implant Site with Piezosurgery vs. Drill: Comparison between the Two Methods in Terms of Postoperative Pain, Surgical Times, and Operational Advantages. BioMed Res. Int. 2019, 2019, 8483658. [Google Scholar] [CrossRef]
- Degidi, M.; Piattelli, A.; Shibli, J.A.; Perrotti, V.; Iezzi, G. Early Bone Formation around Immediately Restored Implants with and without Occlusal Contact: A Human Histologic and Histomorphometric Evaluation. Case Report. Int. J. Oral Maxillofac. Implants 2009, 24, 734–739. [Google Scholar]
- Shibli, J.A.; Mangano, C.; Mangano, F.; Rodrigues, J.A.; Cassoni, A.; Bechara, K.; Ferreia, J.D.B.; Dottore, A.M.; Iezzi, G.; Piattelli, A. Bone-to-Implant Contact around Immediately Loaded Direct Laser Metal-Forming Transitional Implants in Human Posterior Maxilla. J. Periodontol. 2013, 84, 732–737. [Google Scholar] [CrossRef]
- Iezzi, G.; Piattelli, A.; Mangano, C.; Shibli, J.A.; Vantaggiato, G.; Frosecchi, M.; Di Chiara, C.; Perrotti, V. Peri-Implant Bone Tissues around Retrieved Human Implants after Time Periods Longer than 5 Years: A Retrospective Histologic and Histomorphometric Evaluation of 8 Cases. Odontology 2014, 102, 116–121. [Google Scholar] [CrossRef]
- Lucchese, A.; Carinci, F.; Brunelli, G.; Monguzzi, R. Everstick® and Ribbond® Fiber Reinforced Composites: Scanning Electron Microscope (SEM) Comparative Analysis. Pediatr. Dent. 2011, 3, 17. [Google Scholar]
- Rigo, L.; Viscioni, A.; Franco, M.; Lucchese, A.; Zollino, I.; Brunelli, G.; Carinci, F. Overdentures on Implants Placed in Bone Augmented with Fresh Frozen Bone. Minerva Stomatol. 2011, 60, 5–14. [Google Scholar] [CrossRef] [PubMed]
- Danza, M.; Zollino, I.; Avantaggiato, A.; Lucchese, A.; Carinci, F. Distance between Implants Has a Potential Impact of Crestal Bone Resorption. Saudi Dent. J. 2011, 23, 129–133. [Google Scholar] [CrossRef] [PubMed]
- y Baena, R.R.; Lupi, S.M.; Pastorino, R.; Maiorana, C.; Lucchese, A.; Rizzo, S. Radiographic Evaluation of Regenerated Bone Following Poly(Lactic-Co-Glycolic) Acid/Hydroxyapatite and Deproteinized Bovine Bone Graft in Sinus Lifting. J. Craniofacial Surg. 2013, 24, 845–848. [Google Scholar] [CrossRef]
- Amari, Y.; Piattelli, A.; Apaza Alccayhuaman, K.A.; Mesa, N.F.; Ferri, M.; Iezzi, G.; Botticelli, D. Bone Healing at Non-Submerged Implants Installed with Different Insertion Torques: A Split-Mouth Histomorphometric Randomized Controlled Trial. Int. J. Implant Dent. 2019, 5, 39. [Google Scholar] [CrossRef]
- Gandini, P.; Schiavi, A.; Manuelli, M.; Camassa, D. Epidemiological Survey of Caries Occurrence in School Age Children. Mondo Ortod. 1989, 14, 63–72. [Google Scholar]
- Roncati, M.; Polizzi, E.; Cingano, L.; Gherlone, E.F.; Lucchese, A. Un ausilio all’igiene orale in pazienti diversamente abili. Dent. Cadmos 2013, 81, 447–452. [Google Scholar] [CrossRef]
- Prati, C.; Chersoni, S.; Lucchese, A.; Pashley, D.H.; Mongiorgi, R. Dentin Permeability after Toothbrushing with Different Toothpastes. Am. J. Dent. 1999, 12, 190–193. [Google Scholar]
- Palmieri, A.; Zollino, I.; Clauser, L.; Lucchese, A.; Girardi, A.; Farinella, F.; Carinci, F. Biological Effect of Resorbable Plates on Normal Osteoblasts and Osteoblasts Derived from Pfeiffer Syndrome. J. Craniofacial Surg. 2011, 22, 860–863. [Google Scholar] [CrossRef]
- Matarese, G.; Isola, G.; Ramaglia, L.; Dalessandri, D.; Lucchese, A.; Alibrandi, A.; Fabiano, F.; Cordasco, G. Periodontal Biotype: Characteristic, Prevalence and Dimensions Related to Dental Malocclusion. Minerva Stomatol. 2016, 65, 231–238. [Google Scholar] [PubMed]
- Rodriguez y Baena, R.; Pastorino, R.; Gherlone, E.; Perillo, L.; Saturnino, S.; Lucchese, A. Histomorphometric Evaluation of Two Different Bone Substitutes in Sinus Augmentation Procedures: A Randomized Controlled Trial in Humans. Int. J. Oral Maxillofac. Implants 2017, 32, 188–194. [Google Scholar] [CrossRef] [PubMed]
- Manuelli, M. A Peaceful Man. Prog. Orthod. 2012, 13, 1. [Google Scholar] [CrossRef]
- Bertossi, D.; Giampaoli, G.; Lucchese, A.; Manuelli, M.; Albanese, M.; Nocini, R.; Nocini, P.F. The Skin Rejuvenation Associated Treatment—Fraxel Laser, Microbotox, and Low G Prime Hyaluronic Acid: Preliminary Results. Lasers Med. Sci. 2019, 34, 1449–1455. [Google Scholar] [CrossRef]



| Insertion Torque [N/cm] | Mean | SD |
|---|---|---|
| CRYSTAL 3.8 | 16.83 | 1.947 |
| CRYSTAL 4.8 | 19.1 | 1.236 |
| ELISIR 3.8 | 12.65 | 3.034 |
| ELISIR 4.8 | 20.75 | 3.514 |
| Insertion Torque | Mean Diff. | 95.00% CI of Diff. | Adjusted p Value |
|---|---|---|---|
| CRYSTAL 3.8 vs. CRYSTAL 4.8 | −2.275 | −3.819 to −0.7306 | 0.0008 |
| CRYSTAL 3.8 vs. ELISIR 3.8 | 4.175 | 2.631 to 5.719 | <0.0001 |
| CRYSTAL 3.8 vs. ELISIR 4.8 | −3.925 | −5.469 to −2.381 | <0.0001 |
| CRYSTAL 4.8 vs. ELISIR 3.8 | 6.450 | 4.906 to 7.994 | <0.0001 |
| CRYSTAL 4.8 vs. ELISIR 4.8 | −1.650 | −3.194 to −0.1056 | 0.0297 |
| Removal [N/cm] | Mean | SD |
|---|---|---|
| CRYSTAL 3.8 | 5.85 | 1.099 |
| CRYSTAL 4.8 | 8.45 | 1.28 |
| ELISIR 3.8 | 10.2 | 3.057 |
| ELISIR 4.8 | 15.85 | 3.215 |
| Removal | Mean Diff. | 95.00% CI of Diff. | Adjusted p Value |
|---|---|---|---|
| CRYSTAL 3.8 vs. CRYSTAL 4.8 | −2.600 | −4.014 to −1.186 | <0.0001 |
| CRYSTAL 3.8 vs. ELISIR 3.8 | −4.350 | −5.764 to −2.936 | <0.0001 |
| CRYSTAL 3.8 vs. ELISIR 4.8 | −10.00 | −11.41 to −8.586 | <0.0001 |
| CRYSTAL 4.8 vs. ELISIR 3.8 | −1.750 | −3.164 to −0.3359 | 0.0072 |
| CRYSTAL 4.8 vs. ELISIR 4.8 | −7.400 | −8.814 to −5.986 | <0.0001 |
| Periotest | Mean | SD |
|---|---|---|
| CRYSTAL 3.8 | 4.3 | 1.1 |
| CRYSTAL 4.8 | 5.1 | 1.4 |
| ELISIR 3.8 | 4.1 | 1.6 |
| ELISIR 4.8 | 2.0 | 0.4 |
| Periotest | Mean Diff. | 95.00% CI of Diff. | Adjusted p Value |
|---|---|---|---|
| CRYSTAL 3.8 vs. CRYSTAL 4.8 | −1.534 | −2.771 to −0.2966 | 0.0085 |
| CRYSTAL 3.8 vs. ELISIR 3.8 | 0.5813 | −0.6559 to 1.818 | 0.6632 |
| CRYSTAL 3.8 vs. ELISIR 4.8 | 4.239 | 3.002 to 5.476 | <0.0001 |
| CRYSTAL 4.8 vs. ELISIR 3.8 | 2.124 | 0.8866 to 3.361 | 0.0001 |
| CRYSTAL 4.8 vs. ELISIR 4.8 | –1.534 | –2.771 to –0.2966 | 0.0085 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fanali, S.; Tumedei, M.; Pignatelli, P.; Lucchese, A.; Inchingolo, F.; Piattelli, A.; Iezzi, G. Comparative In Vitro Evaluation of the Primary Stability in D3 Synthetic Bone of Two Different Shapes and Pitches of the Implant Threads. Appl. Sci. 2021, 11, 5612. https://doi.org/10.3390/app11125612
Fanali S, Tumedei M, Pignatelli P, Lucchese A, Inchingolo F, Piattelli A, Iezzi G. Comparative In Vitro Evaluation of the Primary Stability in D3 Synthetic Bone of Two Different Shapes and Pitches of the Implant Threads. Applied Sciences. 2021; 11(12):5612. https://doi.org/10.3390/app11125612
Chicago/Turabian StyleFanali, Stefano, Margherita Tumedei, Pamela Pignatelli, Alessandra Lucchese, Francesco Inchingolo, Adriano Piattelli, and Giovanna Iezzi. 2021. "Comparative In Vitro Evaluation of the Primary Stability in D3 Synthetic Bone of Two Different Shapes and Pitches of the Implant Threads" Applied Sciences 11, no. 12: 5612. https://doi.org/10.3390/app11125612
APA StyleFanali, S., Tumedei, M., Pignatelli, P., Lucchese, A., Inchingolo, F., Piattelli, A., & Iezzi, G. (2021). Comparative In Vitro Evaluation of the Primary Stability in D3 Synthetic Bone of Two Different Shapes and Pitches of the Implant Threads. Applied Sciences, 11(12), 5612. https://doi.org/10.3390/app11125612











