MR Image Changes of Normal-Appearing Brain Tissue after Radiotherapy
Abstract
Simple Summary
Abstract
1. Introduction
2. Determination of Anatomical/Morphological Changes in Normal-Appearing Tissue after Radiotherapy
3. Determination of Microstructural Changes in Normal-Appearing Tissue after Radiotherapy
4. Determination of Vascular Changes in Normal-Appearing Tissue after Radiotherapy
4.1. Perfusion-Weighted Imaging
4.2. Susceptibility-Weighted Imaging
5. Determination of Metabolic Changes in Normal-Appearing Tissue after Radiotherapy
6. Conclusions and Summary
7. Review Criteria
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Stupp, R.; Hegi, M.E.; Mason, W.P.; van den Bent, M.J.; Taphoorn, M.J.B.; Janzer, R.C.; Ludwin, S.K.; Allgeier, A.; Fisher, B.; Belanger, K.; et al. Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol. 2009, 10, 459–466. [Google Scholar] [CrossRef]
- Owonikoko, T.K.; Arbiser, J.; Zelnak, A.; Shu, H.-K.G.; Shim, H.; Robin, A.M.; Kalkanis, S.N.; Whitsett, T.G.; Salhia, B.; Tran, N.L.; et al. Current approaches to the treatment of metastatic brain tumours. Nat. Rev. Clin. Oncol. 2014, 11, 203–222. [Google Scholar] [CrossRef]
- McTyre, E.; Scott, J.; Chinnaiyan, P. Whole brain radiotherapy for brain metastasis. Surg. Neurol. Int. 2013, 4, S236–S244. [Google Scholar] [CrossRef]
- Chang, S.M.; Parney, I.F.; Huang, W.; Anderson, F.A.; Asher, A.L.; Bernstein, M.; Lillehei, K.O.; Brem, H.; Berger, M.S.; Laws, E.R. Patterns of care for adults with newly diagnosed malignant glioma. JAMA 2005, 293, 557–564. [Google Scholar] [CrossRef]
- Wu, P.H.; Coultrap, S.; Pinnix, C.; Davies, K.D.; Tailor, R.; Ang, K.K.; Browning, M.D.; Grosshans, D.R. Radiation induces acute alterations in neuronal function. PLoS ONE 2012, 7, e37677. [Google Scholar] [CrossRef]
- Makale, M.T.; McDonald, C.R.; Hattangadi-Gluth, J.A.; Kesari, S. Mechanisms of radiotherapy-associated cognitive disability in patients with brain tumours. Nat. Rev. Neurol. 2017, 13, 52–64. [Google Scholar] [CrossRef]
- Tofilon, P.J.; Fike, J.R. The Radioresponse of the Central Nervous System: A Dynamic Process. Radiat. Res. 2000, 153, 357–370. [Google Scholar] [CrossRef]
- Mildenberger, M.; Beach, T.G.; McGeer, E.G.; Ludgate, C.M. An animal model of prophylactic cranial irradiation: Histologic effects at acute, early and delayed stages. Int. J. Radiat. Oncol. Biol. Phys. 1990, 18, 1051–1060. [Google Scholar] [CrossRef]
- Béhin, A.; Delattre, J.-Y. Complications of radiation therapy on the brain and spinal cord. Semin. Neurol. 2004, 24, 405–417. [Google Scholar] [CrossRef] [PubMed]
- Miyawaki, D.; Murakami, M.; Demizu, Y.; Sasaki, R.; Niwa, Y.; Terashima, K.; Nishimura, H.; Hishikawa, Y.; Sugimura, K. Brain injury after proton therapy or carbon ion therapy for head-and-neck cancer and skull base tumors. Int. J. Radiat. Oncol. Biol. Phys. 2009, 75, 378–384. [Google Scholar] [CrossRef] [PubMed]
- Parvez, K.; Parvez, A.; Zadeh, G. The diagnosis and treatment of pseudoprogression, radiation necrosis and brain tumor recurrence. Int. J. Mol. Sci. 2014, 15, 11832–11846. [Google Scholar] [CrossRef]
- Sheline, G.E.; Wara, W.M.; Smith, V. Therapeutic irradiation and brain injury. Int. J. Radiat. Oncol. Biol. Phys. 1980, 6, 1215–1228. [Google Scholar] [CrossRef]
- Greene-Schloesser, D.; Robbins, M.E.; Peiffer, A.M.; Shaw, E.G.; Wheeler, K.T.; Chan, M.D. Radiation-induced brain injury: A review. Front. Oncol. 2012, 2, 73. [Google Scholar] [CrossRef] [PubMed]
- Frost, M.H.; Sloan, J.A. Quality of life measurements: A soft outcome—Or is it? Am. J. Manag. Care 2002, 8, S574–S579. [Google Scholar] [PubMed]
- Meyers, C.A.; Geara, F.; Wong, P.-F.; Morrison, W.H. Neurocognitive effects of therapeutic irradiation for base of skull tumors. Int. J. Radiat. Oncol. Biol. Phys. 2000, 46, 51–55. [Google Scholar] [CrossRef]
- Merchant, T.E.; Conklin, H.M.; Wu, S.; Lustig, R.H.; Xiong, X. Late effects of conformal radiation therapy for pediatric patients with low-grade glioma: Prospective evaluation of cognitive, endocrine, and hearing deficits. J. Clin. Oncol. 2009, 27, 3691–3697. [Google Scholar] [CrossRef]
- Barazzuol, L.; Coppes, R.P.; van Luijk, P. Prevention and treatment of radiotherapy-induced side effects. Mol. Oncol. 2020, 14, 1538–1554. [Google Scholar] [CrossRef]
- Armstrong, C.L.; Gyato, K.; Awadalla, A.W.; Lustig, R.; Tochner, Z.A. A critical review of the clinical effects of therapeutic irradiation damage to the brain: The roots of controversy. Neuropsychol. Rev. 2004, 14, 65–86. [Google Scholar] [CrossRef]
- Walker, A.J.; Ruzevick, J.; Malayeri, A.A.; Rigamonti, D.; Lim, M.; Redmond, K.J.; Kleinberg, L. Postradiation imaging changes in the CNS: How can we differentiate between treatment effect and disease progression? Future Oncol. 2014, 10, 1277–1297. [Google Scholar] [CrossRef]
- Verma, N.; Cowperthwaite, M.C.; Burnett, M.G.; Markey, M.K. Differentiating tumor recurrence from treatment necrosis: A review of neuro-oncologic imaging strategies. Neuro Oncol. 2013, 15, 515–534. [Google Scholar] [CrossRef]
- Kłos, J.; van Laar, P.J.; Sinnige, P.F.; Enting, R.H.; Kramer, M.C.A.; van der Weide, H.L.; van Buchem, M.A.; Dierckx, R.A.J.O.; Borra, R.J.H.; van der Hoorn, A. Quantifying effects of radiotherapy-induced microvascular injury; review of established and emerging brain MRI techniques. Radiother. Oncol. 2019, 140, 41–53. [Google Scholar] [CrossRef]
- Welzel, T.; Tanner, J.M. Nebenwirkungen nach Strahlentherapie in der Bildgebung. Radiologe 2018, 58, 754–761. [Google Scholar] [CrossRef]
- Yang, J.; Xu, Z.; Gao, J.; Liao, C.; Wang, P.; Liu, Y.; Ke, T.; Li, Q.; Han, D. Evaluation of early acute radiation-induced brain injury: Hybrid multifunctional MRI-based study. Magn. Reson. Imaging 2018, 54, 101–108. [Google Scholar] [CrossRef]
- Tringale, K.R.; Nguyen, T.T.; Karunamuni, R.; Seibert, T.; Huynh-Le, M.-P.; Connor, M.; Moiseenko, V.; Gorman, M.K.; Marshall, A.; Tibbs, M.D.; et al. Quantitative Imaging Biomarkers of Damage to Critical Memory Regions Are Associated With Post-Radiation Therapy Memory Performance in Brain Tumor Patients. Int. J. Radiat. Oncol. Biol. Phys. 2019, 105, 773–783. [Google Scholar] [CrossRef] [PubMed]
- Bálentová, S.; Hnilicová, P.; Kalenská, D.; Baranovičová, E.; Muríň, P.; Bittšanský, M.; Hajtmanová, E.; Lehotský, J.; Adamkov, M. Metabolic and histopathological changes in the brain and plasma of rats exposed to fractionated whole-brain irradiation. Brain Res. 2019, 1708, 146–159. [Google Scholar] [CrossRef] [PubMed]
- Tian, Y.; Shi, Z.; Yang, S.; Chen, Y.; Bao, S. Changes in myelin basic protein and demyelination in the rat brain within 3 months of single 2-, 10-, or 30-Gy whole-brain radiation treatments. J. Neurosurg. 2008, 109, 881–888. [Google Scholar] [CrossRef] [PubMed]
- Chan, K.C.; Khong, P.-L.; Cheung, M.M.; Wang, S.; Cai, K.-X.; Wu, E.X. MRI of late microstructural and metabolic alterations in radiation-induced brain injuries. J. Magn. Reson. Imaging 2009, 29, 1013–1020. [Google Scholar] [CrossRef]
- Tanyildizi, Y.; Keweloh, S.; Neu, M.A.; Russo, A.; Wingerter, A.; Weyer-Elberich, V.; Stockinger, M.; Schmidberger, H.; Brockmann, M.A.; Faber, J. Radiation-induced vascular changes in the intracranial irradiation field in medulloblastoma survivors: An MRI study. Radiother. Oncol. 2019, 136, 50–55. [Google Scholar] [CrossRef]
- Reddick, W.E.; Mulhern, R.K.; Elkin, T.; Glass, J.O.; Merchant, T.E.; Langston, J.W. A hybrid neural network analysis of subtle brain volume differences in children surviving brain tumors. Magn. Reson. Imaging 1998, 16, 413–421. [Google Scholar] [CrossRef]
- Reddickaij, W.E.; Russell, J.; Glass, J.O.; Xiong, X.; Mulhern, R.K.; Langston, J.W.; Merchant, T.E.; Kun, L.E.; Gajjar, A. Subtle white matter volume differences in children treated for medulloblastoma with conventional or reduced dose craniospinal irradiation. Magn. Reson. Imaging 2000, 18, 787–793. [Google Scholar] [CrossRef]
- Reddick, W.E.; White, H.A.; Glass, J.O.; Wheeler, G.C.; Thompson, S.J.; Gajjar, A.; Leigh, L.; Mulhern, R.K. Developmental model relating white matter volume to neurocognitive deficits in pediatric brain tumor survivors. Cancer 2003, 97, 2512–2519. [Google Scholar] [CrossRef]
- Reddick, W.E.; Glass, J.O.; Palmer, S.L.; Wu, S.; Gajjar, A.; Langston, J.W.; Kun, L.E.; Xiong, X.; Mulhern, R.K. Atypical white matter volume development in children following craniospinal irradiation. Neuro Oncol. 2005, 7, 12–19. [Google Scholar] [CrossRef] [PubMed]
- Mulhern, R.K.; Palmer, S.L.; Reddick, W.E.; Glass, J.O.; Kun, L.E.; Taylor, J.; Langston, J.; Gajjar, A. Risks of young age for selected neurocognitive deficits in medulloblastoma are associated with white matter loss. J. Clin. Oncol. 2001, 19, 472–479. [Google Scholar] [CrossRef] [PubMed]
- Mulhern, R.K.; Reddick, W.E.; Palmer, S.L.; Glass, J.O.; Elkin, T.D.; Kun, L.E.; Taylor, J.; Langston, J.; Gajjar, A. Neurocognitive deficits in medulloblastoma survivors and white matter loss. Ann Neurol. 1999, 46, 834–841. [Google Scholar] [CrossRef]
- Gommlich, A.; Raschke, F.; Wahl, H.; Troost, E.G.C. Retrospective assessment of MRI-based volumetric changes of normal tissues in glioma patients following radio(chemo)therapy. Clin. Transl. Radiat. Oncol. 2018, 8, 17–21. [Google Scholar] [CrossRef] [PubMed]
- Petr, J.; Platzek, I.; Hofheinz, F.; Mutsaerts, H.J.M.M.; Asllani, I.; van Osch, M.J.P.; Seidlitz, A.; Krukowski, P.; Gommlich, A.; Beuthien-Baumann, B.; et al. Photon vs. proton radiochemotherapy: Effects on brain tissue volume and perfusion. Radiother. Oncol. 2018, 128, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Prust, M.J.; Jafari-Khouzani, K.; Kalpathy-Cramer, J.; Polaskova, P.; Batchelor, T.T.; Gerstner, E.R.; Dietrich, J. Standard chemoradiation for glioblastoma results in progressive brain volume loss. Neurology 2015, 85, 683–691. [Google Scholar] [CrossRef]
- Nagel, B.J.; Palmer, S.L.; Reddick, W.E.; Glass, J.O.; Helton, K.J.; Wu, S.; Xiong, X.; Kun, L.E.; Gajjar, A.; Mulhern, R.K. Abnormal hippocampal development in children with medulloblastoma treated with risk-adapted irradiation. Ajnr Am. J. Neuroradiol. 2004, 25, 1575–1582. [Google Scholar]
- Hong, A.; Hallock, H.; Valenzuela, M.; Lo, S.; Steel, V.; Paton, E.; Ng, D.; Jacobsen, K.D.; Reisse, C.H.; Fogarty, G.B. Change in the Hippocampal Volume After Whole-Brain Radiation Therapy With or Without Hippocampal Avoidance Technique. Int. J. Radiat. Oncol. Biol. Phys. 2015, 93, E82. [Google Scholar] [CrossRef]
- Shi, L.; Du, F.-L.; Sun, Z.-W.; Zhang, L.; Chen, Y.-Y.; Xie, T.-M.; Li, P.-J.; Huang, S.; Dong, B.-Q.; Zhang, M.-M. Radiation-induced gray matter atrophy in patients with nasopharyngeal carcinoma after intensity modulated radiotherapy: A MRI magnetic resonance imaging voxel-based morphometry study. Quant. Imaging Med. Surg. 2018, 8, 902–909. [Google Scholar] [CrossRef]
- Takeshita, Y.; Watanabe, K.; Kakeda, S.; Hamamura, T.; Sugimoto, K.; Masaki, H.; Ueda, I.; Igata, N.; Ohguri, T.; Korogi, Y. Early volume reduction of the hippocampus after whole-brain radiation therapy: An automated brain structure segmentation study. Jpn. J. Radiol. 2020, 38, 118–125. [Google Scholar] [CrossRef]
- Seibert, T.M.; Karunamuni, R.; Bartsch, H.; Kaifi, S.; Krishnan, A.P.; Dalia, Y.; Burkeen, J.; Murzin, V.; Moiseenko, V.; Kuperman, J.; et al. Radiation Dose-Dependent Hippocampal Atrophy Detected With Longitudinal Volumetric Magnetic Resonance Imaging. Int. J. Radiat. Oncol. Biol. Phys. 2017, 97, 263–269. [Google Scholar] [CrossRef]
- Olsson, E.; Eckerström, C.; Berg, G.; Borga, M.; Ekholm, S.; Johannsson, G.; Ribbelin, S.; Starck, G.; Wysocka, A.; Löfdahl, E.; et al. Hippocampal volumes in patients exposed to low-dose radiation to the basal brain. A case-control study in long-term survivors from cancer in the head and neck region. Radiat. Oncol. 2012, 7, 202. [Google Scholar] [CrossRef]
- Nagtegaal, S.H.J.; David, S.; Philippens, M.E.P.; Snijders, T.J.; Leemans, A.; Verhoeff, J.J.C. Dose-dependent volume loss in subcortical deep grey matter structures after cranial radiotherapy. Clin. Transl. Radiat. Oncol. 2021, 26, 35–41. [Google Scholar] [CrossRef]
- Huynh-Le, M.-P.; Karunamuni, R.; Moiseenko, V.; Farid, N.; McDonald, C.R.; Hattangadi-Gluth, J.A.; Seibert, T.M. Dose-dependent atrophy of the amygdala after radiotherapy. Radiother. Oncol. 2019, 136, 44–49. [Google Scholar] [CrossRef]
- Palmer, S.L.; Reddick, W.E.; Glass, J.O.; Gajjar, A.; Goloubeva, O.; Mulhern, R.K. Decline in corpus callosum volume among pediatric patients with medulloblastoma: Longitudinal MR imaging study. Ajnr Am. J. Neuroradiol. 2002, 23, 1088–1094. [Google Scholar]
- Liu, A.K.; Marcus, K.J.; Fischl, B.; Grant, P.E.; Poussaint, T.Y.; Rivkin, M.J.; Davis, P.; Tarbell, N.J.; Yock, T.I. Changes in cerebral cortex of children treated for medulloblastoma. Int. J. Radiat. Oncol. Biol. Phys. 2007, 68, 992–998. [Google Scholar] [CrossRef]
- Seibert, T.M.; Karunamuni, R.; Kaifi, S.; Burkeen, J.; Connor, M.; Krishnan, A.P.; White, N.S.; Farid, N.; Bartsch, H.; Murzin, V.; et al. Cerebral Cortex Regions Selectively Vulnerable to Radiation Dose-Dependent Atrophy. Int. J. Radiat. Oncol. Biol. Phys. 2017, 97, 910–918. [Google Scholar] [CrossRef]
- Karunamuni, R.A.; Moore, K.L.; Seibert, T.M.; Li, N.; White, N.S.; Bartsch, H.; Carmona, R.; Marshall, D.; McDonald, C.R.; Farid, N.; et al. Radiation sparing of cerebral cortex in brain tumor patients using quantitative neuroimaging. Radiother. Oncol. 2016, 118, 29–34. [Google Scholar] [CrossRef]
- Karunamuni, R.; Bartsch, H.; White, N.S.; Moiseenko, V.; Carmona, R.; Marshall, D.C.; Seibert, T.M.; McDonald, C.R.; Farid, N.; Krishnan, A.; et al. Dose-Dependent Cortical Thinning After Partial Brain Irradiation in High-Grade Glioma. Int. J. Radiat. Oncol. Biol. Phys. 2016, 94, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Raschke, F.; Seidlitz, A.; Wesemann, T.; Löck, S.; Jentsch, C.; Platzek, I.; Petr, J.; van den Hoff, J.; Kotzerke, J.; Beuthien-Baumann, B.; et al. Dose dependent cerebellar atrophy in glioma patients after radio(chemo)therapy. Radiother. Oncol. 2020, 150, 262–267. [Google Scholar] [CrossRef]
- Ailion, A.S.; King, T.Z.; Wang, L.; Fox, M.E.; Mao, H.; Morris, R.M.; Crosson, B. Cerebellar Atrophy in Adult Survivors of Childhood Cerebellar Tumor. J. Int. Neuropsychol. Soc. 2016, 22, 501–511. [Google Scholar] [CrossRef] [PubMed]
- Scahill, R.I.; Frost, C.; Jenkins, R.; Whitwell, J.L.; Rossor, M.N.; Fox, N.C. A longitudinal study of brain volume changes in normal aging using serial registered magnetic resonance imaging. Arch. Neurol. 2003, 60, 989–994. [Google Scholar] [CrossRef]
- Good, C.D.; Johnsrude, I.S.; Ashburner, J.; Henson, R.N.; Friston, K.J.; Frackowiak, R.S. A voxel-based morphometric study of ageing in 465 normal adult human brains. Neuroimage 2001, 14, 21–36. [Google Scholar] [CrossRef] [PubMed]
- Giedd, J.N.; Blumenthal, J.; Jeffries, N.O.; Rajapakse, J.C.; Vaituzis, A.; Liu, H.; Berry, Y.C.; Tobin, M.; Nelson, J.; Castellanos, F. Development of the human corpus callosum during childhood and adolescence: A longitudinal MRI study. Prog. Neuro Psychopharmacol. Biol. Psychiatry 1999, 23, 571–588. [Google Scholar] [CrossRef]
- Giedd, J.N.; Rumsey, J.M.; Castellanos, F.; Rajapakse, J.C.; Kaysen, D.; Catherine Vaituzis, A.; Vauss, Y.C.; Hamburger, S.D.; Rapoport, J.L. A quantitative MRI study of the corpus callosum in children and adolescents. Dev. Brain Res. 1996, 91, 274–280. [Google Scholar] [CrossRef]
- Schuff, N.; Woerner, N.; Boreta, L.; Kornfield, T.; Shaw, L.M.; Trojanowski, J.Q.; Thompson, P.M.; Jack, C.R.; Weiner, M.W. MRI of hippocampal volume loss in early Alzheimer’s disease in relation to ApoE genotype and biomarkers. Brain 2009, 132, 1067–1077. [Google Scholar] [CrossRef]
- Sá, M.J.; Ruela, C.; Madeira, M.D. Dendritic right/left asymmetries in the neurons of the human hippocampal formation: A quantitative Golgi study. Arq. Neuropsiquiatr. 2007, 65, 1105–1113. [Google Scholar] [CrossRef][Green Version]
- Poulin, S.P.; Dautoff, R.; Morris, J.C.; Barrett, L.F.; Dickerson, B.C. Amygdala atrophy is prominent in early Alzheimer’s disease and relates to symptom severity. Psychiatry Res. 2011, 194, 7–13. [Google Scholar] [CrossRef]
- Soininen, H.S.; Partanen, K.; Pitkänen, A.; Vainio, P.; Hänninen, T.; Hallikainen, M.; Koivisto, K.; Riekkinen, P.J. Volumetric MRI analysis of the amygdala and the hippocampus in subjects with age-associated memory impairment: Correlation to visual and verbal memory. Neurology 1994, 44, 1660–1668. [Google Scholar] [CrossRef]
- Principles of Neural Science, 4th ed.; Kandel, E.R., Schwartz, J.H., Jessell, T.M., Eds.; McGraw-Hill Health Professions Division: New York, NY, USA, 2000; ISBN 0838577016. [Google Scholar]
- Cabeza, R.; Nyberg, L. Imaging cognition II: An empirical review of 275 PET and fMRI studies. J. Cogn. Neurosci. 2000, 12, 1–47. [Google Scholar] [CrossRef] [PubMed]
- Sabuncu, M.R.; Desikan, R.S.; Sepulcre, J.; Yeo, B.T.T.; Liu, H.; Schmansky, N.J.; Reuter, M.; Weiner, M.W.; Buckner, R.L.; Sperling, R.A.; et al. The dynamics of cortical and hippocampal atrophy in Alzheimer disease. Arch. Neurol. 2011, 68, 1040–1048. [Google Scholar] [CrossRef]
- Salat, D.H.; Buckner, R.L.; Snyder, A.Z.; Greve, D.N.; Desikan, R.S.R.; Busa, E.; Morris, J.C.; Dale, A.M.; Fischl, B. Thinning of the cerebral cortex in aging. Cereb. Cortex 2004, 14, 721–730. [Google Scholar] [CrossRef]
- Brun, A.; Englund, E. Regional pattern of degeneration in Alzheimer’s disease: Neuronal loss and histopathological grading. Histopathology 1981, 5, 549–564. [Google Scholar] [CrossRef]
- Palmer, S.L.; Armstrong, C.; Onar-Thomas, A.; Wu, S.; Wallace, D.; Bonner, M.J.; Schreiber, J.; Swain, M.; Chapieski, L.; Mabbott, D.; et al. Processing speed, attention, and working memory after treatment for medulloblastoma: An international, prospective, and longitudinal study. J. Clin. Oncol. 2013, 31, 3494–3500. [Google Scholar] [CrossRef]
- Khong, P.-L.; Kwong, D.L.W.; Chan, G.C.F.; Sham, J.S.T.; Chan, F.-L.; Ooi, G.-C. Diffusion-tensor imaging for the detection and quantification of treatment-induced white matter injury in children with medulloblastoma: A pilot study. Ajnr Am. J. Neuroradiol. 2003, 24, 734–740. [Google Scholar] [PubMed]
- Chawla, S.; Wang, S.; Kim, S.; Sheriff, S.; Lee, P.; Rengan, R.; Lin, A.; Melhem, E.; Maudsley, A.; Poptani, H. Radiation injury to the normal brain measured by 3D-echo-planar spectroscopic imaging and diffusion tensor imaging: Initial experience. J. Neuroimaging 2015, 25, 97–104. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.-Z.; Qiu, S.-J.; Lv, X.-F.; Wang, Y.-Y.; Liang, Y.; Xiong, W.-F.; Ouyang, Z.-B. Diffusion tensor imaging and 1H-MRS study on radiation-induced brain injury after nasopharyngeal carcinoma radiotherapy. Clin. Radiol. 2012, 67, 340–345. [Google Scholar] [CrossRef] [PubMed]
- Mabbott, D.J.; Noseworthy, M.D.; Bouffet, E.; Rockel, C.; Laughlin, S. Diffusion tensor imaging of white matter after cranial radiation in children for medulloblastoma: Correlation with IQ. Neuro Oncol. 2006, 8, 244–252. [Google Scholar] [CrossRef] [PubMed]
- Xiong, W.F.; Qiu, S.J.; Wang, H.Z.; Lv, X.F. 1H-MR spectroscopy and diffusion tensor imaging of normal-appearing temporal white matter in patients with nasopharyngeal carcinoma after irradiation: Initial experience. J. Magn. Reson. Imaging 2013, 37, 101–108. [Google Scholar] [CrossRef] [PubMed]
- Duan, F.; Cheng, J.; Jiang, J.; Chang, J.; Zhang, Y.; Qiu, S. Whole-brain changes in white matter microstructure after radiotherapy for nasopharyngeal carcinoma: A diffusion tensor imaging study. Eur. Arch. Otorhinolaryngol. 2016, 273, 4453–4459. [Google Scholar] [CrossRef]
- Leung, L.H.T.; Ooi, G.C.; Kwong, D.L.W.; Chan, G.C.F.; Cao, G.; Khong, P.L. White-matter diffusion anisotropy after chemo-irradiation: A statistical parametric mapping study and histogram analysis. Neuroimage 2004, 21, 261–268. [Google Scholar] [CrossRef]
- Qiu, D.; Kwong, D.L.W.; Chan, G.C.F.; Leung, L.H.T.; Khong, P.-L. Diffusion tensor magnetic resonance imaging finding of discrepant fractional anisotropy between the frontal and parietal lobes after whole-brain irradiation in childhood medulloblastoma survivors: Reflection of regional white matter radiosensitivity? Int. J. Radiat. Oncol. Biol. Phys. 2007, 69, 846–851. [Google Scholar] [CrossRef] [PubMed]
- Welzel, T.; Niethammer, A.; Mende, U.; Heiland, S.; Wenz, F.; Debus, J.; Krempien, R. Diffusion tensor imaging screening of radiation-induced changes in the white matter after prophylactic cranial irradiation of patients with small cell lung cancer: First results of a prospective study. Ajnr Am. J. Neuroradiol. 2008, 29, 379–383. [Google Scholar] [CrossRef]
- Makola, M.; Douglas Ris, M.; Mahone, E.M.; Yeates, K.O.; Cecil, K.M. Long-term effects of radiation therapy on white matter of the corpus callosum: A diffusion tensor imaging study in children. Pediatr. Radiol. 2017, 47, 1809–1816. [Google Scholar] [CrossRef]
- Nagesh, V.; Tsien, C.I.; Chenevert, T.L.; Ross, B.D.; Lawrence, T.S.; Junick, L.; Cao, Y. Radiation-induced changes in normal-appearing white matter in patients with cerebral tumors: A diffusion tensor imaging study. Int. J. Radiat. Oncol. Biol. Phys. 2008, 70, 1002–1010. [Google Scholar] [CrossRef] [PubMed]
- Nazem-Zadeh, M.-R.; Chapman, C.H.; Lawrence, T.L.; Tsien, C.I.; Cao, Y. Radiation therapy effects on white matter fiber tracts of the limbic circuit. Med. Phys. 2012, 39, 5603–5613. [Google Scholar] [CrossRef]
- Connor, M.; Karunamuni, R.; McDonald, C.; Seibert, T.; White, N.; Moiseenko, V.; Bartsch, H.; Farid, N.; Kuperman, J.; Krishnan, A.; et al. Regional susceptibility to dose-dependent white matter damage after brain radiotherapy. Radiother. Oncol. 2017, 123, 209–217. [Google Scholar] [CrossRef] [PubMed]
- Connor, M.; Karunamuni, R.; McDonald, C.; White, N.; Pettersson, N.; Moiseenko, V.; Seibert, T.; Marshall, D.; Cervino, L.; Bartsch, H.; et al. Dose-dependent white matter damage after brain radiotherapy. Radiother. Oncol. 2016, 121, 209–216. [Google Scholar] [CrossRef]
- Kitahara, S.; Nakasu, S.; Murata, K.; Sho, K.; Ito, R. Evaluation of treatment-induced cerebral white matter injury by using diffusion-tensor MR imaging: Initial experience. Ajnr Am. J. Neuroradiol. 2005, 26, 2200–2206. [Google Scholar]
- Hope, T.R.; Vardal, J.; Bjørnerud, A.; Larsson, C.; Arnesen, M.R.; Salo, R.A.; Groote, I.R. Serial diffusion tensor imaging for early detection of radiation-induced injuries to normal-appearing white matter in high-grade glioma patients. J. Magn. Reson. Imaging 2015, 41, 414–423. [Google Scholar] [CrossRef] [PubMed]
- Haris, M.; Kumar, S.; Raj, M.K.; Das, K.J.M.; Sapru, S.; Behari, S.; Rathore, R.K.S.; Narayana, P.A.; Gupta, R.K. Serial diffusion tensor imaging to characterize radiation-induced changes in normal-appearing white matter following radiotherapy in patients with adult low-grade gliomas. Radiat. Med. 2008, 26, 140–150. [Google Scholar] [CrossRef]
- Nilsen, L.B.; Digernes, I.; Grøvik, E.; Saxhaug, C.; Latysheva, A.; Geier, O.; Breivik, B.; Sætre, D.O.; Jacobsen, K.D.; Helland, Å.; et al. Responses in the diffusivity and vascular function of the irradiated normal brain are seen up until 18 months following SRS of brain metastases. Neurooncol. Adv. 2020, 2, vdaa028. [Google Scholar] [CrossRef] [PubMed]
- Chapman, C.H.; Nagesh, V.; Sundgren, P.C.; Buchtel, H.; Chenevert, T.L.; Junck, L.; Lawrence, T.S.; Tsien, C.I.; Cao, Y. Diffusion tensor imaging of normal-appearing white matter as biomarker for radiation-induced late delayed cognitive decline. Int. J. Radiat. Oncol. Biol. Phys. 2012, 82, 2033–2040. [Google Scholar] [CrossRef] [PubMed]
- Chapman, C.H.; Nazem-Zadeh, M.; Lee, O.E.; Schipper, M.J.; Tsien, C.I.; Lawrence, T.S.; Cao, Y. Regional variation in brain white matter diffusion index changes following chemoradiotherapy: A prospective study using tract-based spatial statistics. PLoS ONE 2013, 8, e57768. [Google Scholar] [CrossRef] [PubMed]
- Chapman, C.H.; Zhu, T.; Nazem-Zadeh, M.; Tao, Y.; Buchtel, H.A.; Tsien, C.I.; Lawrence, T.S.; Cao, Y. Diffusion tensor imaging predicts cognitive function change following partial brain radiotherapy for low-grade and benign tumors. Radiother. Oncol. 2016, 120, 234–240. [Google Scholar] [CrossRef] [PubMed]
- Zhu, T.; Chapman, C.H.; Tsien, C.; Kim, M.; Spratt, D.E.; Lawrence, T.S.; Cao, Y. Effect of the Maximum Dose on White Matter Fiber Bundles Using Longitudinal Diffusion Tensor Imaging. Int. J. Radiat. Oncol. Biol. Phys. 2016, 96, 696–705. [Google Scholar] [CrossRef] [PubMed]
- Raschke, F.; Wesemann, T.; Wahl, H.; Appold, S.; Krause, M.; Linn, J.; Troost, E.G.C. Reduced diffusion in normal appearing white matter of glioma patients following radio(chemo)therapy. Radiother. Oncol. 2019, 140, 110–115. [Google Scholar] [CrossRef]
- Belka, C.; Budach, W.; Kortmann, R.D.; Bamberg, M. Radiation induced CNS toxicity--molecular and cellular mechanisms. Br. J. Cancer 2001, 85, 1233–1239. [Google Scholar] [CrossRef]
- Wang, S.; Wu, E.X.; Qiu, D.; Leung, L.H.T.; Lau, H.-F.; Khong, P.-L. Longitudinal diffusion tensor magnetic resonance imaging study of radiation-induced white matter damage in a rat model. Cancer Res. 2009, 69, 1190–1198. [Google Scholar] [CrossRef]
- Song, S.-K.; Sun, S.-W.; Ju, W.-K.; Lin, S.-J.; Cross, A.H.; Neufeld, A.H. Diffusion tensor imaging detects and differentiates axon and myelin degeneration in mouse optic nerve after retinal ischemia. Neuroimage 2003, 20, 1714–1722. [Google Scholar] [CrossRef]
- Song, S.-K.; Sun, S.-W.; Ramsbottom, M.J.; Chang, C.; Russell, J.; Cross, A.H. Dysmyelination revealed through MRI as increased radial (but unchanged axial) diffusion of water. Neuroimage 2002, 17, 1429–1436. [Google Scholar] [CrossRef]
- Fung, S.H.; Roccatagliata, L.; Gonzalez, R.G.; Schaefer, P.W. MR diffusion imaging in ischemic stroke. Neuroimaging Clin. N. Am. 2011, 21, 345–377. [Google Scholar] [CrossRef] [PubMed]
- Petr, J.; Platzek, I.; Seidlitz, A.; Mutsaerts, H.J.M.M.; Hofheinz, F.; Schramm, G.; Maus, J.; Beuthien-Baumann, B.; Krause, M.; van den Hoff, J. Early and late effects of radiochemotherapy on cerebral blood flow in glioblastoma patients measured with non-invasive perfusion MRI. Radiother. Oncol. 2016, 118, 24–28. [Google Scholar] [CrossRef] [PubMed]
- Dünger, L. Analyse dosisabhängiger Veränderungen der Magnetresonanz-Diffusion in der weißen Substanz bei Patienten mit hirneigenen Tumoren nach erfolgter Photonen- oder Protonentherapie. M. Sc. Thesis, Technische Universität Dresden, Dresden, Germany, 2019. [Google Scholar]
- Wenz, F.; Rempp, K.; Hess, T.; Debus, J.; Brix, G.; Engenhart, R.; Knopp, M.V.; van Kaick, G.; Wannenmacher, M. Effect of radiation on blood volume in low-grade astrocytomas and normal brain tissue: Quantification with dynamic susceptibility contrast MR imaging. Ajr Am. J. Roentgenol. 1996, 166, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Price, S.J.; Jena, R.; Green, H.A.L.; Kirkby, N.F.; Lynch, A.G.; Coles, C.E.; Pickard, J.D.; Gillard, J.H.; Burnet, N.G. Early radiotherapy dose response and lack of hypersensitivity effect in normal brain tissue: A sequential dynamic susceptibility imaging study of cerebral perfusion. Clin. Oncol. (R Coll. Radiol.) 2007, 19, 577–587. [Google Scholar] [CrossRef]
- Lee, M.C.; Cha, S.; Chang, S.M.; Nelson, S.J. Dynamic susceptibility contrast perfusion imaging of radiation effects in normal-appearing brain tissue: Changes in the first-pass and recirculation phases. J. Magn. Reson. Imaging 2005, 21, 683–693. [Google Scholar] [CrossRef] [PubMed]
- Fuss, M.; Wenz, F.; Scholdei, R.; Essig, M.; Debus, J.; Knopp, M.V.; Wannenmacher, M. Radiation-induced regional cerebral blood volume (rCBV) changes in normal brain and low-grade astrocytomas: Quantification and time and dose-dependent occurrence. Int. J. Radiat. Oncol. Biol. Phys. 2000, 48, 53–58. [Google Scholar] [CrossRef]
- Fahlström, M.; Blomquist, E.; Nyholm, T.; Larsson, E.-M. Perfusion Magnetic Resonance Imaging Changes in Normal Appearing Brain Tissue after Radiotherapy in Glioblastoma Patients may Confound Longitudinal Evaluation of Treatment Response. Radiol. Oncol. 2018, 52, 143–151. [Google Scholar] [CrossRef] [PubMed]
- Fahlström, M.; Fransson, S.; Blomquist, E.; Nyholm, T.; Larsson, E.-M. Dynamic contrast-enhanced magnetic resonance imaging may act as a biomarker for vascular damage in normal appearing brain tissue after radiotherapy in patients with glioblastoma. ACTA Radiol. Open 2018, 7. [Google Scholar] [CrossRef]
- Cao, Y.; Tsien, C.I.; Sundgren, P.C.; Nagesh, V.; Normolle, D.; Buchtel, H.; Junck, L.; Lawrence, T.S. Dynamic contrast-enhanced magnetic resonance imaging as a biomarker for prediction of radiation-induced neurocognitive dysfunction. Clin. Cancer Res. 2009, 15, 1747–1754. [Google Scholar] [CrossRef]
- Jakubovic, R.; Sahgal, A.; Ruschin, M.; Pejovic-Milic, A.; Milwid, R.; Aviv, R.I. Non Tumor Perfusion Changes Following Stereotactic Radiosurgery to Brain Metastases. Technol. Cancer Res. Treat. 2014. [Google Scholar] [CrossRef] [PubMed]
- Ljubimova, N.V.; Levitman, M.K.; Plotnikova, E.D.; Eidus, L.K. Endothelial cell population dynamics in rat brain after local irradiation. Br. J. Radiol. 1991, 64, 934–940. [Google Scholar] [CrossRef] [PubMed]
- Calvo, W.; Hopewell, J.W.; Reinhold, H.S.; Yeung, T.K. Time- and dose-related changes in the white matter of the rat brain after single doses of X rays. Br. J. Radiol. 1988, 61, 1043–1052. [Google Scholar] [CrossRef] [PubMed]
- Brown, W.R.; Thore, C.R.; Moody, D.M.; Robbins, M.E.; Wheeler, K.T. Vascular damage after fractionated whole-brain irradiation in rats. Radiat. Res. 2005, 164, 662–668. [Google Scholar] [CrossRef]
- Lupo, J.M.; Chuang, C.F.; Chang, S.M.; Barani, I.J.; Jimenez, B.; Hess, C.P.; Nelson, S.J. 7-Tesla susceptibility-weighted imaging to assess the effects of radiotherapy on normal-appearing brain in patients with glioma. Int. J. Radiat. Oncol. Biol. Phys. 2012, 82, e493–e500. [Google Scholar] [CrossRef]
- Lupo, J.M.; Molinaro, A.M.; Essock-Burns, E.; Butowski, N.; Chang, S.M.; Cha, S.; Nelson, S.J. The effects of anti-angiogenic therapy on the formation of radiation-induced microbleeds in normal brain tissue of patients with glioma. Neuro Oncol. 2016, 18, 87–95. [Google Scholar] [CrossRef]
- Peters, S.; Pahl, R.; Claviez, A.; Jansen, O. Detection of irreversible changes in susceptibility-weighted images after whole-brain irradiation of children. Neuroradiology 2013, 55, 853–859. [Google Scholar] [CrossRef]
- Moats, R.A.; Watson, L.; Shonk, T.; Tokuyama, S.; Braslau, D.; Eto, R.; Mandigo, J.C.; Ross, B.D. Added value of automated clinical proton MR spectroscopy of the brain. J. Comput. Assist. Tomogr. 1995, 19, 480–491. [Google Scholar] [CrossRef]
- Wang, Z.; Zimmerman, R.A.; Sauter, R. Proton MR spectroscopy of the brain: Clinically useful information obtained in assessing CNS diseases in children. Ajr Am. J. Roentgenol. 1996, 167, 191–199. [Google Scholar] [CrossRef][Green Version]
- Negendank, W.G.; Sauter, R.; Brown, T.R.; Evelhoch, J.L.; Falini, A.; Gotsis, E.D.; Heerschap, A.; Kamada, K.; Lee, B.C.; Mengeot, M.M.; et al. Proton magnetic resonance spectroscopy in patients with glial tumors: A multicenter study. J. Neurosurg. 1996, 84, 449–458. [Google Scholar] [CrossRef]
- Kizu, O.; Naruse, S.; Furuya, S.; Morishita, H.; Ide, M.; Maeda, T.; Ueda, S. Application of proton chemical shift imaging in monitoring of gamma knife radiosurgery on brain tumors. Magn. Reson. Imaging 1998, 16, 197–204. [Google Scholar] [CrossRef]
- Rand, S.D.; Prost, R.; Haughton, V.; Mark, L.; Strainer, J.; Johansen, J.; Kim, T.A.; Chetty, V.K.; Mueller, W.; Meyer, G.; et al. Accuracy of single-voxel proton MR spectroscopy in distinguishing neoplastic from nonneoplastic brain lesions. AJNR Am. J. Neuroradiol. 1997, 18, 1695–1704. [Google Scholar]
- Kaminaga, T.; Shirai, K. Radiation-induced brain metabolic changes in the acute and early delayed phase detected with quantitative proton magnetic resonance spectroscopy. J. Comput. Assist. Tomogr. 2005, 29, 293–297. [Google Scholar] [CrossRef]
- Estève, F.; Rubin, C.; Grand, S.; Kolodié, H.; Le Bas, J.-F. Transient metabolic changes observed with proton MR spectroscopy in normal human brain after radiation therapy. Int. J. Radiat. Oncol. Biol. Phys. 1998, 40, 279–286. [Google Scholar] [CrossRef]
- Chong, V.F.; Rumpel, H.; Fan, Y.F.; Mukherji, S.K. Temporal lobe changes following radiation therapy: Imaging and proton MR spectroscopic findings. Eur. Radiol. 2001, 11, 317–324. [Google Scholar] [CrossRef] [PubMed]
- Usenius, T.; Usenius, J.-P.; Tenhunen, M.; Vainio, P.; Johansson, R.; Soimakallio, S.; Kauppinen, R. Radiation-induced changes in human brain metabolites as studied by 1H nuclear magnetic resonance spectroscopy in vivo. Int. J. Radiat. Oncol. Biol. Phys. 1995, 33, 719–724. [Google Scholar] [CrossRef]
- Movsas, B.; Li, B.S.; Babb, J.S.; Fowble, B.L.; Nicolaou, N.; Gonen, O. Quantifying radiation therapy-induced brain injury with whole-brain proton MR spectroscopy: Initial observations. Radiology 2001, 221, 327–331. [Google Scholar] [CrossRef]
- Szigety, S.K.; Allen, P.S.; Huyser-Wierenga, D.; Urtasun, R.C. The effect of radiation on normal human CNS as detected by NMR spectroscopy. Int. J. Radiat. Oncol. Biol. Phys. 1993, 25, 695–701. [Google Scholar] [CrossRef]
- Lee, M.C.; Pirzkall, A.; McKnight, T.R.; Nelson, S.J. 1H-MRSI of radiation effects in normal-appearing white matter: Dose-dependence and impact on automated spectral classification. J. Magn. Reson. Imaging 2004, 19, 379–388. [Google Scholar] [CrossRef]
- Matulewicz, Ł.; Sokół, M.; Michnik, A.; Wydmański, J. Long-term normal-appearing brain tissue monitoring after irradiation using proton magnetic resonance spectroscopy in vivo: Statistical analysis of a large group of patients. Int. J. Radiat. Oncol. Biol. Phys. 2006, 66, 825–832. [Google Scholar] [CrossRef]
- Waldrop, S.M.; Davis, P.C.; Padgett, C.A.; Shapiro, M.B.; Morris, R. Treatment of brain tumors in children is associated with abnormal MR spectroscopic ratios in brain tissue remote from the tumor site. AJNR Am. J. Neuroradiol. 1998, 19, 963–970. [Google Scholar]
- Blamek, S.; Wydmański, J.; Sokół, M.; Matulewicz, L.; Boguszewicz, L. Magnetic resonance spectroscopic evaluation of brain tissue metabolism after irradiation for pediatric brain tumors in long-term survivors: A report of two cases. Acta Neurochir. Suppl. 2010, 106, 191–194. [Google Scholar] [CrossRef]
- Virta, A.; Patronas, N.; Raman, R.; Dwyer, A.; Barnett, A.; Bonavita, S.; Tedeschi, G.; Lundbom, N. Spectroscopic imaging of radiation-induced effects in the white matter of glioma patients. Magn. Reson. Imaging 2000, 18, 851–857. [Google Scholar] [CrossRef]
- Sundgren, P.C.; Nagesh, V.; Elias, A.; Tsien, C.; Junck, L.; Gomez Hassan, D.M.; Lawrence, T.S.; Chenevert, T.L.; Rogers, L.; McKeever, P.; et al. Metabolic alterations: A biomarker for radiation-induced normal brain injury-an MR spectroscopy study. J. Magn. Reson. Imaging 2009, 29, 291–297. [Google Scholar] [CrossRef] [PubMed]
- Rutkowski, T.; Tarnawski, R.; Sokol, M.; Maciejewski, B. 1h-mr spectroscopy of normal brain tissue before and after postoperative radiotherapy because of primary brain tumors. Int. J. Radiat. Oncol. Biol. Phys. 2003, 56, 1381–1389. [Google Scholar] [CrossRef]
- Simmons, M.L.; Frondoza, C.G.; Coyle, J.T. Immunocytochemical localization of N-acetyl-aspartate with monoclonal antibodies. Neuroscience 1991, 45, 37–45. [Google Scholar] [CrossRef]
- Moffett, J.R.; Namboodiri, M.A.; Cangro, C.B.; Neale, J.H. Immunohistochemical localization of N-acetylaspartate in rat brain. Neuroreport 1991, 2, 131–134. [Google Scholar] [CrossRef] [PubMed]
- Guerrini, L.; Belli, G.; Cellerini, M.; Nencini, P.; Mascalchi, M. Proton MR spectroscopy of cerebellitis. Magn. Reson. Imaging 2002, 20, 619–622. [Google Scholar] [CrossRef]
- Demougeot, C.; Garnier, P.; Mossiat, C.; Bertrand, N.; Giroud, M.; Beley, A.; Marie, C. N-Acetylaspartate, a marker of both cellular dysfunction and neuronal loss: Its relevance to studies of acute brain injury. J. Neurochem. 2001, 77, 408–415. [Google Scholar] [CrossRef] [PubMed]
- Cendes, F.; Andermann, F.; Preul, M.C.; Arnold, D.L. Lateralization of temporal lobe epilepsy based on regional metabolic abnormalities in proton magnetic resonance spectroscopic images. Ann. Neurol. 1994, 35, 211–216. [Google Scholar] [CrossRef] [PubMed]
- Uno, M.; Harada, M.; Nagahiro, S. Quantitative evaluation of cerebral metabolites and cerebral blood flow in patients with carotid stenosis. Neurol. Res. 2001, 23, 573–580. [Google Scholar] [CrossRef] [PubMed]
- Hida, K.; Kwee, I.L.; Nakada, T. In vivo 1H and 31P NMR spectroscopy of the developing rat brain. Magn. Reson. Med. 1992, 23, 31–36. [Google Scholar] [CrossRef]
- Rubin, P.; Whitaker, J.N.; Ceckler, T.L.; Nelson, D.; Gregory, P.K.; Baggs, R.B.; Constine, L.S.; Herman, P.K. Myelin basic protein and magnetic resonance imaging for diagnosing radiation myelopathy. Int. J. Radiat. Oncol. Biol. Phys. 1988, 15, 1371–1381. [Google Scholar] [CrossRef]
- Zhang, X.L.; Jiang, M.; Qiu, S.J.; Zhang, Y. An 1H-MRS study on radioencephalopathy caused by radiotherapy of nasopharyngeal carcinoma. Chin. J. Radiol. 2004, 2004, 570–574. [Google Scholar]
- Song, Q.; Xia, L.M.; Wang, C.Y.; Feng, D.-Y. 1H-MRS study on radiation induced injury of the brain in early acute reaction stage after nasopharyngeal carcinoma radiotherapy. Chin. J. Radiol. 2006, 2006, 590–593. [Google Scholar]
- Shemesh, N.; Sadan, O.; Melamed, E.; Offen, D.; Cohen, Y. Longitudinal MRI and MRSI characterization of the quinolinic acid rat model for excitotoxicity: Peculiar apparent diffusion coefficients and recovery of N-acetyl aspartate levels. Nmr Biomed. 2010, 23, 196–206. [Google Scholar] [CrossRef] [PubMed]
- Wilding, C.S.; Cadwell, K.; Tawn, E.J.; Relton, C.L.; Taylor, G.A.; Chinnery, P.F.; Turnbull, D.M. Mitochondrial DNA mutations in individuals occupationally exposed to ionizing radiation. Radiat. Res. 2006, 165, 202–207. [Google Scholar] [CrossRef]
- Wong, C.S.; van der Kogel, A.J. Mechanisms of radiation injury to the central nervous system: Implications for neuroprotection. Mol. Interv. 2004, 4, 273–284. [Google Scholar] [CrossRef]
- Lange, T.; Dydak, U.; Roberts, T.P.L.; Rowley, H.A.; Bjeljac, M.; Boesiger, P. Pitfalls in lactate measurements at 3T. AJNR Am. J. Neuroradiol. 2006, 27, 895–901. [Google Scholar]
- Charles-Edwards, G.D.; Jan, W.; To, M.; Maxwell, D.; Keevil, S.F.; Robinson, R. Non-invasive detection and quantification of human foetal brain lactate in utero by magnetic resonance spectroscopy. Prenat. Diagn. 2010, 30, 260–266. [Google Scholar] [CrossRef] [PubMed]
- Rubin, P.; Constine, L.; Nelson, D.F. Principles and Practice in Radiation Oncology. In ALERT Adverse Late Effects of Cancer Treatment, 2nd ed.; Perez, C.A., Brady, L.W., Eds.; Springer-Verlag Berlin Heidelberg: Berlin/Heidelberg, Germany, 2014; pp. 138–142. [Google Scholar]
- Englund, E.; Brun, A. White matter changes in dementia of Alzheimer’s type: The difference in vulnerability between cell compartments. Histopathology 1990, 16, 433–439. [Google Scholar] [CrossRef] [PubMed]


| Reference | Number of Patients | Patient Age [yr] | Disease (WHO Grade) | Radiation Dose | Timing of Radiological Follow-Up | Magnetic Field Strength [T] | MRI Sequence(s) | Tissue Assessed | Main Findings/Alterations |
|---|---|---|---|---|---|---|---|---|---|
| Nagtegaal et al., 2021 [44] | 31 | 50 ± 15 | G (II–IV) | 50.4–60 Gy | ≥one follow-up 270–360 d post-RT | 3 | T1w | GM structures | Atrophy in all GM structures except caudate nucleus |
| Raschke et al., 2020 [51] | 91 | 52.3 ± 14.5 | G (I–IV) | 54 Gy or 60 Gy | 3, 6, 9, 12, 15, 18, 21 mo post-RT | 3 | T1w | Cerebellum | Cerebellar atrophy |
| Takeshita et al., 2020 [41] | 20 | 66.2 ± 9.7 | MB | 30 Gy/10 fractions | 0–3 mo, 4–7 mo, 8–11 mo post-RT | 3 | T1w | Hippocampus | Hippocampal atrophy |
| Huynh-Le et al., 2019 [45] | 52 | 19–77 | G (III–IV) | 50.4 Gy to 60 Gy | 1 y post-RT | 3 | T1w | Amygdala | Amygdala atrophy |
| Gommlich et al., 2018 [35] | 26 | 24–74 | G (II, III) | >54 Gy | no uniform time intervals | 1.5 and 3 | T1w | WM, GM | WM atrophy, unchanged GM volume |
| Petr et al., 2018 [36] | 57 | 54.3 ± 14.2 | GBM | 60 Gy | 3 mo and 6 mo post-RT | 3 | T1w | WM, GM | GM and WM atrophy |
| Shi et al., 2018 [40] | 40 | 49.3 ± 11.6 | NPC | 12 Gy (WB) max. 72 Gy (partially) | ≥12 mo post-RT | 3 | T1w | GM | Cortical GM atrophy in left hippocampus, right pulvinar, and right middle temporal gyrus |
| Seibert et al., 2017 [42] | 52 | 19–77 | primary BT | 54–60 Gy | 9–15 mo post-RT | 3 | T1w | Hippocampus | Hippocampal atrophy |
| Seibert et al., 2017 [48] | 54 | 19–77 | BT | 54–60 Gy | 9–15 mo post-RT | 3 | T1w | Cerebral cortex | Cortical atrophy in entorhinal and interior parietal ROIs, not in primary cortex |
| Ailion et al., 2016 [52] | 25 | 9 ± 5 | Cerebellar T | n.a. | 15 ± 5 yr post-RT | 3 | T1w | Cerebellum | Cerebellar atrophy |
| Karunamuni et al., 2016 [49] | 15 | 40–77 | G (HG) | 59.4–60 Gy | 1 y post-RT | 3 | T1w | Cortex | RT dose above 28.6 Gy results in >20% probability of cortical atrophy |
| Karunamuni et al., 2015 [50] | 15 | 40–77 | G (HG) | 59.4–60 Gy | 1 y post-RT | 3 | T1w | Cortex | Cortical atrophy, strongest in temporal and limbic cortex |
| Hong et al., 2015 [39] | 20 | 27–83 | MBM | 30 Gy/10 fractions | 6 mo post-RT | n.a. | n.a. | Hippocampus | Hippocampal avoidance can minimize hippocampal atrophy |
| Prust et al., 2015 [37] | 8 | 35–70 | GBM | 60 Gy | weekly during CRT, monthly until 6 mo pre-RT | 3 | T1w | WB, GM, WM, anterior lateral ventricle, hippocampal volume | WB and GM atrophy, unchanged WM and hippocampal volume, anterior lateral ventricle volume increase |
| Olsson et al., 2012 [43] | 15 | 31–65 | HNC | 1.5–9.3 Gy | 4–10 yr post-RT | 1.5 | T1w, T2w | Hippocampus | No hippocampal atrophy compared to healthy controls |
| Liu et al., 2007 [47] | 9 | 5.4–13.9 | MB | 54 Gy | 1.0–8.2 yr post diagnosis | 1.5 | T1w | Cortex | Cortical thinning |
| Reddick et al., 2005 [32] | 52 | 3.5–20.0 | MB | 35–40 Gy | 0.2–7.9 yr post-RT | 1.5 | T1w, T2w, PD | WM | Less developed normal appearing WM volume compared to healthy controls |
| Nagel et al., 2004 [38] | 25 | 4.8–13.0 | MB | 23.4 Gy (average risk) 36–39.6 Gy (high risk) | 0.56 yr interval post-RT | 1.5 | radiofrequency-spoiled, fast low-angle shot, 3D sequence | Hippocampus | Right and left hippocampal atrophy |
| Reddick et al., 2003 [31] | 40 | 1.7–14.8 | pediatric BT | 35.2 Gy (WB) 53.1–70.2 Gy (local) | 2.6–15.3 yr post-RT | 1.5 | T1w, T2w, PD | WM | Association between WM atrophy and reduced IQ and attentional ability |
| Palmer et al., 2002 [46] | 35 | 3.2–17.2 | MB | 23.4 Gy (average risk) 36–39.6 Gy (high risk) 55.8 Gy (posterior fossa boost) | year 1–2: 3 mo interval, year 3–8: 6 mo interval | 1.5 | T1w | Corpus callosum | Decline of corpus callosum areas |
| Mulhern et al., 2001 [33] | 42 | <21 | MB | 49–54 Gy | ≥1 yr post-RT | 1.5 | T1w, T2w, PD | WM | WM atrophy, young age at CRT associated with worth neurocognitive performance |
| Reddick et al., 2000 [30] | 26 | 3.2–16.2 | MB | 36 Gy (conventional) 23.4 Gy (reduced) | mean 18.7 mo post-RT min. 4 MR examination | 1.5 | T1w, T2w, PD | WM | WM atrophy |
| Mulhern et al., 1999 [34] | 18 | <21 | MB | 23.4–36 Gy CRT 49–54 Gy (posterior fossa boost) | 3.8 ± 2.6 yr post-RT | 1.5 | T1w, T2w, PD | WM | WM atrophy after RT may partially explain changes in IQ and cognitive function |
| Reddick et al., 1998 [29] | 15 | 5.6–21 | MB | 25–55 Gy (WB) 55–65 Gy (focal posterior fossa) | 1.2–10.6 yr post-RT | 1.5 | T1w, T2w, PD | WM, GM | WM atrophy, unchanged GM volume |
| Reference | Number of Patients | Patient Age [yr] | Disease (WHO Grade) | Radiation Dose | Timing of Radiological Follow-Up | Magnetic Field Strength [T] | MRI Sequence(s) | Tissue Assessed | Main Findings/Alterations |
|---|---|---|---|---|---|---|---|---|---|
| Dünger et al., 2019 [96] | 70 | 23–82 | GBM | ≤60 Gy | 3 mo intervals in 3–33 mo post-RT | 3 | DWI | WM | MD ↓ |
| Raschke et al., 2019 [89] | 22 | 47.8 ± 13.9 | G | 54–60 Gy | 3, 6, 9,12,15, 18 mo post-RT | 3 | DTI, 2D FFE (T2*) | WM | MD ↓, RD ↓, AD ↓, T2* ↓ |
| Tringale et al., 2019 | 22 | 20–75 | primary BT | 50.4–60 Gy | 3, 6, 12 mo post-RT | 3 | DWI | Medial temporal lobe regions | MD ↑, FA ↓ |
| Connor et al., 2017 [79] | 49 | 24–84 | G (LG, II–IV) | 40.5–60 Gy | 9–12 mo post-RT | 3 | DTI | WM tracts | MD ↑, RD ↑, FA ↓ |
| Makola et al., 2017 [76] | 14 | 10.1 ± 4.1 | pediatric BT | 52.75 Gy | 3–12 mo post-surgery, follow-up 2 yr later | 1.5 & 3 | DTI | Corpus callosum | RD ↑, FA ↓ |
| Chapman et al., 2016 [87] | 27 | 26–71 | LG/benign T | 54 Gy | pre-RT, during RT, end of RT | 3 | DTI | Parahippocampal cingulum WM | AD ↓, RD ↑ |
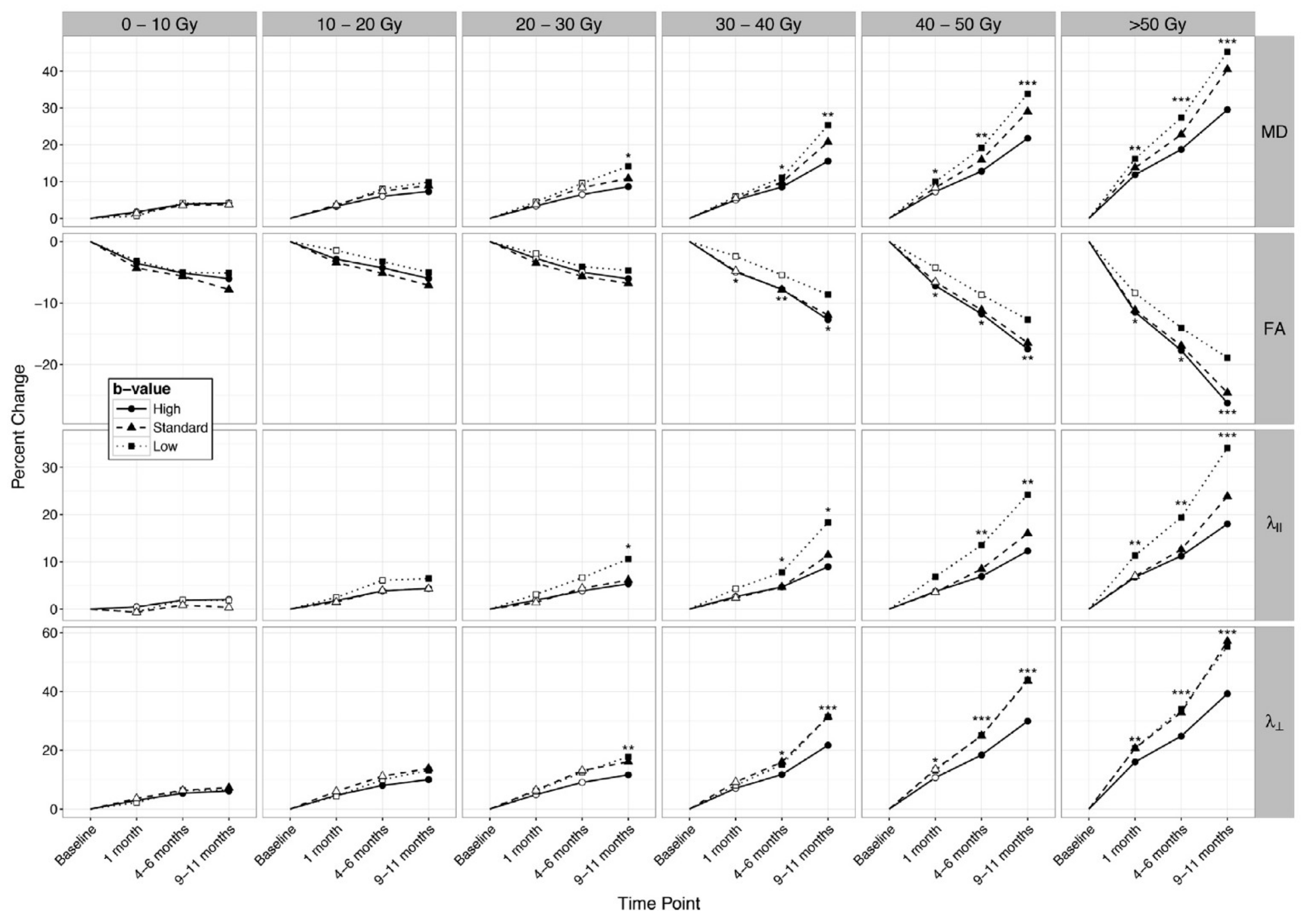
| Connor et al., 2016 [80] | 15 | 40–84 | G (HG) | 40.05–60 Gy | 1 mo, 4–6 mo, 9–11 mo post-RT | 3 | DTI | WM | MD ↑, AD ↑, RD ↑, FA ↓ |
| Duan et al., 2016 [72] | 81 | 19–65 | NPC | 66–74 Gy | <6 mo, 6–12 mo, >12 mo post-RT | 3 | DTI | WM | MD ↑, FA ↓ |
| Zhu et al., 2016 [88] | 33 | 25–72 | LG/benign T | 54 Gy | 6 MRI until 18 mo post-RT | 1.5 & 3 | DTI | WM fiber bundles | AD ↓, RD ↓ |
| Chawla et al., 2015 [68] | 7 | 47–76 | G (HG) | 25–40 Gy | 30.43 ± 9.02 d post-RT | 3 | DTI | Hippocampus, genu corpus callosum | MD ↑, FA ↓ |
| Hope et al., 2015 [82] | 18 | 33–66 | G (HG) | 60 Gy | every 2 w during RT, 2 w, 3 mo, 6 mo post-RT | 3 | DTI | WM | MD ↑, AD ↑, RD ↑ |
| Chapman et al., 2013 [86] | 14 | 40–76 | metastases (primary: LC, M) | 30 Gy/37.5 Gy | end of RT, 1 mo post-RT | 3 | DTI | WM structures | FA ↓, RD ↑ |
| Xiong et al., 2013 [71] | 55 | 19–71 | NPC | 66–75 Gy | 0–3 mo, 3–6 mo, 6–9 mo, 9–12 mo, >12 mo post-RT | 3 | DTI | WM | AD ↓, RD ↑, FA ↓ |
| Chapman et al., 2012 [85] | 10 | 25–71 | LG/benign T | 54 Gy | week 3 & 6 during RT, 10, 30, 78 w post-RT | 1.5 | DTI | Parahippocampal cingulum bundle & temporal lobe WM | AD ↓, RD ↑ |
| Nazem-Zadeh et al., 2012 [78] | 12 | 53.5 | BM | 30 Gy/37.5 Gy | end of RT, 1 mo post-RT | 3 | DTI | Fiber tracts limbic circuit | MD ↑, FA ↓ |
| Wang et al., 2012 [69] | 48 | 16–74 | NPC | 68–75 Gy | <6 mo, 6–12 mo, >12 mo post-RT | 3 | DTI | temporal lobe | AD ↓, FA ↓ |
| Haris et al., 2008 [83] | 5 | 41.6 ± 11.8 | G (II) | 54 Gy | 3, 8, 14 mo pre-RT | 1.5 | DTI | - | MD ↑, FA ↓ |
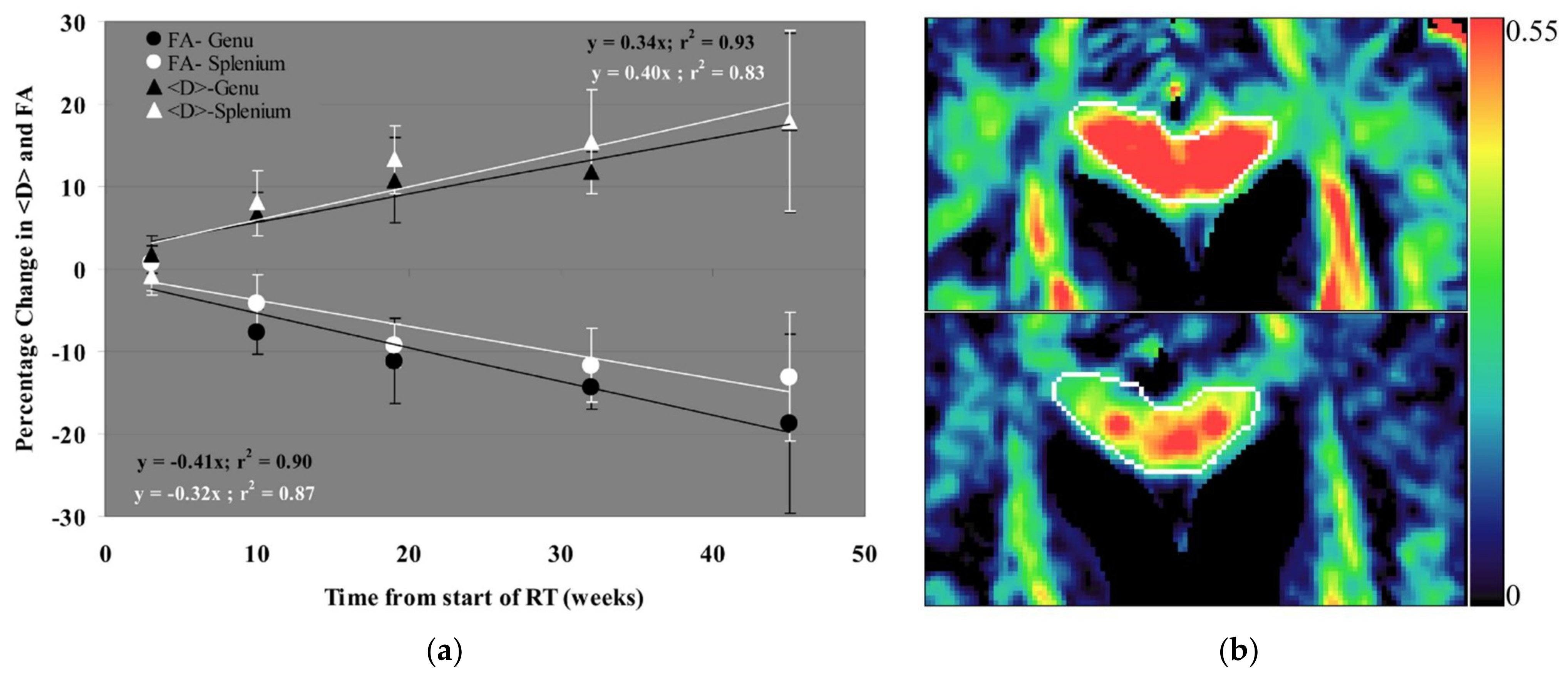
| Nagesh et al., 2008 [77] | 25 | 23–75 | G (HG & LG), benign T | 50–81 Gy | 3, 10, 19, 32, 45 w post-RT | 1.5 | DTI | Genu & splenium corpus callosum | MD ↑, AD ↑, RD ↑, FA ↓ |
| Welzel et al., 2008 [75] | 16 | 45–67 | small cell LC | 30 Gy | end of RT, 6 w post-RT | 1.5 | DTI, T2w | Supra- & infratentorial WM | FA ↓ |
| Qiu et al., 2007 [74] | 22 | 8.1 ± 4.6 | MB | 50–55.8 Gy | 3.9 ± 2.9 yr post-RT | 1.5 | DTI | Frontal & parietal lobes | FA ↓ |
| Mabbott et al., 2006 [70] | 8 | 7.5 ± 3.9 | MB | 55.4 Gy | 2.50 ± 0.72 yr post-RT | 1.5 | DTI | WM | MD ↑, FA ↓ |
| Kitahara et al., 2005 [81] | 8 | 26–70 | BT, L | 30–60 Gy | 0–2 mo, 3–5 mo, 6–9 mo, 10–12 mo post-RT | 1.5 | DTI | WM | MD ↑, FA ↓ |
| Leung et al., 2004 [73] | 16 | 8.8 ± 4.6 | MB | 50–55.8 Gy | 3.1 ± 1.8 yr post-RT | 1.5 | DTI | WM | FA ↓ |
| Khong et al., 2003 [67] | 9 | 3–14 | MB | 50.4–54 Gy | 1–6 yr post-RT | 1.5 | DTI | WM | FA ↓ |
| Reference | Number of Patients | Patient Age [yr] | Disease (WHO Grade) | Radiation Dose | Timing of Radiological Follow-Up | Magnetic Field Strength [T] | MRI Sequence | Tissue Assessed | Main Finding/Alteration |
|---|---|---|---|---|---|---|---|---|---|
| Nilsen et al., 2020 [84] | 40 | 42–84 | MM, metastases from non-small cell LC | 15–25 Gy | 3, 6, 9, 12, 18 mo post-SRS | 3 | DSC | GM, WM | Microvascular CBF ↓, microvascular CBV↓, vessel density ↓ |
| Fahlström et al., 2018 [101] | 10 | 55 ± 88 | GBM (III, IV) | 60 Gy | 3.1, 34.4, 103.3 d post-RT | 1.5 | DSC | GM, WM | WM, GM: rCBV ↓, rCBF ↓ |
| Fahlström et al., 2018 [102] | 12 | 55.9 ± 10.8 | G (III, IV) | 60 Gy | 3.3, 30.6, 101.6, 185.7 d post-RT | 1.5 | DCE | GM, WM | Ktrans ↔, ve ↔ |
| Petr et al., 2018 [36] | 67 | 54.9 ± 14.0 | GBM | 60 Gy | 3, 6 mo post-RT | 3 | ASL | GM, WM | GM: CBF ↓ |
| Lupo et al., 2016 [109] | 17 | 25–66 | G (HG) | n.a. | 8 mo–4.5 yr post-RT | 3 | SWI | Brain | Appearance of microbleeds |
| Petr et al., 2016 [95] | 24 | 54.3 ± 14.1 | GBM | 60 Gy | 3, 6, 9 mo post-RT | 3 | ASL | GM | CBF ↓ |
| Jakubovic et al., 2014 [104] | 19 | ≥18 | BM | 16–24 Gy | 1 w, 1 mo post-SRS | 1.5 | DSC | GM, WM | WM, GM: rCBF↑, rCBV ↑ |
| Peters et al., 2013 [110] | 7 | 13 ± 4 | MB | 29.5 Gy | 4–62 mo post-RT | 3 | SWI | Brain | SWI lesions |
| Lupo et al., 2012 [108] | 25 | 29–71 | G (II–IV) | n.a. | until 20 yr post-RT | 7 | SWI | Brain | Appearance of microbleeds |
| Cao et al., 2009 [103] | 10 | 25–71 | G (LG), MG, CP, benign T | 50.4–59.4 Gy | week 3, 6 during RT, 1, 6 mo post-RT | 1.5 | DCE | High-dose region brain | vp ↑, Ktrans ↑ |
| Price et al., 2007 [98] | 4 | 25–49 | AA (LG) | 54 Gy | after 1st fraction, end of RT, 1, 3 mo post-RT | 3 | DSC | Periventricular WM | rCBV↓, rCBF ↓ |
| Lee et al., 2005 [99] | 22 | 26–73 | G (II, IV) | 60 Gy | first 4 mo post-RT | 1.5 | DSC | WM | Recirculation phase ↓ |
| Fuss et al., 2000 [100] | 25 | 28–59 | Fibrillary AA (II) | 60–66 Gy | 6 w post-RT, in 6 mo intervals | 1.5 | DSC | GM WM | GM/WM: CBV ↓ |
| Wenz et al., 1996 [97] | 13 | 40–78 | Multiple intracerebral metastases, small-cell LC (prophylactic RT) | 30–40 Gy | during and until 79 mo post-RT | 1.5 | DSC | GM WM | GM/WM: CBV ↓ |
| Reference | Number of Patients | Patient Age [yr] | Disease (Grade) | Radiation Dose | Timing of Radiological Follow-Up | Magnetic Field Strength [T] | MRS Sequence | Tissue Assessed | Main Findings/Alterations |
|---|---|---|---|---|---|---|---|---|---|
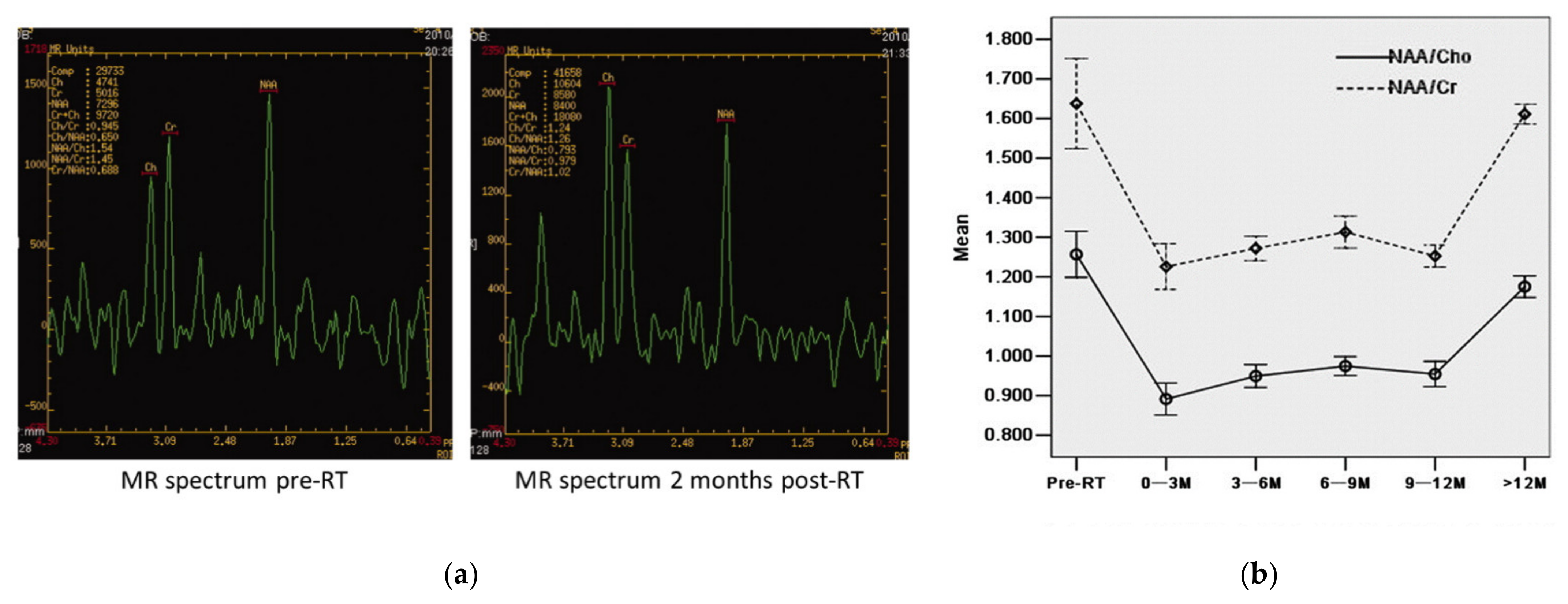
| Chawla et al., 2015 [68] | 7 (4 BM, 3 LC) | 47–76 | BM & LC | BM: WBRT 30–40 Gy LC: PCI 25 Gy/10 fractions | 30.5 ± 9.2 d post-RT | 3 | 3D EPSI | Bilateral GM and WM substructures | NAA/Cr ↓, Cho/Cr ↑ |
| Xiong et al., 2013 [71] | 55 | 19–71 | NPC | 66–75 Gy | 0–3 mo, 3–6 mo, 6–9 mo, 9–12 mo, >12 mo post-RT | 3 | 2D PRESS (LTE) | ROI in WM of bilateral temporal lobes | NAA/Cho ↓, NAA/Cr ↓ |
| Wang et al., 2012 [69] | 48 | 16–74 | NPC | 68–75 Gy | 1 mo—7 yr, divided in <6 mo, 6–12 mo, >12 mo post-RT | 3 | 2D PRESS (LTE) | Three voxel regions in bilateral temporal lobe WM | NAA/Cho ↓, NAA/Cr ↓ |
| Blamek et al., 2010 [125] | 2 | P1: 17 P2: 13 | P1: MB P2: central region T | P1: WBRT: 59.4 Gy (posterior fossa boost) & 30 Gy (craniospinal RT) P2: WBRT: 45 Gy | P1: 8 yr post-RT P2: 20 yr post-RT | n.a. | SV PRESS (STE) | P1: Voxels in cerebellum left and right; P2: Voxels in frontal left, occipital left and right | NAA/Cr ↔, Cho/Cr ↔ |
| Sundgren et al., 2009 [127] | 11 | 25–71 | G (LG), benign T | 50.4–59.4 Gy | 3, 6 w during RT, 1, 6 mo post-RT | 1.5 | 2D PRESS (LTE) | ≥14 voxels in brain (no cerebellum or pons) | NAA/Cho ↑, NAA/Cr ↓, Cho/Cr ↓ |
| Matulewicz et al., 2006 [123] | 100 | 19–74 | G (I–IV) | 60 Gy | one follow-up during 2 yr post-RT | 2 | SV PRESS (STE) | Voxels in WM | NAA/Cho ↓, Cho/Cr ↑ |
| Kaminaga et al., 2005 [116] | 20 | 42–75 | LC, BC and malignant L | 40–50 Gy | 8.5 ± 4.6 d & 3.6 ± 0.5 mo post-RT | 1.5 | SV PRESS (multi-TE) | ROI in occipital lobe cortex containing WM | NAA ↓, Cho ↑ |
| Lee et al., 2004 [122] | 10 | 54.7 ± 15.8 | G (IV) | 60.0 ± 6.9 Gy | end of RT, 2, 4, 6 mo post-RT | 1.5 | 3D PRESS (LTE) | Voxels with >70% WM | NAA/Cho↓, NAA/Cr ↓, NAA ↓, Cho/Cr ↑, Cho ↑ |
| Rutkowski et al., 2003 [128] | 43 | 16–63 | primary glial T | 60 Gy | 9–12 mo post-RT | 2 | SV PRESS (STE) | Voxel in low-, medium- and high-dose brain | NAA/Cr ↓ |
| Chong et al., 2001 [118] | 18 | 38–64 | NPC | 59.4–124.8 Gy | 3–9.6 yr post-RT | 2 | SV PRESS (STE) | Voxels in temporal lobes | NAA ↓, Cho ↔, Cr ↔ |
| Movsas et al., 2001 [120] | 8 | 39–70 | LC | 30.0–37.5 Gy | 20–46 d between baseline and follow-up | 1.5 | WB MRS | Average WB | NAA ↓ |
| Virta et al., 2000 [126] | 9 | 46–61 | G (AA II–III, ODG III, GBM) | 55.0–70.4 Gy | 0.5–10.5 yr post-RT | 1.5 | Multi-slice spin echo (LTE) | ROI in WM | NAA/Cho ↑, NAA/Cr ↔, Cho/Cr ↓ |
| Esteve et al., 1998 [117] | 11 | 44 ± 11 | G (II–IV), metastatic T | 60 Gy (G), 30 Gy (WBRT after metastasectomy) | 1, 4, 8 mo post-RT | 1.5 | SV PRESS (LTE) | VOI in contralateral hemisphere | NAA/Cho ↓, NAA/Cr ↓, NAA ↓, Cho ↑ |
| Waldrop et al., 1998 [124] | 70 | 2–22 | primary brain neoplasms | 40.0–67.2 Gy | n.a. | 1.5 | SV PRESS (LTE) | Voxels of right or left frontal lobe, containing WM and GM | NAA/Cho ↓, NAA/Cr ↓ |
| Usenis et al., 1995 [119] | 8 | 36–67 | BT | 59–62 Gy | 0.5–13 yr post-RT | 1.5 | SV PRESS (LTE) | VOI in parietal, frontal, temporal, or cerebellar brain (high or medium dose) | NAA ↔, Cho ↔, Cr ↔ |
| Szigety et al., 1993 [121] | 13 (31P) 10 (1H) | 24–55 (31P) 40 ± 11 (1H) | G (HG & LG), Pituitary adenoma, ODG | ≤80 Gy | end of RT, 2, 4, 8, 12, 24 mo post-RT | 1.5 | SV STEAM (LTE) (1H) SV (31P) | Brain parenchyma (each ipsilateral high-dose and contralateral low-dose area) | NAA/Cho ↓, Cho/Cr ↑, Cho ↑ |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Witzmann, K.; Raschke, F.; Troost, E.G.C. MR Image Changes of Normal-Appearing Brain Tissue after Radiotherapy. Cancers 2021, 13, 1573. https://doi.org/10.3390/cancers13071573
Witzmann K, Raschke F, Troost EGC. MR Image Changes of Normal-Appearing Brain Tissue after Radiotherapy. Cancers. 2021; 13(7):1573. https://doi.org/10.3390/cancers13071573
Chicago/Turabian StyleWitzmann, Katharina, Felix Raschke, and Esther G. C. Troost. 2021. "MR Image Changes of Normal-Appearing Brain Tissue after Radiotherapy" Cancers 13, no. 7: 1573. https://doi.org/10.3390/cancers13071573
APA StyleWitzmann, K., Raschke, F., & Troost, E. G. C. (2021). MR Image Changes of Normal-Appearing Brain Tissue after Radiotherapy. Cancers, 13(7), 1573. https://doi.org/10.3390/cancers13071573






