Toward an Evidence-Based Definition and Classification of Carbohydrate Food Quality: An Expert Panel Report
Abstract
:1. Introduction
2. Carbohydrate Foods: More Than Just Simple or Complex Carbohydrates
3. Examination of Current Criteria Used to Define Macronutrient Quality
3.1. Nutrient-, Food-, and Health-Based Indicators—Lessons from Protein Quality Scores
3.2. Carbohydrate Food Quality Indicators
4. Review of the Evidence Linking Carbohydrate Food Quality to Nutrient Intake, Diet Quality, and Health Outcomes
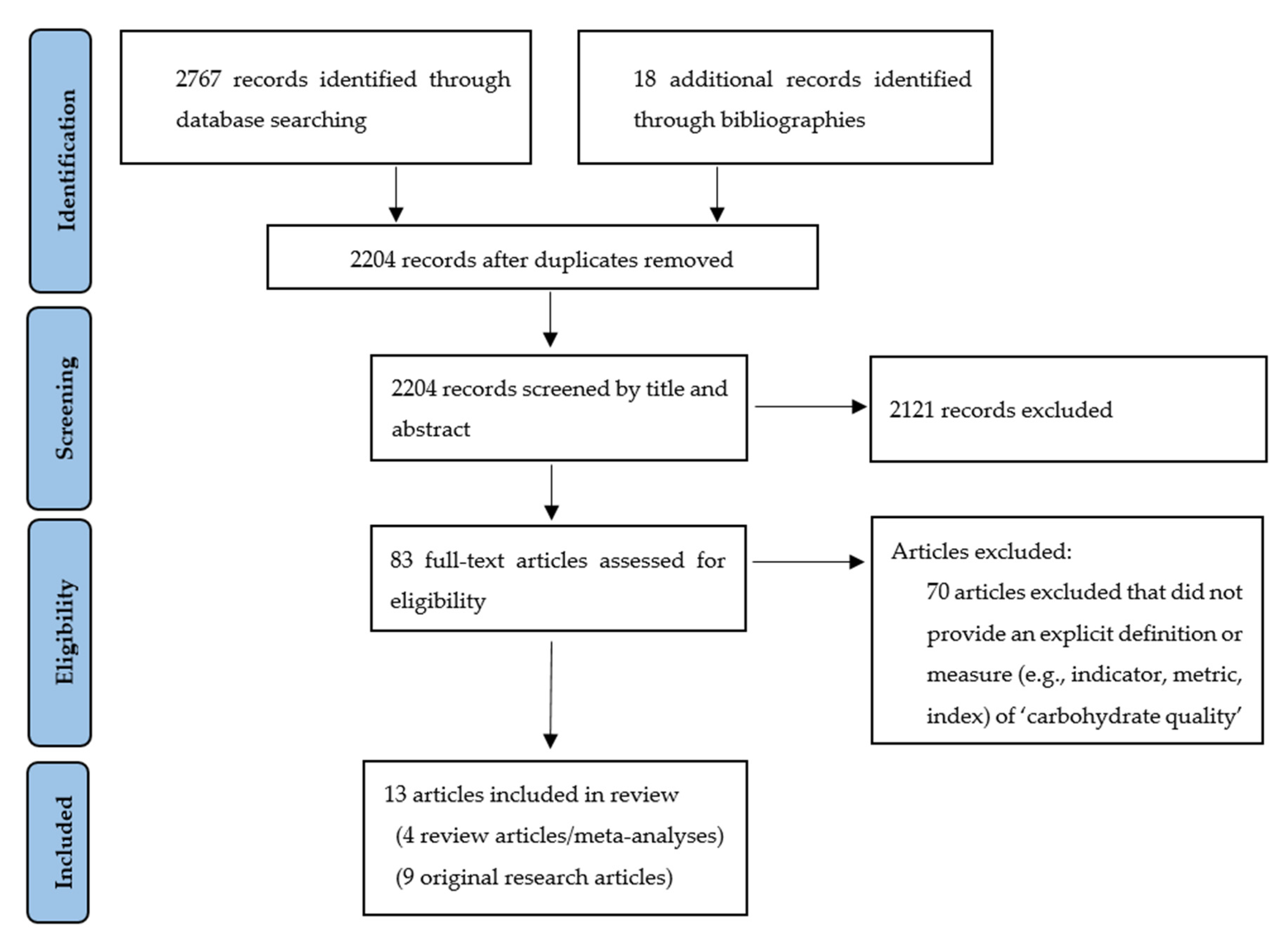
4.1. Methodology—Scoping Review of Carbohydrate Quality Indicators
4.2. Results from Scoping Review
4.3. Glycemic Index/Load Considerations
4.4. Total Fiber and Carbohydrate:Fiber Ratios
5. Next Steps for Developing Quantitative Metrics to Assess Carbohydrate Food Quality
Nutrient Profiling—A Method to Assess the Nutrient Density of Foods
6. Main Principles for Carbohydrate Food Quality Assessment and Metric Development
- (1)
- Overall, the QCC-SAC recognized seven principles that could help guide the development of a standardized metric for characterizing CF quality: Assessment of CF quality should be based on nutrient composition data that are accurate, reliable and in the public domain. The USDA FoodData Central is a valuable resource that fits these criteria.
- (2)
- CFs come from many sources, most of which are plant-based. A nutrient profiling model that is both food group and category specific is ideal.
- (3)
- CF quality can be driven by multiple factors from enrichment and fortification, to added sugar content and sodium: potassium ratios. These factors should be further investigated for inclusion in a CF quality metric.
- (4)
- CF quality assessment should be based on nutrient- and food-based indicators until more reliable data are available.
- (5)
- The CF quality metric should utilize a holistic approach, incorporating new data on topics such as affordability, bioactive compound content, and environmental impacts as they become available. Much more data and evidence will be required before most of these are additions are possible.
- (6)
- The CF quality metric should be aligned with, and be able to operate within, already validated dietary guidance tools such as food-based dietary guidelines (FBDGs), FDA-approved nutrition and health claims, and on-package food labels. The FDA does not view GI/GL as a characteristic of the food alone, nor does it have a database dedicated to GI or GL values.
- (7)
- The CF quality metric should be easily expandable and able to accommodate additional inputs as new evidence becomes available.
- (8)
- The CF quality metric should be culturally inclusive, translatable, and easy-to-use. The main goal of the metric is to help with the implementation of dietary guidelines in promoting better food choice for improved diet quality and health.
7. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Food and Agriculture Organization of the United Nations. FAOSTAT Database Collections. 2021. Available online: www.fao.org/faostat/en/ (accessed on 26 January 2021).
- Liu, Y.S.; Wu, Q.J.; Xia, Y.; Zhang, J.Y.; Jiang, Y.T.; Chang, Q.; Zhao, Y.H. Carbohydrate intake and risk of metabolic syndrome: A dose-response meta-analysis of observational studies. Nutr. Metab. Cardiovasc. Dis. 2019, 29, 1288–1298. [Google Scholar] [CrossRef]
- Mazidi, M.; Katsiki, N.; Mikhailidis, D.P.; Sattar, N.; Banach, M. Lower carbohydrate diets and all-cause and cause-specific mortality: A population-based cohort study and pooling of prospective studies. Eur. Heart J. 2019, 40, 2870–2879. [Google Scholar] [CrossRef] [Green Version]
- Wali, J.A.; Raubenheimer, D.; Senior, A.M.; Le Couteur, D.G.; Simpson, S.J. Cardio-metabolic consequences of dietary carbohydrates: Reconciling contradictions using nutritional geometry. Cardiovasc. Res. 2021, 117, 386–401. [Google Scholar] [CrossRef]
- Herforth, A.; Arimond, M.; Alvarez-Sanchez, C.; Coates, J.; Christianson, K.; Muehlhoff, E. A Global Review of Food-Based Dietary Guidelines. Adv. Nutr. 2019, 10, 590–605. [Google Scholar] [CrossRef] [Green Version]
- U.S. Department of Agriculture; U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 9th ed.; U.S. Department of Agriculture: Washington, DC, USA; U.S. Department of Health and Human Services: Washington, DC, USA, 2020.
- Seidelmann, S.B.; Claggett, B.; Cheng, S.; Henglin, M.; Shah, A.; Steffen, L.M.; Folsom, A.R.; Rimm, E.B.; Willett, W.C.; Solomon, S.D. Dietary carbohydrate intake and mortality: A prospective cohort study and meta-analysis. Lancet Public Health 2018, 3, e419–e428. [Google Scholar] [CrossRef] [Green Version]
- Kanter, M. High-Quality Carbohydrates: A Concept in Search of a Definition. Nutr. Today 2019, 54, 289–295. [Google Scholar] [CrossRef]
- FDA. Interactive Nutrition Facts Label-Total Carbohydrate; FDA: Silver Spring, MD, USA, 2020.
- FDA. Authorized Health Claims That Meet the Significant Scientific Agreement (SSA) Standard; FDA: Silver Spring, MD, USA, 2018.
- Kollannoor-Samuel, G.; Shebl, F.M.; Hawley, N.L.; Perez-Escamilla, R. Nutrition facts panel use is associated with higher diet quality and lower glycated hemoglobin concentrations in US adults with undiagnosed prediabetes. Am. J. Clin. Nutr. 2016, 104, 1639–1646. [Google Scholar] [CrossRef]
- Auestad, N.; Hurley, J.S.; Fulgoni, V.L., 3rd; Schweitzer, C.M. Contribution of Food Groups to Energy and Nutrient Intakes in Five Developed Countries. Nutrients 2015, 7, 4593–4618. [Google Scholar] [CrossRef]
- Kopf, J.C.; Suhr, M.J.; Clarke, J.; Eyun, S.I.; Riethoven, J.M.; Ramer-Tait, A.E.; Rose, D.J. Role of whole grains versus fruits and vegetables in reducing subclinical inflammation and promoting gastrointestinal health in individuals affected by overweight and obesity: A randomized controlled trial. Nutr. J. 2018, 17, 72. [Google Scholar] [CrossRef] [Green Version]
- Katz, D.L.; Doughty, K.N.; Geagan, K.; Jenkins, D.A.; Gardner, C.D. Perspective: The Public Health Case for Modernizing the Definition of Protein Quality. Adv. Nutr. 2019, 10, 755–764. [Google Scholar] [CrossRef]
- Fernandez-Lazaro, C.I.; Zazpe, I.; Santiago, S.; Toledo, E.; Barberia-Latasa, M.; Martinez-Gonzalez, M.A. Association of carbohydrate quality and all-cause mortality in the SUN Project: A prospective cohort study. Clin. Nutr. 2020. [Google Scholar] [CrossRef] [PubMed]
- Sanchez-Villegas, A.; Zazpe, I.; Santiago, S.; Perez-Cornago, A.; Martinez-Gonzalez, M.A.; Lahortiga-Ramos, F. Added sugars and sugar-sweetened beverage consumption, dietary carbohydrate index and depression risk in the Seguimiento Universidad de Navarra (SUN) Project. Br. J. Nutr. 2018, 119, 211–221. [Google Scholar] [CrossRef] [Green Version]
- Santiago, S.; Zazpe, I.; Bes-Rastrollo, M.; Sanchez-Tainta, A.; Sayon-Orea, C.; de la Fuente-Arrillaga, C.; Benito, S.; Martinez, J.A.; Martinez-Gonzalez, M.A. Carbohydrate quality, weight change and incident obesity in a Mediterranean cohort: The SUN Project. Eur. J. Clin. Nutr. 2015, 69, 297–302. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zazpe, I.; Sanchez-Tainta, A.; Santiago, S.; de la Fuente-Arrillaga, C.; Bes-Rastrollo, M.; Martinez, J.A.; Martinez-Gonzalez, M.A.; Investigators, S.U.N.P. Association between dietary carbohydrate intake quality and micronutrient intake adequacy in a Mediterranean cohort: The SUN (Seguimiento Universidad de Navarra) Project. Br. J. Nutr. 2014, 111, 2000–2009. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zazpe, I.; Santiago, S.; Gea, A.; Ruiz-Canela, M.; Carlos, S.; Bes-Rastrollo, M.; Martinez-Gonzalez, M.A. Association between a dietary carbohydrate index and cardiovascular disease in the SUN (Seguimiento Universidad de Navarra) Project. Nutr. Metab. Cardiovasc. Dis. 2016, 26, 1048–1056. [Google Scholar] [CrossRef] [PubMed]
- Suara, S.B.; Siassi, F.; Saaka, M.; Rahimi Foroshani, A.; Sotoudeh, G. Association between Carbohydrate Quality Index and general and abdominal obesity in women: A cross-sectional study from Ghana. BMJ Open 2019, 9, e033038. [Google Scholar] [CrossRef] [Green Version]
- Kim, D.Y.; Kim, S.H.; Lim, H. Association between dietary carbohydrate quality and the prevalence of obesity and hypertension. J. Hum. Nutr. Diet. 2018, 31, 587–596. [Google Scholar] [CrossRef]
- Augustin, L.S.; Kendall, C.W.; Jenkins, D.J.; Willett, W.C.; Astrup, A.; Barclay, A.W.; Bjorck, I.; Brand-Miller, J.C.; Brighenti, F.; Buyken, A.E.; et al. Glycemic index, glycemic load and glycemic response: An International Scientific Consensus Summit from the International Carbohydrate Quality Consortium (ICQC). Nutr. Metab. Cardiovasc. Dis. 2015, 25, 795–815. [Google Scholar] [CrossRef] [Green Version]
- Buyken, A.E.; Goletzke, J.; Joslowski, G.; Felbick, A.; Cheng, G.; Herder, C.; Brand-Miller, J.C. Association between carbohydrate quality and inflammatory markers: Systematic review of observational and interventional studies. Am. J. Clin. Nutr. 2014, 99, 813–833. [Google Scholar] [CrossRef] [Green Version]
- Hardy, D.S.; Garvin, J.T.; Xu, H. Carbohydrate quality, glycemic index, glycemic load and cardiometabolic risks in the US, Europe and Asia: A dose-response meta-analysis. Nutr. Metab. Cardiovasc. Dis. 2020, 30, 853–871. [Google Scholar] [CrossRef]
- Reynolds, A.; Mann, J.; Cummings, J.; Winter, N.; Mete, E.; Te Morenga, L. Carbohydrate quality and human health: A series of systematic reviews and meta-analyses. Lancet 2019, 393, 434–445. [Google Scholar] [CrossRef] [Green Version]
- Sawicki, C.M.; Lichtenstein, A.H.; Rogers, G.T.; Jacques, P.F.; Ma, J.; Saltzman, E.; McKeown, N.M. Comparison of Indices of Carbohydrate Quality and Food Sources of Dietary Fiber on Longitudinal Changes in Waist Circumference in the Framingham Offspring Cohort. Nutrients 2021, 13, 997. [Google Scholar] [CrossRef] [PubMed]
- AlEssa, H.B.; Cohen, R.; Malik, V.S.; Adebamowo, S.N.; Rimm, E.B.; Manson, J.E.; Willett, W.C.; Hu, F.B. Carbohydrate quality and quantity and risk of coronary heart disease among US women and men. Am. J. Clin. Nutr. 2018, 107, 257–267. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Rehm, C.D.; Shi, P.; McKeown, N.M.; Mozaffarian, D.; Micha, R. A comparison of different practical indices for assessing carbohydrate quality among carbohydrate-rich processed products in the US. PLoS ONE 2020, 15, e0231572. [Google Scholar] [CrossRef]
- Lee, J.S.; Sreenivasulu, N.; Hamilton, R.S.; Kohli, A. Brown Rice, a Diet Rich in Health Promoting Properties. J. Nutr. Sci. Vitaminol. 2019, 65, S26–S28. [Google Scholar] [CrossRef] [Green Version]
- Visvanathan, R.; Jayathilake, C.; Chaminda Jayawardana, B.; Liyanage, R. Health-beneficial properties of potato and compounds of interest. J. Sci. Food Agric. 2016, 96, 4850–4860. [Google Scholar] [CrossRef] [PubMed]
- Augustin, L.S.A.; Aas, A.M.; Astrup, A.; Atkinson, F.S.; Baer-Sinnott, S.; Barclay, A.W.; Brand-Miller, J.C.; Brighenti, F.; Bullo, M.; Buyken, A.E.; et al. Dietary Fibre Consensus from the International Carbohydrate Quality Consortium (ICQC). Nutrients 2020, 12, 2553. [Google Scholar] [CrossRef]
- Zeevi, D.; Korem, T.; Zmora, N.; Israeli, D.; Rothschild, D.; Weinberger, A.; Ben-Yacov, O.; Lador, D.; Avnit-Sagi, T.; Lotan-Pompan, M.; et al. Personalized Nutrition by Prediction of Glycemic Responses. Cell 2015, 163, 1079–1094. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Wolever, T.M.; Vorster, H.H.; Bjorck, I.; Brand-Miller, J.; Brighenti, F.; Mann, J.I.; Ramdath, D.D.; Granfeldt, Y.; Holt, S.; Perry, T.L.; et al. Determination of the glycaemic index of foods: Interlaboratory study. Eur. J. Clin. Nutr. 2003, 57, 475–482. [Google Scholar] [CrossRef] [Green Version]
- Atkinson, F.S.; Brand-Miller, J.C.; Foster-Powell, K.; Buyken, A.E.; Goletzke, J. International tables of glycemic index and glycemic load values 2021: A systematic review. Am. J. Clin. Nutr. 2021. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Matthan, N.R.; Ausman, L.M.; Lichtenstein, A.H. Effect of macronutrients and fiber on postprandial glycemic responses and meal glycemic index and glycemic load value determinations. Am. J. Clin. Nutr. 2017, 105, 842–853. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Zafar, M.I.; Mills, K.E.; Zheng, J.; Regmi, A.; Hu, S.Q.; Gou, L.; Chen, L.L. Low-glycemic index diets as an intervention for diabetes: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2019, 110, 891–902. [Google Scholar] [CrossRef] [PubMed]
- Livesey, G.; Taylor, R.; Livesey, H.F.; Buyken, A.E.; Jenkins, D.J.A.; Augustin, L.S.A.; Sievenpiper, J.L.; Barclay, A.W.; Liu, S.; Wolever, T.M.S.; et al. Dietary Glycemic Index and Load and the Risk of Type 2 Diabetes: A Systematic Review and Updated Meta-Analyses of Prospective Cohort Studies. Nutrients 2019, 11, 1280. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Vega-Lopez, S.; Venn, B.J.; Slavin, J.L. Relevance of the Glycemic Index and Glycemic Load for Body Weight, Diabetes, and Cardiovascular Disease. Nutrients 2018, 10, 1361. [Google Scholar] [CrossRef] [Green Version]
- Poon, T.; Labonte, M.E.; Mulligan, C.; Ahmed, M.; Dickinson, K.M.; L’Abbe, M.R. Comparison of nutrient profiling models for assessing the nutritional quality of foods: A validation study. Br. J. Nutr. 2018, 120, 567–582. [Google Scholar] [CrossRef] [PubMed]
- Drewnowski, A.; Fulgoni, V.L., 3rd. New Nutrient Rich Food Nutrient Density Models That Include Nutrients and MyPlate Food Groups. Front. Nutr. 2020, 7, 107. [Google Scholar] [CrossRef]
| Protein | Fat | Carbohydrates | |
|---|---|---|---|
| Common Descriptive Indicators for Determining Macronutrient or Food Quality | Plant/Animal-Sourced Complete/Incomplete Essential Amino Acids | Plant/Animal-Sourced | Food Groups (e.g., Grains, Vegetables, Legumes, Fruits, Discretionary Foods) |
| High/Low in Branched-Chain Amino Acids | Saturated/MUFA + PUFA | Whole Grain/Refined Grain/ Enriched Grain | |
| The Protein Digestibility-Corrected Amino Acid Score (PDCAAS) | Solid/Liquid at Room Temp | Simple/Complex | |
| Lean/Fatty Protein Foods | Short-, Medium-, Long-Chain Fatty Acids | High/Low in Fiber | |
| Trans/Cis Bonds | Processed/Unprocessed | ||
| Omega-3 or Omega 3:6 Ratio | Solid/Liquid Form | ||
| Intrinsic/Added Sugars | |||
| Intrinsic/Added Fiber | |||
| Common Physiological Measures and Health Outcomes for Determining Macronutrient or Food Quality | Protein Synthesis Rates | Postprandial Lipemia | Glycemic Index/Load |
| Muscle Mass/Function | Fasting Blood Lipids | Fasting Glucose/HbA1c | |
| Growth Rate in Children | Insulin Secretion/Resistance | Insulin Secretion/Resistance | |
| Protein/Calorie Malnutrition | Inflammatory Markers | Hydrogen/Methane in Breath | |
| Stunting/Wasting | Body Weight | Body Weight | |
| Type 2 Diabetes | Type 2 Diabetes | ||
| Cardiovascular Disease | Cardiovascular Disease | ||
| Dental Caries | |||
| Gut Microbiota |
| Food Chemistry and Composition | Food and Meal Consumption Context | Physiological Responses | Diet Quality and Health Outcomes | Sustainability Impacts |
|---|---|---|---|---|
| Macronutrient content (types and ratios) | Interactions with other foods and ingredients in a meal or dietary pattern | Glucoregulation (glycemic index/load, insulin response, etc.) | Nutrient adequacy | Public health effects |
| Food matrix effects | Consumer characteristics (age, health status, other demographic considerations) | Blood lipids (postprandial lipemia, fasting triglycerides, cholesterol, etc.) | Alignment with Healthy Eating Index (HEI) | Environmental impacts |
| Carbohydrate characteristics (fiber, starch, sugar—types, amounts, and ratios) | Lifestyle factors (level of physical activity, stress, sleep, etc.) | Inflammatory and immune markers | Food group variety or diversity | Socio-Cultural impacts |
| Micronutrients (especially of public health concern) | Consumption patterns (frequency of intake, speed of ingestion, etc.) | Multi-omics (genomics, proteomics, metabolomics) | Chronic disease risk or incidence | Economic impacts |
| Bioactive food components (phytonutrients, prebiotics, probiotics) | Food form, processing, and preparation | Gut microbiome | Mortality statistics |
| Nutrient-Based Indicators | Food-Based Indicators | Health-Based Indicators | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Total Fiber | Cereal Fiber | 10:1 Carb:Fiber Ratio | Carb: Cereal Fiber Ratio | Starch: Cereal Fiber Ratio | Whole Grain | Whole Grain: Total Carb Ratio | Solid Carb: Total Carb Ratio | Glycemic Index/ Response | |
| Buyken 2014 [23] | X | X | X | ||||||
| Zazpe 2014 [18] | X | X | X | X | |||||
| Augustin 2015 [22] | X | ||||||||
| Zazpe 2016 [19] | X | X | X | X | |||||
| AlEssa 2018 [27] | X | X | X | ||||||
| Reynolds 2019 [25] | X | X | X | ||||||
| Hardy 2020 [24] | X | X | X | ||||||
| Liu 2020 [28] | X | ||||||||
| Sawicki 2021 [26] | X | X | X | X | X | X | X | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Comerford, K.B.; Papanikolaou, Y.; Jones, J.M.; Rodriguez, J.; Slavin, J.; Angadi, S.; Drewnowski, A. Toward an Evidence-Based Definition and Classification of Carbohydrate Food Quality: An Expert Panel Report. Nutrients 2021, 13, 2667. https://doi.org/10.3390/nu13082667
Comerford KB, Papanikolaou Y, Jones JM, Rodriguez J, Slavin J, Angadi S, Drewnowski A. Toward an Evidence-Based Definition and Classification of Carbohydrate Food Quality: An Expert Panel Report. Nutrients. 2021; 13(8):2667. https://doi.org/10.3390/nu13082667
Chicago/Turabian StyleComerford, Kevin B., Yanni Papanikolaou, Julie Miller Jones, Judith Rodriguez, Joanne Slavin, Siddhartha Angadi, and Adam Drewnowski. 2021. "Toward an Evidence-Based Definition and Classification of Carbohydrate Food Quality: An Expert Panel Report" Nutrients 13, no. 8: 2667. https://doi.org/10.3390/nu13082667
APA StyleComerford, K. B., Papanikolaou, Y., Jones, J. M., Rodriguez, J., Slavin, J., Angadi, S., & Drewnowski, A. (2021). Toward an Evidence-Based Definition and Classification of Carbohydrate Food Quality: An Expert Panel Report. Nutrients, 13(8), 2667. https://doi.org/10.3390/nu13082667






