The Ambiguous Role of Caffeine in Migraine Headache: From Trigger to Treatment
Abstract
1. Introduction
1.1. Caffeine
1.2. Caffeine’s Influence on Health
1.3. Caffeine and Cerebral Blood Flow
1.4. Caffeine′s Effects on Pain and Non-Migraine Headache
1.5. Caffeine and Migraine
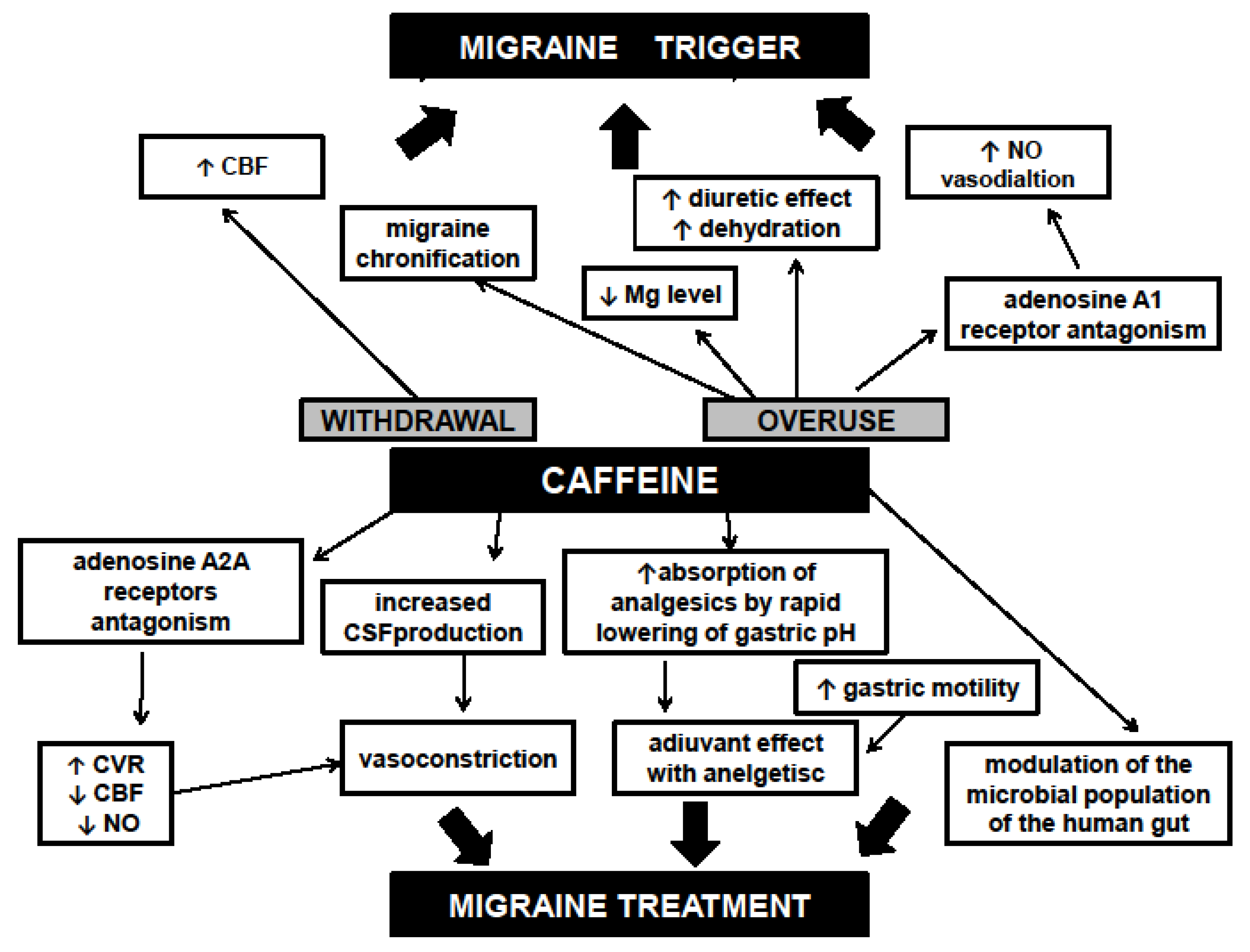
1.5.1. Caffeine as Migraine Treatment: Potential Mechanism of Action 1
1.5.2. Caffeine as a Migraine Trigger: Potential Mechanism of Action
2. Materials and Methods
3. Results and Discussion
3.1. Prevalence of Caffeine as a Migraine Trigger Factor
3.2. Caffeine as Acute Migraine Treatment
3.3. Recommendations for Migraine Patients Regarding Caffeine Use
- Individuals with migraines must be aware of the amount of caffeine they consume daily. They should carefully identify all caffeine products consumed daily, including coffee, tea, soft drinks, energy drinks, and medications.
- Migraine sufferers who are regular caffeine consumers and wish to continue drinking caffeinated beverages, should keep their daily caffeine intake as consistent as possible. They should also choose coffee as a preferable caffeine source because of the additional health benefit. Those who wish to cease caffeine consumption should gradually taper their intake over several weeks.
- Daily intake of caffeine should be limited to less than 200 mg/day (about two servings of caffeinated beverage).
- Patients should continue to consume caffeine regularly every day, preferably at a consistent time, and should not discontinue it during the weekend. They should avoid sleeping longer on weekends to prevent caffeine withdrawal headache.
- Caffeine-containing analgesics are safe and effective in treating migraine attacks, but their consumption should be limited to two days during the week to avoid medication overuse headache.
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Steiner, T.J.; Stovner, L.J.; Birbeck, G.L. Migraine: The seventh disabler. Headache 2013, 53, 227–229. [Google Scholar] [CrossRef] [PubMed]
- Collaborators, G.H. Global, regional, and national burden of migraine and tension-type headache, 1990–2016: A systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol. 2018, 17, 954–976. [Google Scholar]
- Headache Classification Committee of the International Headache Society (IHS). The International Classification of Headache Disorders 3rd edition. Cephalalgia 2018, 38, 1–211. [Google Scholar] [CrossRef] [PubMed]
- Alstadhaug, K.B.; Andreou, A.P. Caffeine and Primary (Migraine) Headaches-Friend or Foe? Front. Neurol. 2019, 10, 1275. [Google Scholar] [CrossRef] [PubMed]
- Hindiyeh, N.A.; Zhang, N.; Farrar, M.; Banerjee, P.; Lombard, L.; Aurora, S.K. The Role of Diet and Nutrition in Migraine Triggers and Treatment: A Systematic Literature Review. Headache 2020. [Google Scholar] [CrossRef]
- Lipton, R.B.; Diener, H.C.; Robbins, M.S.; Garas, S.Y.; Patel, K. Caffeine in the management of patients with headache. J. Headache Pain 2017, 18, 107. [Google Scholar] [CrossRef]
- Spencer, B. Caffeine withdrawal: A model for migraine? Headache 2002, 42, 561–562. [Google Scholar] [CrossRef]
- Ward, N.; Whitney, C.; Avery, D.; Dunner, D. The analgesic effects of caffeine in headache. Pain 1991, 44, 151–155. [Google Scholar] [CrossRef]
- Ogawa, N.; Ueki, H. Clinical importance of caffeine dependence and abuse. Psychiatry Clin. Neurosci. 2007, 61, 263–268. [Google Scholar] [CrossRef]
- Heckman, M.A.; Weil, J.; Gonzalez de Mejia, E. Caffeine (1, 3, 7-trimethylxanthine) in foods: A comprehensive review on consumption, functionality, safety, and regulatory matters. J. Food Sci. 2010, 75, R77–R87. [Google Scholar] [CrossRef]
- Fried, N.T.; Elliott, M.B.; Oshinsky, M.L. The Role of Adenosine Signaling in Headache: A Review. Brain Sci. 2017, 7, 30. [Google Scholar] [CrossRef]
- Baratloo, A.; Rouhipour, A.; Forouzanfar, M.M.; Safari, S.; Amiri, M.; Negida, A. The Role of Caffeine in Pain Management: A Brief Literature Review. Anesth Pain Med. 2016, 6, e33193. [Google Scholar] [CrossRef] [PubMed]
- Haskell-Ramsay, C.F.; Jackson, P.A.; Forster, J.S.; Dodd, F.L.; Bowerbank, S.L.; Kennedy, D.O. The Acute Effects of Caffeinated Black Coffee on Cognition and Mood in Healthy Young and Older Adults. Nutrients 2018, 10, 1386. [Google Scholar] [CrossRef]
- Nawrot, P.; Jordan, S.; Eastwood, J.; Rotstein, J.; Hugenholtz, A.; Feeley, M. Effects of caffeine on human health. Food Addit. Contam. 2003, 20, 1–30. [Google Scholar] [CrossRef]
- Miners, J.O.; Birkett, D.J. The use of caffeine as a metabolic probe for human drug metabolizing enzymes. Gen. Pharmacol. 1996, 27, 245–249. [Google Scholar] [CrossRef]
- Grosso, G.; Godos, J.; Galvano, F.; Giovannucci, E.L. Coffee, Caffeine, and Health Outcomes: An Umbrella Review. Annu. Rev. Nutr. 2017, 37, 131–156. [Google Scholar] [CrossRef] [PubMed]
- Nehlig, A. Effects of coffee/caffeine on brain health and disease: What should I tell my patients? Pract. Neurol. 2016, 16, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Cornelis, M.C. The Impact of Caffeine and Coffee on Human Health. Nutrients 2019, 11, 416. [Google Scholar] [CrossRef]
- Bruce, C.; Yates, D.H.; Thomas, P.S. Caffeine decreases exhaled nitric oxide. Thorax 2002, 57, 361–363. [Google Scholar] [CrossRef]
- Umemura, T.; Ueda, K.; Nishioka, K.; Hidaka, T.; Takemoto, H.; Nakamura, S.; Jitsuiki, D.; Soga, J.; Goto, C.; Chayama, K.; et al. Effects of acute administration of caffeine on vascular function. Am. J. Cardiol. 2006, 98, 1538–1541. [Google Scholar] [CrossRef]
- Higashi, Y. Coffee and Endothelial Function: A Coffee Paradox? Nutrients 2019, 11, 2104. [Google Scholar] [CrossRef] [PubMed]
- Joris, P.J.; Mensink, R.P.; Adam, T.C.; Liu, T.T. Cerebral Blood Flow Measurements in Adults: A Review on the Effects of Dietary Factors and Exercise. Nutrients 2018, 10, 530. [Google Scholar] [CrossRef] [PubMed]
- Gererd, D. Coffee and Health; John Libbey Eurotext: Esher, UK, 1994. [Google Scholar]
- Vidyasagar, R.; Greyling, A.; Draijer, R.; Corfield, D.R.; Parkes, L.M. The effect of black tea and caffeine on regional cerebral blood flow measured with arterial spin labeling. J. Cereb. Blood Flow Metab. 2013, 33, 963–968. [Google Scholar] [CrossRef] [PubMed]
- Haanes, K.A.; Labastida-Ramírez, A.; Chan, K.Y.; de Vries, R.; Shook, B.; Jackson, P.; Zhang, J.; Flores, C.M.; Danser, A.H.J.; Villalón, C.M.; et al. Characterization of the trigeminovascular actions of several adenosine A. J. Headache Pain 2018, 19, 41. [Google Scholar] [CrossRef]
- Yang, H.S.; Liang, Z.; Yao, J.F.; Shen, X.; Frederick, B.D.; Tong, Y. Vascular effects of caffeine found in BOLD fMRI. J. Neurosci. Res. 2019, 97, 456–466. [Google Scholar] [CrossRef] [PubMed]
- Xu, F.; Liu, P.; Pekar, J.J.; Lu, H. Does acute caffeine ingestion alter brain metabolism in young adults? Neuroimage 2015, 110, 39–47. [Google Scholar] [CrossRef]
- Blaha, M.; Benes, V.; Douville, C.M.; Newell, D.W. The effect of caffeine on dilated cerebral circulation and on diagnostic CO2 reactivity testing. J. Clin. Neurosci. 2007, 14, 464–467. [Google Scholar] [CrossRef]
- Lunt, M.J.; Ragab, S.; Birch, A.A.; Schley, D.; Jenkinson, D.F. Comparison of caffeine-induced changes in cerebral blood flow and middle cerebral artery blood velocity shows that caffeine reduces middle cerebral artery diameter. Physiol. Meas. 2004, 25, 467–474. [Google Scholar] [CrossRef]
- Addicott, M.A.; Yang, L.L.; Peiffer, A.M.; Burnett, L.R.; Burdette, J.H.; Chen, M.Y.; Hayasaka, S.; Kraft, R.A.; Maldjian, J.A.; Laurienti, P.J. The effect of daily caffeine use on cerebral blood flow: How much caffeine can we tolerate? Hum. Brain Mapp. 2009, 30, 3102–3114. [Google Scholar] [CrossRef]
- Couturier, E.G.; Laman, D.M.; van Duijn, M.A.; van Duijn, H. Influence of caffeine and caffeine withdrawal on headache and cerebral blood flow velocities. Cephalalgia 1997, 17, 188–190. [Google Scholar] [CrossRef]
- Sigmon, S.C.; Herning, R.I.; Better, W.; Cadet, J.L.; Griffiths, R.R. Caffeine withdrawal, acute effects, tolerance, and absence of net beneficial effects of chronic administration: Cerebral blood flow velocity, quantitative EEG, and subjective effects. Psychopharmacology (Berl.) 2009, 204, 573–585. [Google Scholar] [CrossRef] [PubMed]
- Marchand, S.; Li, J.; Charest, J. Effects of caffeine on analgesia from transcutaneous electrical nerve stimulation. N. Engl. J. Med. 1995, 333, 325–326. [Google Scholar] [CrossRef] [PubMed]
- Derry, C.J.; Derry, S.; Moore, R.A. Caffeine as an analgesic adjuvant for acute pain in adults. Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef]
- Laska, E.M.; Sunshine, A.; Mueller, F.; Elvers, W.B.; Siegel, C.; Rubin, A. Caffeine as an analgesic adjuvant. JAMA 1984, 251, 1711–1718. [Google Scholar] [CrossRef]
- Zaeem, Z.; Zhou, L.; Dilli, E. Headaches: A Review of the Role of Dietary Factors. Curr. Neurol. Neurosci. Rep. 2016, 16, 101. [Google Scholar] [CrossRef] [PubMed]
- Liang, J.F.; Wang, S.J. Hypnic headache: A review of clinical features, therapeutic options and outcomes. Cephalalgia 2014, 34, 795–805. [Google Scholar] [CrossRef]
- Basurto Ona, X.; Osorio, D.; Bonfill Cosp, X. Drug therapy for treating post-dural puncture headache. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef] [PubMed]
- Han, M.E.; Kim, H.J.; Lee, Y.S.; Kim, D.H.; Choi, J.T.; Pan, C.S.; Yoon, S.; Baek, S.Y.; Kim, B.S.; Kim, J.B.; et al. Regulation of cerebrospinal fluid production by caffeine consumption. BMC Neurosci. 2009, 10, 110. [Google Scholar] [CrossRef]
- Kalladka, D.; Siddiqui, A.; Tyagi, A.; Newman, E. Reversible cerebral vasoconstriction syndrome secondary to caffeine withdrawal. Scott. Med. J. 2018, 63, 22–24. [Google Scholar] [CrossRef] [PubMed]
- Chattha, N.; Webb, T.; Hargroves, D.; Balogun, I.; Bertoni, M. Reversible cerebral vasoconstriction syndrome after sudden caffeine withdrawal. Br. J. Hosp. Med. (Lond.) 2019, 80, 730–731. [Google Scholar] [CrossRef]
- Manzoni, G.C. Cluster headache and lifestyle: Remarks on a population of 374 male patients. Cephalalgia 1999, 19, 88–94. [Google Scholar] [CrossRef] [PubMed]
- Scher, A.I.; Stewart, W.F.; Lipton, R.B. Caffeine as a risk factor for chronic daily headache: A population-based study. Neurology 2004, 63, 2022–2027. [Google Scholar] [CrossRef]
- Kluonaitis, K.; Petrauskiene, E.; Ryliskiene, K. Clinical characteristics and overuse patterns of medication overuse headache: Retrospective case-series study. Clin. Neurol. Neurosurg. 2017, 163, 124–127. [Google Scholar] [CrossRef] [PubMed]
- Dong, Z.; Chen, X.; Steiner, T.J.; Hou, L.; Di, H.; He, M.; Dai, W.; Pan, M.; Zhang, M.; Liu, R.; et al. Medication-overuse headache in China: Clinical profile, and an evaluation of the ICHD-3 beta diagnostic criteria. Cephalalgia 2015, 35, 644–651. [Google Scholar] [CrossRef] [PubMed]
- Diamond, S.; Balm, T.K.; Freitag, F.G. Ibuprofen plus caffeine in the treatment of tension-type headache. Clin. Pharmacol. Ther. 2000, 68, 312–319. [Google Scholar] [CrossRef]
- Jacobs, B.; Dussor, G. Neurovascular contributions to migraine: Moving beyond vasodilation. Neuroscience 2016, 338, 130–144. [Google Scholar] [CrossRef]
- Guieu, R.; Devaux, C.; Henry, H.; Bechis, G.; Pouget, J.; Mallet, D.; Sampieri, F.; Juin, M.; Gola, R.; Rochat, H. Adenosine and migraine. Can. J. Neurol. Sci. 1998, 25, 55–58. [Google Scholar] [CrossRef]
- Aurora, S.K.; Kori, S.H.; Barrodale, P.; McDonald, S.A.; Haseley, D. Gastric stasis in migraine: More than just a paroxysmal abnormality during a migraine attack. Headache 2006, 46, 57–63. [Google Scholar] [CrossRef]
- Silberstein, S. Gastrointestinal manifestations of migraine: Meeting the treatment challenges. Headache 2013, 53, 1–3. [Google Scholar] [CrossRef]
- Messlinger, K.; Lennerz, J.K.; Eberhardt, M.; Fischer, M.J. CGRP and NO in the trigeminal system: Mechanisms and role in headache generation. Headache 2012, 52, 1411–1427. [Google Scholar] [CrossRef]
- González, S.; Salazar, N.; Ruiz-Saavedra, S.; Gómez-Martín, M.; de Los Reyes-Gavilán, C.G.; Gueimonde, M. Long-Term Coffee Consumption is Associated with Fecal Microbial Composition in Humans. Nutrients 2020, 12, 1287. [Google Scholar] [CrossRef]
- Arzani, M.; Jahromi, S.R.; Ghorbani, Z.; Vahabizad, F.; Martelletti, P.; Ghaemi, A.; Sacco, S.; Togha, M.; On behalf of the School of Advanced Studies of the European Headache Federation (EHF-SAS). Gut-brain Axis and migraine headache: A comprehensive review. J. Headache Pain 2020, 21, 15. [Google Scholar] [CrossRef] [PubMed]
- Martami, F.; Togha, M.; Seifishahpar, M.; Ghorbani, Z.; Ansari, H.; Karimi, T.; Jahromi, S.R. The effects of a multispecies probiotic supplement on inflammatory markers and episodic and chronic migraine characteristics: A randomized double-blind controlled trial. Cephalalgia 2019, 39, 841–853. [Google Scholar] [CrossRef]
- Lipton, R.B.; Pavlovic, J.M.; Haut, S.R.; Grosberg, B.M.; Buse, D.C. Methodological issues in studying trigger factors and premonitory features of migraine. Headache 2014, 54, 1661–1669. [Google Scholar] [CrossRef] [PubMed]
- Peroutka, S.J. What turns on a migraine? A systematic review of migraine precipitating factors. Curr. Pain Headache Rep. 2014, 18, 454. [Google Scholar] [CrossRef] [PubMed]
- Mollaoğlu, M. Trigger factors in migraine patients. J. Health Psychol. 2013, 18, 984–994. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann, J.; Recober, A. Migraine and triggers: Post hoc ergo propter hoc? Curr. Pain Headache Rep. 2013, 17, 370. [Google Scholar] [CrossRef]
- Wöber, C.; Wöber-Bingöl, C. Triggers of migraine and tension-type headache. Handb. Clin. Neurol. 2010, 97, 161–172. [Google Scholar]
- Rockett, F.C.; Castro, K.; de Oliveira, V.R.; da Silveira, P.A.; Chaves, M.L.F.; Perry, I.D.S. Perceived migraine triggers: Do dietary factors play a role? Nutr. Hosp. 2012, 27, 483–489. [Google Scholar]
- Aguggia, M.; Saracco, M.G. Pathophysiology of migraine chronification. Neurol. Sci. 2010, 31, S15–S17. [Google Scholar] [CrossRef]
- Bigal, M.E.; Lipton, R.B. Modifiable risk factors for migraine progression. Headache 2006, 46, 1334–1343. [Google Scholar] [CrossRef]
- Guendler, V.Z.; Mercante, J.P.; Ribeiro, R.T.; Zukerman, E.; Peres, M.F. Factors associated with acute medication overuse in chronic migraine patients. Einstein (Sao Paulo) 2012, 10, 312–317. [Google Scholar] [CrossRef]
- Bergman, E.A.; Massey, L.K.; Wise, K.J.; Sherrard, D.J. Effects of dietary caffeine on renal handling of minerals in adult women. Life Sci. 1990, 47, 557–564. [Google Scholar] [CrossRef]
- Kirkland, A.E.; Sarlo, G.L.; Holton, K.F. The Role of Magnesium in Neurological Disorders. Nutrients 2018, 10, 730. [Google Scholar] [CrossRef] [PubMed]
- Wöber, C.; Brannath, W.; Schmidt, K.; Kapitan, M.; Rudel, E.; Wessely, P.; Wöber-Bingöl, C.; Group, P.S. Prospective analysis of factors related to migraine attacks: The PAMINA study. Cephalalgia 2007, 27, 304–314. [Google Scholar] [CrossRef] [PubMed]
- Seal, A.D.; Bardis, C.N.; Gavrieli, A.; Grigorakis, P.; Adams, J.D.; Arnaoutis, G.; Yannakoulia, M.; Kavouras, S.A. Coffee with High but Not Low Caffeine Content Augments Fluid and Electrolyte Excretion at Rest. Front. Nutr. 2017, 4, 40. [Google Scholar] [CrossRef]
- Couturier, E.G.; Hering, R.; Steiner, T.J. Weekend attacks in migraine patients: Caused by caffeine withdrawal? Cephalalgia 1992, 12, 99–100. [Google Scholar] [CrossRef]
- Schulte, L.H.; Jürgens, T.P.; May, A. Photo-, osmo- and phonophobia in the premonitory phase of migraine: Mistaking symptoms for triggers? J. Headache Pain 2015, 16, 14. [Google Scholar] [CrossRef]
- Yalcin, N.; Chen, S.P.; Yu, E.S.; Liu, T.T.; Yen, J.C.; Atalay, Y.B.; Qin, T.; Celik, F.; van den Maagdenberg, A.M.; Moskowitz, M.A.; et al. Caffeine does not affect susceptibility to cortical spreading depolarization in mice. J. Cereb. Blood Flow Metab. 2019, 39, 740–750. [Google Scholar] [CrossRef]
- Goadsby, P.J.; Silberstein, S.D. Migraine triggers: Harnessing the messages of clinical practice. Neurology 2013, 80, 424–425. [Google Scholar] [CrossRef]
- Martin, P.R. Managing headache triggers: Think ‘coping’ not ‘avoidance’. Cephalalgia 2010, 30, 634–637. [Google Scholar] [CrossRef] [PubMed]
- Mikulec, A.A.; Faraji, F.; Kinsella, L.J. Evaluation of the efficacy of caffeine cessation, nortriptyline, and topiramate therapy in vestibular migraine and complex dizziness of unknown etiology. Am. J. Otolaryngol. 2012, 33, 121–127. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.J.; Choi, H.A.; Choi, H.; Chung, C.S. Caffeine discontinuation improves acute migraine treatment: A prospective clinic-based study. J. Headache Pain 2016, 17, 71. [Google Scholar] [CrossRef] [PubMed]
- Mostofsky, E.; Mittleman, M.A.; Buettner, C.; Li, W.; Bertisch, S.M. Prospective Cohort Study of Caffeinated Beverage Intake as a Potential Trigger of Headaches among Migraineurs. Am. J. Med. 2019, 132, 984–991. [Google Scholar] [CrossRef] [PubMed]
- Beh, S.C.; Masrour, S.; Smith, S.V.; Friedman, D.I. The Spectrum of Vestibular Migraine: Clinical Features, Triggers, and Examination Findings. Headache 2019, 59, 727–740. [Google Scholar] [CrossRef] [PubMed]
- Tai, M.S.; Yap, J.F.; Goh, C.B. Dietary trigger factors of migraine and tension-type headache in a South East Asian country. J. Pain Res. 2018, 11, 1255–1261. [Google Scholar] [CrossRef]
- Taheri, S. Effect of exclusion of frequently consumed dietary triggers in a cohort of children with chronic primary headache. Nutr. Health 2017, 23, 47–50. [Google Scholar] [CrossRef]
- Park, J.W.; Chu, M.K.; Kim, J.M.; Park, S.G.; Cho, S.J. Analysis of Trigger Factors in Episodic Migraineurs Using a Smartphone Headache Diary Applications. PLoS ONE 2016, 11, e0149577. [Google Scholar] [CrossRef]
- Peris, F.; Donoghue, S.; Torres, F.; Mian, A.; Wöber, C. Towards improved migraine management: Determining potential trigger factors in individual patients. Cephalalgia 2017, 37, 452–463. [Google Scholar] [CrossRef]
- Rist, P.M.; Buring, J.E.; Kurth, T. Dietary patterns according to headache and migraine status: A cross-sectional study. Cephalalgia 2015, 35, 767–775. [Google Scholar] [CrossRef]
- Fraga, M.D.; Pinho, R.S.; Andreoni, S.; Vitalle, M.S.; Fisberg, M.; Peres, M.F.; Vilanova, L.C.; Masruha, M.R. Trigger factors mainly from the environmental type are reported by adolescents with migraine. Arq. Neuropsiquiatr. 2013, 71, 290–293. [Google Scholar] [CrossRef] [PubMed]
- Neut, D.; Fily, A.; Cuvellier, J.C.; Vallée, L. The prevalence of triggers in paediatric migraine: A questionnaire study in 102 children and adolescents. J. Headache Pain 2012, 13, 61–65. [Google Scholar] [CrossRef] [PubMed]
- Schürks, M.; Buring, J.E.; Kurth, T. Migraine features, associated symptoms and triggers: A principal component analysis in the Women’s Health Study. Cephalalgia 2011, 31, 861–869. [Google Scholar] [CrossRef]
- Yadav, R.K.; Kalita, J.; Misra, U.K. A study of triggers of migraine in India. Pain Med. 2010, 11, 44–47. [Google Scholar] [CrossRef] [PubMed]
- Hauge, A.W.; Kirchmann, M.; Olesen, J. Trigger factors in migraine with aura. Cephalalgia 2010, 30, 346–353. [Google Scholar] [CrossRef]
- Andress-Rothrock, D.; King, W.; Rothrock, J. An analysis of migraine triggers in a clinic-based population. Headache 2010, 50, 1366–1370. [Google Scholar] [CrossRef]
- Chakravarty, A.; Mukherjee, A.; Roy, D. Trigger factors in childhood migraine: A clinic-based study from eastern India. J. Headache Pain 2009, 10, 375–380. [Google Scholar] [CrossRef]
- Fukui, P.T.; Gonçalves, T.R.; Strabelli, C.G.; Lucchino, N.M.; Matos, F.C.; Santos, J.P.; Zukerman, E.; Zukerman-Guendler, V.; Mercante, J.P.; Masruha, M.R.; et al. Trigger factors in migraine patients. Arq. Neuropsiquiatr. 2008, 66, 494–499. [Google Scholar] [CrossRef]
- Wöber, C.; Holzhammer, J.; Zeitlhofer, J.; Wessely, P.; Wöber-Bingöl, C. Trigger factors of migraine and tension-type headache: Experience and knowledge of the patients. J. Headache Pain 2006, 7, 188–195. [Google Scholar] [CrossRef]
- Takeshima, T.; Ishizaki, K.; Fukuhara, Y.; Ijiri, T.; Kusumi, M.; Wakutani, Y.; Mori, M.; Kawashima, M.; Kowa, H.; Adachi, Y.; et al. Population-based door-to-door survey of migraine in Japan: The Daisen study. Headache 2004, 44, 8–19. [Google Scholar] [CrossRef]
- Bánk, J.; Márton, S. Hungarian migraine epidemiology. Headache 2000, 40, 164–169. [Google Scholar] [CrossRef] [PubMed]
- Van den Bergh, V.; Amery, W.K.; Waelkens, J. Trigger factors in migraine: A study conducted by the Belgian Migraine Society. Headache 1987, 27, 191–196. [Google Scholar] [CrossRef] [PubMed]
- Hagen, K.; Thoresen, K.; Stovner, L.J.; Zwart, J.A. High dietary caffeine consumption is associated with a modest increase in headache prevalence: Results from the Head-HUNT Study. J. Headache Pain 2009, 10, 153–159. [Google Scholar] [CrossRef] [PubMed]
- Baratloo, A.; Mirbaha, S.; Delavar Kasmaei, H.; Payandemehr, P.; Elmaraezy, A.; Negida, A. Intravenous caffeine citrate vs. magnesium sulfate for reducing pain in patients with acute migraine headache; a prospective quasi-experimental study. Korean J. Pain 2017, 30, 176–182. [Google Scholar] [CrossRef] [PubMed]
- Goldstein, J.; Hagen, M.; Gold, M. Results of a multicenter, double-blind, randomized, parallel-group, placebo-controlled, single-dose study comparing the fixed combination of acetaminophen, acetylsalicylic acid, and caffeine with ibuprofen for acute treatment of patients with severe migraine. Cephalalgia 2014, 34, 1070–1078. [Google Scholar]
- Pini, L.A.; Guerzoni, S.; Cainazzo, M.; Ciccarese, M.; Prudenzano, M.P.; Livrea, P. Comparison of tolerability and efficacy of a combination of paracetamol + caffeine and sumatriptan in the treatment of migraine attack: A randomized, double-blind, double-dummy, cross-over study. J. Headache Pain 2012, 13, 669–675. [Google Scholar] [CrossRef]
- Láinez, M.J.; Galván, J.; Heras, J.; Vila, C. Crossover, double-blind clinical trial comparing almotriptan and ergotamine plus caffeine for acute migraine therapy. Eur. J. Neurol. 2007, 14, 269–275. [Google Scholar] [CrossRef]
- Goldstein, J.; Silberstein, S.D.; Saper, J.R.; Ryan, R.E.; Lipton, R.B. Acetaminophen, aspirin, and caffeine in combination versus ibuprofen for acute migraine: Results from a multicenter, double-blind, randomized, parallel-group, single-dose, placebo-controlled study. Headache 2006, 46, 444–453. [Google Scholar] [CrossRef]
- Goldstein, J.; Silberstein, S.D.; Saper, J.R.; Elkind, A.H.; Smith, T.R.; Gallagher, R.M.; Battikha, J.P.; Hoffman, H.; Baggish, J. Acetaminophen, aspirin, and caffeine versus sumatriptan succinate in the early treatment of migraine: Results from the ASSET trial. Headache 2005, 45, 973–982. [Google Scholar] [CrossRef]
- Peroutka, S.J.; Lyon, J.A.; Swarbrick, J.; Lipton, R.B.; Kolodner, K.; Goldstein, J. Efficacy of diclofenac sodium softgel 100 mg with or without caffeine 100 mg in migraine without aura: A randomized, double-blind, crossover study. Headache 2004, 44, 136–141. [Google Scholar] [CrossRef] [PubMed]
| Author (Year) | Study Design | Study Design (Method of Identifying Trigger Factors) | Study Group: Type of Headache (Number of Participants) | Study Population Age (Years) | Coffee/Caffeine Reported as a Trigger Factor (%) | Additional Information |
|---|---|---|---|---|---|---|
| Beh 2019 [76] | Retrospective cross-sectional | Retrospective chart review | Vestibular migraine (n = 131) | No data | 11.5 | |
| Tai 2018 [77] | Prospective cross-sectional | Comprehensive dietary checklist | Migraine (n = 319) | Migraine 37.1 ± 14.3 | Migraine 25.4 | Caffeine significantly associated with migraines compared to TTH |
| TTH 15.1 | ||||||
| TTH (n = 365) | TTH 46.5 ± 18.1 | |||||
| MWA (n = 188) | ||||||
| MA (n = 128) | ||||||
| CM (n = 91) | ||||||
| Taheri 2017 [78] | Prospective observational case series | Food diary | Migraine (n = 65) | Range 10–15 | 28 | 87% of patients achieved complete resolution of headaches by exclusion of 1–3 triggers |
| TTH (n = 50) | Mean 10.5 | |||||
| Park 2016 [79] | Prospective cross-sectional | Smartphone headache diary application | Episodic migraine (n = 62) | Mean 37.7 ± 8.6 | 2.4 | |
| MWA (n = 60) | ||||||
| MA (n = 2) | ||||||
| Peris 2016 [80] | Prospective cross-sectional | Detailed 90-day paper diary database from PAMINA migraine study | Migraine (n = 326) | No data | 7.7 | |
| Rist 2014 [81] | Cross-sectional study among participants in the Women’s Health Study | Semi-quantitative food frequency questionnaire | Non-migraine headache (n = 5573) | Mean 53.6 | Not applicable | Patients with non-migraine headache more likely to have low intake of coffee; women who experienced migraine were less likely to have low intake of coffee compared to those with non-migraine headache |
| Migraine (n = 7042) | ||||||
| MWA (n = 2972) | ||||||
| MA (n = 1974) | ||||||
| Mollaoglu 2013 [57] | Prospective cross-sectional | Interview TF checklist | Migraine (n = 146) | Mean 36.32 | 6.3 | |
| MWA (n = 73) | ||||||
| MA (n = 53) | ||||||
| Fraga 2013 [82] | Prospective cross-sectional | Predetermined list of trigger factors | Migraine (n = 100) | Range 10–20 | Total 14 | |
| EM female 17.85 | ||||||
| EM (n = 50) | EM male 0 | |||||
| CM (n = 50) | CM female 19.51 | |||||
| CM male 12.5 | ||||||
| Camboim Rockett 2012 [60] | Cross-sectional | Predetermined list of 22 dietary factors | Migraine (n = 123) | Mean 43.2 ± 13.9 | Migraine after caffeine consumption | |
| MWA (n = 84) | ||||||
| MA (n = 39) | Occasional 10–15 | |||||
| Consistent <10 | ||||||
| Caffeine withdrawal | ||||||
| Occasional 10–15 | ||||||
| Consistent 20–30 | ||||||
| Neut 2012 [83] | Retrospective | Predetermined list of TFs | Migraine (n = 102) | Mean 12 | Cola drinks 8.8 | |
| Range 7–16 | ||||||
| MWA (n = 71) | ||||||
| MA (n = 22) | ||||||
| Schürks 2011 [84] | Cross-sectional | Mailed migraine-specific questionnaire | Women′s Health Study (n = 1675) | No data | Coffee 8.1 | |
| Cola drinks 5 | ||||||
| Yadav 2010 [85] | Prospective cross-sectional | Questionnaire | Migraine without aura (n = 182) | Mean 30.7 | None | No subjects reported coffee or caffeine withdrawal as a trigger |
| Range 14–58 | ||||||
| Hauge 2010 [86] | Cross-sectional | Questionnaire listing 16 trigger factors | Migraine with aura (n = 347) | Mean 51 | Caffeine withdrawal 20–30 | |
| Andress-Rothrock 2010 [87] | Prospective cross-sectional | Headache trigger checklist | Migraine (n = 200) | Mean 41.1 | 8 | |
| Range 16–75 | ||||||
| EM (n = 56) | ||||||
| CM (n = 144) | ||||||
| Chakravarty 2009 [88] | Prospective and retrospective cross-sectional | Migraine trigger checklist | Migraine (n = 200) | Range 7–15 | Caffeinated drinks | |
| MWA (n = 197) | Retrospective study 0 | |||||
| MA (n = 3) | ||||||
| Prospective study 0 | ||||||
| Fukui 2008 [89] | Prospective cross-sectional | Predetermined list of TGGs | Migraine (n = 200) | Mean 37.7 | 14.5 (12.96% females, 21.05% males) | |
| Wöber 2006 [90] | Cross-sectional | Two predetermined TF checklists (patients′ personal experience and theoretical knowledge) | Migraine (n = 71) | Range 18–65 | Theoretical knowledge 25 | Difference between theoretical knowledge and personal experience of coffee was statistically significant |
| Personal experience 10 | ||||||
| TTH (n = 49) | Migraine 36.8 ± 11.4 | |||||
| TTH 39.5 ± 12.7 | ||||||
| Takeschima 2004 [91] | Door-to-door survey | Structured questionnaires | Headache (n = 1628) | No data | None | Odds ratio of coffee and tea consumption significantly higher in migraineurs compared to TTH sufferers |
| migraine (n = 342) | ||||||
| MWA (n = 301) | ||||||
| MA (n = 41) | ||||||
| Bank 2000 [92] | Population-based epidemiological survey | Self-administered headache questionnaire | Migraine (n = 62) | Mean | None | |
| Women 41 | ||||||
| Men 43 | ||||||
| Van Den Bergh 1987 [93] | Retrospective | Unstructured recall/free self-report | Migraine (n = 217) | Mean 40 | 6.4 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nowaczewska, M.; Wiciński, M.; Kaźmierczak, W. The Ambiguous Role of Caffeine in Migraine Headache: From Trigger to Treatment. Nutrients 2020, 12, 2259. https://doi.org/10.3390/nu12082259
Nowaczewska M, Wiciński M, Kaźmierczak W. The Ambiguous Role of Caffeine in Migraine Headache: From Trigger to Treatment. Nutrients. 2020; 12(8):2259. https://doi.org/10.3390/nu12082259
Chicago/Turabian StyleNowaczewska, Magdalena, Michał Wiciński, and Wojciech Kaźmierczak. 2020. "The Ambiguous Role of Caffeine in Migraine Headache: From Trigger to Treatment" Nutrients 12, no. 8: 2259. https://doi.org/10.3390/nu12082259
APA StyleNowaczewska, M., Wiciński, M., & Kaźmierczak, W. (2020). The Ambiguous Role of Caffeine in Migraine Headache: From Trigger to Treatment. Nutrients, 12(8), 2259. https://doi.org/10.3390/nu12082259






