Rural–Urban Differences in Dietary Behavior and Obesity: Results of the Riskesdas Study in 10–18-Year-Old Indonesian Children and Adolescents
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population and Design
2.2. Ethical Considerations
2.3. Socio-Demographic and Dietary Behavior Questionnaire
2.4. Anthropometric Data
2.5. Physical Activity Questionnaire
2.6. Statistical Analysis
3. Results
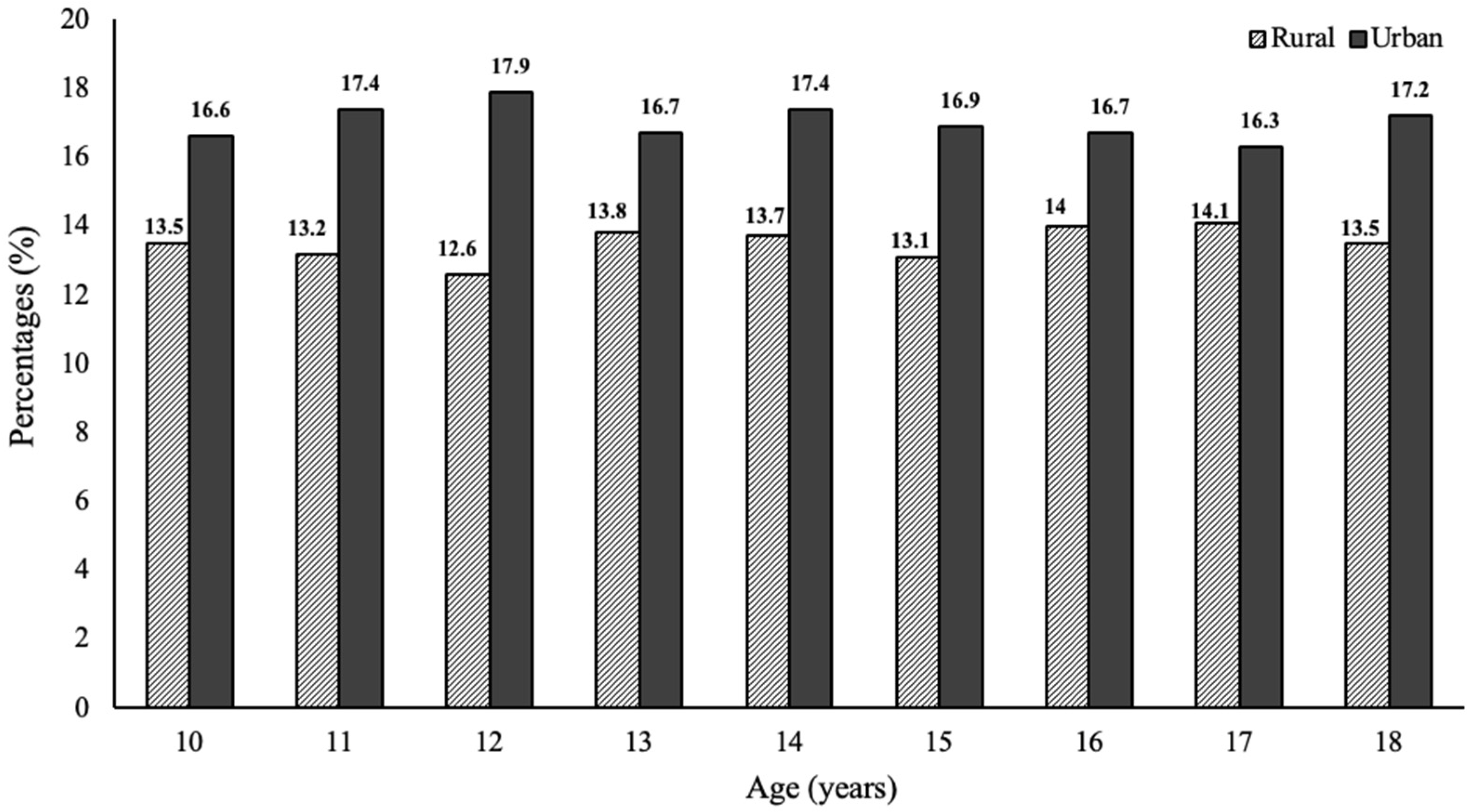
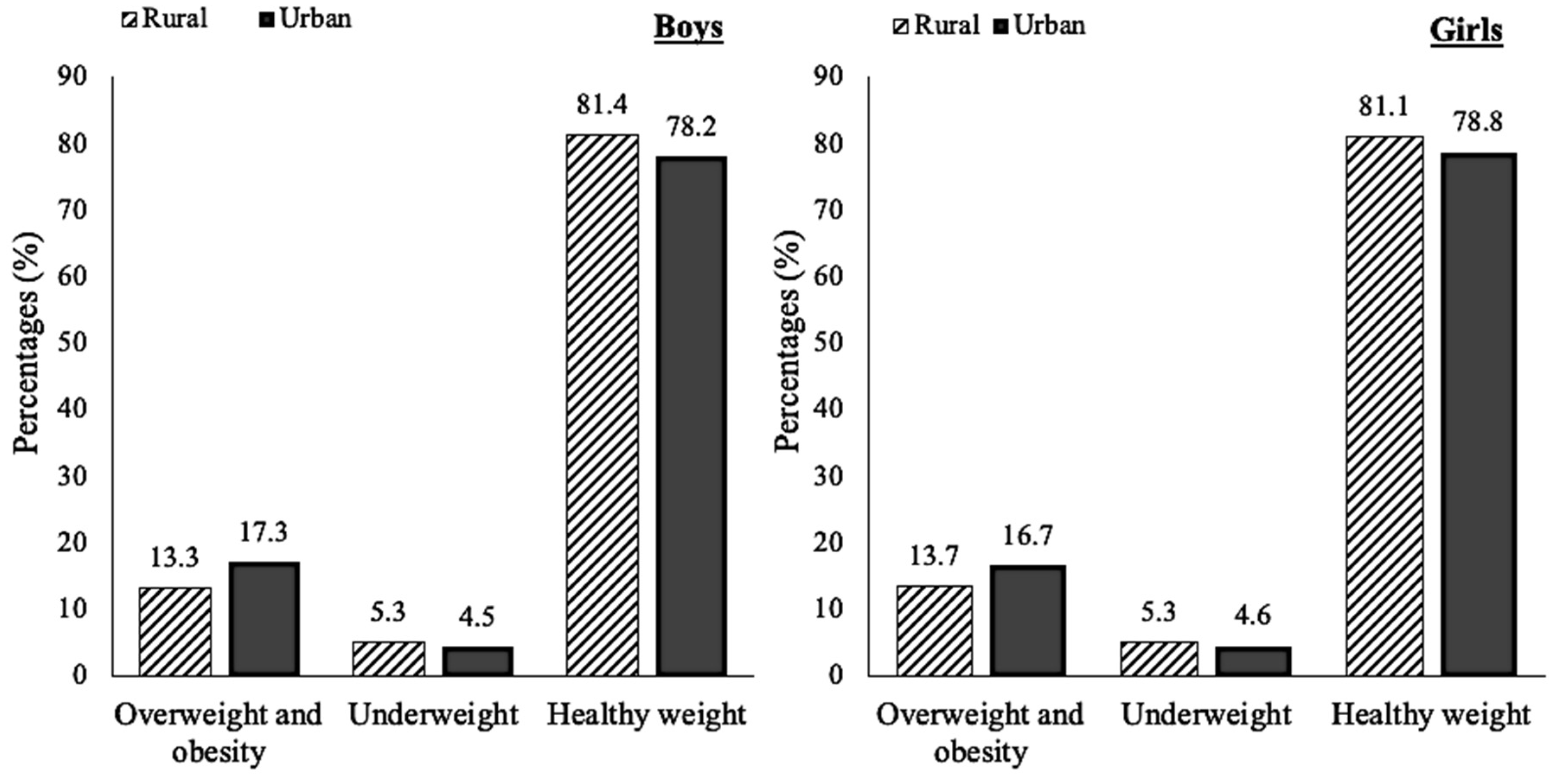
3.1. Prevalence of Obesity in Rural and Urban Areas
3.2. Sedentary Activity and Dietary Behaviour in Rural and Urban Areas
3.3. Overweight and Obesity Risk in Rural and Urban Areas
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ford, N.D.; Patel, S.A.; Narayan, K.V. Obesity in Low- and Middle-Income Countries: Burden, Drivers, and Emerging Challenges. Annu. Rev. Public Health 2017, 38, 145–164. [Google Scholar] [CrossRef] [PubMed]
- Jaacks, L.M.; Kavle, J.; Perry, A.; Nyaku, A. Programming maternal and child overweight and obesity in the context of undernutrition: current evidence and key considerations for low- and middle-income countries. Public Health Nutr. 2017, 20, 1286–1296. [Google Scholar] [CrossRef] [PubMed]
- Jaacks, L.M.; Slining, M.M.; Popkin, B.M. Recent Underweight and Overweight Trends by Rural–Urban Residence among Women in Low- and Middle-Income Countries. J. Nutr. 2014, 145, 352–357. [Google Scholar] [CrossRef] [PubMed]
- Poobalan, A.; Aucott, L. Obesity among Young Adults in Developing Countries: A Systematic Overview. Curr. Obes. Rep. 2016, 5, 2–13. [Google Scholar] [CrossRef] [PubMed]
- Popkin, B.M.; Slining, M.M. New dynamics in global obesity facing low- and middle-income countries. Obes. Rev. 2013, 14, 11–20. [Google Scholar] [CrossRef]
- Williams, E.P.; Mesidor, M.; Winters, K.; Dubbert, P.M.; Wyatt, S.B. Overweight and Obesity: Prevalence, Consequences, and Causes of a Growing Public Health Problem. Curr. Obes. Rep. 2015, 4, 363–370. [Google Scholar] [CrossRef]
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F.; et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; De Onis, M.; Ezzati, M.; Grantham-McGregor, S.; Katz, J.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- National Institute of Health Research and Development. The Main Results of Riskesdas 2018; Ministry of Health: Jakarta, Indonesia, 2018.
- National Institute of Health Research and Development. Riset Kesehatan Dasar 2013; Ministry of Health: Jakarta, Indonesia, 2013.
- Oddo, V.M.; Mueller, N.T.; Pollack, K.M.; Surkan, P.J.; Bleich, S.N.; Jones-Smith, J.C. Maternal employment and childhood overweight in low- and middle-income countries. Public Health Nutr. 2017, 20, 2523–2536. [Google Scholar] [CrossRef]
- Horiuchi, Y.; Kusama, K.; Kanha, S.; Yoshiike, N.; FIDR Research and the FIDR Research Team. Urban-Rural Differences in Nutritional Status and Dietary Intakes of School-Aged Children in Cambodia. Nutrients 2018, 11, 14. [Google Scholar] [CrossRef]
- Le Nguyen, B.K.; Le Thi, H.; Thuy, N.T.; Huu, C.N.; Do, T.T.; Deurenberg, P.; Khouw, I. Double burden of undernutrition and overnutrition in Vietnam in 2011: Results of the SEANUTS study in 0.5–11-year-old children. Br. J. Nutr. 2013, 110, S45–S56. [Google Scholar] [CrossRef] [PubMed]
- Sandjaja, S.; Budiman, B.; Harahap, H.; Ernawati, F.; Soekatri, M.; Widodo, Y.; Sumedi, E.; Rustan, E.; Sofia, G.; Syarief, S.N.; et al. Food consumption and nutritional and biochemical status of 0.5-12-year-old Indonesian children: the SEANUTS study. Br. J. Nutr. 2013, 110, S11–S20. [Google Scholar] [CrossRef] [PubMed]
- Jia, P.; Li, M.; Xue, H.; Lu, L.; Xu, F.; Wang, Y. School environment and policies, child eating behavior and overweight/obesity in urban China: The childhood obesity study in China megacities. Int. J. Obes. 2017, 41, 813–819. [Google Scholar] [CrossRef] [PubMed]
- Ramirez, V.R.; Gonzalez, R.K.; Correa, B.J.E.; Meneses, E.J.F.; Martinez, T.J. Demographic and socioeconomic differences in consumption of sugar-sweetened beverages among Colombian children and adolescents. Nutr. Hosp. 2015, 31, 2479–2486. [Google Scholar]
- Wang, H.; Liu, C.; Fan, H.; Tian, X. Rising food accessibility contributed to the increasing dietary diversity in rural and urban China. Asia Pac. J. Clin. Nutr. 2017, 26, 738–747. [Google Scholar] [PubMed]
- Kerry, S.M.; Emmett, L.; Micah, F.B.; Martin-Peprah, R.; Antwi, S.; Phillips, R.O.; Plange-Rhule, J.; Eastwood, J.B.; Cappuccio, F.P. Rural and semi-urban differences in salt intake, and its dietary sources, in Ashanti, West Africa. Ethn. Dis. 2005, 15, 33–39. [Google Scholar]
- National Institute of Health Research and Development. Indonesia Health Profile 2013; Ministry of Health: Jakarta, Indonesia, 2013.
- Rojroongwasinkul, N.; Kijboonchoo, K.; Wimonpeerapattana, W.; Purttiponthanee, S.; Yamborisut, U.; Boonpraderm, A.; Kunapan, P.; Thasanasuwan, W.; Khouw, I. SEANUTS: The nutritional status and dietary intakes of 0.5–12-year-old Thai children. Br. J. Nutr. 2013, 110, S36–S44. [Google Scholar] [CrossRef]
- Poh, B.K.; Ng, B.K.; Haslinda, M.D.; Shanita, S.N.; Wong, J.E.; Budin, S.B.; Ruzita, A.T.; Ng, L.O.; Khouw, I.; Norimah, A.K. Nutritional status and dietary intakes of children aged 6 months to 12 years: Findings of the Nutrition Survey of Malaysian Children (SEANUTS Malaysia). Br. J. Nutr. 2013, 110, S21–S35. [Google Scholar] [CrossRef]
- Wang, Y.; Lobstein, T. Worldwide trends in childhood overweight and obesity. Pediatr. Obes. 2006, 1, 11–25. [Google Scholar] [CrossRef]
- Siddiqui, S.T.; Kandala, N.B.; Stranges, S. Urbanisation and geographic variation of overweight and obesity in India: A cross-sectional analysis of the Indian Demographic Health Survey 2005–2006. Int. J. Public Health 2015, 60, 717–726. [Google Scholar] [CrossRef]
- Chen, M.; Liu, W.; Tao, X. Evolution and assessment on China’s urbanization 1960–2010: Under-urbanization or over-urbanization? Habitat Int. 2013, 38, 25–33. [Google Scholar] [CrossRef]
- Dong, Y.; Ma, Y.; Dong, B.; Zou, Z.; Hu, P.; Wang, Z.; Yang, Y.; Song, Y.; Ma, J. Geographical variation and urban-rural disparity of overweight and obesity in Chinese school-aged children between 2010 and 2014: Two successive national cross-sectional surveys. BMJ Open 2019, 9, e025559. [Google Scholar] [CrossRef] [PubMed]
- Mbanya, J.C.; Unwin, N.C.; Minkoulou, E.M.; Tournoux, C.; Sobngwi, E.; Porcher, R.; Kengne, A.P.; Fezeu, L.; Gautier, J.F.; Aspray, T.J.; et al. Exposure over the life course to an urban environment and its relation with obesity, diabetes, and hypertension in rural and urban Cameroon. Int. J. Epidemiol. 2004, 33, 769–776. [Google Scholar]
- Peters, R.; Amugsi, D.A.; Mberu, B.; Ensor, T.; Hill, A.J.; Newell, J.N.; Elsey, H. Nutrition transition, overweight and obesity among rural-to-urban migrant women in Kenya. Public Health Nutr. 2019, 22, 3200–3210. [Google Scholar] [CrossRef]
- Lobstein, T.; Baur, L.; Uauy, R. Obesity in children and young people: A crisis in public health. Obes. Rev. 2004, 5, 4–85. [Google Scholar] [CrossRef]
- Sallis, J.F.; Cerin, E.; Conway, T.L.; Adams, M.A.; Frank, L.D.; Pratt, M.; Salvo, D.; Schipperijn, J.; Smith, G.; Cain, K.L.; et al. Physical activity in relation to urban environments in 14 cities worldwide: A cross-sectional study. Lancet 2016, 387, 2207–2217. [Google Scholar] [CrossRef]
- Schroder, H.; Bawaked, R.A.; Ribas-Barba, L.; Izquierdo-Pulido, M.; Roman-Viñas, B.; Fíto, M.; Serra-Majem, L. Cumulative Effect of Obesogenic Behaviours on Adiposity in Spanish Children and Adolescents. Obes. Facts 2017, 10, 584–596. [Google Scholar] [CrossRef]
- Amanzadeh, B.; Sokal-Gutierrez, K.; Barker, J.C. An interpretive study of food, snack and beverage advertisements in rural and urban El Salvador. BMC Public Health 2015, 15, 521. [Google Scholar] [CrossRef]
- Welk, G.J.; Calabro, M.A.; Russell, D.W.; Nicklay, E.; Hensley, L.D.; Joens-Matre, R.R. Rural–Urban Differences in Physical Activity, Physical Fitness, and Overweight Prevalence of Children. J. Rural. Health 2008, 24, 49–54. [Google Scholar]
- Fisher, M.; Juszczak, L.; Friedman, S.B. Sports participation in an urban high school: Academic and psychologic correlates. J. Adolesc. Health 1996, 18, 329–334. [Google Scholar] [CrossRef]
- Reimers, A.K.; Wagner, M.; Alvanides, S.; Steinmayr, A.; Reiner, M.; Schmidt, S.; Wöll, A. Proximity to Sports Facilities and Sports Participation for Adolescents in Germany. PLoS ONE 2014, 9, e93059. [Google Scholar] [CrossRef] [PubMed]
- Van Hecke, L.; Deforche, B.; Van Dyck, D.; De Bourdeaudhuij, I.; Veitch, J.; Van Cauwenberg, J. Social and Physical Environmental Factors Influencing Adolescents’ Physical Activity in Urban Public Open Spaces: A Qualitative Study Using Walk-Along Interviews. PLoS ONE 2016, 11, e0155686. [Google Scholar] [CrossRef] [PubMed]
- Machado-Rodrigues, A.M.; Coelho-E-Silva, M.J.; Mota, J.; Padez, C.; Martins, R.A.; Cumming, S.P.; Riddoch, C.; Malina, R.M. Urban-rural contrasts in fitness, physical activity, and sedentary behaviour in adolescents. Health Promot. Int. 2012, 29, 118–129. [Google Scholar] [CrossRef] [PubMed]
- Jensen, B.W.; Nichols, M.; Allender, S.; de Silva-Sanigorski, A.; Millar, L.; Kremer, P.; Lacy, K.; Swinburn, B. Consumption patterns of sweet drinks in a population of Australian children and adolescents (2003–2008). BMC Public Health 2012, 12, 771. [Google Scholar] [CrossRef] [PubMed]
- Basu, S.; McKee, M.; Galea, G.; Stuckler, D. Relationship of Soft Drink Consumption to Global Overweight, Obesity, and Diabetes: A Cross-National Analysis of 75 Countries. Am. J. Public Health 2013, 103, 2071–2077. [Google Scholar] [CrossRef]
- Malik, V.S.; Schulze, M.B.; Hu, F.B. Intake of sugar-sweetened beverages and weight gain: A systematic review. Am. J. Clin. Nutr. 2006, 84, 274–288. [Google Scholar] [CrossRef]
- Schneider, M.B.; Benjamin, H.J.; Bhatia, J.J.; Abrams, S.A.; De Ferranti, S.D.; Silverstein, J.; Stettler, N.; Thomas, D.W.; Daniels, S.R.; Greer, F.R.; et al. Sports drinks and energy drinks for children and adolescents: Are they appropriate? Pediatrics 2011, 127, 1182–1189. [Google Scholar]
- Alsunni, A.A. Energy Drink Consumption: Beneficial and Adverse Health Effects. Int. J. Health Sci. 2015, 9, 468–474. [Google Scholar] [CrossRef]
- Rush, E.; Schulz, S.; Obolonkin, V.; Simmons, D.; Plank, L. Are energy drinks contributing to the obesity epidemic? Asia Pac. J. Clin. Nutr. 2006, 15, 242–244. [Google Scholar]
- Vartanian, L.R.; Schwartz, M.B.; Brownell, K.D. Effects of Soft Drink Consumption on Nutrition and Health: A Systematic Review and Meta-Analysis. Am. J. Public Health 2007, 97, 667–675. [Google Scholar] [CrossRef]
- Keast, R.S.J.; Swinburn, B.A.; Sayompark, D.; Whitelock, S.; Riddell, L.J. Caffeine increases sugar-sweetened beverage consumption in a free-living population: A randomised controlled trial. Br. J. Nutr. 2015, 113, 366–371. [Google Scholar] [CrossRef] [PubMed]
- Taillie, L.S.; Afeiche, M.C.; Eldridge, A.L.; Popkin, B.M. Increased Snacking and Eating Occasions Are Associated with Higher Energy Intake among Mexican Children Aged 2–13 Years. J. Nutr. 2015, 145, 2570–2577. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.; Lee, J.E.; Chang, Y.; Kim, M.K.; Sung, E.; Shin, H.; Ryu, S. Dietary sodium and potassium intake in relation to non-alcoholic fatty liver disease. Br. J. Nutr. 2016, 116, 1447–1456. [Google Scholar] [CrossRef] [PubMed]
- Lanaspa, M.A.; Kuwabara, M.; Andres-Hernando, A.; Li, N.; Cicerchi, C.; Jensen, T.; Orlicky, D.J.; Roncal-Jimenez, C.A.; Ishimoto, T.; Nakagawa, T.; et al. High salt intake causes leptin resistance and obesity in mice by stimulating endogenous fructose production and metabolism. Proc. Natl. Acad. Sci. USA 2018, 115, 3138–3143. [Google Scholar] [CrossRef]
- Larson, N.I.; Miller, J.M.; Watts, A.W.; Story, M.T.; Neumark-Sztainer, D.R. Adolescent Snacking Behaviors Are Associated with Dietary Intake and Weight Status. J. Nutr. 2016, 146, 1348–1355. [Google Scholar] [CrossRef]
- Vergnaud, A.C.; Norat, T.; Romaguera, D.; Mouw, T.; May, A.M.; Travier, N.; Luan, J.; Wareham, N.; Slimani, N.; Rinaldi, S.; et al. Meat consumption and prospective weight change in participants of the EPIC-PANACEA study. Am. J. Clin. Nutr. 2010, 92, 398–407. [Google Scholar] [CrossRef]
- Wagemakers, J.J.; Prynne, C.J.; Stephen, A.M.; Wadsworth, M.E. Consumption of red or processed meat does not predict risk factors for coronary heart disease; results from a cohort of British adults in 1989 and 1999. Eur. J. Clin. Nutr. 2009, 63, 303–311. [Google Scholar] [CrossRef]
- Esmaillzadeh, A.; Azadbakht, L. Major Dietary Patterns in Relation to General Obesity and Central Adiposity among Iranian Women. J. Nutr. 2008, 138, 358–363. [Google Scholar] [CrossRef]
- Schulze, M.B.; Hu, F.B. Dietary patterns and risk of hypertension, type 2 diabetes mellitus, and coronary heart disease. Curr. Atheroscler. Rep. 2002, 4, 462–467. [Google Scholar] [CrossRef]
- Hu, F.B. Dietary pattern analysis: a new direction in nutritional epidemiology. Curr. Opin. Lipidol. 2002, 13, 3–9. [Google Scholar] [CrossRef]
- Schulze, M.B.; Manson, J.E.; Willett, W.C.; Hu, F.B. Processed meat intake and incidence of Type 2 diabetes in younger and middle-aged women. Diabetologia 2003, 46, 1465–1473. [Google Scholar] [CrossRef] [PubMed]
- Xu, F.; Yin, X.M.; Tong, S.L. Association between excess bodyweight and intake of red meat and vegetables among urban and rural adult Chinese in Nanjing, China. Asia Pac. J. Public Health 2007, 19, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Rouhani, M.H.; Mirseifinezhad, M.; Omrani, N.; Esmaillzadeh, A.; Azadbakht, L. Fast Food Consumption, Quality of Diet, and Obesity among Isfahanian Adolescent Girls. J. Obes. 2012, 2012, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wu, G.D.; Chen, J.; Hoffmann, C.; Bittinger, K.; Chen, Y.Y.; Keilbaugh, S.A.; Bewtra, M.; Knights, D.; Walters, W.A.; Knight, R.; et al. Linking long-term dietary patterns with gut microbial enterotypes. Science 2011, 334, 105–108. [Google Scholar] [CrossRef] [PubMed]
- Cohen, A.K.; Rai, M.; Rehkopf, D.H.; Abrams, B. Educational attainment and obesity: A systematic review. Obes. Rev. 2013, 14, 989–1005. [Google Scholar] [CrossRef] [PubMed]
- Hajian-Tilaki, K.O.; Heidari, B. Association of educational level with risk of obesity and abdominal obesity in Iranian adults. J. Public Health 2009, 32, 202–209. [Google Scholar] [CrossRef] [PubMed]
- Al Yateem, N.; Rossiter, R. Nutritional knowledge and habits of adolescents aged 9 to 13 years in Sharjah, United Arab Emirates: A crosssectional study. East. Mediterr. Health J. 2017, 23, 551–558. [Google Scholar] [CrossRef]
- Trichesa, R.M.; Giuglianib, E.R.J. Obesity, eating habits and nutritional knowledge among school children. Rev. Saude Publica 2005, 39, 541. [Google Scholar]
- Sigmund, E.; Sigmundová, D.; Badura, P.; Gecková, A.M. Health-related parental indicators and their association with healthy weight and overweight/obese children’s physical activity. BMC Public Health 2018, 18, 676. [Google Scholar] [CrossRef]
- Robinson, E.; Sutin, A.R. Parents’ Perceptions of Their Children as Overweight and Children’s Weight Concerns and Weight Gain. Psychol. Sci. 2017, 28, 320–329. [Google Scholar] [CrossRef]

| Variables (Ref vs. Risk) | Overweight and Obese | ||||||
|---|---|---|---|---|---|---|---|
| Rural and Urban (n = 155,645) | Rural (n = 83,820) | Urban (n = 71,825) | |||||
| OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Residency | Rural | ref | |||||
| Urban | 1.32 *** | 1.28–1.35 | - | - | - | - | |
| Gender | Girls | ref | ref | ref | |||
| Boys | 1.01 | 0.98–1.04 | 0.97 | 0.93–1.01 | 1.05 * | 1.01–1.10 | |
| Age | 15–18 years | ref | ref | ref | |||
| 10–14 years | 1.06 * | 1.02–1.10 | 1.03 | 0.97–1.08 | 1.10 * | 1.04–1.17 | |
| Education level | |||||||
| High | ref | ref | ref | ||||
| Low (not completed in primary school) | 0.92 * | 0.89–0.96 | 0.93 * | 0.87–0.98 | 0.91 * | 0.86–0.97 | |
| Sedentary activity | |||||||
| <2 h/day | ref | ref | ref | ||||
| 2–4 h/day | 1.12 *** | 1.08–1.18 | 1.10 * | 1.03–1.17 | 1.11 * | 1.04–1.19 | |
| >4–6 h/day | 1.09 *** | 1.05–1.14 | 1.09 * | 1.03–1.16 | 1.06 | 0.99–1.14 | |
| >6–8h/day | 1.09 * | 1.02–1.16 | 1.07 | 0.98–1.18 | 1.05 | 0.95–1.15 | |
| >8 h/day | 1.15 *** | 1.08–1.22 | 1.06 | 0.96–1.16 | 1.13 * | 1.04–1.23 | |
| Sugar-sweetened beverages and foods | |||||||
| <1 time/day | ref | ref | ref | ||||
| ≥1 time/day | 0.97 | 0.94–1.00 | 0.98 | 0.94–1.02 | 0.95 * | 0.92–0.99 | |
| Coffee consumption | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.01 | 0.96–1.06 | 1.04 | 0.98–1.11 | 0.96 | 0.89–1.03 | |
| Caffeinated soft drinks and energy drinks consumption | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.11 * | 1.03–.19 | 1.10 | 0.99–1.22 | 1.12 * | 1.01–1.23 | |
| Fatty fried foods | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.00 | 0.96–1.03 | 0.96 | 0.92–1.01 | 1.03 | 0.99–1.07 | |
| Refined carbohydrate | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.01 | 0.97–1.05 | 0.98 | 0.92–1.03 | 1.04 | 0.99–1.09 | |
| Salty foods | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.03 | 0.99–1.07 | 1.09 * | 1.04–1.15 | 0.98 | 0.93–1.03 | |
| Instant noodle | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 0.95 * | 0.91–0.99 | 0.95 | 0.89–1.01 | 0.95 | 0.90–1.01 | |
| Preserved meats | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 0.95 | 0.89–1.01 | 0.93 | 0.83–1.03 | 0.97 | 0.89–1.06 | |
| Grilled foods | <1 time/day | ref | ref | ref | |||
| ≥1 time/day | 1.19 *** | 1.12–1.26 | 1.32 * | 1.22–1.42 | 1.03 | 0.94–1.14 | |
| Vegetables and fruits | ≥5 portion/day | ref | ref | ref | |||
| <5 portion/day | 0.92 * | 0.88–0.98 | 0.96 | 0.89–1.04 | 0.90 * | 0.83–0.96 | |
| Variables | Boys | p-Value | Girls | p-Value | ||
|---|---|---|---|---|---|---|
| Rural (n = 43,207) | Urban (n = 36,219) | Rural (n = 40,613) | Urban (n = 35,606) | |||
| Sugar-sweetened beverages and foods | ||||||
| <1 time/day | 51.2 | 44.0 | <0.0001 | 53.2 | 46.1 | <0.0001 |
| ≥1 time/day | 48.8 | 56.0 | 46.8 | 53.9 | ||
| Coffee consumption | ||||||
| <1 time/day | 83.7 | 88.9 | <0.0001 | 90.8 | 94.9 | <0.0001 |
| ≥1 time/day | 16.3 | 11.1 | 9.2 | 5.1 | ||
| Caffeinated soft drinks and energy drinks consumption | ||||||
| <1 time/day | 95.6 | 95.0 | <0.0001 | 96.6 | 96.2 | 0.0011 |
| ≥1 time/day | 4.4 | 5.0 | 3.4 | 3.8 | ||
| Fatty fried foods | ||||||
| <1 time/day | 70.3 | 62.0 | <0.0001 | 69.3 | 61.2 | <0.0001 |
| ≥1 time/day | 29.7 | 38.0 | 30.7 | 38.8 | ||
| Refined carbohydrate | ||||||
| <1 time/day | 84.6 | 76.8 | <0.0001 | 83.2 | 75.9 | <0.0001 |
| ≥1 time/day | 15.4 | 23.2 | 16.8 | 24.1 | ||
| Salty foods | ||||||
| <1 time/day | 78.9 | 79.1 | 0.5847 | 78.9 | 78.3 | 0.0536 |
| ≥1 time/day | 21.1 | 20.9 | 21.1 | 21.7 | ||
| Instant noodle | ||||||
| <1 time/day | 85.5 | 85.2 | 0.3081 | 85.4 | 85.6 | 0.3937 |
| ≥1 time/day | 14.5 | 14.8 | 14.6 | 14.4 | ||
| Preserved meats | ||||||
| <1 time/day | 96.0 | 93.8 | <0.0001 | 95.9 | 93.5 | <0.0001 |
| ≥1 time/day | 4.0 | 6.2 | 4.1 | 6.5 | ||
| Grilled foods | ||||||
| <1 time/day | 92.8 | 95.1 | <0.0001 | 93.1 | 94.9 | <0.0001 |
| ≥1 time/day | 7.2 | 4.9 | 6.9 | 5.1 | ||
| Vegetables and fruits | ||||||
| ≥5 portion/day | 6.7 | 7.4 | 0.0001 | 6.8 | 7.0 | 0.2831 |
| <5 portion/day | 93.3 | 92.6 | 93.2 | 93.0 | ||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nurwanti, E.; Hadi, H.; Chang, J.-S.; Chao, J.C.-J.; Paramashanti, B.A.; Gittelsohn, J.; Bai, C.-H. Rural–Urban Differences in Dietary Behavior and Obesity: Results of the Riskesdas Study in 10–18-Year-Old Indonesian Children and Adolescents. Nutrients 2019, 11, 2813. https://doi.org/10.3390/nu11112813
Nurwanti E, Hadi H, Chang J-S, Chao JC-J, Paramashanti BA, Gittelsohn J, Bai C-H. Rural–Urban Differences in Dietary Behavior and Obesity: Results of the Riskesdas Study in 10–18-Year-Old Indonesian Children and Adolescents. Nutrients. 2019; 11(11):2813. https://doi.org/10.3390/nu11112813
Chicago/Turabian StyleNurwanti, Esti, Hamam Hadi, Jung-Su Chang, Jane C.-J. Chao, Bunga Astria Paramashanti, Joel Gittelsohn, and Chyi-Huey Bai. 2019. "Rural–Urban Differences in Dietary Behavior and Obesity: Results of the Riskesdas Study in 10–18-Year-Old Indonesian Children and Adolescents" Nutrients 11, no. 11: 2813. https://doi.org/10.3390/nu11112813
APA StyleNurwanti, E., Hadi, H., Chang, J.-S., Chao, J. C.-J., Paramashanti, B. A., Gittelsohn, J., & Bai, C.-H. (2019). Rural–Urban Differences in Dietary Behavior and Obesity: Results of the Riskesdas Study in 10–18-Year-Old Indonesian Children and Adolescents. Nutrients, 11(11), 2813. https://doi.org/10.3390/nu11112813






