Daily Intake of Milk Powder and Risk of Celiac Disease in Early Childhood: A Nested Case-Control Study
Abstract
1. Introduction
2. Subjects and Methods
2.1. Study Population
2.2. Screening for Celiac Disease
2.3. Study Design
2.4. Dietary Assessment
2.5. Statistical Analysis
3. Results
4. Discussion
Author Contributions
Acknowledgments
Colorado Clinical Center
Finland Clinical Center
Georgia/Florida Clinical Center
Germany Clinical Center
Sweden Clinical Center
Washington Clinical Center
Pennsylvania Satellite Center
Data Coordinating Center
Project scientist
Autoantibody Reference Laboratories
HLA Reference Laboratory
Repository
Other contributors
Committees
Trial Identification Number
Conflicts of Interest
References
- Liu, E.; Lee, H.S.; Aronsson, C.A.; Hagopian, W.A.; Koletzko, S.; Rewers, M.J.; Eisenbarth, G.S.; Bingley, P.J.; Bonifacio, E.; Simell, V.; et al. Risk of pediatric celiac disease according to HLA haplotype and country. N. Engl. J. Med. 2014, 371, 42–49. [Google Scholar] [CrossRef] [PubMed]
- Ivarsson, A.; Myléus, A.; Norström, F.; van der Pals, M.; Rosén, A.; Högberg, L.; Danielsson, L.; Halvarsson, B.; Hammarroth, S.; Hernell, O.; et al. Prevalence of childhood celiac disease and changes in infant feeding. Pediatrics 2013, 131, e687–e694. [Google Scholar] [CrossRef] [PubMed]
- Aronsson, C.A.; Lee, H.S.; Koletzko, S.; Uusitalo, U.; Yang, J.; Virtanen, S.M.; Liu, E.; Lernmark, A.; Norris, J.M.; Agardh, D.; et al. Effects of Gluten Intake on Risk of Celiac Disease: A Case-Control Study on a Swedish Birth Cohort. Clin. Gastroenterol. Hepatol. 2016, 14, 403–409. [Google Scholar] [CrossRef] [PubMed]
- Dieterich, W.; Laag, E.; Schöpper, H.; Volta, U.; Ferguson, A.; Gillett, H.; Riecken, E.O.; Schuppan, D. Autoantibodies to tissue transglutaminase as predictors of celiac disease. Gastroenterology 1998, 115, 1317–1321. [Google Scholar] [CrossRef]
- Hyytinen, M.; Savilahti, E.; Virtanen, S.M.; Härkönen, T.; Ilonen, J.; Luopajärvi, K.; Uibo, R.; Vaarala, O.; Åkerblom, H.K.; Knip, M.; et al. Avoidance of Cow's Milk-based Formula for At-risk Infants Does Not Reduce Development of Celiac Disease: A Randomized Controlled Trial. Gastroenterology 2017, 153, 961–970. [Google Scholar] [CrossRef] [PubMed]
- Almquist-Tangen, G.; Dahlgren, J.; Roswall, J.; Bergman, S.; Alm, B. Milk cereal drink increases BMI risk at 12 and 18 months, but formula does not. Acta Paediatr. 2013, 102, 1174–1179. [Google Scholar] [CrossRef] [PubMed]
- Kellow, N.J.; Savige, G.S. Dietary advanced glycation end-product restriction for the attenuation of insulin resistance, oxidative stress and endothelial dysfunction: A systematic review. Eur. J. Clin. Nutr. 2013, 67, 239–248. [Google Scholar] [CrossRef] [PubMed]
- Van Puyvelde, K.; Mets, T.; Njemini, R.; Beyer, I.; Bautmans, I. Effect of advanced glycation end product intake on inflammation and aging: A systematic review. Nutr. Rev. 2014, 72, 638–650. [Google Scholar] [CrossRef] [PubMed]
- Plaza, M.; Östman, E.; Tareke, E. Maillard Reaction Products in Powder Based for Infants and Toddlers. Eur. J. Nutr. Food Saf. 2016, 6, 65–74. [Google Scholar] [CrossRef]
- Hagopian, W.A.; Erlich, H.; Lernmark, Å.; Rewers, M.; Ziegler, A.G.; Simell, O.; Akolkar, B.; Vogt, R., Jr.; Blair, A.; Llonen, J.; et al. The Environmental Determinants of Diabetes in the Young (TEDDY): Genetic criteria and international diabetes risk screening of 421 000 infants. Pediatr. Diabetes 2011, 12, 733–743. [Google Scholar] [CrossRef] [PubMed]
- Livsmedelsverket. Swedish National Food Composition Database. 2016. Available online: http://www7.slv.se/SokNaringsinnehall (accessed on 8 December 2016).
- Hoppe, C.; Trolle, E.; Gondolf, U.H.; Husby, S. Gluten intake in 6-36-month-old Danish infants and children based on a national survey. J. Nutr. Sci. 2013, 2, 1–7. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids; The National Academies Press: Washington, DC, USA, 2005. [Google Scholar]
- Gibson, R.S. Priciples of Nutritional Assessment, 2nd ed.; Oxford University Press: New York, NY, USA, 2005. [Google Scholar]
- Ivarsson, A.; Hernell, O.; Stenlund, H.; Persson, L.Å. Breast-feeding protects against celiac disease. Am. J. Clin. Nutr. 2002, 75, 914–921. [Google Scholar] [CrossRef] [PubMed]
- Akobeng, A.K.; Ramanan, A.V.; Buchan, I.; Heller, R.F. Effect of breast feeding on risk of coeliac disease: A systematic review and meta-analysis of observational studies. Arch. Dis. Child. 2006, 91, 39–43. [Google Scholar] [CrossRef] [PubMed]
- Lachat, C.; Hawwash, D.; Ocké, M.C.; Berg, C.; Forsum, E.; Hörnell, A.; Larsson, C.I.; Sonestedt, E.; Wirfält, E.; Åkessonet, A.; et al. Strengthening the Reporting of Observational Studies in Epidemiology—nutritional epidemiology (STROBE-nut): An extension of the STROBE statement. Nutr. Bull. 2016, 41, 240–251. [Google Scholar] [CrossRef] [PubMed]

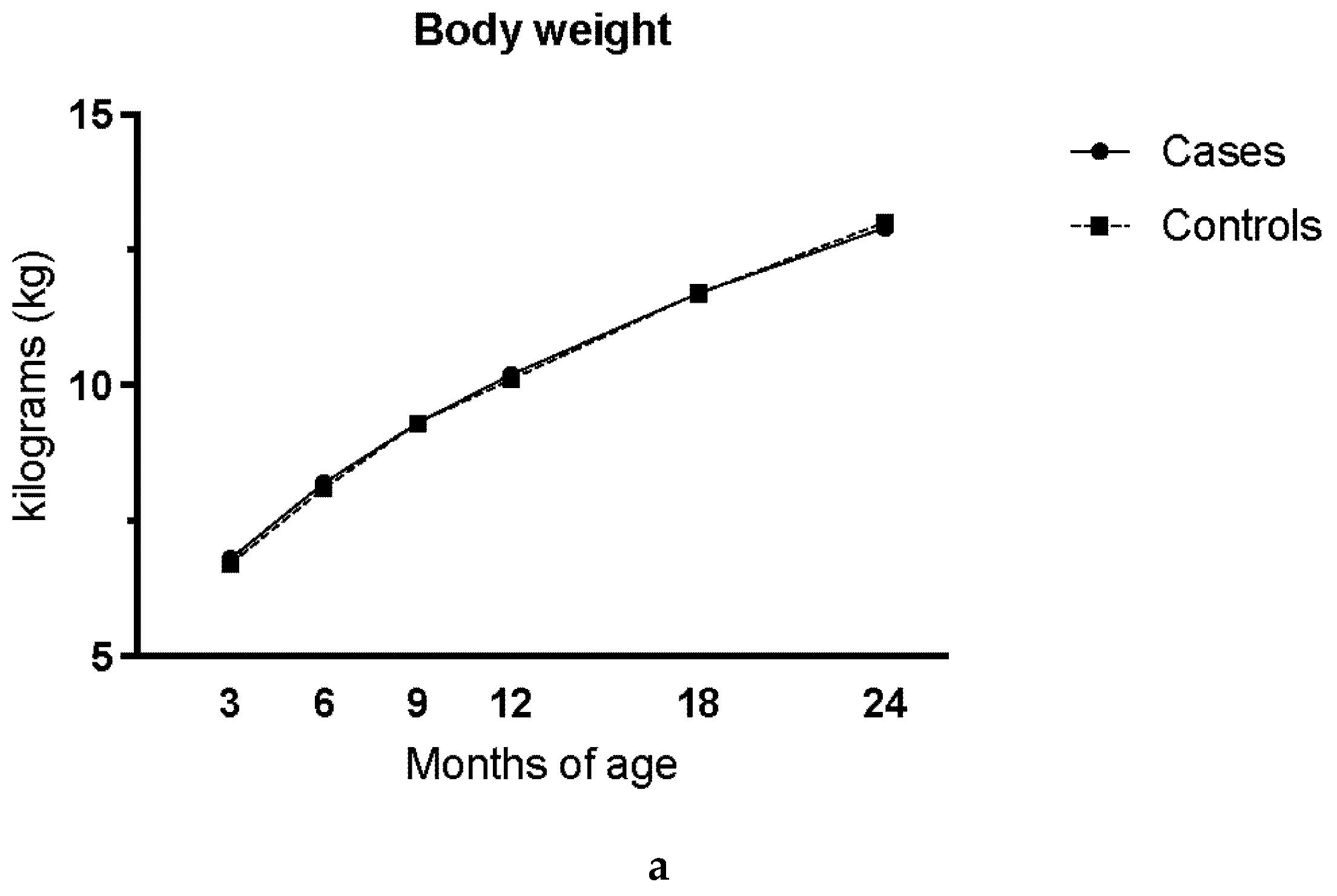
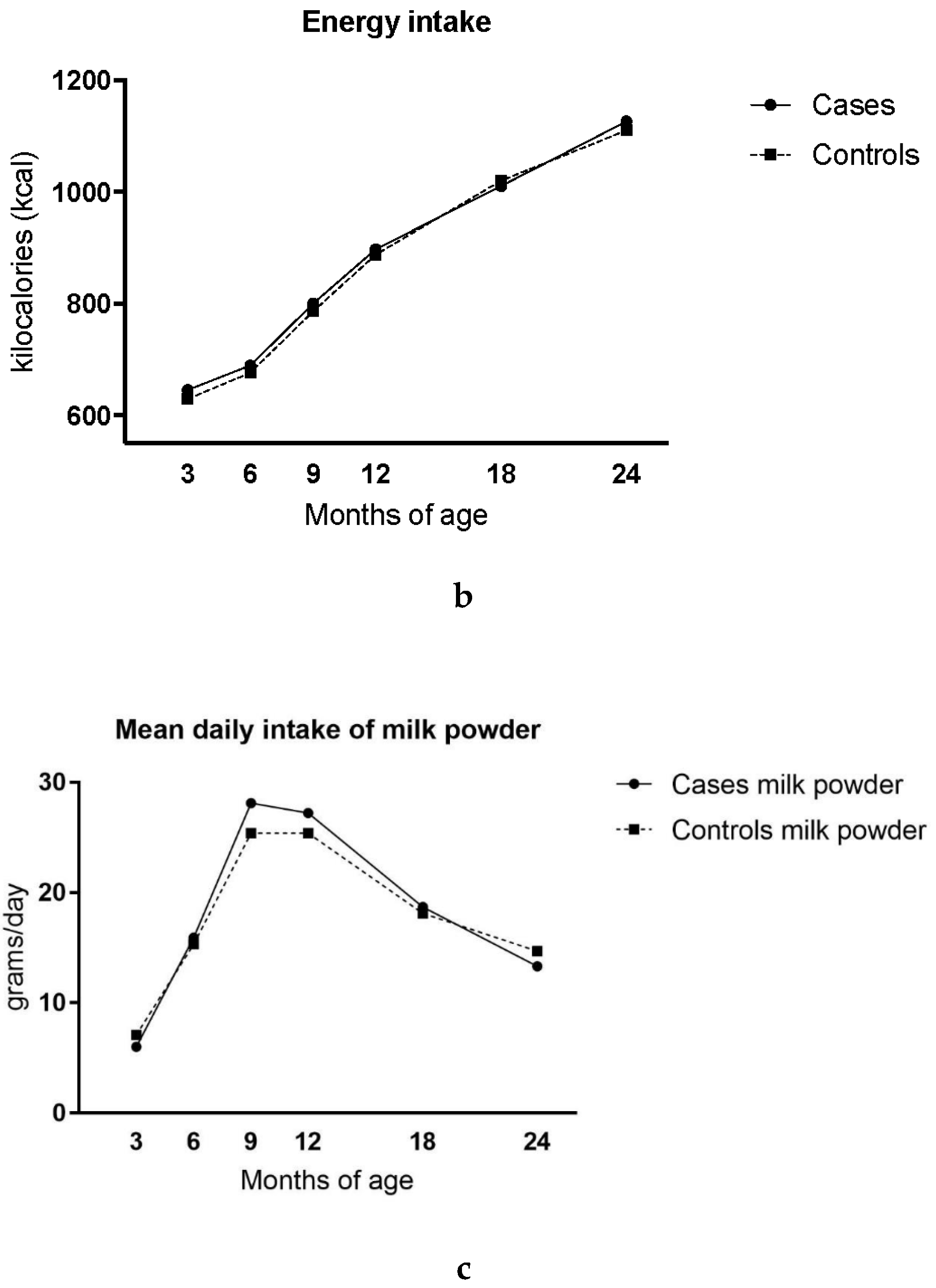
| Matching Variable | Cases N = 207 (%) |
|---|---|
| Sex | |
| - Female | 131 (63.3) |
| - Male | 76 (36.7) |
| Birth year | |
| - 2004 | 11 (5.3) |
| - 2005 | 39 (18.8) |
| - 2006 | 28 (13.5) |
| - 2007 | 41 (19.8) |
| - 2008 | 37 (17.9) |
| - 2009 | 46 (22.2) |
| - 2010 | 5 (2.4) |
| HLA-genotype | |
| - DQ2/DQ8 | 64 (30.9) |
| - DQ8/DQ8 | 35 (16.9) |
| - DQ2/DQ2 | 100 (48.3) |
| - Other | 8 (3.9) |
| Time point | Number of cases analyzed | Number of cases missing intake | Milk powder intake (g/day) | Milk powder intake (g/kg/day) | ||
|---|---|---|---|---|---|---|
| OR (CI 95%) | p-value | OR (CI 95%) | p-value | |||
| Last intake 1 | 207 | 0 | 1.0 (0.99–1.01) | 0.937 | 0.99 (0.87–1.13) | 0.861 |
| Total intake 2 | 207 | 0 | 1.0 (1.0–1.00) | 0.662 | 1.0 (0.98–1.03) | 0.763 |
| Intake at | ||||||
| 3 months | 207 | 0 | 0.99 (0.97–1.01) | 0.159 | 0.92 (0.83–1.02) | 0.125 |
| 6 months | 202 | 5 | 1.0 (0.99–1.02) | 0.643 | 1.02 (0.91–1.13) | 0.788 |
| 9 months | 198 | 9 | 1.01 (1.0–1.02) | 0.069 | 1.09 (0.99–1.19) | 0.072 |
| 12 months | 192 | 9 | 1.01 (1.0–1.02) | 0.181 | 1.08 (0.96–1.21) | 0.184 |
| 18 months | 146 | 21 | 1.0 (0.98–1.02) | 0.983 | 1.01 (0.84–1.21) | 0.923 |
| 24 months | 103 | 19 | 0.99 (0.97–1.01) | 0.202 | 0.88 (0.69–1.12) | 0.301 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hård af Segerstad, E.M.; Lee, H.-S.; Andrén Aronsson, C.; Yang, J.; Uusitalo, U.; Sjöholm, I.; Rayner, M.; Kurppa, K.; Virtanen, S.M.; Norris, J.M.; et al. Daily Intake of Milk Powder and Risk of Celiac Disease in Early Childhood: A Nested Case-Control Study. Nutrients 2018, 10, 550. https://doi.org/10.3390/nu10050550
Hård af Segerstad EM, Lee H-S, Andrén Aronsson C, Yang J, Uusitalo U, Sjöholm I, Rayner M, Kurppa K, Virtanen SM, Norris JM, et al. Daily Intake of Milk Powder and Risk of Celiac Disease in Early Childhood: A Nested Case-Control Study. Nutrients. 2018; 10(5):550. https://doi.org/10.3390/nu10050550
Chicago/Turabian StyleHård af Segerstad, Elin M., Hye-Seung Lee, Carin Andrén Aronsson, Jimin Yang, Ulla Uusitalo, Ingegerd Sjöholm, Marilyn Rayner, Kalle Kurppa, Suvi M. Virtanen, Jill M. Norris, and et al. 2018. "Daily Intake of Milk Powder and Risk of Celiac Disease in Early Childhood: A Nested Case-Control Study" Nutrients 10, no. 5: 550. https://doi.org/10.3390/nu10050550
APA StyleHård af Segerstad, E. M., Lee, H.-S., Andrén Aronsson, C., Yang, J., Uusitalo, U., Sjöholm, I., Rayner, M., Kurppa, K., Virtanen, S. M., Norris, J. M., Agardh, D., & On behalf of the TEDDY Study Group. (2018). Daily Intake of Milk Powder and Risk of Celiac Disease in Early Childhood: A Nested Case-Control Study. Nutrients, 10(5), 550. https://doi.org/10.3390/nu10050550





