Exercise Preferences in Young Adults with Cancer—The YOUEX Study
Abstract
1. Introduction
2. Materials and Methods
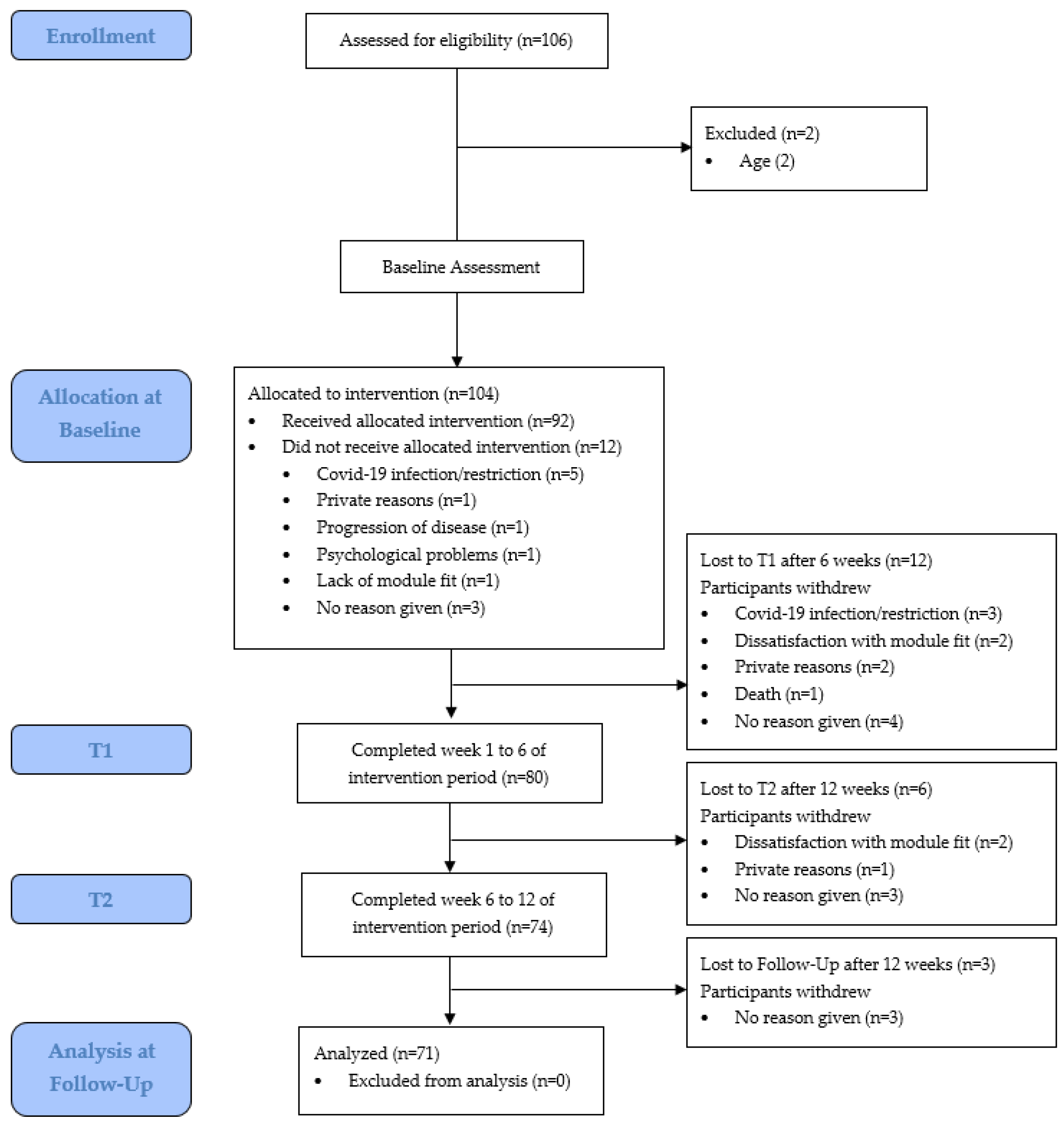
2.1. Study Design
2.2. Participants and Recruitment
2.3. YOUEX Exercise Intervention Modules
- Module 1 (M1): supervised, group-based, online exercise program once a week
- Module 2 (M2): unsupervised, individual home-based training with an online-training app at least once per week
- Module 3 (M3): participation in a supervised, in-person exercise program close to place of residence at least once per week
2.4. Outcomes and Study Instruments
2.4.1. Physical Activity
2.4.2. Module Selection and Exercise Preferences
2.4.3. Impact of the COVID-19 Pandemic
2.5. Statistical Analysis
2.6. Qualitative Analysis
3. Results
3.1. Patient Characteristics
3.2. Physical Activity
3.3. Module Selection and Exercise Preferences
3.3.1. Initial Module Selection at T0
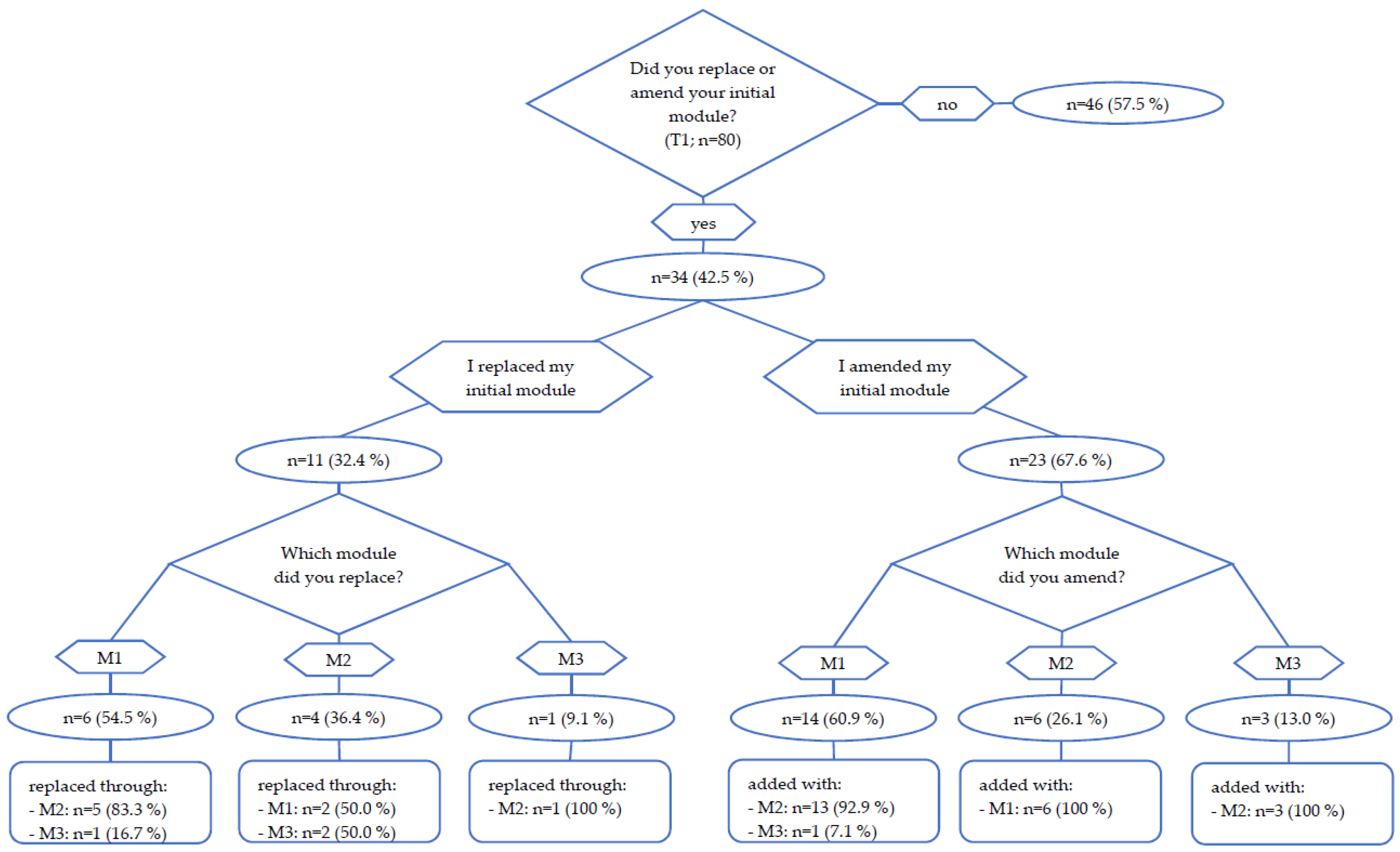
3.3.2. Module Change at T1
3.3.3. Subgroup Analysis of Patient Characteristics According to Module Selection at T0
3.4. Impact of COVID-19 Pandemic
4. Discussion
4.1. Physical Activity
4.2. Module Selection and Exercise Preferences
4.3. Implementation of the YOUEX Exercise Programs and the Impact of COVID-19
4.4. Limitations
4.5. Further Research
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Brandenbarg, D.; Korsten, J.H.W.M.; Berger, M.Y.; Berendsen, A.J. The effect of physical activity on fatigue among survivors of colorectal cancer: A systematic review and meta-analysis. Support. Care Cancer 2018, 26, 393–403. [Google Scholar] [CrossRef] [PubMed]
- Wagoner, C.W.; Lee, J.T.; Battaglini, C.L. Community-based exercise programs and cancer-related fatigue: A systematic review and meta-analysis. Support. Care Cancer 2021, 29, 4921–4929. [Google Scholar] [CrossRef]
- Gebruers, n.; Camberlin, M.; Theunissen, F.; Tjalma, W.; Verbelen, H.; Van Soom, T.; van Breda, E. The effect of training interventions on physical performance, quality of life, and fatigue in patients receiving breast cancer treatment: A systematic review. Support. Care Cancer 2019, 27, 109–122. [Google Scholar] [CrossRef] [PubMed]
- Buffart, L.M.; Sweegers, M.G.; May, A.M.; Chinapaw, M.J.; van Vulpen, J.K.; Newton, R.U.; Galvão, D.A.; Aaronson, N.K.; Stuiver, M.M.; Jacobsen, P.B.; et al. Targeting exercise interventions to patients with cancer in need: An individual patient data meta-analysis. J. Natl. Cancer Inst. 2018, 110, 1190–1200. [Google Scholar] [CrossRef]
- Müller, J.; Weiler, M.; Schneeweiss, A.; Haag, G.M.; Steindorf, K.; Wick, W.; Wiskemann, J. Preventive effect of sensorimotor exercise and resistance training on chemotherapy-induced peripheral neuropathy: A randomised-controlled trial. Br. J. Cancer 2021, 125, 955–965. [Google Scholar] [CrossRef]
- Kleckner, I.R.; Kamen, C.; Gewandter, J.S.; Mohile, n.A.; Heckler, C.E.; Culakova, E.; Fung, C.; Janelsins, M.C.; Asare, M.; Lin, P.J.; et al. Effects of exercise during chemotherapy on chemotherapy-induced peripheral neuropathy: A multicenter, randomized controlled trial. Support. Care Cancer 2018, 26, 1019–1028. [Google Scholar] [CrossRef]
- Zimmer, P.; Trebing, S.; Timmers-Trebing, U.; Schenk, A.; Paust, R.; Bloch, W.; Rudolph, R.; Streckmann, F.; Baumann, F.T. Eight-week, multimodal exercise counteracts a progress of chemotherapy-induced peripheral neuropathy and improves balance and strength in metastasized colorectal cancer patients: A randomized controlled trial. Support. Care Cancer 2018, 26, 615–624. [Google Scholar] [CrossRef]
- Zhang, X.; Brown, J.C.; Paskett, E.D.; Zemel, B.S.; Cheville, A.L.; Schmitz, K.H. Changes in arm tissue composition with slowly progressive weight-lifting among women with breast cancer-related lymphedema. Breast Cancer Res. Treat. 2017, 164, 79–88. [Google Scholar] [CrossRef] [PubMed]
- Rogan, S.; Taeymans, J.; Luginbuehl, H.; Aebi, M.; Mahnig, S.; Gebruers, N. Therapy modalities to reduce lymphoedema in female breast cancer patients: A systematic review and meta-analysis. Breast Cancer Res. Treat. 2016, 159, 1–14. [Google Scholar] [CrossRef]
- Zhang, X.; Li, Y.; Liu, D. Effects of exercise on the quality of life in breast cancer patients: A systematic review of randomized controlled trials. Support. Care Cancer 2019, 27, 9–21. [Google Scholar] [CrossRef]
- Sweegers, M.G.; Altenburg, T.M.; Chinapaw, M.J.; Kalter, J.; Verdonck-de Leeuw, I.M.; Courneya, K.S.; Newton, R.U.; Aaronson, N.K.; Jacobsen, P.B.; Brug, J.; et al. Which exercise prescriptions improve quality of life and physical function in patients with cancer during and following treatment? A systematic review and meta-analysis of randomised controlled trials. Br. J. Sports Med. 2018, 52, 505–513. [Google Scholar] [CrossRef]
- Buffart, L.M.; Kalter, J.; Sweegers, M.G.; Courneya, K.S.; Newton, R.U.; Aaronson, n.K.; Jacobsen, P.B.; May, A.M.; Galvao, D.A.; Chinapaw, M.J.; et al. Effects and moderators of exercise on quality of life and physical function in patients with cancer: An individual patient data meta-analysis of 34 RCTs. Cancer Treat. Rev. 2017, 52, 91–104. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.; Morielli, A.R.; Heer, E.; Kirkham, A.A.; Cheung, W.Y.; Usmani, N.; Friedenreich, C.M.; Courneya, K.S. Effects of exercise on cancer treatment efficacy: A systematic review of preclinical and clinical studies. Cancer Res. 2021, 81, 4889–4895. [Google Scholar] [CrossRef] [PubMed]
- Friedenreich, C.M.; Stone, C.R.; Cheung, W.Y.; Hayes, S.C. Physical activity and mortality in cancer survivors: A systematic review and meta-analysis. JNCI Cancer Spectr. 2019, 4, pkz080. [Google Scholar] [CrossRef]
- Patel, A.V.; Friedenreich, C.M.; Moore, S.C.; Hayes, S.C.; Silver, J.K.; Campbell, K.L.; Winters-Stone, K.; Gerber, L.H.; George, S.M.; Fulton, J.E.; et al. American College of Sports Medicine Roundtable Report on Physical Activity, Sedentary Behavior, and Cancer Prevention and Control. Med. Sci. Sports Exerc. 2019, 51, 2391–2402. [Google Scholar] [CrossRef] [PubMed]
- Campbell, K.L.; Winters-Stone, K.M.; Wiskemann, J.; May, A.M.; Schwartz, A.L.; Courneya, K.S.; Zucker, D.S.; Matthews, C.E.; Ligibel, J.A.; Gerber, L.H.; et al. Exercise Guidelines for Cancer Survivors: Consensus Statement from International Multidisciplinary Roundtable. Med. Sci. Sports Exerc. 2019, 51, 2375–2390. [Google Scholar] [CrossRef]
- Bull, F.C.; Al-Ansari, S.S.; Biddle, S.; Borodulin, K.; Buman, M.P.; Cardon, G.; Carty, C.; Chaput, J.P.; Chastin, S.; Chou, R.; et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 2020, 54, 1451–1462. [Google Scholar] [CrossRef]
- Lewis, D.R.; Siembida, E.J.; Seibel, n.L.; Smith, A.W.; Mariotto, A.B. Survival outcomes for cancer types with the highest death rates for adolescents and young adults, 1975–2016. Cancer 2021, 127, 4277–4286. [Google Scholar] [CrossRef]
- Pugh, G.; Below, N.; Fisher, A.; Reynolds, J.; Epstone, S. Trekstock RENEW: Evaluation of a 12-week exercise referral programme for young adult cancer survivors delivered by a cancer charity. Support. Care Cancer 2020, 28, 5803–5812. [Google Scholar] [CrossRef]
- Munsie, C.; Ebert, J.; Joske, D.; Ackland, T. The benefit of physical activity in adolescent and young adult cancer patients during and after treatment: A systematic review. J. Adolesc. Young Adult. Oncol. 2019, 8, 512–524. [Google Scholar] [CrossRef]
- Desandes, E.; Stark, D.P. Epidemiology of adolescents and young adults with cancer in Europe. Tumors Adolesc. Young Adults 2016, 43, 1–15. [Google Scholar] [CrossRef]
- Barr, R.D.; Ferrari, A.; Ries, L.; Whelan, J.; Bleyer, W.A. Cancer in adolescents and young adults: A narrative review of the current status and a view of the future. JAMA Pediatr. 2016, 170, 495–501. [Google Scholar] [CrossRef] [PubMed]
- Coccia, P.F.; Pappo, A.S.; Beaupin, L.; Borges, V.F.; Borinstein, S.C.; Chugh, R.; Dinner, S.; Folbrecht, J.; Frazier, A.L.; Goldsby, R.; et al. Adolescent and young adult oncology, version 2. 2018, NCCN clinical practice guidelines in oncology. J. Natl. Compr. Cancer Netw. 2018, 16, 66–97. [Google Scholar] [CrossRef]
- Beulertz, J.; Prokop, A.; Rustler, V.; Bloch, W.; Felsch, M.; Baumann, F.T. Effects of a 6-month, group-based, therapeutic exercise program for childhood cancer outpatients on motor performance, level of activity, and quality of life. Pediatr. Blood Cancer 2016, 63, 127–132. [Google Scholar] [CrossRef]
- Braam, K.I.; van der Torre, P.; Takken, T.; Veening, M.A.; van Dulmen-den Broeder, E.; Kaspers, G.J. Physical exercise training interventions for children and young adults during and after treatment for childhood cancer. Cochrane Database Syst. Rev. 2013, 4, Cd008796. [Google Scholar] [CrossRef]
- Le, A.; Mitchell, H.R.; Zheng, D.J.; Rotatori, J.; Fahey, J.T.; Ness, K.K.; Kadan-Lottick, N.S. A home-based physical activity intervention using activity trackers in survivors of childhood cancer: A pilot study. Pediatr. Blood Cancer 2017, 64, 387–394. [Google Scholar] [CrossRef]
- Morales, J.S.; Valenzuela, P.L.; Herrera-Olivares, A.M.; Baño-Rodrigo, A.; Castillo-García, A.; Rincón-Castanedo, C.; Martín-Ruiz, A.; San-Juan, A.F.; Fiuza-Luces, C.; Lucia, A. Exercise interventions and cardiovascular health in childhood cancer: A meta-analysis. Int. J. Sports Med. 2020, 41, 141–153. [Google Scholar] [CrossRef]
- Morales, J.S.; Valenzuela, P.L.; Rincón-Castanedo, C.; Takken, T.; Fiuza-Luces, C.; Santos-Lozano, A.; Lucia, A. Exercise training in childhood cancer: A systematic review and meta-analysis of randomized controlled trials. Cancer Treat. Rev. 2018, 70, 154–167. [Google Scholar] [CrossRef]
- Shi, Q.; Zheng, J.; Liu, K. Supervised exercise interventions in childhood cancer survivors: A systematic review and meta-analysis of randomized controlled trials. Children 2022, 9, 824. [Google Scholar] [CrossRef]
- Neuer Themenbereich “Bewegung & Sport bei Krebs” im JUNGEN KREBSPORTAL Online. Available online: https://junge-erwachsene-mit-krebs.de/neuer-themenbereich-bewegung-sport-bei-krebs-im-jungen-krebsportal-online/ (accessed on 8 August 2022).
- Adams, S.C.; Petrella, A.; Sabiston, C.M.; Vani, M.F.; Gupta, A.; Trinh, L.; Matthew, A.G.; Hamilton, R.J.; Mina, D.S. Preferences for exercise and physical activity support in adolescent and young adult cancer survivors: A cross-sectional survey. Support. Care Cancer 2021, 29, 4113–4127. [Google Scholar] [CrossRef]
- Godin, G.; Shephard, R.J. A simple method to assess exercise behavior in the community. Can. J. Appl. Sport Sci. 1985, 10, 141–146. [Google Scholar] [PubMed]
- Bender, R.; Lange, S. Adjusting for multiple testing—When and how? J. Clin. Epidemiol. 2001, 54, 343–349. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Erlbaum Associates: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Kuckartz, U. Einführung in Die Computergestützte Analyse Qualitativer Daten, 3rd ed.; Verlag für Sozialwissenschaften: Wiesbaden, Germany, 2010. [Google Scholar]
- Mehnert, A.; Müller, D.; Lehmann, C.; Koch, U. Die deutsche Version des NCCN Distress-Thermometers. Z. Psychiatr. Psychol. Und Psychother. 2006, 54, 213–223. [Google Scholar] [CrossRef]
- Stössel, S.; Neu, M.A.; Oschwald, V.; Söntgerath, R.; Däggelmann, J.; Eckert, K.; Hamacher, V.; Baumann, F.T.; Bloch, W.; Faber, J. Physical activity behaviour in children and adolescents before, during and after cancer treatment. Sport Sci. Health 2020, 16, 347–353. [Google Scholar] [CrossRef]
- Christensen, J.F.; Simonsen, C.; Hojman, P. Exercise training in cancer control and treatment. Compr. Physiol. 2018, 9, 165–205. [Google Scholar] [CrossRef] [PubMed]
- Voland, A.; Köppel, M.; Wiskemann, J. Evaluation des Netzwerk OnkoAktiv aus Patientenperspektive. B&G Beweg. Gesundh. 2022, 38, 103–109. [Google Scholar]
- Sweegers, M.G.; Buffart, L.M.; van Veldhuizen, W.M.; Geleijn, E.; Verheul, H.M.W.; Brug, J.; Chinapaw, M.J.M.; Altenburg, T.M. How does a supervised exercise program improve quality of life in patients with cancer? A concept mapping study examining patients’ perspectives. Oncologist 2019, 24, e374–e383. [Google Scholar] [CrossRef] [PubMed]
- Saultier, P.; Vallet, C.; Sotteau, F.; Hamidou, Z.; Gentet, J.C.; Barlogis, V.; Curtillet, C.; Verschuur, A.; Revon-Riviere, G.; Galambrun, C.; et al. A randomized trial of physical activity in children and adolescents with cancer. Cancers 2021, 13, 121. [Google Scholar] [CrossRef]
- Beller, R.; Bennstein, S.B.; Götte, M. Effects of exercise interventions on immune function in children and adolescents with cancer and HSCT recipients—A systematic review. Front. Immunol. 2021, 12, 746171. [Google Scholar] [CrossRef]
- Devine, K.A.; Viola, A.; Levonyan-Radloff, K.; Mackowski, n.; Bozzini, B.; Chandler, A.; Xu, B.; Ohman-Strickland, P.; Mayans, S.; Farrar-Anton, A.; et al. Feasibility of FitSurvivor: A technology-enhanced group-based fitness intervention for adolescent and young adult survivors of childhood cancer. Pediatr. Blood Cancer 2020, 67, e28530. [Google Scholar] [CrossRef]
- McKeon, G.; Papadopoulos, E.; Firth, J.; Joshi, R.; Teasdale, S.; Newby, J.; Rosenbaum, S. Social media interventions targeting exercise and diet behaviours in people with noncommunicable diseases (NCDs): A systematic review. Internet Interv. 2022, 27, 100497. [Google Scholar] [CrossRef]
- Gondos, A.; Hiripi, E.; Holleczek, B.; Luttmann, S.; Eberle, A.; Brenner, H. Survival among adolescents and young adults with cancer in Germany and the United States: An international comparison. Int. J. Cancer 2013, 133, 2207–2215. [Google Scholar] [CrossRef] [PubMed]
- Devine, K.A.; Viola, A.S.; Coups, E.J.; Wu, Y.P. Digital health interventions for adolescent and young adult cancer survivors. JCO Clin. Cancer Inform. 2018, 2, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, J.A.; Baker, K.S.; Moreno, M.A.; Whitlock, K.; Abbey-Lambertz, M.; Waite, A.; Colburn, T.; Chow, E.J. A Fitbit and Facebook mHealth intervention for promoting physical activity among adolescent and young adult childhood cancer survivors: A pilot study. Pediatr. Blood Cancer 2017, 64, e26660. [Google Scholar] [CrossRef] [PubMed]
- Götte, M.; Seidel, C.C.; Kesting, S.V.; Rosenbaum, D.; Boos, J. Objectively measured versus self-reported physical activity in children and adolescents with cancer. PLoS ONE 2017, 12, e0172216. [Google Scholar] [CrossRef] [PubMed]

| Characteristics | n (%) | Mean ± SD | Median | Range |
|---|---|---|---|---|
| Age (years) | 92 | 31.9 ± 4.9 | 32.5 | 19–39 |
| Gender | ||||
| Female | 86 (93.5) | |||
| Male | 6 (6.5) | |||
| Body composition | ||||
| Height (cm) | 92 | 169.9 ± 7.1 | 170.0 | 146–190 |
| Weight (kg) | 92 | 68.2 ± 11.5 | 66.5 | 48–102 |
| BMI (kg/m2) | 92 | 23.6 ± 3.8 | 23.3 | 17.5–35.7 |
| Disease | ||||
| Breast cancer | 51 (55.4) | |||
| (Non-)Hodgkin lymphoma | 17 (18.5) | |||
| Sarcoma | 4 (4.3) | |||
| Leukemia | 3 (3.3) | |||
| Brain tumor | 3 (3.3) | |||
| Other | 14 (15.2) | |||
| Disease progression | ||||
| Metastasis | 17 (18.5) | |||
| Relapse | 13 (14.1) | |||
| Treatment | ||||
| Surgery | 68 (73.9) | |||
| Chemotherapy | ||||
| Total | 84 (91.3) | |||
| Ongoing | 18 (19.6) | |||
| Radiotherapy | ||||
| Total | 49 (53.3) | |||
| Ongoing | 1 (1.1) | |||
| Immunotherapy | ||||
| Total | 10 (10.9) | |||
| Ongoing | 5 (5.4) | |||
| Hormone therapy | ||||
| Total | 35 (38.0) | |||
| Ongoing | 26 (28.3) | |||
| Other therapy | ||||
| Total | 22 (23.9) | |||
| Antibody | 15 (16.3) | |||
| Stem cell transplantation | 5 (5.4) | |||
| Other | 2 (2.2) | |||
| Education | ||||
| Middle school | 2 (2.2) | |||
| Vocational training | 9 (9.8) | |||
| University entrance qualification | 24 (26.1) | |||
| University degree | 54 (58.7) | |||
| Other degree | 3 (3.3) | |||
| Employment | ||||
| Employed, currently working | 36 (39.1) | |||
| Employed but on medical leave | 35 (38.0) | |||
| Still in education | 17 (18.5) | |||
| Housewife/houseman | 1 (1.1) | |||
| Retired | 2 (2.2) | |||
| Unemployed | 1 (1.1) | |||
| Family situation | ||||
| Married/permanent relationship | 57 (62.0) | |||
| Single | 32 (34.8) | |||
| Divorced | 2 (2.2) | |||
| Smoking behavior | ||||
| Smoker | 0 (0) | |||
| Non-smoker | 92 (100) | |||
| Social media usage behavior | ||||
| Smartphone/tablet (h/week) | 90 | 12.5 ± 8.5 | 10.7 | 1–42 |
| PC (h/week) | 91 | 11.8 ± 15.1 | 4 | 0–60 |
| Frequency of social media use (h/week) | ||||
| 91 | 3.4 ± 1.0 | 4 | 1–4 | |
| 91 | 2.6 ± 1.2 | 3 | 1–4 | |
| YouTube | 91 | 2.3 ± 0.8 | 2 | 1–4 |
| 91 | 1.2 ± 0.5 | 1 | 1–4 | |
| Tik Tok | 91 | 1.1 ± 0.4 | 1 | 1–4 |
| Twitch | 91 | 1.1 ± 0.3 | 1 | 1–4 |
| NCCN Distress 1 | 91 | 6.18 ± 2.1 | 6 | 1–10 |
| Pre-Diagnosis | Post-Diagnosis | T1 | T2 | p Value | |||||
|---|---|---|---|---|---|---|---|---|---|
| n | M ± SD | n | M ± SD | n | M ± SD | n | M ± SD | ||
| Light PA (min/week) | 69 | 154.8 ± 142.7 | 69 | 194.1 ± 176.2 | 69 | 205.9 ± 203.1 | 69 | 206.2 ± 236.4 | 0.270 |
| Moderate PA (min/week) | 70 | 83.4 ± 81.4 | 70 | 76.1 ± 95.4 | 70 | 119.4 ± 116.2 *,# | 70 | 116.8 ± 94.8 * | <0.001 |
| Vigorous PA (min/week) | 69 | 86.1 ± 94.5 | 69 | 46.9 ± 71.7 # | 69 | 68.3 ± 77.5 | 69 | 69.4 ± 65.6 * | <0.001 |
| Total PA (min/week) | 66 | 325.8 ± 210.9 | 66 | 322.0 ± 245.7 | 66 | 397.1 ± 256.3 * | 66 | 399.9 ± 315.7 * | <0.001 |
| M1 (n = 32) | M2 (n = 50) | M3 (n = 10) | ||||
|---|---|---|---|---|---|---|
| n | % | n | % | n | % | |
| Treatment status * | ||||||
| During acute therapy | 7 | 21.9 | 6 | 12.0 | 5 | 50.0 |
| Before or after acute therapy | 25 | 78.1 | 44 | 88.0 | 5 | 50.0 |
| Employment | ||||||
| Employed | 14 | 43.8 | 19 | 38.0 | 3 | 30.0 |
| On medical leave | 14 | 43.8 | 17 | 34.0 | 4 | 40.0 |
| Still in education | 4 | 12.5 | 12 | 24.0 | 1 | 10.0 |
| Not employed | 0 | 0.0 | 2 | 4.0 | 2 | 20.0 |
| n (%) | Mean ± SD | Median | Range | Percentile | ||
|---|---|---|---|---|---|---|
| 25 | 75 | |||||
| M1 | 68 (73.9) | 5.1 ± 2.6 | 5.0 | 1 to 10 | 3.0 | 7.0 |
| M2 | 68 (73.9) | 7.2 ± 2.8 | 7.5 | 1 to 10 | 5.0 | 9.5 |
| M3 | 68 (73.9) | 8.4 ± 2.1 | 9.5 | 1 to 10 | 7.0 | 10.0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Voland, A.; Krell, V.; Götte, M.; Niels, T.; Köppel, M.; Wiskemann, J. Exercise Preferences in Young Adults with Cancer—The YOUEX Study. Curr. Oncol. 2023, 30, 1473-1487. https://doi.org/10.3390/curroncol30020113
Voland A, Krell V, Götte M, Niels T, Köppel M, Wiskemann J. Exercise Preferences in Young Adults with Cancer—The YOUEX Study. Current Oncology. 2023; 30(2):1473-1487. https://doi.org/10.3390/curroncol30020113
Chicago/Turabian StyleVoland, Annelie, Verena Krell, Miriam Götte, Timo Niels, Maximilian Köppel, and Joachim Wiskemann. 2023. "Exercise Preferences in Young Adults with Cancer—The YOUEX Study" Current Oncology 30, no. 2: 1473-1487. https://doi.org/10.3390/curroncol30020113
APA StyleVoland, A., Krell, V., Götte, M., Niels, T., Köppel, M., & Wiskemann, J. (2023). Exercise Preferences in Young Adults with Cancer—The YOUEX Study. Current Oncology, 30(2), 1473-1487. https://doi.org/10.3390/curroncol30020113






