Fall Prediction and Prevention Systems: Recent Trends, Challenges, and Future Research Directions
Abstract
1. Introduction
- Fall detection systems alert the user and healthcare provider after a fall has occurred to expedite and improve the medical care provided. These systems are aimed at identifying different kinds of falls: falls from walking or standing, falls from standing on supports, e.g., ladders etc., falls from sleeping or lying in the bed and falls from sitting on a chair. These systems often use threshold-based algorithms to detect falls. The performance metrics of fall detection systems include precision (true positive rate), specificity (true negative rate), and false positive rate.
- Fall prediction systems are aimed at alerting the subjects before the occurrence of a fall thus preventing the emotional and health consequences of a fall. These systems should identify all scenarios and circumstances leading to a fall and provide a framework to predict them. This framework must be constructed based on data acquired from various scenarios surrounding fall-related events. Information on fall-related events is usually collected through questionnaires, fall diaries, and phone calls. This information is often augmented with data collected from various sensors to improve reliability and accuracy.
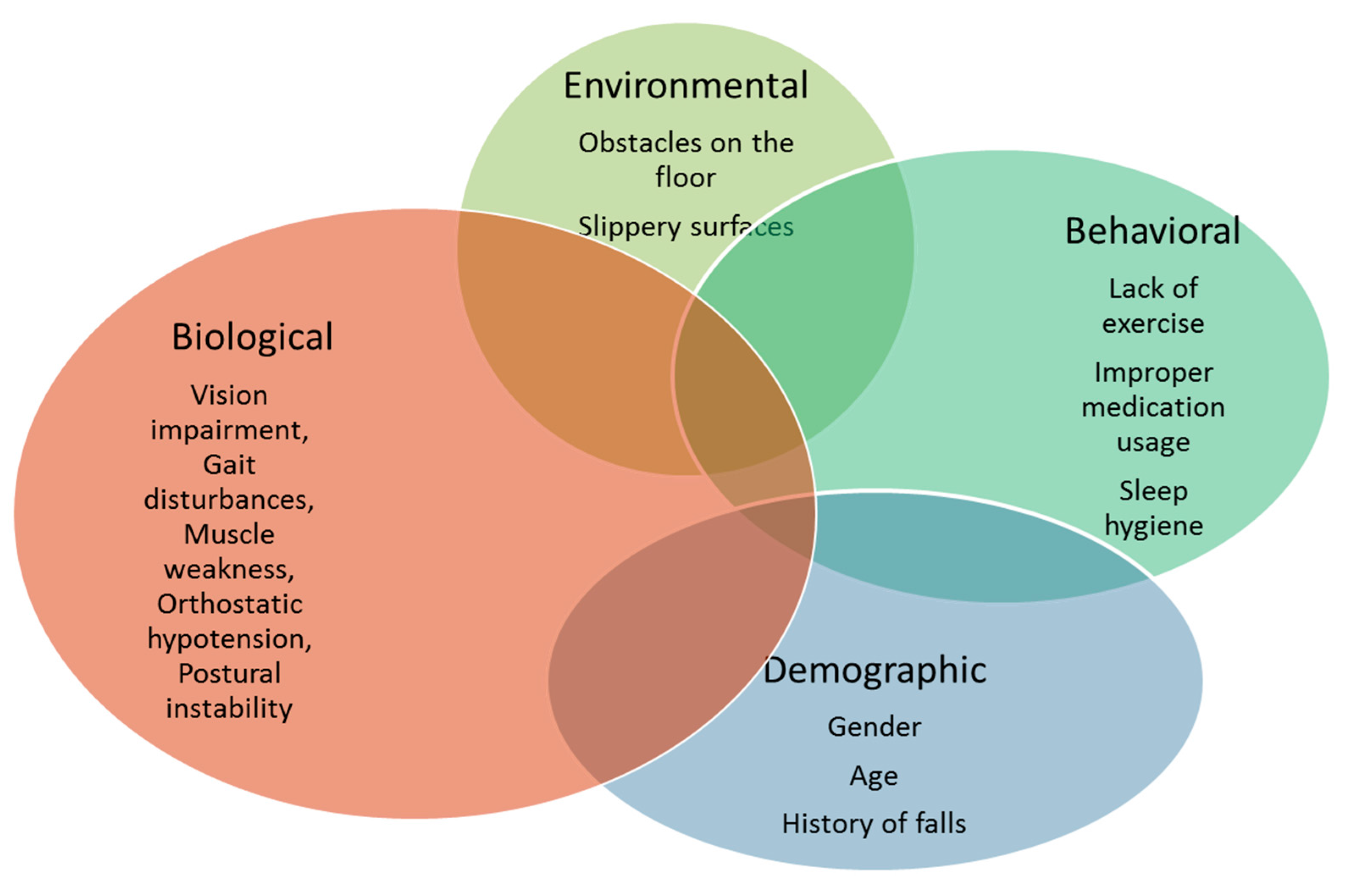
- Fall prediction systems must capture the multifactorial nature of falls for reliable fall risk estimation. These include environmental, physiological, and psychological risk factors. Fall detection systems mainly focus on physiological risk factors such as gait, mobility, and vision.
- Fall detection systems usually focus on developing a fall detection device using wearable sensors that can be integrated into watches, shoes, belts, etc. Fall prediction systems focus on information fusion from both wearable and ambient sensors for reliable estimation of fall risk. These systems also include the design and evaluation of user interfaces such as smartphone applications for fall prevention intervention and educating subjects on fall risk factors.
2. Current Work and Limitations
2.1. Wearable Fall Detection and Prediction Systems
2.2. Ambient Sensors for Fall Detection and Prediction
- Lack of a comprehensive fall prediction system. Existing systems do not address information fusion that captures contextual and physiological data from wearable and ambient sensors for fall risk estimation.
- Dearth of user-friendly interfaces and feedback techniques to actively engage and empower patients towards effective techniques to prevent falls.
- No efficient web interfaces to help clinicians visualize health data and assess fall risk.
3. Fall Prevention Systems
3.1. Current Work
3.2. Fall Prevention Intervention
4. Challenges
4.1. Performance in Real-Life Conditions
4.2. User-Centric Design
4.3. Security and Privacy
4.4. Energy Optimization
5. Recommendations and Future Work
5.1. Information Fusion and Machine Learning
5.2. User Interfaces for Providing Feedback to Clinicians and Patients
5.3. Smart Phone Based Fall Detection and Prediction
5.4. Environmental Fall Risk Factors
5.5. Comparison of IoT-Enabled Systems with Clinical Systems
5.6. Biomedical Signal Based Fall Prediction
5.7. Accuracy of Fall Prediction
6. Conclusions
Conflicts of Interest
References
- Burns, E.R.; Stevens, J.A.; Lee, R. The direct costs of fatal and non-fatal falls among older adults—United States. J. Saf. Res. 2016, 58, 99–103. [Google Scholar] [CrossRef] [PubMed]
- Scheffer, A.C.; Schuurmans, M.J.; Van Dijk, N.; Van Der Hooft, T.; De Rooij, S.E. Fear of falling: Measurement strategy, prevalence, risk factors and consequences among older persons. Age Ageing 2008, 37, 19–24. [Google Scholar] [CrossRef] [PubMed]
- Brownsell, S.; Hawley, M.S. Automatic fall detectors and the fear of falling. J. Telemed. Telecare 2004, 10, 262–266. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, C.J.; Chiang, C.Y.; Huang, C.N.; Chan, C.T.; Hsu, S.J. Development of fall characteristics collection system for fall prevention strategies. In Proceedings of the 5th International Conference on Bioinformatics and Biomedical Engineering, Wuhan, China, 10–12 May 2011; pp. 1–4. [Google Scholar]
- Igual, R.; Medrano, C.; Plaza, I. Challenges, issues and trends in fall detection systems. Biomed. Eng. Online 2013, 12, 66. [Google Scholar] [CrossRef] [PubMed]
- Delahoz, Y.S.; Labrador, M.A. Survey on fall detection and fall prevention using wearable and external sensors. Sensors 2014, 14, 19806–19842. [Google Scholar] [CrossRef] [PubMed]
- Weiss, A.; Brozgol, M.; Dorfman, M.; Herman, T.; Shema, S.; Giladi, N.; Hausdorff, J.M. Does the evaluation of gait quality during daily life provide insight into fall risk? A novel approach using 3-day accelerometer recordings. Neurorehabilit. Neural Repair 2013, 27, 742–752. [Google Scholar] [CrossRef] [PubMed]
- Pannurat, N.; Thiemjarus, S.; Nantajeewarawat, E. Automatic fall monitoring: A review. Sensors 2014, 14, 12900–12936. [Google Scholar] [CrossRef] [PubMed]
- Fortino, G.; Giannantonio, R.; Gravina, R.; Kuryloski, P.; Jafari, R. Enabling effective programming and flexible management of efficient body sensor network applications. IEEE Trans. Hum.-Mach. Syst. 2013, 43, 115–133. [Google Scholar] [CrossRef]
- Chen, M.; Gonzalez, S.; Vasilakos, A.; Cao, H.; Leung, V.C. Body area networks: A survey. Mobile Netw. Appl. 2011, 16, 171–193. [Google Scholar] [CrossRef]
- Tao, W.; Liu, T.; Zheng, R.; Feng, H. Gait analysis using wearable sensors. Sensors 2012, 12, 2255–2283. [Google Scholar] [CrossRef] [PubMed]
- Doheny, E.P.; Walsh, C.; Foran, T.; Greene, B.R.; Fan, C.W.; Cunningham, C.; Kenny, R.A. Falls classification using tri-axial accelerometers during the five-times-sit-to-stand test. Gait Posture 2013, 38, 1021–1025. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.; Park, H.; Bonato, P.; Chan, L.; Rodgers, M. A review of wearable sensors and systems with application in rehabilitation. J. Neuroeng. Rehabil. 2012, 9, 21. [Google Scholar] [CrossRef] [PubMed]
- Wang, K.; Redmond, S.J.; Lovell, N.H. Monitoring for Elderly Care: The Role of Wearable Sensors in Fall Detection and Fall Prediction Research. In Telemedicine and Electronic Medicine 2015; Eren, H., Webster, J.G., Eds.; CRC Press: Boca Raton, FL, USA, 2015; pp. 619–652. [Google Scholar]
- Lara, O.D.; Labrador, M.A. A survey on human activity recognition using wearable sensors. IEEE Commun. Surv. Tutor. 2013, 15, 1192–1209. [Google Scholar] [CrossRef]
- Howcroft, J.; Kofman, J.; Lemaire, E.D. Review of fall risk assessment in geriatric populations using inertial sensors. J. Neuroeng. Rehabil. 2013, 10, 91. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.C.; Huang, C.N.; Chiang, C.Y.; Hsieh, C.J.; Chan, C.T. A Reliable Fall Detection System Based on Wearable Sensor and Signal Magnitude Area for Elderly Residents. In Proceedings of the International Conference on Smart Homes and Health Telematics, Ames, IA, USA, 2–28 July 2008; Springer: Berlin/Heidelberg, Germany, 2010; pp. 267–270. [Google Scholar]
- Bourke, A.K.; Van de Ven, P.; Gamble, M.; O’Connor, R.; Murphy, K.; Bogan, E.; Nelson, J. Evaluation of waist-mounted tri-axial accelerometer based fall-detection algorithms during scripted and continuous unscripted activities. J. Biomech. 2010, 43, 3051–3057. [Google Scholar] [CrossRef] [PubMed]
- Bianchi, F.; Redmond, S.J.; Narayanan, M.R.; Cerutti, S.; Lovell, N.H. Barometric pressure and triaxial accelerometry-based falls event detection. IEEE Trans. Neural Syst. Rehabil. Eng. 2010, 18, 619–627. [Google Scholar] [CrossRef] [PubMed]
- Mathie, M.J.; Coster, A.C.; Lovell, N.H.; Celler, B.G.; Lord, S.R.; Tiedemann, A. A pilot study of long-term monitoring of human movements in the home using accelerometry. J. Telemed. Telecare 2004, 10, 144–151. [Google Scholar] [CrossRef] [PubMed]
- Howcroft, J.; Kofman, J.; Lemaire, E. Prospective fall-risk prediction models for older adults based on wearable sensors. IEEE Trans. Neural Syst. Rehabil. Eng. 2017. [Google Scholar] [CrossRef] [PubMed]
- Sannino, G.; De Falco, I.; De Pietro, G. Detection of falling events through windowing and automatic extraction of sets of rules: Preliminary results. In Proceedings of the IEEE 14th International Conference on Networking, Sensing and Control, Calabria, Italy, 16–18 May 2017; pp. 661–666. [Google Scholar]
- Fortino, G.; Gravina, R. Fall-MobileGuard: A smart real-time fall detection system. In Proceedings of the 10th EAI International Conference on Body Area Networks, Sydney, Australia, 28–30 September 2015; pp. 44–50. [Google Scholar]
- Rougier, C.; Meunier, J.; St-Arnaud, A.; Rousseau, J. Robust video surveillance for fall detection based on human shape deformation. IEEE Trans. Circuits Syst. Video Technol. 2011, 21, 611–622. [Google Scholar] [CrossRef]
- Ozcan, K.; Mahabalagiri, A.; Velipasalar, S. Automatic Fall Detection and Activity Classification by a Wearable Camera. In Distributed Embedded Smart Cameras; Springer: New York, USA, 2014; pp. 151–172. [Google Scholar]
- Hirata, Y.; Komatsuda, S.; Kosuge, K. Fall prevention control of passive intelligent walker based on human model. In Proceedings of the International Conference on Intelligent Robots and Systems, Nick, France, 22–26 September 2008; pp. 1222–1228. [Google Scholar]
- Bian, Z.P.; Hou, J.; Chau, L.P.; Magnenat-Thalmann, N. Fall detection based on body part tracking using a depth camera. IEEE J. Biomed. Health Inf. 2015, 19, 430–439. [Google Scholar] [CrossRef] [PubMed]
- Hilbe, J.; Schulc, E.; Linder, B.; Them, C. Development and alarm threshold evaluation of a side rail integrated sensor technology for the prevention of falls. Int. J. Med. Inf. 2010, 79, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Pisan, Y.; Marin, J.G.; Navarro, K.F. Improving lives: Using Microsoft Kinect to predict the loss of balance for elderly users under cognitive load. In Proceedings of the 9th Australasian Conference on Interactive Entertainment: Matters of Life and Death, Melbourne, Australia, 30 September–1 October 2013. [Google Scholar]
- Kayama, H.; Okamoto, K.; Nishiguchi, S.; Yamada, M.; Kuroda, T.; Aoyama, T. Effect of a Kinect-based exercise game on improving executive cognitive performance in community-dwelling elderly: Case control study. J. Med. Int. Res. 2014, 16, E61. [Google Scholar] [CrossRef] [PubMed]
- Mion, L.C.; Chandler, A.M.; Waters, T.M.; Dietrich, M.S.; Kessler, L.A.; Miller, S.T.; Shorr, R.I. Is it possible to identify risks for injurious falls in hospitalized patients? Jt. Comm. J. Qual. Patient Saf. 2012, 38, 408–413. [Google Scholar] [CrossRef]
- Najafi, B.; Aminian, K.; Loew, F.; Blanc, Y.; Robert, P.A. Measurement of stand-sit and sit-stand transitions using a miniature gyroscope and its application in fall risk evaluation in the elderly. IEEE Trans. Biomed. Eng. 2002, 49, 843–851. [Google Scholar] [CrossRef] [PubMed]
- Cho, C.Y.; Kamen, G. Detecting balance deficits in frequent fallers using clinical and quantitative evaluation tools. J. Am. Geriatr. Soc. 1998, 46, 426–430. [Google Scholar] [CrossRef] [PubMed]
- Shany, T.; Redmond, S.J.; Narayanan, M.R.; Lovell, N.H. Sensors-based wearable systems for monitoring of human movement and falls. IEEE Sens. J. 2012, 12, 658–670. [Google Scholar] [CrossRef]
- Tong, L.; Song, Q.; Ge, Y.; Liu, M. HMM-based human fall detection and prediction method using tri-axial accelerometer. IEEE Sens. J. 2013, 13, 1849–1856. [Google Scholar] [CrossRef]
- Di, P.; Huang, J.; Sekiyama, K.; Fukuda, T. A novel fall prevention scheme for intelligent cane robot by using a motor driven universal joint. In Proceedings of the IEEE International Symposium on Micro-NanoMechatronics and Human Science, Nagoya, Japan, 6–9 November 2011; pp. 391–396. [Google Scholar]
- Majumder, A.J.A.; Zerin, I.; Uddin, M.; Ahamed, S.I.; Smith, R.O. SmartPrediction: A real-time smartphone-based fall risk prediction and prevention system. In Proceedings of the 2013 Research in Adaptive and Convergent Systems, Montreal, QC, Canada, 1–4 October 2013; pp. 434–439. [Google Scholar]
- Chase, C.A.; Mann, K.; Wasek, S.; Arbesman, M. Systematic review of the effect of home modification and fall prevention programs on falls and the performance of community-dwelling older adults. Am. J. Occup. Ther. 2012, 66, 284–291. [Google Scholar] [CrossRef] [PubMed]
- Pighills, A.C.; Torgerson, D.J.; Sheldon, T.A.; Drummond, A.E.; Bland, J.M. Environmental assessment and modification to prevent falls in older people. J. Am. Geriatr. Soc. 2011, 59, 26–33. [Google Scholar] [CrossRef] [PubMed]
- Molina, K.I.; Ricci, N.A.; de Moraes, S.A.; Perracini, M.R. Virtual reality using games for improving physical functioning in older adults: a systematic review. J. Neuroeng. Rehabilit. 2014, 11, 156. [Google Scholar] [CrossRef] [PubMed]
- Ambrose, A.F.; Paul, G.; Hausdorff, J.M. Risk factors for falls among older adults: A review of the literature. Maturitas. 2013, 75, 51–61. [Google Scholar] [CrossRef] [PubMed]
- Montero-Odasso, M.; Verghese, J.; Beauchet, O.; Hausdorff, J.M. Gait and cognition: A complementary approach to understanding brain function and the risk of falling. J. Am. Geriatr. Soc. 2012, 6, 2127–2136. [Google Scholar] [CrossRef] [PubMed]
- De Morais, W.O.; Wickström, N. A serious computer game to assist Tai Chi training for the elderly. In Proceedings of the 2011 IEEE 1st International Conference on Serious Games and Applications for Health (SeGAH), Braga, Portugal, 16–18 November 2011; pp. 1–8. [Google Scholar]
- Horta, E.T.; Lopes, I.C.; Rodrigues, J.J.; Misra, S. Real time falls prevention and detection with biofeedback monitoring solution for mobile environments. In Proceedings of the IEEE 15th International Conference on e-Health Networking, Applications & Services, Lisbon, Portugal, 9–12 October 2013; pp. 594–600. [Google Scholar]
- Visvanathan, R.; Ranasinghe, D.C.; Torres, R.L.S.; Hill, K. Framework for preventing falls in acute hospitals using passive sensor enabled radio frequency identification technology. In Proceedings of the 2012 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Diego, CA, USA, 28 August–1 September 2012; pp. 5858–5862. [Google Scholar]
- Hamm, J.; Money, A.G.; Atwal, A.; Paraskevopoulos, I. Fall prevention intervention technologies: A conceptual framework and survey of the state of the art. J. Biomed. Inf. 2016, 59, 319–345. [Google Scholar] [CrossRef] [PubMed]
- Shi, Y.; Shi, Y.; Wang, X. Fall detection on mobile phones using features from a five-phase model. In Proceedings of the 9th International Conference on Ubiquitous Intelligence and Computing, Fukuoka, Japan, 4–7 September 2012; pp. 951–956. [Google Scholar]
- Silva, P.A.; Nunes, F.; Vasconcelos, A.; Kerwin, M.; Moutinho, R.; Teixeira, P. Using the smartphone accelerometer to monitor fall risk while playing a game: The design and usability evaluation of dance! Don’t fall. In Proceedings of the International Conference on Augmented Cognition, Las Vegas, NV, USA, 21–26 July 2013; Springer: Berlin/Heidelberg, Germany; pp. 754–763. [Google Scholar]
- Jorgensen, M.G.; Laessoe, U.; Hendriksen, C.; Nielsen, O.B.F.; Aagaard, P. Efficacy of Nintendo Wii training on mechanical leg muscle function and postural balance in community-dwelling older adults: A randomized controlled trial. J. Gerontol. Ser. A Biol. Sci. Med. Sci. 2013, 68, 845–852. [Google Scholar] [CrossRef] [PubMed]
- Geraedts, H.A.; Zijlstra, W.; Zhang, W.; Bulstra, S.; Stevens, M. Adherence to and effectiveness of an individually tailored home-based exercise program for frail older adults, driven by mobility monitoring: Design of a prospective cohort study. BMC Public Health 2014, 14, 570. [Google Scholar] [CrossRef] [PubMed]
- Uzor, S.; Baillie, L.; Skelton, D. Senior designers: Empowering seniors to design enjoyable falls rehabilitation tools. In Proceedings of the SIGCHI Conference on Human Factors in Computing Systems, Austin, TX, USA, 5–10 May 2012. [Google Scholar]
- Williams, M.A.; Soiza, R.L.; Jenkinson, A.M.; Stewart, A. Exercising with Computers in Later Life (EXCELL)-pilot and feasibility study of the acceptability of the Nintendo® WiiFit in community-dwelling fallers. BMC Res. Notes 2010, 3, 238. [Google Scholar] [CrossRef] [PubMed]
- Chao, Y.Y.; Scherer, Y.K.; Wu, Y.W.; Lucke, K.T.; Montgomery, C.A. The feasibility of an intervention combining self-efficacy theory and Wii Fit exergames in assisted living residents: A pilot study. Geriatr. Nurs. 2013, 34, 377–382. [Google Scholar] [CrossRef] [PubMed]
- Almer, S.; Kolbitsch, J.; Oberzaucher, J.; Ebner, M. Assessment test framework for collecting and evaluating fall related data using mobile devices. In Computers Helping People with Special Needs; Springer: Berlin, Germany, 2012; pp. 83–90. [Google Scholar]
- Barelle, C.; Vellidou, E.; Koutsouris, D. The BIOTELEKINESY home care service: A holistic concept to prevent fall among the elderly based on ICT and computer vision. In Proceedings of the 10th IEEE International Conference on Information Technology and Applications in Biomedicine (ITAB), Corfu, Greece, 3–5 November 2010. [Google Scholar]
- Brell, M.; Meyer, J.; Frenken, T.; Hein, A. A mobile robot for self-selected gait velocity assessments in assistive environments: A robotic driven approach to bring assistive technologies into established homes. In Proceedings of the 3rd International Conference on Pervasive Technologies Related to Assistive Environments, Samos, Greece, 23–25 June 2010. [Google Scholar]
- Cuddihy, P.E.; Yardibi, T.; Legenzoff, Z.J.; Liu, L.; Phillips, C.E.; Abbott, C.; Skubic, M. Radar walking speed measurements of seniors in their apartments: Technology for fall prevention. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), San Diego, CA, USA, 28 August–1 September 2012. [Google Scholar]
- Greene, B.R.; McGrath, D.; Foran, T.G.; Doheny, E.P.; Caulfield, B. Body-worn sensor based surrogates of minimum ground clearance in elderly fallers and controls. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Boston, MA, USA, 30 August–3 September 2011. [Google Scholar]
- Majumder, A.J.A.; Rahman, F.; Zerin, I.; Ebel, W., Jr.; Ahamed, S.I. iPrevention: Towards a novel real-time smartphonebased fall prevention system. In Proceedings of the 28th Annual ACM Symposium on Applied Computing, Coimbra, Portugal, 18–22 May 2013. [Google Scholar]
- Staranowicz, A.; Brown, G.R.; Mariottini, G.L. Evaluating the accuracy of a mobile Kinect-based gait-monitoring system for fall prediction. In Proceedings of the 6th International Conference on Pervasive Technologies Related to Assistive Environments, Rhodes, Greece, 29–31 May 2013. [Google Scholar]
- Garcia, J.A.; Pisan, Y.; Tan, C.T.; Navarro, K.F. Assessing the Kinect’s capabilities to perform a time-based clinical test for fall risk assessment in older people. In Entertainment Computing—ICEC 2014; Springer: Berlin, Germany, 2014; pp. 100–107. [Google Scholar]
- Rawashdeh, O.; Sa’deh, W.; Rawashdeh, M.; Qu, G.; Ferrari, M.; Harrison, B.; Maddens, M. Development of a low-cost fall intervention system for hospitalized dementia patients. In Proceedings of the IEEE International Conference on Electro/Information Technology (EIT), Indianapolis, IN, USA, 6–8 May 2012. [Google Scholar]
- Schoene, D.; Lord, S.R.; Verhoef, P.; Smith, S.T. A novel video game-based device for measuring stepping performance and fall risk in older people. Arch. Phys. Med. Rehabil. 2011, 92, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Du, R.; Jagtap, V.; Long, Y.; Onwuka, O.; Padir, T. Robotics enabled in-home environment screening for fall risks. In Proceedings of the 2014 Workshop on Mobile Augmented Reality and Robotic Technology-based Systems, Bretton Woods, NH, USA, 16 June 2014. [Google Scholar]
- Bourke, A.K.; de Ven, V.; Gamble, M.; O’Connor, R.; Murphy, K.; Bogan, E.; McQuade, E.; Finucane, P.; OLaighin, G.; Nelson, J. Assessment of waist-worn tri-axial accelerometer based fall-detection algorithms using continuous unsupervised activities. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Buenos Aires, Argentina, 31 August–4 September 2010; pp. 2782–2785. [Google Scholar]
- Zhang, T.; Wang, J.; Xu, L.; Liu, P. Fall detection by wearable sensor and one-class SVM algorithm. In Lecture Notes in Control and Information Science; Huang, D.S., Li, K., Irwin, G.W., Eds.; Springer: Berlin/Heidelberg, Germany, 2006; Volume 345, pp. 858–863. [Google Scholar]
- Allen, N.E.; Schwarzel, A.K.; Canning, C.G. Recurrent falls in Parkinson’s disease: A systematic review. Parkinson’s Dis. 2013, 2013, 906274. [Google Scholar] [CrossRef] [PubMed]
- Ledger, D.; McCaffrey, D. Inside wearables: How the science of human behavior change offers the secret to long-term engagement. Endeav. Partners 2014, 200, 1–17. [Google Scholar]
- Casilari, E.; Luque, R.; Morón, M.J. Analysis of android device-based solutions for fall detection. Sensors 2015, 15, 17827–17894. [Google Scholar] [CrossRef] [PubMed]
- Sultan, N. Making use of cloud computing for healthcare provision: Opportunities and challenges. Int. J. Inf. Manag. 2014, 34, 177–184. [Google Scholar] [CrossRef]
- Zhou, J.; Cao, Z.; Dong, X.; Vasilakos, A.V. Security and privacy for cloud-based IoT: Challenges. IEEE Commun. Mag. 2017, 55, 26–33. [Google Scholar] [CrossRef]
- Williamson, J.; Liu, Q.; Lu, F.; Mohrman, W.; Li, K.; Dick, R.; Shang, L. Data sensing and analysis: Challenges for wearables. In Proceedings of the IEEE 20th Asia and South Pacific Design Automation Conference, Chiba, Japan, 19–22 January 2015; pp. 136–141. [Google Scholar]
- Botta, A.; De Donato, W.; Persico, V.; Pescapé, A. Integration of cloud computing and internet of things: A survey. Future Gen. Comput. Syst. 2016, 56, 684–700. [Google Scholar] [CrossRef]
- Gravina, R.; Alinia, P.; Ghasemzadeh, H.; Fortino, G. Multi-sensor fusion in body sensor networks: State-of-the-art and research challenges. Inf. Fusion 2017, 35, 68–80. [Google Scholar] [CrossRef]
- Diethe, T.; Twomey, N.; Kull, M.; Flach, P.; Craddock, I. Probabilistic Sensor Fusion for Ambient Assisted Living. arXiv, 2017; arXiv:1702.01209. [Google Scholar]
- Habib, M.A.; Mohktar, M.S.; Kamaruzzaman, S.B.; Lim, K.S.; Pin, T.M.; Ibrahim, F. Smartphone-based solutions for fall detection and prevention: Challenges and open issues. Sensors 2014, 14, 7181–7208. [Google Scholar] [CrossRef] [PubMed]
- Webster, D.; Celik, O. Systematic review of Kinect applications in elderly care and stroke rehabilitation. J. Neuroeng. Rehabil. 2014, 11, 108. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, M.; Blake, C.; Cunningham, C.; Boyle, G.; Finucane, C. Correlation of accelerometry with clinical balance tests in older fallers and non-fallers. Age Ageing 2009, 38, 308–313. [Google Scholar] [CrossRef] [PubMed]
- Greene, B.R.; O’Donovan, A.; Romero-Ortuno, R.; Cogan, L.; Scanaill, C.N.; Kenny, R.A. Quantitative falls risk assessment using the timed up and go test. IEEE Trans. Biomed. Eng. 2010, 57, 2918–2926. [Google Scholar] [CrossRef] [PubMed]
- Handojoseno, A.A.; Shine, J.M.; Nguyen, T.N.; Tran, Y.; Lewis, S.J.; Nguyen, H.T. Analysis and prediction of the freezing of gait using EEG brain dynamics. IEEE Trans. Neural Syst. Rehabil. Eng. 2015, 23, 887–896. [Google Scholar] [CrossRef] [PubMed]
- Handojoseno, A.A.; Shine, J.M.; Nguyen, T.N.; Tran, Y.; Lewis, S.J.; Nguyen, H.T. Using EEG spatial correlation, cross frequency energy, and wavelet coefficients for the prediction of Freezing of Gait in Parkinson’s Disease patients. In Proceedings of the 35th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Osaka, Japan, 3–7 July 2013; pp. 4263–4266. [Google Scholar]
- Tripoliti, E.E.; Tzallas, A.T.; Tsipouras, M.G.; Rigas, G.; Bougia, P.; Leontiou, M.; Fotiadis, D.I. Automatic detection of freezing of gait events in patients with Parkinson’s disease. Comput. Methods Progr. Biomed. 2013, 110, 12–26. [Google Scholar] [CrossRef] [PubMed]
- Nieuwboer, A.; Dom, R.; De Weerdt, W.; Desloovere, K.; Janssens, L.; Stijn, V. Electromyographic profiles of gait prior to onset of freezing episodes in patients with Parkinson’s disease. Brain 2004, 127, 1650–1660. [Google Scholar] [CrossRef] [PubMed]
- Roy, S.H.; Cheng, M.S.; Chang, S.S.; Moore, J.; De Luca, G.; Nawab, S.H.; De Luca, C.J. A combined sEMG and accelerometer system for monitoring functional activity in stroke. IEEE Trans. Neural Syst. Rehabil. Eng. 2009, 17, 585–594. [Google Scholar] [CrossRef] [PubMed]
- Yang, B.S.; Liao, S.T. Fall Detecting Using Inertial and Electromyographic Sensors. In Proceedings of the 36th Annual Meeting of the American Society of Biomechanics, Gainsville, FL, USA, 15–18 August 2012. [Google Scholar]
- Xi, X.; Tang, M.; Miran, S.M.; Luo, Z. Evaluation of feature extraction and recognition for activity monitoring and fall detection based on wearable sEMG sensors. Sensors 2017, 17, 1229. [Google Scholar] [CrossRef] [PubMed]
- Leone, A.; Rescio, G.; Caroppo, A.; Siciliano, P. An EMG-based system for pre-impact fall detection. In Proceedings of the IEEE Sensors, Busan, Korea, 1–4 November 2015. [Google Scholar]
- Cheng, J.; Chen, X.; Shen, M. A framework for daily activity monitoring and fall detection based on surface electromyography and accelerometer signals. IEEE J. Biomed. Health Inf. 2013, 17, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Berg, K.; Wood-Dauphine, S.; Williams, J.I.; Gayton, D. Measuring balance in the elderly: Preliminary development of an instrument. Physiother. Can. 1989, 41, 304–311. [Google Scholar] [CrossRef]
- Podsiadlo, D.; Richardson, S. The timed “Up & Go”: A test of basic functional mobility for frail elderly persons. J. Am. Geriatr. Soc. 1991, 39, 142–148. [Google Scholar] [PubMed]
- Wrisley, D.M.; Marchetti, G.F.; Kuharsky, D.K.; Whitney, S.L. Reliability, internal consistency, and validity of data obtained with the functional gait assessment. Phys. Ther. 2004, 84, 906–918. [Google Scholar] [PubMed]
- Horak, F.B.; Wrisley, D.M.; Frank, J. The balance evaluation systems test (BESTest) to differentiate balance deficits. Phys. Ther. 2009, 89, 484–498. [Google Scholar] [CrossRef] [PubMed]
- Duncan, R.P.; Leddy, A.L.; Cavanaugh, J.T.; Dibble, L.E.; Ellis, T.D.; Ford, M.P.; Earhart, G.M. Accuracy of fall prediction in Parkinson disease: Six-month and 12-month prospective analyses. Parkinson’s Dis. 2012, 2012, 237673. [Google Scholar] [CrossRef] [PubMed]
| Article | Sensor | Subjects | Obtrusive | Comments |
|---|---|---|---|---|
| Bourke et al. [18] | Waist mounted accelerometer | 10 young healthy subjects and 10 elderly heathy subjects | medium | Threshold based algorithm achieves 100% specificity and sensitivity with a false-positive rate of less than 1 false-positive (0.6 false-positives) per day of waking hours. |
| Binachi et al. [19] | Waist-mounted wearable sensor system composed of an accelerometer and a barometric pressure sensor. | 20 young healthy volunteers | medium | The proposed system demonstrated an accuracy, sensitivity and specificity of 96.9%, 97.5%, and 96.5%, respectively, in the indoor environment, with no false positives generated during extended testing during activities of daily living. |
| Howcraft et al. [21] | Accelerometers and pressure sensing insoles | 75 individuals who reported six month prospective fall occurrence | Low | The best performing fall prediction system used a neural network, dual-task gait data, and input parameters from head, pelvis, and left shank accelerometers. |
| Sannino et al. [22] | A tag placed on subjects’ chest | real-world database containing a set of fall and non-fall actions | Low | Their method achieves better accuracy than four state of the art machine learning algorithms. |
| Hirata et al. [26] | Proximity sensors attached to walking aid device | unspecified | Low | Their method uses a passive intelligent walker to prevent the user’s fall according to the support polygon and the walking characteristic of the user. |
| Bian et al. [27] | Infrared camera | Four healthy subjects | Medium | The proposed approach uses the infra-red based depth camera that can operate in dark environments. Experimental results show that the accuracy of the proposed algorithm is improved by 11.8% compared with a state-of-the-art fall detection algorithm. |
| Hilbi et al. [28] | Pressure sensors | Older adults in a hospital | Low | The results show that sensitivity and the specificity of the proposed approach are 96% and 99% respectively indicating a satisfactory performance. Further consistently designed studies such as randomized controlled trails are required to show the effect of bed-exit alarm systems on fall risk. |
| Pisan et al. [29] | Microsoft Kinect camera | 57 elderly patients | Medium | Their results show that for users who are at risk of falling, the slowing down in reaction time due to cognitive load is much larger than for users who are not at risk of falling. |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rajagopalan, R.; Litvan, I.; Jung, T.-P. Fall Prediction and Prevention Systems: Recent Trends, Challenges, and Future Research Directions. Sensors 2017, 17, 2509. https://doi.org/10.3390/s17112509
Rajagopalan R, Litvan I, Jung T-P. Fall Prediction and Prevention Systems: Recent Trends, Challenges, and Future Research Directions. Sensors. 2017; 17(11):2509. https://doi.org/10.3390/s17112509
Chicago/Turabian StyleRajagopalan, Ramesh, Irene Litvan, and Tzyy-Ping Jung. 2017. "Fall Prediction and Prevention Systems: Recent Trends, Challenges, and Future Research Directions" Sensors 17, no. 11: 2509. https://doi.org/10.3390/s17112509
APA StyleRajagopalan, R., Litvan, I., & Jung, T.-P. (2017). Fall Prediction and Prevention Systems: Recent Trends, Challenges, and Future Research Directions. Sensors, 17(11), 2509. https://doi.org/10.3390/s17112509





