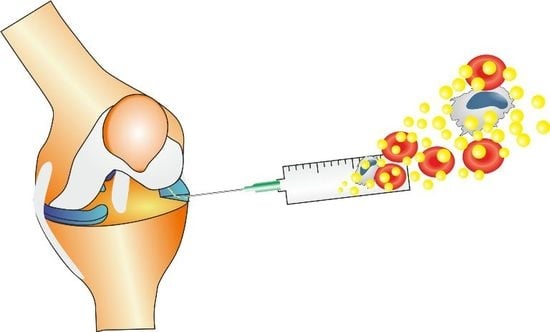
Short-Term Outcomes of Percutaneous Trephination with a Platelet Rich Plasma Intrameniscal Injection for the Repair of Degenerative Meniscal Lesions. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study
Abstract
1. Introduction
2. Results
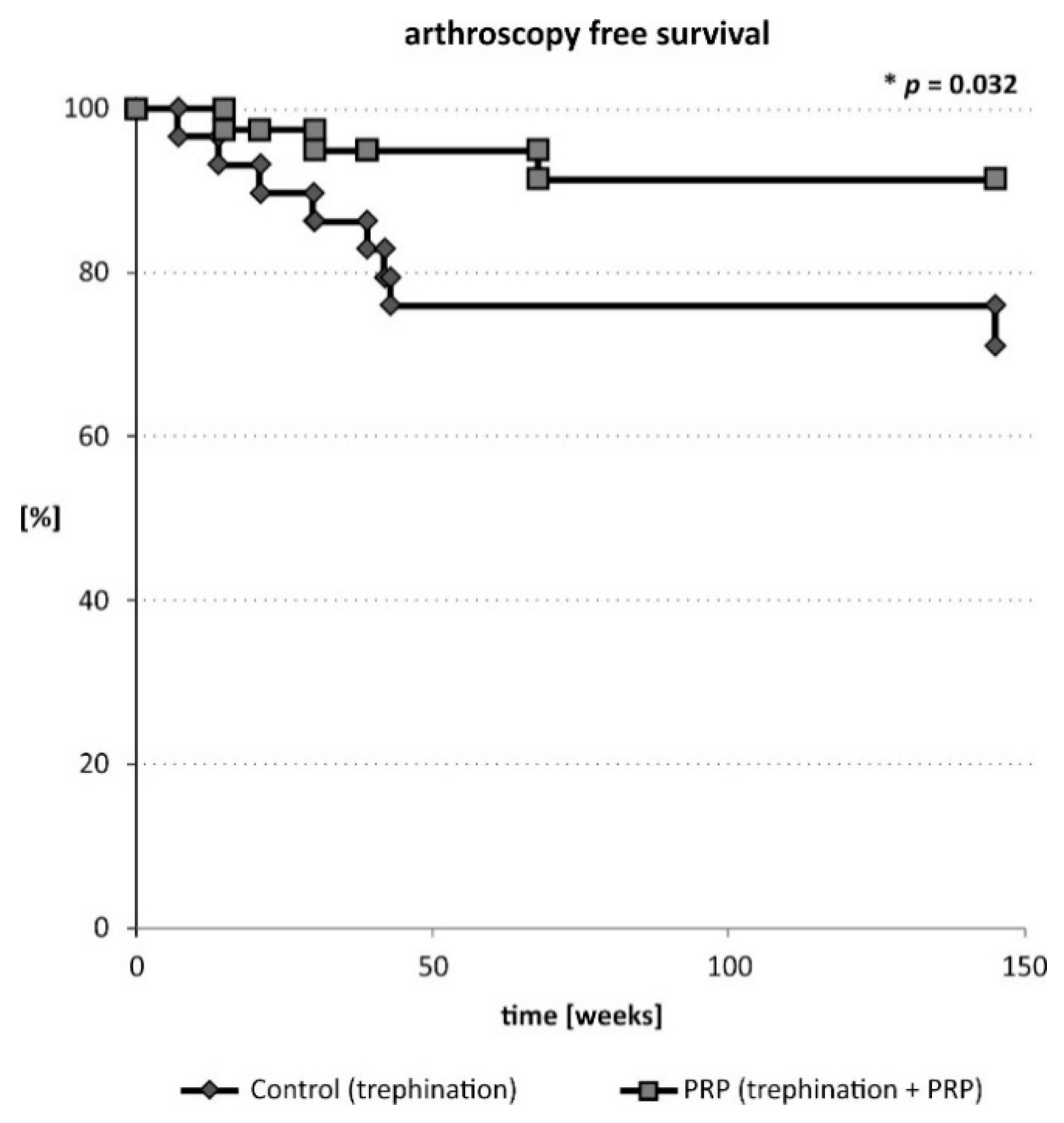
2.1. Primary Outcome
2.2. Secondary Outcomes-Pain
2.3. Secondary Outcomes-Function
2.4. Complications
3. Discussion
3.1. Strengths
3.2. Limitations
4. Materials and Methods
4.1. Trial Design and Informed Consent
4.2. Eligibility Criteria
4.3. PRP and Thrombin Preparation
4.4. Procedures
4.5. Outcomes
4.6. Randomization
4.7. Blinding
4.8. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Hawker, G. Knee Arthroscopy in England and Ontario: Patterns of Use, Changes Over Time and Relationship to Total Knee Replacement. J. Bone Jt. Surg. Am. 2008, 90, 2337. [Google Scholar] [CrossRef] [PubMed]
- Englund, M.; Guermazi, A.; Gale, D.; Hunter, D.J.; Aliabadi, P.; Clancy, M.; Felson, D.T. Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N. Engl. J. Med. 2008, 359, 1108–1115. [Google Scholar] [CrossRef] [PubMed]
- Sihvonen, R.; Paavola, M.; Malmivaara, A.; Itälä, A.; Joukainen, A.; Nurmi, H.; Kalske, J.; Järvinen, T.L.N. Arthroscopic Partial Meniscectomy versus Sham Surgery for a Degenerative Meniscal Tear. N. Engl. J. Med. 2013, 369, 2515–2524. [Google Scholar] [CrossRef]
- Fairbank, T.J. Knee joint changes after meniscectomy. J. Bone Jt.Surg. Br. 1948, 30B, 664–670. [Google Scholar] [CrossRef]
- Noyes, F.R.; Barber-Westin, S.D. Repair of complex and avascular meniscal tears and meniscal transplantation. J. Bone Jt.Surg. Am. 2010, 92, 1012–1029. [Google Scholar]
- Henning, C.E.; Lynch, M.A.; Yearout, K.M.; Vequist, S.W.; Stallbaumer, R.J.; Decker, K.A. Arthroscopic meniscal repair using an exogenous fibrin clot. Clin. Orthop. 1990, 64–72. [Google Scholar] [CrossRef]
- Van Trommel, M.F.; Simonian, P.T.; Potter, H.G.; Wickiewicz, T.L. Arthroscopic meniscal repair with fibrin clot of complete radial tears of the lateral meniscus in the avascular zone. Arthrosc. J. Arthrosc. Relat. Surg. Off. Publ. Arthrosc. Assoc. N. Am. Int. Arthrosc. Assoc. 1998, 14, 360–365. [Google Scholar] [CrossRef]
- Pujol, N.; Tardy, N.; Boisrenoult, P.; Beaufils, P. Long-term outcomes of all-inside meniscal repair. Knee Surg. Sports Traumatol. Arthrosc. 2015, 23, 219–224. [Google Scholar] [CrossRef]
- Kaminski, R.; Kulinski, K.; Kozar-Kaminska, K.; Wielgus, M.; Langner, M.; Wasko, M.K.; Kowalczewski, J.; Pomianowski, S. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study Evaluating Meniscal Healing, Clinical Outcomes and Safety in Patients Undergoing Meniscal Repair of Unstable, Complete Vertical Meniscal Tears (Bucket Handle) Augmented with Platelet-Rich Plasma. BioMed Res. Int. 2018, 2018, 9315815. [Google Scholar]
- Kaminski, R.; Kulinski, K.; Kozar-Kaminska, K.; Wasko, M.K.; Langner, M.; Pomianowski, S. Repair augmentation of unstable, complete vertical meniscal tears with bone marrow venting procedure. A prospective, randomized, double-blind, parallel-group, placebo-controlled study. Arthrosc. J. Arthrosc. Relat. Surg. 2018, 2018, 9315815. [Google Scholar]
- Ahn, J.-H.; Kwon, O.-J.; Nam, T.-S. Arthroscopic Repair of Horizontal Meniscal Cleavage Tears With Marrow-Stimulating Technique. Arthrosc. J. Arthrosc. Relat. Surg. 2015, 31, 92–98. [Google Scholar] [CrossRef] [PubMed]
- Katz, N.P.; Paillard, F.C.; Ekman, E. Determining the clinical importance of treatment benefits for interventions for painful orthopedic conditions. J. Orthop. Surg. 2015, 10, 24. [Google Scholar] [CrossRef] [PubMed]
- Harris, J.D.; Brand, J.C.; Cote, M.P.; Faucett, S.C.; Dhawan, A. Research Pearls: The Significance of Statistics and Perils of Pooling. Part 1: Clinical Versus Statistical Significance. Arthrosc. J. Arthrosc. Relat. Surg. 2017, 33, 1102–1112. [Google Scholar] [CrossRef] [PubMed]
- Greco, N.J.; Anderson, A.F.; Mann, B.J.; Cole, B.J.; Farr, J.; Nissen, C.W.; Irrgang, J.J. Responsiveness of the International Knee Documentation Committee Subjective Knee Form in comparison to the Western Ontario and McMaster Universities Osteoarthritis Index, modified Cincinnati Knee Rating System and Short Form 36 in patients with focal articular cartilage defects. Am. J. Sports Med. 2010, 38, 891–902. [Google Scholar] [PubMed]
- Delos, D.; Rodeo, S.A. Enhancing meniscal repair through biology: Platelet-rich plasma as an alternative strategy. Instr. Course Lect. 2011, 60, 453–460. [Google Scholar] [PubMed]
- Paxton, E.S.; Stock, M.V.; Brophy, R.H. Meniscal Repair Versus Partial Meniscectomy: A Systematic Review Comparing Reoperation Rates and Clinical Outcomes. Arthrosc. J. Arthrosc. Relat. Surg. 2011, 27, 1275–1288. [Google Scholar] [CrossRef]
- Katz, J.N.; Brophy, R.H.; Chaisson, C.E.; de Chaves, L.; Cole, B.J.; Dahm, D.L.; Donnell-Fink, L.A.; Guermazi, A.; Haas, A.K.; Jones, M.H.; et al. Surgery versus Physical Therapy for a Meniscal Tear and Osteoarthritis. N. Engl. J. Med. 2013, 368, 1675–1684. [Google Scholar] [CrossRef]
- Beaufils, P.; Becker, R.; Kopf, S.; Englund, M.; Verdonk, R.; Ollivier, M.; Seil, R. Surgical management of degenerative meniscus lesions: The 2016 ESSKA meniscus consensus. Knee Surg. Sports Traumatol. Arthrosc. 2017, 25, 335–346. [Google Scholar] [CrossRef]
- Siemieniuk, R.A.C.; Harris, I.A.; Agoritsas, T.; Poolman, R.W.; Brignardello-Petersen, R.; Van de Velde, S.; Buchbinder, R.; Englund, M.; Lytvyn, L.; Quinlan, C.; et al. Arthroscopic surgery for degenerative knee arthritis and meniscal tears: A clinical practice guideline. BMJ 2017, 357, j1982. [Google Scholar] [CrossRef]
- Crisci, A.; Crescenzo, U.D.; Crisci, M. Platelet-rich concentrates (L-PRF, PRP) in tissue regeneration: Control of apoptosis and interactions with regenerative cells. J. Clin. Mol. Med. 2018, 1, 1–2. [Google Scholar] [CrossRef]
- Dohan Ehrenfest, D.M.; Bielecki, T.; Jimbo, R.; Barbé, G.; Del Corso, M.; Inchingolo, F.; Sammartino, G. Do the fibrin architecture and leukocyte content influence the growth factor release of platelet concentrates? An evidence-based answer comparing a pure platelet-rich plasma (P-PRP) gel and a leukocyte- and platelet-rich fibrin (L-PRF). Curr. Pharm. Biotechnol. 2012, 13, 1145–1152. [Google Scholar] [CrossRef] [PubMed]
- Ishida, K.; Kuroda, R.; Miwa, M.; Tabata, Y.; Hokugo, A.; Kawamoto, T.; Sasaki, K.; Doita, M.; Kurosaka, M. The Regenerative Effects of Platelet-Rich Plasma on Meniscal Cells In Vitro and Its In Vivo Application with Biodegradable Gelatin Hydrogel. Tissue Eng. 2007, 13, 1103–1112. [Google Scholar] [CrossRef] [PubMed]
- Zellner, J.; Mueller, M.; Berner, A.; Dienstknecht, T.; Kujat, R.; Nerlich, M.; Hennemann, B.; Koller, M.; Prantl, L.; Angele, M.; et al. Role of mesenchymal stem cells in tissue engineering of meniscus. J. Biomed. Mater. Res. A 2010, 94, 1150–1161. [Google Scholar] [CrossRef] [PubMed]
- Andia, I.; Maffulli, N. New biotechnologies for musculoskeletal injuries. Surg. J. R. Coll. Surg. Edinb. Irel. 2018. [Google Scholar] [CrossRef] [PubMed]
- Andia, I.; Maffulli, N. A contemporary view of platelet-rich plasma therapies: Moving toward refined clinical protocols and precise indications. Regen. Med. 2018, 13, 717–728. [Google Scholar] [CrossRef] [PubMed]
- Griffin, J.W.; Hadeed, M.M.; Werner, B.C.; Diduch, D.R.; Carson, E.W.; Miller, M.D. Platelet-rich Plasma in Meniscal Repair: Does Augmentation Improve Surgical Outcomes? Clin. Orthop. Relat. Res. 2015, 473, 1665–1672. [Google Scholar] [CrossRef] [PubMed]
- Strümper, R. Intra-Articular Injections of Autologous Conditioned Serum to Treat Pain from Meniscal Lesions. Sports Med. Int. Open 2017, 1, E200–E205. [Google Scholar] [CrossRef] [PubMed]
- Doral, M.N.; Bilge, O.; Huri, G.; Turhan, E.; Verdonk, R. Modern treatment of meniscal tears. EFORT Open Rev. 2018, 3, 260–268. [Google Scholar] [CrossRef]
- Ghazi Zadeh, L.; Chevrier, A.; Farr, J.; Rodeo, S.A.; Buschmann, M.D. Augmentation Techniques for Meniscus Repair. J. Knee Surg. 2018, 31, 99–116. [Google Scholar] [CrossRef]
- Fox, J.M.; Rintz, K.G.; Ferkel, R.D. Trephination of incomplete meniscal tears. Arthrosc. J. Arthrosc. Relat. Surg. Off. Publ. Arthrosc. Assoc. N. Am. Int. Arthrosc. Assoc. 1993, 9, 451–455. [Google Scholar] [CrossRef]
- Tumia, N.S.; Johnstone, A.J. Platelet derived growth factor-AB enhances knee meniscal cell activity in vitro. The Knee 2009, 16, 73–76. [Google Scholar] [CrossRef] [PubMed]
- Cozma, C.N.; Raducu, L.; Jecan, C.R. Platelet Rich Plasma- mechanism of action and clinical applications. J. Clin. Investig. Surg. 2016, 1, 41–46. [Google Scholar] [CrossRef]
- Brophy, R.H.; Rai, M.F.; Zhang, Z.; Torgomyan, A.; Sandell, L.J. Molecular analysis of age and sex-related gene expression in meniscal tears with and without a concomitant anterior cruciate ligament tear. J. Bone Jt.Surg. Am. 2012, 94, 385–393. [Google Scholar] [CrossRef] [PubMed]
- Dhillon, M.S.; Patel, S.; John, R. PRP in OA knee—Update, current confusions and future options. SICOT-J 2017, 3, 27. [Google Scholar] [CrossRef] [PubMed]
- Pereira, R.C.; Scaranari, M.; Benelli, R.; Strada, P.; Reis, R.L.; Cancedda, R.; Gentili, C. Dual Effect of Platelet Lysate on Human Articular Cartilage: A Maintenance of Chondrogenic Potential and a Transient Proinflammatory Activity Followed by an Inflammation Resolution. Tissue Eng. Part A 2013, 19, 1476–1488. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.-R.; Shon, O.-J.; Park, S.-I.; Kim, H.-J.; Kim, S.; Ahn, M.-W.; Do, S.H. Platelet-Rich Plasma Increases the Levels of Catabolic Molecules and Cellular Dedifferentiation in the Meniscus of a Rabbit Model. Int. J. Mol. Sci. 2016, 17, 120. [Google Scholar] [CrossRef] [PubMed]
- Haleem, A.M.; Singergy, A.A.E.; Sabry, D.; Atta, H.M.; Rashed, L.A.; Chu, C.R.; Shewy, M.T.E.; Azzam, A.; Aziz, M.T.A. The Clinical Use of Human Culture–Expanded Autologous Bone Marrow Mesenchymal Stem Cells Transplanted on Platelet-Rich Fibrin Glue in the Treatment of Articular Cartilage Defects: A Pilot Study and Preliminary Results. CARTILAGE 2010, 1, 253–261. [Google Scholar] [CrossRef]
- Jeyakumar, V.; Niculescu-Morzsa, E.; Bauer, C.; Lacza, Z.; Nehrer, S. Redifferentiation of Articular Chondrocytes by Hyperacute Serum and Platelet Rich Plasma in Collagen Type I Hydrogels. Int. J. Mol. Sci. 2019, 20, 316. [Google Scholar] [CrossRef]
- Lucarelli, E.; Beccheroni, A.; Donati, D.; Sangiorgi, L.; Cenacchi, A.; Del Vento, A.M.; Meotti, C.; Bertoja, A.Z.; Giardino, R.; Fornasari, P.M.; et al. Platelet-derived growth factors enhance proliferation of human stromal stem cells. Biomaterials 2003, 24, 3095–3100. [Google Scholar] [CrossRef]
- Rubio-Azpeitia, E.; Sánchez, P.; Delgado, D.; Andia, I. Adult Cells Combined with Platelet-Rich Plasma for Tendon Healing: Cell Source Options. Orthop. J. Sports Med. 2017, 5, 232596711769084. [Google Scholar] [CrossRef]
- Kubosch, E.J.; Lang, G.; Furst, D.; Kubosch, D.; Izadpanah, K.; Rolauffs, B.; Sudkamp, N.P.; Schmal, H. The Potential for Synovium-derived Stem Cells in Cartilage Repair. Curr. Stem Cell Res. Ther. 2018, 13, 174–184. [Google Scholar] [CrossRef] [PubMed]
- Dean, C.S.; Chahla, J.; Matheny, L.M.; Mitchell, J.J.; LaPrade, R.F. Outcomes After Biologically Augmented Isolated Meniscal Repair with Marrow Venting Are Comparable with Those After Meniscal Repair With Concomitant Anterior Cruciate Ligament Reconstruction. Am. J. Sports Med. 2017, 45, 1341–1348. [Google Scholar] [CrossRef] [PubMed]
- Harrison, P. The Subcommittee on Platelet Physiology The use of platelets in regenerative medicine and proposal for a new classification system: Guidance from the SSC of the ISTH. J. Thromb. Haemost. 2018, 16, 1895–1900. [Google Scholar] [CrossRef] [PubMed]
- Roos, E.M.; Roos, H.P.; Lohmander, L.S.; Ekdahl, C.; Beynnon, B.D. Knee Injury and Osteoarthritis Outcome Score (KOOS)—Development of a self-administered outcome measure. J. Orthop. Sports Phys. Ther. 1998, 28, 88–96. [Google Scholar] [CrossRef]
- Bellamy, N. WOMAC: A 20-year experiential review of a patient-centered self-reported health status questionnaire. J. Rheumatol. 2002, 29, 2473–2476. [Google Scholar] [PubMed]
- Crawford, K.; Briggs, K.K.; Rodkey, W.G.; Steadman, J.R. Reliability, validity and responsiveness of the IKDC score for meniscus injuries of the knee. Arthrosc. J. Arthrosc. Relat. Surg. Off. Publ. Arthrosc. Assoc. N. Am. Int. Arthrosc. Assoc. 2007, 23, 839–844. [Google Scholar] [CrossRef] [PubMed]
- Roos, E.M.; Lohmander, L.S. The Knee injury and Osteoarthritis Outcome Score (KOOS): From joint injury to osteoarthritis. Health Qual. Life Outcomes 2003, 1, 64. [Google Scholar] [CrossRef]
- Suresh, K. An overview of randomization techniques: An unbiased assessment of outcome in clinical research. J. Hum. Reprod. Sci. 2011, 4, 8. [Google Scholar] [CrossRef]
- R Development Core Team. R: A Language and Environment for Statistical Computing; R Foundation for Statistical Computing: Vienna, Austria, 2008. [Google Scholar]
- Malavolta, E.A.; Gracitelli, M.E.C.; Ferreira Neto, A.A.; Assuncao, J.H.; Bordalo-Rodrigues, M.; de Camargo, O.P. Platelet-Rich Plasma in Rotator Cuff Repair: A Prospective Randomized Study. Am. J. Sports Med. 2014, 42, 2446–2454. [Google Scholar] [CrossRef]
- Van der Tweel, I.; Askie, L.; Vandermeer, B.; Ellenberg, S.; Fernandes, R.M.; Saloojee, H.; Bassler, D.; Altman, D.G.; Offringa, M.; van der Lee, J.H.; et al. Standard 4: Determining adequate sample sizes. Pediatrics 2012, 129 (Suppl. S3), S138–S145. [Google Scholar] [CrossRef]
- Stein, T.; Mehling, A.P.; Welsch, F.; von Eisenhart-Rothe, R.; Jäger, A. Long-term outcome after arthroscopic meniscal repair versus arthroscopic partial meniscectomy for traumatic meniscal tears. Am. J. Sports Med. 2010, 38, 1542–1548. [Google Scholar] [CrossRef] [PubMed]
- Järvelä, S.; Sihvonen, R.; Sirkeoja, H.; Järvelä, T. All-Inside Meniscal Repair with Bioabsorbable Meniscal Screws or with Bioabsorbable Meniscus Arrows: A Prospective, Randomized Clinical Study with 2-Year Results. Am. J. Sports Med. 2010, 38, 2211–2217. [Google Scholar] [CrossRef] [PubMed]
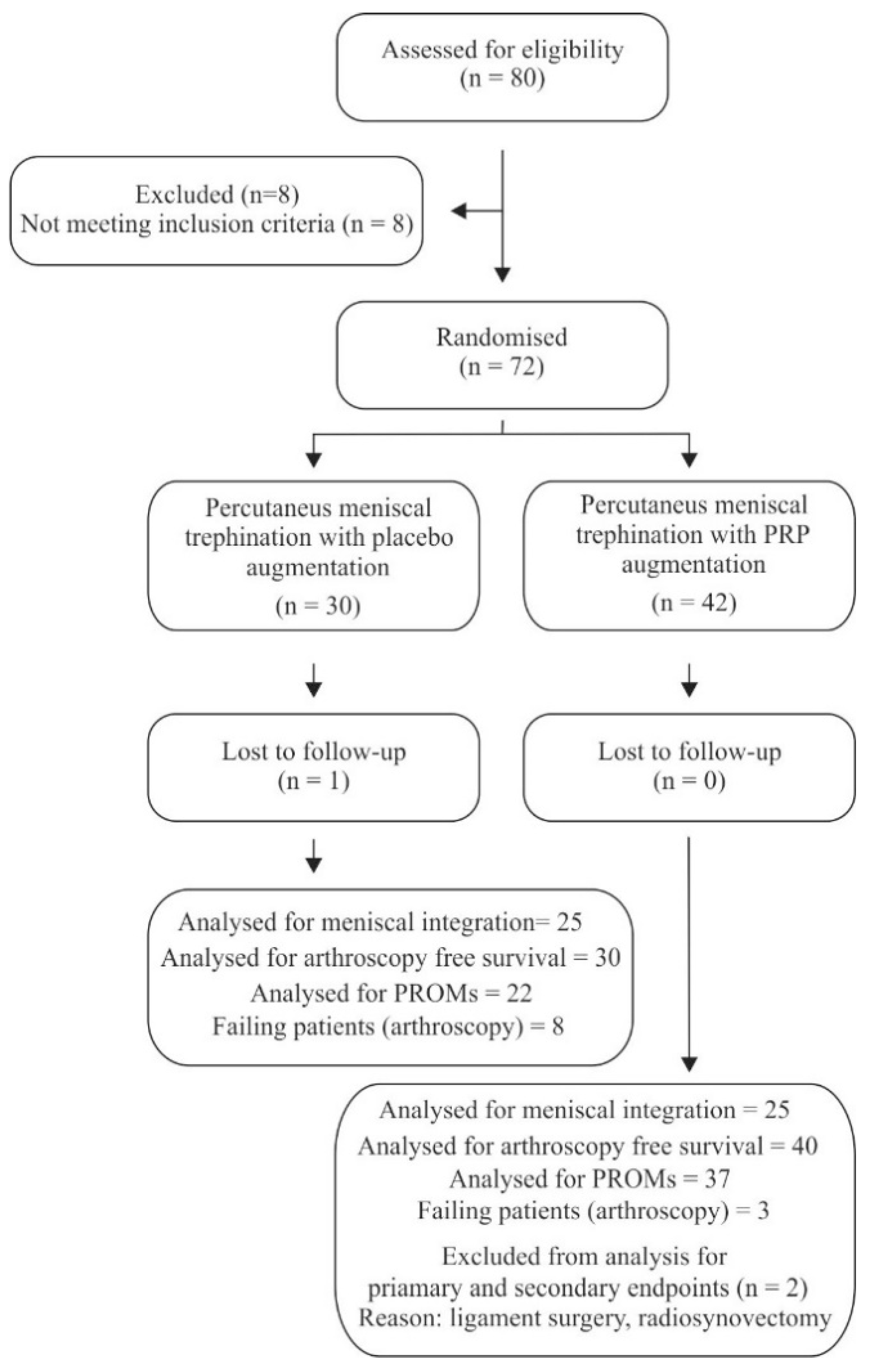
| Control Group (n = 30) | PRP-Treated Group (n = 42) | P-Value | |
|---|---|---|---|
| Age (years) | 46 (27–68) | 44 (18–67) | P = 0.31 |
| Sex (M:F) | 19:11 | 22:20 | P = 0.25 |
| BMI (range) | 28 (21–36) | 27 (19–37) | P = 0.27 |
| Kellgren-Lawrence scale (0 grade:1 grade:2 grade) | 23:7:0 | 30:12:0 | P = 0.79 |
| PRP (PLT × 103/μL) | 732 (220–1586) | 823 (320–1659) | P = 0.16 |
| Meniscus (MM:ML) | 30:0 | 41:1 | P = 0.58 |
| Cumulative Outcome (Assessed Using MRI and Arthroscopy) (P = 0.04) | ||
|---|---|---|
| Outcome | PRP-treated group (n of menisci) | Control group (n of menisci) |
| Healed | 10 | 5 |
| Partially healed | 4 | 3 |
| Failed | 13 | 19 |
| MRI (P = 0.41) | ||
| Outcome | PRP-treated group (n of menisci) | Control group (n of menisci) |
| Healed | 11 | 7 |
| Partially healed | 4 | 4 |
| Failed | 10 | 15 |
| Control Group | PRP Group | ||||
|---|---|---|---|---|---|
| PROM | Pre-Procedure | Post Trephination | Pre-Procedure | Post Trephination | Pa |
| VAS | 4.40 ± 0.07 (3.55–5.25) | 2.05 ± 0.08 (1.27–2.82) | 5.38 ± 0.05 (4.77–5.99) | 1.97 ± 0.05 (1.40–2.55) | 0.39 |
| IKDC | 54.92 ± 0.54 (49.08–60.77) | 88.12 ± 0.89 (79.97–96.28) | 51.99 ± 0.34 (47.62–56.36) | 85.98 ± 0.52 (79.79–92.16) | 0.36 |
| WOMAC | 28.93 ± 0.61 (22.42–35.45) | 7.50 ± 0.59 (2.06–12.94) | 34.36 ± 0.35 (29.90–38.82) | 9.72 ± 0.32 (5.95–13.48) | 0.21 |
| KOOS | |||||
| Pain | 65.30 ± 0.54 (59.51–71.10) | 89.00 ± 0.63 (83.19–94.81) | 57.48 ± 0.30 (57.18–57.78) | 87.24 ± 0.36 (82.99–91.48) | 0.22 |
| Symptoms | 69.86 ± 0.62 (63.18–76.54) | 90.42 ± 0.56 (85.26–95.58) | 63.53 ± 0.39 (63.23–63.83) | 92.03 ± 0.27 (88.80–95.26) | 0.27 |
| ADL | 68.42 ± 0.66 (61.33–75.50) | 92.38 ± 0.61 (86.80–97.95) | 63.70 ± 0.37 (63.40–64.00) | 89.36 ± 0.36 (85.07–93.64) | 0.25 |
| S/R | 33.50 ± 0.62 (26.84–40.16) | 78.98 ± 1.10 (68.83–89.12) | 35.83 ± 0.51 (35.53–36.14) | 69.52 ± 0.77 (60.29–78.74) | 0.11 |
| QoL | 35.00 ± 0.49 (29.73–40.27) | 68.18 ± 1.08 (58.28–78.08) | 37.90 ± 0.26 (37.59–38.20) | 67.06 – 0.55 (60.56–73.56) | 0.42 |
| Control Group | PRP Group | ||||||
|---|---|---|---|---|---|---|---|
| PROM | MCID | Mean Change | Improved by at Least MCID [%] | Mean Change | Improved by at Least MCID [%] | Pa | Pb |
| VAS | 2 [12] | 2.36 ± 0.0.09 (3.86–5.20) | 39 | 3.62 ± 0.07 (2.82–4.43) | 65 | 0.027 | 0.046 |
| IKDC | 16.7 [13] | 33.66 ± 0.84 (25.95–41.36) | 83 | 34.74 ± 0.55 (28.17–41.31) | 78 | 0.48 | 0.48 |
| WOMAC | 11.5 [14] | 21.77 ± 0.67 (15.65–27.90) | 65 | 24.77 ± 0.37 (20.40–29.14) | 86 | 0.16 | 0.053 |
| KOOS | |||||||
| Pain | 16.7 [13] | 24.95 ± 0.62 (19.24–30.66) | 65 | 29.50 ± 0.45 (24.18–34.81) | 73 | 0.17 | 0.36 |
| Symptoms | 17.4 [13] | 18.38 ± 0.82 (10.81–25.95) | 48 | 27.93 ± 0.42 (22.89–32.96) | 76 | 0.016 | 0.028 |
| ADL | 18.4 [13] | 24.61 ± 0.74 (17.79–31.43) | 57 | 26.27 ± 0.39 (21.67–30.87) | 76 | 0.18 | 0.1 |
| S/R | 12.5 [13] | 43.75 ± 1.12 (33.43–54.07) | 83 | 34.65 ± 0.76 (25.57–43.74) | 70 | 0.12 | 0.22 |
| QoL | 15.6 [13] | 32.67 ± 1.06 (22.93–42.41) | 70 | 28.43 ± 0.52 (22.23–34.64) | 76 | 0.29 | 0.41 |
| Inclusion Criteria | Exclusion Criteria |
|---|---|
| skeletally mature patients aged 18–70 years chronic horizontal tears on MRI tear located in the vascular/avascular portion of the meniscus single tear of the medial and/or lateral meniscus | arthritic changes (Kellgren-Lawrence scale >2) discoid meniscus axial leg deformity (valgus > 6 deg)- concomitant chondral defects (> 2 ICRS) Inflammatory diseases (rheumatoid arthritis) chondral defects above ICRS 2 on MRI |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kaminski, R.; Maksymowicz-Wleklik, M.; Kulinski, K.; Kozar-Kaminska, K.; Dabrowska-Thing, A.; Pomianowski, S. Short-Term Outcomes of Percutaneous Trephination with a Platelet Rich Plasma Intrameniscal Injection for the Repair of Degenerative Meniscal Lesions. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study. Int. J. Mol. Sci. 2019, 20, 856. https://doi.org/10.3390/ijms20040856
Kaminski R, Maksymowicz-Wleklik M, Kulinski K, Kozar-Kaminska K, Dabrowska-Thing A, Pomianowski S. Short-Term Outcomes of Percutaneous Trephination with a Platelet Rich Plasma Intrameniscal Injection for the Repair of Degenerative Meniscal Lesions. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study. International Journal of Molecular Sciences. 2019; 20(4):856. https://doi.org/10.3390/ijms20040856
Chicago/Turabian StyleKaminski, Rafal, Marta Maksymowicz-Wleklik, Krzysztof Kulinski, Katarzyna Kozar-Kaminska, Agnieszka Dabrowska-Thing, and Stanislaw Pomianowski. 2019. "Short-Term Outcomes of Percutaneous Trephination with a Platelet Rich Plasma Intrameniscal Injection for the Repair of Degenerative Meniscal Lesions. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study" International Journal of Molecular Sciences 20, no. 4: 856. https://doi.org/10.3390/ijms20040856
APA StyleKaminski, R., Maksymowicz-Wleklik, M., Kulinski, K., Kozar-Kaminska, K., Dabrowska-Thing, A., & Pomianowski, S. (2019). Short-Term Outcomes of Percutaneous Trephination with a Platelet Rich Plasma Intrameniscal Injection for the Repair of Degenerative Meniscal Lesions. A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study. International Journal of Molecular Sciences, 20(4), 856. https://doi.org/10.3390/ijms20040856