The Feasibility of a Novel School Peer-Led Mentoring Model to Improve the Physical Activity Levels and Sedentary Time of Adolescent Girls: The Girls Peer Activity (G-PACT) Project
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants
2.3. Recruitment
Consent
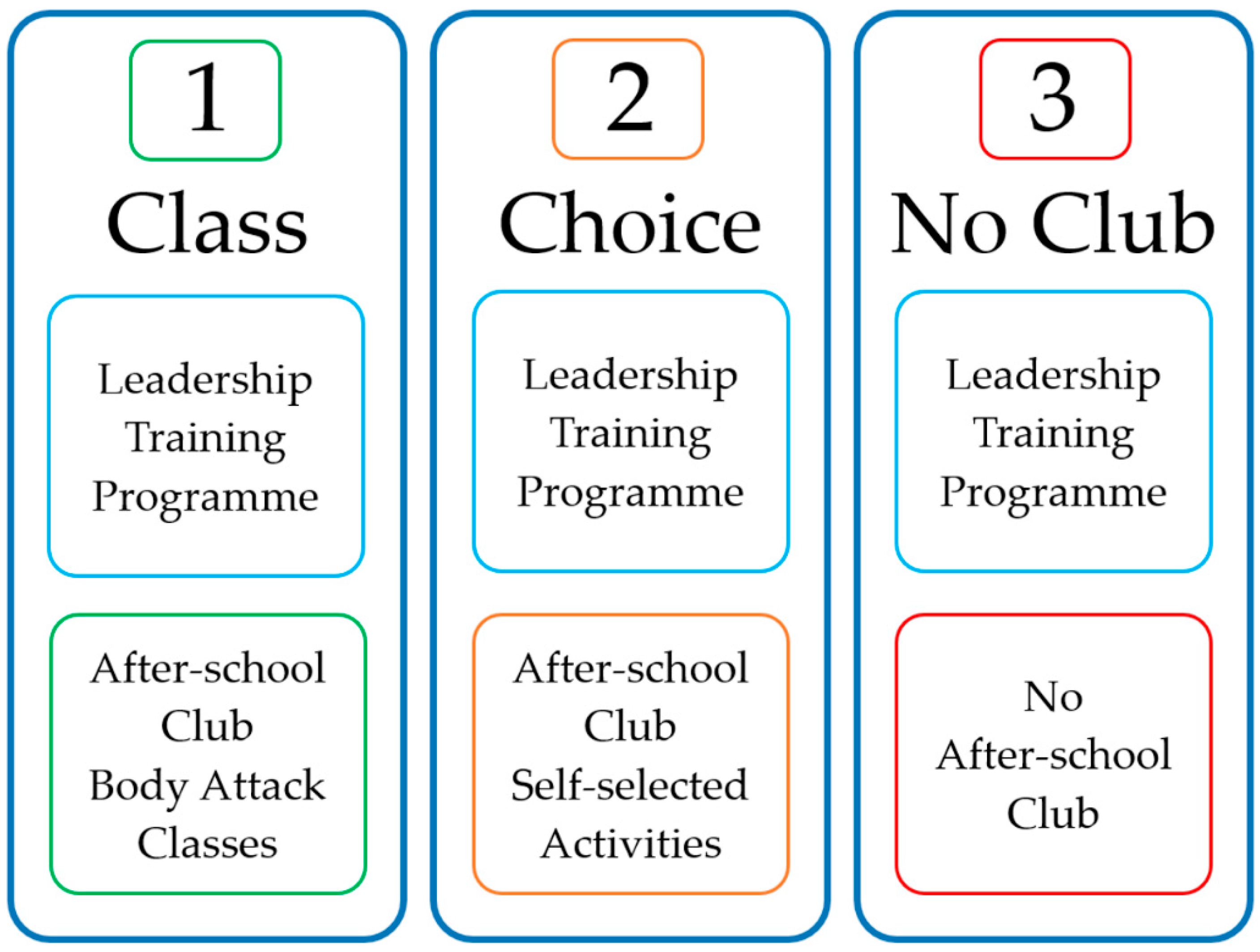
2.4. Description of Intervention
2.4.1. Mentors
2.4.2. Educational Leadership Sessions
2.4.3. Physical Activity Components
2.4.4. Intervention Timeline
2.5. Measures
2.5.1. Anthropometrics
2.5.2. Socioeconomic Status
2.5.3. Recruitment (Aim 1)
2.5.4. Physical Activity Outcomes (Aims 2 and 3)
2.5.5. Psychological Outcomes
2.6. Data Analysis
3. Results
3.1. Recruitment and Data Provision
3.2. Descriptive Information
3.3. Whole Day (7 a.m.–11 p.m.) PA Data
3.4. School Day (9 a.m.–3.15 p.m.) PA Data
3.5. After-School Club Period (3.15 p.m.–4.45 p.m.)
3.6. Subgroup Analyses
3.6.1. Leaders
3.6.2. Peers
3.7. Psychological Outcomes
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Department of Health, Physical Activity, Health Improvement and Protection. Start Active, Stay Active: A Report on Physical Activity for Health from the Four Home Countries’ Chief Medical Officers, 2011. Start Active, Stay Active: Report on Physical Activity in the UK Website. Available online: https://www.gov.uk/government/publications/start-active-stay-active-a-report-on-physical-activity-from-the-four-home-countries-chief-medical-officers (accessed on 2 May 2018).
- Janssen, I.; Leblanc, A.G. Systematic review of the health benefits of physical activity and fitness in school-aged children and youth. Int. J. Behav. Nutr. Phys. Act. 2010, 7, 40–55. [Google Scholar] [CrossRef] [PubMed]
- Biddle, S.J.; Asare, M. Physical activity and mental health in children and adolescents: A review of reviews. Br. J. Sports Med. 2011, 45, 886–895. [Google Scholar] [CrossRef] [PubMed]
- Dumith, S.C.; Gigante, D.P.; Domingues, M.R.; Kohl, H.W. III. Physical activity change during adolescence: A systematic review and a pooled analysis. Int. J. Epidemiol. 2011, 40, 685–698. [Google Scholar] [CrossRef] [PubMed]
- Viner, R.M.; Ozer, E.M.; Denny, S.; Marmot, M.; Resnick, M.; Fatusi, A.; Currie, C. Adolescence and the social determinants of health. Lancet 2012, 379, 1641–1652. [Google Scholar] [CrossRef]
- Cooper, A.R.; Goodman, A.; Page, A.S.; Sherar, L.B.; Esliger, D.W.; van Sluijs, E.M.; Andersen, L.B.; Anderssen, S.; Cardon, G.; Davey, R.; et al. Objectively measured physical activity and sedentary time in youth: The International children’s accelerometry database (ICAD). Int. J. Behav. Nutr. Phys. Act. 2015, 12, 113. [Google Scholar] [CrossRef] [PubMed]
- Hallal, P.C.; Andersen, L.B.; Bull, F.C.; Guthold, R.; Haskell, W.; Ekelund, U. Global physical activity levels: Surveillance progress, pitfalls, and prospects. Lancet 2012, 380, 247–257. [Google Scholar] [CrossRef]
- Sardinha, L.B.; Marques, A.; Minderico, C.; Ekelund, U. Cross-sectional and prospective impact of reallocating sedentary time to physical activity on children’s body composition. Pediatr. Obes. 2017, 12, 373–379. [Google Scholar] [CrossRef] [PubMed]
- Corder, K.; Brown, H.; Schiff, A.; van Sluijs, E.M.F. Feasibility study and pilot cluster-randomised controlled trial of the GoActive intervention aiming to promote physical activity among adolescents: Outcomes and lessons learnt. BMJ Open 2016, 6, e012335. [Google Scholar] [CrossRef] [PubMed]
- Sutherland, R.; Campbell, E.; Lubans, D.; Morgan, P.; Nathan, N.; Okely, A.; Gillham, K.; Davies, L.; Wiggers, J. Physical Activity 4 Everyone’cluster RCT: 24-month physical activity outcomes of a school-based physical activity intervention targeting adolescents. Overall and school day physical activity outcomes. J. Sci. Med. Sport 2017, 20, e110. [Google Scholar] [CrossRef]
- Van Sluijs, E.M.; McMinn, A.M.; Griffin, S.J. Effectiveness of interventions to promote physical activity in children and adolescents: Systematic review of controlled trials. BMJ 2007, 335, 703. [Google Scholar] [CrossRef] [PubMed]
- Owen, M.B.; Curry, W.B.; Kerner, C.; Newson, L.; Fairclough, S.J. The effectiveness of school-based physical activity interventions for adolescent girls: A systematic review and meta-analysis. Prev. Med. 2017, 105, 237–249. [Google Scholar] [CrossRef] [PubMed]
- Pearson, N.; Braithwaite, R.; Biddle, S.J.H. The effectiveness of interventions to increase physical activity among adolescent girls: A Meta-analysis. Acad. Pediatr. 2015, 15, 9–18. [Google Scholar] [CrossRef] [PubMed]
- Black, M.M.; Hager, E.R.; Le, K.; Anliker, J.; Arteaga, S.S.; DiClemente, C.; Gittelsohn, J.; Magder, L.; Papas, M.; Snitker, S. Challenge! Health promotion/obesity prevention mentorship model among urban, black adolescents. Pediatrics 2010, 126, 280–288. [Google Scholar] [CrossRef] [PubMed]
- Campbell, R.; Starkey, F.; Holliday, J.; Audrey, S.; Bloor, M.; Parry-Langdon, N.; Hughes, R.; Moore, L. An informal school-based peer-led intervention for smoking prevention in adolescence (ASSIST): A cluster randomised trial. Lancet 2008, 371, 1595–1602. [Google Scholar] [CrossRef]
- Davey-Rothwell, M.A.; Tobin, K.; Yang, C.; Sun, C.J.; Latkin, C.A. Results of a randomized controlled trial of a peer mentor HIV/STI prevention intervention for women over an 18 month follow-up. AIDS Behav. 2011, 15, 1654–1663. [Google Scholar] [CrossRef] [PubMed]
- Smith, L.H. Cross-age peer mentoring approach to impact the health outcomes of children and families. J. Spec. Pediatr. Nurs. 2011, 16, 220–225. [Google Scholar] [CrossRef] [PubMed]
- Ginis, K.A.M.; Nigg, C.R.; Smith, A.L. Peer-delivered physical activity interventions: An overlooked opportunity for physical activity promotion. Transl. Behav. Med. 2013, 3, 434–443. [Google Scholar] [CrossRef] [PubMed]
- Ommundsen, Y.; Klasson-Heggebø, L.; Anderssen, S.A. Psycho-social and environmental correlates of location-specific physical activity among 9-and 15-year-old Norwegian boys and girls: The European Youth Heart Study. Int. J. Behav. Nutr. Phys. Act. 2006, 3, 32. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Garcia, J.M.; Sirard, J.R.; Deutsch, N.L.; Weltman, A. The influence of friends and psychosocial factors on physical activity and screen time behavior in adolescents: A mixed-methods analysis. J. Behav. Med. 2016, 39, 610–623. [Google Scholar] [CrossRef] [PubMed]
- Sebire, S.J.; Edwards, M.J.; Campbell, R.; Jago, R.; Kipping, R.; Banfield, K.; Tomkinson, K.; Garfield, K.; Lyons, R.A.; Simon, J. Protocol for a feasibility cluster randomised controlled trial of a peer-led school-based intervention to increase the physical activity of adolescent girls (PLAN-A). Pilot Feasibility Stud. 2016, 2, 2. [Google Scholar] [CrossRef] [PubMed]
- Harrington, D.M.; Davies, M.J.; Bodicoat, D.H.; Charles, J.M.; Chudasama, Y.V.; Gorely, T.; Khunti, K.; Plekhanova, T.; Rowlands, A.V.; Sherar, L.B.; et al. Effectiveness of the ‘Girls Active’ school-based physical activity programme: A cluster randomised controlled trial. Int. J. Behav. Nutr. Phys. Act. 2018, 15, 40. [Google Scholar] [CrossRef] [PubMed]
- Brown, H.E.; Whittle, F.; Jong, S.T.; Croxson, C.; Sharp, S.J.; Wilkinson, P.; Wilson, E.C.; van Sluijs, E.M.; Vignoles, A.; Corder, K. A cluster randomised controlled trial to evaluate the effectiveness and cost-effectiveness of the GoActive intervention to increase physical activity among adolescents aged 13–14 years. BMJ Open 2017, 7, e014419. [Google Scholar] [CrossRef] [PubMed]
- Jenkinson, K.A.; Naughton, G.; Benson, A.C. The GLAMA (girls! Lead! Achieve! Mentor! Activate!) physical activity and peer leadership intervention pilot project: A process evaluation using the RE-AIM framework. BMC Public Health 2012, 12, 55. [Google Scholar] [CrossRef] [PubMed]
- Barr-Anderson, D.J.; Laska, M.N.; Veblen-Mortenson, S.; Farbakhsh, K.; Dudovitz, B.; Story, M. A school-based, peer leadership physical activity intervention for 6th graders: Feasibility and results of a pilot study. J. Phys. Act. Health 2012, 9, 492–499. [Google Scholar] [CrossRef] [PubMed]
- Eldridge, S.M.; Chan, C.L.; Campbell, M.J.; Bond, C.M.; Hopewell, S.; Thabane, L.; Lancaster, G.A. CONSORT 2010 statement: Extension to randomised pilot and feasibility trials. Pilot Feasibility Stud. 2016, 2, 64. [Google Scholar] [CrossRef] [PubMed]
- McLennan, D.; Barnes, H.; Noble, M.; Davies, J.; Garratt, E.; Dibben, C. The English Indices of Deprivation 2015; Department for Communities and Local Government: London, UK, 2015.
- Department for Communities and Local Government. The English Indices of Deprivation, 2015. English Indices of Deprivation 2015 Website. Available online: https://www.gov.uk/government/statistics/english-indices-of-deprivation-2015 (accessed on 2 May 2018).
- Patton, M.Q. Qualitative Research; Wiley: Hoboken, NJ, USA, 2005. [Google Scholar]
- Pokorny, S.B.; Jason, L.A.; Schoeny, M.E.; Townsend, S.M.; Curie, C.J. Do participation rates change when active consent procedures replace passive consent. Eval. Rev. 2001, 25, 567–580. [Google Scholar] [CrossRef] [PubMed]
- Spence, S.; White, M.; Adamson, A.J.; Matthews, J.N. Does the use of passive or active consent affect consent or completion rates, or dietary data quality? Repeat cross-sectional survey among school children aged 11–12 years. BMJ Open 2015, 5, e006457. [Google Scholar] [CrossRef] [PubMed]
- Thompson-Haile, A.; Bredin, C.; Leatherdale, S.T. Rationale for Using an Active-Information Passive-Consent Permission Protocol in COMPASS; University of Waterloo: Waterloo, ON, Canada, 2013. [Google Scholar]
- Lawlor, D.A.; Jago, R.; Noble, S.M.; Chittleborough, C.R.; Campbell, R.; Mytton, J.; Howe, L.D.; Peters, T.J.; Kipping, R.R. The Active for Life Year 5 (AFLY5) school based cluster randomised controlled trial: Study protocol for a randomized controlled trial. Trials 2011, 12, 181. [Google Scholar] [CrossRef] [PubMed]
- Bandura, A. Social Foundations of Thought and Action: A Social Cognitive Theory; Prentice Hall: Upper Saddle River, NJ, USA, 1986. [Google Scholar]
- Bandura, A. Self-Efficacy: The Exercise of Control; Macmillan: Basingstoke, UK, 1997. [Google Scholar]
- Bandura, A. Health promotion from the perspective of social cognitive theory. Psychol. Health 1998, 13, 623–649. [Google Scholar] [CrossRef]
- Ryan, R.M.; Deci, E.L. Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. Am. Psychol. 2000, 55, 68. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Richardson, M.; Johnston, M.; Abraham, C.; Francis, J.; Hardeman, W.; Eccles, M.P.; Cane, J.; Wood, C.E. The behavior change technique taxonomy (v1) of 93 hierarchically clustered techniques: Building an international consensus for the reporting of behavior change interventions. Ann. Behav. Med. 2013, 46, 81–95. [Google Scholar] [CrossRef] [PubMed]
- Deci, E.L.; Ryan, R.M. Handbook of Self-Determination Research; University Rochester Press: Rochester, NY, USA, 2002. [Google Scholar]
- Corder, K.; Schiff, A.; Kesten, J.M.; van Sluijs, E.M.F. Development of a universal approach to increase physical activity among adolescents: The GoActive intervention. BMJ Open 2015, 5, e008610. [Google Scholar] [CrossRef] [PubMed]
- Lohman, T.; Roache, A.; Martorell, R. Anthropometric standardization reference manual. Med. Sci. Sports Exerc. 1992, 24, 952. [Google Scholar] [CrossRef]
- Cole, T.J.; Bellizzi, M.C.; Flegal, K.M.; Dietz, W.H. Establishing a standard definition for child overweight and obesity worldwide: International survey. BMJ 2000, 320, 1240. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Clinical Excellence (NICE). Obesity: Identification, Assessment and Management of Overweight and Obesity in Children, Young People and Adults: Partial update of CG43; Department of Health: London, UK, 2014.
- Moore, S.A.; McKay, H.A.; Macdonald, H.; Nettlefold, L.; Baxter-Jones, A.; Cameron, N.; Brasher, P. Enhancing a somatic maturity prediction model. Med. Sci. Sports Exerc. 2015, 47, 1755–1764. [Google Scholar] [CrossRef] [PubMed]
- Mehta, S.K. Waist circumference to height ratio in children and adolescents. Clin. Pediatr. 2015, 54, 652–658. [Google Scholar] [CrossRef] [PubMed]
- Browning, L.M.; Hsieh, S.D.; Ashwell, M. A systematic review of waist-to-height ratio as a screening tool for the prediction of cardiovascular disease and diabetes: 0·5 could be a suitable global boundary value. Nutr. Res. Rev. 2010, 23, 247–269. [Google Scholar] [CrossRef] [PubMed]
- Jago, R.; Sebire, S.J.; Cooper, A.R.; Haase, A.M.; Powell, J.; Davis, L.; McNeill, J.; Montgomery, A.A. Bristol girls dance project feasibility trial: Outcome and process evaluation results. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 83. [Google Scholar] [CrossRef] [PubMed]
- Ekblom, O.; Nyberg, G.; Bak, E.E.; Ekelund, U.; Marcus, C. Validity and comparability of a wrist-worn accelerometer in children. J. Phys. Act. Health 2012, 9, 389–393. [Google Scholar] [CrossRef] [PubMed]
- Fairclough, S.; Noonan, R.; Rowlands, A.; Van Hees, V.; Knowles, Z.; Boddy, L. Wear compliance and activity in children wearing wrist and hip mounted accelerometers. Med. Sci. Sports Exerc. 2016, 48, 245–253. [Google Scholar] [CrossRef] [PubMed]
- Scott, J.; Rowlands, A.; Cliff, D.; Morgan, P.; Plotnikoff, R.; Lubans, D. Comparability and feasibility of wrist- and hip-worn accelerometers in free-living adolescents. J. Sci. Med. Sport 2017, 20, 1101–1106. [Google Scholar] [CrossRef] [PubMed]
- Crouter, S.E.; Flynn, J.I.; Bassett, D.R., Jr. Estimating physical activity in youth using a wrist accelerometer. Med. Sci. Sports Exerc. 2015, 47, 944. [Google Scholar] [CrossRef] [PubMed]
- Trost, S.G.; Pate, R.R.; Freedson, P.S.; Sallis, J.F.; Taylor, W.C. Using objective physical activity measures with youth: How many days of monitoring are needed? Med. Sci. Sports Exerc. 2000, 32, 426. [Google Scholar] [CrossRef] [PubMed]
- Van Hees, V.T.; Gorzelniak, L.; Leon, E.C.D.; Eder, M.; Pias, M.; Taherian, S.; Ekelund, U.; Renström, F.; Franks, P.W.; Horsch, A. Separating movement and gravity components in an acceleration signal and implications for the assessment of human daily physical activity. PLoS ONE 2013, 8, e61691. [Google Scholar] [CrossRef] [PubMed]
- Van Hees, V.T.; Fang, Z.; Langford, J.; Assah, F.; Mohammad, A.; da Silva, I.C.; Trenell, M.I.; White, T.; Wareham, N.J.; Brage, S. Autocalibration of accelerometer data for free-living physical activity assessment using local gravity and temperature: An evaluation on four continents. J. Appl. Physiol. 2014, 117, 738–744. [Google Scholar] [CrossRef] [PubMed]
- Noonan, R.J.; Boddy, L.M.; Kim, Y.; Knowles, Z.R.; Fairclough, S.J. Comparison of children’s free-living physical activity derived from wrist and hip raw accelerations during the segmented week. J. Sports Sci. 2017, 35, 2067–2072. [Google Scholar] [CrossRef] [PubMed]
- Rowlands, A.V.; Cliff, D.P.; Fairclough, S.J.; Boddy, L.M.; Olds, T.S.; Parfitt, G.; Noonan, R.J.; Downs, S.J.; Knowles, Z.R.; Beets, M.W. Moving forward with backward compatibility: Translating wrist accelerometer data. Med. Sci. Sports Exerc. 2016, 48, 2142–2149. [Google Scholar] [CrossRef] [PubMed]
- Taylor, S.L.; Curry, W.B.; Knowles, Z.R.; Noonan, R.J.; McGrane, B.; Fairclough, S.J. Predictors of Segmented School Day Physical Activity and Sedentary Time in Children from a Northwest England Low-Income Community. Int. J. Environ. Res. Public Health 2017, 14, 534. [Google Scholar] [CrossRef] [PubMed]
- Sabia, S.; van Hees, V.T.; Shipley, M.J.; Trenell, M.I.; Hagger-Johnson, G.; Elbaz, A.; Kivimaki, M.; Singh-Manoux, A. Association between questionnaire-and accelerometer-assessed physical activity: The role of sociodemographic factors. Am. J. Epidemiol. 2014, 179, 781–790. [Google Scholar] [CrossRef] [PubMed]
- Nettlefold, L.; McKay, H.; Warburton, D.; McGuire, K.; Bredin, S.; Naylor, P. The challenge of low physical activity during the school day: At recess, lunch and in physical education. Br. J. Sports Med. 2011, 45, 813–819. [Google Scholar] [CrossRef] [PubMed]
- Mooses, K.; Pihu, M.; Riso, E.M.; Hannus, A.; Kaasik, P.; Kull, M. Physical education increases daily moderate to vigorous physical activity and reduces sedentary time. J. School Health 2017, 87, 602–607. [Google Scholar] [CrossRef] [PubMed]
- Hollis, J.; Sutherland, R.; Campbell, L.; Morgan, P.; Lubans, D.; Nathan, N.; Wolfenden, L.; Okely, A.; Davies, L.; Williams, A. Effects of a ‘school-based’physical activity intervention on adiposity in adolescents from economically disadvantaged communities: Secondary outcomes of the ‘Physical Activity 4 Everyone’RCT. Int. J. Obes. 2016, 40, 1486. [Google Scholar] [CrossRef] [PubMed]
- Rich, C.; Geraci, M.; Griffiths, L.; Sera, F.; Dezateux, C.; Cortina-Borja, M. Quality control methods in accelerometer data processing: Defining minimum wear time. PLoS ONE 2013, 8, e67206. [Google Scholar] [CrossRef] [PubMed]
- Hildebrand, M.; van Hees, V.T.; Hansen, B.H.; Ekelund, U. Age group comparability of raw accelerometer output from wrist-and hip-worn monitors. Med. Sci. Sports Exerc. 2014, 46, 1816–1824. [Google Scholar] [CrossRef] [PubMed]
- Hildebrand, M.; Hansen, B.H.; van Hees, V.T.; Ekelund, U. Evaluation of raw acceleration sedentary thresholds in children and adults. Scand. J. Med. Sci. Sports 2017, 27, 1814–1823. [Google Scholar] [CrossRef] [PubMed]
- Kendzierski, D.; DeCarlo, K.J. Physical activity enjoyment scale: Two validation studies. J. Sport Exerc. Psychol. 1991, 13, 50–64. [Google Scholar] [CrossRef]
- Motl, R.W.; Dishman, R.K.; Saunders, R.; Dowda, M.; Felton, G.; Pate, R.R. Measuring enjoyment of physical activity in adolescent girls. Am. J. Prev. Med. 2001, 21, 110–117. [Google Scholar] [CrossRef]
- Tennant, R.; Hiller, L.; Fishwick, R.; Platt, S.; Joseph, S.; Weich, S.; Parkinson, J.; Secker, J.; Stewart-Brown, S. The Warwick-Edinburgh mental well-being scale (WEMWBS): Development and UK validation. Health Qual. Life Outcomes 2007, 5, 63. [Google Scholar] [CrossRef] [PubMed]
- Sallis, J.F.; Grossman, R.M.; Pinski, R.B.; Patterson, T.L.; Nader, P.R. The development of scales to measure social support for diet and exercise behaviors. Prev. Med. 1987, 16, 825–836. [Google Scholar] [CrossRef]
- Motl, R.W.; Dishman, R.K.; Trost, S.G.; Saunders, R.P.; Dowda, M.; Felton, G.; Ward, D.S.; Pate, R.R. Factorial validity and invariance of questionnaires measuring social-cognitive determinants of physical activity among adolescent girls. Prev. Med. 2000, 31, 584–594. [Google Scholar] [CrossRef] [PubMed]
- Ward, D.S.; Saunders, R.P.; Pate, R.R. Physical Activity Interventions in Children and Adolescents; New World Library: Novato, CA, USA, 2007. [Google Scholar]
- Liang, Y.; Lau, P.W.; Huang, W.Y.; Maddison, R.; Baranowski, T. Validity and reliability of questionnaires measuring physical activity self-efficacy, enjoyment, social support among Hong Kong Chinese children. Prev. Med. Rep. 2014, 1, 48–52. [Google Scholar] [CrossRef] [PubMed]
- Clarke, A.; Friede, T.; Putz, R.; Ashdown, J.; Martin, S.; Blake, A.; Adi, Y.; Parkinson, J.; Flynn, P.; Platt, S. Warwick-Edinburgh Mental Well-being Scale (WEMWBS): Validated for teenage school students in England and Scotland. A mixed methods assessment. BMC Public Health 2011, 11, 487. [Google Scholar] [CrossRef] [PubMed]
- Hsu, Y.-W.; Chou, C.-P.; Nguyen-Rodriguez, S.T.; McClain, A.D.; Belcher, B.R.; Spruijt-Metz, D. Influences of social support, perceived barriers, and negative meanings of physical activity on physical activity in middle school students. J. Phys. Act. Health 2011, 8, 210–219. [Google Scholar] [CrossRef] [PubMed]
- Corder, K.; Atkin, A.J.; Ekelund, U.; van Sluijs, E.M. What do adolescents want in order to become more active? BMC Public Health 2013, 13, 718. [Google Scholar] [CrossRef] [PubMed]
- National Health Service (NHS). National Child Measurement Programme; NHS: London, UK, 2018. [Google Scholar]
- Sebire, S.; Edwards, M.; Kesten, J.; May, T.; Banfield, K.; Bird, E.; Tomkinson, K.; Blair, P.; Powell, J.; Jago, R. Process evaluation of the Bristol girls dance project. BMC Public Health 2016, 16, 349. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, F.; Gray, S.; Inchley, J. ‘This choice thing really works…’ Changes in experiences and engagement of adolescent girls in physical education classes, during a school-based physical activity programme. Phys. Educ. Sport Pedagog. 2015, 20, 593–611. [Google Scholar] [CrossRef]
- Mitchell, F.; Inchley, J.; Fleming, J.; Currie, C. A socio-ecological approach to understanding adolescent girls’ engagement and experiences in the PE environment: A case study design. Grad. J. Sport Exerc. Phys. Educ. Res. 2015, 3, 44–62. [Google Scholar]
- Fairclough, S.J.; McGrane, B.; Sanders, G.; Taylor, S.; Owen, M.; Curry, W. A non-equivalent group pilot trial of a school-based physical activity and fitness intervention for 10–11 year old english children: Born to move. BMC Public Health 2016, 16, 861. [Google Scholar] [CrossRef] [PubMed]
- Jago, R.; Edwards, M.J.; Sebire, S.J.; Tomkinson, K.; Bird, E.L.; Banfield, K.; May, T.; Kesten, J.M.; Cooper, A.R.; Powell, J.E. Effect and cost of an after-school dance programme on the physical activity of 11–12 year old girls: The Bristol Girls Dance Project, a school-based cluster randomised controlled trial. Int. J. Behav. Nutr. Phys. Act. 2015, 12, 128. [Google Scholar] [CrossRef] [PubMed]
- Naylor, P.-J.; Nettlefold, L.; Race, D.; Hoy, C.; Ashe, M.C.; Higgins, J.W.; McKay, H.A. Implementation of school based physical activity interventions: A systematic review. Prev. Med. 2015, 72, 95–115. [Google Scholar] [CrossRef] [PubMed]
- Carroll, C.; Patterson, M.; Wood, S.; Booth, A.; Rick, J.; Balain, S. A conceptual framework for implementation fidelity. Implement. Sci. 2007, 2, 40. [Google Scholar] [CrossRef] [PubMed]
- Dishman, R.K.; Motl, R.W.; Saunders, R.; Felton, G.; Ward, D.S.; Dowda, M.; Pate, R.R. Enjoyment Mediates effects of a school-based physical-activity intervention. Med. Sci. Sports Exerc. 2005, 37, 478–487. [Google Scholar] [CrossRef] [PubMed]
- Brooks, F.; Magnusson, J. Physical activity as leisure: The meaning of physical activity for the health and well-being of adolescent women. Health Care Women Int. 2007, 28, 69–87. [Google Scholar] [CrossRef] [PubMed]
- Gebremariam, M.K.; Bergh, I.H.; Andersen, L.F.; Ommundsen, Y.; Bjelland, M.; Lien, N. Stability and change in potential correlates of physical activity and association with pubertal status among Norwegian children in the transition between childhood and adolescence. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 56. [Google Scholar] [CrossRef] [PubMed]
- Best, K.; Ball, K.; Zarnowiecki, D.; Stanley, R.; Dollman, J. In search of consistent predictors of children’s physical activity. Int. J. Environ. Res. Public Health 2017, 14, 1258. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, P.J.; Carraça, E.V.; Markland, D.; Silva, M.N.; Ryan, R.M. Exercise, physical activity, and self-determination theory: A systematic review. Int. J. Behav. Nutr. Phys. Act. 2012, 9, 78. [Google Scholar] [CrossRef] [PubMed]
- Craig, P.; Dieppe, P.; Macintyre, S.; Michie, S.; Nazareth, I.; Petticrew, M. Developing and evaluating complex interventions: The new Medical Research Council guidance. BMJ 2008, 337, a1655. [Google Scholar] [CrossRef] [PubMed]
- Moore, G.F.; Audrey, S.; Barker, M.; Bond, L.; Bonell, C.; Hardeman, W.; Moore, L.; O’Cathain, A.; Tinati, T.; Wight, D. Process evaluation of complex interventions: Medical Research Council guidance. BMJ 2015, 350, h1258. [Google Scholar] [CrossRef] [PubMed]
- Carson, R.L.; Castelli, D.M.; Beighle, A.; Erwin, H. School-based physical activity promotion: A conceptual framework for research and practice. Child. Obes. 2014, 10, 100–106. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. Physical Activity and Health; CDC: Atlanta, GA, USA, 2015.
- McMullen, J.; Ní Chróinín, D.; Tammelin, T.; Pogorzelska, M.; van der Mars, H. International approaches to whole-of-school physical activity promotion. Quest 2015, 67, 384–399. [Google Scholar] [CrossRef]
- Freedson, P.; Bowles, H.R.; Troiano, R.; Haskell, W. Assessment of physical activity using wearable monitors: Recommendations for monitor calibration and use in the field. Med. Sci. Sports Exerc. 2012, 44 (Suppl. 1), S1–S4. [Google Scholar] [CrossRef] [PubMed]
- Peach, D.; Van Hoomissen, J.; Callender, H.L. Exploring the ActiLife® filtration algorithm: Converting raw acceleration data to counts. Physiol. Meas. 2014, 35, 2359–2367. [Google Scholar] [CrossRef] [PubMed]
- Hunter, R.F.; McAneney, H.; Davis, M.; Tully, M.A.; Valente, T.W.; Kee, F. “Hidden” social networks in behavior change interventions. Am. J. Public Health 2015, 105, 513–516. [Google Scholar] [CrossRef] [PubMed]

| Week | Location | Activity |
|---|---|---|
| 1 | University | Introduction & Leadership & PA |
| 2 | School | PA & Motivation |
| 3 | School | PA & Goal setting |
| 4 | School | PA & How to increase activity |
| 5 | School | PA & How to support others |
| 6 | School | Support session |
| 7 | School | Support session |
| School | Number of Girls in Year Group | Opted Out (n, (%)) | Provided Accelerometer Data (n, (%)) | Weekly ASC Attendance (Mean, (%)) | |
|---|---|---|---|---|---|
| Baseline * | Post-INT * | ||||
| 1. Class | 102 | 9 (8.8) | 82 (88.2) | 70 (75.3) | 14 (47) |
| 2. Choice | 76 | 3 (3.9) | 64 (87.7) | 42 (57.5) | 12 (40) |
| 3. No Club | 71 | 3 (4.2) | 60 (88.2) | 45 (66.2) | N/A |
| Total | 249 | 15 (6.0) | 206 (88.0) | 157 (66.3) | N/A |
| 1. Class (n = 93) | 2. Choice (n = 73) | 3. No Club (n = 68) | All Girls (n = 234) | |
|---|---|---|---|---|
| Age (y) | 14.0 (0.3) | 14.0 (0.3) | 14.1 (0.3) | 14.0 (0.3) |
| Stature (cm) | 160.7 (5.8) | 160.4 (5.7) | 161.7 (9.5) | 160.9 (6.9) |
| Body Mass (kg) | 56.8 (10.2) | 55.4 (8.8) | 57.8 (12.1) | 56.7 (10.5) |
| BMI (kg∙m2) | 22.4 (5.9) | 21.7 (3.2) | 22.4 (6.6) | 22.2 (5.6) |
| BMI z-Score | 0.7 (1.0) | 0.7 (0.9) | 0.6 (1.4) | 0.7 (1.1) |
| WHtR | 0.46 (0.04) | 0.44 (0.04) | 0.46 (0.07) | 0.45 (0.05) |
| Maturity Offset (y) | 1.8 (0.4) | 1.8 (0.4) | 1.9 (0.6) | 1.8 (0.5) |
| Weight Status (%) | ||||
| Underweight | 2.2 | 5.5 | 9.2 | 5.2 |
| Normal Weight | 70.0 | 67.3 | 61.6 | 66.7 |
| Overweight/Obese | 27.8 | 27.3 | 29.2 | 28.1 |
| IMD Score | 6.6 (2.6) | 5.7 (3.0) | 6.8 (2.0) | 6.4 (2.6) |
| MVPA (min·day−1) | 23.3 (11.9) | 26.4 (13.3) | 32.2 (12.9) | 26.9 (13.1) |
| MVPA Guidelines (%) | 0 | 3.1 | 3.3 | 1.9 |
| School | Time | ST (Minutes) | Adjusted Difference in Means (95% CI) | MVPA (Minutes) | Adjusted Difference in Means (95% CI) | ||
|---|---|---|---|---|---|---|---|
| Mean | SE | Mean | SE | ||||
| 1. Class | Baseline | 728.0 | 0.0 | −1.6 (−10.0 to 7.5) | 28.7 | 0.0 | 3.2 * (0.8 to 5.7) |
| Post-INT | 726.4 | 4.5 | 31.9 | 1.15 | |||
| 2. Choice | Baseline | 728.0 | 0.0 | 12.9 (2.0 to 20.3) | 28.7 | 0.0 | 1.0 (−1.9 to 2.7) |
| Post-INT | 740.9 | 6.5 | 29.7 | 1.6 | |||
| 3. No Club | Baseline | 728.0 | 0.0 | 17.2 * (4.8 to 26.5) | 28.7 | 0.0 | −3.5 * (−5.8 to −0.5) |
| Post-INT | 745.8 | 5.7 | 25.2 | 1.4 | |||
| School | Time | ST (Minutes) | Adjusted Difference in Means (95% CI) | MVPA (Minutes) | Adjusted Difference in Means (95% CI) | ||
|---|---|---|---|---|---|---|---|
| Mean | SE | Mean | SE | ||||
| 1. Class | Baseline | 281.3 | 0.0 | −4.9 (−8.2 to −0.6) | 10.6 | 0.0 | 1.2 * (0.5 to 2.5) |
| Post-INT | 276.4 | 2.0 | 11.8 | 0.6 | |||
| 2. Choice | Baseline | 281.3 | 0.0 | −3.4 (−9.8 to 0.3) | 10.6 | 0.0 | 1.9 (0.2 to 3.0) |
| Post-INT | 277.9 | 2.9 | 12.5 | 0.8 | |||
| 3. No Club | Baseline | 281.3 | 0.0 | 14.0 ** (9.5 to 18.8) | 10.6 | 0.0 | −2.7 ** (−4.6 to −2.1) |
| Post-INT | 295.3 | 2.6 | 7.9 | 0.7 | |||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Owen, M.B.; Kerner, C.; Taylor, S.L.; Noonan, R.J.; Newson, L.; Kosteli, M.-C.; Curry, W.B.; Fairclough, S.J. The Feasibility of a Novel School Peer-Led Mentoring Model to Improve the Physical Activity Levels and Sedentary Time of Adolescent Girls: The Girls Peer Activity (G-PACT) Project. Children 2018, 5, 67. https://doi.org/10.3390/children5060067
Owen MB, Kerner C, Taylor SL, Noonan RJ, Newson L, Kosteli M-C, Curry WB, Fairclough SJ. The Feasibility of a Novel School Peer-Led Mentoring Model to Improve the Physical Activity Levels and Sedentary Time of Adolescent Girls: The Girls Peer Activity (G-PACT) Project. Children. 2018; 5(6):67. https://doi.org/10.3390/children5060067
Chicago/Turabian StyleOwen, Michael B., Charlotte Kerner, Sarah L. Taylor, Robert J. Noonan, Lisa Newson, Maria-Christina Kosteli, Whitney B. Curry, and Stuart J. Fairclough. 2018. "The Feasibility of a Novel School Peer-Led Mentoring Model to Improve the Physical Activity Levels and Sedentary Time of Adolescent Girls: The Girls Peer Activity (G-PACT) Project" Children 5, no. 6: 67. https://doi.org/10.3390/children5060067
APA StyleOwen, M. B., Kerner, C., Taylor, S. L., Noonan, R. J., Newson, L., Kosteli, M.-C., Curry, W. B., & Fairclough, S. J. (2018). The Feasibility of a Novel School Peer-Led Mentoring Model to Improve the Physical Activity Levels and Sedentary Time of Adolescent Girls: The Girls Peer Activity (G-PACT) Project. Children, 5(6), 67. https://doi.org/10.3390/children5060067






