Activity Classification Feasibility Using Wearables: Considerations for Hip Fracture
Abstract
1. Introduction
- The transitions, like lying to sitting and sitting to standing.
- The ambulatory activities, like climbing the stairs and walking with walking aids.
- Minimizing impairments, like walking with weights, exercycle, and stretching routines.
- Stationary exercise while lying on the back and stomach.
- Stationary exercise while sitting, i.e., straightening the knee from 90-degree flexion to fully extended and then returning to flexed.
- Stationary exercise while standing, like lifting the thigh upwards in front of the body, swinging a leg side to side, stepping up, and squats.
- Exercycle, i.e., time spent cycling on a stationary bike.
2. Wearable Data Collection and Analysis Method
2.1. Wearable Activity Sensing Device System Used
2.2. Activity Data Collection Process
2.3. Activity Data Processing Model
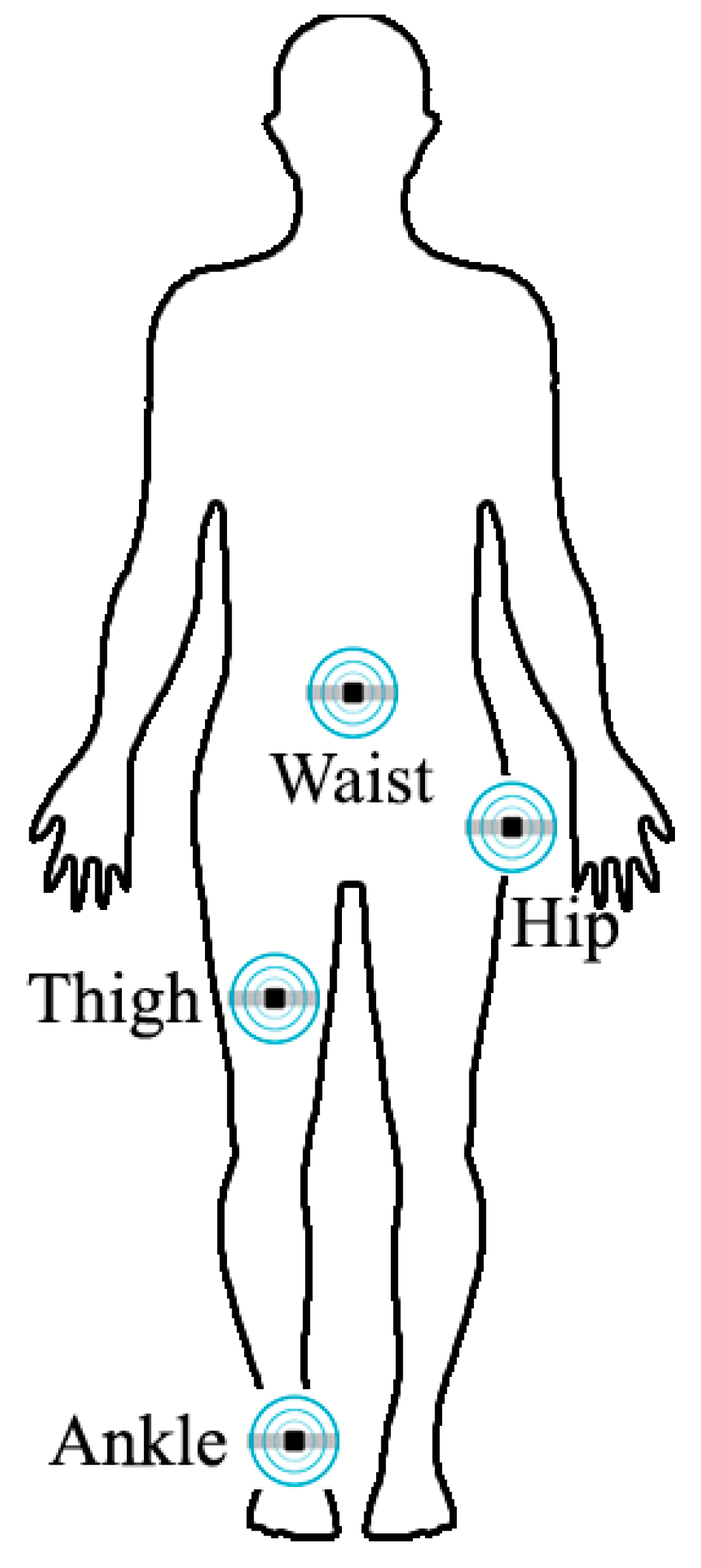
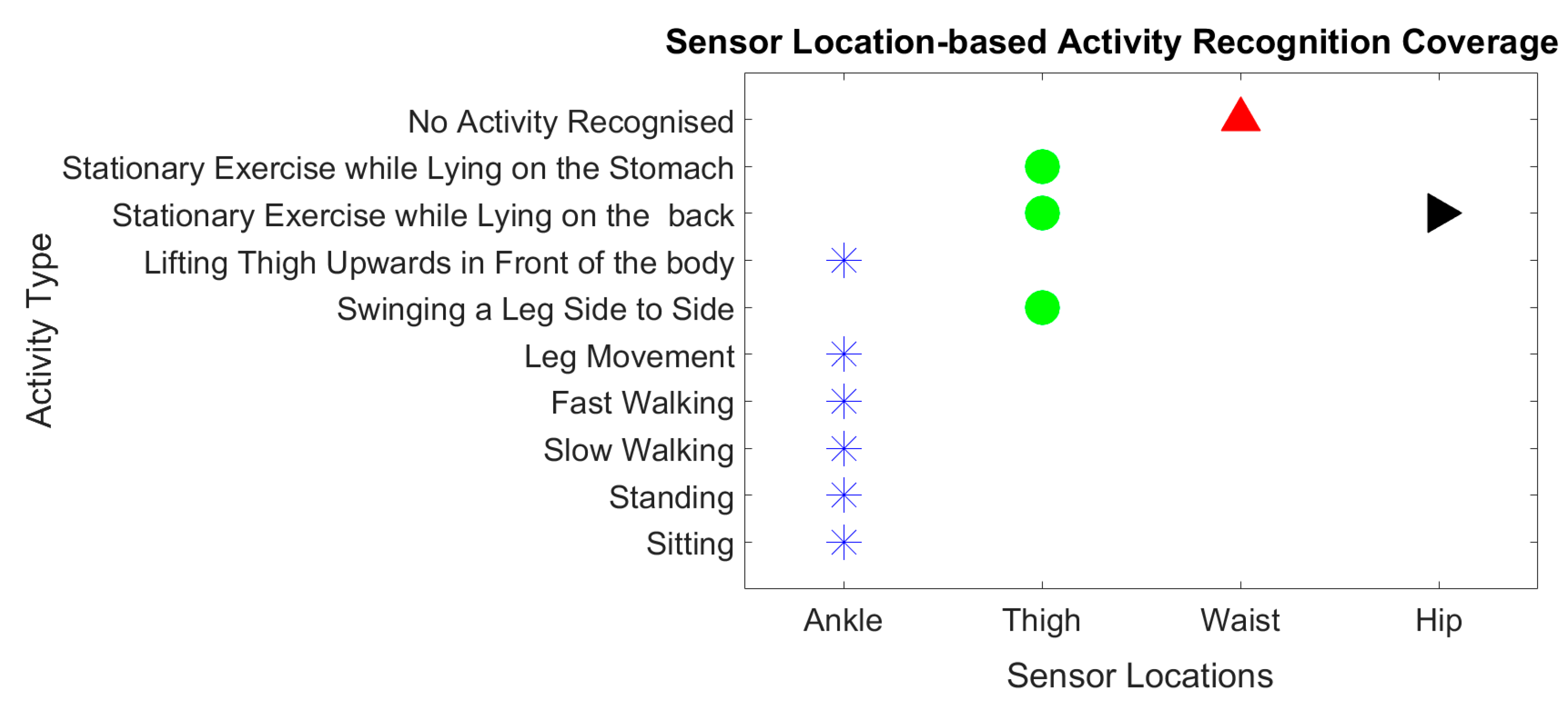
2.4. Considerations for the Body-Worn Sensor
3. Results
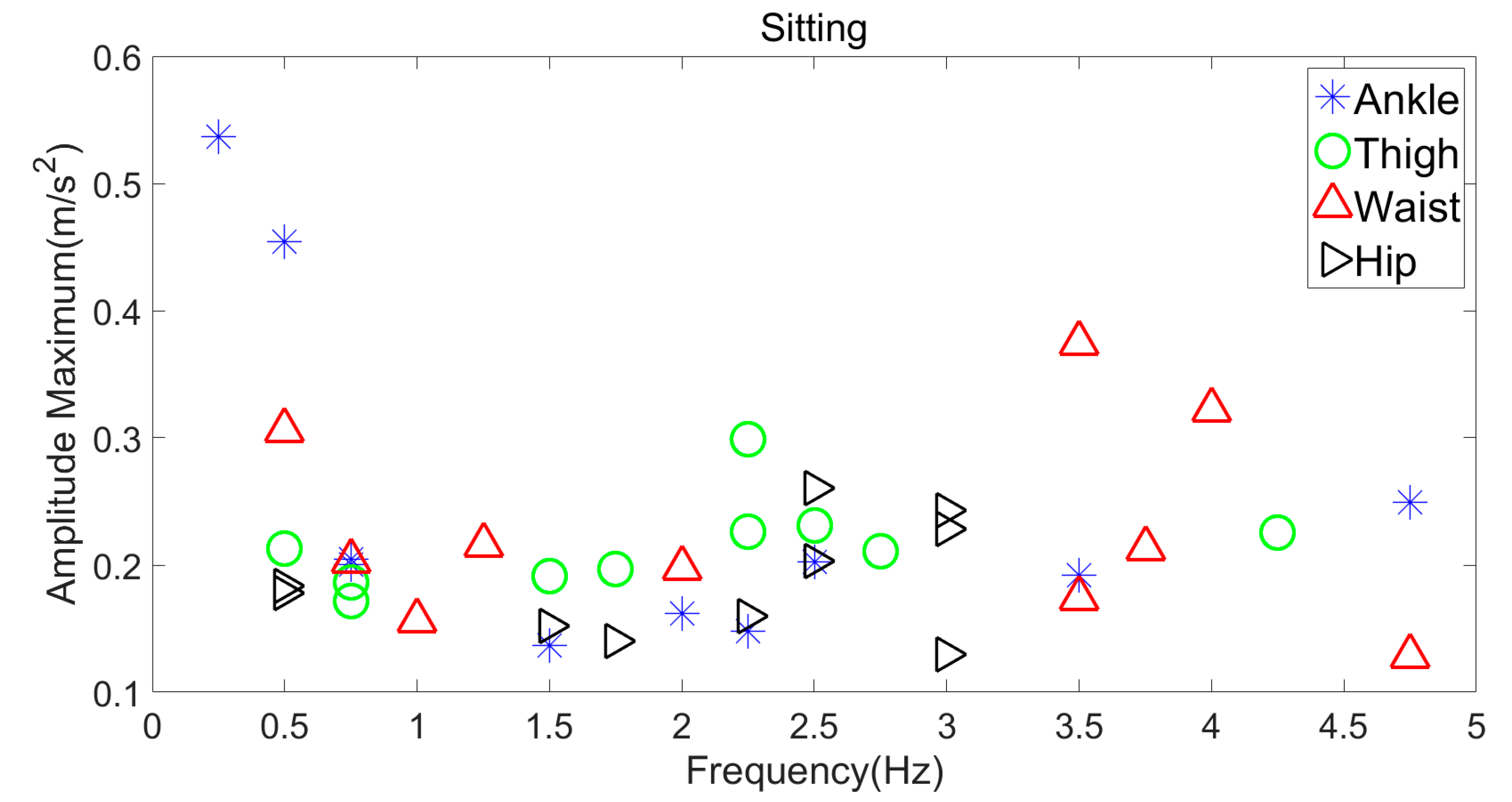
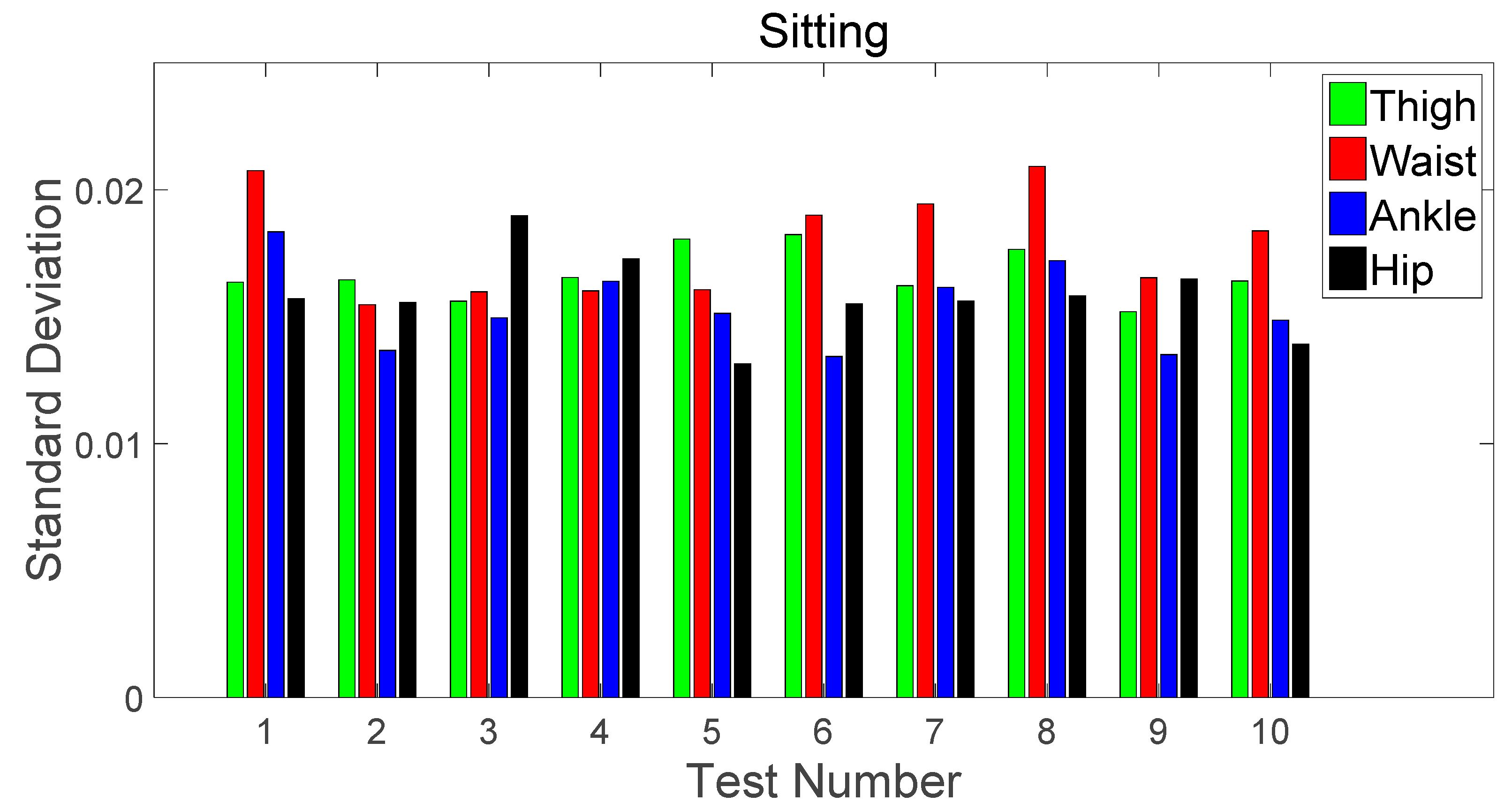
3.1. Static Activities
Sitting vs. Standing
3.2. Ambulatory Activities
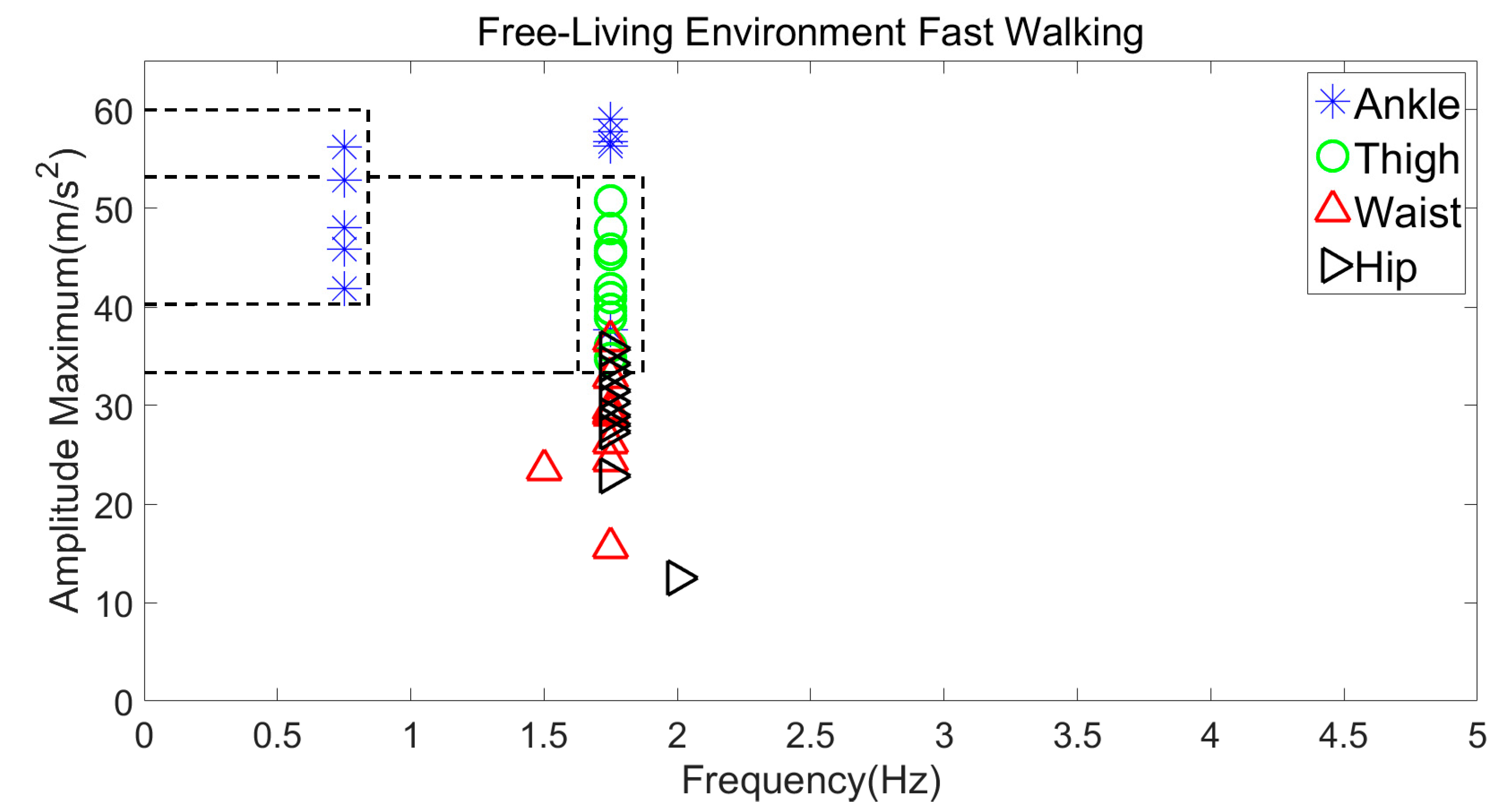
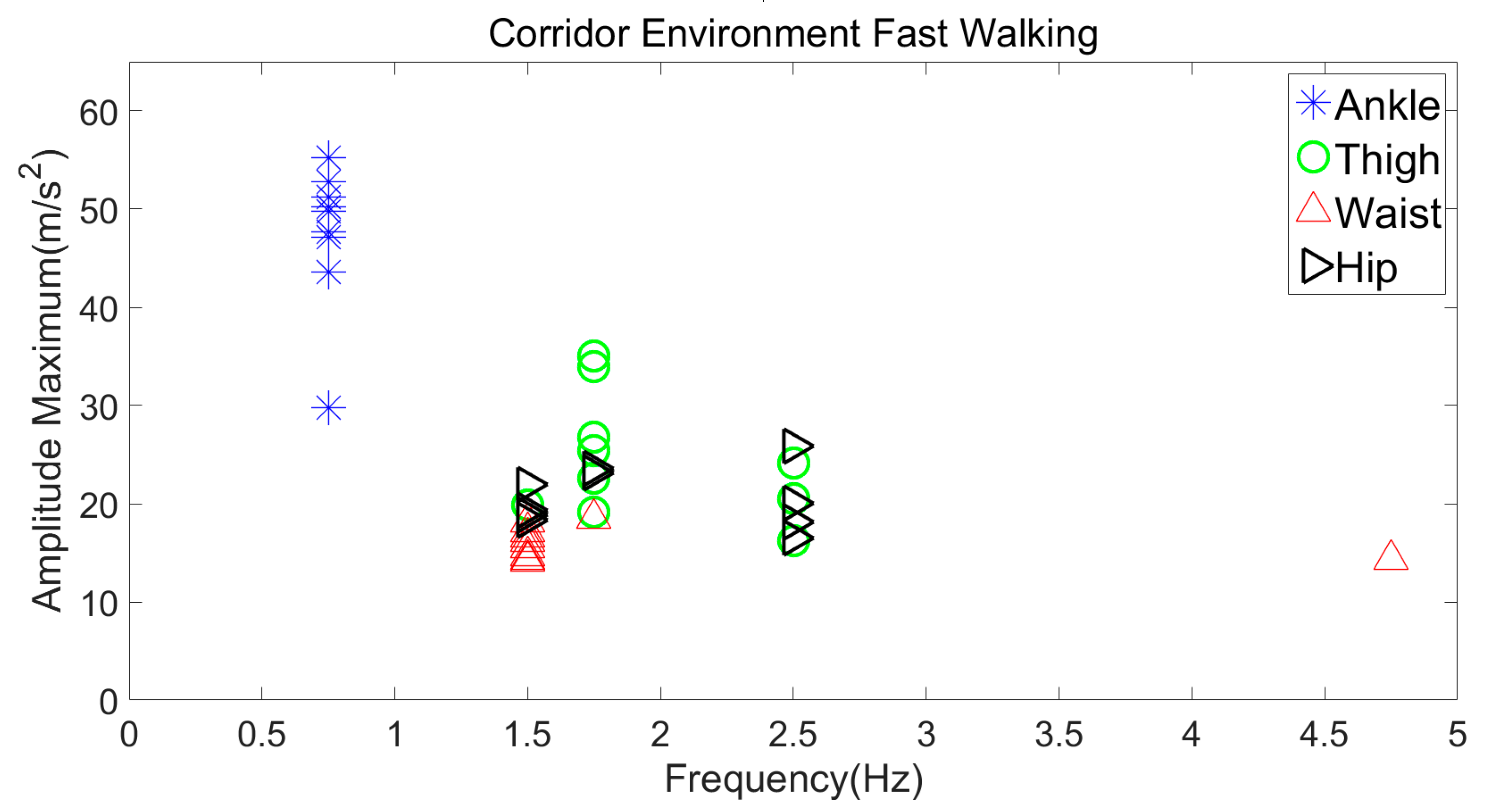
3.2.1. Fast Walking in a Free-Living Environment versus a Corridor Environment
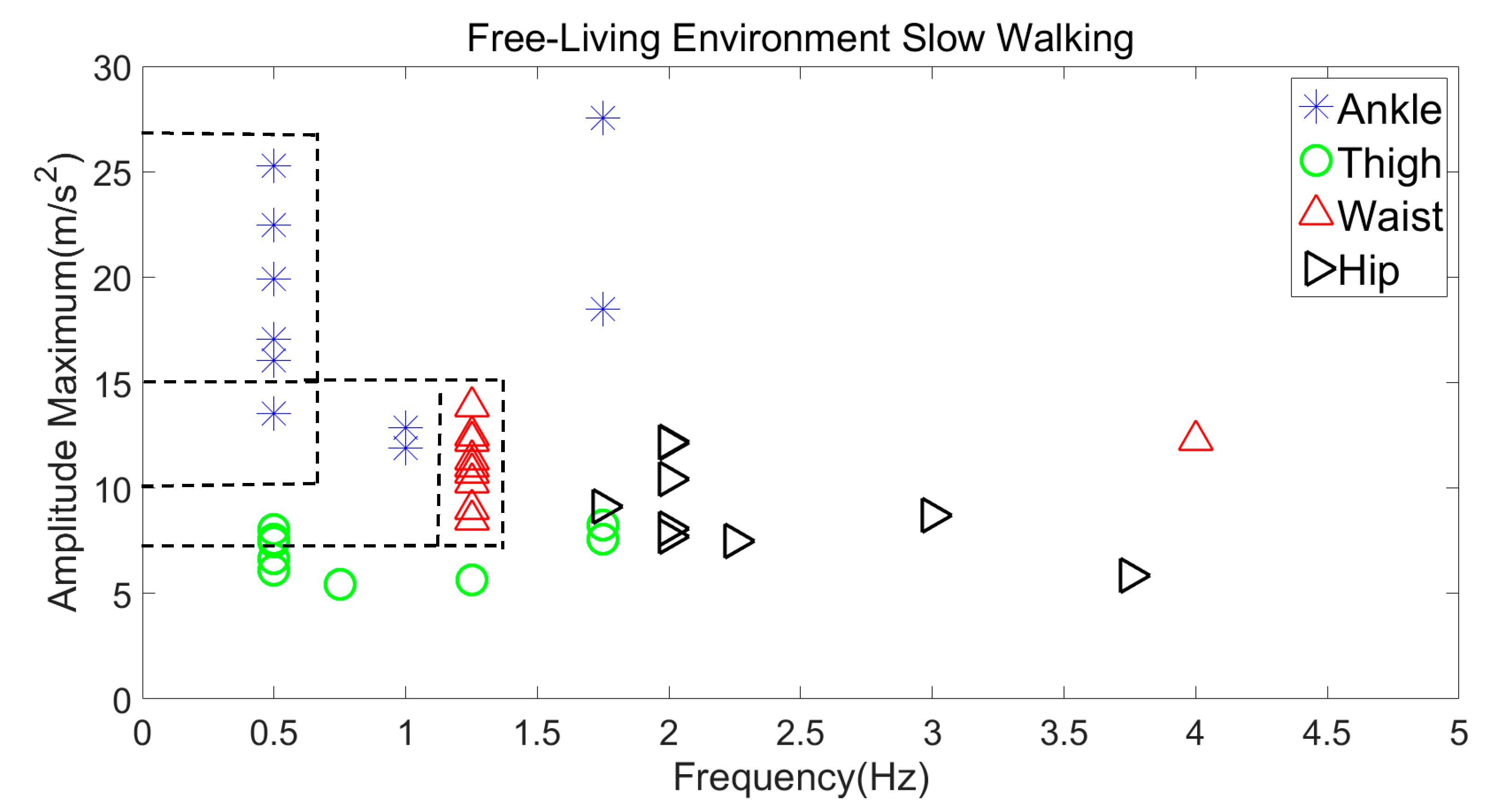
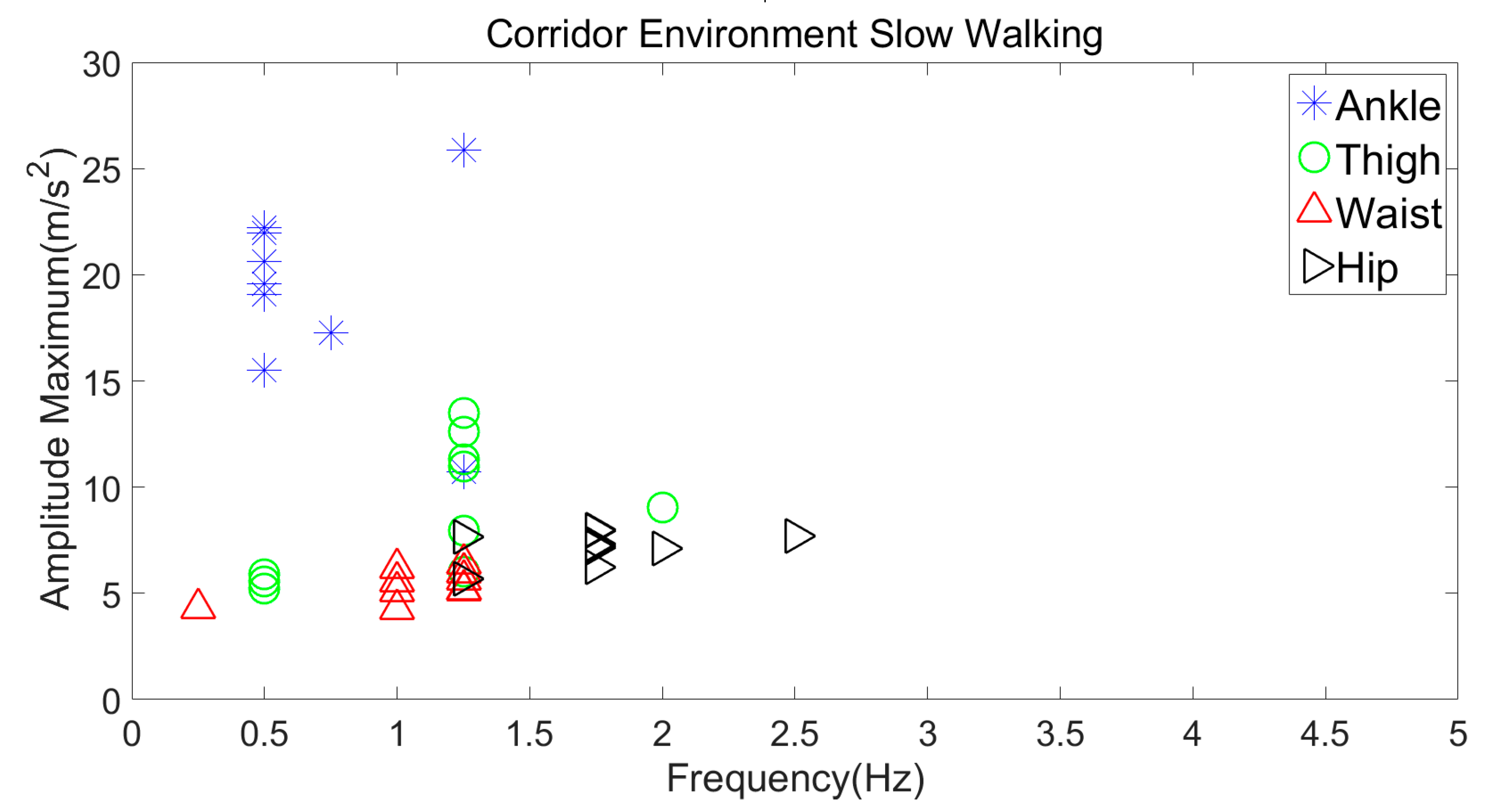
3.2.2. Slow Walking in a Free-Living Environment vs. Corridor Environment
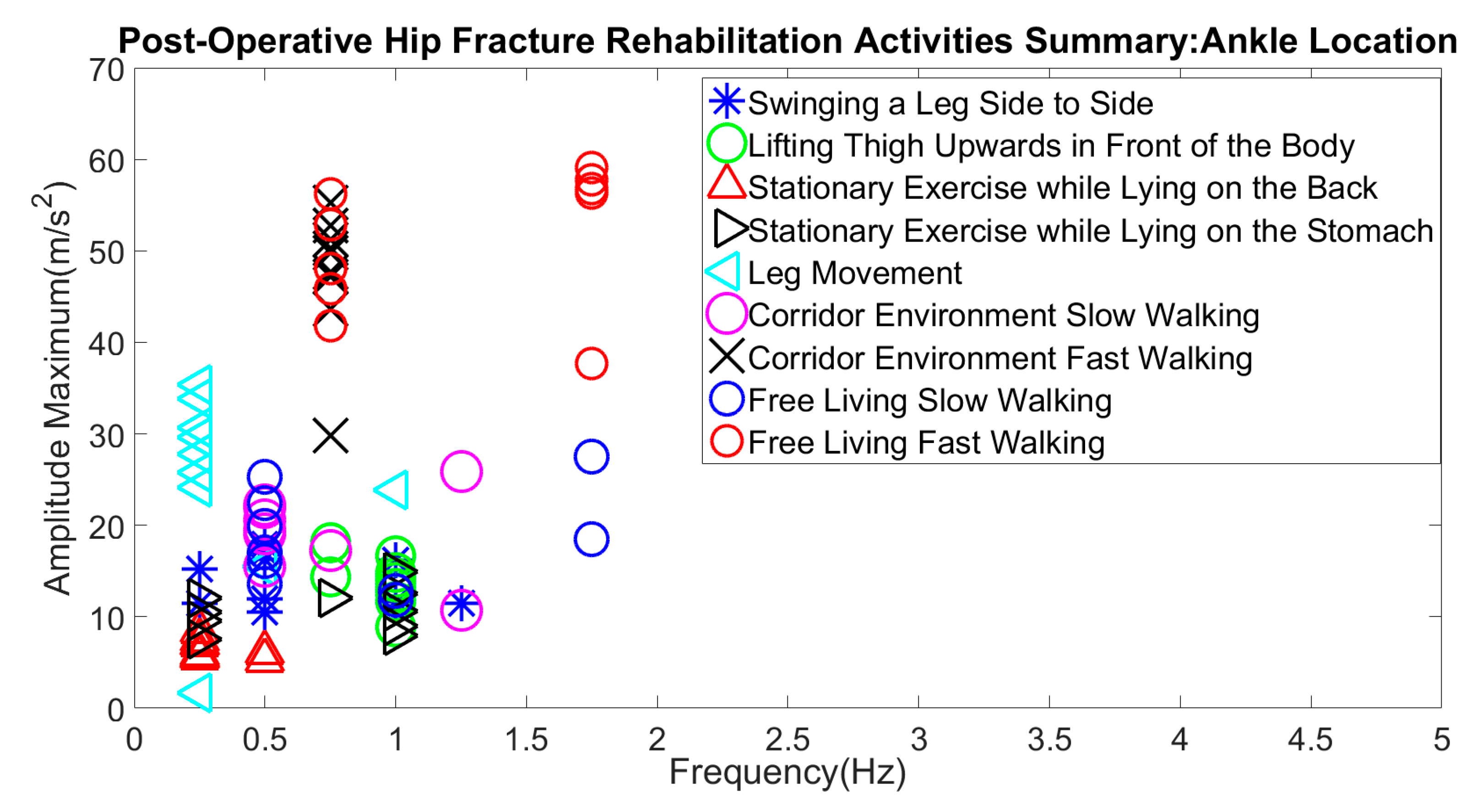
3.3. Hip Fracture Activities
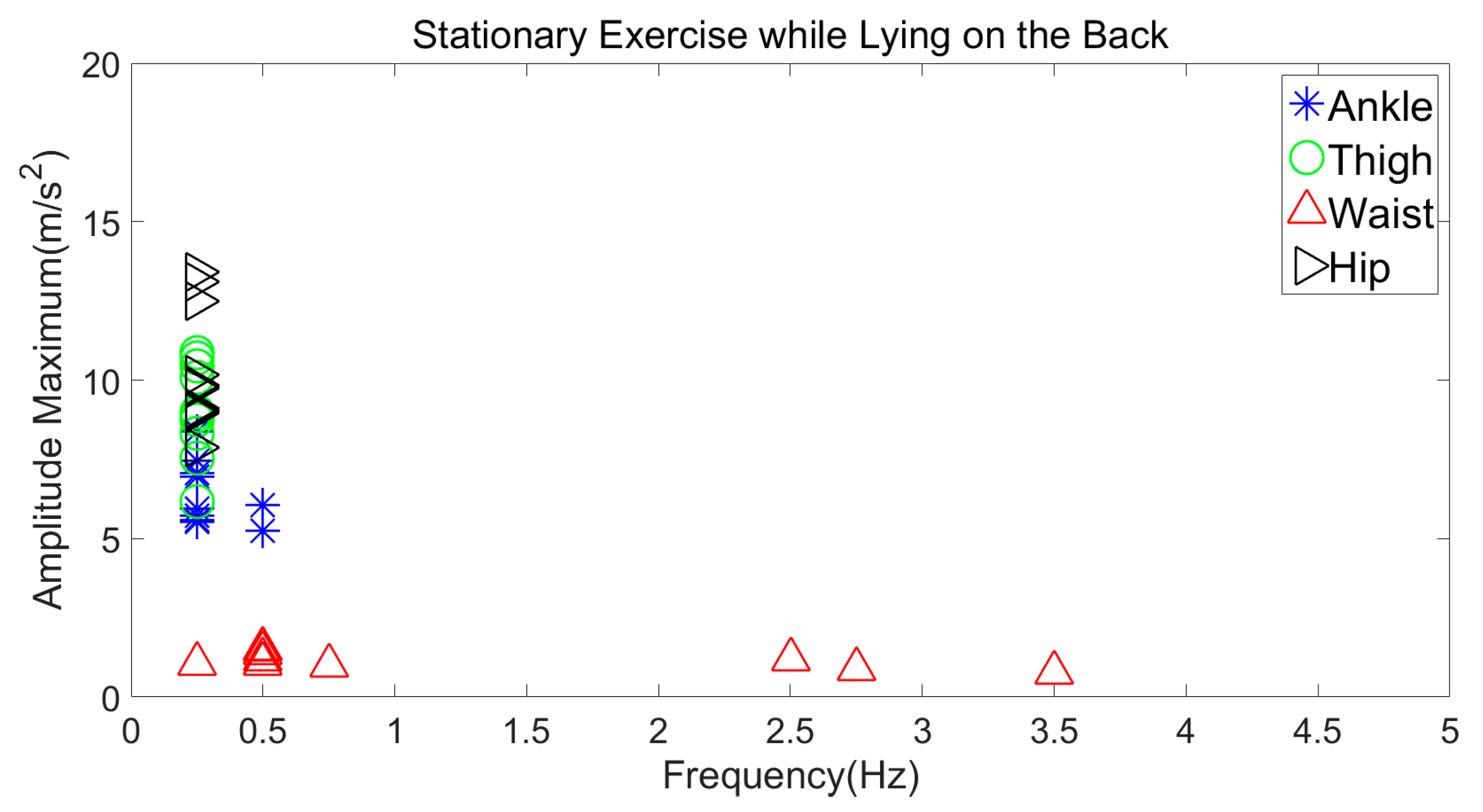
3.3.1. Stationary Exercise while Lying on the Back
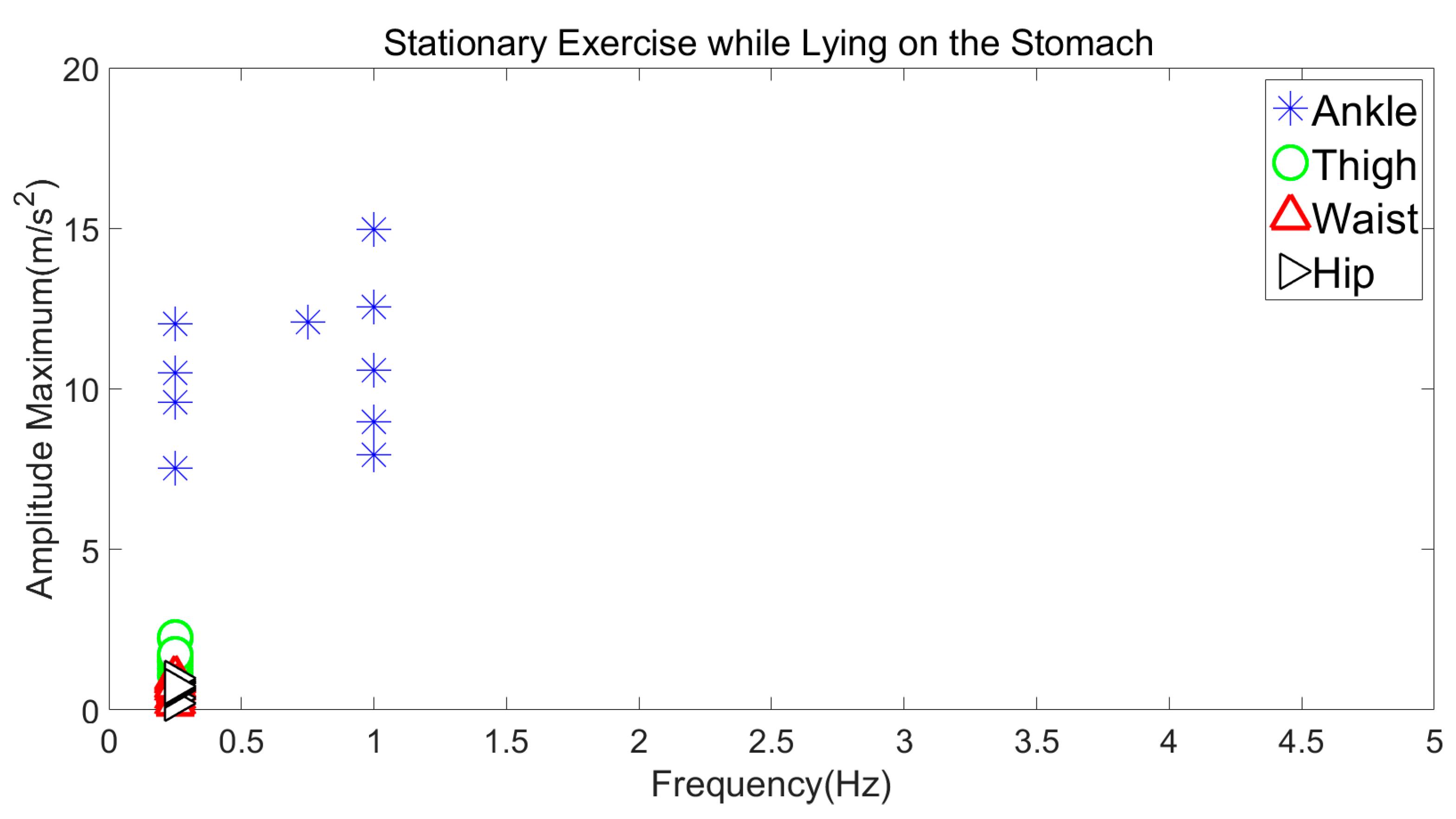
3.3.2. Stationary Exercise while Lying on the Stomach
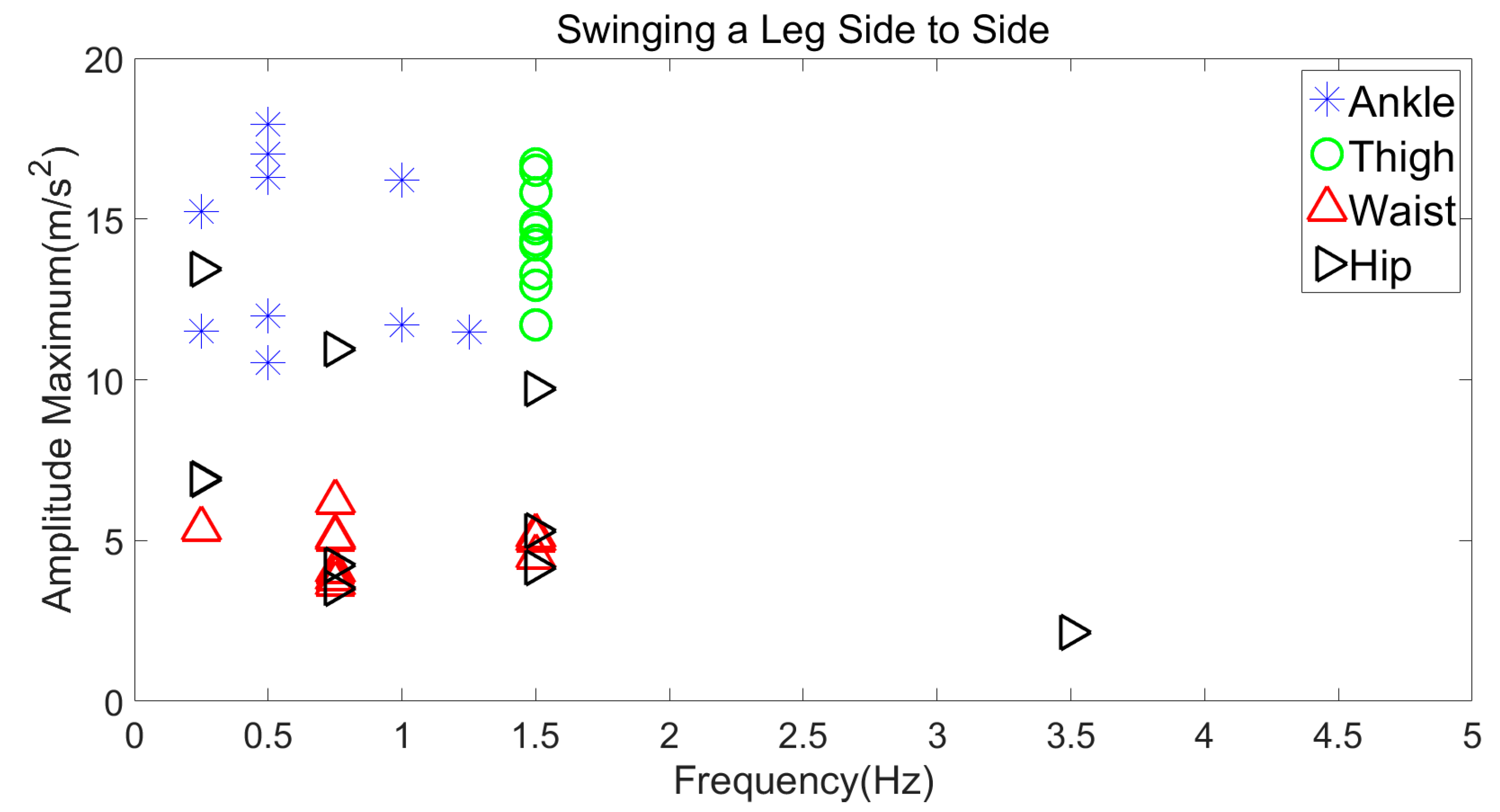
3.3.3. Swinging a Leg Side to Side
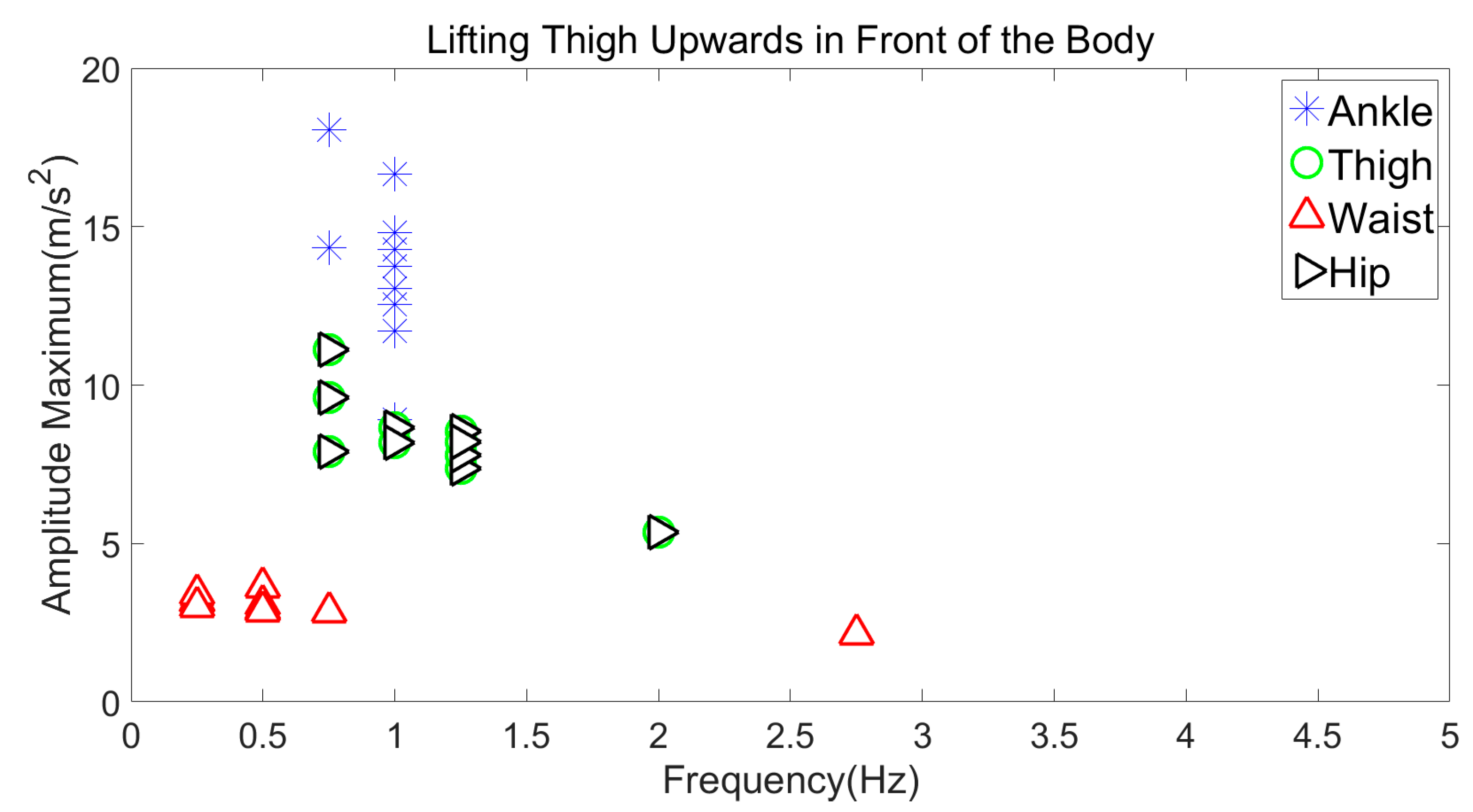
3.3.4. Lifting Thigh Upwards in Front of the Body
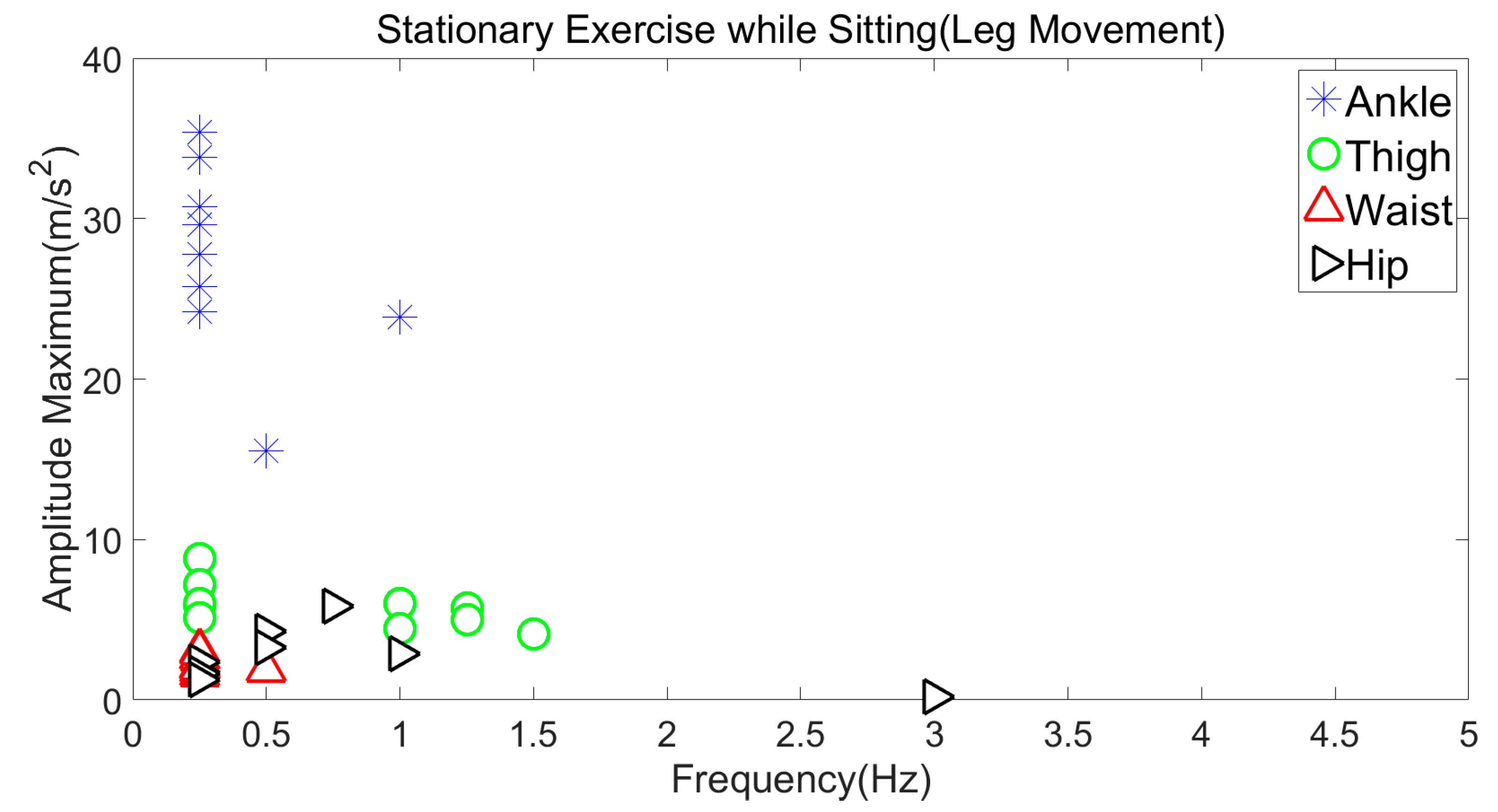
3.3.5. Stationary Exercise while Sitting (Leg Movement)
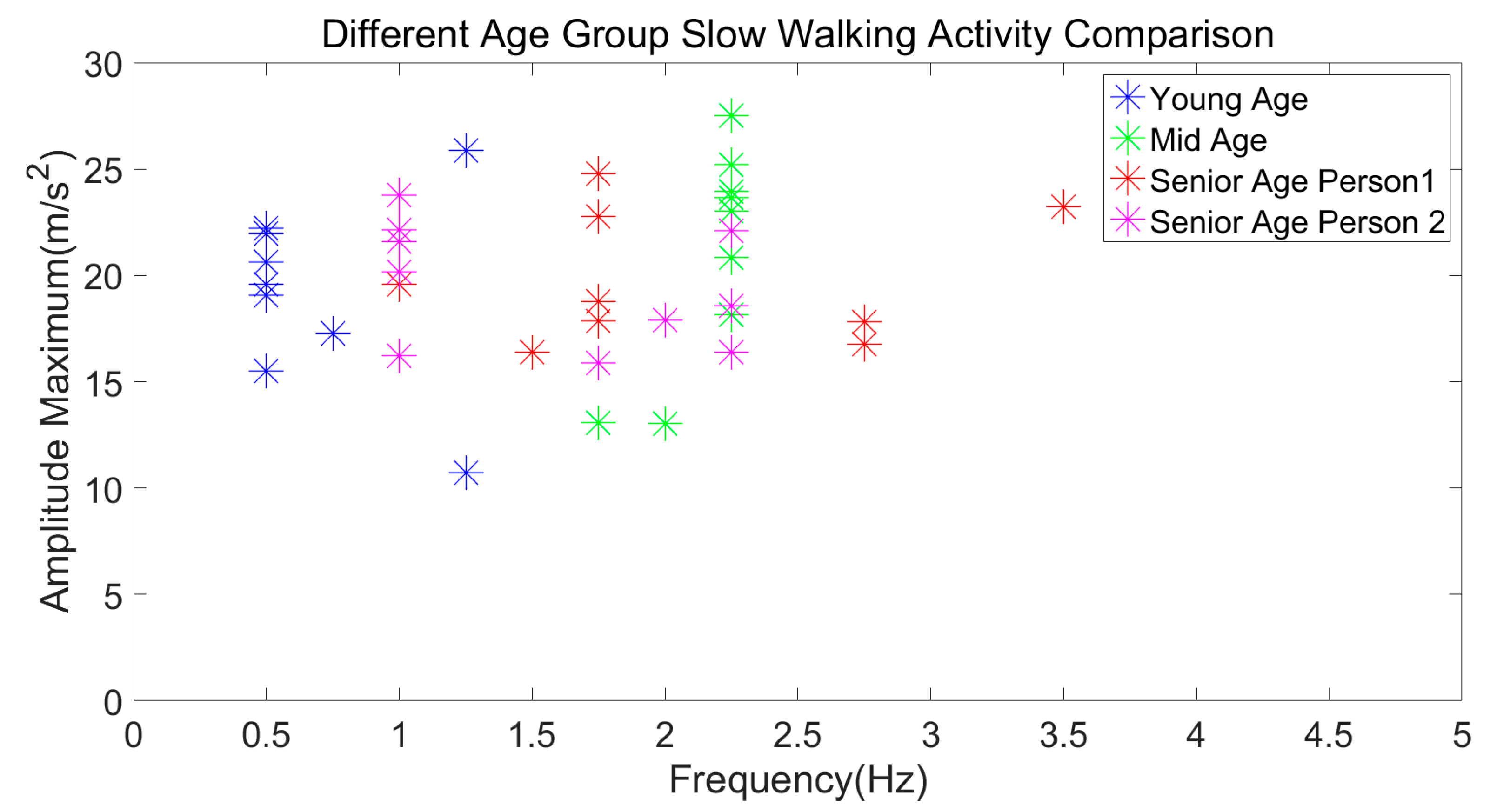
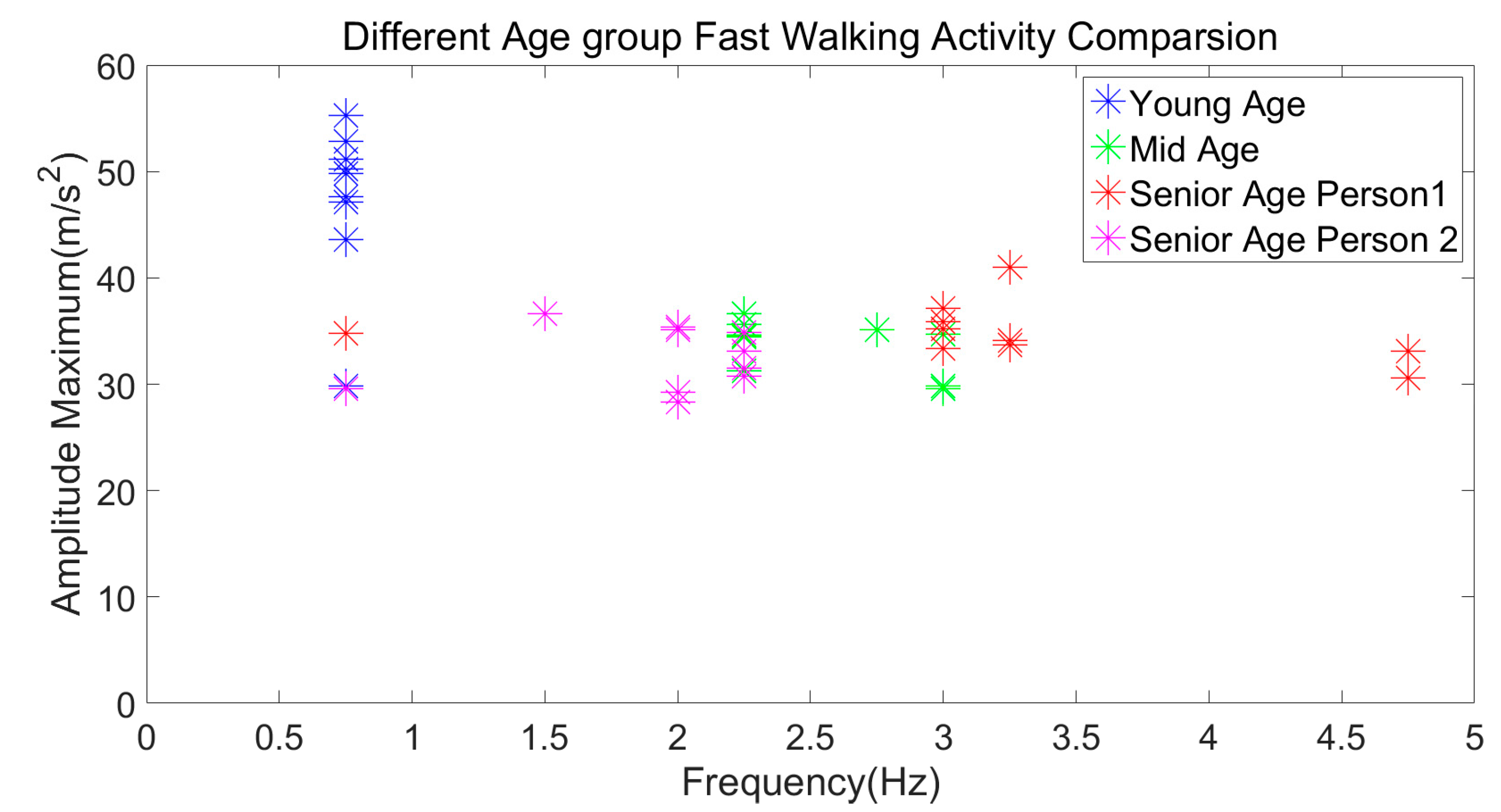
3.3.6. Different Age Group Subjects’ Slow and Fast Walking Activity Comparison
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Beaupre, L. Functional Recovery of Hip Fracture Patients. Available online: boneandjointcanada.com/wp-content/uploads/2014/05/Functional-Recovery_Final.pdf (accessed on 7 July 2017).
- Health Quality & Safety Commission New Zealand. Topic 7—Why Hip Fracture Prevention and Care Matter. Available online: https://www.hqsc.govt.nz/our-programmes/reducing-harm-from-falls/publications-and-resources/publication/2877/ (accessed on 10 June 2017).
- Donohue, K.; Hoevenaars, R.; McEachern, J.; Zeman, E.; Mehta, S. Home-based multidisciplinary rehabilitation following hip fracture surgery: What is the evidence? Rehabil. Res. Pract. 2013, 2013, 875968. [Google Scholar] [CrossRef] [PubMed]
- MCarneiro, B.; Alves, D.P.L.; Mercadante, M.T. Physical therapy in the post-operative of proximal femur fracture in elderly: Literature review. Acta Ortop. Bras. 2013, 21, 175–178. [Google Scholar]
- Magaziner, J.; Hawkes, W.; Hebel, J.R.; Zimmerman, S.I.; Fox, K.M.; Dolan, M.; Felsenthal, G.; Kenzora, J. Recovery from hip fracture in eight areas of function. J. Gerontol. Ser. A-Biol. Sci. Med. 2000, 55, M498–M507. [Google Scholar] [CrossRef]
- Dyer, S.; Diong, J.; Crotty, M.; Sherrington, C. Rehabilitation following hip fracture. In Orthogeriatrics; Springer: Berlin, Germany, 2017; pp. 145–163. [Google Scholar]
- Mukhopadhyay, S.C. Wearable sensors for human activity monitoring: A review. IEEE Sens. J. 2015, 15, 1321–1330. [Google Scholar] [CrossRef]
- Hadjidj, A.; Souil, M.; Bouabdallah, A.; Challal, Y.; Owen, H. Wireless sensor networks for rehabilitation applications: Challenges and opportunities. J. Netw. Comput. Appl. 2013, 36, 1–15. [Google Scholar] [CrossRef]
- Pol, M.C.; Riet, G.T.; van Hartingsveldt, M.; Kröse, B.; de Rooij, S.E.; Buurman, B.M. Effectiveness of sensor monitoring in an occupational therapy rehabilitation program for older individuals after hip fracture, the SO-HIP trial: Study protocol of a three-arm stepped wedge cluster randomized trial. BMC Health Serv. Res. 2017, 17, 3. [Google Scholar] [CrossRef] [PubMed]
- Alberta Health Services. Bone and joint health strategic clinical network. In Your Guide After a Hip Fracture; Alberta Bone and Joint Health Institute: Calgary, AB, Canada, 2015. [Google Scholar]
- Baylor Health Care System. Hip Fracture Guide. Available online: https://www.baylorhealth.com/PhysiciansLocations/Dallas/SpecialtiesServices/Orthopaedics/Documents/Hip%20Fractures%20Guide_Web.pdf (accessed on 10 August 2017).
- Benzinger, P.; Lindemann, U.; Becker, C.; Aminian, K.; Jamour, M.; Flick, S.E. Geriatric rehabilitation after hip fracture. Role of body-fixed sensor measurements of physical activity. Z. Gerontol. Geriatr. 2014, 47, 236–242. [Google Scholar] [CrossRef] [PubMed]
- Schwachmeyer, V.; Damm, P.; Bender, A.; Dymke, J.; Graichen, F.; Bergmann, G. In vivo hip joint loading during post-operative physiotherapeutic exercises. PLoS ONE 2013, 8, e77807. [Google Scholar] [CrossRef] [PubMed]
- Thingstad, P.; Taraldsen, K.; Saltvedt, I.; Sletvold, O.; Vereijken, B.; Lamb, S.E.; Helbostad, J.L. The long-term effect of comprehensive geriatric care on gait after hip fracture: The Trondheim Hip Fracture Trial—A randomised controlled trial. Osteoporos. Int. 2016, 27, 933–942. [Google Scholar] [CrossRef] [PubMed]
- Tsukagoshi, R.; Tateuchi, H.; Fukumoto, Y.; Ibuki, S.; Akiyama, H.; So, K.; Kuroda, Y.; Okumura, H.; Ichihashi, N. Functional performance of female patients more than 6 months after total hip arthroplasty shows greater improvement with weight-bearing exercise than with non-weight-bearing exercise. Randomized controlled trial. Eur. J. Phys. Rehabil. Med. 2014, 50, 665–675. [Google Scholar] [PubMed]
- Moschetti, A.; Fiorini, L.; Esposito, D.; Dario, P.; Cavallo, F. Recognition of Daily Gestures with Wearable Inertial Rings and Bracelets. Sensors 2016, 16, 1341. [Google Scholar] [CrossRef] [PubMed]
- Cornacchia, M.; Ozcan, K.; Zheng, Y.; Velipasalar, S. A survey on activity detection and classification using wearable sensors. IEEE Sens. J. 2017, 17, 386–403. [Google Scholar] [CrossRef]
- Lara, O.D.; Labrador, M.A. A survey on human activity recognition using wearable sensors. IEEE Commun. Surv. Tutor. 2013, 15, 1192–1209. [Google Scholar] [CrossRef]
- Baek, J.; Lee, G.; Park, W.; Yun, B.-J. Accelerometer signal processing for user activity detection. In Proceedings of the International Conference on Knowledge-Based and Intelligent Information and Engineering Systems, Wellington, New Zealand, 20–25 September 2004; pp. 610–617. [Google Scholar]
- Sharma, A.; Purwar, A.; Lee, Y.-D.; Lee, Y.-S.; Chung, W.-Y. Frequency based classification of activities using accelerometer data. In Proceedings of the MFI 2008: IEEE International Conference on Multisensor Fusion and Integration for Intelligent Systems, Seoul, Korea, 20–22 August 2008; pp. 150–153. [Google Scholar]
- Cleland, I.; Kikhia, B.; Nugent, C.; Boytsov, A.; Hallberg, J.; Synnes, K.; McClean, S.; Finlay, D. Optimal placement of accelerometers for the detection of everyday activities. Sensors 2013, 13, 9183–9200. [Google Scholar] [CrossRef] [PubMed]
- Amini, N.; Sarrafzadeh, M.; Vahdatpour, A.; Xu, W. Accelerometer-based on-body sensor localization for health and medical monitoring applications. Pervasive Mob. Comput. 2011, 7, 746–760. [Google Scholar] [CrossRef] [PubMed]
- Gjoreski, H.; Gams, M. Activity/Posture recognition using wearable sensors placed on different body locations. In Proceedings of the (738) Signal and Image Processing and Applications, Crete, Greece, 22–24 June 2011. [Google Scholar]
- Atallah, L.; Lo, B.P.; King, R.C.; Yang, G.-Z. Sensor Placement for Activity Detection Using Wearable Accelerometers. In Proceedings of the International Conference on Body Sensor Networks, Singapore, Singapore, 7–9 June 2010; pp. 24–29. [Google Scholar]
- Sriwan, J.; Suntiamorntut, W. Human activity monitoring system based on WSNs. In Proceedings of the 12th International Joint Conference on Computer Science and Software Engineering (JCSSE), Hatyai, Thailand, 22–24 July 2015; pp. 247–250. [Google Scholar]
- McAdams, E.T.; Gehin, C.; Noury, N.; Ramon, C.; Nocua, R.; Massot, B.; Oliveira, A.; Dittmar, A.; Nugent, C.D.; McLaughlin, J. Biomedical sensors for ambient assisted living. In Advances in Biomedical Sensing, Measurements, Instrumentation and Systems; Mukhopadhyay, S.C., Lay-Ekuakille, A., Eds.; Springer: Berlin, Germany, 2010; pp. 240–262. [Google Scholar]
- Ustev, Y.E.; Incel, O.D.; Ersoy, C. User, device and orientation independent human activity recognition on mobile phones: Challenges and a proposal. In Proceedings of the 2013 ACM conference on Pervasive and ubiquitous computing adjunct publication, Zurich, Switzerland, 8–12 September 2013; pp. 1427–1436. [Google Scholar]




| Activity Type | Amplitude | Frequency |
|---|---|---|
| Slow Walking | 12–28 m/s2 | 0.5–1.75 Hz |
| Fast Walking | 40–60 m/s2 | 0.5–1.75 Hz |
| Lying on Back | 5–9 m/s2 | 0–0.5 Hz |
| Lying on Stomach | 7–15 m/s2 | 0–1 Hz |
| Swinging Leg to Side | 10–18 m/s2 | 0–1.3 Hz |
| Lifting Thigh Upwards | 11–19 m/s2 | 0.9–1.1 Hz |
| Sitting (Leg Movement) | 23–37 m/s2 | 0–0.4 Hz |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Gupta, A.; Al-Anbuky, A.; McNair, P. Activity Classification Feasibility Using Wearables: Considerations for Hip Fracture. J. Sens. Actuator Netw. 2018, 7, 54. https://doi.org/10.3390/jsan7040054
Gupta A, Al-Anbuky A, McNair P. Activity Classification Feasibility Using Wearables: Considerations for Hip Fracture. Journal of Sensor and Actuator Networks. 2018; 7(4):54. https://doi.org/10.3390/jsan7040054
Chicago/Turabian StyleGupta, Akash, Adnan Al-Anbuky, and Peter McNair. 2018. "Activity Classification Feasibility Using Wearables: Considerations for Hip Fracture" Journal of Sensor and Actuator Networks 7, no. 4: 54. https://doi.org/10.3390/jsan7040054
APA StyleGupta, A., Al-Anbuky, A., & McNair, P. (2018). Activity Classification Feasibility Using Wearables: Considerations for Hip Fracture. Journal of Sensor and Actuator Networks, 7(4), 54. https://doi.org/10.3390/jsan7040054






