Natural Ergot Alkaloids in Ocular Pharmacotherapy: Known Molecules for Novel Nanoparticle-Based Delivery Systems
Abstract
1. Introduction
2. Role of Ergot Alkaloids in Reducing Intraocular Pressure
3. Encapsulation of Ergot Alkaloids for Ocular Administration
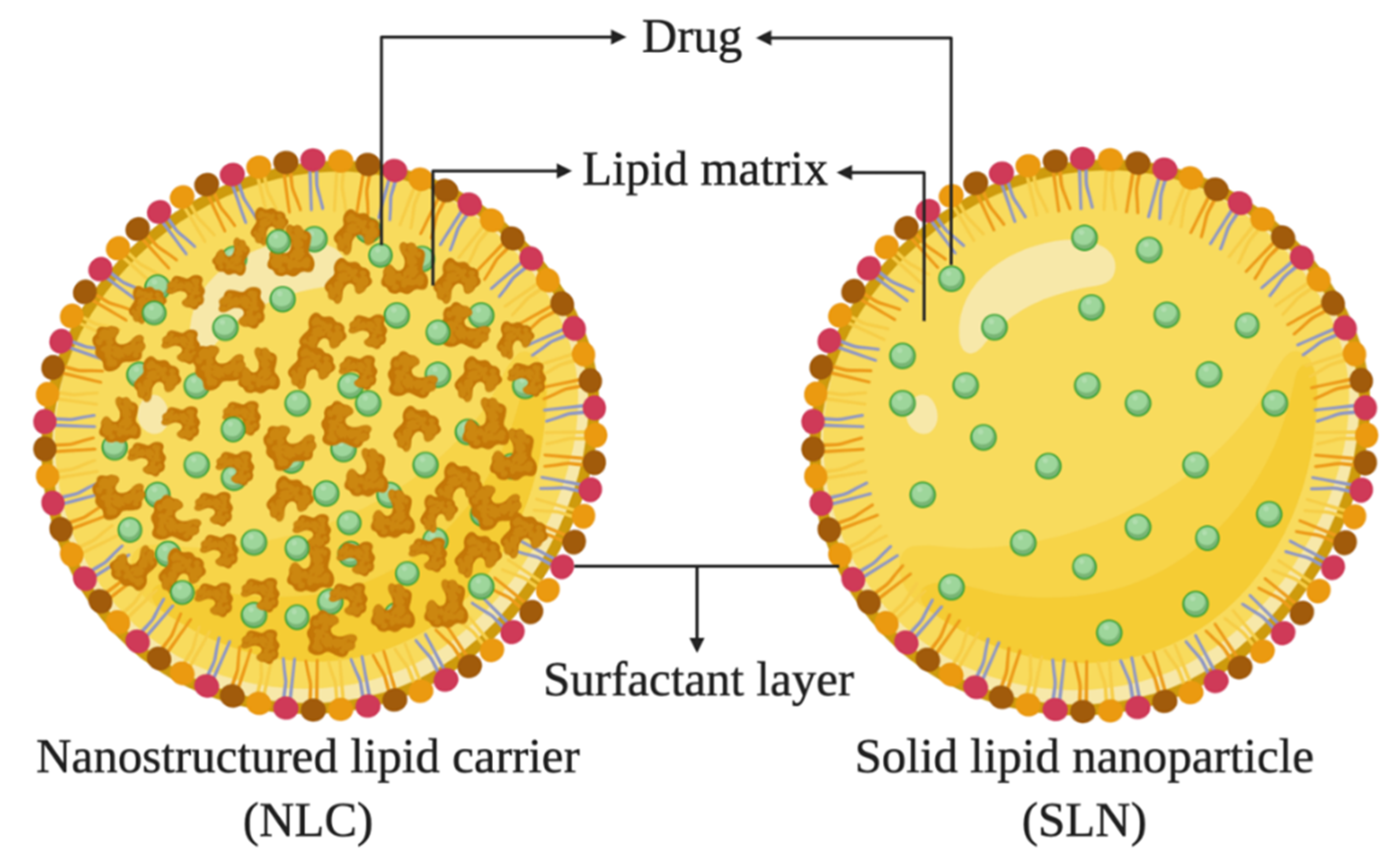
3.1. Lipid Nanoparticles
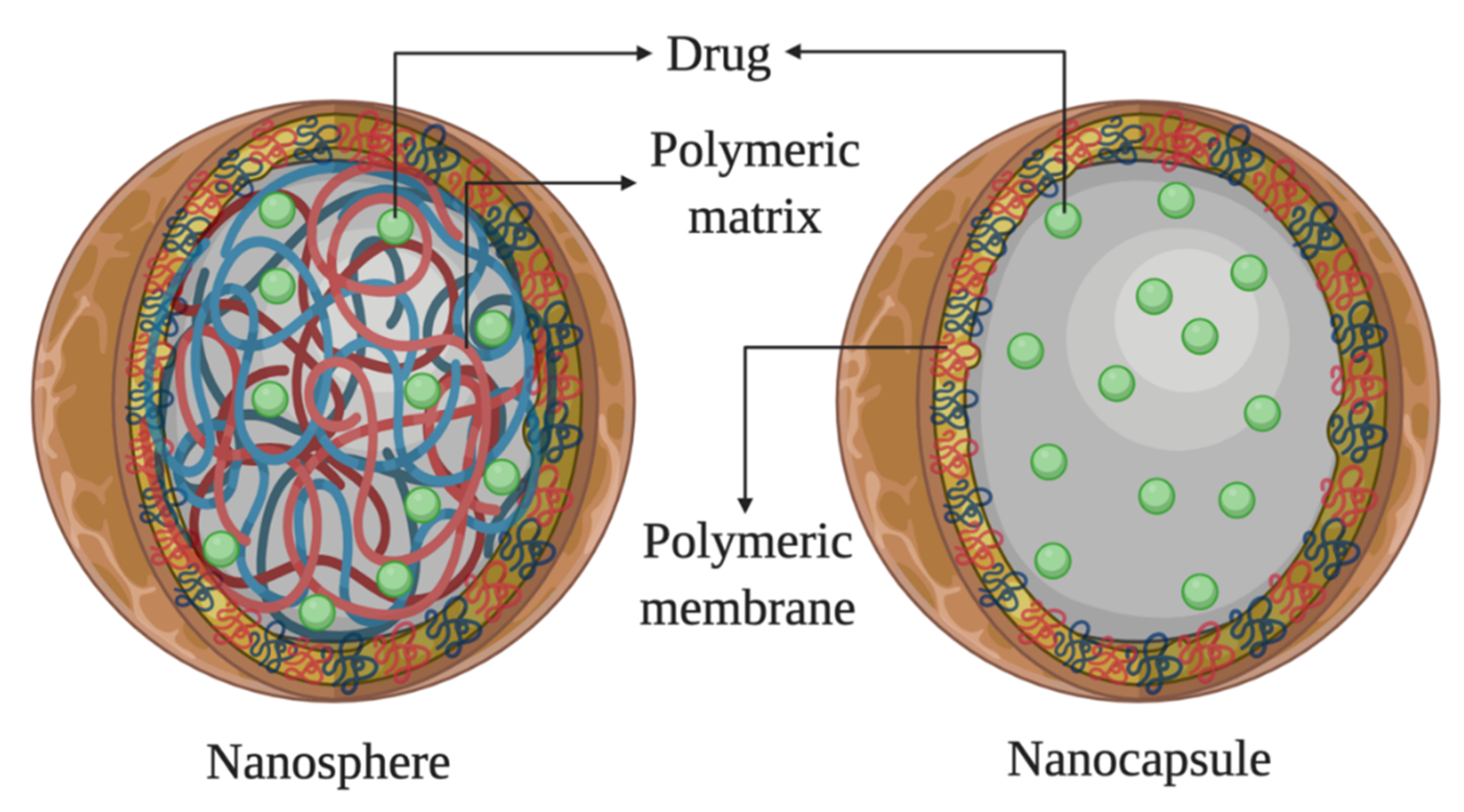
3.2. Polymeric Nanoparticles
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Jakubczyk, D.; Dussart, F. Selected Fungal Natural Products with Antimicrobial Properties. Molecules 2020, 25, 911. [Google Scholar] [CrossRef]
- Robinson, S.L.; Panaccione, D.G. Diversification of ergot alkaloids in natural and modified fungi. Toxins 2015, 7, 201–218. [Google Scholar] [CrossRef] [PubMed]
- Crews, C. Analysis of Ergot Alkaloids. Toxins 2015, 7, 2024–2050. [Google Scholar] [CrossRef] [PubMed]
- Schiff, P.L. Ergot and its alkaloids. Am. J. Pharm. Educ. 2006, 70, 98. [Google Scholar] [CrossRef]
- Agriopoulou, S.; Stamatelopoulou, E.; Varzakas, T. Advances in Occurrence, Importance, and Mycotoxin Control Strategies: Prevention and Detoxification in Foods. Foods 2020, 9, 137. [Google Scholar] [CrossRef]
- Carballo, D.; Tolosa, J.; Ferrer, E.; Berrada, H. Dietary exposure assessment to mycotoxins through total diet studies. A review. Food Chem. Toxicol. 2019, 128, 8–20. [Google Scholar] [CrossRef]
- Scott, P. Ergot alkaloids: Extent of human and animal exposure. World Mycotoxin J. 2009, 2, 141–149. [Google Scholar] [CrossRef]
- Mikušová, P.; Ritieni, A.; Santini, A.; Juhasová, G.; Šrobárová, A. Contamination by moulds of grape berries in Slovakia. Food Addit. Contam. Part A 2010, 27, 738–747. [Google Scholar] [CrossRef] [PubMed]
- Mikušová, P.; Šrobárová, A.; Sulyok, M.; Santini, A. Fusarium fungi and associated metabolites presence on grapes from Slovakia. Mycotoxin Res. 2013, 29, 97–102. [Google Scholar] [CrossRef]
- Santini, A.; Ferracane, R.; Meca, G.; Ritieni, A. Overview of analytical methods for beauvericin and fusaproliferin in food matrices. Anal. Bioanal. Chem. 2009, 395, 1253–1260. [Google Scholar] [CrossRef]
- Rodríguez-Carrasco, Y.; Gaspari, A.; Graziani, G.; Santini, A.; Ritieni, A. Fast analysis of polyphenols and alkaloids in cocoa-based products by ultra-high performance liquid chromatography and Orbitrap high resolution mass spectrometry (UHPLC-Q-Orbitrap-MS/MS). Food Res. Int. 2018, 111, 229–236. [Google Scholar] [CrossRef] [PubMed]
- Ritieni, A.; Santini, A.; Mussap, M.; Ferracane, R.; Bosco, P.; Gazzolo, D.; Galvano, F. Simultaneous determination of mycotoxins in biological fluids by LC-MS/MS. Front. Biosci. (Elite Ed.) 2010, 2, 151–158. [Google Scholar] [CrossRef] [PubMed]
- Amirkia, V.; Heinrich, M. Alkaloids as drug leads—A predictive structural and biodiversity-based analysis. Phytochem. Lett. 2014, 10, xlviii–liii. [Google Scholar] [CrossRef]
- Ahmad, S.; Garg, M.; Tamboli, E.T.; Abdin, M.Z.; Ansari, S.H. In vitro production of alkaloids: Factors, approaches, challenges and prospects. Pharmacogn. Rev. 2013, 7, 27–33. [Google Scholar] [CrossRef]
- Adamski, Z.; Blythe, L.L.; Milella, L.; Bufo, S.A. Biological Activities of Alkaloids: From Toxicology to Pharmacology. Toxins 2020, 12, 210. [Google Scholar] [CrossRef] [PubMed]
- Klotz, J.L. Activities and Effects of Ergot Alkaloids on Livestock Physiology and Production. Toxins 2015, 7, 2801–2821. [Google Scholar] [CrossRef] [PubMed]
- Mulac, D.; Hüwel, S.; Galla, H.-J.; Humpf, H.-U. Permeability of ergot alkaloids across the blood-brain barrier in vitro and influence on the barrier integrity. Mol. Nutr. Food Res. 2012, 56, 475–485. [Google Scholar] [CrossRef]
- Mulac, D.; Humpf, H.U. Cytotoxicity and accumulation of ergot alkaloids in human primary cells. Toxicology 2011, 282, 112–121. [Google Scholar] [CrossRef]
- Sanchez-Lopez, E.; Egea, M.A.; Davis, B.M.; Guo, L.; Espina, M.; Silva, A.M.; Calpena, A.C.; Souto, E.M.B.; Ravindran, N.; Ettcheto, M.; et al. Memantine-Loaded PEGylated Biodegradable Nanoparticles for the Treatment of Glaucoma. Small 2018, 14, 1701808. [Google Scholar] [CrossRef]
- Sánchez-López, E.; Lopez-Machado, A.L.; Bonilla, V.L.; Pizarro, P.G.; Silva, A.M.; Souto, E.B. Lipid nanoparticles as carriers for the treatment of neurodegeneration associated with Alzheimer’s disease and glaucoma: Present and future challenges. Curr. Pharm. Des. 2020, 26, 1235–1250. [Google Scholar] [CrossRef]
- Hertzog, L.H.; Albrecht, K.G.; LaBree, L.; Lee, P.P. Glaucoma care and conformance with preferred practice patterns. Examination of the private, community-based ophthalmologist. Ophthalmology 1996, 103, 1009–1013. [Google Scholar] [CrossRef]
- Singh, R.B.; Ichhpujani, P.; Thakur, S.; Jindal, S. Promising therapeutic drug delivery systems for glaucoma: A comprehensive review. Ther. Adv. Ophthalmol. 2020, 12, 2515841420905740. [Google Scholar] [CrossRef]
- McAlinden, C. Selective laser trabeculoplasty (SLT) vs. other treatment modalities for glaucoma: Systematic review. Eye (Lond. Engl.) 2014, 28, 249–258. [Google Scholar] [CrossRef] [PubMed]
- Weinreb, R.N.; Leung, C.K.S.; Crowston, J.G.; Medeiros, F.A.; Friedman, D.S.; Wiggs, J.L.; Martin, K.R. Primary open-angle glaucoma. Nat. Rev. Dis. Primers 2016, 2, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Thiel, R. Experimental and clinical investigations on the influence of ergotamine (Gynergen) on the intraocular pressure in glaucoma. Klin. Mon. Augenh. 1926, 77, 753. [Google Scholar]
- Kappert, A.; Hadron, W. Experimental and therapeutic investigations with certain new hydrogenated ergot alkaloids in peripheral vascular disorders. Angiology 1950, 1, 520–529. [Google Scholar] [CrossRef]
- Chen, J.-J.; Han, M.-Y.; Gong, T.; Yang, J.-L.; Zhu, P. Recent progress in ergot alkaloid research. RSC Adv. 2017, 7, 27384–27396. [Google Scholar] [CrossRef]
- Berde, B. Pharmacology of ergot alkaloids in clinical use. Med. J. Aust. 1978, 2, 3–13. [Google Scholar] [CrossRef]
- Mukherjee, J.; Menge, M. Progress and Prospects of Ergot Alkaloid Research. In New Products and New Areas of Bioprocess Engineering; Springer: Berlin/Heidelberg, Germany, 2000; pp. 1–20. [Google Scholar] [CrossRef]
- Diotallevi, M.; Auricchio, G. The effect of topically used hydergine on ocular tension. Ophthalmologica 1964, 147, 448–454. [Google Scholar] [CrossRef]
- Al-Sereiti, M.R.; Quik, R.F.; Turner, P. The effect of a single oral dose of pergolide on intraocular pressure and pupil diameter. Br. J. Clin. Pharmacol. 1989, 28, 263–268. [Google Scholar] [CrossRef]
- Elibol, O.; Güler, C.; Yüksel, N. The effects of dopamine, haloperidol and bromocriptine on intraocular pressure. Int. Ophthalmol. 1992, 16, 343–347. [Google Scholar] [CrossRef] [PubMed]
- Potter, D.E.; Ogidigben, M.J.; Chu, T.C. Lisuride acts at multiple sites to induce ocular hypotension and mydriasis. Pharmacology 1998, 57, 249–260. [Google Scholar] [CrossRef] [PubMed]
- Potter, D.E.; Shumate, D.J. Cianergoline Lowers Intraocular Pressure in Rabbits and Monkeys and Inhibits Contraction of the Cat Nictitans by Suppressing Sympathetic Neuronal Function. J. Ocul. Pharmacol. Ther. 1987, 3, 309–321. [Google Scholar] [CrossRef] [PubMed]
- Cavanak, T. Occular Formulation Comprising Bromocriptine. U.S. Patent US4654345A, 31 March 1987. Application Granted. [Google Scholar]
- Gerhards, N.; Neubauer, L.; Tudzynski, P.; Li, S.-M. Biosynthetic Pathways of Ergot Alkaloids. Toxins 2014, 6, 3281–3295. [Google Scholar] [CrossRef]
- Al-Sereiti, M.R.; Coakes, R.L.; O’Sullivan, D.P.; Turner, P. A comparison of the ocular hypotensive effect of 0.025% bromocriptine and 0.25% timolol eye drops in normal human volunteers. Br. J. Clin. Pharmacol. 1989, 28, 443–447. [Google Scholar] [CrossRef] [PubMed]
- Mekki, Q.A.; Warrington, S.J.; Turner, P. Bromocriptine eyedrops lower intraocular pressure without affecting prolactin levels. Lancet (Lond. Engl.) 1984, 1, 287–288. [Google Scholar] [CrossRef]
- Puras, G.; Santafé, J.; Segarra, J.; Garrido, M.; Melena, J. The effect of topical natural ergot alkaloids on the intraocular pressure and aqueous humor dynamics in rabbits with alpha-chymotrypsin-induced ocular hypertension. Graefe’s Arch. Clin. Exp. Ophthalmol. 2002, 240, 322–328. [Google Scholar] [CrossRef]
- Puras, G.; Santafé, J.; Segarra, J.; Garrido, M.; Melena, J. A comparative study of topical natural ergot alkaloids on the intraocular pressure and aqueous humor dynamics in oclular normotensive and alpha-chymotrypsin-induced ocular hypertensive rabbits. Graefe’s Arch. Clin. Exp. Ophthalmol. 2007, 245, 1559–1567. [Google Scholar] [CrossRef]
- Puras, G. Intraocular pressure lowering effect of natural ergot alkaloids and their future applications in ocular pharmacology. In Alkaloids: Properties, Applications and Pharmacological Effects; Cassiano, N.M., Ed.; Nova Science Publishers: Hauppauge, NY, USA, 2011; pp. 37–61. [Google Scholar]
- Santafé Oroz, J.; Segarra Domenech, J.; Garrido García, M.; Pablo Martínez, V. Effects of topical dihydroergocristine on intraocular pressure, aqueous humor dynamics and pupil diameter in conscious rabbits. A comparative study with timolol and pilocarpine. Methods Find. Exp. Clin. Pharmacol. 1991, 13, 231–238. [Google Scholar]
- Rowell, P.P.; Larson, B.T. Ergocryptine and other ergot alkaloids stimulate the release of [3H]dopamine from rat striatal synaptosomes2. J. Anim. Sci. 1999, 77, 1800–1806. [Google Scholar] [CrossRef]
- Abul Kalam, M.; Sultana, Y.; Ali, A.; Aqil, M.; Mishra, A.K.; Chuttani, K.; Aljuffali, I.A.; Alshamsan, A. Part II: Enhancement of transcorneal delivery of gatifloxacin by solid lipid nanoparticles in comparison to commercial aqueous eye drops. J. Biomed. Mater. Res. Part A 2013, 101, 1828–1836. [Google Scholar] [CrossRef] [PubMed]
- Pita-Thomas, D.W.; Goldberg, J.L. Nanotechnology and glaucoma: Little particles for a big disease. Curr. Opin. Ophthalmol. 2013, 24, 130–135. [Google Scholar] [CrossRef] [PubMed]
- Güven, U.M.; Berkman, M.S.; Enel, B.; Yazan, Y. Development and in vitro/in vivo evaluation of thermo-sensitive in situ gelling systems for ocular allergy. Braz. J. Pharm. Sci. 2019, 55. [Google Scholar] [CrossRef]
- McKenzie, B.; Kay, G. Eye gels for ophthalmic delivery. Expert Rev. Ophthalmol. 2015, 10, 127–133. [Google Scholar] [CrossRef]
- Sanchez-Lopez, E.; Espina, M.; Doktorovova, S.; Souto, E.B.; Garcia, M.L. Lipid nanoparticles (SLN, NLC): Overcoming the anatomical and physiological barriers of the eye—Part I-Barriers and determining factors in ocular delivery. Eur. J. Pharm. Biopharm. 2017, 110, 70–75. [Google Scholar] [CrossRef]
- Joseph, M.; Trinh, H.M.; Cholkar, K.; Pal, D.; Mitra, A.K. Recent perspectives on the delivery of biologics to back of the eye. Expert Opin. Drug Deliv. 2016, 1–15. [Google Scholar] [CrossRef]
- Souto, E.B.; Souto, S.B.; Severino, P.; Dias-Ferreira, J.; Naveros, B.C.; Durazzo, A.; Lucarini, M.; Atanasov, A.G.; El Mamouni, S.; Santini, A. Croton argyrophyllus Kunth essential oil - loaded SLN: Optimization and evaluation of antioxidant and antitumoral activities. Molecules 2020. submitted. [Google Scholar]
- Ghate, D.; Edelhauser, H.F. Ocular drug delivery. Expert Opin. Drug Deliv. 2006, 3, 275–287. [Google Scholar] [CrossRef]
- Sánchez-López, E.; Esteruelas, G.; Ortiz, A.; Espina, M.; Prat, J.; Muñoz, M.; Cano, A.; Calpena, A.C.; Ettcheto, M.; Camins, A.; et al. Dexibuprofen Biodegradable Nanoparticles: One Step Closer towards a Better Ocular Interaction Study. Nanomaterials 2020, 10, 720. [Google Scholar] [CrossRef]
- Gonzalez-Mira, E.; Egea, M.A.; Garcia, M.L.; Souto, E.B. Design and ocular tolerance of flurbiprofen loaded ultrasound-engineered NLC. Colloids Surf B Biointerfaces 2010, 81, 412–421. [Google Scholar] [CrossRef]
- Souto, E.B.; Dias-Ferreira, J.; Lopez-Machado, A.; Ettcheto, M.; Cano, A.; Camins Espuny, A.; Espina, M.; Garcia, M.L.; Sanchez-Lopez, E. Advanced Formulation Approaches for Ocular Drug Delivery: State-of-the-Art and Recent Patents. Pharmaceutics 2019, 11, 460. [Google Scholar] [CrossRef] [PubMed]
- Sanchez-Lopez, E.; Espina, M.; Doktorovova, S.; Souto, E.B.; Garcia, M.L. Lipid nanoparticles (SLN, NLC): Overcoming the anatomical and physiological barriers of the eye—Part II—Ocular drug-loaded lipid nanoparticles. Eur. J. Pharm. Biopharm. 2017, 110, 58–69. [Google Scholar] [CrossRef] [PubMed]
- Fangueiro, J.F.; Veiga, F.; Silva, A.M.; Souto, E.B. Ocular Drug Delivery—New Strategies for Targeting Anterior and Posterior Segments of the Eye. Curr. Pharm. Des. 2016, 22, 1135–1146. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Mira, E.; Egea, M.A.; Souto, E.B.; Calpena, A.C.; Garcia, M.L. Optimizing flurbiprofen-loaded NLC by central composite factorial design for ocular delivery. Nanotechnology 2011, 22, 045101. [Google Scholar] [CrossRef]
- Vieira, R.; Severino, P.; Nalone, L.A.; Souto, S.B.; Silva, A.M.; Lucarini, M.; Durazzo, A.; Santini, A.; Souto, E.B. Sucupira Oil-Loaded Nanostructured Lipid Carriers (NLC): Lipid Screening, Factorial Design, Release Profile, and Cytotoxicity. Molecules 2020, 25, 685. [Google Scholar] [CrossRef]
- Souto, E.B.; Souto, S.B.; Zielinska, A.; Durazzo, A.; Lucarini, M.; Santini, A.; Horbańczuk, O.K.; Atanasov, A.G.; Marques, C.; Andrade, L.N.; et al. Perillaldehyde 1,2-epoxide loaded SLN-tailored mAb: Production, physicochemical characterization and in vitro cytotoxicity profile in MCF-7 cell lines. Pharmaceutics 2020, 12, 161. [Google Scholar] [CrossRef]
- Zielinska, A.; Ferreira, N.R.; Durazzo, A.; Lucarini, M.; Cicero, N.; Mamouni, S.E.; Silva, A.M.; Nowak, I.; Santini, A.; Souto, E.B. Development and Optimization of Alpha-Pinene-Loaded Solid Lipid Nanoparticles (SLN) Using Experimental Factorial Design and Dispersion Analysis. Molecules 2019, 24, 2683. [Google Scholar] [CrossRef]
- Rigon, R.B.; Fachinetti, N.; Severino, P.; Durazzo, A.; Lucarini, M.; Atanasov, A.G.; El Mamouni, S.; Chorilli, M.; Santini, A.; Souto, E.B. Quantification of Trans-Resveratrol-Loaded Solid Lipid Nanoparticles by a Validated Reverse-Phase HPLC Photodiode Array. Appl. Sci. 2019, 9, 4961. [Google Scholar] [CrossRef]
- Campos, J.R.; Severino, P.; Santini, A.; Silva, A.M.; Shegokar, R.; Souto, S.B.; Souto, E.B. Chapter 1—Solid lipid nanoparticles (SLN): Prediction of toxicity, metabolism, fate and physicochemical properties. In Nanopharmaceuticals; Shegokar, R., Ed.; Elsevier: Amsterdam, The Netherlands, 2020; pp. 1–15. [Google Scholar] [CrossRef]
- Wadetwar, R.N.; Agrawal, A.R.; Kanojiya, P.S. In situ gel containing Bimatoprost solid lipid nanoparticles for ocular delivery: In-vitro and ex-vivo evaluation. J. Drug Deliv. Sci. Technol. 2020, 56, 101575. [Google Scholar] [CrossRef]
- Doktorovova, S.; Santos, D.L.; Costa, I.; Andreani, T.; Souto, E.B.; Silva, A.M. Cationic solid lipid nanoparticles interfere with the activity of antioxidant enzymes in hepatocellular carcinoma cells. Int. J. Pharm. 2014, 471, 18–27. [Google Scholar] [CrossRef]
- Doktorovova, S.; Shegokar, R.; Rakovsky, E.; Gonzalez-Mira, E.; Lopes, C.M.; Silva, A.M.; Martins-Lopes, P.; Muller, R.H.; Souto, E.B. Cationic solid lipid nanoparticles (cSLN): Structure, stability and DNA binding capacity correlation studies. Int. J. Pharm. 2011, 420, 341–349. [Google Scholar] [CrossRef] [PubMed]
- Fangueiro, J.F.; Andreani, T.; Egea, M.A.; Garcia, M.L.; Souto, S.B.; Silva, A.M.; Souto, E.B. Design of cationic lipid nanoparticles for ocular delivery: Development, characterization and cytotoxicity. Int. J. Pharm. 2014, 461, 64–73. [Google Scholar] [CrossRef] [PubMed]
- Fangueiro, J.F.; Calpena, A.C.; Clares, B.; Andreani, T.; Egea, M.A.; Veiga, F.J.; Garcia, M.L.; Silva, A.M.; Souto, E.B. Biopharmaceutical evaluation of epigallocatechin gallate-loaded cationic lipid nanoparticles (EGCG-LNs): In vivo, in vitro and ex vivo studies. Int. J. Pharm. 2016, 502, 161–169. [Google Scholar] [CrossRef] [PubMed]
- Araujo, J.; Garcia, M.L.; Mallandrich, M.; Souto, E.B.; Calpena, A.C. Release profile and transscleral permeation of triamcinolone acetonide loaded nanostructured lipid carriers (TA-NLC): In vitro and ex vivo studies. Nanomedicine 2012, 8, 1034–1041. [Google Scholar] [CrossRef] [PubMed]
- Araujo, J.; Nikolic, S.; Egea, M.A.; Souto, E.B.; Garcia, M.L. Nanostructured lipid carriers for triamcinolone acetonide delivery to the posterior segment of the eye. Colloids Surf. B Biointerfaces 2011, 88, 150–157. [Google Scholar] [CrossRef]
- Doktorovova, S.; Araujo, J.; Garcia, M.L.; Rakovsky, E.; Souto, E.B. Formulating fluticasone propionate in novel PEG-containing nanostructured lipid carriers (PEG-NLC). Colloids Surf. B Biointerfaces 2010, 75, 538–542. [Google Scholar] [CrossRef]
- Araujo, J.; Gonzalez-Mira, E.; Egea, M.A.; Garcia, M.L.; Souto, E.B. Optimization and physicochemical characterization of a triamcinolone acetonide-loaded NLC for ocular antiangiogenic applications. Int. J. Pharm. 2010, 393, 167–175. [Google Scholar] [CrossRef]
- Araujo, J.; Gonzalez, E.; Egea, M.A.; Garcia, M.L.; Souto, E.B. Nanomedicines for ocular NSAIDs: Safety on drug delivery. Nanomedicine 2009, 5, 394–401. [Google Scholar] [CrossRef]
- Souto, E.B.; Almeida, A.J.; Müller, R.H. Lipid Nanoparticles (SLN®, NLC®) for Cutaneous Drug Delivery: Structure, Protection and Skin Effects. J. Biomed. Nanotechnol. 2007, 3, 317–331. [Google Scholar] [CrossRef]
- Souto, E.B.; Baldim, I.; Oliveira, W.P.; Rao, R.; Yadav, N.; Gama, F.M.; Mahant, S. SLN and NLC for topical, dermal and transdermal drug delivery. Expert Opin. Drug Deliv. 2020, 17, 357–377. [Google Scholar] [CrossRef]
- Zielińska, A.; Ferreira, N.R.; Feliczak-Guzik, A.; Nowak, I.; Souto, E.B. Loading, release profile and accelerated stability assessment of monoterpenes-loaded Solid Lipid Nanoparticles (SLN). Pharm. Dev. Technol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Souto, E.B.; Doktorovova, S.; Gonzalez-Mira, E.; Egea, M.A.; Garcia, M.L. Feasibility of lipid nanoparticles for ocular delivery of anti-inflammatory drugs. Curr. Eye Res. 2010, 35, 537–552. [Google Scholar] [CrossRef]
- Fangueiro, J.F.; Andreani, T.; Fernandes, L.; Garcia, M.L.; Egea, M.A.; Silva, A.M.; Souto, E.B. Physicochemical characterization of epigallocatechin gallate lipid nanoparticles (EGCG-LNs) for ocular instillation. Colloids Surf. B Biointerfaces 2014, 123, 452–460. [Google Scholar] [CrossRef]
- Doktorovova, S.; Kovacevic, A.B.; Garcia, M.L.; Souto, E.B. Preclinical safety of solid lipid nanoparticles and nanostructured lipid carriers: Current evidence from in vitro and in vivo evaluation. Eur. J. Pharm. Biopharm. 2016, 108, 235–252. [Google Scholar] [CrossRef]
- El-Salamouni, N.S.; Farid, R.M.; El-Kamel, A.H.; El-Gamal, S.S. Nanostructured lipid carriers for intraocular brimonidine localisation: Development, in-vitro and in-vivo evaluation. J. Microencapsul. 2018, 35, 102–113. [Google Scholar] [CrossRef]
- Lakhani, P.; Patil, A.; Taskar, P.; Ashour, E.; Majumdar, S. Curcumin-loaded Nanostructured Lipid Carriers for ocular drug delivery: Design optimization and characterization. J. Drug Deliv. Sci. Technol. 2018, 47, 159–166. [Google Scholar] [CrossRef]
- Singh, M.; Guzman-Aranguez, A.; Hussain, A.; Srinivas, C.S.; Kaur, I.P. Solid lipid nanoparticles for ocular delivery of isoniazid: Evaluation, proof of concept and in vivo safety & kinetics. Nanomedicine (Lond. Engl.) 2019, 14, 465–491. [Google Scholar] [CrossRef]
- Khames, A.; Khaleel, M.A.; El-Badawy, M.F.; El-Nezhawy, A.O.H. Natamycin solid lipid nanoparticles—Sustained ocular delivery system of higher corneal penetration against deep fungal keratitis: Preparation and optimization. Int. J. Nanomed. 2019, 14, 2515–2531. [Google Scholar] [CrossRef]
- Sharif Makhmal Zadeh, B.; Niro, H.; Rahim, F.; Esfahani, G. Ocular Delivery System for Propranolol Hydrochloride Based on Nanostructured Lipid Carrier. Sci. Pharm. 2018, 86, 16. [Google Scholar] [CrossRef]
- Yu, Y.; Feng, R.; Yu, S.; Li, J.; Wang, Y.; Song, Y.; Yang, X.; Pan, W.; Li, S. Nanostructured lipid carrier-based pH and temperature dual-responsive hydrogel composed of carboxymethyl chitosan and poloxamer for drug delivery. Int. J. Biol. Macromol. 2018, 114, 462–469. [Google Scholar] [CrossRef]
- Freitas, L.G.A.D.; Isaac, D.L.C.; Lima, E.M.; Souza, L.G.; Abud, M.A.; Reis, R.G.D.; Tannure, W.T.; Ávila, M.P.D. Retinal changes in rabbit after intravitreal injection of sunitinib encapsulated into solid lipid nanoparticles and polymeric nanocapsules. Arq. Bras. Oftalmol. 2018, 81, 408–413. [Google Scholar] [CrossRef] [PubMed]
- Tatke, A.; Dudhipala, N.; Janga, K.Y.; Balguri, S.P.; Avula, B.; Jablonski, M.M.; Majumdar, S. In Situ Gel of Triamcinolone Acetonide-Loaded Solid Lipid Nanoparticles for Improved Topical Ocular Delivery: Tear Kinetics and Ocular Disposition Studies. Nanomaterials 2018, 9, 33. [Google Scholar] [CrossRef] [PubMed]
- Füredi, P.; Pápay, Z.E.; Kovács, K.; Kiss, B.D.; Ludányi, K.; Antal, I.; Klebovich, I. Development and characterization of the voriconazole loaded lipid-based nanoparticles. J. Pharm. Biomed. Anal. 2017, 132, 184–189. [Google Scholar] [CrossRef]
- Yin, J.; Xiang, C.; Lu, G. Cationic lipid emulsions as potential bioadhesive carriers for ophthalmic delivery of palmatine. J. Microencapsul. 2016, 33, 718–724. [Google Scholar] [CrossRef] [PubMed]
- Chhonker, Y.S.; Prasad, Y.D.; Chandasana, H.; Vishvkarma, A.; Mitra, K.; Shukla, P.K.; Bhatta, R.S. Amphotericin-B entrapped lecithin/chitosan nanoparticles for prolonged ocular application. Int. J. Biol. Macromol. 2015, 72, 1451–1458. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Liu, W.; Sorenson, C.M.; Sheibani, N.; Albert, D.M.; Senanayake, T.; Vinogradov, S.; Henkin, J.; Zhang, H.F. Sustaining Intravitreal Residence with L-Arginine Peptide-Conjugated Nanocarriers. Investig. Ophthalmol. Vis. Sci. 2017, 58, 5142–5150. [Google Scholar] [CrossRef] [PubMed]
- Nirbhavane, P.; Sharma, G.; Singh, B.; Begum, G.; Jones, M.-C.; Rauz, S.; Vincent, R.; Denniston, A.K.; Hill, L.J.; Katare, O.P. Triamcinolone acetonide loaded-cationic nano-lipoidal formulation for uveitis: Evidences of improved biopharmaceutical performance and anti-inflammatory activity. Colloids Surf. B Biointerfaces 2020, 190, 110902. [Google Scholar] [CrossRef]
- Klang, S.H.; Frucht-Pery, J.; Hoffman, A.; Benita, S. Physicochemical Characterization and Acute Toxicity Evaluation of a Positively-charged Submicron Emulsion Vehicle. J. Pharm. Pharmacol. 1994, 46, 986–993. [Google Scholar] [CrossRef]
- Liu, R.; Wang, S.; Sun, L.; Fang, S.; Wang, J.; Huang, X.; You, Z.; He, X.; Liu, C. A novel cationic nanostructured lipid carrier for improvement of ocular bioavailability: Design, optimization, in vitro and in vivo evaluation. J. Drug Deliv. Sci. Technol. 2016, 33, 28–36. [Google Scholar] [CrossRef]
- Avachat, A.M.; Parpani, S.S. Formulation and development of bicontinuous nanostructured liquid crystalline particles of efavirenz. Colloids Surf. B Biointerfaces 2015, 126, 87–97. [Google Scholar] [CrossRef]
- Wang, J.; Zhao, F.; Liu, R.; Chen, J.; Zhang, Q.; Lao, R.; Wang, Z.; Jin, X.; Liu, C. Novel cationic lipid nanoparticles as an ophthalmic delivery system for multicomponent drugs: Development, characterization, in vitro permeation, in vivo pharmacokinetic, and molecular dynamics studies. Int. J. Nanomed. 2017, 12, 8115–8127. [Google Scholar] [CrossRef] [PubMed]
- Yaghmur, A.; Glatter, O. Characterization and potential applications of nanostructured aqueous dispersions. Adv. Colloid Interface Sci. 2009, 147, 333–342. [Google Scholar] [CrossRef]
- Doktorovova, S.; Souto, E.B. Nanostructured lipid carrier-based hydrogel formulations for drug delivery: A comprehensive review. Expert Opin. Drug Deliv. 2009, 6, 165–176. [Google Scholar] [CrossRef] [PubMed]
- Kalbáčová, M.; Verdánová, M.; Mravec, F.; Halasová, T.; Pekař, M. Effect of CTAB and CTAB in the presence of hyaluronan on selected human cell types. Colloids Surf. A Physicochem. Eng. Asp. 2014, 460, 204–208. [Google Scholar] [CrossRef]
- Nabi, A.; Tasneem, S.; Jesudason, C.G.; Lee, V.S.; Zain, S.B.M. Study of interaction between cationic surfactant (CTAB) and paracetamol by electrical conductivity, tensiometric and spectroscopic methods. J. Mol. Liq. 2018, 256, 100–107. [Google Scholar] [CrossRef]
- Silva, A.M.; Martins-Gomes, C.; Coutinho, T.E.; Fangueiro, J.F.; Sanchez-Lopez, E.; Pashirova, T.N.; Andreani, T.; Souto, E.B. Soft cationic nanoparticles for drug delivery: Production and cytotoxicity of solid lipid nanoparticles (SLNs). Appl. Sci. 2019, 9, 4438. [Google Scholar] [CrossRef]
- Elansezhian, R.; Ramamoorthy, B.; Nair, P.K. The influence of SDS and CTAB surfactants on the surface morphology and surface topography of electroless Ni–P deposits. J. Mater. Process. Technol. 2009, 209, 233–240. [Google Scholar] [CrossRef]
- Oremusová, J.; Vitková, Z.; Vitko, A.; Tárník, M.; Miklovičová, E.; Ivánková, O.; Murgaš, J.; Krchňák, D. Effect of Molecular Composition of Head Group and Temperature on Micellar Properties of Ionic Surfactants with C12 Alkyl Chain. Molecules 2019, 24, 651. [Google Scholar] [CrossRef]
- Liu, Q.; Liu, S.; Luo, D.; Peng, B. Ultra-Low Interfacial Tension Foam System for Enhanced Oil Recovery. Appl. Sci. 2019, 9, 2155. [Google Scholar] [CrossRef]
- Dukovski, B.J.; Bračko, A.; Šare, M.; Pepić, I.; Lovrić, J. In vitro evaluation of stearylamine cationic nanoemulsions for improved ocular drug delivery. Acta Pharm. (Zagrebcroatia) 2019, 69, 621–634. [Google Scholar] [CrossRef]
- Baig, M.S.; Owida, H.; Njoroge, W.; Yang, Y. Development and evaluation of cationic nanostructured lipid carriers for ophthalmic drug delivery of besifloxacin. J. Drug Deliv. Sci. Technol. 2020, 55, 101496. [Google Scholar] [CrossRef]
- Pignatello, R.; Leonardi, A.; Fuochi, V.; Petronio Petronio, G.; Greco, A.S.; Furneri, P.M. A method for efficient loading of ciprofloxacin hydrochloride in cationic solid lipid nanoparticles: Formulation and microbiological evaluation. Nanomaterials 2018, 8, 304. [Google Scholar] [CrossRef]
- Silva, A.M.; Martins-Gomes, C.; Fangueiro, J.F.; Andreani, T.; Souto, E.B. Comparison of antiproliferative effect of epigallocatechin gallate when loaded into cationic solid lipid nanoparticles against different cell lines. Pharm. Dev. Technol. 2019, 24, 1243–1249. [Google Scholar] [CrossRef] [PubMed]
- Botto, C.; Mauro, N.; Amore, E.; Martorana, E.; Giammona, G.; Bondi, M.L. Surfactant effect on the physicochemical characteristics of cationic solid lipid nanoparticles. Int. J. Pharm. 2017, 516, 334–341. [Google Scholar] [CrossRef] [PubMed]
- Quinteros, D.A.; Ferreira, L.M.; Schaffazick, S.R.; Palma, S.D.; Allemandi, D.A.; Cruz, L. Novel polymeric nanoparticles intended for ophthalmic administration of acetazolamide. J. Pharm. Sci. 2016, 105, 3183–3190. [Google Scholar] [CrossRef]
- Liu, D.; Lian, Y.; Fang, Q.; Liu, L.; Zhang, J.; Li, J. Hyaluronic-acid-modified lipid-polymer hybrid nanoparticles as an efficient ocular delivery platform for moxifloxacin hydrochloride. Int. J. Biol. Macromol. 2018, 116, 1026–1036. [Google Scholar] [CrossRef]
- Balzus, B.; Sahle, F.F.; Hönzke, S.; Gerecke, C.; Schumacher, F.; Hedtrich, S.; Kleuser, B.; Bodmeier, R. Formulation and ex vivo evaluation of polymeric nanoparticles for controlled delivery of corticosteroids to the skin and the corneal epithelium. Eur. J. Pharm. Biopharm. 2017, 115, 122–130. [Google Scholar] [CrossRef]
- Gonzalez-Pizarro, R.; Silva-Abreu, M.; Calpena, A.C.; Egea, M.A.; Espina, M.; García, M.L. Development of fluorometholone-loaded PLGA nanoparticles for treatment of inflammatory disorders of anterior and posterior segments of the eye. Int. J. Pharm. 2018, 547, 338–346. [Google Scholar] [CrossRef]
- Trinh, T.X.; Choi, J.S.; Jeon, H.; Byun, H.G.; Yoon, T.H.; Kim, J. Quasi-SMILES-Based Nano-Quantitative Structure-Activity Relationship Model to Predict the Cytotoxicity of Multiwalled Carbon Nanotubes to Human Lung Cells. Chem. Res. Toxicol. 2018, 31, 183–190. [Google Scholar] [CrossRef]
- Tahara, K.; Karasawa, K.; Onodera, R.; Takeuchi, H. Feasibility of drug delivery to the eye’s posterior segment by topical instillation of PLGA nanoparticles. Asian J. Pharm. Sci. 2017, 12, 394–399. [Google Scholar] [CrossRef]
- Ramos, G.Y.; García, M.L.; Espina, M.G.; Parra, A.C.; Calpena, A.C. Influence of freeze-drying and γ-irradiation in preclinical studies of flurbiprofen polymeric nanoparticles for ocular delivery using d-(+)-trehalose and polyethylene glycol. Int. J. Nanomed. 2016, 11, 4093–4106. [Google Scholar] [CrossRef] [PubMed]
- Lütfi, G.; Müzeyyen, D. Preparation and characterization of polymeric and lipid nanoparticles of pilocarpine HCl for ocular application. Pharm. Dev. Technol. 2013, 18, 701–709. [Google Scholar] [CrossRef] [PubMed]
- Dillen, K.; Vandervoort, J.; Van den Mooter, G.; Ludwig, A. Evaluation of ciprofloxacin-loaded Eudragit RS100 or RL100/PLGA nanoparticles. Int. J. Pharm. 2006, 314, 72–82. [Google Scholar] [CrossRef]
- Duxfield, L.; Sultana, R.; Wang, R.; Englebretsen, V.; Deo, S.; Swift, S.; Rupenthal, I.; Al-Kassas, R. Development of gatifloxacin-loaded cationic polymeric nanoparticles for ocular drug delivery. Pharm. Dev. Technol. 2016, 21, 172–179. [Google Scholar] [CrossRef] [PubMed]
- Fabiano, A.; Piras, A.M.; Guazzelli, L.; Storti, B.; Bizzarri, R.; Zambito, Y. Impact of Different Mucoadhesive Polymeric Nanoparticles Loaded in Thermosensitive Hydrogels on Transcorneal Administration of 5-Fluorouracil. Pharmaceutics 2019, 11, 623. [Google Scholar] [CrossRef] [PubMed]
- Yousry, C.; Elkheshen, S.A.; El-Laithy, H.M.; Essam, T.; Fahmy, R.H. Studying the influence of formulation and process variables on Vancomycin-loaded polymeric nanoparticles as potential carrier for enhanced ophthalmic delivery. Eur. J. Pharm. Sci. 2017, 100, 142–154. [Google Scholar] [CrossRef]
- Mora-Huertas, C.E.; Fessi, H.; Elaissari, A. Polymer-based nanocapsules for drug delivery. Int. J. Pharm. 2010, 385, 113–142. [Google Scholar] [CrossRef]
- Araujo, J.; Vega, E.; Lopes, C.; Egea, M.A.; Garcia, M.L.; Souto, E.B. Effect of polymer viscosity on physicochemical properties and ocular tolerance of FB-loaded PLGA nanospheres. Colloids Surf. B Biointerfaces 2009, 72, 48–56. [Google Scholar] [CrossRef]
- Canadas, C.; Alvarado, H.; Calpena, A.C.; Silva, A.M.; Souto, E.B.; Garcia, M.L.; Abrego, G. In vitro, ex vivo and in vivo characterization of PLGA nanoparticles loading pranoprofen for ocular administration. Int. J. Pharm. 2016, 511, 719–727. [Google Scholar] [CrossRef]
- Sanchez-Lopez, E.; Egea, M.A.; Cano, A.; Espina, M.; Calpena, A.C.; Ettcheto, M.; Camins, A.; Souto, E.B.; Silva, A.M.; Garcia, M.L. PEGylated PLGA nanospheres optimized by design of experiments for ocular administration of dexibuprofen-in vitro, ex vivo and in vivo characterization. Colloids Surf. B Biointerfaces 2016, 145, 241–250. [Google Scholar] [CrossRef]
- Croisfelt, F.M.; Tundisi, L.L.; Ataide, J.A.; Silveira, E.; Tambourgi, E.B.; Jozala, A.F.; Souto, E.M.B.; Mazzola, P.G. Modified-release topical hydrogels: A ten-year review. J. Mater. Sci. 2019, 54, 10963–10983. [Google Scholar] [CrossRef]
- Gratieri, T.; Gelfuso, G.M.; Rocha, E.M.; Sarmento, V.H.; de Freitas, O.; Lopez, R.F.V. A poloxamer/chitosan in situ forming gel with prolonged retention time for ocular delivery. Eur. J. Pharm. Biopharm. 2010, 75, 186–193. [Google Scholar] [CrossRef]
- Bhowmik, M.; Kumari, P.; Sarkar, G.; Bain, M.K.; Bhowmick, B.; Mollick, M.M.; Mondal, D.; Maity, D.; Rana, D.; Bhattacharjee, D.; et al. Effect of xanthan gum and guar gum on in situ gelling ophthalmic drug delivery system based on poloxamer-407. Int. J. Biol. Macromol. 2013, 62, 117–123. [Google Scholar] [CrossRef] [PubMed]
- Nagarwal, R.C.; Kant, S.; Singh, P.N.; Maiti, P.; Pandit, J.K. Polymeric nanoparticulate system: A potential approach for ocular drug delivery. J. Control. Release 2009, 136, 2–13. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, M.D.C.; Santini, A.; Souto, E.B. Chapter 8—Delivery of Antimicrobials by Chitosan-Composed Therapeutic Nanostructures. In Nanostructures for Antimicrobial Therapy; Chapter 8; Anton, F., Alexandru, G., Eds.; Elsevier: Amsterdam, The Netherlands, 2017; pp. 203–222. [Google Scholar] [CrossRef]
- Ogunjimi, A.T.; Melo, S.M.G.; Vargas-Rechia, C.G.; Emery, F.S.; Lopez, R.F.V. Hydrophilic polymeric nanoparticles prepared from Delonix galactomannan with low cytotoxicity for ocular drug delivery. Carbohydr. Polym. 2017, 157, 1065–1075. [Google Scholar] [CrossRef]
- Nicoli, S.; Ferrari, G.; Quarta, M.; Macaluso, C.; Govoni, P.; Dallatana, D.; Santi, P. Porcine sclera as a model of human sclera for in vitro transport experiments: Histology, SEM, and comparative permeability. Mol. Vis. 2009, 15, 259–266. [Google Scholar]
- Yang, X.Z.; Dou, S.; Wang, Y.C.; Long, H.Y.; Xiong, M.H.; Mao, C.Q.; Yao, Y.D.; Wang, J. Single-step assembly of cationic lipid-polymer hybrid nanoparticles for systemic delivery of siRNA. ACS Nano 2012, 6, 4955–4965. [Google Scholar] [CrossRef]
- Carbone, C.; Manno, D.; Serra, A.; Musumeci, T.; Pepe, V.; Tisserand, C.; Puglisi, G. Innovative hybrid vs. polymeric nanocapsules: The influence of the cationic lipid coating on the “4S”. Colloids Surf. B Biointerfaces 2016, 141, 450–457. [Google Scholar] [CrossRef]
- Basaran, E. Ocular Application of Dirithromycin Incorporated Polymeric Nanoparticles: An in Vitro Evaluation/Diritromisin Yuklu Polimerik Nanopartikullerin Okuler Uygulanmasi: In Vitro Degerlendirme. Turk. J. Pharm. Sci. 2017, 14, 191–201. [Google Scholar] [CrossRef]
- Gonzalez-Pizarro, R.; Carvajal-Vidal, P.; Bellowa, L.H.; Calpena, A.C.; Espina, M.; García, M.L. In-situ forming gels containing fluorometholone-loaded polymeric nanoparticles for ocular inflammatory conditions. Colloids Surf. B Biointerfaces 2019, 175, 365–374. [Google Scholar] [CrossRef]
- Zhou, Y.; Fang, A.; Wang, F.; Li, H.; Jin, Q.; Huang, L.; Fu, C.; Zeng, J.; Jin, Z.; Song, X. Core-shell lipid-polymer nanoparticles as a promising ocular drug delivery system to treat glaucoma. Chin. Chem. Lett. 2020, 31, 494–500. [Google Scholar] [CrossRef]
- Salama, A.H.; Mahmoud, A.A.; Kamel, R. A novel method for preparing surface-modified fluocinolone acetonide loaded PLGA nanoparticles for ocular use: In vitro and in vivo evaluations. AAPS PharmSciTech 2016, 17, 1159–1172. [Google Scholar] [CrossRef] [PubMed]
- Yurtdas-Kirimlioglu, G.; Sinan, Ö.; Büyükköroğlu, G.; Yazan, Y. Formulation and in vitro evaluation of moxifloxacin hydrochloride-loaded polymeric nanoparticles for ocular application. Lat. Am. J. Pharm. 2018, 37, 1850–1862. [Google Scholar]
- Mittal, N.; Kaur, G. Investigations on polymeric nanoparticles for ocular delivery. Adv. Polym. Technol. 2019, 2019, 1316249. [Google Scholar] [CrossRef]
| Encapsulated Drug | Lipid System Composition | Average Particle Size (nm) | Polydispersity Index | Zeta Potential (mV) | References |
|---|---|---|---|---|---|
| Brimonidine | NLC: Glyceryl monostearate, castor oil, and Poloxamer® 188 | 152.0 | 0.230 | −44.20 | [79] |
| Curcumin | NLC: Compritol® ATO 888, Gelucire® 50/13, olive oil, and Poloxamer® 188 | 66.8 | 0.170 | NA | [80] |
| Etoposide | SLN: Gelucire 44/14, Compritol® ATO 888, and Tween® 80 | 239.4 | 0.261 | NA | [14] |
| Flurbiprofen | NLC: stearic acid, castor oil, and Tween® 80 | 288.0 | 0.245 | −29.00 | [53] |
| Isoniazid | SLN: Compritol® ATO 888, stearic acid, Tween® 80, and soy lecithin | 149.2 | 0.150 | −0.35 | [81] |
| Natamycin | SLN: Precirol® ATO 5 and Pluronic® F68 | 84.0 | 0.224 | 26.70 | [82] |
| Propranolol | NLC: Compritol® ATO 888, oleic acid, Tween® 80, Span® 80, and Transcutol P | 385.0 to 880.0 | 0.220 to 0.560 | NA | [83] |
| Quercetin | NLC: Compritol® ATO 888, medium-chaintriglyceride, Cremophor EL, and soy lecithin | 75.5 | 0.180 | NA | [84] |
| Sunitinib | SLN: Stearic acid, sodium taurodeoxycholate, and phosphatidylcholine | 140.0 | 0.200 | NA | [85] |
| Triamcinolone acetonide | SLN: Glyceryl monostearate, Compritol® ATO 888, Tween® 80, and Pluronic® F68 | 200.0 to 350.0 | 0.300 to 0.450 | −52.31 to −64.35 | [86] |
| Voriconazole | SLN: Witepsol® W35, Compritol® ATO 888, stearic acid, Tween® 80, and l-α-phosphatidylcholine | 182.0 | 0.269 | NA | [87] |
| Encapsulated Drug | Cationic Lipid Nanoparticles | Average Particle Size (nm) | Polydispersity Index | Zeta Potential (mV) | References |
|---|---|---|---|---|---|
| Epigallocatechin gallate | Solid lipid nanoparticles (SLN): Ascorbic acid, Poloxamer 188, Softisan® S75, CTAB (cetyl trimethylammonium bromide), DDAB (dimethyl dioctadecyl ammonium bromide) | 149.0 and 143.0 | 0.240 and 0.160 | 20.80 and 25.70 | [67] |
| Palmatine | Lipid emulsion: Egg lecithin, oleic acid, α- tocopherol, soybean oil, DOTAP (1,2-dioleoyl-3-trimethylammonium-propane) | 192.4 | 0.281 | 45.00 | [88] |
| NA | Nanoemulsion: Stearylamine, sesame oil, soybean oil, castor oil, Cremophor®EL, Tween 60, Tween 80, glycerol, Pluronic® F68 | 81.0 to 96.0 | 0.110 to 0.251 | −2.00 to 27.00 | [104] |
| Curcumin | Nanostructured lipid carriers (NLC): Glycerinmonostearate, Tween 80, stearic acid, tristearin, Comritol® 888 ATO, Miglyol® 812 | 158.1 | 0.290 | 36.50 | [93] |
| Besifloxacin hydrochloride | Nanostructured lipid carriers (NLC): Compritol 888 ATO, Gelucire 50/13, Labrafac PG, CTAB (cetyl trimethylammonium bromide) | 173.6 | 0.188 | 16.60 | [105] |
| NA | Solid lipid nanoparticles (SLN): Glycerol, Softisan S100, Lipoid S75, soybean phosphatidylcholine | 134.0 and 135.0 | 0.179 and 0.196 | 28.20 | [100] |
| Ciprofloxacin hydrochloride | Solid lipid nanoparticles (SLN): Tween 80, Softisan 100, TEA (trimethylamine), DDAB (dimethyl dioctadecyl ammonium bromide) | 270.0 to 350.0 | 0.250 to 0.340 | −42.00 to 51.00 | [106] |
| NA | Solid lipid nanoparticles (SLN): Glycerol, Softisan S100, Lipoid S75, soybean phosphatidylcholine | 164.5 to 268.5 | 0.155 to 0.192 | −1.00 to −2.00 | [66] |
| Puearin and Scutellarin | Solid lipid nanoparticles (SLN): F-127, Gelucire® 44/14, Tween 80, cholesterol, quaternized carboxymethyl chitosan, lecithin | 181.0 | 0.224 | 23.80 | [95] |
| Epigallocatechin gallate | Solid lipid nanoparticles (SLN): Glycerol, Softisan S100, Lipoid S75, ascorbic acid, Poloxamer 188, DDAB (dimethyl dioctadecyl ammonium bromide) | 143.7 | 0.160 | 25.70 | [107] |
| NA | Solid lipid nanoparticles (SLN): Precirol ATO 5, Brij 76, CTAB (cetyl trimethylammonium bromide), DDAB (dimethyl dioctadecyl ammonium bromide) | 185.0 to 244.0 | 0.350 | 16.00 to 55.00 | [108] |
| Triamcinolone acetonide | Nanostructured lipid carriers (NLC): Transcutol® P, Capmul MCM C10 (Glycerylmonocaprate), Captex 200 P, lecithin, Tween 80, stearylamine, ethanol | 199.0 | 0.326 | 35.80 | [91] |
| Encapsulated Drug | Polymeric Nanoparticle Composition | Average Particle Size (nm) | Polydispersity Index | Zeta Potential (mV) | References |
|---|---|---|---|---|---|
| Acetazolamide | Nanocapsule suspensions: Ethyl cellulose, Eudragit® RS100, Tween 80, Span 60, medium-chain triglycerides | 106.0 to 229.0 | 0.076 to 0.195 | −16.20 to 17.30 | [109] |
| Dirithromycin | Nanoparticles: Kollidon® SR, methanol | 329.6 and 522.2 | 0.425 and 0.539 | −19.50 and −25.50 | [134] |
| Fluorometholone | Nanoparticles: Polylactic-co-glycolic acid (PLGA), Poloxamer 188, acetone | 150.8 | 0.082 | −27.90 | [135] |
| Gatifloxacin | Nanoparticles: Eudragit® RL and RS, acetone, Tween- 80 | 68.0 and 410.0 | 0.408 and 0.280 | 24.45 and 33.30 | [118] |
| Moxifloxacin | Hyaluronic-acid-modified lipid–polymer hybrid nanoparticles (HA-LCS-NPs): Carbodiimide hydrochloride, N-hydroxysuccinimide, DPPE (dipalmitoyl phosphatidylethanolamine), hyaluronic acid | 214.0 | 0.394 | −16.59 | [110] |
| Melatonin | Aqueous core nanocapsules: Polyactic acid, Tween 80, Span 80, Brij® 98, caprylic/capric triglyceride, CTAB (cetyl trimethyl ammonium bromide), DDAB (dimethyl dioctadecyl ammonium bromide) | 193.0 to 218.0 | 0.16 to 0.22 | −36.1 to 31.4 | [133] |
| Brinzolamide | Nanoparticles: Poly(lactic-co-glycolic) acid (PLGA), acetone, polyvinyl alcohol, soybean phosphatidylcholine, cholesterol | 151.0 | NA | −7.53 | [136] |
| Delonix galacto mannan | Nanoparticles: Delonix polymer, sodium hydroxide, Tween 80, Span 80, ethanol | 215.0 to 360.0 | 0.140 to 0.225 | −68.80 to −31.80 | [130] |
| Fluocinolone acetonide | Nanoparticles: PLGA, poloxamer, acetonitrile | 34.0 to 178.0 | 0.16 to 0.52 | −1.43 to 5.25 | [137] |
| Flurbiprofen | Nanoparticles: Poly ε-caprolactone, Poloxamer 188, acetone | 170.6 and 192.5 | 0.087 and 0.139 | −15.50 and −12.00 | [115] |
| Dexamethasone | Nanoparticles: Ethyl cellulose, Eudragit® RS, ethyl acetate, polyvinyl alcohol | 64.0 to 172.0 | 0.058 to 0.218 | −36.00 to 44.00 | [111] |
| 5-Fluorouracil | Nanoparticles: Sulfobutyl chitosan, polymer solution, 1,4-butane sulfone, phosphate buffer pH 7.4 | 294.3 to 390.6 | 0.2 to 0.4 | −3.50 to +9.50 | [119] |
| Vancomycin | Nanoparticles: Poly lactic-co-glycolic acid (PLGA), polycaprolactone, Span 80, acetonitrile, methylene dichloride, liquid paraffin | 155.0 to 8444.0 | 0.222 to 0.893 | −43.15 to 51.55 | [120] |
| Pilocarpine hydrochloride | Nanoparticles: Eudragit® RS100, Gelucire® 44/14, Tween 80, benzalkonium chloride, octadecylamine | 73.0 to 3179.0 | 0.29 to 1 | −2.97 to 85.00 | [116] |
| Moxifloxacin hydrochloride | Nanoparticles: Eudragit® RS100, methanol | 247.1 to 392.4 | 0.23 to 0.68 | 53.90 to 80.40 | [138] |
| Timolol maleate | Nanoparticles: Flax seed gum, acetic acid | 254.5 | 0.345 | −20.30 | [139] |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Baldim, I.; Oliveira, W.P.; Kadian, V.; Rao, R.; Yadav, N.; Mahant, S.; Lucarini, M.; Durazzo, A.; Da Ana, R.; Capasso, R.; et al. Natural Ergot Alkaloids in Ocular Pharmacotherapy: Known Molecules for Novel Nanoparticle-Based Delivery Systems. Biomolecules 2020, 10, 980. https://doi.org/10.3390/biom10070980
Baldim I, Oliveira WP, Kadian V, Rao R, Yadav N, Mahant S, Lucarini M, Durazzo A, Da Ana R, Capasso R, et al. Natural Ergot Alkaloids in Ocular Pharmacotherapy: Known Molecules for Novel Nanoparticle-Based Delivery Systems. Biomolecules. 2020; 10(7):980. https://doi.org/10.3390/biom10070980
Chicago/Turabian StyleBaldim, Iara, Wanderley P. Oliveira, Varsha Kadian, Rekha Rao, Nitesh Yadav, Sheefali Mahant, Massimo Lucarini, Alessandra Durazzo, Raquel Da Ana, Raffaele Capasso, and et al. 2020. "Natural Ergot Alkaloids in Ocular Pharmacotherapy: Known Molecules for Novel Nanoparticle-Based Delivery Systems" Biomolecules 10, no. 7: 980. https://doi.org/10.3390/biom10070980
APA StyleBaldim, I., Oliveira, W. P., Kadian, V., Rao, R., Yadav, N., Mahant, S., Lucarini, M., Durazzo, A., Da Ana, R., Capasso, R., Souto, S. B., Santini, A., & Souto, E. B. (2020). Natural Ergot Alkaloids in Ocular Pharmacotherapy: Known Molecules for Novel Nanoparticle-Based Delivery Systems. Biomolecules, 10(7), 980. https://doi.org/10.3390/biom10070980










